Proceedings of a Workshop
| IN BRIEF | |
|
February 2019 |
School Success: An Opportunity for Population Health
Proceedings of a Workshop—in Brief
The National Academies of Sciences, Engineering, and Medicine’s Roundtable on Population Health Improvement hosted a workshop in Oakland, California, at The California Endowment’s Oakland Conference Center on June 14, 2018. The workshop featured presentations that described the relationship between the health and education sectors and shared examples of public health interventions and activities in schools that support school success and are potential opportunities for population health action.
Joshua Sharfstein from the Johns Hopkins Bloomberg School of Public Health welcomed the participants and conveyed his and other roundtable members’ sense of optimism about promising opportunities for the health and education systems to learn from each other. The day began with two keynote presentations reflecting on how educational attainment influences health outcomes and how health status affects educational performance. The keynote speakers were followed by a number of Ted Talk–style presentations describing school-based public health interventions and the workshop concluded by addressing policies, issues, and opportunities pertaining to shared measurement, legal issues, payment mechanisms, and equity.
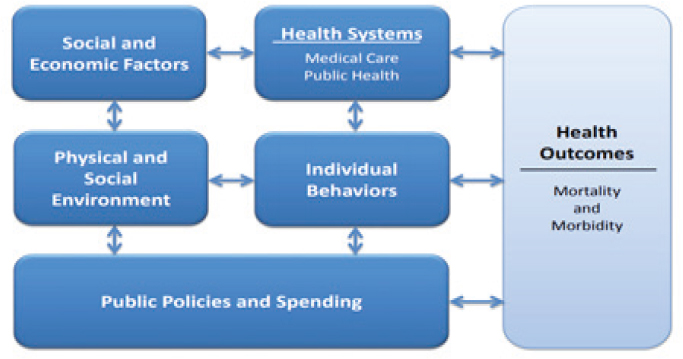
Steven Woolf from the Center on Society and Health at Virginia Commonwealth University articulated why educational success matters for health. Woolf stated that although the health and education systems work toward similar ends, they have functioned as silos for many years without much communication. He presented an overview of what shapes health through five domains: (1) health systems, (2) individual behaviors, (3) the physical and social environment, (4) socioeconomic factors, and (5) public policies and spending (see Figure 1). Woolf stressed that the fifth domain is of specific importance given that it drives the other domains.
Woolf mentioned that through public policies and spending, policy makers, elected officials, and the private sector shape the rest of the domains. He said that the influence of education, income, and wealth as part of the socioeconomic factors are “probably the most powerful predictor[s] of health outcomes” and that the data, evidence, and research to date crystalize the priority. Woolf presented a series of figures illustrating the relationship between health outcomes (all-cause mortality, reporting fair or poor health, physical health, and chronic disease) and education. All of the figures showed that the less educated have worse health outcomes. The data also revealed a health gradient among the different levels of education, and, in general, “the more education people have, the better their health will be,” said Woolf.
Woolf said that in the United States, the tendency is to assume that health is about health care; however, even when there is equal access to health care, the education gradient persists. Woolf also pointed out that the focus on health care in the United States resulted in tremendous amounts of money invested into that system to the detriment of other social determinants of health, like education. In a study1 co-authored by Woolf, the authors calculated how many lives would be saved in the United States through medical advances (new drugs and technologies) and how many lives would be saved if all adults had the mortality rate of people with “some college education.” The researchers found that for every life saved by medical advances, seven would be saved by closing the education gap. In terms of mental
__________________
1 Woolf, S. H., R. E. Johnson, R. L. Phillips, Jr., and M. Philipsen. 2007. Giving everyone the health of the educated: An examination of whether social change would save more lives than medical advances. American Journal of Public Health 97(4):679–683.
![]()
SOURCES: Presentation by S. Woolf, June 14, 2018. Adapted from NRC and IOM (National Research Council and Institute of Medicine). 2013. U.S. Health in International Perspective: Shorter Lives, Poorer Health. Washington DC: The National Academies Press.
health, Woolf said that those with lower education and income levels suffer from higher rates of hopelessness, sadness, and worthlessness. Lately, Woolf stated, researchers are drawing attention to “deaths of despair,” which include deaths from the opioid epidemic, alcoholism, and suicide, and research has shown that such deaths are concentrated among Americans with less educational attainment.
