3
The Family and Community Landscape
The workshop’s second panel session featured three speakers. Jennifer Wolff, professor of health policy and management at the Johns Hopkins Bloomberg School of Public Health, addressed how adults and caregivers need to have difficult conversations to make important decisions. Stephen Thomas, professor of health services administration and director of the Maryland Center for Health Equity at the University of Maryland, College Park, then spoke about how health literacy can be a tool for easing disparities among vulnerable older adults. In the session’s final presentation, Nora Super, director of the Aging and Disability Business Institute of the National Association of Area Agencies on Aging, discussed community living and independence for older adults. An open discussion moderated by Terri Ann Parnell, principal and founder of Health Literacy Partners, followed the three presentations.
GIVING VOICE TO OLDER ADULTS AND CAREGIVERS: DIFFICULT CONVERSATIONS AND DECISIONS1
Jennifer Wolff began her presentation by discussing the broader context of population aging, noting that population aging is a global phenomenon, not just a demographic trend affecting the United States. Today, for the first time in history, there are more individuals aged 65 and older than there are
___________________
1 This section is based on the presentation by Jennifer Wolff, professor of health policy and management at the Johns Hopkins Bloomberg School of Public Health, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
children under age 5 (see Figure 3-1), and the population of older adults is known for its heterogeneity, she added. “I want to emphasize that many older adults have very high health literacy and continue to function at high levels in all facets of life, from academics to business to public service and politics,” said Wolff.
Despite the promise of more years and good health, Wolff said the reality is that most individuals do accumulate age-related deficits, particularly as they enter their 8th, 9th, and 10th decade of life. For example, the numbers of Americans with Alzheimer’s disease and related dementias is expected to roughly triple over the coming 30 years from about 5 million Americans today to 14 million by 2050, driven largely by the aging of the baby boomers into very old ages. “How we as a society plan to meet the needs of the growing numbers of older Americans with complex health needs and disabilities in the decades to come is an important issue that will only become more pressing in the coming years,” said Wolff.
Although heterogeneity is the defining feature of older adults as a population, they are at greater risk on average for being less equipped to successfully navigate health system demands, explained Wolff. As a cohort, older adults tend to be less educated than working-age adults and are less likely to have technology experience and the skills and access to a computer
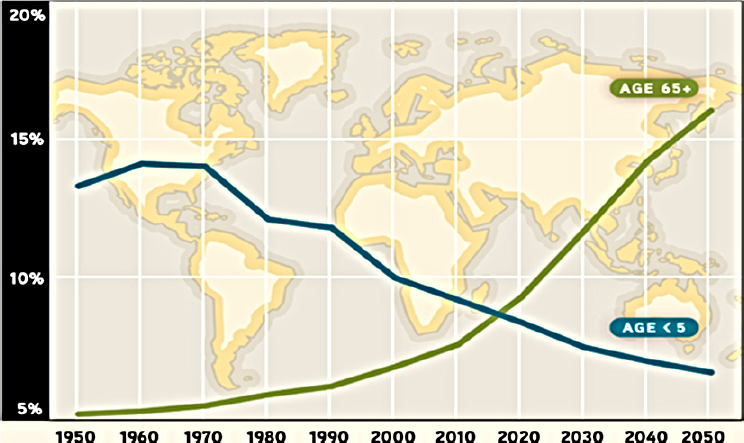
SOURCES: As presented by Jennifer Wolff at the workshop on Health Literacy and Older Adults on March 13, 2018; UN DESA, 2005.
or a mobile device. At the same time, they are at greater risk for age-related physiologic impairments that affect cognitive, hearing, and visual function in ways that leave them less able to participate actively in verbal dialogue, as well as to attain and process information from print content. Wolff said,
Because older adults are at higher risk of low health literacy, they in many ways face double or even triple jeopardy in that they are less able to attain and process information to make appropriate health decisions while confronting a broader range of complex health decisions that bring them into frequent contact with the care delivery system.
