2
Disability and Function
This chapter begins with a brief overview of different models of the concept of disability and discussion of the U.S. Social Security Administration’s (SSA’s) definition of disability and consideration of function within its disability determination process. The latter discussion includes a summary of SSA’s collection and use of occupational information that sets the stage for identification of the physical and mental “functional abilities relevant to work requirements” the committee was asked to consider in its Statement of Task. The chapter continues with a description of the committee’s ecological framework for functional assessment as it relates to work and ends with findings and conclusions. Appendix B provides definitions for many of the terms used in this discussion.
EVOLUTION OF THE CONCEPT OF DISABILITY
The concept of disability has evolved over the past several decades from a medical to a biopsychosocial model. In the medical model, disability is viewed as a feature of a person that is caused by injury, disease, or other health conditions and managed through medical treatment or modification of an individual’s behavior (WHO, 2001, 2002; see also IOM, 1991; Kaplan, 2000). In contrast, the biopsychosocial model views disability as a problem at the societal level; therefore, it is the collective responsibility of society to facilitate the full participation of individuals with disabilities in all aspects of life (Kaplan, 2000; WHO, 2001). The biopsycho-ecological model expands the concept of disability further by recognizing that elements of individuals’ physical and social environments may serve as barriers to or
facilitators that enhance activity and participation along the disablement pathway (Stineman and Streim, 2010). For example, inaccessible buildings and transportation represent barriers to participation for individuals who use wheelchairs, while modifications such as ramps, electric doors, elevators, and the like and wheelchair-accessible public transportation serve as facilitators (NASEM, 2017).
The World Health Organization’s International Classification of Functioning, Disability and Health (ICF) portrays human functioning and disability “as a dynamic interaction between health conditions (diseases, disorders, injuries, traumas, etc.) and contextual factors” (WHO, 2001, p. 8). Figure 2-1 depicts the ICF model of functioning and disability. As shown in the middle tier of the figure, functioning and disability consist of an interplay among body functions and structures at the organ level, activities at the person level, and participation at the societal level. The bottom tier of the figure depicts the contextual factors (environmental and personal) that may affect an individual’s functioning as barriers or facilitators. Environmental factors may be individual, encompassing one’s immediate environment, or societal, encompassing the “formal and informal social structures, services, and overarching approaches or systems in the community or society” that affect one’s functioning. Personal factors include gender, race, ethnicity, age, social and educational background, current and past experiences, behavior patterns, and psychological assets (WHO, 2013).
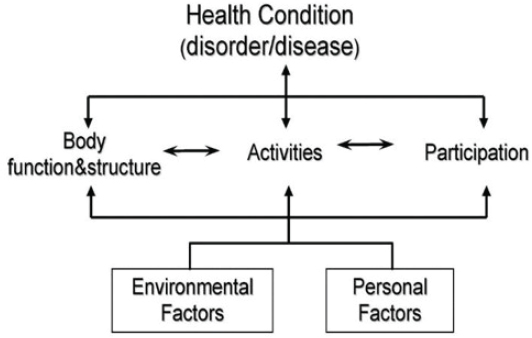
NOTE: The ICF model refers to deficits in body function and structure as “impairments,” deficits in completing activities as “limitations,” and reductions in participation as “restrictions.”
SOURCE: WHO, 2001, p. 18.
In the ICF model, disability is “an umbrella term for impairments [of body functions or structures], activity limitations and participation restrictions” (WHO, 2001, p. 213). Disability arises from “the interaction between an individual (with a health condition) and that individual’s contextual factors (environmental and personal factors)” (WHO, 2001, p. 213).
The ICF model encompasses three levels of functioning (middle tier of Figure 2-1). The first level, body function and structure, includes the “physiological functions of body systems, including psychological functions” and the functioning of body structures, or movement of “anatomical parts of the body such as organs, limbs and their components” (WHO, 2001, p. 213). Decrements in these functions are labeled “impairments” in the ICF model. The second level of functioning is activities—actions or tasks performed by an individual, such as walking, lifting, keyboarding, or problem solving. The ICF calls decrements in this level of functioning “limitations.” The third level of functioning is participation, or the performance of tasks in a societal context. Work is an example of participation. A task is a set of mental and physical activities in which an individual engages to accomplish a specific goal at or by a specific time. Although tasks are incorporated under activities in the ICF model, the committee recognizes them as a discrete intermediary level of functioning between activities and participation. Decrements in participation are called “restrictions” in the ICF model. Accommodations (e.g., assistive technologies, environmental modifications) are environmental contextual factors that act on ICF domains to enhance an individual’s activity and participation.
SOCIAL SECURITY ADMINISTRATION’S CONSIDERATION OF FUNCTION
As stated in Chapter 1, SSA’s definition of disability in adults is “inability to engage in any substantial gainful activity [SGA] by reason of any medically determinable physical or mental impairment which can be expected to result in death or which has lasted or can be expected to last for a continuous period of not less than 12 months.”1 SGA is work activity that “involves doing significant and productive physical or mental duties” or activities that are “done (or intended) for pay or profit,” regardless of whether a profit is realized.2 This work activity includes both an individual’s previous work, if any, and, considering age, education, and work experience, any other kind of substantial gainful work that exists in the national economy. For SSA, “disability” refers to work disability. More broadly, work disability may be understood as an inability to participate in work on a “regular
___________________
1 42 U.S.C. 423; see also 20 CFR 404.1505; 20 CFR 416.905.
2 20 CFR 404.1510; 20 CFR 416.910; 20 CFR 404.1572; 20 CFR 416.972.
and continuing basis” (8 hours per day, 5 days per week, or an equivalent work schedule [SSA, 2018g]), which would place it under “participation” on the far right side of the ICF model (see Figure 2-1).
