6
Potassium: Dietary Reference Intakes Based on Chronic Disease
This chapter presents the evidence on indicators that could potentially inform the potassium Dietary Reference Intakes (DRIs) based on chronic disease and the committee’s determination regarding its ability to establish a potassium Chronic Disease Risk Reduction Intake (CDRR). In its application of the recommendations in the Guiding Principles for Developing Dietary Reference Intakes Based on Chronic Disease (Guiding Principles Report) (NASEM, 2017), the committee first reviewed the evidence on chronic disease indicators. For indicators with at least moderate strength of evidence for a causal relationship, the committee characterized the intake–response relationship. This evidence informed the committee’s conclusion regarding the potassium CDRR.
REVIEW OF CHRONIC DISEASE INDICATORS
The Guiding Principles Report recommended:
The ideal outcome used to establish chronic disease [DRIs] should be the chronic disease of interest, as defined by accepted diagnostic criteria, including composite endpoints, when applicable. Surrogate markers could be considered with the goal of using the findings as supporting information of results based on the chronic disease of interest. (NASEM, 2017, p. 123)
In accordance with this guidance and the first step of the DRI organizing framework (see Chapter 1, Box 1-2), the committee reviewed evidence for the causal relationship between potassium intake and indicators that
could potentially inform the potassium CDRRs, which included chronic disease endpoints and surrogate markers (see Table 6-1).
Evidence on the indicators reviewed in this chapter was drawn primarily from the Agency for Healthcare Research and Quality systematic review, Sodium and Potassium Intake: Effects on Chronic Disease Outcomes and Risks (AHRQ Systematic Review) (Newberry et al., 2018). Therefore, the evidence reflects the methodologies used in the AHRQ Systematic Review, including the approach to the literature search, application of the inclusion/exclusion criteria, assessment of risk of bias, and determination of the strength of evidence. The committee also conducted supplemental literature searches for select indicators not included in the AHRQ Systematic Review (see Appendixes D and E).
Approach to Reviewing Indicators
Use of Different Study Designs
In its application of the Guiding Principles Report (NASEM, 2017), the committee considered the use of evidence from different study designs in its derivation of the potassium CDRRs. As compared to randomized controlled trials, observational studies are inherently weaker for establishing causal relationships and begin at a lower strength of evidence rating in the Grading of Recommendations Assessment, Development and Evalua-
TABLE 6-1 Potential Chronic Disease Indicators Reviewed for a Causal Relationship with Potassium Intake, in Order of Presentation
| Indicator | 2005 DRI Report | AHRQ Systematic Review | Committee’s Supplemental Literature Search |
|---|---|---|---|
| All-cause mortality | X | ||
| Cardiovascular disease | X | ||
| Coronary heart disease | X | X | |
| Myocardial infarction | X | ||
| Stroke | X | X | |
| Blood pressure | X | X | |
| Kidney stones | X | X | |
| Chronic kidney disease | X | ||
| Osteoporosis and related indicators | Xa | X | |
| Type 2 diabetes, glycemic control, and insulin sensitivity | X |
NOTE: AHRQ = Agency for Healthcare Research and Quality; DRI = Dietary Reference Intake.
aThe 2005 DRI Report reviewed evidence on bone demineralization.
tion (GRADE) system (Guyatt et al., 2011). The strength of evidence from observational studies can be upgraded, for instance, when the relationship cannot be explained by uncontrolled confounding, when there is a large effect size, or when there is a strong intake–response relationship.
In accordance with the first step of the DRI organizing framework and the guidance provided in the Guiding Principles Report (NASEM, 2017), the committee first sought to identify evidence intake of at least moderate strength that established causality between potassium intake and a chronic disease indicator. To that end, the committee placed the highest value on evidence from randomized controlled trials (i.e., evidence of effect). Evidence from observational studies (i.e., evidence of association) is described throughout this chapter to summarize the landscape of evidence on the relationship between potassium and chronic disease. In its application of the Guiding Principles Report, however, the committee recognized the challenges of using observational studies to derive a potassium CDRR, because it is difficult to establish causality from observational data and it is difficult to determine the independent effect of potassium, owing to its collinearity with other nutrients. The committee therefore decided that if there was sufficient strength of evidence from trials alone, only such evidence would be used to establish the potassium CDRRs. It also decided that individual observational studies rated as low risk of bias could serve as supportive evidence, particularly when evidence from randomized controlled trials was few or unavailable, but would not serve as the sole evidence used to derive the potassium CDRRs.
Committee-Conducted Meta-Analyses
The committee rated the AHRQ Systematic Review as being of moderate quality, as guided by AMSTAR 2 criteria (for additional details, see Appendix C).1 One of the domains that the AHRQ Systematic Review did not adequately cover related to investigation and explanation of the causes of heterogeneity in the results of meta-analyses. The committee determined that exploring sources of heterogeneity was essential for fully evaluating the strength of evidence, particularly when inconsistency was a concern in the body of evidence (for an explanation of the importance of explaining heterogeneity, see Chapter 2). Thus, the committee undertook analyses to explore heterogeneity in the trial evidence on the relationship between potassium supplementation and blood pressure (for details, see the Blood Pressure section below).
___________________
1 AMSTAR stands for A Measurement Tool to Assess Systematic Reviews.
Review of Evidence on Indicators
The committee sought evidence on the independent effect of potassium intake on chronic disease risk. In the AHRQ Systematic Review, Chang et al. (2006) was included as evidence for the effect of potassium on all-cause mortality, cardiovascular disease mortality, and coronary heart disease mortality. The study assessed the effect of potassium-enriched salt on outcomes among elderly male veterans living in five retirement homes in northern Taiwan. Because the intervention concomitantly reduced sodium intake while increasing potassium intake, evidence from Chang et al. (2006) is presented in the discussion of the moderating effect of potassium (see Chapter 3).
The sections that follow present the body of evidence for a relationship between potassium intake and the potential chronic disease indicators outlined in Table 6-1. For context, evidence and conclusions presented in the Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate (2005 DRI Report) (IOM, 2005) are summarized for each indicator.
All-Cause Mortality
All-cause mortality is a clearly defined endpoint that is not specific to any chronic disease, but is heavily influenced by chronic disease mortalities. As such, it was included in context of potentially informing the potassium CDRR.
Evidence presented in the 2005 DRI Report The relationship between potassium intake and all-cause mortality was not reviewed in the 2005 DRI Report.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on all-cause mortality. Six observational studies assessed the association between potassium intake and all-cause mortality among generally healthy adults. Results were mixed among the four studies that assessed potassium intake through measurement of urinary potassium excretion—two studies did not find an association (Geleijnse et al., 2007; Kieneker et al., 2016b) while the other two reported an inverse relationship (BMJ, 1998; O’Donnell et al., 2014; Tunstall-Pedoe et al., 1997). Three studies that assessed potassium intake through self-report methods found an inverse relationship between potassium intake and all-cause mortality (Geleijnse et al., 2007; Seth et al., 2014; Yang et al., 2011). All studies were rated as having moderate
or high risk of bias. The AHRQ Systematic Review characterized the evidence as insufficient to identify an association between potassium intake and all-cause mortality.
The modifying effect of hypertension, established cardiovascular disease or high-risk diabetes, or chronic kidney disease on the relationship between potassium and all-cause mortality was also investigated. The AHRQ Systematic Review identified five observational studies (Dunkler et al., 2015; He et al., 2016; Leonberg-Yoo et al., 2017; O’Donnell et al., 2011; Yang et al., 2011). Findings across the studies were mixed, and all studies were rated as having moderate or high risk of bias. The AHRQ Systematic Review characterized the evidence on the modifying effect of chronic disease on the association between potassium intake and all-cause mortality as insufficient.
Committee’s synthesis of the evidence The lack of randomized controlled trials in which potassium intake was the only component of the diet modulated limits the committee’s ability to determine if potassium intake has an independent effect on all-cause mortality risk.
The observational studies included in the AHRQ Systematic Review were all rated as having moderate or high risk of bias and provided inconsistent evidence of an association between potassium intake and all-cause mortality. Studies that measured urinary potassium excretion varied in approach, and included collection of multiple 24-hour urines (Kieneker et al., 2016b), a single 24-hour urine (BMJ, 1998; Tunstall-Pedoe et al., 1997), timed overnight urine (Geleijnse et al., 2007), and a spot urine sample using the Kawasaki equation to estimate 24-hour potassium excretion (O’Donnell et al., 2014). The studies applied different statistical adjustments to control for potential confounders. The two studies that did not find an association (Geleijnse et al., 2007; Kieneker et al., 2016b) adjusted for a variety of demographic, lifestyle, and health factors, including urinary sodium excretion. The two studies that reported an inverse association made some of the statistical adjustments, but neither included urinary sodium excretion. One analysis only adjusted for age (Tunstall-Pedoe et al., 1997).
Studies based on self-reported dietary intake assessment methodologies found an inverse association between potassium intake and all-cause mortality. The risk-of-bias ratings for these studies were moderate or high. The analyses included statistical adjustments for various demographic, lifestyle, and health factors. Despite the consistency of the results from analyses based on dietary intake methodologies, the committee is unable to attribute the relationship to potassium intake because statistical adjustments may not be complete and causality cannot be determined.
Given the lack of randomized controlled trials and inconsistent results from observational studies that used a variety of potassium assessment
methodologies, had different statistical adjustments for potential confounding variables, and were rated as having moderate or high risk of bias, the committee is in agreement with the AHRQ Systematic Review assessment that there is insufficient evidence for a relationship between potassium intake and all-cause mortality.
Cardiovascular Disease
Evidence presented in the 2005 DRI Report The 2005 DRI Report included evidence on the relationship between potassium intake and the prevention of cardiovascular disease, specifically stroke and coronary heart disease (described below individually). Evidence on the relationship between potassium intake and cardiovascular disease, broadly, was not specifically reviewed.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on cardiovascular disease mortality and morbidity. Observational studies that assessed the association between urinary potassium excretion and composite cardiovascular disease outcomes among generally healthy adult populations mostly reported nonstatistically significant relationships (Cook et al., 2009; Kieneker et al., 2016b; O’Donnell et al., 2014). Similarly, no association was found between urinary potassium excretion and a composite cardiovascular disease outcome in a cohort of adults with mild to moderate chronic kidney disease (Mills et al., 2016). Among the studies reporting on combined cardiovascular disease morbidity and mortality, only one (Cook et al., 2009) was rated as having a low risk of bias; the other studies were rated as having a moderate or high risk of bias. Although generally similar, the definition of the composite cardiovascular disease outcome slightly varied across studies. The AHRQ Systematic Review characterized the evidence as insufficient to be able to identify an association between potassium intake and cardiovascular disease morbidity and mortality.
No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on cardiovascular disease mortality. Three observational studies in generally healthy adult populations provided mixed results regarding the association between potassium intake and cardiovascular disease mortality (Geleijnse et al., 2007; O’Donnell et al., 2014; Yang et al., 2011). These studies varied in potassium intake ascertainment that included spot urine sample, timed overnight urine sample, food frequency questionnaire, and 24-hour dietary recall. One study, conducted in adults with established cardiovascular disease or high-risk diabetes, did not find a statistically significant relationship
between baseline spot urine potassium excretion and risk of cardiovascular disease mortality (O’Donnell et al., 2011). All studies were rated as having a moderate or high risk of bias. The AHRQ Systematic Review characterized this evidence as insufficient to identify an association between potassium intake and cardiovascular disease mortality.
Committee’s synthesis of the evidence The lack of randomized controlled trials in which potassium intake is the only component of the diet modulated limits the committee’s ability to determine if potassium intake has an independent effect on the risk of cardiovascular disease mortality or combined cardiovascular outcomes.
The association between potassium intake and combined cardiovascular disease outcomes was not statistically significant in the observational studies included in the AHRQ Systematic Review. Findings were mixed among studies that assessed the association between urinary potassium excretion and cardiovascular mortality among various populations, with O’Donnell et al. (2014) reporting an inverse relationship, and Geleijnse et al. (2007) and a separate study by O’Donnell et al. (2011) reporting no significant associations. Studies with data collected through self-reported dietary intake methodologies were also mixed; an analysis based on food frequency questionnaires reported no significant relationship (Geleijnse et al., 2007) whereas an analysis based on 24-hour recalls reported an inverse relationship (Yang et al., 2011).
