BS
Summary
The Centers for Medicare & Medicaid Services (CMS) have been moving from volume-based, fee-for-service payment to value-based payment (VBP), which aims to improve health care quality, health outcomes, and patient care experiences, while also controlling costs. Since the passage of the Patient Protection and Affordable Care Act in 2010, CMS has implemented a variety of VBP strategies, including incentive programs and risk-based alternative payment models such as bundled (episode-based) payments and accountable care organizations (Burwell, 2015). Emerging evidence suggests that providers disproportionately serving patients with social risk factors for poor health outcomes may be more likely to fare poorly on quality rankings and to receive financial penalties, and less likely to receive financial rewards (Berenson and Shih, 2012; Chien et al., 2007; Friedberg et al., 2010; Gilman et al., 2014, 2015; Joynt and Jha, 2013; Joynt and Rosenthal, 2012; Joynt et al., 2011; Karve et al., 2008; Ly et al., 2010; MedPAC, 2013; Mehta et al., 2008; Rajaram et al., 2015; Ryan, 2013; Shih et al., 2015; Sjoding and Cooke, 2014; Williams et al., 2014). However, an analysis of actual penalties incurred under the Hospital Readmissions Reduction Program for fiscal year 2013 reported that safety-net hospitals incurred only slightly higher penalties than non–safety-net hospitals (Sheingold et al., 2016). The drivers of these disparities in both health care quality and health outcomes are poorly understood, and differences in interpretation have led to divergent concerns about the potential effect of VBP on health equity.1
STATEMENT OF TASK
In an effort to better distinguish the drivers of variations in performance among providers disproportionately serving socially at-risk populations and to identify methods to account for social risk factors in Medicare payment programs, the Department of Health and Human Services acting through the Office of the Assistant Secretary of Planning and Evaluation (ASPE), contracted with the National Academies of Sciences, Engineering, and Medicine to convene an ad hoc committee to identify best practices of high-performing hospitals, health plans, and other providers that serve disproportionately higher shares of socioeconomically disadvantaged populations and compare those best practices to practices of low-performing providers serving similar patient populations. The committee comprises expertise in health care quality, clinical medicine, health services research, health disparities, social determinants of health, risk adjustment, and Medicare programs (see Appendix F for biographical sketches). This report is the second in a series of five brief reports that aim to inform ASPE analyses that account for social risk factors in Medicare payment programs mandated through the Improving Medicare Post-Acute Care Transformation (IMPACT) Act. In its first report (NASEM, 2016), the committee presented a conceptual framework and described the results of a literature search linking five social risk factors (socioeconomic position; race, ethnicity, and cultural context; gender; social relationships; and residential and community context) and health literacy to health-related measures of importance to Medicare payment and quality programs. Details of the statement of task and the sequence of reports can be found in Box B1-1. The committee will release reports every 3 months, addressing each item in the statement of task in turn. The statement of task requests committee recommendations only in the fourth report.
PERFORMANCE OF PROVIDERS DISPROPORTIONATELY SERVING SOCIALLY AT-RISK POPULATIONS
As described in the committee’s first report (See Appendix A) (NASEM, 2016), socially at-risk populations include individuals with social risk factors for poor health outcomes such as low socioeconomic position, social isolation, residing in a disadvantaged neighborhood, identifying as a racial or an ethnic minority, having a non-normative gender or sexual orientation, and having limited health literacy. Although these populations receive care from a wide range of providers, they are disproportionately repre-
___________________
1 Health equity means that every person has the opportunity to attain his or her full health potential and no one is disadvantaged from achieving this potential because of social position or other socially determined circumstances. A health disparity refers to a difference in a health outcome or a health determinant between populations (CDC, 2015).
sented among the patients treated by a small subset of providers, including safety-net hospitals, minority-serving institutions, critical access hospitals, and community health centers (Bach et al., 2004; Jha et al., 2007, 2008). Evidence suggests the performance of these providers may differ systematically from providers serving the general population. In particular, hospitals disproportionately serving socially at-risk populations may provide lower-quality care and have worse patient outcomes compared to hospitals serving the general population on average (Girotra et al., 2012; Jha et al., 2011; Popescu et al., 2009). However, there is also evidence of substantial variation in performance among these providers, and some achieve performance scores on par with the top performers among all hospitals (Gaskin et al., 2011; Jha et al., 2008). Additionally, literature suggests that the performance of safety-net and minority-serving providers of ambulatory care is more mixed, and in many cases better compared to providers serving the general population (Goldman et al., 2012; Hall et al., 2014; Laiteerapong et al., 2014; Lopez et al., 2015; O’Malley et al., 2007; Rothkopf et al., 2011; Sequist et al., 2008).
