This panel focused on current programs to strengthen the medical educational pipeline through greater support of underrepresented minority students, and especially Black boys and men. André L. Churchwell, M.D.,1 presented a pipeline program for undergraduate students at Vanderbilt University. James L. Moore III, Ph.D.,2 discussed lessons learned from work at the Todd A. Bell National Resource Center on the African American Male at The Ohio State University. Marja Hurley, M.D.,3 described a range of pipeline programs at UConn Health. Joan Y. Reede, M.D., M.S., M.P.H., M.B.A.,4 described pipeline programs and lessons learned at Harvard Medical School. Freeman Hrabowski III, Ph.D.,5 moderated the session and led a brief discussion following the presentations.
MEYERHOFF SCHOLARS PROGRAM
Freeman Hrabowski III, Ph.D. President University of Maryland, Baltimore County
To launch the discussion, Hrabowski briefly described the Meyerhoff Scholars Program at the UMBC,6 which provides financial support, men-
___________________
1 Churchwell is Levi Watkins, Jr., M.D. chair and chief diversity officer at the Vanderbilt University Medical Center and senior associate dean for diversity affairs at the Vanderbilt University School of Medicine.
2 Moore is interim vice provost for diversity and inclusion and chief diversity officer, executive director of the Todd A. Bell National Resource Center on the African American Male, and College of Education and Human Ecology distinguished professor of urban education at The Ohio State University.
3 Hurley is professor of medicine and orthopedics at the University of Connecticut (UConn) School of Medicine and associate dean for the Health Career Opportunity Programs at UConn Health.
4 Reede is dean for diversity and community partnership at Harvard Medical School.
5 Hrabowski is president of the University of Maryland, Baltimore County (UMBC).
6 For more information about the Meyerhoff Scholars Program, see https://meyerhoff.umbc.edu (accessed February 28, 2018).
toring and advising, and exposure to research to undergraduate students committed to increasing the representation of minorities in science and engineering and to obtaining Ph.D. degrees in math, science, and engineering.7 He commented on the program’s successes, noting that UMBC is the top producer of African American M.D./Ph.D. recipients, having produced 42 M.D./Ph.D.s since 2000, with relative parity among men and women. From his experience with the Meyerhoff program, Hrabowski identified key elements necessary for successful pipeline programs. First, he emphasized the importance of a school’s commitment to increasing the number of African American science graduates. He remarked, “If we really want to see a difference . . . the culture of the institution has to change. It has to be a priority.” He elaborated that both faculty and leadership, including top administrative staff like university presidents and deans, are crucial to driving change. Second, he noted the importance of applying evidence and data, saying “We are much too warm and fuzzy when talking about these issues. We need to focus on having a culture that will emphasize analytics and look at who succeeds and what it takes to succeed.” Finally, Hrabowski underscored the importance of building cohorts that collaborate, support each other, and are accountable to each other, and which are also supported by mentors.
VANDERBILT UNIVERSITY SCHOOL OF MEDICINE AFRICAN AMERICAN AND DISADVANTAGED STUDENT PIPELINE PROGRAM
André L. Churchwell, M.D. Levi Watkins Jr., M.D. Chair and Chief Diversity Officer Vanderbilt University Medical Center Professor of Medicine (Cardiology), Professor of Radiology and Radiological Sciences, Professor of Biomedical Engineering, and Senior Associate Dean for Diversity Affairs Vanderbilt University School of Medicine
The Vanderbilt University School of Medicine (VUSM) recently implemented a “short pipeline” program. The program is a partnership among three Historically Black Colleges and Universities (HBCUs)—Morehouse College, Spelman College, and Fisk University. The fourth institution included in the partnership, Berea College, has a long history of provid-
___________________
7 The first cohort of Meyerhoff Scholars comprised 19 African American men. The second cohort expanded to include African American women, and in 1996, the program was opened to students of all backgrounds. For the 2017–2018 academic year, 260 students enrolled in the program, of whom 63 percent identify as African American, 15 percent as Caucasian, 11 percent as Asian, 10 percent as Hispanic, and 1 percent as Native American.
