2
The Landscape for the Next Generation of Researchers
The career trajectory of an independent researcher in the biomedical1 or behavioral sciences has undergone striking changes in recent decades, as have the training, research, and funding environments they inhabit. These changes affect the foundation of the biomedical research enterprise, specifically the researchers who discover new knowledge, drive innovation, and promote worldwide health.
In this chapter, the committee describes the promise, opportunities, and challenges of the current landscape for the next generation of researchers as they pursue a path to independence. The discussion is divided into the several phases of that path—commencing with doctoral and medical training; the move for many to postdoctoral experiences; the transition to independent research opportunities in academic and non-academic domains; and the pursuit of funding and other challenges that investigators face as they seek to establish a sustainable and fruitful career.
DOCTORAL AND MEDICAL TRAINING IN BIOMEDICAL RESEARCH
As of fall 2015, more than 140,000 students were enrolled in U.S. graduate school programs in the biomedical and health sciences.2 Of that population,
___________________
1 In this report, “biomedical” refers to the full range of biological, biomedical, behavioral, and health sciences supported by the National Institutes of Health (NIH).
2 National Science Foundation (NSF). Survey of Graduate Students and Postdoctorates in Science and Engineering, Table 9: Graduate students in science, engineering, and health in all institutions, by detailed field: 2010–15. https://ncsesdata.nsf.gov/datatables/gradpostdoc/2015/html/GSS2015_DST_09.html (accessed December 14, 2017). Included in this accounting are the following fields:
64 percent were women, 20 percent held temporary visas, and 19 percent were from racial and ethnic groups traditionally underrepresented in science and engineering.3 In the same year, more than 11,000 biological, biomedical, and health students earned their Ph.D. or equivalent doctorate degree.4 Of those doctorate recipients, 56 percent were women, 24 percent held temporary visas, and 9 percent were from traditionally underrepresented minority groups. In 2016, approximately 19,000 people in the United States received a medical degree, with 46 percent women and 10 percent from underrepresented minority groups.5 Of those who graduated with a medical degree in the United States in 2016, 602 graduated with an M.D.-Ph.D., and, of those, 38 percent were female6 and 5 percent were from underrepresented minority groups.7
The nature of doctoral training in the United States is outside the scope of this report, but is the topic of another National Academies study.8 However, a few observations about doctoral training periods are relevant to the mandate of this committee. First, the median time from matriculation to a Ph.D. in the life sciences was 6.7 years in 2015, declining from 7.7 years in 1990.9 Although the age at which researchers secure their first major NIH grant has increased during the past several decades, this increase is not due to a longer duration of doctoral training. However, the average length of training for M.D.-Ph.D. recipients has increased, from 6.6 years in the 1980s to 8 years in 2012 (National Institutes of Health, 2014), so increases in the average age of research independence for M.D.-Ph.D. recipients could be connected to longer training periods.
___________________
anatomy, biochemistry, biology, biometry and epidemiology, biophysics, cell and molecular biology, entomology and parasitology, genetics, microbiology, immunology, virology, nutrition, pathology, pharmacology and toxicology, physiology, biosciences, neurobiology and neuroscience, and health.
3 NSF defines underrepresented minorities as comprising three racial or ethnic minority groups (blacks, Hispanics, and American Indians or Alaska Natives) whose representation in science and engineering education or employment is smaller than their representation in the U.S. population. NSF. Women, Minorities, and Persons with Disabilities in Science and Engineering 2017. https://www.nsf.gov/statistics/2017/nsf17310/digest/glossary-and-key-to-acronyms/ (accessed February 7, 2018).
4 NSF. Survey of Earned Doctorates 2015, Table 12: Doctorate recipients, by subfield of study: 2005-2015. https://www.nsf.gov/statistics/2017/nsf17306/datatables/tab-12.htm (accessed December 14, 2017).
5 American Association of Medical Colleges (AAMC). Table B-4: Total U.S. medical school graduates by race/ethnicity and sex, 2012-2013 through 2016-2017. https://www.aamc.org/download/321536/data/factstableb4.pdf (accessed January 24, 2018).
6 Data provided courtesy of AAMC and available from public access file.
7 AAMC. Table B-13: Race/ethnicity responses (alone and in combination) of MD-PhD graduates of U.S. medical schools, 2012-2013 through 2016-2017. https://www.aamc.org/download/450638/data/factstableb13.pdf (accessed January 24, 2018).
8 National Academies of Sciences, Engineering, and Medicine. Graduate Education for the 21st Century. http://www.nas.edu/GradEd (accessed February 7, 2018).
9 NSF. Survey of Earned Doctorates 2015, Table 31: Median years to doctorate, by broad field of study: Selected years, 1990–2015. https://www.nsf.gov/statistics/2017/nsf17306/datatables/tab-31.htm (accessed December 14, 2017).
Second, the number of individuals obtaining Ph.D.’s in the biomedical sciences has steadily increased, and the majority of them will continue their training after receiving their degrees. A recent analysis showed that the annual number of individuals receiving a biomedical Ph.D. more than doubled during the period 1980 to 2010, while the percentage of individuals starting their careers in a postdoctoral position largely remained steady at about 82.5 percent (Kahn and Ginther, 2017). The increase in the number of Ph.D.’s, combined with the continued trend of biomedical doctorate recipients pursuing a postdoctoral experience after graduation, has contributed to a dramatic rise in the number of individuals in the United States in postdoctoral research positions.
THE POSTDOCTORAL RESEARCH EXPERIENCE
The postdoctoral experience is a temporary period of training following the award of a doctoral or medical degree to gain additional scientific, technical, and professional skills that advance the careers of Ph.D.’s, M.D.’s, and M.D.-Ph.D.’s. As discussed in the 2014 National Academies of Sciences report, The Postdoctoral Experience Revisited, the National Science Foundation (NSF), National Institutes of Health (NIH), Association of American Medical Colleges (AAMC), and the National Postdoctoral Association (NPA) all formalized definitions of postdoctoral researchers in the mid-2000s (National Academy of Sciences et al., 2014a). Their definitions and characterizations (updated for 2018) are provided in Box 2-1.
While receiving valuable research training, postdoctoral researchers play an indispensable role in the research enterprise, “performing a substantial portion of the nation’s research in every setting” (Institute of Medicine et al., 2000, p. 10). Understanding their experiences and outcomes is challenging, however, because of well-documented problems with the available data (National Institutes of Health, 2012a, p. 9; National Academy of Sciences et al., 2014a). These challenges include inconsistent titles and definitions for postdoctoral researchers, as well as inconsistent data on their employment experiences, pay, benefits, and duration of their appointment across institutions. As a result, estimates of the total number of biomedical postdoctoral researchers in the United States range widely from 30,000 to 80,000. Some data sets, such as the NSF Survey of Graduate Students and Postdoctorates in Science and Engineering (GSS), count only postdoctoral researchers employed at U.S. degree-granting institutions and not those employed by industry or research institutions. There have been repeated calls to collect and disseminate demographic and outcomes data on postdoctoral populations to guide both individual and policy decisions, but no national efforts have been sustained. More recently, NSF has developed and piloted the Early Career Doctorates Survey to gather in-depth information about individuals who earned an initial doctoral degree within the past 10 years, including non-citizens as well as U.S. citizens and permanent residents.
Despite these data limitations, one can tease out some broad trends about the postdoctoral population at U.S. degree-granting institutions. The NSF GSS reported that nearly 39,000 individuals were working in postdoctoral positions in the biomedical and health sciences in 2015,10 and the gender, race, and ethnicity
___________________
10 NSF. Survey of Graduate Students and Postdoctorates in Science and Engineering, Table 43: Female postdoctoral appointees in science, engineering, and health in all institutions, by detailed field, citizenship, ethnicity, and race: 2015. https://ncsesdata.nsf.gov/datatables/gradpostdoc/2015/html/GSS2015_DST_43.html (accessed January 23, 2018). Included in this accounting are the following fields: anatomy, biochemistry, biology, biometry and epidemiology, biophysics, cell and molecular
of those postdoctoral researchers did not reflect the demographics of newly minted biomedical doctorates from that same year. While 56 percent of doctorate recipients in 2015 were women, only 46 percent of postdoctoral researchers in the same fields were women. In addition, 9 percent of the biomedical Ph.D.’s were awarded to individuals from underrepresented minority groups in 2015, but only 5 percent of postdoctoral researchers in those fields were from those same groups.
