5
Examples of Communities Tackling Health Inequity
Communities across the United States are developing and putting into action strategies that can contribute to the reduction of health inequities. Too often these community efforts go unmentioned in the media while stories of blight, crime, or community unrest receive more attention. The committee was asked to identify and examine six or more examples of community-based solutions (see the report conceptual model in Figure 5-1) that address health inequities, drawing from interventions or activities that intentionally or indirectly promote equal opportunities for health. The examples identified in this chapter span health and non-health sectors and take into account the range of factors that contribute to health inequity in the United States, such as systems of employment, public safety, housing, transportation, education, and others. The committee provides a summary of each example to demonstrate both the innovative work conducted by communities and the challenges that they face. The committee also comments on a number of crosscutting essential elements that show promise for promoting health equity in communities. Finally, the committee summarizes a number of lessons learned from both the success and the failures of the strategies described.
PROCESS OF SELECTION
The committee engaged in a robust process, described in complete detail in the Chapter 5 Annex, to review a total of 105 examples gathered and select the 9 community examples that are outlined in this chapter.
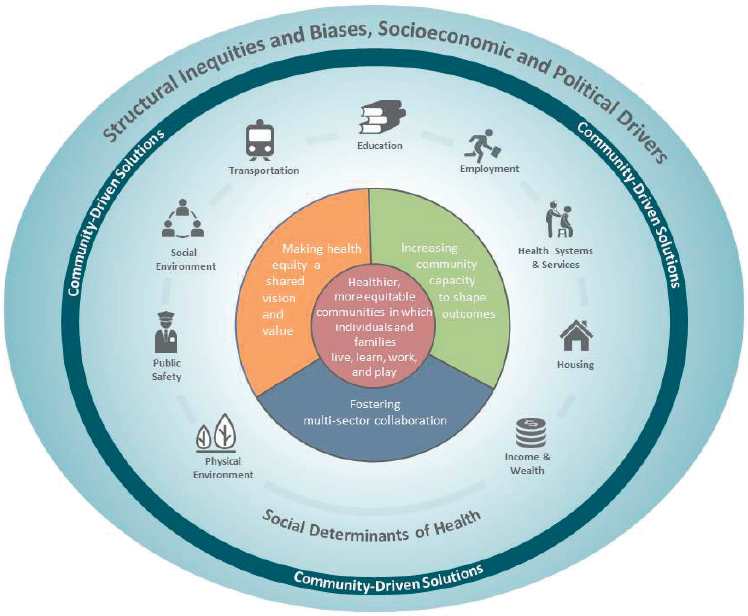
NOTE: The community-driven solutions are highlighted here to convey the focus of this chapter.
In brief, the committee queried local and state organizations, relevant philanthropic organizations, researchers and others; reviewed relevant reports and publications on the topic of community health; and undertook a literature review. It is important to note that the committee did not evaluate the overall effectiveness of these community efforts. Rather, the committee sought out community-driven solutions that target the social determinants of health with strong links to health outcomes, as evidenced by the literature. The committee developed three sets of criteria to guide the selection of the case studies:
- Core criteria: All examples chosen for this chapter must
- address at least one (preferably more) of the nine social determinants of health identified by the committee (education, employment, health systems and services, housing, income
- community-driven
- multi-sectoral
- evidence-informed
and wealth, physical environment, public safety, social environment, and transportation) and be
- Aspirational criteria: Examples were considered based on the convening organization’s ability to engage nontraditional partners and to work in an interdisciplinary and multilevel manner and also on the documentation of plans to achieve outcomes and sustain the effort.
- Contextual criteria: Examples were chosen to reflect a diversity of communities, populations, solutions, and demographic characteristics.
COMMUNITY EXAMPLES1
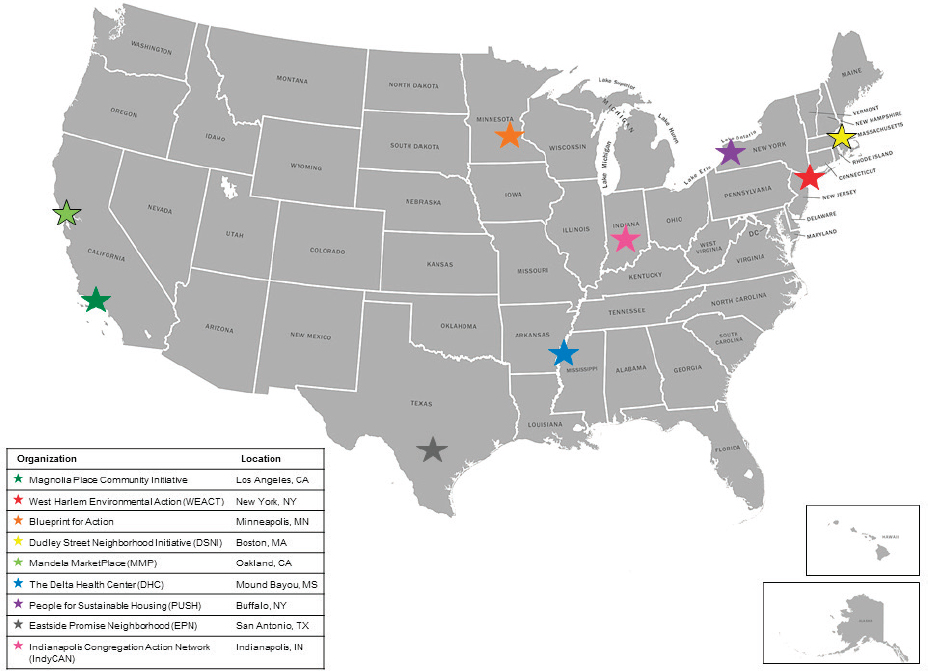
The following section summarizes the strategies of nine communities whose efforts focus on addressing the social determinants of health across a number of different geographic locations, environments, and community challenges (see Figure 5-2 for the geographic distribution). These summaries highlight the core and aspirational criteria that the committee developed and the approach that each community took toward making health equity a shared vision and value, increasing community capacity to shape outcomes and fostering multi-sector collaboration as well as showing how the strategies addressed the broader socioeconomic and political context to ultimately achieve healthier, more equitable communities. For easy reference, Table 5-1 lists the nine communities, the social (or environmental, or economic) determinants of health they address, and the key sectors with which each community partnered to implement its solutions. The community efforts described are not intended to reflect the full range of communities across the United States and of effective community-driven efforts to improve well-being and health equity. For example, the communities do not include an example from the lesbian, gay, bisexual, and transgender (LGBT) community or one that reflects individuals with disabilities or individuals with mental illness.2
___________________
1 Community examples are provided in alphabetical order.
2 For example, LGBT advocates, addressing the regulatory hurdles to timely and appropriate research for better AIDS treatments, protested and advocated for change and succeeded in substantially altering the way the National Institutes of Health reviews and conducts human subjects research across all domains. For other examples of successful efforts among these groups, see http://dralegal.org/cases (accessed July 17, 2016) for a list of lawsuits conducted by Disability Rights Advocates, the mental health parity work conducted by the National Alliance on Mental Illness (NAMI), or the Bithlo Transformation Effort (http://stakeholderhealth.org/transformative-partnership/case-study-bithlo [accessed August 28, 2016]).
Each of the nine community initiatives is at a different phase of development: some have been around for more than 40 years, while others emerged in the past few years, and each has a unique approach. Because the examples went beyond traditional health or health care approaches, the outcomes are often tied to specific project goals rather than to the long-term health outcomes that emerge from these benefits. For example, a community whose focus is on housing might measure the number of low-income housing units that became available, and a community effort focused on education might measure improvement in third-grade reading levels or increased levels of high school graduation rates—all measures that are proxies for the long-term achievement of improved health. The committee also used these examples to identify some of the intangible qualities needed to initiate, maintain, and sustain community efforts.
The committee was inspired by the communities described in this chapter and is grateful to them for their willingness to share their history and accomplishments for this report. These examples serve as a proof of principle that communities can mobilize to promote effective change that addresses multiple determinants of health. These examples are not blueprints. Exact replicas of these communities’ interventions might not work in other communities, but their lessons learned will prove valuable to many communities that hope to create positive change.
Minneapolis Blueprint for Action to Prevent Youth Violence3

Background and History

The Minneapolis Blueprint for Action to Prevent Youth Violence4 is a community-driven, grassroots response to the issue of youth violence, originally developed in 2008. From 2002 to 2011, homicide was
___________________
3 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
4 For more information, see http://www.minneapolismn.gov/health/youth/yvp/blueprint (accessed September 13, 2016).
TABLE 5-1 Nine Community Examples—Brief Information
| Blueprint for Action | Delta Health Center | Dudley Street Neighborhood Initiative | Eastside Promise Neighborhood | |
|---|---|---|---|---|
| Location | Minneapolis, MN | Mississippi Delta | Boston, MA | San Antonio, TX |
| Social determinant of health | ||||
| Education | • | • | •* | |
| Employment | • | •* | • | |
| Health systems and services | • | •* | ||
| Housing | • | |||
| Income and wealth | • | • | ||
| Physical environment | • | • | •* | • |
| Public safety | •* | • | • | |
| Social environment | • | • | • | |
| Transportation | • | • | ||
| Key community partners | County and city departments, local school district, local youth agencies, faith-based organizations, local businesses | Community health associations, educational institutions, agricultural co-ops | Other community stakeholder organizations, educational institutions, nonprofit organizations | Local nonprofits, local school district, city agencies, faith-based organizations, educational institutions, health providers, local elected officials |
| Outcomes |
From 2007–2015:
|
|
From 2014–2015:
|
From 2015–2016, number of survey respondents who answered that:
Child care is available to them when needed most of the time or sometimes increased from 80% to 100% |
| Indianapolis Congregation Action Network | Magnolia Community Initiative | Mandela MarketPlace | People United for Sustainable Housing | WE ACT for Environmental Justice |
|---|---|---|---|---|
| Indianapolis, IN | Los Angeles, CA | Oakland, CA | Buffalo, NY | West Harlem, NY |
| • | • | |||
| • | • | • | ||
| • | ||||
| •* | • | |||
| • | ||||
| • | •* | • | •* | |
| • | ||||
| • | •* | • | • | • |
| • | • | |||
| Faith-based organizations, businesses, government, community leaders | More than 70 partner organizations, including government, nonprofit, for-profit, faith, and community group associations that connect programs and providers | Local businesses, educational institutions, youth development organizations, housing developers, government agencies, foundations | Government agencies (housing, energy, parks), local elected officials, nonprofits and NGOs, private-sector businesses | Academic institutions and CBPRers, housing groups, legal partners, energy and solar providers, government agencies, local elected officials |
|
|
|
|
|
| Blueprint for Action | Delta Health Center | Dudley Street Neighborhood Initiative | Eastside Promise Neighborhood | |
|---|---|---|---|---|
|
They work with others to improve their neighborhood increased from 58% to 83% Their neighborhood has safe places for kids to play increased from 40% to 67% |
NOTES: Outcomes as calculated and reported by each of the community initiatives. An asterisk (*) denotes the main social (or environmental or economic) determinant(s) of health on which the community focused. BPA = bisphenol A; CBPR = community-based participatory research; NGO = nongovernmental organization; PICO = People Improving Communities through Organization.
the leading cause of death among Minneapolis residents ages 15–24 years, accounting for 39 percent of deaths in this age group and disproportionately affecting youth of color (Blueprint for Action, 2013). Resident perceptions of safety differed across racial/ethnic groups as well. In 2006, a county survey revealed that gangs were considered a neighborhood problem by 40 percent of Hispanics, 35 percent of African Americans, 24 percent of Asians/Pacific Islanders, and 11 percent of whites (see Table 5-2 for data on Minneapolis demographics) (Blueprint for Action, 2013).
By 2008, the city of Minneapolis had already been expending its resources through various law enforcement strategies to address the staggering rates of youth violence, but the city was not seeing sufficient results from those efforts (Zanjani, 2011). A call for governmental action
| Indianapolis Congregation Action Network | Magnolia Community Initiative | Mandela MarketPlace | People United for Sustainable Housing | WE ACT for Environmental Justice |
|---|---|---|---|---|
|
|
|
housing units, number of employed workers, amount of carbon emission reduction, and utility bill cost savings for low-income households |
phthalates in consumer products, pesticides, and flame retardants |
was put out by community members and stakeholders, including members of an advisory group comprised of youth-serving organizations and community leaders who were knowledgeable about the various cultural communities in Minneapolis.
The outcome was the first Blueprint for Action, which is a coordinated, strategic plan to apply the public health approach to violence prevention through evidence-based strategies and by engaging multiple partners and stakeholders. The mayor recommended a roster of stakeholders to engage and the city council adopted a motion that specifically identified partners to include in the process of development. Leaders who came together to develop the blueprint included representatives from law enforcement, juvenile supervision, public health, youth programs,
TABLE 5-2 City of Minneapolis Demographics
| Total | ~410,939 residents |
| Race/Ethnicity | 63.8% White |
| 18.6% African American | |
| 10.5% Latino or Hispanic | |
| 5.6% Asian | |
| 2.0% Native American/American Indian | |
| Gender | 49.7% female |
| Age | 6.9% under 5 years |
| 20.2% under 18 years | |
| 8.0 % 65 years and over | |
| Education | 89% completed high school |
| 16% received bachelor’s degree or higher | |
| Employment | 3.3% unemployed |
| Income | $50,767 median income |
| 22.6% in poverty |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: BLS, 2016; U.S. Census Bureau, 2015b.
education, social services, faith communities, neighborhoods, and city and county government. The goals of the current blueprint5 are to
- foster violence-free social environments
- promote positive opportunities and connections to trusted adults for all youth
- intervene with youth and their families at first sign of risk
- restore youth who have gone down the wrong path
- protect children and youth from violence in the community
These goals provided a framework under which to align the many programs, services, and other efforts that were incorporated into the blueprint, some of which were already under implementation by community groups, nonprofits, and government agencies in Minneapolis.
When the call for action to respond to youth violence was received, a citywide collaborative effort, supported by the Minneapolis Foundation and the mayor, was undertaken. First, the Minneapolis City Council passed a resolution declaring youth violence a public health issue and it created a steering committee that led to the development of the Blueprint for Action. The Minneapolis health department and Minneapolis
___________________
5 For more information on the 2013 Blueprint for Action, see http://www.minneapolismn.gov/www/groups/public/@health/documents/webcontent/wcms1p-114466.pdf (accessed September 13, 2016).
Foundation examined youth arrest and detention data and upstream risk and protective factors for youth violence. This evidence informed such blueprint program components as employment programs, an anonymous tip line, a gang prevention and healthy youth development curriculum, and a neighborhood clean sweep program.6
Across neighborhoods, disparities in economic conditions are apparent throughout the city of Minneapolis. For example, the annual household income is quite different in such low-income communities as Near North (median income $24,733) and Phillips (median income $25,125) than it is in communities such as Southwest (median income $94,667, a nearly fourfold difference) (Minnesota Compass, 2016). The blueprint was developed with the understanding that the communities suffering from concentrated poverty were also experiencing disproportionate amounts of youth violence. According to a county-level survey in 2010, more than half (57 percent) of the adults in the Camden and Near North communities and about one-third (33 percent) of the adults in the Central, Phillips, and Powderhorn communities cited gangs as a serious problem, compared with only 10 percent of adults who lived in other neighborhoods of Minneapolis (Blueprint for Action, 2013).
Initially, the program focused on youth ages 8–17 who resided in neighborhoods experiencing the highest rates of crime and violence. In 2009 the program expanded to 22 neighborhoods, and the target age range was extended to age 24, based on indicators that demonstrated a higher risk of youth violence in Minneapolis for this population. These indicators were based on data compiled by the local health department from sources across various sectors, including the U.S. Census, the Minneapolis Police Department, Minnesota Hospital Association, and the Minneapolis Park and Recreation Board. The blueprint also developed criteria factors for the target neighborhoods based on available data:
- rate of homicides
- rate of violent crime
- rate of firearm-related assault injuries
- population under 15 years of age
- percent of families in poverty with related children under 18
- access to a Minneapolis Park and Recreation center
According to the Minneapolis Health Department, “the ultimate success of the blueprint is reliant on the extent to which community
___________________
6 For a list of the ongoing activities under the Blueprint for Action, see http://www.minneapolismn.gov/www/groups/public/@health/documents/webcontent/wcms1p-114466.pdf (accessed September 19, 2016).
stakeholders remain a part of the process” (Blueprint for Action, 2013). Community stakeholders include neighborhood associations, faith groups, schools, libraries, parks, local businesses, and block clubs. Furthermore, the blueprint connects with other communities facing similar challenges and applying a prevention approach to violence through networks such as the Prevention Institute’s UNITY initiative, the National Forum on Youth Violence Prevention (see Figure 5-3 for alignment of goals with the National Forum), and Cities United.
Solutions to Address the Social Determinants of Health
The underlying causes and correlates of violence overlap substantially with those of health inequity (Prevention Institute, 2011). Therefore, a multidisciplinary public health approach to the issue of youth violence, such as the one taken by Blueprint for Action, can have a significant impact on the social determinants of health.
Public safety The primary goal of the blueprint is to reduce homicides and firearm-related injuries, in addition to improving juvenile interactions with the criminal justice system as needed. One program that seeks to do
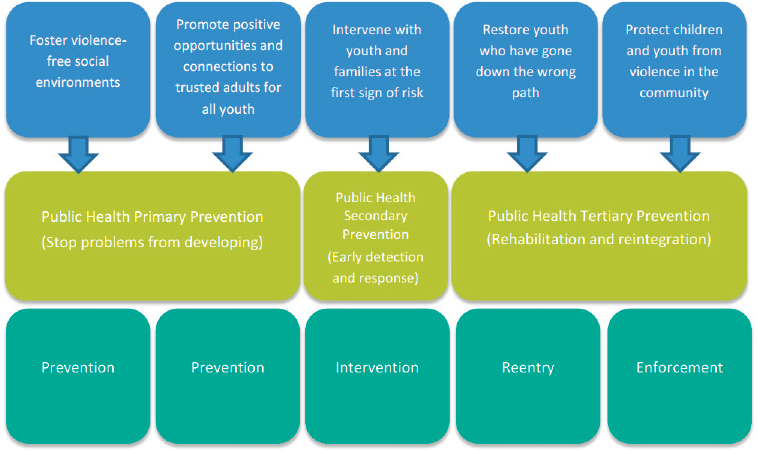
SOURCE: Blueprint for Action, 2013. Used with permission.
this is the Speak Up tip line, a confidential tip line for youth to report a threat of weapons in the community. The idea for this tip line originated from feedback given by young men in a dialogue portion of a meeting to develop the blueprint. While Speak Up received about 10–12 calls per month, data show that usage of the tip line is highly correlated with the amount of funding allocated to public awareness campaigning in the community.7 The blueprint also employs youth outreach teams in downtown Minneapolis and at high schools to facilitate the creation of an environment that redirects youth to positive activities.
For youth at risk of violent injury, the blueprint offers Inspiring Youth, a case management program, in addition to parental education and support for the youth’s families. The program serves 60 youth per year, with plans to increase the number of youth served in 2017. Inspiring Youth has received $100,000 per year from the City of Minneapolis general fund and $45,000 in 2016 and again in 2017 from the Minnesota Department of Public Safety Office of Justice Programs in the form of a Youth Intervention Program grant.
Inspiring Youth developed out of a repeated experience that the mayor had when he attended funerals of young people. He often heard ‘I knew this would happen’ from community members who knew the young person. The program was created to both identify youth at risk of being injured violently and to offer them support and services to help them avoid the risk of being involved in violence. —Gretchen Musicant, Commissioner of Health, City of Minneapolis Health Department, 2016
The blueprint implements BUILD, a gang prevention and healthy youth development curriculum for middle schoolers, and provides school resource officers who are evaluated based in part on the number of positive interactions they have with students. The BUILD curriculum provides youth with opportunities to learn about positive decision making, goal setting, and conflict resolution. Thus far, BUILD has been implemented at 10 sites, with the recent development of BUILD Leaders, a program focused on older youth, ages 18–24. Currently, there are two culturally specific groups applying this model in a Native American and an African American community.
Employment The blueprint provides employment and workforce development opportunities for youth as an alternative to engaging in delinquent or violent behavior. The North4 program is operated by Emerge, a place-based community development agency, and provides workforce and life skills training for youth who are gang-involved and who have
___________________
7 Source available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
had previous involvement with the juvenile justice system. This program works to remove barriers to employment that former offenders face when reintegrating into society. Another program designed to create employment opportunities for youth and reduce gang violence is BUILD Leaders, a program that employs older youth to teach an anti-gang curriculum to younger youth. Step Up is a summer employment program for youth (ages 16–21) in the private, nonprofit, and government sectors.
Physical environment The blueprint seeks to create and maintain a physical environment that is conducive to safe and peaceful activities in the community. For example, pop-up parks are part of a collaborative effort with the Minneapolis Park Board to bring activities to abandoned properties, under-programmed parks, and community events. This also entails an innovative graffiti prevention program which is designed to assist communities with projects for removing and preventing graffiti (see Figure 5-4). The Neighborhood Clean Sweep program partners with neighborhood associations to make neighborhoods cleaner.

NOTE: Used with permission by the artist.
Social environment As listed in its core goals, the blueprint is intended to foster a culture of nonviolence and positive interactions between youth and adults. The city’s participation in the national Youth Violence Prevention Week annually features community-based organizations that are fostering pro-social activities for youth and peacemaker awards for youth and adults. The awards result in a small financial grant to schools for additional peacemaking activities. Additionally, the blueprint has succeeded in expanding summer hours for out-of-school time, for youth to engage in structured, positive activities.
Health systems and services The blueprint has partnered with two local level I trauma center hospitals to improve health care services for victims of violence. Together, they developed a protocol for intervening and providing psychosocial assessments within 24 hours to every youth (ages 10–24) presenting with a violent injury to the emergency room. This protocol is active in one of the two hospitals, with plans to expand implementation to the other hospital. The blueprint’s next step is to implement an emergency department-based program at a level I trauma center hospital that connects youth injured violently with a staff member who knows the community to facilitate access to post-discharge resources and case management. Also in the planning phase is Project Connect, a program that addresses adolescent dating violence at school-based clinics in local high schools. Project Connect is funded by a state grant from the U.S. Department of Justice’s Office on Violence Against Women.
Education In addition to the above-mentioned activities in the school setting (e.g., school resource officers and Project Connect), the blueprint supports college scholarships for local students. The Power of You program provides tuition-free scholarships for community college which have been demonstrated to increase the number of students attending college and also retention rates (Minneapolis CPED, 2011). In fact, 80 percent of recipients report that the scholarship influenced their decision to go to college (Minneapolis CPED, 2011).
Transportation Because a lack of access to transportation can be a barrier to accessing important resources, especially in neighborhoods with high rates of violence, the blueprint seeks to increase access to safe transit for youth. Students in Minneapolis high schools are given free bus passes for transportation to and from school and to meet other transportation needs as well.
Data and Outcomes
The blueprint is intended to reduce outcomes that are measured systematically at the local level, such as number of firearm-related assault injuries, the number of youth homicides, the number of youth involved in violent crime, and other various outcomes related to the goals of the blueprint. Minneapolis collects data on performance measures and indicators for each goal across multiple sectors. Results Minneapolis8 is a management tool the city uses to systematically track performance toward achieving its goals, with data coming from the Minneapolis Police Department, schools, the Minneapolis hospital association, Department of Community Planning and Economic Development, and more. A review panel of city and community leaders meets to track progress and discuss strategies on key performance measures. By regularly tracking performance data at these “progress conferences,” city leaders identify areas where the city is excelling as well as opportunities for improvement. Following the implementation of the blueprint, Minneapolis saw an improvement in key outcomes. From 2007 to 2015, the number of youth gunshot victims decreased 62 percent, the number of youth victims of crime decreased by 34 percent, and the number of youth arrests with a gun decreased by 76 percent (City of Minneapolis, 2016).
Promoting Health Equity: Key Elements
The impetus for the blueprint originated from a shared vision for a unified city in which all youth are safe and able to thrive (Blueprint for Action, 2013). Achieving this vision will require a shift in norms and values throughout the community. Community members identified increased communication and outreach about blueprint efforts as well as the availability of safe spaces for youth as priorities for the blueprint in order to mobilize community members around the vision for a violence-free social environment (Blueprint for Action, 2013).
According to Sasha Cotton, the youth violence prevention coordinator at the Blueprint for Action, multi-sector collaboration has been essential to achieving outcomes in Minneapolis. Working closely with other city departments (e.g., juvenile corrections, police department), the county, the school district, local youth-serving agencies, faith-based organizations, local businesses, and other community stakeholders has given the effort a diversity of opinion and perspectives. The multi-sector partnerships required increased communication to reduce the redundancy of programs
___________________
8 For more information, see http://www.ci.minneapolis.mn.us/coordinator/rm/index.htm (accessed September 19, 2016).
across agencies (Zanjani, 2011). Other elements that are key to sustained relationships across sectors include relationship building through identifying co-benefits, shared responsibility, and strong leadership. These partnerships allowed for the coordination of data collection from various sectors to inform the blueprint’s objectives and priorities in addition to systematically tracking progress.
The blueprint has resulted in an increased capacity across multiple levels in Minneapolis, including the creation of a Youth Violence Prevention Executive Committee and a youth congress. The youth congress created a mechanism for youth to influence decisions and policies on education, housing, safety, employment, transportation, and health (Rybak, 2012). The youth congress has been able to shape important educational and employment programs such as The Power of You scholarship program.
The blueprint has also been able to leverage resources to support community-driven youth development initiatives. In the past 3 years, the Blueprint Approved Institute was created to build the organizational capacity of small community-based organizations serving youth. The institute provides a mechanism for grassroots organizations to gain insights into city government processes, in addition to providing opportunities for the city government to better meet the needs of the community it serves. One of the objectives of the Blueprint Approved Institute is to empower community-based organizations to have better success in competing for grant funding.
Challenges and Lessons Learned
One of the major barriers to sustaining the work of the blueprint, a plan that seeks to address community-level violence, is the transitional nature of the public’s interests and of public administration. To begin with, the issue of violence is not uniform from one neighborhood to the next. Each community will have varying concerns, needs, and tailored approaches for achieving its goals, which are always evolving with respect to current events. Furthermore, interests and priorities can shift with the advent of new political administrations. The blueprint team cites strong leadership and deep connections to the community as elements that are critical to stabilizing a plan such as Blueprint for Action across neighborhoods and over time.
Sustaining Success
In 2009 the City of Minneapolis successfully lobbied for the passage of state legislation—the Youth Violence Prevention Act of 2009—which declared youth violence as a public health issue statewide and created
three additional pilot sites in Minnesota. During the first year of the blueprint, the city budget adopted by the mayor included $175,000 to support implementation. Over the years, both ongoing and one-time funding from the city has been augmented by state and national grants as well as by some private philanthropic grants. As a result of the blueprint’s success, blueprint recommendations continue to inform budget decisions made by the mayor and city council. In order to maintain the cross-sector relationships, biweekly multi-jurisdictional meetings are held to facilitate shared information, relationship building, and problem solving. Furthermore, the blueprint established a youth violence prevention coordinator position which is housed in the Minneapolis Health Department. The placement of this role in the city’s health agency, rather than in an elected official’s office, has been a critical component of the sustainability of the initiative.
Delta Health Center9