Older adults also face a health insurance environment that is more complex than for typical working-age adults, she added. Citing a 2006 paper (Hanoch and Rice, 2006) that argues that Medicare beneficiaries, in the aftermath of the introduction of the Medicare Part D benefit, are faced with too many choices, she noted that income and eligibility intersect in a range of highly complex decisions that can hamper rational decision making, particularly among individuals who have lower educational attainment or cognitive impairment (Kuye et al., 2013).
Although low health literacy can affect an important but relatively narrow set of decisions related to enrollment in a health insurance plan, the adequacy of health literacy does affect a much broader range of decisions, said Wolff. These many decisions include routine daily activities, such as when and how to access appropriate and timely medical care, knowing and understanding treatments and adhering to them, and accessing publicly available benefits and community service. Low health literacy can make it difficult for older adults to hire and fire direct care workers who can help them manage functional impairments and to prepare for future long-term care and medical needs in the event of incapacity by purchasing private long-term care insurance plans or engaging in advanced care planning.
Shifting gears, Wolff addressed the role that families often play in bridging health literacy deficits. Citing the Institute of Medicine report Retooling for an Aging America (IOM, 2008), Wolff pointed out that family caregivers typically fall into that role accidentally and without any formal training. The report, she said, contrasts the family caregiver workforce with the health professional workforce, which is well educated and credentialed to function in a narrower scope of practice and typically in settings specifically intended for care delivery. The more recent National Academies report Families Caring for an Aging America (NASEM, 2016) makes a number of important recommendations that call for specific research, policy, and practice change to support a shift toward family-centered care. Some of these recommendations, she said, may be relevant to the roundtable’s deliberations.
One major finding from the latter report is that family-centered care is the reality in which many older adults manage their health. “We know, for example, that two-thirds of older adults with disabilities manage their health in the community with the help of family caregivers,” said Wolff, who was a member of the committee that authored the report. She and her colleagues have found that about 40 percent of older adults regularly attend medical appointments with a family or other unpaid companion (Wolff and Roter, 2008, 2011; Wolff and Spillman, 2014; Wolff et al., 2012). These adults, she said, tend to be sicker, have a lower education level, and are more likely to have cognitive impairment. Family members are not present just at a single visit, but tend to be involved consistently over time, which she said speaks to the role that family members play in coordinating care. Her research, she said, showed that the roles family members play are highly varied and can both benefit as well as detract from the quality of communication (Wolff and Roter, 2012; Wolff et al., 2014, 2015, 2017b). “For example, we know that when older adults with lower mental health function attend medical visits with a family member, those visits tend to be shorter and there is less discussion of psychosocial issues,” said Wolff.
In one study, she and a colleague asked about older adults’ engagement in health care activities and how they prefer to involve both doctors as well as family members and friends in medical decisions (Wolff and Boyd, 2015). They found that more than two-thirds of older adults reported managing their health independently, nearly 20 percent co-managed their health with family or friends, and 11 percent reported delegating management of their health to family or others (see Figure 3-2). For each of these three groups, Wolff and her colleague examined preferences for making medical decisions independently. More than three-quarters of older adults who self-manage their health report making medical decisions independently, whereas less than half of older adults who report co-managing their health or delegating their health management activities to others make decisions independently. Wolff said,
Collectively, these data speak to the heterogeneity of older adults and support the notion that respecting older adults’ preferences mean predominantly different things to different people. For some, it means respecting patients’ autonomy. For others, it means either engaging families collaboratively or allowing families to make decisions on behalf of the older adult.
One of the major conclusions of Families Caring for an Aging America was that there are numerous challenges to providing structural support for family caregivers and care delivery, said Wolff. For example, the traditional entrenched systems that govern financing and delivery of services are not well aligned to support family caregivers. In addition, the bioethical and
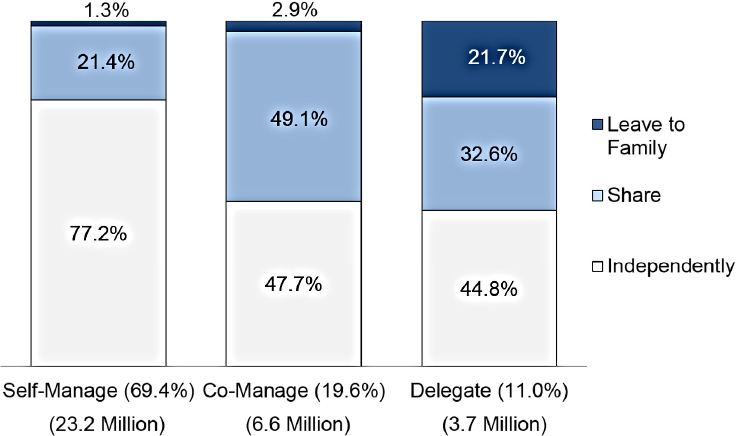
SOURCES: As presented by Jennifer Wolff at the workshop on Health Literacy and Older Adults on March 13, 2018; Wolff and Boyd, 2015.