A substantial proportion of biomedical postdoctoral researchers are not U.S. citizens or permanent residents. Of the biomedical postdoctoral researchers included in the 2015 NSF GSS, 53 percent held temporary visas and 31 percent reported earning their degrees in a foreign country. Moreover, the origin of the degree was unknown for 33 percent of biomedical postdoctoral researchers surveyed the same year.11 These percentages reflect both the openness of U.S. biomedical training and labor markets and the attractiveness of U.S. research careers to international scholars. It is also the case that some countries encourage recent Ph.D.’s to seek postdoctoral training in the United States.12
In the extramurally funded biomedical sciences, postdoctoral researchers at U.S. degree-granting institutions are supported largely by NIH funding mechanisms. In 2016, approximately 10 percent of postdoctoral researchers in the biomedical, behavioral, social, and clinical sciences were supported on federal fellowships and traineeships, such as the Ruth L. Kirschstein Individual National Research Service Award (NRSA) postdoctoral fellowship (F32), which provides support to individual postdoctoral fellows, and the Ruth L. Kirschstein Institutional NRSA training grant (T32), which provides support to institutions to develop training opportunities for selected individuals.13 That same year, 46 percent of postdoctoral researchers were supported on a federal research grant, which is awarded to a principal investigator (PI) and supports individuals selected by the PI, and 44 percent received non-federal support. Of postdoctoral researchers specifically supported by NIH in 2016, approximately 79 percent of them were supported on research project grants (RPGs) and 19 percent were supported on a fellowship or traineeship.14
___________________
biology, entomology and parasitology, genetics, microbiology, immunology, virology, nutrition, pathology, pharmacology and toxicology, physiology, biosciences, neurobiology and neuroscience, and health.
11 NSF. Survey of Graduate Students and Postdoctorates in Science and Engineering 2015, Table 48: Postdoctoral appointees in science, engineering, and health in all institutions, by detailed field and origin of doctoral degree: 2015. https://ncsesdata.nsf.gov/gradpostdoc/2015/html/GSS2015_DST_48.html (accessed February 7, 2018).
12 See the international commissioned papers for this study, available at http://www.nas.edu/NextGen/resources.
13 NIH Data Book. Primary Source of Support for Postdoctorates. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=263andcatId=20 (accessed December 14, 2017).
14 NSF. Survey of Graduate Students and Postdoctorates in Science and Engineering 2016, Table 41: Postdoctoral appointees in science, engineering, and health in all institutions, by field, primary source of support, and primary mechanism of support: 2016. https://ncsesdata.nsf.gov/gradpostdoc/2016/html/GSS2016_DST_41.html (accessed March 6, 2018).
NIH training grants, such as individual F32 and institutional T32 awards, are restricted to U.S. citizens and permanent residents, undergo peer review of the research and training plan, and include stipulations for professional development and mentoring by eligible mentors. For postdoctoral researchers, obtaining a fellowship is often considered a step toward professional independence, but significantly fewer postdoctoral researchers are supported on fellowships and training grants than on RPGs. In fact, the number of postdoctoral researchers supported on F32 grants was lower in 2016 (516 awards) than any year since 1998.15 For postdoctoral researchers supported on an RPG, NIH states, “Staff in postdoctoral positions engaged in research, while not generally pursuing an additional degree, are expected to be actively engaged in their training and career development under their research appointments as Post-Docs.”16 However, there is neither a requirement to include a plan for training and professional development in the grant application, an assessment of the PI as a mentor, nor any other formal mechanism to ensure quality training and mentorship opportunities. In 2014 NIH implemented a policy that RPG Research Performance Progress Reports (RPPRs) must include a brief description of how and whether Individual Development Plans (IDPs) are used to manage the career development of students and postdoctoral researchers associated with that award.17 These deficiencies contribute to a longstanding concern about a disparity in the treatment of postdoctoral researchers between RPGs and training grants (National Research Council, 2005). Moreover, because only U.S. citizens or nationals or lawful permanent residents are eligible for NIH-funded fellowships or training grants, postdoctoral researchers from other countries are significantly less likely to receive mandated training and professional development.
The fastest growing and second most prevalent source of postdoctoral support at degree-granting institutions is non-federal organizations, such as philanthropies, research centers, universities, the private sector, and professional societies.18 The Health Research Alliance, a national consortium of more than 70 nongovernmental, nonprofit funders of biomedical research and training, provided $866 million in research awards in 2012.19 Of that amount, 44 percent was for early-career development and training, including programs such as the American Cancer Society’s Postdoctoral Fellowship Award and the Damon Runyon Cancer Research Foundation’s Postdoctoral Research Fellowship. These organizations try to identify gaps in
___________________
15 NIH Data Book. Kirschstein-NRSA post-doctoral fellowships (F32): Competing applications, awards, and success rates. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=106andcatId=13 (accessed February 9, 2018).
16 NIH. OMB Clarifies Guidance on the Dual Role of Student and Postdoctoral Researchers. https://grants.nih.gov/grants/guide/notice-files/NOT-OD-15-008.html (accessed February 7, 2018).
17 See https://grants.nih.gov/grants/guide/notice-files/not-od-14-113.html (accessed March 16, 2018).
18 NIH Data Book. Primary Source of Support for Postdoctorates. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=263andcatId=20 (accessed December 14, 2017).
19 See https://issuu.com/kfowlerdesign/docs/hra_report_grantsanalysis_highres (accessed January 19, 2018).
funding where they can provide “risk capital” for innovative but risky initiatives, an agenda that includes supporting unproven but promising postdoctoral researchers and other early-career researchers who, “because of their career stage and lack of track record, are unlikely to procure significant federal funding for their ideas until they are at a much later career stage.”20
In addition to those postdoctoral researchers described above who work in degree-granting institutions, there are many employed in industry, national laboratories, and non-academic research institutions. The size of the postdoctoral workforce in those sectors is not clear, but the roles and experiences of these postdoctoral researchers and their peers in academia are notably different. According to the National Academies report The Postdoctoral Experience Revisited (National Academy of Sciences et al., 2014a, p.3), their “roles are better defined, salaries are higher, terms are shorter, and the connection to career development is clearer.”
It is difficult to determine with accuracy the length of time researchers spend in their postdoctoral positions and whether that duration has changed over time. One recent analysis, however, found that the duration has held relatively constant over the past several decades at 4.5 years (Kahn and Ginther, 2017). There appeared to be a slight decrease in the duration after the late 1990s, perhaps attributable to a gradual move by some universities to cap postdoctoral periods at their institutions. Even so, approximately 20 percent of postdoctoral fellows in 2005 had spent 7 or more years in postdoctoral research positions (Kahn and Ginther, 2017). It is unclear whether these postdoctoral researchers had prolonged postdoctoral experiences because (1) they came from institutions with shorter doctoral training periods, (2) they required additional training because of their specific research areas, (3) they were in a “holding pattern” because of the scarce availability of independent academic research positions, or (4) other unknown reasons. Importantly, the data from this analysis are only included up to 2006, so it is unclear whether these trends persisted over the following decade. Despite calls in prior reports for improved data collection on postdoctoral researchers, it remains challenging to find comprehensive quantitative and qualitative data about the postdoctoral research experience.
Several surveys in recent years have revealed qualitative aspects of the postdoctoral experience. Respondents in a national survey of 1,002 American biological and life science postdoctoral researchers reported lower clarity on career goals during the postdoctoral experience than upon entry into or departure from Ph.D. programs (Gibbs et al., 2015). In a separate study, only 4 percent of biological and life sciences postdoctoral researchers reported feeling a “severe lack of information” regarding research careers in academia, but that number increased to 21 percent in government, 34 percent in established companies, and 42 percent in start-ups (Sauermann and Roach, 2016). Finally, those doctorates
___________________
20 See https://www.healthra.org/download-resource/?resource-url=/wp-content/uploads/2013/08/Robertson_ebook.pdf (accessed March 16, 2018).
who had not thought about their careers at all were more likely to pursue a postdoctoral experience than those who had (Sauermann and Roach, 2016). These results are broadly consistent with prior reports that highlight a persistent lack of communication about the broad range of career prospects and educational and training opportunities for doctoral and postdoctoral researchers (National Academy of Sciences et al., 2014a).
NIH has developed initiatives to address the need for postdoctoral career development. For postdoctoral researchers supported on NRSA awards, NIH requires institutions to offer preparation for research-related and research-intensive careers in various sectors, such as academic institutions, government agencies, for-profit businesses, and private foundations.21 In 2013, NIH launched the Strengthening the Biomedical Research Workforce program through the NIH Common Fund as one component of a trans-NIH strategy to enhance training opportunities for early-career scientists to prepare them for a variety of research-related career options.22 A core component of this program is the NIH Director’s Biomedical Research Workforce Innovation Awards to enhance biomedical research training, more commonly called the Broadening Experiences in Scientific Training (BEST) awards.23 These 5-year awards are intended to support innovation in both graduate student and postdoctoral researcher training. Although a broad evaluation of BEST is not yet available, the awarded institutions convene annually to share data, develop best practices, and discuss program sustainability.
