1
A Design Thinking, Systems Approach to Well-Being
INTRODUCTION TO THE WORKSHOP
The mental health and well-being of health professionals is a topic that is “broad, exceptionally relevant, and urgent to address,” said Zohray Talib, a member of the workshop planning committee who helped lead the charge. Stress in the health professions is “so ubiquitous, it is almost inevitable.” It is both a local and a global issue, and affects professionals in all stages of their careers, said Talib. To explore this topic, the Global Forum on Innovation in Health Professional Education (the Forum) held a 1.5-day workshop, titled A Systems-Approach to Alleviating Work-Induced Stress and Improving Health, Well-Being, and Resilience of Health Professionals Within and Beyond Education.
This workshop was the result of a multiyear discussion among members of the Forum, who knew of many ongoing conversations about stress and burnout in virtually all of the health professions, and in many parts of the world. These forum members, said Talib, wanted to find a unique value the Forum could bring to this conversation. The group—who also assisted with the planning of the workshop—identified several ways the Forum could contribute and further the conversation. First, the Forum brought together participants from more than 19 different health professions, and, as such, “the inter-disciplinary aspect makes this conversation particularly unique,” said Talib. Second is the leadership perspective, as most of the participants on the Forum and at the workshop are leaders in the health professions field, in both education and practice. Finally, said Talib, the Forum chose to look at stress, burnout, and well-being from a systems level,
rather than emphasizing individual actions or programs that are aimed at well-being. To better understand the issues and to guide the structure of the workshop, individual members of the planning committee reached out to more than 40 leaders in both the health and education sectors to hear about the challenges and successes they have experienced in their time as leaders. A synopsis of these conversations is found in Appendix C of this report.
The planning committee gleaned several insights from these conversations with leaders that built on personal experiences. First, whether health professionals are working in an urban hospital in the United States or a rural health clinic in the mountains of Tajikistan, stress and burnout are ubiquitous. Second, even in disparate settings with varying resources, the issues faced by health professionals around the world are similar, including financial stresses, problems with infrastructure, moral stress and compassion fatigue, and difficulties with power and hierarchy among professionals. Talib noted the different manifestations these stressors display depending upon the context. Most urgently, said Talib, is the need to address health professional well-being because of the significant effects it has throughout the system. Stress and burnout of the workforce affect patient outcomes and patient experiences. Well-being affects workforce turnover, which can affect quality of care. Finally, health professional well-being affects the financial bottom line of health systems; these effects are important to acknowledge as they “often drive change,” concluded Talib.
Talib walked participants through the objectives and the structure of the workshop (see Box 1-1 for the Statement of Task). She described the goal of the workshop as providing participants with “seeds of different examples of how others have addressed this issue,” with the hope that participants will return to their own systems with fresh ideas and perspectives on making changes. The workshop focus, said Talib, is on a design thinking, systems approach that is human centered, while also considering how all the pieces of a system work together. Talib emphasized that the workshop “is not the beginning and the end” but rather an inflection point for participants to reflect, continue the conversation, and drive progress forward.
DESIGN THINKING, SYSTEMS APPROACH
Mary Jo Kreitzer, a member of the planning committee who worked with Talib in setting the foundation for the workshop, is also the founder and director of the Earl E. Bakken Center for Spirituality and Healing at the University of Minnesota. Kreitzer introduced the workshop participants to the concept of a “design thinking, systems approach.” This concept is a combination of two different perspectives on making change: a systems thinking approach and design thinking approach. A systems approach, said Kreitzer, looks at problems and potential solutions through the lens of
the entire system (see Box 1-2 for components of a systems approach). A change in one part of the system can have dramatic effects on other parts of the system—for better or for worse. This is why it is important to look at each component of the system and how one profession or work unit interacts with other parts of the system so an intervention in one part of an organization does not negatively affect other parts, Kreitzer continued.
