1
Introduction
A pressing challenge in the modern health care system is the gap between education and clinical practice, said Malcolm Cox, member of the Global Forum on Innovation in Health Professional Education (the Forum). Emerging technologies have the potential to bridge this gap by creating the kind of team-based learning environments and clinical approaches that are increasingly necessary in the modern health care system both in the United States and around the world. To explore these technologies and their potential for improving education and practice, the Forum hosted a workshop titled Improving Health Professional Education and Practice Through Technology. The 1.5-day workshop, held in Washington, DC, on November 16 and 17, 2017, was attended by participants from 19 different health professions, from countries including Australia, Canada, Qatar, Switzerland, and the United States. The objective of the workshop was:
Explore effective use of technologies as tools for bridging identified gaps within and between health professions education and practice in order to optimize learning, performance, and access in high-, middle-, and low-income areas while ensuring the well-being of the formal and informal health workforce.1
The full Statement of Task is in Appendix A.
USING TECHNOLOGY TO ADDRESS CURRENT CHALLENGES
Pamela Jeffries, a member of the planning committee, welcomed participants to the event and gave a brief overview of some of the current challenges in health care and how technology may address these challenges and improve both education and clinical practice. The workshop, said Jeffries, confronts a major problem in the preparation of health professionals: the gap between academia and clinical practice. Jeffries explained that while health professional students are learning new knowledge, skills, and attitudes while in their educational environments, it is not clear that what they are learning matches the demand for what is needed in practice.
Javaid Sheikh, dean of the Weill Cornell Medical College in Qatar, expanded on this with a reminder: “What looks good on paper . . . does not always succeed in real life.” The health care market should theoretically respond to demand, resulting in a good match between the health needs of the population and the preparedness and supply of health professionals, Sheikh continued. However, in real life, there are a number of mismatches in the market that result in inefficiencies, underserved populations, and expensive care. The true population health needs are not reflected in the demand for care, in part because of perverse incentives that prioritize curative care over preventive care, which is often not reimbursed. As described in a previous forum workshop on the financial economics of health professions education (NASEM, 2017), the demand for care does not match perfectly with the supply of care, owing to a saturated labor market and the fact that health professionals tend to aggregate in certain geographic regions and specialties, said Sheikh. Health professions education and training do not necessarily align with the needs of the population or the demands of the market (see Figure 1-1).
To remedy these mismatches, said Jeffries, it will be necessary to transform health professions education in order to more closely match the skills and knowledge needed in the real world. She asked, “Are we limited in how
___________________
1 The informal health workforce, sometimes called the “shadow workforce,” includes caregivers who did not go through formal health professional training such as family members who provide care for loved ones (Phillips et al., 2016).
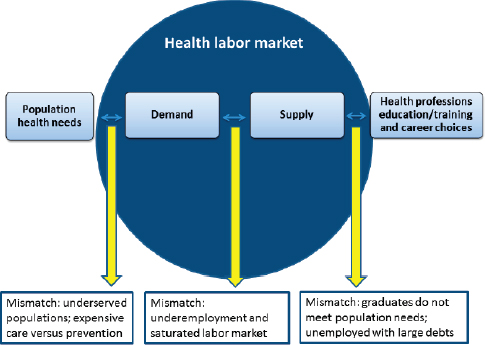
SOURCES: Presented by Sheikh, November 16, 2017. From NASEM, 2017.
we teach in academic settings because of obstacles that prevent us from replicating real practice? Or are there opportunities in simulation to teach students the full scope of practice in a controlled, but realistic environment?” To address these questions, the workshop explored ways to bridge the gap using technology and innovative approaches through presentations and discussions about existing, emerging, and futuristic technologies from multiple disciplines and multiple countries. The hope, said Jeffries, is that the use of these technologies can help to “overcome challenges to improve the education of our practitioners and ultimately improve our health care quality and patient outcomes.” To set the stage, Jeffries described five issues in health professions education and health care that technology has the potential to improve: the new generation of learners, clinical education, faculty shortage, changes in health care, and cost.
New Generation of Learners
Students joining the health professions are no longer digital immigrants, but digital natives, said Jeffries. These learners understand technology better than any generation before them—and better than their faculty—and typically have numerous devices at their fingertips ready to retrieve information, communicate, and explore across borders. They also have certain expectations coming into their learning environment; evidence has shown that current learners expect their faculty to use technology in education and to incorporate the technologies needed for their profession (McKnight et al., 2016). Current learners are able to use certain technologies as a platform for learning, particularly in underserved areas where geographically it may be a challenge to attend classes, have clinical experiences, or embark on a learning experience without the assistance of technology. For example, said Jeffries, midwives in Bangladesh are learning new ways to implement mother–baby care through videos, social media, and other technologies. Technological platforms are no longer a novelty for students, but an expectation, as demonstrated through their way of living, being, and learning.
