Summary
Health equity is the state in which everyone has the opportunity to attain full health potential and no one is disadvantaged from achieving this potential because of social position or any other socially defined circumstance. Health equity and opportunity are inextricably linked. Currently in the United States, the burdens of disease and poor health and the benefits of well-being and good health are inequitably distributed. This inequitable distribution is caused by social, environmental, economic, and structural factors that shape health and are themselves distributed unequally, with pronounced differences in opportunities for health.
Community is any configuration of individuals, families, and groups whose values, characteristics, interests, geography, or social relations unite them in some way (adapted from Dreher, 20161). However, the word is used to denote both the people living in a place and the place itself. In this report the committee generally focuses on shared geography—in other words, community is defined as the people living in a place such as a neighborhood. Therefore, a community-based solution is an action, policy, program, or law that is driven by community members, affects local factors that can influence health, and has the potential to advance health equity.
___________________
1 Draft manuscript from Melanie C. Dreher, Rush University Medical Center, provided to staff on February 19, 2016, for the Committee on Community-Based Solutions to Promote Health Equity in the United States. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office. For more information, email PARO@nas.edu.
The potential of community-based solutions to advance health equity is a focus because the Robert Wood Johnson Foundation (RWJF) asked the Committee on Community-Based Solutions to Promote Health Equity in the United States to consider solutions that could be identified, developed, and implemented at the local or community level. However, the report focus should not be interpreted to suggest that community-based solutions represent the primary or sole strategy or the best opportunity to promote health equity (see Box S-1 for an outline of the report in brief). Communities exist in a milieu of national-, state-, and local-level policies, forces, and programs that enable and support or interfere with and impede the ability of community residents and their partners to address the conditions that lead to health inequity. Therefore, the power of community actors is a necessary and essential, but not a sufficient, ingredient in promoting health equity.
In addition to the support of high-level policies, such as those that address structural inequities (e.g., residential segregation), community-based solutions described in this report also rely on multi-sectoral and multilevel collaborations and approaches: for example, engaging businesses, the faith community, and other nontraditional partners. It is a strength of multi-sectoral collaboration and efforts that are not primarily health-focused that they, by definition, ensure diverse approaches to
improving community health and well-being. Such diverse approaches also are a manifestation of the fact that not all communities start out observing the differences in life expectancy between one side of town and another and seek to address those inequities. Some communities aim to improve high school graduation, expand affordable housing, or create jobs. This report is for communities that believe improving health among their residents is important, but it is also for communities that believe better transit, more affordable housing, safer streets, and more small businesses are important. Whether health is the end or the means to an end, communities can benefit by understanding how health is connected to other goals important to them, and that improving education, housing, safety, employment, or the environment can also help improve health and mitigate health inequity.
HEALTH EQUITY IS CRUCIAL
Health equity is fundamental to the idea of living a good life and building a vibrant society because of its practical, economic, and civic implications. Shifts in economic mobility, income inequality, and persisting legacies of social problems such as structural racism are hampering the attainment of health equity, causing economic loss, and, most overwhelmingly, the loss of human lives and potential.
Although moral arguments to promote health equity exist,2 promoting health equity could afford considerable economic, national security, and other benefits. The premise that there is social mobility, the opportunity to succeed with hard work, and the opportunity to achieve prosperity is fundamental to the “American Dream” (Carr and Wiemers, 2016). However, recent research demonstrates that worsening social, economic, and environmental factors are affecting the public’s health in serious ways that compromise opportunity for all (Chetty et al., 2016; Rudolph et al., 2015; Woolf et al., 2015).
Health inequity is costly. For example, a 2009 analysis by LaVeist and colleagues found that “eliminating health disparities for minorities would have reduced direct medical care expenditures by $229.4 billion for the years 2003–2006” (LaVeist et al., 2009, p. 4). In 2009 the Urban Institute
___________________
2 For example, Jones and colleagues cite valuing all people equally as foundational to the concept of equity, noting that the equal worth of all people is at the core of the human rights principle that all human beings equally possess certain rights (Jones, 2009). Braveman and colleagues point out that health differences adversely affecting socially disadvantaged groups are particularly unacceptable because ill health can be an obstacle to overcoming social disadvantage. They further note that this “consideration resonates with common sense notions of fairness, as well as with ethical concepts of justice” (Braveman et al., 2011, p. S150).
projected that from 2009 to 2018, racial disparities in health would cost U.S. health insurers approximately $337 billion total (Waidmann, 2009). Disparities in access to and in the quality of care (e.g., delayed care, inadequate coverage) account for a portion of these costs.
Beyond adding to health care costs, health inequity has consequences for the U.S. economy, national security, business viability, and public finances. In the domain of national security, diminished health means a diminished capacity to participate in military service—a concern shared by hundreds of senior military leaders. More than 75 percent of 17- to 24-year-olds—more than 26 million young adults—in the United States cannot qualify to serve in the armed forces because they experience persistent health problems—often untreated, ranging from obesity to dependencies on prescription and nonprescription drugs—are poorly educated, or have been convicted of a felony (Christeson et al., 2009). Nearly one-third (32 percent) of all young people experience health problems—other than their weight—that will keep them from serving. Many are disqualified from serving for asthma, eyesight or hearing problems, mental health issues, or recent treatment for attention deficit hyperactivity disorder. Navy Rear Admiral Robert Besal (ret.) has asserted that young people who are physically unfit for “productive employment or military service represent a staggering loss of individual potential and collective strength for the nation as well” (Council for a Strong America, 2016).
Just as a healthy military is viewed as a necessity for national security, a healthy, productive workforce is a prerequisite for a thriving economy (HERO, 2015; IOM, 2015a). The impact of poor health on private businesses is significant. Research from the Urban Institute shows that those young adults with health problems who cannot find jobs in the mainstream economy are less productive and generate higher health care costs for businesses (Woolf et al., 2015).
Three indicators provide summary information about the overall health of a population or subpopulation: infant mortality, age-adjusted death rates, and life expectancy. In international rankings, the United States ranks lower than other wealthy nations on each of these indicators; data on U.S. states show that racial and ethnic disparities are found in each of these indicators (NRC and IOM, 2013; OECD, 2015). In addition to sharp and persistent racial and ethnic disparities, other significant trends have surfaced: a slight decline in life expectancy of white women in the past several years (Arias, 2016), income inequality, drug use, suicide, and the relative deprivations of rural life have all emerged as key themes.
Report Conceptual Model
As part of its statement of task, the committee was asked to review the state of health disparities in the United States and to explore the
underlying conditions and root causes contributing to health inequities and the interdependent nature of the factors that create them. The committee drew on existing literature and comprehensive reviews to examine the state of health disparities by race and ethnicity, gender, sexual orientation, and disability status, highlighting those populations that are disproportionately affected by inequity. Health disparities stem from systematic differences—those that are preventable and unjust—among groups and communities occupying unequal positions in society (Graham, 2004).
Figure S-1 is a conceptual model that grounds the report of the Committee on Community-Based Solutions to Promote Health Equity in the
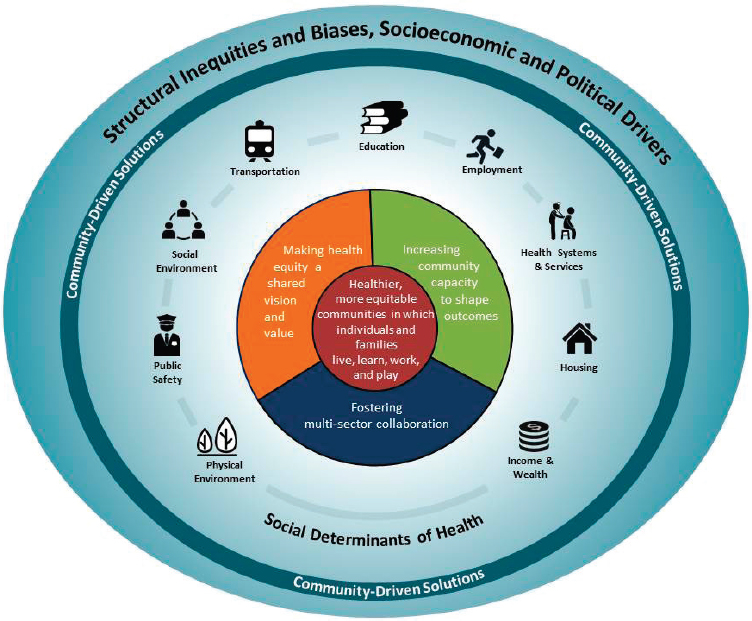
NOTES: Multi-sector collaboration can include partners from agriculture, banking/finance, business/industry, economic development, education, health care, housing, human/social services, justice, labor, land use and management, media, public health, transportation, and workforce development, among other sectors.