SSA uses a five-step evaluation process in determining whether an adult meets the definition of disability.3
- In the first step, SSA considers applicants’ work activity in the past year. If an applicant is working at SGA, SSA will not proceed with a disability determination. SGA is defined as “work that—(a) involves doing significant and productive physical or mental duties; and (b) is done (or intended) for pay or profit.”4 To be eligible for a disability determination, in 2019 a nonblind individual must not earn more than $1,220 per month after deduction of impairment-related work expenses (SSA, 2019). Examples of impairment-related work expenses that can be deducted include certain attendant care services, medical devices, equipment, and prostheses (SSA, 2015c). For Social Security Disability Insurance applicants, insured status is verified, while for Supplemental Security Income applicants, countable income and assets are verified to be below thresholds.
- In step 2, SSA determines whether applicants have a medically determinable physical or mental impairment or a combination of impairments that meets severity and duration requirements. According to SSA’s Program Operations Manual System, “when medical evidence establishes only a slight abnormality or a combination of slight abnormalities which would have no more than a minimum effect on an individual’s ability to work, such impairment(s) will be found [to be] ‘not severe,’ and a determination of ‘not disabled’ will be made” (SSA, 2012). Applicants will also be denied in step 2 if their impairment neither is “expected to result in death” nor “has lasted or can be expected to last for a continuous period of not less than 12 months.”5
- In step 3, SSA assesses an applicant’s impairment using the Listing of Impairments (SSA, 2017b), a regulatory list of medical conditions and criteria created by SSA to assist in disability determination. The Listing of Impairments describes, for each of the major body systems, impairments that SSA considers to be severe enough to prevent a person from performing any gainful activity, regardless of his or her age, education, or work experience. Step 3 serves as a “screen-in” step. If an applicant’s impairment “meets” or “equals”
___________________
3 See 20 CFR 404.1520; 20 CFR 416.920.
4 20 CFR 404.1510; 20 CFR 416.910.
5 20 CFR 404.1505; 20 CFR 416.905.
-
a listing, the applicant is allowed benefits. To meet a listing, an applicant must have a medically determinable impairment that satisfies all of the criteria for that listing (SSA, 2018c). An impairment equals a listing if it is “at least equal in severity and duration to the criteria of any listed impairment” (SSA, 2018d). Applicants proceed to step 4 when their impairment is severe but does not meet or medically equal any listing within the Listing of Impairments.
- In step 4, SSA assesses whether applicants’ physical or mental residual functional capacity (RFC) allows them to perform past relevant work.6 SSA defines RFC as “the most [an applicant] can still do despite [his or her impairment-related] limitations” or restrictions7 on “a regular and continuing basis”8 (SSA, 2017a). Applicants able to perform past relevant work are denied benefits, while applicants unable to do so proceed to step 5.
- At step 5, SSA considers applicants’ RFC and such vocational factors as age, education, and work experience, including transferrable skills in determining whether they can perform other work in the national economy. Applicants determined to be unable to adjust to performing other work are allowed benefits, while those who are determined able to adjust are denied.
In determining whether an applicant’s impairment(s) is severe and meets or medically equals a listing or assessing an applicant’s RFC, SSA gathers various information. This includes functional information from the applicant, relevant health care providers, and third parties about the applicant’s impairment-related symptoms, such as pain, that may affect what he or she can do in a work setting. SSA considers function at several points in the five-step evaluation process. Functional criteria are built into a number of the adult listings in the Listing of Impairments SSA considers at step 3 (SSA, 2017b) (see Annex Table 2-1). These listings include both impairments and limitations in activity, using the ICF terminology. SSA also considers function in its assessment of applicants’ physical and/or mental RFC at steps 4 and 5. In some cases, RFC, particularly mental RFC, is a refinement of activity performance taken from the Listing of Impairments.
SSA uses different forms to collect functional information. The job activity section of the adult disability report form (SSA-3368-BK) collects functional information related to the number of hours an employee
___________________
6 “Past relevant work” refers to “work that you have done within the past 15 years, that was substantial gainful activity, and that lasted long enough for you to learn to do it” (20 CFR 404.1560).
7 These are functional limitations in activities according to the ICF approach, but they may also include data on restrictions on participation in work.
8 20 CFR 404.1545; 20 CFR 416.945.
performed such tasks as walking, standing, sitting, climbing, stooping, kneeling, crouching, crawling, handling large objects, and reaching (SSA, 2015a). The information collected on lifting and carrying includes detail on the amount of weight lifted and how frequently (one-third to two-thirds of the workday) and how far the object had to be carried.
A second form, the function report form (SSA-3373-BK),9 asks how the applicant’s illness, injury, or condition limits his or her ability to work (SSA, 2015b). In addition, the form asks detailed questions about various daily activities. The applicant also is asked whether his or her illness, injury, or condition affects the ability to dress, bathe, care for hair, shave, self-feed, and use the toilet. Questions about meals, house- and yardwork, getting around, shopping, money, hobbies and interests, and social activities are asked as well. Also collected is information about which physical and mental abilities—including lifting, walking, memory, concentration, understanding, and following instructions—have been affected by the applicant’s injury/illness.
A third form, the psychiatric review technique form (SSA-2506-BK),10 is completed by the disability examiner or the medical consultant (MC) or the psychological consultant (PC). The MC or PC has overall responsibility for the assessment of medical severity and for the content of the form. The form includes the criteria in the mental disorders listings, and is used to record the presence or absence of the listing criteria and the rating of the degree of functional limitation.11
Two other forms address physical and mental RFC and are described in the following section.