Since the release of the AHRQ Systematic Review, two additional observational studies meeting the AHRQ Systematic Review inclusion criteria have been published related to composite cardiovascular disease outcomes. Prentice et al. (2017) used data from the usual diet arm of the Women’s Health Initiative (WHI) Dietary Modification Trial and from the WHI Observation Study to assess the relationship between potassium intake measured by a baseline food frequency questionnaire and total cardiovascular disease among 86,444 postmenopausal women (high risk of bias study). An inverse relationship was found between baseline potassium intake (calibrated using urinary excretion) and total cardiovascular disease (coronary heart disease and stroke; hazard ratio [HR] = 0.86 [95% confidence interval {CI}: 0.75, 0.98]).2,3 The findings were slightly attenuated when using uncalibrated potassium intake (HR = 0.96 [95% CI: 0.94,
___________________
2 To correct for biases in the self-reported dietary intake data, potassium intakes from the food frequency questionnaires were calibrated using an equation developed from 24-hour urine samples and potential confounding variables on a subsample of 450 participants in the WHI Observational Study.
3 Findings were similar for an analysis expanding the definition of total cardiovascular disease to include coronary heart disease, stroke, coronary artery bypass graft, and percutaneous coronary intervention (HR = 0.87 [95% CI = 0.76, 0.99]).
0.98]). In an analysis of 6.5 years of follow-up in the Tehran Lipid and Glucose Study, baseline potassium intake as assessed by food frequency questionnaire was not associated with cardiovascular disease among 1,576 adults 30 years of age and older (high risk of bias study) (Mirmiran et al., 2018).
Given the lack of randomized controlled trials and inconsistent results among observational studies, all of which were rated as having a moderate or high risk of bias except one, the committee is in agreement with the AHRQ Systematic Review assessment that there is insufficient evidence for a relationship between potassium intake and either risk of combined cardiovascular disease mortality and morbidity or risk of cardiovascular disease mortality. The dietary assessment calibration approach used in Prentice et al. (2017) may have implications for future research, as the calibration can potentially correct for biases in the dietary intake assessment data, but this study alone is not strong enough to change the strength of the evidence grade.
Coronary Heart Disease
Evidence presented in the 2005 DRI Report The 2005 DRI Report included evidence from three prospective cohort studies that assessed the relationship between potassium intake and coronary heart disease (Bazzano et al., 2001; Khaw and Barrett-Connor, 1987; Tunstall-Pedoe et al., 1997). Findings were mixed. Evidence for coronary heart disease was not used to determine, support, or justify the potassium reference values established in the 2005 DRI Report.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on coronary heart disease morbidity and mortality. Two observational studies assessing the association between potassium intake and combined coronary heart disease morbidity and mortality met inclusion criteria. One study reported no significant differences in risk by quintile of urinary potassium excretion, based on multiple samples; the study was rated as having a moderate risk of bias (Kieneker et al., 2016b). The other study reported an inverse relationship, based on a single 24-hour urinary potassium excretion at baseline and was rated as having a high risk of bias (BMJ, 1998; Tunstall-Pedoe et al., 1997). The AHRQ Systematic Review characterized the evidence as insufficient to identify an association between potassium intake and coronary heart disease morbidity and mortality.
No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on coronary heart disease mortality. Two observational studies assessed the
relationship between potassium intake and coronary heart disease mortality. Both reported an inverse relationship, with hazards of coronary heart disease mortality decreasing with increasing potassium excretion or intake, based on a single 24-hour urinary potassium excretion at baseline (BMJ, 1998; Tunstall-Pedoe et al., 1997) or intake 24-hour dietary recalls (Yang et al., 2011). The studies were rated as having a moderate and high risk of bias. The AHRQ Systematic Review characterized the evidence as insufficient to be able to identify an association between potassium intake and coronary heart disease mortality.
Committee’s synthesis of the evidence The lack of randomized controlled trials in which potassium intake is the only component of the diet modulated limits the committee’s ability to determine if potassium intake has an independent effect on the risk of coronary heart disease mortality or combined coronary heart disease morbidity and mortality.
Two studies included in the AHRQ Systematic Review assessed the association between potassium intake and combined coronary heart disease morbidity and mortality. One of the studies only adjusted for age in its analyses and did not report confidence intervals (Tunstall-Pedoe et al., 1997). The other study did not find a statistically significant association between the average of multiple 24-hour urinary potassium excretions and coronary heart disease morbidity and mortality (HR, per 1,017 mg/d [26 mmol/d] increase in urinary potassium excretion = 0.90 [95% CI: 0.77, 1.04]) (Kieneker et al., 2016b). Since the release of the AHRQ Systematic Review, an additional study meeting inclusion criteria has reported an inverse relationship between calibrated potassium intake and coronary heart disease (inclusive of nonfatal myocardial infarction and coronary death; HR = 0.85 [95% CI: 0.73, 0.99]), based on data from the WHI Dietary Modification Trial and from the WHI Observation Study (Prentice et al., 2017). The findings were slightly attenuated when using uncalibrated potassium intake (HR = 0.94 [95% CI: 0.92, 0.97]).
Two studies included in the AHRQ Systematic Review suggest there is an inverse association between potassium intake and coronary heart disease mortality. As described above, one of the studies had incomplete exploration and reporting of the analyses (Tunstall-Pedoe et al., 1997). The other study reported decreased hazard for coronary heart disease mortality for each quartile of intake, as compared to the first quartile of usual potassium intake at baseline (1,793 mg/d [80 mmol/d]) (Yang et al., 2011). Since the release of the AHRQ Systematic Review, an additional study meeting the inclusion criteria reported an inverse relationship between calibrated potassium intake and coronary death, with a decrease in risk for every 20 percent increase in calibrated potassium intake (HR = 0.84 [95% CI: 0.74, 0.98]) (Prentice et al., 2017). The findings were slightly attenuated when using uncalibrated potassium intake (HR = 0.93 [95% CI: 0.89,
0.97]). The analyses adjusted for a variety of demographic, lifestyle, and health factors;4 however, neither body mass index nor incident hypertension were included in the disease risk model, to prevent overcorrection.
Given the lack of a randomized controlled trial and the observational studies having a moderate or high risk of bias the committee is in agreement with the AHRQ Systematic Review assessment that there is insufficient evidence on the relationship between potassium intake and coronary heart disease.
Myocardial Infarction
Evidence presented in the 2005 DRI Report Evidence on the relationship between potassium intake and myocardial infarction was not reviewed in the 2005 DRI Report.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on myocardial infarction. Two observational studies assessed the relationship between potassium intake and myocardial infarction in a cohort of generally healthy adults (Geleijnse et al., 2007; O’Donnell et al., 2014). Neither study found a statistically significant relationship between potassium excretion and myocardial infarction. The AHRQ Systematic Review rated both studies as having a high risk of bias, and characterized the evidence on the association between potassium intake and myocardial infarction as insufficient.
The AHRQ Systematic Review also included studies that assessed the association between potassium intake and myocardial infarction in a cohort of adults with hypertension (Alderman et al., 1997), mild to moderate chronic kidney disease (Mills et al., 2016), or established cardiovascular disease or high-risk diabetes (O’Donnell et al., 2011). None of the studies identified a statistically significant association between potassium intake and myocardial infarction. The AHRQ Systematic Review rated the studies as having a moderate or high risk of bias, and characterized the evidence on the moderating effect of select chronic diseases on the association between potassium intake and myocardial infarction as insufficient.
Committee’s synthesis of the evidence The lack of randomized controlled trials in which potassium intake is the only component of the diet modulated limits the committee’s ability to determine if potassium intake has
___________________
4 Adjusted for age, race/ethnicity, educational level, family history of premature cardiovascular disease, cigarette smoking status, treated diabetes, statin use, aspirin use, prior postmenopausal hormone therapy use, and an estimate of recreational physical activity.
an independent effect on the risk of myocardial infarction. None of the observational studies included in the AHRQ Systematic Review identified a statistically significant association between various measures of urinary potassium excretion and myocardial infarction. Since the release of the AHRQ Systematic Review, an additional study meeting inclusion criteria has reported an inverse relationship between calibrated potassium intake and nonfatal myocardial infarction (HR = 0.83 [95% CI: 0.72, 0.96]) (Prentice et al., 2017). The findings were slightly attenuated when using uncalibrated potassium intake (HR = 0.94 [95% CI: 0.92, 0.97]).
Given the lack of randomized controlled trials and the moderate or high risk of bias observational studies that, with the exception of one, did not find a statistically significant association between potassium intake and myocardial infarction, the committee is in agreement with the AHRQ Systematic Review assessment that there is insufficient evidence for a relationship between potassium intake and myocardial infarction.
Stroke
Evidence presented in the 2005 DRI Report The 2005 DRI Report summarized eight observational studies on potassium intake and stroke (Ascherio et al., 1998; Bazzano et al., 2001; Fang et al., 2000; Green et al., 2002; Iso et al., 1999; Khaw and Barrett-Connor, 1987; Lee et al., 1988; Sasaki et al., 1995). Several, but not all, of the studies found an inverse relationship between potassium intake and stroke-associated morbidity and mortality.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials met the AHRQ Systematic Review inclusion criteria for this outcome. Fifteen observational studies assessing the association between potassium intake and stroke were included.
Three studies assessed the association between urinary potassium excretion and stroke. Two of the studies did not find a statistically significant relationship (Geleijnse et al., 2007; Kieneker et al., 2016b). One study reported that the odds for stroke was significantly lower for those with estimated potassium excretions of 1,500–1,999 mg/d (38–51 mmol/d), as compared to those with urinary potassium excretions < 1,500 mg/d (< 38 mmol/d) (odds ratio [OR] = 0.82 [95% CI: 0.68, 0.99]); odds of stroke were not statistically lower for any of the higher categories of urinary potassium excretion, as compared to the < 1,500 mg/d (< 38 mmol/d) group (O’Donnell et al., 2014). The three studies were rated as having a moderate or high risk of bias. The AHRQ Systematic Review described the relationship between urinary potassium excretion and stroke as inconsistent.
Results from studies that used dietary intake assessment methodologies to assess the association between potassium intake and stroke were
also mixed. Three studies collected 24-hour dietary recalls. Bazzano et al. (2001) reported a statistically significant decrease in risk only between the first and second quartile of potassium intake (< 1,353 mg/d [< 34.6 mmol/d] versus 1,353–1,947 mg/d [35–50 mmol/d], respectively), but not at higher intake levels. Using data from the same cohort, Fang et al. (2000) found an inverse relationship between potassium intake and risk of stroke mortality among black males and white males; the relationship did not reach statistical significance among black females, white females, normotensive females, females with hypertension, or normotensive males. Another study, however, reported risk of stroke-related mortality to have an inverse relationship with potassium intake, particularly among women (Khaw and Barrett-Connor, 1987). Findings were mixed among studies that assessed potassium intake through food frequency questionnaire. Several did not find a statistically significant relationship between potassium intake and stroke (Adebamowo et al., 2015; Ascherio et al., 1998; Geleijnse et al., 2007; Larsson et al., 2008, 2011a; Sluijs et al., 2014). Some of the studies found a statistically significant relationship, notably in adults not using diuretics (Green et al., 2002) and normotensive postmenopausal women (Seth et al., 2014). All studies were rated as having a moderate or high risk of bias. The AHRQ Systematic Review characterized the statistical significance of the associations between potassium intake and stroke as mixed among studies that used dietary intake assessment methodologies.
The relationship between potassium intake and stroke was also assessed among population groups characterized by a chronic disease or condition. In an analysis based on the first National Health and Nutrition Examination Survey Epidemiological Follow-Up Study data, relative risk of stroke mortality was reported to be higher among hypertensive males with lower potassium intake, but such a relationship was not found among hypertensive females (Fang et al., 2000). Based on an analysis of data from the Swedish Mammography Cohort, relative risk of stroke tended to be lower among women with a history of hypertension with higher potassium intakes, although not all comparisons to the first quintile of intake reached statistical significance (Larsson et al., 2011a). Among postmenopausal women with hypertension participating in the WHI Observational Study, there were no statistically significant risk reductions in all comparisons to the first quartile of intake (< 1,925 mg/d [< 49 mmol/d]) (Seth et al., 2014). Statistically significant lower hazards of stroke were found among adults with established cardiovascular disease or high-risk diabetes with higher potassium excretion, as compared to those with the lowest potassium excretion (< 1,500 mg/d [< 38 mmol/d]) (O’Donnell et al., 2011). In an analysis of adults with mild to moderate chronic kidney disease, cumulative mean potassium excretion from three 24-hour urinary measurements was not associated with stroke risk (Mills et al., 2016). All studies were rated as having a moderate or high risk of bias.