SOURCES: Informed by the Robert Wood Johnson Foundation (RWJF) Culture of Health Action Framework and the Prevention Institute’s Systems Framework to Achieve an Equitable Culture of Health.
United States. The model adapts elements of the RWJF Culture of Health Action Framework and the Prevention Institute’s Systems Framework to Achieve an Equitable Culture of Health. The figure applies the culture of health lens to the committee’s understanding of the underlying causes and conditions of health inequity in addition to the community-based solutions that promote health equity.
Unlike a logic model, which is linear and progresses neatly from inputs to outputs and outcomes, the model in Figure S-1 is circular to reflect the topic’s complexity, with inputs shown in the outer circle and background—depicting the context of structural inequities, socioeconomic and political drivers, and determinants of health in which health inequities and community-driven solutions exist. Community-driven solutions that target the nine determinants of health listed in the model (e.g., education, housing) likely share three key elements the committee identified at the beginning of its work. The committee adapted two action areas of the Culture of Health Action Framework“Making health equity a shared vision and value” and “Fostering multi-sector collaboration”as two elements of community-based solutions to promote health equity. Based on the committee’s information-gathering sessions, relevant literature, and committee deliberations, the committee also articulated a third element: “Increasing community capacity to shape outcomes.” These elements of community-based efforts are discussed in Chapter 4. The RWJF action area “Creating healthier, more equitable communities” has been incorporated into the model at the center of the diagram as the outcome of the community-driven solutions.
The community examples featured in this report (see Chapter 5) highlight solutions that have been implemented at the community level to target one or more of the nine determinants of health using the three elements identified in the model. These solutions, which hold health equity (or its determinants) as a shared vision and value, increase community capacity to shape outcomes, and foster multi-sector collaboration, can help create equal opportunity for health, which is the foundation for health equity.
MANY FACTORS SHAPE HEALTH AND HEALTH EQUITY
The committee took a multifactor view of health status and health inequities, in recognition that only some aspects of a person’s health status depend on individual behaviors and choice. Community-wide problems such as poverty, unemployment, low educational attainment, inadequate housing, lack of public transportation, exposure to violence, and neighborhood deterioration (social or physical) shape health and contribute to health inequities. The historic and ongoing interplay of structures,
policies, norms, and demographic and geographic patterns shapes the life of every individual across the country, and its effects persist over multiple generations (Braveman and Gottlieb, 2014; Krieger, 2014; Marmot et al., 2010; Williams and Collins, 2001). These factors are not intractable, and such inequities3 can be mitigated by policies and community action in powerful ways (see Chapter 3 for a discussion of these factors).
It is becoming clearer that health insurance coverage alone will not address health disparities, including those across race, ethnicity, socioeconomic status (SES), and geography (Kenney and Huntress, 2012; Ubri and Artiga, 2016). Signed into law in 2010, the Patient Protection and Affordable Care Act (ACA) has accelerated progress toward health equity by expanding health insurance coverage to about 20 million Americans (Uberoi et al., 2016). However, challenges remain to fully addressing health care equity, including policy hurdles affecting access and utilization among subgroups of the population.4
Health inequity arises from root causes that could be organized in two clusters:
- Intrapersonal, interpersonal, institutional, and systemic mechanisms (also referred to as structural inequities) that organize the distribution of power and resources differentially across lines of race, gender, class, sexual orientation, gender expression, and other dimensions of individual and group identity.
- The unequal allocation of power and resources—including goods, services, and societal attention—which manifests itself in unequal social, economic, and environmental conditions, also called the determinants of health.
Interventions targeting those factors hold the greatest promise for promoting health equity. The root causes of inequity are diverse, complex, evolving, and interdependent in nature (Williams and Collins, 2001), and while society has made substantial progress toward equity, disparities in health outcomes and opportunities for health persist. Poverty, race, and ethnicity continue to be associated with poorer health and poorer
___________________
3 That is, differences that exist among specific population groups in the United States in the attainment of full health potential and in the incidence, prevalence, mortality, and burden of disease and other adverse health conditions (NIH, 2014).
4 For example, a lack of coverage for some immigrants and asylum seekers or those subject to deferred action for childhood arrivals; a limited system capacity or competence to care for some populations, such as lesbian, gay, bisexual, or transsexual (LGBT) persons (e.g., newly covered partners of insured LGBT individuals); and the lack of health data to monitor the health needs of some populations (e.g., for American Indians, of whom approximately 20 percent live on rural reservations) (Kruse et al., 2016).
conditions for health. For example, evidence indicates that the conditions that exist in low-income communities, such as concentrated poverty, low housing values, and low high school graduation rates, foster violence and increase the risk of homicide (Prevention Institute, 2011). Those conditions themselves are shaped by interconnected structures, policies, and norms that affect people differently along lines of class, race, and ethnicity. Taking low high school graduation rates, for example, research indicates that race and class differences in adverse childhood experiences, chronic stress and trauma, and lead exposure in the environment affect children’s ability to learn (Aizer et al., 2015; Bethell et al., 2014; Jimenez et al., 2016; Levy et al., 2016). Moreover, a growing body of research indicates that minority students are disproportionately affected by school discipline policies that lead students to drop out of school (Howard, 2010; Losen et al., 2015; Reardon et al., 2012; Skiba et al., 2011; Smith and Harper, 2015). Chapters 3 and 6 describe more of the evidence on how inequitable structures, policies, and norms influence the determinants—from housing to education to employment—that make it considerably harder for people who are poor and for people of color to achieve good health.
Conclusion 3-2: Based on its review of evidence, the committee concludes that health inequities are the result of more than individual choice or random occurrence. They are the result of the historic and ongoing interplay of inequitable structures, policies, and norms that shape lives.
These structures, policies, and norms—such as segregation, redlining and foreclosure, and implicit bias—play out on the terrain of the social, economic, environmental, and cultural determinants of health.
COMMUNITY AGENCY TO PROMOTE HEALTH EQUITY
A community is the place where one lives, works, and plays. It serves as the bedrock of health that shapes lives and behaviors. Indeed, as detailed in Chapters 2 and 3, research consistently indicates that where one lives is a greater predictor of one’s health than individual characteristics or behaviors. Communities encompass multiple spheres of interaction, from the individual to the organizational level to the physical setting, and each level of interaction affects health outcomes. Communities also are unique in the nature and extent of health inequities, and so are the means to address those issues, such as the locus of power and community values.
Communities across the United States are developing and putting into action strategies to reduce health inequities. Often these community efforts go unseen in the media, while stories of blight, crime, or
community unrest are more visible. Community assets can be built, leveraged, and modified and can create a context in which to foster health equity. The committee was asked to identify and examine six or more examples of community-based solutions that address health inequities, drawing from deliberate and indirect interventions or activities that promote equal opportunity for health. The nine examples in Chapter 5 span health and non-health sectors and take into account the range of factors that contribute to health inequity in the United States, such as systems of employment, public safety, housing, transportation, education, and others. See Table S-1 for a list and brief description of each community example. The committee used a set of core inclusion criteria to select the examples for this report. According to these core criteria, the community examples must
- address at least one (or preferably more) of the nine social determinants of health identified by the committee—education, employment, health systems and services, housing, income and wealth, physical environment, public safety, social environment, and transportation—and be:
- community-driven;
- multi-sectoral; and
- evidence-informed.
