PROGRESSING BEYOND CONTINUING EDUCATION
Holly Wise, American Council of Academic Physical Therapy
As part of her opening remarks, Wise asked the workshop participants, “What is high-value continuing professional development (CPD) and does it make sense to support it?” Wise said that the topic of CPD is of critical importance because a workforce of knowledgeable health professionals is essential to the discovery and application of health practices to prevent disease and promote well-being. However, the professional workforce is not consistently prepared to provide high-quality health care and ensure patient safety. Referring to the 2010 Institute of Medicine (IOM) report Redesigning Continuing Education in the Health Professions, Wise highlighted the authors’ conclusion that the continuing education (CE) system for health professionals was not working, as there were major flaws in the way that CE was conducted, financed, regulated, and evaluated. The authors further determined that a new comprehensive vision of CPD was needed to ensure that all health professionals engage effectively in a process of lifelong learning aimed at improving patient care and population health. CE is often associated with didactic teacher-centered learning—using methods such as lectures conducted in auditoriums—and is associated with seat time or continuing education units rather than competency units. In contrast, CPD is a more holistic approach that encompasses a broader variety of learning methods and theories, said Wise. CPD is learner driven and tailored to individual needs, and includes concepts such as self-directed learning and practice-based learning. CPD “stretches beyond the ‘classroom’ to the point of care,” concluded Wise.
CPD IN THE CONTEXT OF A HEALTH PROFESSIONAL’S CAREER
Ronald Cervero, Uniformed Services University of the Health Sciences
After this broad overview, Cervero continued the discussion by looking at CPD in the context of a health professional’s career. He said that CPD “is by far the longest phase” of any health professional’s career. The other phases—general education, specialized prelicensure programs, and induction into practice—are of comparatively short duration (see Figure 2-1). However, while there has been an incredible amount of financial resources and intellectual and regulatory effort put into the other phases in order to build a “magnificent system of health professions education,” there has been much less investment in the final and longest phase. Cervero said “We send out our health professionals for 30 to 40 years, pretty much on [their] own.”
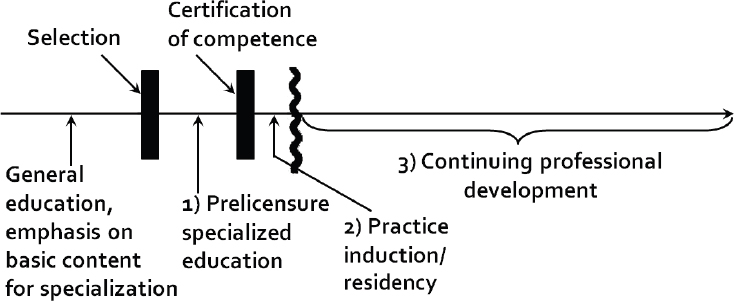
SOURCE: Presented by and used with permission from Ronald Cervero, April 6, 2017.
Cervero brought the conversation back to outcomes and quality by citing efforts of the International Pharmaceutical Federation to progress and adopt their definition of CPD (FIP, 2014), and the 2010 IOM report that emphasized performance improvement over seat time (IOM, 2010). He noted five goals from this 2010 report for preparing health professionals that were first described in the 2003 IOM report Health Professions Education: A Bridge to Quality. In it, the authors state that effective CPD should ensure that health professionals can provide patient-centered care, work in interprofessional teams, employ evidence-based practice, apply quality improvement, and use health informatics (IOM, 2003). According to Cervero, using these elements creates a seamless system of lifelong professional development that begins in the first two educational phases and continues through professional development. To effectively incorporate these elements into CPD interventions, Cervero said that CPD should do the following:
- Be learner driven
- Be tailored to individual needs
- Use a broad variety of learning methods
- Include organizational and systems factors
- Focus on clinical as well as other practice-related content, such as communication and business
Cervero noted the progress that has been made in recent years in defining and promoting CPD in the United States, with systems of accreditation, recertification, and relicensure beginning to move away from CE and toward CPD (see Chapter 5). A recent article in Academic Medicine talks
about why this broad view is so important (McMahon, 2017). In it, he said, continuing education is described as having evolved into what is now a multidisciplinary approach for “engaging clinicians where they live and work and learn.” It includes teamwork, mentoring, real-time feedback, technology-enabled learning, and relationship building.
But despite such progress, what has been largely unexplored is the concept of the value of CPD. How can high-value CPD improve quality, safety, and effectiveness? How can high-value CPD meet the quadruple aim of health care—improving population health, enhancing patient experience, reducing per capita cost, and improving work life of health care providers? Can the value of CPD be measured and quantified in a way that makes a convincing business case for investing in CPD? To begin answering these questions, Cervero turned the podium over to Elena Karahanna, professor of business in the Management Information System Department at the University of Georgia, to walk workshop participants through the process of building a business case.
