In digital health, public and private sectors have primarily relied on a “push” approach, in which the public and private sectors push technologies out to the communities and programs, to deliver health through technology-enabled initiatives. In contrast, “pull” programs rely on empowering communities to provide their input into the technologies they want and need to address their specific health-related challenges. Such community-driven pull approaches, which get buy-in from both sides from the start of a project, can increase the acceptance and adoption of innovation from both the system that is establishing technologies and the individuals using the technologies. Questions arise as to how communities can be empowered to take an active role in pull programs, what incentives are needed to create the pull from communities, and what role community health workers can play in promoting pull from their communities. Such an approach can benefit from documenting the outcomes of digital health initiatives in order to understand what is driving success or scale.
This panel addressed these issues using examples of pull programs in the digital health space in low- and middle-income countries (LMICs). The panelists were Christoph Pimmer from the University of Applied Sciences and Arts, Northwestern Switzerland FHNW; Adele Waugaman from the U.S. Agency for International Development (USAID); Larissa Fast, Fulbright-Schuman Research Scholar at Uppsala University and the University of Manchester; and Kaakpema Yelpaala of access.mobile International. Robert Bollinger moderated the panel and the subsequent open discussion with the workshop participants.
SOCIAL MOBILE MEDIA TO CONNECT, TRAIN, MANAGE, AND EMPOWER HEALTH WORKERS
In his work, Christoph Pimmer has focused on the role that mobile social media, including social networking applications such as Facebook and instant messaging applications such as WhatsApp, can play in supporting health professionals in general and community health workers specifically (Pimmer and Tulenko, 2016). Social media platforms, he explained, fall on a spectrum between those applications for small and bounded groups, or closed user groups, such as WhatsApp, and applications that can tie together large, nearly boundary-free networks. A major difference between mobile instant messaging and social network sites is accessibility, where instant messaging apps are simple and, in the case of WhatsApp, enable the exchange of audio messages that make them particularly useful for people of lower literacy levels, while social networking applications are usually more complex and also require higher levels of digital literacy to use effectively. Pimmer noted that almost all of the projects he and his collaborators have implemented with nurses and health workers in Nigeria, South Africa, and Zambia use WhatsApp as the primary social media platform.
Mobile social media can provide four key functions for health workers: social, knowledge-related, organizational, and political. The social dimension is centered around professional connectedness that, Pimmer noted, addresses professional isolation, which the World Health Organization (WHO) has identified as an important cause of the attrition of community health workers and nurses (WHO, 2009, 2010b). One example of how social media can increase social and professional connectedness is a Facebook site created independently by a Nepalese doctor. Tens of thousands of users, including doctors, other health workers, medical students, and even patients from Nepal and across Asia exchange some 1,500 interactions per week via this Facebook page. The discussions have included sharing experiences, the discussion of professional identities, values, medical procedures, and answering medical questions (Pimmer et al., 2012). In recent, still unpublished work, Pimmer and collaborators found further associations between social media use and professional connectedness. The findings suggest that the informal and nonguided use of WhatsApp by Nigerian nursing students during their clinical placements in the field can be associated with lower levels of professional isolation and higher levels of professional social capital.
In addition to connectedness, almost all mobile social media spaces promote forms of formal or informal knowledge exchange, said Pimmer. Informal knowledge exchange and learning is common, he said, in groups or teams of community health workers or nurses, and he has seen many
examples of these health workers using mobile social media to support one another in problem solving and learning activities. Results from a recent survey study underpin the value of mobile instant messaging technologies, such as WhatsApp, to enable knowledge creation and sharing, collaborative problem solving, and supporting formal education and professional development across a wide range of global health settings.
Social network sites are increasingly popular. Nurses in rural South Africa, for example, use a closed Facebook group, which they access via their mobile devices, to consult among themselves when facing difficult cases (Pimmer et al., 2014). There is also potential to successfully leverage social networking sites in formal education settings. Pimmer and his colleagues have used closed Facebook groups to teach and coach rural nurses and midwives (Pimmer et al., 2016a,b). He said:
Of course, social mobile media spaces are not better than specific learning platform in terms of their functional repertoire, but their distinguishing feature is accessibility, which means in many contexts these tools are already in the hands of health professionals.
Another advantage can be reduced technical support needs. He added that in a project in South Africa, his team observed that nurses were asking their children or their neighbors’ children for technical help with Facebook when needed and very little support from the project team was required.
