5
Potential Best Practices and Policy Options
In the final panel of the workshop, three presenters discussed their ideas about best practices and policy options for including minorities in clinical trials. They did so largely by drawing on their experiences with Asian Americans, Pacific Islanders, Native Americans, and Native Alaskans, but the lessons they drew apply much more broadly. In particular, all speakers emphasized the critical role of community involvement throughout the research process for meaningful inclusion of minorities in clinical trials.
POTENTIAL BEST PRACTICES AND POLICIES FOR INCLUSION OF ASIAN AMERICANS INTO CLINICAL TRIALS
Urban Asian Americans and Pacific Islanders in the Midwest—which are the populations at the center of the work done by Karen Kim, dean for faculty affairs and head of the Office of Community Engagement and Cancer Disparities at the University of Chicago—have several characteristics that increase the difficulty of involving them in clinical trials. First, the populations are relatively small compared with other populations and the populations of Asian Americans on the East and West Coasts. The populations also are heterogeneous, with many cultural and linguistic subgroups. About 70 percent of all Asian Americans in the United States are foreign born, and about 30 percent are limited English proficient, Kim noted. The health care system is not well equipped to handle the cultural and language needs of these populations. Asian Americans’ reputation as a “model minority,” marked by generally good health and educational achievement, is belied by the structural barriers and adversity facing the members of these groups.
“Unfortunately, this model minority status often creates hostility from other minority groups. ‘You do not have problems; look at us.’ This sense of hierarchy and competitiveness [is] really challenging,” she explained.
In addition, data on Asian Americans tend to be statistically unreliable, not analyzed, or not collected in the first place, Kim explained. Subgroups tend to be aggregated, or data from one subgroup are extrapolated to others, even when such methods are inappropriate. As a result, Asian Americans are in many ways “a nonrecognized minority in the health care system,” said Kim.
Kim described several policies that can increase the representation of Asian Americans and could be applied with other populations. One is to make study designs adaptable to include diverse but relatively small populations. This can be complicated by the need to involve people with limited English proficiency in the design and implementation of studies, which can create budget pressures for translations. But involving the community as an equal partner needs to start at the beginning rather than being an afterthought, Kim said. One approach is to form community advisory boards, she said. Another is to flip the structure and have studies done in the community with academic advisory boards. Several initiatives have demonstrated how communities can be involved in the planning and implementation of studies, including research sponsored by PCORI, community clinical oncology programs, and practice-based research networks. “We are starting to shift the process and the place where research is done,” said Kim. “The successful recruitment models often are happening in the communities themselves,” she added.
As an example of how these policies can be instituted, Kim described an ongoing study called the Partnership for Healthier Asians, which has been funded by the Agency for Healthcare Research and Quality. The partnership uses a market-oriented dissemination framework to take evidence-based information into limited English proficient populations in Chicago, Illinois. It has sought to make changes in the health care system and in the community through collaboration, including capacity building at the community level and joint priority setting.
As an example of a specific issue, Kim mentioned that the Asian American community has a low rate of colorectal cancer screening compared with other racial and ethnic groups. Surveys revealed that many Asian Americans thought that screening was something they would do only when they exhibited symptoms of a problem. The Screen for Life campaign of the Centers for Disease Control and Prevention (CDC) had only one campaign picture featuring an Asian American, and the campaign was not resonating with the population. Meetings created an infrastructure for the dissemination of information, which was time consuming and costly, said Kim, but also effective. New posters featuring members of Asian American communities
were used to change attitudes. In essence, said Kim, the project created its own infrastructure and tools to support the needs of the community.
The community partnership also took the lead in authoring papers. The initial publication of the research went to the community first in the form of a community-generated white paper, which helped the community build capacity and infrastructure around the disease.
Kim cited several other factors that can increase participation. One is a new paradigm for peer review to be more diverse and to recognize diverse participation. Who is on a review panel and who makes decisions about funding are both critically important issues, said Kim.
Another important policy issue involves the academic reward structure. Academics traditionally are rewarded for writing papers that appear in journals, but could rewards also be based on the outcomes of the work a researcher does, such as a community brief?