The AHRQ Systematic Review concluded that there was insufficient evidence to identify associations of potassium intake with stroke. Evidence on the moderating effect of chronic diseases or conditions was also characterized as insufficient.
Committee’s synthesis of the evidence The lack of randomized controlled trials in which potassium intake is the only component of the diet modulated limits the committee’s ability to determine if potassium intake has an independent effect on stroke.
The association between potassium intake and risk of stroke did not reach statistical significance in many of the observational studies included in the AHRQ Systematic Review. Since the release of the AHRQ Systematic Review, an additional study meeting the inclusion criteria has been published suggesting that there was a nonstatistically significant inverse relationship between calibrated potassium intake and total stroke (HR for 20 percent increase in potassium intake = 0.88 [95% CI: 0.78, 1.01]) (Prentice et al., 2017).
The conclusion of insufficient evidence reached in the AHRQ Systematic Review appears to differ from conclusions reached in several recent systematic evidence reviews and meta-analyses of prospective cohort studies on potassium intake and risk of stroke (Aburto et al., 2013; D’Elia et al., 2014; Larsson et al., 2011b; Vinceti et al., 2016). The AHRQ Systematic Review considered these reviews by identifying individual studies within each that met its inclusion criteria (i.e., used them for reference mining). As such, the origin of the apparent different conclusions is not that the AHRQ Systematic Review considered a different collection of literature, but that it had different inclusion criteria and approach.5 Unlike the other systematic reviews, the AHRQ Systematic Review did not conduct meta-analyses using the prospective cohort data; pooled estimates are, therefore, not available for comparison. A brief summary of methodologies and findings from other syntheses of the observational evidence on the relationship between potassium intake and risk of stroke is provided below:
- Larsson et al. (2011b) identified 10 prospective cohort studies, all of which collected either 24-hour dietary recalls or food frequency questionnaire data. No risk-of-bias assessment was described. The pooled relative risk for total stroke for 1,000 mg/d (26 mmol/d) increase in potassium was 0.89 ([95% CI: 0.83, 0.96], I2 = 51 percent). Removing one of the studies (Khaw and Barrett-Connor, 1987) reduced the heterogeneity to 21 percent. Although the methodology
___________________
5 For example, Umesawa et al. (2008) and Weng et al. (2008) were both listed as excluded from the AHRQ Systematic Review because “the intervention [was] not of interest.”
-
was not provided, Adebamowo et al. (2015) reported updating this meta-analysis with new estimates from analyses of Nurses’ Health Study I and II data and a study by Sluijs et al. (2014). The pooled relative risk for total stroke for 1,000 mg/d increase in potassium was 0.91 ([95% CI: 0.88, 0.94], I2 was not reported).
- Aburto et al. (2013) reported that, based on nine cohort studies, risk of incident stroke was reduced with higher intake of potassium (risk ratio [RR] = 0.76 [95% CI: 0.66, 0.89], I2 = 59 percent). Using the GRADE system, the strength of the evidence for a protective effect of higher potassium intake on incident stroke was graded as low.
- D’Elia et al. (2011) included nine studies that were assessed through an adapted quality scoring system from Downs and Black. Higher potassium intake (average weighted difference 1,640 mg/d [42 mmol/d]) had an inverse relationship with stroke (RR = 0.79 [95% CI: 0.68, 0.90], I2 = 55 percent). None of the factors assessed through meta-regression (quality score, length of follow-up, recruitment year, population potassium intake at baseline, between group difference in potassium intake) had a significant influence on the estimate. A 2014 update of this systematic review added three additional analyses, including one analysis in which the potassium exposure was based on a baseline spot urine sample (D’Elia et al., 2014). Methodological details of the process by which the systematic review was updated were not provided. For every 1,000 mg/d (26 mmol/d) increase in potassium intake, there was a 10 percent reduction in stroke risk (RR = 0.90 [95% CI: 0.84, 0.96], I2 = 47 percent).
- Vinceti et al. (2016) included 16 studies in their meta-analysis. The Newcastle-Ottawa assessment scale was used to assess the studies; any measure of urinary potassium excretion was considered higher quality. The authors multiplied baseline potassium exposure expressed as 24-hour urinary excretion by 1.3 to convert it to an estimate of dietary intake. The pooled risk ratio for stroke was estimated to be 0.87 ([95% CI: 0.80, 0.94], I2 = 46 percent).6 When stratified by type of potassium intake assessment methodology, the pooled risk ratio estimate of the four studies based on urinary excretion was higher and had wider confidence intervals than that of the pooled estimate based on 12 studies that assessed potassium exposure through dietary assessment methodologies. In a spline regression analysis, stroke risk reduced with increased intake to approximately 3,518 mg/d (90 mmol/d). The analyses suggested that the relationship between potassium intake and stroke may not
___________________
6 Estimate is for the most adjusted model. Additional analyses also explore the implications of using estimates not adjusted for blood pressure or hypertension status.
be linear. Only two studies in the analysis, however, had estimates of potassium intakes of 4,691 mg/d (120 mmol/d) or greater.
Larsson et al. (2011b) and Vinceti et al. (2016) both explored whether the relationship between potassium intake and stroke varied by stroke type. Each produced pooled estimates from the subset of studies that provided such data. Both analyses suggested a significant inverse relationship with ischemic stroke. The relationship between potassium intake and hemorrhagic stroke was not statistically significant in either report, except in an analysis in which Vinceti et al. (2016) did not control for blood pressure or hypertension status.
There is some observational evidence to suggest that potassium intake may have an inverse relationship with risk of stroke and, based on the summaries above, limited evidence to suggest that the relationship may be more relevant to ischemic stroke, as opposed to hemorrhagic stroke (Larsson et al., 2011b; Vinceti et al., 2016). However, recent systematic reviews that have assessed the strength of evidence have graded the evidence as either insufficient (Newberry et al., 2018) or low (Aburto et al., 2013). The Guiding Principles Report recommended strength of evidence for a causal relationship should be at least moderate to be used to establish a DRI based on chronic disease. Given that the evidence on the relationship is entirely derived from analyses of observational data, and therefore limits the committee’s ability to determine the independent effect of potassium, the strength of evidence on the causal relationship between potassium intake and stroke does not qualify for a moderate rating. The committee is in agreement with the AHRQ Systematic Review assessment that there is insufficient evidence on the association between potassium intake and stroke.
Blood Pressure
Evidence presented in the 2005 DRI Report The 2005 DRI Report reviewed observational studies, interventional trials, and a meta-analysis to assess the relationship between potassium intake and blood pressure. Integral to the use of the blood pressure evidence in the 2005 DRI Report were considerations regarding interpretation, which are outlined in Box 6-1.
Two findings on the relationship between potassium intake and blood pressure were described as part of the evidence base that informed the potassium AI for adults.7 First, one intake–response trial reported that potassium intake of 4,700 mg/d (120 mmol/d), of which 3,519 mg/d (90 mmol/d)
___________________
7 The potassium AI for adults 19–50 years of age served as the foundation for setting the potassium AI for children, adolescents, older adults, pregnant women, and lactating women.
was administered as potassium bicarbonate capsules, markedly reduced the prevalence of salt sensitivity among normotensive African American men (Morris et al., 1999).8 Second, several clinical trials reported total potassium intake of approximately 3,100–4,700 mg/d (80–120 mmol/d) reduced blood pressure among normotensive adults; most studies included a potassium supplement. This evidence, together with evidence on the relationship between potassium intake and kidney stones, was used in the 2005 DRI Report to establish the potassium Adequate Intake (AI) for adults at 4,700 mg/d (120 mmol/d).
___________________
8Morris et al. (1999) was not included in the AHRQ Systematic Review. There were no key questions about salt-sensitive blood pressure changes. Furthermore, the provision of potassium was only 3 weeks in length, which is shorter than the inclusion criteria for the AHRQ Systematic Review.
Evidence provided in the AHRQ Systematic Review The AHRQ Systematic Review included two key questions that sought to assess the relationship between potassium intake and blood pressure (see Chapter 1, Box 1-3). One of the key questions focused on the effect of potassium interventions on blood pressure (i.e., randomized controlled trials). Corresponding evidence included interventions in which participants received advice and coaching to increase dietary potassium intake and trials that used potassium supplements to increase potassium intake. The other key question assessed the evidence of an association between potassium intake and blood pressure (i.e., observational studies).
As the intent of this review of evidence is to evaluate the causality between potassium intake and a chronic disease indicator, the summary below focuses on the trial data. However, it is noted that the AHRQ Systematic Review concluded that there was low strength of evidence to suggest that higher potassium intake is inconsistently associated with lower adjusted blood pressure in adults, based on 10 analyses of observational data. There was no evidence to indicate that higher potassium intake is associated with a decrease in hypertension incidence. There was insufficient evidence to draw conclusions about the modifying effect of sex, age, race, ethnicity, hypertension status, or obesity status.
Adults The AHRQ Systematic Review identified three parallel randomized controlled trials (Miller et al., 2016; Nowson and Morgan, 1988; Siani et al., 1991) and one crossover trial (Berry et al., 2010) that examined the effect of increasing potassium intake from foods alone on blood pressure. All were conducted in adult participants with mild or well-controlled hypertension. Nowson and Morgan (1988) reported a significant effect of dietary potassium intake on blood pressure. Siani et al. (1991) found that, although there was no difference in blood pressure between groups at the end of the study, the dietary potassium intervention group had greater reductions in antihypertensive drug therapy, as compared to the control group (p < .001). The other two studies reported no statistically significant effect (Berry et al., 2010; Miller et al., 2016). The studies had various risk-of-bias ratings (low, moderate, high, and unclear). Grading the strength of the evidence as low, the AHRQ Systematic Review concluded that there was no evidence to suggest increasing dietary potassium through food alone affects blood pressure.
The AHRQ Systematic Review identified 10 parallel randomized controlled trials and 8 crossover trials that examined the effect of potassium supplements, as compared to placebo. A random-effects meta-analysis across the 18 trials resulted in a mean difference in systolic blood pressure of –6.43 mm Hg ([95% CI: –11.06, –1.80], I2 = 94 percent). The high heterogeneity was noted. Omitting studies with high or unclear risk of bias
did not substantially change the pooled estimate. For diastolic blood pressure, the pooled estimate across the 18 trials resulted in a mean difference of −3.50 mm Hg ([95% CI: –6.10, –0.89], I2 = 93 percent). The analyses were also stratified by hypertension status. The pooled effect estimates for normotensive adults suggested a possible beneficial effect on systolic and diastolic blood pressure, but it was no longer statistically significant. Pooled estimates among adults with prehypertension and hypertension were similar to those in the overall meta-analysis.
The AHRQ Systematic Review concluded that there was moderate strength of evidence that increased potassium intake from dietary supplements reduces blood pressure in adults with prehypertension and hypertension, and that there was low strength of evidence that potassium supplementation does not decrease blood pressure among normotensive adults. The AHRQ Systematic Review also determined that there was insufficient evidence to draw any conclusions about whether sex, race, or ethnicity modifies the effect of potassium supplementation on blood pressure among adults.
