5
Regional Perspectives from the Northeast
In Panel 3, moderated by Paul A. Biedrzycki, the geographic focus shifted to the Northeast. First, Celia Quinn discussed emergency preparedness in New York City (NYC), with a focus on the city health department’s experience with Hurricane Sandy and the expectation that extreme weather events will be more frequent in the future. Next, Matt Cahillane discussed New Hampshire’s use of the Centers for Disease Control and Prevention’s (CDC’s) Building Resilience Against Climate Effects (BRACE) framework and described several local-level, climate-related public health projects under way across the state. Lastly, Kristin Baja provided an overview of Baltimore’s unique approach to climate planning, one that incorporates climate change into the city’s generalized all-hazard mitigation plan and that focuses on equity. This chapter summarizes these three presentations. Key points made by the panelists are presented in Box 5-1.
In the open panel discussion with the workshop audience, a range of issues were addressed: collaboration across the different sectors of the NYC health care system; mortality and other outcomes of the Hurricane Sandy evaluation; alert, disaster, and fatigue; an elaboration of Baltimore’s incorporation of climate planning into its All-Hazards Mitigation Plan; funding for all of the various programs discussed by the panelists; and whether and how the different planning approaches discussed by the panelists had been scaled from approaches others had taken and whether and how the approaches could be scaled up even further, for example, to a national level. The discussions around each of these issues are summarized at the end of this chapter.
HEALTH CARE EMERGENCY PREPAREDNESS IN NEW YORK CITY1
Celia Quinn opened by stating that the bulk of the work that NYC’s Office of Emergency and Preparedness Response does to support the city’s
___________________
1 This section summarizes information presented by Celia Quinn, director, Bureau of Health Care System Readiness, New York City Department of Health and Mental Hygiene Office of Emergency Preparedness and Response, New York.
health care system to respond safely and effectively in all emergencies is directly informed by the city’s experience during Hurricane Sandy and the expectation that extreme weather events will be more frequent in the future.
She emphasized that she would be looking through the lens of health care system resiliency to tell the Hurricane Sandy story, including impacts of the storm, how the health care system responded both immediately and during ongoing recovery, and how the entire experience changed the thinking about health care system preparedness in NYC. She emphasized the importance of a resiliency approach in today’s increasingly unpredictable climate.
Additionally, she noted that she would first be drawing on the NYC Special Initiative for Rebuilding and Resiliency report, A Stronger, More Resilient New York, which was part of the mayor’s PlaNYC initiative (City of New York, 2013), and second, various health department documents, including a community checklist for health sector resilience informed by Hurricane Sandy (Toner et al., 2017). She also noted that the focus throughout her presentation would be on planning and response coordination, not infrastructure. This was not because NYC is not working to make its health care system infrastructure more resilient to a changing climate, but because planning and response are her expertise and an area in which the NYC health department is taking a lead role.
NYC’s Health Care System
Like the city itself, Quinn said, NYC’s health care system, which serves all of the city’s more than 8 million residents, is diverse and complex. She identified four sectors: (1) acute care and psychiatric hospitals, which at the time of Hurricane Sandy included three Veterans Health Administration hospitals; (2) residential providers, which include NYC’s 173 licensed nursing homes, 77 licensed adult care facilities, and more than 1,000 other resident programs that provide housing support for people with substance abuse disorders, developmental disabilities, and other behavioral and mental health problems; (3) community-based providers, which Quinn described as any provider in the community that offers ambulatory care services, including nearly 500 federally qualified health centers, more than 100 dialysis centers, 67 methadone maintenance treatment programs, and “countless” other providers located in more than 10,000 buildings across the 5 boroughs; and (4) home-based care providers, which Quinn said was difficult to describe, but the number is rapidly growing and is estimated to have been serving more than 100,000 households at the time of Hurricane Sandy.
The providers and facilities across these four sectors make up an interconnected web of health care services, with an impact to any one service having, Quinn said, a “cascading” effect on the others. To provide a sense
of the number of facilities at risk for coastal storm impacts, Quinn mentioned a 2014 analysis showing that NYC has 67 health care facilities in the highest risk flood zones. These facilities include 11 hospitals, 33 nursing homes, and 23 adult care facilities for a total of 15,289 licensed beds.
Quinn asserted that before discussing the NYC health care system experience with Hurricane Sandy, it would be helpful to discuss the city’s experience with Hurricane Irene, which preceded Sandy by about 14 months. Irene ended up causing less damage than originally predicted. Nonetheless, she said, its approach prompted an evacuation of health care facilities in advance of the storm, thus providing the city with an opportunity to test its evacuation system. Yet to some, Quinn explained, the risks of an evacuation to patients and staff, combined with the expense of the Irene evacuation operation, seemed to have been unnecessary when it turned out that the storm was not as severe as originally predicted. Ultimately, NYC and New York state used the experience to make some improvements in planning for future pre-storm evacuations. Yet, at the same time, this newly gained firsthand knowledge of the risks of a large-scale evaluation, combined with the ultimate ease of repatriation to undamaged facilities after Irene had passed, influence decision making at many levels as Hurricane Sandy approached the NYC area just over 1 year later. As a result, although lessons were learned across the health care system from responding to Hurricane Irene, Hurricane Sandy proved challenging in unexpected ways.
Evacuations and Other Impacts of Hurricane Sandy on NYC’s Health Care System
Hurricane Sandy was a highly unusual storm, Quinn continued to explain. First, it was unusually massive, with a wind field of nearly three times that of Katrina. Plus, it took an unusual course, what Quinn called “the rare westward hook,” moving out into the Atlantic before making a sharp left turn and hitting New Jersey squarely on the coast. In addition, it was unfortunately timed, making landfall coincident with a high spring tide due to a full moon. The storm surge in lower Manhattan ultimately reached 14 feet, a new record, which was 30 percent higher than the previous record set in 1960. Finally, the course of the storm pushed water up New York Harbor, leading to two different types of damage—first, wind and wave damage to coastal communities on the Atlantic coast, and second, still water flooding in the upper harbor and water damage to mechanical, electrical, and telecommunication systems.