Clinical Education
There are many challenges in clinical education that educators, practitioners, and leaders all have to navigate, said Jeffries. Typically, health professional students are assigned to clinical sites, and their clinical practice is conducted in parallel with their didactic courses. Securing appropriate clinical sites for all health professional students is a major challenge. The American Association of Colleges of Nurses reported that 64,000 qualified applicants eligible for baccalaureate and graduate nursing education were not admitted to programs because of the lack of clinical sites, faculty shortage, and a lack of preceptors needed for graduate clinical education (AACN, 2017). In a recent survey of medical schools, half reported concerns about the availability of residency positions for their students after graduate school, and 85 percent indicated concerns about finding clinical sites and qualified clinical preceptors (AAMC, 2018). Jeffries asked, “How can technology help to remedy these challenges with our admissions and acceptance of needed qualified students entering our health professions?” She noted that while technology may be an important part of the answer to this problem, the implementation “isn’t as easy as one would think,” owing to legal and policy issues that must be considered. For example, getting state authorization for online distance education learning can be challenging, as requirements and rules differ from state to state.
Faculty Shortage
The shortage of qualified nursing faculty is another major challenge in preparing health professionals, Jeffries said. Existing nursing faculty are aging: the average age of a doctorally prepared professor is 62 years old and the average of a doctorally prepared associate professor is 58 years old (AACN, 2017). As current health professionals retire, and the population ages and requires more health care, the pipeline of health professionals must keep up with demand. In medicine, one-third of physicians are over the age of 55 (AAMC, 2016). Without an adequate number of faculty to teach, the output of prepared health professionals will continue to not meet the demand of a growing population. However, through the use of technologies, said Jeffries, there is the potential for supporting a larger group of faculty to teach health professions; using experienced, retired faculty in some aspect; and making content scalable and accessible. For example, massive, open online courses could be one tool to help to deliver, scale up, and extend content to health professions students across the globe. Jeffries said that the idea of providing open source materials and information is a very nontraditional concept in higher education, but one that has great potential.
Changes in Health Care
The health care environment is changing, said Jeffries, with shifts from acute care to chronic care, with the demand for global aspects of care, and with the never-ending need to prepare for unique types of medical challenges (e.g., the Ebola epidemic) that require just-in-time learning. It is essential that practitioners be prepared to deliver high-quality patient care, whether in an acute care environment or a primary care setting such as a rural community clinic in an underserved area, said Jeffries. Health care practitioners must understand population health, social determinants, and have the knowledge and skills to work with diverse communities in diverse areas. Just-in-time learning requires that health professionals be nimble and ready to deploy new knowledge, best practices, and new interventions when necessary. “How can technology prepare our health professions students, interns, residents, and practicing providers for this new world?” asked Jeffries. “How can the use of technologies help prepare our practitioners for these environments, challenges, and to care for populations and communities in addition to individual clients?”
Cost
As with any venture, said Jeffries, the cost and financial implications must be considered. While new technologies are often costly to develop and
disseminate, there is the potential for cost savings as well. Using technology to disseminate education to health professionals could be a way to teach thousands of health care providers across the globe while eliminating barriers to access, reducing costs, and ensuring consistency in quality and delivery. However, those who do not have access to the Internet or technologies may be left behind, said Jeffries, furthering the financial divide.
CONCLUSION
Jeffries told participants that the workshop was centered around the idea that technology is only a platform or a tool to use for education, not an end unto itself. Technology is embedded in everyday life, including health professions education, communication, and as a way to access information. Rural communities are dependent on the use of technology, such as the use of mobile phones to connect and educate health professionals in rural African regions. Technology can help to connect, empower, and support health professionals, wherever they may practice. “Harnessing the power of technologies allows us to make an impact in communities by creating a culture of health, supporting education, giving support for addictions, or just notifying about annual flu shots,” said Jeffries.
REFERENCES
AACN (American Association of College of Nurses). 2017. Nursing faculty shortage fact sheet. http://www.aacnnursing.org/Portals/42/News/Factsheets/Faculty-Shortage-Factsheet-2017.pdf (accessed March 21, 2018).
AAMC (Association of American Medical Colleges). 2016. The complexities of physician supply and demand: Projections from 2014 to 2025 https://www.heartland.org/publications-resources/publications/2016-update-the-complexities-of-physiciansupply-and-demand-projections-from-2014-to-2025 (accessed August 16, 2018).
AAMC. 2018. Results of the 2017 medical school enrollment survey. www.aamc.org/MSE SurveyResults (accessed August 16, 2018).
McKnight, K., K. O’Malley, R. Ruzic, M. K. Horsley, J. J. Franey, and K. Bassett. 2016. Teaching in a digital age: How educators use technology to improve student learning. Journal of Research on Technology in Education 48(3):194–211.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Future financial economics of health professional education: Proceedings of a workshop. Washington, DC: The National Academies Press. https://doi.org/10.17226/24736.
Phillips, S. S., D. M. Ragas, N. Hajjar, L. S. Tom, X. Dong, and M. A. Simon. 2016. Leveraging the experiences of informal caregivers to create future healthcare workforce options. Journal of the American Geriatrics Society 64(1):174–180.