legal regulatory frameworks that prioritize patient privacy and the protection of personal health information often impede access for family members despite the fact that it may be appropriate and beneficial when they are involved in coordination of care or managing medications or prescribed treatments for older adults in the community, she added. Moreover, when providers are formulating care plans that will require assistance in bridging deficits in physical or cognitive function, family members typically are not involved in those discussions. “As a result,” said Wolff, “the caregiver’s ability or knowledge to manage care is of questionable veracity or simply not asked for.”
The lack of a defined role for family members in care delivery in both face-to-face and electronic interactions often leaves them in an adversarial position with providers when it comes to advocating on the behalf of a patient, having a voice in care delivery, or being able to access information needed to manage care effectively. To help remedy this situation, Wolff and her colleagues have been iteratively developing and testing a patient/family agenda-setting checklist that is meant to be completed in the waiting room in advance of a medical encounter. The strategy, she explained, is predicated on the idea that these family members, or companions, are motivated to support patients during medical visits, but they may not know about the
patient’s concerns about the encounter as well as the patient’s preferences for communication assistance.
The checklist takes the patient and family through two different activities designed to get them on the same page by aligning their perspectives on the agenda for the visit and clarifying the role of the companion in the visit. A pilot study, which excluded older adults with significant cognitive impairment, found that this approach was feasible, acceptable, and led to improvements in the patient-centeredness of care from coded audio tapes of medical visits (Wolff et al., 2014). A subsequent study, just completed, focused on older adults with cognitive impairment in primary care and also found promising results. Overwhelmingly, said Wolff, patients wanted family members to play an active role in communicating during the visit. The study found that patients’ and families’ concerns for their visit sometimes aligned, but sometimes did not. Patients, she said, were more concerned about memory problems and trouble concentrating or making decisions, while families were more concerned about bladder or bowel problems and planning for serious illness or progression of current illness.
Wolff concluded her presentation by commenting on strategies for engaging families in electronic communication through a consumer-oriented patient portal. As Zimmerman mentioned in the first panel, electronic interactions are increasingly becoming a mainstream mode of communication, but older adults often do not have enough technology skills and access to technology to be able to engage in electronic interactions. There are several reasons, however, that engaging families through the patient portal could be beneficial in terms of capturing and respecting patients’ preferences for involving family in terms of engaging family, she said. Many EHR vendors even offer the capacity to allow patients to enroll family care partners and to provide them with their own identity credentials.
In studies conducted in partnership with the Geisinger Health System, Wolff and her colleagues surveyed Geisinger patients who had registered for the patient portal and had shared access with a family member or friend. They found that more than a decade after this functionality became available, less than 1 percent of adult patients had shared access to their patient portal account with a family member or friend (Wolff et al., 2016b). Patients’ motivations for sharing access varied widely by age, said Wolff, with the older the individuals, the more likely the reason for sharing access was that the patients themselves did not use a computer (see Figure 3-3). Older individuals were also more likely to report that the care partner helped them to manage their health (Wolff et al., 2016a). Wolff and her colleagues surveyed care partners and found that they were far less likely to be suspected of having low health literacy (Wolff et al., 2017a). In general, care partners had more education, higher levels of Internet use, and more regular use of the patient portal (see Figure 3-4).
