Proceedings of a Workshop
INTRODUCTION1
Millions of people—infants, children, adults, and their families—are currently coping with serious illness in the United States. Efforts are intensifying to improve overall care quality through the delivery of person-centered and family-oriented services, for patients of all ages and across disease stages, care settings, and specialties. While aging baby boomers are increasing the proportion of patients in the Medicare population over time, the sickest and most vulnerable patients needing health system support and other services to meet their complex needs can be found across the age spectrum and in a broad range of care settings, from perinatal care to geriatric care.
Recognizing the need to thoughtfully consider and address the challenges and opportunities in efforts to improve care quality and value, the Roundtable on Quality Care for People with Serious Illness of the National Academies of Sciences, Engineering, and Medicine held the public workshop Integrating the Patient and Caregiver Voice into Serious Illness Care.
___________________
1 The planning committee’s role was limited to planning the workshop, and the Proceedings of a Workshop was prepared by the rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants, and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine, and they should not be construed as reflecting any group consensus.
This workshop, held on December 15, 2016, in Washington, DC, was the first in a series planned by the roundtable, and was designed specifically to bring together diverse personal perspectives and experiences about priorities and values that are important to patients and families coping with serious illness, and to consider solutions that support integration of these priorities and values in practice.
The Roundtable on Quality Care for People with Serious Illness serves to convene stakeholders from government, academia, industry, professional associations, nonprofit advocacy organizations, and philanthropies. Inspired by and expanding on the work of the 2014 Institute of Medicine (IOM) consensus study report Dying in America: Improving Quality and Honoring Individual Preferences Near the End of Life (IOM, 2015),2 the roundtable aims to foster ongoing dialogue about critical policy and research issues to accelerate and sustain progress in care for people of all ages experiencing serious illness.
In his introductory remarks opening the workshop, James Tulsky, chair of the department of psychosocial oncology and palliative care at Dana-Farber Cancer Institute, chief of the division of palliative medicine at Brigham and Women’s Hospital, and professor of medicine and co-director at the center for palliative care at Harvard Medical School, applauded the focus on placing patients and their families at the center of every session, noting that the roundtable membership agreed to launch its work by focusing on the voices of the people living with serious illness. Acknowledging the lifetime passion of many in the room working with people with serious illness (many of whom had faced serious illness themselves), the planning committee co-chair JoAnne Reifsnyder agreed. Reifsnyder, who is chief nursing officer and executive vice president of clinical operations at Genesis Healthcare, noted that the voice of the patient really is “the voice of all of us, the people we serve, and also our experience as well.”
Planning committee co-chair Rebecca Kirch, executive vice president of health care quality and value at the National Patient Advocate Foundation, set the stage for the workshop by explaining how the central theme of the agenda was framed to put people at the heart of health care. Among the many different perspectives offered throughout the day, she explained,
___________________
2 As of March 2016, the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine continues the consensus studies and convening activities previously carried out by the Institute of Medicine (IOM). The IOM name is used to refer to publications issued prior to July 2015.
“a common theme across the diseases, disciplines, geographies, and age spans is that people and professionals are really wired to talk about the quality of how they are living.” Elaborating on this central theme supporting quality of life and the lived experience for patients and caregivers at any age and any stage of illness, she said people want to talk about the quality of life, not death, even if they know they are dying. The planning committee took this insight to heart in organizing the workshop agenda around what patients and family say is most important to them.
The workshop format combined interviews of caregiver and clinician pairings with moderated panel presentations and interactive audience discussion exploring a range of topics, including
- gaps, challenges, and strategic solutions for integrating patient, caregiver, and family voices into person-centered care services delivery across ages, diagnoses, and disciplines;
- opportunities for supporting spirituality, values, beliefs, priorities, and preferences to provide comfort and meaning for patients and loved ones coping with serious illness;
- addressing health equity, poverty effects, and outcomes disparities experienced by patients and caregivers among geographically and ethnically diverse and vulnerable populations;
- advancing person-centered and family-oriented care through community outreach initiatives involving support of chaplaincy, spiritual counselors, community health workers, and others tuned to patient and family needs and preferences;
- nurturing healthier connections among patients, caregivers, and clinicians through training and development of person-centered communication skills that support integration of patient and family values in care planning and shared decision making;
- integrating impairment-driven prehabilitation and rehabilitation services to complement palliative care and other services delivery focused on supporting patient and caregiver quality of life, functional goals, and priorities;
- implementing a relationship-centered approach to addressing unique challenges, such as providing team-based perinatal and neonatal care for seriously ill infants and their families; and
- innovations, interventions, and insights for supporting and normalizing conversations about patient and family needs, values, and preferences and implementing them in practice.
Throughout the workshop’s four sessions, the panelists and audience shared many examples of what was described by Amy Berman, senior program officer with The John A. Hartford Foundation, as “a deeply human conversation” among people who received care and the providers of their care. The workshop’s first session featured patient, caregiver, and clinician perspectives, which served to present a holistic view of optimal quality care that goes beyond clinical care to address psychosocial, emotional, and spiritual needs. The second session focused on meeting the needs of vulnerable populations that might not have access to high-quality care, and on minimizing the resulting health disparities in an effort to ensure that everyone receives the care and services that matter most to them. The third session highlighted approaches that can be implemented in the clinical environment as well as within communities to support quality care and quality-of-life needs for seriously ill people of all ages and in all disease stages throughout their life course. The final session featured examples of proven tools, interventions, and market research findings that help improve and advance earlier and more frequent clinical and community conversations about what seriously ill patients and their families want, need, and prioritize throughout the continuum of care.
This Proceedings of a Workshop summarizes the presentations and discussions. A broad range of views and ideas were presented. A summary of suggestions for potential actions from individual workshop participants is provided in Box 1. The workshop Statement of Task can be found in Appendix A, and the workshop agenda can be found in Appendix B. The workshop speakers’ presentations (as PDF and audio files) have been archived online.3
INTEGRATING THE PATIENT, CAREGIVER, AND FAMILY VOICE INTO SERIOUS ILLNESS CARE: CHALLENGES AND OPPORTUNITIES
Amy Berman (featured in the photo on the following page) opened the first session of the workshop by sharing that she is a person living with a serious illness, and comes to the session from “a place of great honesty and respect and keen appreciation for the difficulty of people sharing their story”
___________________
3 For additional information, see http://www.nationalacademies.org/hmd/Activities/HealthServices/QualityCareforSeriousIllnessRoundtable/2016-DEC-15.aspx (accessed May 2, 2017).
about the most difficult times in their life. She also described the opening session as a story about transformation—for the patients, the caregivers, and the practitioners involved in their care, noting that “this is an amazing opportunity to hear what the meaning is of palliative care and good care in serious illness and end of life.”
Berman noted the diverse composition of the workshop audience, which included a broad array of patients, caregivers, advocates, grassroots mobilizers, and professionals in policy, clinical, and community practice, representing the fields of hospice, palliative care, rehabilitation, social work, chaplaincy, spiritual counseling, pediatrics, geriatrics, neonatology, disease specialties, and others. Berman observed that every single person in the room has had “a deeply human experience that connects us all.” She urged participants to “integrate it in every cell in your body because that’s really what it takes to do things right.”
The Evolving Landscape of Serious Illness Care

Further setting the stage for the first session, Berman provided some specific examples of how the serious illness care landscape continues to evolve. She mentioned the anticipated arrival of the new administration and members of Congress, which she said will likely bring many changes. Although such change may create a sense of uncertainty, it could also be an opportunity. Berman also described the growing “pop gestalt” movement that aims to bring about changes in health care to better align treatment with people’s values and preferences. She said this movement has been bolstered by resonant messaging in Atul Gawande’s best-seller Being Mortal (Gawande, 2014), as well as Paul and Lucy Kalanithi’s tragic yet inspirational story captured in When Breath Becomes Air (Kalanithi, 2016). “People care about their life and the choices that they get to make in their life,” noted Berman. “They are increasingly demanding care that fits their desires, their goals, and their values.”
While payment mechanisms that could encourage more goal-oriented communication in the clinical context remain nascent, Berman pointed out that the decision by the Centers for Medicare & Medicaid Services (CMS) to reimburse physicians for advance care planning conversations (one of the recommendations contained in the Dying in America report (IOM, 2015) has offered a very helpful start.
Berman also described another feature of the changing landscape, which is the movement in some states to support the concept of medical aid in dying. This allows a terminally ill, mentally capable person with a prognosis for living less than 6 months to request from a physician a prescription for medication the patient could self-administer to hasten death in a peaceful manner. Before providing any such prescription, she explained, the physician must confirm that the person is fully informed and must also provide information about additional care options at the end of life, including comfort care, such as pain control and other components of hospice care. Medical aid in dying is currently authorized in five states,4 either through statute or court decision: California, Montana, Oregon, Vermont, and Washington (Compassion & Choices, 2016).
These are just a few examples of the evolving landscape, which Berman noted continues to move in a direction that offers opportunities for improving serious illness care to meet people’s needs throughout their lives, including at earlier stages in the care continuum. As an example, she referenced findings from the Hartford Foundation’s 2016 survey of physicians about their advance care planning conversation practices since CMS started reimbursing them. While 99 percent of responding doctors agreed that these conversations were part of their job, they cited a lack of support systems and training as barriers, with roughly half reporting they do not know what to say (PerryUndem Research/Communication, 2016).
This clarion call to prioritize communication skills training for clinicians echoed the earlier mentioned IOM report Dying in America, which presented a series of recommendations to improve the quality of care for seriously ill people at the end of life (IOM, 2015). That report served as the foundation for the planning committee’s determination to focus this workshop on personal perspectives about quality of living with serious illness. The IOM report also documented the pivotal role hospice has played to improve
___________________
4 In addition, the End of Life Options Act went into effect in Colorado on December 16, 2016. See https://www.colorado.gov/pacific/cdphe/medical-aid-dying (accessed May 2, 2017).
end of life care and associated conversations. Many workshop participants noted that efforts by hospice and others have contributed significantly to the evolving landscape of serious illness care in which treatment and services are increasingly aligned with patients’ personal preferences at earlier stages in their illness.
Personal Perspectives on the Essential Elements of Optimal Care
In her introduction of the first workshop session, which featured caregivers paired with a pediatrician and a geriatrician, Berman explained that the stories they would share about their experiences and approaches illustrate optimal care. The two sets of presenters, Berman explained, serve as “examples for the nation” of what high-quality, person-centered care involves.
The Lord Family’s Pediatric Care Experience
“My daughter Cameron, at the age of 6 months, was diagnosed with the rare and still fatal disease infantile Tay-Sachs.” So began Blyth Lord, founder and executive director of Courageous Parents Network, as she shared her experience as the parent of a child destined to die young. Tay-Sachs disease results from a genetic mutation that alters the central nervous system’s ability to metabolize certain lipids properly, and the subsequent accumulation of these lipids kills nerve cells. As the disease progresses, the affected child experiences terrible seizures and gradually loses control of his or her muscles and eventually the ability to swallow. Lord related the journey she, her husband Charlie, and their firstborn daughter Taylor took over Cameron’s short lifetime (the Lord family is featured in the photo on the following page, with Cameron being held on her father’s lap). This journey, she said, was all about giving Cameron the best quality of life she could have for as long as she was alive. It was a transformative experience, one that turned grief into healing and action, and it was a journey made possible because their pediatrician asked about and listened to their desires for their daughter and became a partner in, rather than a director of, her care.
Lord recounted how her daughter’s pediatrician, Richard Goldstein, assistant professor of pediatrics at Boston Children’s Hospital and Harvard Medical School, remained Cameron’s primary doctor throughout her illness, even when she was referred to a neurologist, a nutritionist, and a pain management specialist. “Rick never outsourced her care, and that was a

particularly critical piece of our journey with our daughter because it felt like a team effort and something that was very sacred and very important as there were difficult decisions to make along the way, and Rick helped us do that,” said Lord. Another key member of the care team was a grief counselor who worked with the family throughout Cameron’s life and after it ended, supported them in their bereavement.
One unusual aspect of the Lords’ experience was that they shared it with Charlie’s identical twin brother Tim, and sister-in-law Allison, whose son Hayden also had been diagnosed with infantile Tay-Sachs. “Within a month we had learned that these two beautiful children in one family were going to die because there was and still is no treatment or cure for the disease,” said Lord. “We were already very close, but we got much closer in this really profound thing that we were doing together.”
Cameron was never able to sit upright on her own, she never crawled, and as the disease progressed, she went from being an animated, happy, cheer-
ful, and expressive baby to one who could not even show affect in her face, which Lord said was particularly difficult for her and her husband. Eventually, Cameron lost the ability to swallow, an inevitable outcome that Goldstein had prepared the Lords to expect in his role of telling them what was coming and what decisions they would have to make as the disease progressed. Lord spoke of how important that forecasting and anticipatory guidance was for the whole family. “Ultimately, as a parent you are going to have to make a decision about feeding and feeding tubes, and we did that work with Rick,” said Lord. “We did this also in conversation with my brother- and sister-in-law . . . about what we wanted for our children, and that is actually not typical. It was really extraordinary that we had this other couple who we trusted completely and who were going through the exact same thing.”
“I do not remember having the ‘A Ha!’ moment together,” Lord continued, “but I know that the four of us together made the decision that for each of us we did not want to give our children a feeding tube. This disease takes away so much that for us, quality of life did not mean quantity of life.” Calling that one of the most profound decisions they made, again with Goldstein’s continuous support, Lord also talked about having to make frequent decisions about whether to treat Cameron’s recurring pneumonia. Eventually they decided not to do so, and Cameron died peacefully at home soon after her second birthday. Lord explained that their nephew Hayden had died when he was 2.5 years old and Cameron died 5 months later at age 2, “so we had 18 months . . . where quality of life was what it was all about.”
Having an infant with an incurable and fatal disease had an obvious life-changing impact on the Lords, but it also had a life-changing effect on their pediatrician, Goldstein. Even before helping the Lords through the diagnosis, treatment, and death of their daughter, Goldstein was one of those pediatricians who chose to treat the most seriously ill children. “They were the VIPs of my practice,” said Goldstein, who noted that at the time Cameron was born, pediatric palliative care was a very “de novo” practice, but that he was drawn to what he called “meaning-based medicine that reckoned with the primal responsibilities that parents have for their children regardless of what happened.”
Cameron was a particularly difficult case for Goldstein because his daughter and the Lords’ first child were the same age and went to the same preschool, and his second child and Cameron were born within 1 month of each other. Medicine, he said, is often about looking through a window when it comes to detaching oneself emotionally from a hard case, but with Cameron, it was as if he was looking into a mirror. “That challenged me in
an important way,” said Goldstein. “Cameron Lord is somebody that I carry with me through my life and my career and is so important to who I am because I learned not just about the provision of care, the responsibilities, and all of the complications, but I learned about myself and I learned about a kind of empathic medicine.” Beside the personal connection, what made this experience “horrible” was the knowledge that the Tay-Sachs diagnosis comes with a predictable and inevitably fatal trajectory. Knowing that the seizures Cameron suffered would steadily worsen and become intractable, Goldstein said, “I needed to help them steel themselves for that and for understanding that their child would die shortly afterward.”
Goldstein characterized his first interactions with the Lords as “fairly typical for what happens when people are a little bit over their head.” He focused on the technical—making sure the diagnosis was correct, for example—and making sure the Lords’ older daughter, Taylor, was healthy. When he delivered the bad news, the Lords were “as braced as they could be, but we drew together,” he recalled. “It was black and tender at the same time.” Goldstein explained “and then I gave them some time because I knew that however they were going to get through it, it would be their solution and the more I could help them get to their solution, the better off things would be.” Lord remembered the moment vividly when Goldstein was escorting them to his office, noting that “there was a lot of care as you brought us in” and when he turned to them and said, “I am sorry.” In describing the scene, Lord said, “They were your only words for a while, which, needless to say, was the only thing one could really say.”
After Cameron died, the Lords reflected on the things that had gone well for them compared to the experience of their nephew’s parents, who did not receive the same kind of supportive care from their son’s pediatrician. “There were things that did not go well for them, which we learned from and were able to do differently, partially because we knew what we did not want and partially because we had Rick to help us,” said Lord. “I saw firsthand the value of palliative care, and I wanted all parents in this situation to receive palliative care.”
