5
High-Quality Care for Everyone: Making Informal Care Visible and Addressing Care Under Extreme Adversity
Much of this report addresses the quality of care provided by formal health care systems in more or less well-organized settings. In many parts of the world, however, significant portions of the population lack access to high-quality, formal providers—either public or private—so they must seek care elsewhere. For millions, this means receiving care from informal providers (IPs) who lack formal training but are well known in the community.
In the Indian state of Madhya Pradesh, for example, 77 percent of rural primary care is provided by IPs (Das and Mohpal, 2016). Millions more people are suffering in fragile or failed states, or in humanitarian relief settings without strong oversight or regulation of care. The majority of these sources of care operate outside of formal health care systems, meaning that their patients are receiving care that may not be regulated, measured, or coordinated with other providers. In such settings, follow-up over time may also be extremely difficult. Taken together, these alternative care systems and the corresponding lack of scrutiny and transparency subject millions of people worldwide to care of completely unknown quality.
This chapter begins with an overview of what is known about the demographics and profiles of IPs, the types of work they do, the patients they treat, and the quality of care they deliver. The chapter then explores settings of extreme adversity, estimates the number of people requiring health care in such settings, attempts to shed light on their specific needs, and briefly reviews relevant research and best practices. The chapter ends with a summary and recommendations.
INFORMAL HEALTH CARE PROVIDERS: OVERVIEW
The size of the informal health care sector varies substantially by region—for example, it accounts for 55 percent of all providers in India (Prasada Rao et al., 2017), 77 percent in Uganda (Konde-Lule et al., 2010), and 87 percent in Bangladesh (Ahmed et al., 2009). But it is, by all accounts, enormous—far too large to be ignored in a global agenda for improving the quality of care. Understanding how this sector functions is critical to improving health in low-resource settings (George and Iyer, 2013).
Who Are Informal Providers and Who Is Seeking Their Care?
In light of an inconsistent definition of IPs, Sudhinaraset and colleagues (2013) developed a helpful working definition, of which the committee selected three components:
Caregivers lacking formal training with a defined curriculum who also meet at least two of the following three criteria:
- receive payments (usually undocumented) from patients rather than institutions;
- operate outside the purview of regulations, registration, or any official oversight; and
- may be part of professional associations that do not have certification or regulatory authority.
Using this definition, Sudhinaraset and colleagues (2013) found that IPs had very high patient loads and sometimes represented more than half of all providers in Asia and Africa. They also found that the health sector globally has a significant number of IPs who operate in a variety of health areas. They may include community health workers (CHWs), allopathic providers, traditional healers, faith healers, homeopaths (Ahmed et al., 2009), or often people who are trained in one area but practicing in another—for example, trained pharmacists acting informally as doctors in their neighborhoods. The committee agrees with this working definition but would remove the part regarding training, as that becomes very difficult to define and categorize with CHWs. Instead, the committee highlights the importance of these IPs operating beyond the purview of regulatory oversight, being unlicensed, or providing a service beyond the scope of their license.
While IPs can fall into several categories, a study in Bangladesh, India, and Nigeria found that the majority are fairly well educated, having completed levels of secondary school and even beyond (Center for Health Market Innovations, 2010). While most lack formal medical training, most have some type of training, such as courses offered commercially, public training for CHWs, or some type of apprenticeship. Cases do exist of fraudulent IPs who are trying to deceive patients and who are driven more by a profit motive than by any strong desire to offer care of high quality (Bloom et al., 2011; Cross and MacGregor, 2010). But several studies demonstrate that the motivations of many IPs go well beyond only making money and include, for example, pursuit of social standing, knowledge acquisition, and community solidarity (Sieverding and Beyeler, 2016). For instance, volunteer CHWs in South Asia and sub-Saharan Africa have espoused social recognition and personal empowerment as reasons for becoming an IP, not linked directly to financial gain (Glenton et al., 2010; Gopalan et al., 2012; Kasteng et al., 2016). Likewise, medicine vendors in northwest Cameroon see themselves as gatekeepers for access to strong medications and take that responsibility seriously (Hughes et al., 2013).
Many people use IPs because they are available, while formally trained nurses and physicians are in very short supply. For example, the ratio of traditional healers to population in Africa is 1:500, while the ratio of medical doctors to population is 1:40,000 (Abdullahi, 2011). This imbalance is more pronounced in rural than in urban areas; urban populations in African countries typically have greater access to formal providers. Yet, even urban residents sometimes use traditional medicine more often than they use formally trained caregivers (Bamidele et al., 2009). Even in countries with easy access to well-established formal care, such as Singapore and South Korea, people commonly still use traditional medicine because of cultural or historical influences (WPRO, 2012). In India, most people seek care in the private sector, where providers’ qualifications vary from a medical
degree to one based on traditional medicine (e.g., Ayurveda) to no training at all. Most visits, however, may tend to be to underqualified providers, as indicated by a study on health-seeking behavior in rural India. That study found that 70 of every 100 visits to a health care provider were to unqualified private providers, whereas 8 of every 100 visits were to qualified public providers (MAQARI Team, 2011).
How Good Is the Care in the Informal Sector?
Health care providers of any kind—whether providing care, advising on treatment options, or dispensing medications—should ideally be trusted professionals. But the large numbers and diverse nature of IPs, who typically operate outside of regulatory oversight, raise legitimate concerns about the quality of care they provide. The default assumption tends to be that because IPs lack standard qualifications, they deliver services of substantially lower quality relative to formally trained medical doctors, nurses, and pharmacists. But actual data on that comparison are scarce, and findings are mixed. The relevant evidence is difficult to parse, in part because IPs are such a highly variable group. Some IPs, for example, act as apprentices to formal doctors for several years, while others have almost no involvement in the formal health care sector before setting up shop.
Because a large proportion of people in India seeks care from IPs, that nation has yielded some of the best data on the topic. Gautham and colleagues (2014) studied IPs in two different settings in India and found that more than two-thirds were able to manage common conditions competently, although they did prescribe more drugs than necessary. Das and colleagues (2012) used a gold standard method—standardized patients (that is, people recruited and trained to simulate symptoms and complaints)—to assess quality of care in rural and urban India across a large number of studies, and found only modest differences between trained and untrained practitioners in their adherence to approved checklists. They also found no differences in the likelihood of providing an accurate diagnosis or correct treatment (Das et al., 2012). A study in Nigeria found that medicine vendors—a common type of IP—knew about the government malaria policy, with nearly 60 percent indicating correctly that artemisinin-based combination therapy (ACT) was the first-line treatment. More than three-quarters of those studied took adequate patient histories, and nearly half prescribed ACT properly (Center for Health Market Innovations, 2010).
While the evidence suggests that IPs are only modestly less knowledgeable than formal providers, factors other than the store of knowledge also drive the quality of care. It is known, for instance, that a very large know-do gap exists in health care delivery throughout the world (see Chapter 2). That is, providers—whether formal or informal—often fail to act on
knowledge that they appear to have. In low-resource settings, there can be a substantial difference between what providers appear to know in standardized testing (such as clinical vignette testing) and what they do when caring for an actual patient (see also Chapter 4) (Mohanan et al., 2015). A study conducted in Delhi, India, compared the performance of formal providers on vignettes with their performance when a standardized patient presented with the same symptoms. The researchers found that for standardized patients, the doctors were less likely to recommend appropriate tests and to make referrals than they were in the vignette-based testing (10 percent versus 73 percent) (Das et al., 2015). These results highlight that a lack of knowledge among providers is not necessarily the limiting factor for high-quality care in low-resource settings. Instead, providers often have knowledge that they do not translate into practice. Much more research is needed on how to help providers—both informal and formal—strengthen the connection between knowledge and practice.
Just as a knowledge base is insufficient to ensure high-quality care, the same is true for structural inputs alone. Studies find only very weak links between the structural inputs to health care facilities, such as medical equipment and patient loads, and the quality of care. This is the case in both rural and urban environments. Researchers argue that quality gaps cannot be closed by simply conducting more training or adding more doctors. Instead, as discussed in Chapter 2, quality improvement on all fronts will require systemic changes and proper designs to make a holistic impact on health care quality. Examples of such systemic changes include increasing accountability through community monitoring (Björkman and Svensson, 2009), finding ways to attract clinicians who are intrinsically motivated, and motivating current employees—whether in the formal or informal sector—through encouragement and scrutiny from peers (Brock et al., 2012). Since IPs operate outside of regulatory authority, the level of quality of the care they deliver is largely unknown. Countries need a national strategy for identifying these IPs and for measuring their work processes and outcomes.
What Are the Benefits and Risks of Care Received from Informal Providers?
While many organizations, especially those representing formal providers, are skeptical of IPs, the reality is that IPs represent a significant portion of providers and that efforts to eliminate them—or to ignore them—have not been successful. Whatever a nation’s strategy toward IPs may be, understanding both the benefits and risks of their care is critical to making wise decisions. In countries without robust health care coverage, patients are often limited to seeing providers whose fees they can afford. Because IPs are relatively inexpensive, they are often the providers of
choice for ailments that are not life-threatening. A study in Bangladesh, for example, found that the median cost of treatment by a formal physician was 5 times higher than that of a village doctor and 15 times higher than that of a traditional healer (ICDDR, B, 2009). IPs also typically have more forgiving payment policies, such as sliding scales or deferred payment options (Sudhinaraset et al., 2013).
