5
Potential Strategies for Strengthening the Nation’s Health Security
Our understanding of the health security and disaster landscape has been evolving, Inglesby remarked. It is an opportune time to rethink some strategies for strengthening the nation’s health security by building on successful programs and experimenting with new approaches. Although many workshop participants and presenters seemed to agree that there is room to advance, the numerous suggestions for where and how the improvements should be implemented demonstrated that focus, prioritization, and agreement among stakeholders are a necessary first step. By developing and realizing a collective vision, we can advance health security in the United States.
RETHINKING STRATEGIES
Dodgen called for shifting the conversation away from reacting to the most recent disaster response. He explained that devoting attention to the past is part of why funds are consistently appropriated to singular types of disaster or response strategies rather than system-wide preparedness and resilience. Evolve toward construing preparedness as a general concept, suggested Kurilla, rather than identifying a threat and then focusing on being prepared for that threat. Putting a one-size-fits-all system in place for responding to a wide range of emergencies will not work, he warned. Similarly, David Blazes, senior program officer, Epidemiology and Surveillance, Vaccine Development, Global Health Program, Bill & Melinda Gates Foundation, suggested focusing on preparedness itself as a significant area, rather than as a precursor to response. Often, Blazes noted, critical gaps
are not exposed until a threat presents itself: for instance, the poor quality of dengue diagnostics became apparent only after the emergence of the Zika virus.
DEVELOPING A SHARED AGENDA
Maher called for a clearer distinction between reactive preparedness (the current state) and proactive preparedness, which should be the nation’s objective. Stripling called for national distillation of the mission of health care and public health preparedness, response, and recovery in a way that is specific enough that it can be tied to specific data points and can be measured using an agreed-upon set of metrics in the future.
According to Maher, achieving this goal will require establishing a common definition of the problem and the shared dilemma. Even though each group or each perspective brought to the table will work toward that common objective in a different way, Maher emphasized that the different pieces of the puzzle must fit together: “That is the future of public health emergency management. How do we get to the table to break down some of those barriers, recreate the rules, or evolve the rules so that we can do these things quicker and then they’ll be more well thought out, more effective, more efficient, and we can do more with less?”
Phillips also recommended establishing a clear, credible mission, with public and congressional support, that details what is required to fulfill the charge to preserve and protect the nation’s health security. She also noted that a global partnership is necessary for domestic preparedness. Hick explained that preparing for a range of physical, cyber, and human threats requires setting goals and objectives, identifying the infrastructure that needs protection, carefully assessing and analyzing those risks to that specific area, implementing risk management activities, and then measuring the effectiveness of those interventions to the degree possible.
Marinissen provided ideas for changing one paradigm by framing international assistance and response as a national security issue rather than a selfless humanitarian act. She illustrated with the example of a longstanding cooperative agreement with Panama that provided a small amount of financial support ($100,000 per year). As a direct result of that existing relationship, Panama was willing to provide desperately needed samples to U.S. labs to develop and validate diagnostics during the onset of the Zika virus outbreak. She warned that in the case of a potential emergency requiring diagnostics and protection for all Americans, as well as the rest of the world, CDC is the only entity capable of doing so rapidly and disseminating the information:
There are going to be many situations, like MERS-CoV or Zika virus, where we are going to need samples or we are going to need countermeasures or supply chain products from other countries. We have to be very strategic. This does not mean that we are going to help 196 WHO-member states and give our money freely without evaluation, without proper metrics, but we need to be very strategic. We need to see what is the benefit for our nation.
Shah suggested leveraging the fact that most Americans support international efforts to improve health in developing countries. Hanfling called for more direct engagement with international partners, by first looking, in particular, at WHO Global Reform and the Global Emergency Workforce, and then promulgating and moving forward a very distinct strategy that brings states, USAID, HHS, and DoD together as domestic partners to work with international partners in clarifying response objectives. Sharon Medcalf, director and assistant professor, Center for Biosecurity, Biopreparedness, and Emerging Infectious Diseases, University of Nebraska Medical Center, also suggested concentrating on international collaboration, such as by conducting joint forums with WHO, Médecins Sans Frontières, and other international organizations, and beginning with a small number of collaborative projects that are low-hanging fruit.
