Section III
Public Health Implications of E-Cigarettes
While e-cigarettes might cause youth who use them to transition to use of combustible tobacco products, they could increase adult cessation of combustible tobacco cigarettes if they are used frequently. Across a range of studies and outcomes, e-cigarettes pose less risk to an individual than combustible tobacco cigarettes. With the range of assumptions used, population modeling projects that there would be net public health harm in the short and long term if the products do not increase combustible tobacco cessation in adults. Factors that would maximize potential health benefits associated with these products include determining with more precision whether and under which conditions e-cigarettes could serve as an effective smoking cessation aid, discouraging their use among youth through standard tobacco control strategies such as education and access restrictions, and increasing their safety through data-driven engineering and design.
Understanding the public health implications of e-cigarette use at the population level requires consideration of not only the risks of e-cigarettes on individual health outcomes, as described in the preceding chapters, but also the relation between e-cigarette use and use of other tobacco products—namely, combustible tobacco cigarettes. Given the well-documented and strong influence of combustible tobacco cigarette smoking on health (HHS, 2014) and the emerging evidence that, although not harm free, e-cigarettes likely expose users to lower health risks compared with combustible tobacco cigarettes, any link between e-cigarette use and patterns of combustible tobacco cigarette smoking would have a considerable impact on both individual and population health. Thus, a question
relevant to the committee’s task is whether and to what extent e-cigarette use affects patterns of combustible tobacco cigarette smoking. The challenge of evaluating the effect of e-cigarette use on combustible tobacco cigarette use is that e-cigarettes could influence combustible tobacco cigarette smoking through a number of pathways, which together could lead to net public health benefit or harm. To understand the potential effects of e-cigarette use on combustible tobacco cigarette smoking, the committee developed a conceptual framework illustrating these plausible pathways, or the possible transitions among e-cigarette use, cigarette smoking, and non-use (see Figure III-1). There are many plausible pathways, and smoking and tobacco use trajectories are often complex. To assess the potential effects of e-cigarette use on combustible tobacco cigarette smoking and corresponding health effects, this section of the report focuses on the influence of e-cigarette use on combustible tobacco cigarette use initiation and cessation, as well as the harm from e-cigarettes relative to that from combustible tobacco cigarettes.
Combustible tobacco cigarette initiation reflects transitions from no smoking to established or regular smoking, and therefore involves multiple steps within the tobacco progression trajectory. Consequently, to study markers along the continuum of smoking initiation, the committee first examined transitions from never smoking combustible tobacco cigarettes to any report of ever using combustible tobacco cigarettes, alone or concurrent with e-cigarettes (dual use). Ever use could reflect either a period
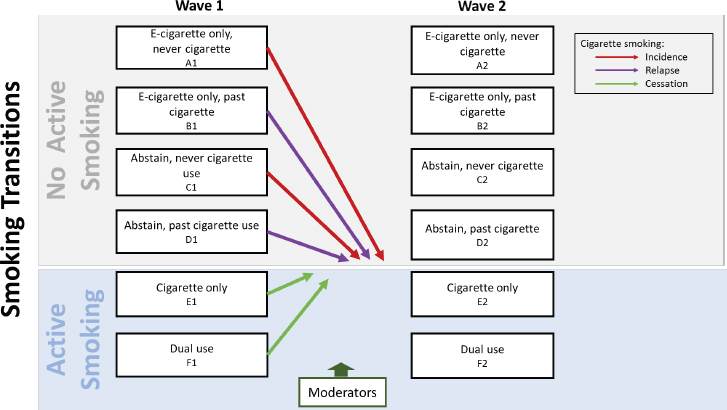
of temporary experimentation that does not progress to regular smoking or the beginning of a trajectory toward becoming a regular smoker. Thus, the committee then examined the progression to becoming a regular smoker as indicated by increases in the frequency (i.e., number of days used in past 30), intensity (i.e., cigarettes smoked per day on smoking day), and duration (i.e., length of time in which smoking behavior continues versus ceases following initiation) of smoking after becoming an ever smoker. In the framework, cigarette initiation is depicted by the red arrows that denote any transition from non-smoking to smoking. Estimates of e-cigarettes as a risk factor for cigarette initiation most commonly involve a ratio of these red lines, such as the level of combustible tobacco cigarette initiation among e-cigarette users as compared with those who do not use e-cigarettes.
Because nearly all adult combustible tobacco cigarette smokers report first use of cigarettes before age 26 (IOM, 2015), smoking initiation pertains primarily to youth and young adults. E-cigarette use among youth and young adults could influence subsequent combustible tobacco cigarette initiation in several ways. One scenario is that youth and young adults begin using e-cigarettes and subsequently initiate use of combustible tobacco cigarettes, either through switching or in addition to e-cigarettes. In this scenario, e-cigarette use is associated with combustible tobacco cigarette smoking initiation and thus tobacco-related health risks. Another scenario suggests that some portion of youth and young adults who otherwise would have begun smoking combustible tobacco cigarettes would not do so, and would instead begin using e-cigarettes. Here, e-cigarette use would reduce or delay initiation of combustible tobacco cigarette use and could reduce tobacco-related health risks. These potential pathways and corresponding evidence are described further in Chapter 16.