The committee also strove to capture examples of communities that were able to engage nontraditional partners, work in an interdisciplinary and multilevel manner, and document plans to achieve their outcomes and sustain its efforts. These communities represent a diversity of geography, environments, challenges, and resources. Chapter 5 provides a summary of each example to demonstrate the innovative work conducted by communities and the challenges they face. In Chapter 5 the committee comments on a number of crosscutting essential elements that show promise for promoting health equity in communities. These elements include, but are not limited to, creating a shared vision and building trust in the community, leadership development, building a diverse network of partners through relationship building and mutual accountability, governing processes that have a grassroots component, fostering creativity, leveraging resources, and training and commissioning technical expertise where necessary.
To succeed, communities need evidence (from research); a broader context of policy, resources, and political will that nurtures local efforts; and tools.
TABLE S-1 Overview of Community Examples to Promote Health Equity
| Name Location |
Brief Description | Primary Social Determinant(s) of Health Targeted |
|---|---|---|
| Blueprint for Action Minneapolis, MN |
A strategic plan that employs the public health approach to youth violence prevention that arose from a community-driven, grassroots response to the issue. | Public safety |
| Delta Health Center Mound Bayou, MS |
The first rural federally qualified health center, employing a community-oriented primary care model. | Health systems and services |
| Dudley Street Neighborhood Initiative Boston, MA |
A nonprofit, community-driven organization that empowers residents to drive economic development and neighborhood revitalization. | Physical environment Employment |
| Eastside Promise Neighborhood San Antonio, TX |
An implementation site of the Promise Neighborhood grant program, developing collaborative solutions to address barriers to education. | Education |
| Indianapolis Congregation Action Network Indianapolis, IN |
A multi-faith, nonpartisan organization that catalyzes marginalized people and faith communities to organize for racial and economic equity. | Employment Public safety |
| Magnolia Community Initiative Los Angeles, CA |
An initiative that seeks to increase social connectedness, community mobilization, and access to vital supports and services to improve outcomes for children. | Social environment |
| Mandela MarketPlace Oakland, CA |
A nonprofit organization that addresses issues of food insecurity and economic divestment through the creation of sustainable food systems. | Physical environment |
| People United for Sustainable Housing Buffalo, NY |
A nonprofit organization that mobilizes residents to secure quality, affordable housing and advance economic justice. | Housing |
| WE ACT for Environmental Justice Harlem, NY |
A nonprofit organization that engages in community organizing, community-based participatory research, and advocacy to confront environmental injustice. | Physical environment |
DISPARITIES AND THEIR ROOTS
Health disparity research has evolved from describing associations (e.g., between SES and health) to describing the mechanisms linking SES and health, to more recent work on the interactions among factors (Adler and Stewart, 2010). More epidemiological studies employing a combination of research strategies (i.e., mixed-methods qualitative and quantitative research) in addressing health disparities are needed to provide guidance for community interventions in this complex arena (Diez Roux and Mair, 2010).
Conclusion 2-1: To enable researchers to fully document and understand health inequities, to provide the foundation for solution development, and to measure solution outcomes longitudinally, the following are needed:
-
An expansion of current health disparity indicators and indices to include other groups beyond African Americans and whites, such as Hispanics and their major subgroups, Native Americans, Asian Americans, Pacific Islanders, and mixed race, in addition to LGBT individuals, people with disabilities, and military veterans.
- Including consideration of methods to generate stable estimates of disparities through oversampling certain populations where necessary.
- An expansion of metrics and indicators capturing the broader definition of health, including health equity and the social determinants of health.
- Longer-term studies, as many health outcomes take years (or decades) to see quantifiable changes in health outcomes related to the social determinants of health.
- Studies examining the ways in which a single structural factor may influence multiple health outcomes.
- Increased funding opportunities dedicated to developing and testing relevant theories, measures, and scientific methods, with the goal of enhancing the rigor with which investigators examine structural inequities such as structural racism and health disparities.
Unequal treatment in the health care delivery system has been well documented elsewhere (IOM, 2003), as has implicit bias and the need for cultural competence (IOM, 2003; Sabin et al., 2009). Greater diversity in the health sector workforce could help improve cultural competence and offer additional benefits (Cooper et al., 2003). Also, additional research could inform health care organizations, academic health centers, and others about the effects of and effective strategies to address the health-related harms of structural racism and implicit and explicit bias across
categories of race, ethnicity, gender, disability status, age, sexual orientation, gender identity, and other marginalized statuses. For example, the literature does not clearly elucidate the relationship between health care workforce pipeline programs (e.g., to grow the numbers of minority providers) and their impact on the social determinants of health for poor and underserved communities.
Recommendation 3-1: The committee recommends that research funders5 support research on (a) health disparities that examines the multiple effects of structural racism (e.g., segregation) and implicit and explicit bias across different categories of marginalized status on health and health care delivery; and (b) effective strategies to reduce and mitigate the effects of explicit and implicit bias.
There have been promising developments in the search for interventions to address implicit bias, but more research is needed, and engaging community members in this and other aspects of research on health disparities is important for ethical and practical reasons (Minkler et al., 2010; Mosavel et al., 2011; Salway et al., 2015). In the context of implicit bias in workplaces and business settings, including individuals with relevant expertise in informing and conducting the research could also be helpful. Therefore, research teams could be composed of such nontraditional participants as community members and local business leaders, in addition to academic researchers.
Recommendation 3-2: The committee recommends that research funders support and academic institutions convene multidisciplinary research teams that include nonacademics to (a) understand the cognitive and affective processes of implicit bias and (b) test interventions that disrupt and change these processes toward sustainable solutions.
As communities pursue broader change in the conditions for health, they find a dearth of systematic, organized information and guidance to help them: set common goals and measures of success; select multifaceted and mutually reinforcing strategies, grounded in strong theory; align implementation efforts; and make the necessary system and community-level changes to adapt and continuously improve. A centralized resource for communities is needed, and several partially relevant models exist,
___________________
5 Funders include government agencies, private foundations, and other sources such as academic centers of higher education.
some of which could potentially be modified to operate in an expanded capacity. These include the County Health Rankings (CHR) What Works for Health database, the U.S. Centers for Disease Control and Prevention’s (CDC’s) Community Health Improvement (CHI) Navigator, and also, perhaps, the Agency for Healthcare Research and Quality’s Measures Clearinghouse and the National Library of Medicine (which serves as a knowledge curation resource through its special queries). The CHR What Works for Health database provides information for community health improvement organized by expected beneficial outcomes, potential beneficial outcomes, evidence of effectiveness, impact on disparities, implementation examples, implementation resources, and citations. The CHI Navigator is intended for individuals and groups who lead or participate in CHI work “within hospitals and health systems, public health agencies, and other community organizations. It is a one-stop shop that offers community stakeholders expert-vetted tools and resources for: depicting visually the who, what, where, and how of improving community health; making the case for collaborative approaches to community health improvement; establishing and maintaining effective collaborations; and finding interventions that work for the greatest impact on health and well-being for all” (CDC, 2015). The Urban Institute Metropolitan Housing and Communities Policy Center’s What Works Collaborative6 is another evidence database that conducts research to support evidence-based housing and urban policy. Another resource is the Guide to Community Preventive Services,7 whose health equity focus includes systematic reviews examining the influence of educational interventions on long-term health.
Recommendation 4-1: A public–private consortium8 should create a publicly available repository of evidence to inform and guide efforts to promote health equity at the community level. The consortium should also offer support to communities, including technical assistance.
___________________
6 For more information, see http://www.urban.org/policy-centers/metropolitan-housingand-communities-policy-center/projects/what-works-collaborative (accessed October 28, 2016).
