1
Introduction
Imagine what the United States would be like if all sectors of society joined together to use current knowledge to establish policies, communities, and programs designed to ensure that all young people have an opportunity to thrive. Envision that 10 years from now, the U.S. Surgeon General can celebrate that children’s healthy development has become a foundational value, and as a result, effective programs to promote mental, emotional, and behavioral (MEB) health and development are in place. The Surgeon General is able to document decreases in rates of MEB disorders of all types and evidence that increasing proportions of young people are attaining adulthood having met key developmental milestones, and having developed the skills and attributes they need to lead meaningful, productive, and engaged lives.
The United States has far to go to achieve this vision, although scholars have produced a substantial body of research on the tools needed to do so and how to apply them. In a 2009 report on preventing MEB disorders in children and youth, the National Research Council and Institute of Medicine (NRC and IOM)1 concluded that “the scientific foundation has been created for the nation to begin to create a society in which young people arrive at adulthood with the skills, interests, assets, and health habits needed to live healthy, happy, and productive lives in caring relationships with others” (NRC and IOM, 2009, p. 13). The United States has not yet taken advantage of this foundational knowledge.
In the decade since the 2009 NRC and IOM report was published, a growing body of research has significantly strengthened this foundation. The scientific basis for designing and implementing programs to support healthy MEB development and prevent MEB disorders has been falling into place, and there is no reason why the United States cannot achieve the vision of a nation of healthy young people who grow up to be healthy adults.
___________________
1 National Academies of Sciences, Engineering, and Medicine reports can be downloaded for free at https://www.nap.edu.
CHARGE TO THE COMMMITTEE
To address the critical gap between achievable goals and actual progress in MEB health and development, the Substance Abuse and Mental Health Services Administration of the U.S. Department of Health and Human Services, joined by the Centers for Disease Control and Prevention and the National Institutes of Health, asked the National Academies to conduct a study of progress in fostering healthy MEB development among children and youth. The National Academies convened the Committee on Fostering Healthy Mental, Emotional, and Behavioral Development Among Children and Youth to carry out this work; the committee’s members have expertise in behavioral research, child development, child and adolescent psychiatry, education, epidemiology, evaluation research, health care services, implementation science, neuroscience, pediatrics, prevention research, program development, public health, and public policy (see Appendix C for biographical sketches of the committee members). The committee was asked to review and synthesize the available research and data on key advances in this area since the 2009 report was published, identify key challenges to further progress, and offer recommendations for acting on the existing body of research; see Box 1-1 for the committee’s charge.
This report presents the committee’s response to its charge. It offers an expanded view of the nature of healthy MEB development for children and youth (from fetuses and infants through older adolescents and young adults) and an updated review of strategies for promoting healthy MEB development and preventing MEB disorders. It also describes recent progress in understanding what is necessary to implement such strategies effectively. It sets forth the committee’s recommendations regarding a national agenda for fostering healthy MEB development among children and youth, and outlines research needed to address remaining gaps in the understanding of MEB development and how it can be strengthened. Box 1-2 presents key terms used in this report.
CONTEXT FOR THE STUDY
This report builds on and updates a 1994 Institute of Medicine report (IOM, 1994), as well as the 2009 report referenced above (NRC and IOM, 2009). Each of these reports highlights developments in relevant research and includes recommendations for the continued improvement of MEB health in children and youth. Nevertheless, MEB health remains a primary concern because the nation is not effectively mitigating the risks that contribute to poor MEB health outcomes; these risks are prevalent and current data do not show improvement over past years.
As our charge directed, we focus both on the promotion of healthy MEB development and the prevention of MEB disorders, and we note that there are no crisp boundaries between healthy MEB development and disorder in the lives of children and youth. Many factors contribute to positive MEB development or hinder it in ways that may be subtle and even contradictory. The experience of
most children will likely fall somewhere in the middle of a continuum from robust positive development to serious disorder, and may fluctuate with family characteristics and other life circumstances.