IRBs need to be trained to understand the value of diverse participation and inclusion, said Kim. For example, excluding non-English speakers from a clinical trial is understandable because of the cost of translation, but it can generate problems for the trial. “How are we going to move the bar forward and close this disparity gap if we can’t even study these individuals?” she asked. One study found that less than 22 percent of IRBs report clinical research with limited-English proficient populations (Glickman et al., 2011). The need for human protections remains as important as ever, Kim acknowledged, but IRBs also need to understand the value of diverse participation, which may result in study designs that are somewhat different than for larger populations. In addition, cultural competency training for the members of IRBs can help them understand the issues involved.
As an example of what is possible, Kim cited the language capacity of students at the Pritzker School of Medicine at the University of Chicago, where nearly half the incoming medical school class is able to speak Spanish. Yet of this group, only one person who was not Asian spoke an Asian language, and Asian Americans tend not to work with Asian American populations because of the difficulty of the work. “We need to shift that thinking,” she urged.
Kim urged applying new methodologies to allow oversampling that can ensure representation. Sampling can be done in different ways, depending on the community and the context. She also urged that data be disaggregated, even if doing so raises issues about the power of findings. “There has to be a better way to think about how data on Asian Americans can be reported,” she said.
Health information technology can be used to increase access to diverse populations; for example, PCORnet1 is doing this well, according to Kim.
___________________
1 The National Patient-Centered Clinical Research Network.
Technology can reach not just a population in one geographic region but across the nation, which can increase the statistical reliability of data on minority populations.
She urged greater cultural competency among researchers. Also, global does not equal local, in that what happens in another country does not necessarily reflect what happens in the United States.
Surveys conducted as part of the Partnership for Healthier Asians study found that more than half of respondents said they would participate if they knew more about clinical trials. As pointed out earlier, though it is widely claimed that minority groups are less willing than non-Hispanic whites to participate in health research, there are only small differences by race and ethnicity in willingness to participate. As Kim said, “We should not be making assumptions; we should just ask.”
Kim also pointed toward the difficulties with paying high indirect costs on a grant when the research is done outside of an institution. When the institution receives more funding than the communities in which a study is being conducted, priorities may be skewed. This is “something to start thinking about,” she said.
POTENTIAL BEST PRACTICES AND POLICIES FOR INCLUSION OF NATIVE AMERICANS INTO CLINICAL TRIALS
Many of the observations made about Asian Americans and Pacific Islanders apply as well to Native Americans and Alaska Natives, said Teshia Solomon, associate professor of family medicine and head of the Native American Research and Training Center at the University of Arizona. But American Indians and Alaska Natives are distinct in some ways. They suffer some of the highest rates of health disparities among minority populations. They also exhibit greater differences between tribal and urban populations, with between 50 and 70 percent of the population identified in the U.S. Census living in urban communities but migrating to other communities for health care or other reasons. The health system is complex, and even when American Indians receive free health care, “Not all free health care is good health care,” said Solomon. Members of the group live in poverty, are located in remote regions, face discrimination, and are vulnerable in other ways. Many American Indians and Alaska Natives are members of sovereign nations within the United States, which have unique relationships with the federal government. The federal government has a responsibility to Indian tribal communities to provide health care, but each tribe has distinct laws and institutional structures, and researchers need to be aware of these differences to work effectively with these populations, said Solomon. In addition, IRB processes with tribes can be lengthy and complicated.
Accurate and complete data are critical, said Solomon. Partial, incomplete, or missing data are not useful and can contribute to stereotypes and misinformation.
Solomon became interested in this issue when the original sampling design for the National Children’s Study focused on Native American women from three counties in Arizona, who do not necessarily represent women from other areas, Alaska Natives, or urban Indians. To broaden recruitment, she and her colleagues developed a tool kit that could be used by the study centers in urban communities. As part of this process, they did six focus groups with women aged 18 to 40 and one focus group with men aged 18 to 50.
The process yielded several policy recommendations that Solomon described at the workshop. One is to allot time to build trust between researchers and communities. Solomon said that it generally takes about a year, and maybe longer, to work with a specific community, and processes involving IRBs can take longer than that.
