11
A Comprehensive, National Approach
The committee’s primary charge was to consider how the United States can take advantage of foundational and newer evidence to become “a society in which young people arrive at adulthood with the skills, interests, assets, and health habits needed to live healthy, happy, and productive lives in caring relationships with others” (National Research Council and Institute of Medicine, 2009, p. 13), a goal that the 2009 report suggested was within reach. Implicitly, the committee was also tasked with considering why that goal has not yet been realized. To carry out this charge, we have looked across research from the past decade and examined how it builds on what was previously known. In Parts I, II, and III of this report, we examine influences on mental, emotional, and behavioral (MEB) development and means of designing, testing, and implementing effective strategies for promoting it. In this closing chapter, we discuss how this body of knowledge can be leveraged effectively to promote MEB health and prevent MEB problems in children and youth—to help all young people flourish. We begin with our conclusions about what is needed to substantially improve MEB health in children and adolescents. We then present our recommendations for making this happen and a research agenda to address gaps in the evidence about interventions and the best ways to change outcomes at a population level. We close with a look at aspirations for a future in which healthy MEB development is a national priority.
AN INTEGRATED APPROACH TO PROMOTING MEB HEALTH
Our review of the biological and environmental influences on MEB development revealed that MEB development is more complex and interactive than was understood a decade ago. Even a brief, simplified sketch of the influences discussed in Chapter 2 suggests the complexity of the interactions involved. When a baby is born, her MEB development has already been shaped both by her own genes and by aspects of her parents’ lives, from the food her mother has eaten and the air she has been breathing to both parents’ own mental and emotional health, the nature of their employment, and the characteristics of the city and neighborhood in which they live. As a child grows, her development is further shaped by her family’s emotional interactions and economic
circumstances, the quality of her schooling, her physical surroundings and lifestyle, and more. At the same time, she helps to shape her own environment and circumstances in an ongoing interactive process. New research has also shown that each of these factors may influence how other factors affect this child: perhaps the mother’s economic situation compromises her nutrition while she is pregnant, prevents her from leaving a home with an abusive partner, or contributes to a preterm delivery. Or perhaps she lives in a safe neighborhood with ample access to healthy food. Such factors in turn both influence her child’s developing brain and affect later learning and development through the dynamic interplay of environment and genes.
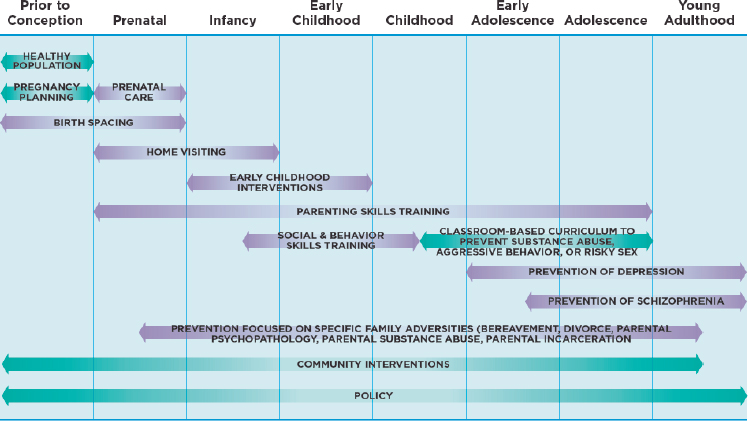
The increasingly sophisticated picture of the interrelated influences on MEB development that emerges from the research reviewed in this report provides a rich context for research on strategies for promoting MEB health and preventing MEB problems in children and youth, described in Part II of this report. The chapters in Part II examine evidence for strategies targeting both risk and protective factors that influence multiple outcomes, and ways to promote healthy development and resilience. They describe interventions that can be implemented universally at home and in health care and education settings, as well as a range of policy tools that can be effective. Overall, we found that effective strategies designed to support individuals and families, populations, and multiple generations are critical to achieving significant benefits. Figure 11-1 (which appears in Chapter 1 as Figure 1-4) illustrates the importance of looking both across the life course and across intervention settings, highlighting the need for an array of diverse types of interventions to address threats to healthy MEB development, especially in communities challenged by poverty and inequity. Particularly promising are strategies aimed at treating maternal depression, improving parenting practices and school climate, providing guidance in the context of well-child health care, and coordinating related community resources.
Part III explores the state of research regarding what is required to implement such strategies effectively across populations. While the science of implementation is still developing, current work indicates that effective implementation encompasses careful research to identify the core components that make an intervention or policy work and then how an effective intervention can be put to work in diverse settings and communities and on a large scale. Coordination of effective partnerships, local resources, and innovative approaches to providing the supports needed to scale up and sustain effective approaches are key, as are ongoing evaluation, adaptation, and improvement based on continued monitoring of MEB outcomes and other data.
From the body of work reviewed for this study, it is clear that achieving meaningful improvements in MEB health and development will require an integrated approach that leverages the full range of findings from this research and the full range of entities that can contribute.
Much of the research we have discussed points clearly to the key influence of broad societal factors, such as poverty, inequality, and discrimination, on MEB health and development. While the influence of these societal factors and the associated consequences for the lives of children and their families is obvious to any observant person, establishing empirical evidence of the links between such broad, distal factors and MEB development requires tracing numerous specific associations and building the case. Today, that case has been made. The totality of the evidence shows that broad societal factors both contribute significantly to constellations of risk factors and poor developmental outcomes and limit what can be accomplished with a single program or policy, even if it is very effective.
Because many of the greatest threats to young people’s healthy MEB development are concentrated in neighborhoods and rural areas of high intergenerational poverty, it follows that a great opportunity to advance the MEB health of America’s young people will come from transforming these neighborhoods and rural areas into communities where children can flourish. Success over the next 10 years will be limited unless concerted attention is paid to the specific challenges in these geographic areas of need and to disorders and lack of flourishing that are evident across the population of children and youth in the United States. However, evidence supporting the effectiveness of specific measures to promote MEB health by tackling the constellation of risks—including poverty, income inequality, and discrimination—that affect lower-income children and youth is more limited; this is discussed below. Therefore, targeted research is needed to establish such links.