By identifying the root causes of problems, and teasing out dynamics that could be shifted, organizations can avoid or minimize the potential for unintended consequences. To illustrate this idea, Kreitzer gave the example of a health system that is suffering from a high degree of burnout among its staff. One of the factors causing burnout may be the stress of perpetually working with not enough staff, possibly because of budgetary constraints or because of a high staff turnover rate. High turnover rates have a variety of root causes that include a failure of leadership, stressful work environ-
ments, or a lack of financial and other resources, said Kreitzer. There will no doubt be other reasons specific to a single organization that should be fully explored, but it is the thought process that Kreitzer emphasized. Change agents should investigate potential causes of burnout until all of the factors leading to burnout within the organization are understood. Kreitzer said that one benefit of this systems approach is that “unless you really know what the problem is, it is so easy to throw solutions that may or may not have an impact.”
Design thinking, continued Kreitzer, is a specific and thoughtful process for identifying the problems within a system and for developing potential solutions. It is “based on the simple yet radical idea that the people who face the problem every day are most likely the ones who hold the keys to the solutions.” Kreitzer noted that the process for identifying problems and solutions often entails “getting smart people together in a room” to discuss the issue and to impose a top-down solution. By contrast, design thinkers work with multiple stakeholders who actively engage in identifying the problems and remedies so the resulting solutions are the product of a collaborative, thoughtful, and iterative effort from various perspectives.
As described by Tim Brown (2009), design thinking encompasses three aspects: desirability, feasibility, and viability. The goal of desirability is to fully understand the problems within the organization by asking what people are “hearing and seeing and feeling and thinking.” This process of identifying the “deeply felt needs” of various stakeholders is sometimes referred to as human-centered design or empathy, said Kreitzer. The second aspect—feasibility—requires stakeholders and planners to look at what is possible in the organization in terms of existing and potential capacity, human resources, processes, and technology. Finally, the third aspect is vi-
ability, which requires considering how a change can be implemented and sustained over time. Kreitzer said that it is critical to think about how an initiative can be “hardwired into the organization” so it has a higher likelihood of continuing long past the point of implementation.
Desirability, feasibility, and viability describe the issues to be discussed during a design thinking process. The process itself, said Kreitzer, can be described in the three phases of inspiration, ideation, and implementation. In the inspiration phase, perspectives from all stakeholders are gathered through methods including literature searches, individual and group interviews, listening, observation, and shadowing. In the ideation phase, stakeholders brainstorm and discuss potential solutions, preferably in a creative and welcoming environment. Once ideas are identified, they can be implemented in order to test prototypes. Rather than trying to perfect an idea before implementation, design thinking uses an iterative process of testing and refining in order to find a solution that works for all stakeholders.
During the course of the workshop, said Kreitzer, participants will hear about individual and organizational strategies that have been used to address health professional well-being in various settings. She urged participants to keep both the systems approach and the design thinking process in mind while listening to these presentations. Participants should listen for ways in which small changes affected entire organizations, she said, and ways in which stakeholders were engaged and active in the process of problem solving. Kreitzer introduced the speakers for the first session—Tim van de Grift and Pinar Keskinocak—who presented case studies of projects that used aspects of design thinking or a systems approach in both education and practice.
CASE STUDIES: APPLYING DESIGN THINKING AND SYSTEMS APPROACHES
Design Thinking as a Tool for Interdisciplinary Education in Health Care
Tim C. van de Grift, Vrije Universiteit (VU)
University Medical Center Amsterdam
van de Grift, psychiatry resident at the Vrije Universiteit (VU) University Medical Center Amsterdam, talked about his experiences in applying design thinking as a tool for interprofessional education in health care. He called attention to the rapidly changing health care environment where health professionals and educators are expected to adapt to these changes while keeping up with the ever-increasing influx of new knowledge. These transformations and pressures create an environment of uncertainty and stress. Design thinking is useful in this context, said van de Grift, because
it teaches people how they can influence and change their environment. Quoting Buckminster Fuller, he said “The best way to predict the future is to design it” (Bruton, 2012). The same is true for an environment—the best way to fix an unproductive workplace is to be actively involved in redesigning it. van de Grift emphasized points made earlier by Kreitzer that design thinking requires collaboration, empathy, creativity, agency, and problem solving. He defined design thinking as “a method to structurally assess situations, to reduce the uncertainty, and to work towards a certain focus, design prototypes, and finally design specific solutions.”