PROMOTING A CULTURE OF LEARNING AND SHARING
Multiple participants highlighted the need for the field to adopt a culture of learning and sharing, most notably by culling and applying lessons learned from past experiences, particularly during inter-emergency periods. However, Kurilla advised against focusing too heavily on lessons learned and, in effect, “always fighting the last war.” Find balance between celebrating successes and learning from every experience, suggested a participant:
It is deep in our DNA that every outbreak is a chance to find out what is going wrong; every difficult case is a chance to figure out how to do it better next time. That is how we are trained, how we think, and how we improve. We need to have a very firm barrier between that and also telling the story of the successes. We need to learn things from what we do not do well enough. But at the same time, we cannot be shy about telling stories of successes.
Blazes suggested making failure more transparent and learning from it. Stripling suggested creating an easily accessible national database or data warehouse of lessons learned from 10 years of detailed after-action reports and how they have been applied across jurisdictions, which might be housed at the NLM.
Hu-Primmer explained that rapid data collection, rapid aggregation, rapid transformation, and rapid analytics all feed into a “data life cycle” that helps to refine and better understand what additional data need to be collected. A potential focus area for moving forward, therefore, is facilitating rapid bidirectional communication to ensure there are positive optimal outcomes; to improve preparedness, response, and recovery efficacy and effectiveness; and to make sure decision makers have the right information at the right time.
Research should be integrated into ICS if it can be done on a quick-enough feedback loop that it will actually improve the response, according to Stripling. He noted that in the Zika virus response, they attempted to formally integrate research into ICS via an ongoing quality improvement unit tasked with improving response and partnering with research organizations to carry out collaborative studies. This strategy was not fully successful because the timeline required to carry out sound scientific research is longer than the response timeline.
Do not treat paradoxes the same way you treat problems, advised Pavia: problems have solutions that are achievable through creativity and persistence; paradoxes are fundamental problems that cannot be fixed (e.g., people do not appreciate prevention until something bad happens). He warned that devoting too much effort to attacking paradoxes leads to frustration and that fundamental paradoxes should be accepted as a state of being and the focus should be on problems that can be solved (e.g., how to engage more partners rather than getting them to appreciate preparedness in advance). Phillips urged the government to become more creative and innovative in finding solutions to recurring challenges, such as communicating the importance of health security.
PRACTICE AND REINFORCEMENT
Effective collaboration, trust building, and understanding others’ perspectives can only come from practical experience, noted Runnels: “You cannot think your way into a new way of being.” Redd concurred, noting that organizations need experience working with other organizations to improve cross-cultural understanding and operational barriers.
Lien reflected that local communities are being asked to fulfill a tremendous amount of preparedness, response, and recovery capabilities, but they are not being provided with the time and resources to focus on building sustainable systems and infrastructure. She suggested that focusing on a smaller number of objectives, rather than many of them, would improve the ability to achieve sustained long-term improvements.
Exercises are a simple way to practice and reinforce new ways of doing business. Employ a more aggressive exercise schedule to boost collabora-
tion and productivity using serious drills with real evaluations, advised Bruce Evans of the National Association of Emergency Medical Technicians. Marinissen proposed using exercises to bring the complex issues of responding to national and global health security threats to those who have access to the resources and the ability to make decisions. She suggested working with HHS/ASPR and DHS to create a series of exercises on the need to invest in pandemic preparedness targeted to the financial sector (both public and private). Danila made a similar suggestion of carrying out exercises and tabletops with federal and state elected officials about the spread of a highly lethal microbe in the United States to demonstrate the importance of maintaining the core public health infrastructure.
Managers and leaders should reward the behaviors they want to see repeated and avoid inadvertently rewarding the wrong behavior, advised Dodgen. At the policy level, he explained that reinforcements include funding and attention to certain populations and issues, and the few incentives currently available may not be for the right things. He suggested rewarding positive behavior such as “above and beyond” collaboration, multijurisdictional exercise, coordination, and innovation.
