9
Conclusion
“Of all the forms of inequality, injustice in health care is the most shocking and inhumane.” —Dr. Martin Luther King, Jr.
“Poverty is not an accident. Like slavery and apartheid, it is man-made and can be removed by the actions of human beings.” —Nelson Mandela
For many years researchers, public health practitioners, and others have known that health status in this country and around the world is determined as much by socioeconomic as biologic or behavioral factors. Despite that recognition, approaches to improving health status and health outcomes have narrowly centered on improving medical interventions, technologies, systems, and access. Beyond clinical approaches, some health promotion strategies have focused on changing behavior, despite the robust evidence indicating that they are ineffective in addressing health inequities (Baum and Fisher, 2014). Although these strategies play a role in improving population health, it has become amply clear that they are necessary but not sufficient. Health is the result of much more than health care; the social, economic, environmental, and structural factors—for example, education, poverty, housing, and structural racism—that shape health outcomes also create health inequities. Addressing and putting an end to health inequities will only be possible if society and decision makers broaden their view of health to fully grasp how steep and unjust disparities in social and other conditions limit, thwart, and even destroy some people’s ability to live healthy and full lives.
This report spotlights community interventions to address health inequity because communities are the unit in which individuals and families live, learn, work, and play. Thriving communities provide opportunities for people to live healthy lives. The opposite is also true. Communities that are unsafe, provide poor educational and economic opportunities, and offer weak infrastructure and surroundings also have poor health status. However, such realities are not destiny, and communities across the country have shown their resilience and ability to be agents of social change, as described throughout this report and especially in the community examples highlighted in Chapter 5. This ability to catalyze change can not only affect social and economic status but can also have a powerful impact on reducing health inequity.
This report highlights what is known about health inequity and its root causes: social, economic, environmental, and structural inequities. Because of their historically entrenched nature, such structural inequities as structural racism are highlighted as a major root cause of health inequity. Other root causes include inequities in education—which is highlighted as a key social determinant of health because of the well-documented impact it has on health and income—and income, which affects health status along with housing, transportation, and access to health care services. The committee concluded that health inequities are the result of much more than individual choice; they are the result of the historic and ongoing interplay of inequitable structures, policies, norms, and demographic and geographic patterns that shape lives and play out in the social, economic, environmental, and structural determinants of health (Braveman and Gottlieb, 2014; Krieger et al., 1997; Marmot et al., 2010; Williams and Collins, 2001).
Community solutions, such as those described in the report, have the best chance of being effective in addressing health inequities when implemented in the context of an enabling environment with supportive laws and policies (described in Chapter 6) and with a range of collaborators from a variety of relevant sectors (described in Chapter 7). The community-based solutions that the committee highlights as promising are characterized by (1) having a shared vision and values regarding what was needed in their community—whether or not health equity was explicitly acknowledged in that vision—and on how to move forward to address those needs; (2) enhancing community capacity by harnessing the power of communities; and (3) embracing and building on cross-sector collaboration. The committee also found that (see Chapters 4 and 5 for more details)
- Advances in health equity involve local community action, but always in collaboration with a range of partners.
- Community initiatives create positive change and improve results through many different pathways, and no one solution can serve as an exact template to be scaled or generalized.
- Robust initiatives demonstrate a focus on developing the next generation of leaders as well as flexibility, creativity, and resilience.
- Community collaboration can help create lasting change when all stakeholders agree on a shared commitment to results and to systematic learning from their experience and evolving research.
- Effective community solutions involve collaboration across professional, organizational, and bureaucratic boundaries; draw on the experience of practitioners and residents; and are informed by evidence.
- A mutual commitment to realizing co-benefits can facilitate the creation and sustainability of partnerships across sectors.
- Effective community solutions create a capacity for residents to identify key issues and to participate in devising strategies to meet their needs and build on their strengths while recognizing the power of systems and other forces outside the community to enhance or undermine the effectiveness of their efforts.
- Communities recognize the importance of sustainability in their approach to multiple and diverse sources of funding, to maintaining accountability, and to nurturing leadership.
In addition to providing a rationale for the community as the locus for confronting health inequities (see Chapter 4) and exploring community examples (see Chapter 5), the report highlights some of the helpful tools available to communities (see Chapter 8); describes the evidence on root causes and outlines some research and data needs (see Chapter 3); reviews the state of health disparities (see Chapter 2); discusses the national policy terrain (see Chapter 6); and explores the actions and engagement of different sectors and potential community partners (see Chapter 7).
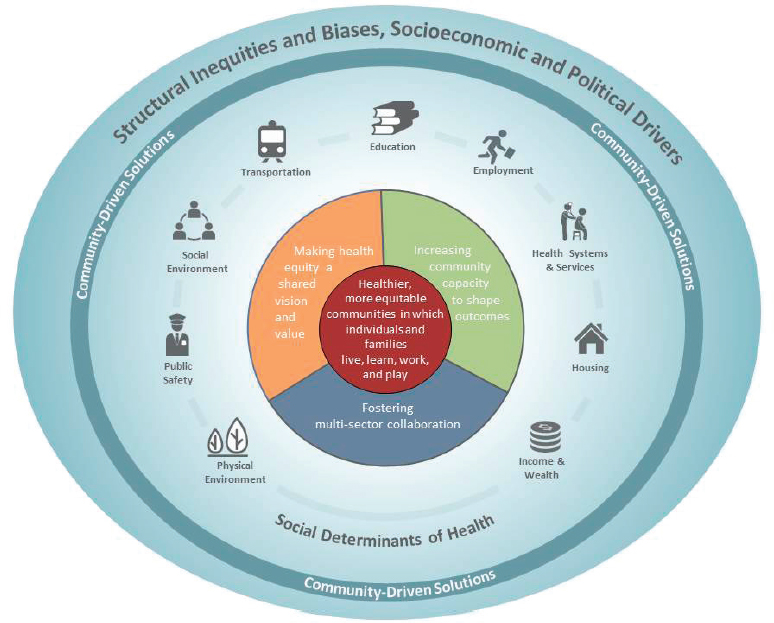
As discussed in the report, communities have agency, voice, and power, and multi-actor, multi-sectoral community partnerships can drive the identification, development, and implementation of solutions to promote health equity. However, a supportive policy and resource environment is needed to facilitate community efforts. The report provides evidence of both the critical need and the opportunity to address health inequity and of the key role that community-based solutions can play. It also outlines a path toward using a health focus as a lever in building a more equal, just, and fair society and to approaching the goal depicted at the center of the report conceptual model (see Figure 9-1): healthier, more equitable communities in which individuals and families live, learn, work, and play.
REFERENCES
Baum, F., and M. Fisher. 2014. Why behavioural health promotion endures despite its failure to reduce health inequities. Sociology of Health & Illness 36(2):213–225.
Braveman, P., and L. Gottlieb. 2014. The social determinants of health: It’s time to consider the causes of the causes. Public Health Reports 129(Suppl 2):19–31.
Krieger, N., D. R. Williams, and N. E. Moss. 1997. Measuring social class in U.S. public health research: Concepts, methodologies, and guidelines. Annual Review of Public Health 18(1):341–378.
Marmot, M., J. Allen, P. Goldblatt, T. Boyce, D. McNeish, M. Grady, and I. Geddes. 2010. Fair society, healthy lives: Strategic review of health inequalities in England post–2010. London: The Marmot Review.
Williams, D. R., and C. Collins. 2001. Racial residential segregation: A fundamental cause of racial disparities in health. Public Health Reports 116(5):404–416.