Background and History

Delta Health Center, Inc. (DHC) had its origins in 1965 as the first neighborhood health center established under the auspices of the Office of Economic Opportunity (OEO). It ultimately became the first rural federally qualified health center (FQHC).10 DHC provides primary medical and dental care services to individuals and families who reside in Bolivar, Sunflower, Washington, Issaquena, and Sharkey counties in the Mississippi Delta. Employing a community-oriented primary care (COPC) model, DHC develops and implements community development initiatives and projects, all coordinated through the clinic. DHC operates nine community health centers in Mound Bayou (the primary
___________________
9 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
10 For more information, see http://www.deltahealthcenter.org (accessed September 26, 2016).
site), Greenville (two sites), Indianola, Cleveland, Moorehead, Hollandale, Mayersville, and Rolling Fork.
Not long after the authorization of the Community Action program of the OEO in 1964, the staff began to explore whether it might be able to support some substantial changes in how health care for poor populations was organized. The challenge was to improve the health and well-being of low-income families—and, as public health official Alonzo Yerby put it at a 1965 White House conference, to assure that poor people would no longer be “forced to barter their dignity for their health” (Schorr, 1988).
Two developments moved these ideas from visions to real possibilities. First, the passage of Medicare and Medicaid legislation in 1965 meant that there would be a significant source of funding that could support newly designed service structures in disadvantaged communities. Second, a group of health care reformers, led by Jack Geiger11 of Harvard University and Count Gibson of Tufts University, came to OEO with thoughtful plans for new entities they called neighborhood health centers. These would be established where the needs were greatest, with the Mississippi Delta as a prime example: an area of concentrated poverty where the infant mortality rate was 70 deaths per 1,000 live births (Longlett et al., 2001), the median family income was $900 per year, and the median level of education was 5 years (Geiger, 2002).
The first OEO health center grant was made in 1966 to create DHC in Mound Bayou, with the goal of demonstrating that it was possible to provide high-quality health care and related services and supports to many who had never benefited from the U.S. health care system and to do so in ways that would be cost-effective. Geiger was then appointed as project director for DHC.12 The Mississippi Delta community continues to face barriers to health (see Table 5-3 for demographic data). DHC provides services to more than half of the population living below the federal poverty level in the Mississippi Delta. Mound Bayou, the town where DHC’s main campus is located, is the oldest predominantly African American community in the country. The level of black-white residential segregation in Bolivar County measures at 61 out of a total 10013 on the index of dissimilarity (County Health Rankings, 2016a).
___________________
11 For an oral history interview with Jack Geiger conducted by John Dittmer in 2013, see https://www.loc.gov/item/afc2010039_crhp0076 (accessed September 26, 2016).
12 For a short film (produced and directed by Judy Schader Rogers in 1970) that documents the origin of the Delta Health Center, see https://vimeo.com/6659667 (accessed October 17, 2016).
13 The residential segregation index ranges from 0 (complete integration) to 100 (complete segregation).
TABLE 5-3 Demographics of the Delta Health Center Catchment Population
| Total | ~9,629 residents |
| Race/ethnicity | 98% African American |
| 1.0% White | |
| <1.0% Latino or Hispanic | |
| Health | 27.8% uninsured |
| 35.6% Medicaid patients | |
| 48.7% patients with asthma | |
| 21.6% patients with diabetes | |
| Age | 27.7% under 18 years |
| 61.2% 18–64 years | |
| 11.1% 65 years and over | |
| Education | 73.5% high school graduate in Bolivar County |
| Income | 98.2% patients at or below federal poverty line |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: HRSA, 2015; U.S. Census Bureau, 2015a.
Community-Oriented Primary Care Model
COPC is a systematic approach to health care derived from principles in the disciplines of epidemiology, primary care, preventive medicine, and health promotion which was first pioneered by Sidney and Emily Kark in a South African rural community (Geiger, 2002; Longlett et al., 2001). Geiger asserts that although community development and social change are not explicit goals of the COPC model, they are implicit in the model’s emphasis on community organization and local participation with health professionals (Geiger, 2002). DHC employs this model using a multipronged approach that includes the development and implementation of community development projects that improve health, such as an agricultural cooperative, transportation company, and an integrated primary health care system. The integrated primary care system consists of multidisciplinary teams of physicians, nurses, and health educators. COPC also moves beyond the traditional integration of “community engagement” (e.g., a community advisory board). Rather than involving the community in COPC practice, it involves the practice in basic processes and structures within the community (IOM, 1983).
Solutions to Address the Social Determinants of Health
Although DHC is a health care service provider for the community, it targets more than just health care by using insights from the COPC model to act on multiple factors outside of the traditional health care setting that are pertinent to the community.
Health systems and services DHC provides comprehensive health care services at nine sites. Services include dental care; a diabetes clinic; family medical care; a laboratory; nutritional counseling from dieticians; pediatric care; a pharmacy; social services support from licensed social workers; women’s health care services; obstetrics, neonatal, and gynecological care; and X-ray services. DHC also offers a smoking cessation program and provides referrals to local mental health centers for its patients. To better meet patients’ needs, DHC offers a prescription assistance program for those without prescription coverage who meet income guidelines. Furthermore, the patients’ ability to pay is determined using a sliding-scale self-pay tool, based on the 2015 poverty guidelines published by the U.S. Department of Health and Human Services.
Start Strong is a DHC outreach program that targets maternity patients with the goal of reducing barriers and providing incentives for patients to see a provider during their first trimester. Through group counseling and providing access to healthy produce and other essential goods, the program has been able to engage maternity patients who were not initially obtaining usual care during their pregnancies.
Education In the 1970s, DHC established an office of education which sought out aspiring high school and college graduates, assisting them with college and professional school applications as well as connecting them with scholarship information and university contacts (Geiger, 2002). At night DHC also offered high school and college preparatory courses for students. Some of the students who benefited from these educational services returned to work for DHC in various positions—as a clinical director, a staff pediatrician, and executive director (Geiger, 2002). There are plans to reinstate some classes at DHC—specifically, General Education Development (GED) test courses for community residents. Today, DHC partners with the tri-county school system to invite youth ages 14–18 who have an interest in medical careers to shadow providers and assist with local health fairs.
Social environment DHC improves social capital by creating ties to community-based institutions to address the race- and class-based isolation of poor and minority communities (Geiger, 2002). Among these institutions were 10 local community health associations, each of which had a community center and associated programs.
Physical environment DHC developed an agricultural co-op, the North Bolivar County Farm Co-op, with the assistance of a foundation grant from the Federation of Southern Cooperatives in 1968 (see Figure 5-5).

SOURCE: Photo by Dan Bernstein. Used with permission.
This initiative brought together 1,000 families to harness their labor and operate a 600-acre vegetable farm, building on agricultural skills that were already present in the community. DHC still operates a farm on 6.8 acres of land, producing fruits and vegetables that are made available to its patient population. This work is done in collaboration with Delta Fresh Foods14 Initiative, which provides funding, and Alcorn State University, which assists with farming services. In an effort to encourage healthy eating, the DHC diabetes clinic initiated a program, Ticket to Pick It, in which patients who visit the clinic receive a ticket that allows them to access fresh produce on the farm at no cost.
Income and wealth In the 1960s the health council of DHC sought to end local discriminatory banking practices. DHC leveraged its funding by proposing that it would deposit the council’s funding and cash flow
___________________
14 For more information on Delta Fresh Foods, see http://deltafreshfoods.org (accessed September 28, 2016).
with the first local bank that opened a branch in a predominately African American neighborhood, hired community residents as tellers, and engaged in fair employment and mortgage loan practices (Geiger, 2002).
Transportation DHC provides transportation services to and from the clinic sites for all patients in partnership with the Bolivar County Community Action Agency. This service is intended to mitigate the effects of a lack of access to transit as a barrier to receiving health care services. Specifically, maternity patients with children at home but no child care would be unable to visit the center. DHC ensures that transportation for multiple passengers is provided to patients for this reason. In addition, DHC operates a car seat initiative for maternity patients, in which mothers are trained to safely install and use car seats and car seats are provided to each participating family at no cost. In 2016, DHC donated more than 200 car seats to maternity patients.
Data and Outcomes
As a Health Resources and Services Administration health center program grantee, DHC is required to report on the center’s performance using measures defined in the Uniform Data System (UDS) every year. UDS measures include patient characteristics (e.g., race/ethnicity, age, income status, insurance status, homelessness, and more), clinical data (e.g., rates of preventive screening services and chronic disease management), and cost data (e.g., grant expenditures and cost per patient). The adoption of electronic medical records and the availability of annual data facilitate data collection for trend analyses. For example, the rate of low-birthweight babies has decreased from 20.7 percent in 2013 to 3.8 percent in 2015 (HRSA, 2015). DHC staff attributes this in part to the increase in obstetrics and gynecology providers on-site over the past few years and also to the targeted programs for maternity patients.
Promoting Health Equity: Key Elements
DHC works across sectors and disciplines to serve the needs of the community in the Mississippi Delta. In 2015 the center partnered with educational institutions such as Emory University and Mississippi State University to engage student volunteers who worked on affordable housing and gardening projects (see Figure 5-6).
DHC illustrates the potential outcomes of capacity building in a community over a sustained period of time. For the past 40 years it has been owned and operated by the North Bolivar County Health and Civic

SOURCE: DHC, 2015. Used with permission.
Improvement Association, an organization that the center played a role in creating with the community (Geiger, 2016).
Challenges and Lessons Learned
One of the challenges that DHC currently faces in serving its community is the significant number of residents who fall in the health insurance coverage gap, which amounts to 108,000 people in the state overall (Garfield and Damico, 2016). Among these residents, 52 percent are people of color, 54 percent are women, and 58 percent are in a working family
(Garfield and Damico, 2016). Mississippi is one of the states that opted not to expand Medicaid coverage through the provision of the Patient Protection and Affordable Care Act (ACA), an expansion that estimates indicate could have provided insurance coverage for an additional 181,000 residents in Mississippi (Garfield and Damico, 2016).
Overcoming the historical mistrust of medical institutions among underserved communities and the fear of privacy violations among patients has been a challenge for DHC staff. By remaining visible and active in community activities (e.g., festivals, health fairs, career day in schools), in addition to being transparent about adhering to Health Insurance Portability and Accountability Act privacy rules, DHC has worked to build trust among community residents. DHC also adapts to the literacy needs of its patient population, a high proportion of which have low literacy levels. DHC trains patient navigators to tailor services to a patient’s level of literacy.
DHC, being a rural and community-based health center, has found it challenging to secure a network of providers. Many of the current programs and initiatives that DHC engages in are informed by provider interactions with patients, which instruct providers about the barriers patients face and contributing upstream factors that shape them (e.g., a lack of money for transportation, child care issues, and illiteracy). As a result, DHC also trains its providers to be advocates for their patients.
Geiger wrote in 2002 that there are two important lessons to be learned from DHC’s history:
- communities suffering from poverty are rich in potential and ingenuity; and
- health services have the capacity to address the root causes of poor health through community development and the social change that it produces (Geiger, 2002).
Sustaining Success
As an FQHC, DHC receives funding from the federal government and abides by the requirements in Section 330 of the Public Health Service Act. It initially received funding in 1965 and is governed and overseen by a board of directors. Other sources of funding for DHC include the Mississippi Department of Health, W.K. Kellogg Foundation ($825,000 during 2014–2017), and Delta Fresh Foods. Furthermore, as an FQHC, 51 percent of the DHC board of directors must be drawn from current patients in the program. The success of DHC led to the establishment of 200-plus health centers in the United States by 1973 and approximately 1,200 by 2010 (Longlett et al., 2001).
According to DHC, the center prides itself in being a “one-stop shop” for community residents in a rural community where convenience is rare. DHC builds off of the legacy of the center’s community-driven origins and has provided a centralized space where the community can access medical care, social services, insurance assistance, a pharmacy, and other important resources necessary to empower residents to lead healthy lives.
Dudley Street Neighborhood Initiative15

Background and History

The Dudley Street Neighborhood Initiative (DSNI) is a nonprofit, community-driven organization located in the Roxbury and North Dorchester neighborhoods of Boston, Massachusetts. Established in 1984, its mission is “to empower Dudley residents to organize, plan for, create, and control a vibrant, diverse, and high quality neighborhood in collaboration with community partners” (DSNI, 2016d). One of DSNI’s distinguishing strengths is its focus on channeling individual concerns into a collective voice to achieve shared goals and facilitate community empowerment. DSNI originated from and continues to be shaped by residents’ ability to leverage their collective power to influence and control the changes taking place in their community. In addition to its emphasis on community empowerment to carry out its mission, DSNI also focuses on sustainable economic development and youth opportunities and development. The organization’s commitment to these values is a key factor in its successful implementation over the past three decades of various initiatives aimed at improving the health and well-being of the community it serves.
As a community organizing and planning group, DSNI’s membership includes approximately 3,600 residents as well as community stakeholder
___________________
15 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
TABLE 5-4 Dudley Village Campus Demographics
| Total | ~27,500 Residents |
| Race/ethnicity | 57% African American |
| 28% Latino | |
| 20% Cape Verdean | |
| Gender | 53% female |
| Age | 26% of residents are under age 18 |
| 62% of households with at least one child age 0–17 | |
| Education | 81% completed high school |
| 11% of residents over age 25 have a bachelor’s degree | |
| Employment | 17% unemployed |
| Income | Median household income is $34,000 |
| 62% spend almost one-third of their monthly income on rent | |
| Language | 47% speak a language other than English at home |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: DSNI, 2016a; 2014–2015 American Community Survey.
groups, such as other nonprofits, religious institutions, educational institutions, and local businesses. Participation from low-income residents is encouraged through low-cost, sliding-scale membership dues. The structure of DSNI’s 35-member board of directors is designed to reflect the diversity of the community (see Table 5-4 for demographic information of the community DSNI serves, known as the Dudley Village Campus). Four board seats are reserved for African American residents, four for Cape Verdean residents, four for Latino residents, four for white residents, four for youth, seven seats for local health and human service nonprofits, two for community development corporations, two for small businesses, two for religious organizations, and two seats for residents appointed by the board (DSNI, 2016b).
DSNI’s founding was in response to residents’ concerns and frustrations over the deterioration of their community caused by arson fires and dumping (DSNI, 2016c). Broader socioeconomic issues such as disinvestment, poverty, and white flight had also negatively affected the neighborhoods of the community and led to further resident discontent. DSNI was founded with assistance from the Mabel Louise Riley Foundation, a foundation based in Boston that expressed interest in assisting the Dudley area after a site visit. In 1984 the Riley Foundation convened a group of community stakeholder groups, forming the Dudley Advisory Group. A neighborhood revitalization plan was proposed to residents but met with overwhelming dissatisfaction at the lack of resident representation on the governing board. By 1985 a revised plan was designed by a broadly

SOURCE: Personal communication with DSNI staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
representative group which established a resident majority on the board and firm community control of redevelopment.
In 1986 DSNI launched Don’t Dump on Us (see Figure 5-7 for a button from this community revitalization campaign), its first neighborhood revitalization campaign, which cleaned vacant lots and shut down illegal trash transfer stations. During this time, a comprehensive neighborhood revitalization plan was also developed and officially adopted by the city of Boston in 1987.
Community Land Trust Model
One of DSNI’s most notable accomplishments was its establishment of an urban community land trust (CLT).16 CLTs have existed for more than 45 years in the United States, with more than 270 in various cities across the country (Cho et al., 2016), but the establishment of DSNI’s CLT in 1988 was particularly noteworthy as it was the first time a community group sought out and won the power of eminent domain to acquire vacant land for resident-led development. Furthermore, it remains the second-largest CLT in the country. In the year of its founding, the organization purchased vacant lots in Boston to rebuild the land into affordable housing, urban agricultural and gardening sites, a town commons, parks and
___________________
16 The National Community Land Trust Network describes community land trusts with the following description: “CLTs develop rural and urban agriculture projects, commercial spaces to serve local communities, affordable rental and cooperative housing projects, and conserve land or urban green spaces. However, the heart of their work is the creation of homes that remain permanently affordable, providing successful homeownership opportunities for generations of lower income families” (National Community Land Trust Network, 2016).
playgrounds, a charter school, community facilities, and spaces for new businesses. DSNI’s CLT, known as Dudley Neighbors, Inc., owns more than 30 acres of land, providing 226 units of permanently affordable housing to low-income residents (Cho et al., 2016). An analysis of the CLT’s stabilizing effects on neighborhoods shows lower vacancy and foreclosure rates and higher owner-occupancy rates (Dwyer, 2015). Dudley Neighbors also provides affordable land to urban farmers. Many urban agricultural and gardening activities have emerged from the establishment of the land trust, including several farms (some commercial and others operated by The Food Project, a local nonprofit), many community gardens, and a 10,000-square-foot greenhouse (Loh and Shear, 2015).
Boston Promise Initiative
The U.S. Department of Education awarded DSNI a Promise Neighborhood planning grant of $500,000 in 2010 and a $5,000,000 implementation grant in 2012, from which DSNI launched the Boston Promise Initiative. The initiative is intended to support families, schools, and neighborhoods in ensuring that every child in the community has “cradle to career” opportunities to succeed through access to quality education, social support systems, and safe environments. The Boston Promise Initiative has developed and implemented several initiatives that aim to achieve these outcomes, many of which emphasize teen involvement in youth education. The initiative also aims to build organizational capacity by leveraging information gained from social network analysis.
Solutions to Address the Social Determinants of Health
DSNI has developed and implemented a range of community initiatives to address the social determinants of health. Many of these initiatives are operated through partnerships with a range of other community stakeholder organizations. Several initiatives focus their efforts on specific, more vulnerable populations within the community.
Housing Dudley Neighbors, Inc., promotes the CLT model to provide affordable housing and encourage community control of land development (DSNI, 2016e; Dudley Neighbors, 2016). In partnership with the Dorchester Bay Economic Development Corporation and Nuestra Comunidad Development Corporation, Dudley Neighbors ensures affordable housing for low-income residents by selling homes built by these local development corporations to qualifying residents at affordable prices (Cho et al., 2016). This model provides a sustainable alternative to allowing the housing market to inflate prices and create unjust financial barriers
for low-income residents seeking to become homeowners (Cho et al., 2016). DSNI also participates in the Greater Boston Community Land Trust Network in cooperation with other local organizations to further promote the development of affordable housing and open spaces through the community land trust model (DSNI, 2016e).
In addition to reducing barriers to affordable housing, another goal of DSNI is to reduce homelessness and provide services to support individuals and families at risk of becoming homeless. In partnership with Project Hope, a nonprofit based in Boston providing supportive housing services, DSNI established the No Child Goes Homeless initiative to support children and their families facing homelessness or possible eviction by providing services and other resources made available through a network of schools, city agencies, and other service providers (Boston Promise Initiative, 2016; DSNI, 2016e). In 2016, DSNI and Project Hope participated in a city-level conversation hosted by the Boston Department of Neighborhood Development, which also included the mayor’s chief of education, the Boston Housing Authority, and leaders from Boston Public Schools. At this meeting, the No Child Goes Homeless initiative was highlighted as a promising practice. Project Hope and DSNI were asked to shape and potentially lead a pilot to demonstrate the effectiveness of cross-sector collaboration for replication across the city.
Education In conjunction with community empowerment and sustainable economic development, DSNI prioritizes youth leadership development and has launched a range of initiatives that provide opportunities and enable access to quality education for youth of all ages. Achieve Connect Thrive (ACT) is an evidence-based framework developed by DSNI to improve academic performance and facilitate successful career opportunities. The Learning Our Value in Education campaign holds educational events that are open to all community members to attend, and DSNI also supports a youth committee and an education committee to further facilitate educational opportunities for residents and community leaders. The Boston Promise Initiative also supports an early childhood education initiative called Dudley Children Thrive, which fosters a network of teachers and parents of children ages 5 and under. The initiative is intended to promote early childhood literacy and school readiness by encouraging parents to read to their children (Sandel et al., 2016). The School Readiness Roundtable brings early childhood educators and policy makers face-to-face with parents from the neighborhood, where they openly discuss strategies that work and those that do not to support young children.
DSNI’s early learning work illustrates how neighborhood-level interventions can improve childhood opportunity and lift children out of
poverty (Sandel et al., 2016). In 2015, 50 percent of families participating in the initiative had increased the number of times they read to their children, and 80 percent read to their children three or more times per week (DSNI, 2016c). DSNI also implements many other educational efforts to support youth and their families from early childhood through higher education, including parent advocacy and leadership programs, the Highland Street AmeriCorps mentoring program, a youth council, a college readiness program, and a young alumni network.
Employment DSNI works to increase employment opportunities for residents of racial and ethnic minority backgrounds, women, and women of racial and ethnic minority backgrounds through the Dudley Workforce Collaborative, which supports business developers to increase the number of construction work hours offered to residents in these marginalized groups. For construction related to the Boston Promise Initiative, the collaborative was successful in ensuring that 51 and 15 percent of the construction workforce consisted of racial and ethnic minorities and women, respectively (DSNI, 2016e). In 2013, DSNI helped secure 44 percent of total subcontract value on Choice Neighborhoods construction projects for minority-owned enterprises, totaling $16,438,519, with an additional 10 percent of subcontract value for women-owned enterprises, totaling $3,656,263 (DSNI, 2016c).
Physical environment DSNI supports food security by partnering with two other Boston-based nonprofits—the Food Project and Alternatives for Community & Environment—to increase residents’ access to healthy and locally grown food options through the Dudley Real Food Hub and to provide loans for new and existing local food businesses. The collaborative effort also provides opportunities for residents, particularly youth, to participate in community gardening and educational activities to increase awareness and encourage consumption of healthy and locally sourced food options. As part of the Dudley Real Food Hub, Commonwealth Kitchen, an equipment-sharing incubator, has supported more than 50 community-based food businesses. Additionally, with DSNI’s endorsement, a neighborhood grocery store, FT & Davey’s Supermarket, successfully raised $5,000 from the community to purchase an industrial freezer, a key component in the local fresh produce distribution chain.
Public safety DSNI works to address public safety issues. In 2012, a series of shootings prompted the organization to convene a diverse group of community stakeholders, including local officers from the Boston Police Department, to support neighborhood watch groups. After the widely publicized closing of a state drug lab in 2012, following a scandal in which
it was revealed that more than 24,000 drug cases from 2003 to 2012 were compromised, DSNI’s advocacy efforts, in coordination with other community stakeholders, helped secure $5 million from the state to support community-based reentry services.
Social environment Another of DSNI’s goals is to improve the community’s cultural and artistic economy. The organization leads the Fairmont Cultural Corridor, an initiative begun in 2012 through which local artists, businesses, and arts and cultural organizations collaborate to implement activities such as art installations, public place-making, and outdoor markets (Fairmont Cultural Corridor, 2016). The arts create thriving public spaces for the neighborhood, and DSNI also engages residents in participatory action research to co-create knowledge about the neighborhood. Residents have been recruited and paid as researchers in neighborhood surveys for the Boston Promise Initiative and for studies commissioned by the Healthy Neighborhoods Equity Fund, a participatory action research initiative investigating the effects of real estate development on residents’ health.
The arts and data merge in the form of interactive data visualizations at neighborhood events. In 2015, DSNI conducted a focus group with young people about their perceptions of future success. The transcript from the focus group was turned into a word cloud, and the words from the word cloud were burned onto wood blocks left over from an art installation. The blocks were then given to children to create their own found poems (see Figure 5-8). The activity provides a strong example of how the arts and data can work together to inform and inspire community residents.
Data and Outcomes
DSNI’s initiatives aspire to achieve the following community change outcomes:
- strong and healthy families
- vibrant and thriving communities
- children entering school ready to succeed
- successful students and schools
- postsecondary completion and career readiness
DSNI has made progress in achieving these outcomes through its many initiatives. The Dudley Real Food Hub has facilitated a community-driven planning process to identify key strategies for helping families improve their food environment, and families have also strengthened

