4
Design Features of Accessible Housing for Older Adults and Individuals with Disabilities
The workshop’s second panel featured three presentations on design features needed in accessible housing to support the health, well-being, and independence of older adults and individuals with disabilities. Bryce Ward, the director of health care research at the University of Montana’s Bureau of Business and Economic Research, spoke about the connection between accessibility in the home and quality of life for older adults and those with disabilities. Corneil Montgomery, a senior program specialist in Habitat for Humanity International’s Aging in Place program, and Patricia Tedesco, the coordinator of the Home Access Program at the Vermont Center for Independent Living, then discussed their organizations’ efforts to increase the stock of affordable and accessible housing. An open discussion moderated by Elena Fazio from the Office of Performance and Evaluation at the Administration for Community Living followed the three presentations.
LIFE STARTS AT HOME: LINKING HOME ENVIRONMENT AND QUALITY OF LIFE FOR PEOPLE WITH DISABILITIES
Bryce Ward
Director, Health Care Research
Bureau of Business and Economic Research
University of Montana
Bryce Ward of the University of Montana began his presentation by talking about his grandfather, a man who had been a very socially engaged person when he was younger. As his grandfather aged, however, his mobility became more limited, and in the last several years of his life he rarely left his bedroom other than to go to a dialysis center. Nonetheless, Ward said his grandfather remained lucid and would happily engage in conversation in his room. Ward said that later, once he was an adult, he wondered why his grandfather could not come downstairs and socialize with the rest of his family if he was mobile enough to go to dialysis treatment. “How much of it was his health, and how much of it was other things, such as his environment?” Ward asked, noting that his grandparents lived in a multistory home that was not particularly accessible. “How much better would his life have been, how much bigger could we have expanded his choice set, if we had been successful at convincing them they should have moved to a different house or invested more in modifying the house?”
Ward said that stories like his grandfather’s story are not uncommon. The Bureau of Labor Statistics’ American Time Use Survey,1 for example, showed that people in poor health spend 4 additional hours watching television each day. Ward said he wondered if improving the way older adults and individuals with disabilities interact with their home environment would increase their choice set and improve their quality of life. He and his colleagues are in the early stages of testing this hypothesis.
Data from the U.S. Census Bureau’s American Housing Survey2 provide some support for this hypothesis, Ward said. These data show that although households with at least one individual who uses some form of mobility equipment—a cane, crutch, wheelchair, or powered scooter—are more likely to have accessibility features in the home, many households that might benefit from these features still do not have them (see Table 4-1 and Figure 4-1). For example, 72 percent of households with a member who uses mobility equipment do not live on the ground floor of their buildings and do not have access to an elevator. Similarly, nearly two--
___________________
1 For more information, see https://www.bls.gov/tus (accessed February 27, 2017).
2 For more information, see https://www.census.gov/programs-surveys/ahs (accessed February 27, 2017).
TABLE 4-1 Features in U.S. Homes That Can Be Inaccessible Based on Whether a Household Member Uses Mobility Equipment
| Feature | Percentage of Households Where Member Uses Mobility Equipment | Percentage of Households Where No Members Use Mobility Equipment |
|---|---|---|
| Stepped entrance | 57.2% | 60.9% |
| Upstairs with no elevator* | 71.6% | 81.7% |
| No grab bars in bathroom | 62.3% | 86.7% |
| No entry level bathroom** | 18.5% | 20.9% |
| No entry level bedroom** | 32.4% | 42.2% |
NOTES: *Apartments not on the ground floor. **Multistory units.
SOURCE: Ward presentation, December 12, 2016.
thirds of individuals who use mobility equipment live in homes that do not have grab bars in the bathroom. These rates are high across all regions of the United States, Ward said (see Table 4-1), and they span urban and rural communities (see Figure 4-1). In rural areas, Ward said, some 91 percent of people who live in multistory apartment buildings and use
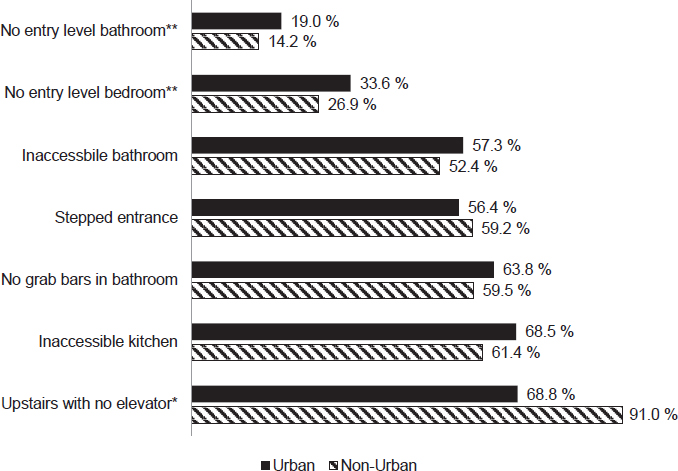
NOTES: *Apartments not on the ground floor. **Multistory units.