At the University of Amsterdam, van de Grift and his colleagues developed a 6-month course on design thinking called “Hacking Healthcare” (van de Grift and Kroeze, 2016). Medical and psychology students were teamed up with art students and asked to design solutions for health care providers, using the “inspiration, ideation, implementation” approach (see Figure 1-1). While Figure 1-1 presents the three phases as linear, van de Grift noted, it is an iterative process in which ideas are continually tested against stakeholder perspectives and refined.
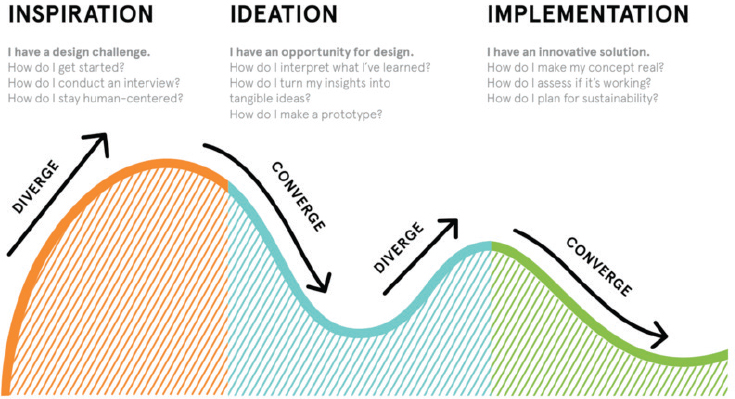
SOURCE: Presented by van de Grift, April 26, 2018. Used with permission from IDEO.org.
Inspiration
The inspiration phase, said van de Grift, focuses on getting a problem statement and a user profile: what is the core problem that needs to be addressed, and who is the end user of the design? For this phase, it is critical that students gather as much information as possible about as many stakeholders as possible. One interesting method for doing so, said van de Grift, is participatory research such as shadowing patients during their hospital stay. This type of research gives students insight on the patient experience and may spark ideas of how to improve. However, van de Grift noted that one pitfall of the observation process is that sometimes researchers only see what they are expecting to see. Another potential problem in this phase is involving only the most accessible stakeholders; van de Grift stated the importance of engaging stakeholders who are more skeptical of the process or from lower resource environments. After researchers have made conclusions based on the initial information gathered during this phase, it is critical they return to the stakeholders in order to ensure they have correctly interpreted the information and made appropriate conclusions.
As an example of the research performed by students at the University of Amsterdam, van de Grift described the efforts of students who had been tasked with designing a more humane psychiatric ward. The students stayed overnight at the ward, went to a museum, took surveys, conducted interviews, and talked with staff and patients about how they would design the space. From all of their research, the students discovered it was the way the ward was designed that prevented a more patient-centered focus. This realization led to a spatial redesign that included a working station and coffee bar to promote more informal interactions between staff and patients (see Figure 1-2).
Ideation
The phase of ideation is about generating solutions to a specific problem, said van de Grift. He recommended that “really low resource” methods be used for this phase—papers, cardboard, sticky notes—in order to get “quick and rough” kinds of ideas. It is important to “go wild” during this phase, van de Grift said, and to not let issues of feasibility get in the way of generating ideas. Once some solutions are identified, it is essential to go back to the stakeholders to get their feedback and to incorporate their advice into the next round of ideation. If planners try to finalize ideas before they get feedback from stakeholders, emphasized van de Grift, it makes it less likely that stakeholders will give their honest opinions.