MEB disorders often emerge during childhood or adolescence: 75 percent develop by age 24, and one-half of all adolescents have had some mental disorder.2 Rates of particular disorders vary by population subgroup and also fluctuate over time, but overall they are concerning, to say the least. Nearly 20 percent of adults—approximately 46.6 million individuals—experience a mental illness in the course of 1 year, and rates of diagnosis have been steady across age groups since 2008 (Kamal, 2017). Anxiety disorders are the most common MEB disorders among children and adolescents (31.9%), followed by behavior disorders (19.1%), depression (14.3%), and substance disorders (11.4%). Approximately 40 percent of young people who meet the criteria for one of these disorders also meet the criteria for at least one of the others. And rates of depression, suicide, and self-harm among young people have been increasing (Olfson, 2018):
- College counseling centers have reported that the percentage of students seeking treatment or guidance for anxiety increased from 40.4 percent in 2010 to 50.6 percent in 2016 (though this increase could reflect increased willingness to seek help) (Olfson, 2018).
- For college students who seek treatment services, anxiety and depression are the most common primary concerns. When students seeking treatment services were asked to “check all that apply” from a list of 44 concerns, 62.2 percent checked anxiety and 49.7 percent checked depression (Center for Collegiate Mental Health, 2018).
- While there has been some overall decline in substance use rates among young people, opioid-related morbidity and mortality have been increasing (Olfson, 2018).
- In 2015, suicide was the second most common cause of death among young people aged 15 to 24 and the third most common among those aged 10 to 14 (Olfson, 2018).
___________________
2 Unless otherwise noted, data in this paragraph are taken from the National Institutes of Mental Health, see https://www.nimh.nih.gov/health/statistics/mental-illness.shtml.
- Between 2005 and 2014, the proportion of U.S. adolescents who reported experiencing a major depressive episode in the past year increased from 8.7 percent to 11.3 percent (Mojtabai, Olfson, and Han, 2016).
MEB disorders are a growing burden for affected young people and their families. They hinder young people’s development into healthy and “economically productive and engaged citizens” (Center for the Study of Social Policy, 2012, p. 4), and in 2015 accounted for the highest rates of disability in the U.S. population (Kamal, 2017). One study of high school dropouts found that almost one-quarter of the students had demonstrated depressive symptoms in the 3 months prior to leaving school (Dupéré et al., 2018). The approximately 12 percent of young people ages 16–24 who are neither in school nor employed—often referred to as disconnected or “opportunity” youth—are at particular risk for a range of negative outcomes over the life course, including chronic unemployment, poverty, future mental health issues, criminal behaviors, incarceration, poor health, and early mortality, although the data do not indicate whether they are disconnected because of their mental health problems or the reverse (Fernandes-Alcantara, 2015; Hair et al., 2009; Sissons and Jones, 2012). Among adults who are homeless or incarcerated and youth involved in the juvenile justice system, moreover, rates of mental illness are much higher than those among the general population (National Alliance on Mental Illness, 2015). Mental health issues may, of course, lead to disconnection, homelessness, and related consequences, and the stresses of these situations may trigger or exacerbate mental health and substance abuse problems. Nearly one-fourth of adults in a nationally representative survey sample reported having been exposed to at least three adverse childhood experiences, which are known as antecedents of concerning MEB outcomes (Merrick et al., 2018), and more than one-half (57.7%) of children experience at least one exposure to violence in 1 year (Finkelhor et al., 2015).
Furthermore, youth without a diagnosable MEB disorder do not necessarily experience positive mental health development. Researchers have begun to examine flourishing in children, a way of defining positive MEB development independent of the presence or absence of an MEB disorder. A recent study used data from the National Survey of Children’s Health to measure an index of flourishing in U.S. children, which encompassed their interest and curiosity in learning new things, persistence in completing tasks, and capacity to regulate emotions (Bethell, Gombojav, and Whitaker, 2019). The authors estimated that fewer than one-half (40.3%) of children in the United States met the criteria for flourishing (Bethell, Gombojav, and Whitaker, 2019). They found that children who live in households with an income greater than or equal to 400 percent of the federal poverty line are more likely to meet the criteria than are children who live in households with incomes below 400 percent of the federal poverty line. They found further that children who experience no adverse childhood experiences are much more likely to meet the criteria for flourishing than are children who
experience four or more such experiences (47.9% versus 20.6%). However, there is much less variation when the data are stratified by household income: 35.6 percent of children living in households with incomes below 100 percent of the federal poverty line meet the criteria for flourishing, compared with 46.9 percent of children living at 400 percent or more of the federal poverty line.