The committee also considered using publicly reported performance data from providers relevant to Medicare beneficiaries—Medicare Hospital Compare hospital data and Medicare Advantage and Medicare Part D Star Ratings health plan data—to identify high-performing providers disproportionately serving socially at-risk populations. To do so would have engaged the committee in original empirical research, uncommon in reports from the National Academies, especially given the time frame the committee faces. The committee identified several challenges to identifying universally high performers. As described in the literature (e.g., Gaskin et al., 2011; Girotra et al., 2012; Jha et al., 2005, 2008; McHugh et al., 2014), there exists substantial variability in performance across measures and practice areas within organizations and across time for all providers. Individual providers perform well and poorly on different measures and in different practice areas. Moreover, there is little stability in performance over time, such that a high performer one year may perform poorly the next. Additionally, a provider’s performance on any individual measure or domain may not generalize to its overall performance and vice versa (Medicare.gov, n.d.; Shwartz et al., 2011).
Given these challenges, the committee did not embark on original research and depended on the published literature described above. Therefore, the committee was unable to identify high- or low-performing providers if interpreted as universally high or low performers across all providers, let alone those disproportionately serving socially at-risk populations. As a result, the committee was also unable to identify high- or low-performing providers who disproportionately serve socially at-risk populations. Despite these challenges:
- The committee found that some providers disproportionately serving socially at-risk populations achieved performance that was higher than their peer organizations and on par with the highest performers among all providers.
PRACTICES TO IMPROVE CARE FOR SOCIALLY AT-RISK POPULATIONS
The complex, interacting nature of the drivers of variation in the quality of care and health care outcomes makes it difficult to draw clear conclusions about what precisely drives this variation among providers that disproportionately serve socially at-risk populations. Combined with the fact that, as described in the previous section, the committee was unable to identify universally high- or low-performing providers, it follows that it is also problematic to then identify practices associated with the performance of universally high- and low-performing providers, let alone among those disproportionately serving socially at-risk populations, and to make comparisons between them. Thus, the committee turned to case studies to identify specific practices used either to improve performance or achieve high performance for socially at-risk populations or to mitigate the effects of social risk factors on their patient population’s health outcomes within specific facilities.
The committee reviewed both the peer-reviewed and grey literature in order to identify innovations, interventions, and other strategies providers disproportionately serving socially at-risk populations have implemented to improve care and outcomes for their patients. The committee reached out to organizations known to conduct research or represent providers disproportionately serving socially at-risk populations (Alliance of Community Health Plans, America’s Essential Hospitals, America’s Health Insurance Plans, and The Commonwealth Fund) and asked for help identifying relevant case studies, especially those that are not within the peer-reviewed published literature. These organizations submitted 60 case studies.
The committee reviewed the case studies submitted, as well as the published literature. The evidence identified through these searches has substantial limitations—few rigorous (controlled) evaluations, unlikely to be generalizable, and limited outcome data. Additionally, the relative performance of individual providers compared to their peers was not well documented. Given these limitations, the committee was not able to identify “best practices” if interpreted as uniform and universal strategies to provide high-quality care for socially at-risk populations and was not able to make comparisons between high- and low-performing providers, even among case studies. Furthermore, because community context is a central determinant of what is needed, acceptable, and feasible in different configu-
rations of problems and resources, universal and uniform “best practices” to improve care for all patients within a population and in all settings may not be desirable (Curry et al., 2011; Joynt et al., 2014). Nevertheless,
- The committee found examples of specific strategies implemented in specific community contexts by providers serving socially at-risk populations with the goal to improve health care quality and health outcomes.