As an example of the ideation phase, van de Grift shared his students’ work at a home for dementia patients. The students had already identified a
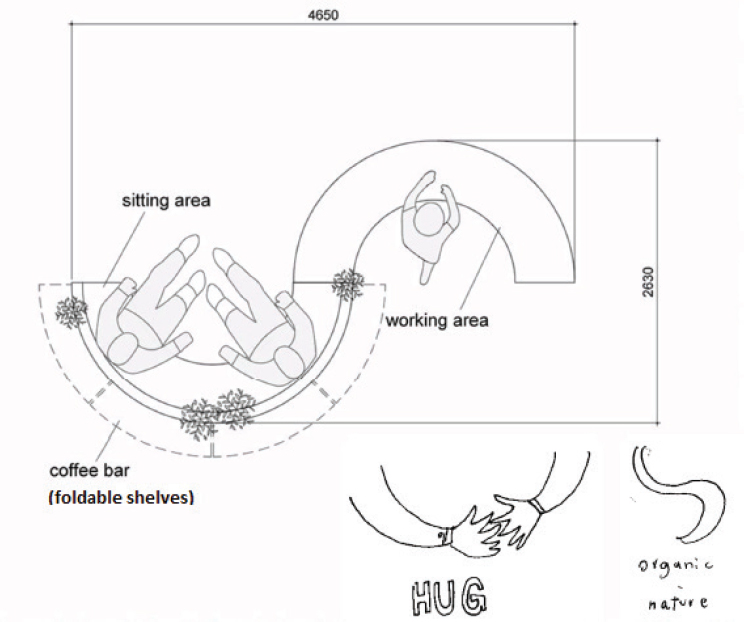
SOURCE: Presented by van de Grift, April 26, 2018.
problem: the home did a good job of welcoming people to the community, but it did not have a space or rituals for patients to discuss loss of their own identity or loss of other patients. To begin the problem-solving process, students and patients gathered together to discuss ideas while also making art with clay; this art project provided patients who struggled with expressing themselves verbally with another outlet for sharing their ideas. The solution, developed by patients, was to have a plate-drawing workshop, where each patient would represent their own identity on a plate. Once per week, the patients would use the plates during lunch and discuss their losses.
Implementation
No matter how carefully planned a solution is, it cannot be put into place and sustained without a thought-out implementation plan, said van de Grift. An implementation plan can resemble a business plan, with the
costs and revenues at each step of implementation laid out. An alternative way of presenting an implementation plan is through a “user journey,” where each step of using the new product or system is laid out from the perspective of the user. The format of an implementation plan will vary depending on the context of the organization. For example, some organizations may require a large evidence base before implementing a program, while other organizations may require a detailed cost analysis.
In conclusion, van de Grift said the design thinking process provides a structure for interdisciplinary and interprofessional partners and stakeholders to collaborate on solving problems, and it does so while giving stakeholders agency and the ability to influence their own environment.
In response to van de Grift’s presentation, workshop participants shared their own experiences with stakeholder-based problem solving. Susan Scrimshaw, a forum member, shared a story about her work in health clinics in Panama. To get perspectives from all stakeholders in the clinics, the clinic staff came together in a circle and performed role-plays of problematic interactions. For example, staff acted out examples of rudeness to a patient, or of a staff member being condescending to another staff member. Scrimshaw said that this exercise was useful in two ways. First, it treated all the staff members—from janitors to doctors—as equals; and second, it allowed people to put themselves in others’ shoes and empathize with their experiences.