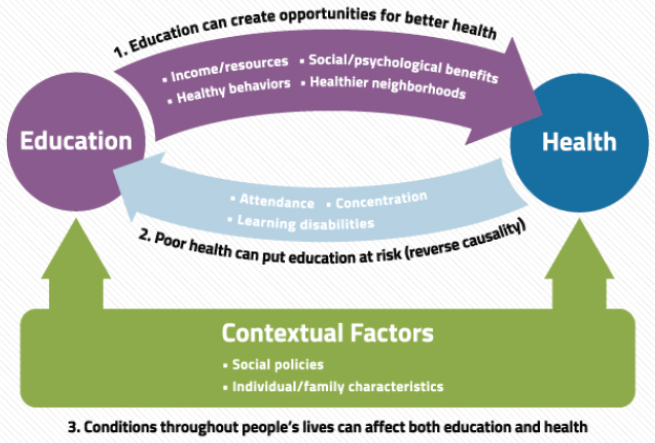
Woolf declared that it is well understood that someone with a higher education level will have the ability to access more economic resources through better jobs that pay well and offer benefits such as health insurance and better living conditions in a healthy neighborhood free of hazards that negatively affect health. However, Woolf said, one of the objectives of the workshop was to explore how better health results in improved educational outcomes (see Figure 2). Woolf stressed that contextual factors must be examined when assessing the relationship between health and education. For example, an upbringing with stress and trauma can cause toxic stress in children who then experience higher rates of risk for depression, substance abuse, and other diseases later in life. Another contextual factor is geography. For example, in Chicago there is a marked difference in life expectancy by census tract, with the Southside of Chicago experiencing much lower life expectancies and educational attainment than the rest of Chicago. He explained that low-income neighborhoods have lower property values and thus lower taxes funding the school systems, which affect factors like racial segregation. Thus, the living environment can affect a child’s ability to succeed in school and his or her health trajectory.
Woolf concluded by stating that efforts are in place to draw the connections between the community and the child’s experience in school. The Centers for Disease Control and Prevention, for example, has a “whole school, whole community, whole child model” that is being implemented in the St. Louis and Normandy school systems (in St. Louis) to apply a holistic approach to help provide community resources that are available to children.
Charles Basch from Teacher’s College at Columbia University delivered the second keynote speech. Basch articulated that schools are one of the key social instructions that shape the lives of children. He cautioned that although the reverse connection between health and education can be assumed, it has only been in the past 20 years that research has uncovered the reasons why. The basic idea was to understand that aside from the quality, organization, and financing of schools, the ability of children to be motivated and “ready to learn” is a factor influenced by health. Basch shared that the majority of his research focused on urban minority youth from low-income families, school-age youth, and certain health problems that can be feasibly addressed in a school setting.
Because schools cannot address every health problem, Basch stated, they have to prioritize based on the prevalence of health problems and disparities; the evidence supporting the causal pathways between health and educational outcomes; and the existence of promising programs and policies to address those outcomes. Based on that set of criteria, Basch presented research on eight health barriers to learning: (1) poor vision, (2) poorly controlled asthma, (3) teen pregnancy, (4) aggression and violence, (5) physical inactivity, (6) skipping breakfast and hunger, (7) attention deficit and hyperactivity disorder, and (8) oral health problems. By themselves or in combination, these health concerns negatively influenced educational outcomes by impeding sensory perception (visual acuity), cognition (memory, attention, integrating information, emotional regulation), and connectedness (relationships), and by contributing to chronic absenteeism and
Source: Presentation of S. Woolf, June 14, 2018. Center on Society and Health.
higher school dropout rates. Basch added that because many of these health concerns are concomitant and have effects that are additive and synergistic, schools need to address multiple health barriers to learning simultaneously in order to have measureable impact. School-specific priorities can be set by quantifying the magnitude and severity of health concerns; assessing the importance, feasibility, and acceptability of the programs available to be implemented, and involving the community in an ongoing process of prioritization. He expressed that the application of high-quality, evidence-based interventions is important, but even more important is the coordination that the application requires. A coordinated approach is an attempt to break down the education and health silos. Basch emphasized that what is needed is a multi-stakeholder approach that includes families, health service providers, community organizations, philanthropic organizations, government agencies, and institutions of higher education.