The organizational function of mobile social media can help manage and coordinate what is often a distributed and remote workforce. Recently, said Pimmer, he studied how rural community health workers in Malawi used WhatsApp groups to organize campaigns, meetings, and drug distribution efforts involving workers in widely dispersed communities (Pimmer et al., 2017). Such organizing efforts increased the speed at which the health workers would complete their tasks and projects. In much the same way, social mobile media can give health workers and the communities in which they work the opportunity to organize themselves across communities in remote regions, and by doing so, increase their ability to accumulate and exercise power. In one instance, some 1,500 emergency department staff members in Taiwan created a Facebook group to voice concerns about poor processes and other work-related problems in their facilities (Abdul et al., 2011). Within weeks, this group had triggered what Pimmer said was a “quite stunning, multipart dialogue with different stakeholders, including the health ministry and even the health minister.” Eventually, breaking down communicative and hierarchical boundaries via social media resulted in the initiation of a reorganization process which had not been possible before.
In the digital health landscape, mobile social media can play a complementary role to the more traditional function that most digital health tools play today, which is to capture and process structured health data and transmit them to a central authority. Mobile social media, in contrast, offers opportunities for more flexible and less-structured communication, particularly among groups or networks of health workers. Given the massive adoption patterns of mobile social media that are already occurring among health professionals, health workers, and communities, these informal virtual communities and networks are likely to grow with important implications for improving care in LMICs. However, to fully leverage the potential of the emerging media landscape, it is important to address associated constraints and risks in a proactive manner, Pimmer said in closing. This involves the consideration of issues such as digital professionalism (e.g., learning how to protect a patient’s privacy), the economics of participation (avoid further excluding the most marginalized groups), information quality (i.e., spreading of rumors and false news), and regulation related to the spread and use of mobile social media in health care.
VALUE PROPOSITION FOR PULLING DATA FROM THE COMMUNITY
Adele Waugaman’s role in the USAID Global Health Bureau has been to support the development of interoperable and scalable digital technologies to overcome some of the fragmentation and duplication of digital health systems that affect health care delivery in LMICs. As an example, she discussed the research she and colleague Larissa Fast conducted on how data and information flowed in West Africa during the 2014–2015 Ebola outbreak there and whether digital technologies made a difference in those flows (Fast and Waugaman, 2016).
During the course of interviewing some 130 people representing 60 organizations, Waugaman said that she and Fast heard anecdotes reporting that it could take as long as 3 weeks to get Ebola case information from the field to the central government offices for inclusion in the weekly situation reports on the outbreak. However, when digitized from the point of collection, data and information could flow more quickly and efficiently—up to 38 times more quickly, and with 21 percent fewer errors, according to research by the Gobee Group (Fast and Waugaman, 2016). Digital technologies also increased the plurality of the actors engaged in data collection and management. “We saw examples of citizens and frontline health workers communicating directly with health ministries and nongovernmental organizations in ways that were not possible at scale without the digitization of data,” said Waugaman. In addition, they
saw an increase in the directionality of data and information flow so that information—along with acknowledgments and appreciation—could flow from health ministries back to the communities as well as horizontally among peer groups. With paper-based case records, she explained, data moved primarily one way out of the communities for aggregation and decision making, with little information flowing back to the communities about what was happening in neighboring districts, for example.
Turning to specific examples, Waugaman discussed the mHero project, which was run by IntraHealth in close collaboration with the Liberian Ministry of Health and with support from USAID and other partners. This project was unusual, she said, in that it was successfully piloted during a crisis, which is not an optimal time to test new technology. In this case, however, the mHero technology was integrating two systems that were already at scale—the IRIS human resources information system and the RapidPRO SMS bulk text messaging program—and was able to knit them together in a way that enabled the Liberian health ministry to communicate directly with its remote and widely scattered workforce. Waugaman explained that during the outbreak, many health workers fell ill or were otherwise not reporting for duty, so the health ministry needed some way to understand who was available and what training level they had received. “Setting up direct, real-time communications between health workers and the ministry of health enabled them to do that,” said Waugaman. The success of this project, she noted, can be seen in the technology’s continued use today by the Liberian Ministry of Health, which has incorporated these two-way, digitized communications with its remote workforce into the national digital health strategy.
Another example of pushing data out of the community was the Ebola Community Action Platform (ECAP), a project in which numerous nongovernmental organizations used digital data and information they collected on mobile phones about community knowledge, attitudes, and perceptions about Ebola. These data, said Waugaman, were critical for informing the social mobilization response that proved to play an essential role in stemming the spread of Ebola. This program, led by more than 800 social mobilizers, reached some 2 million people in more than 3,000 communities across Liberia by using phones with Open Data Kit software and the WhatsApp peer-to-peer group messaging app. ECAP aggregated the data coming from Liberia and made it publicly available so social mobilizers involved in the Ebola response could gain insights into how they could leverage current understanding of the outbreak to change behavior through better messaging.