She recommended selecting the right community leader with whom to work and partnering with community organizations. Validation from communities can transfer to other communities. “If I did good work in Oklahoma, it may . . . transfer to my work in Arizona. I can guarantee you that if you did bad work in Oklahoma, it will definitely be heard of in Arizona,” she said.
She insisted that communities need to get something in return for collaborating in a project. Important findings about diabetes have come from projects involving Native American communities, Solomon observed, yet these communities still have the highest rates of diabetes in the nation.
She also urged researchers to acknowledge the private and uncomfortable nature of the discussions they may be having with people, adding that “If you are talking about biological samples or you are talking about a disease, to some researchers it is a study, to other people it is their lives.”
Building trust means collaborating. Communities can prefer to work with individuals from local agencies and organizations that are trusted. “Having role models who look like the community that you are working with is incredibly important,” said Solomon. In this way, local community members can be trained and community capacity built.
Having Native American staff and consistent staff is important. Physicians tend to turn over in Indian country, but the nursing staff is generally more consistent over time. Having familiar faces who are advocating for or collaborating on a project also can build respect and trust. One example is having an elder or respected community member talking on a video about the importance of a study.
Messages need to be culturally appealing, with respect for traditional meanings, Solomon observed. For example, women are considered sacred,
and the relationship between a mother and child or a father and child is as important as showing just a picture of a baby.
In addition, support for community champions, both in terms of fiscal support and capacity building, can develop relationships and trust. “They are giving you a gift,” said Solomon. “They are giving the field of science a gift. They are giving . . . health research a gift. You have to have respect for that,” she explained.
Researchers need to be visible at community events, Solomon continued. These might be county fairs, rodeos, or dinners at people’s homes. She noted that “You are going to do everything required, as if you were going to see your family, because that is what you are trying to do—build a family.”
Knowing your audience allows ideas and messages to be presented through a Native American lens. The daily lives of participants take precedence over the concerns of a study. How are people going to get to a study? Do they need housing? How are they going to make arrangements with employers?
A systematic tracking system can counter the unreliability of phone service and mobility challenges. When participants can be seen at multiple facilities over numerous years, keeping track of individuals can be difficult.
Outreach can create links with many different agencies, activities, and groups, such as local health care clinics, community colleges, vocational and job training programs, American Indian and Alaska Native church groups, language programs, food banks, child care, parenting programs, and adult education programs. At the same time, word of mouth remains the best way to communicate with American Indian and Alaska Native populations, said Solomon. But word of mouth does not necessarily mean face to face, so it could be something heard on the radio or from a friend or relative.
Native Americans and Alaska Natives in urban communities said that they rely heavily on social media, Solomon reported. Some cities may have Chinatowns, but they do not have American Indian towns. Native American people may have gathering places, but they also communicate in other ways, including tribal newsletters and radio stations. They also still go to powwows, which Solomon called “a universal language for urban American Indians.”
People need detailed information about a study, including its purpose, how samples will be gathered, how those samples will be used, who is collecting the data, and whether the study has involved other American Indian communities. People also want to know about the benefits not only to individuals but to families and the community as a whole, Solomon observed.
A COOPERATIVE GROUP PERSPECTIVE ON POTENTIAL BEST PRACTICES AND POLICY OPTIONS
More than 60 percent of the patients enrolled in cancer clinical trials have come through NCI Cooperative Groups.2 These groups have a central core, usually at an academic center, with affiliated organizations. The trials they conduct undergo peer review and auditing, and they adhere to NIH policies for the inclusion of women and minorities. However, said Sandra Brooks, chief medical officer of CompleteCare Health Network, “Specific strategies are needed to further realize the intent of those policies.”
Though more minorities have been enrolled in cancer clinical trials in recent years, they remain underrepresented compared with their representation in the population (see Figure 5-1). Furthermore, the representation of minority groups in the population will continue to grow, demanding even greater efforts to increase their representation in clinical trials.
