8
Implementing Family-Focused Preventive Interventions
David Hawkins, University of Washington, introduced the workshop session on family-focused preventive interventions by highlighting the importance of adult caretakers in promoting children’s well-being. He cautioned that universal interventions such as parenting workshops may increase health disparities, because those who are most able to utilize these preventive interventions are those who have enough time to participate, childcare options during the intervention workshops, and access to transportation to get to the workshops. Attendees were asked to consider how to provide the tools and resources parents need to succeed in their child-rearing roles in a way that increases health equity. Hawkins referenced a recent Child Trends article that found parents often receive insufficient information from pediatricians and seek information on parenting skills from the Internet (Bartlett et al., 2017). In an effort to achieve health equity across populations, he concluded, it is necessary to address the inconsistency in resources offered to parents that will allow them to best support their children as they grow.
Joyce Javier, University of Southern California Keck School of Medicine, and Lourdes Molleda Rojas, University of Miami, gave presentations on how family-focused preventive interventions have been implemented in Filipino and Latino communities, despite barriers they both face.
INCREASING ACCESS TO PARENTING INFORMATION AND TOOLS
Building Supports for the Los Angeles Filipino Community
Joyce Javier focused on how to address health disparities among minority immigrant populations and increase parents’ access to skills and tools from trusted sources such as pediatricians. Her research focuses on the Filipino population, the second largest Asian subgroup in the United States and the largest Asian subgroup in California (U.S. Census Bureau, 2012). Despite the size and growth of this population, Filipinos are often referred to as an “invisible minority” due to the lack of health-related research and programs targeted to them, which has resulted in notable disparities. According to a 2001 study from the Centers for Disease Control and Prevention, Filipina adolescents in grades 9–12 had the highest rate of suicidal thoughts among all other ethnic groups in the study. Of the group of Filipinas who reported having suicidal thoughts, nearly one-half committed suicide within the following year (Centers for Disease Control and Prevention, 2001). Other studies have shown higher rates of teen pregnancy, depression, anxiety, and drug use in the Filipino-American population (Javier et al., 2007).
Over the past decade, Javier has partnered with the Filipino community in Los Angeles to identify how to prevent certain risky behaviors among adolescents and to find possible solutions. Javier’s research team started with a community needs assessment, engaging with church leaders, parents, teenagers, teachers, and health and mental health providers. The assessment focused on children’s school-age years and sought ways to promote parent-child relationships before children reach adolescence. One provider suggested that Javier use The Incredible Years program and implement the program in churches in an effort to avoid issues of stigma.1
Javier and her team received a grant to test The Incredible Years program in local church settings and found that the intervention was culturally acceptable in the Filipino community. The results of the study found decreases in parenting stress; increases in the use of positive discipline, such as praise; decreases in physical punishment; and improvements in both internalizing and externalizing symptoms.
While these results were promising, Javier reported that only 20 percent of the parents who were initially contacted for the study agreed to participate. In an effort to increase participation, Javier and her team sought input from the study’s Community Advisory Board. Board members indicated that they were hesitant to focus on the problems in their community or “air
___________________
1 For more information, see http://www.incredibleyears.com.
dirty laundry.” Instead, they suggested shifting the focus of the program to how it promotes social and academic success in youth. Parents from the initial pilot study also suggested more parents might enroll if they were made aware of the existing disparities that impact the Filipino community.
Increasing Demand
A second grant allowed Javier and her team to design a video intervention focused on increasing enrollment rates. This video intervention was created based on the health belief model and the theory of planned behavior. The video included statistics on existing health disparities that impact the Filipino community to promote more parental engagement. Javier’s research team looked at two outcomes from this intervention study: intention to enroll in The Incredible Years in the next 6 months and the number of parents who participated in the program. The intervention enrolled 215 parents in various communities with dense populations of Filipino families. Javier noted that the most common place where parents agreed to participate in the study was in a primary care setting; 45 percent of parents who participated enrolled through a pediatrician.
Javier’s study found that parents in the intervention group had significantly greater odds (OR = 2.7) of enrollment in The Incredible Years than the control group. Her team also found that the intervention video affected perceived susceptibility and new knowledge affected intention to enroll, which led to actual enrollment. In examining why the video worked, Javier found that the effect of the intervention video on enrollment was mediated by increasing knowledge among parents of Filipino behavioral-specific disparities. Javier is continuing to participate in community dialogues to develop a shared definition of childhood mental health in the Filipino community.