Quinn suspected that many people can recall images of the health care evacuations that occurred as a result of Hurricane Sandy—patients being carried by hand down dark stairwells illuminated only by the light of cell phones, long lines of ambulances waiting to move patients out of nursing
homes and hospitals that were suddenly without generator power, and families searching for loved ones who had been emergency evacuated out of long-term care facilities and transferred to city-run special medical needs shelters.
Although the story of Sandy’s impact on the health care system goes beyond health care evacuations and touches on every component of the health care system, health care evacuations played an important role, Quinn continued. In total, 37 NYC health care facilities were evacuated. This included 5 acute care hospitals, 1 psychiatric hospital, 17 nursing homes, and 14 adult care facilities. The health department’s count of evacuated persons from these health care facilities was 6,451. Quinn noted, however, that this number does not include patients who were rapidly discharged from hospitals or nursing homes or transferred between or within networks in advance of the storm. She suspected that many more patients were affected. By the department’s best estimate, approximately 1,800 of the more than 6,000 persons evacuated were transported to special medical-needs shelters. Additionally, several hospitals set up long-term care units in alternate spaces, such as cafeterias and conference rooms, to accommodate influxes of evacuated long-term care residents transferred by emergency medical services.
Also, as planned, the New York State Department of Health activated the Healthcare Evacuation Center (HEC) to coordinate the evacuation and repatriation of health care facilities. HEC is led by the state health department, Quinn noted, but is supported by key NYC stakeholders, including the city’s local health department and emergency management agency, the Greater New York Hospital Association, and others. At the time, she said, HEC had been designed with Hurricane Irene–like conditions in mind, which meant that the HEC leadership and staff had to continually modify their protocols and procedures to accommodate evacuations conducted during and after the storm, as opposed to pre-storm. Plus, Quinn added, the facilities supported by HEC experienced lengthy recovery periods, complicating repatriation.
In addition to the evacuations, Quinn continued, the NYC health care system experienced many other impacts. Ten hospitals remained open and did not evacuate in spite of power outages and flooding. At least 65 long-term care facilities lost power at some point during and after the storm. More than 500 buildings that housed community providers were in inundated areas. Those 500 buildings, Quinn noted, represented 5 percent of all the buildings in NYC that house community providers. Another 1,200 buildings were located in areas that lost power. All provider types, but particularly home-based care providers, were significantly impacted by transportation disruption, travel bans, and lack of access to fuel.
Quinn explained that one result of these varied impacts of Hurricane Sandy was an overall reduction in health care system capacity. In the im-
mediate days after Sandy, city-wide hospital bed capacity was reduced by 8 percent. The same 8 percent reduction was also observed in the long-term care sector in the immediate days after the storm, with about 5 percent fewer long-term care beds available 4 weeks after the storm. Primary care and mental health services were also impacted, especially in hard-hit areas. According to Quinn, a 2014 survey conducted by the city health department indicated that, among 40 primary care providers in the Rockaways, a neighborhood in NYC, 95 percent closed or relocated at some point due to Sandy. Of those, 38 percent were closed for more than a month.
Meanwhile, as the health care system was experiencing an overall reduced capacity, Quinn added, some parts of the system were experiencing a surge in demand for services. Not only did some emergency departments see storm-related increases in emergency department visits, but the NYC health department syndromic surveillance system also identified a surge of visits for basic medical needs, including methadone (for patients in methadone maintenance treatment programs), oxygen, dialysis, and medication refills.
Key Concepts Highlighted by the Hurricane Sandy Experience
Rather than lessons learned, Quinn preferred the term “key concepts,” that is, “things that we knew ahead of Sandy, but were just really brought home by the experiences we had during that storm.”
The first is that NYC’s health care services are interdependent. Thus, even if hospitals have well-developed emergency plans for evacuation and shelter, less-resourced, non-acute, long-term care, and ambulatory services are still vulnerable to disasters. Importantly, Quinn explained, these vulnerabilities have a direct and immediate impact on hospitals.
Second, health care evacuation decision making is complex. Safe evacuation, she observed, takes time. The decision to evacuate must be made more than 72 hours before a storm arrives, that is, during a period of time when the forecast is likely to be uncertain and the weather beautiful. Because the risk of evacuating fragile patients may outweigh the risk of sheltering in place, she said, “the consequences of a decision to evacuate can truly be life or death.” She went on to say, “Of course, hindsight is 20/20, so leaders will be criticized for bad outcomes, regardless of whether their decision in the moment was the right one.”
A third key concept driven home by the Sandy experience, Quinn continued, is the need for surge spaces of different types. Special medical needs shelters and even hospitals are not designed to accommodate the needs of residents of nursing homes and adult care facilities. Yet, long-term care facilities are typically already operating at 100 percent capacity, with significant barriers to increasing surge capacity in that sector.
A final key concept is that planning for coastal storm and other natural
disasters needs to consider both immediate and long-term interruptions to health care services. Following the storm, ambulatory services in some hard-hit areas remained closed for a long period of time, Quinn observed, and some long-term facilities never reopened.
Building a More Resilient Health Care System
Quinn described several ways that these key concepts are being translated into actions to develop a more resilient NYC health care system. First are the strategies outlined in the A Stronger, More Resilient New York report (City of New York, 2013). These include ensuring critical providers’ operability through redundancy and the prevention of physical damage and reducing barriers to care during and after emergencies.
Next, Quinn remarked on the state health department having made enormous strides in improving HEC operations, specifically in developing an online system for tracking evacuations and transportation requests.
Additionally, the NYC health department has leveraged hospital preparedness programs and public health emergency preparedness funds to support a number of programs designed to improve health care system preparedness. Many of these programs, Quinn noted, focus directly on the long-term care sector. For example, the department has provided nearly all NYC long-term care facilities with radios for redundant communications, and also offers a free technical assistance program for nursing homes and adult care facilities. Since 2015, the city health department has been collaborating with the local hospital association, the Greater New York Hospital Association, to co-lead an interdisciplinary workgroup to address some of the challenges of large-scale patient evacuations. The focus has been on providing guidance for hospitals around standardized patient transfer forms and face sheets (which contain basic patient identifying, admissions, and discharge information), agreeing on definitions for bed types to facilitate the matching of patients to receiving hospitals, and working on plans for advancing access to medical records between sending and receiving facilities.