One of the benefits of the ECAP project was that it gave workers who were going into complex and, at times, dangerous environments a peer-to-peer messaging platform that they could use to keep in touch
with and provide encouragement to others who were doing similar work. Waugaman said that many field workers reported that this peer support was critical, in some cases even more important than financial compensation, in motivating them to continue to work in difficult conditions. She also heard reports that United Methodist Church clergy in West Africa, who used the WhatsApp mobile chat platform to communicate with one another prior to the Ebola outbreak, were using it to report on cases in their communities. In one instance, a clergy member in Sierra Leone saw that a woman likely infected with Ebola was being transferred to a clinic that would have been unprepared to treat her. He used WhatsApp to alert the right people so that the patient could be diverted to a properly resourced clinic.
The use of digital technologies also increased accountability, said Waugaman. For example, in Guinea, the use of GPS-enabled smartphones to collect contact tracing data created an additional layer of transparency around where, specifically, data was collected. It also enabled managers to see where there were gaps in data that were coming in from the field in near real time, enabling them to identify possible problems and correct them quickly. Finally, she said, the use of real-time data improved programming to make it more directly relevant in the field.
The Dey Say Program in Liberia, run by a nongovernmental organization called Internews, used a combination of text messaging and non-digital media to learn what rumors were spreading in communities and then address those rumors. UNICEF created a short code phone number that it provided free of charge to hundreds of health workers, nongovernmental organizations, and volunteers on the ground throughout Liberia. The short code could be used to report, by text, rumors about Ebola in their communities. The program analyzed the rumors and provided corrected information to local broadcast journalists, who were able to host locally recognized and trusted experts to debunk rumors over the radio.
These examples, said Waugaman, illustrate how digital technologies can help both pull data from and push data to communities and engage community members in public health initiatives. However, she cautioned, “This is not just an ‘add water’ type solution. There are a number of different supporting and corollary investments that need to be made to enable the effective integration of digital technologies.”
To illustrate what some of those supporting investments can be, Fast described what the data situation was like at the beginning of the Ebola outbreak in Liberia. As Waugaman had mentioned, case information from health facilities were initially collected on paper. At one point in the outbreak, some 500 cases per week produced up to 5,000 pages of information that had to be digitized and updated per week. This helps to explain time delays in getting data from around the country to the health ministry.
Once the data were aggregated, they were released in situation reports published on PDFs that were not machine readable, and therefore were not easily accessible for other purposes, such as publishing the data on dashboards, disease modeling, or forecasting.
Another issue was that field workers collected data on a number of different platforms and sent the data to the ministry via multiple reporting streams that often ended up in different data silos. For most nongovernmental organization workers, Excel spreadsheets served as the primary mechanism for data collection, but some treatment centers had electronic data collection too. For the latter, that raised questions about how to keep and use digital data in a “hot” (or Ebola-contaminated) zone, as well as how to maintain and then decontaminate electronic equipment in a hot zone. Combining these variables with the lack of common standards and data-sharing protocols complicated the compilation and aggregation of data across systems and actors, said Fast.
On top of that, there were inconsistencies in the terminology used to describe Ebola cases. For example definitions of the primary categories of suspected, probable, and confirmed cases differed across the affected countries, and in some cases, those definitions changed over the course of the epidemic. While not surprising given that the responses themselves were run by the national governments, it meant that aggregating across the countries became more difficult during the outbreak.
Based on this experience, Fast and Waugaman came up with a set of recommendations that they encapsulated in a visual aid adapted with permission from the data use cycle created by PATH and its partner Vital Wave (see Figure 5-1). These recommendations, said Fast, echo many of the comments made throughout the day, such as the need for standards for coordinated investment in health infrastructure to support digital health, as well as economic and social development and investment in the physical infrastructure needed to extend digital connectivity. As an example of the latter, Fast showed a map comparing cell phone coverage for West Africa in 2014 and those regions suitable for zoonotic, or animal-borne, disease outbreaks. The map revealed that there was a complete lack of cell phone coverage in some areas most suitable for zoonotic disease outbreaks. Another mapping exercise comparing cell phone coverage and the location of health facilities in Liberia showed why health workers in some clinics were unable to report on the outbreak. In some cases, said Fast, the workers had connectivity, but lacked the funds to contact the national coordination centers.