She discovered then that what came to be called palliative care was a rarity in pediatrics, so it became her mission to spread the word and to help pediatric palliative care grow as a field. The Lord family started a small foundation, the Cameron and Hayden Lord Foundation, that the children’s grandparents funded initially and friends and family now support with annual donations. “With that funding, we promote pediatric palliative care programming and research, as well as medical research,” said Lord. She
wanted to do more, however, and in 2013 Lord founded the Courageous Parents Network.5 This nonprofit promotes pediatric palliative care and helps families hear and learn from other families who have gone through similar experiences, to be part of a supportive community, and to benefit from each other’s counsel in the way she and Charlie and Tim and Allison were able to do as a supportive foursome. “We use it as a platform for parents who have received palliative care to share their story with families who do not yet know about it,” said Lord. The goal, she added, is for families to understand its value, to ask for it, and say yes if it is offered to them. Too many parents, she said, think palliative care means hospice care and that they have to surrender all hope for their child.
After caring for Cameron and growing frustrated with some of the business changes affecting the way he practiced medicine, Goldstein left pediatric primary care and joined the emerging field of palliative care. “I knew some people who were early implementers, pioneers in the field, and liked them, liked what they were about, liked what they were talking about, and so I moved in that direction,” said Goldstein. Today, he practices palliative care at Boston Children’s Hospital and the Dana-Farber Cancer Institute, and as Lord put it, “is still working his magic with these other families.”
In closing their discussion, Berman asked Goldstein to explain what he views as the difference between primary and specialty palliative care. The skill set for primary palliative care, Goldstein said, “is and ought to be a generalist-enhanced, communication-relational kind of medical care that places a great premium on continuity of care and effective sensitive communication.” He went on to say that primary care clinicians in peoples’ lives are in an “extraordinarily powerful situation to do this very well.” Referencing the resource issue that not enough subspecialty trained pediatric palliative care clinicians are available in the workforce, Goldstein cautioned that they cannot and should not be dealing with every person who is sick and every person who is dying. But some seriously ill patients, he explained, some just have higher levels of needs based on their histories, symptom progression, and how medicalized their lives are after the diagnosis. To Goldstein, subspecialty palliative care—in addition to informing and supporting primary palliative care—has an important focus in that way.
As a final thought, Goldstein said he was grateful that this workshop included pediatric palliative care in its discussions. “We are a rounding error
___________________
5 For additional information, see https://courageousparentsnetwork.org (accessed May 2, 2017).
in terms of patient numbers in palliative care and in terms of costs and charges, but I think pediatric palliative care is important because the way we treat the sickest of our children reflects in very important ways on who we are as a people, what we choose to respond to, what we say is important and worth investing in,” he said. His reason for making that statement, he added, is that the Affordable Care Act contains an essential provision for concurrent care in children, which makes pediatric palliative care possible financially for many families. Eliminating concurrent care, he said, would have a significantly detrimental impact on the field.
The West Family’s Adult Care Experience
Susan West, volunteer for the Hertzberg Palliative Care Institute at the Icahn School of Medicine at Mount Sinai, had a different experience caring for her husband Doug, who was diagnosed with Sjögren’s syndrome and eventually died in 1995. Her experience did not feature consistent physician support such as the Lords received from Goldstein, but that changed when the Wests (featured in the photo on the following page) met Diane Meier, who was then a geriatrician and is now director of the Center to Advance Palliative Care and professor of geriatrics and palliative care at the Icahn School of Medicine at Mount Sinai.
Before coming under Meier’s care, Doug had been to countless doctors and had received one misdiagnosis after another. Sjögren’s syndrome, an autoimmune disease that primarily affects the body’s fluid-producing glands, is rare in men, and none of the physicians he saw were able to tell Susan and him what was causing his extreme pain. As his then-mysterious condition progressed, he developed osteoporosis in his upper back from the massive doses of prednisone he had been taking and was referred to Meier, who at the time was studying pain and osteoporosis. West remembers Meier mentioning palliative care at their first meeting with her and having no idea what she was talking about. “I just wanted her to help us so I just didn’t pay much attention to that word,” said West.
When Meier joined the faculty at Mount Sinai, the field of geriatrics was 1 year old, and she was charged with establishing a practice dealing with osteoporosis, which had been the subject of the research she had done as a Fellow at the Oregon Health & Science University. “When Doug and Susie came to see me, their story was the exemplar of everything that is wrong in medicine,” she said. “He was seeing 12 different doctors, and nobody had an answer. Everyone was sending him from one specialist to another . . . no

one was responsible. There was no quarterback.” By the time the Wests met Meier, Doug’s osteoporosis had progressed to a point where it was irreversible. Meier remembers Doug being in tremendous pain and profoundly fatigued. “I just could not help myself,” Meier said when recollecting what came next. “I was there as a subspecialist to help him with his bones, but I saw the gap [in his care] and I just had to step up, not because that was my role, because it was not.”
In caring for Doug, Meier went from being a subspecialist to a primary care physician. Her first step was to convene a meeting of all of the doctors treating Doug to get them all speaking to one another about how to plan for and coordinate his care. “Because there was no electronic health record, no one even knew what everyone else was thinking,” said Meier. West remembered that it was most distressing for her husband to have to repeat his story every time he was treated by a new physician or admitted to a new hospital. Meier, West recalled, “was the only doctor of all these doctors that held his hand.”
Meier drew some important distinctions between the Lords’ story and the Wests’ story. The Lords, she said, had a diagnosis from the beginning and knew exactly what to expect. “We had the opposite situation, with a complete lack of clarity about what was going on,” said Meier. “The uncer-
tainty was a key part of the suffering.” Even after he was finally diagnosed with Sjögren’s syndrome, no one had ever heard of it, and so no one understood why he had such terrible symptoms. “It would have been better if it was cancer because people would have been able to tell a story around it,” said Meier. She recalled that the lack of a diagnostic label caused Doug tremendous existential distress, and West said the outside world’s reaction to her husband’s mysterious illness caused her to close in on herself, lose herself in her work, and refuse most offers of help caring for her husband, who worked as a financial analyst throughout his entire illness and treatment.
Reflecting back on her experience caring for Doug, Meier described it “like sunlight through a magnifying glass that started a fire in me. It just aligned everything I had been thinking kind of unconsciously about what we have to do.” As it turns out, fortune favored the prepared mind, as she put it, because at that very moment the Soros Fund and the Robert Wood Johnson Foundation started providing funding for the new field of palliative care. With the Wests serving as a catalyst, Meier applied for funding and was able to change careers and become someone who Berman described as “a major force driving the field forward.”
Not long after Doug passed away, Susan was “dismissed” from her job at a publishing company, and she turned to Meier, who spent many hours stressing the importance of West talking to someone about her grief. Eventually, Meier asked West if she wanted to help in her department, and as time went on she was spending an increasing amount of time volunteering at Mount Sinai. Eventually, she endowed an annual lecture in Doug’s memory and to honor Meier. She also helped with a 10-year fundraising effort that enabled Mount Sinai to open a dedicated palliative care unit. Comparing what life was like before and after Meier introduced her and her husband to what is now called palliative care, West said the difference was tremendous and transformed the last 18 months of her husband’s life.
Berman synthesized key messages that emerged from the discussions with Lord, West, Goldstein, and Meier to reinforce what they talked about in describing optimal care:
- meaningful medicine
- transformation
- relationships and partnerships among the provider, the seriously ill person, and the family
- meeting clinical needs that are not being met
- helping patients and families with existential and spiritual needs and preparing them
“This is the range of what palliative care is and what good care for people who are seriously ill offers, and it is the thing that transforms life,” said Berman. As a person living with advanced breast cancer “who lives and breathes it every day,” Berman offered a tagline for palliative care: “the best friend of the seriously ill.”
Family Caregivers
The experiences of both the Lords and the Wests illustrate the central role of family caregivers to the overall success of care for a person with serious illness. The experiences also highlight the significant impact on the caregiver. In noting that she went to every doctor appointment with her husband, West wondered if that eventually contributed to being let go by her employer. In West’s words, she described feeling “beside myself most of the time.” Nearly 18 million individuals in the United States are family caregivers of adults aged 65 and older according to a 2016 report, Families Caring for an Aging America. The report noted that family caregiving can affect the mental and physical health of the caregiver, including depression, anxiety, stress, and emotional difficulties, and cause economic harm, including loss of income and employment opportunities. The report highlighted research that education and skills training aimed at supporting caregivers can have a positive impact on the quality of care delivered as well as improve the quality of life for both the caregiver and the person being cared for (NASEM, 2016).
A number of workshop speakers and participants also emphasized the critical role of family caregivers. Kimberly Johnson, associate professor of geriatrics at Duke University School of Medicine, for example, did so by describing two contrasting experiences with serious illness in her family. She explained that her maternal grandmother, who died before Johnson was born, lived in rural Mississippi and died in her late 30s from what was likely uterine cancer. Johnson’s aunt shared with her how difficult it was when her grandmother asked to be released from the hospital so that she could die at home. The aunt recalled for Johnson that “there was no help. There were no people who came to the house. No doctors, no nurses, no hospice.” The family, the aunt explained to Johnson, “just did the best that they could.” Johnson juxtaposed this experience with that of her pater-
nal grandmother, with whom she grew up. Johnson explained that her grandmother developed congestive heart failure 2 years before she died. Fortunately she had many daughters, Johnson pointed out, and in order to respond to her preference to be cared for at home, the daughters took turns moving in and caring for her; “and they did this in the setting of having their own families, so they were in an out of her home so that she could stay there,” explained Johnson. Her grandmother did enroll in hospice in the last 4 months of her life, and Johnson recalled how her “quality of life during that time was significantly better.” Ultimately, her grandmother was transferred to the hospital as she did not want to die in her home. Though hospice was available for her paternal grandmother, Johnson said she thinks “about how palliative care at the 2-year mark before death could have meant so much more time doing the things that were important to her at home.”
Shonta Chambers, executive vice president for health equity initiatives and community engagement at the Patient Advocate Foundation, stressed the need to consider the impact of serious illness on the caregiver as well as the patient. She noted that she speaks from personal experience, as she is a caregiver to her mother who has lived with multiple sclerosis for the past 22 years. Chambers shared that being a caregiver “has been an experience . . . one where I don’t fully understand what she is experiencing, but because she is mother, mother feels like I should be living my life” rather than having to take care of her.
Chambers emphasized the importance of ensuring that caregivers have the supports they need—be they emotional, spiritual, or financial, noting that serious illness has an impact on the entire family, and in many cases “threatens the very financial stability of the entire family,” as “once a chronic condition comes into play, everything gets turned upside down.” She pointed out that this is the case for all families, even those of means, but “it just becomes more financially toxic for those populations that are already very limited in their resources, already are experiencing disparities” in access to health and social services among other things. Chambers also emphasized the importance of engaging the caregivers in the conversations: “It is no longer just solely focusing on the patient, but all the surrounding pieces that you need to bring into play” to orchestrate care for the seriously ill.
Joy Buck, professor at the West Virginia University School of Nursing, highlighted the “exceedingly high” caregiver burden in West Virginia, and the intergenerational impact in a state where the expectation is that “kin take care of kin.” She noted that surveys she conducted revealed that children were taking care of family members throughout the state. Buck cited
one case of a 6-year-old who was caring for her grandmother who had chronic obstructive pulmonary disease. The child was told to call 911 if something happened to her grandmother. Buck also pointed out that in 2005, 22 percent of students who dropped out of high school did so because of family caregiving responsibilities (Bridgeland et al., 2006).
Karen Steinhauser, health scientist with the Center for Health Services Research in Primary Care at the Durham, North Carolina, Veterans Affairs Center and associate professor of medicine at the Duke University Medical Center, noted that “there can often be a gap between what we call objective burden or demands that are placed on a caregiver, and their own subjective experience of the extent to which they feel burdened, and those who have a stronger sense of meaning about the caregiver role have a lower sense of subjective burden.” Steinhauser pointed out the wide range of coping strategies and resources of caregivers; some people are able to meet those demands and adapt, whereas others are overwhelmed and have a difficult time meeting the multiple demands of caregiving. Steinhauser noted that “there are lots of fancy measures that can help us assess caregiver burden and where they are and we have also found that simply asking the single question: ‘Do you need help?’ works nearly as well as asking some of those burden questions in a clinical way.”
Rebecca Sudore, professor of medicine at the University of California, San Francisco, called attention to recognizing and providing support for the multiple decisions caregivers have to make: “I think oftentimes when we think about advance care planning, we think about one decision about end of life. But again, as a geriatrician, my patients and the family members that take care of them are making many decisions over time. People need support for that.”
For a person living with a serious illness, the ability to contribute to other people’s lives helps them make meaning of the situation, said Steinhauser, but part of making meaning for someone with serious illness can also involve letting others contribute to their care. Gwen Darien, executive vice president for patient advocacy at the National Patient Advocate Foundation, said when she received her second diagnosis of cancer several years ago, her 17-year-old stepdaughter wanted badly to help, but her response was always that she was fine and did not need any help. “I was supposed to be taking care of her,” said Darien. She soon realized, however, that allowing her stepdaughter to help was probably the best thing she could do to ease her mind. “So every day when she came home from school, she got into bed and held my hand while we binge-watched mysteries, and when I
was better, she went back to her life,” said Darien. “Allowing her to help me was as important as not being a burden to her because I would have been a bigger burden to her if I would not have allowed her to help me.”
Berman shared a similar story, asking her daughter, who has an accounting degree, to take over her checkbook. “That may sound silly, but that is the thing that is calming to her,” said Berman, who acknowledged that she does not like balancing her checkbook. “She knows that she is being a help to me. So even in these little, everyday things, the ways we can include families and give meaning to them that they are being supportive of a larger aim, which is making a transition to a time without us a little bit easier,” Berman explained. Lord expressed it in this way: “What we have to hold onto after is what our role was when we cared for them . . . feeling like you have done the best you possibly could in the face of this serious illness—regardless of who the loved one is—is what you hold on to after.”
EXPANDING ACCESS TO PALLIATIVE CARE
Many of the workshop panelists’ remarks underscored the IOM’s Dying in America report’s findings about the value of integrating palliative care with disease-directed treatment. The report found that “Ideally, health care harmonizes with social, psychological, and spiritual support” to achieve the highest possible quality of life for people of all ages with serious illnesses and that “a palliative approach can offer patients and families the best chance of maintaining the highest quality of life for the longest possible time” (IOM 2015, p. 45).
Palliative care as a medical specialty6 has been one of the fastest growing fields in the U.S. health care system over the past decade (Center to Advance Palliative Care, 2015; Hughes and Smith, 2014), and numerous studies have shown that palliative care benefits patients, caregivers, and clinicians (Gomes et al., 2013; Kavalieratos et al. 2016) while also reducing costs (Morrison et al., 2008, 2011; Payne et al., 2002; Smith et al., 2014). For the most part, these studies refer to specialty palliative care delivered by clinicians such as Goldstein and Meier, who work at medical centers and large hospitals, yet as the IOM report underscored and workshop panelists reinforced, trained palliative care specialists remain in short supply (Kamal
___________________
6 The field of Hospice and Palliative Medicine was officially recognized as a subspecialty by the American Board of Medical Specialties in 2006 and the American Osteopathic Association in 2007. See http://aahpm.org/career/certification (accessed May 2, 2017).
et al., 2017). Consequently, many seriously ill patients and families rely on the services of other clinicians who provide medical care, but may lack training and experience necessary to meet their individual palliative care needs for maximizing quality of life. Recognizing these challenges, workshop speakers described efforts to accelerate the expansion of palliative care’s reach to all communities where the majority of seriously ill adults, infants, and children receive their care. Such broadened access will require dedicated commitment to developing primary palliative care skills and reliable payment mechanisms for deployment of those learned skills across the entire workforce.
From Goldstein’s perspective of having been both a primary care provider and a specialist, leaving all of the responsibility for providing palliative care to a specialist misses a valuable opportunity. “The power of primary palliative care,” he said, “is that it puts the primary care clinician in an extraordinarily powerful position to work as a team with the patient and family to put the patient and family at the heart of care and provide the highest possible quality of life for a seriously ill individual.” Because palliative care has no one-size-fits-all approach, the clinician who best knows a patient’s medical condition and life circumstances and who has most likely developed a trusting relationship with the patient—the primary care provider—is in an ideal position to craft a care plan that meets the needs and desires of the patient and family and coordinate delivery of that plan. Terry Altilio, social work coordinator at Mount Sinai Beth Israel Medical Center, pointed out that many people do not have a primary care provider and will never have the continuity of care and the type of relationship with a clinician that the Lords and Wests had with Goldstein and Meier, respectively.