IDENTIFYING SYSTEMS PRACTICES
Committee members identified commonalities from the review of the case studies, informed also by the literature and, in some cases, members’ empirical research or professional experience delivering care to socially at-risk populations. The common themes describe a set of practices delivered within a system of collaborating partners, not to specific health care interventions, and are consonant with research findings from the quality improvement literature and related clinical interventions designed to decrease disparities. Note that “system” as used here is not limited to a single health care organization, but refers more generally to a set of interconnected actors who work together to accomplish a common purpose—in this case to improve health equity and outcomes for socially at-risk populations. In this approach, the system is mainly composed of medical providers as well as partnering social service agencies, public health agencies, community organizations, and the community in which those medical providers are embedded. The medical providers may be formally (i.e., through legal arrangements) or informally related to the external partners, but all serve the same community or geographic region. These practices pertain to all health systems that serve socially at-risk populations, not only those providers disproportionately serving socially at-risk populations use.
The committee concluded that six community-informed and patient-centered systems practices show promise for improving care for socially at-risk populations:
- Commitment to health equity: Value and promote health equity and hold yourself accountable
- Data and measurement: Understand your population’s health, risk factors, and patterns of care
- Comprehensive needs assessment: Identify, anticipate, and respond to clinical and social needs
- Collaborative partnerships: Collaborate within and across provider teams and service sectors to deliver care
- Care continuity: Plan care and care transitions to prepare for patients’ changing clinical and social needs
- Engaging patients in their care: Design individualized care to promote the health of individuals in the community setting
As shown in Figure BS-1, the committee conceives of this system as grounded in community-informed and patient-centered care and emerging out of a commitment to health equity. This commitment supports and drives the other population-based practices, resulting in individualized care that promotes the health of the patient in his or her community context. Although in reality, a provider simultaneously engages in each systems
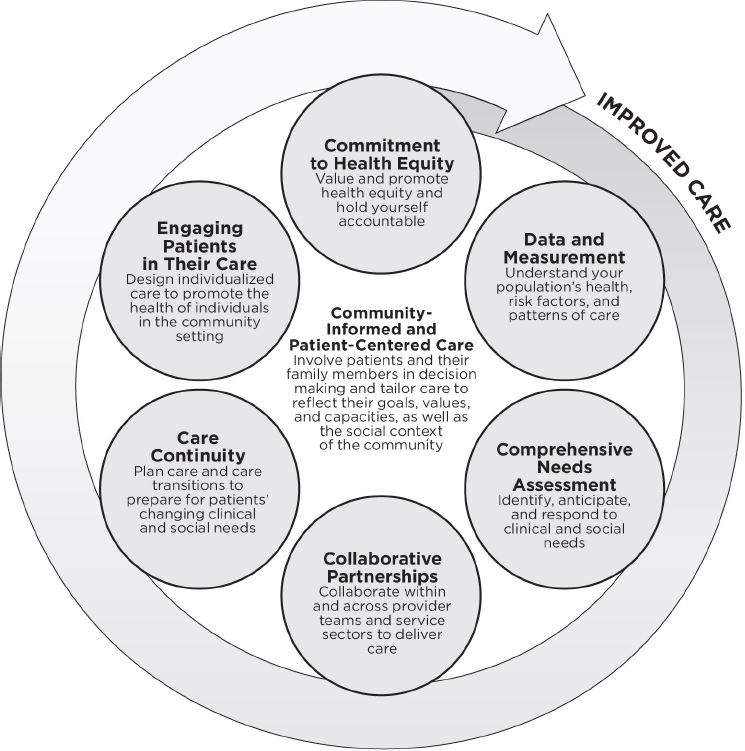
practice, each practice captures a thought process and set of decisions that logically influence the next. For example, a system may already conduct a comprehensive needs assessment, but this assessment will be fundamentally different when driven by a commitment to health equity and includes social need in addition to clinical needs. The value and resources that flow from this commitment drive changes in other processes, such as collaborating with social service agencies in the community, which supports enhanced planning for care transitions. Finally, the hard work of providing high-quality care is never done; this systems approach provides a continuous process for improvement.
