3
Emerging Insights (Ecological)
FACTORS INFLUENCING THE 50+: CHALLENGES IN MEETING DIETARY NEEDS
Julie Locher, Professor in the Departments of Medicine and Health Care Organization and Policy at the University of Alabama at Birmingham (UAB), opened her talk by showing several models that can be used to understand the dimensions of food security, the stages of nutritional risk, and the multiplicity of influences and factors at various levels that affect the food choices and behaviors of older adults. The World Health Organization (WHO) model includes food availability, food access, and food use as “Pillars of Food Security” (FAO, 2006; WHO, 2016). Another model is an approach for identifying nutritional risk, and ultimately, various types of malnutrition. The ecological model shows all the societal and individual levels in which an individual exists: individual, interpersonal, institutional, community, and public policy (McLeroy et al., 1988) (see Figure 3-1). Finally, there is the multidimensional model (Locher et al., 2008, 2009) (see Figure 3-2).
Locher noted that one of the limitations of the final model, and indeed, much of the work that has been done in the area of nutrition and aging, is that it is based on individual self-report of dietary intake. The other thing she explained about the model is that it assumes that the relationships between eating behaviors and health outcomes operate in the direction shown in the model. In fact, however, these relationships are not so straightforward, and the effects could go in the opposite direction.
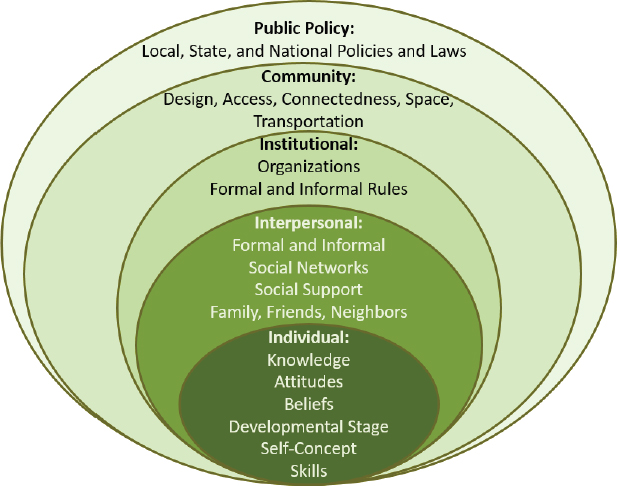
SOURCES: Presented by Julie Locher on October 28, 2015 (McLeroy et al., 1988).
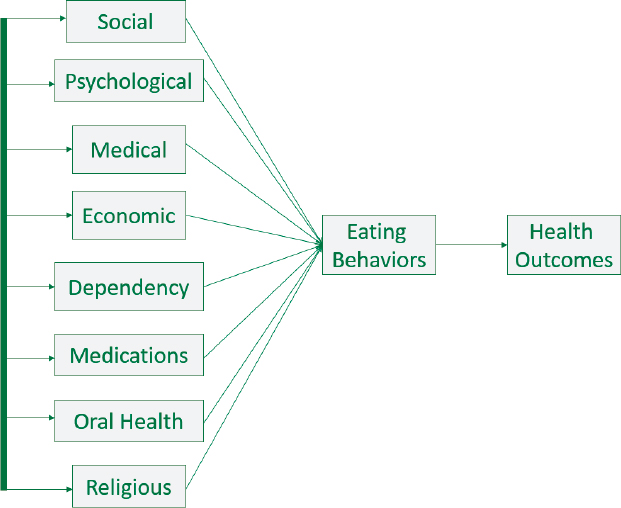
SOURCES: Presented by Julie Locher on October 28, 2015 (Locher et al., 2008, 2009).
The Concept of Food Choice
Locher continued by defining the concept of food choices, as actions that involve making a food-related decision when faced with two or more options. Food choices can be made at the global, societal, community, institutional, organizational, or individual level. Food choices made at the individual level are influenced by decisions that are made at all of the other levels. In addition, food behaviors happen as a sequence (Sobal and Bisogni, 2009) (see Figure 3-3).
Locher noted that her research often involves lengthy data collection instruments and, as an ice breaker, she often asks people what their favorite foods are. The foods that people prefer to eat are those that are based on people’s early experiences and are specific to what they ate in their household and specific to their region (Yang et al., 2013). Locher described factors influencing food choices at various levels (see Box 3-1).