Residual Functional Capacity
An RFC assessment
- is based primarily on medical evidence but may also include observation or description of limitations (e.g., lay evidence, including the claimant’s statement);
- describes what an individual is able to do, despite functional limitations resulting from a medically determinable impairment(s) and impairment-related symptoms; and
___________________
9 Additional forms include SSA-3380-BK, which collects the same information but from third-party sources, and SSA-3385-BK, which is used to collect information from a former employer about an applicant’s functioning in a work setting. This text has been revised since prepublication release.
10 Form SSA-2506-BK (01-2017) UF, obtained via personal communication with Joanna Firmin, Social Security Administration, February 23, 2018.
11 This text has been revised since prepublication release.
- is an administrative determination of an individual’s capacity to perform work-related physical and mental activities (excerpted from SSA, 2018e).
In terms of content, an RFC
- Describes work-related functions a person can do on a sustained basis.
- Addresses all functional capabilities and provides a written analysis of how the evidence in file supports or refutes the following:
- claimant allegations (including allegations of symptoms, such as pain, and their effects on functioning).
- descriptions, observations, and all conclusions of all treating and examining sources.
- other pertinent medical and nonmedical evidence.
- Resolves all issues of functional capacity pertinent to a determination of ability to do past relevant work or other work.
- Provides conclusions as to functional capabilities (with a citation of pertinent evidence) and the reasoning to support these findings (excerpted from SSA, 2018e).
SSA MCs and PCs evaluate physical and mental RFC, respectively, although the disability examiner may assist in completion of the RFC assessment forms in some cases (SSA, 2018e). SSA uses the information about applicants’ RFC to make a determination at step 4 or 5 of the disability evaluation process. If a determination is appealed, a new RFC assessment is made at each adjudicative level. Typically, RFC is assessed by the MC/PC at the initial and reconsideration level. An administrative law judge assesses the RFC at the hearing level, and an administrative appeals judge assesses RFC at the Appeals Council level.12
Physical RFC is based on all the relevant evidence in the applicant’s case record, such as medical signs and laboratory findings, effects of treatment, reports of daily activities, lay evidence, recorded observations, medical source statements, effects of symptoms, evidence from attempts to work, need for a structured living environment, and work evaluations (SSA, 2018f). Exertional limitations on the physical RFC assessment form (SSA-4734-BK) (SSA, 2004) refer to the weight an individual can lift and/or carry, including upward pulling, and with what frequency. “Occasionally” means “from very little up to one-third of an 8-hour workday (cumulative, not continuous),” and “frequently” means “for one-third to two-thirds of an 8-hour workday (cumulative, not continuous)” (SSA, 2004). Weights range
___________________
12 20 CFR 404.1546. This text has been revised since prepublication release.
from less than 10 pounds to 100 pounds or more (occasionally) and less than 10 pounds to 50 pounds or more (frequently). Other exertional limitations include the length of time an applicant can stand and/or walk and sit, as well as any limitation in pushing and/or pulling, including the operation of hand and/or foot controls. Postural limitations assessed include climbing (ramp/stairs, ladder/rope/scaffolds), balancing, stooping, kneeling, crouching, and crawling. Manipulative limitations include reaching in all directions, including overhead; handling (gross manipulation); fingering (fine manipulation); and feeling (skin receptors). Visual limitations are assessed for near and far acuity, depth perception, accommodation, color vision, and field of vision. Communicative limitations include hearing and speaking. Environmental exposure limitations are noted as well, for extreme cold or heat; wetness; humidity; noise; vibration; fumes, odors, dusts, gases, and poor ventilation; and hazards, such as machinery or heights.
Mental RFC again is based on all the relevant evidence in the applicant’s case record. The mental RFC assessment form (SSA-4734-F4-SUP) (SSA, n.d.) asks for the PC’s summary conclusions derived from the evidence in an applicant’s file. Twenty mental activities in four categories (understanding and memory, sustained concentration and persistence, social interaction, and adaptation) are summarized in terms of the individual’s ability to sustain them over the course of an 8-hour workday and a 5-day workweek. Each mental activity is rated as “no evidence of limitation,” “not significantly limited,” “moderately limited,” “markedly limited,” or “not ratable on available evidence.” The form also contains a section for the PC to elaborate on the summary conclusions in narrative form, including any clarifying information and explanations of any conclusions that “differ from those of treating medical sources or from the individual’s allegations.”
Occupational Information
In addition to RFC, SSA must consider occupational information at steps 4 and 5 of the sequential evaluation process. As described previously, SSA must determine whether individuals’ RFC allows them to perform past relevant work at step 4 or, along with such vocational factors as age, education, and work experience, including transferrable skills, allows them to adjust to any other work in the national economy at step 5.
SSA’s primary source of information about work in the national economy is the U.S. Department of Labor’s Dictionary of Occupation Titles (DOT), originally developed in 1938 (SSA, 2018a). The U.S. Department of Labor stopped updating the DOT in 1991 and in 1998 replaced it with the Occupational Information Network (O*NET) (SSA, 2018a), a database of occupation characteristics and worker attributes for almost 1,000 occupations (O*NET Resource Center, 2018a).
Despite the wealth of information contained in O*NET, numerous reports have concluded that the database does not fully meet SSA’s disability adjudication needs (GAO, 2002a,b; IOM, 1998, 2002; NRC, 2010; Social Security Advisory Board, 2001). Accordingly, in addition to using information from O*NET, SSA currently is developing a new Occupational Information System (OIS) to serve as the main source of occupational information for its disability adjudication process (SSA, 2018a). The OIS will include occupation-related data from multiple sources13 and will provide SSA with updated occupational information that is measured and defined in a way tailored to meet SSA’s specific program needs (SSA, 2018a). As described by SSA, “the OIS will define work as it is generally performed in the national economy; it will describe the ways in which most workers carry out the typical tasks associated with the critical functions of their occupations” (SSA, 2018a).