Beyond affordability, another benefit to using IPs is that they are in some ways more accountable and more familiar. Many people choose to use IPs even when there is, at least theoretically, a public clinic nearby that provides free services. The reasons for this are complex but include the high rates of absenteeism in public clinics and the greater degree of familiarity with private IPs, since they often have strong local roots in their own communities. Although IPs may not be formally regulated, some argue that it is easier to keep them “in check” relative to formal providers since their practice depends on maintaining good relationships with their community. Their accountability is, in this sense, direct. Conversely, formal providers working in public clinics are often from outside the local community and are posted in those clinics for short periods of time. A study in India found that more than half of the IPs surveyed were born in the same block or district where they practiced, rendering them well-known and often trusted members of the community (Center for Health Market Innovations, 2010). Typically, they are cognizant of or aligned with the values and beliefs of the people in their community. They may also be more flexible than the formal care system in the services they provide. As researchers found in Uganda, for example, they may be more willing to make home visits, especially with respect to women’s reproductive care (Kiapi-iwa and Hart, 2004). While this issue may become less important in the future if formal health care systems shift to become more community-based, for now, getting to a formal clinic or hospital in many places is enough of a barrier to lead patients and families to choose IPs instead. There also is typically less turnover among IPs than in formal facilities, increasing their familiarity to their community.
One example illustrating the benefits is an integral part of India’s National Rural Health Mission. The goal is to provide every village in the country with an an accredited social health activist (ASHA), who acts as a trained CHW serving as a link between the community and the public health system. While their formal medical training is limited, ASHAs act as a primary source of education on health practices and aim to increase the utilization of health services (National Health Mision, n.d.). The ASHA program was launched in 2005, and its work was key in reducing the infant mortality rate from more than 50 to 34 deaths per 1,000 live births by 2016 (IANS, 2017).
Of course, care from IPs carries substantial risk. Some examples associated with traditional and complementary medicine include use of poor--
quality or counterfeit products and treatment by unqualified practitioners who can miss or delay diagnoses, with dire clinical consequences. IPs can be sources of misleading information or be directly responsible for adverse medical events, such as side effects or harmful treatment interactions (WHO, 2013). A review in Bangladesh in 2009, for example, found that just 14 percent of the drugs used by IPs to treat diarrhea, pneumonia, fever, and colds were appropriate (in line with treatment guidelines) (Bhuiya, 2009). Authors of the studies described above in Bangladesh, India, and Nigeria also caution that IPs have been shown to engage in detrimental, unnecessary, and wasteful medical practices, such as conducting insufficient testing prior to diagnosis, performing unnecessary injections, and overprescribing (Center for Health Market Innovations, 2010). Of course, these problems are also found among formal providers, sometimes at nearly comparable rates.
What Can Be Done to Improve Care in the Informal Sector?
What can nations do to improve care in the informal sector? The dearth of formal research on the patterns, behaviors, and outcomes of that sector limits strong conclusions, but research does support some sensible steps. While the many different contexts and types of IPs make generalized recommendations difficult, one critical issue across the board is addressing the gap between IPs’ knowledge and practice. It is also important to understand where in the scope of practice IPs can contribute positively to a health system. In the end, of course, each country needs to have a contextual understanding of how its IPs fit within and serve the country’s cultures and populations. Research suggests several plausible steps toward improvement, some of which are described below: acknowledging IPs, leveraging traditional healers, defining scopes of practice, and implementing various types of interventions.
Acknowledging Informal Providers
The notion of formalizing IPs is hotly contested, but evidence supports at the very least identifying them and incorporating them to supplement the health care workforce in many areas of the world, as well as leveraging their strengths within their trusting communities (discussed in the following section). Researchers argue that the formal health care sector should design a strategy for integrating IPs into the mainstream system to ease pressure on a typically overburdened system, especially in low-resource settings such as Bangladesh (Ahmed et al., 2009). This strategy would be especially important for middle-income countries that need to reach their poor and vulnerable populations to overcome the historical inequities in their health
care systems. Because drug vendors are one of the most common types of IP, working with them could be a first step in engaging the informal health care sector. Bringing them into the mainstream health care system “to provide appropriate drug dosages and referrals” could help reach poorer populations (Sudhinaraset et al., 2013, p. 9). For example, a high percentage of Tanzanian citizens obtain their medicines from private shops, often located close to their homes with convenient hours. However, prior to 2003 the sellers were often unregulated or unlicensed, illegally selling prescription-only products, or untrained (Embrey et al., 2016). In 2003, a public–private partnership—the Accredited Drug Dispensing Outlet (ADDO) program—developed an accreditation scheme and increased training, education, and supervision of staff responsible for dispensing medicines. An evaluation of ADDOs in the region of Ruvuma after 8 years of implementation showed the program to be not only successful, but also sustainable and scalable (WHO, 2014). Traditional medicine practitioners offer another entry point. Ahmed and colleagues (2009) found that using institutional training, registration, and licensing to make traditional medicine practitioners more reliable might decrease health care costs and the demand pressures faced by a health care system.
With the global shift toward person-centered health care systems, the goals of providing services near the patient, integrating care across the continuum, and linking care to community services are paramount. Although IPs are currently weakly regulated in most places, they can, if operating in the same community as formal providers, offer additional capacity for screening, referrals, coordination, and case management. Given the realities of many low-resource settings, it is unclear whether an accessible, high-quality health care system made up only of formal providers is achievable, at least in the conceivable future (Sieverding and Beyeler, 2016). While some policy makers may see a purely formal system as the ultimate goal, in the interim, acknowledging, incorporating, and improving the care of IPs may be a more pragmatic approach to a person-centered health care system. Many IPs interviewed in rural Nigeria consider themselves to be part of the village health system, and they believe they play an important role in the community’s primary care (Sieverding and Beyeler, 2016). To take full advantage of that notion, it will be important to develop interventions to support collaborative working relationships between the formal and informal sectors. As a start, the committee believes countries could include IPs in counting so that more knowledge can be generated about their practices and patients. In addition, countries could train IPs, where appropriate, to help buttress a formal health care sector that badly needs additional workforce capacity.
Leveraging Traditional Healers
Traditional healers are often the first point of consultation in many communities worldwide for health issues. In some countries, they work largely within the formal system; in others, they do not (Omaswa, 2006). As of 2003, traditional medicine made up 40 percent of all health care delivered in China, 71 percent in Chile, 40 percent in Colombia, and 65 percent in rural India (WHO, 2003). In parts of Africa, herbal medication is the primary treatment for approximately 60 percent of children with febrile symptoms, and in North America and Africa up to 75 percent of people living with HIV/AIDS use traditional medicine (WHO, 2003). Even in developed countries, traditional and alternative medicines have grown in popularity.
Leveraging IPs’ familiarity and access to community populations is one potential and feasible way to improve the quality of care in those communities. A Cochrane review on implementation strategies for health systems, for example, found that training traditional healers may improve their knowledge and patient management and referral practices for sexually transmitted diseases and HIV (Pantoja et al., 2017). Many countries are beginning to realize the value that traditional healers can bring to their formal health care systems. To meet this new demand, the World Health Organization (WHO) has developed an updated strategy on Traditional Medicine for 2014–2023 with two key goals:
(1) to support member states in harnessing the potential contribution of traditional medicine to health, wellness, and person-centered health care; and (2) to promote the safe and effective use of traditional medicine through the regulation of products, practices, and practitioners. (WHO, 2013, p. 6)
These two goals could guide countries in integrating various types of IPs into their formal networks to extend their reach and coverage of populations while still ensuring safety and quality. WHO cites the projected rise in the global burden of chronic disease as the most pressing reason for strengthening this collaboration between the conventional medicine and traditional medicine sectors (WHO, 2013).
Defining Scopes of Practice
Another approach the committee believes can benefit quality of care is defining the scopes of practice of IPs. As discussed previously, highly variable and diverse groups of practitioners make up the broader IP category. For this reason, and because of the lack of acknowledgment and oversight
from regulatory bodies and country governments, it is extremely difficult to tell when IPs are operating within the scope of practice in which they can perform competently. A study in South Africa, for example, found that traditional healers practice with guidelines often unwritten and legally unregulated—the opposite of the current practice of South African formal health care practitioners regulated by statute (Duvenhage and Louw, 2016). And a recent study on preeclampsia in Nigeria found that CHWs interviewed did not regularly give antihypertensives for emergency preeclampsia and eclampsia, even though such treatment is dictated by international guidelines, because many were concerned that doing so was outside of their scope of practice (Sotunsa et al., 2016).
On the other hand, some types of IPs, such as CHWs, have often had training and are familiar with their scope of practice. Many countries have standard tiers for CHW types with defined scopes of practice. Ethiopia, for example, has a two-tiered system through its Health Extension Program—the Health Development Army (HDA) volunteers and the Health Extension Workers (HEWs) (Zulliger, 2014). The HDA lower-level volunteer cadre works just a few hours a week in the community in the areas of newborn nutrition and family practices, while the HEWs, a higher-level cadre, are trained for longer, with a scope of practice that includes treatment of children with malaria, pneumonia, diarrhea, and newborn sepsis (Leon et al., 2015).