RESOURCE AND SUSTAINABILITY CONSIDERATIONS
Both the availability of resources and the alignment of financial incentives that makes practices to improve the quality of care, health, and other outcomes for socially at-risk populations sustainable are prerequisites for the adoption and sustainability of these practices and programs. Resources can incentivize reducing disparities by not only explicitly directing resources to reduce disparities or targeting interventions at socially at-risk populations (such as greater investment in safety-net systems), but also by incorporating equitable care and outcomes into accountability processes (e.g., Berenson and Shih, 2012; Chin, 2016; Zuckerman et al., 2016).
In terms of sustainability, interventions that improve health and quality of care or reduce utilization and cost are only feasible to maintain if the provider is paid in such a way that profits (revenues minus costs) are higher with the intervention than without (e.g., global payment, shared savings, financial incentives). Because most of the efforts described in this report involve fixed costs and potentially shared benefits across multiple payers, their economic feasibility depends not only on Medicare’s payment system but also that of other payers. As health care systems increasingly partner with external organizations and other sectors, this will include non–health care stakeholders as well (e.g., Corrigan and Fisher, 2014). All things equal, environments in which a greater share of a provider’s revenue is derived from such VBP methods will make it more sustainable for providers to invest in programs that generate value (improved quality and reduced cost).
PUTTING THIS REPORT IN CONTEXT
The committee’s task in this report centered on identifying what high-quality health systems serving socially at-risk populations do to achieve good health outcomes for their patients. As the committee described, it is possible to deliver high-quality care to these populations and the committee outlined certain systems practices that could be instrumental in achieving
that goal. In the next and third report, the committee returns to the question of which social risk factors could be accounted for in Medicare value-based purchasing programs and how. Nothing in this second report should be interpreted as foreshadowing what the committee will conclude in the third report. However, this report does show that socially at-risk populations do not need to experience low-quality care and bad health care outcomes. Providers can feasibly respond to incentives to deliver high-quality and good-value care to socially at-risk populations.
REFERENCES
Bach, P. B., H. H. Pham, D. Schrag, R. C. Tate, and J. L. Hargraves. 2004. Primary care physicians who treat blacks and whites. New England Journal of Medicine 351(6):575–584.
Berenson, J., and A. Shih. 2012. Higher readmissions at safety-net hospitals and potential policy solutions. Issue Brief (Commonwealth Fund) 34:1–16.
Burwell, S. M. 2015. Setting value-based payment goals—HHS efforts to improve U.S. health care. New England Journal of Medicine 372(10):897–899.
CDC (Centers for Disease Control and Prevention). 2015. Health equity. http://www.cdc.gov/chronicdisease/healthequity (accessed February 16, 2016).
Chien, A. T., M. H. Chin, A. M. Davis, and L. P. Casalino. 2007. Pay for performance, public reporting, and racial disparities in health care: How are programs being designed? Medical Care Research and Review 64(5 Suppl):283s–304s.
Chin, M. H. 2016. Creating the business case for achieving health equity. Journal of General Internal Medicine [Epub ahead of print].
Corrigan, J. M., and E. S. Fisher. 2014. Accountable health communities: Insights from state health reform initiatives. http://tdi.dartmouth.edu/images/uploads/AccountHealthComm-WhPaperFinal.pdf (accessed March 7, 2016).
Curry, L. A., E. Spatz, E. Cherlin, J. W. Thompson, D. Berg, H. H. Ting, C. Decker, H. M. Krumholz, and E. H. Bradley. 2011. What distinguishes top-performing hospitals in acute myocardial infarction mortality rates? A qualitative study. Annals of Internal Medicine 154(6):384–390.
Friedberg, M. W., D. G. Safran, K. Coltin, M. Dresser, and E. C. Schneider. 2010. Paying for performance in primary care: Potential impact on practices and disparities. Health Affairs (Millwood) 29(5):926–932.
Gaskin, D. J., C. S. Spencer, P. Richard, G. Anderson, N. R. Powe, and T. A. LaVeist. 2011. Do minority patients use lower quality hospitals? Inquiry 48(3):209–220.