A comprehensive exploration of these issues was beyond this committee’s charge, but work in this area is ongoing. A 2019 National Academies report, A Roadmap to Reducing Child Poverty (National Academies of Sciences, Engineering, and Medicine, 2019), examines the evidence regarding the costs of child poverty to society, as well as programs and policies that can reduce the number of U.S. children living in poverty. These issues are a key context for the present report, but our focus is on what can be done now to improve MEB health and development while society continues to work on the underlying causes of adversity, such as poverty, racism, and adverse experiences, affecting children and youth.
Before presenting our recommendations for pursuing this national agenda, we note that while this committee worked independently to develop conclusions and recommendations focused on MEB health, we were struck by the parallels between our thinking and the conclusions and recommendations of numerous other National Academies committees. Table 11-1 shows areas addressed by conclusions and recommendations from a sampling of relevant National Academies reports published in the past 10 years; a fuller version of this table, included as Appendix A, shows the relevant conclusions and recommendations from these reports. We wish to highlight that of the 19 reports listed, 11 address the importance of coordinating efforts and systems to develop an integrated approach to promoting the health and well-being of children, youth, and families; 16 address the critical importance of accurate and comprehensive data collection to inform policy makers and the public about the status of populations, the services they are provided, and outcomes of those services; and 7 identify the key role of poverty and concentrated disadvantage.
The confluence of these messages both supports and amplifies this committee’s recommendations with respect to fostering MEB development and health. The fact that so many reports have made similar recommendations that have yet to be fully implemented highlights the urgency of adopting a new tack. The kinds of interventions that can support and promote healthy MEB development are intimately linked to multiple sectors, including education, health, social and human services, and business, and to public health objectives. And as noted above, the risks and challenges associated with economic disadvantage in the United States influence not only growing children’s MEB health but also their physical health and development, their academic achievement, and their entry into the world of work. It is our hope that our recommendations can be considered vital components of a broader effort to address these urgent national challenges. We would not advocate waiting to accomplish goals for MEB health until other measures needed to foster children’s health and well-being are in place, but believe that the accumulated weight of the conclusions and recommendations presented in the body of work summarized in Table 11-1 and the evidence documented in this report is sufficient to motivate rapid and unwavering pursuit of healthy MEB development for every child and youth.
TABLE 11-1 Confluence of National Academies Recommendations Relating to Health and Well-Being and Public Health Monitoring
| Date | Report | Conclusions or Recommendations Related to | ||
|---|---|---|---|---|
| Coordination of Efforts | Monitoring | Effects of Poverty/Disadvantage | ||
| 2009 | Adolescent Health Services: Missing Opportunities | x | x | |
| 2010 | Accounting for Health and Health Care: Approaches to Measuring the Sources and Costs of Their Improvement | x | ||
| 2011 | For the Public’s Health: The Role of Measurement in Action and Accountability | x | ||
| 2012 | Primary Care and Public Health: Exploring Integration to Improve Population Health | x | ||
| 2014 | Capturing Social and Behavioral Domains and Measures in Electronic Health Records: Phase 2 | x | ||
| 2014 | Implementing Juvenile Justice Reform: The Federal Role | x | x | |
| 2015 | Vital Signs: Core Metrics for Health and Health Care Progress | x | x | |
| 2015 | Mental Disorders and Disabilities Among Low-Income Children | x | ||
| 2015 | Investing in the Health and Well-Being of Young Adults | x | x | |
| Date | Report | Conclusions or Recommendations Related to | ||
|---|---|---|---|---|
| Coordination of Efforts | Monitoring | Effects of Poverty/Disadvantage | ||
| 2016 | Advancing the Power of Economic Evidence to Inform Investments in Children, Youth, and Families | x | ||
| 2016 | Parenting Matters: Supporting Parents of Children Ages 0–8 | x | x | |
| 2016 | Ending Discrimination Against People with Mental and Substance Use Disorders: The Evidence for Stigma Change | x | x | |
| 2017 | Communities in Action: Pathways to Health Equity | x | x | x |
| 2018 | Transforming the Financing of Early Care and Education | x | ||
| 2019 | A Roadmap for Reducing Child Poverty | x | x | |
| 2019 | The Promise of Adolescence: Realizing Opportunity for All Youth | x | x | |
| 2019 | Strengthening the Military Family Readiness System for a Changing American Society | x | x | |
| 2019 | Monitoring Educational Equity | x | x | x |
| 2019 | Vibrant and Healthy Kids: Aligning Science, Practice, and Policy to Advance Health Equity | x | x | x |
RECOMMENDATIONS: A NATIONAL AGENDA FOR IMPROVING THE MEB HEALTH OF CHILDREN AND YOUTH
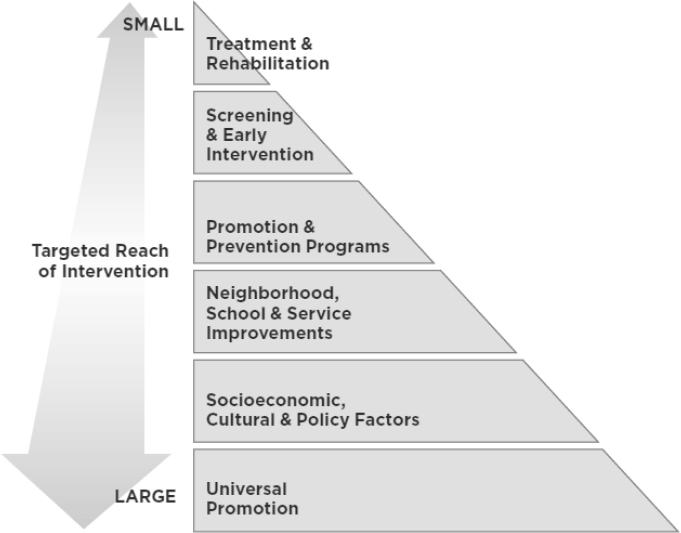
Figure 11-2 illustrates how interventions at multiple levels can be layered to form a robust response to improve the MEB health of children and youth. Universal promotion and prevention efforts provide a foundation that serves the broadest populations. Screening for risk or concerning behaviors and early intervention address the needs of individuals or groups of children and families; risk mitigation, treatment, and rehabilitation serving individuals and families provide help for those who do not benefit from promotion and prevention efforts. Meaningful improvements in MEB health are within reach if efforts at these levels are supported and sustained, if available resources across sectors are coordinated around carefully defined shared goals, and if concerted attention is paid to the challenges of scaling up promising health promotion and disorder prevention strategies at the universal, selective, and indicated levels.
