2
Older Adults Who Need Caregiving and the Family Caregivers Who Help Them
ABSTRACT: This chapter sets the stage for the remainder of the report and has two principal objectives. The first is to describe the older adult population with care needs because of health or functional limitations and the family caregivers who help them. The second is to review demographic and societal trends affecting the demand for and supply of family caregivers, including the marked growth in and aging of the older adult population; the increasing diversity of the older adult population; the changing nature of family relationships; women’s growing participation in the workforce; and the declining size of American families.
Chapter 1 noted that millions of Americans in every walk of life are engaged in or affected by family caregiving for older adults. The faces and experiences of these individuals and the older adults they care for are as varied as the nation’s population. American families are more diverse—ethnically, racially, economically, religiously, and in many other ways—than ever. So are their living arrangements and basic notions of what constitutes family. As the previous chapter reported, the committee approached its assessment of family caregiving with the view that family caregivers of older adults may be relatives, partners, friends, or neighbors whose caregiving is driven primarily by a personal relationship.
This chapter sets the stage for the remainder of the report by describing the estimated number and characteristics of older adults who need help with self-care, mobility, or household activities for health or function-
ing reasons, and the family caregivers who help them. It also reviews the demographic and other societal trends that will affect the nation’s capacity to care for older adults in the future.
PREVALENCE OF THE NEED FOR A CAREGIVER
The need for help with everyday activities is not an inevitable consequence of aging (Feder, 2015; He and Larsen, 2014; NRC, 2012; Stone, 2015). Limitations in physical health and functioning, mental health, and/or cognitive functioning—not age—are the primary reasons why older adults need help from others. Living longer, however, often means living with impairments that may affect one’s ability to perform daily activities. As people age, they are increasingly likely to develop a physical or cognitive impairment that impacts their ability to function independently (Adams et al., 2013; Anderson, 2010; CMS, 2012; Wolff and Jacobs, 2015). Between ages 85 and 89 years, for example, more than half of older adults (58.5 percent) receive a family caregiver’s help because of health problems or functional limitations (Freedman and Spillman, 2014a). From age 90 years and onward, only a minority of individuals (24 percent) do not need some help from others.
Whether rates of disability among older adults will increase significantly in the future is uncertain. Although the prevalence of major chronic diseases—including cancer, diabetes, heart disease, hypertension, lung disease, and stroke—are expected to increase among older adults (Gaudette et al., 2015), research suggests that future disability rates may not (NIH, 2010). Numerous factors may lead to declines in disability including, for example, improvements in medical treatments, increases in health-improving behaviors, improvements in socioeconomic and education levels, as well as increased use of assistive technologies. Future research may also bring new therapies that can prevent or minimize disability from stroke, diabetes, and other conditions.
Understanding the Available Data
Examining the prevalence and nature of family caregiving of older adults is challenging because researchers use different assumptions and survey methods for identifying the older adults who need help and who their caregivers are. Estimates of the need for caregiving, for example, are highly sensitive to how disability is defined. A definition that includes older adults who need help with household activities will generate significantly larger estimates than one that is based on needs for help with self-care (Freedman and Spillman, 2014a). Surveys with long reference periods (e.g., 1 year) will generate larger estimates than surveys with short reference periods (e.g.,
1 month) because they are more likely to include individuals who have short-term, intensive needs during, for example, an acute illness or injury (Giovannetti and Wolff, 2010).
Due to resource constraints, all the surveys that are relevant to family caregiving are limited in size, which in turn limits subgroup analyses. No current survey has sufficient power to assess the needs and experiences of older adults and their caregivers by all of the varied subgroups of interest, including those defined by race and ethnicity, rural residence, or sexual orientation. It is also important to recognize that while data are available on older adults who need but do not have a family caregiver, it has not been analyzed. About 20 percent of the National Health and Aging Trends Study (NHATS) respondents report receiving no help despite having difficulty with self-care, mobility, or household activities. They are able to remain independent by using assistive devices, paid help, and/or restricting their activities. Comparisons between these individuals and older adults who receive help are not available (Freedman and Spillman, 2014a; Freedman et al., 2014).
Disability surveys typically identify older adults with functional limitations by asking respondents (or their proxies) about their ability, difficulty, or need for assistance in taking care of themselves. But no two surveys ask about the limitations in precisely the same way. The most common questions focus on self-care activities (often referred to as activities of daily living or ADLs) such as bathing, eating, dressing, and toileting; transferring (getting in and out of bed); mobility (getting around inside or outside one’s home or building); and household activities (instrumental activities of daily living or IADLs) such as using the telephone, taking medications, managing money, doing housework and laundry, preparing meals, and shopping for groceries.1
Although difficulty performing household activities creates a need for assistance from others, difficulty with self-care suggests a need for more intensive help.
National Health and Aging Trends Study and the National Survey of Caregivers
The prevalence data presented in this chapter (and throughout this report) are derived primarily from NHATS and its companion National Study of Caregiving (NSOC). The federally-funded NHATS, a longitudinal survey first fielded in 2011, was specifically designed to document how functioning in daily life changes with age (Freedman et al., 2011). It draws
___________________
1 Although ADLs and IADLs are commonly used to characterize levels of disability, neither is consistently defined in the literature.
from a nationally representative sample of Medicare beneficiaries (age 65 and older) in the continental United States who live independently or in a senior community, assisted living facility, nursing home, or other residential setting (Freedman et al., 2013; Kasper et al., 2014). NHATS employs a disability measurement protocol that includes activities characteristic of the traditional ADL and IADL measures as well as other contributing aspects of disability, such as physical, sensory, and cognitive capacity; the ability to carry out essential activities independently; and participation and restrictions in valued activities (Freedman et al., 2011). It also uses a protocol that has been assessed for sensitivity and specificity for identifying care recipients who have “probable dementia” relative to an actual diagnosis of dementia (Kasper et al., 2013, 2014).2
NSOC is a survey of the family and other unpaid caregivers named by NHATS respondents who reported receiving help for health or functioning reasons. NHATS asks older adults to name all the people who helped them; most identified only one person. NSOC estimates, which are reviewed later in the chapter, do not include family caregivers of nursing home residents. Thus, population-based estimates on the number of family caregivers assisting older adults in nursing homes are not available. It is not possible to use NSOC data to estimate the number of caregivers who are helping more than one older adult (e.g., an adult child caring for two parents with impairments). See Appendix E for a description of the committee’s analyses of NHATS and NSOC.
What Kind of Assistance Do Older Adults Need?
Figure 2-1 provides an overall picture of the number and proportion of older adults who receive help. In 2011, the majority of older adults (71 percent) did not receive assistance for health or functioning reasons (Freedman and Spillman, 2014b). However, 17 percent or 6.3 million older adults received help with household tasks or self-care (defined here as bathing, dressing, eating, toileting, or mobility) due to health or functioning limitations other than dementia, while another 9 percent or 3.5 million older adults received help because they had dementia. Three percent (1.1 million) resided in a nursing home. Chapter 3 describes the full range of supports that family caregivers provide to older adults, including emotional support, help with medical/nursing tasks, and care coordination.
___________________
2 NHATS respondents were considered to have “probable dementia,” which includes individuals whose doctor said they had dementia or Alzheimer’s disease and individuals classified as having probable dementia based on results from a proxy screening instrument and several cognitive tests. For details on the NHATS dementia protocol, see Kasper et al., 2013.
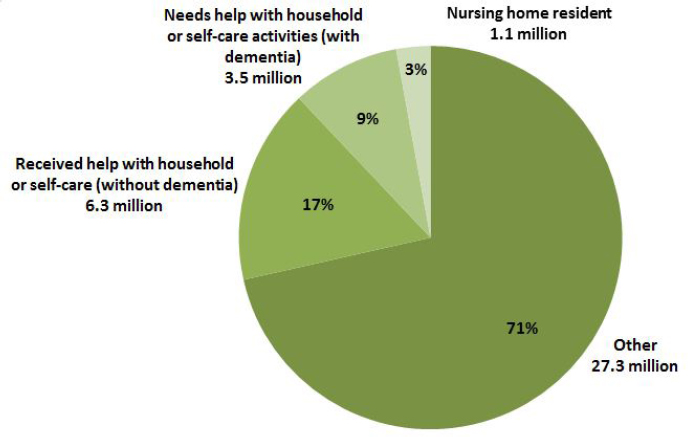
NOTES: As reported by Medicare beneficiaries age 65 and older (or their proxy). Household help includes assistance (for health or functioning reasons only) with laundry, hot meals, shopping for personal items, paying bills/banking, and/or handling medications. “Self-care” refers to bathing, dressing, eating, toileting, or getting in and out of bed. “Other” refers primarily to individuals who receive no help, but also includes persons who may have had help with household activities from someone for reasons other than health or functioning.