Since 2002, WHO has been calling for defined scopes of practice for traditional healers as part of a regional strategy for traditional medicine, with the responsibility for establishing standards and training resting with practitioners, educational institutions, and governments (WPRO, 2012). This may not be accomplished overnight, but together with the committee’s previous call to acknowledge and formally count IPs, an important step forward would be for countries to define scopes of practice for various types of IP where possible and appropriate. With reference to the design principles set forth in Chapter 2, the transformation process the committee calls for throughout this report emphasizes continual feedback, learning, and improvement. Accordingly, those whose scope of practice is already defined could advance this transformation by connecting with other similar practitioners and providers and revisiting gaps and models, as in the Nigeria example above, to improve their country’s health care quality.
Implementing Interventions
The most common recommendations for improving informal care found in the systematic review of Sudhinaraset and colleagues (2013) are for educational interventions, such as capacity-building training, patient education programs, and continuing education requirements. While these
interventions would be directed at IPs, there is also a need to educate formal providers in traditional or complementary medicine to augment their understanding. Numerous universities in the Economic Community of West African States have already recognized this need and included transcendental meditation in their medical and pharmaceutical curriculum (AFRO, 2011). A large number of studies also call for oversight and regulation of IPs, as well quality assurance by way of professional associations. Process interventions were frequently recommended as well, including such activities as promoting dialogue and developing working relationships among formal and informal providers (Sudhinaraset et al., 2013).
In a separate review, Shah and colleagues (2011) present a conceptual framework for considering the types of interventions that could be implemented in the informal system (see Figure 5-1). Successful interventions for child health involve changing the environment of incentives and accountability, focusing on the higher levels of the health system illustrated in the committee’s framework in Figure 2-2 in Chapter 2. In Uganda, for example, common goals and expectations for diagnosis and treatment of child illness were developed through negotiation sessions with private providers, leading to significant improvements in the majority of items measured (Tawfik et al., 2006).
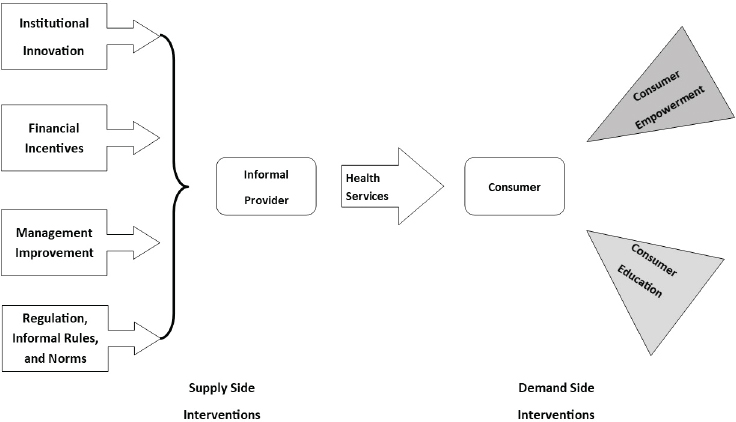
SOURCE: Shah, N. M., W. R. Brieger, and D. H. Peters. 2011. Figure in “Can interventions improve health services from informal private providers in low and middle-income countries? A comprehensive review of the literature.” Health Policy and Planning 26(4):278. By permission of Oxford University Press.
It should be noted that very few studies have called for increased access to formal providers to reduce the need for IPs, partly because such efforts are unlikely to be successful. Sudhinaraset and colleagues (2013) recommend that interventions not be reliant on individual-level behavior changes alone as they are extremely difficult to influence; rather, a combination of market-based and regulatory approaches with rigorous evaluations may prove to be successful for improving the quality of informal care. They identify quality improvement strategies that combine providing training with improving market conditions, such as provider incentives and accountability, as being most successful (Shah et al., 2011).
Supporting this finding, a 2010 review identified training as one of the most common interventions, but ineffective on its own. Training was most successful when paired with initiatives that changed institutional relationships and incentives (Shah et al., 2011). More specifically, studies employing training alone found positive outcomes just 21 percent of the time, but when training was combined with other strategies, the rate of positive outcomes was nearly 60 percent (Shah et al., 2011). While this finding does not negate the importance of training providers at the community level, more successful approaches included measurement and disclosure of performance. In a large randomized controlled trial, Das and colleagues (2016) found that a 12-week intervention that entailed training IPs substantially improved case management rates—the IPs were more likely to make the correct diagnoses and offer proper treatments. Yet, while these results are promising, the intervention unfortunately had no impact on rates of unnecessary prescribing. Truly understanding the effectiveness of training will require more rigorous research designs to document longer-term outcomes and better incorporate contextual factors (Shah et al., 2011). High-quality intervention research targeting IPs and measuring population-level outcomes is a major need.
What Is Left to Understand?
Much more is unknown than known regarding IPs, even though a very large proportion of the world’s population seeks them out frequently to meet health care needs. At a foundational level, common definitions of IPs and a common understanding of what types of providers exist and what services they provide are needed. The systematic review of Sudhinaraset and colleagues (2013) calls for a better understanding of patient choices and knowledge. And crucially, research is needed to examine the quality of IPs, beyond just their knowledge base, since knowledge alone has been proven to be a poor indicator of clinical quality.
In addition, studies are needed to understand traditional medicine in greater depth to help countries develop their frameworks and strategies, especially since many countries continue to incorporate traditional
healers and practitioners into their formal health care systems. This trend transcends income level; as noted earlier, many high-income countries also see growing use of alternative medicine and complementary therapies. In Australia, for example, visits to complementary health professionals increased more than 50 percent from 1995 to 2005 (Australian Bureau of Statistics, 2008). Likewise, the use of acupuncture, a traditional Chinese medicinal practice, is now recognized by 103 member states within WHO (WHO, 2013). With so many modalities from different regions being used worldwide, the assurance of quality in traditional medicine can benefit from heightened levels of cooperation among countries to define and support access to safe products and practices from this sector (WHO, 2013).
As of 2012, 73 WHO member states had established national research institutes for traditional and herbal medicine, and 119 were regulating herbal medicines. Yet, 105 member states cited “lack of research data” as a top difficulty with respect to regulatory issues related to the practices of traditional medicine, and 68 cited a lack of financial support for research on traditional medicine as a challenge (WHO, 2013). Clearly, this represents an opportunity for the global community to bring together centuries of varied experience and research and regulatory experts to improve the quality of traditional medicine.
HEALTH CARE QUALITY IN SETTINGS OF EXTREME ADVERSITY
The challenges of assuring and improving the quality of care in low-resource settings are magnified in settings of extreme adversity, defined by Leatherman and colleagues (in press) as “comprising but not limited to fragile states, conflict-affected areas, and sustained humanitarian crises.” The growth in connectivity in the past decade has increased awareness of the many instances of suffering, war, and conflict in the world, as well as of the growing numbers of people displaced from their homes. In 2016, 1.8 billion people, or 24 percent of the world’s population, lived in fragile contexts, a figure predicted to grow to 3.3 billion by 2050 (OECD, 2018a). The proportion of those living in extreme poverty in fragile contexts is also increasing (see Figure 5-2).
Such situations are highly nuanced and complex, and do not yet benefit from an easy definition or clear nosology. Databases such as the Fragile States Index (FSI), a tool for measuring in real time when tensions in a country outweigh the capacity to deal with them, can now provide early warning for the international community (FSI, 2017).
With the explosion of migration in recent years, many refugee camps with austere conditions have formed in countries that are not themselves considered failed or fragile states, such as France, Jordan, and recently
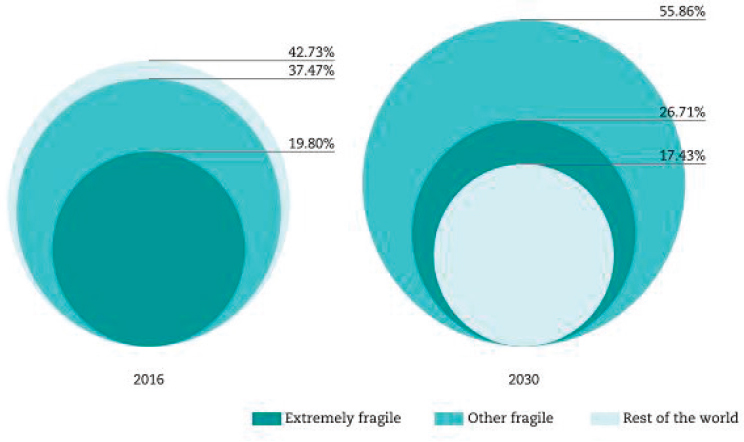
SOURCE: OECD, 2018b.
Bangladesh. In countries such as Nigeria, regions of thriving economic activity with strong governance and social structure may coexist with other regions that are plagued by terrorist groups (e.g., Boko Haram) and that lack the security and services found elsewhere in the country. Countries vary along the spectrum of “fragility,” leading to highly variable needs. Venezuela, for example, although historically having a strong economy, has descended into high rates of violent crime and hunger, with little access to medical supplies. At the other end of the spectrum are countries, such as Iraq and Afghanistan, that are emerging from years of war but with newly functioning governments. One obstacle these settings all have in common is their lack of reliable and timely access to high-quality health care. Some may have little to no health care at all, while others may have a fragmented mix provided by international nongovernmental organizations (NGOs) and local health care practitioners who have stayed behind when most of the well-educated population has fled. Because of the constraints and limited resources in these settings, the first priority has historically been to get any care available to the population and worry about quality afterwards, but this approach is misguided. Quality and access efforts need to be linked as any type of health care is offered, and the committee would argue that it is perhaps more important to assure quality in these settings than anywhere else. The committee has chosen to characterize these chaotic and uncertain environments as “settings of extreme adversity” so as to shine a light on
the dearth of quality health care affecting a huge proportion of the global population, many of whom are women and children.