The relevant agencies of the federal government—led by the U.S. Department of Health and Human Services—are well positioned to lead an effort to take advantage of the benefits a comprehensive, integrated strategy could bring. They have the capacity to set the agenda for such a national effort; to garner public support for this agenda; and to enlist public and private entities at the national, state, and local levels, including other government agencies such as the Department of Education, foundations, professional organizations, and advocacy organizations (Cruden et al., 2016).
In conceiving this approach, we were inspired by the example set by the Decade of the Brain from 1990 to 1999, during which the National Institutes of Health mobilized research and public health support to foster research on the brain and greater public understanding of its importance. This effort is credited with generating remarkable progress in neuroscience, including the development of new subspecialties and therapies for neurological disorders and recognition of risks to brain development (Jones and Mendell, 1999; Shonkoff and Levitt, 2010). A similarly broad-based effort to improve MEB health—which could be organized under the rubric of Decade of Children and Youth and led by the U.S. Department of Health and Human Services—would be designed to (1) raise awareness of the social and economic gains that would be realized by improving environments, strengthening families, and supporting healthy child development, and (2) engage multiple sectors of society as a coalition to carry out this work. We are not recommending simply another time set aside to educate the public about a set of issues, but a decade of concentrated action. Because of the urgency of the need, we stress to the relevant agencies the importance of laying out the elements of this agenda now and building them over time. A genuine cultural change will be needed to support this agenda. We offer recommendations in three areas: federal leadership and partnership, implementation and scale-up, and monitoring.
Federal Leadership and Partnership
Given the numerous issues that compete for the attention of policy makers at every level of government, the MEB health of children, youth, and families will not become a national priority by happenstance. Federal agencies are in the best position to articulate the reasons why MEB health deserves national attention and the nature of necessary efforts. Federal leadership will be essential if MEB health is to become a true priority, and the relevant federal agencies can also play a leading role in guiding policy, engaging public and private partners, and directing resources to those efforts. We direct our recommendations to federal agencies whose purview encompasses child welfare and child, youth, and family health: we suggest that the U.S. Department of Health and Human Services take the lead but that the U.S. Department of Education and other relevant agencies also be an integral part of the effort so their objectives can be aligned and their resources coordinated.
- insufficiency, and underemployment—that can contribute to unhealthy MEB development;
- promoting coverage of behavioral health services for children and caregivers, especially those needed during pregnancy and the postpartum period and those offered by parenting programs, in reimbursement for private health insurance and Medicaid, encompassing both behavioral health promotion and risk prevention;
- setting expectations for the adoption and evaluation of programs known to enhance social and emotional development in schools, in health care settings, and in communities;
- supporting consistent polices on accreditation, certification, and licensing requirements for a multidisciplinary workforce oriented toward healthy MEB development in children and youth; and
- supporting and collaborating with local and state initiatives that contribute to healthy MEB development.
A thorough review of the mechanisms that government agencies could use to pursue these objectives was beyond the scope of this committee’s work; we do not provide specific guidance on a comprehensive plan for strengthening child and adolescent MEB health through federal policy. However, there is much on which to build. For example, the National Prevention, Health Promotion and Public Health Council, acting under the direction of the Surgeon General of the United States, articulated a National Prevention Strategy in 2011 (National Prevention Council, 2011). This strategy laid out strategic directions and priorities for federal agencies that include establishing healthy and safe community environments, eliminating health disparities, and fostering mental and emotional well-being. In turn, the Centers for Disease Control and Prevention has articulated a collaborative approach for government entities and others that are pursuing those priorities, Health in All Policies (HiAP). This approach “integrates and articulates health considerations into policymaking across sectors to improve the health of all communities and people. HiAP recognizes that health is created by a multitude of factors beyond healthcare and, in many cases, beyond the scope of traditional public health activities” (Centers for Disease Control and Prevention, 2016).1 Resources associated with HiAP include a guide for state and local governments, a clearinghouse policy resource center, and compendia of experiences from local public health departments, and evidence-based prevention and cross-sector approaches.
Other innovations by federal agencies provide examples of collaborative leadership:
___________________
- Medicaid waivers for screening and treatment of maternal depression during pediatric visits. Many states have taken advantage of guidance from the Centers for Medicare & Medicaid Services on the use of Medicaid funds to support maternal treatment during pediatric visits (Wachino, 2016).2 This guidance is critical to the support of the nearly half of young mothers living in poverty who experience depression during the first year of their child’s life.
- Guidance from the Office of the National Coordinator for Health Information Technology (ONC) on telehealth that encourages positive interactions among family members and clinicians (Bobinet and Petito, 2015).3 The ONC provided new guidance to encourage increased access for rural families and those with limited physical access to medical services, among others, with special attention to the need for families to communicate about well-being.
- Medicaid waivers for states to coordinate home visiting, maternal opioid services, and early intervention for children. Illinois was among the first states to commit to piloting cross-sector services to address maternal addiction and early childhood developmental outcomes in an innovative program (Illinois Department of Healthcare and Family Services, 2018).4
Implementation and Scale-Up
Progress in successfully scaling up interventions for which research has produced evidence of effectiveness will be essential for improving MEB development among children and youth at the population level. Ongoing research in implementation science is providing new insights into best practices for implementing interventions at scale, and as discussed below, this research deserves continuing support. Although many questions about the implementation process remain unanswered, research to date has provided a strong basis for intensified efforts to take effective interventions to scale and carefully study their results.
___________________
2 See https://www.medicaid.gov/federal-policy-guidance/downloads/cib051116.pdf.
3 See https://www.healthit.gov/sites/default/files/DesigningConsumerCenteredTelehealtheVisit-ONC-WHITEPAPER-2015V2edits.pdf.
4 See https://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Waivers/1115/downloads/il/il-behave-health-transform-fs.pdf.
- support research and demonstration projects to determine the effectiveness of promising interventions for MEB health promotion, prevention of MEB disorders, and population screening at large scales, including the implementation of effective in-person and digital interventions;
- support states and local jurisdictions in developing cross-sector partnerships among schools, employers, the health care system, community-based organizations, and others to advance the scale-up of effective promotion and prevention interventions;
- support states and local jurisdictions in developing innovative funding mechanisms that can be sustained through changes in political leadership or funding shortfalls;
- use economic evaluation tools and other methods to analyze such factors as costs and availability of funding, benefit/cost ratio, level of complexity, and need for supportive infrastructure; and
- document needs and develop strategies for sustainability over time.
