5
Integrating Data and Evidence into Communication Strategies in the Field
The second day of the workshop began with presentations from three individuals who were on the ground implementing communication strategies during the Ebola and Zika outbreak responses: Reverend John Sumo, director of the Health Promotion Division in the Liberian Ministry of Health; Julienne Anoko, a social anthropologist from the Sorbonne University; and Katherine Lyon Daniel, associate director for communication at the U.S. Centers for Disease Control and Prevention (CDC).
USING DATA TO REFINE COMMUNICATION STRATEGIES
Sumo began by providing a list of lessons learned from the field during Liberia’s first experience dealing with Ebola. The health system in Liberia, he explained, was not prepared to respond effectively to the epidemic, and the situation grew worse because of the damage the epidemic inflicted on the health system itself and the socioeconomic context of the entire country. He noted the situation was made more difficult by conflicting messages that did not resonate with the public and instead had the effect of producing misconceptions, disbelief, fear, community distrust, and community resistance to actions that might have reduced the severity of the epidemic. Fear and distrust kept Liberians from seeking care at Ebola treatment units (ETUs) and hospitals, he said, and religious and cultural practices affected smooth communication within the community.
Sumo noted that data played an important role in helping Liberia see its way through the Ebola outbreak. One key dataset came from epidemiologic surveillance, he explained. The first case in the country was reported
in March 2014 from Lofa County; over the course of the outbreak more than 11,000 people were suspected of having or confirmed to have Ebola, including 375 health care workers. Nearly 5,000 people died, including 189 health care workers. Of those who survived, 46 percent were males and 54 percent were females. The number of confirmed cases per day peaked in early October 2014, and by April 2015 no new cases were being reported (see Figure 5-1). The epidemiologic surveillance data provided key information on the communities affected and on other priority diseases.
In addition to the epidemiologic surveillance data, an anthropological study provided some basic information regarding the reasons for community fears, distrust, denial, and quality of care that led people to delay seeking care, said Sumo. He noted that cultural and religious beliefs led to widespread opposition to cremation and contributed to Ebola-related stigmatization of patients, relatives, and close associates. This study also highlighted the public’s concern about ETUs and what happened to individuals taken to these units, which helped explain why Ebola deaths occurred primarily at home and why those infected with Ebola, or sick for some other reason, were often hidden from health officials.
To understand the knowledge, attitudes, and practices of people in affected communities, Sumo and his colleagues studied community perceptions of Ebola. This study helped determine the level of awareness
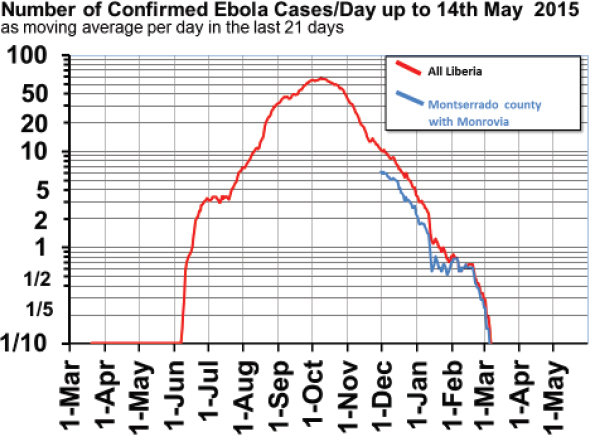
SOURCES: Sumo presentation, December 14, 2016; data from Ministry of Health, Liberia.
about current practices for preventing and controlling Ebola and identify community-appropriate practices that would reduce the risk of contracting or spreading the virus. It also helped gauge the success of social mobilization efforts and fine-tune messages and the overall communication strategy, said Sumo.
A rapid assessment of messages, materials, and activities helped Sumo and his colleagues in the health ministry gather information from intended audiences that they used to redesign the messages they were generating. This assessment looked at how well people in affected communities understood the ministry’s messages and the need to change behaviors to help prevent others in the community and their families from becoming infected. This rapid assessment also provided information on community involvement in and support for the Ebola response.