These and other analyses led Fast and Waugaman to recommend that countries should conduct baseline surveys to identify the strengths and weaknesses of their digital infrastructures. Other recommendations address some of the personnel and institutional needs, and Fast said that
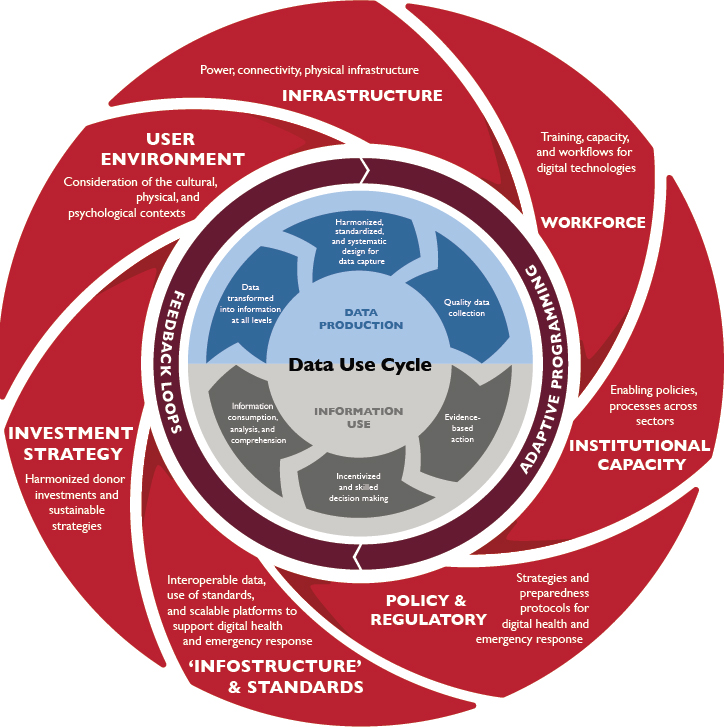
SOURCES: As presented by Adele Waugaman on May 10, 2017. Adapted with permission from the Data Use Cycle graphic created by PATH and Vital Wave (https://www.usaid.gov/sites/default/files/documents/15396/FightingEbolaWithInformation.pdf [accessed January 19, 2018]) for publication in Fighting Ebola with Information by Larissa Fast and Adele Waugaman, 2016.
one key lesson from the report was that personnel and institutional shortcomings are often more difficult to address than technical ones. “Technological solutions exist,” said Fast, noting that addressing institutional and workforce capacity, such as policies, processes, workflows, and data literacy take time to address. As a result, while data and technology may solve some problems, they often create new ones that arise from a lack of trained data scientists and analysts and governance policies.
Fast noted that while technology enables the generation of an ever-increasing amount of data at an ever-increasing speed, there is still a lack of understanding about how cultural, social, and behavioral issues can either promote or prevent the use of data or even digital technologies. “It is a physical context issue, but also about social aspects and whether people trust the information source,” said Fast. Trusted messengers, she said, are crucial, as is the ability to collect data in both online and offline environments. In addition, while data visualization can help promote data use, having too many dashboards displaying information that does not respond to the specific needs of the intended users is not necessarily helpful, she said. The final set of recommendations from their study was to coordinate investments in digital health, as well as in the development of common standards on both technical aspects and content to enable data to be shared and compared.
BOTTOM-UP INNOVATION TO IMPROVE PATIENT ENGAGEMENT
When Kaakpema Yelpaala, a public health practitioner who had worked in the Caribbean, East Africa, and Ghana, founded access.mobile in 2011, his goal was to address the challenge of sustaining impactful digital health solutions with a business model not reliant on funding cycles and trends of donors. He used private investments to build a digital health company that engages with communities and the private sector directly on a value basis for the benefit of patients.
His approach was to listen, learn, and evolve. Whatever technology access.mobile would develop would be built from the ground up using human-centered design principles and tailored to market needs with essential functionality. This approach was informed by many years on the ground, repeatedly asking questions of potential users, understanding their needs, and continually improving the technology in response to those needs. One of the advantages of working with mobile and Web-based solutions is that they can be easily adjusted, expanded, and evolved, said Yelpaala. His team relies heavily on evidence-based solutions, user feedback and data, and their own personal experiences in the field. Bottom-up innovation, Yelpaala added, requires addressing a significant problem that users want fixed and to do so with the simplest product possible. Getting feedback from early adopters is important to the process, as is providing users with information and incentives to try and keep using the technology.