Growing Challenges in the Number and Distribution of This Population
The number of people worldwide who are currently living in some type of extreme adversity, whether for humanitarian, war, refugee, or fragile state reasons, has continued to grow in recent years as a result of ongoing sociopolitical conflicts. As this number and the number of countries involved grow, it becomes increasingly difficult for the limited scale of global resources and initiatives to address the problems adequately. Before issuing specific calls for action, however, it is imperative to understand more about these various situations, how many people are subject to what types of environment, and what their true needs are so that those in the global community can prioritize what is most needed and mobilize appropriately for action.
According to the World Bank (2018a), half of the world’s poor—2 billion people—live in fragile or conflict-affected states, and more than 50 percent of all refugees in 2014 were children for whom access to education, health care, and other essential services was severely limited. Globally in 2015, the world saw a record high number of people—more than 65 million—who endured forced displacement because of conflict or persecution (UNHCR, 2016). Data from the Organisation for Economic Co-operation and Development (OECD) paint an even bleaker picture, indicating that half of the 836 million people living in poverty today globally are living in fragile contexts—a proportion projected to reach 80 percent by 2030 (OECD, 2018a). Thus, traditional avenues of development and bilateral aid and historical global health efforts are unlikely to reach the vast majority of this population.
Service Readiness and System Inputs to Health Care
Chapter 2 describes some of the basic inputs or foundations for any health care system. In most high-income settings, these foundations can be fairly assumed to be present and functional. In many low-resource settings, however, the foundations of the health care system can be variable throughout a country. In settings of extreme adversity, the quality of the inputs to the system and general service readiness is even lower, and may vary widely on a daily basis depending on the status of the power grid, existential threats (such as bombs), and the available workforce. Although it has been noted throughout this report that these types of foundations do not necessarily dictate the quality of care being provided in a particular location, their absence can certainly be expected to have a profound impact on the care that can be provided.
Although an increase in the workforce or training alone is inadequate to meet the demand for quality health care in typical low-income settings, the environmental issues that come with the lack of infrastructure and medical supplies in settings of extreme adversity compound the gaps in quality. A systematic review on surgical capacity in 21 low- and middle-income countries (LMICs), for example, revealed that less than two-thirds of hospitals regularly offering surgical care had access to a continuous electricity source or generator (Chawla et al., 2018), a point illustrated vividly during the committee’s site visits to hospitals in Goma, Democratic Republic of the Congo (DRC). Lead doctors at hospitals in Goma highlighted the unstable power grid and the lack of working generators as critical causes of mortality and morbidity among their patients, especially in such settings as the neonatal ward, with babies in incubators.1
Quantifying the Burden of Poor-Quality Care in Adverse Environments
Looking at countries facing extreme adversity as a subset of LMICs, one finds a disproportionate burden of low-quality care for certain conditions. The team that conducted the analyses for quality dimensions in Chapter 4 also performed analyses on a subset of countries that are classified as fragile states to gain a better understanding of the quality of health care delivered in these adverse contexts, although the lack of available data limits these findings in ways similar to those discussed in Chapter 4, and these numbers thus represent the committee’s best estimates. In the case of quality-related neonatal mortality (unnecessary mortality among those with access to care), for example, an estimated 22.7 percent of deaths occur in fragile states annually, even though these states represent only 8.5 percent of the LMIC population (see Table 5-1). For other measures, such as lung cancer mortality, this proportion is much smaller (0.4 percent). This differential may be due to underreporting of cancers in fragile states, shorter life expectancies, or other factors. In addition, the definition used to identify fragile states is conservative and is at the national level—all countries with an FSI of 100 or above.2
___________________
1 Personal communication, E. K. Muhindo, General Reference Hospital, North Kivu, DRC, December 15, 2017.
2 The FSI, produced by the Fund for Peace (FFP), is a tool intended to highlight the normal pressures that all states experience and identify when those pressures may be outweighing a state’s capacity. The FSI includes 178 states and is based on a triangulated approach to data collection through content analysis, quantitative data, and qualitative review (FSI, 2017). Fragile states included here and in Table 5-1 are Afghanistan, Chad, Cote d’Ivoire, Democratic Republic of the Congo, Guinea, Guinea Bissau, Haiti, Iraq, Nigeria, Pakistan, Somalia, South Sudan, Sudan, Syria, Yeman, and Zimbabwe.
| Cause of Death | Proportion of Quality-Related Deaths* in Fragile States (%) | No. of Quality-Related Deaths in Fragile States | No. of Quality-Related Deaths in LMICs (total) |
|---|---|---|---|
| Neonatal Mortality | 22.7 | 51,173 | 462,131 |
| Maternal Mortality | 11.6 | 5,055 | 43,602 |
| Lung Cancer Mortality | 0.4 | 552 | 130,000 |
*Quality-related death is defined as excess death occurring among all patients with access to care, using high-income countries as a benchmark to define excess.
SOURCE: See Appendix D.
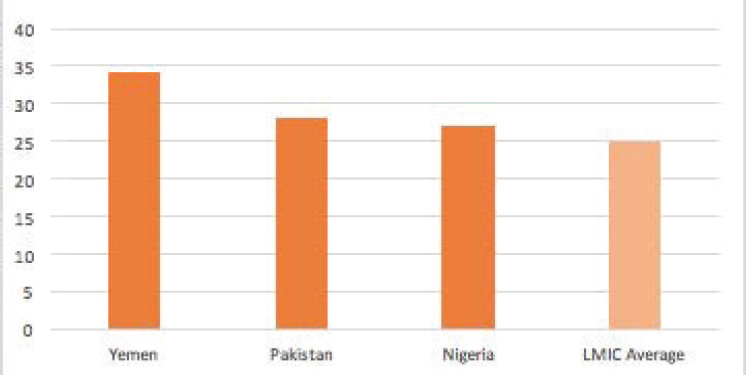
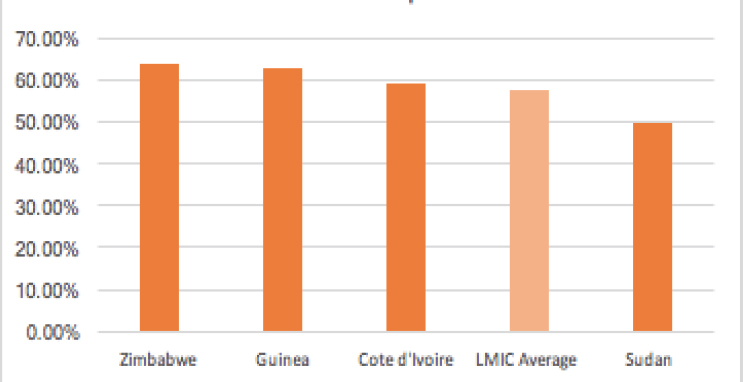
With regard to person-centeredness, it appears that people in the fragile states for which data are available are more dissatisfied with their care on average relative to people in all LMICs, at 29.7 percent and 24.9 percent, respectively (see Figure 5-3). With the exception of Sudan, people in fragile states also report higher rates of disrespect than the LMIC average, 59 percent versus 57.6 percent (see Figure 5-4).
While differences should be interpreted cautiously, lack of consumer choice (and the corresponding assumption that people in contexts of adversity may rate their care artificially high) is cited as a reason not to focus on or collect data on person-centeredness in these contexts. Yet, these data suggest that people faced with extreme adversity may retain the ability to pass judgment on the quality of care they receive. These data may also represent an underestimate of dissatisfaction and rates of disrespect.
Needs and Priorities in Adverse Environments
Although health care providers, including both humanitarian and local workers, try to “do no harm” and provide the best care possible given their situations and resources, caregivers in these settings of extreme adversity are likely have priorities that differ from those in more stable settings. Simply providing access to lifesaving care has historically been the priority, but as the numbers of people in extreme adverse circumstances worldwide rise and as the crises responsible for these circumstances shift to protracted status rather than being just acute emergencies, the need for health care services across the continuum from preventive to palliative care is increasingly being acknowledged.
Given the amount of violence and trauma to which both adults and children bear witness, mental and emotional health care is a top priority
for populations in these settings. After several years of war, nearly half of Syrian children now show signs of posttraumatic stress disorder (PTSD), and one-quarter of them face developmental challenges (Karasapan, 2016). Researchers examining health-seeking behavior in Mosul in the period immediately following ISIS (Islamic State in Iraq and Syria) occupation found that emotional and mental health problems were leading illnesses for both adults and children (Marquez, 2016). Likewise, the Rohingya refugee situation in Bangladesh has escalated in the past 12 months, with nearly 1 million refugees crossing into Bangladesh from Myanmar as of February 2018 (WHO, 2018b). Not surprisingly, large numbers of these refugees have suffered serious mental and psychosocial impacts from their displacement, as well as from violent and traumatic experiences during their journey. Humanitarian responders recognize, as with refugees from Syria, the need for increased accessibility of specialized mental health services and greater capacity for these services within the primary care workforce. But given the breadth and depth of the problem, services must go beyond meeting basic needs and leverage community-based health care systems (Marquez, 2016).