In 2012, SSA entered into an interagency agreement with the U.S. Bureau of Labor Statistics (BLS) to collect updated occupational information for use in the OIS (SSA, 2018a). To collect this information, BLS developed the Occupational Requirements Survey (ORS), which includes data elements that capture the physical demands and environmental conditions of work, as well as the necessary vocational preparation. Although the OIS will mirror many of the data elements from the DOT, it also will provide more detail about occupational requirements (SSA, 2018b). In addition to assigning exertional levels to occupations similar to those found in the DOT, for example, the OIS will contain information about the amount of standing or walking required by jobs and whether jobs require driving, using a keyboard, and reaching overhead (SSA, 2018b). In addition, the ORS eventually will collect data on the mental and cognitive requirements of occupations, although collection of these data elements is still being refined (SSA, 2018a).14 Some DOT elements, such as color vision and balancing, will be excluded (SSA, 2018b).
FUNCTIONAL ABILITIES RELEVANT TO WORK REQUIREMENTS
The committee’s Statement of Task (see Box 1-1 in Chapter 1) includes providing information about the assessment of physical and mental “functional abilities relevant to work requirements.” The Statement of Task specifically mentions functional abilities relevant to work requirements “as
___________________
13 Sources of data include the U.S. Bureau of Labor Statistics (BLS), O*NET, and the Military Occupational Classification.
14 The July 2017 version of the Occupation Requirements Survey (ORS) Collection Manual (DOL, 2017) included a set of “cognitive elements” that informed the committee’s writing of this report. These cognitive elements were updated subsequently in an August 2018 version of the ORS Collection Manual (DOL, 2018).
defined by the U.S. Bureau of Labor Statistics’ Occupational Requirements Survey (ORS)” and “as defined by the U.S. Department of Labor for the Occupational Information System (OIS).”
Occupational Requirements Survey (ORS) Data Elements
The data elements on physical and cognitive15 demands in the ORS make up the “functional abilities relevant to work requirements as defined by the … ORS” referred to in the committee’s Statement of Task.16 BLS defines “job demands” as “the knowledge, cognitive abilities, and physical actions required to perform critical tasks, as well as environmental conditions experienced while completing critical job tasks” (DOL, 2018, p. 6).17 Job demands include observable physical activities, such as standing, lifting, reaching, typing, and driving, as well as unobservable behaviors, such as learning and applying knowledge, perception, and problem solving (DOL, 2018, p. 6). In addition to driving, the ORS collects data on 24 physical job demands in 10 categories: sitting versus standing/walking; lifting/carrying; pushing/pulling; reaching; manipulation; keyboarding; stooping, crouching, kneeling, and crawling; climbing; speaking/hearing requirements; and vision (DOL, 2018, p. 88). The 2017 ORS Collection Manual also identifies five cognitive demand data elements: decision making, work review, pace, adaptability, and work-related personal interactions (DOL, 2017, p. 52).18 Of these, work review (i.e., the frequency with which an employee’s work is checked to ensure performance standards are being met) is not a worker characteristic or functional ability, whereas the remaining four depend on characteristics or abilities of the worker.
___________________
15 The ORS Collection Manual (DOL, 2017, 2018) uses the term “cognitive” to refer to elements the committee considers more broadly to be mental demands of work.
16 As previously noted, the committee’s work was informed by the July 2017 version of the ORS Collection Manual (DOL, 2017), which subsequently was updated in August 2018 (DOL, 2018). References to the ORS Collection Manual have been updated to the 2018 version wherever doing so would not result in a substantive change to the report text. Because the ORS cognitive elements were substantially revised, references to the 2017 ORS Manual have been retained for those elements.
17 Critical job tasks are activities “workers must perform to carry out their critical job function(s). A task is considered critical when it is a primary and required component of the critical job function(s)” (DOL, 2018, p. 3).
18 The 2018 ORS Collection Manual identifies the following cognitive elements: problem solving, work review, pace, personal contacts (verbal interactions and people skills), and interactions with the general public/crowds and telework (DOL, 2018, p. 63).
Occupational Information Network (O*NET) Data Elements
Because O*NET is an additional source of data for the OIS, the abilities captured in O*NET, as well as the data elements captured by the ORS, are relevant to the committee’s consideration of “functional abilities relevant to work requirements as defined … for the OIS.” O*NET contains occupational data organized into six domains that encompass attributes, characteristics, and requirements of occupations and workers (O*NET Resource Center, 2018b). The three job-oriented domains are occupational requirements, including work activities and work context; workforce characteristics; and occupation-specific information. The three worker-oriented domains are worker characteristics, including abilities, occupational interests, and work values and styles; worker requirements, including knowledge, skills, and education; and experience requirements, including experience and training. Of these categories, worker abilities are of particular relevance to this study. Abilities, defined as “enduring attributes of the individual that influence performance,” include cognitive, psychomotor, physical, and sensory abilities (O*NET Resource Center, 2018b).
Work Participation
The physical and mental functional abilities relevant to work requirements addressed by the committee are described in Chapters 5 and 6, respectively. It is important to note that whereas the committee’s Statement of Task focuses on the functional assessment of people, the ORS, O*NET, and ultimately the OIS contain information about the physical and mental demands of jobs. For example, while the worker abilities captured in O*NET are characteristics of people, the data collected pertain to the requirements of specific occupations in terms of which abilities are required for a given job. Although the worker abilities in O*NET and the physical and proposed cognitive demands collected in the ORS may be affected by physical or mental impairments and are to some extent amenable to functional assessment, many instruments used to assess function do not necessarily correlate with individuals’ ability to perform work-related activities.