Clinicians outside the palliative care specialty field are stepping up to fill these gaps, Goldstein acknowledged. “There are plenty of people who as a matter of their own character step into this space,” he said, and “I do think that they touch a lot of lives.” An anecdote provided by Marian Grant, director of policy and professional engagement at the Coalition to Transform Advanced Care, illustrated Goldstein’s assertion that primary palliative care is growing. Several weeks earlier, she attended a symposium on palliative care sponsored by the Lehigh Valley Health Network, where 150 people were in attendance, most of whom were not palliative care providers. In fact, one attendee was a 65-year-old completing a fellowship in palliative care, after having practiced primary care for decades.
Although such examples are encouraging, Meier pointed to another reality: The reality today is that “we pretty much abandon people [when
they would benefit from palliative care] because what gets paid for is hospital care, ambulances, short-term home care, and hospice if you are predictably dying soon, but the great majority of people with serious illness are not predictably dying, and live for years with serious illness, functional decline, and high caregiver burden. They are not hospice eligible7 and are pretty much out of luck unless they have money and can pay out of pocket for the support they need. That is the truth, and it is appalling.”
Meier believes the ability of health care systems to provide palliative care is significantly affected by what is and is not paid for by insurers, particularly Medicare and Medicaid. “Some of us have philanthropic dollars we use to pay for chaplains, and chaplains do a lot of this work. Social workers do a lot of this work, too, if they are not wholly subsumed in discharge planning, but I would say that our system has evolved to a point where if it’s not ‘medically necessary’—and a lot of psychosocial and spiritual care does not count as medically necessary under Medicare reimbursement—those things are honored in the breach, not because they are not important, but because we cannot find reliable ways to pay for them,” Meier observed. The one possible exception to that situation is with pediatric palliative care, said Goldstein, who added, “I think that maybe there is a different kind of investment in a children’s hospital and the focus on the family allows that.”
Meier suggested that one way to address the lack of universal reimbursement for palliative care is to get the public to demand it as a key aspect of optimal care. “We need a public awareness campaign that makes the public angry if they are not getting it,” said Meier. Lord seconded that idea and noted that she has met some very angry parents who were either referred to palliative care too late or who were never offered it. “Finding a way to harness that anger in a way that is activating would be good,” said Lord.
Jeff Cohn, medical director of Common Practice, pointed out that reducing existing barriers may be as important as increasing people’s ability to demand the care they need and deserve. “The reason why so many of us feel as though we are not empowered is because we are going up against a brick wall or something that is imposed by the health care system,” he said. That brick wall affects both patients and providers, he said, and providers
___________________
7 The Medicare hospice benefit defines hospice eligibility as appropriate for patients once two doctors have provided a prognosis of 6 months to live if the disease follows its usual course, the patient has decided to forgo disease-modifying treatment in favor of palliative care for comfort, and the patient has signed a statement choosing hospice care over other Medicare-covered treatments for the terminal illness (CMS, 2016).
have the responsibility to make it clear that they need time to talk and listen to patients and build relationships with them. Ellen Goodman, founder of The Conversation Project, added that creating the time and space for conversation will not only benefit patients and their families, but providers, too. “If the clinician does not feel like they have some measure of control over the work they do,” she said, “it is a lousy way to live.” Nick Jehlen, founding partner at Common Practice, added, “There is no more powerful force for change than for somebody to believe that they are doing the job that they got into health care to do. It is a magical moment to watch a nurse provide care that she knows a patient really wants.”
Consistent Messaging About Palliative Care
Many of the first session speakers noted that palliative care access will continue to increase as the public becomes more aware of its benefits, boosted by consistent use of language describing the services that is understandable to patients and families and emphasizes the benefits they want (see Box 2). For example, when a referred patient asks Meier what she does, she draws on this consumer-tested description to explain that the patient’s doctors asked her to see what she can do to help improve that person’s quality of life and add an extra layer of support for both patient and care-
givers. That, said Meier, is audience- and research-tested language that is understandable, meaningful, and valuable to patients and family members (Center to Advance Palliative Care, 2011). “It is not about what we are not going to do, it is about what we are going to do alongside a patient’s regular doctors at their request,” she said. The language also clearly conveys palliative care’s focus on maximizing quality of life.
Drawing on his experience in pediatric practice, Goldstein elaborated on Meier’s description, explaining that “In the face of serious illness, you have many specialists, admirable people who devote their lives to a part of the body, an organ, a lung, a kidney, a liver, but livers do not suffer, and parents do not parent livers. You need somebody who, in addition to doing everything that they can for those small parts, steps back with you and looks at the whole experience and makes sure that at the end of whatever happens, you’ve met your sacred obligation to your child to be a parent in the face of illness.” His message to parents is that while they may feel less qualified to be a parent given how ill their child is, his job is to make sure they are the most qualified people in the room to advise the medical team and make the difficult decisions that may lie ahead.
Both Meier and Goldstein view palliative care as a means to start a conversation with patients, parents, family members, and other caregivers, for conversation and dialogue are essential if patients and caregivers are to be active participants in providing the best care possible for those facing serious illness. Conversation and dialogue are also needed to understand how patients and families prefer to receive their medical information, and to provide the emotional, social, and perhaps even financial support that caregivers need as they face the demands of providing care for someone with a serious and often chronic illness.
Developing Primary Palliative Care Skills
Drawing on learned communication skills to explore what a patient facing serious illness really wants is critically important, explained Anthony Back, professor of oncology at the University of Washington and Fred Hutchinson Cancer Research Center and co-director of the Cambia Palliative Care Center for Excellence. Back recounted how as a young oncologist he learned not to tell patients too much about what was going to happen to them, and his experiences dealing with patients under those circumstances left him wondering if he could keep practicing medicine in that way. Today, however, he knows there is a different way to talk to patients. Recently, for
example, he saw a patient with metastatic pancreatic cancer, and he started his conversation with this man by asking what was important to him. The man responded that he wanted to go home. Since he had finished his clinical trial, Back sent him home. One week later, Back received a picture in the mail of his patient and his family fishing on the Snake River. “His family now has these amazing memories of hanging out with him in the water catching fish,” said Back. This experience was in contrast to Back’s earlier patient interactions because he did not know enough at the time to ask them what was most important to them.
Back pointed out that too many physicians still feel uncomfortable talking with their patients about values and goals. Back highlighted findings of the 2016 survey by The John A. Hartford Foundation, Cambia Healthcare Foundation, and the California Health Care Foundation (PerryUndem Research/Communication, 2016). The survey asked 736 physicians practicing in the United States about advance care planning, and while nearly all doctors thought it was important and three-quarters said it was their job to do so, only 14 percent actually undertook advance care planning and billed Medicare. This finding revealed clearly the “huge disconnect between what doctors think they should be doing and what they actually do,” Back explained.
Back noted that even when physicians do initiate conversations with patients about values and goals, they do not necessarily do it well. Back shared an example of some of the words doctors actually used that came from a study he conducted among oncology fellows (Larrieux et al., 2015). “They say things like, ‘Do you want us to do CPR? I mean, pump on your chest like you might have seen on TV, if your heart stops?’” In Back’s opinion, “that is what happens if you have a rule that says we are going to pay you to do this, and you send an untrained physician in there to do it. This is what they are going to say. It happens a lot right now.” The physician will then compound their initial error, explained Back, by continuing to talk, reciting medical facts while the patient becomes increasingly upset, because patients’ emotional responses can make physicians uncomfortable. “The best thing they know how to do is to just keep talking,” said Back.
Physicians cite a number of reasons why they avoid having these conversations with seriously ill patients. Two-thirds say they do not have the time, 60 percent say they are not sure the time is right, and 46 percent are unsure of what to say. This may be because 68 percent of physicians report they had no formal communication skills training on how to talk about care for serious illness (PerryUndem Research/Communication, 2016). In one
study, James Tulsky and colleagues found that oncologists at two large academic medical centers that provide cancer care made empathic statements in only 11 percent of their conversations (Tulsky et al., 2011). “This is not about being nice because there are data showing that if you as a physician respond to emotions from people, they retain more of the information you are trying to tell them,” said Back. “This is about compassion, but it is also about doing your job and getting the information across.”
Back explained that communication training now typically relies on residents watching PowerPoint presentations that are not effective in helping them to learn essential conversational skills, “so they leave their training feeling like emotion is a threat. What they do is they say the patients are not ready. It is not okay.” Back estimated that some 2 million patients with serious illnesses are at risk of dying this year and every year. “That is the magnitude of the problem we are facing with clinician training,” said Back. “That is the number of patients who are at risk every year because they do not have a clinician who can conduct a good conversation or they have a clinician who does damage with their conversation.” Referring to Goldstein and Meier, Back said, “You saw two masters who taught themselves how to do it, like we all have taught ourselves to do it. It takes a while, and it probably took me 20 years to learn how to do this. The question is, can we afford to wait that long for the next generation of physicians to learn these skills? Of course not.”
ADDRESSING SOCIOCULTURAL DIFFERENCES AND NEEDS IN UNDERSERVED COMMUNITIES
Despite increasing evidence as to the benefits of palliative care, many individuals and families are unaware of it, do not know how to access it, or cannot afford it, explained a number of speakers at the workshop. These speakers included Shonta Chambers, Kimberly Johnson, and Stacy Fischer, associate professor of general internal medicine at the University of Colorado School of Medicine. For some individuals and families, particularly those in rural and underserved communities, the societal context is a barrier to receiving appropriate care for serious illness. As an example, Chambers noted that some communities lack easy access to medical care, so individuals will have to take a day off from work, with no pay, and spend hours on public transportation to receive medical care for themselves or a loved one.
For many vulnerable populations, the complexity of health care is a barrier. Low literacy and low health literacy, for example, negatively affect
an individual’s ability to engage with the health care system, let alone access palliative care (NASEM, 2016). Moreover, individuals with disabilities who attempt to participate actively in their health care are often confronted by environmental and structural barriers, as well as cultural orientations that result in their experiencing undertreatment as a form of discrimination because “people assume they don’t have quality of life,” noted one workshop participant. Moderator Bob Bergamini, medical director for palliative care at Mercy Clinic Children’s Cancer and Hematology and representing the Supportive Care Coalition, agreed. He noted that “children with disabilities also find an incredible number of assumptions, presumptions, and biases against them” that result in lack of attention to their suffering and discomfort.
As several of the workshop’s presentations made clear, geographic location, culture, and ethnicity play important roles in determining how to talk to individuals about palliative care; how different individuals and families will react to the offer of palliative care or hospice; how families will be engaged in the care of their loved ones; and what access they will have to palliative care. Rural patients, for example, may live hours from a medical center with a palliative care program, and inner-city patients might spend just as long taking public transportation to get to a program in their area. However, as Chambers noted, making a program physically accessible does not mean people will necessarily take advantage of it because they may, in fact, not know about it. “We have to be intentional and deliberate in our approach to make sure that those populations across this country that are the most vulnerable have a direct pipeline to connect with us,” said Chambers.
Chambers pointed out that the Patient Advocate Foundation realized that reaching individuals in underserved communities would require a variety of approaches that reflect not only geographical differences, but differences in racial and ethnic perspectives. “We have to understand the context in which people live their lives,” she said. “We have to ask them what is important in the context of their health in their community.” From that, she said, “we take the message that we want to communicate to them, and we tailor it in a way that is reflective of what is important to them and move it forward.”
In addition, considerations about health insurance, transportation, and inability to access screening services during working hours because of employment or other constraints, Chambers said, are also “very much a part of the social context in which individuals across our country are making their health care decisions every single day.” Chambers stressed the criti-
cal importance of uniting all of the community human and social service organizations with the medical systems, while inviting racial, geographic, and ethnically diverse populations to the table to talk about how they want to receive the support and services they need. If we come out of our silos to realize the true value of our collective impact, she said, “Only then will we truly begin to see the disparities in our country subside.”
Improving Quality of Life and Health Outcomes for Latino Populations
Stacy Fischer learned the importance of appreciating cultural values and integrating them into care when she conducted focus groups on serious illness care with Latino patients at patient centers and clinics in Denver. Discussions with these groups revealed serious gaps in understanding about serious illness care, particularly issues related to advance care planning. One finding, for example, was that Latino patients who had been admitted to the hospital within the previous 24 hours and who should have been counseled on advance care planning were much less likely than other patients to understand what an advance directive was or even remember having been counseled. On the other hand, when they did understand, they were actually more likely to have completed an advance directive. Another finding revealed interesting interactions between income and ethnicity. For example, the poorest group of Latino patients—those earning less than $15,000 per year—were more likely to report they were satisfied with pain management, while only 20 percent of Latinos making more than $30,000 per year were satisfied with their pain management. The opposite pattern held true for white patients (Fischer et al., 2015). However, an examination of subjective reports of pain revealed that the pain level was about 4.5, with 10 being the highest. “Clearly, people’s experiences, perspectives, and expectations were different, and we need to address that,” said Fischer.
In conversations with some of the Spanish-speaking focus groups involved in her research, core values repeatedly were raised. For example, family was incredibly important in every aspect of care, as were trust and personalization. “A pamphlet was not going to do it,” said Fischer, who added that a doctor’s appointment was more than just a clinical encounter to these individuals; rather it was about establishing rapport and finding connection. One barrier to seeking palliative care was the direct translation of “hospice” to hospicio, which translates directly as orphanage, a place where people are left when family can no longer care for them, or nursing
home, as well as the notion of fatilismo, the belief that nothing can change one’s destiny or fate and that doing something could hasten the bad things that were destined to happen.
From these conversations, Fischer and her colleagues designed Apoyo con Cariño, which roughly translates to Support with Caring, a patient navigation intervention to improve palliative care outcomes for Latinos with advanced illness. This intervention was based on the pioneering work of Harold Freeman at Harlem Hospital Center in New York City. He showed that navigation services dramatically improved outcomes for breast cancer patients of low economic status, 94 percent of whom were African Americans (Freeman and Rodriguez, 2011; Oluwole et al., 2003). In this case, Fischer and her colleagues conducted a randomized controlled trial involving 223 Latino adults 18 years or older who had some form of advanced cancer (Fischer et al., 2015). The intervention group received culturally tailored and linguistically appropriate materials covering advance care planning, pain management, and hospice care, plus a home visit from a patient navigator. The control group received only the written materials. The navigators, all of whom were bicultural, bilingual, and members of the community served by this intervention, conducted culturally tailored discussions grounded in core Latino values and informed a partnership with a community advisory panel. Some of the home visits were scheduled for the evenings and on weekends so that family members who might be working could participate.
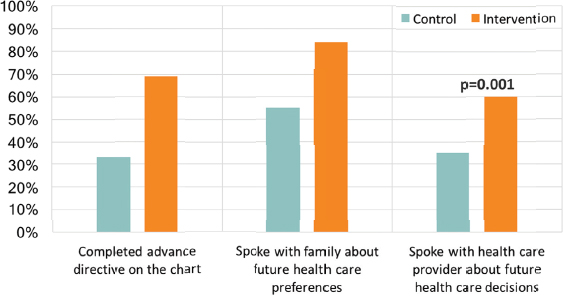
This intervention proved to be quite effective, said Fischer. Nearly 70 percent of those receiving the intervention had a completed advance directive in their medical record compared to 32 percent of the control group. More importantly, she said, over 80 percent of the intervention group reported speaking with family members about future health care preferences and 60 percent had that discussion with a health care provider, compared with fewer than 60 percent and just over 30 percent, respectively, in the control group (see Figure 1). Scores on pain management did not differ significantly, though they were lower in the intervention group, and both groups reported their pain level was low overall (Fischer et al., 2015).
In considering scores related to quality of life, there were statistically significant differences in physical symptom burden, and overall the members of both groups reported high scores on emotional and existential measures and the support they received. When asked about their perspective on hospice care, the differences between the two groups were quite significant. Nearly 90 percent of the intervention group said they would
SOURCE: As presented by Stacy Fischer, December 15, 2016.
recommend hospice for a loved one or would use hospice themselves in the future, compared with about 65 percent in the control group (Fischer et al., 2015) (see Figure 2).