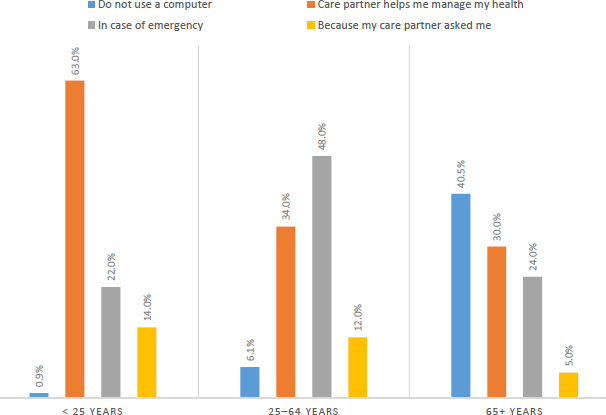
SOURCES: Adapted from a presentation by Jennifer Wolff at the workshop on Health Literacy and Older Adults on March 13, 2018; Wolff et al., 2016a.
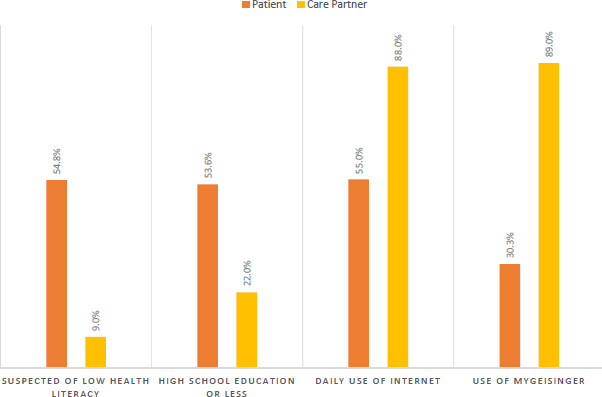
SOURCES: Adapted from a presentation by Jennifer Wolff at the workshop on Health Literacy and Older Adults on March 13, 2018; Wolff et al., 2017a.
In summary, Wolff said that older adults are best characterized by heterogeneity. They vary widely in health literacy, and many desire or require family when sharing information with providers of care, making health care decisions, and managing their health. Health system processes to recognize, engage, and support families of older adults are notably absent, she said, but engaging family may hold promise as a strategy to bridge health literacy challenges in older adults’ face-to-face encounters and electronic interactions.
HEALTH LITERACY AS A TOOL TO EASE DISPARITIES AMONG VULNERABLE OLDER ADULTS2
“Institutional commitment matters. It cannot be lip service,” said Stephen Thomas as he began his presentation. “The people we serve are tired of being studied because they are still suffering. That is my message to all of us investigators here. It is time to start taking action.” Health literacy, he added, should not be talked about without doing so in the context of the social determinants of health. The same is true of age, he said. “Age must be contextualized.” Thomas continued:
Our aim here is to move beyond a biomedical model to address the underlying drivers of these disparities, address issues such as breaking the cycle of poverty, increase access to quality care, eliminate environmental hazards in homes and neighborhoods, and implement interventions that have been tailored to the very communities we are trying to reach.
In his opinion, everyone attending the workshop should be ashamed and sad that so much of the accumulated research has not been implemented to address health disparities, and they should be angry at the decline of empathy in the health system. “There is something wrong in our system when we have lost the ‘caring’ part of care giving,” said Thomas.
According to Healthy People 2020, a health disparity is a “particular type of health difference that is closely linked with social, economic, and/or environmental disadvantage.”3 This difference, said Thomas, is often caused by something such as systemic discrimination. The flip side of health disparity is health equity, which again, according to Healthy People
___________________
2 This section is based on the presentation by Stephen Thomas, professor of health services administration and director of the Maryland Center for Health Equity at the University of Maryland School of Public Health, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
3 For more information, see www.healthypeople.gov/2020/about/foundation-healthmeasures/disparities (accessed April 3, 2018).
2020, is “the attainment of the highest level of health for all people.”4 It is unfortunate, he added, that the highest attainable level in the United States is not the best in the world. “We should be ashamed about that, too,” said Thomas.