It is promising that multiple initiatives are aimed at providing postdoctoral researchers with career development opportunities, but an economic analysis of career paths for biomedical doctorates reveals that the postdoctoral experience can come at a substantial opportunity cost. Recent data indicate that postdoctoral training may not provide a positive financial return for more than a decade if the postdoctoral researcher later pursues jobs outside of academia. Biomedical Ph.D.’s in postdoctoral research positions earn an average of $45,000 per year for several years. In comparison, biomedical Ph.D.’s who enter the workforce immediately after degree attainment earn a median starting salary of $73,662. It can take 12 to 15 years after degree attainment for the postdoctoral research cohort to make up the lost earnings. The salary advantage in private industry for foregoing a postdoctoral position is especially pronounced for Ph.D.’s conducting biomedical research (Kahn and Ginther, 2017). Despite repeated recommendations to increase postdoctoral stipends and salaries (American Academy of Arts and Sciences, 2014; FASEB, 2015; McDowell et al., 2014; National Academy of Sciences et al., 2014a; National Institutes of Health, 2012a; National Research Council, 2011), the 2017 starting postdoctoral stipend of $47,484 for NRSA
___________________
21 See https://grants.nih.gov/grants/guide/pa-files/PA-18-403.html (accessed December 14, 2017).
22 See https://commonfund.nih.gov/workforce (accessed December 14, 2017).
23 See https://grants.nih.gov/grants/guide/rfa-files/RFA-RM-12-022.html (accessed December 14, 2017).
grants remains below the National Academies 2014 recommended salary of $50,000 in 2014 dollars, or approximately $52,700 in 2018 dollars.24
Postdoctoral researchers in the United States face persistent and troubling challenges. First, they face fierce competition for a limited number of academic faculty positions. Second, they are a vulnerable part of the biomedical workforce because these positions are short-term and thus susceptible to fluctuations in federal research budgets. Third, although they seek these positions to enhance their skills, they are principally supported on RPGs in individual laboratories across the institution, which does not ensure quality mentoring and training experiences. At the core of concerns about the postdoctoral research experience is whether it provides value to postdoctoral researchers and prepares them for a variety of research careers outside of academia, and whether it proportionately and adequately supports diverse populations. Without comprehensive and longitudinal data on the postdoctoral population, however, it is difficult to develop evidence-based recommendations for improving the quality of the postdoctoral experience and recruiting an appropriate number of promising scientists from diverse populations into the biomedical research enterprise.
TRANSITION TO INDEPENDENT RESEARCH POSITIONS
In general, postdoctoral experience is considered necessary preparation for research positions in academia, but it does not guarantee advancement to such a position. According to one survey, 60 percent of postdoctoral researchers in biological and life sciences who graduated before 2013 reported that they accepted their position primarily to secure a faculty tenure-track position (Sauermann and Roach, 2016). However, another recent analysis showed that only 27.4 percent of employed individuals, regardless of their cohort, previously employed in biomedical postdoctoral research had tenure-track or tenured positions (Kahn and Ginther, 2017). The same mismatch between career aspiration and reality plays out more notably for recently trained cohorts, as studies show that greater than 50 percent of Ph.D.’s in the biological and life sciences rank a faculty research position as their desired career (Sauermann and Roach, 2012). As of 2013, however, only 18 percent of all U.S.-trained Ph.D.’s were employed in tenure-track or tenured positions 6 to 10 years after completing their Ph.D. training (Figure 2-1).
The percentage of Ph.D.’s in tenure-track positions has declined significantly in recent years. Partially contributing to this decline is increased hiring of new faculty in nontenure-eligible appointments.25 According to Figure 2-1, in 1993, slightly greater than 10 percent of individuals were in tenure-track or tenured faculty positions within 5 years of degree attainment, but that percentage dropped to 6 percent by 2013. Only 18 percent of biomedical Ph.D.’s 6 to 10 years post
___________________
24 See https://grants.nih.gov/grants/guide/notice-files/NOT-OD-16-131.html (accessed January 19, 2018).
25 See https://www.aamc.org/download/434462/data/june2015aib.pdf (accessed December 14, 2017).
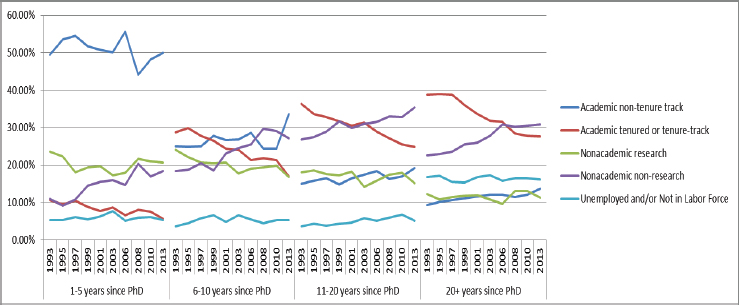
SOURCE: Prepared by Donna Ginther, University of Kansas (previously unpublished). The use of NSF data does not imply NSF endorsement of the research, research methods, or conclusions contained in this report.
degree attainment held academic tenure-track or tenured positions in 2013, compared to 29 percent in 1993.26 An analysis from the AAMC supports a similar trend at medical colleges, where 73 percent of full-time basic science Ph.D. faculty were on tenure-eligible tracks in 2014, compared to 82 percent in 1984.27
As the percentage of biomedical Ph.D.’s in tenure-track or tenured faculty positions has declined, their representation has notably increased in two other sectors: academic non-tenure track positions and non-academic non-research positions. The former includes postdoctoral researchers, as well as instructors, adjunct professors, non-tenured research professors, and staff scientists. Data about the latter are limited, but sources such as the Survey of Doctorate Recipients (SDR) suggest that the category likely encompasses a wide variety of positions across many employment sectors.
The declining probability of transitioning into an academic research position reflects the relatively flat job market in academia coupled with a growing supply of individuals trained in the biomedical sciences. Several factors contribute to the flat job market for early-career investigators. First, although the “number of bio-medical academic tenured/TT jobs did grow (by 150 percent, ~8,700 jobs) from 1981–2013,” this increase could not keep pace with the “278 percent (102,000 people) increase in new U.S. Ph.D.s” (Kahn and Ginther, 2017, p. 92). Second, the abolition of mandatory retirement has allowed faculty to stay in their jobs longer, contingent on meeting performance expectations. A 2011 study of
___________________
26 NSF. Survey of Doctorate Recipients. Employment trends from 1993 to 2013, calculated courtesy of Donna Ginther.
27 See https://www.aamc.org/download/434462/data/june2015aib.pdf (accessed December 14, 2017).
full-time faculty members over age 60 found that 75 percent reported that they expected to work past “customary” retirement age, a shift that is reflected in the rising number of older investigators supported by NIH (National Academy of Sciences et al., 2014b). Between 1998 and 2014, the proportion of NIH-supported investigators over age 65 increased from 5 to 12 percent, while the percentage of investigators under age 50 declined from 54 to 39 percent (Figure 2-2).
A related factor contributing to the flat nature of the academic labor market is the considerable costs associated with recruiting a new faculty member, including startup packages that can exceed $1 million (Dorsey et al., 2009; Joiner, 2005). At the same time, the profit margins from clinical activity in academic health centers, which have traditionally been used to partially subsidize the research enterprise, are under increasing pressure. Further, public institutions have faced declining financial support from their state and local governments.
Physician-Scientists
One group of crucial contributors to biomedical research are physician-scientists—scientists with professional degrees28 and training in clinical medicine who engage in biomedical research. As defined in the 2014 NIH Physician-Scientist Workforce Working Group Report (National Institutes of Health, 2014), physician-scientists typically engage in both clinical care and basic or clinical research, although not always at the same point in their career. The combination of training and experience allows the physician-scientist to contribute a unique perspective and affords them the opportunity to translate clinical observations to the laboratory to help identify the mechanisms of disease, as well as to apply the findings of basic science to patient care.
Physician-scientists also face challenges early in their research careers, including a lack of protected research time, loan repayment obligations, prolonged training, and a need for additional mentoring (National Institutes of Health, 2014). The 2014 NIH Physician-Scientist Workforce advisory committee estimated that about 1,000 physicians need to enter the research workforce each year to maintain the current physician-scientist workforce, but a significant number of physician-scientists move out of research when they are unable to renew their first NIH award (Dickler et al., 2007). NIH offers a variety of support mechanisms that are available to physician-scientists, such as the Loan Repayment Award (LRP), the Mentored Clinical Scientist Research Career Development Award (K08), the Career Transition Award (K22), the Pathway to Independence Award (K99/R00), and the Mentored Patient-Oriented Research Career Development Award (K23). However, certain pressures, including the increasing costs of obtaining a medical degree, the prolonged training period to develop clinical and research competen-
___________________
28 As defined in the NIH Physician Scientist Workforce Report, these professional degrees include individuals with M.D., D.O., D.D.S./D.M.D., D.V.M./V.M.D., or nurses with research doctoral degrees.
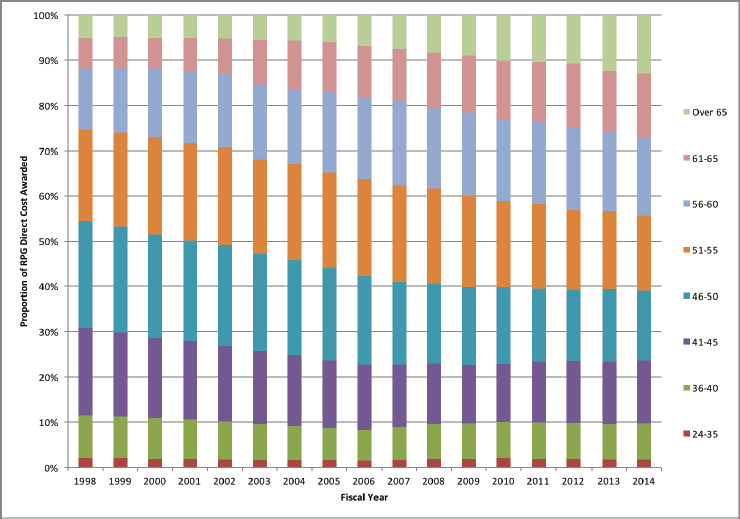
SOURCE: Data and visualization from https://nexus.od.nih.gov/all/2015/03/25/age-of-investigator/ (accessed January 19, 2018).
cies, hospital funding pressures, and increasing clinical responsibilities, make it difficult for physician-scientists to pursue research.
