Board on Children, Youth, and Families |
May 2016 |
Ensuring Quality and Accessible Care for Children with Disabilities and Complex Health and Educational Needs—Workshop in Brief
A PERSONAL PERSPECTIVE
The workshop began with a panel of three people whose lives have been profoundly shaped by their experiences with complex health and educational needs: the mother of a child who developed severe problems and needs at an early age; a graduate student who has lived with a life-long disability; and the mother of a young man who developed schizophrenia in his teens.
J-Jaye Hurley’s son Jackson was a normally developing boy until the age of 18 months, when he developed a serious viral infection and was hospitalized for 8 days. “He was never the same again,” his mother said. He was diagnosed with autism spectrum disorder, attention deficit hyperactivity disorder, mitochondrial disease, and an immune deficiency. In addition, he has a genetic pain disorder that had him screaming in pain for 3 years until the disorder was diagnosed and medicines to treat it were begun.
Hurley described the many steps her family has taken to provide Jackson with the medical care and therapies he needs, an education, home care (including keeping him from wandering), and activities he enjoys. As the southeast regional autism response team coordinator for Autism Speaks, she also took on the task of showing other parents how to advocate and care for their children. “When he was born, I thought Jackson was going to change the world,” said Hurley. “I believe he still is. He has changed me. Because of him, I will fight and learn and advocate for Jackson and for the millions of families just like mine, because he is very, very special and I am his special-needs mom.”
![]()
Jill Plevinsky, a 3rd-year graduate student studying to become a clinical pediatric psychologist, was diagnosed with Crohn’s disease when she was 7 years old. Her parents worked closely with the schools to arrange for accommodations through a 504 plan. They also encouraged her to become involved with organizations that work on behalf of those with similar conditions on medical care and social supports.
Plevinsky stressed the difficulty many young people with complex health and educational needs have in transitioning from pediatric systems of care to adult systems. Adolescents are hesitant “to leave their pediatric providers, because there’s a lot of attachment that happens there,” she said. Although some pediatric hospitals have good partnerships with adult institutions, including transition clinics that allow for a smoother transition, it is not widespread. In addition to the challenges of transitioning from pediatric systems of care, Plevinsky also noted that young adults face financial challenges when insurance does not fully cover the costs of treatments and medications necessary to manage chronic conditions.
Victoria Costello, a parent advocate and science journalist with the Public Library of Science, spoke about the 10 years she spent working with her son, who was diagnosed with paranoid schizophrenia at age 16. She became a leader of the movement for early intervention for psychosis and participated in a campaign to include early psychosis in the latest edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM). Although the DSM was not changed, Costello emphasized that early treatment and diagnosis worked for her son, who is without symptoms today. “He is always going to be an eccentric and unusual young man, but he is absolutely fine,” she said.
Costello also lauded the effects of a 1 percent tax on high-income earners in California that was targeted for a mental health services fund. Those tax dollars have supported early psychosis clinics and peer support programs that would not have been funded otherwise, she said.
INCREASED PREVALENCE
The prevalence of childhood disabilities has risen steadily in recent decades in the United States, noted Maureen Durkin, professor of population health sciences and Waisman Center investigator at the University of Wisconsin–Madison. In part, this rise in prevalence is due to the even more dramatic reduction in childhood mortality over the past century—from 10 percent of children who did not live past their 1st birthday in 1915 to about 0.6 percent today. “There’s no doubt that the improvements in survival, especially of children with special health care needs, during this time period have contributed to increases in prevalence,” she said. For example, in 1960 the average life expectancy for a child with Down syndrome was estimated at about 10 years; today, due to advances in health care and other services, it is about 60 years.
Durkin also noted that the prevalence of mental disabilities has been rising faster than that of physical disabilities. For example, data from the National Survey of Children with Special Health Care Needs show an increase in childhood disability from about 13 percent in 2001 to about 20 percent in 2011-2012, with a shift in needs from physical disabilities to mental health conditions and behavioral disorders (Bethell et al., 2002). In addition, the percentage of children with activity limitations due to health, based on parent reporting, has quadrupled over the past five decades, though some of the increase reflects more children living with their families and not in institutions: see Figure 1.
