2
Environmental Facilitators Framework
As part of the statement of task for this study outlined by the U.S. Social Security Administration (SSA) (see Box 1-1 in Chapter 1), the committee was asked to “provide definitions and explanations of relevant terms, including assistive technology and workplace reasonable accommodations.” To meet this objective, the committee, in addition to providing definitions of the terms identified by SSA in a glossary (see Appendix B), developed an environmental facilitators framework based on the model of disability in the International Classification of Functioning, Disability and Health (ICF). This chapter begins with an overview of the ICF and related models. It then provides a detailed description of the committee’s environmental facilitators framework. The chapter ends with findings and conclusions.
Before proceeding, it is important to understand as context for the ICF and the committee’s framework the evolution of the concept of disability over the past quarter century from a medical to a biopsychosocial model. The medical model identifies disability as a “feature of the person” caused by disease, injury, or some other health condition (WHO, 2001, 2002, p. 8; see also IOM, 1991; Kaplan, 2000). According to that model, disability is managed through medical care in the form of individual treatment or through adjustments or changes to behavior (Kaplan, 2000; WHO, 2001). Conversely, the biopsychosocial model identifies disability as a problem at the societal level, with the goal of integrating all individuals into society (Kaplan, 2000; Whiteneck, 2006; WHO, 2001). Therefore, managing disability is the collective responsibility of society to allow for the full participation of individuals with disabilities in all aspects of life (Kaplan, 2000; WHO, 2001). This evolution of the concept of disability is reflected in the
ICF, related disability models, and the committee’s environmental facilitators framework.
THE INTERNATIONAL CLASSIFICATION OF FUNCTIONING, DISABILITY AND HEALTH AND RELATED MODELS
In 1980, the World Health Organization (WHO) issued the International Classification of Impairments, Disabilities, and Handicaps (ICIDH) as a tool for organizing the consequences of disease into three distinct classifications: impairment at the organ level, disability at the person level, and handicap at the societal level (WHO, 1980). However, the labeling of “handicap” at the societal level and the failure to include environmental factors created some problems in the use of the ICIDH (IOM, 2006; WHO, 1980). The latter factors are explicitly incorporated in both earlier and later models of disability. A model developed by Nagi (1965) initiated research into the environmental factors at the family, community, and society levels that affect disability as an outcome. And Fougeyrollas (1995) clarified the usefulness of a holistic model that stresses the role of environmental factors in social participation for individuals with disabilities.
In 2001, the WHO published the ICF as a revision to the ICIDH. The ICF is a classification scheme that identifies and describes the relationships among the various factors that interact to effect health and function. Its revised classifications of disability are body structure and function at the organ level, activity at the person level, and participation at the societal level. Environmental factors are incorporated into the conceptualization of disability, and the term “handicap” is eliminated to expand the scope of the model and allow for the description of positive experiences (WHO, 2001). Specifically, the ICF conceptualizes an individual’s functioning as the interaction among his/her health condition, environmental factors, and personal factors.
The information in the ICF is organized into two parts: functioning and disability and contextual factors. As shown in Figure 2-1, functioning and disability (the middle tier of the figure) consist of body functions and structures and activities and participation, while contextual factors (the bottom tier) consist of both environmental and personal factors. Body functions are defined as the “physiological functions of body systems (including psychological functions)” and body structures as the “anatomical parts of the body such as organs, limbs and their components” (WHO, 2001, p. 10).
Environmental factors “refer to all aspects of the external or extrinsic world that form the context of an individual’s life and, as such, have an impact on that person’s functioning” (WHO, 2001, p. 213). These factors can be classified into two levels—individual and societal. The individual level encompasses the immediate environment of the individual, while the
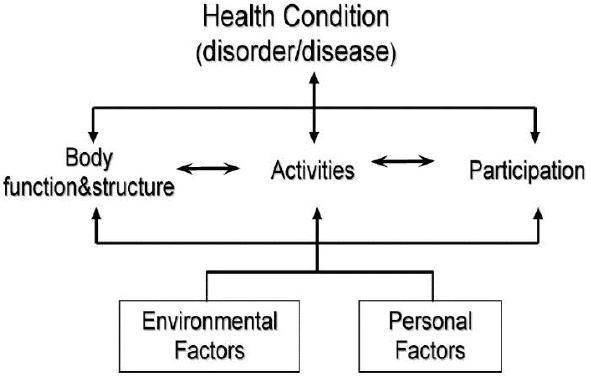
SOURCE: WHO, 2001.