SOURCE: Data from the 2011 NHATS.
Figure 2-2 further illustrates the huge impact of dementia on caregiving needs. Of the 4.9 million older adults who received help with self-care, 3.5 million (71.4 percent) were classified as having probable dementia. People with more advanced dementia may require constant supervision to protect themselves and others from harm—even if they are able to perform some self-care or household tasks. Individuals in the early stages of dementia may also require support, including assistance with paying bills, personal care, mobility tasks, and surrogacy (Black et al., 2013). With disease progression, people with dementia also experience a wide range of co-morbidities, including vision, hearing, and mobility limitations.
An important note is that estimates of average need, such as those in Figure 2-1 and Figure 2-2, mask substantial variation in the amount of time older adults need help due to an impairment. In a recent microsimulation, for example, Favreault and Dey (2016) projected the distribution in the
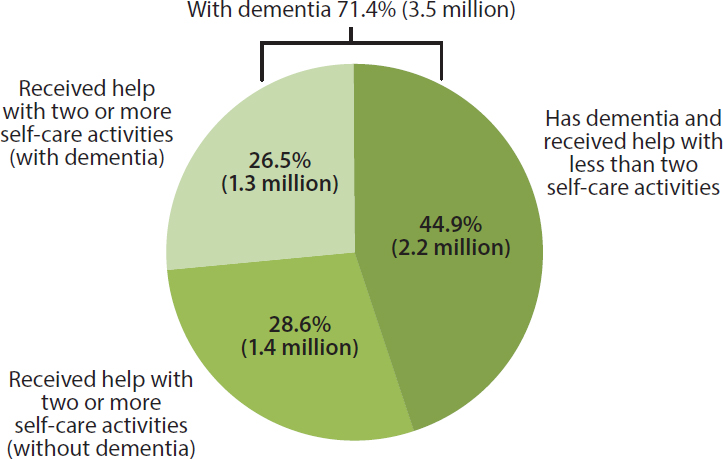
NOTES: As reported by Medicare beneficiaries age 65 and older (or their proxy) for the prior month. Self-care activities include bathing, dressing, eating, toileting, or getting in and out of bed. “Probable dementia” includes individuals whose doctor said they had dementia or Alzheimer’s disease and individuals classified as having probable dementia based on results from a proxy screening instrument and several cognitive tests. Excludes nursing home residents.
SOURCE: Data from the 2011 NHATS.
number of years that an older adult could anticipate needing long-term services and supports (LTSS) (see Table 2-1). They estimated that upon turning age 65, more than half of individuals (52.3 percent) can expect some period of time when they will need help with at least two ADLs (i.e., eating, toileting, transferring, bathing, dressing, or continence) for at least 90 days or need supervision for health and safety threats due to severe cognitive impairment. However, the duration of such need is quite variable, less than 1 year for 18.9 percent of people and more than 5 years for 13.9 percent of people. The simulation also estimated substantial differences in need between men and women. Women (17.8 percent) are much more likely than men (9.8 percent) to need LTSS for 5 years or more.
| Number of Years Disabled | All (Percentage) | Men (Percentage) | Women (Percentage) |
|---|---|---|---|
| None | 47.7 | 53.3 | 42.5 |
| Less than 1 year | 18.9 | 18.4 | 19.4 |
| 1-1.99 years | 7.8 | 7.4 | 8.1 |
| 2-4.99 years | 11.7 | 11.1 | 12.3 |
| More than 5 years | 13.9 | 9.8 | 17.8 |
NOTES: Includes persons needing assistance (including nursing home residents) with at least two activities of daily living (i.e., eating, toileting, transferring, bathing, dressing, or continence) for at least 90 days or needing supervision for health and safety threats due to severe cognitive impairment. Percentages may not total to 100 due to rounding.
SOURCE: Favreault and Dey, 2016.
WHO ARE THE FAMILY CAREGIVERS OF OLDER ADULTS?
The committee examined two subgroups of family caregivers: those who help an older adult with any need (see Figure 2-1) because of health or functioning reasons and those caregivers who help “high-need” older adults (see Figure 2-2 and Table 2-2). “High-need” is used to describe individuals with probable dementia or who need help with at least two self-care activities (i.e., bathing, dressing, eating, toileting, or getting in and out of bed).
According to NSOC, 17.7 million individuals were caregivers of an older adult in 2011 because of health or functioning reasons or approximately 7.7 percent of the total U.S. population age 20 and older (see Table 2-2). Nearly half of those caregivers (8.5 million) provided care to a high-need older adult. This estimate does not include caregivers of nursing home residents, and comparable information about the number of family caregivers assisting older adults in nursing homes is not available.
For most family caregivers, caregiving is not a short-term obligation. Only 15 percent of NSOC caregivers had provided care for 1 year or less at the time of the survey whereas nearly 70 percent were caregiving for 2 to 10 years, and 15 percent had already provided care for more than 10 years by the time of the survey (see Table 2-3). The median number of years of family care for older adults with high needs was 5 years.3 This is an important finding because, as discussed in Chapter 3 and Chapter 4, family caregivers are more likely to suffer negative consequences (e.g.,
___________________
3 Committee NSOC calculations.
| Care Recipient’s Level of Need | Number of Caregivers | Percentage of Adults Age 20+ |
|---|---|---|
| Any need in mobility, self-care, or household activities due to health or functioning limitations | 17.7 million | 7.7 |
| High-need: care recipient has probable dementia and/or needs assistance with two or more self-care activities | 8.5 million | 3.7 |
NOTES: Includes family caregivers of Medicare beneficiaries age 65 and older in the continental United States who resided in community or residential care settings (other than nursing homes) and received help with self-care, mobility, or household activities for health or functioning reasons. “Self-care” refers to bathing, dressing, eating, toileting, or getting in and out of bed. “Probable dementia” includes individuals whose doctor said they had dementia or Alzheimer’s disease and individuals classified as having probable dementia based on results from a proxy screening instrument and several cognitive tests.
SOURCES: Data from the 2011 NHATS and the companion NSOC.
| Average Number of Years | Percentage |
|---|---|
| 1 year or less | 15.3 |
| 2 to 4 years | 34.7 |
| 5 to 10 years | 34.9 |
| More than 10 years | 15.1 |
NOTES: Includes family caregivers of Medicare beneficiaries age 65 and older in the continental United States who resided in community or residential care settings (other than nursing homes) and received help with self-care, mobility, or household activities for health or functioning reasons. Respondents were asked “How many years have you been helping the care recipient?” Responses were given in whole numbers.
SOURCES: Data from the 2011 NHATS and the companion NSOC.
anxiety, depression, social isolation, and financial losses) the longer they are engaged in caregiving.
Some researchers distinguish between primary caregivers—individuals who self-identify as having primary responsibility for providing care and/or who spend the most time providing care—from secondary caregivers—individuals who provide intermittent supplementary or complementary help to the care recipient. Spouses and daughters are more likely to be primary
caregivers and men and non-relatives are more likely to play a secondary caregiving role. Primary caregivers typically provide many more hours of care than secondary caregivers and make the majority of decisions regarding care provision to the care recipient (Chadiha et al., 2011; Tennstedt et al., 1989). Although it is widely recognized that caregiving may be distributed among multiple family members and friends, relatively little is known about the number of caregivers who play a secondary role, the types and amount of help they provide, and the extent to which relationships between primary and secondary caregivers are supportive or conflictual.
Anticipating Future Years as a Caregiver of an Older Adult
Adults may be called on to provide care to an older adult more than once in their lifetime. Young adults, for example, may participate in the care of their grandparents; adults in their 50s and 60s may care for one or both parents, parents-in-law, a spouse/partner, other relatives, or friends; and older adults may provide care to spouses, siblings, or friends and neighbors. The committee could not find published estimates of the likelihood of becoming a caregiver over a lifetime or for how long. To consider the latter question, the committee commissioned an analysis, by Vicki A. Freedman, Ph.D., to estimate the average number of years and percentage of remaining life that U.S. adults might expect to spend caring for an older adult who needs help with activities of daily living. Table 2-4 presents the key findings in this analysis. Appendix D contains the complete analysis and describes the methodology in detail.