Disability rates can differ among populations groups, Durkin observed. For example, the prevalence of autism spectrum disorder, which also has risen dramatically in recent years, is higher in white children than in black and Hispanic children. Across ethnic and racial groups, autism spectrum disorder also is found at higher prevalences in higher income families than in medium and lower income families. Are these differences “because those are the ones who are getting access to services?” asked Durkin. “If it is, then we might need to do something to make sure that the children in greatest need are actually being identified and having access to services.” Durkin also noted that definitions of disability differ among agencies and programs, which makes it difficult to monitor disability rates and levels.
Investments made in improving the lives of children with special health care needs benefit everyone, Durkin said. For example, sidewalk curb cuts, electronic communication devices, and other barrier-free technologies serve not only people with disabilities, but also everyone else. In addition, all children and their families gain empathy and the ability to appreciate diversity even as they benefit in other ways from reduced health disparities.
IMPLICATIONS FOR BEHAVIORAL HEALTH
Serious medical conditions have many implications for behavioral health. As such, they highlight many of the broad themes discussed at the workshop, including a two-generation approach toward children and their families, the need for measures of health and well-being, and the benefits of working simultaneously across disciplines and conditions.
An example of a behavioral health condition is the traumatic stress caused by the psychological and physiological responses of children and their families to pain, injury, medical procedures, and invasive or frightening treatment experiences. As Anne Kazak, professor of pediatrics at the Sidney Kimmel Medical School of Thomas Jefferson University pointed out, traumatic stress and associated emotional reactions can seriously impair a child’s or family member’s functioning. Kazak and her colleagues have developed a psychosocial assessment tool (PAT) that scores for psychosocial risk and provides family-centered reports to support decision making and communication. Across 6,500 administrations of the PAT, 55 percent of families were determined to need only universal supports, while 34 percent were determined to need targeted interventions, and 11 percent were deemed to need clinical treatment. Kazak also noted that she and her colleagues have developed an intervention model that integrates behavioral therapy and work with families around symptoms of traumatic stress.
Robin Everhart, assistant professor of psychology at Virginia Commonwealth University, discussed pediatric asthma, another condition that has behavioral components in both children and families. Pediatric asthma occurs at very different rates in different population groups, with modifiable factors, including beliefs about asthma and medications, illness management, psychological stress within families, exposure to indoor allergens and outdoor allergens and pollution, and environmental stresses. Everhart has studied the development and implementation of interventions in Richmond, Virginia, where rates of pediatric asthma are especially high. Take-home messages from her research include the major influences on asthma of communities and fami-
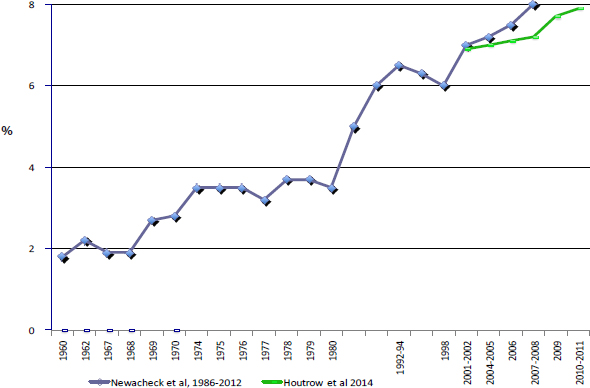
FIGURE 1 Rise in the percentage of children (ages birth to 17) with activity limitations due to health.
SOURCE: Durkin presentation, 2015 [http://sites.nationalacademies.org/dbasse/bcyf/dbasse_170078].
lies, including caregivers’ health and psychological well-being. In particular, meeting the needs of the family is critical. She said “What is it that you need, and how could we help you?”
The inclusion of children with disabilities in multiple social settings involves the behavioral responses not only of those children and their families. Torrie Dunlap, chief executive officer of Kids Included Together (KIT), has been teaching inclusive practices to organizations that serve children. Using a blended live and online learning model, KIT builds capacity in child- and community-based programs, including preschools, summer camps, afterschool programs, sports leagues, and scouting. “When providers have the training and support that they need, they are capable of meeting the needs of children with diverse abilities,” said Dunlap.
