
Each year, more than 100,000 people in the United States need a kidney transplant. Less than 20 percent of them get one. On average, 13 people die each day waiting for a kidney. Often relatives and friends who are eager to donate are told their blood type or immune systems are incompatible. An unrelated volunteer donor could be a life-saver, but finding those donors can be a struggle; there’s no nationwide system to match patients and potential donors. Though this might sound like a medical problem, it’s actually exactly the kind of problem an economist can help solve through an innovative use of social science.
In the news, economists are often portrayed as number crunchers hidden away in universities. But they also journey out into the world, discovering problems and then charting a course to a solution. By applying economic theories to the shortage of kidneys, scientists have been able to save lives, cut medical costs, and reduce misery. Their innovations have spurred medical progress.
“Economics is about the real world,” said Alvin Roth, a Stanford University economist, when he won the Nobel Prize in 2012 for his work on matching markets, including the kidney donor matching problem. “We are interested in how people lead their lives.” The kidney donor dilemma is the perfect challenge for social scientists, because they are adept at studying complex systems, figuring out how they go wrong and how they can be improved.

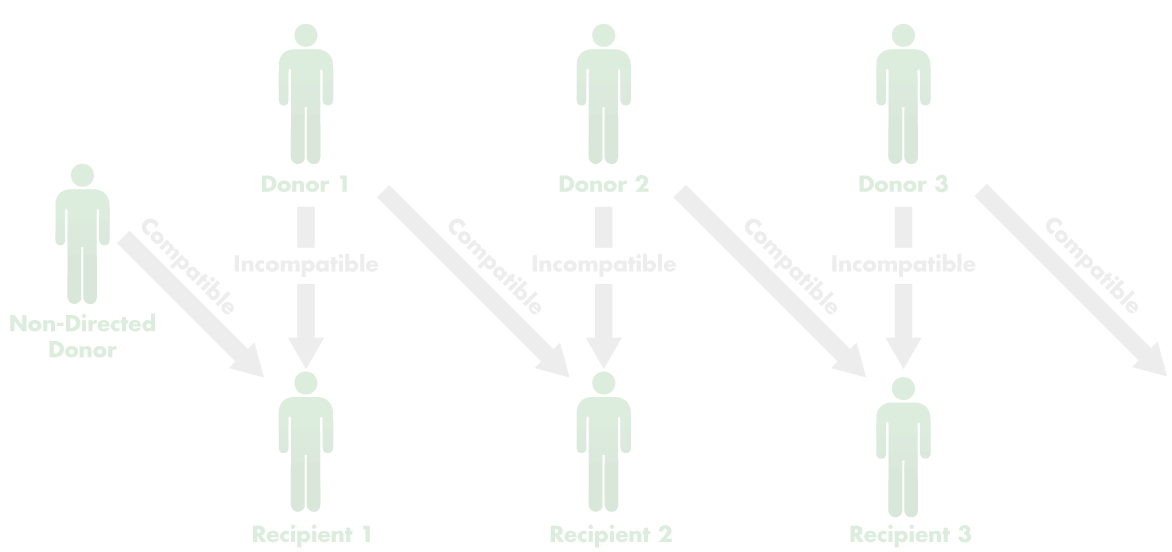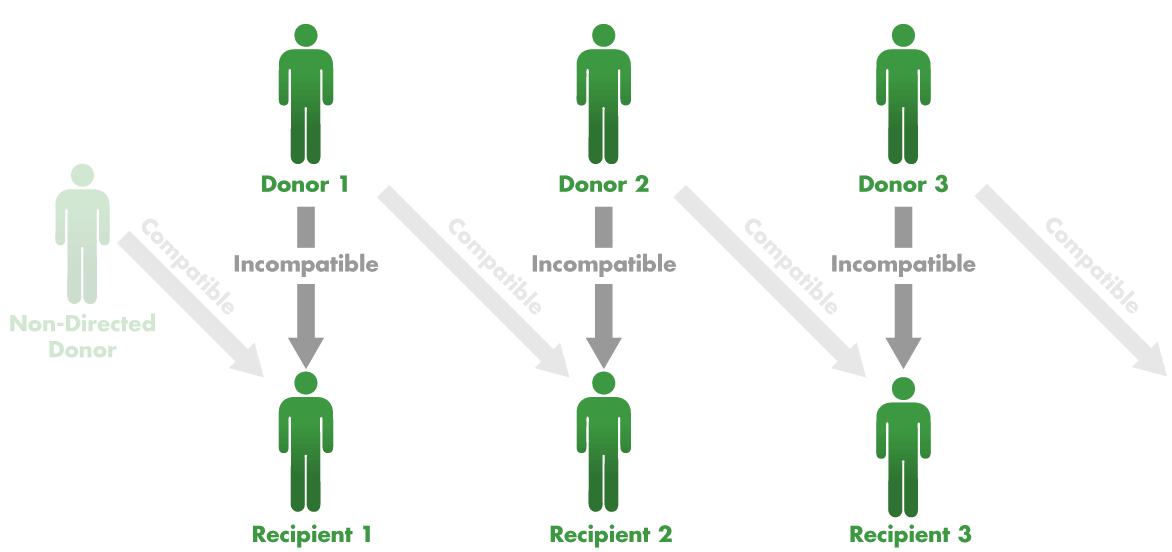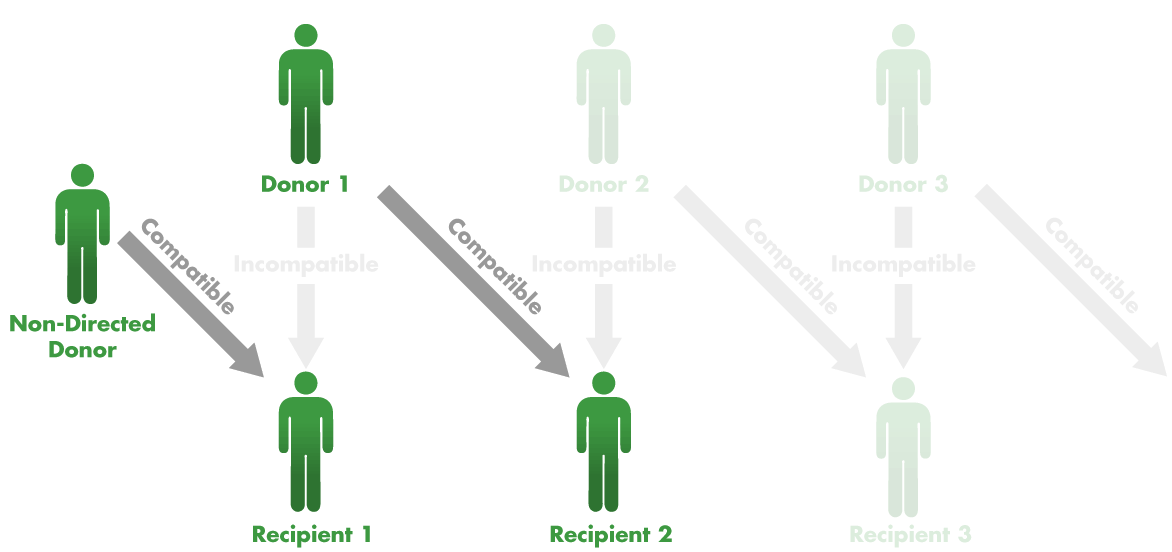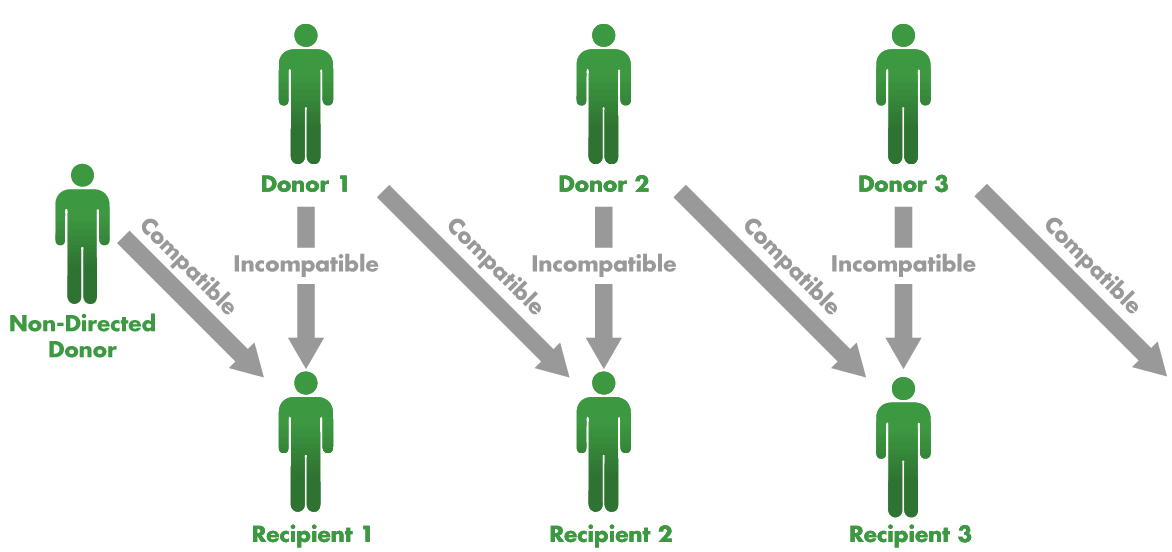
Someone in need of a kidney transplant has to find a donor with a compatible immune system so the donated kidney won’t be rejected. There aren’t enough organs from deceased donors, and finding a compatible living donor can be a long process. Often a patient has a friend or family member eager to donate, but that person is biologically incompatible. Transplant surgeons tried to overcome this problem by connecting two patients with incompatible donors so they could swap donors for compatible matches. But there still weren’t enough matchable pairs in local and regional transplant pools to make much of a dent in the backlog. That made sense to Roth. “To make a market work, it has to be thick,” Roth says. “You have to have a lot of people involved.”