Staff Scientists
A biomedical research career path that is drawing interest from across the biomedical research enterprise is that of staff, or “professional,” scientists. Staff scientists29 with Ph.D.’s provide essential functions as part of institutional core facilities or semi-permanent laboratory staff. They possess a full suite of research and analytical skills and often remain with research projects longer than graduate students and postdoctoral researchers. In some institutions, staff scientists can apply for their own federal research funding. A robust staff scientist path can offer investigators the promise of a sustainable academic research career outside of the traditional research faculty route, potentially easing the logjam of trainees waiting for such opportunities in postdoctoral positions. Written input from several professional societies, testimony to the committee, and statements from prominent
___________________
29 See https://www.ncbi.nlm.nih.gov/pubmed/26625903 (accessed March 6, 2018).
scientists reveal a strong interest in providing support for more staff scientist positions. At the same time, additional research is needed to fully understand the potential impact of this population of researchers on the biomedical research ecosystem if the number of these positions were to grow.
Non-academic Research Positions
In 2013, slightly greater than 60 percent of biomedical Ph.D.’s in the United States worked outside of academia,30 compared to slightly greater than 40 percent in 1993.31 The pharmaceutical industry trains postdoctoral researchers in biological and behavioral sciences, who often transition into successful positions in the biopharmaceutical industry as group leaders, section heads, and distinguished scientist positions after their fellowships. To foster innovation, biopharmaceutical companies often collaborate with the government and the next generation of entrepreneurially minded basic and clinical science researchers through enterprises such as Small Business Innovation Research and Small Business Technology Transfer grants and the National Center for Advancing Translational Sciences.
The private sector also supports biomedical researchers through innovation health care accelerators and incubators such as StartUp Health and OneStart. Currently, several hundred state, national, and global networks of investors, partners, and customers who typically form peer networks provide financial support (i.e., direct funding and investment resources), education, mentoring, and coaching to promote the cutting edge of biomedical science.
One analysis of focus group responses suggests that personal values, combined with frustrations about long training periods, low postdoctoral researcher salaries, tight grant funding, and a highly competitive job market, have diminished biomedical scientists’ interest in faculty research careers and has guided them toward non-academic careers (Gibbs and Griffin, 2013). However, as Figure 2-1 shows, the percentage of biomedical doctorates who are 1 to 5 years post degree attainment and are conducting research in non-academic positions has remained relatively steady between 1993 and 2013 (Figure 2-1). In contrast, the percentage of such doctorates in non-academic non-research positions has increased. More data are needed in this area to better understand the availability of and interest in non-academic research and non-research pathways.
___________________
30 “Biomedical” here includes biological and health sciences, but because of the nature of the SDR this figure likely includes subfields previously excluded in other calculations in this chapter. NSF. Survey of Doctoral Recipients 2013, Table 42: Employed doctoral scientists and engineers, by occupation and sector of employment: 2013. https://ncsesdata.nsf.gov/doctoratework/2013/html/SDR2013_DST42.html (accessed February 2, 2018).
31 NSF. Survey of Doctoral Recipients 1993, Table 20: Doctoral scientists and engineers, by field of doctorate and sector of employment: 1993. https://wayback.archive-it.org/5902/20160210235206/http://www.nsf.gov/statistics/s0893/dstable.htm (accessed February 2, 2018).
FUNDING FOR AN INDEPENDENT RESEARCH CAREER
For those postdoctoral researchers who hope to transition into academic research positions, access to research funding is crucial. That funding, however, is increasingly competitive. According to data provided by NIH, until the late 1990s, a newly hired assistant professor’s first grant was most likely an NIH Type 1 (new) research project grant (R01) or equivalent award. The R01 is the flagship NIH RPG and remains an important benchmark for success on the path to independent research. Between 1998 and 2003, the NIH budget nearly doubled from roughly $13 billion to $27 billion ($21 billion in 1995 constant dollars) (Figure 2-3), and the success rate for type 1 competing R01-equivalent awards peaked at approximately 26 percent in 2000. However, the percentage of research awards to new investigators dropped steadily during those years, and, according to the 2005 National Academies Bridges to Independence report, it appears that “those with existing funding and established research programs received increased funding, in part to hire additional postdoctoral and graduate student researchers and further exacerbate the imbalance between trained researchers and available positions” (National Research Council, 2005, p. 40).
Since the doubling ended in 2004, NIH appropriations have declined in constant dollars, and the success rate for R01-equivalent awards has decreased rapidly for both established and new investigators32 (Figure 2-3). The NIH budget received a supplemental bump in the American Recovery and Reinvestment Act (ARRA)33 in 2009 and 2010, while sequestration in 2013 required a 5 percent ($1.55 billion) cut in the budget.34
The consequences of these significant funding changes can be compounded by the fact that NIH commits its funding to PIs in multi-year tranches—the average R01 grant is 3 to 5 years in duration, although funds are disbursed annually. At any given moment, close to 80 percent of NIH appropriations are committed to ongoing projects (Berg, 2016), with only the remainder available for new projects. Therefore, the size of the pool for new and competing projects in any given year is sensitive to year-to-year changes in the appropriation level. Between 1998 and 2006, the success rate for R01-equivalent awards for new investigators declined from 23 to 15 percent35 (Figure 2-4).
One reason for the decline in success rates since 2004 is the change over time in the NIH budget. Another is the increase in the number of investigators seeking NIH funding each year. The number of applications for all NIH awards rose
___________________
32 NIH defined “new investigators” as a program director/principal investigator (PD/PI) who has not previously competed successfully as a PD/PI for a substantial independent research award. https://grants.nih.gov/policy/early-investigators/index.htm (accessed January 19, 2018).
33 See https://www.treasury.gov/initiatives/recovery/Pages/recovery-act.aspx.
34 See https://www.nih.gov/news-events/news-releases/fact-sheet-impact-sequestration-national-institutes-health (accessed January 19, 2018).
35 See https://report.nih.gov/NIHDatabook/Charts/Default.aspx?sid=1&index=0&catId=13&chartId=136 (accessed March 29, 2018).
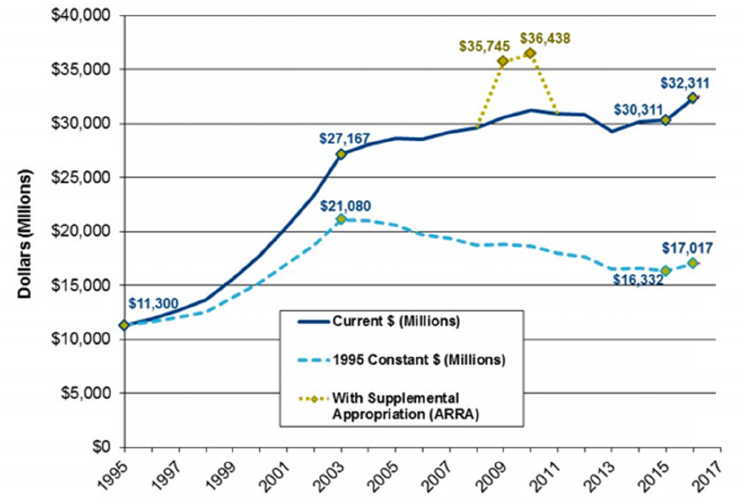
SOURCE: Adapted from http://www.faseb.org/Portals/2/PDFs/opa/2017/NIH%20Grants%20Slideshow.pptx.
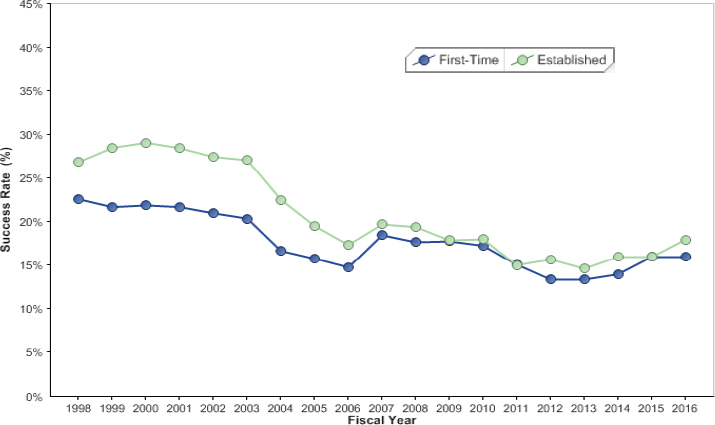
SOURCE: https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=Y&chartId=136&catId=13 (accessed January 19, 2018).
steadily from 19,663 in 1998 to 41,420 in 2016 (Figure 2-5), while the number of applications for the Type 1 R01 awards increased by 97 percent for established investigators and 42 percent for new investigators.36,37 In 2016, of more than 40,000 PIs that submitted competing RPG applications, only 11,434 (or 28%) received funding. Also that year, nearly 30,000 eligible biomedical investigators were unable to secure NIH funding to support their research (Figure 2-5), leading many to characterize the current biomedical ecosystem as “hypercompetitive,” a situation with a stark imbalance between the dollars available for research and the expanding U.S. scientific community (Alberts et al., 2014; Fochler et al., 2016; Kamerlin, 2015; Kimble et al., 2015).