The last speaker at the session, Amy Houtrow, associate professor in the Department of Physical Medicine and Rehabilitation at Children’s Hospital Pittsburgh, discussed the systems of care for children with complex health and educational needs, including not just the health care system, but also the education, foster care, juvenile justice, and other systems. A major determinant of health and well-being is whether or not there is coordination across the many systems that are involved, which requires communication, she said. Team-based care for children with complex conditions can be multicoordinated, intercoordinated, or transcoordinated. In the first approach, multicoordination, many disciplines work together in the same setting at the same time, though they have different goals. In the second approach, intercoordination, communication about goals is key so that all team members are working toward common goals. In the third approach, transcoordination, disciplinary boundaries are blurred to better achieve shared goals and produce synergies. In transdisciplinary team-based care, “sharing goals, at the knuckles of the intersection between disciplines, is often the best way to keep the ball in the air,” said Houtrow.
DEVELOPMENTAL DISABILITIES THAT EMERGE IN CHILDHOOD
In the next workshop session, the presenter used autism—one of many developmental disabilities that emerge in childhood—as an example of how a particular set of conditions can reveal the many factors that influence interventions, including settings, approaches, funding, families, research, practices, and policies. Heather Johnson, acting director and chair of the Family and Woman’s Health Nurse Practitioner Programs at the Uniformed Services University of the Health Sciences (USUHS) Daniel K. Inouye Graduate School of Nursing, talked about not only her experiences as a family nurse practitioner at USUHS, but also of her experiences as the mother of a son with autism spectrum disorder. Her family encountered many difficulties with finding services, getting to those services, getting the services covered by insurance, and then going through the whole process again when they moved from Atlanta to the Washington, D.C., area. From her family’s experiences, she concluded that parents have a major role as advocates and that pediatricians need to help parents assume this role. In addition, every child and family is different and has different needs, she stressed. Evidence-based practice does not mean just using practices that are based on good evidence, but using evidence to shape practice, including assessments of the individual characteristics of patients and their family members.
Connie Kasari, professor of human development and psychiatry at the University of California, Los Angeles, similarly observed that many children need a combination or sequence of interventions and that methodologies need to be personalized or tailored for individuals and for sites. “Our goal is to have all children make progress,” she said, which can require the children who are not responding to one intervention are moved to another intervention. In addition, she emphasized the gap between research and practice, both because the research on which an intervention is based may not reflect the population in which it is implemented and because of a lack of implementation fidelity.
Problem behaviors, such as aggression, self-injury, and property destruction can place particularly great demands on families and health care providers and can negatively affect almost every facet of a caregiver’s daily life. Treatment components based on the purpose—that is, the function—that the behavior serves for the individual are consistently more effective than treatments based on the type of problem behavior, said Nathan Call, director of the Severe Behavior Program at the Marcus Autism Center in Atlanta. Levels of service that fit with a continuum of severity, from universal and preventive interventions to tertiary care for the most severe behaviors, also can help caregivers cope. He noted, however, that insurance reimbursement is a major consideration in whether many services can be delivered.
The session concluded with David Mandell, associate professor of psychiatry and pediatrics at the University of Pennsylvania’s Perelman School of Medicine, who pointed out that policies implemented in recent decades have increased access to autism services, but they have not necessarily resulted in a commensurate increase in the quality of care or in important outcomes. Younger cohorts have a higher rate of psychiatric hospitalizations than older cohorts, and more children are in more segregated environments in public schools now than in the 1990s. Interventions that focus specifically on the behaviors of teachers and other practitioners can help ensure that the intent of policies of increased access is realized, he said.
EARLY IDENTIFICATION AND INTERVENTIONS
Mental health and substance use disorders often arise early in adolescence and young adulthood, yet many years can go by before people with these very serious conditions receive treatment. A panel of four speakers looked at several of these disorders, including depression, bipolar disorder, and schizophrenia. Mary Fristad, professor and vice chair of research and academic affairs at the Department of Psychiatry and Behavioral Health at Ohio State University’s Wexner Medical Center, observed that early intervention has the potential to reduce disability for these three conditions. For example, one randomized controlled trial found that eight sessions of psychoeducational psychotherapy for 8- to 12-year-olds produced a fourfold decrease in conversion to bipolar spectrum disorder. This and other studies suggest, she said, “that we can potentially alter the staging with early intervention.”