Children and adolescents One parallel randomized controlled trial and one controlled trial assessing the effect of potassium supplementation on blood pressure in children and adolescents met the AHRQ Systematic Review inclusion criteria. In the randomized controlled trial, 210 adolescents (mean: 13 years of age at baseline) in the top 15th percentile for blood pressure were randomized to a low-sodium diet, potassium chloride supplementation, or placebo control for 3 years (Sinaiko et al., 1993). The potassium supplement was scaled to body weight (39 mg/kg bodyweight/d [1 mmol/kg bodyweight/d], with a maximum of 3,128 mg/d [80 mmol/d]). Girls in the potassium supplement group had a significantly lower increase in systolic blood pressure, whereas the boys in the potassium supplement group did not have the same effect. The change in systolic and diastolic blood pressure at the end of the trial was not significantly different between the placebo and the potassium supplementation groups. The slope of change in blood pressure was significantly different between boys and girls in the potassium supplementation group. The other trial assessed 38 sets of homozygous twins (mean: 11.6 ± 3.8 years of age at baseline), during which one twin received potassium supplementation and the other twin received a placebo for a period of 4 weeks (Miller et al., 1987). There was no significant difference in blood pressure in paired comparisons. Based on this evidence, the AHRQ Systematic Review concluded that there was insufficient evidence to draw any conclusions about the effects of potassium supplementation on blood pressure in children and adolescents.
Committee’s synthesis of the evidence The committee identified the lack of exploration of potential sources of heterogeneity as a key limitation of
the AHRQ Systematic Review report (for an explanation regarding heterogeneity, see Chapter 2, and for the committee’s assessment of the AHRQ Systematic Review, see Appendix C). Given the extensive variation seen among the studies, the committee further explored heterogeneity in the trials of potassium supplementation and blood pressure. Two members of the committee reviewed the primary publications of the trials included in the AHRQ Systematic Review; relatively small transcription errors were corrected. Trials mentioned in the text of the AHRQ Systematic Review but not included in meta-analysis were also identified. A description of changes made are listed in Box 6-2.
The committee’s analysis includes 16 trials of potassium supplements only. As described above, there were four trials of dietary intervention to increase potassium intake. The dietary trials, however, are excluded from this analysis owing to concerns about collinearity between potassium and other nutrients. Most of the potassium supplementation trials used potassium chloride. Some included potassium citrate or potassium bicarbonate, but potassium chloride was used primarily in the AHRQ Systematic Review and used preferentially in the committee’s analysis. The analysis was a random-effects meta-analysis done using the metafor package in the software package R.9 The Knapp-Hartung variance estimate is reported for all summary effects. Because the results from Obel (1989) were an apparent outlier, all analyses were repeated without this trial.
Updated results for blood pressure Despite some changes in the studies and corrections to individual study effects, the overall results were similar to those reported in the AHRQ Systematic Review; increased potassium intake through potassium supplementation decreased blood pressure. The estimated net difference in systolic blood pressure was −6.87 mm Hg [95% CI: −12.12, −1.61] (see Figure 6-1), and in diastolic blood pressure it was −3.57 mm Hg [95% CI: −6.52, −0.63] (see Figure 6-2). There was still much heterogeneity with overall I2 values of 94 to 97 percent, with more heterogeneity in the parallel trials than the crossover trials (98 versus 71 percent for systolic blood pressure and 96 versus 66 percent for diastolic blood pressure, respectively). Restricting the included studies to those that used potassium chloride supplements made little difference. When the Obel (1989) trial was eliminated, there was only a small reduction in heterogeneity, though the estimated effects were smaller, with net differences of –4.42 mm Hg ([95% CI: −6.92, −1.91], I2 = 83 percent) for systolic blood pressure and −2.53 mm Hg ([95% CI: −4.73, −0.32], I2 = 86 percent) for diastolic blood pressure.
___________________
9 A collection of functions for conducting meta-analyses is in the statistical software package R.
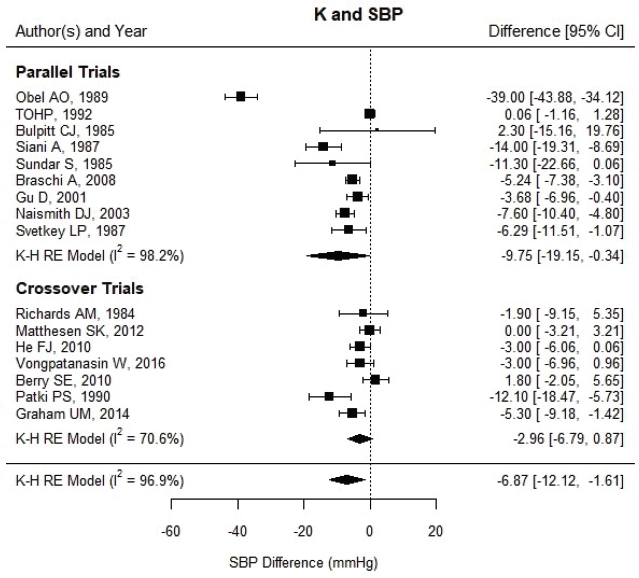
NOTES: Studies are listed by the last name of the first author and year of publication. CI = confidence interval; I2 = statistic that describes the percent of variation across studies due to heterogeneity; K = potassium; K-H = Knapp-Hartung variance estimate; RE = random-effects; SBP = systolic blood pressure; TOHP = Trials of Hypertension Prevention.
There were no differences in effect by achieved net differences in potassium excretion (see Figure 6-3), including after eliminating the Obel (1989) outlier, indicating a lack of an intake–response relationship. There were also no differences by sodium excretion, duration of trial, year, or sample size, including after eliminating the Obel (1989) outlier. There was a suggested difference in effect on net systolic blood pressure difference by baseline systolic blood pressure (slope = –0.245 per mm Hg, p = .046) (see Figure 6-4), but this was attenuated after eliminating Obel (1989) (slope = –0.085 per mm Hg, p = .26). The I2 values remained high at 95 percent (82 percent without Obel, 1989). Effects were stronger among studies including any hypertensive participants with a net systolic difference of −8.16 mm Hg
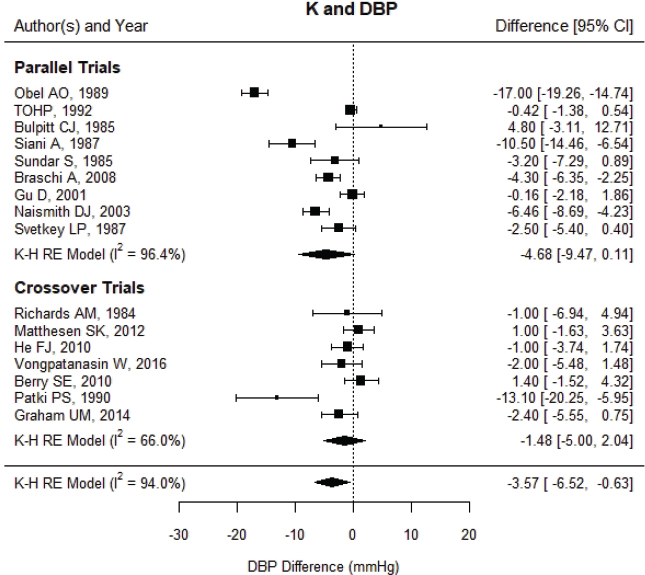
NOTES: Studies are listed by the last name of the first author and year of publication. CI = confidence interval; DBP = diastolic blood pressure; I2 = statistic that describes the percent of variation across studies due to heterogeneity; K = potassium; K-H = Knapp-Hartung variance estimate; RE = random-effects; TOHP = Trials of Hypertension Prevention.
[95% CI: −14.58, −1.74] (see Figure 6-5). In the three trials that did not include participants with hypertension, the net difference was not statistically significant. The lack of an intake–response relationship with net change in potassium excretion was observed in both those with and without hypertension at baseline. Similar results with respect to eliminating the outlier and separating studies by hypertension status were seen for diastolic blood pressure (see Figure 6-6).
Committee’s interpretation Overall there was a significant reduction in both systolic and diastolic blood pressure with potassium supplementation, with an average difference of −6.87/−3.57 mm Hg (or −4.42/−2.53 mm Hg,
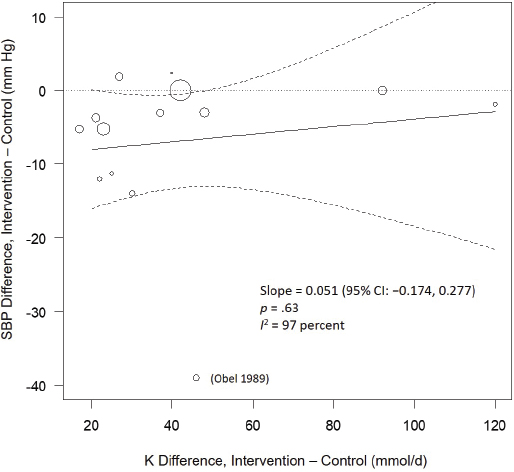
NOTE: CI = confidence interval; I2 = statistic that describes the percent of variation across studies due to heterogeneity; K = potassium; SBP = systolic blood pressure.
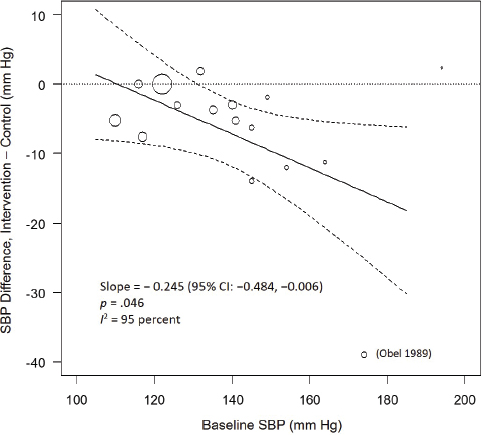
NOTE: CI = confidence interval; I2 = statistic that describes the percent of variation across studies due to heterogeneity; SBP = systolic blood pressure.
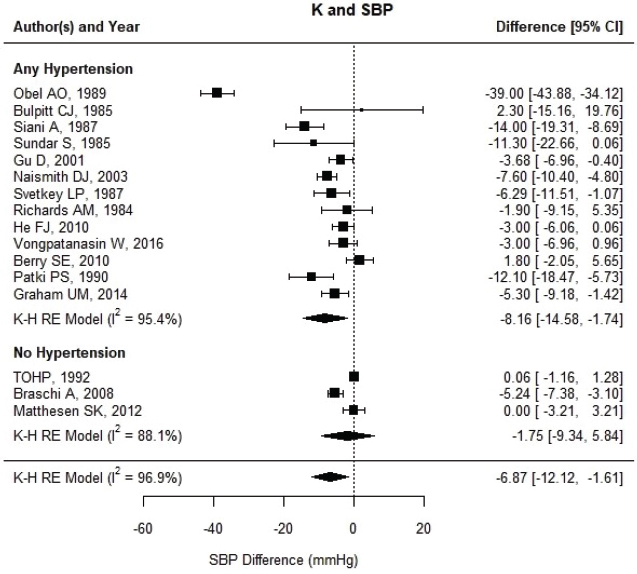
NOTES: Studies are listed by the last name of the first author and year of publication. CI = confidence interval; I2 = statistic that describes the percent of variation across studies due to heterogeneity; K = potassium; K-H = Knapp-Hartung variance estimate; RE = random-effects; SBP = systolic blood pressure; TOHP = Trials of Hypertension Prevention.
after excluding Obel, 1989), respectively. The effect was somewhat stronger in parallel than crossover trials, and stronger among those with hypertension. There was a large amount of heterogeneity, however, with overall I2 values of 94 to 97 percent. The heterogeneity was affected by one large outlier, but remained after excluding this trial. This variability could not be resolved by controlling for the other factors examined, including by intake–response relationship (net change in potassium level). These meta-analyses, however, are limited by their ecologic nature10 and the lack of individual participant data.
___________________
10 Meaning the unit of analysis is not individual-level data.
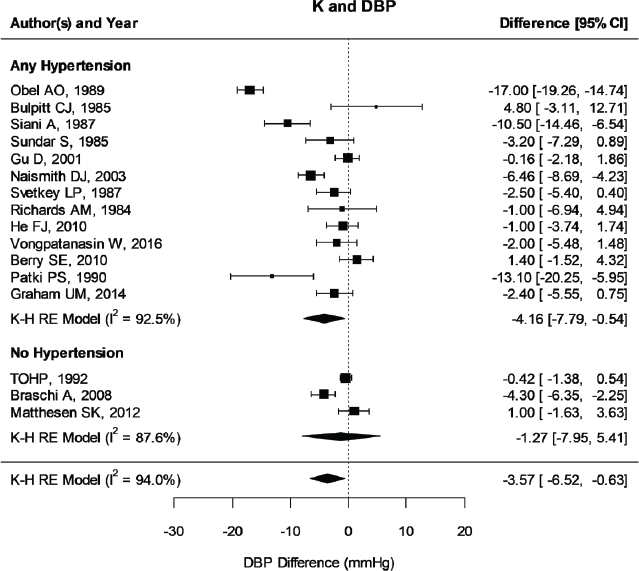
NOTES: Studies are listed by the last name of the first author and year of publication. CI = confidence interval; DBP = diastolic blood pressure; I2 = statistic that describes the percent of variation across studies due to heterogeneity; K = potassium; K-H = Knapp-Hartung variance estimate; RE = random-effects; TOHP = Trials of Hypertension Prevention.