Yelpaala noted that access.mobile is a growth-stage company that raised money from friends and family and then a Series A investment to fund its initial growth. Some 150 hospitals and clinics serving approxi-
mately 2 million patients use its end-to-end patient engagement solutions and generate between 100,000 and 200,000 messages a month related to patient health concerns. At the time of the workshop, the company was in the process of increasing its reach to 400 facilities, with three out of the top four private hospitals in Kenya using his solution as well as private hospitals in Uganda and Tanzania, and was building partnerships with large companies and the teenager companies Neal Myrick discussed earlier. In Yelpaala’s opinion, the way for a small company such as his to engage in a public–private partnership is to first establish partnerships with bigger organizations to help overcome initial market challenges and credibility while remaining nimble to adapt and innovate to market needs until ready for scale.
Among the challenges for developing and implementing digital health solutions in Africa, said Yelpaala, are the need to create the space for digital health, which is a new and evolving market in Africa, and the need to change the way people seek and use health care. It is also challenging, he said, to develop a business model for scaling in a market driven by foreign aid and nongovernmental organizations and in which there is limited capital available for growth. The lack of interoperability, connectivity, and readiness to adopt digital technologies are additional challenges. At the same time, he said, there are opportunities to push the digital frontier of health care in Africa. Partnerships, he said, can increase benefits and decrease fragmentation, and policy developments could enable governments to facilitate advances in the quality and value of health care. The awareness of digital health benefits is also increasing in Africa.
Yelpaala noted in closing that there is no one-size-fits-all solution for every user in any ecosystem. His suggestion is to think about end users in clusters, to engage with and develop solutions for each cluster, and to be flexible in the solutions offered to the users.
DISCUSSION
Robert Bollinger commented on the two models for leveraging information technologies that were presented. The first model, described by Fast, Pimmer, and Waugaman, was the more organic of the two in that it provides communities with mobile phones, social media tools (or using technologies which already exist), and support and lets the users develop or adopt applications. The second model, presented by Yelpaala, is a more structured approach for delivering information technologies to communities that relies more on finding ways to build in responses from the community and optimizing delivery. Given those two models, he asked the panelists for their thoughts on how much of this work should be
organic versus structured and strategically incentivized. In particular, he explained, he was thinking about community health workers, who are used to going out and getting what they need and therefore might be more amenable to an organic approach, but who could benefit from strategic incentives in the form of pay-for-performance or professional development, for example.
Pimmer replied that community health workers need support, but unfortunately, they are perhaps the last members of the health care ecosystem to be given access to technology and the associated support systems. Nevertheless, he added, the deployment of digital media and especially of mobile instant messaging is gaining momentum, and it will be in the hands of many more community health workers in the near future. The first challenge then, he said, is that the general social mobile media apps may be too generic for some forms of usage by community health workers, and would need to be complemented by special apps, which are more complicated to implement and that is where the organic evolution of these technologies will need support. However, a great deal of basic communication functions can be already realized with the help of openly available and widely used tools. To foster the bottom-up adoption, his approach has been to go into communities and learn about innovative practices that communities and health workers are developing and then help them to spread those innovations to other communities. However, he commented, given the risks and challenges associated with the current adoption patterns of mobile social media, health workers, health professionals, and health care organizations do require more systematic guidance on how to use social media tools in a responsible way aligned with ethical guidelines and to assess the effect of their social media activities.
In thinking about how to further empower community health workers with information technologies, Waugaman said that there needs to be a shift in the way organizations think about who will be mining and consuming data. In most cases, health care organizations and government ministries are used to being the ultimate authorities on data, but they will need to figure out ways of sharing data effectively with the sources of the data to better empower frontline health workers and other health care providers. This shift in mindset becomes easier when moving from a paper-based data reporting system to one where data are recorded, transmitted, and analyzed in digital form—but it still needs to occur, and it will take time. Bollinger added how important that culture shift is given that the next Ebola epidemic will not be detected initially by researchers from a U.S. university, but by community workers. “Community health workers have to be incentivized not just to wait for a question, but to actually contribute to this system,” he said.
Bollinger remarked that the LMIC setting, with fewer legacy systems,
offers the opportunity to try new things, particularly with regard to delivering care in a disseminated manner, that is, out from centralized facilities and into local communities. He asked the panelists for recommendations on how to better leverage the community-based care model and technology to better manage both disease outbreaks and chronic care, both in the setting of underserved populations and back into the more traditional setting of Western medicine. Yelpaala replied that solutions can come back into the Western context, but it will require the right partners to translate solution approaches from one market context to another.
Fast agreed that context is crucial, and Pimmer added that the development of digital professionalism will have to be a part of any effort to make better use of community health workers regardless of the setting. Waugaman, with the final comment, said that large donor organizations and nongovernmental organizations will need to learn to listen to a larger audience that is communicating in new ways and tie that back to the customer through adaptive programming.
This page intentionally left blank.