Brenda Zierler, a forum member, told participants about her experience using an approach similar to design thinking in combination with “liberating structures,” a framework for facilitating conversations in order to get everyone engaged (Center for Health Sciences Interprofessional Education Research and Practice, 2017). A heart failure care team was experiencing challenges with communication, nurse retention, staff turnover, and patient satisfaction that resulted in poor outcomes overall. Zierler’s team brought the staff together to talk about how they communicated and worked together, and how improvements could be made. Zierler said that while her team “had lots of ideas of how they could improve,” it was essential that the ideas come directly from the staff. One technique they used to gather ideas was to have everyone write down their “boldest idea” for improving the function of the team, and then cards were passed around and read anonymously. Another approach Zierler used with the group was something she called “What I need from you.” In this exercise, representatives from each area present—including medicine, nursing, patients, and social work—each thought about what they could ask of the other professions to make things work better. For example, the nurses asked the physicians to show up at the same time every day before rounds. The physician representative discussed this idea with the other physicians, figured out whether it was possible and
what changes would need to be made, then returned to the nurses with an answer that was either yes, no, or we will try.
Systems Engineering to Reduce Stress and Burnout in Health Systems
Pinar Keskinocak, Georgia Institute of Technology
Keskinocak, William W. George Chair and professor in the Stewart School of Industrial Engineering at the Georgia Institute of Technology, and director of the Center for Health and Humanitarian Systems, spoke about using a systems approach to improve the well-being of health professionals. First, Keskinocak emphasized the complexity of health systems: there are multiple stakeholders, different types of physical spaces, limited resources, objectives and incentives that are sometimes misaligned, and uncertainty around patients’ arrival times to their appointments, surgery durations, staff availability, and the volume and types of patients arriving at an emergency department. Partly because of the complexity of the system, there are a number of factors that contribute to stress and burnout among health professionals:
- Work demands and pressures not matched to knowledge, abilities, and needs
- Insufficient support from supervisors and colleagues
- Little control over work processes
- Unsatisfactory working conditions, such as workload, pace, and hours
- Culture of the work environment
- Poor design or management of the system
These factors can affect mental and physical health, absenteeism, turnover rates, errors, and patient outcomes, said Keskinocak. Initiatives to improve the well-being of health professionals have largely focused on supporting individuals—for example, mindfulness training, support groups, and skills training. Initiatives that focus on changing the system are much less common, but they have the potential to be more effective. Examples of system-level interventions include changes to policies or programs, redesigning processes or workflows, changing incentive structures, reworking protocols, and improving scheduling. Making a change at the system level, and more importantly, carefully evaluating the effect of a change in one part of the system, not only locally but on the entire system, has the potential to create a work environment that facilitates wellness, rather than exacerbate stress. Keskinocak used a quote by Mark Greenawald to elucidate the fact that while individual-level changes may be beneficial,
they can only have so much effect without systems-level changes: “You can teach physicians mindfulness and meditation techniques, but if you throw them back to the war zone it’s not going to work” (U.S. News & World Report, 2016).
A Systems Engineering Approach
Keskinocak laid out a systems engineering approach for improving the well-being of health professionals and the functioning of health organizations.1 There are three steps for assessing the current state of the situation, she said. First, one should start by identifying the symptoms—where are the problems and who is affected by these problems? Second, the magnitude of the problem should be measured or quantified to the extent possible. Third, any and all potential root causes of the problems should be identified, as well as possible bottlenecks that could exacerbate an already crowded system. She emphasized that sometimes the root may lie elsewhere in the system, not necessarily where the symptoms are observed, and hence, a careful evaluation of the entire system is needed.
After these three steps are completed, a road map toward an improved state can then be built with interventions that are designed to improve the system. Part of the road map should include an assessment of potential effects of the interventions in various parts of the system and the stakeholders, such as how the interventions will affect the cost of care, quality of care, and access to care. Keskinocak emphasized the importance of developing solutions that are based on an understanding of what the stakeholders view as helpful or valuable. Finally, once a plan is implemented, it is important to evaluate the actual effect of the changes made, and circle back for future improvements. Evaluation is critical for addressing unforeseen consequences, scaling up a program, and adding to the knowledge base of what does and does not work.