The committee’s refinement of the AHRQ Systematic Review was not able to identify an explanation for the observed heterogeneity, and therefore the committee reaffirmed the AHRQ Systematic Review rating of the strength of evidence between increased potassium intake (achieved by potassium supplementation) and decreased blood pressure as moderate. This rating is based on a downgrade for unexplained inconsistency. Importantly, the committee’s reanalysis could not discern an intake–response gradient where greater intervention was correlated with greater effect, and meta-regression suggested a nonsignificant inverse relationship (see Figure 6-3). Additionally, the observed effects of increased potassium intakes through potassium supplementation on blood pressure appeared to be
primarily limited to adults with hypertension with no significant effects in normotensive adults and adults with prehypertension.
The Guiding Principles Report recommended that surrogate markers could be used as supporting evidence for establishing the DRI based on chronic disease, but that the surrogate marker should meet the qualification criteria for their purpose and be specific to each nutrient (NASEM, 2017, p. 8). Pursuant to this guidance, the committee considered whether blood pressure could serve as a surrogate marker for the relationship between potassium intake and chronic disease endpoints. Qualification of blood pressure as a surrogate marker implies that studies measuring blood pressure as an outcome of increasing potassium intake can be used in support of establishing a CDRR. There is a lack of clear supporting benefit of potassium alone on cardiovascular and mortality outcomes. Without such evidence, the committee is unable to consider blood pressure as a qualified surrogate marker in the context of potassium interventions.
Given the lack of an intake–response relationship, and in accordance with guidance in the Guiding Principles Report on use of qualified surrogate markers in establishing DRIs based on chronic disease, the committee did not find the sufficient evidence to use blood pressure as an indicator to establish a potassium CDRR.
Kidney Stones
Evidence presented in the 2005 DRI Report The 2005 DRI Report presented findings from a double-blind, placebo-controlled trial evaluating the effects of 30–60 mmol/d potassium citrate on recurrent kidney stones in 57 patients, 27–64 years of age (Barcelo et al., 1993). Usual diet was consumed throughout the trial, and dietary potassium intake was not directly assessed, although urinary potassium was measured. Estimated potassium intake in the treatment group from intake of the supplement and dietary sources was estimated to be 3,600–4,700 mg/d (92–120 mmol/d). After 3 years, the rate of stone formation in the treatment group was significantly lower than in the control group (0.1 stone/patient-year versus 1.1 stones/patient-year; p < .001).
The 2005 DRI Report also cited three large studies with evidence of an association between potassium and kidney stones (Curhan et al., 1993, 1997; Hirvonen et al., 1999). A strong inverse relationship between potassium intake estimated from a food frequency questionnaire and risk of kidney stones was reported in analyses of observational data from the Health Professionals’ Follow-Up Study and the Nurses’ Health Study I (Curhan et al., 1993, 1997). A Finnish study of male smokers found that risk of kidney stones decreased between the first and second quartile of potassium intake, as assessed by food frequency questionnaire, but that higher intakes did not confer additional risk reduction (Hirvonen et al., 1999). The findings at
higher intakes in the Finnish study were noted as possibly being attributed to higher potassium intake than in the United States.
Evidence from the 3-year double-blind controlled trial of the effect of potassium citrate on kidney stone reoccurrence (Barcelo et al., 1993), coupled with the evidence on blood pressure, was used in the 2005 DRI Report to establish the potassium AI for adults at 4,700 mg/d (120 mmol/d).
Evidence provided in the AHRQ Systematic Review One trial assessing the effect of potassium intake on the risk of kidney stones was included in the AHRQ Systematic Review. The study was the same trial used to establish the potassium AI in the 2005 DRI Report, described above (Barcelo et al., 1993). No additional trials were identified. The AHRQ Systematic Review concluded that there was insufficient evidence to draw conclusions about the effect of higher potassium intake on the risk for kidney stones.
Two observational studies, which included analyses of four cohorts, met the inclusion criteria for the AHRQ Systematic Review. One of the studies was summarized in the 2005 DRI Report, described above (Hirvonen et al., 1999). The other study expands on the other work described in the 2005 DRI Report and assessed the association between dietary potassium intake and risk of incident kidney stones using three large cohort studies conducted in the United States—Health Professionals’ Follow-Up Study, Nurses’ Health Study I, and the Nurses’ Health Study II (Ferraro et al., 2016). A significant inverse relationship between potassium intake and kidney stones was observed in all three cohorts. Due to heterogeneity, the cohorts were not pooled. The findings did not appear to differ significantly by sex. The AHRQ Systematic Review rated both of the included studies as having a high risk of bias and concluded that there was low strength of evidence to suggest that higher potassium exposure is associated with lower risk for kidney stones. The AHRQ Systematic Review also concluded that there was insufficient evidence to determine the moderating effect of hypertension or obesity status on the relationship between potassium intake and kidney stones.
Committee’s synthesis of the evidence The available evidence on the relationship between potassium intake and kidney stone risk is similar to that which was reviewed in the 2005 DRI Report. No new trials meeting the AHRQ Systematic Review inclusion criteria have since been published. The observational studies cannot independently confirm that potassium per se is the dietary component associated with observed benefits. The committee is in agreement with the AHRQ Systematic Review that the evidence on the effect (i.e., from trials) of potassium intake and kidney stones is insufficient. The committee also agrees with the AHRQ Systematic Review that there
is low strength of evidence that higher potassium intake may be associated with lower risk of kidney stones.
Chronic Kidney Disease
Evidence presented in the 2005 DRI Report The 2005 DRI Report characterized patients with chronic kidney disease as a population in which the AI was not suitable owing to being predisposed to hyperkalemia, particularly those who use angiotensin-converting enzyme inhibitor therapy. Chronic kidney disease was not reviewed in the 2005 DRI Report as a potential indicator for establishing a potassium DRI value.
Evidence provided in the AHRQ Systematic Review No randomized controlled trials meeting the AHRQ Systematic Review inclusion criteria evaluated the independent effect of potassium intake on the risk of chronic kidney disease.
Two observational studies assessed the association between potassium intake and chronic kidney disease. An inverse association between urinary potassium excretion and chronic kidney disease was identified among participants in the Prevention of Renal and Vascular End-Stage Disease cohort (Kieneker et al., 2016a); for each standard deviation decrease in urinary potassium excretion (821 mg/d [21 mmol/d]), risk of developing chronic kidney disease increased by 16 percent.11 In another prospective cohort, the highest quintile of potassium intake (5,519 mg/d [141 mmol/d]), assessed by food frequency questionnaire at baseline, was associated with a reduced hazard of death attributable to renal cause and dialysis as compared to the lowest quintile of potassium intake (1,801 mg/d [46 mmol/d]) (Smyth et al., 2016). The AHRQ Systematic Review concluded that there was insufficient evidence to draw conclusions about the relationship between potassium intake and the risk for chronic kidney disease.
Committee’s synthesis of the evidence The committee agrees with the AHRQ Systematic Review that the evidence is insufficient on the relationship between potassium intake and chronic kidney disease; the committee also agrees with the 2005 DRI Report that patients with chronic kidney disease are not an appropriate population for establishing a DRI value, which are meant for the apparently healthy population. Due to the risk of hyperkalemia, patients with chronic kidney disease are further discussed as a special consideration in Chapter 7.
___________________
11 Model adjusted for age; sex; height; weight; smoking status; alcohol consumption; parental history of chronic kidney disease; race; diabetes; baseline estimated glomerular filtration rate; and urinary sodium, calcium, urea, albumin, and creatinine excretion.
Osteoporosis and Related Indicators
One of the considerations previously factored into characterizing potassium intake needs centers around the concept of acid–base balance. Potassium-rich foods, such as fruits and vegetables, provide bicarbonate precursors, which are thought to play a role in neutralizing diet-induced acidosis. Diets that are higher in foods that produce noncarbonic acids (e.g., animal protein, cereal grains) and lower in foods that provide bicarbonate precursors, consumed over a long period of time, are thought to have negative metabolic effects owing to the body’s attempt to counter the diet-induced acidosis. One such buffering mechanism is to dissolve the bone matrix. Given this biological plausibility, the committee reviewed the evidence presented in the 2005 DRI Report and evidence that has since emerged.
Evidence presented in the 2005 DRI Report The 2005 DRI Report included trials that explored the relationship between potassium intake and bone demineralization in consideration for establishing the potassium DRIs for adequacy. Sebastian et al. (1994) assessed the effect of potassium bicarbonate (60–120 mmol/d per 60 kg body weight) for a period of 18 days among 18 postmenopausal women. The study reported that concentrations of a marker of bone formation significantly increased and urinary marker of bone reabsorption significantly decreased during the supplementation period; urinary calcium excretion also decreased. Maurer et al. (2003) reported that, during 7 days of the bicarbonate salt supplementation, urinary markers of bone resorption decreased among nine healthy young adults; urinary calcium excretion also significantly decreased. Among 21 adult patients with recurrent kidney stones who were treated with potassium citrate for at least 11 months (range: 11–120 months), bone mineral density in L2 through L4 in the spine increased, but urinary calcium excretion did not change (Pak et al., 2002). Lemann et al. (1991) assessed the effect of 4 days of potassium chloride, potassium bicarbonate, sodium chloride, and sodium bicarbonate supplementation in healthy adults. Urinary calcium excretion decreased during potassium administrations, which was not seen during the sodium administrations.
The 2005 DRI Report also included observational studies that explored the relationship between potassium intake and bone demineralization. Five cross-sectional studies and one longitudinal study provided evidence that potassium intake and/or urinary potassium excretion was positively associated with bone mineral density. The observational evidence for the relationship between potassium intake and bone loss was not used as the primary data to establish the potassium AI in the 2005 DRI Report, but was described as being supporting evidence.
Evidence from the committee’s supplemental literature search Evidence suggests that potassium intake has a hypocalciuric effect (Frassetto et al., 2005; Lemann et al., 1989), which potentially has implications for bone integrity. Urinary calcium excretion, however, can be affected by a variety of factors other than changes to the bone. Although evidence of a relationship between potassium intake and urinary calcium may point to a biological interdependence, the committee is unable to attribute it to an effect on the risk of osteoporosis. Studies have also assessed the relationship between potassium intake and bone turnover markers (Dawson-Hughes, 2009, 2015; He et al., 2010; Marangella et al., 2004; Moseley et al., 2013). Although bone turnover markers have the potential to clarify the biological mechanism by which a relationship exists, the committee was concerned about the validation of such markers and using such evidence to inform the potassium CDRR. The relationship between risk of fracture and bone formation marker (serum procollagen type I N propeptide) and a bone resorption marker (serum C-terminal cross-linking telopeptide of type I collagen) has been characterized as modest (Johansson et al., 2014). To that end, the committee’s evidence review focused on outcomes related to osteoporosis (including osteoporotic fracture) and bone mineral density. Details of the committee’s supplemental literature search, including inclusion criteria and summary tables of findings, are presented in Appendix E.
Osteoporotic facture No randomized controlled trials meeting the inclusion criteria evaluated the independent effect of potassium intake on the risk of osteoporotic fracture. One case-cohort study was identified. There were no statistically significant differences for risk of total, hip, spine, or wrist fracture across the sex-specific quintiles of potassium intake or evidence of a trend in fracture risk across the sex-specific quintiles of potassium intake (Hayhoe et al., 2015). The study was rated as having a moderate risk of bias.