Faced with an increasing number of applicants for research awards—and concern about the ability of new investigators to compete for funding in that environment—NIH sought to boost support for new investigators by instituting a policy in fiscal year (FY)2007 to maintain comparable success rates for type 1 R01-equivalent applications from both experienced and new investigators.38 NIH also established a policy that the majority of awarded new investigators should be early-stage investigators (ESIs),39 defined as a “Program Director/Principal Investigator (PD/PI) who has completed their terminal research degree or end of post-graduate clinical training, whichever date is later, within the past 10 years and who has not previously competed successfully as PD/PI for a substantial NIH independent research award.”40 This new policy benefits both new investigators and ESIs by requiring peer reviewers to focus more on the proposed approach in grant applications than on an investigator’s track record, and to expect less preliminary data than would be provided by established investigators.41 NIH Institutes routinely fund ESI applications that score outside of the normal funding range by maintaining a separate payline for competing, investigator-initiated ESI R01 applications.42 For example, in FY2017, the payline for ESI applications to
___________________
36 NIH Data Book. Research and Training Grants: Competing Applications by Mechanism and Selected Activity Codes. https://report.nih.gov/nihdatabook/ (accessed February 2, 2018).
37 See https://www.nih.gov/news-events/nih-research-grants-digital-press-kit (accessed January 19, 2018).
38 See https://archives.nih.gov/asites/grants/08-22-2017/grants/guide/notice-files/NOT-OD-09-013.html (accessed December 15, 2017); https://archives.nih.gov/asites/grants/08-22-2017/grants/guide/notice-files/NOT-OD-07-030.html (accessed March 16, 2018).
39 See https://grants.nih.gov/grants/guide/notice-files/NOT-OD-09-013.html (accessed February 8, 2018).
40 See https://grants.nih.gov/policy/early-investigators/index.htm (accessed January 19, 2018).
41 With the development of the Next Generation Researcher Initiative in 2017, NIH no longer uses the term new investigator and instead uses the term early-stage investigator (ESI).
42 Since 2007, NIH Institutes and Centers (ICs) have maintained policies to guide enhanced funding for new investigators or ESIs. A recent Next Generation Researcher Initiative (NGRI) at NIH emphasized ESIs. However, grants from both new investigators and ESIs are still identified in eRAcommons (the online interface for NIH grants) and reviewed separately from grants from established investigators. An NIH NGRI advisory committee to the director and NIH ICs are currently discussing final recommendations on policies to enhance independence and research funding for early-stage and new researchers.
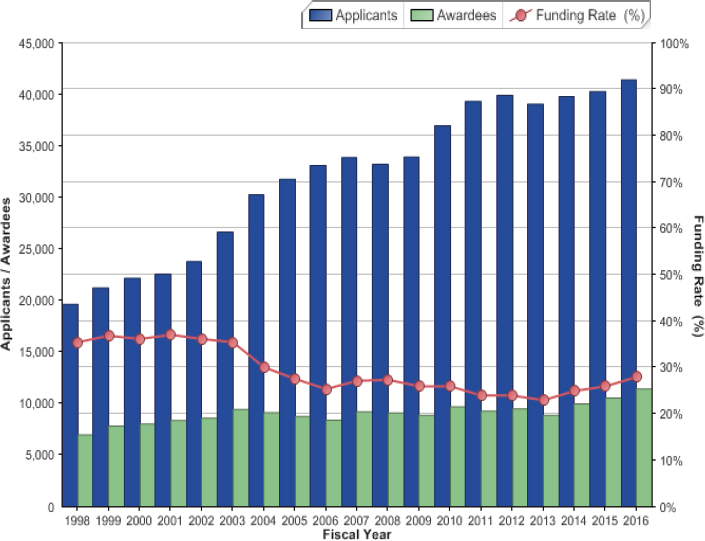
SOURCE: Data from NIH Data Book. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=Y&chartId=164&catId=13 (accessed January 19, 2018).
the National Heart, Lung, and Blood Institute (NHLBI) was set at 10 percentile points above the regular R01 payline.43
This new investigator policy went into effect in FY2007, and the number of new investigator R01 awardees increased slightly between 2008 and 2010 (Figure 2-6)44 (these data exclude awards made from the ARRA in 2009 and 2010). However, in 2013, the number of new investigator awardees dipped to 2005 levels, which coincided with budget sequestration. NIH estimated that sequestration resulted in approximately 640 fewer RPG awardees compared to FY2012, but it is unclear how new investigators and ESIs were affected.45 Since sequestration,
___________________
43 See https://www.nhlbi.nih.gov/research/funding/general/current-operating-guidelines (accessed December 15, 2017).
44 See https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=168andcatId=22 (accessed December 15, 2017).
45 NIH. Fact Sheet: Impact of Sequestration on the National Institutes of Health. https://www.nih.gov/news-events/news-releases/fact-sheet-impact-sequestration-national-institutes-health (accessed December 15, 2017).
the number of new investigators awarded R01-equivalents has increased, but not as rapidly as for established investigators.
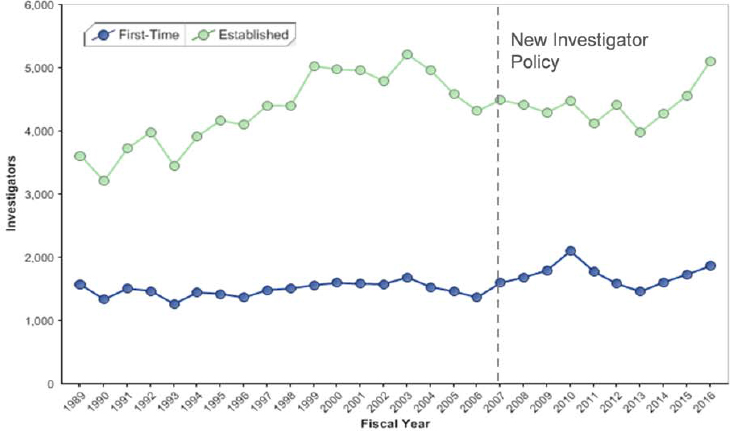
SOURCE: Data and visualization from NIH Data Book. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=Y&chartId=168&catId=22 (accessed February 8, 2018).
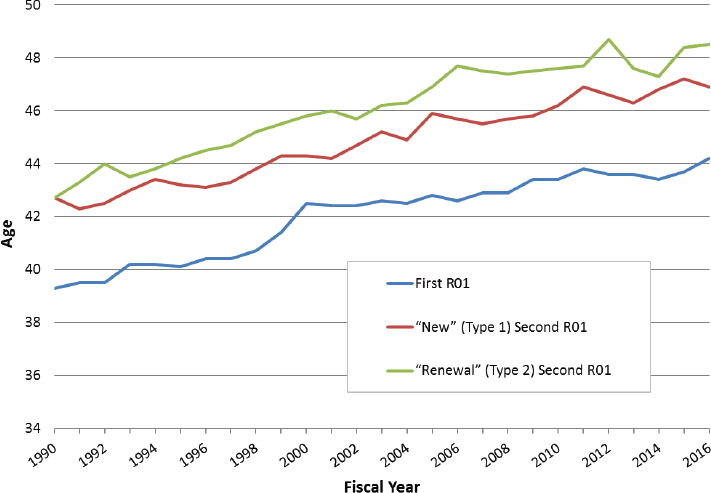
Although NIH’s new investigator policy leveled success rates between new and established investigators and temporarily boosted the number of new investigators receiving R01-equivalent awards, the average age of first receipt of an R01-equivalent award rose from 39.3 in 1990 to 44.2 in 2016.46 This increase applies across Ph.D.’s (from 38.9 to 43.3), M.D.’s (from 39.9 to 46.5), and M.D.-Ph.D.’s (from 40.2 to 45.9) (Figure 2-7). In addition, the number of NIH-supported researchers under age 46 has declined over a 32-year period,47 even after implementation of new investigator and ESI policies.48
The precise reason for why the age of receipt of the first NIH R01-equivalent award has increased, even as the success rate of new investigators relative to
___________________
46 Data provided courtesy of NIH.
47 See https://www.nap.edu/catalog/11249/bridges-to-independence-fostering-the-independence-of-new-investigators-in (accessed January 19, 2018).
48 See https://grants.nih.gov/grants/guide/notice-files/NOT-OD-08-121.html.
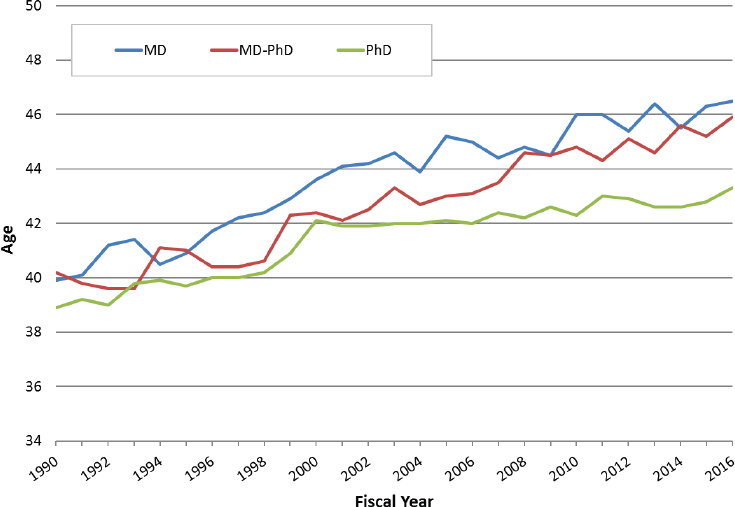
SOURCE: Data provided courtesy of NIH.