Joaquin Tamayo of Stand for Children moderated the five 7-minute Ted Talk style presentations. The first presenter was Megan Collins of the Wilmer Eye Institute at Johns Hopkins University, who discussed Vision for Baltimore. Collins explained that the risk of impaired academic performance is definite, and yet about 75 percent of children age 13 or younger do not know they have a vision problem. More often than not, vision problems are detected during school screenings; however, different states mandate vision screenings at different points in time. She explained that in the traditional visual care paradigm, the school notifies parents of a failed vision screening and then the family is responsible for securing eyeglasses. Barring any access barriers (e.g., cost, time, transportation), there are still challenges to contend with, like the student actually wearing the glasses, breaking them, or losing them. Collins explained that only about 5 percent of children who fail a vision screen are actually obtaining glasses in the community. Collins shared how Vision for Baltimore seeks to address the gaps in the traditional paradigm by providing every aspect of vision care at the school level. The initiative is 2 years old and executed by the Baltimore City Health Department, Johns Hopkins University, the Baltimore City Public School System, Vision to Learn, and Warby Parker. The 3-year program entails vision screenings performed by the health department and over the next 3 years will serve 150 schools in Baltimore City. Children who fail the vision screening are referred to a well-equipped mobile clinic where licensed optometrists perform eye exams, and the child gets to choose the Warby Parker frames he or she wants to wear at the mobile clinic. Two to 4 weeks after the eye exam, the children are fitted with their glasses. To ensure that the children wear their glasses, a system is in place where school staff monitor the children. In terms of evaluation, the academic impact of this program will be assessed by Johns Hopkins University.
Kimi Sakashita from the Alameda County Health Care Services Agency explained that the county is the sixth largest in California and one of the most culturally and economically diverse. Sakashita highlighted that there was a 15-year life expectancy disparity between an African American child residing in the Oakland flatlands or west Oakland, and a Caucasian child living in San Francisco’s most affluent areas or the Oakland Hills. Sakashita stated there would never be
one intervention or one organization that could address the causes of such a disparity. Therefore, she expressed, there is a need for a common agenda “with shared results across health and education sectors to achieve measurable and lasting change.” She explained that in Alameda County, the health agency, along with education, businesses, and philanthropy partners, carry out school health initiatives that support families and the physical, social, and emotional health of the students. The systems integration approach and the use of partnerships help achieve results through activities and services, she explained. One of the key services provided is access to school-based health centers. The county supports 29 centers with $100,000 each for the school year and provides medical, dental, and mental health services, as well as health education and youth development and leadership activities, including career pathways. Sakashita explained that the county uses the evaluation model Results-Based Accountability developed by Mark Friedman. There are three guiding evaluation questions: (1) How much did we do? (2) How well did we do it? and (3) Is anyone better off? Another project carried out by the department involves 15 school health centers that applied trauma informed care at each site. Sakashita reported that about 35 percent of students that screened positive for trauma needed follow-up care and 86 percent of those were connected to actual services. Sakashita emphasized that speaking in a language that is important to educators, sustaining partnerships and relationships, and building trust among them was the way to keep moving forward. She concluded that a system that serves those students and families who need it the most would benefit from the improved coordination of services.
Jill Halterman of the University of Rochester School of Medicine and Dentistry spoke via video about The Preventive Care Program for Urban Children with Asthma. The burden of asthma is substantial as it affects 1 in 11 children (about 7 million in the United States) and results in $50 billion in medical expenses annually. Halterman explained that there are also disparities in asthma, with a higher prevalence among Puerto Rican and non-Hispanic Black children, as well as children living in poverty. Halterman added that asthma is the leading cause of missed school days for children, totaling 13.8 million missed days. Halterman noted that the National Asthma Survey revealed that only 20 percent of children had optimal control of their asthma, 43 percent had persistent asthma with preventive medication use, and 37 percent had persistent asthma with no preventive medication use, representing preventable morbidity. The Preventive Care Program for Urban Children with Asthma focused on the delivery of effective medication to children via school-based programs because this setting provides the opportunity to identify high-risk children and build optimized systems of care. The program collaborated with the Rochester City School District’s school nurse program to implement both directly observed treatment (DOT) to ensure asthma medication adherence at least when the child attends school and treatment adjustment for those children who were adherent but still had asthma management issues in 60 preschools, elementary, and secondary schools. The school-based asthma therapy trial resulted in a 25 percent reduction of symptoms during day and night, asthma attacks, days absent from school, and activity limitations. The program also incorporates telemedicine as a mechanism to link children with primary care sites where they can access the appropriate preventive medication, which can be administered at school through DOT. Halterman observed that the health care and school partnerships can lead to improved symptoms, decreased absenteeism, and enhanced school engagement and attention, which is expected to contribute to improved academic outcomes and school success.