Freedman’s analysis drew from the 2011 Current Population Survey, life tables from the National Center for Health Statistics, and the 2011 NSOC and NHATS datasets to develop assumptions about future prevalence of disability, numbers of available caregivers, and mortality rates. The analysis assumed that current age-specific caregiving rates (based on NSOC data) and life expectancy (based on the life tables) would not change over the life of the hypothetical cohort. These assumptions—unavoidable because of the available data and time to conduct the analysis—are an important limitation of the analysis. Actual caregiving rates in the future may differ and will depend on numerous factors that are difficult to predict, such as rates of late-life disability, family size and composition, competing demands from work and family, the availability and affordability of paid caregivers, new technologies, and cultural norms (Kaye, 2013; Marks, 1996; Stone, 2015). Future mortality rates are similarly uncertain, reflecting demographers’ differing views about future life expectancy (Social Security Trustees Report, 2015).
Another important note is that because these are estimates of an average for the overall adult population, they do not convey the considerable
| Age Group | Older Adults with One or More Activity Limitations | High-Need Older Adults | ||||||
|---|---|---|---|---|---|---|---|---|
| All Family Caregivers | Men | Women | All Family Caregivers | |||||
| Average Number of Years Spent Caregiving | Percentage of Remaining Life | Average Number of Years Spent Caregiving | Percentage of Remaining Life | Average Number of Years Spent Caregiving | Percentage of Remaining Life | Average Number of Years Spent Caregiving | Percentage of Remaining Life | |
| 20-29 | 5.1 | 8.6 | 4.1 | 7.2 | 6.1 | 9.9 | 2.4 | 4.1 |
| 30-39 | 5.0 | 10.0 | 4.0 | 8.4 | 6.0 | 11.5 | 2.4 | 4.7 |
| 40-49 | 4.8 | 11.9 | 3.9 | 10.1 | 5.7 | 13.4 | 2.3 | 5.6 |
| 50-59 | 4.2 | 13.5 | 3.5 | 11.9 | 4.9 | 14.9 | 2.0 | 6.2 |
| 60-69 | 3.3 | 14.4 | 2.9 | 13.8 | 3.7 | 15.0 | 1.5 | 6.5 |
| 70-79 | 2.2 | 14.1 | 2.2 | 15.8 | 2.1 | 12.8 | 0.9 | 6.0 |
| 80+ | 1.0 | 11.5 | 1.3 | 15.7 | 0.8 | 8.8 | 0.5 | 6.1 |
NOTE: Estimates are averages that include people who never become caregivers, but exclude people who assist older adults who reside in nursing homes. Family caregivers are adults age 20 or older who assist an older adult who needs help because of health or functioning reasons. High-need older adults have probable dementia or need help with at least two self-care activities (bathing, dressing, eating, toileting, or getting in and out of bed). Excludes caregivers of nursing home residents.
SOURCE: Freedman, 2015 (see Appendix D).
variation in individual caregiving experiences. The average duration of caregiving is based on the experiences of individuals who will never be a caregiver and as well as individuals who will be a caregiver for many years, even decades. Estimates of the variation of lifetime caregiving as well as the proportion of people who never become caregivers unfortunately do not exist; however, other available evidence suggests that the variation is substantial (Miyawaki, 2016).
Table 2-4 provides Freedman’s projections for U.S. adults in different age groups for two levels of need for caregiving: first, caring for older adults who need any help because of health or functioning reasons and, second, caring for high-need older adults (as defined by the committee above). The analysis estimates that adults in their 20s will, on average, spend 5.1 years—or 8.6 percent of their remaining lifetime—caring for an older adult with at least one activity limitation. Nearly half of these caregiving years (2.4 years) are estimated to be spent providing care to a high-need older adult. These estimates are averages that include those who will never become caregivers as well as those who will provide care—to one or more older adults and in varying durations. The average number of years spent caregiving by those who do become caregivers, of course, is higher than the overall average, but the methods used here cannot estimate that magnitude.
Women are estimated to spend more years caregiving than men—on average 6.1 years or nearly 10 percent of their adult life—whereas men are estimated to spend on average 4.1 years or just more than 7 percent of their adult life. The percentage of remaining life to be spent providing care peaks at different ages for men and women. For men, once they reach age 70, nearly 16 percent of their remaining lifetime—or 1 to 2 years—is spent caring for an older adult. For women, this figure peaks between ages 50 and 69, when about 15 percent of their remaining lifetime—or about 4 to 5 years—is spent caring.
Characteristics of Family Caregivers of Older Adults4
Tables 2-5 and 2-6 describe an array of factors that characterize the population of family caregivers helping older adults. Although caregiver surveys often produce differing estimates of the size of the caregiver population, national surveys consistently show that caregivers are predominantly middle-aged daughters or spouses (Johnson and Wiener, 2006; Spillman and Pezzin, 2000; Wolff and Kasper, 2006). Women have always made up
___________________
4 This section draws primarily from the 2011 NSOC. As noted earlier, the family caregivers included in NSOC data are caregivers of Medicare beneficiaries age 65 and older in the continental United States who need help due to health or functioning. Caregivers of nursing home residents are excluded.
| Characteristic | Family Caregivers (percentage) | High-Need Caregivers (percentage) | U.S. Adults (percentage) |
|---|---|---|---|
| Age | |||
|
20-44 |
14.7 | 15.6 | 33.6 |
|
45-54 |
23.7 | 23.4 | 14.3 |
|
55-64 |
26.8 | 28.4 | 12.2 |
|
65-74 |
18.9 | 16.3 | 7.2 |
|
75+ |
13.4 | 13.0 | 6.1 |
| Gender | |||
|
Male |
38.3 | 36.2 | 48.5 |
|
Female |
61.7 | 63.8 | 51.5 |
| Race/ethnicity | |||
|
White, non-Hispanic |
70.9 | 66.4 | 67.0 |
|
Black, non-Hispanic |
12.6 | 12.4 | 12.0 |
|
Other, non-Hispanic |
4.8 | 5.7 | 6.0 |
|
Hispanic |
11.6 | 15.2 | 15.0 |
| Education | |||
|
Less than high school |
12.9 | 13.1 | 14.1 |
|
High school graduate or equivalent |
25.5 | 24.8 | 28.4 |
|
More than high school/less than bachelor’s degree |
33.2 | 35.4 | 29.0 |
|
Bachelor’s degree or higher |
26.9 | 24.9 | 28.5 |
NOTES: Includes family caregivers of Medicare beneficiaries age 65 and older in the continental United States who resided in community or residential care settings (other than nursing homes) and received help with self-care, mobility, or household activities for health or functioning reasons. “High-need” refers to caregivers of older adults who have probable dementia or need assistance with two or more self-care activities (bathing, dressing, eating, toileting, or getting in and out of bed). Percentages are for adults age 20 and older except for race/ethnicity of the overall U.S. population (18 and older) and the education level of the overall U.S. population (25 and older). Percentages for caregivers may not total 100 due to missing data.
SOURCES: Family caregiver data, 2011 NHATS/NSOC; overall U.S. data, Kids Count Data Center, 2015; and U.S. Census Bureau, 2016a,b.
the majority of the nation’s caregivers (NAC and AARP Public Policy Institute, 1997, 2004, 2009, 2015a; Penrod et al., 1995; Pinquart and Sörensen, 2006; Yee and Schulz, 2000), although some evidence shows that men are assuming increasing roles in caregiving (NAC and AARP Public Policy Institute, 2015a; Spillman et al., 2000), especially in the lesbian, gay, bisexual, and transgender (LGBT) community (Grossman et al., 2007; Hughes and
Kentlyn, 2011). In 2011, roughly 62 percent of NSOC caregivers were female (see Table 2-5) and more than one-third were daughters, daughters-in-law, or stepdaughters of the care recipient (see Table 2-6). Those three groups may play an even greater role in caring for high-need individuals; 38 percent of family caregivers for high-need older adults were daughters, daughters-in-law, or stepdaughters compared to 33.6 percent of all caregivers. Women also make up a majority of NSOC care recipients, as 70 percent of both all-need and high-need NSOC care recipients were female. Half of the NSOC caregivers were between the ages of 45 and 64 (50.5 percent), but nearly one-third (32.3 percent) were older adults themselves.