Locher then asked a fundamental question: Why does food choice even matter? She explained that the choices people make have consequences, such as over-consumption and obesity. Efforts designed to change some aspect of food choice must be cognizant of how individuals make those decisions. For example, research is starting to show that “choices” have less to do with individual “free will” and more to do with other factors, many of which are social, political, and environmental. Referring to work done by Brian Wansink and colleague, Locher stated that it is estimated that people make 221 decisions per day about eating (Wansink and Sobal,
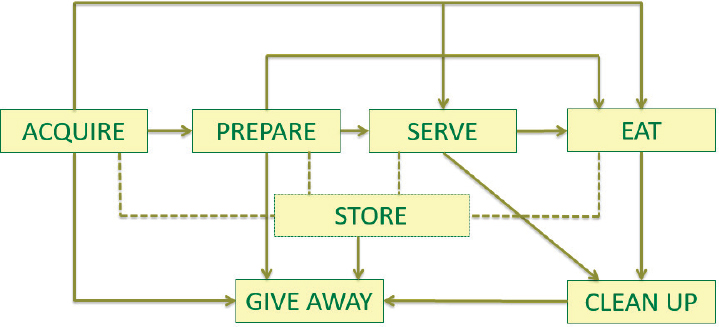
SOURCES: Presented by Julie Locher on October 28, 2015 (Sobal and Bisogni, 2009; reprinted with permission).
2007). More than 200 of these are made without conscious deliberation. Individuals’ capacity to make rational decisions about food are constrained by the information available to them, any cognitive processing limitations they may have, and the time they have for decision making. Their choices are made based upon environmental cues, social expectations, distractions, and other people they are with. Locher concluded her presentation by noting that insights from behavioral economics may be very useful in designing intervention studies in nutrition and aging.
FOOD SECURITY AMONG OLDER ADULTS
Craig Gundersen, Soybean Industry Endowed Professor in Agricultural Strategy in the Department of Agricultural and Consumer Economics at the University of Illinois, opened his presentation with the official definition
of food insecurity used in the United States. He noted that a household is placed into food security categories based on responses to 18 items on the U.S. Department of Agriculture’s (USDA’s) Core Food Security Module (CFSM).1 These items include “I worried whether our food would run out before we got money to buy more,” “Did you or the other adults in your household ever cut the size of your meals or skip meals because there wasn’t enough money for food,” “Were you ever hungry but did not eat because you couldn’t afford enough food,” “In the last 12 months did you or other adults in your household ever not eat for a whole day because there wasn’t enough money for food?”
Since 2008, James Ziliak and Gundersen have issued an annual report on the extent of food insecurity among seniors in the United States (Ziliak and Gundersen, 2009, 2012, 2013, 2014, 2015; Ziliak et al., 2008). Based on trends uncovered in those reports, Gundersen reported that food insecurity rates have remained very high among seniors, rising from about 5 million older adults in 2001 up to almost 10 million in 2013. However, these overall numbers hide considerable variation across the United States. For example, North Dakota had the lowest rate, with about 2 to 3 percent of older adults being food insecure, whereas in Arkansas, more than 26 percent of older adults are food insecure.
Factors That Increase the Risk of Food Insecurity
Gundersen then went on to explain several factors that influence the probability of food insecurity. Although food insecurity occurs across the income spectrum, those who are at the lowest level of income have the highest rates of food insecurity. This is to be expected, but in fact, almost 30 percent of food insecure households have incomes above 20 percent of the poverty line. Gundersen stated that this needs to be considered when policies and interventions to address food insecurity are developed.
Gundersen also explained that in studies Ziliak and he have conducted, food insecurity is more likely among older adults living at or below the poverty line who do not have a high school degree, who are African American or Hispanic, who are divorced or separated, who are living in multigenerational households with a grandchild, and who are younger. Gundersen concluded that all of these factors should be recognized and considered in policy making.
___________________
1 Based on the number of affirmative responses to the CFSM, households are categorized as marginally food insecure (threat of hunger) (1 or more affirmative responses); food insecure (at risk of hunger) (3 or more affirmative responses); or very low food secure (facing hunger) (8 or more affirmative responses in households with children or 6 or more affirmative responses in households without children).
Gundersen went on to present findings about the effects of food insecurity on nutrient intakes and health outcomes of adults age 60 and older. Being food insecure reduces nutrient intakes across the board. In addition, compared to food secure older adults, those who are food insecure have higher rates of depression, congestive heart failure, heart attack, chest pain, and asthma. Gundersen also noted that they also have more limitations in activities of daily living and a lower probability of being in excellent health.
Addressing Food Insecurity
Given these findings, Gundersen asked, “What can we do?” He stated that one successful program that addresses food insecurity is the Supplemental Nutrition Assistance Program (SNAP), formerly known as the Food Stamp Program, and that data show that food insecurity rates are less among SNAP participants compared to eligible nonparticipants. Unlike other federal nutrition programs, SNAP is available across the entire age spectrum, and the eligibility criteria are lower for seniors. One reasonable action therefore, concluded Gundersen, is to encourage participation in SNAP among older adults. To do that, he noted that more knowledge is needed about why this group has lower participation rates than do other age groups. One factor may be that older adults living in multigenerational families may be caring for grandchildren for a large part of the month. However, they are not necessarily the primary caregiver and, therefore, cannot get SNAP benefits where levels are based on everyone in the household. If the benefits they do receive don’t recognize the presence of others in the household, the amount may not be sufficient. One way to address this, suggested Gundersen, would be to ensure household size is correctly characterized in multigenerational households. More broadly, increasing benefit levels for seniors, especially those at the lower levels of SNAP benefits, would be worth considering.