7 For more information, see https://www.thecommunityguide.org/topic/health-equity (accessed October 28, 2016).
8 This could be done through such mechanisms as a collaboration among CDC (home of the Community Health Improvement Navigator initiative), university-based centers (see the example of the University of Wisconsin Population Health Institute that operates the County Health Rankings [CHR] What Works for Health database), and one or more philanthropic organizations.
The repository would include databases that provide information at the national, state, and metropolitan levels as well as for smaller local geographies such as census tracts; information on effective interventions and approaches; and the knowledge necessary to strengthen the capacity of communities to act on topics such as education, income, employment, transportation, nutrition, civil rights, housing, and other determinants of health by race, ethnicity, gender, disability status, age, sexual identity/orientation, and other demographic characteristics.
POLICY CONTEXT AND PARTNERS
Adding to the complexity of developing and implementing community interventions to promote health equity are significant changes in the sociocultural, demographic, economic, and political landscape affecting health disparities and the social determinants of health. These changes include an increase in income inequality (e.g., incomes in the top 10 percent average 9 times the income of the bottom 90 percent, and incomes in the top 0.1 percent are more than 184 times those of the bottom 90 percent); the demographic shift to a larger proportion of people of color in the U.S. population (e.g., by 2040, the number of U.S. counties in which the majority of the population is people of color is expected to more than double), with implications for expanding health inequity; and increasing disparities. Recent events involving race and law enforcement relations have offered a disturbing illustration of systematically unequal treatment that is causing fear, mistrust, anger, and divisiveness. Moreover, there is a growing bipartisan recognition that mass incarceration, which affects individuals of color disproportionately, plays a major role in damaging families and communities, constitutes an unsustainable use of taxpayer dollars, and, in connection with the larger policy milieu in both the private and the public sector, leads to poor employment prospects and voting disenfranchisement (Clear, 2008; NRC, 2014). These current realities serve as reminders that the vision of a truly inclusive and equitable society is not yet within reach. However, community-driven solutions, such as those that his report highlights, can help move the nation in that direction. For example, Multnomah County, Oregon, applies an “equity and empowerment lens” to local policy (Multnomah County, 2014a,b, n.d.), and Seattle–King County implemented an “equity in all policies” approach to all decision making and annually reports on what it terms “the determinants of equity” in the county (Beatty and Foster, 2015).
In a 2011 Institute of Medicine (IOM) report, the authoring committee recommended that “states and the federal government develop and employ a Health In All Policies (HIAP) approach to consider the health effects—both positive and negative—of major legislation, regulations,
and other policies that could potentially have a meaningful impact on the public’s health” (IOM, 2011, p. 9). The committee further recommended that “state and federal governments evaluate the health effects and costs of major legislation, regulations, and policies that could have a meaningful impact on health. This evaluation should occur before and after enactment” (p. 11). The recommendation below is made with acknowledgment of the ongoing work in many jurisdictions around the country and of the previous IOM recommendations.
Recommendation 6-1: All government agencies that support or conduct planning related to land use, housing, transportation, and other areas that affect populations at high risk of health inequity should:
- Add specific requirements to outreach processes to ensure robust and authentic community participation in policy development.
- Collaborate with public health agencies and others to ensure a broad consideration of unintended consequences for health and well-being, including whether the benefits and burdens will be equitably distributed.9
- Highlight the co-benefits of—or shared “wins” that could be achieved by—considering health equity in the development of comprehensive plans10 (e.g., improving public transit in transit-poor areas supports physical activity, promotes health equity, and creates more sustainable communities).
- Prioritize affordable housing, implement strategies to mitigate and avoid displacement (and its serious health effects), and document outcomes.
An additional way to think about promoting community-based strategies for reducing education and health disparities is to consider the existing infrastructure of policies and programs within the education sector with an eye for how this infrastructure might be strengthened, modified, and expanded in the interest of improving health outcomes. The committee considered the role of the education sector in shaping health and health equity, given the strong relationship between educational achievement and health outcomes. Recently updated requirements for school
___________________
9 See Recommendation 7 in For the Public’s Health: Revitalizing Law and Policy to Meet New Challenges (IOM, 2011).
10 See, for example, ChangeLab Solutions’ “Model Comprehensive Plan Language on Complete Streets” (ChangeLab Solutions, 2016).
assessment of student health needs also appear to align well with needs assessments required in the health sector, for both public health agencies and tax-exempt hospitals and health systems (IRS, 2016; PHAB, 2011).
Recommendation 6-2: State departments of education should provide guidance to schools on how to conduct assessments of student health needs and of the school health and wellness environment. This guidance should outline a process by which schools can identify model needs assessments, including those with a focus on student health and wellness.
Recommendation 6-3: To support schools in collecting data on student and community health, tax-exempt hospitals and health systems and state and local public health agencies should:
- Make schools aware of existing health needs assessments to help them leverage current data collection and analyses.11
- Assist schools and school districts in identifying and accessing data on key health indicators that should inform school needs assessments and any related school improvement plans.
Hospitals are demonstrating greater interest in community-wide health investments and underlying factors that affect population health, rather than maintaining a more narrow focus on health care services and funding offsets. In Can Hospitals Heal America’s Communities, Norris and Howard (2015) write that “addressing these social determinants of health through their business and non-clinical practices (for example, through purchasing, hiring, and investments), hospitals and health systems can produce increased measurably beneficial impacts on population and community health” (pp. 1–2). Examples of efforts to build, hire, and invest locally include Kaiser Permanente in California and elsewhere and ProMedica in Cleveland (NASEM, 2016d).
Recommendation 6-4: Through multi-sectoral partnerships, hospitals and health care systems should focus their community benefit dollars to pursue long-term strategies (including changes in law, policies, and systems) to build healthier neighborhoods, expand access to housing, drive economic development, and advance other upstream initiatives aimed at eradicating the root causes of poor health, especially in low-income
___________________
11 See, for example, the Healthy Students, Promising Futures tool kit from the U.S. Departments of Education and Health and Human Services (ED, 2016a).
communities. Hospital and health systems should also advocate for the expansion of efficient and effective services responding to health-related social needs12 for vulnerable populations and people living in poverty.
Because health care payment reform (among other public policies) may have unintended consequences such as reproducing health disparities, efforts to mitigate negative consequences are needed. However, mitigating efforts can be addressed only by including the perspectives of populations most affected by such programs.
Recommendation 6-5: Government and nongovernment payers and providers should expand policies aiming to improve the quality of care, improve population health, and control health care costs13 to include a specific focus on improving population health for the most vulnerable and underserved. As one strategy to support a focus on health disparities, the Centers for Medicare & Medicaid Services could undertake research on payment reforms that could spur accounting for social risk factors in the value-based payment programs it oversees.
The National Academies’ Committee on Accounting for Socioeconomic Status in Medicare Payment Programs has shown in its reports (NASEM, 2016a,b,c,e) that value-based payment systems that do not account for social risk factors can have unintended adverse consequences, including providers and health plans avoiding low-income patients and underpayment to providers disproportionately serving socially at-risk populations (such as safety-net providers). These unintended consequences could in turn lead to deterioration in the quality of health care for socially at-risk populations and widening health disparities. That committee has stated that reducing disparities in access, quality, and outcomes is one of four policy goals in accounting for social risk factors (NASEM, 2016a,b,c,e), and its reports suggest that reforms to value-based payment programs that compensate providers fairly and increase fairness and
___________________
12Alley et al. (2016) describe services addressing health-related social needs, including transportation and housing. Others define services addressing such needs as “wraparound services,” referring to linkages or services health care providers can offer to ensure, for example, that patients have transportation to routine health care appointments, have adequate food in their homes, and obtain legal (e.g., for tenant-landlord disputes about environmental exposure to asthma triggers) or social service assistance. See, for example, (Bell and Cohen, 2009).
13 Better care, better population health, and lower cost are often described as the Triple Aim (Berwick et al., 2008).
accuracy in public reporting can help achieve goals to reduce disparities and improve quality and efficiency of care for all patients.