Bone mineral density Three randomized controlled trials meeting the inclusion criteria evaluated the effect of potassium intake on bone mineral density. A 2-year placebo-controlled trial among 203 postmenopausal women reported no statistically significant differences in lumbar spine or total hip bone mineral density among participants receiving potassium citrate in high or low dose (Macdonald et al., 2008). The study was rated as having a low risk of bias. In a separate 2-year randomized controlled trial among 169 adults 65 years of age and older, participants in the potassium citrate supplementation group experienced a net increase of areal bone mineral density and, as compared to the placebo group, had a significant net effect on measures of total volumetric bone mineral density in the dominant and nondominant radium and tibia (Jehle et al., 2013). The study was
rated as having a low risk of bias. In a 1-year trial of 83 postmenopausal women with osteopenia, randomized to receive either potassium citrate or placebo, no significant changes in lumbar spine, total hip, or femoral net bone mineral density were found in either group (Gregory et al., 2015). The study was rated as having a low risk of bias.
Three observational studies on the association between potassium intake and bone mineral density were identified. In a study of 266 postmenopausal women, those in the highest quartile of urinary potassium excretion had higher total hip bone mineral density and total bone mineral density at year 5, as compared to those in the lowest quartile of potassium excretion (Zhu et al., 2009). The study was rated as having a high risk of bias. In a study of 891 healthy pre-, peri-, and postmenopausal women, there were significant positive correlations between energy-adjusted intake of several dietary components (including potassium) and change in femoral neck bone mineral density, but only among pre- and perimenopausal women who had never taken hormone replacement therapy (Macdonald et al., 2004). The study was rated as having a moderate risk of bias. In a 2-year study of 125 female competitive distance runners (18–26 years of age), potassium intake and other dietary components were associated with increases in whole-body bone mineral density (Nieves et al., 2010); controlling for calcium intake attenuated the relationships with potassium but did not change its statistical significance. The study was rated as having a moderate risk of bias.
Committee’s synthesis of the evidence The committee’s supplemental literature search did not reveal any randomized controlled trials assessing the effect of potassium intake on osteoporotic fracture, and one prospective cohort study did not reveal a statistically significant relationship. Evidence on the relationship between potassium intake and the outcome of osteoporosis is therefore considered insufficient.
Evidence of the relationship between potassium intake and bone mineral density was mixed among randomized controlled trials. Trials differed from each other with respect to the populations assessed, co-administration of calcium and vitamin D, and doses of potassium citrate provided, which potentially contributed to the inconsistent results. Findings from a trial by Jehle et al. (2006) suggest that the potassium citrate may have a different effect on bone mineral density than potassium chloride, which makes it difficult to attribute observed effects to potassium per se. This is particularly important when considering diet as the source of potassium, as many potassium-rich foods are high in bicarbonate precursors. It is difficult to discern if the effect on bone mineral density is attributable to potassium intake or influences of foods rich in bicarbonate precursors or other dietary constituents. Studies have found positive associations between potassium intake and bone mineral density, although other dietary components also
share a positive or negative relationship, as well. Given inconsistencies and a limited ability to attribute an effect to potassium per se, the committee determined the evidence on the relationship between potassium intake and bone mineral density as insufficient.
Type 2 Diabetes, Glycemic Control, and Insulin Sensitivity
Evidence presented in the 2005 DRI Report The 2005 DRI Report did not review evidence on the relationship between potassium intake and type 2 diabetes, glycemic control, or insulin sensitivity.
Evidence provided in the AHRQ Systematic Review The AHRQ Systematic Review included individuals with type 2 diabetes as a subgroup of consideration throughout the key questions. There was insufficient evidence to determine if potassium intake has a differential effect on individuals with diabetes, with respect to the cardiovascular and renal indicators. The AHRQ Systematic Review did not review evidence on the relationship between potassium intake and type 2 diabetes, glycemic control, or insulin sensitivity.
Evidence from the committee’s supplemental literature search One randomized controlled trial on the effect of potassium supplementation on glucose control and tolerance was identified. A 12-week pilot study randomized 27 African American adults with prediabetes to receive either potassium chloride or placebo (Chatterjee et al., 2017). Fasting glucose levels were significantly improved for the potassium supplementation group as compared to the placebo group at the end of the study; statistically significant differences in glucose tolerance between the groups, however, were not identified at the end of the trial. The study was rated as having a low risk of bias.
Three prospective cohort studies that assessed the relationship between potassium intake and risk of type 2 diabetes were identified. One study, with 18 years of follow-up, did not find an association between baseline potassium excretion and risk of type 2 diabetes (Hu et al., 2005); the study was rated as having a high risk of bias. A separate study found participants in the lowest quintile of potassium excretion (238–1,380 mg/d [6–35 mmol/d]) had increased risk of incident diabetes (HR = 2.45 [95% CI: 1.08, 5.59]), as compared to the highest quintile of urinary potassium excretion (2,862–6,256 mg/d [73–160 mmol/d]) (Chatterjee et al., 2012). Dietary history data were also available on a subset of participants in this cohort; based on 20 years of follow-up, risk of incident diabetes was not significantly different across quintiles of dietary potassium intake, although there was evidence to suggest an inverse relationship existed among African American participants, but not white participants. Risk of bias for this
study was rated as moderate. Chatterjee et al. (2010) reported that, in models that adjusted for possible confounders, baseline potassium intake was not significantly associated with incident diabetes among 12,209 adults. This study was rated as having a high risk of bias.
Committee’s synthesis of the evidence The committee’s supplemental literature search identified one randomized controlled trial assessing the effect of potassium on a measure of glucose control. As a pilot study in a small group of participants for a relatively short period of time, the available trial data are insufficient for the committee to make a determination regarding whether potassium intake affects glucose control. Evidence on the relationship between potassium intake and incident diabetes risk was also explored. Findings across the observational studies are inconsistent. The evidence on the relationship between potassium intake and type 2 diabetes, glucose control, and insulin sensitivity is considered insufficient.
THE COMMITTEE’S CONCLUSION REGARDING CHRONIC DISEASE RISK REDUCTION INTAKES FOR POTASSIUM
The body of evidence for the relationship between potassium intake and chronic disease is limited. Many of the indicators reviewed by the committee had little to no data from randomized controlled trials, which prevented the committee from being able to establish a causal relationship with potassium. Diets rich in potassium are typically also rich in other micronutrients and dietary components that could contribute to an apparent effect attributed to potassium. For this reason, the committee gave greater emphasis to potassium supplementation data from clinical trials, even though potassium supplementation is not the source of usual potassium intake in the population.
The indicator with the most clinical trial data for potassium supplementation is blood pressure. Meta-analyses across these trials indicate that potassium intake has an overall beneficial effect on both systolic and diastolic blood pressure, particularly among adults with hypertension. However, the meta-analysis also showed a considerable amount of heterogeneity across trials. In its refinement of the analysis in the AHRQ Systematic Review, the committee explored multiple potential sources of heterogeneity, including the removal of an outlier study and consideration of an intake–response relationship, but none explained more than a small portion of the observed heterogeneity. Thus, the strength of evidence for potassium and blood pressure was rated as moderate owing to this unexplained inconsistency across studies.
Although a moderate strength of evidence would be sufficient to consider for supporting a CDRR, the committee did not use blood pressure
as an indicator for chronic disease risk for two key reasons. First, as per the guidance in the Guiding Principles Report, the ideal indicator for establishing a DRI based on chronic disease is a chronic disease endpoint; qualified surrogate markers are primarily intended to be used as supporting evidence. The strength of evidence to support a causal relationship between increased potassium intake and related chronic disease outcomes, such as cardiovascular disease outcomes or hypertension, was graded as low or insufficient. Without evidence on the relationship between increases in potassium intake and risk of chronic disease outcomes, blood pressure cannot be considered a qualified surrogate marker in the context of potassium interventions. Second, even if blood pressure could be used to establish a potassium CDRR, there is a lack of evidence of an intake–response relationship, as studies with greater contrasts in potassium intake between intervention and control groups did not tend to also have greater reductions in blood pressure. As described in the Guiding Principles Report, an intake–response relationship is one of the evidentiary components of establishing a DRI based on chronic disease. Therefore, because of the limitations of the body of evidence described above (lack of intake–response gradient, low or inadequate strength of evidence for related chronic disease outcomes), the committee judged that a potassium CDRR based solely on blood pressure evidence was not congruent with the guidance provided in the Guiding Principles Report.
The committee concludes that, although there is moderate strength of evidence for a causal relationship between potassium supplementation and reductions in blood pressure, heterogeneity across studies, lack of evidence for an intake–response relationship, and lack of supporting evidence for benefit of potassium on cardiovascular disease prevents the committee from establishing a potassium Chronic Disease Risk Reduction Intake (CDRR).
The committee notes that its determination regarding the potassium CDRR should not be interpreted as statement about a lack of an effect of potassium intake on chronic disease outcomes. Rather, the committee’s conclusion regarding the potassium CDRR likely reflects a lack of evidence. There is moderate strength of evidence on the relationship between potassium intake and blood pressure, based on potassium supplementation trials. There is a lack of evidence on the intake–response relationship between potassium intake and blood pressure and a lack of evidence regarding the relationship between potassium intake and chronic disease endpoints. Addressing these research gaps could provide a more definitive determination regarding the effect of potassium intake on chronic disease endpoints and thereby possibly inform the derivation of a potas-
sium CDRR in the future. The committee outlines such research gaps in Chapter 12.
REFERENCES
Aburto, N. J., S. Hanson, H. Gutierrez, L. Hooper, P. Elliott, and F. P. Cappuccio. 2013. Effect of increased potassium intake on cardiovascular risk factors and disease: Systematic review and meta-analyses. BMJ 346:f1378.
Adebamowo, S. N., D. Spiegelman, W. C. Willett, and K. M. Rexrode. 2015. Association between intakes of magnesium, potassium, and calcium and risk of stroke: 2 cohorts of US women and updated meta-analyses. American Journal of Clinical Nutrition 101(6):1269-1277.
Alderman, M., J. Sealey, H. Cohen, S. Madhavan, and J. Laragh. 1997. Urinary sodium excretion and myocardial infarction in hypertensive patients: A prospective cohort study. American Journal of Clinical Nutrition 65(2 Suppl):682s-686s.
Ascherio, A., E. B. Rimm, M. A. Hernan, E. L. Giovannucci, I. Kawachi, M. J. Stampfer, and W. C. Willett. 1998. Intake of potassium, magnesium, calcium, and fiber and risk of stroke among US men. Circulation 98(12):1198-1204.
Barcelo, P., O. Wuhl, E. Servitge, A. Rousaud, and C. Y. Pak. 1993. Randomized double-blind study of potassium citrate in idiopathic hypocitraturic calcium nephrolithiasis. Journal of Urology 150(6):1761-1764.
Bazzano, L. A., J. He, L. G. Ogden, C. Loria, S. Vupputuri, L. Myers, and P. K. Whelton. 2001. Dietary potassium intake and risk of stroke in US men and women: National Health and Nutrition Examination Survey I epidemiologic follow-up study. Stroke 32(7):1473-1480.
Becerra-Tomas, N., M. Guasch-Ferre, J. Quilez, J. Merino, R. Ferre, A. Diaz-Lopez, M. Bullo, P. Hernandez-Alonso, A. Palau-Galindo, and J. Salas-Salvado. 2015. Effect of functional bread rich in potassium, gamma-aminobutyric acid and angiotensin-converting enzyme inhibitors on blood pressure, glucose metabolism and endothelial function: A double-blind randomized crossover clinical trial. Medicine (Baltimore) 94(46):e1807.
Berry, S. E., U. Z. Mulla, P. J. Chowienczyk, and T. A. Sanders. 2010. Increased potassium intake from fruit and vegetables or supplements does not lower blood pressure or improve vascular function in UK men and women with early hypertension: A randomised controlled trial. British Journal of Nutrition 104(12):1839-1847.
BMJ. 1998. Comparison of the prediction by 27 different factors of coronary heart disease and death in men and women of the Scottish Heart Health Study: Cohort study. BMJ 316(7148):1881.
Braschi, A., and D. J. Naismith. 2008. The effect of a dietary supplement of potassium chloride or potassium citrate on blood pressure in predominantly normotensive volunteers. British Journal of Nutrition 99(6):1284-1292.