Caregivers’ family ties to care recipients are an important policy consideration because the nature of these relationships can determine the caregiver’s access to family and medical leave or paid sick days to care for a seriously ill relative or access to their health information. For example, in most states the Family and Medical Leave Act (FMLA) pertains only to workers caring for spouses, domestic partners, children, and parents (Mayer, 2013)—omitting nearly one in four caregivers (23.7 percent) and
| Family Relationship | All Caregivers (percentage) | High-Need Caregivers (percentage) |
|---|---|---|
| Relationship to recipient | ||
|
Spouse |
21.5 | 18.1 |
|
Daughter, daughter-in-law, stepdaughter |
33.6 | 38.0 |
|
Son, son-in-law, stepson |
21.2 | 21.8 |
|
Other |
23.7 | 22.1 |
| Marital status | ||
|
Married/partnered |
66.6 | 66.1 |
|
Separated/divorced |
11.6 | 12.0 |
|
Widowed |
5.9 | 6.0 |
|
Never married |
14.3 | 13.7 |
| Lives with the care recipient | ||
|
Yes |
43.8 | 42.2 |
| Children younger than 18 | ||
|
None |
82.9 | 81.0 |
|
Any |
15.7 | 17.1 |
NOTES: Includes family caregivers of Medicare beneficiaries age 65 and older in the continental United States who resided in community or residential care settings (other than nursing homes) and received help with self-care, mobility, or household activities for health or functioning reasons. “High-need” refers to caregivers of older adults who have probable dementia or need assistance with two or more self-care activities (bathing, dressing, eating, toileting, or getting in and out of bed). Percentages may not total 100 due to missing data.
SOURCES: Data from the 2011 NHATS and the companion NSOC.
likely many others because stepchildren and sons- and daughters-in-law are not eligible for FMLA benefits (see Table 2-6).5,6 Half of the NSOC caregivers (50.3 percent) were employed.
Same-generation caregivers (usually an older adult’s spouse) have different physical and cognitive capabilities and commitment to caregiving than next-generation caregivers (usually an older adult’s children). Because same-generation caregivers of older adults are older than next-generation caregivers, they are at a higher risk of age-related physical and cognitive declines including chronic illness and some level of disability. Same-generation caregivers are also more likely to feel that caregiving is an obligation. A recent study found that 60 percent of spousal caregivers reported having no choice in taking on the caregiving role while 51 percent of adult children reported having no choice (Schulz et al., 2012).
Concern is growing about the impact of caregiving on those who live far from care recipients because of the expense of travel, difficulties in communication about care recipients’ health and LTSS needs, and other logistical challenges in meeting someone’s needs from a distance (Bevan et al., 2012; Cagle and Munn, 2012; Wolf and Longino, 2005). Nevertheless, evidence suggests that most family caregivers live near the care recipient if they do not live together (Johnson and Wiener, 2006; NAC and AARP Public Policy Institute, 2015b; Spillman and Pezzin, 2000; Wolff and Kasper, 2006). A large proportion of NSOC respondents (43.8 percent) live with the care recipient (also known as co-residents), including high-need individuals (see Table 2-6). This is an important group because, as Chapter 3 will discuss, co-resident caregivers are at increased risk of adverse physical and psychological outcomes (Monin and Schulz, 2009; Schulz et al., 2007, 2009). Spouses who are caregivers of older adults are especially vulnerable to such adverse outcomes (Capistrant et al., 2012; Dassel and Carr, 2014; Ji et al., 2012; Schulz et al., 2009). More than one in five (21.5 percent) NSOC caregivers were spouses.
The racial and ethnic makeup of the caregiver population in 2011 largely reflected the overall U.S. population, including the racial and ethnic makeup of the high-need caregiver group (see Table 2-5). One important gap in nationally representative survey data, such as NSOC, is the incompleteness of data about the prevalence and characteristics among diverse subgroups of caregivers. Data from non-representative samples suggests that important differences may exist. For example, a meta-analysis of 116
___________________
5 FMLA requires certain employers to provide job-protected, unpaid leave to employees caring for certain seriously ill family members. See Chapter 4 for a review of FMLA and other workplace issues affecting family caregivers.
6 The number of caregivers who are stepchildren or in-laws of care recipients cannot be calculated from NSOC data.
caregiving studies in the gerontological literature found that multicultural caregivers were more likely to be younger, non-spouses and to be less well-off economically compared with white non-Hispanic caregivers, though the effect sizes were modest (Pinquart and Sörensen, 2005). Trends in the racial and ethnic makeup of the United States are reviewed below.
SOCIAL AND DEMOGRAPHIC TRENDS AFFECTING CAREGIVING
A number of current and future social and demographic trends will likely affect both the need for eldercare and the availability of potential family caregivers for older adults in the future. In 2012, 43.1 million or 13.7 percent of U.S. residents were age 65 and older (see Table 2-7). At
| Number (in 1,000s) | Percentage of U.S. Population | |
|---|---|---|
| Total U.S. population | 313,914 | 100.0 |
|
65+ |
43,145 | 13.7 |
| Age cohorts | Percentage of 65+ population | |
|
65-69 |
13,977 | 32.4 |
|
70-74 |
10,008 | 23.2 |
|
75-79 |
7,490 | 17.4 |
|
80-84 |
5,783 | 13.4 |
|
85+ |
5,887 | 13.6 |
| Race | ||
|
White |
37,095 | 86.0 |
|
Black |
3,781 | 8.8 |
|
American Indian or Alaska Native |
266 | .6 |
|
Asian |
1,628 | 3.8 |
|
Pacific Islander |
42 | .1 |
|
Two or more races |
333 | .8 |
| Hispanic origin | ||
|
Hispanic |
3,144 | 7.3 |
|
Non-Hispanic |
40,002 | 92.7 |
NOTE: The above U.S. Census racial categories are defined as white (with origins in Europe, the Middle East, or North Africa), Black or African American (with origins in the black racial groups of Africa), Asian (with origins in the Far East, Southeast Asia, or the Indian subcontinent), Native Hawaiian or other Pacific Islander, American Indians or Alaska Natives, and “some other race.”
SOURCE: Ortman et al., 2014.
that time, 86 percent of the older adult population was white; 8.8 percent, African American; 7.3 percent, of Hispanic origin (any race); 3.8 percent, Asian; and 1.5 percent, others (American Indian, Alaska Native, Pacific Islander, or multiracial). This one-time snapshot, however, belies an older population that is rapidly changing not only in numbers and racial and ethnic makeup, but in numerous other ways. The nation is in the midst of historic demographic change that has substantial implications for older adults and their families, providers of health care services and LTSS, the national economy, and society overall (Colby and Ortman, 2014; Frey, 2014; IOM, 2008; Mather et al., 2015; NRC, 2012). These trends, described below, make clear that in the future, if not now, the older adult population needing help is likely to exceed the capacity of family caregivers to provide it. The effects of these unprecedented demographic trends will depend, in part, on the actions that public and private decision makers take in the coming years to lessen the strain on the daily lives of caregiving families.
Rapidly Increasing Numbers Especially Among the Oldest Old
Much has been written about the aging of the baby boomer population (Colby and Ortman, 2014; IOM, 2008; Frey, 2014; Mather et al., 2015). According to the U.S. Census, by 2030—just 14 years after the publication of this report—more than one in five of U.S. residents will be age 65 or older (see Figure 2-3) (Ortman et al., 2014). This represents a 40.7 percent increase in the size of the older population between 2012 and 2030. By contrast, the overall U.S. population is expected to grow only 12.4 percent—from 313.9 million to 358.5 million—during the same time period.
The dramatic rise in the total number of older Americans is not due solely to the increasing numbers of baby boomers turning 65. Older adults—whether male or female, white or African American, Hispanic or non-Hispanic—are expected to live increasingly longer lives in future decades (Ortman et al., 2014). With increasing life spans and the growing older adult boomer population, the U.S. Census Bureau projects significant growth in the number of the oldest of the older age groups. For example, the projection for 2030 is that more than 19 million U.S. residents will be age 80 or older; by 2050, this population is forecast to grow to more than 30 million (Ortman et al., 2014). The impact of the age distribution of the older adult population on the need for family caregiving is likely to be substantial. The number of individuals most likely to need intensive support from family caregivers—people in their 80s and beyond—is growing the fastest among the older age cohorts. From 2012 to 2050, the proportion of the U.S. older adult population, age 80 and older, is projected to climb from 27 to 37 percent (Ortman et al., 2014).