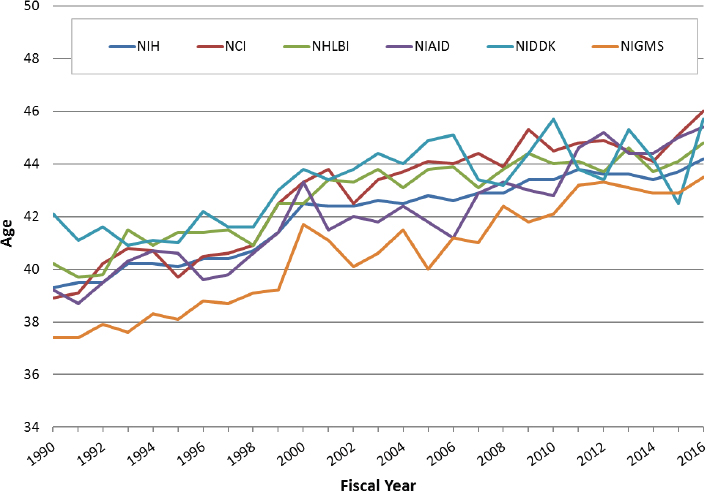
established investigators has stabilized, is unclear and a matter of debate.49 NIH data show that the number of years to first R01 since the investigator’s last degree has increased over time as well, suggesting that the increase in the age at first R01 cannot be explained by any delays in the start or culmination of doctoral education (Figure 2-8). The data also show that the number of years on average between an investigator’s first R01 and second R01 has mostly held steady over time, suggesting that whatever is causing the delays over time in the capacity of investigators to obtain their first R01 is largely confined to the pursuit of that first grant (Figure 2-9). Finally, the rise in the age exists across NIH Institutes, which suggests an effect of larger workforce trends that apply across all areas of biomedical research (Figure 2-10). The rise persists across race50 and gender51 as well.
___________________
49 Many researchers consider the phenomenon of investigators delaying retirement, and therefore continuing to compete with new investigators in the NIH pool, as one leading factor (Heggenness et al., 2017; Levitt and Levitt, 2017).
50 From 1990 to 2016, the age at first R01-equivalent for white, Asian, and multi-race investigators increased from 39.1 to 44.1, while the age for underrepresented minorities increased from 38.9 to 43.3. Data provided courtesy of NIH.
51 From 1990 to 2016, the age at first R01-equivalent for female investigators increased from 39.7 to 44.2, while the age for male investigators increased from 39.1 to 44.2. Data provided courtesy of NIH.
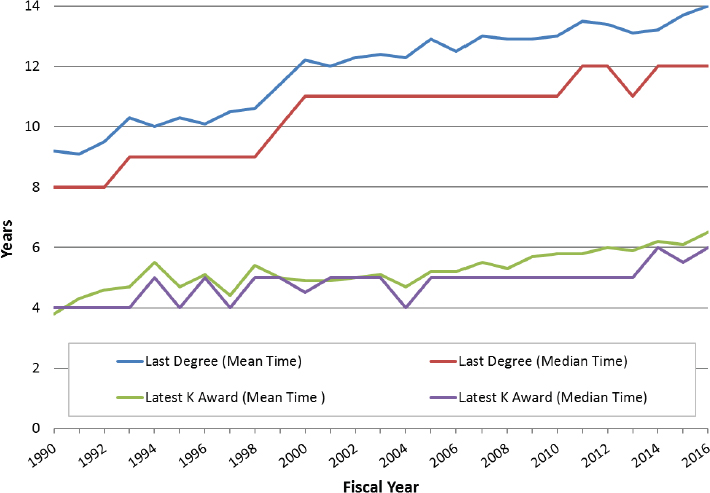
SOURCE: Data provided courtesy of NIH.
SOURCE: Data provided courtesy of NIH.
SOURCE: Data provided courtesy of NIH.
Today, even when ESIs and new investigators do receive an R01-equivalent award, they often confront the challenge of the declining purchasing power of these awards, because the size of these awards has not tracked with either overall inflation or the rising cost of conducting research as measured by the Biomedical Research and Development Price Index,52 despite some increase in the average costs for R01s when adjusted for inflation. As a result, investigators often need to secure more than one source of financial support to establish and sustain their laboratories.
Additional avenues of federal research support for emerging biomedical researchers include NIH’s Exploratory/Developmental Research Grant Award (R21), NIH Director’s New Innovator Award (DP2), Early Independence Award (DP5), and Pathway to Independence Award (K99/R00). According to NIH, the nonrenewable R21 grant mechanism, as opposed to the renewable R01 award, is intended to encourage exploratory or developmental research by providing support for the early and conceptual stages of project development, usually defined as lasting no longer than 2 years. Although R21 awards are not specifically designed to support ESIs, data provided by NIH highlights the fact that the R01 is increasingly giving way to the R21 and other awards as the research grant that starts investiga-
___________________
52 See https://officeofbudget.od.nih.gov/gbipriceindexes.html (accessed January 19, 2018).
tors’ NIH-funded career (Figure 2-11). Each year, roughly the same number of investigators now apply for an R21 and an R01 as their first grant.53 These trends are observed across all age cohorts.54
R21 awards may be regarded as an opportunity to secure initial funding for an emerging investigator’s independent research career, but analysis of R21 awardees shows that receipt of the award does not increase the success rate for receiving an R01-equivalent award.55 Not all individual NIH Institutes offer R21 awards, and data provided by NIH show that applications for R21 awards have increased to the point where success rates for receiving the award are now lower than for R01-equivalent awards, at 15 percent and 20 percent, respectively, in 2016.56 In addition, R21 awards provide less funding over a shorter time period compared to R01-equivalent awards, and thus are less ideal for establishing an independent research career. The combined budget for direct costs for the 2-year R21 project period may not exceed $275,000, and no more than $150,000 may be requested in any single year.57 In 2016, the average cost of competing R21 awards was $221,434, whereas the average cost for an R01 award, which can span 5 years, was $476,631 per year.58 The higher level of funding and longer funding period for R01 grants are designed to provide researchers with the time and resources necessary to collect and publish data that represent a substantial addition to biomedical knowledge.
The NIH Director’s New Innovator Award (DP2) program offers a small number of awards through the NIH Common Fund to support highly innovative research from promising ESIs. DP2 applicants can request up to $1.5 million in direct costs spread over the 5-year grant period. Data on the DP2 awards indicate that awardees have a higher rate of application for R01 awards compared to a matched cohort of ESIs who receive R01 awards, although DP2 awardees are not more successful at receiving an R01 award (National Institutes of Health, 2017). Although the DP2 award seems to be an important mechanism for supporting ESIs as they transition into research independence, NIH expects to make only 33 awards in 2018, depending on availability of funds in the NIH Common Fund. This represents a decrease from the 55 awards in 2017.59
Developed in response to the National Academies Bridges to Independence report (National Research Council, 2005), NIH launched the K99/R00 Pathway to Independence awards in 2006 to
___________________
53 Data provided courtesy of NIH.
54 Data provided courtesy of NIH.
55 Open Mike Blog. R01 and R21 Applications and Awards: Trends and Relationships Across NIH. https://nexus.od.nih.gov/all/2016/11/04/nih-r01-r21/ (accessed February 8, 2018).
56 See https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=202andcatId=2 (accessed February 9, 2018).
57 See https://grants.nih.gov/grants/funding/funding_program.htm (accessed January 19, 2018).
58 See https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=294andcatId=2 (accessed February 8, 2018).
59 See https://commonfund.nih.gov/newinnovator/faq (accessed December 15, 2017).
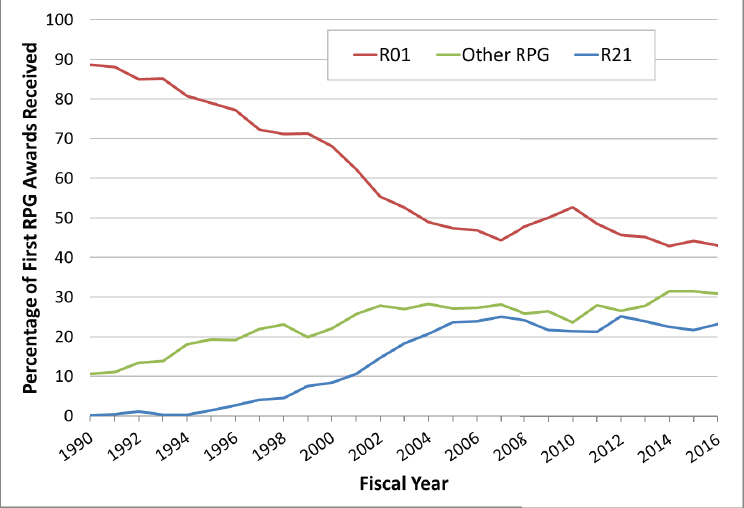
NOTE: Other RPGs for purposes of this figure include a range of R-series, DP-series, P-series, and U-series awards.