Gilman, M., E. K. Adams, J. M. Hockenberry, I. B. Wilson, A. S. Milstein, and E. R. Becker. 2014. California safety-net hospitals likely to be penalized by ACA value, readmission, and meaningful-use programs. Health Affairs (Millwood) 33(8):1314–1322.
Gilman, M., E. K. Adams, J. M. Hockenberry, A. S. Milstein, I. B. Wilson, and E. R. Becker. 2015. Safety-net hospitals more likely than other hospitals to fare poorly under Medicare’s value-based purchasing. Health Affairs (Millwood) 34(3):398–405.
Girotra, S., P. Cram, and I. Popescu. 2012. Patient satisfaction at America’s lowest performing hospitals. Circulation: Cardiovascular Outcomes and Quality 5(3):365–372.
Goldman, L. E., P. W. Chu, H. Tran, M. J. Romano, and R. S. Stafford. 2012. Federally qualified health centers and private practice performance on ambulatory care measures. American Journal of Preventive Medicine 43(2):142–149.
Hall, Y. N., P. Xu, G. M. Chertow, and J. Himmelfarb. 2014. Characteristics and performance of minority-serving dialysis facilities. Health Services Research Journal 49(3):971–991.
Jha, A. K., Z. Li, E. J. Orav, and A. M. Epstein. 2005. Care in U.S. hospitals—the Hospital Quality Alliance program. New England Journal of Medicine 353(3):265–274.
Jha, A. K., E. J. Orav, Z. Li, and A. M. Epstein. 2007. Concentration and quality of hospitals that care for elderly black patients. Archives of Internal Medicine 167(11):1177–1182.
Jha, A. K., E. J. Orav, J. Zheng, and A. M. Epstein. 2008. The characteristics and performance of hospitals that care for elderly Hispanic Americans. Health Affairs (Millwood) 27(2):528–537.
Jha, A. K., E. J. Orav, and A. M. Epstein. 2011. Low-quality, high-cost hospitals, mainly in South, care for sharply higher shares of elderly black, Hispanic, and Medicaid patients. Health Affairs (Millwood) 30(10):1904–1911.
Joynt, K. E., and A. K. Jha. 2013. A path forward on Medicare readmissions. New England Journal of Medicine 368(13):1175–1177.
Joynt, K. E., and M. B. Rosenthal. 2012. Hospital value-based purchasing: Will Medicare’s new policy exacerbate disparities? Circulation: Cardiovascular Outcomes and Quality 5(2):148–149.
Joynt, K. E., E. J. Orav, and A. K. Jha. 2011. Thirty-day readmission rates for Medicare beneficiaries by race and site of care. Journal of the American Medical Association 305(7):675–681.
Joynt, K. E., N. Sarma, A. M. Epstein, A. K. Jha, and J. S. Weissman. 2014. Challenges in reducing readmissions: Lessons from leadership and frontline personnel at eight minority-serving hospitals. The Joint Commission Journal on Quality and Patient Safety 40(10):435–437.
Karve, A. M., F. S. Ou, B. L. Lytle, and E. D. Peterson. 2008. Potential unintended financial consequences of pay-for-performance on the quality of care for minority patients. American Heart Journal 155(3):571–576.
Laiteerapong, N., J. Kirby, Y. Gao, T. C. Yu, R. Sharma, R. Nocon, S. M. Lee, M. H. Chin, A. G. Nathan, Q. Ngo-Metzger, and E. S. Huang. 2014. Health care utilization and receipt of preventive care for patients seen at federally funded health centers compared to other sites of primary care. Health Services Research Journal 49(5):1498–1518.
Lopez, L., N. Cook, and L. Hicks. 2015. Improved quality of care for cardiovascular disease for Latinos seen in high proportion Latino vs. low proportion Latino clinics. Ethnicity & Disease 25(1):3–10.
Ly, D. P., L. Lopez, T. Isaac, and A. K. Jha. 2010. How do black-serving hospitals perform on patient safety indicators?: Implications for national public reporting and pay-for-performance. Medical Care 48(12):1133–1137.