Javier observed that pediatricians are only briefly exposed to training about parenting during their residency, which may be why it is not a focus in primary care. She initially became involved when she partnered with a psychologist running trial groups and thought parenting support was something that could help the families in her clinics.
To gain support for these two studies, Javier and her team used different methods to engage stakeholders. The team held multiple meetings over 9 months with clinic administrators to determine how to refer patients and identify barriers affecting further collaboration. Javier said she became “The Incredible Years champion” and promoted the program to pediatricians and pediatric residents through lectures on the benefits of evidence-based parenting interventions. She solicited advice from developmental and behavioral pediatricians on how to promote more referrals and how to integrate parenting interventions into primary care. Javier also established
a partnership with her hospital’s employee child development center to provide childcare for the families who participated in the intervention. Her research team managed to have some of their intervention teachers hired by the childcare center so that skills from The Incredible Years were also used in the center. They also held a 1-day management training on The Incredible Years for 30 teachers.
Addressing Demand
Javier highlighted barriers to implementation that her team experienced. She anticipated the stigma associated with referral to a behavioral health intervention, so rather than asking for children with behavioral issues to be referred, her program was open to any family who wanted to participate. A second barrier was a lack of grant funding. Javier noted that the LA County Department of Mental Health funds early intervention and prevention programs. To integrate the program into primary care, Javier saw the patients before and after the first and last parenting group so she could be the bridge between the mental health group and the pediatrician.
Javier reported that 41 parents have been referred to her program, and 24 have participated. This 56 percent enrollment rate shows an increase from the 20 percent rate from her first study. The program has enrolled predominantly male patients, mostly Spanish speaking and with an average age of 4.5 years. The full program is 18 weeks long, and the mean number of sessions attended is 12.5. During the intake process, many patients were found to have ADHD. Some patients were found to have anxiety and disruptive behavior not otherwise specified.
Evaluation of The Incredible Years has shown overall that when parents participate during their child’s preschool years, the children are less likely to be obese in adolescence. In the future, Javier would like to look at the impact of The Incredible Years on utilization of pediatric health services, in part to make the case to funders and insurers that this program should be reimbursed. She would also like to look into whether The Incredible Years decreases hospitalization and ER visits. Javier and her team are currently piloting a 6- to 8-week universal version of The Incredible Years in a primary care setting and a Filipino cultural school.
Javier addressed the issue of sustainability by noting the LA County Department of Mental Health has announced a Community Outreach Services Branch. The goal of this branch is to increase the number of individuals receiving prevention and early intervention and to do so in a culturally appropriate manner. The branch is also trying to reach out to people who are not formal clients of the mental health care system, using providers who are outside of the county mental health system. The Incredible Years is now on the list of programs that is offered to people in the community.
To conclude, Javier stated that increasing knowledge of adolescent risky behaviors can increase enrollment of parents in evidence-based parenting interventions. She noted that community engagement is a critical tool to recruit understudied populations. She also highlighted the importance of learning how to implement evidence-based practices in real-world settings. Parenting and primary care can reduce stigma associated with these programs and help promote parenting skills, not just as tools for addressing mental or behavioral issues, but also for addressing other health issues.
SUPPORTING PARENTS IN PRIMARY CARE
Lourdes Molleda Rojas reiterated that parenting programs are known to prevent mental, emotional, and behavioral health problems in youth. She summarized a review by Sandler and colleagues (2014) that found parenting programs can reduce externalizing problems such as conduct disorders and social aggression, as well as internalizing problems such as anxiety, substance use and abuse, and high-risk sexual behaviors. These programs have also been found to increase self-regulation and self-esteem and to improve academic success. They also help parents to build skills, including effective communication with their children, she noted.