MAKING A BUSINESS CASE
Elena Karahanna, University of Georgia
Karahanna first defined the purpose of a business case:
to provide the basis for making a decision as to whether or not to move forward with a specific project. . . . Therefore, it has to describe the initiative, it has to justify why this particular initiative is needed, it has to identify the costs, and it has to identify the benefits that will be derived from this initiative, and it also has to identify any risks that might derail the project.
Karahanna noted that while there are numerous templates that can be used to build a business case, there are five essential components: problem description, business requirements, business benefits, costs, and risk assessment and feasibility. Karahanna used an example of a health maintenance organization’s (HMO’s) diabetes management intervention to elucidate each component of the business case.1
Problem Description
The problem description is the why of the business case: Why is there a need to take action? What is the problem, and why does it need to be
___________________
1 This example is based on the field report “The Business Case for Diabetes Disease Management at Two Managed Care Organizations: A Case Study of HealthPartners and Independent Health Association” (Beaulieu et al., 2003).
solved? What is the general idea behind the solution that is being proposed? Karahanna noted that a problem description must be both compelling and convincing both in terms of the problem and in terms of the proposed solution. It must describe a real problem that is worth solving in an effort to convince the decision maker, who is typically the investing entity, that the proposed solution has the potential to actually address the problem.
The example, diabetes, is one of the most common—and most costly—chronic diseases. Lack of proper treatment can lead to blindness, end-stage renal disease, nerve damage and amputations, heart disease, or stroke. Diabetes care is often poorly managed, and the disease exacts a high toll on society in terms of health costs and lost productivity. Over the past 5 to 10 years, new types of care management strategies for diabetes have emerged and been adopted by some providers. They all fall under the definition of disease management. Different programs offer different services, but a few key elements are common to all programs. The basic idea is that diabetic patients’ long-term health can be improved and medical care costs can be saved if patients learn about their disease and become active participants in managing their health. The focus of disease management is on prevention and control rather than on acute care. The aim is to improve the coordination of care and reduce the number of hospitalizations and severe complications among diabetic patients.
Business Requirements
The business requirements description is the how component of a business plan. How will the described problem be addressed? What are the specific components of the proposed solution? What is the scope of the project, and what is not included in the scope? Who are the stakeholders, and how will they be involved? During this step, it may be appropriate to perform a needs assessment in order to fully understand stakeholder perspectives and the needs of the targeted community. This may involve, for example, interviews or focus groups, mapping processes and identifying inefficiencies, error-prone steps or pain points, examining best practices, and performing gap analyses.
For the diabetes example, a diabetes management intervention must include the following:
- Patient and physician education
- Programs about weight control and other lifestyle changes for members
- Adherence to clinical guidelines
- Nurse case management
- Monitoring and tracking
Business Benefits
Defining the business benefits of a project answers the what questions. What are the business objectives that the project aims to achieve? What are the benefits (e.g., reduced cost, improved quality) that will be derived from the project? Business objectives need to be specific and verifiable, associated with a time frame, and associated with a stakeholder.
In the diabetes example, the objectives are many:
- Reduce costs for specialist visits by 30 percent by year 2.
- Reduce the number of emergency room visits by 5 percent during the first year and by 25 percent by year 3.
- Reduce hospital inpatient stays by 20 percent by year 3.
- Reduce costs from managing blindness by 12 percent by year 5.
- Reduce the number of amputations by 35 percent by year 5.
- Reduce the number of end-stage renal failures by 40 percent by year 5.
- Reduce hemoglobin A1C levels by 15 percent by year 2.
- Increase the average life expectancy of diabetic patients by 2 percent by year 5.
- Achieve an average of 80 percent of the patients being satisfied with the program by year 2.
Costs
The fourth component of a business plan estimates the costs involved in carrying out the project. These costs can include both development and operating costs, tangible costs (e.g., salaries of training staff), and intangible costs (e.g., loss of employee morale). Costs should be quantified, if possible, and should identify stakeholders and timeframe.