ing undergraduate education for minority and international students. The program is designed to support underrepresented minorities who intend to pursue medical education, which provides a direct path for admission to VUSM. The program applies holistic criteria to select undergraduate premedical students. The program then connects selected students with faculty and current medical student mentors and provides tutoring and academic support throughout their 4 years. Students also participate in a summer program that includes coursework in the basic sciences, Medical College Admission Test (MCAT) preparation, and research experiences. Students are provisionally admitted to VUSM and those who maintain a grade point average and achieve MCAT scores that have been jointly agreed upon by the undergraduate schools and VUSM matriculate into VUSM. The first cohort of four rising college sophomores was inducted in the summer of 2017.8 As a lesson for other schools that intend to replicate or scale this type of program, Churchwell identified commitment from leadership, including both the belief that the program is important, and the commitment of financial resources, as key to the program’s successful implementation. He added,
The goal here is to try to create some type of connection. . . . [We] believe that this is an important thing to do, number one. Number two, the students feel warm and fuzzy, and they are connected to us. Three, we try to diminish the idea of [applying for and matriculating to medical school] being just an insurmountable hurdle by going through the selection process and giving them the premed curriculum and a lot of tests along the way to generate their confidence to build their idea of success of coming into [VUSM].
Churchwell also presented his Marshall Plan for American education, a proposal to create a national pipeline program to support a broader range of underrepresented minorities and disadvantaged groups. In this program, Churchwell envisions schools of the Association of American Universities as statewide hubs, supported by a national superstructure that is connected to the federal government. These hubs would be connected to HBCUs and other colleges, K–12 school systems, state and national educational departments and leadership, education experts, and philanthropic organizations, among others. See Figure 5-1 for more detail.
___________________
8 For more information on the VUSM “short pipeline” program, see https://news.vanderbilt.edu/2017/07/27/school-of-medicine-programs-enhancing-diversity-of-applicants (accessed February 28, 2018).
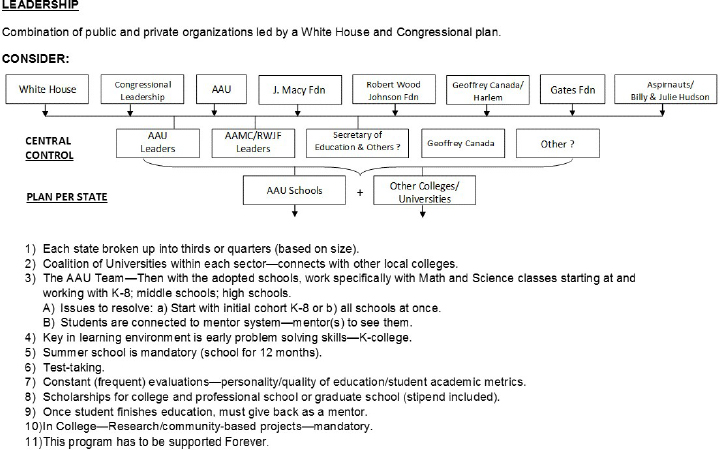
NOTE: AAMC = Association of American Medical Colleges; AAU = Association of American Universities; Fdn = Foundation; J. Macy Fdn = The Josiah Macy Jr. Foundation; K = kindergarten; RWJF = Robert Wood Johnson Foundation.
SOURCE: Presentation by André L. Churchwell, November 20, 2018.