Blueprints for Health Youth Development has identified as least 28 family-based parenting programs shown to be effective. Some of these programs, such as TripleP, Nurse-Family Partnership, and The Incredible Years, are widely disseminated. Other emerging programs, such as Generation PMTO, Family Check-Up, Strong African American Families, and Familias Unidas, are also effective but are struggling to disseminate widely. Rojas noted that there are several barriers that have prevented these programs from disseminating, including a lack of resources. These family-based parenting interventions are usually offered in clinics, community settings, and schools. However, there is now a movement to offer these programs in primary care settings. The American Academy of Pediatrics recommends parents take their children to a pediatrician more than nine times before the age of 2, which means there are at least nine opportunities for a parent and child to talk together to a physician about health. Schools also mandate physical exams, providing another time when children are visiting physicians with their parents to discuss health. According to the America’s Children survey, the percentage of children ages birth to 17 who had a well-child or adolescent visit in the previous year increased from 73 percent in 1997 to 84 percent in 2013 (Federal Interagency Forum on Child and Family Statistics, n.d.). Rojas said that research also shows a pediatrician’s office is a trusted local and family-friendly setting because families know their pediatricians as well as the nurses and office staff.
Familias Unidas
Familias Unidas was created by Hispanic investigators Dr. Hilda Pantin and Dr. Guillermo Prado and is staffed by a majority Hispanic team, Rojas said. It is a family-centered, evidence-based intervention that aims to prevent behavior problems such as adolescent substance use and risky sexual behaviors in Hispanic youth by improving family functioning. The program was developed 15 years ago based on evidence showing significant health disparities between Hispanic youth when compared to other races: Hispanic youth were initiating substance use earlier and there were higher rates of HIV infection in Hispanic youth compared to white youth, disparities that still persist. A recent survey found that Hispanic students in grades 9–12 reported feeling sad or hopeless, using electronic vapor products, and having five other drug or alcohol use behaviors at a higher rate than white or black students. Another study found that Hispanics have the highest annual prevalence in 12th grade for using dangerous drugs such as crack. A 2015 survey found Hispanic/Latinos account for 24 percent of new HIV cases in the United States, even though they account for only about 18 percent of the total population. Rojas also noted that gonorrhea and chlamydia rates are 1.7 and 1.9 times higher, respectively, for Hispanics than for whites.
Familias Unidas attempts to address these issues using the ecodevelopmental theory that places adolescents in the center of different worlds, Rojas explained (Pantin et al., 2003; see Figure 8-1). These worlds include their family, their peers, and larger macro systems such as cultural values and immigration policies. The theory is based on the idea that to help an adolescent, the family and peer contexts must be addressed. Rojas said that family-based interventions, especially for Latinos, strengthen the family, which acts as a strong protective factor for major behavioral health issues.
Rojas described Familias Unidas as a 12-week intervention program for families facilitated and delivered by a Hispanic community member. According to Rojas, the facilitator is usually established in the community as a school counselor, mental health worker, or social worker. Throughout the program, six to eight parents participate in 2-hour meetings with a facilitator to discuss parenting strategies. At the beginning of the program the topics are broad, such as how parents can communicate and form bonds with their children. As the program progresses, the topics become more challenging and include conversations about drug use, sex, and condom use. After the completion of these small group meetings, the parents have one-on-one meetings with their child, guided by the facilitator, to practice these skills. Rojas reported that in four efficacy and efficiency trials that compared youth in this program to youth in control conditions, Familias Unidas participants report 20 percent less drug use, 30 percent fewer
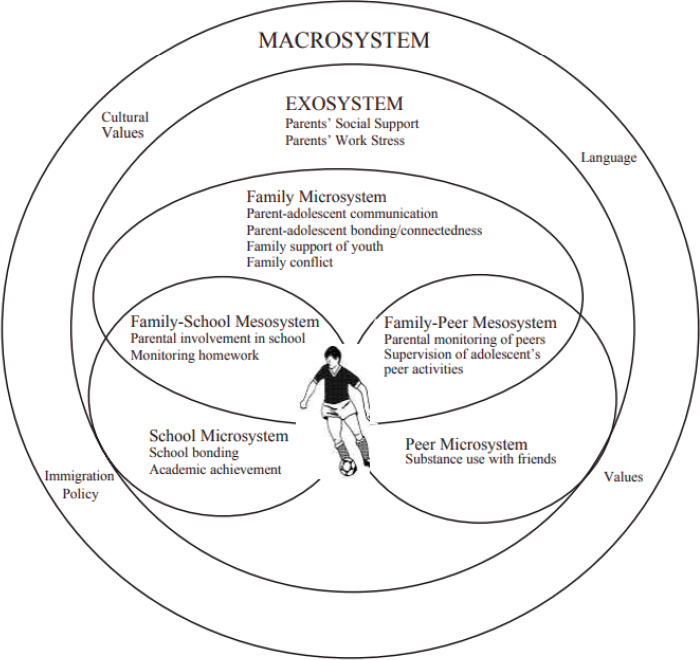
SOURCE: Pantin et al. (2003).