Civil rights, health, and environmental justice laws and policies provide a framework that promotes equal access to publicly funded resources and prohibit discrimination based on race, color, national origin, income, gender, disability, and other factors. This is a crosscutting framework that applies across different areas such as health, park access, education, housing, transportation, and others. Using the framework to support community-driven solutions draws on lessons from the civil rights movement and related movements, such as the women’s movement. Specific actions by several federal agencies illustrate how civil rights can be promoted to advance health equity through the planning framework.
Conclusion 6-1: In the committee’s judgment, civil rights approaches have helped mitigate the negative impacts of many forms of social and health discrimination. Continuing this work is needed to overcome discrimination and the structural barriers that affect health.
Conclusion 6-2: The committee concludes that using civil rights approaches in devising and implementing community solutions to promote health equity can guard against unjustified and unnecessary discriminatory impacts, as well as against intentional discrimination in programs that affect health. For example, those implementing community solutions can employ methods and data in ways that include full and fair participation by diverse communities.
The philanthropy sector has a number of tools available to support communities as they design, implement, and evaluate interventions to promote health equity. In broad categories, these tools include convening, leadership and capacity development, model testing, topic studies and reports, project and program funding, advocacy support, and social movement building. Advocacy funding may present challenges for certain foundations for which funding issue-specific advocacy strategies, such as lobbying, is prohibited by federal tax law. Nevertheless, such foundations can support advocacy groups with general operating funds (as distinguished from program-specific funds) that can be used to lobby, as long as the foundation is not involved with decision making about what issues the advocacy group chooses to take on. Foundations can also support social movement building by providing support for organizations that use community organizing to address important social issues.
Recommendation 7-1: Foundations and other funders should support community interventions to promote health equity by:
- Supporting community organizing around important social determinants of health;
- Supporting community capacity building;
- Supporting education, compliance, and enforcement related to civil rights laws; and
- Prioritizing health equity and equity in the social determinants of health through investments in low-income and minority communities.
Past IOM reports have reflected on the limitations of randomized controlled trials for public health and related research and on the need for a broader array of research tools to inform community health improvement efforts (IOM, 2012; IOM and NRC, 2013). To inform community-based efforts to promote health equity, novel research is needed, but to make that possible, changes to the dominant research paradigm are needed.
While social epidemiology has made highly important contributions to our understanding of the social determinants of health and population health, it “does not have the breadth, or imply all of the multiple interactions and pathways” involved in population health (Kindig and Stoddart, 2003, p. 382). Thus, models for the training of population and place-based scientists and practitioners are needed in order to develop the research required to guide upstream approaches, including place-based interventions, which address contextual factors that shape major public health problems such as obesity, interpersonal violence, infant and maternal health problems, cardiovascular diseases, infectious diseases, substance use disorders, and mental health disorders. Therefore, based on the committee’s expertise and its examination of the available evidence, the committee recommends the following:
Recommendation 7-2: A number of actions to improve the knowledge base for informing and guiding communities should be taken, including
- Public and private research funders should support communities and their academic partners in the collection, analysis, and application of evidence from the experience of practitioners, from leaders of community-based organizations, and from traditionally underrepresented participants who are typically left out of such partnerships.
- Universities, policy centers, and academic publications should modify current incentive14 structures to encourage and reward more research on the social distribu-
___________________
14 Such incentives may include funding, publication standards, and rules governing tenure.
-
tion of risks and resources and the systematic generation and dissemination of the evidence needed to guide the complex, multi-faceted interventions that are most likely to reduce inequities in health outcomes.15
- Academic programs should promote the development of and dialogue on theory, methods, and the training of students to create a more useful knowledge base in the next generation of researchers on how to design, implement, and evaluate place-based initiatives to improve community health.
Anchor institutions—a wide range of local institutions that include hospitals and universities, local government, sports venues, and museums—are “firmly rooted in their locales” and constitute “sticky capital” (i.e., capital that is resistant to change). Such institutions: (1) are affected by their local environment and, as such, have a stake in the health of surrounding communities; (2) have a moral and an ethical responsibility to contribute to the well-being of surrounding communities because they can make a difference; and (3) when involved in solving real-world local problems, are more likely to advance learning, research, teaching, and service (Harkavy et al., 2014).
Rubin and Rose (2015) and others (Martin et al., 2005; Miller and Rivera, n.d.; O’Mara, 2012) have highlighted the complex, sometimes contentious relationships and history between anchor institutions and their communities (e.g., community perception that they receive no benefit and may even be harmed by the local anchor institution). However, the potential of anchor institutions to engage with communities to improve well-being has also been explored and numerous examples provided (Dubb et al., 2013; Norris and Howard, 2015; NTFAI, 2010). Anchor institution motivations to engage with community partners vary and may include one or more of the following: “an economic self-interest in helping ensure that the communities in which they are based are safe, vibrant, and healthy” (Serang et al., 2013, p. 4); an interest in contributing to economic development; a sense of social responsibility; and a desire to pursue public–private partnerships to address mutually relevant challenges. The
___________________
15 SQUIRE (Standards for Quality Improvement Reporting Excellence) is an example of concerted efforts by leaders in one sector—health care—to change powerful incentives. SQUIRE guidelines provide an explicit framework for reporting new knowledge about system-level work to improve the quality, safety, and value of health care in the hope of shifting the emphasis and rewards from a near-exclusive emphasis on experimental findings to examining interventions closely, carefully, and in detail; generating important new knowledge about systems of care; and learning about how best to change those systems (Davidoff and Batalden, 2005).
anchor institution approach of an articulated mission, strategies, and metrics to improve community conditions has gained increasing attention and buy-in in a number of major metropolitan areas (e.g., Cleveland, Ohio; Detroit, Michigan; Philadelphia, Pennsylvania; Phoenix, Arizona). Such anchors have made significant investments, usually with a number of other anchor partners including city government and, often, private investors. Data on how such efforts have improved the living conditions of long-term and low-income residents are not yet available.
Recommendation 7-3: The committee recommends that anchor institutions (such as universities, hospitals, and businesses) make expanding opportunities to promote health equity in their community a strategic priority. This should be done by:
- Deploying specific strategies to address the multiple determinants of health on which anchors can have a direct impact or through multi-sector collaboration; and
- Assessing the negative and positive impacts of anchor institutions in their communities and how negative impacts may be mitigated.16
Policy makers include a wide variety of actors (e.g., city council members, mayors, school board members, state legislators, etc.) whose work spans the spectrum from very local policy development, such as zoning, to national policy development, such as the Fair Housing Act. Furthermore, policy shapes the social determinants of health and the conditions of communities (IOM, 2011). Historically, policy has arguably been a driver of health inequity (e.g., redlining and urban renewal policies) (Williams and Collins, 2001). Thus, policy makers can play a significant leadership role in advancing progress in communities toward health equity.
Recommendation 7-4: The committee recommends that local policy makers assess policies, programs, initiatives, and funding allocations for their potential to create or increase health inequities in their communities.
Public health agencies can bring data, epidemiologic expertise, partnerships, and community engagement capacity in addition to commitments to achieving health equity. Because of previously established relationships, public health agencies are also natural conveners of certain health equity stakeholders, including health care systems, community organizations, and insurance companies. In addition, because
___________________
16 See, for example, McNeely and Norris (2015).
nontraditional partnerships are needed to successfully address the social, economic, and environmental factors influencing health equity, public health agencies can become conveners of community development organizations, faith-based organizations, businesses, and governmental agencies (e.g., transportation, housing, education). Furthermore, public health agencies have some of the data needed to link nontraditional partners’ work and interests to health and can serve as a source of evidence-based approaches that nontraditional partners can implement or support. The capacity of public health agencies as data repositories could be enhanced if more data were available and stratified by neighborhood levels for specific populations and health-related indicators, and if agencies could obtain data from a range of public- and private-sector sources, analyze it, and share it with partners and users in the community in a timely manner (RESOLVE, 2014).