The Experience of African Americans with Serious Illness
Raising awareness about serious illness care and building trust and connections as Fischer described are equally important in addressing health disparities that lead to poorer outcomes in African American communities, noted Johnson. She referenced the IOM report Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care (IOM, 2003) and reflected on the data demonstrating that compared with whites, African Americans receive lower-quality care across a number of diseases and care settings. She stressed that those differences have real consequences. Compared with whites, she said, African Americans are less likely to have their pain adequately assessed or treated across symptoms for whatever reasons. They are also more likely to report difficulties with provider communication, she continued, and less satisfied with the quality of that communication. To further illustrate her point, Johnson recalled a conversation in which her grandmother talked to her about these disparities. She said, “You
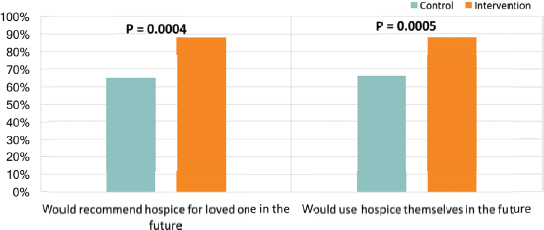
SOURCE: As presented by Stacy Fischer, December 15, 2016.
grew up here and so you know that ‘Black folks’ have a lot of problems. We cannot get good care for anything we have and so why would you not be trying to figure out how you could actually keep us from getting the many medical problems we have or actually making us live longer and getting the right treatment for those things?”
For Johnson, a thoughtful response to her grandmother’s question and the vexing problem of disparities requires thinking about equity throughout the continuum of illness, starting with disease prevention and appropriate treatment. It also includes efforts to improve interactions and experiences of serious illness care at that other end of the spectrum that ensures that the kind of care people receive is reflective of their goals, values, and beliefs. “There are unmet needs among African Americans no matter where you look in the health care continuum and certainly serious illness and end of life are no exception to that” explained Johnson. Even when the kinds of conversations occur about treatment preferences that we all believe should happen, she said, African Americans are also still less likely to get the kind of care they want. Equity is a key quality care domain, Johnson explained, and it requires ensuring that people receive the highest quality care “no matter where they are in the continuum of illness, no matter what they look like or what other personal characteristics they may have.”
Despite increasing enrollment in hospice services, Johnson explained that the rate of hospice use among African Americans is lower than that among whites and has remained constant over time (see Figure 3). Johnson’s primary research focus has been on hospice use in African American com-
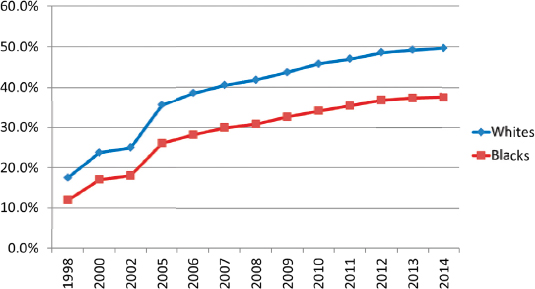
SOURCES: As presented by Kimberly Johnson, December 15, 2016. Data from Medicare Payment Advisory Commission, 2016.
munities. The lessons learned from this work, she said, can also help to inform how we raise awareness and bring palliative care upstream in this population. For example, we know that knowledge is power, Johnson said, and exposing these populations to information about hospice generates more positive attitudes toward the use of hospice so they would be more likely to use it in the future. We also know that African Americans are more likely to want life-prolonging therapies even in the face of a poor prognosis, although that number is only a minority of them, she clarified, so it is important that these populations understand that palliative care is not related to giving something up. Respecting the fact that there are individual beliefs, preferences, and treatments, she said, it is helpful to explain palliative care as therapy that makes one feel better, helps and supports one’s family, and can be provided alongside and in addition to life-prolonging therapy.
Although there are materials designed to raise awareness specifically among African Americans, care providers are in the position to have the strongest effect by improving their ability to communicate with and listen to patients and families. “The fact is that when you are seriously ill, health care is not the only thing you need, and for African Americans who have lower income and fewer resources, those same challenges that they face in
getting food, clothing, and shelter are only magnified in the setting of serious illness when someone can no longer work,” Johnson underscored, “so we have to think about providing care that addresses all of those things.”
Targeting places where people live, work, and worship can also serve as a means of raising awareness and providing services in the African American community. The Visiting Nurse Service of New York developed Harlem’s Hospice Outreach Program Effort, or Project HOPE, to target medical professionals and potential hospice patients in Harlem and the surrounding area to overcome barriers that prevent African Americans from getting better end-of-life and serious illness care. Beauty and barber shops in urban areas are also serving as conduits for health information in African American communities. Duke University, said Johnson, has developed a program that churches can use to educate their congregations about advance care planning and serious illness care.
The University of North Carolina, said Johnson, created a program called Circles of Care that helps organizations in the African American community to assemble care teams. The lay members of these care teams receive training to provide practical support, such as getting patients to their appointments, and information on advance care planning and hospice. “This program has been shown to be quite effective in improving quality of life and accessing the everyday things people need, whether they are seriously ill or not,” said Johnson. She noted two programs that were effective, but no longer exist because of funding cutbacks: Balm in Gilead and the Harlem Palliative Care Network. Both programs were based on the idea that it takes a village to care for someone with a serious illness, especially when they have lower income and fewer resources. The common thread between these two programs was that they included partnerships among health care institutions, home care providers, community service organizations, faith communities, and social service organizations. “They were successful because they were able to coordinate care over all of the domains that we care about,” said Johnson. As a closing call to action, Johnson urged the importance of developing systems that are “flexible enough to provide equitable care to people no matter what they look like, where they live, what they have, and what they do not have.” Johnson ended with Martin Luther King, Jr.’s quote, “Of all the forms of inequality, injustice in health is the most shocking and inhumane.”
Community Engagement Strategies in Rural Communities
The importance of developing strategic opportunities for community engagement and professional capacity building was explored by Joy Buck, who described specific initiatives she has undertaken in West Virginia to improve access to health care for rural communities. Buck described the “reality” in West Virginia, a state in which the health status of the population is very poor; the state comes in last in terms of patient outcomes in areas such as diabetes, heart disease, hypertension, preventable death, and preventable hospitalizations.
Buck explained that many people in their 30s and 40s are experiencing serious illnesses that “should be chronic and people should be living with for a very long time, but they are not.” Most of the programs in West Virginia are designed for people who are aging. While the state does have one of the oldest populations in the nation, Buck explained, the issue is that “the next generation is not going to get there” because they are dying at much earlier ages.
Bridges to Healthy Transitions, the research initiative housed in a regional medical campus in the eastern part of West Virginia that Buck developed, takes a community orientation approach using palliative care’s domains as a quality framework. It focuses on primary and secondary prevention to help take care of the next generation, working to translate primary palliative care into standard practices. Buck explained that the program builds on work she had done with HIV and AIDS in the 1980s. The program works to develop capacity at the community level and at the professional level and then establishes connections or bridges between the two. Through community partnerships, collaborations, and volunteer networks, such as Meals on Wheels, for example, the program has provided home assessment and primary palliative care training to the people closest to the seriously ill population, namely, she said, “the people they feel the most comfortable talking with about these things.”
Buck described several studies she has been involved in that seek to translate palliative care science into tailored interventions at multiple levels (see Table 1). One project, Building Capacity for Rural Integrated Palliative Care, supported by the National Institute of Nursing Research (NINR), for example, found that a major issue for patients is that they are often not given the tools to help themselves even though their preferences are for self-management. Another key theme is the significant impact of the caregiver burden on family members, and the common concern on the part
TABLE 1 Projects to Provide Advance Care for Rural West Virginians with Serious Illnesses
| Projects | Focus |
|---|---|
| Building Capacity for Rural Integrated Palliative Care (1 R15 NR012298-01) | “Give me something so I can help myself” |
| “Do I have to die so my daughter can have a life?” | |
| “They don’t listen; they don’t hear me” | |
| Building Bridges to Integrated Palliative Care: A Lay/Interprofessional Educational Collaborative | Organization of care; communication; symptom assessment and management |
| Educational intervention, toolkits, visit structure and processes | |
| WV Elder Transitions in Chronic and Advanced Illness | WV PEL and Senior Center CNA Training Programs for High School Students |
| HSTA projects exploring child caregiving in West Virginia | |
| University Healthcare CHNA Cycle 1 and Cycle 2 | Bridge to community transformation initiative (Public Health) Shift and investment in community-based recovery programs; harm reduction Leadership/maximizing synergy among diverse community initiatives |
NOTE: CHNA = Community Health Needs Assessment; CNA = Certified Nursing Assistant; HSTA = Health Sciences and Technology Academy; PEL = Partnership for Elder Living; WV = West Virginia.
SOURCE: As presented by Joy Buck, December 15, 2016.
of people living with serious illness with what is happening to their family. Finally, patients often talk about something they used to be able to do but can no longer do, and this may be an indication of functional decline and/or disease progression. Buck explained that her team integrated these “three important clues” into their lay/interprofessional education collaborative, which worked with a skilled nursing facility and a primary care center. The collaborative developed an educational program and toolkits to target two key areas: communication, and symptom assessment and management.
Buck described projects, including the Elder Transitions in Chronic and Advanced Illness Project, which developed the high school curriculum for a certified nursing assistant educational program designed to build skill sets for young people that would also help meet community health needs. Finally, the Community Health Needs Assessment project focused on developing increased capacity to address behavioral health needs in the community.
In describing the community assessment initiatives and bridges to informal care networks established in her state, Buck underscored the importance of understanding and addressing medical, nursing, and social work subcultures in respectful ways. She also discussed the impact of payment policies on access to care, noting that “we look for reimbursement, but there is always going to be this gap. People keep falling through the cracks in between those regulatory barriers.” She explained that they attempt to collect cost data as part of their research studies.
Noting that she is a historian by training, Buck closed her presentation with one of her favorite quotes from Albert Einstein: “We cannot solve our problems with the same thinking we used when we created them.” She left the workshop participants with the question: “What are we going to be doing differently this time?”
ADDRESSING SERIOUS ILLNESS IN PERINATAL AND NEONATAL CARE SETTINGS
Lessons learned about the delivery of palliative care in perinatal and neonatal care settings, building relationships, and honoring ritual as key components of serious illness care were highlighted by Kathy Kobler, advanced practice nurse coordinator in the Center for Fetal Care and Pediatrics Palliative and Supportive Care programs at Advocate Children’s Hospital in Park Ridge, Illinois. Perhaps no serious illness setting has a bigger impact on a family than when that illness affects an unborn child. “Within the United States, we are seeing a growing trend of perinatal palliative care programs to specifically address the needs of those families who hear before birth that their baby may not live long,” noted Kobler. She explained that these programs are available at both academic medical centers and community-based health systems, and that a survey of these programs found that every one of them administered both to the physical needs of the newborn and to the spiritual and emotional needs of the family members (Denney-Koelsch et al., 2016). “What we see come through loud and clear
about these programs is that it is an interdisciplinary team approach,” said Kobler. “Many of these programs have coordinators of care that are often nurses, chaplains, or social workers who become that key point person, that navigator for the family as they take in medical information and then make decisions.” Some 82 percent of the 75 programs surveyed, she noted, have a team member available around the clock to meet parents’ needs (Denney-Koelsch et al., 2016).
Kobler cited a study showing that these programs can help parents who receive a prenatal diagnosis of a lethal fetal condition work through their experience so that they would not have regrets regarding how they had cared for their child (Cote-Arsenault and Denney-Koelsch, 2016). These parents expressed the need for help in understanding the extent of their child’s medical conditions and what it will mean for that child to live well, even for a very short time. As Kobler explained, these families made clear “that they want time to be connected in relationship, to prepare, and to be able to advocate” for the baby with integrity.
To meet that expressed need, Kobler and her palliative care colleagues around the country are working to establish a relationship with the medical care team early in the prenatal process. “Some of these babies, after they are born, are going to need medical care for quite some time, and being able to introduce the parents and families to their pediatric team members, giving families those options before the babies are even born, to connect with the pediatric team, to engage in a relationship,” is important, she said. The general approach is to establish an open and supportive dialogue with the parents to assess what the pregnancy means to the parents, how they understand the baby’s diagnosis and what it means with regard to prognosis, and what the parents’ expectations are for their baby’s care. These conversations, said Kobler, aim to understand the cultural and spiritual beliefs that may affect a family’s decision-making process and identify those support systems available to the family outside of the prenatal palliative care environment (Boss et al., 2011; Kobler and Limbo, 2011; Munson and Leuthner, 2007).
Kobler and her colleagues work to co-create goals of care that reflect the parents’ preferences for their baby’s care, a process that involves the entire care team working together over the course of the baby’s lifetime. This extended conversation, Kobler explained, helps the family weigh treatment benefits and burdens in determining what is in the baby’s best interest and recognizes that decisions may change as the baby’s life unfolds. She also noted that her team works to address the needs not only of the parents, but also of those big brothers and sisters who are waiting to welcome those
babies into the family. One thing Kobler has heard from expecting parents who have received a serious illness diagnosis for their unborn child is that there are more than enough people talking about their child dying, but no one to talk to about the child’s life and the family’s life.
These conversations by themselves can help parents cope during the pregnancy, but they also serve as the foundation for a plan of care. At the Center for Fetal Care, every family has opportunities to speak with a neonatologist who can provide a holistic view of the baby’s care needs (Miquel-Verges et al., 2009) and with pediatric specialists to discuss options for interventions specific to the baby’s condition. The Center also crafts an individualized plan for education, lactation, and sibling support. Kobler then disseminates the care plan to ensure that every care team member is aware of what the parents believe is important to them and what their hopes are for the care of their child (Loyet et al., 2016). At the same time, a care team member is designated as the primary contact person for the parents and family members.
Kobler cited a study that found that mothers who know their babies may not live long after delivery have simple goals: to shelter their babies from as much suffering as possible, to nurture them in the same way they would if their child were healthy, and to socialize and share their babies with others (Limbo and Kobler, 2013). She noted that these final acts are important to parents after their baby’s death, suggesting that parents should have every opportunity to care for their babies in ways that are normal and natural to them and again pointing to the importance of integrating the family’s desires in the child’s care plan.
When developing the neonatal portion of the care plan, Kobler speaks with parents about their overall goal of care for labor and delivery, the preferred site and mode of delivery, and what type of medical interventions, if any, they want available for their baby. Parents also talk about whether they want other family members present and if they want the delivery recorded or accorded some culturally or religiously important ritual. They develop a communication plan for how they want to let family and friends know about their child after birth. Kobler also works with the labor and delivery staff, and the neonatal intensive care unit (NICU) and postpartum teams to help the parents prepare for the birth of their child. “Sometimes, all of a baby’s care happens right in the parents’ arms and they never go to a neonatal setting or regular newborn nursery,” said Kobler. She and the care team also talk with the parents about what it will mean if the baby continues to survive and thrive after the mother is ready to go home from the hospital.
In some cases, the baby can go home, and community palliative care teams provide in-home support for the baby and family. Some parents can and want to discuss what happens if their child does not live long, she added.
Once the baby is born, the care team’s approach is to let the baby lead the way. “We have made the best guesses ahead of time and tried to make plans, but we want to let the baby lead the way,” said Kobler. “We are constantly assessing and refocusing with families, all within a family-centered approach, to honor their wishes and preferences along the way.” She recounted a conversation she had just prior to the workshop with a family that was in the process of taking in the scope of their newborn son’s serious illness. The mother looked at her and told her that she was trying to make decisions for her son in a way that would reflect his desires if he could make them known. “That became a theme then as we continued our discussions and interactions together,” she said.
One aspect of prenatal palliative care that interests Kobler is the role of ritual and the honoring of meaningful moments. “We all have a deep human need to want to make sense and to acknowledge when important things happen in our lives,” she said. In her experience, ritual can be transforming for the parent, the family, and the child, as well as for the care team. In one instance, a nurse on her team listened closely to a parent who was anticipating having her baby home by Christmas, which the nurse knew was not possible. But also knowing how important the Christmas time was to the mother, the nurse organized Christmas for the family in the hospital, complete with ornaments bearing their child’s footprints. In other cases, ritual can mean reading special books to the child. “I think of one mother who read Goodnight Moon over the phone to her baby in the NICU and to her other children at home,” said Kobler. “When it came time for the baby’s end of life to unfold, the family brought in their dog-eared copy of Goodnight Moon to read as the ventilator tube was removed, except they changed words and said ‘Goodnight NICU, goodnight beeps and buzzes, goodnight nurses that we love.’”