Lafta and colleagues (in press) identify as other challenges in Mosul the shortage of medications and equipment, especially pediatric medicines and medicines to treat chronic conditions; the lack of health care professionals and the collapse of their salaries (likely related); and the weak coordination among providers in shelters, with limited access to follow-up on patients referred for hospitalization (Marquez, 2016). Other conditions affecting large numbers of patients in Mosul included diarrhea, hypertension, and noncommunicable diseases (NCDs). These problems were also identified as priorities by providers in Venezuela, with National Public Radio (NPR) reporting that the entire Venezuelan health care system is on the verge of collapse (Raphelson, 2018). The Pharmaceutical Federation of Venezuela estimates that the country has a shortage of 85 percent of medicines (Reuters Staff, 2017), while some hospitals lack electricity, and more than 13,000 doctors have left the country in the past few years because of the deteriorating circumstances (Trejos, 2017). These numbers were reflected in a front page tragedy early in 2018 when a Major League U.S. baseball player died in his native Venezuela because antibiotics to treat his pneumonia were difficult to find (Raphelson, 2018).
While initial priorities upon settling the Rohingya refugees in Bangladesh are clean water and sanitation to prevent disease, nutrition is also critical. More than 400,000 of those in the refugee and host community populations require emergency nutrition interventions (WHO, 2018b). Responders worry that without immediate scale-up of interventions, nearly 150,000 children under 5 will suffer from acute malnutrition. Unfortunately, nutrition needs to be a priority in these settings beyond the aftermath of a crisis. A recent observational study in Afghanistan found the
prevalence of undernutrition to be among the highest in the world, with child wasting exceeding 20 percent in high-conflict regions (Akseer et al., 2018). Stunting was extremely variable, with prevalence ranging from 4 percent to 84 percent depending on the district.
Variability and Challenges of Providing Care
While the health issues described above are the more immediate and acute ones that emerge in crisis settings, rightfully demanding attention and resources from donors and health care providers, other chronic and persistent conditions also exist. The lack of adequate knowledge or infrastructure for addressing these more chronic conditions creates gaps in already fragmented and underresourced systems. More than 80 percent of the 629,000 Syrian refugees in Jordan, for example, are settled not in camps but in communities within the country, reflecting a broader trend globally (UNHCR, 2015). As might be expected from the growing burden of NCDs worldwide, a growing percentage of displaced older populations from middle-income countries require care for their chronic conditions. This changing profile demands a different set of services than humanitarian and other responders are typically familiar with providing, and it places a heavy strain on the host country’s health care system (Akseer et al., 2018). In the particular case of Syrians, the population had high rates of smoking, high body mass indexes, and elevated blood sugar before the conflict began in 2010, yet very little attention had been given to NCD prevention and health promotion (Doocy et al., 2016). Thus, with the population now spread out across various settlement locations, addressing NCDs systematically has become extremely challenging. Several experts identify a shortage of guidance on NCDs in various emergency guidelines and policies, leading to a gap in adequate health care for populations during and following emergencies (Demaio et al., 2013).
Another health care issue that has advocates but often lacks supporting data is reproductive health care and gender-based violence in contexts of conflict, humanitarian crisis, or failed states. Sexual violence is common in these settings of extreme adversity, and it is exacerbated by separation from traditional communities and a breakdown in law and order. At the 2016 World Humanitarian Summit, WHO called attention to sexual and reproductive health needs, particularly among women and girls. Of the 100 million who were targeted in 2015 with humanitarian aid, WHO estimates that 26 million, or more than one-fourth, were women and girls of reproductive age (WHO, 2018c). The disintegration of society in these settings often increases women’s exposure to threats including sexual violence, unwanted pregnancy, unsafe abortion, increased rates of HIV and other sexually transmitted infections, and maternal illness or death. Thus,
despite much attention in the global discourse to adolescent girls and young women, in these types of emergency contexts they are at high risk for sexual violence, as well as for human trafficking and forced marriage, and the services to help them are weak. And these issues often persist even after a conflict ends, as social norms can reinforce gender-based violence. Liberia, for example, continues to have some of the highest levels of sexual violence and abuse toward women worldwide even though its conflict ended more than 10 years ago (Samuels et al., 2017).
Reproductive health care in humanitarian settings was not seen as a priority until the mid-1990s, when donors, governments, and NGOs came together to urge increased advocacy and research and provided manuals and guidance on interventions in the field (Barot, 2017). Yet, while these efforts provided much support and encouragement, repeated evaluations, even as recently as 2014, highlighted key remaining gaps in service delivery, such as failure to immediately implement provision of the minimum initial services necessary at the onset of an emergency (IAWG, 2015). Some barriers to addressing these gaps are cultural, but many also involve a lack of relevant research and financial resources (Barot, 2017). One approach that could help fill these gaps would be to include women and girls in the planning and management of policies and programs for these types of emergencies, in accordance with the fundamental principles of person-centered design discussed in Chapter 2. This approach could be valuable not only after a crisis but also during peacetime to allow for the building of preparedness and resilience before an emergency occurs.
In addition to the challenges of the variability of illnesses and conditions in adverse settings, the vast number of health care providers and actors involved in a conflict zone or refugee camp results in an even more complex problem—coordination (see Box 5-1). For example, long-term progress in providing quality health care for all Afghan citizens will require a “combination of specific goal-oriented projects, foreign aid, domestic responsibility, and time” (WHO, 2018a). Given its history of conflict, damaged infrastructure, and dearth of providers, Afghanistan will need to utilize diverse resources to rebuild its health sector (WHO, 2018a).
Evidence Available to Guide Health Care Leaders
Both country-specific information and a general understanding of the evidence base are needed to address quality issues in contexts of extreme adversity systematically. An evidence base is lacking even for a country such as Iraq, which has a long-standing history of multiple conflicts and fragility; identification of poor-quality areas and methods with which to address deficiencies are still sorely needed (Al Hilfi et al., 2013). Some evidence is available that can be applied to similar settings to improve health outcomes.
For example, health care quality fared the best in Afghanistan when both patient and provider were female (Hansen et al., 2008), likely because of the many cultural and religious challenges that surround interactions between men and women who are unmarried. Thus, just encouraging and incentivizing more female providers to increase the number practicing could improve the quality of care. Another nonhealth intervention found to be successful, also in Afghanistan, was the emergence of community councils that managed the oversight of health facilities. Likely because of their reputations in the community and the consequent accountability, their activity was a predictor of higher-quality care (Edward et al., 2012).
Some interventions, such as supervision and feedback, are found more traditionally within health care systems. In the same Afghanistan study, better supervision in the form of increased supervisory visits was associated with improvements in quality (Edward et al., 2012). Other studies have also shown supportive supervision to be a key motivating factor for provider performance (Naimoli et al., 2006). Another systemic intervention with
successful outcomes in multiple postconflict settings is integrating mental health services into more routine care delivery or primary care systems, discussed below.
Integrating Mental Health in Postconflict Settings
Addressing the growing burden of mental health needs in postconflict settings will be a continual challenge, especially since many of these locations may not have a high-functioning health care system and lack resources to dedicate to these problems. Many countries have already endured similar issues and challenges and provide both failures and successes from which to learn. As an example of how dire this problem can be, data show that ongoing exposure to conflict and violence in Gaza has resulted in nearly 70 percent of adolescents developing PTSD, 40 percent having moderate to severe levels of depression, and 95 percent having severe anxiety (Elbedour et al., 2007). While these levels seem shockingly high, many studies in the Middle East region confirm this alarming burden (Dimitry, 2011). To address the problem, money for mental health care is often focused at the hospital level, leading to an uneven distribution of resources. Decision makers in Gaza have made progress, however, in moving from a hospital focus toward more community-based services, as described for future systems in Chapter 3, and slowly integrating mental health into primary health care (Saymah et al., 2015). This design is also supported for other postconflict settings, where typical efforts are narrowly focused on a population or a single intervention. Instead, it would be better if leaders of those efforts systematically took a longer-term perspective and employed multilevel care packages with entry points outside of typical health care settings, focused instead in the community (Betancourt et al., 2010; Jordans et al., 2009). Other studies also have confirmed the feasibility of having primary care workers take on mental health care in multiple postconflict settings around the world (Mendenhall et al., 2014).
Unsuccessful Interventions
The levels of some inputs to the health care delivery system, as described in the earlier discussion of service readiness, are assumed to be associated with high quality. However, research has shown that this is not always the case. In the previously described Afghanistan study looking at the quality of primary care services, for example, researchers found that neither remoteness, facility type, in-service training, nor timely salaries were associated with a change in quality (Hansen et al., 2008). Understanding what interventions have no effect, at least in a given context, is important so that countries can target limited resources toward efforts that do move
the needle on outcomes and do not simply streamline processes or improve access without yielding results for patients.