depression symptoms, 60 percent more condom use, and 88 percent less cigarette use.
According to Rojas, although the program has shown significant positive outcomes, there are still barriers to progress. For example, parents have to commit to 2 hours every week to participate in the program. The facilitators also have to commit to this time, and often have to drive families home at the end of a meeting. Additionally, the program faces a lack of financial resources to pay for the facilitator.
To address these barriers, the developers of the program created an Internet adaptation called eHealth Familias Unidas. The adaptation still follows the core values of the ecodevelopmental theory, but the parent group sessions are replaced with online videos. The videos use a telenovela-style format that parallels the topics of discussion from the intervention.
The intervention also includes an educational talk show segment where the lead clinical supervisor talks to parents in the community about the issues and asks them to respond to the telenovela. Parents participate in interactive exercises such as answering questions like “What are the goals for your family?” Data are collected for the facilitator so that goals can be addressed via teleconference meetings with the families. Rojas said this decreased the burden on families and facilitators by reducing the number of facilitator sessions from 12 to 4, and shortened the duration of each session to 45 minutes. The adapted program ensures intervention fidelity by making sure parents receive the intended materials.
Rojas shared that the Familias Unidas team has partnered with 40 public schools in Miami-Dade County to distribute both the traditional face-to-face program and the eHealth version. The next focus is to move to primary care settings. The team conducted a pilot study in a primary care clinic that enrolled 48 Hispanic adolescents between the ages of 12 and 16, along with their parents. Participants were randomized into eHealth Familias Unidas or care as usual. In this small pilot study, 93 percent of families approached in the clinic agreed to participate. Of these families, 93.5 percent of families actually engaged in the intervention, defined as at least watching the first session and contacting the facilitator. Additionally, 89 percent of these families completed post-intervention assessments.
On the basis of the findings from this pilot study, Rojas wanted to get feedback from clinical personnel, facilitators, and parents on how feasible and acceptable it is to bring a behavioral health prevention program into clinics. Through interviews with these stakeholders, three themes emerged. First, it is important to establish the relevance of the intervention to the setting and population. Second, pediatric primary care facilities are places families frequently visit. Finally, the team learned it is important to promote the clinic as a trusted setting to improve children’s behavioral health. Rojas noted that an additional benefit of recruiting families in the primary care setting is that the physician is aware that the parents are participating in this online program.
Rojas described a new trial recruiting 456 Hispanic adolescents and their parents. This trial is training nurses and students in need of clinical hours to deliver the intervention to families. Mobile clinics are also in use to reach the underserved areas in Miami as well as other communities. After participants are recruited into the trial, there will be follow-up visits in the participants’ home at 6 months, 12 months, 24 months, and 36 months.
DISCUSSION HIGHLIGHTS
Hawkins summarized several key takeaways from the two presentations. They included the idea that interventions can be successful when integrated into primary care settings, especially if they are culturally
appropriate. Additionally, technology may have a role to play in these interventions. He also noted that the success of these two programs demonstrates the willingness of primary care providers to support family-focused interventions.
In response to a question about the high participation rates in the Familias Unidas pilot study, Rojas said she believes families want to participate because of the context in which the services are provided. According to Rojas, families are expecting to receive services in a health setting and this program offers them an additional service. Alternatively, in a school setting, families are not expecting these services. She noted that these observations are based on qualitative data for a limited sample of families.
During the discussion session, workshop participants also talked about making these programs culturally acceptable. Both presenters said they made an effort to explain to families that The Incredible Years and Familias Unidas are prevention programs, and participation in them does not mean there is something wrong that needs to be corrected.
This page intentionally left blank.