McHugh, M., J. Neimeyer, E. Powell, R. K. Khare, and J. G. Adams. 2014. Is emergency department quality related to other hospital quality domains? Academic Emergency Medicine 21(5):551–557.
Medicare.gov. n.d. About Hospital Compare data. https://www.medicare.gov/hospitalcompare/Data/About.html (accessed February 16, 2016).
MedPAC (Medicare Payment Advisory Commission). 2013. Chapter 4: Refining the Hospital Readmissions Reduction Program. In Report to the Congress: Medicare and the health care delivery system. Washington, DC: MedPAC.
Mehta, R. H., L. Liang, A. M. Karve, A. F. Hernandez, J. S. Rumsfeld, G. C. Fonarow, and E. D. Peterson. 2008. Association of patient case-mix adjustment, hospital process performance rankings, and eligibility for financial incentives. Journal of the American Medical Association 300(16):1897–1903.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Accounting for social risk factors in Medicare payment: Identifying social risk factors. Washington, DC: The National Academies Press.
O’Malley, A. S., H. H. Pham, D. Schrag, B. Wu, and P. B. Bach. 2007. Potentially avoidable hospitalizations for COPD and pneumonia: The role of physician and practice characteristics. Medical Care 45(6):562–570.
Popescu, I., R. M. Werner, M. S. Vaughan-Sarrazin, and P. Cram. 2009. Characteristics and outcomes of America’s lowest-performing hospitals: An analysis of acute myocardial infarction hospital care in the United States. Circulation: Cardiovascular Outcomes and Quality 2(3):221–227.
Rajaram, R., J. W. Chung, C. V. Kinnier, C. Barnard, S. Mohanty, E. S. Pavey, M. C. McHugh, and K. Y. Bilimoria. 2015. Hospital characteristics associated with penalties in the Centers for Medicare & Medicaid Services Hospital-Acquired Condition Reduction Program. Journal of the American Medical Association 314(4):375–383.
Rothkopf, J., K. Brookler, S. Wadhwa, and M. Sajovetz. 2011. Medicaid patients seen at federally qualified health centers use hospital services less than those seen by private providers. Health Affairs (Millwood) 30(7):1335–1342.
Ryan, A. M. 2013. Will value-based purchasing increase disparities in care? New England Journal of Medicine 369(26):2472–2474.
Sequist, T. D., G. M. Fitzmaurice, R. Marshall, S. Shaykevich, D. G. Safran, and J. Z. Ayanian. 2008. Physician performance and racial disparities in diabetes mellitus care. Archives of Internal Medicine 168(11):1145–1151.
Sheingold, S. H., R. Zuckerman, and A. Shartzer. 2016. Understanding Medicare hospital readmission rates and differing penalties between safety-net and other hospitals. Health Affairs (Millwood) 35(1):124–131.
Shih, T., A. M. Ryan, A. A. Gonzalez, and J. B. Dimick. 2015. Medicare’s Hospital Readmissions Reduction Program in surgery may disproportionately affect minority-serving hospitals. Annals of Surgery 261(6):1027–1031.
Shwartz, M., A. B. Cohen, J. D. Restuccia, Z. J. Ren, A. Labonte, C. Theokary, R. Kang, and J. Horwitt. 2011. How well can we identify the high-performing hospital? Medical Care Research and Review 68(3):290–310.
Sjoding, M. W., and C. R. Cooke. 2014. Readmission penalties for chronic obstructive pulmonary disease will further stress hospitals caring for vulnerable patient populations. American Journal of Respiratory and Critical Care Medicine 190(9):1072–1074.
Williams, K. A., Sr., A. A. Javed, M. S. Hamid, and A. M. Williams. 2014. Medicare readmission penalties in Detroit. New England Journal of Medicine 371(11):1077–1078.
Zuckerman, D., V. Duncan, and K. Parker. 2016. Building a culture of health equity at the federal level. http://nam.edu/wp-content/uploads/2016/03/Building-a-Culture-of-Health-Equity-at-the-Federal-Level.pdf (accessed March 10, 2016).