In the diabetes example, two types of costs are defined—development costs and operating costs:
- Development costs
- Development cost of the system (information technology personnel salaries, software, hardware)
- Costs of developing educational material for patients and physicians
-
Operating costs
- Higher premiums for health insurance (for patients)
- Costs of additional nurses and administrative staff
- Increased costs because of more visits to nutritionists and exercise counselors
- Increased lab costs
Feasibility and Risk Assessment
The final component of a business case assesses the risk of a proposed initiative from a financial (see next section), organizational, and technical perspective. It is designed to answer two questions: (1) Can we proceed with this project, and (2) If so, should we? The feasibility assessment looks at whether the organization has the means and expertise to carry out the project. For example, is there organizational knowledge of the domain, and does the organization have the financial resources, human resources, organizational capacity, and time to commit to the proposed activity? The feasibility assessment also involves performing a stakeholder analysis to identify potential resistance to the proposed initiative by specific stakeholder groups, especially those groups whose buy-in and cooperation are critical to the success of the initiative. The risk assessment considers the potential risks of proceeding (or of not proceeding), and whether these risks can be mitigated. The risks may be tangible or intangible and may include risks to the organization as a whole, to individual health professionals, to the patients, or to other stakeholders.
The diabetes example includes the following considerations:
- Technical considerations
- Does the organization have the technical know-how to develop the initiative? If not, can it hire external expertise?
- How large is the initiative?
- How complex is the initiative (e.g., how many interdependencies does it have, how many organizations/units does it involve)?
- Identify stakeholders, and ask the following for each stakeholder group:
- Do the potential users like the idea?
- Will the users actually use it if it is implemented?
- Do they have reasons to resist it? Are there any negative effects?
- How much power do they have? Is their resistance material to the success of the initiative?
- Things to consider include the following:
- Lack of time
- Lack of incentives
- Power shifts
- Fear of change of job responsibilities
- Fear of loss of employment
- Reversal of long-standing procedures
- Loss of control
- Organizational considerations
- Do the organization’s power people support it?
- Does it fit the strategy and long-term plans of the organization (strategic alignment)?
- How well does the new system fit the organizational culture?
Financial Assessments
Once the problem and potential solution have been described, and the benefits, costs, and risks of the project have been identified, financial analyses can be performed (e.g., cost–benefit, cost-effectiveness, cost utility, or cost feasibility analysis). While financial analyses are an important part of the business case, Karahanna said that there may be circumstances in which implementing a project may not make sense from a purely financial standpoint, but the intangible or nonfinancial benefits may be sufficiently compelling to move forward anyway. Karahanna presented a linear synopsis of the process for making a business case (see Figure 2-2), but she
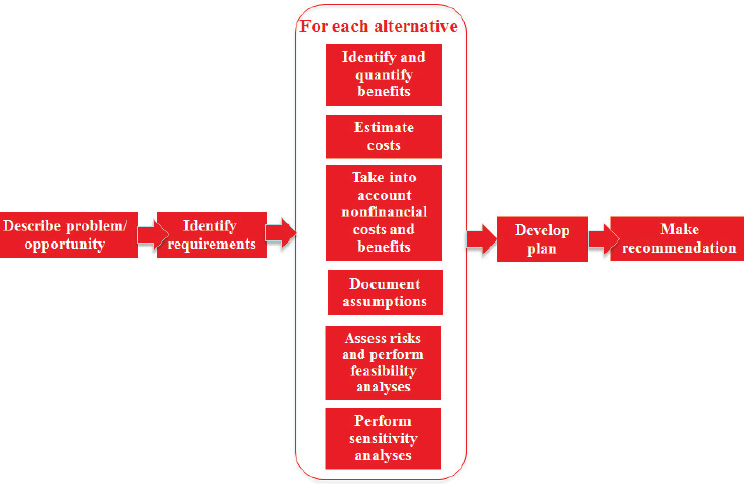
SOURCE: Presented by Elena Karahanna, April 6, 2017.
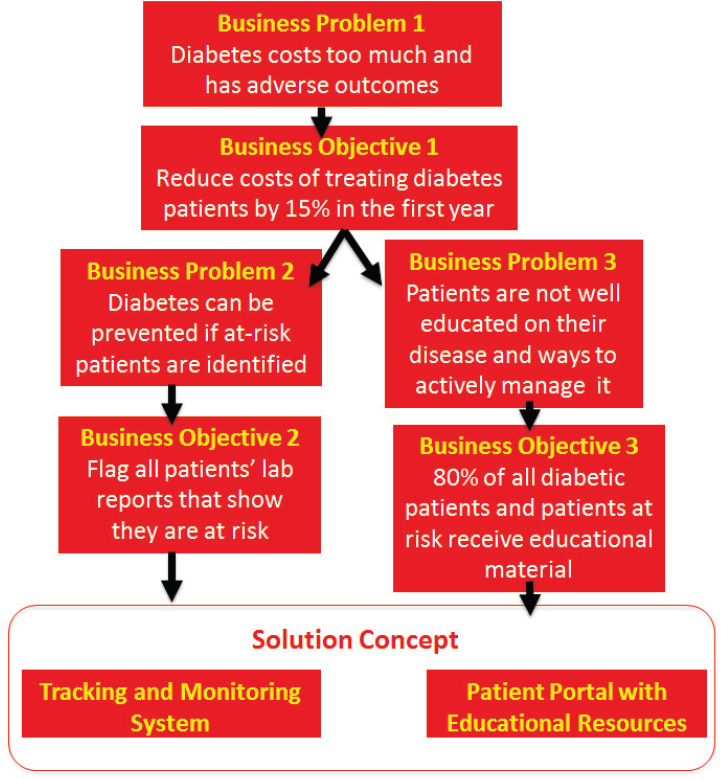
SOURCE: Presented by Elena Karahanna, April 6, 2017.