History matters, Thomas said, and these issues of health literacy and access to care have been present throughout the history of America, especially for African Americans. Booker T. Washington was the first to recognize that African Americans had to take charge of their own health, and from 1915 to 1951, he launched the National Negro Health Movement, which in the 1930s became the federal Office of Negro Health Works. In 1951, in the name of integration, the office was decommissioned, but in 1985, the Secretary of Health and Human Services created the Office of Minority Health with what Thomas said was “almost amnesia to the success of the Negro Health Movement.” He noted that many African Americans, not long out of slavery and still hampered by Jim Crow laws, could not read, but this movement worked because of the creative methods used to engage the population. “This experience should be harvested for what we should be doing today,” said Thomas.
Underlying health disparities, Thomas said, is an issue of trust in the medical profession, which is to be expected given the negative African American experience with the health care profession, including the Tuskegee Syphilis Study, among others. The Tuskegee Syphilis Study used sophisticated plain-language methods, not to empower the men enrolled in the study, but to get them to do what the researchers wanted them to do. “It was never a secret,” said Thomas. “They learned the cues of the community and manipulated them to get what they wanted.” Those same methods, however, can be used for good, which is part of what the NIH Bioethics Research Infrastructure Initiative is trying to do to build trust in the African American and other minority communities.5
The first generation of disparities research to achieve health equity documented the problem, and the second generation explained the reasons the problem exists. This workshop, said Thomas, has put cognitive decline on the table as one reason, and research has shown that poverty is another reason. Third generation research provides answers, such as those developed by the work with Geisinger that Wolff described. The problem, he said, is that “our science lives in our journals and is not being implemented,” which is why he and several colleagues have called for a fourth generation of disparities research (Thomas et al., 2011). This fourth generation of disparities research is tied to social determinants and recognizes
___________________
4 For more information, see www.healthypeople.gov/2020/about/foundation-healthmeasures/disparities (accessed April 3, 2018).
5 For more information, see www.buildingtrustumd.org (accessed April 3, 2018).
the role that race and poverty play and builds off the previous generation of research to act and restore credibility in the very communities that have lost trust in the medical and research professions.
To illustrate what acting looks like, Thomas first reminded the workshop of a 2001 federal campaign called Take a Loved One to the Doctor Day. This expensive program developed great materials and a good website, he said, but in the communities where health disparities are the greatest, people did not have a doctor. The basic idea, though, was good, and he and his collaborators have turned it on its head to produce Take a Health Professional to the People Day. “What we did was take physicians, nurses, pharmacists, the whole array of us, out of the hospital and we put them in Black barbershops and beauty salons,” Thomas explained. As an aside, he noted that no self-respecting African American barber would ever tell a customer that he would get them in and out in 15 minutes.
Thomas and his team have taken this one step further and created Health Advocates In-Reach and Research (HAIR), a network of 10 barber shops and beauty salons in African American neighborhoods in the Washington, DC, metropolitan area that hosts health professionals with the goal of reducing health disparities through community building and health education (Linnan et al., 2012). He and his team are now launching the National Association of Black Barbershops and Salons for Health to bring health professionals to a new place for engaging the nation’s most vulnerable citizens. As a final note, he pointed out that physicians would love to have the relationship with their patients that these barbers and salon operators have with their customers.
COMMUNITY LIVING, FOSTERING ENGAGEMENT, AND INDEPENDENCE6
Returning to the subject of aging, Nora Super first recounted the four key themes of the White House Conference on Aging, which was held in 2015: retirement security, healthy aging, long-term services and supports (LTSS), and elder justice.7 The White House’s focus on healthy aging focused on four main priorities: promoting health and preventing injury, optimizing cognitive health, maximizing independence, and promoting community and civic engagement. Although she has worked on healthy aging issues for years, she noted that when she served as executive director of the White
___________________
6 This section is based on the presentation by Nora Super, director of the Aging and Disability Business Institute of the National Association of Area Agencies on Aging, and the statements are not endorsed or verified by the National Academies of Sciences, Engineering, and Medicine.
7 For more information, see archive.whitehouseconferenceonaging.gov (accessed April 4, 2018).
House Conference on Aging, she learned about programs on aging at the Departments of Housing and Urban Development, Labor, Transportation, and Treasury, which she did not know existed. One piece of information from the discussions on preventive health services was that health professionals do not do a good job explaining for their older patients, particularly those from minority populations, what preventive services are available free for all Medicare beneficiaries.