societal level refers to “formal and informal social structures, services, and overarching approaches or systems in the community or society that impact the individual” (WHO, 2001, p. 17). Examples of environmental factors include job market, geographic location, noise level, built environment, and transportation. Built environment encompasses all of the tools individuals need to perform work activities. Transportation is another environmental factor that is necessary for an individual to participate fully in employment.
Personal factors represent influences on functioning particular to the individual (WHO, 2013). Given the large variation in society and culture and even a lack of clarity with respect to these factors, they are not classified within the ICF (WHO, 2013). Yet, while developing a classification for personal factors can be challenging, it also represents an opportunity. Including this type of information in data collection could assist investigators in providing “empirical background for the future development of personal factors in the ICF” (WHO, 2013, p. 26), and codifying personal factors in the ICF could help in conveying “information important for a complete description of the functioning profile” (WHO, 2013, p. 40). Personal factors that may affect functioning include gender, race, ethnicity, age, social and educational background, past and current experiences and life events, behavior patterns, and psychological assets (WHO, 2013).
Both environmental and personal factors act as facilitators or barriers along the disablement pathway. As a facilitator, assistive technology is an
environmental factor that can help reduce the effects of an impairment. Conversely, certain features in the built environment may act as barriers that prevent an individual with a disability from completing a task.
The biopsycho-ecological model expands on the biomedical and biopsychosocial models to encourage a more comprehensive understanding of illness, injury, activity limitation, and restriction of participation at the interface between the person and the environment (Stineman and Streim, 2010). This model operates through health environmental integration, which recognizes complex interactions beginning at the cellular level and ending at the individual’s experience of the environment (Stineman and Streim, 2010).
One effort that begins to identify the role and pathways of contextual (i.e., environmental and personal) interventions in the disablement/enablement process within an ICF framework is the modification of the ICF developed by the National Health and Aging Trends Study (Freedman, 2009). This modification entails the inclusion of a new domain—“accommodations” (see Figure 2-2)—defined as behavioral responses to changes in capacity. Accommodations include the receipt of help, assistive technology, environmental modifications, and other compensatory strategies (Freedman, 2009) that act on the interactions among the ICF domains to enhance activity and participation.