SOURCE: Ward presentation, December 12, 2016.
mobility equipment do not have access to an elevator. “That makes it hard to engage in one’s community,” Ward said.
Ward and his colleagues are now conducting a study—called the Health and Home Survey—for which they surveyed households in three communities across the United States and asked survey participants about features of their home, how they feel while using those different features, and what percentage of maximal exertion is required for individuals in the home to engage in home activities, such as activities of daily living, entering and exiting the home, and preparing meals. For people with a mobility impairment, Ward and his colleagues found that these activities require two- to three-fold more exertion than for a person without a mobility impairment. In other words, Ward said, people with a mobility impairment have a harder time engaging in their houses. Moreover, the data also show that people who have a mobility impairment and could use an accessibility feature, such as a grab bar, exert far more energy engaging in the related activity, such as bathing, than do those who do not have a mobility impairment. “This suggests, but does not prove, that perhaps we can change this by changing our housing environments,” Ward said.
Data from the U.S. Census Bureau’s American Time Use Survey show that people without impairments spend about 33 percent more time—i.e., 38 more minutes—each day on household activities than do those with a mobility impairment. This includes activities such as gardening or food preparation and cleanup. Similarly, Ward said, people with impairments are less likely to report any time spent washing, dressing, or grooming, and when they do engage in these activities it takes them longer to accomplish them. These limitations matter, Ward said, because people who do not wash, dress, or groom themselves are substantially less likely to leave their home.
Ward said that his work has also shown that there is a 30 percent decline in the rate at which people say they participate in social and recreational activities for every standard deviation increase in how much time they report exerting themselves while bathing. While not conclusive yet, these data provide a link between living in houses that have many features that are not accessible and being less likely to get out into the world and engage in the social or recreational activities that are a determinant of quality of life. However, Ward said, getting people out of the house is not the only important issue, as there is also evidence suggesting that being able to do things at home such as housework makes people with mobility impairments happy and increases their sense of purpose.
Taken together, Ward said in conclusion, the data that he and his colleagues have collected suggest that it is important to enable people who have a disability to engage in more activity, whether it is engagement in
activities in the home or in activities to get out of the home. “A potentially important part of allowing us to do all that is making your home more livable and more accessible because life does start at home,” he said.
HABITAT FOR HUMANITY: HELPING PEOPLE AGE IN PLACE
Corneil Montgomery
Senior Program Specialist, Aging in Place
Habitat for Humanity International
Habitat for Humanity International’s strategic vision is to have community impact by improving housing conditions, to have sector impact by partnering with other organizations to increase shelter access, and to have societal impact by inspiring action to end poverty in housing, said Corneil Montgomery of Habitat for Humanity International. Helping people age in place aligns with that strategy in three ways: it leverages shelter as a catalyst for community transformation; it increases the capacity to serve the most vulnerable; and it mobilizes volunteers as hearts, hands, and voices for the cause of adequate and affordable housing. Montgomery said that in 2015 approximately 13,000 volunteers ages 65 and older participated in the organization’s projects in communities across the United States and that the organization prides itself in the way it uses older adults as volunteers.
Montgomery said that the national office of Habit for Humanity International has set a goal for itself to assess the housing needs of older adults, which means assessing not only the physical infrastructure of their homes but also considering the aspirations, preferences, and needs of the individuals living in those homes. In addition, as part of its Aging in Place program, the national office is encouraging local offices3 to engage in larger community improvement projects, such as streetscaping, building community gardens, and helping local residents improve their financial literacy skills. He said, too, that some of the local offices are developing and testing new models of housing, such as townhomes and co-housing, from which the national office can learn and then share best practices throughout the organization.
The Aging in Place program has adopted a holistic approach to housing that requires partnering with community-based organizations to respond to a variety of needs in a community, such as health, transportation, mobility, and food access. The local office in Savannah, Georgia, for example, has a
___________________
3 Montgomery explained that each of the 1,400 local Habitat for Humanity International offices in the United States is an independent, nonprofit organization. The national office can advise the local offices, but it cannot dictate what they do.
partnership with Meals on Wheels America4 to study the effect that housing has on food security. This partnership also uses the volunteers of Meals on Wheels America to comprehensively assess the homes to which they deliver meals. Meals on Wheels America’s assessment tools and questionnaires also enable Habitat for Humanity International to better understand the individual needs of families. Recently Habitat for Humanity International has also begun collecting data to determine the value of having universal design features in the homes it builds—i.e., no-step entry, wide doorways and hallways, easily accessible controls and switches, easy-to-use handles, and one-floor living—by measuring falls prevented, emergency room visits, quality of life, and cost savings to Medicaid and other parts of the health care system.
