4
Leadership in Organizational Resilience
ORGANIZATIONAL RESILIENCE
David Ballard, American Psychological Association
“Over the past day of the workshop,” said Ballard from the Center for Organizational Excellence at the American Psychological Association (APA), “many topics came up related to organizational resilience.” These include well-being, stress, meaningfulness of work, mindfulness, a climate that is supportive of employees, and self-care. The audience also heard about a variety of pathways to healthy, resilient organizations, he said, before asserting that there is “not a cookie cutter approach.” Organizations must customize their methods and initiatives to meet their own unique organizational circumstances and employees. That said, a common thread that is or should be across all approaches is human centeredness and a focus on human behavior, he added. This is “psychology’s area of expertise.” The Center for Organizational Excellence “works to enhance the functioning of individuals, groups, organizations, and communities through the application of psychology to a wide range of workplace issues.” The center, said Ballard, does this by creating healthy, resilient environments based on the knowledge and research from psychology. Often what they find, he said, is that implementation of evidence-based programs are necessary but not sufficient for change because underlying psychological factors are not addressed along with the program.
Ballard discussed the concept of resilience, and the importance of defining and measuring resilience in order to improve it. Resilience is a term that is used often but there is a “lack of conceptual clarity around it.” A 2011
article found 104 different definitions of resilience in the literature (Sinclair and Britt, 2013). At times, resilience is described as a trait, other times, as a state of being, and still additional authors refer to resilience as a skill set that can be developed. Organizations looking to increase their resilience, said Ballard, need a way to measure resilience so they know if their initiatives are effective. The operational definition of resilience also matters as organizations work with employees not simply to “buffer themselves from the stressors” but to help people bounce back from the stressors they face. Ballard said there is no single answer to how to define resilience, and each organization must decide how to approach their employees within the context and goals of their unique situation.
One definition that is often used, said Ballard, is “demonstration of positive adaptation in the face of significant adversity” (Britt et al., 2013). However, this definition does not apply particularly well to organizational resilience, because most organizations do not face “significant adversity” on a regular basis, and thus changes to resilience cannot be measured. For most organizations, the discussion about resilience relates to day-to-day, low-level work stressors such as overload of responsibilities, lack of clarity around roles, inappropriate expectations, and interpersonal conflict. For these organizations, Ballard said, McEwen’s definition of resilience is useful: “The capacity to manage the everyday stress of work while staying healthy, adapting and learning from setbacks and preparing for future challenges proactively” (McEwen, 2018).
APA surveys the U.S. workforce to measure attitudes, opinions, and work experience. Part of this survey looks at resilience using the Brief Resilience Scale, which asks people to rate themselves on six statements (Smith et al., 2008):
- I tend to bounce back quickly after hard times.
- It does not take me long to recover from a stressful event.
- I usually come through difficult times with little trouble.
- I have a hard time making it through stressful events.
- It is hard for me to snap back when something bad happens.
- I tend to take a long time to get over setbacks in my life.
APA’s survey revealed that about 15–20 percent of workers have a difficult time getting back to normal after a stressful event. While this is a relatively small number, said Ballard, it can have a significant effect on an organization. A worker’s lack of resilience is likely to affect not only his own performance but also the functioning and well-being of his colleagues and team.
In dealing with stress and mental health, many organizations put the emphasis on individual-level interventions, said Ballard. For example, or-
ganizations may provide stress management training, brown bag meetings, employee assistance programs, and other interventions designed to help individuals cope with stress. These programs are helpful, said Ballard, but without addressing systems-level issues, they can be a “colossal waste of resources.” Systems-level interventions include initiatives such as aligning hiring and selection practices to the realities of the job, allowing autonomy and control in the workplace, and providing a predictable and healthy environment. When organizations take on the shared responsibility for employees’ mental health by creating a supportive environment, they create a culture in which employees can thrive and do their best work.
In addition, said Ballard, a positive work environment makes employees feel they are being treated fairly by their employer, which has far-reaching implications. Ballard explained that when employees do not feel they are treated equitably, they are less motivated to do their best, are less satisfied with their job, experience greater chronic work stress, are more cynical and negative at work, and are more likely to want to leave their job. Clearly, these consequences affect not just the employee but the entire organization. Similar consequences are seen in employees who do not trust their employer or who do not feel valued by their employer.
Another factor that greatly affects the well-being of employees is support from senior leaders in the organization. “We hear all the time that senior leadership support is important,” said Ballard, but “we have never seen data that actually demonstrate it, so we wanted to measure it” to see if it is true. To measure the importance of leadership, APA looked at the differences between employees who said their leaders supported the climate of well-being, compared to those who said their leaders were not supportive. On every measure, supported employees showed more resilience, well-being, and a likelihood to engage in wellness activities. For example:
- Eighty-six percent of supported employees feel valued, compared to 12 percent of nonsupported employees.