Heidi Schumacher of the District of Columbia Office of the State Superintendent of Education began by explaining that chronic absenteeism is defined as missing 10 percent or more of the school year. The average school year is 180 days, which means 18 days, or about 3.5 weeks, are missed. Many times, she explained, that translates to a child missing 2 or 3 days of school per month throughout the year, which many families normalize and do not recognize that the absenteeism requires attention. The issue with chronic absenteeism is that it not only affects academic success for the current academic year, but also future years and is ultimately a predictor of the likelihood of graduation. Schumacher said that the health care community realizes that the reasons why children are chronically absent are the same reasons they go to the doctor, and that the same social determinants of health that keep children from accessing adequate health care (lack of transportation, homelessness, child care) are the same ones that contribute to their absenteeism. Yet, the health care and school systems have not completely aligned the approaches to screen for the social determinants of health and recommend interventions. To address the issue, the DC and Baltimore school systems have started to leverage the relationships between families and child health care providers to address the social determinants of health. In order to do so, she explained, infrastructures must be set up to support interventions, starting with data sharing. Interventions to address chronic absenteeism require a timely and proactive systematic data-sharing mechanism, Schumacher explained. The health information exchange is a system by which providers have access to health data collected from hospitals, laboratories, and other entities. Schumacher explained that the DC public schools have linked their information system to the health information exchange, where first there is a matching process between the patient and student records, and then the system pushes bi-weekly reports to primary care doctors based on patient panels to identify how many of their patients missed school. Schumacher added that setting up the data infrastructure needed consent as required by the Family
Educational Rights and Privacy Act (FERPA), which is the education equivalent of the Health Insurance Portability and Accountability Act (HIPAA). The DC school system elicited broad stakeholder (including family) feedback about topics such as data sharing, confidentiality, and privacy. After input was gathered, a one-page letter and consent form was included in the schools’ enrollment packages and 75 percent of families consented to the data sharing between the systems. Schumacher explained that with the data-sharing infrastructure and consents in place, the next actionable step was distributing a survey for child health care providers through the local chapter of the American Academy of Pediatrics. Schumacher stated that the responses have helped the DC school system learn the training needs, how to better help clinicians understand chronic absenteeism, how the clinical space operationalizes the information it receives from the schools, and what resources are already available to it to pursue integration. Schumacher closed by stating that the pilot project is looking forward to evaluation over the coming years.
Jennifer Dillaha of the Arkansas Department of Health described how her state has used school-based influenza vaccination as a tool to reduce school absenteeism. Dillaha explained that Arkansas has the political will to improve conditions because many people are committed to making a difference in the state. Arkansas has a centralized state health department without any local health departments; the state operates at least one unit in each of the 75 counties. The local units offer childhood immunizations; the Special Supplemental Nutrition Program for Women, Infants, and Children; and family planning and prenatal care, among other population-based public health services. Dillaha explained that in 2007, the local health units started collaborating with local school districts to conduct school-based vaccination clinics each fall and is now in its 11th year. The collaboration between public health and school staff includes addressing several challenges, Dillaha stated. Among these challenges are the planning of the clinics; preparing materials, including bilingual (English and Spanish) vaccine education forms; verification of parental consent; transporting vaccines while maintaining the cold-chain; documenting doses for billing when possible; and data entry into the immunization registry. During the 2017–2018 school year, there were about 480,000 students enrolled in more than 1,000 public schools. A flu vaccination clinic was hosted in 953 schools over a 2-month period, resulting in 120,000 doses administered, which represents a vaccination rate of 25 percent in the student population. The Arkansas Department of Health compared the flu vaccination rates with all-cause absenteeism during the 8-week period of the peak flu season (the worst since 1953) to account for the severity of the flu season. The study found that a 10 percentage point increase in the vaccination rate was associated with a 0.23 percentage point decrease in absenteeism, translating to a 45,000 school-student-day reduction in absenteeism.