In fiscal year 2016, Montgomery said, local Habitat for Humanity International affiliates completed 6,094 repairs, which is a substantial increase from the 1,800 repairs completed in fiscal year 2015. Of the homes repaired in fiscal year 2016, 43 percent had an older adult living in the home, and 33 percent had an individual with a disability living in the home. Single women were head of household for half of the repaired homes, while single men were head of household for 14 percent of the repaired homes; 20 percent had at least one child under the age of 18. Montgomery said that when a local chapter works with families on repairs, it does not simply make the repairs and leave, but rather it partners with the families to learn about all of their needs and then coordinates with other organizations to address those needs that Habitat for Humanity International cannot address. The local chapter also conducts a pre- and post-repair assessment to find out if these families love where they live, if their health improves, and if the repairs prevent falls and improve other indicators of well-being.
Montgomery said that Habitat for Humanity International has several key accessibility improvements that it would like to install in all homes (see Box 4-1) but this is not possible, so the organization partners with families to both empower them and provide them with advice on best practices for home accessibility. The majority of Habitat for Humanity International homes have 80 percent of these features, which has been accomplished through partnership with families and local funding organizations.
Families that receive housing benefits from Habitat for Humanity International must participate in the building, rehabbing, or repairing of their homes. Those who cannot perform physical tasks can participate by engaging experts and the community. In order to fund these
___________________
4 For more information, see http://www.mealsonwheelsamerica.org (accessed March 2, 2017).
projects, Habitat for Humanity International provides its local affiliates with price repayment guidelines that are on a sliding scale. A typical payment for a repair will cost the family in the range of $50 to $100 per month for 36 months, although the local affiliates try to leverage as many local resources as possible to keep costs at a minimum for the families. Montgomery said that these projects use some local U.S. Department for Housing and Urban Development (HUD) funding. In addition, some affiliates leverage funding from Medicaid to make the modifications. The Greater Memphis, Tennessee, affiliate and Salt Lake Valley, Utah, affiliate are already leveraging pay-for-success funding and studying whether they might be able to use health care system community benefit funds to do repairs and improvements that can help people stay healthy and in their homes.
Looking ahead, in the short term Habitat for Humanity International plans to increase the number of home repairs it does by 5 percent, to enable greater mobility and visitability for 20 percent of the homes repaired, and to reduce the risk of falls in 20 percent of the homes repaired. Over the next 3 years, the national office will work with 10 local affiliates in a variety of communities to develop more evidence-based practices and to track, document, and analyze data to determine the cost–benefit ratio for specific housing and non-housing interventions in terms of fall prevention, food insecurity, isolation, and mobility. Over the long term,
Montgomery said, the goal is to affect the low-income older-adult generation so that more of them are able to stay and thrive in their homes and communities of choice.
THE VERMONT CENTER FOR INDEPENDENT LIVING: IMPROVING HOME ACCESS
Patricia Tedesco
Coordinator, Home Access Program
Vermont Center for Independent Living
The Vermont Center for Independent Living (VCIL), a statewide nonprofit organization, opened its doors in 1979. The Home Access program was added in 1983 to fund and build accessibility features for households where there is someone who has a permanent physical or mobility disability and where the household income is below 80 percent of the HUD median household income for the homeowner’s county, said Patricia Tedesco of VCIL. Renters and families living in mobile homes can also apply for assistance, but only with explicit permission from the property owner.
After someone applies for assistance, the program sends a form to the applicant’s physician to verify that the applicant has a disability and that the proposed home modifications would enable that person to live more independently or avoid moving into a nursing home. This also ensures a direct relationship between the home access program and an individual’s health care provider, Tedesco said. Once program staff approve an application and put a project on the wait list, the applicant receives a “possible donor” letter that he or she can take to public service groups, faith-based organizations, or any other source of funding. The letter explains what the project is and how much the applicant needs to raise as “leverage funding”—$2,000 for a bathroom modification or $1,000 for a ramp, for example. The program also connects the applicant with a VCIL peer advocate counselor who can help the applicant look for leverage funding. At the same time, Tedesco said, she also begins “hunting for money.” If the applicant has multiple sclerosis, for example, she contacts the National Multiple Sclerosis Society, which has funds set aside for these types of projects. Tedesco said that volunteer time counts toward leverage funding using a formula the program developed to calculate the value of the labor it would have to pay for in the absence of volunteer labor. The one exception to the leverage funding requirement is if the desired modification will enable an individual to leave a nursing home and return home. “If they cannot get into their home because they do not have a ramp or their bathroom is not accessible, and that is the only reason they are in
the nursing home, no leverage funding is required and they move to the top of the list,” Tedesco said.