- Ninety-one percent of supported employees feel motivated at their jobs, compared to 38 percent of nonsupported employees.
- Fifty-five percent of supported employees regularly participate in health and wellness efforts, compared to 18 percent of nonsupported employees.
- Seventy-three percent of supported employees believe the organization helps employees develop a healthy lifestyle, compared to 11 percent of nonsupported employees (APA, 2016).
Ballard underscored the importance of these data showing that when senior leaders are supportive of building a positive and healthy work environment, outcomes are “better across the board.”
APA has developed a psychologically healthy workplace model (see Figure 4-1). It is not about individual programs or policies, said Ballard, but about “the collection of activities” in which organizations engage. Health promotion and wellness efforts are part of a psychologically healthy workplace, but these efforts interact with and work in tandem with growth and development opportunities, work–life balance, the opportunities to be involved and recognized in the workplace, and good communication. Employee well-being and organizational functioning are affected by these factors that also affect each other, said Ballard. An employee who works at a better functioning, healthier organization is going to have a greater sense of well-being and a more stable mental state, and in turn, healthy employees contribute more to a well-functioning organization.
LEADERSHIP FOR HEALTH AND WELLNESS
Ballard’s presentation emphasized the importance of supportive leadership for health and wellness in the workplace, employee well-being, organizational performance, and organizational resilience. His remarks opened the door for Elizabeth Goldblatt from the Academic Collaborative for Integrative Health, who oversaw the next session. In this session, Forum members and organizational leaders interviewed each other
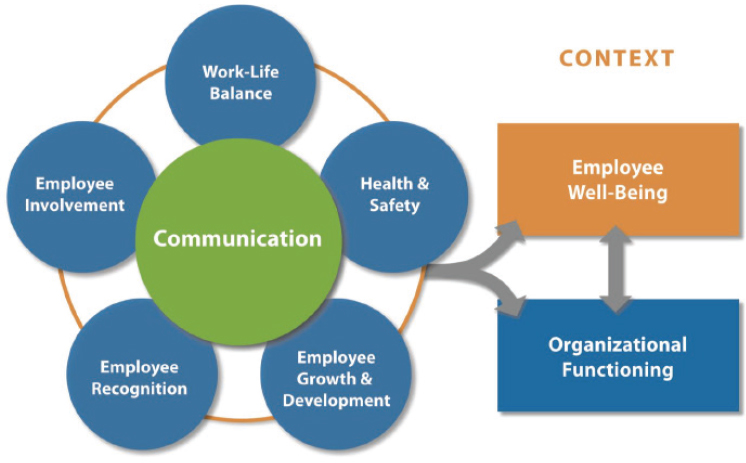
SOURCES: Presented by Ballard, April 19, 2018; APA, 2016. Reprinted with permission from APA.
about the varied ways in which they support their employees and how they themselves cope with the stress of working in what Goldblatt called today’s “do more with less” model of care. The interviews uncovered insights from leaders as architects of an optimal system, as role models for wellness practice, as models of vulnerability, and as collaborators with other leaders.
Tracy Gaudet, Interviewed by John Weeks
Tracy Gaudet is currently the executive director of the Office of Patient-Centered Care and Cultural Transformation with the U.S. Department of Veterans Affairs (VA), but has long been engaged in the movement toward a focus on Whole Health. She spent 20 years working in integrative medicine at the University of Arizona and at Duke University. Gaudet responded to Weeks’s opening of the interview by describing her work within the office she directs as caring for the entire person through a Whole Health lens. Whole Health, she explained, is about designing health care by asking: “If health care were truly about helping people to live their fullest life … what would it look like?” Gaudet said that designing health care in this way is “not just adding a little fluff around the corners,” but about fundamentally changing how health care works. There is an enormous amount of enthusiasm and momentum for this transformation, she said, and it is “largely because the health care professionals and the employees want and need this.” While disease care is still important, she acknowledged, this transformation is about rewiring the system so all aspects of health and well-being are at the center, rather than solely focusing on disease.
She noted that because the VA has always been a multifaceted agency for veterans—for example, providing resources for education and housing—the VA is particularly receptive to adopting this model. In addition, the structure of the VA allows for a great deal of learning about how to implement a Whole Health perspective. Gaudet said that because the VA can study outcomes, costs, and use within its system, it will be able to demonstrate the cost-utility of shifting to a Whole Health model for the private sector.