Kobler made a point of recognizing her colleagues, the physicians, nurses, chaplains, social workers, child-life specialists, and lactation consultants who work with these families. “Our goal is that we can help them find that centered place in the middle of the storm,” she said. Kobler noted, though, that the team members asked her for some ritual they might use to help them cope with the challenges of working with these families. “We asked them to ground themselves by holding onto something in the unit, and guess what they held onto?” she asked. “Each other.”
ADDRESSING IMPAIRMENTS THROUGH THE INTEGRATION OF PREHABILITATION AND REHABILITATION SERVICES
Two other aspects of quality care delivery for people facing serious illness are rehabilitation and prehabilitation. These two services focus specifically on addressing impairments to reduce disability and restore function for individuals with serious illness. Julie Silver, associate professor and associate chair, strategic initiatives at Harvard Medical School’s Department of Physical Medicine and Rehabilitation and Spaulding Rehabilitation Hospital, recalled that when she went through breast cancer treatment she became sicker and sicker as treatment progressed. Finally, when the treatment ended and she was sicker than she had ever been, her oncologist said, “Okay, you are done. Try to heal yourself.” Chemotherapy had eliminated her cancer, but left her with significant impairment. However, her doctor offered her neither palliative care nor rehabilitation therapy. “I had to figure out how to fix all of these different things, and I can tell you that general exercise did not fix them.”
The point of that short story, she explained, was to illustrate how important it is to screen patients for impairments. “We need to identify them in order to treat them so that patients have better outcomes, because impairments are often very predictive of disability,” said Silver, noting that impairment is what shows up on an exam and disability is what someone cannot do because of that impairment. Impairment-driven rehabilitation, she explained, focuses on a specific problem.
Physiatrists such as Silver are medical rehabilitation specialists who for the most part treat people with serious illness, and she recommended that palliative care teams include the support of rehabilitation professionals to help them address unnecessary suffering (Silver et al., 2013), particularly given that most hospitals have a rehabilitation department and that rehabilitation services are covered by insurance. In addition, she said, physical and functional problems that negatively affect quality of life can be addressed by rehabilitation (Banks et al., 2010; Penttinen et al., 2011; Weaver et al., 2012). “We know that when people feel better physically, their quality of life improves,” said Silver. As a final note on this point, she cited findings from a study of 529 older adults with cancer, 65 percent of whom had potentially modifiable deficits that needed physical or occupational therapy. However, only 9 percent received any rehabilitative therapy (Pergolotti et al., 2015).
Prehabilitation, Silver explained, is a process that occurs between the
time of diagnosis and the beginning of acute treatment and includes physical and psychological assessments that establish a baseline functional level, identify impairments, and provide interventions that promote physical and psychological health to reduce the incidence and/or severity of future impairments (Silver et al., 2013). While prehabilitation has gained some traction in connection with orthopedic surgeries such as joint replacement, studies have shown that prehabilitation improves outcomes from a variety of medical procedures connected with serious illness (Dickinson and Blackmon, 2015; Dunne et al., 2016). In one study Silver mentioned, researchers provided preoperative nutritional support to cancer patients who showed no clinical signs of malnutrition. The results of this randomized controlled trial showed that patients who received supplements, compared with those who had received a nutritional placebo, had fewer and less severe postoperative complications (Kabata et al., 2015). She added that while it would be easy to send a patient off to do exercises or take a nutritional supplement on their own, the further the patient is from the care team, the less effective prehabilitation becomes.
Silver emphasized that rehabilitation and prehabilitation should be important components of meeting the Institute for Healthcare Improvement Triple Aim for patients with serious illnesses.8 This is particularly true for cancer patients and for individuals with well-studied progressive illnesses. “We can predict the kinds of impairments people have because we have a lot of information on that,” said Silver. “We should be anticipating them and helping them in advance.” Given that, she said, every patient with a serious illness should be sent for prehabilitation or rehabilitation screening. In the oncology setting, she added, prehabilitation and rehabilitation can be the difference between being accepted into a clinical trial or not.
Christian Sinclair, representing the American Academy of Hospice and Palliative Medicine, pointed out the need to help the clinical workforce understand the precise rehabilitation needs of seriously ill patients. Of particular importance is clarifying how patients with impairments can be identified and referred appropriately and at an early enough point in the process in order to make the best use of prehabilitation and rehabilitation services as part of quality care planning and delivery. Terry Altilio noted that many patients seen by palliative care teams in consultative service, such as oncology, become increasingly deconditioned as they lie in bed day after
___________________
8 For additional information, please see http://www.ihi.org/Engage/Initiatives/TripleAim/Pages/default.aspx (accessed May 2, 2017).
day. This creates a “life-threatening” circumstance if patients have to discontinue treatment because of poor performance status, she said, and earlier rehabilitation and/or prehabilitation could really help prevent this. “Raising consciousness about that in the palliative care world I think is really important when the goal of a patient is to get treatment and to extend their life as long as possible,” Altilio concluded. Silver agreed, emphasizing the opportunity for palliative care and rehabilitation services to work together as referral resources for each other, urging that “you sort of owe it to your patients, and rehab will really help you.”
SUPPORTING SPIRITUAL, SOCIAL, AND PSYCHOLOGICAL NEEDS
Several workshop speakers addressed the critical importance of integrating the social, psychological, and spiritual aspects of comprehensive quality care for people and caregivers coping with serious illness. In thinking about the connection between these three related but distinct aspects of a person’s well-being, Karen Steinhauser described the benefits in helping patients and caregivers think about meaning, purpose, connection, peace, and hope. Understanding these realms, she said, can help identify the best interventions for addressing them and helping the patient and family with the challenges that come with serious illness.
Making Meaning
One of the concerns Steinhauser has heard from people living with a have serious illness is that they do not want their families burdened, and that they want their families to be prepared for what lies ahead. Berman, who is living with a serious illness, said she talks frequently to her adult daughter about what will come during the course of her illness, but even more so, she is taking the time to do things with her daughter, such as decorating according to her daughter’s taste. “I want to leave her remembering that I helped her do things that are important to her,” said Berman, “that it is it not just about the clinical, but it is all about life.”
Goldstein remarked that in the pediatric setting, parents often express great worry about crushing the hopes of their children who have a serious illness. At the same time, asking ill children what they worry most about elicits the response that they are worried about hurting their parents. What he has seen, though, is that by encouraging parents and children to talk
about those worries, the terrible psychological isolation each is feeling evaporates, and the room fills with positive feelings. “It is one of the easiest interventions we have,” said Goldstein, and it illustrates how important conversation is in the serious illness setting.
Encouraging such heart-to-heart talks between the seriously ill person and family members can help to alleviate or even prevent the regret that family members often feel after their loved one dies. Lord recounted that one of the most profound conversations she has had in her work with the Courageous Parents Network was with a mother whose 9-year-old daughter died from cancer. “She had deep grief missing her daughter, but she had no regrets because she and her daughter had the conversation about the fact that she was dying and her daughter talked about what she wanted her coffin to look like and where she wanted to be buried,” said Lord. This was a family of tremendous spiritual faith, and the palliative care team encouraged the family to have those conversations to honor their anticipatory grief and help their healing, and the mother said that while they were sad, these conversations were filled with hope and were very important to have had in the long run.
Addressing Suffering Through Spirituality Support
The role of spirituality in palliative care has been defined as, “The aspect of humanity that refers to the way individuals seek and express meaning and purpose and the way they experience their connectedness to the moment, to self, to others, to nature, and to the significant or sacred” (Puchalski et al., 2009, p. 887). This definition, said Steinhauser, stresses connectedness, which she said points to the importance of relationships, and it explicitly highlights the need that individuals have to find meaning in life based on what is important to each individual. Meaning, she said, is what enlivens an individual and makes that person feel most alive. It is the lens through which humans interpret and respond to their life experiences.
Spirituality is integral to people’s lives, noted Steinhauser, and studies have shown that spirituality is particularly important to both patients and families in acute health care situations. In the Coping with Cancer Study, funded by the National Cancer Institute and the National Institute of Mental Health, 88 percent of the patients surveyed said spirituality or religion was important to them (Balboni et al., 2010), and other studies reported similar findings (Egan et al., 2016; Phelps et al., 2009). The rates were even higher among African Americans and Latinos, she noted. In a
study of patients undergoing palliative radiation therapy for cancer, even those patients who said they were neither spiritual nor religious reported having spiritual needs (Hollant et al., 2015). “We know that beliefs and practices are central to how we cope with illness,” said Steinhauser. Research has shown, for example, that people who have negative religious coping strategies—those that focus on shaming or damnation—have particularly negative outcomes around quality of life, depression, and anxiety when living with illness (Hebert et al., 2009; Pargament et al., 2004; Tarakeshwar et al., 2006). “We also know that satisfaction and quality of life in the setting of serious illness are significantly higher when spiritual care is attended to, and that when people have unmet spiritual needs, costs actually increase,” she explained (Balboni et al., 2010).
Steinhauser’s point in citing these findings was to stress how important it is to understand a patient’s and family’s spiritual beliefs and needs, even though it may be awkward or difficult to have that kind of conversation. When asked how clinicians might talk to patients and families about their spiritual needs, Steinhauser suggested simply asking how they can support the patient and the family can start the conversation. Other conversation starters would include asking: “Are there important beliefs that inform the choices that you are going to make that I need to know about?” “Is there a community that is supportive to you that we should be including in this?” “To what extent are you at peace about the situation?”
Cultural Humility and Spirituality
For Reverend Alice Cabotaje, clinical pastoral education supervisor in the Massachusetts General Hospital Chaplaincy Department, spirituality merges with kapwa, a core cultural concept from her native Philippines that reflects the unity of self and others and acknowledges shared identity and the dignity of others. Kapwa, she said, encourages an unobtrusive approach to talking with patients and family members about their spiritual needs. “When I draw on kapwa, it helps me to be sensitive to the verbal, non-verbal, facial, and bodily cues of my patients, their caregivers, loved ones, and staff,” she explained. “In doing so, I find that it helps me gain their trust. I am able to see and hear them, feel what it is like to be in their shoes and accompany them in their joy, their pain, and their sorrows, and most especially, their vulnerability.” Cabotaje added that because kapwa encourages modesty and humility, “it helps me be a container holding them
regardless of their faith tradition, regardless of their culture, and regardless of their socioeconomic background.”
As a chaplain, Cabotaje is guided by two definitions of spirituality—the one Steinhauser provided and a second one from Reverend Michelle Shields (Shields et al., 2015). Reverend Shields defined spirituality as encompassing the dimension of life that reflects the needs to seek meaning and direction to find self-worth and to belong to community and to be loved and to love, often facilitated through seeking reconciliation when relationships are broken. “This definition helps me seek to recognize each patient’s individuality in terms of their deepest need and in order to evaluate where they are located along the path of healing and wholeness,” said Cabotaje. “At the same time, these definitions encourage me to be culturally sensitive and humble, and that means giving up the role of an expert on the patient’s or caregiver’s culture and faith tradition and instead become a student to them in order to provide spiritual care that is aligned with their preferences, their values, their beliefs, their spiritual needs.” She cited the Zen teacher Shunryu Suzuki, who said, “In the beginner’s mind there are many possibilities, but in the expert’s mind there are few,” as something to consider when engaging in conversation with patients and family members.
To illustrate the importance of surrendering the role of expert and listening with an open mind, Cabotaje told the story of a 71-year-old Vietnamese Buddhist father, Vin, who was terminally ill, and his 21-year-old daughter. The medical team caring for this man was unanimous in their opinion that he was dying and in a great deal of pain, and that the current treatments they were providing him were merely postponing the date of his death while causing unnecessary suffering. The team recommended comfort measures, but the patient’s youngest of three daughters, who was the closest to her father and was his medical decision maker, expressed her firm reluctance about these recommendations. Feeling distress in facing this dilemma of keeping their patient alive while seeing him in so much pain and suffering, the medical team consulted with the hospital’s ethics committee, which counseled that a spiritual approach might be more effective than a medical one for talking with the daughter about relief of her father’s suffering.
When Cabotaje went to talk to the daughter, she stood for a while outside of the patient’s room and watched father and daughter interact lovingly with one another. Pulling the daughter aside, she told the daughter that she could see how devoted she was to her father and what a strong bond there was between them. The daughter told Cabotaje that her father did not want to go as he was worried about leaving her without much in the way
of monetary wealth. She also talked about her sadness and pain because she and her father would not be able to do the things they had planned, saying she wished they had more time and she will miss him so much. Cabotaje encouraged her to say more about her father. The daughter smiled, then spoke about how she would miss the way her father’s ears stood up and the way he stood by her bedroom door with his hand over his waist when he woke her in the morning. She told Cabotaje how gentle he is, about his love of gardening, the way he savors his food, and that he works not so much for the money, but for the joy he gets from his co-workers. They talked about the importance of savoring every moment with him, and the daughter acknowledged that her father is leaving her with his rich legacy of integrity and perseverance, which means she will “bring him anywhere and everywhere I go.”
The daughter then recounted that the doctors told her that her father will not get better and suggested he be moved to palliative care. Her eyes flashed in anger, Cabotaje recalled, and she said her father would not want that because it would be as if he was giving up and he would not want to give up. He survived imprisonment during the Vietnam War, and believes he would survive this. She explained he is a Buddhist and does not mind suffering because it purifies him. That was the key statement, the one that opened the door to the support Cabotaje was able to give to this young woman in emotional pain. “I affirm that suffering can be purifying, but there is also unnecessary suffering that causes harm and distress,” said Cabotaje. The daughter continued to listen, and Cabotaje shared that in the Buddhist tradition, a calm state of mind is important when dying in order to afford a peaceful transition and be reborn to a better life. The daughter said she would think about that. Both Cabotaje and the daughter cried together, and as the daughter wiped her tears, she told Cabotaje how good it felt to be able to talk at length about her father.
After the daughter returned to her father’s room, Cabotaje spoke with the medical team and asked that they give the family time to process the conversation they just had. Four days later, when Cabotaje checked in with the daughter, she said she had come to acknowledge her father’s suffering and accept that he is dying, having told her father that he had tried his best to live, and now she wanted him to feel at peace. The family arranged for a Vietnamese Buddhist priest to perform the needed rituals, and asked to meet with the medical team about their father’s end-of-life care goals. As the sisters observed their father’s increased suffering, they asked the medical team to transfer him to comfort measures only. He was moved to a large
room with a view, and Vin died shortly afterward, peacefully, with his daughters by his side.
Cabotaje also shared the story of caring for a 50-year-old Filipina Catholic, transgender women, Dana, who had contracted a fungal infection in her lungs, and was angry because she was told to consider palliative care. When they met, the patient told Cabotaje she was afraid of dying and was “not ready to meet God.” Through their conversation about her faith and prayer, however, the patient found her way to accept where she was and now “could be fine with God in the same way.” This transition brought out an important opportunity for Dana to ask forgiveness for shouting at her bedside nurse, Joan, who actually had felt uncomfortable about caring for Dana because she was transgender. Dana’s gesture of seeking Joan’s forgiveness helped the two of them connect so that Joan was able to provide Dana with loving, attentive care during her last days.
Robert Bergamini offered a final story illustrating the importance of addressing spirituality as part of holistic, person-centered care. One of his patients, a 15-year-old boy with an incurable tumor, knew he would die if his tumor came back, and when Bergamini delivered that news to him, the young man smiled and said that was an answer to a prayer. “You know that my spirituality, my faith has been very important to me, and I prayed for healing. If God heals my soul by letting my body die, I am not going to argue with it,” said the young man. However, as Bergamini recounted, the young man, without breaking eye contact or taking a breath, said, “You know, your job is different now. Suffering is a bad thing, and suffering can make me doubt my faith, so just as you have protected my health up until now, you now have to protect my faith and make the path smooth. I want to enjoy life, whatever life I have, but I want you to make the path smooth.” A few weeks after the boy died, his parents presented Bergamini with a gift that their son had asked them to get for him. “It was a ball cap with MODAT, for Missouri Department of Transportation, embroidered on it,” said Bergamini, “and it came with a little note from him that said, ‘Thanks for making a smooth road.’”