Building on Lessons Learned from Other Regions
Although it has faced many years of war, Afghanistan has made important strides in reducing maternal and infant mortality despite ongoing insecurity, and that experience offers lessons for other states in similar positions. These improvements have been attributed to the Afghanistan Ministry of Health’s service delivery model, investments in data collection and verification, and government ownership (World Bank, 2018b). Together with NGO Health Cluster partners and WHO, the Ministry of Health assembled an essential package of health interventions called the Basic Package of Health Services (BPHS). The BPHS defines which services should be provided by which type of primary health care facility and establishes standards that need to be met. Since its creation, BPHS services are now available to 77 percent of the Afghan population (WHO, 2018a).
As seen in countries such as Rwanda and Timor-Leste, the quickest option for providing health care services to populations following civil war or nationwide tragedy and strife is through contracting with national or international NGOs. At some point, however, this option becomes unsustainable and less attractive as the country recovers and regains ownership of its governing mechanisms. In Timor-Leste, after periods of prolonged conflict, a citizen-run interim health authority was established, which enabled donors to shift funding away from NGOs to the newly established ministry. This shift phased out the NGOs and built the local capacity needed for a strong public system. Researchers found evidence that use of health services grew during and after the ministry’s implementation (Alonso and Brugha, 2006). However, such a transfer of authority and management could be precarious in these recovering settings, and additional research is needed to verify whether this transition is one that can be applied at scale and what considerations all parties will need to take into account throughout the process for it to be successful.
Established in Japan for decades, a simple tool such as a maternal and child health (MCH) handbook can be used in settings of extreme adversity, with important implications for improving care. The Japan International Cooperation Agency (JICA) began supporting the development of such a handbook in Indonesia in 1993; it was adopted nationwide and informed future iterations in more low-resource settings (Katsuma, n.d.). In 2008, an Arabic version of the handbook was introduced to refugees in Palestine in cooperation with JICA and the United Nations Children’s Fund, and a modern update was digitized for smartphones. Use of the handbook in Palestine was tested for its association with quality of antenatal services
in 2017. Researchers found that handbook users were significantly more likely to receive “all three kinds of medical tests and … information on five or more health education topics,” even after adjusting for confounders (Kitabayashi et al., 2017, p. 2161). Such a handbook can act as a portable checklist, with the patient at the center, to promote the committee’s design principles of coordination and integration and improved adherence to standards of care. This proof of concept for MCH is now being broadened to lifestyle-related diseases such as the NCD priorities mentioned previously in this chapter. If information on these conditions can be blended and accessible via smartphone, refugees can be empowered to take greater ownership of and participate in decision making on their health, managing their own health data across national borders even when their environment offers little in the way of health care infrastructure.
Multistakeholder Collaboration
To provide high-quality care in a coordinated manner in such austere and extremely chaotic settings, collaboration among stakeholders is paramount. In the Mosul study cited earlier, for example, respondents highlighted cost and transportation as top barriers to seeking formal health care (Lafta et al., in press). If services within the community are not accessible, they will not be used, making it easier for other, less qualified actors to fill the void. Afghanistan was able to have a national health policy in place just 3 years after the collapse of the Taliban. Much of that accomplishment was attributable to increased partnerships with NGOs, which led to improved quality of health care for the poorest in Afghanistan (Hansen et al., 2008). By contrast, Iraq is struggling to build a central health care system, and with no health insurance yet in place, everyone currently pays for private health care out of pocket (Al Hilfi et al., 2013). Compounding these financial challenges for the population is the fact that there are no guidelines or regulations for private hospitals, making quality difficult to assure. Although a quality unit is built into the Iraq Ministry of Health, the culture has not yet caught up with the policy change, and there are no national performance standards. With the anticipated rapid development of the private sector in health care worldwide, researchers worry that the public sector will be at a great disadvantage unless quality improvement is taken more seriously (Al Hilfi et al., 2013).
Critical Nature of Validation
Given the clear lack of evidence for quality status and improvement interventions in low-resource settings, let alone within settings of extreme adversity, the argument for more research can easily be made. However,
the context is important in all situations, and is no less important here. Although rigorous observational studies and clinical trials may yield findings that could be applied in settings of extreme adversity, they need to be validated by those practicing on the ground. Experts working in the field, whether NGOs, local providers, or multilateral representatives, can serve as the source for vetting interventions and findings that are proven successful in sanitized study settings.
SUMMARY AND RECOMMENDATIONS
While the lack of available data and challenging environments make it difficult for leaders and policy makers to know where to begin, there are successes and new approaches emerging from many regions. Additional research investment can augment this knowledge base even further. In addition, global learning networks and collaboratives can provide opportunities to share lessons across countries and settings. As emphasized throughout this report, however, contextual application of evidence and interventions from various environments is critical. There will be no “magic bullet” solution to these complex problems; rather, each country and health system will need to tailor its approaches to best fit the needs of its own citizens and populations.
Care in the Informal Sector
Vast numbers of people receive care from IPs worldwide, with utilization rates in some countries exceeding 75 percent. Much is still unknown about the precise numbers of IPs and about who is using them, but the research that is available makes clear that the quality of their care is poor, although often no worse than that of the formal sector. This is a health care challenge, but one that also represents an opportunity. Researchers have identified promising interventions for addressing the quality concerns within the informal health care sector while also relieving pressure on the formal system. These include
- working with drug vendors, one of the most common types of IP, to bring them into the mainstream system so they can provide appropriate drug dosages and referrals to reach poorer populations;
- using institutional training, registration, and licensing to make traditional medicine practitioners more accountable and reduce the cost of care in the formal system;
- including IPs in counting of providers so more knowledge can be generated about their practices and patients;
- training traditional healers to improve their knowledge and patient management and referral practices for sexually transmitted diseases and HIV;
- defining scopes of practice for various types of IPs where possible and appropriate; and
- increasing opportunities for research to inform the regulation of traditional medicine.
Conclusion: Governments and leaders in the formal health care system need to acknowledge that informal providers in all countries deliver a significant proportion of health services. Bringing these providers closer to mainstream care delivery to the extent possible so they can be monitored, measured, and improved can help improve the quality of their care for large numbers of people.
Recommendation 5-1: Incorporate the Informal Care Sector in the Pursuit of Improved Care Delivery
Country governments should integrate informal care providers into their national health strategies and quality monitoring and improvement efforts. To this end, they should acknowledge that these informal providers exist and undertake efforts to assess and improve the care they provide, such as through education, training, and incentives, to the full extent possible.
Health Care in Settings of Extreme Adversity
About 2 billion people live in fragile states and conflict settings worldwide. Their access to high-quality care is unreliable at best, often nonexistent. Research on health care in these contexts is scarce, leaving health care leaders and providers with an unclear picture of what interventions lead to best outcomes and what to prioritize with limited funds. Although not robust and generalizable enough to apply in every case, evidence has emerged that offers lessons to guide leaders in improving quality in these contexts, as described in this chapter. In summary, those lessons include
- improved quality in Afghanistan when both patient and provider were female, and through the use of community councils that managed oversight of health care facilities;
- the benefit of increased supportive, supervisory visits in Afghanistan and Morocco;
- the potential to integrate mental health services into routine care delivery or primary care systems, especially with entry points in the community; and
- increased likelihood of receiving medical tests and information on health topics as a result of providing refugees in Palestine handbooks with which to track their care.
Conclusion: Assuring health care quality in chaotic, unstable, or unsafe settings where government is often weak or inconsistent in its role of delivering and overseeing public services has long been wrongly deemed a luxury. Indeed, the opposite is true. Given the extreme vulnerability of the people in these settings, providing them with high-quality care is arguably more important than is the case anywhere else. There is an urgent need to understand what interventions work to improve care under conditions of extreme adversity so they can be implemented as soon as possible to reduce mortality, harm, human suffering, and the waste of already insufficient resources.
Recommendation 5-2: Make Settings of Extreme Adversity a High Priority
National governments, multilateral institutions, nongovernmental organizations (NGOs), bilateral donors, humanitarian stakeholders, and philanthropic donors should make studying and improving the quality of care in settings of extreme adversity a high priority. More specifically:
- The international humanitarian system, multilateral organizations, and NGOs should identify priorities for assessing the quality of care in these settings and develop strategies for its improvement. Emphasis should be placed on addressing conditions that are particularly burdensome in these settings, such as treating conflict-related trauma and mental illness, optimizing the patient experience to ensure trust in providers, protecting providers from harm, and adequately managing chronic diseases.
- The National Institutes of Health (NIH) and other research funders should support primary and implementation research aimed at identifying what interventions work and in what contexts to improve health outcomes in fragile states and austere environments.
- Multilateral organizations and the United Nations System should create multistakeholder collaborations for the purposes of reviewing and vetting the available evidence; developing consensus on promising interventions for improvement; and identifying issues of leadership and accountability for quality of care in particular circumstances, such as conflict zones, humanitarian crises, and fragile states.
REFERENCES
Abdullahi, A. A. 2011. Trends and challenges of traditional medicine in Africa. African Journal of Traditional, Complementary, and Alternative Medicines 8(5 Suppl.):115–123.
AFRO (WHO Regional Office for Africa). 2011. Progress report on decade of traditional medicine in the African region. Brazzaville, Congo: AFRO.
Ahmed, S. M., M. A. Hossain, and M. R. Chowdhury. 2009. Informal sector providers in Bangladesh: How equipped are they to provide rational health care? Health Policy and Planning 24(6):467–478.