Leaders as Role Models
John Weeks, a planning committee member, asked Gaudet what she does to maintain her own health and well-being. Gaudet described the core of her self-care is to just “sit on a pillow and breathe.” This practice of meditation allows her to let go of the daily stress, and to focus on breathing rather than chasing happiness, she said. Recently, Gaudet has been centering her meditation on one thought: “What if nothing is wrong?”
In addition to practices such as meditation that can help individuals cope with some types of stress, cultural change within the workplace has the potential of changing the well-being of an organization. Weeks asked Gaudet to discuss one specific action she has taken to change the work culture at the VA. Gaudet said advances in technology have created an expectation that people will be available 24 hours per day. She takes pains to lower this expectation within her team by telling them she does not want to see emails coming in after hours or in the middle of the night. She also tries to model this expectation. Gaudet noted that sometimes it is necessary for her to write emails on the weekend, but instead of sending them immediately, she saves them as drafts to be sent on Monday. Workshop participants shared more ideas for culture change, which appear in Chapter 5.
As a leader, said Gaudet, it is critically important that she model behaviors and practices that contribute to well-being for several reasons. First, employees are likely to see the work practices of leaders as expectations and strive to meet those expectations. To illustrate her point, Gaudet reiterated the example of leaders who are connected to email 24/7; they set a bar for employees who assume they too must always be ready to respond to their supervisor or colleagues at any hour of the day. Second, leaders can show that well-being is a journey, rather than an end. Gaudet said a “greater gift” to people is showing how to engage in self-care without dictating specific goals. Third, leaders should seek ways to “bake” well-being into the day-to-day practices of the organization. Exposing people to mindfulness and other wellness practices is helpful, said Gaudet, but they are unlikely to use them until they have personal firsthand experience. Gaudet said that she makes an effort to incorporate well-being practices into the workday. She offered personal suggestions from her workplace including starting every meeting with a moment of mindfulness, encouraging random acts of kindness, and having “gratefulness rounds.” The fourth and final modeling of behavior, said Gaudet, is for leaders to help people reflect on their well-being and on practices that promote well-being. She added that when people reflect on how a practice affected their work, they “begin to see the benefits—the personal benefits and the professional benefits—and it begins to shift the culture.”
Gaudet described shifting the culture of well-being at work as similar to rewiring the entire health care system. Instead of focusing on fixing what is wrong, the focus needs to be on proactively cultivating well-being and health. When people find a sense of purpose, and build their life and practices around working toward that purpose, “everything flips,” she said before offering her final thought. Many people focus on innovating and developing new tools and programs, but innovation is not the only answer she cautioned, instead, “We need to do it, to model it, and to put our oomph behind it.”
Jason Eliot, Interviewed by Kathrin Eliot
Kathrin Eliot, a forum member, interviewed Jason Eliot, who is the chief experience and talent officer at INTEGRIS Health, the largest provider of health care in Oklahoma. Within INTEGRIS Health, J. Eliot is responsible for human resources, clinical education, and community benefit initiatives, and he has sought to find ways of managing and reducing the stress experienced by both employees and leaders within their system. He described taking a “consumer experience” perspective in everything he does. This entails working to find a level of common experience for patients in the INTEGRIS system, which consists of 10 hospitals, 500 physicians, and 10,000 employees. The consumer experience perspective blends nicely with the human resource perspective, said J. Eliot, because creating a consistent culture of well-being across the system benefits patients, providers, and staff alike.
Consumer-Focused Systems Approach
J. Eliot described how he came to use a systems model to address wellbeing within INTEGRIS. The organization wanted to improve well-being, not just for physicians, but for all providers, clinicians, and staff, he said, because the patients’ experience is affected by everyone they come in contact with. One of the challenges INTEGRIS faced involved different disciplines focusing on different aspects of practice. Each discipline had its own causes of stress and burnout leading to siloed solutions, rather than looking at how to design the entire system so it would function better. J. Eliot compared the process to the advent of the iPhone. Before the iPhone, said J. Eliot, companies worked in siloes so one company made the very best camera, one made the best calculator, and one made the best phone. Steve Jobs stepped in and said, “No, what you really want to be making is this.” Pointing to his iPhone, J. Eliot continued by saying, this “is all of those in one.” J. Eliot used this example with employees from across his organization to get them to see the value in designing an entire system that would support the patient at the center, rather than optimizing each individual piece.