Community Is Good Medicine: The Roles and Contributions of Chaplaincy in Providing Person-Centered Care
“Part of what we have been good at traditionally as health care chaplains is walking into a room, not knowing what is there, and meeting people where they are and bringing a non-anxious presence to whatever is
going on,” said Reverend Malcom Marler, director of pastoral care at The University of Alabama at Birmingham (UAB) Medicine. These same skills that help “make sense of chaos” can help meet the need for connecting inpatient and outpatient communication and process, and stretch the reach into the community, including caring for people when they are at home. This includes opportunities for chaplaincy to support advance care planning and other person-centered care issues by building enduring relationships through the energy of coordinated community support teams.
When UAB hired Marler in 1994 to be the first full-time chaplain in an HIV/AIDS clinic, he had to learn quickly how to build community as a way to end the discrimination that many faith communities were engaging in with regard to HIV/AIDS patients. “We had to learn how to engage people’s head, heart, and feet,” said Marler. “We had to teach them about HIV so they would not be scared.” One technique he used was to interview HIV/AIDS patients in front of faith communities and then recruit members of that faith community to form support teams for these individuals. As the tide turned in the battle against HIV/AIDS and patients began recovering from this disease, the support teams started looking for a new mission, and Marler gave it to them—to reach out to other people with serious illness in the community and then teach him and others what it was like to apply what they learned supporting HIV/AIDS patients to caring for others with serious illness. Eventually, said Marler, UAB developed a train-the-trainer program that has conducted 125 2-day training programs in 37 states. “We just listened,” said Marler. “Now we have 10 best practices and have taught 5,000 people who started 10,000 teams.”
The challenge of supporting seriously ill patients in the community persists, he said. Some of the chaplains he works with believe that local faith communities provide support for patients when they leave the hospital, but Marler said that is only partly true. “Churches are like medical care—we are really good at crisis response, but not so good with chronic care,” said Marler. He calls this the oven response. “We hear about somebody getting sick, we turn on the oven, cook something, and take them something to eat.”
Such a response can be heartwarming for the cook, but as Marler put it, “just because we are good at it does not mean that is what the patient will love.” The key, he said, is to have a conversation with the patient and family members and find out what kind of help they truly need. The goal of this conversation is to avoid “helping” in ways that do not make life simpler for the patient and family. The solution to this problem, he said, has been
to appoint one person on each care team who is a trusted friend and good organizer to serve as the team leader. Now, when he or one of the hospital’s other chaplains goes into a patient’s room, he asks if anyone outside of the family has offered to help, and if so, did the patient have a ready list of tasks for the potential helpers. That list goes to the team leader, who then coordinates taking care of those items. In the situation where a patient does not have anyone in his or her life to call on, Marler approaches a church community and asks them to be partners and care for that individual.
The goal of these efforts, said Marler, is to encourage chaplains to think more broadly about their mission. “We can no longer be focused only on the person in front of us, and when we walk out of the room we do not think any more about that patient,” said Marler. “What we are trying to do is extend our care out into the community by teaching other people, such as friends and neighbors.” The team’s efforts can actually help prevent readmissions, unwanted emergency department trips, and other areas of concern, focusing its support on making sure the individual has a ride to his or her doctor’s appointment, ensuring nutritious food is available, and providing the type of emotional support to help people overcome loneliness, “which is one of the biggest killers in our society today,” said Marler. In his opinion, there is a growing need for chaplains to stretch outside the silo of thinking only about addressing the patient’s spiritual needs. “The whole body, mind, and spirit affect each other,” he said. When we follow the best practices we have learned by engaging chaplains as extenders in helping to create reserves of trained community partner teams that activate to meet patients’ key needs in the community, it can “be a win‒win for everybody.”
PRIORITIZING COMMUNICATION AND CONNECTIONS
Throughout the workshop, speakers recounted stories of their experiences with patients and families that displayed a commitment to building relationships and the importance of connectivity and communication as the best way to gain trust and uncover the true wishes and goals of patients and families. In each case, the willingness to engage patients and family members, to be vulnerable and step into an intimate space with them, was a key to building that successful relationship. For some, doing so seems natural, but many health care professionals find such conversations challenging and awkward. As several speakers and participants have acknowledged, this is because few actually receive formal training on how to have conversations about patient and family preferences and desires in the face of serious illness.
Jerry Johnson, professor of medicine and chief of the Division of Geriatric Medicine at the University of Pennsylvania Perelman School of Medicine, noted that a big challenge for health professionals is admitting that their patients with serious illness are dying. “I think that is important because it helps frame tradeoffs that can occur,” said Johnson. He also said that while he finds the words “palliative care” comforting, they can confuse patients if they don’t understand precisely what palliative care entails.
Goldstein, responding to Johnson’s comment, said that as a palliative care specialist, he is in the unique position of giving someone the worst news possible and being thanked for it. However, no matter how bad the news is and no matter how difficult the path ahead might be, he has to trust that his role is to strengthen his relationship with his sick patients because there is important work to do. “Fundamentally, they need to trust you. You have to be the one person who walks in that room who they can look to and say, ‘Help me out, help me through this.’ That is what animates me in terms of developing the skills of people in training, but it also animates me to take a kind of risk in dealing with patients,” said Goldstein.
Meier referred to the work of Back, Robert Arnold, and Tulsky (Back et al., 2009), who popularized the strategy of “Ask-Tell-Ask.” This simple back-and-forth cycle between the patient and health professional aims to address four essential components: the patient’s perspective, information that needs to be delivered, response to the patient’s emotions, and recommendations by the professional. “It is understanding where the person is and then asking them how they like to get information about their illness,” said Meier. Some patients, she said, want to know every detail about their illness and what lies ahead, others only want a general outline, and 5 to 10 percent do not want to know at all. For this last group, she asks whom the patient would trust for her to talk with about their illness.
Meier said that once she delivers difficult news, she stops talking because the patient is not likely to hear anything afterward. “What feels like a really long time to us is probably 2 or 3 minutes, but it feels endless because we are being silent, which we are not comfortable with as doctors,” said Meier. Eventually, though, the patient will start asking questions. Listening carefully to those questions will provide insights into how the patient is processing information and where they want to go with that information. “It is ask-tell-ask, ask-tell-ask, and it is a teachable skill, but no one from our generation ever got that during our training,” she added. She noted that these communication skills can be taught in the same way that medical students learn other vital skills, where the actions are reinforced enough
times that they become automatic. “Every clinician needs this skill, but we have a long way to go for that to be the standard of medical education and competency assessment,” said Meier.
Learning Person-Centered Communication Skills
Back noted that numerous studies have shown that with appropriate training, physicians and other health professionals can learn better communication skills that would enable them to speak with their patients about serious illness (Arnold et al., 2015; Back et al., 2009; Clayton et al., 2013; IOM, 2015). “The training that really works changes behavior,” Back said, and the benefits of that training persist over time (Fallowfield et al., 2003). After training, physicians use more empathy, ask more questions to understand their patients, have more conversations to explore patient values, and have higher levels of patient trust (Tulsky et al., 2011). Back added that good training leads to a self-reinforcing cycle where better connection with patients rewards clinicians for their improved communication skills and prompts them to continue to improve those skills. “They feel they are doing the real work they are supposed to do, so they keep using these skills,” said Back. In fact, he said, clinicians actually like this training, and think it is a worthwhile investment. One study revealed that 95 percent of oncology fellows rated the training highly or very highly (Larrieux et al., 2015). “It is not necessarily something that you would have to subject them to. Once they get into it, they realize instantly how important it is,” he noted.
Unfortunately, said Back, these trainings have been accessible solely through research studies. To address that shortcoming, Back, Tulsky, Arnold, and Kelly Edwards created a nonprofit organization, VitalTalk,9 to disseminate what they have learned about the communication skills they have developed over the past decade. Back likened the courses VitalTalk offers to a flight simulator for difficult conversations. There is also a VitalTalk app for smartphones to reinforce the lessons from these courses. Over the past 2 years, said Back, VitalTalk has conducted trainings across the country. Among those trained, burnout scores have fallen and Hospital Consumer Assessment of Healthcare Providers and Systems scores have risen (Boissy et al., 2016). Back said that making the transition from randomized studies to using VitalTalk has increased the ability to produce trainers more than tenfold. Reflecting on the data showing how
___________________
9 For additional information, see http://vitaltalk.org (accessed on May 2, 2017).
practitioners who have experienced interactive communication courses have less burnout while also doing a better job, Back suggested “there is a very important issue here related to the quadruple aim about clinician well-being and them connecting with their patients better.”
The bottom line, said Back, is that, while many patients are at risk if clinicians do not develop these communication skills, the type of evidence-based training he described is very effective in improving provider–patient conversations and connections. Back said he hopes that, going forward, policies are developed to foster a clinician workforce that prioritizes those skills to put patients first when having meaningful, informative conversations. Such policies, he said, could provide real incentives, beyond continuing medical education credits, for all types of clinicians to invest in their own skills training, incentives that do not exist today. In addition, Back noted that these courses should be more accessible to clinicians. Although the current CMS reimbursement for having an advance care planning conversation is important, the survey data made clear that payment alone without skills training does not improve likelihood or adequacy of these serious illness conversations. Back pointed out that electronic health records also need to be improved to better inform physicians about which patients are at highest risk, but he believes that clinician training for all health care professionals is key to solving this problem.
Back closed his remarks by sharing examples of cancer patients he has cared for recently who are doing what is important for them despite their advanced disease, for example, playing with grandchildren, enjoying painting, going to see Bruce Springsteen in concert, and traveling in Italy. “There is a huge amount of life that is possible for our patients if we have the skills to ask them what is really important,” he explained. “The other system things to improve person-centered care will not take the place of this,” he emphasized, and if we do not equip the workforce with skills they need to comfortably and adequately handle these conversations, “it will all fall apart.”
TOOLS THAT HELP MATCH TREATMENTS TO VALUES
In addition to equipping the workforce through training, other strategies to improve communication include tools that help align treatment and care for those facing serious illness with their personal values and preferences. Several workshop speakers described a number of these tools and
strategies designed to facilitate conversations and enable people to become more engaged in their own care.
Engaging People in Their Own Care: The Conversation Project
The Conversation Project is a public engagement campaign dedicated to ensure that everyone’s wishes for end-of-life care are expressed and respected, Goodman explained. It is based on a deep recognition that health care professionals need to listen to the stories that their patients have to tell and on a theory of social change that says communities need to bring change into institutions, where it is accepted and improved, and then sent back out into the community. “What we wanted to do was to get people to the proverbial kitchen table to talk about their wishes, their values, how they wanted to live with the people they loved, and to do it before there is a crisis, because as we all know, a crisis is a terrible time to learn,” said Goodman.
From the start, Goodman and her colleagues recognized that when many people initiate hard conversations, they need a script or outline to get them started and guide them. They created a set of tools that are not medical and do not have an endless checklist of procedures. “They are about values and about what matters to you, not what is the matter with you,” said Goodman. These tools include two different conversation starter kits to foster discussions with family members and doctors and two specialty starter kits for parents of seriously ill children and for families and loved ones of people with Alzheimer’s disease and other forms of dementia. These starter kits, she said, have been translated into multiple languages, are available to download free from the organization’s website,10 and have been used by more than a million people. The Conversation Project is developing a new tool for release in 2017 called How to Pick a Health Care Proxy, How to Be a Health Care Proxy.
At the request of people who have used these conversation starter kits, The Conversation Project has started working with faith-based communities, financial advisors, estate planning attorneys, Area Councils on Aging, libraries, and civic organizations to disseminate these tools more broadly within communities and to help those who meet with families in various capacities to develop better conversation skills. As an example, Goodman said that faith leaders have no more training than doctors and nurses do in
___________________
10 For additional information, see http://theconversationproject.org/starter-kits (accessed on May 2, 2017).
having these conversations. Today, The Conversation Project has 400 people in 44 states working to get these kits into the hands of those who need them.
In Goodman’s opinion, The Conversation Project’s most important work has been to bring people’s stories to the attention of the media and the public, an effort that included creating a public service announcement (PSA) campaign. “Every meeting that many of us have attended talks about the importance of a public engagement campaign, and yet it keeps getting dropped to the bottom of the list,” said Goodman. She and her colleagues designed, tested, and piloted a PSA campaign in the Boston subway system in conjunction with Facebook pop-up ads, the latter of which increased traffic to the organization’s website by 200 percent, she said. The most popular messages turned out to be simple ones: “Some things should not go unsaid” and “When it comes to end-of-life care, talking matters.” The campaign’s Twitter hashtag was #talkingmatters, she added.
The Conversation Project emphasizes early conversations because the focus needs to be on living well to the end, not on dying. A survey she and her colleagues conducted found that 90 percent of Americans believe these conversations are important, although only 30 percent have had them. When asked why they had not yet had these conversations, the first reason was that it was too soon, so a slogan Goodman and her colleagues now use is “It’s Always Too Soon Until It’s Too Late.” Goodman emphasized the importance of their role as “change agents” in communities to share the wide array of proven tools and trainings that offer “new and innovative ways to listen and encourage people to share their values and have them respected.” She explained, “[w]e need that voice of the community going in, as well as the responsiveness of the health care clinician community. That is the way change happens.”
Teaching Behaviors That Improve Conversation: Common Practice’s “Hello”
Conversations are key to providing high-quality care for people with serious illness. “The reality is that just about every one of us is going to find ourselves in a situation where we talk about serious illness at some point in our lives and probably many times,” said Jehlen, and the challenge is to have that conversation in a productive manner. Jehlen noted that studies have shown that when one spouse discusses work stress and the other spouse responds with advice, it is usually not well received. Instead, the conversation tends to end and shift to a different topic (Pearlin and McCall, 1990).
However, if the spouse listens and expresses empathy, then offers advice, the conversation is much more likely to go well because both spouses will believe the other spouse listened. Jehlen explained that was the goal of his work with colleagues at Common Practice in developing the game “Hello” (formerly called My Gift of Grace): “to facilitate conversations where people feel listened to and understood, even under challenging conditions.”
Jehlen told a story about a nurse at an inpatient hospice in Delaware with whom he worked recently. The nurse walked into a room with a new patient, a man in his 50s who was in a coma and unable to communicate. The nurse had a list of things to go over with the family, but rather than pepper the family with questions about his medical history and medications, the nurse turned to the patient’s wife and daughter and asked them to tell him something personal about the patient. The wife struggled a bit with that question, but the daughter said, “I know exactly what to say. He is a great dad.” The nurse wrote that down, then told that story to the rest of the staff. “This created a pattern where any staff member that entered the room had a starting point,” he explained. “When you start with something that is important to the patient and the family, conversations about values and goals get much easier,” said Jehlen. Stating that this is the kind of care everyone wants, he added, “We call it person-centered care, but what it really means is that you enter into a conversation with me as a person with all the complex and messy and beautiful things that go along with that.”
In this type of conversation, people learn how to care for one another, but this type of conversation does not happen often enough, said Jehlen. “The problem is we are scared to have those conversations, to ask personal questions. We are nervous to bring up embarrassing topics about ourselves,” he said. “Many of us struggle to have these kinds of conversations with our own family, so it is not a big surprise that we struggle to have them with nurses and doctors.”
The good news, he said, is that research has identified the types of behaviors that improve conversations. For example, groups that take turns speaking and pay attention to non-verbal cues are more likely to successfully navigate conversations about embarrassing, sensitive, or personal topics (Woolley et al., 2010). On the other hand, people are often dissatisfied with a conversation when there is not a good balance between the task of the conversation—a question about a symptom or treatment, for instance—the relationship-forming bond between people, and their own identities and expressions of autonomy (Caughlin, 2010).
The bad news, said Jehlen, is that knowing to resist the impulse to jump
in and give advice is one thing, but following through on that knowledge is another. “That is just not how behavior change works—knowing what to do and doing it are two entirely different things,” he said. Jehlen pointed out things that make conversations go well are mostly steps that one person cannot do on his/her own because conversations are a team event and require all parties to work together to get the best results. “To work better as a team, we need to give people a different kind of solution, one that does not depend on every person knowing what behaviors lead to better conversations, and that does not depend on everyone changing those behaviors while they are under stress,” said Jehlen.
He and his colleagues have developed two tools designed to help moderate conversations. The first is a game called Hello, which encourages people to take turns and listen, and prompts players to talk about those tasks and relational and identity goals that are essential to great conversations in a way that users report to be fun (Van Scoy et al., 2016b). The game can be played with children, families, caregivers, and patients, said Jehlen, and it works in large groups. “It works because it is a tool that manages the hard parts of a conversation, so that players can relax and be themselves,” he said. The result, he added, is that when people feel good about these conversations, it leads to action. A recent study found that 78 percent of the people who played the game went on to take an advance care planning action (Van Scoy et al., 2016a). “There is no magic here,” said Jehlen. “This is what happens when you give people a simple tool that nudges everyone toward better conversational behaviors.”