ENVIRONMENTAL FACILITATORS FRAMEWORK
In the context of the evolution of the understanding of disability described above, it is evident that SSA’s approach to disability is based on a medical model rather than a biopsychosocial model that stresses the importance of environmental factors. Particularly, the agency’s current focus is on impairment mitigation and functional capacity as mandated by legislation. More all-encompassing definitions based on the biopsychosocial model, including those adopted by the U.S. Congress in the Americans with Disabilities Act (ADA), the WHO in the ICF, and the U.S. Centers for Disease Control and Prevention (CDC), identify disability as a problem that results from the interaction of a person’s impairments and functional capacity with external factors, recognizing the significant role of the environment in contributing to disability. Specifically, the ADA recognizes that full participation of individuals with disabilities in society is dependent on the use of accessible designs to remove physical environmental barriers in public and private facilities, while reasonable accommodations are crucial for achieving full participation in the workplace (IOM, 2006). In addition, the CDC identifies the difficulty of a person with a disability to perform certain activities and interact with the surrounding world (CDC, 2016). For SSA, the importance of the biopsychosocial model is not solely in understanding disability but, more importantly, in clearly identifying environmental
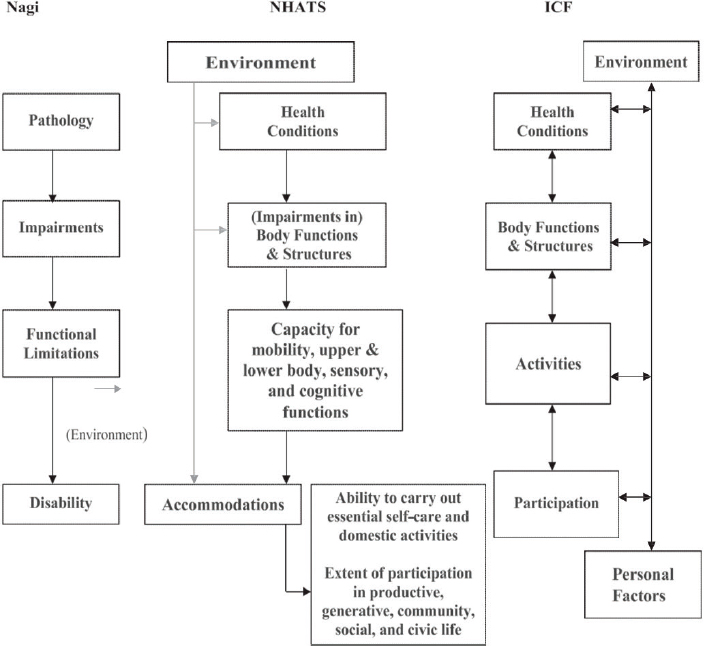
SOURCE: Freedman, V. A. 2009. Adopting the ICF language for studying late-life disability: A field of dreams? The Journals of Gerontology, Series A: Biological Sciences and Medical Sciences 64(11):1172-1174, Published by Oxford University Press on behalf of the Gerontological Society of America.
factors as potential focal points for interventions. Accordingly, the committee developed the environmental facilitators framework depicted in Figure 2-3, based on the ICF.
Framework Description
The environmental facilitators framework illustrated in Figure 2-3 is a conceptual model showing potential relationships. It builds on the ICF to identify specific environmental interventions and the pathways along which
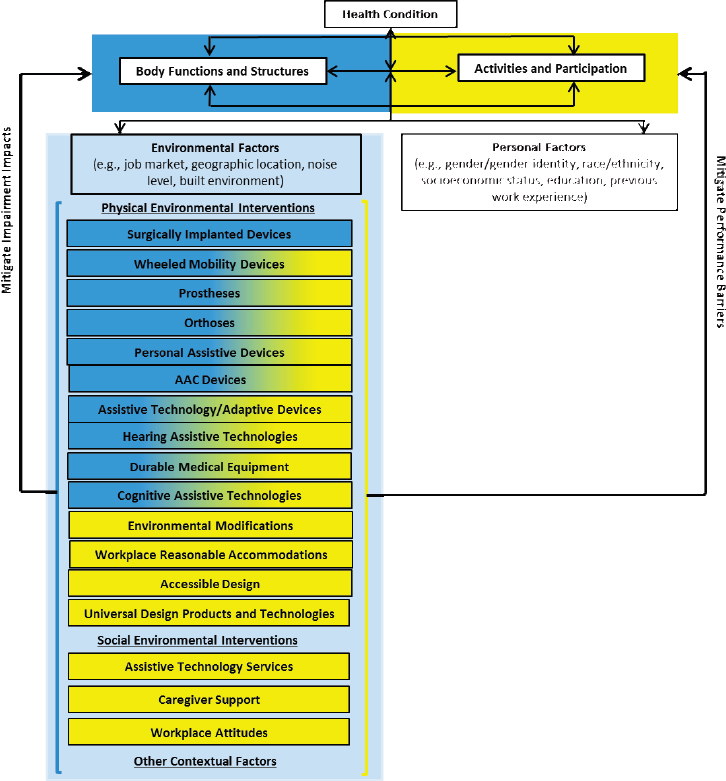
NOTES: The extent to which environmental interventions mitigate the impact of impairments (blue) and performance barriers (yellow) is based on the committee’s expert opinion. AAC = augmentative and alternative communication.
those interventions can act either to mitigate the impact of impairment by restoring or replacing relevant body structure and/or function or to enhance activities and participation by mitigating performance barriers. The former interventions target organ system impairment(s), while the latter target contextual factors.