With this systems approach in mind, Keskinocak told workshop participants about four different initiatives that made broad modifications directed at changing the environment, rather than individuals. One was designed specifically to reduce clinician burnout. It resulted in a drop in burnout rates from 53 percent to 13 percent, along with a rise in productivity, making this a cost neutral program (Wright and Katz, 2018). The second was a pilot project that used outside funding to offer incentives to those who engaged in activities that typically go unrecognized, such as mentoring, serving on committees, and filling shifts for colleagues who need support. Those who received the rewards—including time for academic pursuits or
___________________
1 See Chapter 3 for a description of systems engineering application through a breakout group discussion.
home assistance like house cleaning and meal delivery—felt a greater sense of support. There was also less turnover in that department.
Keskinocak’s third example of an initiative drew from the Carilion Clinic, a large health system in Virginia with 7 hospitals, 1 medical school, 240 health care facilities, and more than 12,000 employees. A survey of the health workers uncovered high rates of burnout among members of their staff: 59 percent of physicians, 65 percent of residents in specialty training, and 50 percent of medical students, physician assistants, and nurse practitioners (AMA Wire, 2018). By identifying and correcting inefficiencies in the system, clinicians found they had more time to spend with patients. These adjustments improved patient and clinician satisfaction.
The fourth and final initiative Keskinocak described looked at workflow in a new pediatric intensive care unit (PICU). Keskinocak explained that processes used in the old PICU did not translate well to the new space. To address these workflow issues, Keskinocak and her colleagues mapped the current state of the rounding process to better understand individuals’ movements in the system and where there were identified opportunities for change. There was substantial stakeholder involvement in the entire process; nurses, patients, families, and physicians provided feedback about the current situation and ideas about how to improve coordination. The rounding process was streamlined by implementing standardized routines, reducing variation and waste at each step, and focusing on the essential components (Vats et al., 2012). One change that was particularly interesting from a systems perspective, said Keskinocak, revolved around how radiology rounds were done. Originally, the providers would go to a different floor to view images and then return to patient rooms. However, available technology meant that images could be viewed in patients’ rooms. Making this change allowed providers to discuss images with patients and save time traveling to a different floor.
REFERENCES
AMA (American Medical Association) Wire. 2018. Alarming survey results spark 7 system changes to buck burnout. https://wire.ama-assn.org/practice-management/alarmingsurvey-results-spark-7-system-changes-buck-burnout (accessed June 20, 2018).
Brown, T. 2009. Change by design: How design thinking transforms organizations and inspires innovation. New York: HarperCollins.
Bruton, D. 2012. Design education and institutional transformation. In Computational design methods and technologies: Applications in CAD, CAM and CAE education, edited by N. Gu. Hershey, PA: IGI Global. Pp. 351–364.
Center for Health Sciences Interprofessional Education Research and Practice. 2017. Heart failure teams transforming relationships. https://collaborate.uw.edu/2017/02/2747 (accessed June 20, 2018).
IDEO.org. n.d. Our approach. https://www.ideo.org/approach (accessed July 5, 2018).
U.S. News & World Report. 2016. Diagnosis: Burnout. https://www.usnews.com/news/articles/2016-09-08/doctors-battle-burnout-to-save-themselves-and-their-patients (accessed June 29, 2018).
van de Grift, T. C., and R. Kroeze. 2016. Design thinking as a tool for interdisciplinary education in health care. Academic Medicine 91(9):1234–1238.
Vats, A., K. H Goin, M. Villarreal, T. Yilmaz Gozbasi, J. Fortenberry, and P. Keskinocak. 2012. The impact of a lean rounding process in a pediatric intensive care unit. Critical Care Medicine. 40(2):608–617.
Wright, A. A., and I. T. Katz. 2018. Beyond burnout—redesigning care to restore meaning and sanity for physicians. New England Journal of Medicine 378(4):309–311.
This page intentionally left blank.