The economic burden of MEB disorders is also great, and can be calculated in a number of ways. U.S. spending on mental illness was estimated at $89 billion for 2013, but mental illness is also associated with loss of earnings and productivity and other indirect costs (Kamal, 2017). Investing in the healthy MEB development of the next generation therefore promises not only benefits for individuals, families, and communities but also economic savings and benefits. Indeed, the nation’s economic and civic well-being depend on a healthy adult population capable of productive work and stable relationships.
There are many ways to think about what constitutes healthy MEB development, but the differences among them are subtle. The committee took a broad view that encompasses not only the absence of disorder but also the idea that all children and youth deserve to have a meaningful and engaged life. We regard MEB health as fundamental to their success in whatever they undertake. We therefore believe that the stagnant progress in fostering healthy MEB development and preventing MEB disorders is worthy of national concern and attention to issues beyond those addressed in the 1994 and 2009 studies.
The IOM (1994) and NRC and IOM (2009) reports provide a valuable foundation for addressing these challenges. The former describes approaches to the treatment of MEB disorders and emphasizes the importance of extending the spectrum of mental health interventions beyond treatment to prevention and maintenance (i.e., sustaining the effects of treatments). That report includes a half-moon figure used to depict the interventions, including those provided through the specialty care sector, such as long-term management and rehabilitation, but also prevention activities (see Figure 1-1). As shown in the figure, the 1994 report recommends that, in addition to treatment and maintenance services, the nation consider the importance of (1) universal prevention, which focuses on entire populations of children and adolescents, not just those with specific risk factors, in schools, primary care, or other community settings; (2) selective prevention, aimed at children with identified risks; and (3) indicated prevention, for those beginning to exhibit symptoms, to forestall development of full-blown clinical episodes.
The 2009 update of the 1994 report (NRC and IOM, 2009) focuses greater attention on prevention of mental disorders and recommends the implementation of interventions designed to promote MEB health. It describes evidence regarding interventions for improving the MEB outcomes of children and youth, points to the need to make those interventions available on a large scale, and emphasizes several key points:
- Prevention requires a paradigm shift.
- Mental health and physical health are inseparable.
- Successful prevention is inherently interdisciplinary.
- MEB disorders are developmental.
- Coordinated community-level systems are needed to support young people.
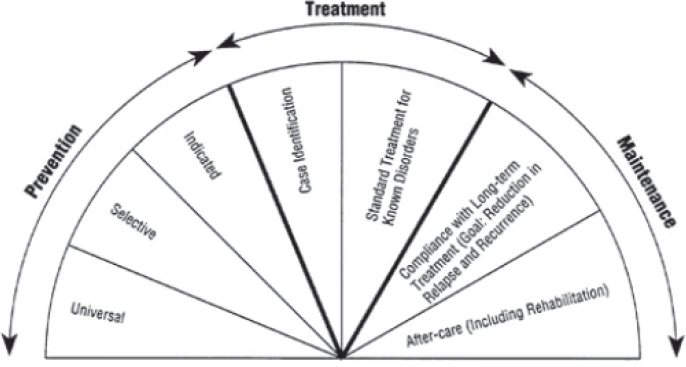
SOURCE: IOM (1994).
The 2009 report includes an updated version of the half-moon figure from the 1994 report, reflecting the role of both promotion of MEB health and prevention of MEB disorders (see Figure 1-2).
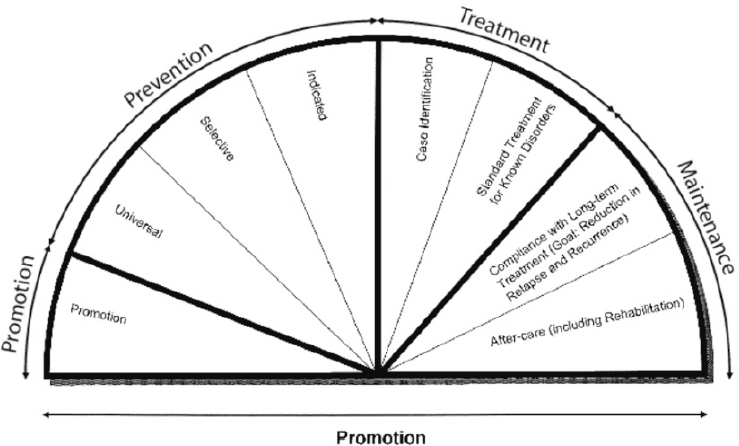
SOURCE: NRC and IOM (2009).