The next session of the workshop featured the state of Oregon as a case example of health and education sector collaboration to improve specific educational outcomes. Phyllis Meadows from the Kresge Foundation introduced the three speakers: Lillian Shirley of the Oregon Health Authority, Janet Meyer of HealthShare of Oregon (a coordinated care organization [CCO]), and Dianne Kilkenny from Morrow County Health Department. Shirley began by stating that Oregon is working to implement research and tools that link health and education through its state plan, which works with coordinated care organizations and schools. The tagline for this work is “Healthy Kids Learn Better.” Shirley explained that Oregon organized its health care transformation around the triple aim: better health, better care, and lower cost. By pursuing the triple aim, payers, providers, and policy makers have looked to the community and community institutions for solutions as strategies to achieve those aims. Shirley mentioned that at the school level, Oregon tracks data that impact school attendance, and found that some of the areas that received attention were physical activity, nutrition, substance abuse, safety concerns, and unintended pregnancies. Shirley mentioned that the data provided by the public health sector help different jurisdictions prioritize and support interventions within specific communities. Shirley mentioned that the Medicaid transformation reform rallied payers, health systems, and legislators to the table given that every stakeholder was losing money, and 5 years after the transformation Oregon has seen improved quality and care and a decrease in cost across the state. If system transformation is where Oregon started, Shirley clarified that the integration of health and human services with community problem-solving is where the state wants to go. Shirley stressed the importance of formal agreements to sustain cross-sector endeavors at the state level. She concluded by stating that the Oregon approach includes a focus on relationships, agreements, target initiatives, progress tracking through metrics, and incentives to reflect accountability.
Meyer explained how a Medicaid-managed care plan entered the realm of school success. Meyer explained that she was given the task of identifying “high utilizers” and achieving the CCO incentive metrics to receive bonus money from Medicaid. She said that to understand the reason for high utilization of health care by certain individuals, the CCO had to delve into their social pathway. Meyer mentioned that high-utilization individuals had lives of trauma and adverse events that led them to use the health care system. Meyer said the medical director of the managed care plan suggested going upstream to assess kindergarten readiness as a means of addressing the issues afflicting the high utilizers. Meyer mentioned that many of the metrics to meet under Oregon’s CCO program already pertain to children (e.g., developmental screening, adolescent well-visits, screening for kids in foster care) and were being met, but that after the CCO “checked
the box” there were needs left unaddressed. After realizing that the CCO was not going to be able to “fix” the high utilizers, the CCO started delving into early-life health in spite of reservations about entering an unknown space. The health care system is in constant contact with the pediatric population until the age of 5, and so the managed care plan designed Project Echo. This project trains providers and pediatricians to address developmental issues in children. On the human services side, the managed care plan invested in a 3-year program called Help Me Grow, which helps families connect with services. Meyer explained that in 2017 the board of directors of HealthShare of Oregon approved the Ready and Resilient plan, which builds on prior work and focuses on kindergarten readiness and connecting families to services. The program uses a collective impact framework, and in terms of kindergarten readiness, HealthShare of Oregon is working with early-learning hubs and community-based organizations like United Way and Social Ventures Partners, which also financially support the plan. Meyer mentioned that in order to arrive at the plan, there were 6 years of prior discussion pertaining to building infrastructure and building a system of care with an indirect return on investment that is felt at the community and family levels, as well as by tax payers, but not necessarily the investor. Medicaid served as existing scaffolding to support families and, she concluded, using it to address the issues that lead to high utilization is an investment worth making.