Gundersen then commented on the discussions over whether SNAP participants should have restrictions on what they can and cannot purchase. He noted that this approach would have multiple negative ramifications, including that it would greatly stigmatize SNAP participants. He continued, saying that restrictions would be especially demeaning for older adults if they meant that they were not allowed to purchase items for their grandchildren. Restrictions on SNAP purchases, Gundersen stated, would patronize older Americans, and people should consider this when having discussions over restrictions.
Another approach, suggested Gundersen, is to reach out to the socially isolated. Many older adults have disabilities and challenges with mobility issues. How can we help them? They, too, may need higher SNAP benefit
levels. More needs to be done, said Gundersen, to understand the challenges older adults face so that efforts to address food insecurity can be effective.
A third approach, Gundersen proposed, is to recognize the importance of informal food assistance programs, such as Feeding America®, food banks, and Meals on Wheels™. These programs are important for those whose SNAP benefits run out before the end of the month as well as for those who are ineligible for SNAP.
Potential Priorities for Future Research
Gundersen concluded his talk by outlining several research directions that could help inform programs and policies to address food insecurity among older adults:
- Why is there a negative age gradient (why are younger older adults more likely to be food insecure than older older adults)?
- How do the dynamics of multigenerational households influence food insecurity?
- How do chronic health conditions influence food insecurity and vice versa?
- How might allowing home-delivered meals to be purchased with SNAP benefits influence food insecurity rates?
SPECIAL CONSIDERATIONS FOR MEETING THE DIETARY NEEDS OF VULNERABLE GROUPS
Joseph Sharkey is a Professor in the Department of Health Promotion and Community Health Sciences and Founding Director of the Program for Research and Outreach-Engagement on Nutrition and Health Disparities Solutions at the Texas A&M School of Public Health. He began his presentation by defining vulnerable populations as including underrepresented groups, underserved communities, racial and ethnic minorities, immigrant groups, and refugees. He went on to explain that the focus of his work has been with marginalized, impoverished colonias (i.e., neighborhoods) along the border of Texas and Mexico, as well as more recently those in southern New Mexico and Arizona. Sharkey explained that these colonias are important because the national epidemic of chronic diseases is more pronounced along the border than in other areas of the country, that they have persistent food insecurity and hunger, and that they are geographically isolated with limited access to food and social services (Ogden et al., 2010; Sharkey et al., 2011, 2012). This population is hard to reach, underrepresented, and mistrustful of researchers. He emphasized that meeting
their dietary needs is challenging given this complex physical, social, and demographic environment.
Considering the Meaning of “Resources”
Sharkey then asked workshop participants to think about the concept of resources, with this backdrop in mind. A traditional approach to thinking about resources can include economic resources (e.g., employment, income sources, benefits), community resources (e.g., transportation systems, neighbors, access to and availability of different types of food stores and food places, access to and use of nutrition assistance programs), family and household resources (e.g., relatives, household composition, nature of food sharing within the family, adequacy of cooking and food storage facilities), and individual resources (e.g., knowledge, skills, individual capacity).
Sharkey suggested that this way of thinking about resources is not sufficient. Rather, resources should be understood as having an overlay of several contextual domains (Sharkey et al., 2013) (see Figure 3-4).
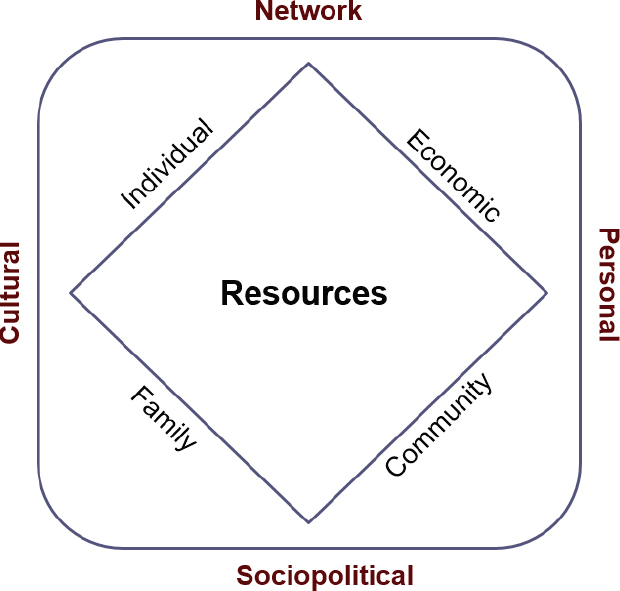
SOURCES: Presented by Joseph Sharkey on October 28, 2015 (Ashing-Giwa, 2005; Sharkey et al., 2013).