Though the vast majority of people want to stay in their homes as they age, many will need support and assistance to do that. As a result, the need for support and services for older Americans will increase as people age (Freedman and Spillman, 2014a). In fact, said Super, a new study showed that 59 percent of the population over age 80 needs LTSS. For those who live in rural communities, there are big challenges to finding and accessing that support, challenges that are exacerbated by the fact that those communities themselves are aging. In some areas of the country, said Super, more than one-quarter of the population is over the age of 65. To help older adults find the supports they need, the National Association of Area Agencies on Aging (n4a) runs a national call center and the Eldercare Locator website.8 Most of the callers are older adults and not their caregivers, said Super, and the top reasons for calls include a need for transportation, home and community-based day services, housing options, medical services and supplies, and health insurance information.
The complexity of the Medicare and Medicaid systems can overwhelm many older adults regardless of education level, said Super, and yet Congress has threatened to eliminate federal funding for state insurance counseling programs that provide unbiased research and help patients navigate these systems. Transportation is another disconnect, she noted, between what older adults need to remain independent and what the health care system provides. Super noted that of the people who call the Eldercare Locator looking for help with transportation, the majority are seeking help for current needs for transportation to medical appointments, and yet many health care plans complain about no-show rates among older adults. As an example of how one community dealt with this problem, a Medicare Advantage plan partnered with a Boston area agency on aging program to arrange for transportation services to bring older adults to their medical appointments. One elderly wheelchair-bound patient who lived on a third floor and had regularly missed her appointments has never missed one since this program began.
Social isolation among older adults is an issue starting to be noticed by the research community and policy makers. One in five people over
___________________
8 For more information, see www.eldercare.acl.gov/Public/Index.aspx (accessed April 4, 2018).
age 50 is affected by isolation (AARP Foundation, 2014), and isolation is associated with functional decline and a 45 percent greater risk of death. Prolonged isolation, said Super, can be as bad for one’s health as smoking 15 cigarettes per day. She noted that Meals on Wheels America has observed that one in four people who receive their meals at home have dementia and live alone.
To address some of the issues that older Americans with dementia face, the White House Conference on Aging launched Dementia Friendly America, 1 of 75 initiatives to come from the conference.9 This program, modeled after Minnesota’s ACT on Alzheimer’s program10 and run by n4a, has the goal of catalyzing a movement to more effectively support those living with dementia and their care partners. Dementia Friendly America began with 8 pilot states that hoped to have 15 participating communities within the year, but the program exceeded its goal and now has more than 200 Dementia Friendly America communities in 37 states. Dementia, said Super, is an issue that cuts across racial, economic, and partisan boundaries.
The Aging and Disability Business Institute at n4a works to connect community-based organizations with the health care sector. Super explained that the health care sector has shown a growing interest in working on the social determinants of health, and community-based organizations are the experts in these areas, particularly in working with more complex patients, such as those with disabilities and older adults. By bringing health systems and community-based organizations together, the Business Institute hopes to teach each of those sectors how to talk to and work with one another. It offers a resource center that provides nuts and bolts instruction on how to structure service contracts, for example, and how to work toward making policy changes that can benefit those in need.
One of Super’s favorite programs, also launched at the White House Conference on Aging, is the Geriatric Workforce Enhancement Program developed by the Health Resources and Services Administration. This program aims to create a workforce that maximizes patient and family engagement and improves health outcomes for older adults by integrating geriatrics with primary care as a means of addressing the severe shortage of geriatricians. The program emphasizes creating and delivering community-based programs that will provide patients, families, and caregivers with knowledge and skills to improve health outcomes and the quality of care for older adults. One program in the Fort Worth area, for example, has brought together the University of North Texas Health Science Center, Texas Christian University, JPS Health System, and the Area Agency on Aging of Tarrant County to train and deploy a range of health profession-
___________________
9 For more information, see www.dfamerica.org (accessed April 4, 2018).
10 For more information, see www.actonalz.org (accessed April 4, 2018).
als throughout the region, including doctors, nurses, physician assistants, pharmacists, physical therapists, social workers, and dieticians, to improve care for older adults.