Resiliency as a Primary Goal
Quinn shared some final thoughts on resiliency and why she thinks a changing climate requires approaching health care system preparedness with resiliency as a primary goal.
First, she noted that when a disaster impacts the health care system, the system is going to break in the places where it is already the weakest. If a long-term care facility “is already squeaking by on razor-thin margins just to stay open on a good day, they are going to have difficulty accommodating a surge of 20 percent of their licensed beds during a storm,” she said.
As another example, in a community with few primary care sites, if one or more of those are damaged in a hurricane, then that community, which already had difficulty accessing care, now has no ability to access health care services. For Quinn, this observation means, she said, “health care system preparedness has to go well beyond making plans or even training and exercising those plans. We need to move towards a resiliency framework where our goal is to make our day-to-day system stronger [and one that offers] more consistently high-quality health care services to everyone in our communities.” She said that unless that kind of everyday strength and high quality is achieved, it should come as no surprise that a health care system cannot do what it needs to do when an emergency happens.
Although her remarks were based on coastal storms and the need to build more resilient health care systems with the capacity to respond to the more frequent extreme weather events that likely will occur in future years, Quinn stressed that climate change has other effects as well. In her opinion, responses to these other effects, especially as they grow increasingly unpredictable, will also benefit from using a resiliency lens to strengthen health care systems and to ensure more equitable and high-quality health care. As just one example, she cited the threat of emerging infectious diseases. Responding to this threat requires stronger day-to-day infection control practices, consistent adherence to recommended travel screening for patients with possible communicable diseases, and improved communication between health care facilities and public health authorities. As another example, the potential for worsening heat waves makes clear the need to consider adequate housing and access to city services as a public health problem and to ensure that health care facilities can manage a brief heat-related patient surge as easily as they can manage a peak seasonal flu surge.
In conclusion, to ensure the best possible outcomes for all community members, Quinn called for more resilient and adaptable systems and for stronger relationships and better collaboration before, during, and after emergencies.
PLANNING FOR CLIMATE CHANGE IN NEW HAMPSHIRE2
Matt Cahillane began by discussing how to start a conversation on climate change and its impact in the northeast without even mentioning the words “climate change.” Specifically, he suggested saying either “it is getting warmer” or “it is getting wetter” or mentioning “extreme weather,” “sea-level rise,” or “storm surge.” Not only does not mentioning “climate change” avoid argument, but, in his opinion, the conversations, particularly
___________________
2 This section summarizes information presented by Matt Cahillane, New Hampshire Department of Health and Human Services, Concord, New Hampshire.
around extreme events, can become very memorable. He showed a handful of images of past extreme weather events in New Hampshire, including images from the Keene floods in 2005, the 2008 ice storm, Hurricane Irene in 2011, and a southern New Hampshire heat wave in 2015. Using events like these as starting points for a conversation, he explained, allows him to “get in and engage people and talk about things that affected their life in the state.”
He then went on to discuss several climate and health projects currently under way in New Hampshire and work that he has been involved with under a CDC BRACE grant.
Climate and Health Projects in New Hampshire
Currently, New Hampshire is involved with four local climate-related public health projects. The first is a heat stress and elders project that has been under way in the Upper Valley, near Dartmouth College, for the past 2 years. The second, in the Lakes Region, is on habitat change, ticks, and tick-borne disease, mostly Lyme disease. The third is a storms and resilience project in the Monadnock area of the state. The fourth is another, newer heat stress study, but in the Greater Nashua area.
Additionally, the state is involved with multiple research studies in climate and health. As just one example, in the Portsmouth area, researchers are testing oysters for Vibrio bacteria to determine whether cooling and shading the shellfish can reduce the risk of foodborne disease. He noted that there have been a few recent Vibrio outbreaks up and down the eastern seaboard and that more should be expected if the water temperature in the ocean continues to rise.
In addition to these public health projects, the state is also conducting two state-level studies out of its main state offices in Concord. One is a weather and injury study at Plymouth State University; the other is a study on heat stress and emergency department visits.
The Building Resilience Against Climate Effects Framework
CDC’s BRACE framework has been very helpful for New Hampshire’s state-level work, Cahillane continued (see Figure 5-1), and he and colleagues are hoping to adapt the framework at a local level as well. He described the framework as a five-phase public health improvement cycle. The first step is the forecasting of climate impacts and the assessing of vulnerabilities. For New Hampshire, this involves working with the state’s academic institutions to downscale data from large global models so that they are applicable to New Hampshire, which has its own topography, and predicting how climate is going to change in different regions of the state.

SOURCES: Cahillane presentation, March 13, 2017; CDC, 2017.
They are trying to predict, for example, how many days will have temperatures over 95°F and how many precipitation events will involve one or more inches. These forecasts and assessments, Cahillane said, help local communities to better understand the changes for which they will have to prepare.
The second phase of the BRACE framework is projecting disease burden. This is probably the most challenging component of the process, Cahillane said. The state health department does more retrospective work than it does projections into the future, he explained. However, it does a bit of projecting work with aging and demographics. Plus, now it is attempting to predict the effect of extended pollen seasons on asthma and allergies and determine whether the effects can be quantified.
Third is the assessment of public health interventions and identification of evidence-based public health practices with known impacts on current problems and perhaps future problems as well. For example, Cahillane asked, is there a good intervention for asthma? The answer, he said, is “yes.” He referred to the CDC Guide to Community Preventive Services (CDC, 2017). But for things like weather-related slips and falls, heat stress,
and other similar issues, there is not enough information, he noted. He remarked that the New Hampshire state public health office is working to build that evidence base.
The fourth phase of the framework is developing and implementing a climate change adaptation plan, which Cahillane described as “basically, putting together a plan that looks like it is going to work well, that reflects a community’s needs and resources, and that is feasible for that same population.”
The final phase of the BRACE framework is evaluation. In other words, Cahillane asked, did what was implemented actually work? Can it be reproduced at the local level? Is the evidence base being built? Can performance be improved by understanding what has happened?
Cahillane went on to discuss in more detail how each of these five steps is being implemented in New Hampshire.