Certain physical demands of jobs, such as sitting, standing, walking, lifting, and climbing, may correlate more directly than mental/cognitive demands with activities that are amenable to functional assessment. For example, a functional capacity evaluation can help determine an individual’s (in) ability to perform specific physical activities (e.g., sitting, standing, walking, lifting, climbing) safely, if not the ability to perform the activities on a sufficiently sustained basis to maintain work participation on a regular and continuing basis. Similarly, individuals’ visual acuity and hearing can
be measured using standardized instruments. These are among the physical activities or characteristics of individuals that may also be identified as physical demands or requirements of jobs. But the correlation between an individual’s measurable mental/cognitive abilities and, for example, the four relevant cognitive job demands defined in the ORS is less straightforward. The terms or concepts used to describe the cognitive demands of jobs differ from those typically used in the functional assessment of individuals’ mental abilities. The 2017 ORS Collection Manual specifies three levels of decision making19 and directs the collection of information on “the highest level of independent judgment a worker is expected to use to perform the critical tasks of the occupation” (DOL, 2017, p. 53). Individuals’ ability to use independent judgment as specified in the three levels of decision making defined in the ORS is not something health professionals specifically assess when they conduct cognitive assessments. Similarly, assessment of individuals’ functional abilities with respect to adaptability and work-related personal interactions is more complex than assessment of whether and how long an individual can sit, stand, or walk. The less direct the correlation between assessment measures for physical and mental functional abilities and the work requirements captured by the ORS for the OIS, the greater will be the challenge for cross-walking between the functional assessment of individuals’ abilities and the demands of jobs.
Another challenge is the extrapolation from assessment of functional abilities (“activities” in ICF parlance) to the ability to perform tasks or to meta-task as required for work participation. A person may be capable of performing each activity or even each task separately, but not be able to coordinate and sequence them together. In addition, most functional assessments capture a person’s functional abilities at a particular point in time. A person may successfully pass a variety of episodic assessments but, as discussed further below, be unable to engage in repetitive or continued performance over time. The relationship among activities, tasks, and ability to perform work is developed further in the following section.
___________________
19 “1. Employee uses independent judgment to select from a limited number of predetermined actions.… 2. Employee uses independent judgment to determine the most appropriate course of action in situations that do not have set responses.… 3. Employee uses independent judgment to make decisions by choosing from a large number of possibilities in situations where a high degree of uncertainty or complexity may exist” (DOL, 2017, p. 53).
AN ECOLOGICAL FRAMEWORK FOR FUNCTIONAL ASSESSMENT FOR WORK
Activities, Tasks, and Ability to Perform Work
Evaluation of the ability to perform a single work activity needs to be viewed with respect to the context and practical relevance of an individual’s being able to perform work and hold a job. For example, an individual might successfully pass a number of functional tests for a given, single activity, such as lifting a 10-pound box in a controlled and coached environment; however, this same individual might prove unable to engage in continued performance of this activity because of his or her health condition (e.g., cardiac condition). Environmental factors, both physical (e.g., light, noise, air quality) and organizational (e.g., work policy, psychosocial factors), also may make individuals incapable of engaging in continuous performance of work-related activities because of their heath condition. For example, an individual with multiple sclerosis may be able to do work when it is cool but unable to do it in heat (air-conditioned versus outside), or a person with significant distractibility or attention problems may be able to work in a quiet setting but not in a highly stimulating setting.
SSA is interested in an individual’s ability to perform sustained work-related physical and mental activities in a work setting on a “regular and continuing basis,” meaning 8 hours per day, 5 days per week, or an equivalent work schedule (SSA, 2018g).20 As a result, information from functional assessments needs to be considered within the context of completing a job.
Hierarchy of Job and Tasks Analyses
The hierarchy of job and task analyses, together with considerations of ergonomics and human factors, provides a framework for describing how single functional assessments fit into the context of sustained work (see Figure 2-2). Jobs are comprised of tasks, which in turn are comprised of activities. At the highest level, job analysis provides information on the overall job requirements and the work performed. The analysis creates a list of tasks that are the requirements or responsibilities for the job. These tasks are analogous to the critical job tasks identified for different occupations in the OIS. For example, the job analysis of a worker managing the drive-through window of a limited-service restaurant may list such tasks as take and enter the order of the customer, collect the items of the order, process payment for the order (cash, credit card), and deliver the order to
___________________
20 It should be noted that many jobs in reality require a longer workweek, which could affect a worker’s ability to return to his or her job at the prior level of work.
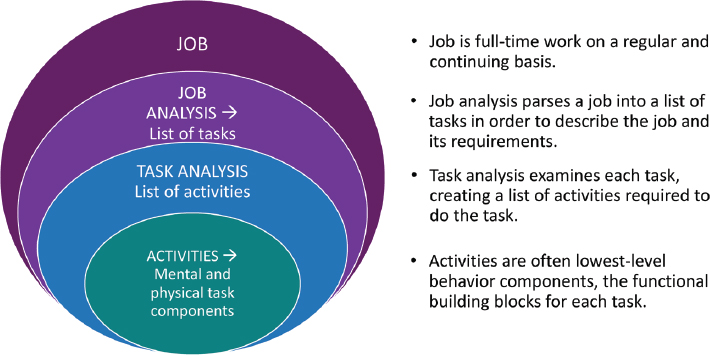
the customer.21 Task analysis then creates a list of activities (mental and physical) required to accomplish the goal of a specific task. Continuing with the above example, collecting the items of the order will include remembering the components of the order, walking to the food station (drink, sandwich, or fryer), lifting and carrying the items, and visually recognizing and inspecting the items.