THE OHIO STATE UNIVERSITY BELL NATIONAL RESOURCE CENTER ON THE AFRICAN AMERICAN MALE
James L. Moore III, Ph.D. Interim Vice Provost for Diversity and Inclusion and Chief Diversity Officer Executive Director, Todd A. Bell National Resource Center on the African American Male College of Education and Human Ecology Distinguished Professor of Urban Education The Ohio State University
Moore began his presentation by highlighting the need to focus on racial disparities and not just socioeconomic status. He reasoned that, although race and socioeconomic status are correlated, focusing solely on low-income students may miss capturing Black students of higher socioeconomic position who still underperform and are underrepresented
relative to peers of other racial and ethnic backgrounds, and especially compared with White peers. Moore next described what he called his “ethos of excellence,” which states that attaining achievements (e.g., educational and professional attainment) is the product of competence (or skills), and confidence (or will). Focusing on the latter, he distinguished between persistence and resilience. He commented, “Persistence is the constant sustained effort. Resilience is bouncing back. How do we help young people—you don’t even have to motivate them; they get up just on their own and they do their work on their own.” Moore also identified several psychological barriers that can discourage Black men from pursuing medical and science careers. These include “invisibility syndrome,”9 an emotional response to discrimination and racism “when [a student’s] sense of humanity has not been affirmed,” and the minority tax,10 or additional responsibilities placed on minorities and the expectation that these minorities represent their otherness across an institution, among others.
Moore briefly discussed the history and mission of the Bell National Resource Center on the African American Male11 at The Ohio State University, which examines and addresses issues pertaining to African American males throughout the life span. The center conducts research and produces reports on and identifies best practices regarding African American men, and serves as a resource on African American men for government agencies and colleges and universities across the country. The center also supports and fosters community among African American men at The Ohio State University, offering professional development, counseling, and positive reinforcement for achieving academic goals, as well as connecting students to research experiences, scholarships, and other opportunities.
From the center’s research, Moore identified five factors that influence the life and career development of African American men: interests, preparation, experiences, connections, and opportunity. In terms of interests, he commented that although they know how to get people interested in science, technology, engineering, and mathematics (STEM), less is known about how to sustain these interests. With regard to preparation, he emphasized that, although many discussions focus on K–12 education, preparation is needed throughout the educational pipeline. Experiences refer to the need to ensure that students “have experiences
___________________
9 For more information on invisibility syndrome, see https://www.ncbi.nlm.nih.gov/pubmed/10702848 (accessed February 28, 2018).
10 For more information on the minority tax, see Darrell Kirch’s presentation in Chapter 2. Also see https://bmcmededuc.biomedcentral.com/articles/10.1186/s12909-015-0290-9 (accessed February 21, 2018) and https://jamanetwork.com/journals/jama/fullarticle/2625322 (accessed February 21, 2018).
11 For more information on the Bell National Resource Center on the African American Male, see https://odi.osu.edu/bell-national-resource-center (accessed April 30, 2018).
that are indicative to the spaces in which they are expected to work.” Connections pertain primarily to connecting students to mentors. Finally, regarding opportunity, Moore described the need to not only offer opportunities to African American male students, but also to get them to take opportunities when offered.
AETNA HEALTH PROFESSIONS PARTNERSHIP INITIATIVE (HPPI) SCHOLARS DOCTORS PIPELINE
Marja Hurley, M.D. Professor of Medicine and Orthopedics, UConn School of Medicine Associate Dean for Health Career Opportunity Programs, UConn Health
The Department of Health Career Opportunity Programs at UConn Health administers the Aetna Health Professions Partnership Initiative (HPPI) Scholars Doctors Pipeline, a continuous pipeline of programs for students in middle school through college, as well as their parents (see Figure 5-2).12 The pipeline program seeks to develop the pool of underrepresented minority applicants to health professional schools, primarily at UConn. For the middle school and high school programs, the program partners with two public school systems, the New Britain and Hartford public school systems; for the undergraduate programs, it partners with local universities, including the UConn campuses in Storrs and Hartford, Connecticut, and Central Connecticut State University. These programs include science and nonscience academic enrichment, college and test preparation, exposure to STEM careers (e.g., clinical shadowing), research experience, mentoring, professional development, and opportunities for presentation. The Department of Health Career Opportunity Programs promotes an academically and socially supportive environment for those students who matriculate to UConn health professional schools.
Hurley provided select program outcomes. The Senior Doctors Academy offers year-round enrichment and, for qualified students, an earned stipend to high school seniors who are interested in medicine, dental medicine, or biomedical research, and who come from low-income families and/or are in the first generation in their families to attend college.13 Of 171 participants, 5 are currently enrolled in the UConn School of
___________________
12 For more information on the Aetna Health Professions Partnership Initiative (HPPI) Scholars Doctors Pipeline programs at UConn Health, see https://health.uconn.edu/hcop (accessed February 28, 2018).