SOURCE: Personal communication with DSNI staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
their financial literacy through enrollment in Fair Chance for Family Success. Cultural initiatives such as the Fairmont Cultural Corridor have contributed to more vibrant and thriving communities. Dudley Neighbors, Inc., has contributed to the creation of a Chinatown community land trust and, as a certified state community development corporation, secured $100,000 in community tax investment credits. To help children achieve greater school readiness, residents and community stakeholders have convened working groups to assist families with children ages 0 to 5. To increase opportunity for students to succeed in school, mentoring programs have matched 18 students with mentors of color who are primarily from the neighborhood. The No Child Goes Homeless program has also provided support services to students and their families at risk of eviction. Greater career readiness has also been accomplished, with 48 young people hired and efforts under way to engage youth 18 to 24 years old to develop educational and career pathways.
DSNI’s peer-to-peer financial literacy and learning program, Fair Chance for Family Success, has enrolled 100 families and achieved significant outcomes since the initiative began in 2014. Table 5-5 displays some of Fair Chance’s key outcomes and results.
As a Promise Neighborhood grantee, DSNI reports data collected for 15 Government Performance Results Act (GPRA) indicators, which are measures that quantify achievement of outcomes related to health care services, education, exercise, nutrition, exercise, and others. Table 5-6 provides some of the key results DSNI has measured from 2014 to 2015.
TABLE 5-5 Results of DSNI’s Fair Chance for Family Success Program (2014–2016)
| Outcome | Result (n = 74) |
|---|---|
| Average amount in savings accounts | Increased from $3.43 to $1,555.26 |
| Average amount in checking accounts | Increased from $200.51 to $775.83 |
| Average amount in total assets | Increased from $452.42 to $5,899.46 |
| Average subsidy income | Reduced from $128.25 to $47.56 |
SOURCE: Personal communication from Andrew Seeder to National Academies staff on September 21, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
TABLE 5-6 Results Related to GRPA Indicators
| Outcome | 2014 | 2015 |
|---|---|---|
| Percent of kindergarteners who demonstrate at the beginning of the school year age-appropriate functioning across multiple domains of early learning (n = 116) | 59% | 65% |
| Percent of high school students at or above grade level according to state mathematics assessments (n = 64) | 36% | 63% |
| Four-year adjusted cohort graduation rate (n = 72) | 51% | 82% |
| Percent of students who enroll in a 2-year or 4-year college or university after graduation (n = 86) | 48% | 69% |
| Percent of children who participate in at least 60 minutes of vigorous physical activity daily (n = 142) | 16% | 22% |
| Percent of children who consume five or more servings of fruits and vegetables daily (n = 195) | 27% | 30% |
| Student mobility rate (n = 1,871 [total enrollment of schools]) | 61% | 46% |
SOURCE: Personal communication from Andrew Seeder to National Academies staff on September 21, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
Promoting Health Equity: Key Elements
Since its early days up to the present, one of DSNI’s main goals has been to empower the Dudley community by “changing residents’ perceptions of their neighborhood and of their own power to change the conditions in which they live” (Schorr, 1997). In carrying out this goal, the organization has cultivated a shared vision among residents, families, local organizations, and local businesses to achieve a healthier and more vibrant community. DSNI has fostered increased community engagement and a greater sense of community within neighborhoods previously ravaged by unjust disinvestment and policies that led to poor health outcomes. The organization’s many ongoing efforts emphasize access to basic needs such as housing and education as well as emphasizing economic opportunity and healthy behavior in driving a unified vision of health equity.
As evidenced by its diverse and growing membership of individuals and stakeholder groups, DSNI recognizes the need to foster multi-sector collaboration to achieve a more vibrant community of healthier residents. Its encouragement of and engagement in collaboration with various entities spanning many different sectors is one of its core strengths. Through efforts relating to its community land trust, the organization engages with development organizations and other nonprofits to improve housing and land use management. Through initiatives such as the Boston Promise Initiative, Dudley Real Food Hub, Dudley Workforce Collaborative, and Fairmont Cultural Corridor, the organization engages with businesses, local arts and cultural institutions, and other nonprofits to improve economic, agricultural, and cultural development. Partnerships with educational institutions are also well established through DSNI’s range of youth education programs.
DSNI builds social capital and community leadership among residents to create a thriving community. The Boston Promise Initiative’s Fair Chance for Family Success, a peer-to-peer financial learning support network funded by the Family Independence Initiative, has achieved significant quantifiable outcomes. Over the course of 2 years, from 2014 to 2016, families in Fair Chance saw average savings increase from $3.43 to $1,553.36, while average checking account balances increased from $200.51 to $775.83. On average, total assets increased from $452.42 to $5,899.46. The Fair Chance program is a model for how peer-to-peer social networks can drive social change.
DSNI’s commitment to youth development has also built strong capacity among its younger residents to sustain and build on the work begun by the previous generation and create greater opportunities for future generations. Many of DSNI’s educational initiatives specifically support the needs of children of low-income, impoverished, and homeless
families, providing needed services and social support as well as pathways to educational and career success. These initiatives not only contribute to reducing health disparities but also facilitate the development of youth in the community into the next generation of community leaders who give back to the community that has supported them and their success. Building youth capacity has thus contributed to a cycle of residents helping residents, which has helped sustain DSNI’s success over the past three decades since its founding.
DSNI is a values-first organization; it is a data-informed organization driven by values. In working with youth, for example, DSNI recognizes the power of the neighborhood’s young people who want to be engaged and play a leadership role in the community. When youth are offered a supportive and challenging leadership environment that values their engagement, perspective, and growth, they are empowered to invest in their own and their community’s development. This means that young people are at the table and actively providing their voices during decision-making processes. Additionally, DSNI organizes to ensure that anchor institutions make upstream investments in the social determinants of health in alignment with the ACA’s changes to how hospitals and other health providers make investments in community health. DSNI and its partners are moving forward with a major campaign to reassert community voice in the determination of needs, community benefits agreements, and payments in lieu of taxes.
Challenges and Lessons Learned
One of DSNI’s most significant challenges is convincing residents to prioritize long-term gains over short-term benefits. Many low-income residents prioritize day-to-day needs and emergency conditions, such as the risk of eviction, paying bills, and feeding and getting their kids to school. To help these families achieve healthier outcomes, DSNI is interested in strategies to mitigate the effects of these barriers and to shift residents’ thinking from short to long term.
A critical component of DSNI’s success has been its innovative and inclusive approach to governance through its board of directors. The board is guided by a vision of collective leadership, and its membership is representative of the community both through racial/ethnic composition and youth involvement. Additionally, the board’s joint decision making with the City of Boston for development of community-owned land has led to the building of housing, open and green neighborhood spaces, and local businesses that meet the needs of community residents.
Sustaining Success
Youth development is a core component of DSNI’s work which has helped to sustain its success. Investing in youth has helped to achieve long-term community change and yielded substantial long-term benefits, as some youth who participate in DSNI’s work expand their participation, developing into leaders as full-time staff members (Bhatt and Dubb, 2015). DSNI also provides opportunities for residents to develop leadership skills through activities such as its Sustainable Economic Development Committee, through which residents gain valuable training and real-world experience in community organizing, planning, and development.
Through organizing, residents get the chance to take leadership responsibility and apply some of what they’ve learned to the real world. Facilitating a meeting with a developer and hammering out a community benefits agreement is something you can take a workshop on, but it’s different in the real world.
—Harry Smith, Director of Sustainable Economic Development,
Dudley Street Neighborhood Initiative
Eastside Promise Neighborhood17

Background and History

The Eastside Promise Neighborhood (EPN) was founded as an implementation site of the U.S. Department of Education (ED) Promise Neighborhood grant program, which provides funding to nonprofit organizations, educational institutions, and Indian tribes to support the revitalization of disadvantaged communities through investment in youth education and development (ED, 2016). The Promise Neighborhood goals are based on the 10 promises listed in Table 5-7.
___________________
17 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
TABLE 5-7 Eastside Promise Neighborhood 10 Promises
| Educational Success | Family and Community Support |
|---|---|
|
|
SOURCE: EPN, 2016a.
EPN emerged from a 2010 planning grant awarded to the United Way of San Antonio and Bexar County to continue the process of revitalizing the Eastside neighborhood of San Antonio, Texas, by identifying the factors that affect academic success and to design a plan to create a collection of solutions to improve educational outcomes in schools throughout the area. Using the $312,000 1-year planning grant to inform and develop a Promise Neighborhood proposal, a community stakeholder group of residents and local experts conducted a variety of information-gathering activities, including a needs assessment, focus groups, and forums for community discussion. The needs assessment identified problems in the local school system, including inadequate access to quality early education programs, low-performing schools, low graduation rates, poor student health outcomes, and insufficient or ineffective social support services. A proposal to address these community needs was developed and submitted, and in 2011, a 5-year $23.7 million (EPN, 2016b) implementation grant was awarded to launch EPN as a joint initiative of the United Way of San Antonio and Bexar County, the San Antonio Independent School District, the San Antonio Housing Authority, Family Services Association, the City of San Antonio, the P–16+ Council, Community Information Now, and SA2020.18 The area is also home to a U.S. Department of Housing and Urban Development Choice Initiative, a U.S. Department of Labor Promise Zone Designation, and two Byrne Criminal Justice initiatives. The term “EastPoint” is used to describe the area of collective impact for all of the activity occurring as a result of this significant federal investment.
___________________
18 SA2020 is “a community vision and movement born from a series of public forums in 2010 to develop goals for improving San Antonio by the year 2020.” For more information, see http://www.sanantonio.gov/sustainability/SA2020.aspx (accessed December 5, 2016).
EPN’s mission is to “[unite] institutional and resident stakeholders to leverage and strengthen the neighborhood’s assets and resources so that children and families are inspired to stay, grow, graduate, and stay” (EPN, 2016c). Its 5-year goal was “to break down traditional government and non-profit silos” to develop and implement more collaborative solutions to address the complex barriers faced by students in disinvested neighborhoods (EPN, 2016b).
In the 1950s the Eastside neighborhood was a predominately African American community afflicted with segregation in housing, schools, and businesses. In addition to a 2.58 percent decrease in the population since 2000 (compared to a 16 percent overall increase in San Antonio), the race and ethnicity distribution of EPN’s population has also changed over the past two decades. See Table 5-8 for a summary of EastPoint demographics. Although the community has a rich cultural history and includes more than 50 churches, 6 EPN-designated schools, almost 300 businesses, and an array of social service organizations, its residents face significant socioeconomic disadvantages that negatively affect their attainment of good health. The American Community Survey found that from 2005 to 2009 the neighborhood’s annual median household income was $19,766, as compared with $43,087 for all of San Antonio (Drennon, 2011; PolicyLink, 2014). In the same time period, about 60.1 percent of children were living in poverty, almost three times the national child poverty rate of 21.9 percent (Drennon, 2011; PolicyLink, 2014). Many families in the community are younger than the average in San Antonio and experience higher rates of poverty (Drennon, 2011; PolicyLink, 2014). Educational outcomes are also worse than in San Antonio, as access to and quality of early childhood education, schools, and social support services are low (Drennon, 2011; PolicyLink, 2014).
TABLE 5-8 EastPoint Demographics
| Total | ~18,000 residents (2010) |
| Race/Ethnicity | ~68% Hispanic |
| ~25% African American | |
| ~7% white | |
| Income | Annual median household income from 2005 to 2009: $19,766 |
| 60.1% of children living in poverty |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: Drennon, 2011; PolicyLink, 2014.
Solutions to Address the Social Determinants of Health
EPN focuses on improving educational outcomes through many programs that provide educational and growth opportunities for children and youth from early childhood through postsecondary education and career support.
Education EPN is committed to providing a sustainable pathway for youth to achieve educational success and be ready for college or the workforce. Its goal of establishing family and community stability reflects its recognition that environmental barriers must be addressed in order for children to achieve educational and employment success. EPN’s vision is for students to graduate from high school ready for college, careers, and self-sufficiency with the support of a revitalized and thriving community. Its cradle-to-career pathway consists of the promises that the community strives to make to its youth in supporting their education and development. Figure 5-9 illustrates the types of community resources that are available to achieve each goal along the pathway.19 Healthy and financially stable families who have access to social support and services are the foundation of the pathway. School readiness, access to quality education (including early childhood; science, technology, engineering, and mathematics [STEM]; post-secondary; and trade certification opportunities), meaningful engagement from parents and caregivers, and a safe environment are also emphasized as essential components of EPN’s pathway to achieving academic success.
EPN partners with the San Antonio Independent School District (SAISD) to create a continuous, integrated pipeline to success for students attending the schools in the EPN, which include the Tynan Early Childhood Education center; three elementary schools (Bowden, Washington, and Pershing Elementary Schools); Wheatley Middle School, which serves as the District’s site for a ED-funded Community School; and Sam Houston High School. SAISD redesigned its education plan to emphasize successful and sustainable STEM education for students. Other priorities in the redesigned plan include meeting state standards in all core subjects and strengthening teacher capacity through increased training. EPN’s talent development strategy, led by Trinity University, has also been integrated into the district’s new 5-year Blueprint for Excellence plan.
EPN provides funding and support for a number of programs that improve early childhood education and school readiness, including a number of Texas Rising Star–accredited early childhood centers and
___________________
19 A video describing EPN’s 10 promises is available at http://eastsidepromise.org/the-results (accessed December 5, 2016).
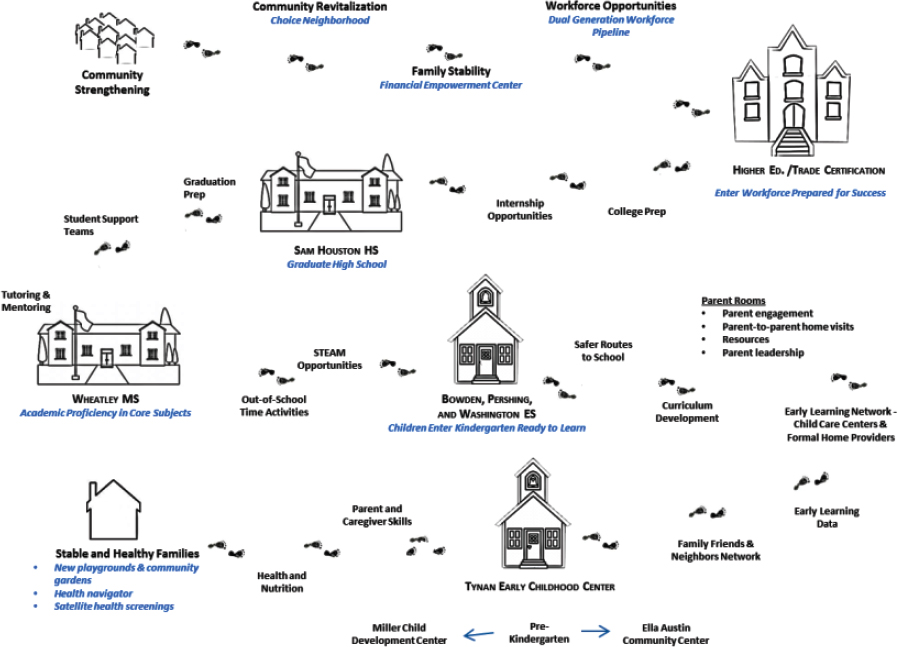
SOURCE: EPN, 2013. Used with permission.
summer camps; an online resource known as Ready Rosie to support kindergarten readiness; a Family, Friends, and Neighbors Network operated by the Family Service Association; a free Home Instruction for Parents of Preschool Youngsters program, managed by Catholic Charities, which encourages early reading; expert early childhood consultants to support quality improvements at the centers; and, thanks to a Chase Foundation grant, expanded opportunities for center staff to pursue a child development associate (CDA) certificate and associate of arts (AA) credentials. For the early childhood programs, 73 percent of licensed slots at the three child care centers in the area are currently utilized (244 out of 335). The target of 25 participants for the Family, Friends, and Neighbors Network has been exceeded, with 33 enrolled, and the available slots for CDA and AA participation were utilized at 100 percent.
EPN also implements a number of programs in collaboration with partners to promote educational success through secondary and postsecondary education. City Year, a nonprofit that partners with at-risk schools in impoverished communities to provide support to vulnerable students and teachers, partners with EPN to pair trained young adults (corps members) with students identified as most at risk from Wheatley Middle School and Sam Houston High School. Corps members support these vulnerable students to overcome attendance problems and achieve academic success.20 EPN and its partners also provide students with resources to learn more about and enroll in colleges and universities. SAISD also receives funding from the ED’s Gaining Early Awareness and Readiness for Undergraduate Programs to provide college readiness coaches, summer camps and programs, and other resources to prospective college applicants.
EPN-supported internship programs to develop leadership capacity and to provide career opportunities for talented youth were augmented by a Citibank grant to support a college match savings program for neighborhood students. Partnerships with several nonprofits (including the Boys and Girls Clubs of San Antonio, the Girl Scouts of Southwest Texas, HIS Bridgebuilders, and the YMCA of Greater San Antonio) provide afterschool and summer programs that emphasize STEM education. Figure 5-10 summarizes EPN’s cradle-to-career pipeline.
Meaningful parent and caregiver engagement is an essential aspect of EPN’s educational programming. In partnership with the Family Service Association’s Family–School–Community Partnership, United Way, SAISD, and City Year, EPN facilitates a range of services such as parent-led home visits, parent training, and school-based family activities
___________________
20 For more information on City Year and its partnership with EPN, see http://eastsidepromise.org/city-year (accessed December 5, 2016).
SOURCE: EPN, n.d. Used with permission.
to deepen parent and caregiver involvement and empower families to resolve problems such as chronic absenteeism.
Physical environment In addition to educational success, EPN also works to improve the health of its community through investment in other social determinants of health. In addition to partnerships that have created children’s playgrounds, community gardens, and farmer’s markets, access to healthy food is also addressed through a partnership with the San Antonio Food Bank to provide families with fresh produce. Public safety for youth has also been addressed. The Byrne grant enabled EPN to contract with the San Antonio Police Department to provide additional patrols in the mornings and afternoons to ensure that the pathways to school were safe. In addition, a new initiative launched at one of EPN’s elementary schools for the 2015 to 2016 school year is the Walking School Bus program, which involves adult supervision of children walking to and from school. The program addresses student safety concerns due to factors such as crime and unsafe construction as well as reducing tardiness, improving attendance, and improving students’ health and well-being.
Data and Outcomes
United Way and its partners committed early in EPN’s development to using data and community input to drive the initiative’s decision-making process. During EPN’s planning grant process, a review of longitudinal academic performance data revealed that only 31 percent of neighborhood children entered kindergarten with readiness skills. As a result, many of EPN’s solutions related to early education were launched at the very beginning of the initiative. For programming developed during the implementation phase of the grant, EPN subcommittees participated in strategic planning sessions that resulted in identifying solutions which were ultimately sent to the advisory council for approval. The programs outlined above were either identified during the planning phase or developed during the implementation phase. Community input was prevalent throughout, either as a part of the numerous meetings held during the planning phase or as a part of work done at the subcommittee or advisory council level.
EPN’s subcommittees spend time reviewing data associated with the funded programs, including usage rates and performance metrics. As part of its review, if a program is started that does not resonate with the community, the subcommittee evaluates the process for improvement before the next round of funding. For example, after the initial funding was provided for farmers markets, data revealed that a large number of customers were not from the footprint (the area being served). The committee changed the location of the markets to the community school and also provided funding for nutrition education and cooking classes to ensure that families understood the importance of utilizing fresh fruits and vegetables in their daily diets. Additionally, EPN and United Way staff review contracts on a bimonthly basis, including performance metrics, financials, and narrative reports submitted by funded agencies. This contract review process provides an opportunity for staff members to provide ongoing technical assistance for providers and consistent dialogue for program improvement. When EPN discovered that the out-of-school-time partners were not having the desired impact on academic achievement, a community of practice was created to give the partners the opportunity to collectively review the data and cross-pollinate best practices.
EPN’s theory of change is guided by 21 neighborhood goals which include targets set by community members and stakeholders. The goals are developed based on the ED’s Government Performance Results Act indicators, which are standard measurements for all Promise Neighborhood grant recipients. The target-setting process was conducted using the results-based accountability (RBA) framework and included 13 meetings with more than 200 residents, content experts, and partners and 10 small
group meetings with over 50 individuals from specific workgroups (e.g., the Dual Generation Workforce Pipeline workgroup) or specific partnerships (e.g., Out of School Time providers, City Year, all SAISD campus principals and their teams). The RBA framework structures participation and dialogue by focusing on the end game and affords the opportunity for the necessary negotiations and debates which must be part of a community-owned agenda. Table 5-9 displays EPN’s 10 promises as well as some of the key outcomes that the initiative has achieved in these areas.21 Data to measure this progress have been collected on an annual basis through a neighborhood survey, a literacy assessment, an early development assessment, a census of child care enrollment, a collection of administrative data and annual graduation rates, and a school climate survey.
Promoting Health Equity: Key Elements
Through the role of committees in its governance process, EPN fosters a shared community vision for better educational and health outcomes. EPN supports four community committees comprised of residents, community stakeholders, content experts, and local partners who meet regularly to address issues related to early childhood learning, health and wellness, education, and school and neighborhood safety. The Promise and Choice Together (PaCT) Health and Wellness Committee, for example, has reviewed data collected from 6th- to 12th-grade students on fruit and vegetable consumption and participation in physical activity to develop several of its solutions. Furthermore, a health consultant funded by EPN has served on the committee and facilitated the committee’s inclusion of Healthy People 2020 metrics related to health and wellness in order to develop interventions. EPN’s committees have fostered shared accountability among resident participants and strengthened educational success and health equity as a shared vision.
EPN collaborates with organizations from many different sectors. Its key partners include the United Way of San Antonio and Bexar County, The Annie E. Casey Foundation, SAISD, the City of San Antonio, Ella Austin Community Center, Goodwill Industries, Alamo Colleges, St. Philip’s College, San Antonio Growth on the Eastside, San Antonio Housing Authority, Workforce Solutions Alamo, Family Services Association, and the San Antonio Police Department. These core partnerships were formed during the planning phase of the process or the early implementation
___________________
21 For more information on initiatives related to each of the 10 promises as well as outcomes data and targets for past years, see http://eastsidepromise.org/the-results (accessed December 5, 2016).
TABLE 5-9 EPN’s 10 Promises and Key Outcome Measures
| Promise 1 | Children enter kindergarten ready to succeed in school. |
|
| Promise 2 | Students improve academic performance and are proficient in core subjects. |
|
| Promise 3 | Students successfully transition from elementary to middle to high school. |
|
| Promise 4 | Students graduate from high school. |
|
| Promise 5 | Students earn a college degree or a job training certification. |
|
| Promise 6 | Students are healthy, and their educational performance improves by accessing aligned learning and enrichment activities. |
|
| Promise 7 | Students feel safe at school and in their community. |
|
| Promise 8 | Students live in stable communities. |
| Promise 9 | Families and community members support learning in Promise Neighborhood schools. |
|
| Promise 10 | Students have access to 21st-century learning tools. |
|
a The Wheatley Courts demolition and the relocation of families outside the footprint in early 2014 may have had an impact on the mobility of students at the target schools.
b Compared to the baseline year, Bowden and Wheatley have shown improvement, Sam Houston stayed virtually unchanged, and Pershing and Washington experienced increased mobility. Compared to the 2015 to 2016 target of 20 percent, only Bowden Elementary is close to meeting the target with a 23.6 percent mobility rate.
SOURCE: EPN, 2016a.
phase and are maintained through regularly scheduled meetings at the subcommittee, staff, and leadership levels. The mutual accountability structure for EastPoint has three levels of partnership and accountability. The structure includes periodic reports to the mayor and city council of San Antonio delivered by the anchor partners. These reports include an overview of the progress of each of the major initiatives occurring as a part of the EastPoint collective impact model.
Some of the other organizations that EPN has partnered with are public libraries, faith-based organizations, sororities and fraternities, the National Association for the Advancement of Colored People (NAACP), and the San Antonio Spurs. Its key partners in carrying out its health and wellness initiatives include the Martinez Street Women’s Center, the San Antonio Food Bank, Methodist Health Care Ministries, the City of San Antonio, University Health Systems, CommuniCare, SAISD, University of the Incarnate Word Bowden Eye Care and Health Center, the San Antonio Metropolitan Health District, HIS Bridgebuilders, and the University of Texas Health Science Center.22 Additionally, EPN engages with local politicians in its governance process. Representatives from the mayor’s and city councilmen’s offices have designated seats on EPN’s advisory council. Staff members from the offices of local elected officials are also invited to serve as members of EPN subcommittees.
___________________
22 For a full list of organizations who partner with EPN, see http://eastsidepromise.org/the-partners (accessed December 5, 2016).
EPN has built resident capacity through its process of holding subcommittee and advisory council meetings that include representation from neighborhood associations. These neighborhood associations are composed of residents and property owners who hold regular community meetings to discuss and advocate for causes raised by their membership. Each has its own governing rules with elected leadership and may collect voluntary dues. Currently, three exist in EPN: Dignowity Hills, Government Hill Alliance, and Harvard Place/East Lawn.
EPN has developed organizational capacity by taking advantage of a DOE investment in training in results-based accountability. RBA is “a management tool that can facilitate collaboration among human service agencies, as a method of decentralizing services, and as an innovative regulatory process” (Schilder, 1997). Several of EPN’s staff members and community partners received RBA training in the initiative’s early implementation phases. RBA continues to inform the work of EPN and its partners in ongoing development and implementation of its programs.
Challenges and Lessons Learned
An important element contributing to EPN’s success has been its development and use of a process or framework to guide its governance process. EPN’s subcommittees have used RBA to develop and implement a range of health and educational programming. Another important aspect of EPN’s programmatic development has been the use of data to guide decision making, monitor progress over time, and make corrections and adjustments as necessary. EPN partners with a community data intermediary called CI:Now (Community Information Now), which has, over time, built a data warehouse and multiuser bridge underwritten by three funding sources and which enables the review of relevant student and family indicators to monitor progress across a range of programs (EPN, 2016b).
One of EPN’s ongoing challenges is ensuring that informal and formal communication systems successfully facilitate knowledge of the variety of resources available to community residents, as many families face transportation and access barriers and may not be aware of the resources and events available to them. EPN includes three neighborhoods, each with its own distinct characteristics and communication challenges. Developing a multipronged approach to reach residents across the footprint is an area for continuous improvement. The preferred method of communication continues to be “word of mouth,” as it generally comes from a vetted source that has a connection to the community. The Family–School–Community Partnership, which places Parent Rooms at each campus,
and the school district’s Parent Family Liaisons are the main distribution points, as they are highly connected to families in the footprint. EPN also created the position of family navigator to help connect families to available programs and events in the area. Finally, the Health and Wellness Committee recommended a solution that included hiring community connectors who visit homes to conduct an information and referral assessment to assist those with children ages 0 to 5 with accessing a medical home. These promotora-style peer home visitors also provide information about upcoming events and resources, including job fairs and career training opportunities in the neighborhood.
Over time, the implementation team has experienced some challenges that affected its problem-solving role and effectiveness. In recognition of this changing dynamic, plans are under way to ensure that the leadership of the implementation team is fortified to serve in its intended role and prepare for the transition to post-grant sustainability. The tri-chairs of the implementation team have agreed to participate in a self-assessment of the team’s current structure to provide insight to help identify and determine areas that may need adjustments for continued success in implementing collective initiatives.
Sustaining Success
EPN displays a deep commitment of accountability to the neighborhood. Entering the final stage of the EPN grant, sustainability is a key discussion. Stakeholders—including residents, volunteers, and organizations indigenous to the footprint—have begun sustainability efforts with a focus on creating a long-term strategy that identifies successful solutions to increase service value and build capacity for the most promising practices to be financially sustained. A series of meetings will be held in 2016, including community information-sharing sessions; visits to local neighborhood association meetings coined as “EPN Road Shows”; and community subject matter convenings to identify sustainable solutions, partner agencies who are interested in carrying the work forward, and potential areas for capacity-building for those partner agencies and gaps in service if no partner can be identified. The information captured will be used to design an EPN-recommended long-term sustainability strategy that will be submitted to the advisory council for approval and shared with the coordinating council. This will serve as a recommendation from the EPN community regarding the community’s voice for what its members feel is needed to stay on the course to success—a true reflection of the community-driven approach that initially launched EPN’s work. The EPN plan should also serve as a template for the future sustainability work