Forecasting Impacts and Assessing Vulnerabilities
In addition to working with local universities and other modeling experts to better understand some of the more complex downscaling of global data, the state health department also relies on CDC guidance to assess vulnerabilities (CDC, 2014). Additionally, they use existing tools, such as the New Hampshire Social Vulnerability Index (SVI), and websites with regional hazard data. The New Hampshire SVI, Cahillane explained, is based on Census data and is a composite indicator of more than 14 metrics, such as education, income, disability, age, and whether someone is living alone (see Figure 5-2). When a disaster hits a community, regardless of whether the disaster is natural or not, the vulnerability index provides a sense of how well a community will likely be able to adapt to the changes and helps planning at the state and, to a lesser extent, the local level.
Projecting Local Health Burdens
Cahillane reiterated the challenge of this step of the BRACE framework. One of the existing tools that the state public health department uses to assess health trends is its dynamic web portal, NH WISDOM.3 By plugging in health outcomes or behavioral issues that they want to examine, users can view county- and city-level trends. While the portal does not provide community-level details yet, Cahillane explained it is helpful because users can determine immediately whether, for example, slips and falls are higher in some regions (e.g., as they are in the greater Monadnock area) or
___________________
3 See https://wisdome.dhhs.nh.gov (accessed March 9, 2017).
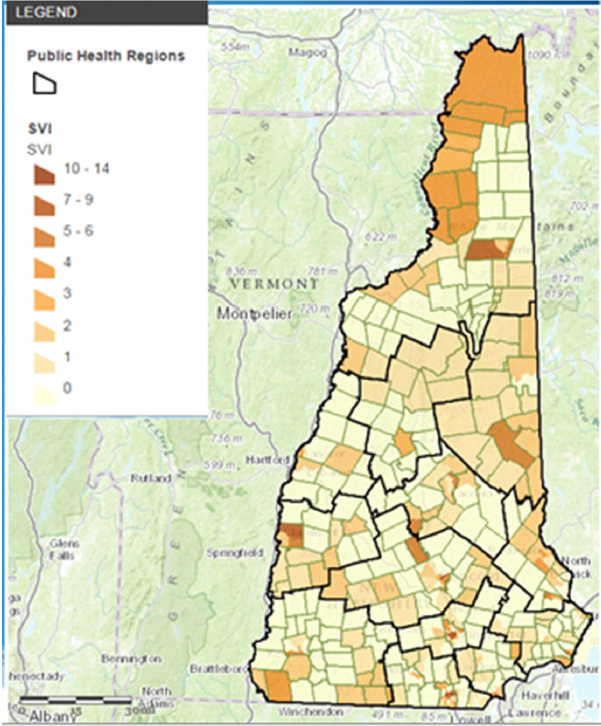
NOTE: SVI scores for public health regions across New Hampshire; scores are composite indicators of more than 14 socioeconomic, demographic, and housing and transportation metrics.
SOURCE: Cahillane presentation, March 13, 2017; reprinted with permission from Cahillane; New Hampshire Department of Health and Human Services, 2017.
lower in others (e.g., as they are in greater Nashua) compared with average rates across the state.
State-wide priority health issues that have risen to the top as a result of this work, Cahillane continued, include heat stress; habitat change (with an impact on ticks and Lyme disease); and extreme weather-related injury and resilience. Priority areas in development include the effect of rising water temperatures on bacteria (with implications for shellfish safety) and
changing precipitation and watershed-related health outcomes (e.g., the health impacts of the weather becoming wetter, or drier, depending on the season).
Assessing Public Health Interventions
Based on these priority health issues, the state health department has been working with local communities to define exposure pathways. For example, with Lyme disease, Cahillane asked, “where are the places that an intervention at the individual level would break exposure?” This could include helping individuals to avoid tick habitats, helping people to apply repellant, or helping people to learn to do tick checks. He said, “We are always looking for a place where we can break that cycle.”
In addition to defining exposure pathways, the state is also reviewing existing evidence, for example, by conducting literature reviews. But conducting these reviews at the local level is a challenge, Cahillane explained, because local health departments often do not have epidemiologists who can do this work.
Meanwhile, the state is also continually building its evidence base, for example, through work conducted as part of the New England Heat Study. In cooperation with Maine and Rhode Island, New Hampshire is trying to pull data together to evaluate temperature changes over time and their effects. He noted that this is a retrospective study in that, for example, they are examining the effects of past warmest days, not just with respect to how many people showed up in the emergency department because they had dehydration, heat stress, or an elevated temperature, but also with respect to the wide range of moderate impacts associated with heat. Cahillane noted that the number of people with respiratory, cardiovascular, or kidney disease who show up in the emergency department during periods of high temperature is actually larger than the number of people who show up for heat-related injuries—information the health department is working to share with communities.
Finally, with respect to the use of existing tools for assessing interventions, Cahillane mentioned again CDC’s The Guide to Community Preventive Services. Additionally, he mentioned the CDC Communities of Practice effort at the national level that is encouraging states to dig into the literature and understand it better.
Developing a State Strategic Plan
State-level strategic planning involves identifying ways to build workforce capacity, improving education and outreach, and improving policies. Cahillane stressed that it is not just legislation that needs to be addressed,
but also policies at the local level. This could include, for example, something as simple as deciding whether a daycare center should have an opt-in or opt-out policy for using repellants. Currently, he said, the centers have an opt-in policy, whereby parents who want repellants applied to their children must sign a form. But if repellants (i.e., exposure to chemicals in the repellants) are less risky than contracting Lyme disease, having an opt-out policy would be more effective, so parents who do not want repellants applied can opt out.
Cahillane reminded the workshop audience of the four state-level public health intervention projects currently under way in New Hampshire and then discussed in more detail the two projects that are a little further along. First, the Upper Valley Heat Project in the Dartmouth region has, thus far, involved engaging with local advisors to assess wants, needs, and hazards; hiring a regional planning commission to conduct the assessment; prioritizing areas of rising temperatures, heat stress, and injury; targeting older adults, particularly those living in the community (i.e., as opposed to living in nursing homes) and shut-ins; intervening via education lectures to caregivers and older adults on risk factors; and evaluating the results with a before and after test of caregivers’ skills in heat risk factors.