Another promising program is the Seniors Assisting in Geriatric Education program, which Super said reminds her of the barbershop and beauty shop program that Thomas described. Interprofessional student teams visit older adults in their homes, where many of the students work with an older adult for the first time. There, they may learn that an older adult’s skin is thinner and her veins pop out. In many cases, the medical residents learn that the Meals on Wheels delivery is the only meal some older adults receive all day and yet they share that meal with their pets. “It brings a new understanding of what health means to physicians and health professionals,” said Super, “so prescribing a drug in the hospital might not be the best thing if these people are not even getting basic nutrition at their homes.”
DISCUSSION
Parnell started the discussion by commenting on Wolff’s remark about the lack of a defined role for family caregivers. She asked Wolff and Thomas for suggestions on developing strategies that could be more inclusive of family caregivers while still respecting patient preferences. Wolff replied that the challenge of defining a role for family in delivering care starts with nomenclature. “We often refer to family caregivers as ‘family caregivers,’ but the people who are providing care often do not identify with that term,” said Wolff.
For many people, that is just what you do if you are a spouse or an adult child, so how we identify what the roles are and what the triggers are that move someone from a more normative to a caregiver role is a challenge.
She noted, too, that family members are often serving in roles that are not always about health and disability, such as serving as translators or as a walking medical record.
One strategy Wolff has taken has been to focus on developing simple strategies that are feasible to implement and that empower patients and families to have the discussions needed to clarify what help the patient would like to have. This type of discussion is important, said Wolff, because the patients should establish the role their family plays in managing care. At the same time, clinicians need to be brought into these discussions so they can understand and respect that when patients rely on a family member for care that the family member must be part of the discussion. In her opinion, there are several cultural and technological shifts that will help include family caregivers in discussions with a patient’s clinical team. She
noted that one shift is the move toward the diffusion of consumer-oriented health information. Another shift is that patients can often now share access to their patient portals with their caregivers, according to their preferences.
Thomas noted that in the neighborhoods where he has lived, family is not at all related by blood, so the dynamics of involving those individuals in care become complicated because of legal issues. For him, the solution is to reintroduce medical students and residents to the concept of social medicine and getting care back into caregiving. Super pointed out that as health systems are paying increasing attention to the social determinants of health, they tend to want to re-create services, medicalize them, and not work with the community-based organizations that are already providing those services and are trusted partners in the community. Often, a small contract between a health system and a community-based organization to hire one extra person to handle care coordination and follow-up is a much more effective approach than creating a new service that does not have the same standing in the community. “Recognizing what both parties can bring to the table, allowing them to practice at their highest level, and working in the community are some of the successes that we’ll have in addressing the aging population,” said Super.
Winston Wong from Kaiser Permanente asked the panelists for their perspectives on introducing telehealth technologies into interactions with older adults, and if there are any warnings they would give health care systems with regard to how to leverage that technology in a way that adversely affects communication among the patient, caregiver, and clinician. Super replied that there is a great deal of promise in telehealth, though too often the developers of applications may never have interacted with an older adult. At the same time, Lyft and Uber are trying to serve as a means of getting older adults to medical appointments and are trying to design apps that an older person could use without getting confused. She also noted that there was a program that gave older adults an iPad and assigned them to a nurse who could follow up with them as a means of reducing readmissions. What this program discovered was that the older adults liked this form of communication because they did not want people coming to their homes and seeing how messy they might be. The program was also able to connect culturally competent health professionals with participants who better identified with their ethnicity. The result was that outcomes improved for these adults.
Thomas said it is important to not let technology be a cop-out. “High tech works after high touch, and the real promise is not in portals,” said Thomas, who pointed out that people are not using the portals that already exist. An area where he does see promise is in the miniaturization of diagnostic tools that will enable the clinical team to monitor patients remotely or allow the clinical team to take the diagnostic equipment with them into the community. One issue that will need to be addressed, though, is
shame—the feeling that people do not want to be judged for the condition of their homes. He also noted that talking about telehealth in the context of saving money, rather than improving care, diminishes the power of the technology and the people who provide care.