Concluding his presentation, Sumo said data were an important tool for determining if social- and behavioral-change messages were resonating with their intended audiences. Data also provided information to serve as a basis for planning and decision making. He noted that, when the ministry began its messaging effort, it stressed how deadly the infection is and that it has no cure, which caused additional problems rather than remedying existing challenges. Data informed the process of rethinking those messages, leading to improved community engagement that helped mitigate public fears, increased demand for care and other services, and prevented the spread of the virus.
A BOTTOM-UP APPROACH TO A SUCCESSFUL RESPONSE
Anoko began her presentation by discussing some of the practical steps she learned through her experience working with the United Nations and the World Health Organization (WHO) teams responding to Ebola and Zika outbreaks in Guinea and Cabo Verde, respectively. The first step, she said, is to build trust by developing a strong partnership with communities that gets them to own the situation. “The outbreak is not your outbreak. It is the community’s outbreak and is a community issue, so they have to be at the center of all of the interventions you are trying to do,” said Anoko. She further explained that achieving this first step requires embedding a social anthropologist in the communication team, which needs to meet with local administrative and traditional authorities to share knowledge—not give a lesson—about the outbreak, establish the need for community ownership, and create a list of all stakeholders and partners, not just the key ones. “When you arrive at a community, you will have a key partner there and they will say they are the one talking in the name of the community, but be careful—they are not always credible and influential,” said Anoko.
The local authorities, she pointed out, should then lead a community
gathering to provide information about the outbreak and the need for community ownership and involvement of credible and influential people from the community. Anoko explained that subsequent dialogue sessions, focus groups, and workshops with community members allow them to select influential and credible people, including men and women, traditional authorities, and religious representatives, according to the community’s criteria. She noted that the team’s social anthropologist can play an essential role in identifying some unexpected individuals. She added that it is important for these discussions to include the motivation criteria of the selected individuals as a means of ensuring transparency and building trust. In many instances, the selected individuals will want to be paid for their time. In some communities, Anoko and her colleagues were asked to provide water or build a school.
In Guinea, a surprising trusted and influential person in one town was a woman selling food from a street cart at the bottom of a mountain that housed the ETU at the top of the mountain. A large crowd gathered around this woman, so Anoko went over, ordered rice and potato leaves, and listened to the conversations, which were filled with rumors, misinformation, and beliefs about Ebola. Among the rumors was that white men at the ETUs were removing organs from patients and taking them to the United States. When conversing with the gathered crowd, Anoko learned that this woman was considered a trusted source of information on Ebola. After the crowd dispersed, Anoko and her colleagues spoke with the food vendor and provided her with correct information to dispel rumors and correct untruths about Ebola and the treatment center. “That lady was the unexpected person who fought Ebola with us,” said Anoko.
When the Ebola outbreak first began in Guinea, it took 6 months for the government to acknowledge that its top-down approach was not working to control the outbreak. However, within 2 months of applying this bottom-up approach in Télimélé, some 200 kilometers east-northeast of the capital Conakry, the outbreak was controlled thanks to community ownership and involvement. Unfortunately, said Anoko, this approach was not extended to the entire country. In Cabo Verde, health officials began employing this bottom-up approach some 10 months after the first cases of Zika and resulting microcephaly were confirmed when it became clear the population had an inappropriately low perception of risk regarding Zika. The outbreak is still ongoing there, and the health ministry is still implementing this bottom-up approach to risk communication, Anoko said.
Overcoming Resistance
With regard to strategies to overcome resisting populations that want to follow their own interpretations of interventions to control and contain
a disease such as Ebola or Zika, Anoko and her collaborators started by establishing a strong partnership with public and private research institutions to provide evidence and data to help counter the fact that even the national authority in Cabo Verde did not perceive the risk from Zika to be substantial. That perception created a problem, said Anoko, because people in Cabo Verde trust their health system, politicians, and other authorities. “If the authority does not perceive the risk, the community will not perceive the risk, so we cannot blame the community if they say they want to do it their own way,” said Anoko. However, once the authorities were convinced of the risk from Zika, the community immediately changed its attitudes and risk behaviors.