Jehlen noted that the nurse he mentioned earlier as well as the facility’s staff had already played this game and grown comfortable with this type of person-centered conversation. The Common Practice team also worked with staff to create a new tool for health care professionals to use with patients and families. When the nurse had asked the family to tell him something about the patient, the nurse was actually reading from a card that said, “In order to provide you with the best care possible, what three non-medical facts should your doctor know about you?” After writing the answer on the card, the nurse then posted it above the handwashing station so that every doctor, nurse, janitor, social worker, family, and friend would see it. “They get a nudge to talk about this patient as a person every time they enter the room,” said Jehlen.
As a final thought, Jehlen noted that health care organizations do not just tell staff members about the importance of handwashing and then expect them to find a way to disinfect their hands—they give them simple
tools and make them widely available. “We should be using tools for great conversations as often as we use tools for better handwashing because conversations are just that important to providing care, and they deserve to be treated that way,” he said.
Supporting Advance Care Planning Through Online Skills-Building Tools: PREPARE
A decade ago, Sudore and her colleagues created easy-to-read advance directives that doubled completion rates in California (Sudore et al., 2007). Although the advance directives are available for free in 10 languages, Sudore realized they are not sufficient to address effectively the challenge of providing care that reflects the desires of patients and caregivers. “Often, when we think about advance care planning, we think about one decision about the end of life, but as a geriatrician, I see my patients and family members making many decisions over time, and people need support for that,” said Sudore. The missing piece, she said, is providing people with skills ahead of time to identify what is most important to them and how they want to live, and then communicate that with loved ones and providers. “How do you take what you know is important to you and translate that into medical care?” asked Sudore. “I will tell you that as clinicians, oftentimes we expect patients to be able to do that, but it is a hard task to do.”
To address this challenge, Sudore and her colleagues developed an interactive, multimedia website called PREPARE for Your Care11 (Sudore and Fried, 2010; Sudore et al., 2014) (see Figure 4). The website walks people through five steps at their own pace to create an action plan.
Based on the premise that modeling behavior is key to behavior change, the website features videos demonstrating how to complete each of the five steps. As people go through the PREPARE program, they are able to answer questions about their values and goals, in the form of both checkboxes and sections where they can write their own stories if they so desire. A pilot study found that this approach improved patient engagement in advance care planning in a group of low-income seniors, 92 percent of whom had never used a computer before (Sudore et al., 2014). Sudore explained that this was a group of chronically ill, disenfranchised adults, only 40 percent of whom had engaged in any form of advance care planning. However,
___________________
11 For additional information, see https://www.prepareforyourcare.org/page (accessed May 2, 2017).
SOURCE: As presented by Rebecca Sudore, December 15, 2016.
within only 1 week of going through PREPARE, that number increased to 100 percent. A subsequent randomized trial involving patients at the San Francisco Veterans Affairs Medical Center found that, based on an objective chart review, the rate of advance care planning increased from 1 percent to 35 percent (Sudore et al., 2015).
Sudore outlined key elements of successful advance care planning in the medical environment, including educating clinicians and other health care professionals, as well as tools that activate patients to discuss their priorities and preferences. As she explained, the goal is to ensure that the tools are accessible and easy to use. Sudore and her colleagues are now creating toolkits that include newsletters, posters, and email announcements for community organizations to use to disseminate PREPARE into the community. They have also worked with colleagues at the University of California Hastings College of Law to translate the easy-to-read advance directives for use in all 50 states and to integrate them into PREPARE. The output, then, is a legal document containing all of the answers about values and goals that Sudore hopes will increase the chances that a patient’s wishes will be honored. Her team is also working to incorporate this document into the electronic health record, although she noted that the multitude of electronic health record systems makes this a difficult task.
Using Market Research to Find Out What People Want
Peter Mitchell, chair and chief creative officer at SalterMitchell, described the extensive market research his firm conducted on behalf of Compassion & Choices. Mitchell said, at its core, integrating the patient and caregiver voice into serious illness care would seem to be a simple matter of empowering patients and caregivers and changing some behaviors among clinicians. “It should be no problem, but of course, this is completely wrong,” said Mitchell. His market research firm conducted interviews with a wide range of people inside and outside of the medical profession with the assumption that patients and their family members could engage at the time of a terminal diagnosis and came to two conclusions: (1) there is no clear recognition of the terminal until the end, and (2) people do not believe they need more power to control their care. Rather, they believe doctors will do their best and everything will work out well.
In Mitchell’s opinion, there is a point in the journey of a patient with serious illness where there is a transition from a position of independence, in which the key actors are the patient and family, to one of dependence, in which doctors and the health care system become key actors (see Figure 5). That transition point is when the discussion turns to the benefits and burdens of care, where the most important decisions occur, and according to the interviews he and his colleagues conducted, it is the time when those with serious illness have definite wants from the system: They want help
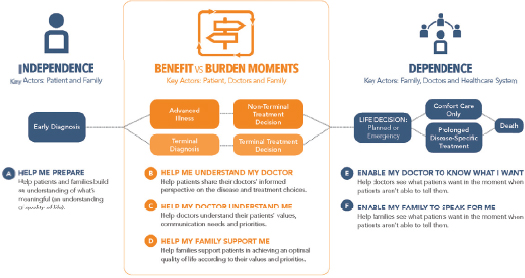
SOURCE: As presented by Peter Mitchell, December 15, 2016.
understanding their doctors, they want help for their doctors to understand them, and they want help for their family to provide support for their care.
This formative research led Mitchell to believe that effective end-of-life tools might work to ease this time of transition for patients and families, but further interviews discovered that people actually want tools for better living, not better dying. Moreover, Mitchell explained, while the project’s initial intention was to work with consumers to create market forces that would demand change to which doctors would respond, their research also revealed that seriously ill people “are really not in the demanding mood” and “are not really ready to have this big campaign.” Instead, Mitchell elaborated, they realized the real disruptions or triggers come from the questions people ask and the importance to them of the relationships they build with their care team. These conversations, he said, which help doctors think of patients as people, are the fundamental foundation for building those relationships.
Using these market research findings, his group developed two products for Compassion & Choices. The first is an online “Trust Card,” which prompts people to answer three questions about their values and goals for care, and the program creates a customized card patients can hand to their doctors to help support knowing them as people. The other tool is a “Diagnosis Decoder” that is designed to help people figure out what role they want to play in their care, supporting them with the question prompts they may want to ask in the context of their particular condition based on their own input.
Dissemination of Tools and Training
Following the presentations, the speakers discussed the factors that can contribute to people feeling either powerful or powerless. Sudore observed that disenfranchised populations may not think of their doctor as someone they can talk to about helping them with their concerns. She explained that, while many people see their doctor often, many others have limited access in both rural and urban areas and do not view their doctor as someone with whom they have a trusting relationship. She urged participants to remember the importance of developing and disseminating different tools and strategies to support diverse groups of people. This includes those who have or are likely to develop a close relationship with their care team, and those who, for example, may be seeing a new resident who is the only doctor available
to see them or any of a number of scenarios in which they do not see their regular doctor on a consistent basis.
Buck picked up on that point, emphasizing the critical importance of community proximity and “tapping into the people they talk to” and understanding what their beliefs are as a key strategy for building needed bridges and supports for these populations. Noting these can be two very different worlds, she also explained how sharing with clinicians the transcripts of what people are really saying is happening in the community can be an effective “sensitizing” tool as part of workforce communication skills training, helping clinicians to develop skills that enable them to listen and respond to people’s beliefs and values so they feel heard. Mitchell echoed the importance of equalizing the playing field by honoring the expertise patients bring to the table about what is important to them, pointing out that “you are the only person who is an expert on you.”
The panelists also talked about the importance of supporting these conversations earlier so it becomes “normal” to have them upstream, before people confront serious illness. An essential aspect of normalizing these conversations is the opportunity to distribute and balance power in the relationship. In particular, several speakers highlighted the importance of encouraging others to listen. Jehlen explained, “One of the things that happens when you use a tool that makes people take turns is that people without any power in the room start to speak.” In playing Hello, for example, Jehlen has observed the power of the game’s rule requiring that one must listen when other people are speaking—particularly when a physician playing the game would have to remain quiet in turn. Goodman agreed, explaining that her observation in The Conversation Project videos are “the people who you wouldn’t expect and the people who don’t have a lot of power, the grandchildren, the people who are a little bit separated off, who get a turn to speak and then can model that for other people.”
Following the panel discussion, Judith Peres, board member of the Social Work Hospice and Palliative Care Network, expressed the challenge of broad dissemination of these tools, including scarce availability of dedicated funds required for broad-based dissemination. Mitchell replied that dissemination is also a challenge, because there are so many issues competing for people’s attention, and absent a massive “Got Milk”–type promotional budget in the many tens of millions of dollars, dissemination requires giving people what they already want instead of convincing them that they want something else. Mitchell said that a feasible dissemination, for example, would focus on a manageable population, such as having hos-
pital staff play the Hello game to learn how to listen as Jehlen described they are doing, or making available products such as the trust card and decoder that primary physicians would want to incorporate into their practice as a helpful plug-in for learning things about their patients. Many speakers and participants agreed that sharing proven trainings and tools such as the ones discussed at the workshop can help these conversations become more common. A key tactic for sustainability and dissemination will involve getting these trainings and tools into systems that already have people flowing through them, rather than basing a dissemination model on screaming from the mountaintop, explained Mitchell, because “it is really expensive to scream from the top of the mountain.”
Goodman agreed that obtaining significant funding for dissemination is difficult, and she believes that tapping into social media may be at least as effective as large-scale public information campaigns. She also expressed optimism that the baby boomer generation will continue to be the agent for a culture change with regard to how its voice will be heard as boomers grow older, develop serious illnesses, and demand care. She likens this to the way that giving birth changed in the United States. “Birth did not change in America because doctors said, ‘Please, come in and bring your video camera.’ It happened because people said giving birth is not just a medical experience. It is a human experience and it should be humanized,” said Goodman. Already, she said, baby boomers are dealing with their elderly parents and with their friends, and themselves, getting sick. “They are not going to go gently into that bad good night,” said Goodman. “They are going to want to do it differently.”
In her mind, this is “a prime moment,” when the way the nation cares for individuals with serious illness is at a tipping point. Reflecting on the controversial “death panel” messaging of a few years ago, Goodwin reminded workshop participants that “we now have payment for having these conversations and the culture has changed.” She cautioned that pushing past the tipping point and not going backward will take focused energy. Mitchell said that will take “catching the imagination of the public by connecting with something.” Goodman agreed, offering that people connect with these issues because “everybody has a story.” That, she said, is the power of the work that we are all doing.
Joanne Lynn, director of Altarum’s Center for Elder Care and Advanced Illness, commented that, while advance care planning needs to be done, it remains only a very small part of comprehensive planning. She noted the importance of knowing about the person’s living situation in order to
determine their needs and the type of community services that are available. Sudore responded that we also need to train the workforce to provide the care that people are saying they want, using tools such as VitalTalk for conversation skills development, and teaching clinicians other primary palliative care skills so they can deliver the comprehensive care people need in their communities. She also talked about thinking of advance care planning as extending beyond medical planning to include “life planning” that involves medical‒legal partnerships, helping people stay in their homes, thinking about what to do to take care of the children, and other support needs people express when involved in care planning.
Mitchell likened normalizing these conversations to “building muscles over time.” You start to change thinking by giving permission for the conversations and working on small pieces that develop different habits. He explained: “You talk about everybody in this equation, the family, the doctor, the patient. All of them are looking for permission to do different things from each other and it is not happening. The family is showing love in a way that ends up being bad for the patient sometimes. The patient is trying to show love by not letting their feelings go. The doctor is trying to show love and show care by not giving as much information as they could. It is that dynamic. It is the small pieces of that dynamic that are huge.”
In closing the session, several workshop participants reflected on the importance of ensuring that tools and strategies are adaptable to an environment that is increasingly reliant on bigger teams that include many players beyond just health professionals, and the importance of bringing patients and families in as part of that team. Patricia Bomba, vice president and medical director at Excellus BlueCross BlueShield, also raised the need to educate the cohort of people who are appropriate for medical orders or physician orders for life-sustaining treatment (MOLST or POLST) to ensure they receive the care that they want in an emergency. This, she said, also involves large system change requiring culture change, public education, and clinician training, and doing so in the context of workflow and policies and procedures. Yet the whole conversation is different, she explained; “It is not about future care; it is about right here and right now.”
Recalling the Patient Self-Determination Act,12 Amy Berman com-
___________________
12 The Patient Self-Determination Act was passed by Congress in 1990 as an amendment to the Omnibus Budget Reconciliation Act of 1990. This legislation required many hospitals, nursing homes, home health agencies, hospice providers, health maintenance organizations, and other health care institutions to provide information about advance health care directives to
mented on the topic of empowerment, asking whether today, if we are to complete an advanced directive, how empowered are we in terms of knowing that the document will be respected? Jehlen responded that while we likely still are not empowered now, he has witnessed “magical moments” with teams where they are working together, trust each other, and therefore learn how to trust the patients and trust the families. At that moment, he explained, “You start to have people actually be empowered and actually make decisions for themselves and have other people get out of their way, leaving some of the power that comes with being a doctor or nurse and put it back into the power of the patients and their families.” Jeff Cohn added to the discussion from the perspective of health professionals, stating that, “if we create the space for the conversations and make it clearer that we really need them in order for us to do our jobs well, then those muscles that have not had the chance to be used within patients and families get used to show how strong they really are.”
FINAL THOUGHTS
The onset of serious illness, whether in an adult, infant, or child, is a time of crisis. As both Sudore and Goodman pointed out during their presentations, a time of crisis is likely to be the worst time to make decisions that reflect the needs, desires, and goals of patients and family members. Reflecting that reality, many of the workshop’s presentations and discussions highlighted two key approaches to consider in order to create person-centered care plans that reflect what matters most to people:
- Pursue and enable earlier communication about people’s values and preferences for their quality of living, deploying tools and community outreach strategies that normalize and systematize these conversations that make individual wishes clear, ideally before serious illness occurs.
- Prioritize primary palliative care skills training for all clinicians and others who care for people coping with serious illness to enhance capacity for assessing needs as well as listening and talking to patients and caregivers so their personal preferences and values are systematically known and honored.
___________________
adult patients upon their admission to the health care facility, though the law does not apply to individual physicians (GAO, 1995).
In her remarks to conclude the workshop, Kirch commented on the powerful quality of care that can emerge from healthy connections among patients, caregivers, and professionals, as was evident in each of the four workshop sessions throughout the day. She highlighted four thematic points synthesizing the day’s discussions:
- Relationships and skilled communication are essential to meaningful medicine and the person-centered experience.
- A huge amount of life is possible for seriously ill infants, children, and adults if we learn how to ask for and embed their expertise about what is important to them.
- Proven tools, training methods, resources, and services are available to help make this happen.
- We all need to think about using our heads, hearts, feet, and voices to increase understanding and awareness that build demand for person-centered care.
As a final thought, Kirch reflected on a comic featuring the late Charles Schultz’s Peanuts characters Charlie Brown and Snoopy sitting on a dock overlooking a lake. Charlie Brown says, “Someday, we will all die, Snoopy!” and Snoopy replies, “True, but on all the other days we will not.” That life-affirming message, even when facing down mortality, she said, became her family’s motto when her mother was diagnosed with amyotrophic lateral sclerosis. First, she explained, her mother wanted to know how she could take steps to relish every moment she had left. As the disease progressed, Rebecca’s mother also wanted to know what to expect “when the other shoe would drop.” That second question, Rebecca explained, became the context for their “magical moment” during an outpatient palliative care conversation they had with Patrick Coyne in Richmond, Virginia. He was the caring nurse who took time to explain in comforting, clear, and compassionate terms what they should expect as her condition deteriorated and how the team would help address those changes, just as they had helped plan for and support relishing the moments.
Some weeks later, Kirch asked her mother what the most important part of her entire experience had been. Using an electronic device to speak, her mother said, “Palliative care helped me stay ahead of the game.” That, said Kirch, should be the marketing message. “We have to figure out how to take that message to the street and make it part of the heart of health care,” she said.