In trying to chart a course through the kidney donor problem, Roth consulted the maps of scientific knowledge drawn by researchers on earlier journeys. One pertained to something called the “stable marriage problem.” For a marriage to be happy, both people need to feel that they found their best possible partner. Back in the 1960s, economist David Gale and mathematician Lloyd Shapley came up with an algorithm that matches people within a group based on individual preferences. The trick with their so-called deferred acceptance formula is that no matches are final until each person has the best possible match, given the preferences on both sides. Another landmark, called the “top trading cycle algorithm,” was added to the map in 1974 when economist Herbert Scarf and Shapley showed how a market can be designed to allow the trade of indivisible goods without using money.
This may sound purely theoretical, but these algorithms are great for solving real-world problems in markets where both sides have a voice, including employment, college roommate assignments, medical school residencies, and public school choice—“markets where prices don’t do all the work,” as Roth puts it.
In all these situations, which are called matching markets, everyone wants the best possible match, but the parties usually have very different goals and priorities. So it’s hard to devise a system that’s fair and doesn’t get bogged down while people ponder their choices. With kidney transplants, for instance, a patient might be unwilling to reveal details about her health because that information could be used to give her a kidney from an older or a sicker donor, even if a better one was available. For a matching market to work, people have to trust the process and feel safe revealing information that could potentially harm them. In the 1980s, Roth showed that deferred acceptance algorithms and top trading cycles make it safe for people to reveal their true wishes.
At first, Roth thought of the kidney donor problem as just an intellectual challenge; he used it as an example in a market design course he taught at Harvard in 2002. But he’s a practical-minded guy. He soon joined forces with Utku Unver, a former graduate student who is now an economic theorist at Boston College, and Tayfun Sonmez, a professor of economics, also at Boston College, who had used matching to allocate dormitory rooms efficiently. They set their sights on a new goal: a kidney exchange clearinghouse that would swiftly find the best possible match.
The first stop in that journey was to talk with doctors who did kidney transplants and ask them how the matching process went wrong. When Roth first contacted Dr. Michael Rees, a transplant surgeon at the University of Toledo, Rees dismissed him. “I didn’t know that economists did anything other than deal with money,” Rees says. “The only name of an economist I knew was Alan Greenspan. I couldn’t believe it when an economist said he could help me with kidney transplants.”
Roth persuaded Rees that he could help find a way by explaining that he had used economists’ understanding of matching markets to fix problems with another national system of keen interest to doctors: the one used for matching medical students with residency programs. The problem there was that the system didn’t account for social changes, like the increased number of two-doctor couples who wanted to live in the same town. The improved algorithm first matches doctors and residencies, then fixes any mismatches that affect couples.
That’s just what Roth and his colleagues did with their algorithm for the kidney market, writing formulas and testing them over and over with computer simulations to make sure the system was fair, reliable, and would not put patients or donors at risk. Soon transplant centers in New England and the Midwest were using the economists’ innovation, matching more patients and donors, and performing more kidney transplants. The improvements made transplants safer and saved millions of dollars in health care costs by getting people off dialysis. And it has saved lives.