The New Hampshire Lakes Region Tick Project has taken a similar approach, Cahillane said, by engaging the local public health advisory council; prioritizing habitat change, tick exposure, and tick-borne disease (e.g., Lyme disease); targeting outdoor youth in recreation programs; intervening via education of adult recreation staff and students to decrease the risk and reduce tick exposure; and evaluating results via pre- and post-testing of staff for risky and protective behaviors.
Evaluating Impact
The evaluations of the Upper Valley Heat Project and New Hampshire Lakes Region Tick Project, Cahillane continued, have revealed a limited ability in the early stages to show quantitative change in knowledge or behaviors via pre- and post-testing. However, both projects have successfully shown some qualitative change in the amount of community collaboration among the local planning commission, recreation department, and elder care services. Additionally, Cahillane suggested that now there may be a stronger case for making changes to policy and rules via engagement with decision-makers, particularly with respect to risks for moderate health impacts. For example, through engagement with the National Weather Service, state efforts have encouraged a lowering of the threshold for when heat warnings are issued.
Lessons Learned
Cahillane concluded by listing some lessons learned. First, a standard planning process, such as the CDC BRACE framework, is worth more than the actual final written plan, which, he said, “often ends up on [the] shelf.” Plus, the framework supports greater collaboration.
Second, engaging with opponents of climate science is rarely successful for the community good. Cahillane said that, based on his experience, many people want to engage in the climate debate because they want to make other people uncomfortable and decrease civil discourse. He quoted Bernard Shaw, “I learned later in life not to wrestle with a pig. You both get dirty, and the pig enjoys it.” Cahillane explained that his intention in quoting Shaw was not to call anyone a pig, rather to emphasize that some people enjoy arguments not because they want to actually engage in discussing what might be an uncomfortable issue, but because they want everybody to feel “dirty” afterward. “If you can get everybody in the room feeling uncomfortable,” he said, “you can suppress that conversation.”
A third and final lesson learned is that a seed grant project led by a local health agency takes a lot of time, patience, and support. Cahillane estimated that getting the four state-level public health intervention projects up and running over the past couple of years has taken more than half his time and that each project has required about $60,000 to $65,000 thus far (i.e., about $20,000 per year per project from the state, plus other support).
CITY OF BALTIMORE: COMMUNITY RESILIENCE IN A CHANGING CLIMATE4
Kristin Baja began by emphasizing that some populations are more vulnerable to the impacts of climate change than others, and thus, it is important to consider equity in climate planning work. Indeed, the City of Baltimore relies on the use of equity as a lens for thinking about climate change and climate planning. Baja then went on to discuss in detail various components of Baltimore’s resilience-based approach to climate planning. First, however, she noted that the city also faces unique climate challenges, stemming from its location. Specifically, Baltimore is located at the top of the Chesapeake Bay and at the base of four major watersheds. “So we basically have water coming from everywhere,” Baja said. At the same time, the city is slowly “sinking” into the bay, she said.
___________________
4 This section summarizes information presented by Kristin Baja, Office of Sustainability, City of Baltimore, Maryland.
Baltimore’s Unique Approach to Climate Planning
Baltimore’s unique approach to climate planning is based on using the federal government’s required All Hazard Mitigation Plan and incorporating climate change into that plan. Baja described the city’s incorporation of climate change into the mitigation plan as “going a little bit against” what is expected in that it acknowledges climate change.
Moreover, not only is Baltimore acknowledging climate change, but the city is using “climate change” in all of its messaging. However, Baja explained, some of the specific language used changes depending on who is participating in the conversation. For example, she and colleagues usually talk about disaster preparedness when talking with residents or business owners. But when talking with their funding community or private partners, they talk about resiliency. She defined resiliency as: “The ability of our community to anticipate, accommodate, and positively adapt to or thrive amidst changing climate conditions or hazard events and enhance quality of life, reliable systems, economic vitality, and conservation of resources for present and future generations.” Baja highlighted “positively adapt to or thrive” as a key component of what Baltimore is trying to do with all of its climate planning.
In addition to its acknowledgment of climate change and focus on resiliency, the city also does something a little different, Baja added, by considering not just climate-related “shocks,” but also “stresses” (see Figure 5-3). Shocks are typically single-event disasters, such as fires, hurricanes, and floods. Stresses, while they can be exacerbated by shocks, are factors that pressure Baltimore on a daily or recurring basis, such as endemic violence and high unemployment. The images of recent Baltimore shocks that are shown in Figure 5-3 are ones that Baja captured on her iPhone. They include a collapsed retaining wall, people attempting to drive through 6 inches of rain that had fallen in just a few hours, and a severe storm known as a derecho. The derecho hit in 2012, knocking out power for about 7 days during one of Baltimore’s highest heat waves (i.e., 95°F and higher for that period of time). While shocks like these are expected to become more severe and more intense in the future, in Baja’s opinion, what is being left out of many conversations are the stressors.
Talking about stressors requires acknowledging the past, Baja explained. In Baltimore, it means acknowledging historic planning practices that have been intentionally racist and have segregated populations. For Baja, it means also acknowledging that she, herself, is a privileged individual who did not experience the racist and segregationist impacts of those historic planning practices. Therefore, when she walks into a room when working as the city’s Climate and Resilience Planner, the first thing she does is acknowledge her privilege and then ask if people are willing to

SOURCE: Baja presentation, March 13, 2017; (top left) reprinted with permission from Baja; Baja, 2016b; (top right) reprinted with permission from Lasinski; Lasinski, 2016; (bottom) reprinted with permission from Baja; Baja, 2016a.
sit down and have a conversation with her. She tells them that she wants to listen, hear their stories, and learn about displacement and what it has meant for their commutes and daily lives. (Baja noted that, from 1951 to 1971, 80 to 90 percent of the 25,000 Baltimore families displaced to build new highways, schools, and housing were Black.)
Baja described what is known as Baltimore’s “Black butterfly” and “white L,” with the Black butterfly representing where African Americans
have been “told” they can live since the 1910 ordinance segregating Blacks and whites by block. The white L is where most of the city’s transportation, as well as the Inner Harbor, are located. Although she did not describe its details, Baja referred to a document put together by Lawrence Brown that lists the advantages in the white L versus the Black butterfly regarding certain policies and practices (Brown, 2016). Additionally, she showed maps illustrating the socioeconomic differences between the Black butterfly and white L, with low income and unemployment being highly prevalent in the Black butterfly area of the city (see Figure 5-4).