In Guinea, the interface between health partners in the country and communities was a point of tension throughout the Ebola response. Local populations wanted to be heard and to share their experiences, but the health teams were not interested in hearing from the community. The unidirectional, top-down flow of information, with experts educating the local population, exacerbated the problem. “This was a great mistake,” said Anoko. “What we needed was more dialogue approaches based on knowledge exchange.” She and her team looked at a variety of factors that might be influencing community response to Ebola protocols and found that two obstacles were the cultural ways of caring for sick individuals and cultural funeral practices, both of which went against standard Ebola biosecurity practices designed to limit transmission. All told, 26 villages resisted Ebola control measures.
Using their bottom-up approach to risk communication, Anoko and her colleagues were able to help communities create their own messages. For example, instead of telling community members that Ebola has no treatment and no vaccine and that individuals with any symptoms should go immediately to the isolation unit, community-developed messages explained that Ebola is a highly contagious and very severe disease and anyone with symptoms should contact the village chief, local health care professional, or community watch committee or call a toll-free number to get advice on what to do next. Community-developed messages stressed that many people recover from Ebola and that going to the ETU not only protects other family members but also provides medical support to help patients “become very robust and powerful to fight Ebola disease,” said Anoko. Community members wanted to be able to bring “good food” to the treatment units—in Guinea that was banana leaves with shrimp and spices—and Anoko and her colleagues negotiated with Doctors Without Borders to allow homemade food in the ETUs.
Another strategy to overcome resistance within communities was to engage them by recruiting Ebola survivors as social mobilizers and showing the community respect by allowing some of their beliefs and practices to
be incorporated in the local response. Anoko stressed that engagement is a sustained process, not a one-time product. “If you engage leaders in this village, know that in the next village you have to do the same up until the end of the outbreak,” she said. She noted that when WHO asked her to come to Guinea at the start of the outbreak in April 2014, her mission was to last 3 weeks. She stayed 2 years.
Addressing rumors and reticence is a key element of a strategy to overcome resistance, which in Guinea involved establishing a rumor task force as a subcommittee of the communication group. The rumor task force collected and analyzed rumors and developed messages to debunk them via interpersonal communication. “We had thousands and thousands of volunteers in the field knocking on doors house to house, debunking rumors, talking to people, and building trust,” Anoko explained. These volunteers even demonstrated washing themselves with bleach and water to show that doing so was not killing or harming them. In addition, Anoko and her colleagues documented any rumors in a magazine they shared twice weekly with authorities to show how they were addressing these rumors. Anoko even managed to get the presidents of Guinea and Sierra Leone to meet at a village on the border to discuss how to stop the Ebola outbreak.
Gaps in Risk Communication and Community Engagement
As part of her work in West Africa, Anoko identified a number of capacity issues that limited the effectiveness of risk communication. At the top of her list was a limited number of communicators to engage in effective risk communication at national and local levels, in part because communicators were unprepared to understand the epidemiologic data and to explain important concepts to the general population. In general, leaders and response partners were not well coordinated and failed to consider risk communication as a crosscutting pillar that can support response efforts. They also lacked technical brochures with practical “how-to-do” items for communities, and little monitoring and evaluation; furthermore, the availability of funds to pay support staff, such as anthropologists, was inconsistent.
The resources to fill these capacity gaps include social anthropologists who can provide knowledge about context and help build intercultural bridges and communicators whose own capabilities are improved and expanded. Standard operating procedures for risk communication would provide tools and tips on how to collect, integrate, and share data. They would also enable the development of an effective and strategic risk communication plan based on data and knowledge, monitoring and evaluation, and sharing information in real time with community stakeholders. Anoko suggested that any risk communication effort should include a data man-
ager to help integrate data from multiple sources and then share data with community partners and decision makers. She also encouraged risk communicators to be openminded and ready to innovate, even at a time of crisis. Above all, she said in closing, it is critically important to listen, respect, and share; to collaborate; to put individuals at the center of all health interventions; to have empathy; and to respect that diversity is richness.