SOURCE: Personal communication with EPN staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
of the coordinating council for EastPoint, the Eastside, and greater San Antonio. Figure 5-11 displays the key actors who drive EPN’s community-driven approach.
The combined leadership of the EastPoint Coordinating Council also recognizes the importance of sustainability in its broadest sense. Initial collaborations and collective successes in the targeted EastPoint footprint have been a testament of how working together can achieve greater success and will be the foundation to the forthcoming initiatives for the City of San Antonio. Considering what has taken place thus far, the city council leadership has allocated funds for the coordinating council to develop a sustainability plan for continued EastPoint revitalization. Following a qualitative and quantitative evaluation of the various grant programs and initiatives, a sustainability plan for EastPoint efforts will be used to develop strategies and recommendations on which programs and initiatives should be replicated in other parts of the Promise Zone and other parts of the city as well as sustainability strategies for replication.
Indianapolis Congregation Action Network23

Background and History

The Indianapolis Congregation Action Network (IndyCAN) is a multiracial, multi-faith, nonpartisan organization in central Indiana that catalyzes marginalized people and faith communities to act collectively for racial and economic equity. Founded in 2012, the mission of IndyCAN is to “build the leadership capacity of low- and moderate-income people who live, work, and worship in central Indiana, empowering them to work alongside service providers, policymakers, and other stakeholders to increase collaboration, leverage resources, and improve the systems impacting their lives.”24 IndyCAN’s expanding alliance reaches tens of thousands of people from Indiana’s 17 largest denominations and the Catholic Archdiocese. IndyCAN is a member of the People Improving Communities through Organization (PICO) National Network,25 a network of faith-based community organizations working to create innovative solutions to problems facing urban, suburban, and rural communities.
IndyCAN seeks to achieve its vision of “Opportunity for All” by building the power of traditionally excluded communities through leadership development, amplifying the prophetic voice, awakening the electorate, and creating strategic partnerships that reshape the environment to advance regional, state, and national policy campaigns (IndyCAN, 2014) (see Figure 5-12). When launched in 2012, IndyCAN had one major goal: to connect 10,000 families affected by economic hardship to employment by addressing the issues of mass incarceration and gun violence, economic dignity, and immigrant integration and inclusion in the community. This overarching goal brought together a large coalition of clergy, people of
___________________
23 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
24 For more information, see http://www.indycan.org/about (accessed September 13, 2016).
25 For more information, see http://www.piconetwork.org (accessed September 13, 2016).
SOURCE: Indianapolis Congregation Action Network. 2014. Annual Strategic Report. Used with permission.
faith, and civic and business leaders. Today, IndyCAN’s “Opportunity for All” Policy Platform has the following objectives:
- create career pathways to jobs of the future
- invest in equitable regional transit that gets people to work
- reduce mass incarceration and gun violence
- and pass a fair, direct, and inclusive pathway to citizenship for 11 million aspiring Americans (IndyCAN, 2014)
The Indianapolis metropolitan area faces many economic and social challenges (see Table 5-10 for the demographics of Marion County). The area has the eighth fastest-growing poverty rate in the nation, which also translates into a lack of economic opportunity (IndyCAN, 2014). The state of Indiana is ranked 49th in the country for economic mobility—that is, the likelihood that a poor child will transition out of poverty and into
TABLE 5-10 Marion County, Indiana, Demographics
| Total | ~934,243 residents |
| Race/Ethnicity | 57.9% white |
| 27.1% African American | |
| 9.8% Latino or Hispanic | |
| 2.6% Asian | |
| 0.5% Native American/American Indian | |
| 0.1% Native Hawaiian/other Pacific Islander | |
| Health | 32% adult obesity |
| 19% adults report having poor or fair health | |
| 19% uninsured | |
| Violence | 45% increase in murder rates (2010–2014) |
| 144 victims of homicide in 2015 | |
| Education | 76% of students graduate from high school |
| Employment | 6.5% unemployed |
| Income | 82% increase in poverty over the last decade |
| 31% of children living in poverty |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: County Health Rankings, 2016b; IndyCAN, 2014, 2016b.
the middle class (IndyCAN, 2014). The percentage of children in Marion County living in single-parent households is among the highest in the state, at 47 percent (County Health Rankings, 2016b). Between 1985 and 2014, the per capita jail population in Marion County doubled, with African Americans being 3.1 times as likely to be in jail than their white counterparts (IndyCAN, 2016b).
Marion County ranks 83rd out of 92 counties in Indiana for health outcomes, and based on measures of health behaviors, clinical care, social and economic factors, and the condition of the physical environment, it ranks last out of 92 counties for health factors (County Health Rankings, 2016b).
The IndyCAN model for action is adapted from the PICO Community Organizing Model as a faith-based, broad-based organizing model that makes shared values and social relationships the binding factors that hold organizations together, rather than specific issue-based organizing. This creates a sustainable vehicle for state wide organizing and building capacity. The organization is rooted in local organizing committees, which engage community members through dialogue, local and regional trainings, and research meetings to identify the priorities of the community. The 38 participating congregations26 that make financial contributions,
___________________
26 For a full list of participating congregations, see http://www.indycan.org/about/congregations (accessed December 5, 2016).
“missional members,” receive training to build capacity among their clergy and laity teams.
IndyCAN has various community, regional, and state-level partners outside of the realm of health. The organization has an extensive legal network, including the American Civil Liberties Union (ACLU), to support its work to protect immigrant families and promote criminal justice reform. IndyCAN leadership holds meetings with local and state-level policy makers, thought leaders, policy experts, and public officials to develop strategies and inform their decisions. IndyCAN has partnered with Indiana University, the University of Minnesota, the University of Wisconsin, the Vera Institute, and others to support community-led research as well.
Integrated Voter Engagement
Integrated Voter Engagement (IVE) is a year-round program that connects voter engagement to issue-based organizing in order to build power, sustainability, and impact over multiple election cycles. IVE is a more sustainable model for voter engagement in contrast to traditional campaigning methods, which tend to be seasonal operations (Paschall, 2016). In preparation for the 2014 midterm elections, IndyCAN volunteers garnered more than 15,000 pledges to vote, including pledges from more than 5,000 unlikely voters who were predominately low-income and people of color (Paschall, 2016). In 2014, IndyCAN doubled the African American and Latino turnout in three pilot districts, and by 2015, IndyCAN voter contact grew to 11 percent of every person that cast a ballot in Marion County, Indiana (IndyCAN, 2016a). IndyCAN has been successful in leveraging the already existing social networks within congregations and clergy voice, seen as credible messengers, to strengthen its voter program. These social networks and relationships are integral to promoting civic engagement and ensuring that people who pledge to vote will follow through (Paschall, 2016).
Addressing the Social Determinants of Health
While at first glance IndyCAN may not appear to be directly targeting health outcomes, it is clear that the work of the organization seeks to improve many of the social and economic determinants of health to achieve its mission of racial and economic equity.
Employment Employment opportunities as a means to promote economic dignity are a critical issue within IndyCAN’s mission, as it supports opening and expanding pathways to jobs with family-sustaining
wages, developing career pipelines that align training with employer needs, and removing barriers to employment, good wages, and benefits. In an effort to expand entry points for low-income and entry-level workers to middle-class careers in high-growth industries, the organization works to align workforce development and educational programs directly to employer needs. Since its founding, IndyCAN has promoted policies that have contributed to 9,738 new jobs and 52,620 trained workers and have removed barriers to employment for 253,600 immigrants, formerly incarcerated “returning citizens,” and excluded workers in the region. For example, IndyCAN advocated for the first local hire requirement implemented in the state, which requires 30 percent of jobs created through downtown development tax increment financing to be directed to local low-income residents and allocates $3.5 million in job training and micro loans for minority businesses, which has resulted in good jobs for residents facing economic hardship (IndyCAN, 2014). IndyCAN also convenes educational institutions, workforce development organizations, and community members to expand the career pipeline by putting best practices, such as on-the-job training, in place.
Public safety Faced with rising homicide and incarceration rates, in addition to the associated costs of violence, IndyCAN has prioritized public safety and incarceration on its agenda. Specifically, the organization strives to reduce violence by advocating for the implementation of the U.S. Department of Justice’s top-rated, evidence-based, nationally recognized strategy, Ceasefire. The Ceasefire approach has cut homicides by 30 to 60 percent in cities across the nation27 by linking those who are at the highest risk of engaging in violence to jobs and alternatives to street life, healing the broken relationship between law enforcement and communities of color, and better integrating immigrants and previously incarcerated individuals into the community. To address recidivism, IndyCAN also promotes strategies such as transitional jobs and housing for the formerly incarcerated. IndyCAN currently partners with the mayor and the county sheriff with the goal of reducing Marion County’s incarceration rate by 20 percent in 2018. This plan includes diversion programs for people with mental illness, addiction, and for low-level nonviolent offenders.
When the city of Indianapolis announced its plans to build a new $1.75 billion criminal justice center in 2014, residents expressed concerns that it would perpetuate the cycle of mass incarceration for low-income communities of color. IndyCAN organized residents and put forth a campaign that “brought together an unparalleled coalition of business, government,
___________________
27 For more information, see https://nnscommunities.org/impact/results (accessed October 18, 2016).

SOURCE: Personal communication with Shoshanna Spector to National Academies staff on September 20, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
and community leaders” that prompted the city council to halt the project and commit to restorative criminal justice reform strategies (Paschall, 2016). IndyCAN’s current Jobs Not Jails initiative is informed by the body of evidence that suggests the disproportionate burden of incarceration on low-income communities of color as well as the importance of employment opportunities in reducing violence and recidivism. Jobs Not Jails outlines concrete steps28 for the city to take to ensure that a new criminal justice center reduces violence and keeps people out of jail. In 2014, IndyCAN successfully campaigned to “ban the box,” leading to the passage of an ordinance that prohibits city or county agencies and vendors from inquiring into an applicant’s conviction history until after the first interview (see Figure 5-13). It should also be noted that the organizing
___________________
28 For more information, see http://www.indycan.org/issues/mass-incarceration (accessed September 14, 2016).
efforts of IndyCAN laid the groundwork for the Indiana Supreme Court decision in September 2016 to end money bail practices for all low-level nonviolent, offenders.
Transportation IndyCAN works to achieve its vision of an equitable public transit system through its Ticket to Opportunity initiative.29 The initiative was developed after the organization commissioned a study that revealed a broad base of support for new investment in mass transit, in addition to the effect that inadequate transit has as a barrier to employment opportunities and other important resources (IndyCAN, 2016a). IndyCAN is organizing to pass a regional transit expansion referendum in November 2016 that will triple bus service in Indianapolis. This expansion is projected to fuel economic development and increase job access for low-income communities threefold (IndyCAN, 2016a). The Ticket to Opportunity field program is initiating dialogue with 80,000 marginalized voters of color through large-scale integrated voter engagement to build sustained capacity for achieving transit equity. Thus far, more than 2,000 community members have communicated with their legislators in town hall sessions, in-person meetings, statehouse visits, calls, letters, and media events in efforts to convince them to support the passage of this bill (IndyCAN, 2014).
Education IndyCAN advocates for increased access to higher education and works to increase the accessibility of higher education to all immigrant students. The organization’s priorities include providing equal access to in-state tuition for all students who graduate from high schools in Indiana and working to pass the DREAM Act in Indiana. IndyCAN is also organizing to expand quality prekindergarten education in the state of Indiana.
Social environment Efforts to improve the social environment are integrated throughout the work of IndyCAN. For example, IndyCAN provides civic gathering places at member congregations in various neighborhoods, many of which do not have other stable venues for civic gathering purposes. Furthermore, IndyCAN develops leaders who become involved in civic engagement, often for the first time. In 2015, IndyCAN trained 874 people who engaged 4,945 participants in its campaigns through personal visits, congregational events, town halls, vigils, research actions, and voter outreach, in addition to shaping IndyCAN’s Jobs Not Jails platform. IndyCAN clergy, staff, and leaders conducted 108 trainings, including
___________________
29 For more information, see http://www.indycan.org/transit/the-ticket-to-opportunity-platform (accessed September 14, 2016).
two leadership assemblies, four strategy team meetings, 96 trainings in congregations, and 12 clergy councils.
Finally, IndyCAN builds relationships and social networks across racial and ethnic differences to strengthen the social fabric of communities and to develop residents’ sense of purpose and self-worth, all of which contribute to social and emotional health.
Data and Outcomes
As a member of the PICO network, many measures of progress that IndyCAN tracks are measures of civic engagement and community organizing. This includes estimates of the numbers of participants at trainings, conferences, and other organizing activities; the number of trainings given; the number of votes secured for particular ballot measures; the size of the voter contact network; and the levels of empowerment. Speer and colleagues found that the average PICO member engages in 76 percent more civic activities than the average resident (Speer et al., 2010) (see Figure 5-14).
IndyCAN also relies on data sources across various sectors to inform and support their platforms on issues such as public safety and transit expansion. For instance, IndyCAN’s goal to reduce incarceration in Marion County will be measured using data submitted to the U.S. Annual
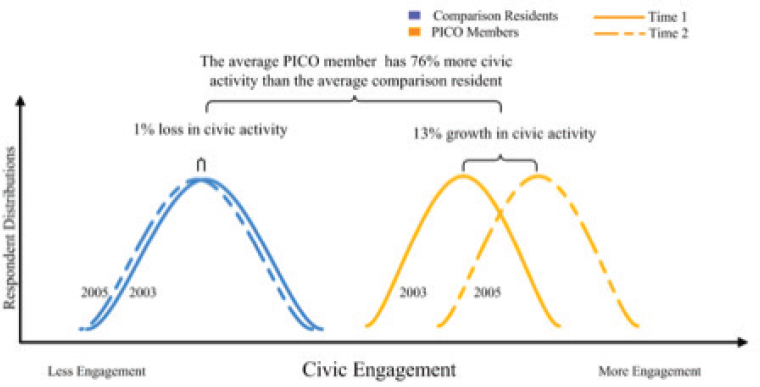
NOTE: This figure is drawn from an unpublished dataset. A subset of these data is presented in Speer et al., 2010.
SOURCE: Speer et al., 2010. Used with permission.
Survey of Jails. IndyCAN aims to build commitment from the U.S. Department of Justice to track and make accessible data to better identify racial disparities and assess outcomes. Additionally, IndyCAN measures access to jobs through expanded transit by using the Indianapolis Metropolitan Planning Organization’s geographic information system mapping data.
Promoting Health Equity: Key Elements
IndyCAN’s main platform, “Opportunity for All,” is based on the premise that every person should have equal opportunity to access the conditions and resources necessary for the region to achieve racial and economic equity. This shared vision of opportunity for all is central to achieving community health, economic growth, and, ultimately, health equity. IndyCAN uses its extensive network of congregations to harness and uplift the collective voice of its communities and, in particular, marginalized populations. IndyCAN also recognizes and uses the power of faith-based leaders to create a shared vision and value among congregants. Religious leaders are a trusted source of guidance in Indiana, which is the 16th “most churched state in the nation” and where one in three voters is Catholic and 84 percent of African Americans say that religion is important to their decision making (IndyCAN, 2016a). IndyCAN works to equip faith-based leaders with the tools to teach and act on the imperative for achieving equity in transit, justice, and economic dignity.
A key element of IndyCAN’s work is the formation of strategic partnerships across sectors to enable the community to act collectively as a region and to leverage collaboration to achieve its shared goals. IndyCAN has been able to create a strong coalition of business, government, and community leaders across sectors to mobilize around issues that are important to residents. Since its founding in 2012, the organization has launched three coalition partner tables covering the areas of transit expansion, immigrant integration, career pathways, and criminal justice reform, with participation from elected officials, policy makers, and several other partners. Collaboration with policy makers and public officials has proven to be vital to achieving long-term, measurable systemic outcomes. Data collection is one of many important activities of IndyCAN that has required partnerships across sectors, including such partners as the Metropolitan Planning Organization, EmployIndy, and the Bureau of Justice Statistics.
IndyCAN builds leadership and community capacity from the grassroots level, empowering individuals into a collaborative, organized movement of people with shared values and power. Through the facilitation of civic gatherings and providing leadership training that teaches residents to use the tools of democracy to improve their communities, IndyCAN is
creating sustained community capacity. Low-income leaders—including people of color, immigrants, and returning citizens—continue to guide all aspects of decision making in the organization. Campaign decisions are initiated by local congregations and then ratified through local organizing committees (LOCs). Low-income LOC leaders maintain an ongoing dialogue with hundreds of low-income families through regular one-on-one conversations, check-in calls, and congregation-wide assemblies to ensure accountability and invite participation in decisions. At least two delegates, elected by each member congregation, vote at six Council of Representative (COR) meetings per year and shape countywide issue campaigns and strategy, set organizational direction, and review the annual budget. COR meetings also provide an entry point for new low-income leaders to participate in the broader organization.
IndyCAN also produces tool kits and other resources30 for communities seeking to initiate dialogue and organize their congregations.
Sustaining Success
In order to sustain its work, IndyCAN raises funds from partners, individual donors, corporations, and foundations. While the primary source of funding is external donors, 25 percent of resources come from fundraising from internal resources.
IndyCAN’s work is building a vehicle for statewide community organizing. The organization has recently begun initial efforts to create a chapter in northeastern Indiana, with plans to scale up across the state over the next 5 years. The organizing infrastructure that IndyCAN has built across an extensive network of local congregations allows for sustained relationships, and the training programs build a sustained capacity to shape outcomes. For example, in 2015 IndyCAN’s training program focused on deepening its capacity to identify and challenge structural racism, race privilege, and implicit bias in all of its policy change campaigns. The training program is often the only place in the area where people gather and build relationships across race, class, and religion to understand the intersections of IndyCAN’s work and build a shared commitment to the work of racial and economic justice.
___________________
30 For more information, see http://www.indycan.org/tools (accessed September 14, 2016).
Magnolia Community Initiative31

Background and History

The Magnolia Community Initiative (MCI) originated from a strategic planning process within the Children’s Bureau of Southern California,32 a private, nonprofit agency, in 2001. By asking, “How can we prevent many of the social ills that rob vulnerable children of their future?” and “How can this be done in an environment where government and philanthropic resources are limited?” the Children’s Bureau identified the key areas that research had shown to be necessary for creating safe and supportive environments in which children achieve the best results and live free of abuse and neglect. Based on this, the Children’s Bureau then became the catalyst for what is now MCI.33 Officially launched in late 2008, MCI’s mission was to “unite the county, city, and community to strengthen individual, family, and neighborhood protective factors by increasing social connectedness, community mobilization, and access to needed supports and services.” Today, more than 70 partners are involved in MCI’s work to transform an entire community by uniting the residents and public and private organizations to change how both residents and organizations think and act as well as how parents behave. The main goal is to improve outcomes for those living in a metro Los Angeles community that is plagued with economic and social barriers. MCI’s approach is a shift from using individual
___________________
31 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
32 For more information, see https://www.all4kids.org (accessed December 5, 2016).
33 For an overview presentation on the MCI, see https://www.youtube.com/watch?v=tc2drcfNHPM (accessed December 5, 2016).
or program-level outcomes to promoting collective responsibility for improving outcomes for children by positively influencing family conditions, neighborhood conditions, protective factors, and positive parenting routines.
MCI’s primary approach is to
- support a learning system that helps partners align their activities toward the mission and strategies of MCI and promote collective actions;
- support a holistic approach characterized by empathy and an understanding that positive neighborhood and family factors need to exist and interact in order to produce health and wellbeing outcomes;
- focus on a linkage system to effectively connect families with appropriate supports;
- promote changes in practice that help organizational partners cope with new demands as they incorporate change and support residents’ positive actions in their own sphere of influence; and
- provide actionable data to inform partners’ efforts and galvanize residents to make changes and achieve improved health and developmental outcomes.
The West Adams, Pico Union, and North Figueroa Corridor neighborhoods served by MCI have 35,000 youth, of which almost one-third are under 5 years of age. (See Table 5-11 for more demographics.) High rates of child abuse, child neglect, and spousal abuse are also present within this community. These neighborhoods are vulnerable, high-need, and
TABLE 5-11 Demographics of MCI Catchment Area in West Adams, Pico Union, and North Figeroa Corridor Neighborhoods
| Total | ~35,000 youth residents |
| Race/ethnicity | 75% Latino |
| 11% Asian | |
| 8% White | |
| 5% African American | |
| Health | 35% of children are obese |
| Education | 40% of children enter kindergarten unprepared |
| 73% of children are not proficient in reading by third grade | |
| 40% of students will not graduate from high school on time | |
| Income | 65% of children live in poverty |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCE: Bowie, 2011.
SOURCE: Bowie, 2011. Used with permission.
low-resource areas with multiple threats, as evidenced by the presence of low-performing schools and low student achievement, high poverty, low employment rates, a high incidence of diabetes and asthma, and high rates of involvement with the child welfare system (Bowie, 2011).
Community Level Change Model
The Magnolia Community Initiative Partners, along with the Children’s Council of Los Angeles and First 5 LA, developed a Community Level Change Model. This model highlights the logic behind building resilience at the individual, family, and societal levels and the community-level changes sought. It is a graphic representation of a theory of change built upon research, some key assumptions, and years of implementing and learning from community-based prevention strategies (see Figure 5-15).
Within the model, the foundation for achieving individual-family and community-level change is increasing the protective factors for and mitigating the risk factors of family and community members. Informed by the Asset Building Community Development Model of John McKnight, resident groups are formed, and by virtue of members coming together to deepen their connections with one another, be each other’s support systems, and learn and grow as individuals, the groups
then become more aware of and involved in improving their neighborhoods (Kretzmann and McKnight, 1993).
Residents participating in neighborhood groups make social connections, increase their resilience for coping with stress, gain knowledge of parenting techniques and the stages of child development, foster their children’s social and emotional growth, and create mutually supportive relationships that provide concrete support in times of need. From these protective factors come a greater sense of community and connectedness plus a move toward civic engagement that is truly resident-owned and resident-led. Resident-owned and -led actions result in partnerships that change institutional policies and practices, transforming and creating neighborhood assets such as high-quality schools and child care, economically viable jobs, good affordable health care and mental health services, safe and affordable housing, safe streets and parks, and other community elements such as libraries, banks, stores, and transportation options. Ultimately, these neighborhood-level assets contribute to the health and well-being of those living within them by contributing to the community-level outcomes of good health, safety and survival, economic well-being, social and emotional well-being, and education and workforce readiness.
Diverse Network of Partners
The Magnolia Community Initiative network includes an array of partners across various sectors. These include multiple partners operated by the Los Angeles County Chief Executive Office, including social services, child support, and child protection; regional organizations responsible for populations of children (e.g., the Los Angeles County Unified School District, Women Infants and Children Nutrition Program, and child care resource and referral); and private and nonprofit community-based organizations providing health care, early care and education, including Head Start and Early Head Start, family support, and banking and economic development services and supports.
The initiative began with a small group of cross-sector organizations recruited by the Children’s Bureau. This core group established the overall approach with which to engage others. Individuals from these organizations coalesced around the shared goal of looking beyond one’s programmatic achievements and embracing the collective goal of improving outcome for the full population of residents within the community, with improved outcomes for young children as the demonstrated marker of this success. Currently, MCI uses an open Web-based platform for communication. There is an orientation process for individuals and agencies asking to join the initiative. However, there are no barriers to entry or exit within MCI. All partners participate voluntarily, contributing what they
can to the collective endeavor. Partners collaborate to align their work and function as a system, shifting from solely delivering individual services to a preventive and holistic approach for each person served (Inkelas and Bowie, 2014).
MCI also created a learning system for partners which consists of meetings, working groups, and improvement projects that build relationships and which aligns actions among agencies and with community residents, improves staff practices, builds agency capacity to better use data to understand the effects of one’s practice, and introduces improvement science approaches to improve change processes. Through their involvement, partners are able to improve their individual practice and staff capacities, reflect with others on how to function as a “system” to improve conditions for children and families, and, ultimately, improve outcomes for their community. It is the voluntary nature of MCI that supports its sustainability, as partners serve without shared funding.
Solutions to Address the Social Determinants of Health
MCI’s approach supports and is in alignment with cross-sector efforts, as each organization provides services within the sector of its competency. MCI then works on processes that enable different sectors across the social determinants of health to function more fully as a system to achieve positive results.
Social environment At the same time, MCI staff facilitates Belong Neighbor Circles, which are structured discussions of residents that introduce the concepts of protective factors, empathy, and belonging, with the goal of motivating residents into action. These discussions are intended to increase personal connections among the participants; expand the relationships of participants within their neighborhood; expand and strengthen participants’ connections to community resources, supports, and information; and empower residents to acknowledge when they have a concern about the well-being of a neighbor or family member and act on those concerns to improve the well-being of individual families and therefore the community at large. Pre- and post-survey data reveal an increase in positive attitudes in the community around available resources, social cohesion, and perceptions of safety (see Figure 5-16).
Data and Outcomes
To collect data to measure community-level outcomes, MCI first created a community profile from publicly available datasets. In addition, MCI used the Early Development Index (EDI), a validated population
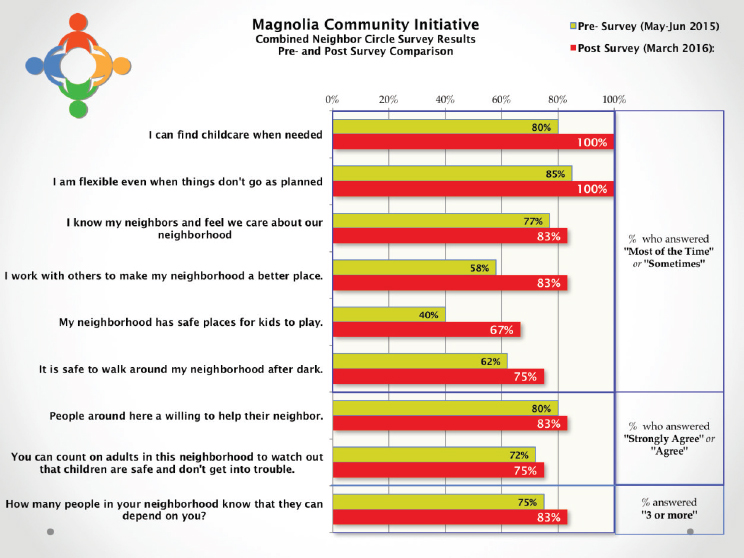
SOURCE: Personal Communication with Ron Brown to National Academies staff on November 18, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas. edu). Used with permission.
measure of children’s well-being. EDI measures child development in 5-year-olds based on their kindergarten teacher’s assessment across the following developmental domains: (1) physical health and well-being, (2) social competence, (3) emotional maturity, (4) language and cognitive skills, and (5) communication skills and general knowledge (Bowie, 2011). The results based on this index can be geographically mapped to neighborhoods (see Figure 5-17).
MCI created a Protective Factor and Community Belonging Survey by drawing items from multiple validated surveys and administered it biannually to individuals living in the catchment area beginning in 2009, with 2015 the most recent year it has been administered. The survey asks about wellness behaviors, protective factors, family conditions, access to services and supports, and contact with network partners.
MCI has also developed a dashboard that displays monthly and quarterly progress on actions related to family behaviors and their experiences
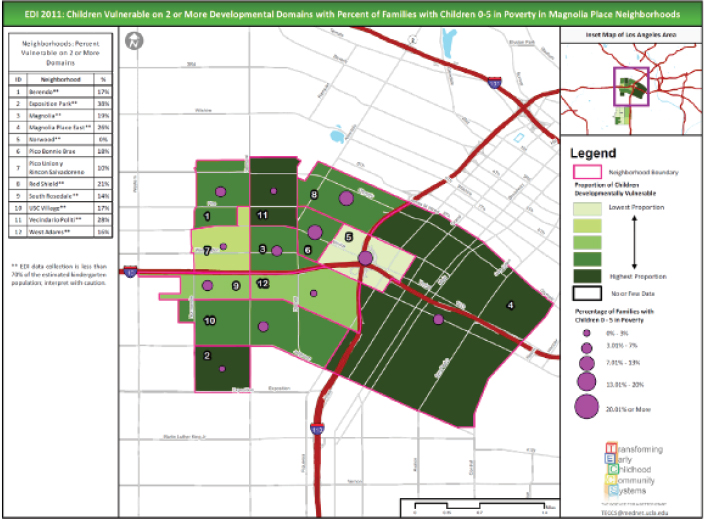
NOTE: The UCLA Center for Healthier Children, Families, and Communities, under license from McMaster University, is implementing the Early Development Instrument with its sublicenses in the United States. The EDI is the copyright of McMaster University and must not be copied, distributed, or used in any way without the prior consent of UCLA or McMaster. @McMaster University, The Offord Centre for Child Studies. Used with permission.
SOURCE: Personal communication with Ron Brown to National Academies staff on November 18, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
with organizational partners. The MCI dashboard includes feedback from residents regarding their experiences while engaged with partner organizations, linkage and referrals made using its MCI CareLinQ system, Innovation group progress, and the latest MCI Community Survey outcomes (2015).
Promoting Health Equity: Key Elements
A shared vision for improved outcomes among children and families is what binds together the network of more than 70 government and private-sector partner organizations that make up MCI. The initiative also works toward a vision for a socially connected community by enhancing the linkages and partnerships within its network. This translates to shared accountability and a fostering of relationships among network partners (i.e., enhancing familiarity with each other, linking clients to one another) to strengthen their impact on the community as a whole (Inkelas and Bowie, 2014).
Engaging residents has been a key component of MCI from its inception. The initiative recognizes that community members and residents need to play an active role not only in working to improve neighborhood and family conditions but also in the stages of providing input on what kind of changes they would like to see. MCI is predicated on the belief that residents who engage with each other within the construct of the initiative will increase community capacity, which is necessary to sustain improvements in child safety, health, and nurturing. To that end, the Belong Campaign34 effort to engage and mobilize residents focuses on strategies to build social connections, develop ties with neighbors, and create leaders (neighborhood ambassadors) who can help connect residents to the resources available in the community. (See Figure 5-18 for a photograph of Belong participants.) By building their network of support, neighbors will have greater opportunities to increase each other’s potential to be a positive force in their families and in their neighborhoods.
MCI also has strategies to improve organizational capacity for using data and cross-systems approaches to improve collective action. The strategies range from innovation groups that are using and teaching improved approaches—which include iterative testing and the use of data and charts for assessing change coupled with an improvement coach—to larger group collective action projects such as prototyping and testing the Web-based linkage and referral platform (CareLinQ). MCI has also developed a fellowship program. Currently in its fourth year, the fellowship
___________________
34 For more information, see https://www.youtube.com/watch?v=CUEtCD_I9iU (accessed December 5, 2016).