Baja emphasized the importance of not just treating everyone equitably (i.e., by providing the necessary support to ensure that everyone has the same access), but removing systemic barriers that cause the inequity in the first place (i.e., certain historic practices and policies).
Equity as a Lens
Using equity as a lens, Baja explained, involves first prioritizing neighborhoods that have the highest vulnerability and historic disinvestment. Next, it also involves actively listening to and engaging with residents. For example, she and her colleagues stay away from PowerPoint and other presentations. They focus instead on interaction. Using equity as a lens, Baja continued, also involves thinking about new opportunities in all of the
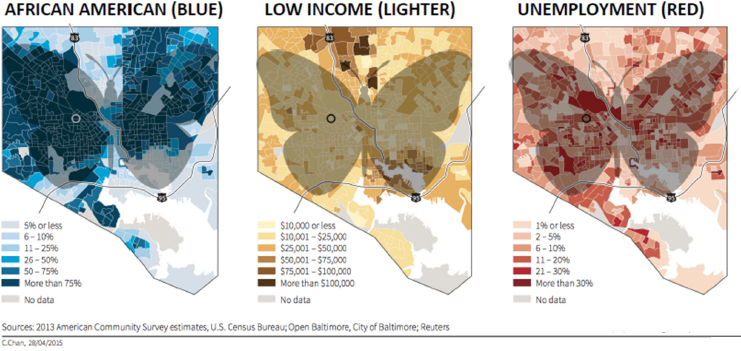
SOURCES: Baja presentation, March 13, 2017; Brown, 2016; adapted and reprinted with permission from Reuters; Reuters, 2015.
city’s different initiatives. Rather than telling people about an infrastructure change, such as a new park, they consider the “whole system” (e.g., job training, green job opportunities). Finally, they try to make sure that individuals who have been overlooked or do not have the resources to get to meetings are being reached, for example, by encouraging residents to choose meeting locations in places that they trust, such as a home, a house of worship, or a community center.
At the actual meetings, Baja and colleagues usually bring in some element that is both interactive and fun so there is additional incentive to be there. They also bring food and offer free childcare, and they try to provide transportation for those who do not have access. She showed images from one meeting, where a 24-foot-long wall of paper had been constructed to illustrate historic racism and practices in Baltimore as they relate to sustainability and resilience, including where changes have occurred and where there are issues that still need to be addressed. At the meetings, Baja and colleagues also ask residents about their own definitions of equity and sustainability, what residents are going to do, and where residents see themselves being part of the city’s efforts. Baja said, “We are looking for implementation partners, not just for feedback.”
Implementation
Baja expressed pride in the fact that Baltimore’s Disaster Preparedness Plan “doesn’t sit on the shelf.” Baja herself uses the plan on a daily basis. It has 231 actions around resiliency. The plan takes a whole-block approach, she explained, which involves thinking about not just the built infrastructure of a neighborhood, but also other opportunities with natural systems (e.g., trees and greening, storm water, heat sensors) and public services (e.g., cool roofs, weatherization, energy education, renewable energy).
An initial, immediate focus of the work that Baja has been involved with in Baltimore, and a focus that Baja perceived as being key to initiating many other city programs, was enhancing community preparedness. They help communities to make plans, build kits, and help each other. The make-a-plan component of the work involves sitting with residents and helping them create an emergency plan and identify their evacuation and sheltering opportunities. The planners also work together with residents to build the emergency kits, rather than the city handing out kits and saying, “Here is your emergency kit.” Baja explained that they talk about every single item that is in the kit, such as how to hand-crank the radio and how to use the solar panel to charge phones. Finally, the help-each-other component of community preparedness is, in Baja’s opinion, the most important piece. It involves doing a lot of asset mapping with community members to identify what exists in the community and what is missing.
Baja went on to discuss several of the community disaster preparedness activities under way, starting with help and safe signs. She described Baltimore as a city of row houses, with tiny streets and many houses packed into those streets. To help the community emergency response teams, as well as first responders, in this environment in the event of an emergency, the city has developed help and safe signs that can be placed in windows indicating whether an occupant needs additional assistance. Baja recalled how they were able to distribute signs to many, but not all, of the 265 Baltimore neighborhoods before the 2015 riots and that many households where the city had conducted outreach did in fact use them during those riots.
Residents have identified several missing pieces in the community preparedness work, Baja continued. For example, many residents do not have access to opportunities to evacuate because they do not have vehicles. Additionally, many residents are not setting aside extra food or water because they are dealing with multiple jobs, childcare, or other pressures on a day-to-day basis that keep them from proactively preparing. The largest missing piece, though, Baja said, is that many residents do not have a safe place to go where they can find trusted information.
In response to the need for safe places with trusted information, the city is currently piloting the concept of resiliency hubs. Baja was unaware of any other city in the United States that has adopted this concept, although she noted that Los Angeles has taken an interest. She defined a resiliency hub as consisting of “a building or set of buildings and neighboring outdoor space that will provide shelter, backup electricity, access to fresh water, and access to resources such as food, ice, charging stations, etc., in the event of an emergency.” Baja and colleagues are working with members of communities to identify trusted neighborhood sites that are already being used daily, such as houses of worship or community centers, that could serve as resiliency hubs. Once these sites are identified, the program then provides funding to enhance or make the site more resilient, for example, by installing solar panels with battery back-up and by providing materials for storing food and water. Thus far (i.e., at the time of this workshop), four pilot hubs are already operational and another two are potentially opening within the next year. The hubs are also being used by other city programs, including health department programs.
In addition to the help and safe signs and resiliency hubs, another specific community-level tool being implemented as part of Baltimore’s disaster preparedness efforts is its ambassador program, a peer-to-peer engagement network of more than 150 ambassadors who help with outreach. The program has divided the city into 10 districts with similar population sizes and assigned a team leader to each district. Each district also has a lead ambassador and several community ambassadors. The team leader
and ambassadors have gone through several trainings on equity and sustainability over the past year and have been provided with toolkits that have surveys, draft presentations, and other tools. Baja remarked that the ambassadors themselves help to design these toolkits, which she said has been “great” because their involvement ensures that they receive the tools they need.