Applying the International Classification of Functioning, Disability and Health (ICF) Disability Model
The concepts of the contextual factors surrounding work and the hierarchy of job and task analyses can be applied to the ICF model of functioning and disability presented earlier in Figure 2-1, providing a conceptual or ecological framework for functional assessment for work (see Figure 2-3). The framework provides a way to organize various sources of information and specific types of tools to assess function as described in subsequent chapters. As previously discussed, the major components of the ICF model include health conditions, body function and structure, and activities and participation. Within the context of the committee’s charge, the specific health conditions include back disorders, cardiac impairments, and depression, to which the committee added traumatic brain injury (see Chapter 7). The
___________________
21 A limitation of this job analysis example is that the list of tasks omits the sequencing of these tasks for each customer, that the sequence for one customer overlaps with the sequences for other customers, and that larger cognitive management tasks are involved in keeping the orders of different customers organized.
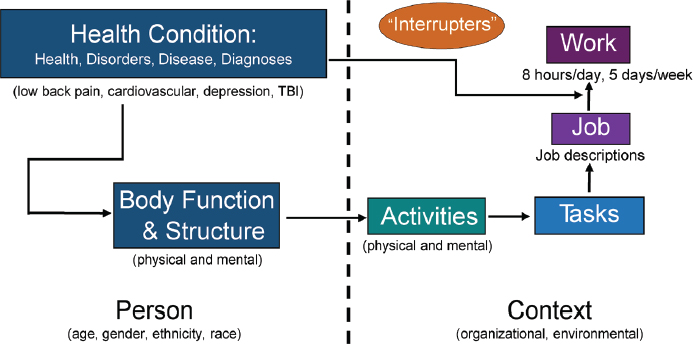
NOTES: The framework provides a structure and a hierarchy for moving from functional assessment of an individual to his or her capacity to perform work. Some components are influenced more by the person (left of the dotted line), while others are influenced more by work factors (right of the dotted line). These factors can overlap and interact. “Interrupters” are factors associated with the individual’s health condition and its treatment (e.g., medication effects, fluctuations in symptoms) that may limit his or her ability to perform work activities on a sustained basis. TBI = traumatic brain injury.
committee’s framework hence considers both mental and physical components for body function and structure and for specific work-related activities. In accordance with the hierarchy of job and task analyses discussed above, the committee added tasks—the combination of both mental and physical activities required to accomplish a specific goal (subsumed under activities in the ICF model)—as a separate component of its framework (see the further discussion below). For purposes of this report, because SSA’s focus is work disability, participation refers to participating in work and being able to hold a job (at least at the level of SGA). In turn, participating in work and being able to hold a job refer to an individual’s ability to perform sustained work-related physical and mental activities in a work setting on a “regular and continuing basis” (8 hours/day, 5 days/week [SSA, 2018g]). The arrows linking tasks to work in Figure 2-3 capture the concepts of task coordination, task sequencing, and other meta-task processes as described previously.
To capture the context of work, the committee’s framework adds the hierarchy of job and task analyses between function and work. As noted, the ICF model considers tasks to be part of activities, where activity is an individual’s execution of a task or action (Jette, 2006, 2009). However,
distinguishing task from activity may be appropriate for the work setting to accord with the functional assessment tools, as well as some of the ORS and O*NET categories. The distinction between task and activity is not absolute and mutually exclusive, however. The concepts and uses of the terms overlap throughout the literature. The two concepts do, however, provide a structure and hierarchy bridging functional assessment of an individual and his or her capacity to perform work. Table 2-1 shows the relationship among terms and concepts from the committee’s conceptual framework, SSA, and the ORS.
To further capture the context of work, specifically pertaining to the ability to perform sustained work-related physical and mental activities in a work setting on a regular and continuing basis, the framework adds “interrupters.” These are factors associated with the individual’s health condition and its treatment that interfere with the ability to perform sustained work activities on a regular and continuing basis. For example, an individual with end-stage renal disease may be quite able to perform all of the physical and mental activities and tasks associated with a job, but require dialysis treatment that interrupts his or her ability to work for 8 hours per day, 5 days per week. Other examples include medications or fluctuations in a condition that prevent or limit the ability to perform sustained work activities and tasks. Another way to think about interrupters is that the health condition and the demands of its treatment conflict with the demands of
| Conceptual Framework | Social Security Administration | Occupational Requirements Survey |
|---|---|---|
| Health condition; body function and structure | Listing of Impairments | — |
| Activities | Listing of Impairments (activity limitations) Residual functional capacity (functional abilities relevant to work requirements) | Physical and cognitive demands |
| Tasks | Ability to perform elements of a job (not observed) | Task lists (critical tasks) |
| Job/work | Ability to maintain a job at the level of substantial gainful activity or above (observed only for those that work) | Job descriptions (critical job functions) |
work. Such conflict is similar to the concept of work–family conflict,22 in which familial responsibilities conflict with and add stress to a worker’s employment. Stressors may interfere with individuals’ ability to sustain work performance especially when they lack adequate stress management skills. Similarly, the imbalance in the work–health interface resulting from an interrupter can create additional, conflicting demands and stress that limit one’s participation in sustained day-to-day work activities.
Individual and work environment factors can contribute to the associations among the framework’s components. Some components are influenced more by the person (left of the dotted line in Figure 2-3), while others are influenced more by work factors (right of the dotted line). These two sets of factors can overlap and interact—hence a dotted line. An increasing number of studies demonstrate that environmental, physical, psychosocial, and organizational factors add to the variability of a person’s capacity to participate in work (DOL, 2019; Shaw et al., 2017). Modifications to community and work environments permit work participation by many individuals who otherwise would be unable to do so (NASEM, 2017). For example, public transportation, including wheelchair-accessible buses, permit travel to work for many individuals with mobility impairments, an issue in areas where public transportation is infrequent or nonexistent (Bezyak et al., 2017). Likewise, worker adaptation programs offered by employers and employee assistance programs can help workers navigate challenges posed by their conditions and retain employment.