Several meetings, trials, and other activities in recent years have generated lists of best practices and policy recommendations for increasing minority representation in clinical trials, Brooks noted. One is to emphasize peer mentors and to recruit minority investigators. Another is to provide incentives for a wider range of physicians to participate, such as protected time or funding. Another is to adopt a quality improvement approach to the clinical trial enterprise at each site and to take into account that developing new sites with new populations takes time.
Brooks cited several factors associated with deciding to participate in a trial, drawing from a prospective study of 781 patients and 150 physicians at 60 sites (Brooks et al., 2015). Of the 781 patients, a trial was available for about 37 percent. In these trials, the number of eligible nonwhite patients who chose to enroll was 78 to 83 percent, so “quite high,” according to Brooks; in contrast, enrollment was only about 45 percent among white patients.
Among the factors that made patients decide to enroll were:
- Enrolling in a trial might help me.
- I would consider a future trial.
- My doctor wanted me to go on a trial.
- I am concerned about my care if I do not go on a trial.
___________________
2 NCI Cooperative Groups, which were first begun in the 1950s, were transformed into the National Clinical Trials Network about 5 years ago.
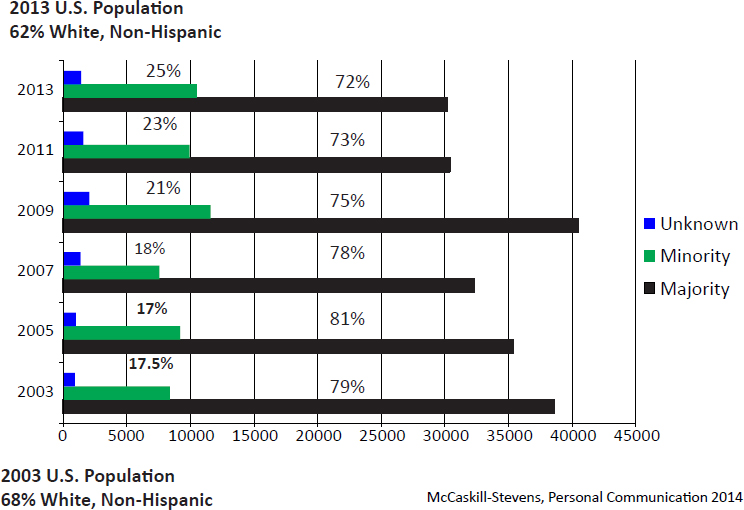
SOURCE: Brooks presentation, April 9, 2015.
Brooks also listed several factors that worked against decisions to participate:
- I felt pressure to enter a trial.
- It is time consuming to participate.
- I provide care to someone without being paid.
- Transportation would be difficult for me.
In this study, African American physicians enrolled patients at a very high rate. In addition, physicians were more likely to enroll a patient if they thought that the patient would not respond well to standard therapy or if they thought that the trial would not take a lot of a patient’s time. African American physicians enrolled at high rates irrespective of the race or ethnicity of the patient, which while not directly answered by the study, may point to the approach of these physicians and their research team, said Brooks, especially in explaining the trial and its associated consents to patients.
Brooks also derived several best practices from a breast cancer preven-
tion trial that sought to improve the enrollment of underserved minorities compared with previous trials. The interventions featured centralized support, outreach workers, patient materials and a website, physician training, partnerships with nontraditional partners such as corporations and foundations, and a working group that focused specifically on novel ways to promote accrual. Minority enrollment nearly doubled compared with a previous prevention trial without a targeted enrollment initiative (McCaskill-Stevens et al., 2013).
Another set of insights came from a survey of physicians accompanied by cultural competency training (Ulrich et al., 2010). According to the survey, only about one-third of respondents had formal mechanisms for screening for eligibility. Also, only about 13 percent of respondents had access to large percentages of minority populations. Some of the resulting actions from that survey included the development of an education and recruitment working group that was charged with looking at how to develop strategies, took kits, and best practices for dissemination, while another working group reviewed the feasibility of protocols. Cultural competency training for physicians and research assistants produced significant differences in cultural attitudes (Ulrich et al., 2010). Additional strategies to address enrollment that Brooks mentioned were the use of community advisory boards that take an active role in projects, input from patient advocates into protocols and materials, and centralized committees focused on disparities.