Wolff agreed that telehealth does have potential to improve care for older adults, but only if it is used in the context of patient preferences and the ability of older adults to use these technologies. Given that caveat, telehealth does have the potential to leverage limited existing resources, such as the geriatric psychiatrist who would never be able to visit every patient personally, but could hold consults via an iPad. “I think it has a lot of promise, but also requires thoughtful attention to developing it in a way that really extends and improves quality of care and efficiency of care,” said Wolff.
Michael McKee from the University of Michigan Medical School reminded the workshop that one in five people have some form of disability, yet disability is often at the tail end when thinking about equity, inclusion, and diversity. Super agreed with McKee and said that the aging and disability communities do not really understand each other. She noted that when the Administration on Aging, the Office on Disability, and the Administration on Developmental Disabilities were combined in 2012 to form the Administration for Community Living, disability organizations and aging organizations were brought together in an arranged marriage that can be uncomfortable at times, particularly given the history of mistreatment of the disabled community by the health care system. At the same time, Super said she has learned a great deal from her colleagues in the disability community about their many challenges and approaches to solutions that are different from those that the aging community has typically addressed.
Wolff agreed with Super that the communities are very different. Individuals who are living with disabilities tend to be working age adults who have grown up with expectations of integration and work, whereas older adults who are experiencing age-related impairments are typically less actively engaged in driving their care. Older adults, she said, “tend to be a little more passive in interacting with the medical community, and they tend to be less interested in sort of consumer-oriented, consumer-directed care.” Wolff noted the challenge of developing specific strategies for dealing with the wide range of disabilities that affect how people interact with and get care from the health care system.
Olayinka Shiyanbola from the University of Wisconsin–Madison commented on the difficulty older adults have in understanding why they are taking specific medications, which points to the importance of pharmacists not only talking to older adults but getting out into the community and meeting these individuals where they live. One thing she has seen, though, is the focus on education versus health literacy in communities of color, and she asked Thomas if he had any insights into why it is given that educa-
tion is not directly related to health literacy. Thomas responded by relaying something a pharmacist told him, which is that pharmacists are more than just distributors of pills and that they often feel marginalized in the hierarchy of medical professionals. What his program does is hold the equivalent of a brown bag day when community members can bring their loved ones’ medication to the barber shop and the pharmacist will answer any questions. How the pharmacists handle billing for their time is something he is unsure about, but the pharmacies that provided their pharmacists seemed more concerned about providing full-fledged health professionals and having them meet and talk to people where they are.
Parson offered a comment that the complexities of decision making in everyday life, beyond those about medical care, are creating challenges for adults as they age. She wondered if the complexity of the health care system is a factor in health decline simply because the overwhelming amount of decisions is helping feed that decline.
Earnestine Willis from the Medical College of Wisconsin asked Thomas if he has studied outcomes from the HAIR program to know if it has precipitated institutional change and if he has considered implementing it in independent living environments. Thomas said no to her second question, largely because he has been operating these programs on a shoestring budget. He is looking for the kind of investment that can disseminate this program into other settings and noted that hospital systems in Maryland are starting to see this type of outreach program as fulfilling their community benefit requirements. One problem, however, is that the health systems are not sharing the data they are collecting, which makes it difficult for him to demonstrate for a broader audience that this program works. He did note that a recent publication highlighted the success of using African American barbershops to address hypertension in African American men (Victor et al., 2018). The one concern Thomas has is that rushing into these humble places could destroy their unique setting. “These are all mom and pop operations where social norms are set,” said Thomas, “but it is the place where we can make change.”
Regarding Willis’s first question, Thomas said he has observed that the doctors talk differently in the barbershop, using plain language automatically. In addition, pulling the clinicians out of their comfort zones helps them feel what the patients feel like when they come to the doctor’s office and is generating a certain amount of empathy. He noted that because of the community that exists inside a barbershop or beauty salon, talking to one person helps educate everyone in the shop because they are all listening. Rosof ended the discussion by reminding the workshop participants of Dr. Donald Berwick’s advice to the Yale Medical School graduating class of 2010: “Take off your white coat and sit among the people who need you and you will learn more perhaps than you have in your 4 years in medical school.”
