REFERENCES
Arnold, R. M., A. L. Back, A. E. Barnato, T. J. Prendergast, L. L. Emlet, I. Karpov, P. H. White, and J. E. Nelson. 2015. The Critical Care Communication project: Improving fellows’ communication skills. Journal of Critical Care 30(2):250–254.
Back, A., R. Arnold, and J. Tulsky. 2009. Mastering communication with seriously ill patients: Balancing honesty with empathy and hope. Cambridge, UK: Cambridge University Press.
Balboni, T. A., M. E. Paulk, M. J. Balboni, A. C. Phelps, E. T. Loggers, A. A. Wright, S. D. Block, E. F. Lewis, J. R. Peteet, and H. G. Prigerson. 2010. Provision of spiritual care to patients with advanced cancer: Associations with medical care and quality of life near death. Journal of Clinical Oncology 28(3):445–452.
Banks, E., J. E. Byles, R. E. Gibson, B. Rodgers, I. K. Latz, I. A. Robinson, A. B. Williamson, and L. R. Jorm. 2010. Is psychological distress in people living with cancer related to the fact of diagnosis, current treatment or level of disability? Findings from a large Australian study. Medical Journal of Australia 193(5 Suppl):S62–S67.
Boissy, A., A. K. Windover, D. Bokar, M. Karafa, K. Neuendorf, R. M. Frankel, J. Merlino, and M. B. Rothberg. 2016. Communication skills training for physicians improves patient satisfaction. Journal of General Internal Medicine 31(7):755–761.
Boss, R., K. Kavanaugh, and K. Kobler. 2011. Prenatal and neonatal palliative care. In Textbook of interdisciplinary pediatric palliative care, edited by J. Wolfe, P. S. Hinds, and B. S. Sourkes. Philadelphia, PA: Elsevier Health Sciences. Pp. 387–401.
Bridgeland, J. M., J. J. Dilulio, and K. B. Morison. 2006. The silent epidemic: Perspectives of high school dropouts. Washington, DC: Civic Enterprises.
Caughlin, J. P. 2010. Invited review article. Journal of Social and Personal Relationships 27(6):824–848.
Center to Advance Palliative Care. 2011. Public opinion research on palliative care: A report based on research by public opinion strategies. New York: Center to Advance Palliative Care.
Center to Advance Palliative Care. 2015. America’s care of serious illness: 2015 state-by-state report card on access to palliative care in our nation’s hospitals.https://reportcard.capc.org (accessed March 27, 2017).
Clayton, J. M., P. N. Butow, A. Waters, R. C. Laidsaar-Powell, A. O’Brien, F. Boyle, A. L. Back, R. M. Arnold, J. A. Tulsky, and M. H. Tattersall. 2013. Evaluation of a novel individualised communication-skills training intervention to improve doctors’ confidence and skills in end-of-life communication. Palliative Medicine 27(3):236–243.
CMS (Centers for Medicare & Medicaid Services). 2016. Medicare & you, 2017. Baltimore, MD: U.S. Department of Health and Human Services, Centers for Medicare & Medicaid Services. https://www.medicare.gov/pubs/pdf/10050-Medicare-and-You.pdf (accessed May 2, 2017).
Compassion & Choices. Medical aid in dying fact sheet.https://www.compassionandchoices.org/wp-content/uploads/2016/02/FS-Medical-Aid-in-Dying-FINAL-2.2.16Approved-for-Public-Distribution.pdf (accessed May 2, 2017).
Cote-Arsenault, D., and E. Denney-Koelsch. 2016. “Have no regrets”: Parents’ experiences and developmental tasks in pregnancy with a lethal fetal diagnosis. Social Science and Medicine 154:100–109.
Denney-Koelsch, E., B. P. Black, D. Cote-Arsenault, C. Wool, S. Kim, and K. Kavanaugh. 2016. A survey of perinatal palliative care programs in the United States: Structure, processes, and outcomes. Journal of Palliative Medicine 19(10):1080–1086.
Dickinson, K. J., and S. H. Blackmon. 2015. Prehabilitation: Prevention is better than cure. Journal of Thoracic and Cardiovascular Surgery 149(2):574–575.
Dunne, D. F., S. Jack, R. P. Jones, L. Jones, D. T. Lythgoe, H. Z. Malik, G. J. Poston, D. H. Palmer, and S. W. Fenwick. 2016. Randomized clinical trial of prehabilitation before planned liver resection. British Journal of Surgery 103(5):504–512.
Egan, R., R. MacLeod, C. Jaye, R. McGee, J. Baxter, P. Herbison, and S. Wood. 2016. Spiritual beliefs, practices, and needs at the end of life: Results from a New Zealand national hospice study. Palliative and Supportive Care 5(2):223–230.
Fallowfield, L., V. Jenkins, V. Farewell, and I. Solis-Trapala. 2003. Enduring impact of communication skills training: Results of a 12-month follow-up. British Journal of Cancer 89(8):1445–1449.
Fischer, S. M., L. Cervantes, R. M. Fink, and J. S. Kutner. 2015. Apoyo con cariño: A pilot randomized controlled trial of a patient navigator intervention to improve palliative care outcomes for Latinos with serious illness. Journal of Pain and Symptom Management 49(4):657–665.
Freeman, H. P., and R. L. Rodriguez. 2011. The history and principles of patient navigation. Cancer 117(150):3539–3542.
GAO (U.S. General Accounting Office). 1995. Patient Self-Determination Act: Providers offer information on advance directives but effectiveness uncertain. https://www.gpo.gov/fdsys/pkg/GAOREPORTS-HEHS-95-135/pdf/GAOREPORTS-HEHS-95-135.pdf (accessed May 2, 2017).
Gawande, A. 2014. Being mortal: Medicine and what matters in the end. New York: Metropolitan Books.
Gomes, B., N. Calanzani, V. Curiale, P. McCrone, and I. J. Higginson. 2013. Effectiveness and cost-effectiveness of home palliative care services for adults with advanced illness and their caregivers. Cochrane Database of Systematic Reviews (6):Cd007760.
Hebert, R., B. Zdaniuk, R. Schulz, and M. Scheier. 2009. Positive and negative religious coping and well-being in women with breast cancer. Journal of Palliative Medicine 12(6):537–545.
Hollant, L., K. Gaines, B. Smart, J. Habboush, H. Biers, A. Day, R. C. Miller, L. Vallow, and K. S. Tzou. 2015. Patient-reported distress symptoms in patients undergoing palliative radiotherapy. Journal of Clinical Oncology 33(29 Suppl):75.
Hughes, M. T., and T. J. Smith. 2014. The growth of palliative care in the United States. Annual Review of Public Health 35:459–475.
IOM (Institute of Medicine). 2003. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The National Academies Press.
IOM. 2015. Dying in America: Improving quality and honoring individual preferences near the end of life. Washington, DC: The National Academies Press.
Kabata, P., T. Jastrzebski, M. Kakol, K. Krol, M. Bobowicz, A. Kosowska, and J. Jaskiewicz. 2015. Preoperative nutritional support in cancer patients with no clinical signs of malnutrition—prospective randomized controlled trial. Supportive Care in Cancer 23(2):365–370.
Kalanithi, P. 2016. When breath becomes air. New York: Random House.
Kamal, A. H., J. H. Bull, K. M. Swetz, S. P. Wolf, T. D. Shanafelt, and E. R. Myers. 2017. Future of the palliative care workforce: Preview to an impending crisis. American Journal of Medicine 130(2):113–114. doi: 10.1016/j.amjmed.2016.08.046.
Kavalieratos, D., J. Corbelli, D. Zhang, J. N. Dionne-Odom, N. C. Ernecoff, J. Hanmer, Z. P. Hoydich, D. Z. Ikejiani, M. Klein-Fedyshin C. Zimmermann, S. C. Morton, R. M. Arnold, L. Heller, and Y. Schenker. 2016. Association Between Palliative Care and Patient and Caregiver Outcomes: A Systematic Review and Meta-analysis. Journal of the American Medical Association 316(20):2104–2114. doi: 10.1001/jama.2016.16840.
Kobler, K., and R. Limbo. 2011. Making a case: Creating a perinatal palliative care service using a perinatal bereavement program model. Journal of Perinatal and Neonatal Nursing 25(1):32–41.
Larrieux, G., B. I. Wachi, J. T. Miura, K. K. Turaga, Christians, T. C. Gamblin, W. L. Peltier, D. E. Weissman, A. B. Nattinger, and F. M. Johnston. 2015. Palliative care training in surgical oncology and hepatobiliary fellowships: A national survey of program directors. Annals of Surgical Oncology 22(3):1181–1186.
Limbo, R., and K. Kobler. 2013. Meaningful moments: Ritual & reflection when a child dies. La Crosse, WI: Gundersen Lutheran Medical Foundation, Inc.
Loyet, M., A. McLean, K. Graham, C. Antoine, and K. Fossick. 2016. The fetal care team: Care for pregnant women carrying a fetus with a serious diagnosis. MCN American Journal of Maternal Child Nursing 41(6):349–355.
Medicare Payment Advisory Commission. 2016. Report to Congress: Medicare and the health care delivery system. Washington, DC: Medicare Payment Advisory Commission.
Miquel-Verges, F., S. L. Woods, S. W. Aucott, R. D. Boss, L. J. Sulpar, and P. K. Donohue. 2009. Prenatal consultation with a neonatologist for congenital anomalies: Parental perceptions. Pediatrics 124(4):e573–e579.
Morrison, R. S., J. D. Penrod, J. B. Cassel, M. Cause-Ellenbogen, A. Litke, L. Spragens, and D. E. Meier. 2008. Cost savings associated with U.S. hospital palliative care consultation programs. Archives of Internal Medicine 168(16):1783–1790.
Morrison, R. S., J. Dietrich, S. Ladwig, T. Quill, J. Sacco, J. Tangeman, and D. E. Meier. 2011. Palliative care consultation teams cut hospital costs for Medicaid beneficiaries. Health Affairs (Project Hope) 30(3):454–463.
Munson, D., and S. R. Leuthner. 2007. Palliative care for the family carrying a fetus with a life-limiting diagnosis. Pediatric Clinics of North America 54(5):xii, 787–798.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Health literacy and palliative care: Workshop summary. Washington, DC: The National Academies Press.
Oluwole, S. F., A. O. Ali, A. Adu, B. P. Blane, B. Barlow, R. Oropeza, and H. P. Freeman. 2003. Impact of a cancer screening program on breast cancer stage at diagnosis in a medically underserved urban community. Journal of the American College of Surgeons 196(2):180–188.
Pargament, K. I., H. G. Koenig, N. Tarakeshwar, and J. Hahn. 2004. Religious coping methods as predictors of psychological, physical and spiritual outcomes among medically ill elderly patients: A two-year longitudinal study. Journal of Health Psychology 9(6):713–730.
Payne, S. K., P. Coyne, and T. J. Smith. 2002. The health economics of palliative care. Oncology (Williston Park) 16(6):801–811.
Pearlin, L., and M. McCall. 1990. Occupational stress and marital support. In Stress between work and family, edited by J. Eckenrode and S. Gore. New York: Plenum Press.
Penttinen, H. M., T. Saarto, P. Kellokumpu-Lehtinen, C. Blomqvist, R. Huovinen, H. Kautiainen, S. Jarvenpaa, R. Nikander, I. Idman, R. Luoto, H. Sievanen, M. Utriainen, L. Vehmanen, A. S. Jaaskelainen, A. Elme, J. Ruohola, M. Luoma, and L. HakamiesBlomqvist. 2011. Quality of life and physical performance and activity of breast cancer patients after adjuvant treatments. Psycho-Oncology 20(11):1211–1220.
Pergolotti, M., A. M. Deal, J. Lavery, B. B. Reeve, and H. B. Muss. 2015. The prevalence of potentially modifiable functional deficits and the subsequent use of occupational and physical therapy by older adults with cancer. Journal of Geriatric Oncology 6(3):194-201.
PerryUndem Research/Communication. 2016. Physicians’ views toward advance care planning and end-of-life care conversations. New York: The John A. Hartford Foundation.
Phelps, A. C., P. K. Maciejewski, M. Nilsson, T. A. Balboni, A. A. Wright, M. E. Paulk, E. Trice, D. Schrag, J. R. Peteet, S. D. Block, and H. G. Prigerson. 2009. Religious coping and use of intensive life-prolonging care near death in patients with advanced cancer. Journal of the American Medical Association 301(11):1140–1147.
Puchalski, C., B. Ferrell, R. Virani, S. Otis-Green, P. Baird, J. Bull, H. Chochinov, G. Handzo, H. Nelson-Becker, M. Prince-Paul, K. Pugliese, and D. Sulmasy. 2009. Improving the quality of spiritual care as a dimension of palliative care: The report of the consensus conference. Journal of Palliative Medicine 12(10):885–904.
Shields, M., A. Kestenbaum, and L. B. Dunn. 2015. Spiritual aim and the work of the chaplain: A model for assessing spiritual needs and outcomes in relationship. Palliative and Supportive Care 13(1):75–89.
Silver, J. K., J. Baima, and R. S. Mayer. 2013. Impairment-driven cancer rehabilitation: An essential component of quality care and survivorship. CA: A Cancer Journal for Clinicians 63(5):295–317.
Smith, S., A. Brick, S. O’Hara, and C. Normand. 2014. Evidence on the cost and cost-effectiveness of palliative care: A literature review. Palliative Medicine 28(2):130–150.
Sudore, R. L., and T. R. Fried. 2010. Redefining the “planning” in advance care planning: Preparing for end-of-life decision making. Annals of Internal Medicine 153(4):256–261.
Sudore, R. L., C. S. Landefeld, D. E. Barnes, K. Lindquist, B. A. Williams, R. Brody, and D. Schillinger. 2007. An advance directive redesigned to meet the literacy level of most adults: A randomized trial. Patient Education and Counseling 69(1-3):165–195.
Sudore, R. L., S. J. Knight, R. D. McMahan, M. Feuz, D. Farrell, Y. Miao, and D. E. Barnes. 2014. A novel website to prepare diverse older adults for decision making and advance care planning: A pilot study. Journal of Pain Symptom Management 47(4):674–686.
Sudore, R., G. M. Le, R. McMahon, M. Feuz, M. Katen, and D. E. Barnes. 2015. The advance care planning PREPARE study among older Veterans with serious and chronic illness: Study protocol for a randomized controlled trial. Trials 16:570.
Tarakeshwar, N., L. C. Vanderwerker, E. Paulk, M. J. Pearce, S. V. Kasl, and H. G. Prigerson. 2006. Religious coping is associated with the quality of life of patients with advanced cancer. Journal of Palliative Medicine 9(3):646–657.
Tulsky, J. A., R. M. Arnold, S. C. Alexander, M. K. Olsen, A. S. Jeffreys, K. L. Rodriguez, C. S. Skinner, D. Farrell, A. P. Abernethy, and K. I. Pollak. 2011. Enhancing communication between oncologists and patients with a computer-based training program: A randomized trial. Annals of Internal Medicine 155(9):593–601.
Van Scoy, L. J., M. J. Green, J. M. Reading, A. M. Scott, C. H. Chuang, and B. H. Levi. 2016a. Can playing an end-of-life conversation game motivate people to engage in advance care planning? American Journal of Hospice and Palliative Care 1(8):754–761.
Van Scoy, L. J., J. M. Reading, A. M. Scott, M. J. Green, and B. H. Levi. 2016b. Conversation game effectively engages groups of individuals in discussions about death and dying. Journal of Palliative Medicine 19(6):661–667.
Weaver, K. E., L. P. Forsythe, B. B. Reeve, C. M. Alfano, J. L. Rodriguez, S. A. Sabatino, N. A. Hawkins, and J. H. Rowland. 2012. Mental and physical health-related quality of life among U.S. cancer survivors: Population estimates from the 2010 National Health Interview Survey. Cancer Epidemiology, Biomarkers & Prevention 21(11):2108–2117.
Woolley, A. W., C. F. Chabris, A. Pentland, N. Hashmi, and T. W. Malone. 2010. Evidence for a collective intelligence factor in the performance of human groups. Science 330(6004):686–688.








































