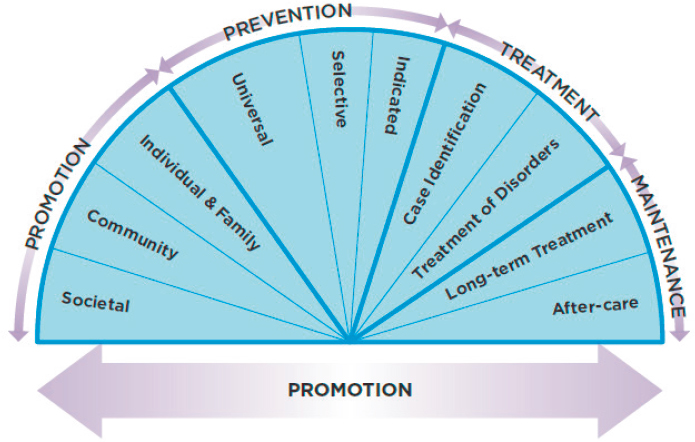
The present committee has again updated this figure. We have reviewed recent developments in the research related to fostering healthy MEB development and wish to highlight the critical importance of actively promoting healthy MEB development across the entire population of children and youth. In our version of the spectrum of interventions, the increased size of the promotion and prevention wedges reflects their importance (see Figure 1-3). While these updates reflect important trends in the research in this field, they also reflect the enduring importance of a spectrum of key tools for fostering MEB health. We emphasize the importance of using those tools to improve MEB development and health, a challenge that must be met if population-level adverse MEB outcomes are to be reduced.
COMMITTEE’S APPROACH TO ITS CHARGE
The 2009 NRC and IOM report focuses on the individual: on single gene influences, single risk factors, single points in development, and individual families and children. Since its release, the critical importance of promoting healthy development, in addition to preventing risks, has been underscored by growing evidence about the key conditions in families, neighborhoods, and communities that encourage or interfere with healthy MEB development, including environmental, biological, and behavioral factors. The committee was struck by the quantity and quality of new science important for understanding the determinants of MEB health and how that knowledge can be used. We highlight
here two strong new bodies of evidence and then discuss how they influenced our study process.
New Research Perspectives
Research in fields including neurobiology, epidemiology, public health, the social and behavioral sciences, implementation science, and prevention science has yielded a remarkable expansion in understanding of the interrelationships among a broad set of influences on MEB development. These insights have important implications for future efforts to foster healthy MEB development. At the same time, researchers have significantly expanded understanding of what is necessary for effective implementation of strategies to promote MEB health and prevent MEB disorders.
Integrated Understanding of Influences on MEB Health
In the past decade, strong evidence has emerged that MEB health is influenced by a dynamic interplay among influences at the biological, family, community (including schools and health care services), and societal levels, starting at preconception and extending through fetal life, infancy, childhood, adolescence, and adulthood. Previous research had identified statistical relationships between brain development and neuronal maturation on the one hand and epigenetic effects and societal influences on the other, but had not established mechanisms that would explain possible connections. New studies have made it possible for the first time to link individual, community, and societal well-being and pathology through clear epidemiological and biological research.
In addition, while prior research had pointed to the influence on development of a wide range of factors, including societal influences such as political values and racism, the period since 2009 has seen the emergence of new research on the critical role of neighborhood residence in life expectancy, income mobility, school performance, and chronic diseases. The striking disparities in outcomes for children and families across many communities based on race/ethnicity and socioeconomic status underscore the powerful influence of the neighborhood and community on children and their families.
Expanded Understanding of Implementation
Progress has occurred in research on how effective interventions can best be implemented. The 2009 NRC and IOM report notes that effective interventions were often not being made widely available or implemented faithfully. Since that time, however, significant investments have been made in research on the implementation and dissemination of strategies. This body of work has begun to yield a fuller picture of what effective implementation entails, showing that adoption of an evidence-based program and faithful adherence to the protocols for its use are necessary but not sufficient. It offers expanded guidance on how
interventions that promote well-being can be scaled and sustained in communities across the country and insights into why research-based implementation strategies have produced limited benefits in the past.