One overlay is the sociopolitical domain, which could include the community’s historical experience, mistrust, and fear. Another is the cultural context, which would include spirituality, language, means of communication, how people want to hear about information and how they share information, their attitudes, their resilience, the strategies people use to address issues in their lives, and whether concepts in one culture translate into another. A third overlay is the network context that includes family identity, especially extended family. Finally, the personal context overlay includes awareness, acceptance, and access. All of those contexts influence the use of available resources.
New Approaches for Addressing Food Insecurity
Sharkey then went on to explain that in the colonias in which he has worked, traditional approaches to meeting the dietary needs of vulnerable older adults have experienced only limited success. This could be due to using top-down and “one-size-fits-all” approaches to intervention planning, lack of consideration of community assets, strengths, or cultural wealth, lack of communication, or limited community collaboration.
Some groups and communities in South Texas and in other border areas have begun to change their approaches, stated Sharkey. These new ways of doing things have included engaging promotoras, who are community health workers. They are respected and trusted by the community, which allows them to help identify problems and solutions. They serve as cultural brokers and provide a link between program staff, academics, and the community. They serve as a sounding board and as a participant in determining whether the materials used and information provided is culturally responsive. They are able to mentor other promotoras. Sharkey concluded by saying that they provide invaluable observational insights and environmental knowledge and have been key to the work he has done in South Texas and Arizona.
Some of the projects Sharkey and his colleagues have conducted over the past several years include a survey of 140 seniors in two communities in South Texas to get the resident perspective, a household and resource survey of 548 people, and 14 focus groups of older adults to understand food access, food availability, and where help is needed most. Sharkey’s team followed these projects with a senior hunger survey of 578 respondents. That survey included a household food inventory and questions about household refrigeration and storage so that the researchers could learn not only whether the respondents had access to food but the resources to store it safely. About 77 percent of the seniors participating in the surveys had less than a seventh grade education. Ninety percent were born in Mexico, more than 92 percent spoke Spanish only, and 95 percent were below the
poverty level. Sharkey noted that an important factor is not the percentage of people living below the poverty level but the extent below the poverty line. More than 50 percent of the participants in these surveys had incomes less than 50 percent of the poverty level. In addition, Sharkey continued, food insecurity begins in childhood and continues through the lifespan but only about 54 percent and 12 percent participated in SNAP and in senior meal programs, respectively.
Sharkey explained that these findings helped identify a need to develop sustainable training and education activities to reduce the risk and presence of hunger using community collaborations that integrate place, services, and population health. The driving force was to improve not only knowledge, but skills in the context of where people live.
With the help of the AARP Foundation, Sharkey and his colleagues developed and pilot tested a program called No Más Hambre (No More Hunger). It targeted the context of the home in which older residents lived. In the short term, the program changed the knowledge, skills, and food sourcing for the community. It created greater awareness of food insecurity among older adults and increased the knowledge and skills of promotoras. Midterm outcomes included increased community linkages, increased capacity for both promotoras and community partners, and empowered older adults at risk of food insecurity.
Sharkey presented some conclusions:
- Older adults are key to identifying issues about food acquisition and food preparation knowledge and skills needed to reduce food insecurity and prevent hunger.
- Focus group discussions provide the venue for exploring individual experiences, sharing information, and determining potential community and individual-based strategies.
- Understanding contextual opportunities and barriers are key to increasing the knowledge and skills of older adults. Individuals and communities have assets, not just needs.
- Community prevention requires the engagement of traditional and nontraditional partners and empowerment of promotoras de salud is important.
He also suggested some priority topics for future research:
- Life span perspective
- Noncharity approaches
- Solutions that engage community residents
- Co-existing programs
- Community engagement
BUILT ENVIRONMENT: WHAT IS IT AND HOW IT INFLUENCES DIETS OF OLDER ADULTS
Irene Yen, an Associate Professor in the Departments of Medicine and Epidemiology and Biostatistics at the University of California, San Francisco, opened her presentation by noting that the built environment field has been expanding rapidly in the past 60 years and much of the recent research has focused on obesity. She explained that in this field, when people think about built environment, they mean the man-made, physical attributes of the surroundings, including structural conditions that affect walkability and recreation. The availability of health-promoting resources (food stores and playgrounds) and undesirable amenities (fast-food restaurants, liquor stores) also are considered (Gomez et al., 2015).