In early 2016 the Governance Institute convened the first in a series of intensive trainings as part of Alignment of Governance & Leadership in Healthcare: Building Momentum for Transformation. The training, which will recur, was designed to orient health care delivery system executives to the potential of interfacing and partnering with the community development sector. Moreover, the Build Healthy Places Network, the Center on Social Disparities in Health, and RWJF have together put forward Making the Case for Linking: Community Development and Health, a brief highlighting multiple models and examples of health and development sector partnerships from around the country (Edmonds et al., 2015). The growing recognition that health is powerfully shaped by place calls on health sector practitioners, researchers, and decision makers to strengthen their relationships with the community development sector, from community development corporations that work to expand opportunity in communities to community development financial institutions and others.
Recommendation 7-5: The committee recommends that public health agencies and other health sector organizations build internal capacity to effectively engage community development partners and to coordinate activities that address the social and economic determinants of health. They should also play a convening or supporting role with local community coalitions to advance health equity.
New federal education legislation, the Every Student Succeeds Act,17 is a new mandate that requires school-level needs assessments, although
___________________
17 S.1177—Every Student Succeeds Act. Public Law 114-95 (December 10, 2015), 114th Cong.
access to quality data may persist as a barrier. For example, not all schools have good data on chronic absenteeism (ED, 2016b). Nor is information on school climate and neighborhood and on the community factors that affect learning widely available. See Chapter 6 for a recommendation (Recommendation 6-2) on state department guidance for student health needs assessments.
Recommendation 7-6: Given the strong effects of educational attainment on health outcomes and their own focus on equity (ED, 2016c), the U.S. Department of Education Institute for Educational Science and other divisions in the department should support states, localities, and their community partners with evidence and technical assistance on the impact of quality early childhood education programs, on interventions that reduce disparities in learning outcomes, and on the keys to success in school transitions (i.e., pre-K and K–12 or K–12 postsecondary).
Given the crucial importance of health equity to the nation’s economic and growth prospects and to communities’ well-being and vibrancy, high-level attention and coordination are needed to ensure that efforts to rein in inequity succeed. The current state of health disparities has severe consequences for the nation, and it is a call to action to stem the high human and economic cost of health inequity. Clearly, considerable support for addressing health equity has been established in the U.S. Department of Health and Human Services and across the executive branch through the Federal Interagency Health Equity Taskforce. In November 2016, the President signed an executive order establishing a community solutions council charged with fostering “collaboration across agencies, policy councils, and offices to coordinate actions, identify working solutions to share broadly, and develop and implement policy recommendations that put the community-driven, locally led vision at the center of policymaking” (The White House, 2016). Sustaining and elevating cross-government effort is important to help galvanize a national effort toward promoting health equity and to encourage ongoing multi-sectoral community-based efforts around the country.
Recommendation 7-7: The committee recommends that key federal government efforts, such as the Community Solutions Council, that are intended to support communities in addressing major challenges, consider integrating health equity as a focus.
A health equity focus could mean undertaking such approaches as:
- Determining how government decisions in health and non-health sectors could affect low-income and minority populations.
- Convening key stakeholders to explore financing structures through which companies, philanthropy, and government can together fund key health equity initiatives, including efforts to generate better, timelier, and more locally relevant data.
The importance of considering the unintended consequences of government policies is evident. For example, Chapter 3 describes examples of historical government policies that shaped government investment, land use, transportation, planning, and other features of communities with disproportionately negative effects on access to housing, safety, social cohesion, family stability, and health outcomes in low-income and minority populations (Freeman and Braconi, 2002; Fullilove and Wallace, 2011; IOM, 2003; Levy et al., 2006; Prevention Institute, 2011; Vélez, 2001; Zuk et al., 2015). Weighing the consequences on health outcomes, however, will require access to more varied and meaningful sources of data and may demand resources for analysis and assessment. The unique circumstances and context of each community (defined by census tract or zip code) may make it difficult to undertake such an assessment of potential consequences in a way that considers their full scope.
Public–private partnerships offer opportunities for innovation and alignment of resources that can achieve greater efficiency and effectiveness. Examples include pay-for-success financing models to support early childhood development and other programs, the Sustainable Communities federal partnership that brought together public- and private-sector actors to align their efforts, and clean energy financing arrangements (IOM, 2015b; PolicyLink, n.d.; Probst, 2014).
TOOLS
In its gathering of community examples and review of the literature, the committee identified a number of guiding principles for community consideration. They are provided in Box S-2, along with the three key elements found in all nine examples of community-based solutions to promote health equity highlighted in Chapter 5.
Chapter 8 provides a range of tools for facilitating multi-sector collaboration, making health equity a shared vision and value, and building capacity to shape outcomes in the community. Depending on a specific community’s needs and current available resources, some tools may be more applicable for them than others. The tools outlined in this chapter include making the case for health equity; meeting data information
needs, with available data sources and interactive tools outlined; adopting theories of change; using civil rights law; medical–legal partnerships; health impact assessments; funding mechanisms; public will building; capacity building for multiple purposes; and a list of community tool kits.
CONCLUDING OBSERVATIONS
There are systemic root causes of health inequities in this country that can seem overwhelming to local communities working to tackle unemployment, concentrated poverty, and school dropout rates. It will take considerable time to address these root causes, and it will require system-level changes to reduce poverty, eliminate structural racism, improve income equality, increase educational opportunity, and fix the laws and policies that perpetuate structural inequities. All actors in the community—businesses, state and local governments, anchor institutions, and other community residents—have the power to change the narrative and help promote health equity. Although the report focuses
on community-based solutions, where possible, promising strategies to address these hard-to-tackle root causes at higher levels are provided, including the policy context and the supportive actions of partners.
REFERENCES
Adler, N. E., and J. Stewart. 2010. Health disparities across the lifespan: Meaning, methods, and mechanisms. Annals of the New York Academy of Sciences 1186:5–23.
Aizer, A., J. Currie, P. Simon, and P. Vivier. 2015. Inequality in lead exposure and the black-white test score gap. Institute for Public Policy and Social Research. https://www.ippsr.msu.edu/research/inequality-lead-exposure-and-black-white-test-score-gap (accessed December 9, 2016).
Alley, D. E., C. N. Asomugha, P. H. Conway, and D. M. Sanghavi. 2016. Accountable Health Communities—Addressing Social Needs through Medicare and Medicaid. The New England Journal of Medicine 374(1):8.
Arias, E. 2016. Changes in life expectancy by race and Hispanic origin in the United States, 2013–2014. Hyattsville, MD: National Center for Health Statistics.
Beatty, A., and D. Foster. 2015. The determinants of equity: Identifying indicators to establish a baseline of equity in King County. King County, WA: King County Office of Performance, Strategy, and Budget.
Bell, J., and L. Cohen. 2009. The Transportation Prescription: Bold new ideas for healthy, equitable transportation reform in America, 2009. Commissioned by the Convergence Partnership. https://www.preventioninstitute.org/sites/default/files/publications/The%20Transportation%20Prescription_0.pdf (accessed December 14, 2016).
Berwick, D. M., T. W. Nolan, and J. Whittington. 2008. The triple aim: Care, health, and cost. Health Affairs 27(3):759–769.
Bethell, C. D., P. Newacheck, E. Hawes, and N. Halfon. 2014. Adverse childhood experiences: Assessing the impact on health and school engagement and the mitigating role of resilience. Health Affairs 33(12):2106–2115.
Braveman, P., and L. Gottlieb. 2014. The social determinants of health: It’s time to consider the causes of the causes. Public Health Reports 129(Suppl 2):19–31.
Braveman, P. A., S. Kumanyika, J. Fielding, T. LaVeist, L. N. Borrell, R. Manderscheid, and A. Troutman. 2011. Health disparities and health equity: The issue is justice. American Journal of Public Health 101(Suppl 1):S149–S155.