Brooks concluded by listing several of the most important factors that she derived from her review of best practices and policies:
- Population-specific recruitment strategies and sites
- Funding and institutional support for targeted infrastructure
- Feedback mechanisms for recruitment goals
- Sensitivity to socioeconomic factors
- Centralized disparities committees
- Workforce and research team diversity
- Cultural competency training for research teams
ACHIEVING DIVERSITY AMONG RESEARCHERS
In the question-and-answer session, the panelists again turned to the topic of how to increase the diversity of the researcher population, which in turn could facilitate more minorities to participate in clinical research.
Kim said that the need for diversity extends to the leadership of the research enterprise and to the people who are driving research. Minority researchers can act as role models for students and inspire them to become researchers themselves. They also can enable students to have experiences that allow them to see the value in research, and specifically
in research on diverse populations. At the same time, involving a diverse set of patients and advocates can demonstrate to young people the effects of research on a community and on individuals.
Solomon noted that she does a lot of student and junior faculty training, and a critically important step in this training is reaching out across a campus and involving the people who are doing work that involves diversity. They can act as role models and mentors in a variety of occupations, fields, and roles. In addition, scholarships and internships can be ways of getting diverse researchers involved in this kind of work, along with filling gaps in the funding of junior faculty.
Brooks cited the importance of early exposure to research, mentoring opportunities, and funding mechanisms to support students and faculty members. These strategies can be both formal and informal, she added.
The moderator of the panel, Francisco García, director and chief medical officer of the Pima County Health Department in Arizona, provided a concrete example of the advantages minority researchers can bring to the recruitment and retention of minorities in clinical trials. In his work at the University of Arizona, he was able to speak Spanish, allowing him to talk directly with patients and Spanish-speaking staff members. He worked not just at the cancer center but at other locations in the community. Everything in the environment was bilingual, and he had a team that “looked like the population that we were trying to recruit.” When he left the university, 48 percent of the more than 4,300 women who had been recruited for trials were Hispanic. “I feel very proud of that accomplishment,” he said.
Yet even this accomplishment was far from perfect, he added, noting that the rates of recruitment for American Indians and African Americans were “not where I wanted.” The techniques used with women of Mexican American background did not necessarily generalize to other settings or populations.
POTENTIAL POLICY CHANGES
A final topic of discussion during the panel was the policy changes needed to bring about changes in practices. Brooks again called attention to funding and to the development of infrastructure. If the goal is to recruit populations that are typically not represented, investigators who have access to those populations need a ramp-up period to develop an infrastructure to support that recruitment, she said. Sometimes the funding mechanism does not bridge from one time period to the next. Institutional support, either for the investigator or for the research enterprise, can bridge these gaps and create an environment in which the value of the enterprise is acknowledged.
Brooks also recommended looking at the exclusion criteria in recruitment strategies as well as involving communities in the development of
recruitment strategies. In addition, she said the monetary and human costs of disparities can demonstrate the potential return on investment to insurance companies, employers, and funders.
Solomon noted that it can take 10 years to build a relationship with a community that will enable research to move forward, so “a 4-year grant is not going to do the job.” Policies that can create more time to build that relationship would be useful. She also emphasized the importance of researchers being able to reach the populations they say, in grant applications, that they plan to reach. Finally, she mentioned making resources available to work directly with communities in culturally appropriate ways, including support for cultural competency training so that researchers know how a clinical trial could affect a community.
García pointed out that the need to have measures of the return on investment to more diverse participation is “probably the greatest need in this arena.” Industry understands on a marketing level the value of diversity, which could offer lessons for other groups. “The diversity of the individuals that are represented in their commercials very much acknowledges the fact that their marketplace is a global one that is far reaching,” he said.
Finally, Kim said that policies are only as good as their implementation, adding that “I do not think we need another laundry list of things. . . . How you enforce the policies that are already existent would be a really great start.”
This page intentionally left blank.