One aspect of the built environment relevant to nutrition and older adults is accessibility to food stores. The USDA has introduced the term “food desert,” which refers to a low-income census tract in which a large number of residents are more than a mile from a grocery store. The USDA has an Internet-based mapping tool that pinpoints the location of food deserts around the United States. Yen also noted that another key aspect of access to food sources is the ability to get to an existing store. Many parts of the United States do not have sidewalks. Even if the store is close by, accessibility will be diminished without the sidewalk (or pedestrian-friendly streets and crosswalks).
Built and Social Environments
Yen then noted that the social environment has become an active area of neighborhood-health research, complementing the work in the built environment. This work encompasses (1) the socioeconomic composition of the resident population, (2) social aspects of neighborhoods (e.g., crime, community support), (3) social capital (i.e., the collective value gained from social networks), and (4) social disorder (e.g., presence of trash, graffiti).
She then illustrated the relationship of built and social environments by describing a study conducted in early 2000 in which the authors found that respondents living in walkable neighborhoods were more likely to know and trust their neighbors and be socially engaged than those in non-walkable communities (Leyden, 2003). Yen explained that if the neighborhood is conducive to walking, residents might be more likely to be out and about and talking to their neighbors. She then described a study specific to older adults that was conducted in Miami’s Little Havana district (Brown et al., 2008). The investigators found that people who sat on their porches not only socialized with people walking by, but they also kept their eye out for neighborhood safety and crime.
Another way that social environment can be measured, continued Yen, is by looking at segregation measures through indices of similarity or ethnic enclave. Yen showed a map of the United States from the 2010 census showing the proportion of Black non-Hispanics all across the country (http://www.remappingdebate.org/mediapopup?content=node/547 [accessed May 6, 2016]). The map shows clearly how areas of the country differ by race composition.
Segregation, Neighborhood Poverty, and Diet
Yen then presented the results of research on racial and ethnic residential segregation, neighborhood poverty, and diet biomarkers to make the point that built and social environments have effects on food intakes and that improving social environments can have positive effects on the built environments and therefore on older adults’ access to healthy food (Yi et al., 2014). She also presented results of work showing the numbers of people living in affluent and low-income neighborhoods are both increasing over time, and this trend corresponds to a steady decline in the proportion of families living in middle-income neighborhoods, suggesting a widening inequality in income across neighborhoods (Bischoff and Reardon, 2013).
Yen ended her talk by reiterating the point made by other presenters that food insecurity and hunger are substantial problems among older adults, and that hunger, obesity, and related conditions are not mutually exclusive. She provided data showing that the prevalence of multiple chronic conditions increases dramatically as people age, with almost half of all people ages 45 to 64 having multiple chronic conditions, and more than 80 percent of those older than 65 having them (Gerteis et al., 2014). Yen concluded that it is difficult for older adults who are at risk of hunger, who live in difficult built and social environments, and who have limited income to achieve the healthy diet recommended for them.
ASSOCIATIONS BETWEEN MOBILITY AND NUTRITION
Richard Allman, Chief Consultant, Geriatrics and Extended Care, U.S. Department of Veterans Affairs (VA), began his presentation with studies he conducted while at the UAB. This research was supported by the National Institute on Aging (NIA) and the VA. He explained that he would describe the prevalence of low body mass index (BMI), high BMI, and nutritional risk factors among community-dwelling older adults, examine the cross-sectional associations between BMI and nutritional risk (unintentional weight loss and a nutritional risk index) with community mobility and provide prospective data on significant and independent associations between these measures with life-space mobility changes up to a 4-year
period of follow-up. Community life-space mobility is defined by the Life-Space Assessment, and was conceptualized as the distance, frequency, and independence of movement or travel that persons had in the 4 weeks before they were evaluated.
Allman stated that he and his colleagues conducted an observational study of aging in five Alabama counties between 1989 and 2009 (Allman et al., 2006). These counties have substantial proportions of African Americans. Participants were selected using a random sampling of Medicare beneficiaries living in these counties. The research team did extensive baseline in-home assessments between 1999 and 2001. The assessment included measures of health, life-space mobility, nutritional risk, and BMI. They also conducted telephone follow-ups every 6 months for up to 8 years to ascertain life-space mobility and mortality outcomes and a number of other measures.
Measuring Life Space Mobility
The primary outcome measure for the study was life-space mobility, as measured by the UAB Life Space Assessment (Baker et al., 2003). Allman’s team asked people about the extent to which they had moved about in their environment in the previous 4 weeks and whether or not they used any kind of assistive device or got help from another person when they moved or traveled. Using these data, the research team developed a scoring algorithm that correlated with observed physical performance measures. Subsequently, they found that this measure also predicted mortality and use of health care.
Allman showed a figure illustrating the average scores at different independent life-space levels2 (see Figure 3-5).