Partnerships among agencies and levels of government and among public and private entities will be the most important aspect of these efforts. The focus of this report is research that has emerged in the past 10 years, but we illustrate in Table 11-2 how efforts at the federal level could cascade to the state and local levels, and how public and private efforts could be integrated to serve the overall objectives of a national agenda. We highlight policies for which evidence indicates potential to ameliorate risks to or promote MEB health at a broad scale, but our primary emphasis is the importance of coordinating efforts and integrating available resources.
A blueprint for this broad-based effort could begin with three objectives:
- Raise public awareness of the critical importance of healthy child, youth, and family MEB development and ways to foster it.
- Build stable coalitions across sectors and entities.
- Address funding and capacity challenges.
Raise Public Awareness
The tobacco control movement is a model for how effective public health advocacy can mobilize society to improve health. This and numerous other National Academies reports (refer to Table 11-1 and Appendix A) have documented in detail what children and adolescents need to develop successfully and the harm experienced by them and society at large when these conditions are not in place. However, there has to date been no successful effort—such as the
tobacco control movement—to educate the public, policy makers, and the leaders of all sectors of society about the nurturing conditions that children and adolescents need and how those conditions can be achieved. If the progress we envision over the next 10 years occurs, it will be because many more people and organizations—as well as policy makers, other leaders, and the research community—become aware of the needs of children and youth, families, neighborhoods, and schools, and because these partners all take steps to support effective strategies that can promote MEB health and reduce MEB problems with a plan that integrates all such efforts. Such mobilization can be achieved if, over the next 10 years, more resources are devoted to educating the public and policy makers about what is needed and what is possible. This education can be provided through stepped-up public education efforts on the part of the Surgeon General, the Centers for Disease Control and Prevention (CDC), the Substance Abuse and Mental Health Services Administration (SAMHSA), other federal agencies, foundations, and advocacy organizations. Coordinated efforts can build public support for policies, practices, and programs that will advance the nurturing conditions needed to improve child and adolescent MEB development.
Build Stable Coalitions Across Sectors and Entities
Every major sector of society has an impact on the well-being of children and adolescents. Chapters 4, 5, and 6, respectively, describe possibilities for supporting MEB health through the public education system,5 the health care system, and the use of government policies at multiple levels, while Chapter 10 examines why the business community has a growing interest in supporting families and healthy MEB development. Other community organizations also have a vital role to play. For example, organized religions have traditionally provided leadership to build cooperation and support for healthy development in communities and can have an important influence on the promotion of programs, policies, practices, and values that are needed to help neighborhoods prioritize efforts to promote healthy MEB development.
___________________
5 We do not ignore the contributions of private schools, which educate approximately 10 percent of U.S. students in preschool through grade 12, but because they are by definition independent of the majority of education and other policies, we emphasize public schooling (http://www.capenet.org/facts.html).
TABLE 11-2 An Integrated Approach to Promoting MEB Health
| Mechanism | Federal/National Level | State Level | Local/Community Level |
|---|---|---|---|
| Public Health Approaches/Coordination |
Federal entities, including HHS, CDC, and the Departments of Education and Justice:
|
State agencies, including Medicaid, public health, and education:
|
Local government bodies, institutions, and agencies:
|
| Mechanism | Federal/National Level | State Level | Local/Community Level |
|---|---|---|---|
| Funding and Other Incentives |
Provide resources for national programs and to states and communities to support
|
|
|
| Mechanism | Federal/National Level | State Level | Local/Community Level |
|---|---|---|---|
| Regulation and Policy |
Provide research-based guidance for local jurisdictions to use in setting MEB-related policies related to
|
|
|
| Mechanism | Federal/National Level | State Level | Local/Community Level |
|---|---|---|---|
| for a multidisciplinary, child-oriented workforce that promotes healthy MEB development | |||
| Private Entity Contributions |
|
|
Local leaders:
Local-level foundations:
|
Thus, coalitions across public and private entities at the local, state, and national levels will be critical to the success of a Decade of Children and Youth. Child and adolescent MEB disorders are interrelated, but approaches to addressing these problems, including funding, currently are largely fragmented, with different agencies and organizations working on different problems and potential solutions. Strategies for addressing these problems tend to focus narrowly on the proximal influences on each problem, with less attention to the more distal influences that affect all of these problems, such as poverty and discrimination in disadvantaged neighborhoods and communities. Moreover, the organizations that are working to address individual problems seldom speak with one voice about which strategies to implement and how. For example, many foundations target children’s well-being, but they rarely work from consensus as to what would have the greatest impact on children’s MEB development. At the same time, reforms in one sector of society, such as the provision of effective parenting interventions by health care organizations, will improve the success of other sectors, such as schools, that benefit when parents are more effective in nurturing their children’s self-regulation. Lead organizations that are well resourced can provide substantial help in developing strong coalitions that can sustain an effort over the long time horizons needed to make substantial progress. Private entities such as foundations can play important roles in this regard.61
Address Funding and Capacity Challenges
Accomplishing the objectives detailed in this report will undoubtedly require new thinking about resources both for programs and research and for the implementation of policies designed to foster healthy MEB development, as well as improved ways to use existing resources. As discussed in Part III of this report, effective implementation of strategies focused on MEB health requires significantly greater capacity and commitment than generally has been recognized. We have emphasized throughout this report that ad hoc approaches targeting specific problems in isolation have less population impact than integrated approaches that can yield far greater benefits, as well as savings in some areas. Moreover, financial support for program initiation and maintenance, including necessary infrastructure costs, needs to encompass funding for research to assess outcomes systematically and to support ongoing improvement. Given that competition for funds to support public policy initiatives is stiff, whether at the federal, state, or local level, attention to creating and implementing interventions that are affordable at scale is a priority. Economists have developed increasingly sophisticated ways to assess the costs and economic benefits to society of financing promotion and prevention efforts, which can be used to
___________________
6 For further discussion of coalition building, see https://evolutioninstitute.org/creating-a-grand-coalition-to-foster-human-wellbeing/.
significantly bolster the case for investments in MEB health. A long-range perspective is needed.