Conversely, an individual’s capacity to hold a particular job in one environment may not extend to the ability to hold the same job in a different environment (e.g., because of the variability in workplace or office location, company, management, and co-workers). In addition, such environmental factors can change over time within the same job. For example, an autistic individual who can successfully perform a computer programming job in one location may not be able to do so in another location where he or she finds the background noise and/or lighting distracting, or actually painful. Likewise, an individual with a respiratory condition who can successfully perform the tasks of a security guard checking IDs in the lobby of a clean office building may not be able to perform those same tasks in a factory that manufactures dusty or dirty substances that negatively affect his or her respiratory condition.
___________________
22 Work–family conflict occurs when an individual experiences incompatible demands of work and family roles, causing participation in both roles to become more difficult (Greenhaus and Beutell, 1985).
Parallels with SSA and ORS Terms and Concepts
As shown in Table 2-1, the committee’s conceptual framework has parallels in the terms used by SSA in its current approaches for assessing disability. Both health condition and body function and structure correlate with SSA’s Listing of Impairments, with many of the listings including limitations in activities along with impairment criteria (see Annex Table 2-1), as previously noted. The list of activities is associated with activity limitations in the Listing of Impairments and SSA’s assessment of RFC. The concept of tasks is related to SSA’s assessment of the capacity to perform elements of a job, which for the most part is not observed, although there may be some computer-assisted evaluations that act as proxies for work tasks. Finally, work correlates with the ability to maintain a job at the level of SGA or above, which is observed only for individuals who work.
The components of the committee’s conceptual framework also parallel components of the ORS (DOL, 2017, 2018) (see Table 2-1). Many of the cognitive and physical job demand data elements in the ORS (DOL, 2017, p. 52ff, 2018, p. 88ff) fall in the area of mental and physical activities in the framework. In addition, several of the cognitive elements, such as pace, adaptability, and personal interactions, also relate to the meta-tasking components of work.
The ORS Collection Manual describes classifying jobs according to O*NET codes and then provides task lists (DOL, 2018, p. 18ff). For example, a critical job function for a hairdresser is to provide beauty services relating to clients’ requests. The job tasks associated with this job function include shampooing, cutting, coloring, and blow drying hair for men, women, and children; recommending styling products; perming hair; waxing eyebrows and facial hair; and creating up-dos for special occasions, such as weddings or proms (DOL, 2018, p. 30). Job task lists such as this fall under the area of job descriptions in the committee’s framework.
Finally, environmental components of work, including temperature, humidity, hazardous contaminants, moving machinery and mechanical parts, heights, vibration, and noise (DOL, 2018, p. 133ff), are captured under “context” in the committee’s framework. These components are limited to the physical work environment, however, and do not encompass other environmental and organizational factors often associated with injury and disability inside or outside of the work setting (Sorensen et al., 2016).
FINDINGS AND CONCLUSIONS
Findings
2-1. Since the statutory language for the determination of disability by the U.S. Social Security Administration (SSA) was formulated, models, nomenclature, and language concerning disability have evolved, and they continue to do so.
2-2. Current models of disability, such as the International Classification of Functioning, Disability and Health (ICF) model, consider disability to involve the effects (limitations) an individual’s health condition places on his or her ability to function and participate fully in society.
2-3. SSA considers functional information at several points in the disability determination process.
2-4. Although the worker abilities in the Occupational Information Network (O*NET) and the physical and proposed cognitive demands collected in the Occupational Requirements Survey (ORS) may be affected by physical or mental impairments and are to some extent amenable to functional assessment, many instruments used to assess function do not necessarily correlate with individuals’ ability to perform work-related activities. In addition, certain physical demands of jobs, such as sitting, standing, walking, lifting, and climbing, may correlate more directly than mental/cognitive demands with activities that are amendable to functional assessment.
2-5. Assessment of individuals’ functional abilities with respect to adaptability and work-related personal interactions is more complicated than assessment of whether and how long an individual can sit, stand, or walk.
2-6. Extrapolation from assessment of functional abilities (“activities” in ICF parlance) to the ability to perform tasks or to meta-task as required for work participation is a challenge.
2-7. To capture the context of work, the committee’s conceptual framework for functional assessment for work adds the hierarchy of job and task analyses between function and work and takes account of personal and contextual (organizational and environmental) factors that influence individuals’ capacity to perform sustained work activities.
2-8. The committee’s conceptual framework includes “interrupters,” factors associated with an individual’s health condition and its treatment that limit the ability to perform sustained work activities on a regular and continuing basis.
2-9. Assessment of the capacity of an individual to work and to sustain full-time work on a regular and continuing basis encompasses many factors that often go beyond whether the person can complete specific individual physical and mental activities or tasks.
2-10. The nature of job requirements has changed over time as the types of jobs available in the national economy have evolved. The Occupational Information System currently in development for use by SSA reflects these changes in jobs and job requirements and is designed to be updated regularly.
2-11. Compared with the committee’s conceptual framework and SSA definitions, the ORS includes more detailed lists of critical tasks and job functions that go beyond impairments (body function and structure and health conditions) and activities considered in isolation.
Conclusions
2-1. In keeping with current models of disability, assessment of individuals’ functional abilities relevant to work requirements is an important part of determining whether they are able to meet workplace demands and sustain work performance on a regular and continuing basis.