As shown in Figure 2-3, environmental factors include physical environmental interventions, social environmental interventions, and other
contextual factors (light blue box). Assistive products and technologies are physical environmental interventions that can either mitigate the impact of impairments by restoring or replacing relevant function (shown in blue), enhance performance and activity by mitigating performance barriers (shown in yellow), or do both in varying degrees (shown in blue and yellow).
As illustrated in Figure 2-3, for example, surgically implanted devices (e.g., artificial joint, cochlear implant) solely mitigate the impact of impairment because they directly affect the individual’s body functions and structures (and therefore are shown in blue). In contrast, wheeled mobility devices, prostheses, orthoses, personal assistive devices, and augmentative and alternative communication devices primarily mitigate the impact of impairment but, depending on the type of device, may also act to reduce performance barriers to participation and activity (and therefore are shown mainly in blue but also in yellow). For instance, the use of a power wheelchair may mitigate the impact of impairment by allowing individuals to have independent mobility. Whereas independent mobility may improve an individual’s capacity to work, it is not directly linked to enhanced performance and participation within a workplace. On the other hand, a standing wheelchair that enables an individual to reach a counter that is required for the performance of a specific work activity is clearly aimed at mitigating a performance barrier.
The greater proportion of yellow for assistive technology/adaptive devices, hearing assistive technologies, durable medical equipment, and cognitive assistive technologies in Figure 2-3 reflects the fact that these interventions equally mitigate the impact of impairment and reduce performance barriers. For example, a hearing assistive technology such as a hearing aid or personal listening device may mitigate impairment by providing an individual with hearing loss with improved audibility of sounds, such as speech or music, regardless of the context. Alternatively, the use of an assistive listening system in the workplace is aimed at enhancing work performance by allowing an individual with hearing loss to participate in a work activity that involves listening to others.
Finally, some interventions (indicated in all yellow) serve solely to mitigate performance barriers to participation in the workplace. They include both physical environmental interventions—such as environmental modifications, workplace reasonable accommodations, accessible design, and universal design products and technologies—and social environmental interventions, including assistive technology services, caregiver support, and workplace attitudes. As mentioned earlier, personal factors also may have an impact on the outcome of interventions. These factors may include gender/gender identity, race/ethnicity, socioeconomic status, education, and previous work experience.
Implications for SSA
The environmental facilitators framework shown in Figure 2-3 can serve as a guide to assist SSA and other organizations in evaluating the effects of impairments and the impact of assistive products and technologies and other environmental interventions on mitigating those effects. It is important for such organizations to assess individuals’ functional capacity when using the products and technologies they normally use to mitigate their impairments. However, capacity and performance do not necessarily imply participation, nor are they necessarily sufficient for predicting work performance. Work participation and performance are directly related to environmental factors beyond the personal assistive products and technologies individuals may use when their ability to execute a particular task or function is being assessed during a disability determination. For instance, environmental modifications and workplace reasonable accommodations are work-specific and vary from place to place, making it difficult to determine an individual’s ability to participate in work activities based on the use of assistive devices alone. Even if an individual with a severe impairment could perform (with or without such devices) the tasks necessary for a particular job with appropriate environmental modifications or accommodations, there is no guarantee that those modifications or accommodations will in fact be available. In short, it is essential to consider a multitude of complex contextual (environmental and personal) factors when assessing an individual’s ability to work. Moreover, environmental modifications and social acceptance are necessary to allow for the full participation of individuals with disabilities in all aspects of life. However, SSA’s medical model approach positions the agency on the side of simply mitigating the impact of impairment. Accordingly, it is unreasonable to expect the agency to factor environmental interventions designed solely to enhance participation, such as environmental modifications, workplace reasonable accommodations, and accessible and universal design, or social environmental interventions, such as workplace attitudes, into its disability determinations. If SSA’s mission were to evolve to encompass facilitating employment among people with disabilities, it would be necessary for the agency to take a more holistic approach that would include an assessment not only of a person’s functional capacity but also the personal and environmental factors shown in Figure 2-3.
FINDINGS AND CONCLUSIONS
Findings
2-1. Some assistive products and technologies can enhance work performance or mitigate impairment, while others may do both.