SOURCE: Data provided courtesy of NIH.
. . . help outstanding postdoctoral researchers with a research and/or clinical doctorate degree complete needed, mentored career development and transition in a timely manner to independent, tenure-track, or equivalent faculty positions. The K99/R00 award is intended to foster the development of a creative, independent research program that will be competitive for subsequent independent funding and that will help advance the mission of the NIH.60
The K99/R00 award is unique among NIH awards in that it combines an initial mentored phase—a K99-supported postdoctoral position—with the investigator’s first independent research support, the R00 phase. This award is available to individuals who have less than 4 years of postdoctoral training, and to non-U.S. citizens and physician-scientists. The K99 phase lasts a maximum of 2 years, and the R00 phase provides up to 3 years of independent research support for individuals who have secured an independent, tenure-track, or equivalent faculty position by the end of the K99 period. In 2016, 231 K99s were awarded
___________________
60 See https://grants.nih.gov/grants/guide/pa-files/PA-16-077.html (accessed December 15, 2017).
with a success rate of 23 percent.61 One recent analysis of the K99/R00 award reveals that recipients have a higher success rate for subsequent R01 and other grants compared to those supported on other K-series career development awards (Carlson et al., 2016).
Additional support for ESIs from NIH includes several innovative Institute-specific programs that seek to support these researchers’ transition to independence: the National Institute of Mental Health (NIMH) Biobehavioral Research Awards for Innovative New Scientists (BRAINS) award, the National Institute of General Medical Sciences (NIGMS) Maximizing Investigators’ Research Award (MIRA), and the NIH Director’s Early Independence Award (DP5). Together, these programs fund only 100 or so awards per year.62
The number of federal research awards to help investigators transition into independent faculty research positions is limited, and postdoctoral researchers are typically not prepared or, often even eligible,63 to submit an R01 application prior to obtaining a faculty appointment. Funding for emerging investigators is generally provided by their host institutions, and universities have reported surges in the size of start-up packages offered to junior faculty. In testimony to the committee, committee member Nancy Andrews, former dean and vice chancellor for academic affairs at Duke University School of Medicine, confirmed this phenomenon: she observed that the current “range for the amount of cash that basic science department assistant professors are offered is probably between about $800,000 and the highest I have heard is $3.5 million nationally . . . but more typically it would be something like $1.2 to $1.8 million, sometimes including three years of salary.” These trends align with data revealing that higher education institutions are the second largest funder of basic science research in this country behind the government (Figure 2-12). This upward pressure may make K99/R00 award recipients more attractive for recruitment to faculty positions at academic institutions because they have been successful at obtaining NIH funding.
OTHER CHALLENGES IN PURSUING RESEARCH CAREERS
Funding remains the paramount concern for early-career scientists, but a 2016 survey of Nature readers highlighted additional areas of concern (Powell, 2016). Of the nearly 12,000 readers who responded to the survey question, “What do you think is the biggest challenge facing early-career scientists?”, the top concerns included not only securing research funding but also balancing work and home responsibilities and navigating the publishing culture. Reports that scientists find themselves spending more time writing grant applications and less time
___________________
61 NIH Data Book. Research Project Grants: Competing Applications, Awards, and Success Rates. https://report.nih.gov/nihdatabook/ (accessed February 2, 2018).
62 See https://grants.nih.gov/grants/guide/rfa-files/RFA-RM-17-008.html and https://loop.nigms.nih.gov/2016/08/first-mira-awards-to-new-and-early-stage-investigators/ (accessed January 19, 2018).
63 Eligibility restrictions often apply to the institution.
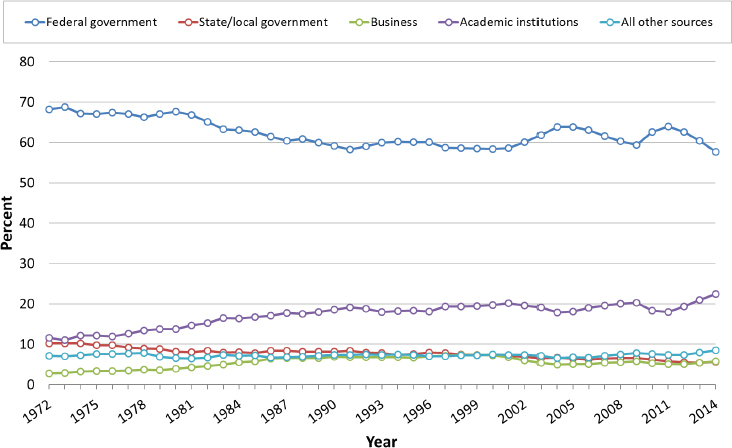
NOTE: Academic institutions’ funds exclude research funds spent from multipurpose accounts.
SOURCE: Adapted from https://www.nsf.gov/statistics/2016/nsb20161/#/report/chapter-5/expenditures-and-funding-for-academic-r-d (accessed January 19, 2018).
doing creative research are borne out by data showing that young investigators are submitting a larger number of grant applications each year than ever before.64 Nearly two-thirds of the survey respondents also said they considered quitting research at some point in their career, and, in fact, it appears that investigators today are leaving the NIH-funded workforce at an accelerated rate relative to the past (Figure 2-13).65
___________________
64 See http://www.unitedformedicalresearch.com/wp-content/uploads/2012/07/Broken-Pipeline.pdf. Data provided courtesy of NIH show that applicants ages 36 to 45 submitted an average of 3.42 grant applications each between 2011 and 2016, an average of 3.11 grant applications each between 2004 and 2010, an average of 2.59 grant applications each between 1998 and 2003 (during the doubling), and an average of 2.98 grant application each from 1990 to 1997. This same trend can be seen in each of the other age cohorts as well.
65 The figure shows data for PIs who received an NIH RPG. Data provided courtesy of NIH also suggest a similar trend for investigators who never obtained an RPG. A greater percentage (58 percent) of investigators who first applied for an RPG during 2004-2010 have failed to receive any funding than investigators who first applied for an RPG during the NIH doubling from 1998 to 2003 (48 percent) or 1990 to 1997 (53 percent). These results are tempered by the fact that investigators from 2004 to 2010 are more likely than earlier cohorts to yet obtain funding at some point in the future.
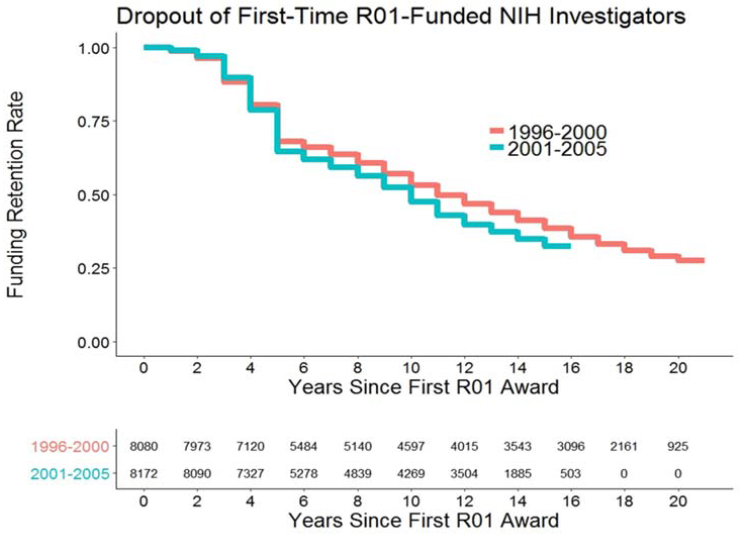
NOTE: Plot shows PI retention rate by years since first R01-equivalent award. Each curve shows dropout (conversely, retention) of investigators after they received their first R01equivalent award. Investigators are grouped into cohorts based on the first fiscal year of their first R01-equivalent award.
SOURCE: Chart provided courtesy of NIH.
Of special concern for the biomedical research enterprise are the enduring barriers to independent faculty research careers faced by women and individuals from underrepresented racial and ethnic groups. As of 2016, women had equivalent NIH RPG success rates and representation in NIH research career development awards as their male counterparts,66 yet the average total research grant size for men was nearly $75,000 more than for women.67 Additionally, faculty positions are often required for eligibility to apply for an NIH grant, but between 2011 and 2012, women represented only 30 percent of biomedical faculty at the assistant, associate, and full professor levels (Valantine et
___________________
66 Research Career Development Award Recipients and Kirschstein-NRSA Trainees and Fellows: Representation of Women, by Activity and Career Stage. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?sid=0andindex=1andcatId=15andchartId=170 (accessed February 9, 2018).