BUILDING THE EVIDENCE BASE FOR POLICY AND OPERATIONS
Many attendees highlighted a need to improve the evidence base for preparedness, response, and recovery. Phillips noted a lack of time spent evaluating progress in the field over the previous 15 years and suggested putting in place an evaluation process to strategically assess what works and what does not across broader and more expansive activities, new responsibilities, new organizational structures, and grant programs that have expanded or collapsed.
Goodman suggested promoting the concept of disaster science, which involves both the inter-emergency science agenda and the during-emergency science agenda (e.g., how to collect data during the event to enable a more effective response). He suggested finding ways to further both those agendas and connect their needs to funding by defining and disseminating science gaps and the research agenda. Develop an action plan to use the ever-increasing amounts of data being collected, not just for the response side, but from a science preparedness perspective1 commented Phillips, who also cautioned against over focusing on infectious disease at the expense of being continually aware of the threat space.
Arnesen remarked that the NLM is home to the NIH Office of Data Sci-
___________________
1 Phillips noted key questions to consider: What data are a common element? What are we learning from that event? How are we turning that immediately back into preparedness and response?
ence, whose new strategic plan focuses heavily on data science and applying the FAIR—findable, accessible, interoperable, and reusable—principle. She explained that the concept of data preparedness (from the Harvard Humanitarian Initiative) connects data, decision making, and response. The aim is to promote the ability of organizations to be ready to responsibly and effectively deploy and manage data collection and analysis tools, techniques, and strategies in a specific operational context before a disaster strikes. Arnesen suggested collaborating with the field of data science, which encompasses open data, data collections, data integration, interoperability, data analysis, translation, knowledge and information management, and dissemination.
Leesa Lin, Harvard University, suggested developing a “rapid science response,” a meaningful, rapid assessment that allows evidence to be used quickly to inform response and decision making. Blazes proposed applying the concept of “precision public health” and promoting open, transparent access to data, because “the best public health decisions will require the best data and in many ways, that equates to the most precise data.” He suggested that data precision is an equity issue (e.g., precision of determining the risk of transmission of Zika virus in neighborhoods), because everyone deserves to have that level of precision when public health decisions are made. Data precision will require better disease surveillance, better civil registration, better lab diagnostics, and better education.
ENCOURAGING THE INTEGRATION OF SYSTEMS
Levy called for a paradigm shift toward conceptualizing health care, public health, the business community, and other sectors as parts of a whole that need to be integrated to provide a better environment for the community at large and better care for the community on a day-to-day basis. She recommended considering what can be done in preparedness and emergency response that contributes to providing everyday care, and conversely, what is being done in everyday care that can also translate into being prepared. Blazes noted that the federated database system has its challenges, but it provides opportunities for incorporating innovations within each of the components for better surveillance and response efforts.2
At the local level, Redlener emphasized that effective recovery requires centralized infrastructure coordination (which is currently lacking) to manage local assets, state assets, federal assets, nonprofits, insurance companies, and banks. In the best-case version of recovery, he suggested, surviving victims would have a case manager who is aware of all of the various governmental and nongovernmental assets available and would coordinate them
___________________
2 A federated database system is a type of meta-database management system that transparently maps multiple autonomous database systems into a single federated database.
for the survivors. In the worst-case version of recovery, surviving victims must become their own case managers, despite dealing with tremendous emotional stress, and find available assets, access them, and complete their recovery on their own.
Marinissen offered several suggestions for how the United States could integrate with international preparedness and response efforts, including participating in the worldwide implementation of IHR to establish a better understanding of the world’s global capacity to respond to emergencies. She pointed to the WHO Health Emergencies Programme as a clear global lead to coordinate emergency response and called for finding ways for the U.S. system to integrate with that structure, as well as developing frameworks to support WHO. Domestic areas of focus highlighted by Marinissen include a better understanding of how the U.S. ICS and National Response Framework align with the WHO health emergency programs.