Mobility and Nutritional Risk
Allman’s team also was interested in seeing the associations of different levels of mobility and nutritional risk. Using the Nutrition Screening Initiative’s DETERMINE checklist, the nutritional risk assessment included questions about their appetite, the regularity of meals, frequency of alcoholic drinks, problems with teeth, mouth, or swallowing, difficulty paying for basics needs, the number of medications used, living alone, unexplained weight loss of 10 pounds or more, and difficulty eating, preparing meals, or shopping. The participants had a wide spectrum of social and economic
___________________
2 Independent life-space levels are levels that a person could achieve without help from another person or use of assistive equipment.
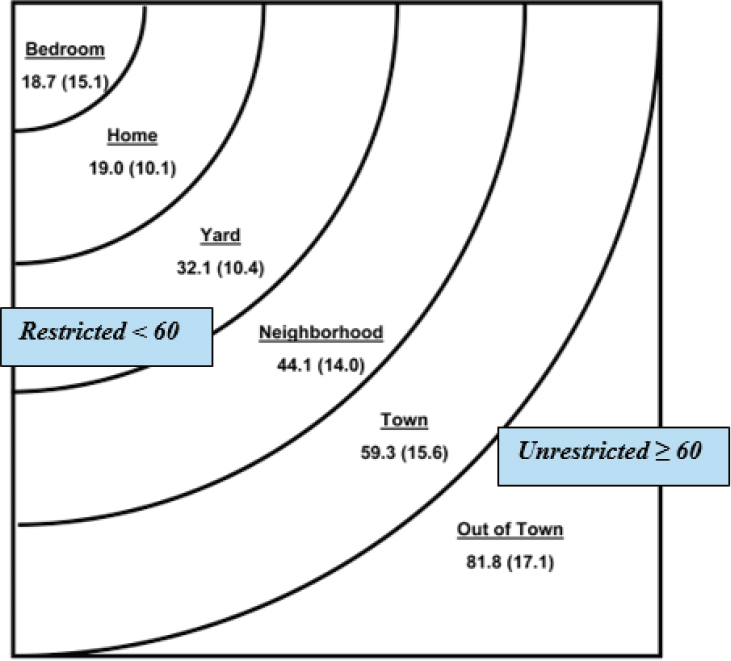
SOURCES: Presented by Richard Allman on October 28, 2015 (adapted from Bowling et al., 2014).
diversity within racial and ethnic groups and a high prevalence of chronic diseases (see Box 3-2).
In addition, 30 percent of the sample scored less than 24 on the Mini-Mental State Examination (MMSE), 16 percent had a score of 5 or greater on the Geriatric Depression Scale (indicating declines in cognitive abilities and increased depressive symptoms), and 20 percent had no physical activity.
Allman then showed the distribution of life-space scores.3 More than 40 percent had restricted community mobility generally limited to the neighborhood or less unless they had help from another person or used an assistive device. About 42 percent of those with BMI greater than or equal to 30 (Obese I) reported that they had gotten out of the room where they slept without help from another person or use of an assistive device in the prior month. In contrast, about 75 percent of persons with a BMI <30 had gotten out of town without any help.
His study found a correlation between BMI and Life-Space Mobility and a significant cross-sectional association between the composite Nutrition Risk Index (NRI) score and independent life-space mobility.
An additional analysis of composite life-space score change by BMI
___________________
3 The higher the score, the more likely it was that the person was driving his or her own vehicle, or independently using public transportation.
over 4 years showed that BMI levels were not associated with accelerated declines over time in the composite life-space score. However, those with BMI of less than 18.5 did have the lowest life-space scores at baseline, and those with more normal BMI (between 18.5 and 30) had higher baseline life-space scores. Additionally, unintentional weight loss was associated with lower baseline life-space and an accelerated decline in community mobility, independent of other factors. The overall conclusions from his work are in Box 3-3.
QUESTION AND ANSWER SESSION
The session discussion opened with a question for Sharkey about the low level of SNAP participation. He responded by saying that an important issue to understand is the length of time the benefits last. For about 40 percent of the SNAP participants in this population, the benefits last 1 week or less. To illustrate the realities of the lives of community members with whom he works, Sharkey then described one of the food insecure households in one of his studies. The mother in this household had two sons, ages 16 and 9. This woman was afraid that her older son could wind up in a gang and be a bad influence on her younger son. To solve this issue,
the mother told her son that he needed to come home after school right away every day and he agreed. However, the boy wanted to bring friends over with him. Sharkey followed up by saying, “Well, what do 16-year-old boys do? They eat.” This story brought to light the dilemma this woman faced: keeping her son safe and away from gangs but also having limited food resources within her home to make coming home more appealing to her son and his friends. Sharkey concluded this story by stating, “Those are the kinds of insights that we’ve got with a lot of the observations and all that we’ve done; you would not have ever even thought about asking on a survey.”