Akseer, N., Z. Bhatti, T. Mashal, S. Soofi, R. Moineddin, R. E. Black, and Z. A. Bhutta. 2018. Geospatial inequalities and determinants of nutritional status among women and children in Afghanistan: An observational study. The Lancet Global Health 6(4):e447–e459.
Al Hilfi, T. K., R. Lafta, and G. Burnham. 2013. Health services in Iraq. The Lancet 381(9870):939–948.
Alonso, A., and R. Brugha. 2006. Rehabilitating the health system after conflict in East Timor: A shift from NGO to government leadership. Health Policy and Planning 21(3):206–216.
Australian Bureau of Statistics. 2008. Australian social trends, 2008: Complementary therapies: Australian Bureau of Statistics. http://www.ausstats.abs.gov.au/Ausstats/subscriber.nsf/0/DE5DE30C9CF6E5E3CA25748E00126A25/$File/41020_2008.pdf (accessed June 3, 2018).
Bamidele, J. O., W. O. Adebimpe, and E. A. Oladele. 2009. Knowledge, attitude and use of alternative medical therapy amongst urban residents of Osun State, southwestern Nigeria. African Journal of Traditional, Complementary, and Alternative Medicines 6(3):281–288.
Barot, S. 2017. In a state of crisis: Meeting the sexual and reproductive health needs of women in humanitarian situations. Guttmacher Policy Review 20:24–30.
Betancourt, T. S., R. T. Brennan, J. Rubin-Smith, G. M. Fitzmaurice, and S. E. Gilman. 2010. Sierra Leone’s former child soldiers: A longitudinal study of risk, protective factors, and mental health. Journal of the American Academy of Child and Adolescent Psychiatry 49(6):606–615.
Bhuiya, A., ed. 2009. Health for the ruralmasses: Insights from Chakaria. https://assets.publishing.service.gov.uk/media/57a08b63ed915d622c000c65/FHSbookHealthforRuralMasses.pdf (accessed June 3, 2018).
Björkman, M., and J. Svensson. 2009. Power to the people: Evidence from a randomized field experiment on community-based monitoring in Uganda. The Quarterly Journal of Economics 124(2):735–769.
Bloom, G., H. Standing, H. Lucas, A. Bhuiya, O. Oladepo, and D. H. Peters. 2011. Making health markets work better for poor people: The case of informal providers. Health Policy Plan 26(Suppl. 1):i45–i52.
Brock, J. M., K. Leonard, and A. Lange. 2012. Generosity norms and intrinsic motivation in health care provision: Evidence from the laboratory and field. http://www.ebrd.com/downloads/research/economics/workingpapers/wp0147.pdf (accessed June 3, 2018).
Center for Health Market Innovations. 2010. Summary: Study on the role of informal providers in health care delivery. https://healthmarketinnovations.org/sites/default/files/IP%20Study_Summary%20for%20HSR_10%2010%2010.pdf (accessed June 3, 2018).
Chawla, S., S. Kurani, S. M. Wren, B. Stewart, G. Burnham, A. Kushner, and T. McIntyre. 2018. Electricity and generator availability in LMIC hospitals: Improving access to safe surgery. Journal of Surgical Research 223:136–141. doi:10.1016/j.jss.2017.10.016.
Cross, J., and H. N. MacGregor. 2010. Knowledge, legitimacy and economic practice in informal markets for medicine: A critical review of research. Social Science & Medicine 71(9):1593–1600.
Das, J., and A. Mohpal. 2016. Socioeconomic status and quality of care in rural India: New evidence from provider and household surveys. Health Affairs 35(10). doi:10.1377/hlthaff.2016.0558.
Das, J., A. Holla, V. Das, M. Mohannan, D. Tabak, and B. Chan. 2012. In urban and rural India, a standardized patient study shows low levels of provider training and huge quality gaps. Health Affairs 31(12):2774–2784.
Das, J., A. Kwan, B. Daniels, S. Satyanarayana, R. Subbaraman, S. Bergkvist, R. K. Das, V. Das, and M. Pai. 2015. Use of standardised patients to assess quality of tuberculosis care: A pilot, cross-sectional study. The Lancet Infectious Diseases 15(11):1305–1313.
Das, J., A. Chowdhury, R. Hussam, and A. V. Banerjee. 2016. The impact of training informal health care providers in India: A randomized controlled trial. Science 354(6308). doi:10.1126/science.aaf7384.
Demaio, A., J. Jamieson, R. Horn, M. de Courten, and S. Tellier. 2013. Non-communicable diseases in emergencies: A call to action. PLoS Currents 5.
Dimitry, L. 2011. A systematic review on the mental health of children and adolescents in areas of armed conflict in the Middle East. Child: Care, Health and Development 38(2):153–161.
Doocy, S., E. Lyles, L. Akhu-Zaheya, A. Oweis, N. Al Ward, and A. Burton. 2016. Health service utilization among Syrian refugees with chronic health conditions in Jordan. PLoS One 11(4):e0150088.
Duvenhage, A., and G. Louw. 2016. The present-day scope of practice and services of the traditional healer in South Africa. Australasian Medical Journal 9(12):481–488.
Edward, A., B. Kumar, H. Niayesh, A. J. Naeem, G. Burnham, and D. H. Peters. 2012. The association of health workforce capacity and quality of pediatric care in Afghanistan. International Journal for Quality in Health Care 24(6):578–586.
Elbedour, S., A. J. Onwuegbuzie, J. Ghannam, J. A. Whitcome, and F. A. Hein. 2007. Post-traumatic stress disorder, depression, and anxiety among Gaza Strip adolescents in the wake of the second uprising (intifada). Child Abuse & Neglect 31(7):719–729.
Embrey, M., C. Vialle-Valentin, A. Dillip, B. Kihiyo, R. Mbwasi, I. A. Semali, J. C. Chalker, J. Liana, R. Lieber, K. Johnson, et al. 2016. Understanding the role of accredited drug dispensing outlets in Tanzania’s health system. PLoS One 11(11):e0164332.
FSI (Fragile States Index). 2017. Fragile States Index: The fund for peace. http://fundforpeace.org/fsi (accessed June 3, 2018).
Gautham, M., K. M. Shyamprasad, R. Singh, A. Zachariah, R. Singh, and G. Bloom. 2014. Informal rural healthcare providers in north and south India. Health Policy and Planning 29(Suppl. 1):i20–i29.
George, A., and A. Iyer. 2013. Unfree markets: Socially embedded informal health providers in northern Karnataka, India. Social Science & Medicine 96:297–304.
Giacaman, R., R. Khatib, and L. Shabaneh. 2009. Health status and health services in the occupied Palestinian territory. The Lancet 373(9666):837–849. doi:10.1016/S0140-6736(09)60107-0.
Glenton, C., I. B. Scheel, S. Pradhan, S. Lewin, S. Hodgins, and V. Shrestha. 2010. The female community health volunteer programme in Nepal: Decision makers’ perceptions of volunteerism, payment and other incentives. Social Science & Medicine 70(12):1920–1927.
Gopalan, S. S., S. Mohanty, and A. Das. 2012. Assessing community health workers’ performance motivation: A mixed-methods approach on India’s Accredited Social Health Activists (ASHA) programme. BMJ Open 2(5). doi:10.1136/bmjopen-2012-001557.
Hansen, P. M., D. H. Peters, A. Edward, S. Gupta, A. Arur, H. Niayesh, and G. Burnham. 2008. Determinants of primary care service quality in Afghanistan. International Journal for Quality in Health Care 20(6):375–383.
Hughes, R., C. R. Chandler, L. J. Mangham-Jefferies, and W. Mbacham. 2013. Medicine sellers’ perspectives on their role in providing health care in north-west Cameroon: A qualitative study. Health Policy and Planning 28(6):636–646.
IANS (Indo-Asian News Service). 2017. India’s ASHA workers: The backbone of primary healthcare in the country’s 6,00,000 villages. Healthcare, November 1. https://www.thenewsminute.com/article/indias-asha-workers-backbone-primary-healthcare-country-s-600000-villages-70904 (accessed August 14, 2018).
IAWG (Inter-Agency Working Group) on Reproductive Health in Crises. 2015. Reproductive health in the changing humanitarian context: Key findings from the IAWG on Reproductive Health in Crises’ 2012–2014 global evaluation. http://www.who.int/hac/global_health_cluster/events/IAWG_Global_Evaluation.pdf (accessed June 3, 2018).
ICDDR, B (International Centre for Diarrhoeal Disease Research, Bangladesh). 2009. Health for the rural masses: Insights from Chakaria. Edited by A. Bhuiyas. Dhaka, Bangladesh: ICDDR, B.
Jordans M. J., W. A. Tol, I. H. Komproe, and J. V. De Jong. 2009. Systematic review of evidence and treatment approaches: Psychosocial and mental health care for children in war. Child and Adolescent Mental Health 14(1):2–14.
Karasapan, O. 2016. Syria’s mental health crisis. https://www.brookings.edu/blog/futuredevelopment/2016/04/25/syrias-mental-health-crisis (accessed May 18, 2018).
Kasteng, F., S. Settumba, K. Källander, and A. Vassall. 2016. Valuing the work of unpaid community health workers and exploring the incentives to volunteering in rural Africa. Health Policy and Planning 31(2):205–216.