Kilkenny began by describing Morrow County, a rural northeastern Oregon county that is part of the largest geographical CCO in Oregon, which includes 12 counties. Each county has a local community advisory committee (LCAC). The LCAC comprises representatives from private business, county government, public health, school districts, the Department of Human Services, and Head Start programs. Kilkenny mentioned that the need for a multi-sectoral approach was based on the realization that the needs of Morrow residents were outside the scope of any one given agency or beyond their respective resources. She explained that although every partner had a specific reason for being part of the LCAC, they were in agreement that they wanted a healthier future for the counties’ residents and that started with a better educational attainment. By sharing resources, she explained, the wellness hubs at schools provide preventive services and health care access and improve health care delivery and equity across the county. She described Morrow county schools as afflicted by high absenteeism rates and high teacher turnover, with declining metrics and resource constraints. Kilkenny added that in the county the (social) minority is the majority, where diversity in cultures, ethnicities, languages, socioeconomics, and geography are represented. One of the concerns of the county was the “mobile students,” those who attended more than one school within one school year and missed 10 consecutive days of school on average, and exit the Oregon education system without earning a diploma or certificate. To address the issue a wrap-around system was created that committed to helping students from the beginning, which includes prenatal to age 5 services, kindergarten readiness, graduation, and workforce readiness. Through partner and self-referrals, care and wrap-around mental and physical services are provided to these groups. Among these services are dental and vision screenings, follow-up exams, and immunizations. The wraparound teams in each school include care and workforce coordinators, counselors, and communicators to do outreach. Aside from addressing the mental and physical health issues of the students, the wellness hubs also address families in need, including food security, medical referrals, and transportation needs.
Meadows introduced the second case study from Cincinnati, Ohio. Robert Kahn and Uma Kotagal (video conferencing) from Cincinnati Children’s Hospital Medical Center (CCH) presented the case study. Kahn began by explaining that the case study was about how the health care and the school systems are working together. Kahn explained that CCH is the provider for 95 percent of admissions in the eight-county area it serves. For its strategic plan for 2020, CCH sought to reach beyond health care to define child health. The starting point was to address the 66,000 children in the city and the 187,000 children in the county in order to track progress on 4 specific outcomes that were of interest: annual infant deaths, hospital bed days disparities (by neighborhoods), thriving at age 5 (healthy minds and bodies of 5-year-olds), and third-grade reading level proficiency. To address these issues, improvement teams were set up with community co-leads and core areas configured to provide guidance for each of the outcomes. In particular to the workshop, the third-grade reading level outcome was supported by an improvement team and the community quality improvement capability core area. Kahn explained that quality improvement (QI) theory and concepts in other industries are being applied to the education space, including the application of models, small-scale rapid testing, the use of huddles and frontline engagement, and population segmentation. These concepts and interventions are shared through training courses, consultations and coaching, and extended learning sessions. Kahn explained that both the hospital and the school district have made system-level changes, including training staff to engage with the other sector and applying QI principles to processes that indirectly affect staff; for example, reducing errors in the payment of teachers to minimize the burdens they deal with on a daily basis. He closed by stating that metrics of child thriving must be added to the deficit metrics, and that learning networks accelerate cross-sector work between the school and health care systems. He added that the integration across sectors must be real and realizable; in other words, supported by theory and an implementation plan. He said the teams also learned that capacity building in QI provides a common platform for measurement, testing, learning, and creating the new integrated system; co-production with parents is key; and finally, finding joy in this type of work enables resilience in teachers, medical providers, and parents.
Marc Gourevitch from NYU Langone Medical Center moderated the last panel session of the workshop, which included Rochelle Davis from the Healthy Schools Campaign, Denise Chrysler from the University of Michigan, Kelly Hall of Pembroke Policy Consulting, and Kent McGuire from the William and Flora Hewlett Foundation. The panel discussed metrics, legal concerns, payment and reimbursement and equity in terms of cross-sector collaboration in health and education.