67 Research Grants: Average Size, by Gender. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=173andcatId=15 (accessed February 9, 2018).
al., 2016). In fact, women represented only 32 percent of all NIH-supported investigators on RPGs.68
It is unclear whether the high rate of attrition for women between Ph.D. attainment and faculty research positions is due to personal choice or hiring discrimination, but the 2007 National Academies report Beyond Bias and Barriers reported that women leave academia because of a lack of mentorship or guidance and difficulty managing family and career responsibilities, among many other socially and culturally influenced factors (National Academy of Sciences et al., 2007). These findings are consistent with those from a 2009 study that revealed that female Ph.D.’s with children, or planning to have children, opted out of the NIH R01 pool in favor of a career they believed would be more compatible with their family work-life plans (Ginther and Kahn, 2006).
Despite longstanding efforts to increase racial and ethnic diversity in the biomedical research workforce, the proportion of individuals from underrepresented minority groups hired into faculty research positions and securing NIH RPGs has not matched their steady gains in Ph.D. attainment (Gibbs et al., 2016). A recent analysis by Meyers et al. (2018) examining underrepresented minority research faculty participation at medical schools reveals significant retention issues between their postdoctoral experiences and faculty research positions. Once in faculty research positions, African Americans applicants experience significant disparities in R01-funding (Ginther et al., 2011). Additionally, African Americans proportionately resubmit fewer R01 applications than do White, Asian, or Hispanic applicants (National Institutes of Health, 2012b). In an analysis spanning 1999 to 2009, 73 percent of applications from African Americans were not discussed in NIH peer review, which may have impacted their resubmission rates (National Institutes of Health, 2012b). The decreased representation of underrepresented minority biomedical postdoctoral and faculty researchers coincides with a decline in NIH-supported training and career development programs with a focus on diversity and remains an area of continued concern (Valantine et al., 2016).
The challenges facing early-career biomedical researchers command urgent and sustained attention. In a Nature article, Jon Lorsch, head of NIGMS, said that the 2016 Nature survey results echo what he hears from early-career scientists as he travels nationwide: “We risk losing a generation of researchers at the prime of their creativity and energy” (Powell, 2016).
REFERENCES
Alberts, B., M. W. Kirschner, S. Tilghman, and H. Varmus. 2014. Rescuing US biomedical research from its systemic flaws. Proceedings of the National Academy of Sciences of the United States of America 111(16):5773-5777.
___________________
68 Research Grant Investigators: Representation of Women, by Mechanism. https://report.nih.gov/NIHDatabook/Charts/Default.aspx?showm=YandchartId=169andcatId=15 (accessed February 9, 2018).
American Academy of Arts and Sciences. 2014. Restoring the foundation: The vital role of research in preserving the American dream. Cambridge, MA: American Academy of Arts and Sciences.
Berg, J. 2016. Modeling the annual number of new and competing NIH research project grants. In ScienceHound. Washington, DC: American Association for the Advancement of Science.
Carlson, D. E., W. C. Wang, and J. D. Scott. 2016. Initial outcomes for the NHLBI K99/R00 pathway to independence program in relation to long-standing career development programs: Implications for trainees, mentors, and institutions. Circulation Research 119(8):904-908.
Dickler, H. B., D. Fang, S. J. Heinig, E. Johnson, and D. Korn. 2007. New physician-investigators receiving National Institutes of Health research project grants: A historical perspective on the “endangered species.” JAMA 297(22):2496-2501.
Dorsey, E. R., B. C. Van Wuyckhuyse, C. A. Beck, W. P. Passalacqua, and D. S. Guzick. 2009. Economics of new faculty hires in basic science. Academic Medicine: Journal of the Association of American Medical Colleges 84(1):26-31.
FASEB (Federation of American Societies for Experimental Biology). 2015. Sustaining discovery in biological and medical sciences: A framework for discussion. Bethesda, MD: Federation of American Societies for Experimental Biology.
Fochler, M., U. Felt, and R. Müller. 2016. Unsustainable growth, hyper-competition, and worth in life science research: Narrowing evaluative repertoires in doctoral and postdoctoral scientists’ work and lives. Minerva 54(2):175-200.
Gibbs, K. D., J. Basson, I. M. Xierali, and D. A. Broniatowski. 2016. Decoupling of the minority PhD talent pool and assistant professor hiring in medical school basic science departments in the US. Elife 5.
Gibbs, K. D., Jr., and K. A. Griffin. 2013. What do I want to be with my PhD? The roles of personal values and structural dynamics in shaping the career interests of recent biomedical science PhD graduates. CBE Life Sciences Education 12(4):711-723.
Gibbs, K. D., J. McGready, and K. Griffin. 2015. Career development among American biomedical postdocs. CBE Life Sciences Education 14(4):ar44.
Ginther, D. K., W. T. Schaffer, J. Schnell, B. Masimore, F. Liu, L. L. Haak, and R. Kington. 2011. Race, ethnicity, and NIH research awards. Science 333(6045):1015-1019.
Ginther, D. K., and S. Kahn. 2006. Does science promote women? Evidence from academia 19732001. Cambridge, MA: National Bureau of Economic Researh.
Heggeness, M. L., K. T. Gunsalus, J. Pacas, and G. McDowell. 2017. The new face of US science. Nature 541(7635):21-23.
Institute of Medicine, National Academy of Sciences, and National Academy of Engineering. 2000. Enhancing the postdoctoral experience for scientists and engineers: A guide for postdoctoral scholars, advisers, institutions, funding organizations, and disciplinary societies. Washington, DC: The National Academies Press.
Joiner, K. A. 2005. A strategy for allocating central funds to support new faculty recruitment. Academic Medicine 80(3):218-224.
Kahn, S., and D. K. Ginther. 2017. The impact of postdoctoral training on early careers in biomedicine. Nature Biotechnology 35(1):90-94.
Kamerlin, S. C. 2015. Hypercompetition in biomedical research evaluation and its impact on young scientist careers. International Microbiology 18(4):253-261.
Kimble, J., W. M. Bement, Q. Chang, B. L. Cox, N. R. Drinkwater, R. L. Gourse, A. A. Hoskins, A. Huttenlocher, P. K. Kreeger, P. F. Lambert, M. R. Mailick, S. Miyamoto, R. L. Moss, K. M. O’Connor-Giles, A. Roopra, K. Saha, and H. S. Seidel. 2015. Strategies from UW-Madison for rescuing biomedical research in the US. Elife 4:e09305.
Levitt, M., and J. Levitt. 2017. Future of fundamental discovery in US biomedical research. Proceedings of the National Academy of Sciences of the United States of America 114(25):6498-6503.
McDowell, G. S., K. T. Gunsalus, D. C. MacKellar, S. A. Mazzilli, V. P. Pai, P. R. Goodwin, E. M. Walsh, A. Robinson-Mosher, T. A. Bowman, J. Kraemer, M. L. Erb, E. Schoenfeld, L. Shokri, J. D. Jackson, A. Islam, M. D. Mattozzi, K. A. Krukenberg, and J. K. Polka. 2014. Shaping the future of research: A perspective from junior scientists. F1000Res 3:291.
Meyers, L. C., A. M. Brown, L. Moneta-Koehler, and R. Chalkley. 2018. Survey of checkpoints along the pathway to diverse biomedical research faculty. PLoS ONE 13(1):e0190606.
National Academy of Sciences, National Academy of Engineering, and Institute of Medicine. 2014a. The postdoctoral experience revisited. Washington, DC: The National Academies Press.
National Academy of Sciences, National Academy of Engineering, and Institute of Medicine. 2014b. The arc of the academic research career: Issues and implications for U.S. science and engineering leadership: Summary of a workshop. Washington, DC: The National Academies Press.
National Academy of Sciences, National Academy of Engineering, and Institute of Medicine. 2007. Beyond bias and barriers: Fulfilling the potential of women in academic science and engineering. Washington, DC: The National Academies Press.
National Institutes of Health. 2014. National Institutes of Health Physician-Scientist Workforce Working Group report. Bethesda, MD: National Institutes of Health.
National Institutes of Health. 2012a. Biomedical Research Workforce Working Group report. Bethesda, MD: National Institutes of Health.
National Institutes of Health. 2012b. Draft report of the Advisory Committee to the Director Working Group on Diversity in the Biomedical Research Workforce. Bethesda, MD: The National Institutes of Health.
National Institutes of Health. 2017. National Institutes of Health Director’s New Innovator Award outcomes evaluation. Bethesda, MD: The National Institutes of Health.
National Research Council. 2011. Research training in the biomedical, behavioral, and clinical research sciences. Washington, DC: The National Academies Press.
National Research Council. 2005. Bridges to independence: Fostering the independence of new investigators in biomedical research. Washington, DC: The National Academies Press.
Powell, K. 2016. Young, talented and fed-up: Scientists tell their stories. Nature 538(7626):446-449.
Sauermann, H., and M. Roach. 2016. Scientific workforce. Why pursue the postdoc path? Science 352(6286):663-664.
Sauermann, H., and M. Roach. 2012. Science PhD career preferences: Levels, changes, and advisor encouragement. PloS One 7(5):e36307.
Valantine, H. A., P. K. Lund, and A. E. Gammie. 2016. From the NIH: A systems approach to increasing the diversity of the biomedical research workforce. CBE Life Sciences Education 15(3).
This page intentionally left blank.






