Carr, M. D., and E. Wiemers. 2016. The decline in lifetime earnings mobility in the U.S.: Evidence from survey-linked administrative data. Washington, DC: Washington Center for Equitable Growth.
CDC (U.S. Centers for Disease Control and Prevention). 2015. CDC community health improvement navigator. http://www.cdc.gov/chinav/ (accessed October 28, 2016).
ChangeLab Solutions. 2016. Model Comprehensive Plan Language on Complete Streets: A framework to embrace complete streets principle. http://www.changelabsolutions.org/publications/comp-plan-language-cs (accessed October 24, 2016).
Chetty, R., M. Stepner, S. Abraham, S. Lin, B. Scuderi, N. Turner, A. Bergeron, and D. Cutler. 2016. The association between income and life expectancy in the United States, 2001–2014. JAMA 315(16):1750–1766.
Christeson, W., A. D. Taggart, and S. Messner-Zidell. 2009. Ready, willing, and unable to serve: 75 percent of young adults cannot join the military. Early education across America is needed to ensure national security. Washington, DC: Mission: Readiness.
Clear, T. R. 2008. The effects of high imprisonment rates on communities. Crime and Justice 37(1):97–132.
Community Tool Box. 2016. Chapter 1. Section 7. Working together for healthier communities: A framework for collaboration among community partnership, support organizations, and funders. http://ctb.ku.edu/en/table-of-contents/overview/model-for-community-change-and-improvement/framework-for-collaboration/main (accessed October 18, 2016).
Cooper, L. A., D. L. Roter, R. L. Johnson, D. E. Ford, D. M. Steinwachs, and N. R. Powe. 2003. Patient-centered communication, ratings of care, and concordance of patient and physician race. Annals of Internal Medicine 139(11):907–915.
Council for a Strong America. 2016. New 50-state index from Council for a Strong America shows most young adults not “citizen-ready”: Crime and inability to join military or workforce present national crisis. Marketwired, September 13.
Davidoff, F., and P. Batalden. 2005. Toward stronger evidence on quality improvement. Draft publication guidelines: The beginning of a consensus project. Quality & Safety in Health Care 14(5):319–325.
Diez Roux, A. V., and C. Mair. 2010. Neighborhoods and health. Annals of the New York Academy of Sciences 1186(1):125–145.
Dubb, S., S. McKinley, and T. Howard. 2013. Achieving the anchor promise: Improving outcomes for low-income children, families and communities. Takoma Park, MD: Democracy Collaborative.
ED (U.S. Department of Education). 2016a. Healthy students, promising futures: State and local action steps and practices to improve school-based health toolkit. https://www2.ed.gov/admins/lead/safety/healthy-students/toolkit.pdf (accessed October 17, 2016).
ED. 2016b. Chronic absenteeism in the nation’s schools: An unprecedented look at a hidden educational crisis. https://www2.ed.gov/datastory/chronicabsenteeism.html (accessed October 28, 2016).
ED. 2016c. The fiscal year 2017 budget: Promoting greater use of evidence and data as a lever for advancing equity. In Homeroom: The Official Blog of the U.S. Department of Education. http://www2.ed.gov/admins/lead/safety/healthy-students/index.html (accessed October 24, 2016).
Edmonds, A., P. Braveman, E. Arkin, and D. Jutte. 2015. Making the case for linking community development and health: A resource for those working to improve low-income communities and the lives of the people living in them. UCSF Center on Social Disparities in Health, Robert Wood Johnson Foundation, and the Build Healthy Places Network.
Freeman, L., and F. Braconi. 2002. Gentrification and displacement. The Urban Prospect 8(1).
FSG (Foundation Strategy Group). 2011. Collective impact. http://www.fsg.org/ideas-in-action/collective-impact (accessed October 18, 2016).
FSG. 2013. Using collective impact in a public health context: Introduction. http://www.fsg.org/blog/using-collective-impact-public-health-context-introduction (accessed October 18, 2016).
Fullilove, M. T., and R. Wallace. 2011. Serial forced displacement in American cities, 1916–2010. Journal of Urban Health 88(3):381–389.
Graham, H. 2004. Social determinants and their unequal distribution: Clarifying policy understandings. Milbank Q 82(1):101–124.
Harkavy, I., M. Hartley, R. A. Hodges, A. Sorrentino, and J. Weeks. 2014. Effective governance of a university as an anchor institution: University of Pennsylvania as a case study. Leadership and Governance in Higher Education 2:98–116.
HERO (Health Enhancement Research Organization). 2015. Exploring the value proposition for workforce health: Business leader attitudes about the role of health as a driver of productivity and performance. http://hero-health.org/wp-content/uploads/2015/02/HPP-Business-Leader-Survey-Full-Report_FINAL.pdf (accessed October 24, 2016).
Howard, T. C. 2010. Why race and culture matter in schools: Closing the achievement gap in America’s classrooms. New York: Teachers College Press.
IOM (Institute of Medicine). 2003. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The National Academies Press.
IOM. 2011. For the public’s health: Revitalizing law and policy to meet new challenges. Washington, DC: The National Academies Press.
IOM. 2012. For the public’s health: Investing in a healthier future. Washington, DC: The National Academies Press.
IOM. 2015a. Business engagement in building healthy communities: Workshop summary. Washington, DC: The National Academies Press.
IOM. 2015b. Financing population health improvement. Washington, DC: The National Academies Press.
IOM and NRC (Institute of Medicine and National Research Council). 2013. Priorities for research to reduce the thread of firearm-related violence. Washington, DC: The National Academies Press.
IRS (Internal Revenue Service). 2016. Statistics for tax returns with EITC. https://www.eitc.irs.gov/EITC-Central/eitcstats?_ga=1.80629535.982617637.1477348670 (accessed December 19, 2016).
Jimenez, M. E., N. E. Reichman, R. Wade, Y. Lin, and L. M. Morrow. 2016. Adverse experiences in early childhood and kindergarten outcomes. Pediatrics 137(2).
Jones, H. 2009. Equity in development: Why it is important and how to achieve it. London, UK: Overseas Development Institute.
Kenney, G. M., and M. Huntress. 2012. The Affordable Care Act: Coverage implications and issues for immigrant families. https://aspe.hhs.gov/basic-report/affordable-care-act-coverage-implications-and-issues-immigrant-families (accessed October 24, 2016).
Kindig, D., and G. Stoddart. 2003. What is population health? American Journal of Public Health 93(3):380–383.
Krieger, N. 2014. Discrimination and Health Inequities. International Journal of Health Services 44(4):643–710.
Kruse, C. S., S. Bouffard, M. Dougherty, and J. S. Parro. 2016. Telemedicine use in rural Native American communities in the era of the ACA: A systematic literature review. Journal of Medical Systems 40(6):145.
LaVeist, T. A., D. J. Gaskin, and P. Richard. 2009. The economic burden of health inequalities in the United States. Washington, DC: Joint Center for Political and Economic Studies.
Levy, D. J., J. A. Heissel, J. A. Richeson, and E. K. Adam. 2016. Psychological and biological responses to race-based social stress as pathways to disparities in educational outcomes. American Psychologist 71(6):455–473.
Levy, D. K., J. Comey, and S. Padilla. 2006. In the face of gentrification: Case studies of local efforts to mitigate displacement. Washington, DC: Urban Institute.
Losen, D., C. Hodson, M. A. Keith II, K. Morrison, and S. Belway. 2015. Are we closing the school discipline gap? Los Angeles: University of California.
Marmot, M., J. Allen, P. Goldblatt, T. Boyce, D. McNeish, M. Grady, and I. Geddes. 2010. Fair society, healthy lives: Strategic review of health inequalities in England post-2010. London: The Marmot Review.
Martin, L. L., H. Smith, and W. Phillips. 2005. Bridging ‘town & gown’ through innovative university-community partnerships. The Innovation Journal: The Public Sector Innovation Journal 10(2). http://www.innovation.cc/volumes-issues/martin-u-partner4final.pdf (accessed October 20, 2016).