Economic evaluations provide stakeholders with information about the costs and returns of investment in interventions intended to improve the well-being of children and youth. Such evaluations can help decision makers understand what level of investment is needed to attain impact, whether investment is a justifiable use of limited resources, who bears the costs and who receives economic benefits, and when returns are expected to accrue. This type of analysis—critical in demonstrating the value to society of attention to efforts to promote MEB health—is the subject of another National Academies consensus study, and this committee did not explore the issues involved in depth (National Academies of Sciences, Engineering, and Medicine, 2016). We note, however, that in the last decade, the demand for economic evaluation has grown as policy makers and researchers have sought more refined ways to assess the impact of interventions. We caution that more work is needed to apply such methods to large-scale interventions and policies and to determine whether findings at smaller scales are borne out at population levels. We also note that making the case for economic benefits, while often attractive, cannot in itself lead to adequate funding for expensive public policies, which will require both savings from smarter investing and a greater extended commitment to children, youth, families, and communities.
Nevertheless, progress in economic evaluation falls squarely within the movement toward evidence-based decision making and increased accountability with respect to public spending (Haskins and Margolis, 2015; Head, 2016; Jennings and Hall, 2012; Maynard, 2006; Siu, Bibbins-Domingo, and Grossman, 2015; White and VanLandingham, 2015). The Washington State Institute for Public Policy and the Pew-MacArthur Results First Initiative have helped broaden the focus of evidence-based policy making to include economic evidence about costs and the comparative return on investment of different policy options (Lee and Aos, 2011; Pew Center on the States, 2012).
Monitoring to Support Needs Assessment, Scale-Up, Improvement, and Research
As discussed in Chapter 9, the collection of information about quality and outcomes is vital to the continuous improvement that fuels effective implementation of interventions that can improve the health of populations. That discussion is oriented to what is needed in a particular implementation effort, but in the context of the national agenda we recommend here, more is possible, and more is needed. Both coordination of existing data sources and the collection of new data will be needed to support meaningful improvements in MEB health.
A significant amount of relevant data about children, youth, and families in the United States is collected by SAMHSA; the CDC; the education and criminal justice systems; health systems; and other entities at the local, state, and federal levels. These data can be harnessed to track a population’s key MEB outcomes and identify specific populations that may need greater resources and new
strategies. There are also data available from the National Survey of Children’s Health (NSCH) by state on positive mental health factors, family resilience, and parent–child connection and how these interact with adverse childhood experiences, poverty, and MEB health.7 There are likely many ways to coordinate existing data from the NSCH, the U.S. census, and other sources to support valuable analyses. We note that the Maternal and Child Health Network has created a compendium of measures of child health used across agencies, focusing on such issues as family health and engagement and social determinants of health.8
A thorough assessment of available sources of data on how children and adolescents are developing and what their family, home, school, and community environments are like was beyond the scope of this study. It appears, however, that although existing data sources may be underused, the nation lacks sufficient data about the social-emotional development and MEB health of young people at the national, state, and local levels to support broad and significant improvement. At present, annual reports on representative samples of children and adolescents provide information about the levels of their MEB disorders, and data are collected annually on the proportion who live in poverty.
A census of localities of concentrated disadvantage for children in the United States would be a valuable basis for planning, but we were unable to find such an analysis. States have data on academic outcomes for students, and periodic reports on children’s health—rates of obesity, asthma, substance use, and premature birth, for example, are available. A variety of surveillance and screening tools are used in jurisdictions across the country (see Appendix B), yet these efforts do not provide the comprehensive, timely data needed by government entities at all levels if they are to understand the challenges to healthy child and adolescent MEB development and the possibilities for fostering MEB health for all children and youth more effectively.
In considering the data collection and monitoring needed to support the national agenda we recommend, we considered the work of other National Academies committees on this topic; Box 11-1 lists objectives for data collection related to developmental health and well-being identified by National Academies committees in the past decade.
We also considered the benefits Canada has found in a monitoring system called the Early Learning Development Instrument (EDI), described in Box 11-2. EDI clearly demonstrates how carefully collected national, state, and local data can support meaningful improvement in MEB health and development (although
___________________
7 See http://www.childhealthdata.org.
8 See http://www.mch-measurement.org; see also http://www.childhealthdata.org for existing variables collected by the NSCH and national and state data and local-area estimates that are or could be made available.
because it relies on teacher reports and census data for children in kindergarten, it does not provide data on early childhood).
The United States needs an improved system for coordinating and collecting data on child and adolescent well-being and the conditions that affect it. Policy makers and the public need information about the status of the nation’s young people if they are to fully understand risks to MEB development and possibilities for improving MEB health. To support efforts to promote MEB health, prevent MEB disorders, and address related problems, therefore, regular collection and coordination of data on indicators of mental, social-emotional, and behavioral development and health at the national, state, and local levels is needed. These data would be used to understand patterns and trends, identify areas of need and vulnerable populations, and support analysis and evaluation of the impact of policies and interventions over time.
- depressed parent, or at school, or influences promoting concerning behaviors, such as the consumption of unhealthful food, the use of nicotine-delivery products and such substances as alcohol and marijuana, and exposure to entertainment media that promote social exclusion, violence, or prejudice;
- access by children, youth, and families to effective health promotion and protective interventions, including preconception and prenatal health care for parents and care for children and youth from infancy through young adulthood; and
- effective programs and policies, including how many such efforts are under way, what interventions are being implemented, how many people they are reaching, who benefits and who does not, and whether they are achieving their intended impact.
RECOMMENDATION 5: The U.S. Department of Health and Human Services’ plans for coordinating the monitoring of the mental, emotional, and behavioral (MEB) health of the U.S. population should include building the capacity to
- track both key data, using (or developing) standardized indicators of positive MEB development and health, and efforts to improve MEB outcomes;
- collect indicator data universally at the local level and aggregate these data to the community, state, regional, and national levels;
- share data across all levels, encompassing both locale-specific data documenting community efforts, including those of the public education system, and national and state data, for use in formulating policy;
- coordinate existing data collection efforts, including community monitoring systems and public health systems for surveillance and screening, at all levels; and
- support regular reporting and analysis of results to identify progress toward improvement goals.
A nonpartisan, nonprofit organization akin to the National Bureau of Economic Research, which played a key role in the development of economic indicators for the nation during the Great Depression in the 1930s, or an entity within the federal government could take the lead in coordinating the collection of relevant data, which could also serve other policy objectives related to children, youth, and families. Although a detailed plan for such a monitoring system is beyond the scope of this report, Appendix B outlines elements that will be critical to the usefulness of such a system for supporting a national agenda to promote
MEB health and describes several programs that illustrate its potential benefits. The plan we suggest is ambitious, but no nation or jurisdiction can attain population-level improvements in the well-being of its young people if it does not monitor and evaluate how they are doing.