13 For more information on the Senior Doctors Academy, see https://health.uconn.edu/hcop/enrichment-programs/senior-doctors-academy (accessed March 16, 2018).
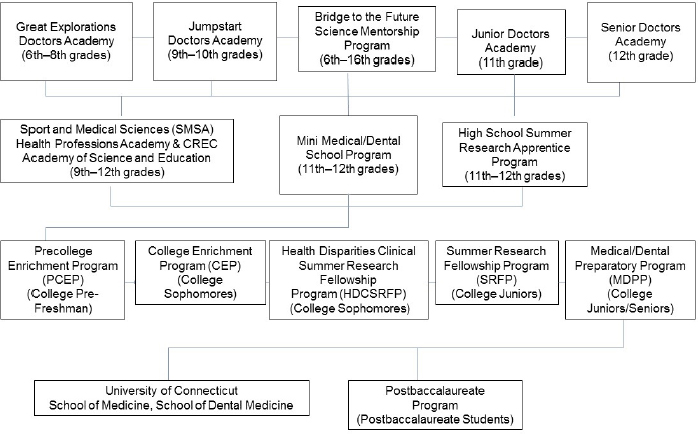
SOURCE: Presentation by Marja Hurley, November 20, 2018.
Medicine, 4 entered pharmacy school, 3 are in nursing, 6 are pursuing allied health professions, 1 is pursuing biomedical research, 1 is enrolled in dental school, and 3 are enrolled in postbaccalaureate programs. There are 70 students still enrolled in undergraduate studies, and 46 students pursued nonhealth professions. Outcomes for 31 are unknown, which includes participants who moved out of the target school districts or who withdrew or were otherwise dismissed from the program. One student is deceased. Hurley commented that sustaining program commitment for all 4 years of high school, especially among Black and Hispanic male students, is challenging.
The Health Disparities Clinical Summer Research Fellowship Program places rising college sophomores, juniors, and seniors or recent college graduates in community health centers or other organizations working with underserved populations.14 The program also requires participants to develop and present a research program related to health disparities. Of 103 participants, 31 entered medical school, 11 entered dental school, 19 entered other health professional schools (e.g., nursing, allied
___________________
14 For more information on the Health Disparities Clinical Summer Research Fellowship Program, see https://health.uconn.edu/hcop/enrichment-programs/health-disparities-clinical-summer-research-fellowship-program (accessed March 16, 2018).
health, pharmacy), 2 are enrolled in graduate programs, 7 decided they were not interested in health careers, and 33 students are still completing their undergraduate degrees. The Medical and Dental Preparatory Program and Summer Research Fellowship Program place undergraduates in a biomedical research lab and provide opportunities for clinical shadowing and presentation. Of 823 program participants from 1996 to 2017, 658 entered the health professions—349 went to medical school, 161 to dental school, 40 to graduate schools, and 109 to other health professions; 39 program graduates pursued careers not in the health professions, and 60 are still undergraduates. Overall, of 195 African American and Hispanic students who graduated from the UConn School of Medicine from 2003 to 2017, 80 participated in HPPI pipeline programs; of 84 African American and Hispanic students who graduated from the UConn School of Dentistry in the same period, 40 participated in pipeline programs.
HARVARD MEDICAL SCHOOL OFFICE FOR DIVERSITY, INCLUSION, AND COMMUNITY PARTNERSHIP
Joan Y. Reede, M.D. Dean for Diversity and Community Partnership Harvard Medical School
Reede started her presentation by pointing out,
We talk about this as though there are these children in the mental health system and children in the educational system and children in our clinics. We are talking about the same children. And when we think of solutions we need to think beyond those of us who are in the health professions; we need to think beyond those in the academy, and [think about] how do our communities come together to support our youth.