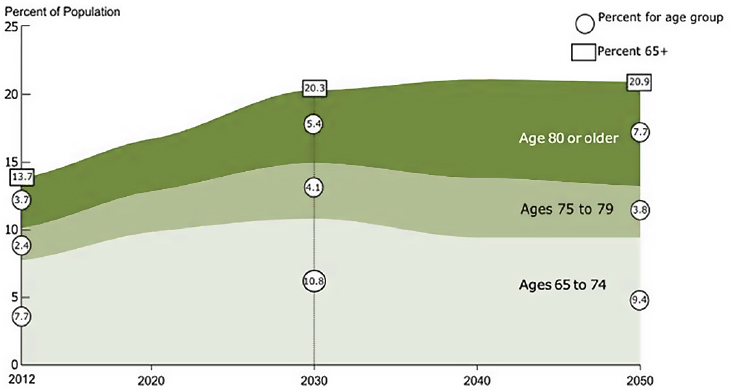
SOURCE: Data drawn from Ortman et al., 2014.
Increasing Diversity
The U.S. population is becoming older, and while non-Hispanic whites today remain the largest single group of older adults, the nation is experiencing a historic shift in the diversity of older racial and ethnic groups (Frey, 2014). Sometime after 2040, no racial or ethnic group will make up the majority of the U.S. population (Frey, 2014). These changes will bring an evolution in the values, preferences, and meanings that individuals bring to family caregiving. Over the coming decades, America’s Hispanic, Asian, and multiracial populations are each expected to more than double in number. Figure 2-4 illustrates the impact of this trend on the makeup of the population older than 65. In 2030, 20.2 million of the 72.8 million older Americans will identify as a member of a minority group. The older Hispanic population is growing faster than any other older age group. In 2030, there will be more than 8 million older Hispanic adults—nearly triple the number 30 years earlier and surpassing the number of African American older adults (7.5 million) (PRB, 2013). During the same period, the number of older, non-Hispanic Asians is forecast to increase from 1.5 million to 3.5 million. By the year 2060, 56 percent of adults ages 65 and older are expected to be non-Hispanic whites (U.S. Census Bureau, 2012).
The literature on caregiving across sexual minorities is sparse. What
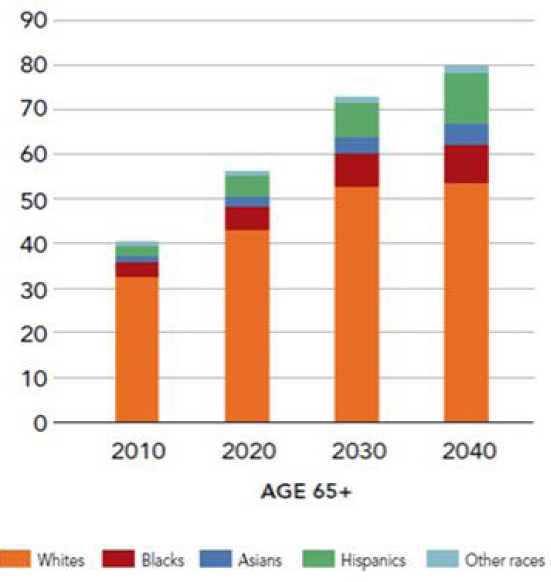
SOURCE: Adapted from Frey, 2014 (Figure 1.3).
does exist indicates that the caregiving experience for persons who identify with the LGBT community is similar to non-LGBT persons. LGBT individuals are more likely to provide care, or receive care, for or from a non-relative than non-LGBT individuals (Fredriksen-Goldsen et al., 2011). How much of this is due to the differing definition of spouse/partner than in the heterosexual community is not known. A recurring problem in empirical studies is the lack of rigorous sampling designs: most samples are small, regional, and lack generalizability, and do not focus on the heterogeneity across specific groups of sexual minorities (Fredriksen-Goldsen and Hooyman, 2007).
Changes in diversity are important for several reasons. First, the nation is moving toward person- and family-centered care as major tenets of quality health care and LTSS. Included in this quality improvement strategy is the idea that respecting the person’s and family’s values, beliefs, and prefer-
ences can improve individual and population health (NQF, 2014). Second, this has far-reaching implications for the provider workforce. Studies show that people often prefer to be treated by health care professionals of the same racial or ethnic background (Acosta and Olsen, 2006; IOM, 2004; Mitchell and Lassiter, 2006; Tarn et al., 2005). Also, a provider from a person’s own background may have a better understanding of culturally appropriate demonstrations of respect for older adults and may also be more likely to speak the same language (Yeo, 2009). For LGBT persons, discrimination by service providers is a major concern; another issue is the lack of culturally appropriate resources for both caregivers and older individuals (Fredriksen-Goldsen and Hooyman, 2007; Fredriksen-Goldsen et al., 2011). Family or surrogate family caregivers are likely to be the best able to provide culturally appropriate care according to the preferences of individual older adults.
Developing programs and services that are both accessible and tailored to the needs of diverse communities of caregivers presents significant challenges. Functional impairments tend to be more prevalent in older minority groups (Schoeni et al., 2009). Moreover, while older adults, in general, are expected to live longer lives in the future, persistent disparities in life expectancy are likely to widen (Olshansky et al., 2012). Much of this difference is associated with disparities in income, education, neighborhood environments, lifetime access to health care, and occupational hazards (PRB, 2013).
Yet, as noted earlier, caregiving research is greatly hampered by the lack of robust data on important differences among subgroups. In the future, federal and other sponsors of population surveys should make the necessary investment to increase sampling of older adults and caregivers to enable meaningful subgroup analyses. Consistent, reliable investment in longitudinal tracking of older adults and their caregivers is also needed.
Changing Family Structures
Caregiving for older adults in the future will depend, in part, on the availability and capacity of their family members to assist them. In previous generations, older adults could often count on large, extended families for help with health and functioning needs—although in most cases the caregiver was either a wife or adult daughter as they are today (Wolff and Kasper, 2006). Current trends in family patterns—including lower fertility, higher rates of childlessness, changes in traditional family structures, and increases in divorce and never-married status—lead to smaller families (especially available children and spouses), which portends a shrinking pool of potential caregivers (Redfoot et al., 2013).
The size of American families continues to drop and, as a consequence, the number of adult children available to help an older parent is declining (see Figure 2-5). Moreover, adult daughters, the backbone of caregiving, are far more likely to be in the workforce and also geographically distant. In addition, as older adults live into their 80s, 90s, and older, their aging children themselves may be living with chronic health problems and limitations in functioning.
Childlessness has also risen across racial and ethnic groups. In the 1970s, 10 percent of American women ended their childbearing years without having a child (Livingston and Cohn, 2010). By 2008, this proportion had doubled to nearly 20 percent. Johnson and colleagues estimate that, from 2010 to 2040, the percentage of frail older adults without a living child will increase from 14 to 21 percent and the percentage with only one or two children will increase from 38 to 49 percent (Johnson et al., 2007) (see Figure 2-5).
Marital status is closely associated with the availability of caregivers and social supports as well as overall economic well-being (Federal Interagency Forum on Aging-Related Statistics, 2012; PRB, 2013). Older adults—particularly women—are less likely to be widowed than in the past (West et al., 2014). Although this may suggest that spouses can be expected to play a greater role in caregiving, other factors suggest otherwise. Between
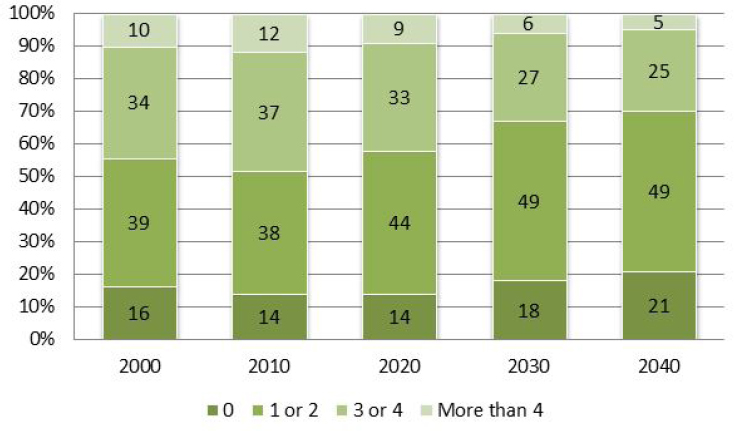
SOURCE: Johnson et al., 2007.