Research in Australia, Denmark, the United Kingdom, Sweden, and Canada has similarly shown that interventions very close to the onset of psychosis can give people a much greater level of symptomatic recovery and greater functional capacity, according to Robert Heinssen, director of the Division of Services and Intervention Research at the National Institute of Mental Health (NIMH). Based on these experiences, NIMH has supported the Recovery After an Initial Schizophrenia Episode (RAISE) Program, which found much greater improvement in a quality-of-life measure in people whose duration of untreated psychosis was less than 18 months in comparison with people who had a longer duration of untreated psychosis. Said Heinssen, “It’s not enough just to offer the right thing; you need to offer the right thing at the right time.” In response to early results from this study, Congress allocated an additional $25 million for first-episode psychosis treatment programs.
Lisa Dixon, professor of psychiatry at Columbia University Medical Center, reported on a program called OnTrackNY, which built on the RAISE program to improve the delivery of first-episode psychosis services in New York. The program has produced a substantial and consistent reduction in hospitalization and an increase in the rates of participation in work and school. “The time is right,” Dixon concluded, “given the science and given the expertise in implementation, to expand and sustain resources for individuals with first-episode psychosis.”
In closing the session, Shay Bilchik, founder and director of the Center for Juvenile Justice Reform at Georgetown University’s McCourt School of Public Policy, called attention to young people who are “dually involved” with the child welfare system and the juvenile justice system. The child welfare and juvenile justice systems often do not know about such children, let alone the underlying behavioral health issues, substance abuse, mental health, or educational challenges a child might have. A treatment model that he and his colleagues have applied seeks to help such children through reduced involvement in the juvenile justice system, the use of preadjudication case dispositions, and by returning children to the child welfare system from the juvenile justice system. The approach includes increasing information sharing, the family voice in decision making, family and youth engagement, joint assessment and case planning, coordinated case management, behavioral health treatment, helping to develop prosocial bonds. The approach has shown “startlingly good” outcomes, according to Bilchik.
THE MEDIA AND PUBLIC PERCEPTIONS AND MISPERCEPTIONS
In the final panel of the workshop, five presenters examined a topic that has often been discussed by the forum but has not been explicitly addressed in one of its workshops: the perceptions and misperceptions of children with disabilities that are created by the media. Science journalist Victoria Costello noted that personal stories help break down the stigma that surrounds mental illnesses. In reference to her book A Lethal Inheritance: A Mother Uncovers the Science Behind Three Generations of Mental Illness (2012), she found that “it was striking how powerful it was for people, for other parents especially, to hear someone talking about their story.”
Steve Silberman, a former science writer for Wired magazine and the author of the book NeuroTribes: The Legacy of Autism and the Future of Neurodiversity (2015), pointed to the rise of the autism advocacy movement as one way of understanding public perceptions of autism and other conditions. These perceptions play on both fear and hope, Silberman observed, and while fear is an excellent way to raise money and motivate policy makers, “it’s not an excellent way to raise children.”
Susan Lanzoni, a historian of science and medicine, has written about caring for her son, who has type 1diabetes. A single vignette, such as her experiences at a summer camp for her son, can reveal a host of issues about children with complex health needs, she said. Similarly, Tony Foleno, senior vice president for research, planning, and evaluation at the Ad Council, emphasized the importance of clarity, simplicity, and emotional appeal. “The most effective [ad] campaigns . . . tell a story and tell it in an emotional, compelling way.”
Emily Willingham, the mother of two sons with special needs, noted that the environment determines disability, not the person. As a result, people have an obligation to create an environment that is functional for everyone. The media have helped and can continue to help shape skills and attitudes that reflect this new notion of disability, she and the other panelists concluded.
REFLECTIONS ON THE WORKSHOP
In the final session of the workshop, the moderators of the panels and reporters from three breakout groups reflected on the major themes that emerged from the workshop. The first breakout group, moderated by C. Hendricks Brown from Northwestern University and Emily Lichvar from the Substance Abuse and Mental Health Services Administration, highlighted ways to move forward even while the evidence base is developing. The second breakout group, moderated by Kelly Kelleher from the Research Institute at Nationwide Children’s Hospital and Angela Lello from Autism Speaks, focused on the importance of better community engagement and increased partnerships for development and implementation of solutions. In addition, they noted that communities, including children and families affected by disabilities, should have more decision-making options for prevention and treatment. The third breakout group, moderated by Andy Shih from Autism Speaks and Ed Schor from the Lucile Packard Foundation for Children’s Health, considered ways to design systems that work for children with complex health care needs. Emerging from that discussion was the need to overcome barriers to coordination and collaboration by taking a public health approach and building integrated systems that include health, education, and social services.