2-2. The concept of disability has evolved to reflect a biopsychosocial model in which disability is perceived as the interaction between an individual’s functional capacity and relevant environmental and personal factors.
2-3. Likewise, based on the International Classification of Functioning, Disability and Health model, understanding a person’s ability to participate in work includes not only the person’s functional capacity but also relevant environmental and personal factors.
2-4. Environmental factors such as job market, geographic location, and built environment can influence how an individual experiences disability.
2-5. Personal factors such as gender/gender identity, race/ethnicity, age, socioeconomic status, insurance coverage, education, and previous work experience can influence how an individual experiences disability.
2-6. A complete evaluation of a person’s functioning would include assistive products and technologies that mitigate the person’s impairments.
2-7. The Social Security Administration’s (SSA’s) current focus is on impairment mitigation and functional capacity as mandated by legislation. Accordingly, the agency’s emphasis is on understanding the role of interventions that mitigate the impact of impairments by restoring or replacing body structure and/or function.
Conclusions
2-1. Assistive products and technologies may mitigate the impact of an impairment sufficiently to allow a person to work. In some cases, however, environmental and personal factors create barriers to employment despite those impairment-mitigating effects. [Finding 2-1]
2-2. Assessment of work participation requires consideration of an individual’s functional capacity plus a multitude of complex environmental and personal factors. [Findings 2-2, 2-3, 2-4, 2-5]
2-3. If SSA’s mission were to evolve to encompass facilitating employment among people with disabilities, a holistic approach that would include an assessment not only of a person’s functional capacity but also of personal and environmental factors would be necessary. [Findings 2-2, 2-3]
2-4. To assess the effects of impairments on a person’s ability to work, it is important to evaluate the person’s functional capacity while using the assistive products and technologies he or she normally uses. [Finding 2-6]
2-5. Given SSA’s current mission, it is unreasonable to expect the agency to factor into its disability determinations environmental interventions designed solely to mitigate performance barriers. [Finding 2-7]
REFERENCES
CDC (U.S. Centers for Disease Control and Prevention). 2016. Disability overview. https://www.cdc.gov/ncbddd/disabilityandhealth/disability.html (accessed March 21, 2017).
Fougeyrollas, P. 1995. Documenting environmental factors for preventing the handicap creation process: Quebec contributions relating to ICIDH and social participation of people with functional differences. Disability and Rehabilitation 17(3-4):145-153.
Freedman, V. A. 2009. Adopting the ICF language for studying late-life disability: A field of dreams? The Journals of Gerontology, Series A: Biological Sciences and Medical Sciences 64(11):1172-1174.
IOM (Institute of Medicine). 1991. Disability in America: Toward a national agenda for prevention. Washington, DC: National Academy Press.
IOM. 2006. Workshop on disability in America: A new look. Washington, DC: The National Academies Press.
Kaplan, D. 2000. The definition of disability: Perspective of the disability community. Journal of Health Care Law and Policy 3(2):352-364.
Nagi, S. 1965. Some conceptual issues in disability and rehabilitation. In Sociology and Rehabilitation, edited by M. B. Sussman. Washington, DC: American Sociological Association.
Stineman, M. G., and J. E. Streim. 2010. The biopsycho-ecological paradigm: A foundational theory for medicine. Physical Medicine and Rehabilitation 2(11):1035-1045.
Whiteneck, G. 2006. Conceptual models of disability: Past, present, and future. In Workshop on disability in America: A new look, edited by M. J. Field, A. M. Jette, and L. Martin. Washington, DC: The National Academies Press. Pp. 50-66.
WHO (World Health Organization). 1980. International Classification of Impairments, Disabilities, and Handicaps: A manual of classification relating to the consequences of disease. Geneva, Switzerland, and Albany, NY: WHO.
WHO. 2001. International Classification of Functioning, Disability and Health. Geneva, Switzerland: WHO.
WHO. 2002. Towards a common language for functioning, disability and health: ICF. Geneva, Switzerland: WHO.
WHO. 2013. How to use the ICF: A practical manual for using the International Classification of Functioning, Disability and Health. Geneva, Switzerland: WHO.