E-cigarette use could affect combustible tobacco use among adult smokers through several pathways, with different implications for public health. For example, it is plausible that e-cigarettes promote cessation of combustible tobacco cigarette smoking. The committee defined cigarette cessation as transitions from any combustible tobacco cigarette smoking to non-smoking. By this definition, cessation may involve the outcome of e-cigarette use alone or non-use of both e-cigarettes and combustible tobacco cigarettes. In other words, smokers could either transition completely from combustible tobacco cigarettes to e-cigarette use only or they could start using e-cigarettes in addition to combustible tobacco cigarettes (dual use) for a limited time, and then completely switch to e-cigarette use alone. Smokers could also subsequently quit both combustible tobacco cigarette and e-cigarette use. As the committee previously concluded, e-cigarettes are likely to expose users to fewer and lower levels
of potentially toxic substances compared with exposure from combustible tobacco cigarettes and thus to confer lower health risks. Therefore, complete switching from combustible tobacco cigarettes to e-cigarettes would be expected to reduce tobacco-related health risks. E-cigarette users who subsequently stopped using both e-cigarettes and combustible tobacco cigarettes would incur additional benefits. In the framework, combustible tobacco cigarette cessation is depicted by the green arrows that denote any transition from smoking to non-smoking. Estimates for e-cigarettes as a cessation tool most commonly involve a ratio using at least one of these green lines, such as the level of cigarette cessation among active smokers (E1) compared with smokers who recently quit and use e-cigarettes as a replacement (recent members of B1). In these scenarios, e-cigarettes would benefit public health.
If, on the other hand, e-cigarettes are not effective cessation aids, e-cigarettes could cause relapse, whereby current e-cigarette use by former or non-active combustible tobacco cigarette users leads these users to transition back to combustible tobacco smoking either alone or concurrently with e-cigarettes. This could occur, for example, if a former smoker uses e-cigarettes under the belief that they are safe and will provide many of the same pleasures as combustible tobacco cigarettes, and follow a path that eventually leads back to active cigarette smoking. In the framework, cigarette relapse is depicted by the purple arrows that denote any transition from non-active to active smoking. As with initiation and cessation, estimates of relapse are based primarily on the ratio of the relevant transition probabilities. In this case, cigarette relapse levels among e-cigarette users are compared with relapse levels among former smokers who do not use e-cigarettes. Among e-cigarette users who relapse, the potential reduction in tobacco-related health risks from a period of temporary switching would likely be minimal. The influence of e-cigarettes on relapse would be especially worrying if e-cigarettes cause relapse among those who otherwise would have remained abstinent from combustible tobacco cigarette smoking, as this would increase both individual and overall public health risk. Discussion of the potential influence of e-cigarettes on combustible tobacco cigarette smoking among current and former adult smokers and corresponding evidence can be found in Chapter 17.
Finally, current smokers could start using e-cigarettes in addition to combustible tobacco cigarettes (dual use) and persist in using both products concurrently. If use of both products led to smoking reduction, this could confer health benefits. However, it is also feasible that dual users do not reduce combustible tobacco cigarette use, which could expose them to adverse health effects from the e-cigarettes in addition to those from combustible tobacco use. Discussion and evidence on the influence of
concurrent e-cigarette and combustible tobacco cigarette use (dual use) on smoking cessation as well as health outcomes are presented in Chapter 18.
In addition to the tobacco use trajectories, the committee considered whether certain factors (or moderators) might strengthen or weaken the association between e-cigarette use and combustible tobacco cigarette use. Much remains unknown about potential moderators, but potentially important moderators that warrant serious consideration include age, motivation of e-cigarette users to smoke or stop smoking, substance vaped in e-cigarettes (e.g., nicotine concentration or flavorings), and whether e-cigarette use is part of a structured cessation program. Information on these moderators is currently scarce, but noted below when available.
To understand the overall effect of these different hypothesized pathways among e-cigarette use, combustible tobacco cigarette smoking, and non-use on the U.S. population as a whole, the committee used population-dynamic modeling and presents results of a range of scenarios in Chapter 19.
REFERENCES
HHS (U.S. Department of Health and Human Services). 2014. The health consequences of smoking—50 years of progress: A report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Disease Prevention and Health Promotion, Office on Smoking and Health.
IOM (Institute of Medicine). 2015. Public health implications of raising the minimum age of legal access to tobacco products. Washington, DC: The National Academies Press.
This page intentionally left blank.