SOURCE: Personal communication with Patricia Bowie to National Academies staff on October 12, 2016. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas. edu). Used with permission.
supports mid-level and emerging agency leaders in building their professional capacity to adopt and support the data, improvement and other approaches that MCI has adopted for itself and its agency and at the same time to continue to deepen and foster cross-sector relationships among the MCI partners.
An especially noteworthy aspect of MCI is its ability to foster and maintain a culture of collaboration with many partners across a variety of sectors and disciplines. The initial recruitment strategy for partners was led by the Children’s Bureau. A factor in the selection of partners that was crucial to facilitating a culture of collaboration was capturing a diverse group committed to the overarching goals of MCI and willing to lead through collaboration and not simply competition. This is especially challenging, because community groups and organizations are constantly shifting between cooperation and competing for limited resources to meet their organizational needs (Bowie, 2011). In MCI, collaborative groups are developed based on interest and are led by those partners with the time, resources, and expertise to advance a project. Leadership within the initiative is informal and not prescriptive, and there is no monetary compensation for participation.
Challenges and Lessons Learned
The challenges to taking on this level of work and desired outcome are seemingly endless. For example, maintaining involvement and participation, fostering cooperation over competition, sustaining one’s own agency or family and having enough time and resources to contribute to a collective good or goal, having sufficient resources to achieve the necessary scale for large-scale change, and tracking progress in ways that are meaningful to a diverse group of key stakeholders, each with varying interests and ways of viewing success.
MCI has embraced a collective response in order to both address the interrelatedness and complexity of today’s problems and to enable equitable access to the opportunities needed to thrive given today’s possibilities. The initiative also recognizes that these collective endeavors require new ways of working, which includes new structures, social processes, and practices from the individuals, organizations, and the larger systems of which they are a part.
Yet there remains very little in the way of sharing the exploration and “testing” of what new structures, processes, and practices might better ensure equitable access and opportunity to thrive in the realities of today’s economy. Maintaining sufficient momentum and sufficient engagement to change culture and practice to achieve better results within any one sector is well documented, and adapting these processes continues to be an ongoing exploration across many fields. However, applying this learning to achieve societal goals and address community-specific challenges remains an ongoing process of exploration, testing, learning, adapting, and resilience to all other things happening at the same time. Maintaining this as the focus is likely to be MCI’s greatest challenge.
Sustaining Success
MCI was not designed as a 5- or 10-year plan, but rather as an approach that will expand over time and over generations within the community and organizations serving the community. For the first 2 years, the MCI director was the only staff member of the initiative. In more recent years, MCI has brought in other staff members to assist in strengthening some of the core support functions for the network. These include a data manager, an improvement coach, the MCI Belong organizing team, and a staff member focused on providing project management support of cross-agency projects. While recognizing that moving to managing a staff team requires a fair amount of time and energy, MCI decided at this time that having a stronger staff infrastructure will ensure success in sustaining MCI’s approach to community change.
The MCI fellowship is a built-in sustainability mechanism which nurtures the next generation of leaders, grounding them in the MCI philosophy and practice. With each alumni group of mid-level managers, MCI ensures that its principles and practices are well integrated back into a partner organization. There is intended focus on passing on the vision, creating shared leadership so that the initiative continues to produce meaningful impacts on population community well-being and achieving the outcomes at a neighborhood level. Importantly, the building of data points over time to demonstrate change in the outcomes for children and families is a vital part of the sustainability strategy in order to ultimately attract ongoing investment and support from government and the philanthropic community. Recently, MCI received a $2 million collaborative gift from the Doris Duke Charitable Foundation and the Tikun Olam Foundation to assist with the data capture and communication strategy for sharing overall progress and lessons learned.
Mandela MarketPlace35

Background and History

Mandela MarketPlace creates sustained community economic development through investments and programming in local solutions to food system challenges in historically marginalized communities. To achieve this, Mandela implements community-informed programming to increase food access and build economic opportunity—addressing issues of economic disinvestment, food insecurity, and health inequity by building on local assets. These programs span the breadth of the food chain, including producer support to increase market share, healthy food accessibility in urban markets, nutrition education and demand stimulation, and food retail business incubation.
Incorporated as a nonprofit in 2004 and based in West Oakland, Mandela MarketPlace’s mission is “to work in partnership with local residents, family farmers, and community-based businesses to improve
___________________
35 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
health, create wealth, and build assets through cooperative food enterprises in low-income communities” (Mandela MarketPlace, 2013). Recognizing that food-based strategies can provide an avenue for sustainable economic development, Mandela’s model emphasizes investment in local communities to reverse the effects of long-term disinvestment and systemic racism.
Located in Alameda County, West Oakland is a historically African American neighborhood in the northwest region of Oakland that is home to about 36,000 people (City-Data.com, 2016b). Mandela MarketPlace’s work has taken place primarily in a subarea of West Oakland with a population of about 25,000 people who have suffered severely from economic disinvestment and environmental injustices.36 In 2010, West Oakland’s population was 64 percent African American, 16 percent Latino, 9 percent Asian/Pacific Islander, and 7 percent white (City-Data.com, 2016b). Between 2000 and 2010, West Oakland’s African American population declined 20 percent, while the number of Asian/Pacific Islander and white residents increased by 39 percent and 135 percent, respectively (Alameda County Public Health Department, 2015). West Oakland has the highest rates of poverty and unemployment in the county, with 45 percent of households earning an annual income of less than $25,000 (Healthy Food Access Portal, 2016). Additionally, only 23 percent of Oakland residents who are eligible for assistance from the Supplemental Nutrition Assistance Program (SNAP) actually receive benefits (FRAC, 2005; Unger and Wooten, 2006). West Oakland also has the highest rates in the county of certain diet-related chronic diseases, including diabetes rates that are three times greater than in the rest of the county (Alameda County Public Health Department, 2008). Approximately 48 percent of adults suffer from obesity (Healthy Food Access Portal, 2016), with persistent disparities by race and ethnicity. The prevalence of obesity by race and ethnicity is 28.9 percent for African Americans, 26.6 percent for Hispanics, and 5.5 percent for Asians/Pacific Islanders (Alameda County Public Health Department, 2014). As the neighborhood is surrounded by two freeways and adjacent to the Port of Oakland, residents of West Oakland suffer from greater exposure to environmental pollution and exposure-related health conditions. Compared to residents of the Bay Area, residents of West Oakland are exposed to three times more diesel pollution (Alameda County Public Health Department, 2014). West Oakland residents are also two and a half times more likely to develop cancer in their lifetime and have the highest rates of asthma hospitalization in the county (Alameda County Public
___________________
36 Personal communication with Mandela MarketPlace staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
TABLE 5-12 West Oakland Demographics
| Total | ~36,000 residents |
| Race/Ethnicity (2010) | 64% African American |
| 9% Asian/Pacific Islander | |
| 16% Latino | |
| 7% white | |
| Education | 7.9% completed high school |
| 7.3% received an associate’s degree | |
| 14.1% received a bachelor’s degree | |
| Income | Median household income in 2013: $38,480 |
| 33.9% below poverty level |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: City-Data.com, 2016b; U.S. Census Bureau, 2010.
Health Department, 2014). See Table 5-12 for a summary of demographic information of West Oakland’s population.
Throughout the early to mid-1990s, West Oakland was a prosperous working-class neighborhood of cultural activity, economic growth, and social activism. Host to a vibrant jazz and blues community in the 1940s and 1950s and the birthplace of the Black Panther Party in the 1960s, West Oakland was the last stop of the Transcontinental Railroad and thus also served as an economic and transportation hub (The Planning History of Oakland, n.d.). The neighborhood experienced devastating economic and cultural decline with the waning of the war economy, the onset of discriminatory housing and redlining policies, and the displacement of African American residents and the destruction of their homes and businesses due to urban renewal (Soliman, n.d.). Disinvestment and discriminatory social policies have had lasting destructive effects on the neighborhood.
For far too long, communities like West Oakland have suffered intentional and sanctioned disinvestment—stripping people of financial assets, social cohesion, and human dignity. The primary challenges [facing West Oakland] are those of a community that is not only unequal but also inequitable. To bridge this equity gap, targeted investment in people and community builds a foundation for community re-investment—a foundation composed of engaged and honored community voices, resources directed specifically to empower those voices, and core values that honor community-owned solutions and economies for community benefit, grounded in a demand for health and a respect for culture.
—Dana Harvey, Executive Director, Mandela MarketPlace
Residents of West Oakland have been rebuilding their community and fighting socioeconomic and environmental injustices that have
lingered from the period of urban renewal. The founding of Mandela MarketPlace stemmed from these ongoing collective efforts, specifically the efforts of residents of color who had become increasingly concerned about the lack of access to affordable healthy food in their neighborhood. Through grassroots organizing efforts, residents established a comprehensive community planning process that recognized the need to provide economic opportunity to low-income residents of color and support under-resourced local farmers and local business owners in creating a sustainable community-owned food system.
In 1998 the University of California Cooperative Extension initiated a food and health needs assessment with the Environmental Justice Institute (EJI) and community residents. The results of the assessment affirmed residents’ recognition of their community’s need for food security and economic opportunity. EJI organized a series of community meetings, town halls, church events, nutrition workshops, and focus groups for residents, from which the West Oakland Food Collaborative was created in 2000 to provide a grassroots platform and community voting process through which residents developed a plan of community ownership and local employment and business expansion. In 2003 the U.S. Department of Agriculture (USDA) awarded a 3-year, $225,000 Community Food Projects grant that helped create the Mandela Farmers Market and the Healthy Neighborhood Store Alliance. In 2004 Mandela MarketPlace was incorporated as a 501(c)(3) nonprofit in order to support the opening and incubation of the Mandela Foods Cooperative. In 2009 Mandela Foods Cooperative opened and remains the only full-service grocery store serving West Oakland, operating as a worker cooperative owned by community members. It was incorporated by community members in 2004 as a worker-owned cooperative with grant and loan support from several sources, including the Walter and Elise Haas Fund, the West Oakland Project Advisory Community, a city council member, and the Oakland Business Development Center.
Solutions to Address the Social Determinants of Health
Mandela MarketPlace has launched a number of programs that increase food security, expand local employment opportunities, build individual and community wealth, provide health and nutrition education, improve the built environment, and strengthen outcomes through integration with the health care sector.
Employment and income Mandela has improved local workforce development by hiring and training local residents and supporting local farmers with a greater distribution network. Residents, farmers, business
owners, and entrepreneurs of the community have also built wealth through opportunities to earn family-sustaining incomes, participate in business and entrepreneurial training, expand their customer bases, and receive microfinance loans.
An example of these opportunities put into action is Mandela Foods Cooperative, a 2,200-square-foot grocery store that stocks fresh produce, 50 percent of which is sourced from local farmers of color who grow their produce sustainably and are members of the Mandela Foods Distribution network, a venture of Mandela MarketPlace. Mandela Foods Cooperative does not sell alcohol, tobacco, or products with high fructose corn syrup. It is collectively owned by worker-owners who are all local residents of color. Currently the store is run by four worker-owners and employs two full-time employees and hopes to expand to eight worker-owners and three full-time employees in the near future. The store serves more than 250 customers daily and since opening has generated sales revenue of more than $4 million ($1 million in 2014 alone), which has benefited its worker-owners as well as members of the Mandela Foods Distribution network. Supported by a 2006 grant from The California Endowment and a 2011 grant from the California Department of Food and Agriculture, the network includes under-resourced farmers of color who operate within 200 miles of the Bay Area and who have access to flexible, no-interest loans that can be repaid with produce through Mandela MarketPlace’s Harvest to Market loan program.37
Physical and social environment Mandela MarketPlace also provides a range of educational programming related to health and nutrition. Its programs include nutrition education workshops, cooking classes, and community outreach events. In partnership with Highland Hospital, Alameda County’s safety net hospital, Mandela provides classes taught by dieticians to high-use patients. As of 2015, Mandela’s educational programs had trained 26 peer educators, 10 youth, and 30 community residents on nutrition and food access. Community control of programmatic planning and allocation of resources has improved the social environment by building social capital among residents and community stakeholders. Mandela partners with local health clinics, hospitals, and senior centers to increase access to affordable healthy foods and provide education about the importance of healthy food consumption. Mandela has provided support to Oakland Based Urban Gardens to create Oakland’s first land trust, a community garden near a local high school, and a park located in a residential neighborhood. Mandela has also supported Planting Justice,
___________________
37 For more information on the Harvest to Market loan program, see http://media.wix.com/ugd/c3e56b_32738ccf66cf47ef9e967f295bcfd280.pdf (accessed December 5, 2016).
an Oakland-based food justice nonprofit, to undertake gardening projects at schools in East Oakland.
Data and Outcomes
Mandela’s current data collection efforts38 include obtaining monthly totals of produce sales through Mandela Foods Distribution; customer tallies at produce stands; randomized tallies of the number of fruit and vegetable customers at corner stores in its Healthy Retail Network; quarterly intercept surveying of fruit and vegetable customers at all retail sites (including corner stores, produce stands, and Mandela Foods Cooperative); customer receipt data from Mandela Foods Cooperative; and bi-weekly inventory records of produce distribution at each corner store. Figure 5-19 illustrates Mandela’s community-owned food system model and some of the key overall outcomes Mandela has achieved.
Promoting Health Equity: Key Elements
Since its founding, Mandela has encouraged shared responsibility among community members and stakeholders in developing programs to achieve better health and socioeconomic outcomes. Meaningful resident and stakeholder engagement has been essential in the organization’s

SOURCE: Mandela MarketPlace, 2013. Used with permission.
___________________
38 Data collection is ongoing, and collected data have not yet been analyzed.
efforts to rebuild and reinvest in communities. Mandela has built a range of partnerships across different sectors to develop collaborative solutions to build healthier and more equitable communities and local food economies.
The integration of economics and health forge natural partnerships among otherwise seemingly different sectors—we do business together, we support improved community health through education and food access, and we promote community ownership of the food system and the economies that develop within and around that system.
—Dana Harvey, Executive Director, Mandela MarketPlace
Mandela’s partnerships have involved businesses, educational institutions, youth development organizations, housing developers, government agencies (at the city, state, and federal levels), foundations, and others. Specific partners have included the University of California, Davis; Nutrition Policy Institute; Alameda Health Systems; Alameda County Public Health Department; East Bay Community Law Center; Sustainable Economies Law Center; PolicyLink; Centro Community Partners; Oakland Housing Authority; Resources for Community Development; Self-Help Credit Union; California FreshWorks Fund; FarmLink; Alameda County’s Community Development Agency; City of Oakland’s Community Action Partnership program; Mercury LLC (an advertising and marketing firm); California Wellness Foundation; Violet World Foundation; and Y & H Soda Foundation. Mandela has also received essential funding support from USDA, specifically from its Agricultural Marketing Service agency, Food Insecurity Nutrition Incentive program, Risk Management Agency, National Institute of Food and Agriculture, and Healthy Food Financing Initiative.39
Mandela’s commitment to achieving better health and socioeconomic outcomes is also evident in its support of building capacity of local enterprises through business start-up support and loans. In 2013 Mandela received a $400,000 grant from the Healthy Food Financing Initiative to establish a $115,000 revolving fund to support local food enterprises and create 20 jobs. The fund has provided support for Mandela Foods Cooperative, Zella’s Soulful Kitchen (a cafe located inside Mandela Foods Cooperative that is owned by a local entrepreneur), and Mandela Foods Distribution as well as three local food enterprises that sell at Mandela Foods Cooperative and other retail outlets. Mandela Foods Cooperative has supported employee and leadership
___________________
39 The Healthy Food Financing Initiative is operated jointly by the U.S. Department of Agriculture, the U.S. Department of Health and Human Services, and the U.S. Department of the Treasury.
development by providing pathways from employment to ownership and training for its worker-owners and employees. Mandela also invests in youth development. From 2007 to 2013, Mandela supported the West Oakland Youth Standing Empowered program, which provided opportunities for local youth to engage in projects related to a range of community issues, including obesity prevention, improvement of walkable infrastructure and transportation, and neighborhood park improvement.
Challenges and Lessons Learned
Meaningful and sustained community engagement has been an essential component of Mandela MarketPlace from its early organizing efforts to the implementation of its many initiatives. The success of Mandela’s programs has also depended on capable and committed leadership within the organization and from the community, including engagement from stakeholders to align community goals and recruit other areas of expertise when needed. During its early organizing phase, community organizers recognized a need for technical expertise in grocery retail and hired external consultants to provide assistance for developing a business model.
Mandela is regularly expanding its efforts to secure continuous sources of funding. Since its incorporation in 2004 as a 501(c)(3) nonprofit, Mandela has been able to leverage multiple funding sources from various foundations and government grant programs to expand and sustain its work. It has successfully secured funding from multiple sources by demonstrating a return on investment (see Figure 5-19) through important outcomes across different areas, including economic benefits from training employees and expanding businesses as well as community benefits from meeting the need for access to affordable healthy foods.40
Sustaining Success
Mandela has implemented several initiatives with community-based partners to sustain its community-owned food and local economies system model. A case study in Mandela’s sustained relationships in community change can be seen in the organization’s longtime work with James Berk, one of Mandela Foods Cooperative’s co-owners. When Berk first walked into Mandela’s office to participate in the CX3 community survey project, in partnership with Alameda County Public Health Department (ACPHD) and the California Department of Public Health (CDPH), he
___________________
40 Personal communication with Mandela MarketPlace staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).
was 15 years old and attending a continuation school in West Oakland. Over the next 6 weeks, Berk and four other teams of adults and youth conducted surveys throughout West Oakland to assess the community for food access and walkability, including surveying corner markets, analyzing advertisements within 1,000 feet of schools, and documenting the condition of sidewalks and signage visible as students and families walked throughout the neighborhood.
Berk, along with and six other youth who were part of the summer program, charged themselves with using the data to identify and act on built environment improvements. With continued support from ACPHD and CDPH, Mandela MarketPlace and the youth team were able to make important changes in their community, building self-efficacy along with a series of projects aimed at improving their community, increasing healthy food access, and launching the Healthy Neighborhood Store Alliance program in West Oakland. Along the way, Berk matured as a leader in the team and in West Oakland. His work was recognized by the Ashoka Foundation, and the team was included in the Ashoka Youth Ventures program, receiving professional support, making presentations to investors, and traveling to other countries to connect with youth activists around the world. Berk was eventually recognized by Robert Redford’s Art of Activism award in 2010 (Henry, 2011). When Mandela Foods Cooperative offered entrepreneurship training classes in an effort to identify new co-owners, Berk was a key participant. He became the youngest worker-owner, at 18 years old, and has remained an integral part of the Mandela family in the 7 years since.41 See Figure 5-20 for a photo of Berk and other employees of Mandela Foods Cooperative.
Recent examples of successful community-driven partnerships include a public awareness campaign to increase health and nutrition knowledge and a multi-sectoral partnership to increase fruit and vegetable consumption for SNAP-eligible hospital patients. To increase awareness of healthy food availability and importance, Mandela partnered with a design firm and the California State Outdoor Advertising Association to develop and implement a strategic public awareness campaign that included twenty billboards placed throughout the county as well as posters and other materials displayed in local businesses. With 169 million views over 3 months, the billboards publicized the importance of healthy food systems to achieve positive health and socioeconomic outcomes and highlighted
___________________
41 To read more about James Berk’s work with Mandela and his achievements, see http://civileats.com/2011/05/06/james-berk-of-mandela-foods-brings-produce-to-his-people-video; http://blog.sfgate.com/inoakland/2010/06/10/local-teen-shines-while-receiving-art-in-activism-award; and http://www.homelessprenatal.org/news/founder-executive-director-martha-ryan-honored-at-redford-center-event (all accessed December 5, 2016).