A follow-up question asked Sharkey to provide some ideas on how researchers and policy makers can work with the idea of “assets.” The participant asking this question noted that researchers often approach research with the idea that it is easier to find associations when looking for bad things. Sharkey responded that his team is much more “on the ground” and are thinking about how to adapt and tailor things to individuals and situations. The promotoras, Sharkey noted, are engaging people in conversation and are identifying strengths and barriers. For example, one strength is that people love to share information. As an example, Sharkey shared a current USDA project he and his colleagues are working on. He described this project as discussions with children ages 7 to 11, while the mothers participate in a type of board game that Sharkey and his assistants created. The board game simulates going through a grocery store, having to make decisions about what to buy. Sharkey explained that not only do the mothers like this board game, they also take copies of it and share them with their families and neighbors. The mothers are excited to find healthier ways to make recipes and report back to the researchers their successes in finding healthier alternatives to classic recipes.
Sharkey concluded by suggesting that the biggest assets are community, neighborhoods, and families and that researchers and policy makers have a responsibility to help the community have a better situation by building on their strengths.
To a question about how behavioral economics might affect food choices if preferences are established at such an early age, Locher replied that she was referring to multiple spaces, ranging from the home environment to the larger community environment as well as things that policymakers and industry do. For example, some of the work that Yen is doing in regard to the built environment shows how people can make very simple changes within their own home environment by having food located in certain places within their refrigerators or on their countertops. Locher stated that she thought that one of the most exciting things about the workshop was the inclusion of industry and things that industry can do in partnership with government. One option for making healthier decisions easier for peo-
ple might be to shift the focus from opting in to the program to opting out. “What if we made SNAP available to everyone who was eligible instead of having the burdensome process of having to apply?” Locher concluded.
A participant asked Gundersen for his thoughts on restrictions that SNAP imposes on certain types of foods and whether taxes on items such as sugar-sweetened beverages are a good idea. Gundersen replied that the restrictions are an example of how poor people are treated in ways that other people are never treated. People at other income levels are never told what groceries they can and cannot buy. He asked, “Why do we think it is appropriate to tell poor people what they can and cannot do when we try to give them a helping hand. It is patronizing and condescending. Let them make their own choices. Spending in low-income households is not very different from spending in higher-income households.” Gundersen pointed out that the main challenge low-income people face is they do not have enough money. With respect to taxes on certain food or beverage items, Gundersen emphasized that great care needs to be taken. He stated that evidence on soda taxes shows that they do not seem to have any impact on anything, but taxes have the greatest impact on poor people. Gundersen believes that these policies are another way to contribute to the debasement and marginalization of poor people. As a sociologist, Gundersen recognizes that people consume food for many reasons other than just physical nourishment, such as nourishment for the soul or as a way to express their cultural identity. Therefore, he said, this aspect also should be considered in setting policies and program requirements.
REFERENCES
Allman, R. M., P. Sawyer, and J. M. Roseman. 2006. The UAB Study of Aging: Background and prospects for insights into life-space mobility among older Americans in rural and urban settings. Aging Health 2(3):417-429.
Ashing-Giwa, K. T. 2005. Can a culturally responsive model for research design bring us closer to addressing participation disparities? Lessons learned from cancer survivorship studies. Ethnicity and Disease 15(1):130-137.
Baker, P. S., E. V. Bodner, R. M. Allman. 2003. Measuring life-space mobility in community-dwelling older adults. Journal of the American Geriatric Society 51(11):1610-1614.
Bischoff, K., and S. F. Reardon. 2013. Residential segregation by income, 1970-2009. Russell Sage Foundation. http://www.russellsage.org/blog/new-paper-residential-segregation-income-1970-2009 (accessed March 7, 2016).
Bowling, C. B., P. Muntner, P. Sawyer, P. W. Sanders, N. Kutner, R. Kennedy, and R. M. Allman. 2014. Community mobility among older adults with reduced kidney function: A study of life-space. American Journal of Kidney Diseases 63(3):429-436.
Brown, S. C., C. A. Mason, T. Perrino, J. L. Lombard, F. Martinez, E. Plater-Zyberk, A. R. Spokane, and J. Szapocznik. 2008. Built environment and physical functioning in Hispanic elders: The role of “eyes on the street.” Environmental Health Perspectives 116(10):1300-1307.
FAO (Food and Agriculture Organization). 2006. Policy brief: Food security.ftp://ftp.fao.org/es/ESA/policybriefs/pb_02.pdf (accessed February 11, 2016).
Gerteis, J., D. Izrael, D. Deitz, L. LeRoy, R. Ricciardi, T. Miller, and J. Basu. 2014. Multiple Chronic Conditions Chartbook. AHRQ Publications No. Q14-0038. Rockville, MD: Agency for Healthcare Research and Quality.