When deciding who to bring to the table, include those decision makers as well as the stakeholders who can help push efforts forward, suggested Barone, not just people who are already in agreement about what needs to be done. He suggested including C-level and government decision makers, customers, end users, patients, and other people in the community who have no background in preparedness but who will be using these services as the ultimate endpoint. George also suggested broaching questions and challenges that decision makers are currently facing, or anticipate facing in the near future, to a range of people working across sectors. Think outside the box by bringing in people from outside health care and emergency preparedness to brainstorm, suggested Freda Lyon of the Emergency Nurses Association and vice president of WellStar Emergency Services.
Look to sectors outside the federal government who are studying how to engage with communities, suggested Phillips. Aaron Firoved, National Biosurveillance Integration Center, DHS, advised that when convening stakeholders from across sectors, health care information needs to be translated and considered in practical terms and in other sectors’ contexts. Dodgen suggested convening people with different needs and engaging them meaningfully, as well as integrating efforts with existing ongoing activities in other systems. For instance, he suggested targeting groups of people who regularly access government-sponsored social services or health care systems such as home visiting, federally qualified health centers, Meals on Wheels, senior programs, and education systems. He suggested that disaster preparedness could integrate with scout badges, American Red Cross, Voluntary Organizations Active in Disaster, emergency department/EMS actions, or HPP coalitions.
At the nexus of the domestic–international interface, Marinissen suggested strengthening both U.S. domestic health security and international health security through multilateral and bilateral partnerships that would
include the creation of frameworks parallel to the international community that could be activated and integrated during an emergency response. Hanfling maintained that coalitions and partnerships matter greatly in response efforts, and that this is an opportunity to build on coalitions like the Coalition for Epidemic Preparedness Innovations and better recognize what resources should be invested within communities, across sectors, and across agencies. Finally, he stressed the importance of supporting rather than slashing budgets.
OPTIMIZING THE EXCHANGE OF INFORMATION
To mitigate the effects of disasters on health care systems, Margolis emphasized that an interoperable, robust, patient-centered electronic health information exchange (HIE) system must enable clinician and patient access to critical information regardless of where they receive care. George noted that key next steps are finding the appropriate technologies and policies for accessing, protecting, and using information from EHRs to facilitate information exchange in a safe and productive way. Hu-Primmer highlighted several of the legal issues that must be resolved, such as data ownership, data use agreements, patient privacy, and cybersecurity. In an increasingly digital world, she explained, electronic data are constantly being uploaded, downloaded, and transmitted wirelessly via many moving pieces feeding into the same gears,3 which must be in place and well-greased in advance to facilitate centralized coordination. To be useful, she maintained, these data must be sent to a centralized location so they can be aggregated and available to extract, manipulate, and analyze.
Ensuring interoperability of data across disparate systems nationwide is critical, according to Stevens (see Box 5-1). Successful interoperability requires building trust to share data, he explained. Technical advancements are needed to ensure data can broadly be sent, received, found, and used, but stakeholders must also address inconsistencies across data formats, problems around data quality, and a lack of trust that inhibits sharing. Unique patient identifiers are not currently used in the United States, although Stevens maintained that they would solve many problems with human error and input. Stevens suggested that a key strategy moving forward will be finding ways to ensure the interoperability of electronic health data working across disparate systems across the country. The target outcome is a learning health system enabled by nationwide interoperability that supports all stakeholders, especially individuals and providers (see Figure 5-1).
___________________
3 Hu-Primmer noted that these pieces include primary care, specialty care, social services, pharmacies, first responders and EMS, EHRs and other health applications, wearables, hospitals, points of dispensation, and public health.
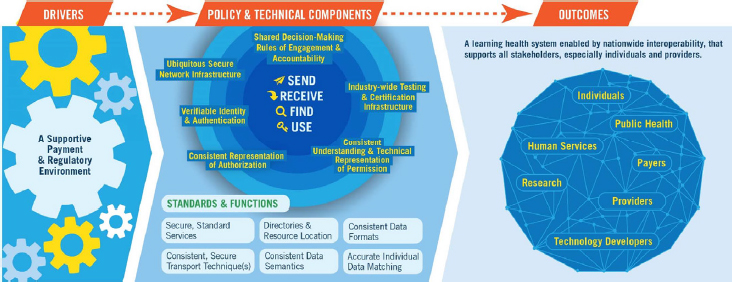
SOURCES: Stevens presentation, March 8, 2017; from the U.S. Department of Homeland Security.