Another key piece of the city’s disaster preparedness efforts, Baja continued, is that instead of just thanking community members for telling their stories and providing information, she and her colleagues in the city office show how they are actually using the information. One way they do this is through Baltimore’s Every Story Counts campaign, which Baja described as a communications campaign “about the amazing people that live in Baltimore that are doing things on their own without support.” She showed an image of a group of women who help immigrants and nonnative English speakers to find resources, health care, and other opportunities within the system.
Additionally, the city makes use of Turtle, a character who Baja and colleagues thought would be a fun way to talk about climate and resiliency with kids. As it turns out, Baja said, adults like Turtle just as much as the kids do. A turtle was chosen not only because turtles are native to Maryland, but also because they carry their homes on their backs and are adaptable to both land and water. Thus, Baja said, they serve as a good image for messaging about preparedness.
Baja and her city colleagues also use a lot of games in their trainings. As an example, she mentioned the “Game of Floods,” which was developed through the Urban Sustainability Directors Network and that the city is adapting for use specifically in Baltimore. The game is actually a vulnerability assessment, Baja noted, but is much more fun and engaging than a typical vulnerability assessment. Players pick a role and then identify how much money and resources are available for that role.
Finally, Baja commented on the many other Baltimore initiatives that her office integrates into its own work, for example, via the resiliency hubs. An example is Vacants to Values, a strategic demolition and vacant lot revitalization program. Baja said, “We are seeing vacant lots as opportunities, rather than something that is negative.”
In conclusion, Baja mentioned that she and her colleagues are trying to measure the impacts of many of these programs as they go along. For example, they have installed 250 heat island sensors in the communities to see if any of the retrofitting they have done to the built environment is having an impact. They are also conducting trainings for community members not just in emergency response, but also in tree care and planting and weed removal.
DISCUSSION
Following Baja’s presentation, she, Quinn, and Cahillane engaged in an open discussion with the audience. Some of the questions were directed at specific state-wide or city-wide climate planning programs (i.e., NYC, Baltimore, or New Hampshire), while others were addressed to all panelists (e.g., funding for their respective programs).
The NYC Health Care System: Collaboration Across Sectors
Moderator Paul Biedrzycki asked Quinn how the four sectors of NYC health are interlinked in other ways in addition to preparing and responding to hurricanes and other weather-related emergencies. Quinn replied that she would be remiss if, in talking about NYC’s health care preparedness efforts, she did not talk about health care coalitions, which she said have been an important national initiative. NYC has several types of such coalitions, with about 23 of them coalescing into what she described as a “coalition of coalitions,” through which all four sectors of the health care system are represented. Additionally, she mentioned increasing efforts to conduct planning exercises and trainings across sectors and the success they have had over the past couple of years bringing health care partners into health department exercises. For example, in 2016, the NYC health department solicited help from a couple of representatives from large health care systems in the planning of a cyber-attack exercise to ensure that the exercise was as realistic as possible. The representatives also participated as observers in the actual exercise.
When the panelists were asked by an unidentified audience member whether any of the communities or agencies conducting emergency preparedness are more likely to also be coordinating health care delivery more generally, Quinn replied that it “goes both ways.” Many changes are under way in the health care delivery system, with many people being taken care of at lower levels of care. This is impacting how hospitals think about emergency management, she said, or at least “it should be” changing how they think about their emergency management programs. Her hope is that, at the same time, all of this emergency preparedness work is also impacted by day-to-day service delivery. “It is my belief,” she said, “that if we are planning for things that are only going to be pulled out during an emergency, we are, first of all, losing an opportunity to improve the health care system that really needs a lot of improvement. But we are also designing systems that are not likely to work in an emergency because they are not being used day to day.”
As an example, she mentioned an NYC health department project being done in collaboration with the Greater New York Hospital Association to
develop improved patient transfer forms. She and her colleagues sat down with a broad group of stakeholders from different health care systems and transfer centers, including physicians, nurses, and emergency managers, to agree on a set of fields of critical information that are necessary for taking care of a patient who is being rapidly transferred during an emergency. The form has since been disseminated to all hospitals, Quinn said, and all hospitals have been asked to implement it as their day-to-day transfer form. In fact, some of the hospital systems have started working with their electronic health record vendors so that simply pushing a button pulls those fields from a patient’s electronic health record. Once this new form is implemented city-wide, Quinn said, the city will have a system whereby all hospitals are using the same information to transfer patients. Not only will transfers be safer, they will also be quicker, improving hospital throughput and making the form a win–win improvement. “We want to see our preparedness program more focused on those day-to-day improvements,” she said.
Hurricane Sandy Evacuation
Quinn was asked by an unidentified audience member whether any data were collected on the impact of the Hurricane Sandy evacuation, with such a sharp disruption in the lives of the estimated 6,000 persons evacuated from health care facilities. For example, were any data collected on mortality or other outcomes? Quinn answered that the estimate did not account for patients who were quickly discharged or transferred before the evacuation order. To her knowledge, no such data were collected.
Alert Fatigue
Sanne Magnan asked the panelists whether, as storms increase, they expect to see any kind of alert or disaster fatigue and if their agencies will work with communities around this fatigue. “I know that people in our agency have disaster response fatigue,” Quinn replied, “myself included.” But there are benefits, she remarked. Having frequent emergencies allows for practicing emergency responses and improving those responses. However, she said, as she had described with Hurricane Irene, “you sometimes take away the wrong lessons.” Also, she said, there is the “boy who cried wolf phenomenon,” which she suspected people in NYC were feeling right “now” (i.e., on the day of this workshop), in light of the “big storm” being predicted for “tomorrow” (i.e., the day after the workshop). In sum, she said, “Yes, we are contemplating a future where we are activated more continuously and trying to figure out how to adapt our systems to meet that challenge.”
Cahillane commented that he and others in northern New England are working with the National Weather Service on that exact issue. Fortunately, he said, northern New England is protected by a temperate environment where it does not get that hot, yet new public health data show that even moderate heat can impact people as much as extreme heat. He asked, “So how is that going to change the number of alerts we do per year?” It used to be that only one or two alerts a year were put out when the temperature rose above 100°F. Lowering that temperature to 95°F would increase the number of alerts per year to about four to eight. The number of alerts is not the only concern, in Cahillane’s opinion; another concern is the way meteorologists communicate to people, nearly every day, he said, “about something else that is going on.” He said, “People are getting hit with a lot all the time.”