I think about our children as swimming upstream, going to schools where they are unprepared, where the schools do not have quality education, or sometimes the resources they need, where they don’t have the mentors, they don’t have the role models, they don’t have the opportunities, but we are telling them to survive.
Oftentimes when we talk about health disparities, we talk about the social determinants of health. Those same social determinants of health are impacting the youth that we’re talking about, and you cannot separate it. Those same issues of if you are hungry, if you don’t have a place to sleep, if you don’t feel safe, they impact your learning.
In addition to these social factors, Reede also identified racism, discrimination, and bias, and resulting effects such as stereotype threat, microaggressions, lack of validation, isolation and exclusion, tokenism,
and “being hypervisible and invisible at the same time” as barriers to these students’ success. She elaborated on the need to address these barriers to advancement throughout the educational pipeline at each of the junctures at which students might enter, exit, and re-enter the pipeline along the multiple paths students might follow.
Reede then described the pipeline programs of the Office for Diversity, Inclusion, and Community Partnerships at Harvard Medical School, themes across the programs, and lessons learned. Harvard programs include educational outreach to K–12 students, the Biomedical Science Careers Program, and The Commonwealth Fund Mongan Fellowships in Minority Health Policy. The educational outreach K–12 programs include in-school programming—developing curricula used in schools, teacher professional development, and working with the College Board to help teachers to teach advanced placement courses—and out-of-school programming for middle and high school students, and college students both during the academic year and during summer breaks.15
The Biomedical Science Careers Program is a partnership between internal Harvard individuals, offices, departments, and institutions, and external partners from industry (e.g., biotechnology, pharmaceutical, and medical device companies), law firms, medical schools, community colleges, and community organizations that produces conferences and symposiums. The program offers scholarships, workshops, mentoring and advising, and other resources to support students from high school through postdoctoral fellowships who wish to pursue biomedical careers. Since it was established in 1991, roughly 13,000 students, residents, and fellows have participated in the program.16 The Commonwealth Fund Mongan Fellowship is a 1-year fellowship for physicians committed to transforming health care delivery systems for vulnerable populations and is a “deliberate effort to create leaders who could create change.” Fellows complete coursework leading to a master of public health or a master of public administration degree at Harvard and participate in forums and seminars with leaders in health care delivery, public policy, and minority health.17
Reede identified the following themes across the Harvard Medical School pipeline programs: continuity, consistency, collaboration, creativ-
___________________
15 For more information on the Harvard Medical School Office of Diversity, Inclusion, and Community Partnerships programs, see https://mfdp.med.harvard.edu (accessed March 2, 2018).
16 For more information on the Biomedical Science Careers Program, see http://www.bscp.org (accessed March 2, 2018).
17 For more information on the Commonwealth Fund Mongan Fellowship in Minority Health, see http://www.commonwealthfund.org/grants-and-fellowships/fellowships/commonwealth-fund-mongan-fellowship-in-minority-health-policy (accessed March 2, 2018) and https://mfdp.med.harvard.edu/cfmf (accessed March 2, 2018).
ity, communication, consideration, and commitment. Continuity refers to continuity of efforts across academic levels, or, ensuring linkages when students bridge different educational levels (e.g., middle to high school). Consistency refers to consistent efforts over time, and not funding or implementing programs for only a few years at a time. Collaboration means not being territorial or competitive across different health professions, allowing students to choose the health career path they desire, and not expecting them to follow the choices made for them. This also includes collaboration across institutions to create a system to support students, not only within their individual schools and universities, but across schools as well. Creativity describes the capacity to be innovative in developing new programs and “not doing the same things that we have always done that did not work.” Communication pertains to communicating with students and meeting them where they are, on the platforms they are using, and not only through traditional academic channels. Consideration refers to recognition and acknowledgment of intersectionality, and people’s multiple identities. Reede commented, “There are all sorts of ways people are in the margins, and we have multiple identities” and queried how academic leaders can recognize those identities. Finally, Reede pointed out the need to identify ways to stay committed to these initiatives and this goal, as well as how to get leadership engaged and committed.
Reede closed her presentation with the following lessons learned from implementing pipeline programs:
- Set an explicit goal or sets of goals.