SITUATIONAL AWARENESS
Developing a system that creates better health care situational awareness would directly improve decision making, according to Margolis. He recommended promoting greater health care situational awareness as a means of capacity building and system strengthening: “By increasing situational awareness and incentivizing the partners to come together, we can not only improve our preparedness for disasters and public health emergencies, but also make more informed decisions every day.” He offered an example from the aviation industry, in which airlines had information about their own safety profile, but were unwilling to share this information due to fears it would be used against them by competitors or the government. To resolve this, the Federal Aviation Administration created and supported the creation of a system known as the Aviation Safety Information Analytic System, a neutral third space to bring everybody together. Through that forum, the airlines identified what information they were willing to share with whom, under what circumstances they were willing to share, and how that information could and could not be used. Most importantly, he noted, this public–private partnership brought the owners of the information together with other interested stakeholders by creating a value proposition that incentivized collaboration. He suggested that a similar system would provide a better understanding of the health care and public health ecosystem (e.g., resources, supply chain, costs, quality, workforce, safety, outcomes, use patterns, planning) during disasters and public health emergencies. Margolis specified that comprehensive situational awareness requires integrating many different data sources, including EHRs, but also other sources of data such as operational data, administrative data, scheduling data, workforce data, inventory management data, and social media information.
MATCHING DATA TO NEED
Stripling remarked, “We have been hungering for data for centuries, for millennia, but . . . the story is not the data. The story is in the impact. . . . We have to focus on our mission on the territory we have to win. Focus on consequences, why we are doing what we are doing, what those objectives are, what those activities are, how we accomplish it. If we can do that, we will be able to force the data within that framework.” He described the New York City health department’s approach for focusing on the objective, not the data, in order to avoid going down the “data rabbit hole.”
Stripling used the 2015 Legionella outbreak in New York City as an illustration of the importance of defining the mission first, then applying the relevant data. The outbreak was known to be caused by one or more dirty cooling towers in an area around the Bronx borough. The health department began assessments, sampling, and outreach to determine the location of the tainted cooling towers based on epidemiological knowledge. The media questioned the status of the thousands of unregulated cooling towers across the entire city, causing an uproar. Rather than allow the primary mission (i.e., identify the dirty towers) to balloon, the health department stayed focused on the primary objective and the data needed to meet it. After identifying the source of the infection, the mission expanded to include regulating cooling towers.
Map the critical data needed to make decisions, recommended Brinsfield, in order to structure the data to the established mission. She suggested picking out the data pieces that are bridges, measuring them, and then mapping those critical places so that state and local public health agencies are provided with precisely (and only) the data they need to make successful decisions. Runnels suggested incorporating the relevant stakeholders into the development of metrics to ensure that only the critical data are mapped.
MESSAGING AND MARKETING
Firoved noted that government officials tend to move slowly in crafting the messaging, and if the government is too hesitant to step into that void, someone else will. He recommended that messaging should be early but accurate, and delivered by trusted speakers who have been identified beforehand. For example, he noted that although CDC is one of the gold standards for public trust about health messages, a local health provider or local fire chief is even more effective at the community level.
Dodgen suggested designing messages for people who need to be persuaded to garner funding, attention, and diligence to preparedness: “We tend to design messages for people who are already persuaded.” Hick suggested framing messages in ways that can be digested and appreciated in
the way that social media are consumed by the public, as well as building local-level trust and using local messengers. Messengers also matter; Laura Holgate, senior fellow, Belfer Center for Science and International Affairs, and visiting scholar, Institute for International Science and Technology Policy, The George Washington University, noted that there is a “ready-made set of civil society communities and private-sector business who all have connection points on the Hill. If we are trying to get the Congress where the American people are, then we need some influencers who are not simply the defenders of federal budgets within the federal government.”