Baja added that in Baltimore, they try to be strategic with their alerts by differentiating among audiences and identifying those who are most vulnerable. For example, people living in flood plains have already experienced massive impacts. The city has thus established with them a categorical rule to evacuate regardless, given the risk of flash flooding. She described Baltimore’s flood plains as “some of the most flood-prone waterways in the country,” with some areas experiencing a 20-foot rise in less than an hour. “Because those areas have been flooded out in the past, they listen,” she said. But it is different with residents, which is why she and her office are placing such an emphasis on making the resiliency hubs fun locations, with games, where people already congregate and spend time.
Baltimore: Incorporating Climate Planning into the All-Hazard Mitigation Plan
Terry Allan of Cuyahoga County Board of Health, Ohio, asked Baja to elaborate on the City of Baltimore’s approach to community-level emergency management. Allan suggested that other communities could emulate that approach. Baja responded that the work began in 2012, when her office decided they wanted to be proactive, rather than reactive, because they knew they were going to “keep on getting hit with these events.” They did it as part of their all-hazard mitigation plan, she explained, because the methodology used in that plan is almost exactly the same as that of a climate adaptation plan. She called it a “very natural overlap.” That is, first, they assessed hazards and vulnerabilities based on historic hazards, then they identified how they were going to mitigate those hazards. Then, they approached both their Maryland emergency management agency and Federal Emergency Management Agency Region 3 representatives and asked if they would be willing to allow this approach. Baja said, “We are really lucky
to have some good support at both the state and federal levels at the same time.”
Now, she said, climate change is 100 percent integrated into the all-hazard mitigation plan. Every action in the plan encompasses climate scenarios, allowing the city to integrate climate change into other big initiatives (e.g., an initiative related to flood plain management). She added that, in her opinion, as climate science changes and as climate hazards occur more frequently, the more these documents should be updated to plan for climate scenarios.
When asked by Jonathan Patz about the importance of optimizing both preparedness and adaptive capacity, Baja said, “We can’t just do actions on mitigation anymore. They have to have co-benefits for adaptation.”
Patz also asked Baja if any of the community initiatives that her office has been developing are paying off in ways that had not been expected. She mentioned some work they have done with the Waterfront Partnership, where they installed a solar-powered water wheel, “Mr. Trash Wheel,” that collects trash from Jones Falls and helps to keep the Inner Harbor cleaner. A couple of added benefits of the wheel are that it keeps boat-clogging agents out of the harbor and that it provides educational opportunities about the use of solar power. As another example, their flood plain work has also provided both educational (i.e., for the real estate community) and insurance (i.e., reduced insurance rates) co-benefits.
Funding
The panelists were asked by an unidentified audience member where they find funding for the different projects and programs they described. Baja replied that Baltimore has been able to secure funding from the Maryland Department of Natural Resources and the National Oceanic and Atmospheric Administration Office for Coastal Management. But the “really cool stuff” they do, she said, such as Turtle and the Every Story Counts communication campaign, is funded through outreach and philanthropy.
In New Hampshire, CDC provides most of the seed money for the projects Cahillane described, he said. “Without a doubt,” he said, “it is all the supporters in Congress and the administration who believe in this work and want to get it done.” Additionally, he underscored the importance of the support of people in the community who want to engage and who give in-kind and work extra hours.
Scaling
Raymond Baxter, a health adviser, observed that all of the programs described by the panelists embody comprehensive planning approaches.
He asked the panelists about the extent to which their respective programs had been scaled up from something that someone else has already done. Additionally, he asked what it would take to then scale up, to a regional, state, or national level, some of the ingredients contributing to the success described by the panelists.
Baja replied that in Baltimore, rather than scaling up, in fact, local officials are scaling down from the larger, national climate datasets. She also emphasized the usefulness of finding trusted contacts in other places with similar histories to share information, such as which toolkits are most useful, and identifying opportunities for the integration of climate planning into other plans. For example, like Baltimore, Milwaukee also is one of the most segregated cities in the country. Trusted experts can be useful too, she remarked, that is, experts who can help to translate information from the scientific and academic communities.
The NYC health department has been working with the NYC health care system since the beginning of the CDC-funded Hospital Preparedness Program in the early 2000s, Quinn commented. Much of that work, she said, has focused on the acute care sector. It has allowed the department to build strong relationships with emergency managers in all of the NYC hospitals. Only since 2013 have they prioritized expanding those relationships and reaching other sectors of the health care system. She said they have seen some success with long-term care, but are still challenged by urgent care, which she said is a rapidly growing and hard-to-enumerate sector of the system. But her greatest worry, she said, in terms of vulnerability to future emergencies, especially coastal storms, is with home-based care. In terms of scaling up even further what NYC has done, in her opinion, that will require strengthening more of the connections among sectors and then bringing that strength to their regional partners across the state, in New Jersey, and throughout the rest of the area.
For Cahillane, the question is, “How do we ensure that the tax dollars we use and the things we do in state government aren’t a waste?” With respect to the BRACE framework he discussed during his presentation, the intervention assessment phase is the one phase where the expectation is that those conducting the assessment will go and find out whether anyone else has implemented the intervention and, if so, if it has been implemented in a similar population. “Let’s gather the good work that has been done already,” he said, “before we jump forward and put it to work.”
Baja added that rather than making more toolkits for local governments, what is needed is “somebody to identify what toolkits actually work.” In response, Pamela Russo mentioned Alonzo Plough’s work in Los Angeles, where he designed a study to test a toolkit in eight different regions of the city, two neighborhoods per region, with some of the neighborhoods receiving standard of care and the others a resilience training
for preparedness (i.e., resiliency to either a hurricane or earthquake or to daily economic or violent stressors). Different components of the evaluation have been published, according to Russo, with respect to which aspects of the toolkit worked and how they refined the kits. The work includes both qualitative and quantitative results.
This page intentionally left blank.




