1990 and 2010, the divorce rates among adults ages 50 and older doubled (Brown and Lin, 2012) and an increasing proportion of women never marry (Jacobsen et al., 2011). Between 1986 and 2009, for example, the percentage of never-married, 50- to 54-year-old non-Hispanic white women tripled from 2.6 to 7.8 percent (Kreider and Ellis, 2011). Among African American women of the same age, the percentage increased fourfold from 6.3 to 24.5 percent. Additionally, LGBT older adults often do not have the same family support systems as heterosexual older adults, particularly because LGBT older adults are less likely to have children and are more likely to live alone (Cahill et al., 2000).
Non-traditional households and complex family structures are far more common than in the past. This change has important implications for family caregiving because adult stepchildren may have weaker feelings of obligation and provide less care to their aging stepparents than their parents (Pew Research Center, 2010; Silverstein and Giarrusso, 2010; van der Pas et al., 2013). Research also shows that divorce negatively impacts the quality of intergenerational relationships between older parents and their adult children and reduces resource transfers from parents to children (Wolf, 2001). Additional research is needed to fully understand how these trends in family structures affect the care of aging adults (Silverstein and Giarrusso, 2010; van der Pas et al., 2013).
In combination, race/ethnicity, low income, and limited education are strongly associated with poor health status and increased functional limitations among older persons (Crimmins and Saito, 2001; Molla et al., 2004; Olshansky et al., 2012). Gender and living arrangement are also important correlates of poverty in old age. Compared to men of the same age in every racial and ethnic group, older women have much higher levels of poverty. They are also more likely to be living alone. In 2014, more than one-third of women (35 percent) older than age 64 lived alone compared to 19 percent of men of the same age (ACL, 2015). The share of older women living alone is substantially higher: 42 percent among women ages 75 to 84 and more than half (56 percent) of women ages 85 and older (U.S. Census Bureau, 2014). The risk of poor health status and poverty that is associated with living alone is particularly worrisome in light of current trends in marriage, divorce, and family size.
Women in the Workforce
As discussed in Chapter 4, more than half of family caregivers of older adults are employed. This proportion is increasing, largely driven by the growing numbers of adult daughters and wives who work (Stone, 2015). In the four decades leading to 2012, women’s participation in the workforce grew by 19 percent, from about one in three women to more than half of
women (Toossi, 2013). The U.S. Bureau of Labor Statistics projects that women’s participation in the workforce will continue to increase during the same years that they are most likely to be caregiving (Toossi, 2013). The percentage of women older than age 54 who work, for example, is expected to increase from 35.1 percent in 2012 to 37.5 percent in 2022. During the same period, the percentage of working women older than age 64—those most likely to be caring for a spouse—is expected to increase from 14.4 to 19.5 percent (Toossi, 2013). This trend is likely to contribute to the widening gap between the supply and demand for family caregivers of older adults.
CONCLUSIONS
The committee’s key findings and conclusions are described in detail in Box 2-1. In summary, this chapter raises profound concerns about the nation’s capacity to meet the needs of its elders. The United States is undergoing historic demographic changes that have significant implications for current and future policy regarding family caregivers of older adults. By 2030, more than one in five U.S. residents will be age 65 or older. Much of the growth in the older population will be among those most likely to need intensive support—people age 80 and older.
While the need for caregiving is rapidly increasing, the size of the potential family caregiver “workforce” is shrinking. Current trends in family patterns, including lower fertility, higher rates of childlessness, and increases in divorce and never-married status, portend a shrinking pool of potential caregivers in the near future. Unlike in the past, older adults will have fewer family members to rely on, may be geographically distant from their children and live alone, and are more likely to be unmarried or divorced.
The committee has relied heavily on national data on older adults and their family caregivers and projections made by others who have used these data to identify the scope of problems related to family caregiving. National data on family caregiving and caregivers will be important in monitoring future progress and challenges in family caregiving. As the population of older adults and their caregivers change in diversity, gender, identity, living arrangements, reliance on new technology, and other ways, national data collection needs to change correspondingly. Without adequate data on family caregivers and caregiving, public and private decision makers will not have the evidence base on which to make sound decisions. Despite the limitations in the available data, the NHATS and NSOC findings presented in this chapter have important implications for individuals and families, as well as policy makers, health and social service providers, employers, and others—particularly in light of the consequences of family caregiving reviewed later in this report. At a minimum, they underscore the enormous commitment of time that family caregivers contribute to the well-being of the large and growing numbers of older Americans with physical and/or cognitive limitations. Yet it is not clear that Americans understand and appreciate the amount of time and the likely demands of being a caregiver sometime in the future. Raising awareness and public education about the needs and challenges of family caregiving of older adults will be a critical step toward preparing the nation as a whole.
REFERENCES
ACL (Administration for Community Living). 2015. A profile of older Americans: 2014. http://www.aoa.acl.gov/Aging_Statistics/Profile/2014/docs/2014-Profile.pdf (accessed May 12, 2015).
Acosta, D., and P. Olsen. 2006. Meeting the needs of regional minority groups: The University of Washington’s programs to increase the American Indian and Alaskan Native physician workforce. Academic Medicine 81(10):863-870.
Adams, P. F., W. K. Kirzinger, and M. E. Martinez. 2013. Summary health statistics for the U.S. population: National Health Interview Survey, 2012. Vital Health Statistics 10(259).
Anderson, G. 2010. Chronic care: Making the case for ongoing care. http://www.rwjf.org/content/dam/farm/reports/reports/2010/rwjf54583 (accessed May 25, 2015).
Bevan, J. L., S. K. Vreeburg, S. Verdugo, and L. Sparks. 2012. Interpersonal conflict and health perceptions in long-distance caregiving relationships. Journal of Health Communication 17(7):747-761.
Black, B. S., D. Johnston, P. V. Rabins, A. Morrison, C. Lyketsos, and Q. M. Samus. 2013. Unmet needs of community-residing persons with dementia and their informal caregivers: Findings from the Maximizing Independence at Home Study. Journal of the American Geriatrics Society 61(12):2087-2095.
Brown, S. L., and I.-F. Lin. 2012. The gray divorce revolution: Rising divorce among middle-aged and older adults, 1990-2010. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 67(6):731-741.
Cagle, J. G., and J. C. Munn. 2012. Long-distance caregiving: A systematic review of the literature. Journal of Gerontological Social Work 55(8):682-707.
Cahill, S., K. South, and J. Spade. 2000. Outing age: Public policy issues affecting gay, lesbian, bisexual, and transgender elders. New York: Policy Institute of the National Gay and Lesbian Taskforce.
Capistrant, B. D., J. R. Moon, L. F. Berkman, and M. M. Glymour. 2012. Current and long-term spousal caregiving and onset of cardiovascular disease. Journal of Epidemiology and Community Health 66(10):951-956.
Chadiha, L. A., S. Feld, and J. Rafferty. 2011. Likelihood of African American primary caregivers and care recipients receiving assistance from secondary caregivers: A rural-urban comparison. Journal of Applied Gerontology 30(4):422-442.
CMS (Centers for Medicare & Medicaid Services). 2012. Chronic conditions among Medicare beneficiaries, Chartbook, 2012 ed.http://www.cms.gov/Research-Statistics-Data-andSystems/Statistics-Trends-and-Reports/Chronic-Conditions/Downloads/2012Chartbook.pdf (accessed April 23, 2015).
Colby, S. L., and J. M. Ortman. 2014. The baby boom cohort in the United States: 2012 to 2060. Current Population Reports, P25-1141. https://www.census.gov/prod/2014pubs/p25-1141.pdf (accessed April 30, 2015).
Crimmins, E. M., and Y. Saito. 2001. Trends in healthy life expectancy in the United States, 1970-1990: Gender, racial, and educational differences. Social Science & Medicine 52(11):1629-1641.
Dassel, K. B., and D. C. Carr. 2014. Does dementia caregiving accelerate frailty? Findings from the Health and Retirement Study. The Gerontologist 56(3):444-450.
Favreault, M., and J. Dey. 2015. ASPE issue brief. Long-term services and supports for older Americans: Risks and financing research brief. Revised February 2016. http://aspe.hhs.gov/basic-report/long-term-services-and-supports-older-americans-risks-and-financingresearch-brief (accessed March 24, 2016).