Dyjack, Abramson, and Dodgen suggested using storytelling to attract sustained support for and investment in preparedness, response, and resilience. According to Kurilla, public health needs are there and people recognize them, and so creating a narrative about what public health does as a way to make a case to a wider audience and allow them to come to their own conclusions is more effective than trying to convince them of a belief from the public health professional perspective.
MAKING THE BUSINESS CASE FOR INVESTMENT
Multiple participants suggested the importance of making compelling return on investment (ROI) analyses to catalyze investment in preparedness, response, and recovery. Brinsfield suggested quantifying the cost of inaction and being more transparent with the public about gaps in public health preparedness and the impact on public safety. Develop an ironclad set of priorities and rationale on why health care and public health preparedness investments should not only be maintained but increased, advised Roslyne Schulman, senior associate director, American Hospital Association. Hick stressed the importance of developing convincing arguments in order to demonstrate an ROI, to protect the institution, and to protect the safety of employees and the community. He called for better examples of business impact analysis for health care and compelling case studies for existing health care infrastructure and ROI arguments. Quantify and articulate the potential losses due to a lack of preparedness,4 suggested Evans, and consider bringing a health economist to the table to assist. Wolf suggested using risk assessment tools and enterprise risk management to make the case for investment. Lin emphasized that evaluation and cost-effectiveness analysis are needed to demonstrate ROI, which will be required to move the public emergency preparedness agenda toward improvements.
___________________
4 For example, Evans noted that if a power grid is down for 10 days, what does that loss look like for pharmaceutical sales when a retail pharmacy does not have backup power and cannot scan labels to get medications out?
FINANCING MECHANISMS
A number of participants suggested solutions for evolving government funding and acquisition rules. At the federal level, Barone proposed finding ways to connect the dots between HHS agencies and to expedite the movement of funds, as well as using contracting and procurement to engage creative minds and innovation from the private sector. As examples of private-sector engagement, he suggested contracting with the private sector to put in place the mechanism of rapid procurement and solicitations. Barone also suggested putting interagency agreements in place to improve the agility of the federal government regarding moving money, as well as adjusting restrictions on how monies can be used during emergencies. Seek out and develop creative funding proposals, suggested Pavia, especially those more closely analogous to insurance, such as an excise tax, that are funded through a constant stream and would allow money to be put forward into a trust fund.
Stripling suggested creating financial guidance to assist local-level public health agencies with the creation of funding packages for federal support and specific assistance for components such as taxes and insurance policies. He additionally suggested producing a financial base plan for diversifying preparedness funding that does not diminish the federal need for grant funding.
Barone drew attention to the overreliance on federal funding and the resulting complacency, arguing that disasters are local, so investment should be local: “Convince local leaders to start investing in local preparedness, or the infrastructure will fail.” He noted that federal programs will inevitably change, but reliance on those programs has created local-level expectations that they will continue to receive federal funds in perpetuity. He commented that “businesses and the private sector look at this as business continuity; the government looks at it as continuity of operations; if we don’t look at public health in the same way and fail our mission, what’s going to happen?”
Consider local-level levers such as surcharges, betterments, or revolving funds to provide resources to support disaster preparedness response and recovery, suggested Runnels. Doug Halley, transportation coordinator, CrossTown Connect, and former director, Acton Public Health Department, noted that in Washington, DC, and other communities with a similar influx of workforce and tourism, it is important to consider every tool possible to understand what the critical need is and what financial mechanisms can be brought to bear. He reported that having partnerships with local businesses has been a useful way to achieve common and overlapping objectives (see Box 5-2).
Lien agreed that there should be more local investment, but warned
that it can be difficult for local communities, coalitions, and health care partnerships to find local businesses willing to contribute, cautioning that there are often a host of assumptions made about how foundations and private-sector businesses are willing to invest. She suggested that communities approach such conversations in more organized ways by helping to define the business case and frame the message to justify and garner investment at the local level and giving it a frame of context so as to justify and present the advantages of investment. Convene private-sector leadership at the national level to discuss priorities and investment preferences, recommended Lien, in order to provide the community-level stakeholders with context and realistic expectations about what they are willing to fund.