Once the funds are in place, the program turns to one of five independent access consultants in Vermont who visit the applicant’s home and develop a plan for the proposed modifications. The scope of work is then sent to three contractors whom VCIL has vetted and trained in an annual contractor seminar. “We work with a vulnerable population, so everybody [providing services] has to have a background check, references, and insurance,” Tedesco said. Once she receives the three bids, usually within 4 weeks, she issues a contract, the project is built, and the access consultant performs a final inspection.
Projects that the home access program has completed include increasing the space beneath a bathroom sink to enable wheelchair access, converting a bathtub into a shower, installing fold-down grab bars, and installing ramps. In fiscal year 2016, Tedesco said the VCIL home access program received $545,000 of funding from the State of Vermont. The program completed 71 projects for 63 individuals with $181,245 of leverage funding and $28,995 of in-kind donations. The completed projects included 33 bathroom modifications, 35 ramps, 2 entrance modifications, and 1 platform lift. The average cost per project was $7,676. The 63 individuals served were an average of 60 years old, included 17 renters and 46 home owners, and had an average household median income of 39 percent of the HUD county median. Over the course of the year, the program received 98 applications, and 51 individuals were on the waiting list at the end of the fiscal year.
Lessons Learned
Tedesco said she has learned several lessons from her work on the home access program. Some lessons were easy to address, such as sending applicants a letter acknowledging that their application has been received, which reduces follow-up phone calls. Another lesson learned was to develop a landlord acknowledgment form, which not only provides details of any proposed modification to the home of a renter but also an invitation to the landlord to attend the initial inspection and to contribute to the project. The form notifies the landlord that he or she will be responsible for any future repairs to the improvements. In the case that an applicant owns their mobile home but does not own the land it sits on, the mobile home park owner needs to acknowledge that the program is building a ramp. Tedesco noted that the program is also moving away from installing permanent ramps to installing modular ramps that can be moved when an individual moves homes.
VCIL’s primary funder has placed a cap of $15,000 on any single
project, so Tedesco used to approve projects with budgets up to $15,000. However, when one project went over budget, she discovered she did not have a mechanism to pay for the additional cost. Tedesco has since capped projects at $13,500 to allow for change orders if they become necessary. Another financial lesson was that applicants must provide their portion of the project’s funding before the project begins. The program has also partnered with Bath Fitter, which creates well-explained financial programs for bathroom retrofitting. She said that she is always seeking feedback from contractors, the access consultants, the people and organizations who provide leverage funding, nurses, and anyone else who can help ensure that she and her coworkers are not making decisions in a bubble but are working collaboratively. “I think that is what leads to some of our success,” she said.
Tedesco concluded her presentation by noting that she and her colleagues are now hosting annual training on the Americans with Disabilities Act guidelines, VCIL’s specifications, and disability awareness for contractors and funding partners. They are also building and supporting relationships with NeighborWorks America5 and other partners that she said she hopes will streamline the funding process and produce better outcomes. Tedesco said she has testified at Vermont’s House and Senate appropriations committee hearings to provide evidence of the importance of home modifications.
DISCUSSION
Winston Wong from Kaiser Permanente noted that some of the nation’s more progressive health care organizations are looking at how to integrate social determinants of health into electronic health records. These organizations are also looking to take more accountability for the social aspects of keeping individuals as healthy as possible and optimizing the health care organizations’ ability to care for their consumers’ chronic conditions. In that context, he asked Montgomery if Habitat for Humanity International has a mechanism for sharing information with its clients’ health care providers and health plans. Montgomery said that Habitat for Humanity International has learned from its Greater Memphis and Salt Lake Valley affiliates, which have strong connections to local hospital systems, about the value of such connections and is starting to have discussions with health care systems. One pilot project, for example, will deploy technology that will allow Habitat for Humanity International to coordinate information sharing with non-housing partners, including health care systems.