Katsuma, Y. n.d. What is required to ensure the human security of refugees? http://www.yomiuri.co.jp/adv/wol/dy/opinion/international_171016.html (accessed June 3, 2018).
Kiapi-iwa, L., and G. J. Hart. 2004. The sexual and reproductive health of young people in Adjumani district, Uganda: Qualitative study of the role of formal, informal and traditional health providers. AIDS Care 16(3):339–347.
Kitabayashi, H., C. Chiang, A. A. A. Al-Shoaibi, Y. Hirakawa, and A. Aoyama. 2017. Association between maternal and child health handbook and quality of antenatal care services in Palestine. Maternal and Child Health Journal 21(12):2161–2168.
Konde-Lule, J., S. N. Gitta, A. Lindfors, S. Okuonzi, V. O. N. Onama, and B. C. Forsberg. 2010. Private and public health care in rural areas of Uganda. BMC International Health and Human Rights 10:29.
Lafta, R., V. Cetorelli, G. Burnham. In press. Health and health seeking in Mosul during ISIS control and liberation: Results from a 40-cluster household survey.
Leatherman, S., S. Patel, J. Stutsman, and D. Jaff. In press. Health care quality in settings of extreme adversity: A review of the literature.
Leon, N., D. Sanders, W. Van Damme, D. Besada, E. Daviaud, N. P. Oliphant, R. Berzal, J. Mason, and T. Doherty. 2015. The role of “hidden” community volunteers in community-based health service delivery platforms: Examples from sub-Saharan Africa. Global Health Action 8:10.3402/gha.v3408.27214.
MAQARI (Medical Advice, Quality, and Availability in Rural India) Team. 2011. Mapping medical providers in India: Four key trends. New Dehli, India: Center for Policy Research.
Marquez, P. V. 2016. Mental health services in situations of conflict, fragility and violence: What to do? The World Bank, November 1. http://blogs.worldbank.org/health/mental-health-services-situations-conflict-fragility-and-violence-what-do (accessed May 18, 2018).
Mendenhall, E., M. J. De Silva, C. Hanlon, I. Petersen, R. Shidhaye, M. Jordans, N. Luitel, J. Ssebunnya, A. Fekadu, V. Patel, et al. 2014. Acceptability and feasibility of using nonspecialist health workers to deliver mental health care: Stakeholder perceptions from the prime district sites in Ethiopia, India, Nepal, South Africa, and Uganda. Social Science & Medicine 118:33–42.
Mohanan, M., M. Vera-Hernández, V. Das, S. Giardili, J. D. Goldhaber-Fiebert, T. L. Rabin, S. S. Raj, J. I. Schwartz, and A. Seth. 2015. The know-do gap in quality of health care for childhood diarrhea and pneumonia in rural India. JAMA Pediatrics 169(4):349–357.
Naimoli, J., A. K Rowe, A. Lyaghfouri, R. Larbi, and L. Aicha Lamrani. 2006. Effect of the integrated management of childhood illness strategy on health care quality in Morocco. International Journal for Quality in Health Care 18(2):134–144.
National Health Mission. n.d. About accredited social health activist (ASHA). http://nhm.gov.in/communitisation/asha/about-asha.html (accessed July 10, 2018).
OECD (Organisation for Economic Co-operation and Development). 2018a. States of fragility reports. http://www.oecd.org/dac/conflict-fragility-resilience/listofstateoffragilityreports.htm (accessed May 18, 2018).
OECD. 2018b. States of fragility reports. Republished with permission of OECD. Permission conveyed through Copyright Clearance Cetner, Inc. http://www.oecd.org/dac/conflictfragility-resilience/listofstateoffragilityreports.htm (accessed May 18, 2018).
Omaswa, F. 2006. Informal health workers—to be encouraged or condemned? Bulletin of the World Health Organization 84(2):81–160.
Pantoja, T., N. Opiyo, S. Lewin, E. Paulsen, A. Ciapponi, C. S. Wiysonge, C. A. Herrera, G. Rada, B. Peñaloza, L. Dudley, M.-P. Gagnon, S. Garcia Marti, and A. D. Oxman. 2017. Implementation strategies for health systems in low-income countries: An overview of systematic reviews. The Cochrane Database of Systematic Reviews (9):CD011086.
Prasada Rao, U., S. Nallapu, and S. Rao. 2017. The rural medical practitioner of India. Journal of Evolution of Medical and Dental Sciences 6(74):5321–5323. doi:10.14260/Jemds/2017/1154.
Raphelson, S. 2018. Venezuela’s health care system ready to collapse amid economic crisis. NPR, February 1. https://www.npr.org/2018/02/01/582469305/venezuelas-health-care-system-ready-to-collapse-amid-economic-crisis (accessed May 18, 2018).
Reuters Staff. 2017. Venezuela’s Maduro asks U.N. to help ease medicine shortages. Reuters, March 25. https://www.reuters.com/article/us-venezuela-health/venezuelas-maduro-asks-u-n-to-help-ease-medicine-shortages-idUSKBN16W063 (accessed May 18, 2018).
Rosen, K. 2018. “Everyone’s sick here”: The abysmal state of health care for Palestinian refugees. Pacific Standard, May 15. https://psmag.com/news/the-abysmal-state-of-healthcare-for-palestinian-refugees (accessed June 3, 2018).
Samuels, F., N. Jones, and B. Abu Hamad. 2017. Psychosocial support for adolescent girls in post-conflict settings: Beyond a health systems approach. Health Policy and Planning 32(Suppl. 5):v40–v51.
Saymah, D., L. Tait, and M. Michail. 2015. An overview of the mental health system in Gaza: An assessment using the World Health Organization’s Assessment Instrument for Mental Health Systems (WHO-AIMS). International Journal of Mental Health Systems 9(1):4.
Shah, N. M., W. R. Brieger, and D. H. Peters. 2011. Can interventions improve health services from informal private providers in low and middle-income countries? A comprehensive review of the literature. Health Policy and Planning 26(4):275–287.
Sieverding, M., and N. Beyeler. 2016. Integrating informal providers into a people-centered health systems approach: Qualitative evidence from local health systems in rural Nigeria. BMC Health Services Research 16:526.
Sotunsa, J. O., M. Vidler, D. O. Akeju, M. O. Osiberu, E. O. Orenuga, O. T. Oladapo, R. Qureshi, D. Sawchuck, O. O. Adetoro, P. von Dadelszen, and O. A. Dada. 2016. Community health workers’ knowledge and practice in relation to pre-eclampsia in Ogun State, Nigeria: An essential bridge to maternal survival. Reproductive Health 13(2):108.
Sudhinaraset, M., M. Ingram, H. K. Lofthouse, and D. Montagu. 2013. What is the role of informal healthcare providers in developing countries? A systematic review. PLoS One 8(2):e54978.
Tawfik, Y., J. Nsungwa‐Sabitii, G. Greer, J. Owor, R. Kesande, and S. Prysor‐Jones. 2006. Negotiating improved case management of childhood illness with formal and informal private practitioners in Uganda. Tropical Medicine & International Health 11(6):967–973.
Trejos, A. 2017. Amid Venezuela political crisis, shortages of medicine soar. USA Today, June 22. https://www.usatoday.com/story/news/world/2017/06/22/venezuela-medicalshortages-doctors-health-care/103039928 (accessed May 18, 2018).
UNHCR (The UN Refugee Agency). 2015. World at war: UNHCR global trends. Geneva, Switzerland: UNHCR.
UNHCR. 2016. Global trends: Forced displacement in 2015. Geneva, Switzerland: UNHCR.
Waterson, T., and D. Nasser. 2017. Access to healthcare for children in Palestine. BMJ Paediatrics Open 1(1):e000115. doi:10.1136/bmjpo-2017-000115.
WHO (World Health Organization). 2003. Traditional medicine: Report by the secretariat. Geneva, Switzerland: WHO.
WHO. 2013. WHO traditional medicine strategy 2014–2023. Hong Kong, China: WHO.
WHO. 2014. Alliances for health policy and systems research flagship report 2014. Geneva, Switzerland: WHO.
WHO. 2018a. From trauma to recovery: Addressing emergency care in Afghanistan. http://www.who.int/features/2018/emergency-care-afghanistan/en (accessed May 18, 2018).
WHO. 2018b. Rohingya refugee crisis in Cox’s Bazar, Bangladesh: Health sector bulletin. Health Sector Bulletin 3. https://reliefweb.int/report/bangladesh/rohingya-refugee-crisis-cox-s-bazar-bangladesh-health-sector-bulletin-no-04-period (accessed June 2, 2018).
WHO. 2018c. Sexual and reproductive health and rights of refugees and migrants. http://www.who.int/reproductivehealth/news/srhr-refugees-migrant/en (accessed May 18, 2018).
World Bank. 2018a. Conflict and fragility. http://ida.worldbank.org/theme/conflict-and-fragility (accessed May 18, 2018).
World Bank. 2018b. Progress in the face of insecurity: Improving health outcomes in Afghanistan. Washington, DC: World Bank.
WPRO (WHO Regional Office for the Western Pacific). 2012. The regional strategy for traditional medicine in the Western Pacific (2011–2020). Manila, Philippines: WPRO.
Zulliger, R. 2014. Ethiopian community health worker programs. http://www.chwcentral.org/blog/ethiopian-community-health-worker-programs (accessed June 20, 2018).
This page intentionally left blank.