The committee was aware that significant advances in treatment have also occurred since the 2009 report was issued. For example, evidence is starting to emerge that treatment for depression administered via the Internet is effective (e.g., Buntrock et al., 2016; Karyotaki et al., 2017), as are evidence-based therapies administered by properly trained and supervised lay health workers (Chibanda et al., 2016; Dias et al., 2019). We reviewed important advances in treatment of maternal depression before, during, and after pregnancy. Some of these developments offer opportunities that are particularly relevant for promotion of MEB health and prevention of MEB disorders. Advances that can better treat milder disorders, address relapses, and prevent youth with disorders from lapsing into more serious psychoses (Fisher et al., 2013) are an important component of any effort to promote MEB health.
These developments are important, but despite this progress, the overall prevalence rates of MEB disorders have not improved; even the most effective treatments go only so far given the many chronic disorders and persistent sources of risk. We note that even where well-studied efficacious treatments are available, children and youth often do not have adequate access to providers who can accurately diagnose and treat MEB disorders. For example, of the 3.1 million children in the United States who experienced depression in 2016, just 41 percent received treatment. While addressing this gap is critical, the committee’s focus was on promoting healthy MEB development; we viewed promotion and prevention efforts to reduce the need for mental health treatment as the overall directive in our statement of task (refer to Box 1-1).
Implications
The important developments summarized above made it clear that the committee would need to look beyond the evidence base for intervention strategies focused on individuals and their families, the primary focus of the 2009 report. We recognized that we would need to apply a much wider lens, and we describe here several specific perspectives that guided us in identifying the topics we would cover and the evidence we would seek.
A Life-Course Approach to Understanding Development
The idea that developmental trajectories for both individuals and populations are strongly affected by social and temporal influences, which is increasingly dominant in public health studies, may seem to be common sense. But the growing evidence of the interplay among genetic, biological, social, and environmental influences on development, beginning before a child is even
conceived, has profound implications for thinking about interventions to promote healthy MEB development.
Recognizing that we would need to look across generations, we sought evidence about multigenerational influences (the lasting effects on a developing child of experiences and exposures in their parents’ and grandparents’ lives); biological, social, and psychological influences with varying effects across developmental phases; and reciprocal influences at the individual, community, and societal levels.3 The complexity of the interactions among these and other influences on MEB development underscored the need to reconsider the individual-centric approach that has been typical in child care and treatment—to consider factors at multiple levels and across sectors that encourage healthy MEB development and promote resiliency.
Although measurement of resiliency and of the positive features of environments and their interactions is in its infancy, we adopted a broader view than the authors of the 2009 report had reason to take. They recognized that there are opportunities for promotion of MEB health and prevention of MEB disorders throughout childhood and adolescence, noting that some interventions work well across all developmental stages but that most have particular effects at specific stages. Research building on that understanding has highlighted the importance of the health of prospective mothers and fathers even prior to conception, as well as the community-level and policy interventions that influence people and families at every age. We therefore examined influences that have effects beginning before conception and at stages of life extending into young adulthood and across generations. That is, we took what is known as a life-course approach, recognizing the importance of risk and protective factors over time; at various developmental phases; and at the individual, community, and societal levels. Figure 1-4 illustrates this approach.
A Public Health Framework for MEB Health Promotion
Our focus on a life-course approach dovetailed with the remarkable growth in research evidence on the complexity of child development and the importance of the interaction among biological, social, and cultural influences from the molecular to the societal level, evidence that has led to an expansion in focus from intervening solely with the individual child (the organism) to intervening at the societal and community levels (the environment). This expanded understanding encouraged us to broaden our focus beyond the prevention strategies that may help the individual child, emphasized in the 2009 report, to health promotion and community wellness approaches that have greater potential to benefit populations
___________________
3 For purposes of exposition, we have organized our discussion of both influences on MEB health and interventions by the individual, community, and societal levels, recognizing that these distinctions are often arbitrary and overlapping.
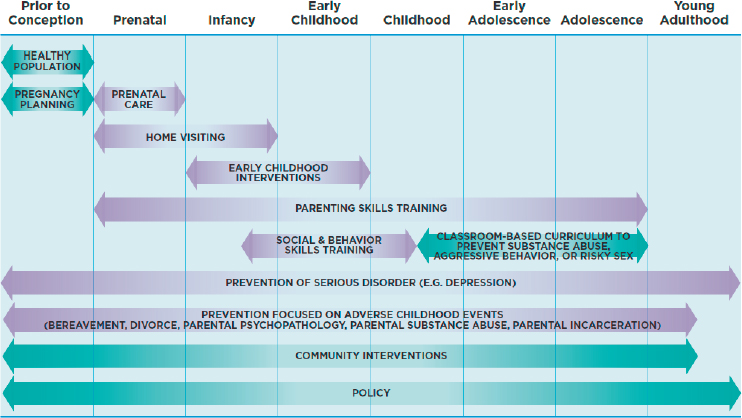
as well as individuals. Accordingly, this report is framed to emphasize the importance of integrating promotion efforts to maximize their impact across the population of children and youth.