THE FRONT LINES: WHERE DATA MEET REALITY
“Zika is the most complex communication challenge that I have seen in my 20-something years at CDC, not only because it is such an important time with very vulnerable families and women, but all the barriers that we heard about yesterday,” said Lyon Daniel to open her presentation. She noted that CDC and other agencies have been trying to control the Aedes aegypti vector for decades with little success, and that some of the most effective interventions—insecticides—are scary to people and unwanted in their communities. “Put all that together from a communication perspective and it is heartbreaking,” she said.
Communication during an emergency, especially in the beginning of an emerging health crisis, is always a heavy lift and often requires capacity building to quickly create, vet, and shape massive amounts of information merely to answer incoming questions from the public and media. “This is before we can work on any kind of proactive work,” said Lyon Daniel. Without a dedicated emergency fund, which CDC has requested to respond to emerging health crises such as Zika, much of the early energy spent in the agency’s communication department is to chase money and resources to support an effective response.
In addition to building capacity, she said, it is important to build flexibility to target key messages for those who need it the most, who are not necessarily the same as those who are the most vocal. Lyon Daniel said she subscribes to former Secretary of State Colin Powell’s 40/70 rule: “You need enough information to give you about a 40 to 70 percent chance of being right and making the right decision and then going with it,” said Lyon Daniel. “You cannot wait until you have 100 percent of the information before you communicate.” As an example, she noted that CDC mounted an immediate response as soon as Miami experienced a Zika outbreak; the preliminary analysis showed an increase in knowledge, awareness, reported behavior, and infection control capacity in Miami as compared to Puerto Rico, where the information about Zika was on the ground much later.
Most important, though, Lyon Daniel stated, is to have a specific strategy that uses the available capacity and flexibility to shape communication specific to each outbreak. “I always tell the communication scientists, first
plan your science-based, theory-driven, accessible, understandable, formative process and outcome evaluation, and then when you get out into the field expect you will immediately need to throw half of it out and adapt.” This strategy has to reflect the reality of the way people get information today, which is not mainly from government, experts, or other traditionally influential sources. “The strategy we have had to work on both for Ebola and for Zika was sharing information people to people,” said Lyon Daniel. As an aside, she recommended CDC’s crisis and emergency risk communication process1 as a good resource for managing risk communication during an emergency.
It is key in today’s communication environment, she added, to use convenient ad hoc sources and engage where people are exchanging information, whether it is local media, social media, or a woman selling food by the roadside. As other speakers have said, Lyon Daniel reiterated, it is also essential to track message uptake and behavior change in real time, to adjust messages and messaging tactics accordingly, and to keep providing information that is fresh, relevant, and compelling.
New targeting strategies for Zika appear to be working, said Lyon Daniel. Ninety percent of the audiences she and her colleagues test know that mosquitoes spread Zika and how to protect themselves from mosquitoes, a big change, she said, from the results of initial testing in February and March 2016. The sexual transmission message is faring less well because the public is having a hard time understanding how a disease spread by mosquitoes can also be passed along through sexual transmission. “Using a condom when you are pregnant does not seem to make sense to anybody,” said Lyon Daniel.
Unlike with Ebola in the United States, where the anxiety level was very high despite a very low risk, anxiety about Zika is low among some high-risk populations. A pregnant woman is likely to be quite aware of the risks of Zika and be taking appropriate action, said Lyon Daniel. However, the man returning from spring break in Puerto Rico likely has no idea he should use mosquito repellant for 3 weeks after returning so he does not spread Zika to uninfected mosquitoes, and that he needs to use a condom for at least 6 months to prevent transmission in case he is infected and not symptomatic.