Davis, who is also the co-chair of the National Collaborative for Education in Health (NCEH), discussed the practice and potential for the health sector to use education metrics to align both sectors to support children’s health. She said the Healthy Schools Campaign (HSC) advocates for policies and practices that support schools in creating student health and school wellness so that all students are in school, healthy, and ready to learn. The HSC takes a policy and systems-level approach to effect change, and the use of metrics and data sharing is critical to long-term sustainable change. The HSC worked with Trust for America’s Health to incorporate health metrics into education accountability systems. Davis added that the NCEH convened a working group on metrics that engages educators, data experts, and others to better understand the education metrics landscape. One of those measures is chronic absenteeism, which includes excused and unexcused absences and suspensions. Davis mentioned that chronic absenteeism is the best proxy for school wellness and student health support. So important is the metric, added Davis, that the U.S. Department of Education’s (ED’s) Office for Civil Rights collects chronic absenteeism data every other year, the Every Student Succeeds Act 2015 (ESSA) requires the metric on every school report card, and 36 states and the District of Columbia have incorporated the metric into their state accountability systems. The campaign also focuses on supporting education staff at the state level and others to expand Medicaid-funded school health services. Through in-depth interviews asking how the health sector used education metrics, the most common metrics were attendance, high school graduation, kindergarten readiness, third-grade reading level, and measures of teacher wellness and turnover. However, their use is complicated by a set of barriers that include data sharing, messaging, and training, as well as needs assessments and evaluation. Davis explained that the accountability structure in the national education policy is ripe for using health metrics and the campaign developed guidance for states to help them think about incorporating health into their needs assessments. She mentioned that institutional support for shared metrics and data systems is still relatively new and that the examples presented at the workshop were innovators breaking new ground.
Chrysler from the Network for Public Health Law Mid-States Region at the University of Michigan School of Public Health explained that the network promotes and supports the use of law to protect the public’s health by providing direct technical assistance; developing and providing training, materials, and practical tools; and connecting individuals to build a public health law community. She explained that attorneys perceive the attempt to break down the silos between the education and health systems differently given that one of the main concerns of lawyers is the protection of these silos to keep the information gathered. Chrysler clarified that relationships built between the two systems, under the law, must also be defined, because the applicability of the law depends on the definition of those relationships. For example, in terms of school-based clinics, whether FERPA or HIPAA apply is contingent on whether it is the school or local health department. She added that risk perception is also different for lawyers; given that laws are often “contradictory, silent, and ambiguous,” they require professional judgment all the time. Attorneys are risk averse, she explained, and if there is any doubt in terms of liability, the answer to a question will be “no.” Where public health sees no risk in sharing data with a school system, a lawyer will. Chrysler mentioned that establishing a relationship with an attorney so that he or she understands the process and context from the beginning is helpful in breaking down the silos. In terms of FERPA, Chrysler explained that is a federal statute and contains regulations adopted by ED, which protect student education records and grants, guarantee parent and student rights, and apply to schools, their agents (e.g., contractors), and programs funded by the department. Education records include anything that pertain to the student maintained by the school (transcripts, disciplinary records, immunization records, and others). She added that FERPA allows for the disclosure of de-identified data, data shared with written consent, or data shared under FERPA exception. Chrysler added that the definitions of “de-identified data” and “consent” differ under FERPA and HIPAA. She concluded that to help with understanding FERPA, ED has resources, model forms, and tutorials that include a data-sharing toolkit for communities written in plain English and can be shared with collaborating partners.
Hall helped establish the Center for Medicare & Medicaid Innovation (CMMI), which held a $10 billion budget destined to make investments in health provider’s business models to improve health care outcomes and lower cost. Hall stated that health care coverage for children in and of itself is important for both health and educational outcomes. She stated that the percentage of uninsured children in the United States is at an all-time low at 5 percent; however, there are states like Texas and Utah where the rates are as high as 13 percent. Hall mentioned that states with Medicaid expansion saw a decrease in the number of uninsured children and the states where Medicaid eligibility was restricted saw an increase in the number of uninsured children. In terms of payments and financial incentives, Hall mentioned that new
models like the CCOs in Oregon are using financial incentives to motivate health care plans to concern themselves with community-based outcomes like educational attainment. In terms of changing hospital and provider behavior, entities need to be motivated, Hall mentioned. She offered the example of the Centers for Medicare & Medicaid Services stopping reimbursement to hospitals for treatment of hospital-acquired conditions or other preventable conditions like urinary tract infections and pressure ulcers. Similarly, in terms of the hospital readmissions program, when hospitals were financially penalized for being in the bottom quintile for readmissions, their rates dropped. Hall mentioned that although these approaches used “sticks” instead of “carrots,” the use of metrics as accountability measures could similarly motivate the multitude of providers to mobilize and change absenteeism rates, for example. Hall added that it is particularly difficult to align shared incentives and savings in terms of children to reduce costs in the health care system because, save for a small number of “high-cost children,” children are already relatively low cost and there is not much room to drive down health care spending in that population. Hall mentioned that through their Medicaid contracts, states can require managed care companies to report on certain data (like community-based measures) without a need for a federal waiver or a legislative endeavor and therefore states have latitude in what they can require.