said that it is actually an iterative process in which each component may be revised as the problem, solution, costs, risks, and benefits are further refined. In particular, the problem description and the business objectives are intertwined, and exploring one can help clarify the other. The business objectives can be made more measurable by asking, “How will we assess whether the problem is solved?” Likewise, the problem description can gain granularity by asking, “What is keeping us from achieving this goal?” (see Figure 2-3). Karahanna noted that a business case usually looks at costs and benefits over a period of 5 years, although a particular business case may
look at a shorter or longer time frame, particularly in the case of a disease intervention in which the disease outcomes take time to manifest.
DISCUSSION
The moderator of the discussion session, Lucy Savitz, assistant vice president for delivery system science in the Institute for Healthcare Delivery Research at Intermountain Healthcare, opened the floor for discussion, and a number of participants responded. Patricia Hinton Walker of the Uniformed Services University of the Health Sciences observed that in the diabetes example that was presented, the true cost and complexity of patient behavior change was underestimated. She noted that behavior change is not a simple consequence of a provider-directed intervention; it requires the active participation and motivation of patients and their caregivers. Savitz agreed with this observation and said that patient behavior change is often influenced by people outside of the clinic setting—from informal caregivers to friends at church—and these influences should be included in a business case whenever possible. Walker guided the discussion back toward CPD, and argued that unidirectional education of health professionals is unlikely to be successful without understanding and engaging the patient and caregiver perspective.
Savitz pointed out that when developing a business case it is important to keep in mind the perspective of the intended audience. For example, a business case made to a health care organization would show a benefit or savings to that particular organization, rather than simply a benefit to society as a whole, because the organization has a fiduciary duty to make financially sound decisions. Karahanna agreed and said that business cases are almost always directed at whoever is funding the project—whether that is a philanthropic organization, a for-profit business, or a nonprofit—and that the business case should reflect the funder’s perspective and motivations.
Malcolm Cox, co-chair of the Global Forum, asked Savitz and Karahanna to comment on the expertise that is necessary to build a business case. Savitz responded that in her experience, it is critical to use a team-based approach when building a business case, and such teams would ideally include clinical experts, researchers, community representatives, and patients and caregivers. She noted that including community partners can lead to unexpected cost savings; for example, in an Intermountain diabetes project, the local farmers’ market provides discounts to patients at no cost to Intermountain. Karahanna suggested adding a member with expertise in business analysis to the team in order to facilitate the process by pulling all the components of the business plan together.
The final comment came from Brenda Zierler of the American Academy of Nursing. She noted that people in the United States can change insur-
ance providers often, making it a challenge to demonstrate a return on investment because the costs and benefits may accrue to different entities. Savitz agreed. This is a challenge, she said, and health care plans need to work together on initiatives that improve health care and health outcomes because they will see benefits accrue to the health care plans collectively, as well as to the population as a whole.
REFERENCES
Beaulieu, N. D., D. M. Cutler, K. E. Ho, D. Horrigan, and G. Ishan. 2003. The business case for diabetes disease management at two managed care organizations: A case study of healthpartners and independent health association. Washington, DC: The Commonweath Fund.
FIP (International Pharmaceutical Federation). 2014. Continuing professional development/ continuing education in pharmacy: Global report. The Hague, The Netherlands: International Pharmaceutical Federation.
IOM (Institute of Medicine). 2003. Health professions education: A bridge to quality. Washington, DC: The National Academies Press.
IOM. 2010. Redesigning continuing education in the health professions. Washington, DC: The National Academies Press.
McMahon, G. T. 2017. The leadership case for investing in continuing professional development. Post author corrections. Invited commentary. Academic Medicine 92(8):1075–1077.
This page intentionally left blank.