Fear, Lyon Daniel noted, is a natural, adaptive response and not a communication failure, so a critical role for risk communication is to help people manage their fear in a productive manner. “We have to stop thinking that when people are fearful, we need to immediately reassure them,” said Lyon Daniel. It is important, she said, to acknowledge fear, empathize, talk about its qualities, but also to never overreassure or tell someone not to
___________________
1 Available at emergency.cdc.gov/cerc (accessed February 21, 2017).
be afraid. Panic can be maladaptive, however, and some of the behaviors people use to cope with fear can be nonproductive.
Lyon Daniel reiterated how valuable community engagement is in the risk communication and response process. “If you do not engage the community and you do not understand what they are saying, you will not understand what they are hearing. It is not what you say; it is what they hear. They have their own experts and their own people they are paying attention to,” she said. Lyon Daniel referred to the concept of a media village, where people shut themselves off from the outside world to protect themselves and only read material that reinforces existing views. She noted that the scientific community tends to have its own media village.
A worrisome trend, Lyon Daniel said, is the growing inability to tell what is real from what is fake. This is not simply a matter of health literacy or science literacy, which are important. “We need a national media literacy action plan,” she said. She concluded her remarks by saying, “Be strategic, do not be afraid of fear, and remember you are in a media village and we have to break down the barriers between that.”
DISCUSSION
Eduardo Gotuzzo, director of the Alexander von Humbolt Instituto de Medicina Tropical, Universidad Peruana Cayetano Heredia, commented that, with most viral outbreaks, 95 percent of the cases appear in the first 10 months, so taking 6 months to prepare a strategic plan cannot happen. Lyon Daniel agreed completely and said the purpose of CDC’s crisis and emergency risk communication plan is to have a response ready when the first call comes in. “From the very second the phone rings, I can immediately go into talking about what we know, what we do not know, and what we are doing to find out. That is critical,” said Lyon Daniel. A critical juncture occurs 24 to 48 hours into an emerging crisis when strategic thinking is imperative so that the communication response does not become one of merely reacting to the loudest voices but instead identifies who is most at risk and who most needs information to protect their health, she noted. In the case of Zika, the most important audience would be pregnant women. Anoko added that getting to the social mobilizers and providing them with critical information in that first 24 to 48 hours of an outbreak is a vital step toward getting ahead of an outbreak instead of merely reacting to it.
Jeffrey Duchin, health officer and chief of the Communicable Disease Epidemiology and Immunization Section for Public Health in Seattle and King County, Washington, asked Sumo and Anoko to list the most important activities from their perspective to sustain going forward to be prepared for the next unpredictable event. Anoko replied that countries
in West Africa are now drafting strategies during this quiet, interepidemic period that will have them much better prepared to respond to the next outbreak. These drafting efforts have support from the highest levels of government, she said. Sumo agreed that having a risk communication strategy in place ahead of time is critical going forward. In Liberia, he and his colleagues are engaging the media now, developing a media toolkit with key messages, and identifying the key channels of communication in communities and building relationships with them. An evaluation team recently assessed Liberia’s preparedness for the next outbreak and identified a few gaps that the health ministry is now working to address.
Jennifer Gardy, senior scientist at the British Columbia Centre for Disease Control and assistant professor at the School of Population and Public Health, University of British Columbia, asked Anoko for examples of innovative and creative approaches to risk communication she has seen in her work. Anoko described a situation in Guinea in which a pregnant woman died while still carrying her baby. According to local culture, the mother and baby had to be buried separately or four generations of women of childbearing age would die while pregnant or in childbirth. The health officials refused to let the community follow their tradition, which resulted in 26 villages protesting and community members raiding the ETU and taking the body away. At that moment, Anoko and her colleagues contacted the main leaders of these communities, who told her there was no solution to this problem, something that as an anthropologist she knew was not true. Her solution was to find the grandson of the man who had organized the ritual in question some 80 years earlier. This grandson organized a new ritual for this specific case that included prayer, dancing, and begging the community’s ancestors to forgive this “bad thing.” Anoko and her team, national authorities, and officials from WHO, Red Cross, and Doctors Without Borders then went to the community and enacted this special ritual, and the community allowed the mother and baby to be buried together.