Finally, the moderators noted that, at several points during the workshop, speakers and participants called for a new White House conference on children, the last of which was held in 1971, and for the establishment of a federal children’s office, one that is situated prominently at the highest levels of the federal government to focus on children’s issues. Such steps would make it possible to reach out to other people and, as observed by Mary Ann McCabe of the George Washington University School of Medicine and George Mason University, “go beyond talking to ourselves.”
REFERENCES
Bethell, C.D., Read, D., Stein, R.E.K., Blumberg, S.J., Wells, N., and Newacheck, P.W. (2002). Identifying children with special health needs: Development and evaluation of a short screening instrument. Ambulatory Pediatrics, 2(1), 38-48.
Durkin, M. (2015). Disability Names and Numbers: Challenges and Opportunities in Nosology, Epidemiology, and Equity/Disparity. Paper presented at the Workshop on Ensuring Quality and Accessible Care for Children with Disabilities and Complex Health and Educational Needs. Available: http://naswebcontent.nas.edu/cs/groups/dbassesite/documents/webpage/c2vf/mtcw/~edisp/dbasse_170078.pdf [May 2016].
Halfon, N., Houtrow, A., Larson, K., and Newacheck, P.W. (2012). The changing landscape of disability in childhood. The Future of Children, 22(1), 13-42.
Houtrow, A. J., Larson, K., Olson, L.M., Newacheck, P.W., and Halfon, N. (2014). Changing trends of childhood disability, 2001-2011. Pediatrics, 134(3), 530-538.
Newacheck, P.W., and Halfon, N. (1998). Prevalence and impact of disabling chronic conditions of childhood. American Journal of Public Health, 88(4), 610-617.
Newacheck, P.W., Budetti, P.P., and Halfon, N. (1986a). Trends in activity-limiting chronic conditions among children. American Journal of Public Health, 76(2), 178-184.
Newacheck, P.W., Halfon, N., and Budetti, P.P. (1986b). Prevalence of activity limiting chronic conditions among children based on household interviews. Journal of Chronic Diseases, 39(2), 63-71.
PLANNING COMMITTEE FOR THE WORKSHOP ON FUNDING OPPORTUNITIES FOR EVIDENCE-BASED PREVENTION AND INTERVENTIONS TO PROMOTE CHILDRENS COGNITIVE, AFFECTIVE, AND BEHAVIORAL HEALTH
ANDY SHIH (Cochair), Autism Speaks; DONALD WERTLIEB (Cochair), American Orthopsychiatric Association; Eliot-Pearson Department of Child Development, Tufts University; WILLIAM R. BEARDSLEE, Baer Prevention Initiatives and Department of Psychiatry, Boston Children’s Hospital; Department of Child Psychiatry, Harvard Medical School; KIRSTEN BERONIO, Division of Behavioral Health and Intellectual Disabilities Policy, Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services; GARY BLAU, Center for Mental Health Services, Substance Abuse and Mental Health Services Administration; THOMAS F. BOAT, Cincinnati Children’s Hospital Medical Center; C. HENDRICKS BROWN, Departments of Psychiatry, Behavioral Sciences, and Preventive Medicine, Feinberg School of Medicine, Northwestern University; AMY GOLDSTEIN, National Institute of Mental Health, National Institutes of Health; LISA GORING, Autism Speaks; J. DAVID HAWKINS, School of Social Work, University of Washington; KELLY J. KELLEHER, Center for Innovation in Pediatric Practice, The Research Institute at Nationwide Children’s Hospital; LAUREL K. LESLIE, American Board of Pediatrics; Tufts University School of Medicine; MARY ANN McCABE, Society for Child and Family Policy and Practice; Society of Pediatric Psychology; School of Medicine, George Washington University; Department of Psychology, George Mason University; CRAIG J. NEWSCHAFFER, A.J. Drexel Autism Institute, School of Public Health, Drexel University; PAT SHEA, Office of Technical Assistance, National Association of State Mental Health Program Directors; STEPHEN SHORE, Ruth S. Ammon School of Education, Adelphi University; JENNIFER TYSON, Office of Juvenile Justice and Delinquency Prevention, U.S. Department of Justice; WENDY KEENAN, Study Director.