A RESEARCH AGENDA
Although a strong foundation of research on which to base the launching of a Decade of Children and Youth exists today, ongoing support for discovery and application research will be essential to continued progress. We first identify key priorities for future research and then briefly discuss two opportunities with particular relevance to researchers interested in MEB health and development.
Research Priorities
Federal support for research relevant to MEB health has tended to focus on treatment and prevention of specific disorders at the expense of investigations of the social and environmental determinants of health and well-being and efforts to promote MEB health population wide (Murray et al., 2015). Our proposed research agenda outlines targets for research in health promotion and risk prevention and their potential impact on the incidence and prevalence of MEB disorders, as well as further progress in the science of program implementation.
We suggest that the greatest progress is likely to come from projects that feature pooled, cross-sector expertise and resources and from population-level studies where scope and ability to track outcomes across phases of development are adequate. Strategies for combining funding from multiple federal agencies and private sources may need to be developed to support studies that are sustained long enough to document the relationships between implementation processes and program outcomes, including tracking of the long-term outcomes, and carried out at a population scale, sampling across multiple communities. We also highlight the importance of work across these topics that identifies testable theoretical models based on hypotheses about core components of interventions and the factors that mediate or moderate them in diverse settings.
Our first priority is to continue building on the strong body of work already emerging about ways to promote healthy development at the population level. We recognize as well the importance of emerging possibilities for reaching populations through school-based interventions and the health care system. Our research priorities also reflect the importance of understanding macro-level influences on MEB development and the challenges of population-level implementation of effective programs.
Research Priority 1: Design and evaluation of interventions to promote healthy MEB development among children and youth at the population level.
Promising research targets include
- interventions that foster MEB development across multiple domains, such as whole-community efforts that focus on individual, family, school, and neighborhood outcomes and mitigate the effects of adverse childhood events;
- enhancement of birth outcomes, focusing on parental health during the preconception and prenatal periods, to optimize neurobehavioral development;
- strengthening of the behavioral and mental health and parenting skills of caregivers and parents, and the creation of safe and supportive community environments for both caregivers/parents and children;
- benefit/cost analysis of healthy parenting programs in obstetric and pediatric settings;
- universal interventions in sites that children encounter routinely and continually, such as preschools, schools, and primary care child health facilities;
- development of biological measures (biomarkers) with which to identify potential candidates for social, psychological, and medical interventions and to track intervention outcomes;
- improved understanding of interactions among genes and environmental variables and the mechanisms mediating social and emotional outcomes across the developmental spectrum to better support the design of interventions;
- assessment of the timing, dose, and duration of interventions to optimize short- and long-term outcomes; and
- the use of digital technology in population-based interventions.
Research Priority 2: Design, evaluation, and implementation of effective school-based interventions.
Promising research targets include
- mechanisms to support social-emotional learning, including mindful awareness approaches;
- rigorous trials of school-based interventions for children and youth at all levels, from preschool to higher education, to better shape these interventions and document the size and duration of their effects, as well as how they affect social, cognitive, and emotional learning;
- identification of the core elements of and amount of exposure to social-emotional learning programs needed to promote sustainable growth in
- social and emotional skills during the preschool and school years and across types of programs and services;
- rigorous trials of interventions designed to improve instruction and classroom management in ways that can improve MEB health, as well as academic success;
- strategies for scaling up proven preschool models in partnership with underresourced communities to ensure acceptability and feasibility;
- optimal intervention doses, effects of continuous prevention interventions that span K–12, and the use of whole-school promotion and prevention approaches;
- methods for delivering a multitiered system of support in all K–12 schools to coordinate the implementation of evidence-based universal, selective, and indicated prevention interventions;
- prevention and reduction of disruptive behavior, anxiety and traumatic stress, drug use, bullying, depression and suicide, dating violence, and school dropout in education settings; and
- interventions for the early childhood and primary and secondary school workforce to promote their own health and well-being and their ability to support the MEB health of students.
Research Priority 3: Development of successful two-generation interventions in health care through exploration of the effectiveness and sustainability of program models for improving MEB development.
Promising research targets include
- development and assessment of programs to improve preconception and prenatal parental physical and mental health;
- implementation research on scaling up of effective parenting approaches in pediatric practice;
- evaluations of outcomes of parenting enhancement programs in obstetric and well-child care;
- identification of core elements of effective interventions; and
- development of digital tools that teach and reinforce healthy practices and increase supportive communication.
Research Priority 4: Strategies to improve MEB development through attention to social, racial, and economic disparities.
Promising research targets include
- population wide trends and variation in MEB health outcomes by subgroups, particularly for underresourced communities and those at highest risk, and community partnerships intended to implement
- culturally and contextually sensitive interventions that address disparities in MEB outcomes;
- long-term outcomes and scale-up potential for effective MEB health promotion and prevention activities for children and adolescents living in underresourced communities;
- impacts of economic development programs, such as livable wage laws, paid parental leave, Earned Income Tax Credit enrollment programs, and Housing Choice Voucher programs on MEB health and development;
- challenges to the implementation, widespread adoption, and sustainability of effective approaches for populations experiencing disparities in MEB outcomes;
- interventions for the child-serving workforce to enhance equity in promotion of the MEB health of all children; and
- identification and evaluation of practices that foster healthy MEB development among diverse cultural groups to determine whether implementation of these practices could decrease disparities and benefit other groups.
Research Priority 5: Design and evaluation of implementation strategies.
Promising research targets include
- identification of core intervention elements and mechanisms of effects to promote intervention fidelity and adaptation in scale-up;
- evaluation of digital tools that counteract “drift” and can be implemented widely as tested in outcome studies;
- infrastructure required to ensure the success and sustainability of interventions, with emphasis on strategies for workforce development;
- design of quality implementation and improvement plans for intervention scale-up;
- decision making about potential trade-offs, such as intervention effectiveness versus reach to achieve population-level management;
- strategies for scaling programs across diverse settings and delivering them effectively, including use of digital technology and tiered intervention structures;
- benefit/cost relationships when interventions are brought to scale;
- identification of incentives that drive favorable implementation outcomes among organizations and systems;
- strategies for blending funding from diverse federal agencies to support implementation at the population level;
- projects that feature cross-sectional expertise and resources to reach all children in need; and
- projects that address the development and use of population-level data systems to identify needs and track outcomes of interventions/projects.