Another challenge J. Eliot encountered was resistance from providers when he talked about the importance of the consumer experience in health care. “We are not serving hamburgers, we are saving lives,” they
said to J. Eliot. To counter this attitude, J. Eliot compared a patient’s experience in a hospital to a traveler’s experience on a plane. On a plane, he said, travelers’ lives are at risk. However, when they get off the plane, they do not thank the pilot for saving their lives. Rather, they compare and choose travel experiences based on the hospitality, food, and general experience. Similarly, patients are now choosing health care based on their overall experience in the health care setting, not on the skills and training and competency of the providers. This can be difficult for providers to understand, said J. Eliot.
Decompression
K. Eliot noted that J. Eliot focused a lot on other people’s well-being in his work, and she asked him to reflect on how he takes care of himself and ensures that he does not get burned out. Like many leaders in the health professions, he responded by describing individual coping mechanisms. “I recently bought 12 acres of land,” he said, so he can spend his days off “fixing fences and chain sawing the trees and feeding the goats.” He admitted that some might not consider manual labor fun, but for him it “feeds [his] soul” and will “extend his work life” because it allows him to relax and recharge. J. Eliot remarked that well-being initiatives often focus on happiness at work, but that relaxation outside of work is equally important. His organization did a survey about employee resiliency, and asked questions about “activation” and “decompression.” Activation questions centered around whether people were happy at work and were passionate about what they did. Decompression questions, on the other hand, looked at whether people could “check out” when they were done with work.
The survey showed that INTEGRIS employees scored high on activation, but that “decompression is where we failed as an organization.” For example, even when employees were off the clock, they were receiving phone calls asking them to cover another shift. J. Eliot said that leaders need to model decompression that would encourage and enable their employees to follow their lead. Self-care—whether it is running, tending goats, or meditating—needs to be a primary focus for leaders. “A leader cannot expect, nor provide, a safe environment for their teams, unless they are at a place where they are at least aware of themselves and at least making steps toward” well-being, he concluded.
Angelo McClain, Interviewed by Sandra Crewe
Sandra Crewe, dean of the Howard University School of Social Work, interviewed Angelo McClain, a forum member and the CEO of the National Association of Social Workers (NASW). Previously, McClain served
for 6 years as the commissioner of the Massachusetts Department of Children and Families, working on issues of abuse and neglect of the state’s most vulnerable children. Crewe interviewed McClain about the stressors of social work in today’s culture, as well as the stressors of working within a system as a person of color. Crewe started by noting that social workers are exposed to stress through work with individuals, groups, organizations, and communities, and even sometimes from questions from family and acquaintances. Through this work, social workers bear the stress of others, experiencing “vicarious trauma, historical trauma, secondary traumatic stress, compassion fatigue, and burnout,” said Crewe.
Systems Perspective
Crewe asked McClain for his thoughts on how to improve the health and well-being of the social services workforce, given the pressures and stressors they face. McClain responded that when he became commissioner in Massachusetts, there was a heavy focus on social worker safety—workers were being threatened and assaulted during the course of their work. However, it soon became clear that a broader approach was needed to improve the general wellness of social workers. By looking at wellness from a systems perspective, said McClain, there were obvious links between the wellness of social workers and the wellness of the families and children they served. He explained:
In order for the children to be protected and nurtured, we need to take care of the families. In order for the families to do what they need to do, the social workers need to treat them right. In order for the workers to treat the families right, the supervisors need to treat them right.
McClain noted how this chain of effects goes all the way to the top levels of leadership. The way the commissioner is treated by the governor, he said, can trickle down and affect the well-being of everyone in the system.
Resilience and Vulnerability
Crewe asked the audience to suggest some definitions for resilience. Resilience, she said, is a term that is commonly used but not well-defined. Workshop participants offered definitions, including
- Honoring our past, being fully present in the moment, and being able to visualize the future
- The ability to not only bounce back from challenges, but to grow stronger from these challenges
- To bend, but not break, and bounce back
Crewe said that while resilience is often viewed as a positive attribute, there can be negative effects if health professionals and others “over-rely on resilience as an intervention, and assume that the person will bounce back.” She said that, particularly in social work, there is a tendency to assume that people’s professional training will enable them to endure any hardship or stress. When an employer relies on resilience, the employer misses an opportunity to help employees through difficult situations and prevent stress and burnout, said Crewe. In opening the conversation to others, J. Eliot underscored the importance of her last thought adding that it is important to not make resilience another burden on employees. People already are dealing with enough stress and overwork, he asserted. Another workshop participant, Simon Fleming, also shared his perspective in disliking the term resilience. “It implies that people should be able to cope with difficulty,” he said, even in the face of the “ongoing relentless never-ending difficulty” of some health care workplaces.