DISCLAIMER: This Workshop in Brief has been prepared by Steve Olson, rapporteur, as a factual summary of the presentations and discussion at the workshop. The statements made are those of the individual speakers and do not necessarily represent the views of all participants, the planning committee, the National Academies of Sciences, Engineering, and Medicine. The planning committee was responsible only for organizing the workshop, identifying the topics, and choosing speakers.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Workshop in Brief was reviewed by Kelly J. Kelleher, Center for Innovation in Pediatric Practice and Health Services Research and Community Health and Services Research, The Research Institute at Nationwide Children’s Hospital and Deborah Klein Walker, U.S. Health, Abt Associates, Cambridge, MA. Patricia Morison, Division of Behavioral and Social Sciences and Education, served as review coordinator. The review comments and draft manuscript remain confidential to protect the integrity of the process.
SPONSORS: The Forum on Promoting Children’s Cognitive Affective and Behavioral Health is partially supported by the American Academy of Pediatrics; the American Board of Pediatrics; the American Orthopsychiatric Association; the American Psychological Association; Autism Speaks; the Centers for Disease Control and Prevention; Community Anti-Drug Coalitions of America; the Conrad N. Hilton Foundation; the Hogg Foundation for Mental Health; the National Institutes of Health; the Robert Wood Johnson Foundation; the Society for Child and Family Policy and Practice; the Society of Clinical Child and Adolescent Psychology; the Society of Pediatric Psychology; Substance Abuse and Mental Health Services Administration; U.S. Department of Health and Human Services, Assistant Secretary for Planning and Evaluation; U.S. Department of Justice.
Copyright © 2016 by the National Academy of Sciences. All rights reserved.
FORUM ON PROMOTING CHILDREN’S COGNITIVE, AFFECTIVE, AND BEHAVIORAL HEALTH
WILLIAM R. BEARDSLEE (Cochair)
Boston Children’s Hospital and Harvard Medical School
C. HENDRICKS BROWN (Cochair)
Feinberg School of Medicine, Northwestern University
KAREEMAH ABDULLAH
Community Anti-Drug Coalitions of America
DARA BLACHMAN-DEMNER
National Institute of Justice, U.S. Department of Justice
THOMAS F. BOAT
Cincinnati Children’s Hospital Medical Center
FELESIA R. BOWEN
School of Nursing, Rutgers University
DAVID A. BRENT
School of Medicine, University of Pittsburgh
LAUREN CALDWELL
American Psychological Association
WILMA P. CROSS
Office of Disease Prevention, National Institutes of Health
ALEXA EGGLESTON
Conrad N. Hilton Foundation
RICHARD G. FRANK
U.S. Department of Health and Human Services
AMY GOLDSTEIN
National Institute of Mental Health, National Institutes of Health
COSTELLA GREEN
Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services
RICK HARWOOD
National Association of State Alcohol and Drug Abuse Directors
J. DAVID HAWKINS
School of Social Work, University of Washington
KIMBERLY E. HOAGWOOD
Society of Clinical Child and Adolescent Psychology and New York University
COLLEEN HORTON
Hogg Foundation for Mental Health, University of Texas at Austin
JENNIFER W. KAMINSKI
U.S. Centers for Disease Control and Prevention
KELLY J. KELLEHER
Nationwide Children’s Hospital
UMA KOTAGAL
Cincinnati Children’s Hospital Medical Center
LAUREL K. LESLIE
American Board of Pediatrics and Tufts University School of Medicine
MARY ANN MCCABE
Society of Pediatric Psychology, Society for Child and Family Policy and Practice, George Washington University, and George Mason University
JENNIFER NG’ANDU
Robert Wood Johnson Foundation
JENNIFER OPPENHEIM
Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services
LAWRENCE A. PALINKAS
School of Social Work, University of Southern California
EVE E. REIDER
National Center for Complementary and Integrative Health, National Institutes of Health
MARY JANE ROTHERAM-BORUS
University of California, Los Angeles
PAT SHEA
National Association of State Mental Health Program Directors
ANDY SHIH
Autism Speaks
BELINDA SIMS
National Institute on Drug Abuse, National Institutes of Health
JOSÉ SZAPOCZNIK
University of Miami
VERA FRANCIS “FAN” TAIT
American Academy of Pediatrics
JENNIFER TYSON
Office of Juvenile Justice and Delinquency Prevention, U.S. Department of Justice
DONALD WERTLIEB
American Orthopsychiatric Association and Tufts University
For additional information about the Forum, visit http://nas.edu/ccab.