Bulpitt, C. J., G. Ferrier, P. J. Lewis, M. Daymond, P. F. Bulpitt, and C. T. Dollery. 1985. Potassium supplementation fails to lower blood pressure in hypertensive patients receiving a potassium losing diuretic. Annals of Clinical Research 17(4):126-130.
Chang, H. Y., Y. W. Hu, C. S. Yue, Y. W. Wen, W. T. Yeh, L. S. Hsu, S. Y. Tsai, and W. H. Pan. 2006. Effect of potassium-enriched salt on cardiovascular mortality and medical expenses of elderly men. American Journal of Clinical Nutrition 83(6):1289-1296.
Chatterjee, R., H. C. Yeh, T. Shafi, E. Selvin, C. Anderson, J. S. Pankow, E. Miller, and F. Brancati. 2010. Serum and dietary potassium and risk of incident type 2 diabetes mellitus: The Atherosclerosis Risk in Communities (ARIC) study. Archives of Internal Medicine 170(19):1745-1751.
Chatterjee, R., L. A. Colangelo, H. C. Yeh, C. A. Anderson, M. L. Daviglus, K. Liu, and F. L. Brancati. 2012. Potassium intake and risk of incident type 2 diabetes mellitus: The Coronary Artery Risk Development in Young Adults (CARDIA) study. Diabetologia 55(5):1295-1303.
Chatterjee, R., C. Slentz, C. A. Davenport, J. Johnson, P. H. Lin, M. Muehlbauer, D. D’Alessio, L. P. Svetkey, and D. Edelman. 2017. Effects of potassium supplements on glucose metabolism in African Americans with prediabetes: A pilot trial. American Journal of Clinical Nutrition 106(6):1431-1438.
Cook, N. R., E. Obarzanek, J. A. Cutler, J. E. Buring, K. M. Rexrode, S. K. Kumanyika, L. J. Appel, and P. K. Whelton. 2009. Joint effects of sodium and potassium intake on subsequent cardiovascular disease: The Trials of Hypertension Prevention follow-up study. Archives of Internal Medicine 169(1):32-40.
Curhan, G. C., W. C. Willett, E. B. Rimm, and M. J. Stampfer. 1993. A prospective study of dietary calcium and other nutrients and the risk of symptomatic kidney stones. New England Journal of Medicine 328(12):833-838.
Curhan, G. C., W. C. Willett, F. E. Speizer, D. Spiegelman, and M. J. Stampfer. 1997. Comparison of dietary calcium with supplemental calcium and other nutrients as factors affecting the risk for kidney stones in women. Annals of Internal Medicine 126(7):497-504.
Dawson-Hughes, B., S. S. Harris, N. J. Palermo, C. Castaneda-Sceppa, H. M. Rasmussen, and G. E. Dallal. 2009. Treatment with potassium bicarbonate lowers calcium excretion and bone resorption in older men and women. Journal of Clinical Endocrinology and Metabolism 94(1):96-102.
Dawson-Hughes, B., S. S. Harris, N. J. Palermo, C. H. Gilhooly, M. K. Shea, R. A. Fielding, and L. Ceglia. 2015. Potassium bicarbonate supplementation lowers bone turnover and calcium excretion in older men and women: A randomized dose-finding trial. Journal of Bone and Mineral Research 30(11):2103-2111.
D’Elia, L., G. Barba, F. P. Cappuccio, and P. Strazzullo. 2011. Potassium intake, stroke, and cardiovascular disease: A meta-analysis of prospective studies. Journal of the American College of Cardiology 57(10):1210-1219.
D’Elia, L., C. Iannotta, P. Sabino, and R. Ippolito. 2014. Potassium-rich diet and risk of stroke: Updated meta-analysis. Nutrition, Metabolism, and Cardiovascular Diseases 24(6):585-587.
Dunkler, D., M. Kohl, K. K. Teo, G. Heinze, M. Dehghan, C. M. Clase, P. Gao, S. Yusuf, J. F. Mann, and R. Oberbauer. 2015. Dietary risk factors for incidence or progression of chronic kidney disease in individuals with type 2 diabetes in the European Union. Nephrology, Dialysis, Transplantation 30(Suppl 4):iv76-iv85.
Fang, J., S. Madhavan, and M. H. Alderman. 2000. Dietary potassium intake and stroke mortality. Stroke 31(7):1532-1537.
Ferraro, P. M., E. I. Mandel, G. C. Curhan, G. Gambaro, and E. N. Taylor. 2016. Dietary protein and potassium, diet-dependent net acid load, and risk of incident kidney stones. Clinical Journal of the American Society of Nephrology 11(10):1834-1844.
Frassetto, L., R. C. Morris, Jr., and A. Sebastian. 2005. Long-term persistence of the urine calcium-lowering effect of potassium bicarbonate in postmenopausal women. Journal of Clinical Endocrinology and Metabolism 90(2):831-834.
Geleijnse, J. M., J. C. M. Witteman, T. Stijnen, M. W. Kloos, A. Hofman, and D. E. Grobbee. 2007. Sodium and potassium intake and risk of cardiovascular events and all-cause mortality: The Rotterdam Study. European Journal of Epidemiology 22(11):763-770.
Graham, U. M., D. R. McCance, I. S. Young, and K. R. Mullan. 2014. A randomised controlled trial evaluating the effect of potassium supplementation on vascular function and the renin-angiotensin-aldosterone system. Journal of Human Hypertension 28(5):333-339.
Green, D. M., A. H. Ropper, R. A. Kronmal, B. M. Psaty, and G. L. Burke. 2002. Serum potassium level and dietary potassium intake as risk factors for stroke. Neurology 59(3):314-320.
Gregory, N. S., R. Kumar, E. M. Stein, E. Alexander, P. Christos, R. S. Bockman, and J. S. Rodman. 2015. Potassium citrate decreases bone resorption in postmenopausal women with osteopenia: A randomized, double-blind clinical trial. Endocrine Practice 21(12):1380-1386.
Gu, D., J. He, X. Wu, X. Duan, and P. K. Whelton. 2001. Effect of potassium supplementation on blood pressure in Chinese: A randomized, placebo-controlled trial. Journal of Hypertension 19(7):1325-1331.
Guyatt, G., A. D. Oxman, E. A. Akl, R. Kunz, G. Vist, J. Brozek, S. Norris, Y. Falck-Ytter, P. Glasziou, H. DeBeer, R. Jaeschke, D. Rind, J. Meerpohl, P. Dahm, and H. J. Schunemann. 2011. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. Journal of Clinical Epidemiology 64(4):383-394.
Hayhoe, R. P., M. A. Lentjes, R. N. Luben, K. T. Khaw, and A. A. Welch. 2015. Dietary magnesium and potassium intakes and circulating magnesium are associated with heel bone ultrasound attenuation and osteoporotic fracture risk in the EPIC-Norfolk cohort study. American Journal of Clinical Nutrition 102(2):376-384.
He, F. J., M. Marciniak, C. Carney, N. D. Markandu, V. Anand, W. D. Fraser, R. N. Dalton, J. C. Kaski, and G. A. MacGregor. 2010. Effects of potassium chloride and potassium bicarbonate on endothelial function, cardiovascular risk factors, and bone turnover in mild hypertensives. Hypertension 55(3):681-688.
He, J., K. T. Mills, L. J. Appel, W. Yang, J. Chen, B. T. Lee, S. E. Rosas, A. Porter, G. Makos, M. R. Weir, L. L. Hamm, and J. W. Kusek. 2016. Urinary sodium and potassium excretion and CKD progression. Journal of the American Society of Nephrology 27(4):1202-1212.
Hirvonen, T., P. Pietinen, M. Virtanen, D. Albanes, and J. Virtamo. 1999. Nutrient intake and use of beverages and the risk of kidney stones among male smokers. American Journal of Epidemiology 150(2):187-194.
Hu, G., P. Jousilahti, M. Peltonen, J. Lindstrom, and J. Tuomilehto. 2005. Urinary sodium and potassium excretion and the risk of type 2 diabetes: A prospective study in Finland. Diabetologia 48(8):1477-1483.
IOM (Institute of Medicine). 2005. Dietary Reference Intakes for water, potassium, sodium, chloride, and sulfate. Washington, DC: The National Academies Press.
Iso, H., M. J. Stampfer, J. E. Manson, K. Rexrode, C. H. Hennekens, G. A. Colditz, F. E. Speizer, and W. C. Willett. 1999. Prospective study of calcium, potassium, and magnesium intake and risk of stroke in women. Stroke 30(9):1772-1779.
Jehle, S., A. Zanetti, J. Muser, H. N. Hulter, and R. Krapf. 2006. Partial neutralization of the acidogenic Western diet with potassium citrate increases bone mass in postmenopausal women with osteopenia. Journal of the American Society of Nephrology 17(11):3213-3222.
Jehle, S., H. N. Hulter, and R. Krapf. 2013. Effect of potassium citrate on bone density, micro-architecture, and fracture risk in healthy older adults without osteoporosis: A randomized controlled trial. Journal of Clinical Endocrinology and Metabolism 98(1):207-217.
Johansson, H., A. Oden, J. A. Kanis, E. V. McCloskey, H. A. Morris, C. Cooper, and S. Vasikaran. 2014. A meta-analysis of reference markers of bone turnover for prediction of fracture. Calcified Tissue International 94(5):560-567.
Khaw, K. T., and E. Barrett-Connor. 1987. Dietary potassium and stroke-associated mortality. A 12-year prospective population study. New England Journal of Medicine 316(5):235-240.
Kieneker, L. M., S. J. Bakker, R. A. de Boer, G. J. Navis, R. T. Gansevoort, and M. M. Joosten. 2016a. Low potassium excretion but not high sodium excretion is associated with increased risk of developing chronic kidney disease. Kidney International 90(4):888-896.
Kieneker, L. M., R. T. Gansevoort, R. A. de Boer, F. P. Brouwers, E. J. Feskens, J. M. Geleijnse, G. Navis, S. J. Bakker, and M. M. Joosten. 2016b. Urinary potassium excretion and risk of cardiovascular events. American Journal of Clinical Nutrition 103(5):1204-1212.
Larsson, S. C., M. J. Virtanen, M. Mars, S. Mannisto, P. Pietinen, D. Albanes, and J. Virtamo. 2008. Magnesium, calcium, potassium, and sodium intakes and risk of stroke in male smokers. Archives of Internal Medicine 168(5):459-465.
Larsson, S. C., J. Virtamo, and A. Wolk. 2011a. Potassium, calcium, and magnesium intakes and risk of stroke in women. American Journal of Epidemiology 174(1):35-43.
Larsson, S. C., N. Orsini, and A. Wolk. 2011b. Dietary potassium intake and risk of stroke: A dose-response meta-analysis of prospective studies. Stroke 42(10):2746-2750.
Lee, C. N., D. M. Reed, C. J. MacLean, K. Yano, and D. Chiu. 1988. Dietary potassium and stroke. New England Journal of Medicine 318(15):995-996.
Lemann, Jr., J., R. W. Gray, and J. A. Pleuss. 1989. Potassium bicarbonate, but not sodium bicarbonate, reduces urinary calcium excretion and improves calcium balance in healthy men. Kidney International 35(2):688-695.
Lemann, Jr., J., J. A. Pleuss, R. W. Gray, and R. G. Hoffmann. 1991. Potassium administration reduces and potassium deprivation increases urinary calcium excretion in healthy adults [corrected]. Kidney International 39(5):973-983.
Leonberg-Yoo, A. K., H. Tighiouart, A. S. Levey, G. J. Beck, and M. J. Sarnak. 2017. Urine potassium excretion, kidney failure, and mortality in CKD. American Journal of Kidney Diseases 69(3):341-349.
Macdonald, H. M., S. A. New, M. H. Golden, M. K. Campbell, and D. M. Reid. 2004. Nutritional associations with bone loss during the menopausal transition: Evidence of a beneficial effect of calcium, alcohol, and fruit and vegetable nutrients and of a detrimental effect of fatty acids. American Journal of Clinical Nutrition 79(1):155-165.