Feder, J. 2015. The challenge of financing long-term care. St. Louis University Journal of Health Law and Policy 8(1):47-60.
Federal Interagency Forum on Aging-Related Statistics. 2012. Older Americans 2012: Key indicators of well-being. http://www.agingstats.gov/agingstatsdotnet/Main_Site/Data/2012_Documents/Docs/EntireChartbook.pdf (accessed April 29, 2015).
Fredriksen-Goldsen, K. I., and N. R. Hooyman. 2007. Caregiving research, services, and policies in historically marginalized communities. Journal of Gay & Lesbian Social Services 18(3-4):129-145.
Fredriksen-Goldsen, K., H. Kim, C. Emlet, A. Muraco, E. Erosheva, C. Hoy-Ellis, J. Goldsen, and H. Petry. 2011. The aging and health report: Disparities and resilience among lesbian, gay, bisexual, and transgender older adults. http://caringandaging.org/wordpress/wp-content/uploads/2011/05/Full-Report-FINAL-11-16-11.pdf (accessed July 1, 2016).
Freedman, V. A., and B. C. Spillman. 2014a. Disability and care needs among older Americans. Milbank Quarterly 92(3):509-541.
Freedman, V. A., and B. C. Spillman. 2014b. The residential continuum from home to nursing home: Size, characteristics and unmet needs of older adults. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 69(Suppl 1):S42-S50.
Freedman, V. A., J. D. Kasper, J. C. Cornman, E. M. Agree, K. Bandeen-Roche, V. Mor, B. C. Spillman, R. Wallace, and D. A. Wolf. 2011. Validation of new measures of disability and functioning in the National Health and Aging Trends Study. Journal of Gerontology 66A(9):1013-1021.
Freedman, V. A., B. C. Spillman, P. M. Andreski, J. C. Cornman, E. M. Crimmins, E. Kramarow, J. Lubitz, L. G. Martin, S. S. Merkin, R. F. Schoeni, T. E. Seeman, and T. A. Waidmann. 2013. Trends in late-life activity limitations in the United States: An update from five national surveys. Demography 50(2):661-671.
Freedman, V. A., J. D. Kasper, B. C. Spillman, E. M. Agree, V. Mor, R. B. Wallace, and D. A. Wolf. 2014. Behavioral adaptation and late-life disability: A new spectrum for assessing public health impacts. American Journal of Public Health 104(2):e88-e94.
Frey, W. 2014. A pivotal period for race in America. In Diversity explosion: How new racial demographics are remaking America. Washington, DC: Brookings Institution Press.
Gaudette, E., B. Tysinger, A. Cassil, and D. Goldman. 2015. Strengthening Medicare for 2030: Health and health care of Medicare beneficiaries in 2030.http://www.brookings.edu/~/media/Research/Files/Papers/2015/06/04-medicare-2030-paper-series/Medicare2030_Chartbook.pdf (accessed April 5, 2016).
Giovannetti, E. R., and J. L. Wolff. 2010. Cross-survey differences in national estimates of numbers of caregivers of disabled older adults. The Milbank Quarterly 88(3):310-349.
Grossman, A., A. D’Augelli, and E. Dragowski. 2007. Caregiving and care receiving among older lesbian, gay, and bisexual adults. Journal of Gay & Lesbian Social Services 18(3/4):15-38.
He, W., and L. J. Larsen. 2014. Older Americans with a disability: 2008-2012. U.S. Census Bureau. American Community Survey Reports (ACS-29). https://www.census.gov/content/dam/Census/library/publications/2014/acs/acs-29.pdf (accessed May 14, 2015).
Hughes, M., and S. Kentlyn. 2011. Older LGBT people’s care networks and communities of practice: A brief note. International Social Work 54(3):436-444.
IOM (Institute of Medicine). 2004. In the nation’s compelling interest: Ensuring diversity in the health care workforce. Washington, DC: The National Academies Press.
IOM. 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
Jacobsen, L. A., M. Mather, and M. Lee. 2011. America’s aging population. Population bulletin 66, no. 1. http://www.prb.org/pdf11/aging-in-america.pdf (accessed May 26, 2015).
Ji, J., B. Zoller, K. Sundquist, and J. Sundquist. 2012. Increased risks of coronary heart disease and stroke among spousal caregivers of cancer patients. Circulation 125(14):1742-1747.
Johnson, R. W., and J. M. Wiener. 2006. A profile of frail older Americans and their caregivers. Washington, DC: Urban Institute.
Johnson, R. W., D. Toohey, and J. M. Wiener. 2007. Meeting the long-term care needs of the baby boomers: How changing families will affect paid helpers and institutions. http://www.urban.org/UploadedPDF/311451_Meeting_Care.pdf (accessed April 9, 2015).
Kasper, J. D., V. A. Freedman, and B. C. Spillman. 2013. Classification of persons by dementia status in the National Health and Aging Trends Study. https://www.nhats.org/scripts/documents/NHATS_Dementia_Technical_Paper_5_Jul2013.pdf (accessed May 20, 2015).
Kasper, J. D., V. A. Freedman, and B. Spillman. 2014. Disability and care needs of older Americans by dementia status: An analysis of the 2011 National Health and Aging Trends Study.http://aspe.hhs.gov/daltcp/reports/2014/NHATS-DS.pdf (accessed February 4, 2015).
Kaye, H. S. 2013. Disability rates for working-age adults and for the elderly have stabilized, but trends for each mean different results for costs. Health Affairs 32(1):127-134.
Kids Count Data Center. 2015. Adult population by race.http://datacenter.kidscount.org/data/Tables/6539-adult-population-by-race?loc=1&loct=1#detailed/1/any/false/ 869,36,868,867,133/68,69,67,12,70,66,71,2800/13517,13518 (accessed March 7, 2016).
Kreider, R. M., and R. Ellis. 2011. Number, timing and duration of marriages and divorces: 2009. U.S. Census Bureau Current Population Reports.https://www.census.gov/prod/2011pubs/p70-125.pdf (accessed May 29, 2015).
Livingston, G., and D. Cohn. 2010. Childlessness up among all women; down among women with advanced degrees. Pew Research Social and Demographic Trends. http://www.pewsocialtrends.org/files/2010/11/758-childless.pdf (accessed May 28, 2015).
Marks, N. F. 1996. Caregiving across the lifespan: National prevalence and predictors. Family Relations 45(1):27-36.
Mather, M., L. A. Jacobsen, and K. M. Pollard. 2015. Aging in the United States. Population Bulletin 70(2):1-18.
Mayer, G. 2013. The Family and Medical Leave Act (FMLA): Policy issues. http://digitalcommons.ilr.cornell.edu/cgi/viewcontent.cgi?article=2316&context=key_workplace (accessed July 18, 2016).
Mitchell, D. A., and S. L. Lassiter. 2006. Addressing health care disparities and increasing workforce diversity: The next step for the dental, medical, and public health professions. American Journal of Public Health 96(12):2093-2097.
Miyawaki, C. E. 2016. Caregiving practice patterns of Asian, Hispanic, and non-Hispanic white American family caregivers of older adults across generations. Journal of Cross-Cultural Gerontology 31(1):35-55.
Molla, M. T., J. H. Madans, and D. K. Wagener. 2004. Differentials in adult mortality and activity limitation by years of education in the United States at the end of the 1990s. Population and Development Review 30(4):625-646.
Monin, J. K., and R. Schulz. 2009. Interpersonal effects of suffering in older adult caregiving relationships. Psychology and Aging 24(3):681-695.
NAC (National Alliance for Caregiving) and AARP Institute. 1997. Family caregiving in the U.S.: Findings from a national survey. http://www.caregiving.org/data/04finalreport.pdf (accessed July 18, 2016).
NAC and AARP Institute. 2004. Caregiving in the U.S.http://www.caregiving.org/data/04finalreport.pdf (accessed July 18, 2016).
NAC and AARP Institute. 2009. Caregiving in the U.S.: A focused look at those caring for someone age 50 or older. http://www.caregiving.org/pdf/research/FINALRegularExSum50plus.pdf (accessed April 14, 2015).
NAC and AARP Public Policy Institute. 2015a. 2015 report: Caregiving in the U.S.http://www.caregiving.org/wp-content/uploads/2015/05/2015_CaregivingintheUS_FinalReport-June-4_WEB.pdf (accessed August 4, 2015).