Gomez, S. L., S. Shariff-Marco, M. DeRouen, T. H. Keegan, I. H. Yen, M. Mujahid, W. A. Satariano, and S. L. Glaser. 2015. The impact of neighborhood social and built environment factors across the cancer continuum: Current research, methodological considerations, and future directions. Cancer 121(14):2314-2330.
Leyden, K. M. 2003. Social capital and the built environment: The importance of walkable neighborhoods. American Journal of Public Health 93(9):1546-1551.
Locher, J. L., C. S. Ritchie, C. O. Robinson, D. L. Roth, D. Smith West, and K. L. Burgio. 2008. A multidimensional approach to understanding under-eating in homebound older adults: The importance of social factors. Gerontologist 48(2):223-234.
Locher, J. L., C. S. Ritchie, D. L. Roth, B. Sen, K. S. Vickers, and L. I. Vailas. 2009. Food choice among homebound older adults: motivations and perceived barriers. The Journal of Nutritional Health and Aging 13(8):659-664.
McLeroy, K. R., D. Bibeau, A. Steckler, and K. Glanz. 1988. An ecological perspective on health promotion programs. Health Education Quarterly 15(4):351-377.
Ogden, C. L., M. D. Carroll, L. R. Curtin, M. M. Lamb, and K. M. Flegal. 2010. Prevalence of high body mass index in US children and adolescents, 2007-2008. JAMA 303(3):242-249.
Sharkey, J. R., W. R. Dean, and C. M. Johnson. 2011. Association of household and community characteristics with adult and child food insecurity among Mexican-origin households in colonias along the Texas-Mexico border. International Journal for Equity in Health 10:19.
Sharkey, J. R., C. Nalty, C. M. Johnson, and W. R. Dean. 2012. Children’s very low food security is associated with increased dietary intakes in energy, fat, and added sugar among Mexican-origin children (6-11 y) in Texas border colonias. BMC Pediatrics 12:16.
Sharkey, J. R., W. R. Dean, and C. C. Nalty. 2013. Child hunger and the protective effects of Supplemental Nutrition Assistance Program (SNAP) and alternative food sources among Mexican-origin families in Texas border colonias. BMC Pediatrics 13:143.
Sobal, J. and C. A. Bisogni. 2009. Constructing food choice decisions. Annals of Behavioral Medicine 38(Suppl 1):S37-S46.
Wansink, B. and J. Sobal. 2007. Mindless eating: The 200 daily food decisions we overlook. Environment and Behavior 39(1):106-123.
WHO (World Health Organization). 2016. Food security.http://www.who.int/trade/glossary/story028/en (accessed February 11, 2016).
Yang, Y., D. R. Buys, S. E. Judd, B. A. Gower, and J. L. Locher. 2013. Favorite foods of older adults living in the Black Belt Region of the United States. Influences of ethnicity, gender, and education. Appetite 63:18-23.
Yi, S.S., R. R. Ruff, M. Jung, and E. N. Waddell. 2014. Racial/ethnic residential segregation, neighborhood poverty and urinary biomarkers of diet in New York City adults. Social Science & Medicine 122:122-129.
Ziliak, J. P., and C. Gundersen. 2009. Senior hunger in the United States: Differences across states and rural and urban areas.http://www.nfesh.org/wp-content/uploads/2013/03/Senior+Hunger+in+the+United+States+2009.pdf (accessed May 23, 2016).
Ziliak, J. P., and C. Gundersen. 2012. The state of senior hunger in America 2010: An annual report.http://www.nfesh.org/wp-content/uploads/2013/03/2010-Senior-Hunger-Report.pdf (accessed May 23, 2016).
Ziliak, J. P., and C. Gundersen. 2013. The state of senior hunger in America 2011: An annual report.http://www.nfesh.org/wp-content/uploads/2013/03/State-of-Senior-Hunger-inAmerica-2011.pdf (accessed May 23, 2016).
Ziliak, J. P., and C. Gundersen. 2014. The state of senior hunger in America 2012: An annual report.http://www.nfesh.org/wp-content/uploads/2014/05/State-of-Senior-Hunger-inAmerica-2012.pdf (accessed May 23, 2016).
Ziliak, J. P., and C. Gundersen. 2015. The state of senior hunger in America 2013: An annual report.http://www.nfesh.org/wp-content/uploads/2015/04/State-of-Senior-Hunger-inAmerica-2013.pdf (accessed May 23, 2016).
Ziliak, J. P., C. Gundersen, and M. Haist. 2008. The causes, consequences, and future of senior hunger in America.http://www.mowaa.org/document.doc?id=13 (accessed May 23, 2016).




