The breadth of the dual goals of promoting healthy MEB development and reducing the incidence and prevalence of MEB disorders among all young people made it evident that a multifaceted public health strategy involving all sectors and institutions serving children and youth would be needed. A public health approach focuses on programs, policies, and practices that affect well-being in a population, including efforts to promote changes in relevant values and norms. To reach entire populations, public health measures must be efficient. Relying not just on program development and evaluation, which have been at the heart of prevention science, a comprehensive public health approach also makes use of public policy, media campaigns, and universal approaches to intervention, such as in health and education systems, because they can affect an entire population. Reducing the population prevalence of MEB disorders will require targeting of factors and settings that offer potential to affect the entire population.
One of the most important advances in public health in the 20th century—progress made in reducing cigarette smoking—provides a model for promoting the well-being of children and adolescents. There are many pharmacological and psychological programs aimed at helping smokers quit, but the large reductions in smoking rates that occurred in the second half of the 20th century (a 58.2% decline in smoking among adults from 1964 to the early 2000s; IOM, 2007) depended on a comprehensive public health movement. This movement mobilized a broad coalition of scientific, public health, and advocacy organizations to expand public understanding of the harmful effects of smoking; introduced financial and location barriers to smoking; and brought about historic changes in public opinion and public policy. Tools used in
the antismoking effort included credible scientific reports; coordination of cultural, media, and legal efforts; policy efforts at the federal, state, and local levels; and monitoring of relevant data. While problems with smoking—and vaping—have not been eradicated within the United States, similar processes hold promise for promoting healthy MEB development.
A Community Approach to Fostering Healthy MEB Development
Children are deeply embedded in communities, which in turn are integrated within the larger society. Public health approaches to promoting healthy MEB development and preventing MEB problems are essential to achieving population-level impacts on MEB health outcomes and may have significant effects on behaviors, but they lack the power to address broader influences on health and development. We recognize that some readers may regard our including consideration of broad societal issues in this report as idealistic or impractical, but the committee members were of one mind from the start that there are two strong reasons for treating these issues as critically important for effectively nurturing healthy development.
First, support at all levels—community, county, state, and federal entities and agencies; foundations; businesses; national advocacy organizations; and scientific organizations—will be required to implement strategies that can improve MEB outcomes for children and adolescents. Evidence-based strategies will achieve positive impacts on MEB health only if they affect not just individual families but also schools, neighborhoods, and communities. It will be essential for multiple service sectors, such as primary health care, behavioral health, child welfare, juvenile justice, education, child care, and other social services, to be part of the solution.
Second, evidence and practical experience both point to the importance of community and policy interventions in pursuing a more nurturing society. Growing evidence is revealing that large-scale prevention efforts implemented with fidelity in communities with high rates of poor outcomes for adolescents can have strong and consistent effects (Fagan et al., 2019). Such results support the idea that the community is an effective unit for intervention because it is small enough to marshal significant resources and large enough to show sustainable population effects; its modest scale also facilitates careful evaluation of outcomes.
In short, our initial review of the emerging research clearly suggested that achieving a society with flourishing children and lower rates of MEB disorders will require changes at every level, from improving the moment-to-moment interactions between a parent and a child to adopting policies at the federal level that affect poverty and disparities in socioeconomic status, education, and health across the nation. We return to these issues at the end of this report.
A Word about Evidence
The study charge (refer to Box 1-1) required us to review relevant evidence spanning a wide range of topics, including the integration of MEB health interventions into primary care and other health care settings; technology-based interventions aimed at preventing specific MEB conditions, such as depression; integration of strategies for the promotion of healthy MEB development into broad public health approaches; the influence of the environmental context on neurobiology; and the implications for strategies to promote healthy MEB development. We looked across stages of development and different environments, and we drew on multiple academic disciplines, ranging from those that rely primarily on laboratory-based research to those that make use of a variety of qualitative research methods.