SOURCE: Mandela MarketPlace, 2016. Used with permission.
the availability of affordable healthy foods through Mandela’s network of stores and produce stands (Chakrabarti, 2016b). Building on Mandela’s existing work with Highland Hospital, Mandela MarketPlace has launched its Fresh Creds program with support from a 3-year $422,500 grant from the Food Insecurity Nutrition Incentive program.42 Mandela stores and produce stands in West, East, and North Oakland provide a 50 percent credit for each dollar spent on fruits and vegetables to low-income hospital patients who receive SNAP, known locally as CalFresh, benefits. Additionally, clinicians from the hospital assist low-income residents to enroll in CalFresh and provide health and nutrition education at Mandela stores. As demand for healthy foods grows, Mandela and its partners are sustaining engagement with partners across different sectors to ensure affordable access to healthy foods for low-income residents, in an area where points of access to receive CalFresh benefits are scarce (Chakrabarti, 2016a).
___________________
42 For more information on the Fresh Creds program, see http://www.mandelamarketplace.org/freshcreds (accessed December 5, 2016).
The organization’s commitment to developing solutions based on the needs and concerns of community residents has also been a critical success factor for sustainability. Mandela MarketPlace plays a key role in resourcing social, physical, and financial equity gaps that historically marginalized people and communities face. The reinvestment in communities and residents, with the ultimate goal that communities own the solutions, drives Mandela’s work toward creating generational sustainability, uplifting cultural diversity, and increasing equal access to resources that cultivate thriving communities.
People United for Sustainable Housing43

Background and History

People United for Sustainable Housing (PUSH) is a nonprofit with a membership base of community residents that focuses on securing sustainable affordable housing for residents of the West Side neighborhood of Buffalo, New York. Its mission is “to mobilize residents to create strong neighborhoods with quality, affordable housing, expand local hiring opportunities, and to advance economic justice” (PUSH, 2012a). The organization’s main activities are in the areas of ensuring affordable housing and living wage jobs, providing needed community services, and advocating for community members’ needs through political activism. PUSH implements all of its many initiatives with a commitment to sustainable economic development.
___________________
43 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
TABLE 5-13 Demographics of Community Served by PUSH
| Total | ~25,000 residents |
| Race/Ethnicity | ~25% African American |
| ~25% Puerto Rican | |
| ~10% Asian | |
| Income | Annual median household income in 2015: ~$26,000 |
| ~40% of residents earned below the federal poverty line |
SOURCE: Bhatt and Dubb, 2015.
The community served by PUSH is primarily low-income, and a majority of the community’s residents live in poor-quality housing. See Table 5-13 for a demographic summary of the community served by PUSH.
The organization was founded in 2005 by Aaron Bartley and Eric Walker, who began their work with a 6-month canvassing effort surveying residents of the West Side. The door-to-door interviews conducted during the Block by Block campaign revealed that residents were concerned about the many hazardous vacant properties in their neighborhoods. PUSH discovered that a subagency of the New York State Housing Finance Agency owned 1,500 vacant, tax-delinquent lots in Buffalo (200 of which were in the West Side), which were then sold to the State of New York Municipal Bond Bank Agency. After that the properties were bundled and sold at a highly inflated price to the investment bank Bear Stearns (which later failed and was sold in the 2007 to 2008 financial crisis). The lots were not rehabilitated and remained vacant. PUSH petitioned for the release of the properties, and when its efforts were unsuccessful, it attempted to publicize the fraudulence through direct action campaigns that took aim at the governor at the time, whose successor eventually dismantled the bond and relinquished the properties back to the city of Buffalo. The lots could then be transferred to and redeveloped by PUSH or any of its partners, and an $8 million fund was established to assist in redevelopment.
Following these events in 2007, PUSH convened a community planning meeting to create a development plan for a 25-square-block area of the West Side where the annual per capita income was $9,000 (PUSH, 2012a). Annual community planning meetings followed, from which the Green Development Zone emerged in 2008. Many of PUSH’s efforts as well as initiatives undertaken in collaboration with other partners take place within this zone of economic development. By 2013 more than 19 residential properties in the development zone had been completed, and a state grant was awarded to redevelop an additional 46 affordable housing units (PUSH, 2012b). The plan for the development zone includes not only the creation of affordable and energy-efficient housing but also
the development of living-wage jobs that encourage a sustainable and community-driven urban economy (Boyer, 2013; PUSH, 2015). Figure 5-21 shows Buffalo residents rallying for energy sustainability.
Solutions to Address the Social Determinants of Health
PUSH operates several suborganizations whose efforts address disparities specific to housing, employment, and the physical and social environments.
Housing and employment The organization’s main activity is reclaiming community control of vacant lots and redeveloping abandoned properties into sustainable, affordable housing for low-income residents. The Buffalo Neighborhood Stabilization Company is a nonprofit subsidiary corporation founded by PUSH that builds affordable housing in the Green Development Zone by operating a land bank in the Massachusetts Avenue Corridor of the West Side. Since 2014 the company has rebuilt more than

SOURCE: Personal communication with PUSH staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
25 vacant lots into affordable apartment units, in total creating about 500 energy-efficient homes for low-income residents.
Another housing initiative founded by PUSH is the Sustainable Neighborhoods Program, drafted in partnership with the state’s housing agencies and signed in 2009. The program provides funding for housing redevelopment projects across the state that are community-driven and emphasize sustainability (PUSH, 2012e).
As part of the development plan for the Green Development Zone, PUSH also emphasizes energy-efficient housing improvement practices and sustainable jobs. PUSH helped to draft Green Jobs–Green New York, which was passed in 2009 with support from a broad-based multi-stakeholder coalition, including members from the labor community and environmentalists. The legislation encourages homeowners to retrofit their homes with energy-efficient upgrades and encourages contractors to hire more workers from marginalized groups. Through its first contract with the New York State Energy and Research Development Authority (NYSERDA) in 2010, PUSH Green was launched to provide weatherization and other house improvement services that promote energy efficiency to homes in western New York. Since 2011 PUSH Green has partnered with NYSERDA installation contractors to retrofit 500 homes. The initiative also focuses on reducing harm caused by indoor pollutants such as lead paint, asbestos, and mold (PUSH, 2012b). Through another NYSERDA grant in 2015, PUSH Green connected low- to moderate-income households to on-site solar photovoltaic incentives and financing offered by New York State.
In 2015 PUSH established PUSH Hiring Hall, a construction company with more than 20 full-time employees from marginalized groups who receive training and earn living wages (see Figure 5-22). Through a partnership with Solar Liberty, the largest solar panel installer in the area, the initiative trains a number of these workers in solar panel installation and provides these services at discount to residents. Over the next 3 years, the partnership will also provide 12 full-time, living-wage jobs in the private sector. PUSH Hiring Hall has also partnered with large developers, including Savarino Companies and Sinatra Development, to place workers in living wage jobs as skilled construction laborers. These development companies are recipients of public subsidies for market rate housing development in the city of Buffalo. Beginning in late 2016 PUSH will also undertake a new project to redevelop a vacant school in the West Side into 32 units of affordable housing specifically for elderly residents and a community hub with a recreational gym, community theater, and office space for local organizations.
PUSH has also expanded its work into other areas of environmental sustainability. PUSH Blue, which focuses on storm water interventions,

SOURCE: Personal communication with PUSH staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
has created more than 10 new living-wage jobs and performed more than 30 projects in the Green Development Zone to help reduce the amount of raw sewage that flows into local water sources.
Partners of PUSH Blue include the Cleveland Botanical Garden, the Buffalo Sewer Authority, and the City of Rochester. As part of the Buffalo Sewer Authority’s implementation of a citywide plan to control combined sewer overflow, PUSH Blue installed 75 bioretention systems on vacant lots owned by the city in 2015 and installed 69 more in 2016 (PUSH, 2015). PUSH also established a subsidiary business44 called PUSH Gro, which markets and sells verniculture compost in partnership with cooperative businesses, including Lexington Cooperative Market and Urban Roots. Figure 5-23 shows a numbr of PUSH volunteers at a green infrastructure installation.
___________________
44 PUSH Gro was established as a benefit corporation. Benefit corporations, or b corps, are “for-profit companies certified by the nonprofit B Lab to meet rigorous standards of social and environmental performance, accountability, and transparency” (B Lab, n.d.).

SOURCE: Personal communication with PUSH staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
Physical environment PUSH has also worked to improve the West Side community’s built environment. In 2011 the Massachusetts Avenue Park campaign successfully lobbied for $350,000 of funding to rehabilitate the largest park in the community (PUSH, 2012c). The organization has also created community gardens and urban agriculture plots in previously vacant lots in the Green Development Zone. It has also encouraged urban agriculture through collaboration with the Massachusetts Avenue Project, a nonprofit that operates a large urban farm on 13 previously vacant lots in the West Side (Massachusetts Avenue Project, 2016). PUSH works to create a more socially supportive environment through its operation of the Grant Street Neighborhood Center, a drop-in community center that provides programs and resources for West Side youth of all ages. Founded in 2009, the center supports an average of 60 youth each day, providing homework help, computers, movies, board games, a dance studio, and arts programs, including a new addition of a West Side Studios stop-frame animation course in partnership with Squeaky Wheel and Ujima Theatre Co., with intended tracks for higher education and workforce in the technology sector. In addition to providing day-to-day academic and
social support, the center aims to provide “a safe, open, and productive space” and to promote youth development and leadership (PUSH, 2015).
Data and Outcomes
PUSH collects data on a number of different measures and is currently conducting a regional mapping project that will map data collected over time to elucidate progress and identify areas where further work is still needed. The measured outcomes include the number of redeveloped housing units, the number of employed workers, the amount of carbon emission reductions, and utility bill cost savings for low-income households. The organization plans to complete the mapping project by the end of 2016.
Promoting Health Equity: Key Elements
From its initial grassroots campaigns to the present day, PUSH’s efforts have consistently reflected the concerns and needs expressed by residents of the community. Seventy-five percent of members of the organization’s board of directors are community residents directly residing in PUSH’s target zone—the Green Development Zone—and the organization convenes a community development committee monthly to determine resident needs and develop solutions to address these needs. The organization also convenes annual community planning congresses and invites professional planners to speak with residents to help identify and address resident concerns. Through these mechanisms, community input on housing, economic, and environmental issues has persisted as the driver of much of PUSH’s work. The partnership between residents and PUSH (and its various suborganizations) ensures that the goals to improve the community are jointly shared.
PUSH has collaborated with many organizations and agencies, increasing stakeholder engagement in achieving its goals and fostering extensive multi-sector partnerships. In addition to partnerships with housing, energy, and parks departments, PUSH has also collaborated with more than 20 nongovernmental organizations, ranging from national organizations and foundations (including the Local Initiatives Support Corporation, People’s Action Institute, Green for All, the First Niagara Foundation, the Center for Community Change, and the Center for Working Families) to other local nonprofits (including the Massachusetts Avenue Project, the Coalition for Economic Justice, the Partnership for the Public Good, VOICE-Buffalo, Open Buffalo, and West Side Housing). PUSH partners with private-sector companies, including a green architecture firm, a network of local contractors, and large banks such
as Citizens, M&T, and HSBC, which have contributed financial donations for projects in the Green Development Zone (Bartley, 2016). The organization advocates for national policy change through its membership in the People’s Action Institute (formerly National People’s Action [NPA]), a network of grassroots organizations rallying around issues related to economic and social justice, and Green for All, a nonprofit that builds participation from minority communities in the green economy and climate change movements. PUSH and the NPA have spoken with the U.S. Department of Housing and Urban Development to encourage its assistance for community redevelopment efforts from federal programs (PUSH, 2012c). Additionally, PUSH held a public forum in 2009 with the Federal Reserve to encourage greater investment in sustainable development from the Community Reinvestment Act and reform lender oversight through the Home Mortgage Disclosure Act (PUSH, 2009).
PUSH’s model of creating a sustainable urban economy through community-based redevelopment and organizing has built community capacity by prioritizing residents’ concerns and encouraging neighborhood leaders to create and implement solutions. Extensive partnership building has helped strengthen the organization’s capacity. Furthermore, many elements of its work could be scalable and transferrable to other low-income communities. For example, the organization’s NetZero House, the first house in the region whose energy consumption is matched by its energy production, has garnered national recognition from media outlets and policy makers (PUSH, 2012d). Additionally, the organization often invites individuals from other organizations to tour the Green Development Zone and gain insights that can be taken back to their own communities.
Challenges and Lessons Learned
The barriers that PUSH has faced in carrying out its work have primarily related to the financing for housing redevelopment and workforce development and training. Premium and maintenance costs for energy-efficient and sustainable construction practices are often higher than for traditional housing redevelopment construction, and covering the premiums with state housing funding programs can be difficult. PUSH has advocated for the state’s funding criteria to be more inclusive of sustainable construction in an effort to overcome this barrier. PUSH also faces challenges in sustaining employment opportunities for workers who receive training from the organization. Building connections with private-sector employers, such as PUSH Hiring Hall’s partnership with Solar Liberty, will continue to be important for overcoming this barrier.
Another barrier is the growing real estate market and early gentrification in the West Side area that has complicated the Buffalo Neighborhood
Stabilization Company’s efforts to acquire land and develop affordable housing. PUSH Hiring Hall has also faced challenges related to the employment-at-will doctrine, which has often been tied to discriminatory and racially motivated hiring, firing, and disciplinary practices.
We’ve tried to position PUSH as a labor-management intermediary in order to protect and advance the interests of otherwise vulnerable contingent construction laborers, most of whom are men of color. We’ve worked to embed protections in our labor contracts, e.g., the right for PUSH to engage the host employer prior to adverse disciplinary action being taken against workers; a progressive disciplinary policy that takes seriously consideration of mitigating circumstances.
—Clarke Gocker, Director of Policy and Initiatives, PUSH Buffalo
WE ACT for Environmental Justice45

Background and History

WE ACT for Environmental Justice (WE ACT), formally known as West Harlem Environmental Action, Inc., is a nonprofit, membership organization that engages in community organizing, community-based participatory research, and advocacy to fight environmental injustices faced by residents of color in West, Central, and East Harlem and Washington Heights/Inwood, marginalized neighborhoods located in northern Manhattan in New York City. WE ACT’s mission is “to build healthy communities by ensuring that people of color and/or low income participate meaningfully in the creation of sound and fair environmental health and protection policies and practices” (WE ACT, 2016a). The organization focuses on improving environmental health and protection through community organizing, policy and legal advocacy, public awareness campaigns, community-based participatory
___________________
45 This summary is an edited account that was prepared on the basis of templates completed by staff of each community initiative. Statements and opinions expressed are those of the community organization and have not been endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
research, civic engagement, and initiatives that influence local, state, and federal environmental health and protection policy and laws. WE ACT also promotes greater inclusion of marginalized communities in environmental reform and decision making by training and educating residents to become informed, empowered voters. See Table 5-14 for demographic information of the community WE ACT serves.
Founded in 1988 by three activists (see Figure 5-24) from West Harlem, WE ACT was the first environmental justice organization in New York City. The organization’s creation was catalyzed by residents’ protests of the North River Sewage Treatment Plant on the Hudson River, which had opened in 1986 and was releasing high levels of toxic emissions and odors. WE ACT cofounders Peggy Shepard, Chuck Sutton, and Vernice Miller-Travis mobilized the community for a civil disobedience protest on January 15, Martin Luther King, Jr. Day, in 1988 (see Figure 5-25). In conjunction with residents protesting across the road from the treatment plant, a small group of community activists and elected officials known as the “The Sewage Seven” rallied directly in front of the plant on the West Side Highway and were arrested for stopping traffic. Over the next few years, WE ACT gained support from local and state elected officials and recruited an environmentalist to research the plant’s operations. In 1992, WE ACT served as the lead plaintiff with the Hamilton Grange Day Care Center and others in a nuisance lawsuit brought against the New York City Department of Environmental Protection (DEP), with pro bono attorneys from the Natural Resources Defense Council (NRDC) and Paul, Weiss, Rifkind, and Wharton. WE ACT cited that racial and class discrimination had motivated the decision to locate the plant in West Harlem rather than in a primarily white neighborhood in the Upper West Side that had originally been chosen for the plant’s location. In late 1993, the parties reached a settlement that mandated a $55 million effort by the city to fix
TABLE 5-14 Harlem Demographics
| Total | ~125,528 residents |
| Race/Ethnicity | 65.0% African American |
| 17.3% Hispanic | |
| 11.7% white | |
| 3.2% Asian | |
| Education | 40.4% completed high school |
| 41.1% completed post-secondary education | |
| Employment | 7.7% of population aged 25 to 64 unemployed |
| Income | Median household income in 2013: $36,395 |
NOTE: Percentages may not add up to 100 percent due to varied reporting, rounding, and missing data from source.
SOURCES: U.S. Census Bureau and American Community Survey data via (statisticalatlas.com, 2016) and (City-Data.com, 2016a).

SOURCE: Personal communication with WE ACT staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.

SOURCE: WE ACT, 2016c. Used with permission.
the plant and established WE ACT and NRDC as monitors to oversee the court-ordered improvements to the plant, including hiring an engineering consultant to ensure that retrofit efforts were completed satisfactorily. The settlement also established a $1.1 million settlement fund to address the environmental concerns of the community, from which WE ACT acquired funds to hire its first three paid staff members in 1994. The settlement also established a $1.1 million Community Environmental Benefits Fund from penalties levied on the New York City DEP by the New York State Department of Environmental Conservation. WE ACT has since grown from a grassroots organizing effort led by a small group of West Harlem activists to a nationally recognized institution that supports and empowers residents to advocate for and achieve more environmentally healthy communities. The organization’s annual budget is about $2 million, with about 85 percent provided by foundations, and it currently has 16 staff members (WE ACT, 2016c).
Civil Rights Law
WE ACT’s origins and present-day efforts are grounded in using civil rights analysis and law to create policy changes that benefit residents and improve the health of communities. In addition to the environmental racism claims in the North River Sewage Treatment Plant case, the second of WE ACT’s earliest activities also used civil rights law to create policy change.
In 1988, WE ACT filed an injunction in the state supreme court calling for an environmental impact statement by the Metropolitan Transit Authority (MTA) over its proposal to build a sixth diesel bus depot uptown in West Harlem, which was already disproportionately burdened by pollution-producing facilities. The northern Manhattan neighborhoods of East, West, and Central Harlem and Washington Heights/Inwood were hosting five of the six Manhattan bus depots. In 2000 WE ACT filed a Title VI46 administrative complaint with the U.S. Department of Transportation against the MTA when it sold a bus depot in the South Bronx and sent 200 buses to over-capacity depots in northern Manhattan where the buses sat—often idling—near homes, schools, and parks. The MTA cited a “business necessity” for its actions at a time when studies were documenting that the Harlem community was experiencing asthma at alarmingly
___________________
46 Title VI of the Civil Rights Act of 1964 (42 U.S.C. § 2000d to 2000d-7): “No person in the United States shall, on the ground of race, color, or national origin, be excluded from participation in, be denied the benefits of, or be subjected to discrimination under any program or activity receiving Federal financial assistance” (GPO, 2010).
higher rates (Corburn et al., 2006; Nicholas et al., 2005), as much as six times the rate of other Manhattan neighborhoods (Wakin, 2001).
From 1991 to 1992, WE ACT, as a member of the Coalition to Save St. Luke’s Hospital, worked with the NAACP Legal Defense Fund, which filed a Title VI complaint with the U.S. Department of Health and Human Services for unjustly transferring maternity and neonatal beds in an uptown hospital to a downtown hospital affiliate.47 The St. Luke’s catchment area includes two large public housing projects that depend on the hospital for health services. In 2004 WE ACT and the NRDC filed a lawsuit against the U.S. Environmental Protection Agency (EPA) for its rat poison standards, which had failed to protect the health of children (WE ACT, 2016d). In 2016 WE ACT and other advocates from across the country partnered with Earthjustice and filed a lawsuit against the EPA for failing to update standards that protect families and their children against neurotoxic lead-based paint and lead dust, which many studies have shown can irreparably hinder children’s learning ability and reduce their IQ (Bellinger, 2008; Needleman et al., 1990).
Solutions to Address the Social Determinants of Health
WE ACT works to build healthier communities by prioritizing identified healthy community indicators: air quality; open and green space; food justice; climate justice; toxic-free products; transportation; waste, pests, and pesticides; land use; and healthy indoor environments. The organization uses community organizing and training, community-based participatory research (CBPR), advocacy, and an empowered grassroots membership base to achieve its goals.
Physical environment WE ACT’s work to improve the physical environmental focuses on improving the built environment, advocating for climate justice, and promoting toxic-free products.
Built environment WE ACT helped to create the West Harlem Piers Park (see Figure 5-26), which transformed a former 69,000-square-foot parking lot into a 105,526-square-foot park, redeveloping the Harlem waterfront to increase options for active living for uptown families. The park opened in 2009 after a decade of community organizing and planning that produced a community-driven plan developed by WE ACT and Manhattan Community Board 9 in partnership with more than 200
___________________
47 Personal communication with WE ACT staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu).