___________________
5 For more information, see http://www.neighborworks.org (accessed March 2, 2017).
José Nuñez from the District of Columbia Department of Housing asked Ward and Montgomery if in their work they consider accessibility from the street to the home in addition to accessibility within the home and if there are federal or state grants to defray the costs of external improvements. Ward said that while the majority of the questions in the American Housing Survey and his program’s Health and Home Survey are about accessibility inside the home, there are survey questions that cover external accessibility from the street to the home. For example, one question asks, “Considering all methods, can you get from the street to the house without going up at least one stair?” Montgomery said that Habitat for Humanity International’s home assessment starts at the street curb, but added that the organization could do a better job of defining external accessibility more explicitly. He added that as Habitat for Humanity International moves from a one-house/one-family approach to a more coordinated approach with communities, the organization will be evaluating accessibility features of entire city blocks.
Robyn Stone of LeadingAge commented that the architects and other consultants she works with have found that lighting is important to accessibility, particularly for individuals with a visual impairment, and that the necessary modifications can be as simple as changing light bulbs. Montgomery replied that access lighting is a critical component of the modifications that Habitat for Humanity International recommends to its affiliates. The organization also recognizes lighting as being an easy to fix and sees it as something that the organization can empower families to do themselves. Tedesco said that her program is limited to making bathroom modifications, widening doorways, and building ramps, but that the program does address lighting that is inside the bathroom. Ward added that questions about lighting are included in the most recent version of the Health and Home Survey.
Emily Rosenoff from the U.S. Department of Health and Human Services asked Montgomery and Tedesco to talk about what gets people to finally ask for help from their programs. Tedesco replied that her program gets calls every day from people in a variety of circumstances. The challenge is that people call and expect to have a ramp installed in a month, not realizing that there is a 2-year waiting list unless they already have leverage funding available. Montgomery responded that most of the calls his program receives occur when people are in crisis, when repairs are needed to address a significant threat to health and safety and the family cannot afford those repairs, or when a doctor or occupational therapist has noted that repairs are needed before the individual can return home. Habitat for Humanity International is trying to be more proactive in raising awareness about its program, he added, so that people can begin planning for their needs in advance rather than waiting until there is a crisis.
Given that housing is a public health issue, Teresa Lee of the Alliance for Home Health Quality and Innovation asked if there could be a way to incentivize primary care providers to ask their patients during annual wellness visits about mobility and accessibility in the home, similar to how primary care providers address advanced illness planning and advance directives. Sarah Szanton from the Johns Hopkins School of Nursing said the Medicare annual wellness visit could serve as a means of being proactive about identifying potential accessibility issues. She said that she thinks this wellness visit should take place in the individual’s home every few years and be reimbursed by Medicare. “Disability . . . is the relationship between the person, what they can do, and what their environment requires. If you are only talking to the person [and not seeing them in their home], you are not seeing that potential gap,” she said. Ward replied that people should have conversations about accessibility not only with their health care provider but also with real estate agents and home builders. “There is all this information that we should start accumulating and start sharing,” he said, “so that people are primed to start asking the question, not at crisis time, but when they are making a housing choice because, as we know, once they get into a house, they frequently do not want to leave it.”
Miriam Kelty of the Washington Area Villages Exchange remarked that in Montgomery County, Maryland, homes with older adults experience fires and death caused by fires more than other homes, and she asked the panelists if their programs include installing smoke detectors. Tedesco said that the access consultant form the VCIL home access program uses includes questions specific to smoke detectors. In addition, the program installs a smoke and carbon monoxide detector in every home in which it does a bathroom modification or ramp installation. Montgomery said that Habitat for Humanity International takes the same approach as VCIL in its inspections and modifications. Kelty added that there are several young technology companies developing home safety equipment and that are looking for opportunities to demonstrate their technologies and thus they may be good partners. Ward said that his program is working on a study to evaluate these types of technology interventions and build an evidence base for programs such as Montgomery’s and Tedesco’s to use. Margaret Campbell of Campbell & Associates reported that IBM is doing a study in which it has partnered with postal carriers in Japan to report on the accessibility and livability issues they see in the homes of the older adults on their delivery routes. The carriers use iPads to report any issues they see. Campbell agreed with Ward and Kelty that data will be critical to determining the need, potential outcomes, and cost-effectiveness of potential technology interventions.
Jeffrey Henderson from the Black Hills Center for American Indian Health asked Ward if he had worked on housing accessibility with the Native American community in Montana. Ward replied that he has worked with that community on health issues, but not specifically on housing yet. Dara Baldwin of the National Disability Rights Network said that most government agencies do not work with Native American communities, though the Bureau of Indian Affairs is starting a program on housing, as is the National Council for American Indians (NCAI). The National Disability Rights Network is working with NCAI on accessibility issues through the Transportation Equity Caucus.6
___________________
6 For more information, see http://www.equitycaucus.org (accessed February 27, 2017).
This page intentionally left blank.