Our goal was to synthesize the conclusions for which strong evidence exists, recognizing that standards of evidence vary across disciplines according to the types of data and analyses that are suitable for different research objectives and contexts. In the chapters that follow, we discuss the kinds of evidence available to evaluate the topics addressed, but we note here that our conclusions and recommendations reflect our collective judgment about the strength of the evidence relevant to each topic. We recognize that opinions differ as to the relative merits of different research approaches for different purposes, but resolving those differences is beyond the scope of this study. For simplicity, we use the term “effective” throughout the report to characterize those approaches we collectively judged to be supported by adequate evidence from studies in multiple settings. We also note that evidence for the benefits of interventions generated in experimental settings does not necessarily translate to the same benefits in other settings, or in broad applications.
STUDY PROCESS
The committee used a variety of strategies to examine evidence on a wide range of topics. Two open public sessions gave us the opportunity to hear multiple perspectives on objectives for promoting MEB health, effective public health messaging strategies, and advances in implementation science.4 We arranged teleconferences to hear from experts on topics including adverse childhood experiences, measurement tools and methodology, National Institutes of Health funding opportunities for prevention activities, public health approaches to fostering MEB health, monitoring of the social-emotional development of young children, prevention and implementation science, and the role of businesses in
___________________
4 Videos and slideshows from these presentations are available on the study website, see http://nas.edu/MEB-Health.
promoting MEB health. We also commissioned two papers to gain additional insights and information:5
- Laws Influencing Healthy Mental, Emotional, and Behavioral Development, by Kelli A. Komro, and
- Recent Trends in Child, Adolescent, and Young Mental, Emotional, and Behavioral Health in the United States, by Mark Olfson.
GUIDE TO THIS REPORT
Part I of the report (Chapter 2) sets the stage with an overview of the individual, family, community, and societal influences that shape MEB development in children and youth. Part II reviews research on effective strategies for promoting healthy MEB development: strategies that address families across multiple generations (Chapter 3), those used in education and health care settings (Chapters 4 and 5, respectively), and policy strategies (Chapter 6). Part II closes with a discussion of the body of evidence regarding interventions and some methodological considerations (Chapter 7). Part III examines the challenges of implementing effective strategies at scale: Chapter 8 describes the foundations on which effective implementation rests, while Chapter 9 looks at the functioning of a robust, sustainable implementation system. Part IV turns to the question of how the nation can take full advantage of this base of knowledge. Chapter 10 briefly reviews progress made since the 2009 NRC and IOM report. Finally, Chapter 11 returns to the vision with which this introductory chapter opened—of the potential impact of a decade in which healthy MEB development for children and youth is a top priority in the United States. In that final chapter, we offer recommendations for pursuing an agenda for fostering healthy MEB development and outline priorities for research to support sustained momentum toward that vision.
REFERENCES
Bethell, C.D., Gombojav, N., and Whitaker, R.C. (2019). Family resilience and connection promote flourishing among U.S. children, even amid adversity. Health Affairs, 38(5), 729–737.
Buntrock, C., Ebert, D.D., Lehr, D., Smit, F., Riper, H., Berking, M., and Cuijpers, P. (2016). Effect of a web-based guided self-help intervention for prevention of major depression in adults with subthreshold depression: A randomized clinical trial. Journal of the American Medical Association, 315(17), 1854–1863.
Center for Collegiate Mental Health. (2018). 2017 annual report. University Park, PA: Penn State University.
___________________
5 These papers are available under the Resources tab for download at https://www.nap.edu/catalog/25201.
Available: https://sites.psu.edu/ccmh/files/2018/01/2017_CCMH_Report-1r3iri4.pdf.
Center for the Study of Social Policy. (2012). Results-based public policy strategies for promoting children’s social, emotional, and behavioral health. Washington, DC: Center for the Study of Social Policy.
Chibanda, D., Weiss, H.A., Verhey, R., Simms, V., Munjoma, R., Rusakaniko, S., Chingono, A., Munetsi, E., Bere, T., Manda, E., Abas, M., and Araya, R. (2016). Effect of a primary care-based psychological intervention on symptoms of common mental disorders in Zimbabwe: A randomized clinical trial. Journal of the American Medical Association, 316(24), 2618–2626.