McGuire directed the workshop attendees to the Communities in Action: Pathways to Health Equity report’s section on education2 for a comprehensive look at the health, equity, and education issues. McGuire stated that ESSA moved the education system toward a more holistic approach because it allowed states and localities the authority to make decisions about how to interpret the law. However, he added, ESSA is far from establishing a set of robust education metrics. He mentioned that there were a few considerations to take into account in terms of metrics. The first was to distinguish that there are metrics that pertain to “in-school” factors like academic and cognitive skills that are predictors of academic success that are the focus of policy makers (literacy, early childhood education) and “non-school” factors that contribute to or inhibit educational attainment (parenting, home learning, and social environments like neighborhood safety and security). McGuire offered that in order to build a robust set of metrics, there are many challenges to face, and among those are factors like segregation, housing patterns, and transportation issues that affect the ability of a student to learn. One possible mechanism to address these challenges, McGuire explained, is to have a solution-based approach versus a problem-based approach and to focus on policy relevant activities. Another approach is to have a technical component to the solution, like capturing data, and having analytic links between key components of the data. He closed by stating that the metrics also have to be malleable; that is, that the measures and indicators must be traceable on the education side and the health side to reveal linkages to attainment.♦♦♦
__________________
2 National Academies of Sciences, Engineering, and Medicine. 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press. https://doi.org/10.17226/24624.
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Carla S. Alvarado as a factual summary of what occurred at the workshop. The statements made are those of the rapporteur or individual workshop participants and do not necessarily represent the views of all workshop participants, the planning committee, or the National Academies of Sciences, Engineering, and Medicine.
PLANNING COMMITTEE FOR USING EDUCATION METRICS TO IMPROVE POPULATION HEALTH OUTCOMES: A WORKSHOP*
Alex Billioux, Centers for Medicare & Medicaid Services; Marc Gourevitch, NYU Langone Health; Robert Kahn, Cincinnati Children’s Hospital Medical Center; Robert Kaplan, Stanford University; Phyllis Meadows, The Kresge Foundation; Elena Rivera, Children’s Institute, Oregon; Heidi Schumacher, District of Columbia Office of the State Superintendent of Education; and Joshua Sharfstein, Johns Hopkins University.
*The National Academies of Sciences, Engineering, and Medicine’s planning committees are solely responsible for organizing the workshop, identifying topics, and choosing speakers. The responsibility for the published Proceedings of a Workshop—in Brief rests with the rapporteur and the institution.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Ihuoma Emenuga, Baltimore City Health Department Youth, Wellness and Community Health, and Cesar De La Vega, ChangeLab Solutions. Lauren Shern, National Academies of Sciences, Engineering, and Medicine, served as review coordinator.
SPONSORS: This workshop was partially supported by Aetna Foundation, Association of American Medical Colleges, The California Endowment, Dartmouth-Hitchcock Medical Center, Health and Human Services Program Support Center, Health Resources and Services Administration, Kaiser Permanente, The Kresge Foundation, Nemours, New York State Health Foundation, NYU School of Medicine’s Department of Population Health, Rethink Health, Robert Wood Johnson Foundation, Samueli Institute, and Wake Forest Baptist Medical Center.
For additional information regarding the workshop, visit http://nationalacademies.org/hmd/Activities/PublicHealth/PopulationHealthImprovementRT/2018-JUN-14.aspx.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2019. School success: An opportunity for population health action: Proceedings of a workshop–in brief. Washington, DC: The National Academies Press. doi: https://doi.org/10.17226/25370.
Health and Medicine Division

Copyright 2019 by the National Academy of Sciences. All rights reserved.