Research Opportunities
Two ongoing developments in social and behavioral research offer opportunities to generate study data relevant to MEB health and development more effectively and efficiently.
Alternative Research Designs and Methods
Research examining the efficacy, effectiveness, and implementation of interventions designed to improve MEB outcomes in young people has consisted largely of randomized controlled trials. These strong research designs have major advantages, but also are costly and time-consuming, and they do not always reflect outcomes in real-world settings. In the case of rapidly changing technologies, such as trials of digital interventions, the operating systems or the social media outlets used may be obsolete by the time the study is published.
One issue that has generated controversy in a number of scientific disciplines is the question of what evidentiary standards should be applied in identifying interventions as clearly efficacious and effective, and thus deserving of policy support and public resources for scale-up. Some have argued that randomized controlled trials should be the standard because it is only by randomly assigning participants to receive or not receive a treatment that researchers can conclusively eliminate sample bias (see Lee et al., 2017, for a discussion). Others have noted that such trials are not ideal or even suitable for some types of research, such as that associated with broad dissemination of previously studied interventions throughout whole communities (Biglan, Ary, and Wagenaar, 2000; Bothwell et al., 2016; Sullivan, 2011). Given the cost and time demands of randomized controlled trials, developing and improving efficient methods for generating evidence represents an important contribution. Significant progress has been made in applying to MEB prevention research alternative research designs that can yield sound findings in contexts akin to the real-world settings where programs are implemented. Some research designs and methods have the potential to reduce cost and improve timeliness as well. A number of well-established methods beyond randomized controlled trials are promising for the study of influences on MEB health and development and the implementation of interventions, including
- pragmatic (real-world) clinical trials,
- comparative effectiveness trials,
- hybrid designs that blend components of efficacy and effectiveness trials,
- trials targeting health policy outcomes,
- carefully structured pre–post observations,
- interrupted time series designs,
- quality improvement research, and
- learning collaboratives that allow for testing and sharing of ideas and resources at multiple sites in the design and implementation of interventions.
Leveraging of New Kinds of Data
As discussed above, an important aspect of the development of the kind of monitoring system needed to support improvements in MEB health will be careful attention to the optimization and coordination of possibilities in the availability of new or existing large-scale data sources and their analysis. This kind of coordination will be beneficial for researchers as well, opening up new possibilities for linking different types of data. We note also that data generated for other purposes may include elements that are applicable and can be repurposed to answer questions relevant to MEB health and development. Information of many sorts is now routinely collected using expanding digital technologies, and most types of records are digitized. One result of these developments is the collection of extremely large datasets that generally can be accessed only using data mining technologies, often referred to as “big data,” which can be of use to researchers interested in MEB health and its promotion. Such administrative data are collected at the local, state, and national levels, such as by social service agencies, school districts, health care systems, and the like (e.g., the census, tax records, juvenile justice records), and can be linked to answer questions about how interventions for promoting MEB health may influence such outcomes as school attendance, arrest rates, and emergency room visits. These data are potentially valuable for directly answering relevant questions or for generating hypotheses that can be tested in more traditional research. Development of a workforce trained to support collaboration among promotion and prevention investigators and those with informatics expertise will be increasingly important to accelerate research that can inform efforts to foster healthy MEB development.
An even more rapidly growing resource is data collected on children, families, and communities through sensors in homes, smartwatches, phones, cars, and many other devices. Other potentially valuable resources include, for example, medical record data and data gleaned from social media platforms, as long as individuals’ privacy is protected and researchers attend to the development of ethical standards for this rapidly evolving research avenue. Ongoing improvements in data collection, mining, and management are supporting new ways of exploring key public health questions in which social scientists and data scientists collaborate to generate hypotheses that can be tested or to identify populations in need of intervention. A promising possibility that requires further development is the use of natural language processing to identify risks for patient suicide in electronic health records (Pestian et al., 2016; Simon et al., 2018) and machine learning algorithms are offering other possibilities for mining large datasets (Gallo et al., 2015; Imel et al., 2019; Wang et al., 2016).
As new analytic tools for mining large datasets continue to be developed, it will be critical to adhere to ethical standards regarding privacy, and be mindful of
the need to consider adapting procedures and standards in light of new technological possibilities. Protection of the privacy of identifiable data must be a high priority, the ownership of personal data must remain with the individual, and the right of individuals to delete their own data must be maintained.
ASPIRATIONS FOR A DECADE OF CHILDREN AND YOUTH
We close with an overview of what would be different from today at the end of a Decade of Children and Youth in which supporting healthy MEB development and working to ensure that every child and adolescent had the opportunity to meet her potential was a national priority:
- Scientists, educators, business leaders, health care systems, human services agencies, and policy makers together would have recognized the critical importance of measuring and tracking the MEB health and development of young people, and of responding to identified needs at the federal, state, and local levels through the allocation of necessary resources.
- Local, state, and national public health campaigns would have raised broad awareness of the need for improved MEB outcomes for children and youth and the social and economic gains that result. These campaigns would have used monitoring data to demonstrate the advantages of living in communities that have made substantial improvements.
- Communities would have been empowered to organize across sectors, with support from state and federal governments, to effectively address child and family wellness and address disparities.
- Families would have been supported in making advantageous decisions about bearing and rearing their children and prioritizing their children’s healthy MEB development, with support from neighborhoods and communities.
- Child care providers and educators would have systematically taken advantage of opportunities to advance the MEB health and development of the children entrusted to them.
- Health care providers would have assumed an obligation to promote fetal as well as child health and development by attending to the MEB health of prospective and actual parents and children and by promoting healthy parenting, neighborhoods, and communities.
- Businesses would have invested in the well-being of employees and supported their employees’ families and neighborhoods, recognizing that the healthy MEB development of children, youth, and families is “good business.”
- Government entities would regularly use data on MEB development in considering policies and funding streams with the potential to promote healthy neighborhoods and family nurturance of children, working across the federal, state, and community levels to implement effective programs and assess their outcomes.
- Scientific efforts to understand and track the social and environmental determinants of healthy MEB development would have been prioritized by an array of funders. Information about genetic and environmental susceptibility to adverse MEB outcomes would have been used in the development of effective interventions and the monitoring of outcomes for individual children, as well as populations of children.
- The Decade of Children and Youth campaign would have resulted in identifiable and continuous improvement of the MEB development and health of young people; recognition of the family, community, and societal advantages of these efforts; and a national resolve to continue investments in a better future as the United States became a world leader in child wellness advocacy.