McNeely, E., and G. Norris. 2015. SHINE summit 2015: Innovating for NetPositive impact: Summary report. Boston, MA: Sustainability and Healthy Initiative for NetPositive Enterprise.
Miller, D. S., and J. D. Rivera. n.d. Town and gown: Understanding the past to improve the future. International Journal of the Humanities 3(8):215–224.
Minkler, M., A. P. Garcia, J. Williams, T. LoPresti, and J. Lilly. 2010. Si se puede: Using participatory research to promote environmental justice in a Latino community in San Diego, California. Journal of Urban Health 87(5):796–812.
Mosavel, M., R. Ahmed, D. Daniels, and C. Simon. 2011. Community researchers conducting health disparities research: Ethical and other insights from fieldwork journaling. Social Science & Medicine 73(1):145–152.
Multnomah County. 2014a. Foundational assumptions of the equity and empowerment lens logic model. https://multco.us/file/31824/download (accessed October 28, 2016).
Multnomah County. 2014b. Multnomah County Office of Diversity and Equity: Equity and empowerment lens. https://multco.us/diversity-equity/equity-and-empowerment-lens (accessed October 24, 2016).
Multnomah County. n.d. What is the equity and empowerment lens?https://multco.us/diversity-equity/equity-and-empowerment-lens (accessed October 28, 2016).
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016a. Accounting for social risk factors in Medicare payment: Identifying social risk factors. Washington, DC: The National Academies Press.
NASEM. 2016b. Accounting for social risk factors in Medicare payment: Criteria, factors, and methods. Washington, DC: The National Academies Press.
NASEM. 2016c. Accounting for social risk factors in Medicare payment: Data. Washington, DC: The National Academies Press.
NASEM. 2016d. The role of business in multisector obesity solutions: Working together for positive change: Workshop in brief. Washington, DC: The National Academies Press.
NASEM. 2016e. Systems practices for the care of socially at-risk populations. Washington, DC: The National Academies Press.
NIH (National Institutes of Health). 2014. Health disparities. http://www.nhlbi.nih.gov/health/educational/healthdisp/ (accessed November 2, 2016).
Norris, T., and T. Howard. 2015. Can Hospitals Heal America’s Communities?
NRC (National Research Council). 2014. The growth of incarceration in the United States: Exploring causes and consequences. Washington, DC: The National Academies Press.
NRC and IOM. 2013. U.S. health in international perspective: Shorter lives, poorer health. Washington, DC: The National Academies Press.
NTFAI (National Task Force on Anchor Institutions). 2010. Anchor institutions task force. http://www.margainc.com/files_images/general/anchor_task_force_statement.pdf (accessed October 20, 2016).
OECD (Organisation for Economic Co-operation and Development). 2015. Health at a glance: OECD indicators. Paris: OECD Publishing.
O’Mara, M. P. 2012. Beyond town and gown: University economic engagement and the legacy of the urban crisis. Journal of Technology Transfer 37(2):234–250.
PHAB (Public Health Accreditation Board). 2011. Public Health Accreditation Board standards & measures, version 1.0. http://www.phaboard.org/wp-content/uploads/PHAB-Standards-and-Measures-Version-1.01.pdf (accessed December 2, 2016).
PolicyLink. n.d. Center for Infrastructure Equity: Sustainable communities. http://www.policylink.org/focus-areas/infrastructure-equity/sustainable-communities (accessed December 1, 2016).
Prevention Institute. 2011. Fact Sheet: Links between violence and health equity. Oakland, CA: Prevention Institute.
Probst, C. S. 2014. Private sector financing and public-private partnerships for financing clean energy. Research Program on Sustainability Policy and Management, Earth Institute, Columbia University.
Prybil, L., F. D. Scutchfield, R. Killian, A. Kelly, G. Mays, A. Carman, S. Levey, A. McGeorge, and D. W. Fardo. 2014. Improving community health through hospital–public health collaboration: Insights and lessons learned from successful partnerships. In Health
Management and Policy Faculty Book Gallery: Book 2. Lexington, KY: Commonwealth Center for Governance Studies, Inc.
Reardon, S. F., R. A. Valentino, and K. A. Shores. 2012. Patterns of literacy among U.S. students. Future of Children 22(2):17–37.
RESOLVE. 2014. The high achieving governmental health department in 2020 as the community chief health strategist. Washington, DC: RESOLVE.
Rubin, V., and K. Rose. 2015. Strategies for strengthening anchor institutions’ community impact. Oakland, CA: PolicyLink.
Rudolph, L., S. Gould, and J. Berko. 2015. Climate change, health, and equity: Opportunities for action. https://www.phi.org/uploads/application/files/h7fjouo1i38v3tu427p9s9kcmhs3oxsi7tsg1fovh3yesd5hxu.pdf (accessed October 24, 2016).
Sabin, J., B. A. Nosek, A. Greenwald, and F. P. Rivara. 2009. Physicians’ implicit and explicit attitudes about race by MD race, ethnicity, and gender. Journal of Health Care for the Poor and Underserved 20(3):896–913.
Salway, S., P. Chowbey, E. Such, and B. Ferguson. 2015. Researching health inequalities with community researchers: Practical, methodological and ethical challenges of an “inclusive” research approach. Research Involvement and Engagement 1(1).
Serang, F., J. P. Thompson, and T. Howard. 2013. The anchor mission: Leveraging the power of anchor institutions to build community wealth. Takoma Park, MD: The Democracy Collaborative.
Skiba, R. J., R. H. Horner, C.-G. Chung, M. K. Rausch, S. L. May, and T. Tobin. 2011. Race is not neutral: A national investigation of African American and Latino disproportionality in school discipline. School Psychology Review 40(1):85–107.
Smith, E. J., and S. R. Harper. 2015. Disproportionate impact of K-12 school suspension and ex-plusion on black students in southern states. Philadelphia, PA: Penn Graduate School of Education Center for the Study of Race and Equity in Education.
The White House. 2016. Executive Order—Establishing a Community Solutions Council. https://www.whitehouse.gov/the-press-office/2016/11/16/executive-order-establishing-community-solutions-council (accessed December 1, 2016).
Uberoi, N., K. Finegold, and E. Gee. 2016. Health insurance coverage and the Affordable Care Act, 2010-2016. Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services.
Ubri, P., and S. Artiga. 2016. Disparities in health and health care: Five key questions and answers. http://files.kff.org/attachment/Issue-Brief-Disparities-in-Health-and-Health-Care-Five-Key-Questions-and-Answers (accessed October 24, 2016).
Vélez, M. B. 2001. Role of public social control in urban neighborhoods: A multi-level analysis of victimization risk. Criminology 39(4):837-864.
Verbitsky-Savitz, N., M. B. Hargreaves, S. Penoyer, N. Morales, B. Coffee-Borden, and E. Whitesell. 2016. Preventing and mitigating the effects of ACEs by building community capacity and resilience: APPI cross-site evaluation findings. Washington, DC: Mathematica Policy Research.
Waidmann, T. 2009. Estimating the cost of racial and ethnic health disparities. Washington, DC: Urban Institute.
Williams, D. R., and C. Collins. 2001. Racial residential segregation: A fundamental cause of racial disparities in health. Public Health Reports 116(5):404–416.
Woolf, S. H., L. Aron, L. Dubay, S. M. Simon, E. Zimmerman, and K. X. Luk. 2015. How are income and wealth linked to health and longevity? Washington, DC: Urban Institute and Virginia Commonwealth University.
Zuk, M., A. H. Bierbaum, K. Chapple, K. Gorska, A. Loukaitou-Sideris, P. Ong, and T. Thomas. 2015 (unpublished). Gentrification, displacement, and role of public investment: A literature review. Federal Reserve Bank of San Francisco.






