Edward You, supervisory special agent in the Weapons of Mass Destruction Directorate of the Federal Bureau of Investigation (FBI), commented that all the discussion so far seemed to place the communication burden solely on the health and scientific communities and their engagement with the public, but he wanted to point out that the onus is on the government as well to participate fully in risk communication. He recounted how, during the anthrax mailing not long after the 9/11 attack, the FBI and CDC had a contentious interaction, but the two agencies have since developed a strong partnership to respond to suspicious events or unusual outbreaks. In addition, the FBI, through existing cooperative biological engagement programs with the U.S. Department of Defense and the U.S. Department of State, as well as under the auspices of the Global Health Security Agenda,
has engaged with agencies in Southeast Asia and Africa to build partnerships in law enforcement, public health, and agriculture. On this last point, he noted the importance of involving the animal and plant health communities given the potential for zoonotic events and their potential impact on human health and the nation’s economy. This involvement, he said, is another aspect of communication and coordination that needs to be taken into account when creating a risk communication plan and the partnerships needed to carry out that plan. Lyon Daniel agreed that it is important to build transnational relationships because global travel and global commerce have expanded the potential for novel infectious disease outbreaks to occur in the United States.
Lonnie King, professor and dean emeritus of The Ohio State University College of Veterinary Medicine, asked Lyon Daniel, as the lead strategist for communication at CDC, how to standardize communication across the many different organizations involved in the partnerships You discussed. He also asked if it was possible to standardize communication among partners in places such as Africa. Lyon Daniel replied that doing so is a huge challenge, particularly in the initial stages of an outbreak when it is crucial to identify who will be affected and who needs to be at the table. “There is no way you can bring everyone who needs to be there immediately, so building in a regular process of touching base is very important,” Lyon Daniel explained. During the Zika outbreak, for example, CDC held a summit with health communicators, local officials, epidemiologists, and vector control experts in early March 2016 to be prepared well before the U.S. mosquito season began. At that point, the CDC website became a repository of information, not so much as a communication tool but so that every partner could see and have access to the same information.
Anoko said she and her colleagues have advocated with national authorities to establish a “coordination communication act” as soon as possible to allow people to work together in a harmonized manner and develop messages together. This coordination was not easy, she said, because countries such as Guinea lacked experience managing an issue of this scale. The United Nations Children’s Fund, WHO, and CDC provided technical assistance to support the national authorities during the crisis and over a 2-year period to help build capacity for the next event. Sumo added that Liberia has created a national health promotion policy and plan that serve as a guide to implementing communication activities across 10 organizations working in the country. Liberia, he noted, has also developed a national message and a materials development committee to pretest and validate the messages that go out to these organizations working in communities.
John Rainford, director of The Warning Project, commented that leadership is critical for coordinating communication, as well as not worrying about “the small stuff” and not expecting that everyone will say
exactly the same thing all the time given different perspectives and different constituencies. Leadership comes, he said, in knowing what is important to coordinate and what is not. He then asked the panelists for any ideas on how to prevent another tragic failure from occurring, referring to the initial response to the Ebola outbreak. Lyon Daniel replied that her understanding of what went wrong in the beginning was making the assumption that groups that had not handled large outbreaks before could do so and that communities that had never been exposed to Ebola before would know more than they actually did. Anoko said it is important to support less-prepared countries during the quiet times and help them build effective communication processes and build and maintain the relationships they will need when an outbreak does occur. Sumo added that providing information that can immediately empower and engage communities to take ownership from the onset of an outbreak is critical.
Responding to the comment about the small stuff, Lyon Daniel said that, too often, communication teams spend time responding to loud or influential voices and their concerns, which turn out to be small stuff. She recommended dedicating part of the communication team to deal with those demands so that the rest of the team can manage the urgent issues.