Dias, A., Azariah, F., Anderson, S.J., Sequeira, M., Cohen, A., Morse, J.Q., Cuijpers, P., Patel, V., and Reynolds, C.F., 3rd. (2019). Effect of a lay counselor intervention on prevention of major depression in older adults living in low- and middle-income countries: A randomized clinical trial. JAMA Psychiatry, 76(1), 13–20.
Dupéré, V., Dion, E., Nault-Brière, F., Archambault, I., Leventhal, T., and Lesage, A. (2018). Revisiting the link between depression symptoms and high school dropout: Timing of exposure matters. Journal of Adolescent Health, 62(2), 205–211.
Fagan, A.A., Hawkins, J.D., Catalano, R.F., and Farrington, D.P. (2019). Communities that care: Building community engagement and capacity to prevent youth behavior problems. New York: Oxford University Press.
Fernandes-Alcantara, A. (2015). Disconnected youth: A look at 16 to 24 year olds who are not working or in school. Washington, DC: Congressional Research Service. Available: https://fas.org/sgp/crs/misc/R40535.pdf.
Finkelhor, D., Turner, H., Shattuck, A., Hamby, S., and Kracke, K. (2015). Children’s exposure to violence, crime, and abuse: An update. Laurel, MD: Office of Juvenile Justice and Delinquency Prevention. Available: https://www.ojjdp.gov/pubs/248547.pdf.
Fisher, M., Loewy, R., Hardy, K., Schlosser, D., and Vinogradov, S. (2013). Cognitive interventions targeting brain plasticity in the prodromal and early phases of schizophrenia. Annual Review of Clinical Psychology, 9, 435–463. doi:10.1146/annurev-clinpsy-032511-143134.
Hair, E.C., Moore, K.A., Ling, T.J., McPhee-Baker, C., Brown, B.V., and Child, T. (2009). Youth who are “disconnected” and those who then reconnect: Assessing the influence of family, programs, peers, and communities. Research brief 2009-37. Washington, DC: Child Trends.
IOM (Institute of Medicine). (1994). Reducing risks for mental disorders: Frontiers for preventive intervention research. Washington, DC: National Academy Press.
———(2007). Ending the tobacco problem: A blueprint for the nation. Washington, DC: The National Academies Press.
Kamal, R. (2017). What are the current costs and outcomes related to mental health and substance abuse disorders? Peterson-Kaiser Health System
Tracker. Available: https://www.healthsystemtracker.org/chart-collection/ current-costs-outcomes-related-mental-health-substance-abuse-disorders /#item-disease-burden-alcohol-use-disorders-higher-average-u-s.
Karyotaki, E., Riper, H., Twisk, J., Hoogendoorn, A., Kleiboer, A., Mira, A., MacKinnon, A., Meyer, B., Botella, C., Littlewood, E., Andersson, G., Christensen, H., Klein, J.P., Schroder, J., Bretón-López, J., Scheider, J., Griffiths, K., Farrer, L., Huibers, M.J.H., Phillips, R., Gilbody, S., Moritz, S., Berger, T., Pop, V., Spek, V., and Cuijpers, P. (2017). Efficacy of self-guided Internet-based Cognitive Behavioral Therapy (ICBT) in treatment of depressive symptoms: An individual participant data meta-analysis. JAMA Psychiatry, 74(4), 351–359. doi:10.1001/jamapsychiatry.2017.0044.
Merrick, M.T., Ford, D.C., Ports, K.A., and Guinn, A.S. (2018). Prevalence of adverse childhood experiences from the 2011–2014 Behavioral Risk Factor Surveillance System in 23 states. JAMA Pediatrics, 172(11), 1038–1044.
Mojtabai, R., Olfson, M., and Han, B. (2016). National trends in the prevalence and treatment of depression in adolescents and young adults. Pediatrics, 138(6). doi:10.1542/peds.2016-1878.
National Alliance on Mental Health. (2013). Mental health by the numbers. Available: https://www.nami.org/learn-more/mental-health-by-thenumbers.
NRC and IOM (National Research Council and Institute of Medicine). (2009). Preventing mental, emotional, and behavioral disorders among young people: Progress and possibilities. Washington, DC: The National Academies Press.
Olfson, M. (2018). Recent trends in child, adolescent, and young adult mental, emotional, and behavioral health in the United States. Committee commission.
Sissons, P., and Jones, K. (2012). Lost in translation? The changing labour market and young people not in employment, education or training. Lancashire, England: The Work Foundation.


