But the system was still not working as well as it could. One problem was that transplant centers traditionally did surgery on a patient and donor at the same time. But operating on even two patient–donor pairs at once was logistically difficult, involving four simultaneous operations. Adding in more pairs to make better matches would challenge the staff and resources of most hospitals. On the other hand, if they added in just one more person, a donor who was willing to give a kidney to anyone, it would make it possible to do many more matches. Not only that, if pairs didn’t have to be matched with other pairs, a chain of transplants could be separated by weeks or months.
This approach to organ donation was new to Matt Jones of Petoskey, Michigan, who contacted Mike Rees about being a “non-directed” donor after he returned home from work early one day and glanced at the TV. “They were doing a news story about a guy from Pennsylvania who traveled to Colorado to donate a kidney,” Jones says. “I thought, that’s weird, I’ve always donated blood and I’m on the bone marrow registry, but I’d never thought about donating an organ. I thought you had to be a relative or something like that.”
So in July 2007, when he was 28, Jones flew to Phoenix to donate a kidney to a 53-year-old woman with polycystic kidney disease. Her husband then gave a kidney to a 32-year-old woman in Toledo, Ohio. Two months later, her mother donated to a woman in Columbus, Ohio. The chain continued for months, until 13 people had new kidneys.
“I’ve met almost everybody in the chain,” Jones says. And they keep track of each other on Facebook. “We all share a very unique bond from being part of it.”

Since then, transplant chains linked by non-directed donors have spread around the world, growing longer and longer, with as many as 34 kidney transplants being performed in 26 different hospitals.
Roth continues to refine the scientific map in the interest of getting more people matched and living healthy, productive lives. And he and his colleagues are also journeying into other matching markets that have a big impact on people’s lives, such as public school lotteries. The New York City schools turned to Roth for help because their system of matching students with schools would grind to a halt while top-ranked students would ponder their choices. Some years, one-third of the city’s students would still be awaiting a seat on the first day of school. And because students and parents knew there was a chance they would be shut out of their top pick, there were incentives to game the system. Principals would withhold slots so they could snap up talented students later, and students would be less than truthful about their top pick.
“A big thing is making it safe for families to tell you what they want,” Roth says. “We make sure that the chance of getting your second choice if you fail to get your first choice is just as good as it would have been if you had listed your second choice as your first choice.”
With the new system, eighth-graders in New York City list their top 12 choices, and are matched well before school starts. When educators, students, and parents saw that they could trust the market, they had less incentive to finagle. The system has since been adopted by schools in Boston, Denver, New Orleans, and Washington, DC. And the social scientists are experimenting with matching markets to see if they can be used to minimize racial and economic disparities in school systems.



Because innovative social science is being used to make progress solving real-world problems, medical residents are able to live with their spouses, students are able to attend the school that’s their best possible option, and people with kidney disease have a better shot at a healthy, productive life. And organ donors have a chance to do good.
Matt Jones is happy his organ donation helped make kidney transplants available to so many people and that the economic theories that made his altruistic act possible also helped Al Roth and Lloyd Shapley gain global recognition. “It was kind of neat,” Jones says. “I tell my kids I was part of something that helped someone win the Nobel Prize.”
This article was written by Nancy Shute for From Research to Reward, a series produced by the National Academy of Sciences. This and other articles in the series can be found at www.nasonline.org/r2r. The Academy, located in Washington, DC, is a society of distinguished scholars dedicated to the use of science and technology for the public welfare. For more than 150 years, it has provided independent, objective scientific advice to the nation.
Please direct comments or questions about this series to Cortney Sloan at csloan@nas.edu.
Photo and Illustration Credits:
Alvin Roth: Pat Greenhouse/Boston Globe • Kidney transplant operation: Roger West, University of Cincinnati College of Medicine • Michael Rees and patients: Andy Morrison/The Blade • Transplant chain graphic: Adapted from PKD Foundation, pkdcure.org • Happy couple on Match Day: UT Southwestern Medical Center • NYC eighth-graders receive offer letters: Stephanie Snyder/Chalkbeat • Background Photos: Surgical team: Tina Manley/Alamy • High school students: Andrew Lamberson
© by the National Academy of Sciences. These materials may be reposted and reproduced solely for non-commercial educational use without the written permission of the National Academy of Sciences.
Credits
A film by Sarah Klein & Tom Mason; Director of Photography: Jon Kasbe; Music by
Ryan Sayward Whittier;
Motion Graphics by
Kathleen Chee;
Special thanks to
Dr. Alvin Roth, Amy & Fielding Daniel, Nobel Media, and Dr. Michael Rees.
Copyright ©
National Academy of Sciences. All rights reserved.
Terms of Use and Privacy Statement