SOURCE: Personal communication with WE ACT staff. Available by request from the National Academies of Sciences, Engineering, and Medicine’s Public Access Records Office (PARO@nas.edu). Used with permission.
residents, representatives from the New York City Department of Parks and Recreation, and local elected officials. In 1999 the community-driven plan was submitted to the New York City Economic Development Corporation, which set aside a variety of commercial development proposals in favor of advancing the community-driven plan to a master plan for the waterfront park and the surrounding neighborhood.
Building on the success of the community-planning process for the Harlem Piers waterfront park, which encourages active living, WE ACT organized a 40-group Northern Manhattan Environmental Justice Coalition in a campaign known as Fair Share, not Lion’s Share. The campaign achieved the decommissioning of the 135th Street marine transfer station (MTS), which resulted in an MTS being rebuilt in the affluent upper eastside of Manhattan. Under former Mayor Bloomberg’s solid waste plan, each borough needed to be self-sufficient and provide for its own waste in order to reduce truck trips through overburdened communities of color and low income in Brooklyn and the South Bronx, where waste transfer stations proliferate. Mayor Bloomberg agreed in 2007 that WE ACT and Community Board 9 could organize community stakeholders to develop
a community-driven plan for redeveloping the former MTS located on the Hudson River next to the new Harlem Piers waterfront park. These efforts created the From Trash to Treasure campaign, which has engaged residents to collaboratively develop a plan for the redevelopment of the 28,000-square-foot MTS. The closure of the MTS eliminated 200 to 300 trucks driving through the community to the MTS, which was operating 24 hours daily.
In response to Columbia University’s plan to develop a satellite campus in the Manhattanville section of West Harlem, between 2005 and 2012 WE ACT and the West Harlem community, acting with Community Board 9, coalesced to hold the university accountable for its land use process that threatened to restrict community access and spur gentrification and displacement. WE ACT developed environmental recommendations to ensure that construction trucks used diesel retrofits and that buildings would be constructed to comply with Leadership in Energy and Environmental Design (LEED) standards. WE ACT partnered with Fordham Law School’s Community Development Law Clinic, which produced legal research on land use and zoning and assisted community residents in developing their testimony for hearings on the environmental impact statement and the city’s Uniform Land Use Review Process, which required city council approval. WE ACT’s Deputy Director Cecil CorbinMark was a lead community negotiator acting to hold the university accountable for providing a community benefits agreement (CBA) of $150 million, with another $150 million provided by the city to relocate two buildings of tenants and to preserve affordable housing. The West Harlem Development Corporation administers the CBA and grants funds to West Harlem groups for projects that improve community health, job training, small business, and arts and culture.
Climate justice With a $100,000 grant from the Kresge Foundation, WE ACT engaged its members and 400 residents from four neighborhoods across northern Manhattan in a series of public workshops in 2015 and developed the Northern Manhattan Climate Action Plan. The plan focuses on energy security, emergency preparedness, and social hubs and emphasizes coordination by community members through bimonthly working groups which advance policy initiatives such as development of microgrids and solar installations for affordable multifamily housing. Other stakeholders who contributed to the development of the plan include academic partners at Columbia University’s Mailman School of Public Health and the Icahn School of Medicine at Mount Sinai, the New York City Mayor’s Office of Resilience and Recovery, elected officials, and consultant Dr. Michael McDonald of the Global Health Response and Resilience Alliance. The implementation strategy identified policy
initiatives necessary to achieve the plan with a 3-year Kresge Foundation grant of $660,000.
In 2008 WE ACT organized the Environmental Justice Leadership Forum on Climate Change, a national coalition of 42 environmental justice organizations across 20 states. The forum publishes a Clean Power Plan Tool Kit,48 which provides guidance for state agencies and stakeholders to conduct civil rights and environmental justice analyses and meaningful engagement with vulnerable communities in planning for and implementing the federal Clean Power Plan rule. Incorporating equity, health, data, and meaningful engagement are key elements of the planning process. The tool kit report published by the forum summarizes the environmental justice analysis under Title VI of the 1964 Civil Rights Act in this way:
- Describe what you plan to do.
- Consider the benefits and burdens for all communities.
- Consider the alternatives.
- Include people of color and low income in the decision-making process.
- Implement a plan to distribute benefits and burdens equitably and avoid discrimination.49
Currently, the forum is working with a consultant to develop an environmental justice analysis for states to guide their development of their state implementation plans.
Nontoxic products In response to growing evidence of the human health effects of harmful chemicals and pesticides, WE ACT worked with the New York Public Interest Research Group (NYPIRG) in 2005 to encourage the New York City Council to pass two bills that were aimed at reducing exposures to toxic chemicals contained in pesticides. Armed with findings from a collaborative 18-year research project of the Columbia Center for Children’s Environmental Health (CCCEH) that has documented the exposure to banned pesticides of 720 mothers and newborns in northern Manhattan and the South Bronx, WE ACT and NYPIRG worked with members of the New York City Council to introduce bills requiring notification of neighbors when pesticides are applied and requiring a
___________________
48 The Clean Power Plan Tool Kit is available at http://www.ejleadershipforum.org/clean-power-plan-tool-kit (accessed December 5, 2016).
49 See page 28 of the Forum’s Environmental Justice State Guidance: How to Incorporate Equity & Justice into Your State Clean Power Planning Approach, available at http://www.ejleadershipforum.org/wp-content/uploads/2016/01/EJ-State-Guidance-updated-March-7.pdf (accessed December 5, 2016).
reduction and elimination in the use of the worst toxic pesticides in New York City’s stockpile. Both bills were passed by the council and signed into law in 2005.
Beginning in 2006 and continuing to the present, WE ACT and Clean and Healthy New York have served as coleaders of the Just Green Partnership, a statewide coalition of environmental, environmental justice, public health, health-affected, labor, and sustainable business advocates who have led the fight in New York to protect children and families from harmful toxic chemicals in many products used daily. In 2010 the U.S. Food and Drug Administration ruled that it could no longer declare that bisphenol A (BPA) was safe. WE ACT and Clean and Healthy New York worked with allies in the Just Green Partnership to implement a ban on BPA in children’s products—including pacifiers, unfilled bottles, and sippy cups—and allowed for BPA-free products to be labeled as such. WE ACT engaged residents of northern Manhattan in signing petitions and postcards urging leaders of the New York State Assembly, Senate, and governor to protect New York’s children from the harmful effects of BPA. In 2010 New York passed a ban on BPA in products used by children ages 3 and younger. In 2012 WE ACT and Clean and Healthy New York worked as the leaders of the Just Green Partnership to ban TCEP, a toxic flame retardant chemical, in children’s products. Using findings from research conducted by CCCEH, WE ACT again engaged its members and northern Manhattan residents in pushing for a change in the law that would better protect their children. At the end of the legislative session in 2012 and with bipartisan support, Governor Cuomo signed into law a bill requiring that TCEP be banned in children’s products in New York.
In 2015, in partnership with the Just Transition Alliance and the Connecticut Coalition for Environmental Justice, WE ACT created a public awareness and education campaign to gain support from the congressional Black and Hispanic caucuses, subcommittees, and other agencies and offices to back the Safer Chemicals, Healthy Families campaign. The campaign advocated for the reform of the Toxic Substances Control Act of 1976, an outdated national law regulating chemical safety that had allowed approximately 82,000 potentially unsafe chemicals to remain in use in the United States. The act was amended in 2016 by the Frank R. Lautenberg Chemical Safety for the 21st Century Act, which mandates safety reviews of chemicals currently in use as well as new chemicals not yet on the market and includes some protections for vulnerable communities.
Transportation In 1997 WE ACT launched its Dump Dirty Diesel campaign to promote public awareness among community residents of the high levels of pollution in many neighborhoods of northern Manhattan due to the toxic diesel exhaust fumes being released by MTA buses and
the elevated risks of respiratory problems, chronic disease, premature mortality, and negative effects on birth outcomes caused by this pollution. The goal of the campaign was to encourage the MTA to renovate its diesel bus depots and invest in buses running on clean sources of energy. In 2000 WE ACT filed a Title VI complaint against the MTA for continuing to invest in diesel buses. As a result of the complaint, the U.S. Department of Transportation mandated that the MTA uphold civil rights law and take environmental concerns into consideration in its future decision making. In 2008 WE ACT, along with the MTA and a community task force, began holding community planning sessions to transform the Mother Clara Hale bus depot to comply with LEED standards. Since then, WE ACT has been successful in pushing the MTA to transform its entire city bus fleet to hybrids and compressed natural gas buses.
In 2011 WE ACT partnered with UPROSE (a Brooklyn-based nonprofit that promotes healthy and resilient communities through environmental, climate, and youth justice), Empire State Future (a coalition of organizations in upstate New York that encourages sustainable and equitable economic growth), and the Tri-State Transportation Campaign (a nonprofit working to reduce dependency on cars in New York, New Jersey, and Connecticut) to create the New York State Transportation Equity Alliance (NYSTEA), a statewide coalition of more than 50 organizations. The coalition’s goal was to help build a more affordable and equitable transportation system in New York, providing improved public transportation options to residents without cars and addressing negative environmental health effects. As a result of the advocacy of NYSTEA and others, the 2014–2015 New York State budget included the first increases for public transit both upstate and downstate in many years. In 2014 WE ACT also established a Transit Riders Action Committee (TRAC) which has organized residents to campaign against unjust transit fare increases and closings of public transit options and to advocate for civil rights protection in transportation policy making (WE ACT, 2016b). The efforts of WE ACT’s TRAC resulted in bus rapid transit service across 125th Street, a congested east-west commercial corridor, and faster bus service for hundreds of Harlem residents to access the job center that is LaGuardia Airport located in the borough of Queens.
Housing In 2014 WE ACT began implementing its Healthy Homes Campaign with the goal of improving health, safety, and quality of life among residents of color and low income in New York City. The project has three objectives: (1) mobilize and build a campaign power base, consisting of members, environment and housing advocates, scientists, policy advocates, government agencies, community-based organizations, and people with health conditions related to poor indoor environmental conditions, in order to identify and marshal efforts to close gaps in housing policies
and codes that violate the warranty of habitability50 and expose vulnerable tenants to environmental toxins and hazards; (2) develop campaign communication strategies that effectively position the campaign for high public visibility and legislative attention and action; and (3) advance effective New York City housing policies that address current housing, building code, and enforcement gaps; protect public health; and reduce harmful indoor environmental exposures. Since launching the campaign, WE ACT has worked to secure citywide healthy housing legislative and regulatory policies aimed at improving health outcomes in multifamily affordable housing by partnering with allies from a broad cross-section of social justice advocacy, housing, government, research, and green building sectors in a collaborative campaign that uses mobilization, convening, and communications strategies to educate city officials to support the Asthma-Free Homes bill pending at the New York City Council—a bill that would require landlords to fix housing violations that affect asthmatic tenants.
Health systems and services WE ACT currently works to improve the methods and practices by which three Harlem-based hospitals engage vulnerable communities in their catchment areas to achieve community health needs assessments and community benefits processes under the Patient Protection and Affordable Care Act. WE ACT aims to identify specific ways that the hospitals can engage with populations in their catchment area, identify community health needs, and determine the exact scope and type of community benefits they could provide in response to community health needs. WE ACT will produce a report that serves as a resource for advocates, policy makers, and hospital leaders seeking to strengthen the impact that hospitals have on the health and well-being of the populations they serve by providing in-depth analyses of the existing community benefits processes and deliverables as well as specific recommendations for improving existing community services based on robust local engagement with a broad cross-section of stakeholders.
Data and Outcomes
WE ACT’s theory of change, including key short-term, intermediate, and long-term outcomes that the organization hopes to achieve, is illustrated in Figure 5-27.
___________________
50 “Most jurisdictions read residential leases to include an implied warranty of habitability. This warranty requires landlords to keep their property ‘habitable,’ even if the lease does specifically require them to make repairs. Furthermore, the warranty conditions a tenant’s duty to pay rent on the landlord’s duty to maintain a habitable living space” (LII, n.d.).
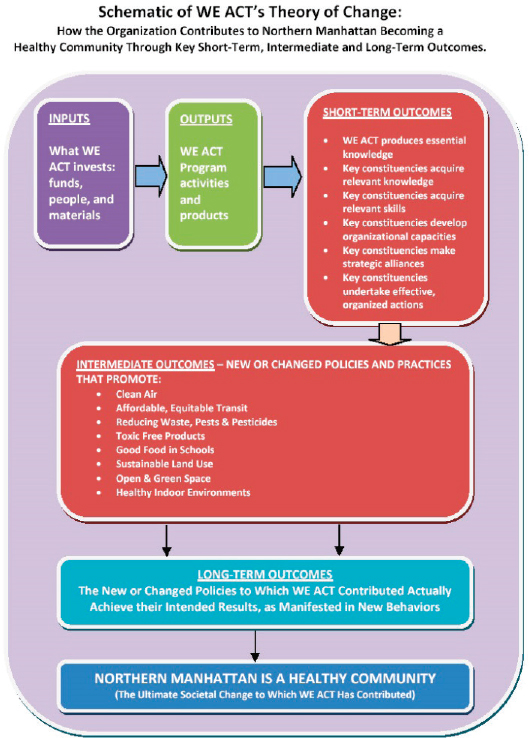
SOURCE: WE ACT, n.d. Used with permission.
WE ACT partners with academic institutions to conduct CBPR and uses data as evidence to drive its campaigns. To demonstrate the effects of air pollutants, harmful chemicals, and pesticides on children’s health and birth outcomes and to advocate for policy changes to improve these outcomes, WE ACT has collected data on air quality by producing maps showing sources of pollution overlaid with health and income data. WE ACT’s data-driven advocacy efforts have led to new policies and legislative reform on issues related to air quality monitoring and the use of harmful compounds such as BPA and phthalates in consumer products, pesticides, and flame retardants.
Promoting Health Equity: Key Elements
WE ACT’s work is based on the concerns of residents and members and driven by community efforts, including community organizing, community planning sessions, town halls, and public meetings between residents and elected officials. All steps in the development and implementation process for each of its initiatives are undertaken with meaningful community engagement, ensuring that the concerns and priorities of residents are the drivers of WE ACT’s work. WE ACT engages partners from a range of sectors, including environmental health, land use and management, transportation, public health, energy, environmental health scientists and practitioners, and the legal system. Partners have included academic institutions, housing groups, law schools, solar energy providers, government agencies, and community-based participatory researchers.
WE ACT has partnered extensively with educational institutions to conduct research and collect data for its advocacy work. Its North River Sewage Treatment Plant complaint was submitted after conducting a CBPR project to determine whether high levels of pollution were to blame for the high rates of asthma among the community’s children, a majority of whom were African American or Latino. With funding from the National Institute of Environmental Health Sciences (NIEHS), WE ACT and CCCEH collaborated to train 17 WE ACT interns to collect data on air quality in the uptown area. The collaborative research effort found unsafe levels of diesel particulates, results that were similar to those of the EPA’s subsequent data collection (Minkler, 2010). WE ACT currently partners with the NIEHS Center for Environmental Health in Northern Manhattan (CEHNM)—which conducts research on the role that environmental pollution plays in the development of neurodegenerative diseases, respiratory diseases, and cancers with environmental risk factors—and CCCEH, both of them located at Columbia University’s Mailman School of Public Health. As cochair of CEHNM’s Community Outreach and Translation Core and a coprincipal investigator of CCCEH’s Community Outreach Education Core, WE ACT disseminates the centers’ research findings to community residents and organizations, health care providers, policy makers, and public interest groups. It organizes community conferences and policy briefings among its researchers, community residents and partners, and policy makers to inform and advocate for safer environmental health policies to protect and improve the health of low-income residents of color. For the past 18 years, WE ACT has had subcontracts with both research centers to carry out this work. CEHNM also provides $25,000 pilot grants to researchers and community partners to study air quality and other neighborhood concerns that affect environmental health. Partners at the research centers have also cooperated to apply for National
Institutes of Health grants (when WE ACT is ineligible to do so) that serve community concerns, such as understanding the impact of social cohesion on outcomes of public housing tenants affected by Hurricane Sandy. WE ACT has partnered with the University of Pittsburgh School of Public Health to study the cumulative effects of stress and air pollution on asthma throughout the five boroughs of New York City; with Montefiore Hospital to research effective methods for training parents on reducing exposure to indoor sources of lead; and with the Icahn School of Medicine at Mount Sinai to study the effects of climate change on children in northern Manhattan.
WE ACT has worked with elected officials and policy makers at the local, state, and national levels. Through its Kellogg Foundation–funded project, Establishing Health Resilience for Vulnerable Asthmatic Children, WE ACT works with partners in Louisiana, Michigan, Mississippi, and New York to strengthen the efficacy of federal strategies to reduce asthma disparities among vulnerable children by assessing the performance of strategies and mobilizing communities to advocate for needed reform. Specifically, the project seeks to understand how the four strategies identified in the Coordinated Federal Action Plan to Reduce Racial and Ethnic Asthma Disparities51 have performed with regard to disparities among children in these communities between the ages of 0 and 8, given how critical these years are in a child’s development. In 2017 WE ACT will disseminate a report on its findings and recommendations for how to improve these strategies. WE ACT has also hosted forums for candidates to speak on environmental justice issues and has trained residents to testify at city council hearings. It has mobilized residents to lobby with state legislators and, through its office in Washington, DC, galvanized residents to advocate for national policy change and legislative reform. WE ACT has also built support for national and global environmental justice movements and has taken on a leadership role in convening environmental justice organizations on climate issues.
WE ACT builds capacity by providing residents with opportunities to develop their leadership skills. In keeping with its theory of change (see Figure 5-27), the organization provides leadership training to community members through its Environmental Health and Justice Leadership Training (EHJLT) program, an 11-week course that educates participants about the issues confronting their northern Manhattan neighborhoods. Upon graduating, the class participants understand the impact of a range of environmental health issues and are ready to address them by taking a leadership role in organizing WE ACT’s membership on related
___________________
51 Available at https://www.epa.gov/asthma/coordinated-federal-action-plan-reduce-racial-and-ethnic-asthma-disparities (accessed October 27, 2016).
campaigns. The EHJLT training program has been adapted to train 60 high school students over 1 week in the predominately Latino Washington Heights Expeditionary Learning School. WE ACT is adapting its leadership training model with community-based organizations and high school students through a partnership with the University of North Carolina’s Center for Environmental Health, Columbia University’s Community Outreach and Engagement Core, and Harvard University’s School of Public Health. The Climate Change and Health Fellows program will foster climate literacy among health professionals as well as high school students.
Challenges and Lessons Learned
As with many other environmental justice organizations, WE ACT has faced challenges in securing funding for its operations. These challenges have served as important opportunities for learning and growth. Funding for community organizing is often difficult to secure, as funders may not fully understand the costs associated with building a base of support for developing and implementing policy initiatives and mobilizing residents to vote, educate, and hold their elected officials accountable. A number of studies, including one by Dr. Daniel Faber at Northeastern University, document that environmental justice organizations receive half of 1 percent of all environmental funding nationally (Faber, 2001). Philanthropy has reported that environmental justice organizations comprise only 2 of the top 20 organizations receiving the small amount of environmental justice funding available (Environmental Grantmakers Association, 2015). Other philanthropy associations report that organizations led by directors of color receive even less funding from foundations (The Greenling Institute, 2006).
Strong grantsmanship has been essential for obtaining multiyear funding. Much of WE ACT’s funding comes from larger foundations and federal grants. Securing funding from individual donors has proven to be particularly challenging, which can be problematic because donors often provide significant funding for general operations, including rent, administrative and fundraising staff, accounting, technological upgrades, and other elements that are critical to an organization’s long-term success. Strong communications and public messaging that bolster the successes of an organization are critical to securing long-term sources of funding. Effective evaluation is also critical. WE ACT includes funding for evaluation consultants in proposals whenever possible and ensures that its staff members receive training in assessing outcomes and project effectiveness.
WE ACT designs its projects through a logic model process to help ensure that positive outcomes are achieved and objectives are met.
Sustaining Success
Vision, strategic planning, and developing a theory of change have been critical to planning the organization’s future direction and identifying the methods and resources necessary to achieve WE ACT’s objectives. Examples include the development of a federal policy office in Washington, DC, strategizing to develop a state legislative presence and exploring development as a 501(c)(4) organization. WE ACT has also sustained its success through strong membership development. Funding for a membership and organizing director took at least 5 years to secure, but in 2 years WE ACT’s organizing team strategically recruited about 400 members who have been engaged in and provide leadership to the organization’s campaigns. An emphasis on community-based planning has also helped to sustain success, engaging residents in visible and viable land use projects that improve community sustainability and public health. Community-based planning has improved social cohesion and created community consensus around projects that would be controversial if handled by city officials without resident input. Partnerships with academic institutions have provided critical data and findings for WE ACT’s evidence-based campaigns and helped to increase the organization’s visibility and credibility among policy makers and the media. Effective staff members are also essential for sustaining success by boosting confidence in the organization from policy makers and philanthropy and creating goodwill in the community.
Key elements that have facilitated WE ACT’s success are its achievement of trust and a shared vision with the northern Manhattan neighborhoods plus a strong engagement with environmental justice organizations around the country. With strong partnerships with other nonprofits and academic institutions with similar goals, the organization has consistently sought outcomes that are beneficial for all stakeholders. WE ACT’s activities have been informed by principles of collaboration developed by academic partners who engage in community efforts as well as formal processes such as the protocol for assessing community excellence developed by the National Association of County and City Health Officials. WE ACT has incorporated these principles and protocols in its work, but it has most successfully sustained its ties to the community through a commitment to resident solidarity over its decades of work. WE ACT has built high levels of trust that have sustained partnerships even after grant periods have ended and thus has created opportunities for ongoing collaboration.
SUMMARY OF CHALLENGES
As evidenced by the case examples discussed in this chapter, the barriers that organizations face in promoting health equity vary from larger contextual issues to more specific programmatic issues. For example, DHC struggles to overcome the challenges of patients who are left in the insurance coverage gap, and EPN works to keep communication systems effective to ensure that residents are aware of the resources made available to them. Also outside of the control of the community organizations highlighted in the chapter are the inevitable changes in political administrations, which can have implications for funding and political will. Another barrier that emerged from the community examples was the challenge of getting community residents to invest their time and energy into upstream factors and more long-term benefits, as compared to immediate needs. DSNI struggles with this, as many of the community residents are preoccupied with satisfying basic needs, such as shelter and food. Just as communities will require individualized approaches to solutions, responses to overcoming barriers should also be tailored to the strengths and needs of the community. The next section discusses how some of the challenges faced by the communities were addressed and other key components that made these communities successful.
SUMMARY OF KEY ELEMENTS, LEVERS, POLICIES, AND STAKEHOLDERS
Chapter 4 discusses the need to build the structures necessary to strengthen community solutions by undertaking systematic efforts to learn from both the successes and the failures in the strategies, initiatives, and other efforts currently under way and being developed. Although reviewing just nine examples does not constitute a systematic review, the communities described in this chapter make it clear that it is possible to act effectively at the community level to modify social determinants of health that may, in turn, reduce health disparities and promote health equity.
All of the nine community examples highlight the three key elements of effective community change from the committee’s central figure: equity as a shared vision and value, increased community capacity, and enhanced multi-sectoral collaboration. Below, the committee addresses some of the ways these nine communities relied on the three key elements and applied a variety of elements, levers, and policies to achieve their desired outcomes.
Changing the Narrative
The most important, and perhaps least tangible, ingredient in all nine examples is the capacity to create a community vision in which residents will feel compelled to invest their time and energy. In a community where resources are scarce, jobs are few, money is tight, and parents cannot afford babysitters, getting started on community action for change may require great sacrifices and courage. Unless there is a belief that change is possible and that it might actually lead to a better quality of life, there will be no motivation for action. Creating a shared vision is the first and most essential task of leaders—a community needs to believe that people can change and that their circumstances can change. Without that willingness to hope for the possibility of change, nothing will get started. Dr. Jack Geiger, one of the early leaders of DHC, has argued that communities suffering from poverty, which are “all too often described only in terms of pathology, are in fact rich in potential and amply supplied with bright and creative people” (Geiger, 2002). This positive message is an example of how to inspire and engage.
Building Trust and Agency
A core element to changing the narrative and engaging the community in action is building trust and reciprocity among community residents and institutions. For many communities that face health inequity, divestment, land use and zoning policies, medical institutions, and other structural drivers have been a source of historical trauma and mistrust, and rightfully so. For DHC, overcoming historical mistrust has been achieved through ultimate transparency and a strong presence in community activities. In addition, over half of the board of directors must consist of current patients of the program. In the neighborhood of the DSNI, divestment had destructive effects on the social and economic environment. When the Riley Foundation first proposed its neighborhood revitalization plan to residents, it was met with discontent due to the lack of community representation. When the advisory group shifted power and ownership to the Dudley community members with a board that was majority residents, a community-driven agenda was established. This type of community power dynamic is reflected in many of the community examples and facilitates the building of trust between community institutions and residents. Trust among residents and other community stakeholders, in addition to the belief that change is possible, is essential for community actors to be empowered and develop agency. Interventions at the community level are uniquely positioned to empower community residents to seek change and galvanize communities to act.
Leadership
The Role of Leaders
In some, but not all, of the case examples, charismatic individuals united or mobilized a community and significant partners around a specific goal. Charismatic leaders can be extremely important in galvanizing change, but not every community may have such a person, at least initially. In some examples, leadership came from outside the community and helped build capacity within the community. This is the case with DHC. When DHC got started in the 1960s, many residents had not yet succeeded in overcoming infamous local barriers to voting. Local leaders took great risk in supporting the initiative, while local government and police were barriers, rather than supporters, of success. Today, DHC is community-owned, and its new generation of leadership and staff has strong community ties and effective partnerships with local government and other institutions. In this and other examples, an outside leader or leaders were successful because of a true partnership with a community, focusing on building capacity and empowerment.
The leaders in the nine examples differed widely in various ways, but they shared the ability to get the community working for change. By embarking on plans for change, leaders were sometimes able to secure relatively early victories, which led to more optimism and engagement. For example, an early protest march by leaders of WE ACT resulted in their arrest while blocking traffic. This arrest increased the visibility of the group and demonstrated its seriousness of purpose, which built community support and led to the group’s successful partnership to sue New York City for greater environmental justice.
Leaders need not only to create hope but also to unite the community in working toward common goals. For IndyCAN, leaders belong to a faith-based network. This is not the only type of partnership that can produce change, but it has significant advantages in working with those who are already closely knit together into coherent congregations and who unite around the importance of large social and spiritual goals. Across the United States, numerous PICO organizations have effectively mobilized faith-based groups for social change.
Leadership Development
For DSNI, a foundation approached a community with a fully formed plan for change, and the community rejected it as ill-suited to its needs. Both the philanthropy and the community were flexible and insightful enough to keep working together and for the community to build the leadership capacity that would make it possible to create its own
successful plan for change with the financial and other resources of the philanthropy in support. The responsivity and commitment of both parties, shown in the effort to continue working on the collaboration despite a setback, was vital to their success. MCI specifically set out through its Belong Campaign to build social connections, develop ties among neighbors, and create leaders. MCI fellowship is a built-in mechanism to develop the next generation of leaders. A few of the examples, including DHC, DSNI, and WE ACT, have persisted for decades. One factor that most likely contributed to the sustainability of these programs was that all focused explicitly on developing the next generation of leaders. DSNI created a Resident Development Institute. DHC set up educational programs for youth and assistance for those applying to college.
Building Diverse Network of Partners
All of these examples demonstrate the power of building an effective network, not just within the community but also with crucial additional partners who can support the community’s goals. The number of partners is less important than the ability to unite a group of partners who may have disparate skills and domains of expertise but who maintain a shared vision. Many of these examples show collaborative interventions across many sectors; these broad partnerships were crucial in affecting change within challenging domains, ranging from youth violence to local poverty and unemployment.