NAC and AARP Public Policy Institute. 2015b. Caregivers of older adults: A focused look at those caring for someone age 50+. http://www.aarp.org/content/dam/aarp/ppi/2015/caregivers-of-older-adults-focused-look.pdf (accessed August 5, 2015).
NIH (National Institutes for Health). 2010. Fact sheet—disability in older adults. http://report.nih.gov/nihfactsheets/Pdfs/DisabilityinOlderAdults(NIA).pdf (accessed May 19, 2015).
NQF (National Quality Forum). 2014. Final report: Addressing performance measure gaps in person-centered care and outcomes.http://www.qualityforum.org/Publications/2014/08/Priority_Setting_for_Healthcare_Performance_Measurement__Addressing_Performance_Measure_Gaps_in_Person-Centered_Care_and_Outcomes.aspx (accessed December 4, 2015).
NRC (National Research Council). 2012. Aging and the macroeconomy: Long-term implications of an older population. Washington, DC: The National Academies Press.
Olshansky, S. J., T. Antonucci, L. Berkman, R. H. Binstock, A. Boersch-Supan, J. T. Cacioppo, B. A. Carnes, L. L. Carstensen, L. P. Fried, D. P. Goldman, J. Jackson, M. Kohli, J. Rother, Y. H. Zheng, and J. Rowe. 2012. Differences in life expectancy due to race and educational differences are widening, and many may not catch up. Health Affairs 31(8):1803-1813.
Ortman, J. M., V. A. Velkoff, and H. Hogan. 2014. An aging nation: The older population in the United States. http://www.census.gov/prod/2014pubs/p25-1140.pdf (accessed April 15, 2015).
Penrod, J. D., R. Kane, R. A. Kane, R. L. Kane, and M. D. Finch. 1995. Who cares? The size, scope and composition of the caregiver support system. The Gerontologist 35(4):489-497.
Pew Research Center. 2010. The decline of marriage and the rise of new families. Washington, DC: Pew Research Center. http://www.pewsocialtrends.org/files/2010/11/pew-socialtrends-2010-families.pdf (accessed July 1, 2016).
Pinquart, M., and S. Sörensen. 2005. Ethnic differences in stressors, resources, and psychological outcomes of family caregiving: A meta-analysis. The Gerontologist 45(1):90-106.
Pinquart, M., and S. Sörensen. 2006. Gender differences in caregivers’ stressors, social resources, and health: An updated meta-analysis. The Journals of Gerontology Series B: Psychological Sciences 61(1):33-45.
PRB (Population Reference Bureau). 2013. The health and life expectancy of older blacks and Hispanics in the United States. http://www.prb.org/pdf13/TodaysResearchAging28.pdf (accessed May 25, 2015).
Redfoot, D., L. Feinberg, and A. Houser. 2013. The aging of the baby boom and the growing care gap: A look at future declines in the availability of family caregivers. http://www.aarp.org/content/dam/aarp/research/public_policy_institute/ltc/2013/baby-boom-and-thegrowing-care-gap-insight-AARP-ppi-ltc.pdf (accessed August 7, 2015).
Schoeni, R. F., V. A. Freedman, and L. G. Martin. 2009. Socioeconomic and demographic disparities in trends in old-age disability. In Health at older ages: The causes and consequences of declining disability among the elderly, edited by D. Cutler and D. A. Wise. Chicago, IL: University of Chicago Press.
Schulz, R., R. S. Hebert, M. A. Dew, S. L. Brown, M. F. Scheier, S. R. Beach, S. J. Czaja, L. M. Martire, D. Coon, K. M. Langa, L. N. Gitlin, A. B. Stevens, and L. Nichols. 2007. Patient suffering and caregiver compassion: New opportunities for research, practice, and policy. The Gerontologist 47(1):4-13.
Schulz, R., S. R. Beach, R. S. Hebert, L. M. Martire, J. K. Monin, C. A. Tompkins, and S. M. Albert. 2009. Spousal suffering and partner’s depression and cardiovascular disease: The Cardiovascular Health Study. The American Journal of Geriatric Psychiatry 17(3):246-254.
Schulz, R., S. R. Beach, T. B. Cook, L. M. Martire, J. M. Tomlinson, and J. K. Monin. 2012. Predictors and consequences of perceived lack of choice in becoming an informal caregiver. Aging & Mental Health 16(6):712-721.
Social Security Trustees Report. 2015. The 2015 annual report of the Board of Trustees of the Federal Old-Age and Survivors Insurance and Federal Disability Insurance Trust Funds. https://www.ssa.gov/oact/tr/2015/tr2015.pdf (accessed July 18, 2016).
Spillman, B. C., and L. E. Pezzin. 2000. Potential and active family caregivers: Changing networks and the “Sandwich Generation.” Milbank Quarterly 78(3):347-374.
Stone, R. I. 2015. Factors affecting the future of family caregiving in the United States. In Family caregiving in the new normal, edited by J. E. Gaugler and R. L. Kane. London, UK: Elsevier.
Silverstein, M. and R. Giarrusso. 2010. Aging and family life: A decade review. Journal of Marriage and Family 72(5):1039-1058.
Tarn, D. M., L. S. Meredith, M. Kagawa-Singer, S. Matsumura, S. Bito, R. K. Oye, H. Liu, K. L. Kahn, S. Fukuhara, and N. S. Wenger. 2005. Trust in one’s physician: The role of ethnic match, autonomy, acculturation, and religiosity among Japanese and Japanese Americans. The Annals of Family Medicine 3(4):339-347.
Tennstedt, S. L., J. B. McKinlay, L. M. Sullivan. 1989. Informal care for frail elders: The role of secondary caregiver. The Gerontologist 29(5):677-683.
Toossi, M. 2013. Monthly labor review. Labor force projection to 2022: The labor force participation rate continues to fall.http://www.bls.gov/opub/mlr/2013/article/labor-forceprojections-to-2022-the-labor-force-participation-rate-continues-to-fall.htm (accessed September 10, 2015).
U.S. Census Bureau. 2012. U.S. Census Bureau projections show a slower growing, older, more diverse nation a half century from now. https://www.census.gov/newsroom/releases/archives/population/cb12-243.html (accessed April 12, 2016).
U.S. Census Bureau. 2014. 2014 Current Population Survey, Annual Social and Economic Supplement.http://ceprdata.org/wp-content/cps/CPS_March_Codebook_2014_traditional.pdf (accessed August 22, 2016).
U.S. Census Bureau. 2016a. American FactFinder. http://factfinder.census.gov/faces/nav/jsf/pages/index.xhtml (accessed March 29, 2016)
U.S. Census Bureau. 2016b. Table HINC-01. Selected characteristics of households, by total money income in 2014. http://www.census.gov/hhes/www/cpstables/032015/hhinc/hinc01_000.htm (accessed January 12, 2016).
van der Pas, S., T. G. Van Tilburg, and M. Silverstein. 2013. Stepfamilies in later life. Journal of Marriage and Family 75(5):1065-1069.
West, L. A., S. Cole, D. Goodkind, and W. He. 2014. 65+ in the United States: 2010. Washington, DC: U.S. Government Printing Office.
Wolf, D. A. 2001. Population change: Friend or foe of the chronic care system? Health Affairs 20(6):28-42.
Wolf, D. A., and C. F. Longino. 2005. “Our increasingly mobile society”? The curious persistence of a false belief. The Gerontologist 45(1):5-11.
Wolff, J. L., and B. J. Jacobs. 2015. Chronic illness trends and the challenges to family caregivers: Organizational and health system barriers. In Family caregiving in the new normal, edited by J. E. Gaugler and R. L. Kane. Oxford, UK: Elsevier. Pp. 79-104.
Wolff, J. L., and J. D. Kasper. 2006. Caregivers of frail elders: Updating a national profile. The Gerontologist 46(3):344-356.
Yee, J. L., and R. Schulz. 2000. Gender differences in psychiatric morbidity among family caregivers: A review and analysis. The Gerontologist 40(2):147-164.
Yeo, G. 2009. How will the U.S. healthcare system meet the challenge of the ethnogeriatric imperative? Journal of the American Geriatrics Society 57(7):1278-1285.
This page intentionally left blank.






