Fleming’s comment resonated with J. Eliot who thought that instead of focusing on resiliency, leaders could focus on restructuring the system so resiliency is only needed in extraordinary circumstances, rather than used as a day-to-day coping mechanism. Another participant, Darla Spence Coffey with the Council on Social Work Education, noted that studies about resilience often look for the extraordinary people who have survived horrific events and coped better than others. She said, “We should not need to be extraordinary to be good health care providers.” Crewe concurred with this idea, and added that “for those who are resilient, there are always those who are not.” Both resilient and nonresilient people are deserving of attention and care, she said.
McClain joined the discussion saying that he compares resilience to water rolling off a duck’s back—the stresses and upsetting situations of social work “roll off” a resilient person and do not affect their functioning. People expect social workers to be “tough,” said McClain, and the culture of social work sometimes reflects this attitude, with social workers insisting they are fine even after horrific events. McClain said that as commissioner, he made a point of telling social workers that “it is okay not to be” fine. He told participants about the time he was having a particularly difficult week, and he told his employees that he could “use a hug … or some really good thoughts or some prayers.” He wanted to demonstrate that asking for help is not a moment of weakness, it is a moment of strength. McClain noted that in our society, people tend to believe that “if you ever have a moment of weakness, you are forever perceived as weak.” McClain argued that
instead, a moment of weakness should be seen as simply that—a moment. “It was a moment. It doesn’t define me,” he said. McClain said it is his job to help his colleagues through their moments of weakness, and hopes they do the same for him.
Racism and Sexism
“We are experiencing an upsurge in racism, sexism, and some of the other isms,” said Crewe. She noted that many clients are the “targets of these isms,” and asked McClain how this affects the stress in the profession. She also asked him to comment on how he is personally impacted by these issues as an African American social worker. McClain responded that while he cannot speak for every African American male, he personally felt a great deal of internalized inferiority. He told participants that when he was in seventh grade, he moved from a predominantly black community to a predominantly white community, and he found himself believing that his white classmates were better than he. Despite becoming salutatorian of his class, these feelings persisted, and it took personal cognitive work to prevent it carrying into his professional work. As a person of color, he feels an obligation “to do right by [his] community.” At the same time, he does not want to use the “tools of the oppressor” to diminish other communities. Crewe added that as a black, female leader, she feels that she is less able to be herself and expose her vulnerabilities. She said that exposing vulnerabilities may deny her some opportunities because of differences in expectations about appropriate behavior for women of color.
Crewe asked McClain if there are specific tools that NASW offers its members to help them deal with these “daily struggles with the isms.” He responded that it starts with the code of ethics, which contain a responsibility to self-care and a responsibility to practice competently. “If you are competent in what you are doing, you are going to get good results,” said McClain, and “you are going to feel good about the work you are doing.” In addition, the professional standards for social work address connections with other professionals, fair salaries, and issues of respect and feeling valued.
Flexibility in Work
Finally, Crewe and McClain discussed the issue of designing flexible and practical work practices to mitigate stress and promote well-being.
McClain said that his main goal is doing “things that make sense” for the employees within a given work context. For example, in Massachusetts, as commissioner he ensured that each staffer had access to a laptop. This allowed employees to work from home when the weather conditions were bad, and it permitted flexible teleworking for those who were approved. In his current position, staff are allowed to use a compressed workweek, in which employees work the same number of hours each pay period, but in 9 days instead of 10. McClain said that caring about staff is not necessarily about offering the same options to everyone, but about individualizing flexibility to fit people’s unique needs.
REFERENCES
APA (American Psychological Association). 2016. 2016 work and well-being survey. http://www.apaexcellence.org/assets/general/2016-work-and-wellbeing-survey-results.pdf (accessed July 6, 2018).
Britt, T. W., R. R. Sinclair, and A. C. McFadden. 2013. Introduction: The meaning and importance of military resilience. In Building psychological resilience in military personnel: Theory and practice. Washington, DC: American Psychological Association.
McEwen, K. 2018. Resilience at work: A framework for coaching and interventions. http://workingwithresilience.com.au/wp-content/uploads/2018/06/R@WWhitePaperMay-2018.pdf (accessed July 7, 2018).
Sinclair, R. R., and T. W. Britt. 2013. Building psychological resilience in military personnel: Theory and practice. Washington, DC: American Psychological Association.
Smith, B. W., J. Dalen, K. Wiggins, E. Tooley, P. Christopher, and J. Bernard. 2008. The brief resilience scale: Assessing the ability to bounce back. International Journal of Behavioral Medicine 15(3):194–200.