The Minneapolis Blueprint for Action to Prevent Youth Violence is a striking example of multi-sectoral collaboration to address youth violence. Leaders, including the mayor, city council, and local philanthropy, along with the community, addressed multiple contributing factors ranging from lack of education, lack of job training, little follow-up with youth who presented to local hospitals with violent injuries, and the failure to reintegrate youth who had experienced legal difficulties into the community. The initiative built platforms for youth success, including college scholarships and youth leadership opportunities. WE ACT has served as a model for many other environmental organizations by forging partnerships among groups that had not previously worked together or thought to do so. These partners include academic institutions, housing groups, clean energy providers, community-based participatory researchers, nonprofits from other domains, and government agencies.
Relationship Building and Mutual Accountability
In creating a network of diverse partners, the communities in the examples created a shared commitment to their goals among partners.
One challenge that arises from collaborative work across sectors and disciplines is the competing interests of the partners. The partnerships within EPN, Blueprint, and MCI are forged with the understanding that if collaboration is effective, co-benefits can be realized. This also creates a mechanism for mutual accountability for resources and outcomes.
Governance Processes
All of the example communities had very specific governing practices and structures that were tailored to the needs and makeup of the community being engaged. Among the communities that had a leadership board, substantial and accurate representation of the community residents was vital. Generally, the communities in the examples employ structured, bottom-up approaches to decision making. IndyCAN employs the local organizing committee leaders to facilitate dialogues with community members, and elected delegates vote on important issues of strategy, budget, and more. EPN also uses committees, which are specialized. MCI uses a more informal and less prescriptive leadership model, which allows partners within the network to take initiative on issues based on interest and on the amount of resources available at the time.
Fostering Creativity
Creativity is another common feature of these initiatives. EPN realized multiple benefits in the domains of exercise, student safety, and community cohesiveness without great expenditure by mobilizing the Walking School Bus. When children at DHC showed clear signs of malnourishment, health professionals actually wrote prescriptions for food and organized a community garden for 1,000 member families, bringing in sustainable and improved nutrition for the community. The DSNI managed to obtain the power of eminent domain over abandoned properties in order to acquire land for resident-led development. This creative strategy opened up vast resources for community projects.
Planning for Sustainability
Leveraging Resources
Sustainability, whether financial or management sustainability, is a major consideration for any community-based solution. DSNI enhanced its sustainability by leveraging its success over 30 years to obtain a Promise Neighborhood grant. Mandela MarketPlace has addressed a different aspect of sustainability, looking to job creation, enhancement of the
market for healthy food, and keeping wealth in the community. PUSH has also focused on creating jobs and job training, looking to maintain the initiative’s benefits over time.
Training and Technical Expertise
Another factor that shapes a community initiative’s sustainability, which many of the case examples capitalized on, is technical expertise and training. Educational institutions have emerged from the case examples as a valuable partner in this respect. WE ACT and IndyCAN partnered with education institutions for data collection and research, and DHC engaged students at local educational institutions to assist with the center’s community projects. In the case of Mandela MarketPlace, when community organizers recognized a need for technical expertise, they commissioned external consultants to provide assistance developing a business model. Others of the example organizations trained within the community to develop the expertise needed. The Blueprint Approved Institute serves this purpose, providing a platform for grassroots organizations to learn about government processes and have the capacity to compete for funds. Training residents in community tools for action and mobilization was another common element of the case examples (EPN, IndyCAN, and WE ACT).
CONCLUSION
These nine examples are markedly diverse, yet as a group they provide common positive features that can inspire other communities to embark on or improve their own programs for change. They also share the capacity to raise the hope that communities, including those faced with daunting issues, can unite to produce real and lasting benefits in health outcomes and numerous related factors. None of these initiatives is a blueprint that can be simply copied and implemented anew in a different community with different residents, different history, and different challenges. Yet these widely varying communities illustrate that there are many different pathways to success.
The three key elements in the conceptual model for this report call attention to building in three domains: shared vision and values, community capacity, and multi-sector collaboration. In each of the nine initiatives described above, innovative and far-reaching efforts in these three domains created change for the better, recognizing and enhancing the potential for improved lives in these vibrant neighborhoods. These initiatives looked at their community challenges from widely varying perspectives. Some sought to link partners through spiritual bonds, while others focused on tackling poverty through job programs and education.
All were savvy in building effective and powerful partnerships. Key community partners—including community groups; local, state, and federal governments; philanthropies; educational institutions; and key local employers—played a vital role in collaborating to develop, implement, and sustain effective community solutions.
With the exception of a few, the communities featured in this chapter did not approach the design and implementation of their solutions with the frame of improving health. Instead, their ultimate goals were safe and affordable housing, economic development and dignity, safety, social cohesion, educational achievement among youth, neighborhood revitalization, or environmental justice—all of which are ingredients for a healthy community and foundational to health equity. The committee acknowledges that underserved communities that are struggling with poverty, violence, or divestment are not likely to have health as a priority on their agendas for improvement. However, the experiences and lessons learned from these nine communities reveal an opportunity for communities to address the social, economic, and environmental factors that contribute to a thriving community as well as improving health. Applying a health equity lens to community-driven solutions allows for the interdisciplinary, collaborative approaches with access to diversified funding sources that the nine communities were able to adopt. This also facilitates the realization of co-benefits (i.e., win-wins) for actors across sectors within the community, and especially for community residents, who can reap the benefits across multiple domains.
All were prudent in seeking diversified funding and carefully allocating resources. Furthermore, all nine communities built capacity among residents to identify key issues and to participate in devising strategies to meet their needs and build on their assets while recognizing the power of systems and other forces outside the community to enhance or undermine the effectiveness of their efforts. Long-lasting initiatives demonstrate wisdom in adapting their strategies and seeking new funding as times change, and in buffering themselves from the inevitable changes in political administrations over time. Box 5-1 outlines some guiding principles that emerged from the committee’s review of the community examples and the existing literature on processes for community action to promote health equity.
Chapter 5 Annex
SELECTION PROCESS FOR COMMUNITY EXAMPLES
Identification
The committee identified potential examples through several avenues. Queries were sent to public health organizations such as the Association of State and Territorial Health Officials and the National Association and County and City Health Officials, philanthropies such as The California Endowment, and nonprofits, including Grantmakers in Health and the Prevention Institute. The committee also heard from many experts at its open meetings (see Appendix C for the meeting agendas) who presented many examples of community efforts to improve health and health equity in a range of sectors. Existing reviews of community efforts, reports on health disparities, healthy community websites, and other related publications were searched for relevant examples. Committee members also submitted examples from their respective fields. Finally, a literature review was undertaken.
Criteria
To guide the selection of the case examples for this report, the committee developed three sets of criteria (see Box 5-2 for a listing of all selection criteria). These criteria were informed by research and practice-based evidence as well as by the expertise of the committee. The first set consists of four core criteria, which must be met by all case examples. These core criteria assure that the examples chosen are substantively significant.
The first core criterion requires that the solution in the example addresses at least one (preferably more) of the nine social determinants of health identified by the committee: education, employment, health systems and services, housing, income and wealth, the physical environment, public safety, the social environment, and transportation. This criterion was informed by the wealth of literature suggesting the importance of targeting the social and economic conditions that affect health, especially at the community level (Bradley et al., 2016; Galea et al., 2011; Heiman and Artiga, 2015; Hood et al., 2016; Wenger, 2012). Furthermore, this criterion is basic to the committee’s charge, which posits that the social determinants of health must be addressed to reduce health inequities.
The second core criterion states that each case example must be community driven. This requires that the solution is initiated by a community member, group, or local government or that prior engagement with the community is evident and subsequently incorporated into the solution.
The community-driven element is significant because it highlights the distinction between solutions that are enacted on behalf of communities and placed in communities versus solutions in which the community is the driving force behind them (IOM, 2012). It is also important to note that the populations affected by health inequity are historically marginalized and underserved groups (Dicent Taillepierre et al., 2016). Community-driven solutions build the capacity and power for these marginalized groups to play a role in shaping their outcomes, which is especially noteworthy for groups that may be distrustful of governmental or medical institutions.
The third core criterion states that the solution must be multi-sectoral, meaning that it engages one or more sectors in addition to a traditional health sector (e.g., public health, health care, etc.). This criterion was drawn from the body of literature citing multi-sector collaboration as a powerful lever for addressing the social determinants of health and building a culture of health (APHA, 2015; Danaher, 2011; Davis et al., 2016; Kottke et al., 2016; Mattessich and Rausch, 2014). Multi-sector collaboration also has implications for the sustainability of the community-driven solutions, which traditionally have been under-resourced. Engaging stakeholders across multiple sectors provides the opportunity for innovative and cost-effective methods to sustain solutions at the community level.
The fourth core criterion requires the solution to be evidence-informed. This entails an assessment of evidence or the best available information to identify a problem and develop a solution that has a measurable outcome. Here, there is considerable flexibility in terms of the type of evidence that will qualify. This flexibility is based on the understanding that low-resource communities that suffer from health inequities often do not have the infrastructure, personnel, or financial resources to provide the highest standard of evidence.
The second set of criteria reflects the elements, processes, and outcomes of community-driven solutions that the committee identified as valuable for promoting health equity. These are not core criteria, in which case an example would be excluded if it did not meet one of them. Rather, they make up a set of aspirational criteria to inform the committee’s selection of the cases. This set of criteria highlights important features of community-driven solutions, such as nontraditional partners or non-health domains (e.g., community organizers, public libraries, PTA groups, etc.) and interdisciplinary or multifactor in nature. This comes from the committee’s understanding that engaging community stakeholders outside of the traditional health disciplines will facilitate cross-sector collaboration in addition to maximizing the impact on the social determinants of health. Such partnerships can increase reach and capacity by drawing on different backgrounds, skill sets, and knowledge bases (HHS, 2014).
For the examples to serve as a vehicle for sharing successful community-driven solutions with other communities affected by health inequities, the committee determined that there should be transferable key elements. All of the examples will be context dependent, and therefore they will not be replicable per se—that is, implemented in identical form. That being said, the key elements are the functions, principles, and activities of the solution that are necessary to achieve similar outcomes. They could practically be applied or adapted to similar contexts in order to scale impact (Schorr, 2016).
The criteria require that solutions illustrated in the examples will have documented their objectives, why those objectives are important, and how the solutions are expected to achieve the desired outcomes. Ideally they will have also thoroughly documented the implementation process so as to identify the key elements and subtleties of how the solutions contribute to success. This includes other significant contextual information such as the particular practice (training and supervisory), funding, regulatory context, and political context of the solutions. Furthermore, a plan for sustainability is outlined as a criterion for the community examples. To ensure sustained impact, the solutions should consider: long-term strategy and structure; funding, operating costs, and other resources; efficient use of resources; potential cost-savings or return on investment; and increased community capacity to shape outcomes.
The third set of criteria was developed to increase the likelihood that the examples will reflect a diversity of communities, populations, solutions, and other demographic characteristics representative of the United States, in addition to the characteristics of the solution itself. As a group the sample of examples should provide some variety in geographic regions and urban–rural classification. The committee also searched for examples that differ across the following population characteristics: race, ethnicity, age, gender identity, sexual orientation status, socioeconomic status, disability status, and other statuses applicable to health inequities. Finally, this set of criteria ensures the inclusion of solutions that integrate civil rights concerns; require changes in the systems, policies, or laws within which the solution was implemented; have various levels of political engagement (e.g., local, state, national); and result in a range of capacities developed within the community.
REFERENCES
Alameda County Public Health Department. 2008. Life and death from unnatural causes: Health and social inequity in Alameda County. Alameda County Public Health Department Community Assessment, Planning, and Evaluation (CAPE) Unit. http://www.acphd.org/data-reports/reports-by-topic/social-and-health-equity/life-and-death-from-unnatural-causes.aspx (accessed October 6, 2016).
Alameda County Public Health Department. 2014. Alameda County health data profile, 2014: Community health status assessment for public health accreditation. Alameda County Public Health Department Community Assessment, Planning, and Education (CAPE) Unit and Division of Communicable Disease Control and Prevention.
Alameda County Public Health Department. 2015 (unpublished). West Oakland race and ethnicity 1940-2015 summary.
APHA (American Public Health Association). 2015. Opportunities for health collaboration: Leveraging community development investments to improve health in low-income neighborhoods. Washington, DC: American Public Health Association.
B Lab. n.d. What are B Corps?https://www.bcorporation.net/what-are-b-corps (accessed October 27, 2016).
Bartley, A. 2016. Green Development Zone. https://www.changemakers.com/sustainableurbanhousing/entries/green-development-zone (accessed September 26, 2016).
Bellinger, D. C. 2008. Very low lead exposures and children’s neurodevelopment. Current Opinion in Pediatrics 20(2):172–177.
Bhatt, K., and S. Dubb. 2015. Educate and empower: Tools for building community wealth. Democracy Collaborative.
BLS (U.S. Bureau of Labor Statistics). 2016. Local area unemployment statistics. http://www.bls.gov/web/metro/laulrgma.htm (accessed November 23, 2016).
Blueprint for Action. 2013. Minneapolis Blueprint for Action to Prevent Youth Violence. Minneapolis, MN: City of Minneapolis Health Department.
Boston Promise Initiative. 2016. No Child Goes Homeless. http://www.promiseboston.org/no-child-goes-homeless.html (accessed September 26, 2016).
Bowie, P. 2011. Getting to scale: The elusive goal. Seattle, WA: Casey Family Programs.
Boyer, M. A. 2013. Green housing: In Buffalo, it’s not just for rich people anymore. Yes! Magazine, February 15.
Bradley, E. H., M. Canavan, E. Rogan, K. Talbert-Slagle, C. Ndumele, L. Taylor, and L. A. Curry. 2016. Variation in health outcomes: The role of spending on social services, public health, and health care, 2000-09. Health Affairs 35(5):760–768.
Chakrabarti, T. 2016a. Growing resources for healthy economies in Alameda County, California. http://nccd.cdc.gov/dchsuccessstories (accessed September 20, 2016).
Chakrabarti, T. 2016b. A high profile for healthy economies. http://nccd.cdc.gov/dchsuccessstories (accessed September 20, 2016).
Cho, S., K. Li, and T. Salzman. 2016. Building a livable Boston: The case for community land trusts. Medford, MA: Tufts University.
City-Data.com. 2016a. Harlem neighborhood in New York, New York (NY), 10030, 10039, 10027, 10026, 10029, 10035, 10037 detailed profile. http://www.city-data.com/neighborhood/Harlem-New-York-NY.html (accessed October 17, 2016).
City-Data.com. 2016b. West Oakland neighborhood in Oakland, California (CA), 94607, 94608 detailed profile. http://www.city-data.com/neighborhood/West-Oakland-Oakland-CA.html (accessed September 26, 2016).
City of Minneapolis. 2016. Results Minneapolis (forthcoming). Minneapolis, MN.
Community Tool Box. 2016. Chapter 1. Section 7. Working together for healthier communities: A framework for collaboration among community partnership, support organizations, and funders. http://ctb.ku.edu/en/table-of-contents/overview/model-for-community-change-and-improvement/framework-for-collaboration/main (accessed October 18, 2016).
Corburn, J., J. Osleeb, and M. Porter. 2006. Urban asthma and the neighbourhood environment in New York City. Health & Place 12(2):167–179.
County Health Rankings. 2016a. Bolivar County snapshot. http://www.countyhealthrankings.org/app/mississippi/2016/rankings/bolivar/county/outcomes/1/snapshot (accessed October 12, 2016).
County Health Rankings. 2016b. Marion County snapshot. http://www.countyhealthrankings.org/app/indiana/2016/rankings/marion/county/outcomes/overall/snapshot (accessed September 14, 2016).
Danaher, A. 2011. Reducing health inequities: Enablers and barriers to inter-sectoral collaboration. Wellesley Institute 3.
Davis, R., S. Savannah, M. Harding, A. Macaysa, and L. F. Parks. 2016. Countering the production of inequities: An emerging systems framework to achieve an equitable culture of health. Oakland, CA: Prevention Institute.
DHC (Delta Health Center). 2015. 2015 Mississippi Delta alternative spring break, Mississippi State University. http://www.deltahealthcenter.org/2015-mississippi-delta-alternative-break-mississippi-state-university (accessed September 19, 2016).
Dicent Taillepierre, J. C., L. Liburd, A. O’Connor, J. Valentine, K. Bouye, D. H. McCree, T. Chapel, and R. Hahn. 2016. Toward achieving health equity: Emerging evidence and program practice. Journal of Public Health Management and Practice 22 (Suppl 1):S43–S49.
Drennon, C. 2011. San Antonio’s Eastside Proimise Zone: A neighborhood profile. Trinity University Urban Studies Program.
DSNI (Dudley Street Neighborhood Initiative). 2016a. About the neighborhood. http://www.dsni.org/about-the-neighborhood (accessed September 26, 2016).
DSNI. 2016b. Board of directors. http://www.dsni.org/new-page (accessed September 26, 2016).
DSNI. 2016c. History. http://www.dsni.org/dsni-historic-timeline (accessed September 26, 2016).
DSNI. 2016d. Home. http://www.dsni.org (accessed September 26, 2016).
DSNI. 2016e. Sustainable economic development. http://www.dsni.org/sustainable-economic-development (accessed September 22, 2016).
Dudley Neighbors, Inc. 2016. Dudley Neighbors Incorporated: The community land trust. http://www.dudleyneighbors.org (accessed September 26, 2016).
Dwyer, L. A. 2015. Mapping impact: An analysis of the dudley street neighborhood initiative land trust. Cambridge, MA: MIT Department of Urban Studies & Planning.
ED (U.S. Department of Education). 2016. Promise neighborhoods. http://www2.ed.gov/programs/promiseneighborhoods/index.html (accessed September 26, 2016).
Environmental Grantmakers Association. 2015. Tracking the field: Volume 5: Analyzing trends in environmental grantmaking.
EPN (Eastside Promise Neighborhood). 2013. Cradle-to-career pathway. http://eastsidepromise.org/wp-content/uploads/2013/03/Cradle-to-Career-Pathway-e1363974021347.png (accessed September 19, 2016).
EPN. 2016a. The 10 promises. http://eastsidepromise.org/the-results (accessed September 22, 2016).
EPN. 2016b. EPN schools. http://eastsidepromise.org/epn-schools (accessed September 22, 2016).
EPN. 2016c. Mission statement. http://eastsidepromise.org/mission-statement (accessed September 26, 2016).
EPN. n.d. Success in education from cradle to career. http://eastsidepromise.org/k-12-pipeline (accessed September 19, 2016).
Faber, D. R. 2001. Green of another color: Building effective partnerships between foundations and the environmental justice movement. Northeastern University Philanthropy and Environmental Justice Research Project.
Fairmont Cultural Corridor. 2016. Fairmont Cultural Corridor: Creating vibrant communities with arts and artists at the center. http://www.fairmountculturalcorridor.org/history (accessed September 26, 2016).
FRAC (Food Research and Action Center). 2005. Food stamp access in urban America: A city-by-city snapshot. Food Research and Action Center. http://frac.org/wp-content/uploads/2009/09/cities2005.pdf (accessed October 6, 2016).
FSG (Foundation Strategy Group). 2011. Collective impact. http://www.fsg.org/ideas-in-action/collective-impact (accessed October 18, 2016).
FSG. 2013. Using collective impact in a public health context: Introduction. http://www.fsg.org/blog/using-collective-impact-public-health-context-introduction (accessed October 18, 2016).
Galea, S., M. Tracy, K. J. Hoggat, C. DiMaggio, and A. Karpati. 2011. Estimated deaths attributable to social factors in the United States. American Journal of Public Health 101(8):1456–1465.
Garfield, R., and A. Damico. 2016. The coverage gap: Uninsured poor adults in states that do not expand Medicaid—an update. Menlo Park, CA: The Henry J. Kaiser Family Foundation
Geiger, H. J. 2002. Community-oriented primary care: A path to community development. American Journal of Public Health 92(11):1713–1716.
Geiger, H. J. 2016. The first community health center in Mississippi: Communities empowering themselves. American Journal of Public Health 106(10):1738–1740.
GPO (U.S. Government Publishing Office). 2010. 42 U.S.C. §2000d to 2000d-7. https://www.gpo.gov/fdsys/pkg/USCODE-2010-title42/pdf/USCODE-2010-title42-chap21subchapV.pdf (accessed September 22, 2016).
The Greenling Institute. 2006. Legislative hearing before the California State Legislative Black Caucus, California Latino Legislative Caucus, and Asian Pacific Islander Legislative Caucus Paper on Foundation Giving to Minority-Led Nonprofits, April 24, 2016, Sacramento, CA.
Healthy Food Access Portal. 2016. Profile: Mandela MarketPlace. http://healthyfoodaccess.org/sites/default/files/HFA%20Portal%20Profile_Mandela%20Marketplace_FINAL2.pdf (accessed September 16, 2016).
Heiman, H. J., and S. Artiga. 2015. Beyond health care: The role of social determinants in promoting health and health equity. Menlo Park, CA: The Henry J. Kaiser Family Foundation.
Henry, S. 2011. James Berk of Mandela Foods brings produce to the people (video). http://civileats.com/2011/05/06/james-berk-of-mandela-foods-brings-produce-to-his-people-video (accessed October 27, 2016).
HHS (U.S. Department of Health and Human Services). 2014. Building sustainable programs: The framework. Rockville, MD: U.S. Department of Health and Human Services.
Hood, C. M., K. P. Gennuso, G. R. Swain, and B. B. Catlin. 2016. County health rankings: Relationships between determinant factors and health outcomes. American Journal of Preventive Medicine 50(2):129–135.
HRSA (Health Resources and Service Administration). 2015. 2015 health center profile. http://bphc.hrsa.gov/uds/datacenter.aspx?q=d&bid=040780&state=MS (accessed September 20, 2016).
IndyCAN (Indianapolis Congregation Action Network). 2014. Indianapolis Congregation Action Network annual strategic report 2012–2014. Indianapolis, IN: IndyCAN.
IndyCAN. 2016a. Indycan “ticket to opportunity” campaign strategy. Indianapolis, IN: IndyCAN.
IndyCAN. 2016b. The people’s agenda for ending mass incarceration and mass criminalization in Marion County. Indianapolis, IN: IndyCAN.
Inkelas, M., and P. Bowie. 2014. The Magnolia Community Initiative: The importance of measurement in improving community well-being. Community Investments 26(1):18–24.
IOM (Institute of Medicine). 1983. Community oriented primary care: New directions for health services delivery. Washington, DC: National Academy Press.
IOM. 2012. An integrated framework for assessing the value of community-based prevention. Washington, DC: The National Academies Press.
Kottke, T. E., M. Stiefel, and N. P. Pronk. 2016. “Well-being in all policies”: Promoting cross-sectoral collaboration to improve people’s lives. http://nam.edu/wp-content/uploads/2016/04/Well-Being-in-All-Policies-Promoting-Cross-Sectoral-Collaboration-to-Improve-Peoples-Lives.pdf (accessed February 22, 2016).
Kretzmann, J. P., and J. L. McKnight. 1993. Building communities from the inside out: A path toward finding and mobilizing a community’s assets. Evanston, IL: Institute for Policy Research.
LII (Legal Information Institute). n.d. Implied warranty of habitability. https://www.law.cornell.edu/wex/implied_warranty_of_habitability (accessed October 27, 2016).
Loh, P., and B. Shear. 2015. Solidarity economy and community development: Emerging cases in three Massachusetts cities. Community Development 46(3):244–260.
Longlett, S. K., J. E. Kruse, and R. M. Wesley. 2001. Community-oriented primary care: Historical perspective. Journal of the American Board of Family Medicine 14(1):54–63.
Mandela MarketPlace. 2013. About us. http://www.mandelamarketplace.org/about_us (accessed September 26, 2016).
Mandela MarketPlace. 2016. Mandela MarketPlace: Building a community-based food system. https://equityis.exposure.co/mandela-marketplace (accessed October 27, 2016).
Massachusetts Avenue Project. 2016. About. http://mass-ave.org/about (accessed September 26, 2016).
Mattessich, P. W., and E. J. Rausch. 2014. Cross-sector collaboration to improve community health: A view of the current landscape. Health Affairs 33(11):1968–1974.
Minkler, M. 2010. Linking science and policy through community-based participatory research to study and address health disparities. American Journal of Public Health 100(Suppl 1):S81–S87.
Minneapolis CPED (Community Planning and Economic Development). 2011. The Minneapolis promise: A campaign for the most prepared workforce in the nation. Minneapolis Department of Community Planning and Economic Development.
Minnesota Compass. 2016. Profiles: Minneapolis-Saint Paul neighborhoods. http://www.mncompass.org/profiles/neighborhoods/minneapolis-saint-paul#!community-areas (accessed September 19, 2016).
National Community Land Trust Network. 2016. FAQ. http://cltnetwork.org/faq (accessed September 22, 2016).
Needleman, H. L., A. Schell, D. Bellinger, A. Leviton, and E. N. Allred. 1990. The long-term effects of exposure to low doses of lead in childhood: An 11-year follow-up report. New England Journal of Medicine 322(2):83–88.
Nicholas, S. W., B. Jean-Louis, B. Ortiz, M. Northridge, K. Shoemaker, R. Vaughan, M. Rome, G. Canada, and V. Hutchinson. 2005. Addressing the childhood asthma crisis in Harlem: The Harlem Children’s Zone asthma initiative. American Journal of Public Health 95(2):245–249.
Paschall, K. 2016. How integrated voter engagement builds power and changes policy. Responsive Philanthropy(1):3–6.
The Planning History of Oakland. n.d. http://oaklandplanninghistory.weebly.com. n.d. The changing face of Oakland: 1945-1990. http://oaklandplanninghistory.weebly.com/the-changing-face-of-oakland.html (accessed October 26, 2016).
PolicyLink. 2014. Eastside Promise Neighborhood. http://www.promiseneighborhoodsinstitute.org/sites/default/files/documents/pni/PNI_san%20antonio_091914_a_0.pdf (accessed September 16, 2016).
Prevention Institute. 2011. Fact sheet: Links between violence and health equity. Oakland, CA: Prevention Institute.
Prybil, L., F. D. Scutchfield, R. Killian, A. Kelly, G. Mays, A. Carman, S. Levey, A. McGeorge, and D. W. Fardo. 2014. Improving community health through hospital-public health collaboration: Insights and lessons learned from successful partnerships. In Health management and policy faculty book gallery: Book 2. Lexington, KY: Commonwealth Center for Governance Studies, Inc.
PUSH (People United for Sustainable Housing). 2009. PUSH wins commitments from the fed!http://pushbuffalo.org/push-wins-commitments-from-the-fed (accessed September 26, 2016).
PUSH. 2012a. About us. http://pushbuffalo.org/about-us (accessed September 26, 2016).
PUSH. 2012b. Building green & affordable housing. http://greendevelopmentzone.org/housing (accessed September 26, 2016).
PUSH. 2012c. National campaigns. http://greendevelopmentzone.org/campaigns/national-campaigns (accessed September 26, 2016).
PUSH. 2012d. NetZero house. http://pushbuffalo.org/netzero-house (accessed September 26, 2016).
PUSH. 2012e. Sustainable neighborhoods. http://greendevelopmentzone.org/campaigns/sustainable-neighborhoods (accessed September 26, 2016).
PUSH. 2015. 2015 annual report. People United for Sustainable Housing.
Rybak, R. T. 2012. City voices and perspectives: R.T. Rybak, mayor of Minneapolis. Urban Networks to Increase Thriving Youth through Violence Prevention, Prevention Institute.
Sandel, M., E. Faugno, A. Mingo, J. Cannon, K. Byrd, D. A. Garcia, S. Collier, E. McClure, and R. B. Jarrett. 2016. Neighborhood-level interventions to improve childhood opportunity and lift children out of poverty. Academic Pediatrics 16(3 Suppl):S128–S135.
Schilder, D. 1997. Overview of results-based accountability: Components of RBA. http://www.hfrp.org/publications-resources/browse-our-publications/overview-of-results-based-accountability-components-of-rba (accessed October 27, 2016).
Schorr, L. 1988. Within our reach: Breaking the cycle of disadvantage. New York: Anchor Books.
Schorr, L. B. 1997. Common purpose: Strengthening families and neighborhoods to rebuild America. New York: Anchor Books.
Schorr, L. B. 2016. Evidence, replication and scaling up. Presented at ASPE HHS Roundtable on building evidence for domestic violence services and interventions, April 26, 2016, Washington, DC.
Soliman, J. n.d. The rise and fall of seventh street in Oakland. http://www.foundsf.org/index.php?title=The_Rise_and_Fall_of_Seventh_Street_in_Oakland (accessed October 26, 2016).
Speer, P. W., A. Peterson, A. Zippay, and B. Christens. 2010. Participation in congregation-based organizing: A mixed-method study of civic engagement. In Using evidence to inform practice for community and organizational change. Chicago, IL: Lyceum Books. Pp. 200–217.
statisticalatlas.com. 2016. Overview of Harlem, New York, New York (neighborhood). http://statisticalatlas.com/neighborhood/New-York/New-York/Harlem/Overview (accessed October 27, 2016).
Unger, S., and H. Wooten. 2006. A food systems assessment for Oakland, CA: Toward a sustainable food plan. Oakland Mayor’s Office of Sustainability and University of California, Berkelely, Department of City and Regional Planning. http://www.eukn.eu/e-library/project/bericht/eventDetail/a-food-systems-assessment-for-oakland-california-toward-a-sustainable-food-plan-2006 (accessed October 22, 2016).
U.S. Census Bureau. 2015a. Education attainment: 2011-2015 American Community Survey 5-year estimates. http://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?src=CF (accessed October 17, 2016).
U.S. Census Bureau. 2015b. Quickfacts: Minneapolis City, Minnesota. http://www.census.gov/quickfacts/table/PST045215/2743000 (accessed November 23, 2016).
Verbitsky-Savitz, N., M. B. Hargreaves, S. Penoyer, N. Morales, B. Coffee-Borden, and E. Whitesell. 2016. Preventing and mitigating the effects of ACEs by building community capacity and resilience: APPI cross-site evaluation findings. Washington, DC: Mathematica Policy Research.
Wakin, D. J. 2001. Breathless. The New York Times, May 13. http://www.nytimes.com/2001/05/13/nyregion/breathless.html?_r=0 (accessed October 17, 2016).
WE ACT. 2016a. Mission: Achieving environmental justice by building healthy communities since 1988. http://www.weact.org/mission (accessed September 22, 2016).
WE ACT. 2016b. NYSTEA. http://www.weact.org/transportationequityalliance (accessed September 22, 2016).
WE ACT. 2016c. History. http://www.weact.org/history (accessed September 22, 2016).
WE ACT. 2016d. Timeline. http://www.weact.org/timeline (accessed September 22, 2016).
WE ACT. n.d. Theory of change. http://www.weact.org/theoryofchange (accessed September 22, 2016).
Wenger, M. 2012. Place matters: Ensuring opportunities for good health for all. Washington, DC: Joint Center for Political and Economic Studies.
Zanjani, B. 2011. City voices and perspectives: Blueprint for Action—preventing violence in Minneapolis. Urban Networks to Increase Thriving Youth through Violence Prevention, Prevention Institute.
This page intentionally left blank.




























































































