REFERENCES
Biglan, A., Ary, D., and Wagenaar, A.C. (2000). The value of interrupted time-series experiments for community intervention research. Prevention Science, 1(1), 31–49.
Bobinet, K., and Petito, J. (2015). Designing the consumer-centered telehealth & evisit experience: Considerations for the future of consumer healthcare. Washington, DC: The Office of National Coordinator for Health Information Technology, U.S. Department of Health and Human Services.
Bothwell, L.E., Greene J.A., Podolsky, S.H., and Jones, D.S. (2016). Assessing the gold standard—lessons from the history of RCTs. New England Journal of Medicine, 374(22), 2175–2181.
Centers for Disease Control and Prevention. (2016). Health in all policies. Available: https://www.cdc.gov/policy/hiap/index.html.
Cruden, G., Kelleher, K., Kellam, S., and Brown, C.H. (2016). Increasing the delivery of preventive health services in public education. American Journal of Preventive Medicine, 51(4), S158–S167.
Gallo, C., Pantin, H., Villamar, J., Prado, G., Tapia, M., Ogihara, M., Cruden, G., and Brown, C.H. (2015). Blending qualitative and computational linguistics methods for fidelity assessment: Experience with the Familias Unidas preventive intervention. Administration and Policy in Mental Health, 42(5), 574–585.
Haskins, R. and Margolis, G. (2015). Show me the evidence: Obama’s fight for rigor and evidence in social policy. Washington, DC: The Brookings Institution Press. Available: https://www.jstor.org/stable/10.7864/j.ctt7zsvr9.
Head, B.W. (2016). Toward more evidence-informed policy making? Public Administration Review, 76(3), 472–484.
Human Early Learning Partnership. (2016). EDI British Columbia provincial report, 2016. Vancouver, BC: University of British Columbia, School of Population and Public Health.
Human Early Learning Partnership. (2018). The early development instrument: Fact sheet. Vancouver, BC: University of British Columbia.
Illinois Department of Healthcare and Family Services. (2018). FAQs for Illinois’ behavioral health transformation—section 1115 demonstration waiver. Springfield: Illinois Department of Healthcare and Family Services.
Imel, Z.E., Pace, B.T., Soma, C.S., Tanana, M., Hirsch, T., Gibson, J., Georgiou, P., Narayanan, S., and Atkins, D.C. (2019). Design feasibility of an automated, machine-learning based feedback system for motivational interviewing. Psychotherapy (Chic), 56(2), 318–328. doi:10.1037/pst0000221.
Jennings, E.T. and Hall, J.L. (2012). Evidence-based practice and the use of information in state agency decision making. Journal of Public Administration Research and Theory, 22(2), 245–266.
Jones, E.G., and Mendell, L.M. (1999). Assessing the decade of the brain. Science, 284(5415), 739.
Lee, K.J., Pascoe, E.M., Billot, L., and Braat, S. (2017). Randomised control trials: What makes them the gold standard in medical research? Available: http://theconversation.com/randomised-control-trials-what-makes-themthe-gold-standard-in-medical-research-78913.
Lee, S., and Aos, S. (2011). Using cost-benefit analysis to understand the value of social interventions. Research on Social Work Practice, 21(6), 682–688.
Maynard, R.A. (2006). Presidential address: Evidence-based decision making: What will it take for the decision makers to care? Journal of Policy Analysis and Management, 25(2), 249–265.
Murray, D.M., Cross, W.P., Simons-Morton, D., Engel, J., Portnoy, B., Wu, J., Watson, P.A., and Olkkola, S. (2015). Enhancing the quality of prevention research supported by the national institutes of health. American Journal of Public Health, 105(1), 9–12.
National Academies of Sciences, Engineering, and Medicine. (2016). Advancing the power of economic evidence to inform investments in children, youth, and families. Washington, DC: The National Academies Press. doi:10.17226/23481.
National Academies of Sciences, Engineering, and Medicine. (2019). A roadmap to reducing child poverty. Washington, DC: The National Academies Press. doi:10.17226/25246.
National Prevention Council. (2011). National prevention strategy: America’s plan for better health and wellness. Washington, DC: U.S. Department of Health and Human Services, Office of the Surgeon General.
National Research Council and Institute of Medicine. (2009). Preventing mental, emotional, behavioral disorders among young people: Progress and
possibilities. Washington, DC: The National Academies Press. doi:10.17226/12480.
Pestian, J.P., Grupp-Phelan, J., Bretonnel Cohen, K., Meyers, G., Richey, L.A., Matykiewicz, P., and Sorter, M.T. (2016). A controlled trial using natural language processing to examine the language of suicidal adolescents in the emergency department. Suicide and Life Threatening Behavior, 46(2), 154–159.
Pew Center on the States. (2012). U.S. state policy. Available: http://www.pewstates.org/projects/results-first-328069.
Shonkoff, J.P., and Levitt, P. (2010). Neuroscience and the future of early childhood policy: Moving from why to what and how. Neuron, 67(5), 689–691.
Simon, G.E., Shortreed, S.M., and Coley, R.Y. (2019). Positive predictive values and potential success of suicide prediction models. JAMA Psychiatry, 76(8), 868–869.
Siu, A.L., Bibbins-Domingo, K., and Grossman, D. (2015). Evidence-based clinical prevention in the era of the Patient Protection and Affordable Care Act: The role of the U.S. Preventive Services Task Force. Journal of the American Medical Association, 314(19), 2021–2022.
Sullivan, G.M. (2011). Getting off the “gold standard”: Randomized controlled trials and education research. Journal of Graduate Medical Education, 3(3), 285–289.
Wachino, V. (2016). Maternal depression screening and treatment: A critical role for Medicaid in the care of mothers and children. Baltimore, MD: Centers for Medicare and Medicaid Services.
Wang, D., Ogihara, M., Gallo, C., Villamar, J.A., Smith, J.D., Vermeer, W., Cruden, G., Benbow, N., and Brown, C.H. (2016). Automatic classification of communication logs into implementation stages via text analysis. Implementation Science, 11(1), 119.
White, D. and VanLandingham, G. (2015). Benefit-cost analysis in the states: Status, impact, and challenges. Journal of Benefit-Cost Analysis, 6(2), 369–399.


