Macdonald, H. M., A. J. Black, L. Aucott, G. Duthie, S. Duthie, R. Sandison, A. C. Hardcastle, S. A. Lanham New, W. D. Fraser, and D. M. Reid. 2008. Effect of potassium citrate supplementation or increased fruit and vegetable intake on bone metabolism in healthy postmenopausal women: A randomized controlled trial. American Journal of Clinical Nutrition 88(2):465-474.
Marangella, M., M. Di Stefano, S. Casalis, S. Berutti, P. D’Amelio, and G. C. Isaia. 2004. Effects of potassium citrate supplementation on bone metabolism. Calcified Tissue International 74(4):330-335.
Matthesen, S. K., T. Larsen, H. Vase, T. G. Lauridsen, and E. B. Pedersen. 2012. Effect of potassium supplementation on renal tubular function, ambulatory blood pressure and pulse wave velocity in healthy humans. Scandinavian Journal of Clinical and Laboratory Investigation 72(1):78-86.
Maurer, M., W. Riesen, J. Muser, H. N. Hulter, and R. Krapf. 2003. Neutralization of Western diet inhibits bone resorption independently of K intake and reduces cortisol secretion in humans. American Journal of Physiology: Renal Physiology 284(1):F32-F40.
Miller, E. R., 3rd, L. A. Cooper, K. A. Carson, N. Y. Wang, L. J. Appel, D. Gayles, J. Charleston, K. White, N. You, Y. Weng, M. Martin-Daniels, B. Bates-Hopkins, I. Robb, W. K. Franz, E. L. Brown, J. P. Halbert, M. C. Albert, A. T. Dalcin, and H. C. Yeh. 2016. A dietary intervention in urban African Americans: Results of the “Five Plus Nuts and Beans” randomized trial. American Journal of Preventive Medicine 50(1):87-95.
Miller, J. Z., M. H. Weinberger, and J. C. Christian. 1987. Blood pressure response to potassium supplementation in normotensive adults and children. Hypertension 10(4):437-442.
Mills, K. T., J. Chen, W. Yang, L. J. Appel, J. W. Kusek, A. Alper, P. Delafontaine, M. G. Keane, E. Mohler, A. Ojo, M. Rahman, A. C. Ricardo, E. Z. Soliman, S. Steigerwalt, R. Townsend, and J. He. 2016. Sodium excretion and the risk of cardiovascular disease in patients with chronic kidney disease. JAMA 315(20):2200-2210.
Mirmiran, P., Z. Bahadoran, P. Nazeri, and F. Azizi. 2018. Dietary sodium to potassium ratio and the incidence of hypertension and cardiovascular disease: A population-based longitudinal study. Clinical and Experimental Hypertension 40(8):772-779.
Morris, Jr., R. C., A. Sebastian, A. Forman, M. Tanaka, and O. Schmidlin. 1999. Normotensive salt sensitivity: Effects of race and dietary potassium. Hypertension 33(1):18-23.
Moseley, K., C. Weaver, L. Appel, A. Sebastian, and D. E. Sellmeyer. 2013. Potassium citrate supplementation results in sustained improvement in calcium balance in older men and women. Journal of Bone and Mineral Research 28(3):497-504.
Naismith, D. J., and A. Braschi. 2003. The effect of low-dose potassium supplementation on blood pressure in apparently healthy volunteers. British Journal of Nutrition 90(1):53-60.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Guiding principles for developing Dietary Reference Intakes based on chronic disease. Washington, DC: The National Academies Press.
Newberry, S. J., M. Chung, C. A. M. Anderson, C. Chen, Z. Fu, A. Tang, N. Zhao, M. Booth, J. Marks, S. Hollands, A. Motala, J. K. Larkin, R. Shanman, and S. Hempel. 2018. Sodium and potassium intake: Effects on chronic disease outcomes and risks. Rockville, MD: Agency for Healthcare Research and Quality.
Nieves, J. W., K. Melsop, M. Curtis, J. L. Kelsey, L. K. Bachrach, G. Greendale, M. F. Sowers, and K. L. Sainani. 2010. Nutritional factors that influence change in bone density and stress fracture risk among young female cross-country runners. PM&R 2(8):740-750.
Nowson, C. A., and T. O. Morgan. 1988. Change in blood pressure in relation to change in nutrients effected by manipulation of dietary sodium and potassium. Clinical and Experimental Pharmacology and Physiology 15(3):225-242.
Obel, A. O. 1989. Placebo-controlled trial of potassium supplements in black patients with mild essential hypertension. Journal of Cardiovascular Pharmacology 14(2):294-296.
O’Donnell, M. J., S. Yusuf, A. Mente, P. Gao, J. F. Mann, K. Teo, M. McQueen, P. Sleight, A. M. Sharma, A. Dans, J. Probstfield, and R. E. Schmieder. 2011. Urinary sodium and potassium excretion and risk of cardiovascular events. JAMA 306(20):2229-2238.
O’Donnell, M., A. Mente, S. Rangarajan, M. J. McQueen, X. Wang, L. Liu, H. Yan, S. F. Lee, P. Mony, A. Devanath, A. Rosengren, P. Lopez-Jaramillo, R. Diaz, A. Avezum, F. Lanas, K. Yusoff, R. Iqbal, R. Ilow, N. Mohammadifard, S. Gulec, A. H. Yusufali, L. Kruger, R. Yusuf, J. Chifamba, C. Kabali, G. Dagenais, S. A. Lear, K. Teo, and S. Yusuf. 2014. Urinary sodium and potassium excretion, mortality, and cardiovascular events. New England Journal of Medicine 371(7):612-623.
Pak, C. Y., R. D. Peterson, and J. Poindexter. 2002. Prevention of spinal bone loss by potassium citrate in cases of calcium urolithiasis. Journal of Urology 168(1):31-34.
Patki, P. S., J. Singh, S. V. Gokhale, P. M. Bulakh, D. S. Shrotri, and B. Patwardhan. 1990. Efficacy of potassium and magnesium in essential hypertension: A double-blind, placebo controlled, crossover study. BMJ 301(6751):521-523.
Prentice, R. L., Y. Huang, M. L. Neuhouser, J. E. Manson, Y. Mossavar-Rahmani, F. Thomas, L. F. Tinker, M. Allison, K. C. Johnson, S. Wassertheil-Smoller, A. Seth, J. E. Rossouw, J. Shikany, L. D. Carbone, L. W. Martin, M. L. Stefanick, B. Haring, and L. Van Horn. 2017. Associations of biomarker-calibrated sodium and potassium intakes with cardiovascular disease risk among postmenopausal women. American Journal of Epidemiology 186(9):1035-1043.
Rahimi, A. R. O., A. Mhmoodpoor, and S. Sanaie. 2007. The effect of high-calcium and high-potassium diet on grade-I hypertension and high normal blood pressure. Pakistan Journal of Medical Sciences 23(4):589-592.
Richards, A. M., M. G. Nicholls, E. A. Espiner, H. Ikram, A. H. Maslowski, E. J. Hamilton, and J. E. Wells. 1984. Blood-pressure response to moderate sodium restriction and to potassium supplementation in mild essential hypertension. Lancet 1(8380):757-761.
Sasaki, S., X. H. Zhang, and H. Kesteloot. 1995. Dietary sodium, potassium, saturated fat, alcohol, and stroke mortality. Stroke 26(5):783-789.
Sebastian, A., S. T. Harris, J. H. Ottaway, K. M. Todd, and R. C. Morris, Jr. 1994. Improved mineral balance and skeletal metabolism in postmenopausal women treated with potassium bicarbonate. New England Journal of Medicine 330(25):1776-1781.
Seth, A., Y. Mossavar-Rahmani, V. Kamensky, B. Silver, K. Lakshminarayan, R. Prentice, L. Van Horn, and S. Wassertheil-Smoller. 2014. Potassium intake and risk of stroke in women with hypertension and nonhypertension in the Women’s Health Initiative. Stroke 45(10):2874-2880.
Siani, A., P. Strazzullo, L. Russo, S. Guglielmi, L. Iacoviello, L. A. Ferrara, and M. Mancini. 1987. Controlled trial of long term oral potassium supplements in patients with mild hypertension. British Medical Journal (Clinical Research Edition) 294(6585):1453-1456.
Siani, A., P. Strazzullo, A. Giacco, D. Pacioni, E. Celentano, and M. Mancini. 1991. Increasing the dietary potassium intake reduces the need for antihypertensive medication. Annals of Internal Medicine 115(10):753-759.
Sinaiko, A. R., O. Gomez-Marin, and R. J. Prineas. 1993. Effect of low sodium diet or potassium supplementation on adolescent blood pressure. Hypertension 21(6 Pt 2):989-994.
Sluijs, I., S. Czernichow, J. W. Beulens, J. M. Boer, Y. T. van der Schouw, W. M. Verschuren, and D. E. Grobbee. 2014. Intakes of potassium, magnesium, and calcium and risk of stroke. Stroke 45(4):1148-1150.
Smyth, A., M. Griffin, S. Yusuf, J. F. Mann, D. Reddan, M. Canavan, J. Newell, and M. O’Donnell. 2016. Diet and major renal outcomes: A prospective cohort study. The NIH-AARP Diet and Health Study. Journal of Renal Nutrition 26(5):288-298.
Sundar, S., K. K. Sachdev, S. K. Vaish, S. K. Bhattacharya, V. P. Singh, and S. K. Agarwal. 1985. Potassium supplementation in essential hypertension—a double blind placebo controlled study. Journal of the Association of Physicians of India 33(12):776-777.
Svetkey, L. P., W. E. Yarger, J. R. Feussner, E. DeLong, and P. E. Klotman. 1987. Double-blind, placebo-controlled trial of potassium chloride in the treatment of mild hypertension. Hypertension 9(5):444-450.
TOHP (Trials of Hypertension Prevention) Collaborative Research Group. 1992. The effects of nonpharmacologic interventions on blood pressure of persons with high normal levels. Results of the trials of hypertension prevention, Phase I. JAMA 267(9):1213-1220.
Tunstall-Pedoe, H., M. Woodward, R. Tavendale, R. A’Brook, and M. K. McCluskey. 1997. Comparison of the prediction by 27 different factors of coronary heart disease and death in men and women of the Scottish Heart Health Study: Cohort study. BMJ 315(7110):722-729.
Umesawa, M., H. Iso, C. Date, A. Yamamoto, H. Toyoshima, Y. Watanabe, S. Kikuchi, A. Koizumi, T. Kondo, Y. Inaba, N. Tanabe, and A. Tamakoshi. 2008. Relations between dietary sodium and potassium intakes and mortality from cardiovascular disease: The Japan Collaborative Cohort Study for Evaluation of Cancer Risks. American Journal of Clinical Nutrition 88(1):195-202.
Vinceti, M., T. Filippini, A. Crippa, A. de Sesmaisons, L. A. Wise, and N. Orsini. 2016. Meta-analysis of potassium intake and the risk of stroke. Journal of the American Heart Association 5(10).
Vongpatanasin, W., P. Peri-Okonny, A. Velasco, D. Arbique, Z. Wang, P. Ravikumar, B. Adams-Huet, O. W. Moe, and C. Y. C. Pak. 2016. Effects of potassium magnesium citrate supplementation on 24-hour ambulatory blood pressure and oxidative stress marker in prehypertensive and hypertensive subjects. American Journal of Cardiology 118(6):849-853.
Weng, L. C., W. T. Yeh, C. H. Bai, H. J. Chen, S. Y. Chuang, H. Y. Chang, B. F. Lin, K. J. Chen, and W. H. Pan. 2008. Is ischemic stroke risk related to folate status or other nutrients correlated with folate intake? Stroke 39(12):3152-3158.
Yang, Q., T. Liu, E. V. Kuklina, W. D. Flanders, Y. Hong, C. Gillespie, M. H. Chang, M. Gwinn, N. Dowling, M. J. Khoury, and F. B. Hu. 2011. Sodium and potassium intake and mortality among US adults: Prospective data from the Third National Health and Nutrition Examination Survey. Archives of Internal Medicine 171(13):1183-1191.
Zhu, K., A. Devine, and R. L. Prince. 2009. The effects of high potassium consumption on bone mineral density in a prospective cohort study of elderly postmenopausal women. Osteoporosis International 20(2):335-340.
This page intentionally left blank.










