- Set a realistic time frame.
- Put forward a rationale for the program, and align it with the organization’s mission.
- Assess data and evaluate programs to build an evidence base of effective programs.
- Have a seamless articulation of programs.
- Create opportunities for multiple points of entry, exit, and re-entry.
- Be flexible and adjust to environmental and policy changes and to local needs.
- Engage communities.
- Cross boundaries and disciplines.
- Think in terms of multilevel and dynamic systems and connections across systems.
- Provide not just academic but also career development.
- Track, monitor, and evaluate for continuous improvement.
DISCUSSION
Wizdom Powell, Ph.D.,18 commented that the discussions of pipeline interventions to increase representation of Black boys in medical education often assume a zero-sum proposition between Black boys and Black girls—or, that increasing focus on boys and men should decrease focus on women and girls. However, she offered that this need not be the case—a focus on Black boys should not reduce efforts that have successfully led to advances and achievements among Black girls. Hrabowski expanded on these comments, saying,
We sometimes end up pitting one group against another, [but] we should be celebrating the success that some African Americans have had . . . it’s the genius of the “and” versus the tyranny of the “or.” We have to keep lifting women up, celebrating what they are doing, and get them to help us push more men to do well.
Reede concurred with Powell and cautioned against inflating the successes of Black girls and women. Despite their advances, she suggested that there is still room for improvement, saying,
I do think this idea of pitting men against women and Black men against Black women makes no kind of sense whatsoever. As we talk about Black women doing better, there are roughly 145 medical schools. There are 180 Black female full professors across [these schools], so there are only like one per medical school, and there are 12 Black female chairs. That doesn’t mean that this is not a critically important issue around our Black men, but we should make sure that we don’t depict this as though the Black women have reached nirvana, because they have not.
Camara Jones, M.D., M.P.H., Ph.D.,19 emphasized the need for structural interventions to even the playing field, which complement the individual-focused pipeline programs. She cautioned,
When we do not name those systems of structured inequity, when we do not say even the word racism, we are complicit with the widespread denial that racism continues to exist. When we don’t talk about those systems and try to address those, when people see that there are uneven outcomes, they blame this one [child] instead of thinking these are chil-
___________________
18 Powell is director of the Health Disparities Institute and associate professor of psychiatry at UConn Health.
19 Jones is senior fellow at the Satcher Health Leadership Institute at Morehouse School of Medicine.
dren with equal potential and they had different circumstances. They say this one was lazy or stupid. And we are all buying into that.
Jones identified three barriers to structural thinking. She said,
There are three huge barriers in this country that we are going to face no matter what we try to do to set it right. The first is this narrow focus on the individual that makes systems and structures either appear to be invisible or irrelevant, and it also makes us feel like what can I do as opposed to what can we do as a collective. The second is that we as a nation are ahistorical, and we act as if the current distribution of resources, advantaged, disadvantaged, is just a happenstance, and we act as if the present is disconnected from the past. The third is this myth of meritocracy. The story goes something like this. If you work hard, you will make it. . . . Now, most people who have made it have worked hard, but there are many others who are working just as hard or harder who will never make it because of this uneven playing field—racism, sexism, heterosexist, all those things that are structured and are perpetuating the uneven playing field.
Hrabowski wrapped up the discussion by identifying the important points made by the panel, in his opinion. First, he identified the need for data, analytics, and rigorous analysis to know which of these pipeline programs and which elements of these programs work. Second, he proposed a focus on undergraduate students in the near term (next few years) as “low hanging fruit.” He commented that there are undergraduate students who are interested in STEM careers, but face challenges, such as a bad grade in a science or math course early in their undergraduate careers, and this experience often discourages them from continuing their pursuit of STEM. Thus, he suggested that this pool of students could become competitive in health professions admission with relatively little support and additional preparation. Finally, he described the need to think more creatively about academic preparation, not restricting undergraduate students who wish to pursue health professions to science majors, and strengthening academic preparation through nonscience coursework.
This page intentionally left blank.