2-2. The evolution of models, nomenclature, and language concerning disability since the statutory language required for use by SSA was formulated makes it difficult to reconcile differences, recognize commonalities, and integrate the conceptual changes into the disability determination process. Yet, SSA’s disability determination process includes consideration of functional information at several points.
2-3. The committee’s conceptual framework for assessing work capacity demonstrates the complexity and challenges of functional assessments, especially the use of instruments that assess only body and structure function or impairment, in extrapolating from individuals’ ability to perform specific activities and tasks to their capacity to perform work and to sustain full-time work on a regular and continuing basis.
REFERENCES
Bezyak, J. L., S. A. Sabella, and R. H. Gattis. 2017. Public transportation: An investigation of barriers for people with disabilities. Journal of Disability Policy Studies 28(1):52–60. doi: 10.1177/1044207317702070.
DOL (U.S. Department of Labor). 2017. Occupational Requirements Survey (ORS): Collection manual, 3rd ed. Washington, DC: U.S. Bureau of Labor Statistics. https://www.bls.gov/ors/about/information-for-survey-participants/pdf/occupational-requirements-surveycollection-manual-072017.pdf (accessed April 3, 2019).
DOL. 2018. Occupational Requirements Survey (ORS): Collection manual, 4th ed. https://www.bls.gov/ors/about/information-for-survey-participants/pdf/occupational-requirements-survey-collection-manual-082018.pdf (accessed April 4, 2019).
DOL. 2019. S@W/R2W research & RETAIN demonstration projects: Research & publications. https://www.dol.gov/odep/topics/SAW-RTW/research-publications.htm (accessed April 3, 2019).
GAO (U.S. General Accounting Office). 2002a. SSA and VA disability programs: Reexamination of disability criteria needed to help ensure program integrity. http://www.gao.gov/new.items/d02597.pdf (accessed April 3, 2019).
GAO. 2002b. SSA disability programs: Fully updating disability criteria has implications for program design. http://www.gao.gov/new.items/d02919t.pdf (accessed April 3, 2019).
Greenhaus, J. H., and N. J. Beutell. 1985. Sources and conflict between work and family roles. Academy of Management Review 10(1):76–88.
IOM (Institute of Medicine). 1991. Disability in America: Toward a national agenda for prevention. Washington, DC: National Academy Press.
IOM. 1998. The Social Security Administration’s decision process: A framework for research, 2nd interim report. Washington, DC: National Academy Press.
IOM. 2002. The dynamics of disability: Measuring and monitoring disability. Washington, DC: The National Academies Press.
Jette, A. M. 2006. Toward a common language for function, disability, and health. Physical Therapy 86(5):726–734.
Jette, A. M. 2009. Toward a common language of disablement. The Journals of Gerontology, Series A: Biological Sciences and Medical Sciences 64(11):1165–1168. doi: 10.1093/gerona/glp093.
Kaplan, D. 2000. The definition of disability: Perspective of the disability community. Journal of Health Care Law and Policy 3(2):352–364.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. The promise of assistive technology to enhance activity and work participation. Washington, DC: The National Academies Press.
NRC (National Research Council). 2010. A database for a changing economy: Review of the Occupational Information Network (O*NET). Washington, DC: The National Academies Press.
O*NET (Occupational Information Network) Resource Center. 2018a. About O*NET. https://www.onetcenter.org/overview.html (accessed April 3, 2019).
O*NET Resource Center. 2018b. The O*NET® content model. https://www.onetcenter.org/dl_files/ContentModel_Summary.pdf (accessed April 3, 2019).
Shaw, W., R. J. Gatchel, J. Christian, and L. Toms Barker. 2017. Improving pain management and support for workers with musculoskeletal disorders: Policies to prevent work disability and job loss, Vol. 1 – Policy Action Paper. SAW/RTW Policy Collaborative, U.S. Department of Labor, Office of Disability Employment Policy.
Social Security Advisory Board. 2001. Charting the future of Social Security’s disability programs: The need for fundamental change. http://www.ssab.gov/Details-Page/ArticleID/153/Charting-the-Future-of-Social-Securitys-Disability-Programs-The-Needfor-Fundamental-Change-January-2001 (accessed April 3, 2019).
Sorensen, G., D. L. McLellan, E. L. Sabbath, J. T. Dennerlein, E. M. Nagler, D. A. Hurtado, N. P. Pronk, and G. R. Wagner. 2016. Integrating worksite health protection and health promotion: A conceptual model for intervention and research. Preventive Medicine 91(October):188–196. doi: 10.1016/j.ypmed.2016.08.005.
SSA (U.S. Social Security Administration). 2004. Physical residual functional capacity assessment form SSA-4734-BK. https://secure.ssa.gov/apps10/poms/images/SSA4/G-SSA4734-U8-1.pdf (accessed April 3, 2019).
SSA. 2012. POMS DI 24505.001: Individual must have a medically determinable severe impairment. https://secure.ssa.gov/poms.nsf/lnx/0424505001 (accessed April 3, 2019).
SSA. 2015a. Disability report adult form SSA-3368-BK. https://www.ssa.gov/forms/ssa-3368.pdf (accessed April 3, 2019).
SSA. 2015b. Function report adult form SSA-3373-BK. https://www.ssa.gov/forms/ssa3373-bk.pdf (accessed April 3, 2019).
SSA. 2015c. POMS DI 10520.001: Impairment-Related Work Expenses (IRWE). https://secure.ssa.gov/poms.nsf/lnx/0410520001 (accessed April 3, 2019).
SSA. 2017a. Adult functional assessment in Social Security disability claims. Presentation to the Committee on Functional Assessment for Adults with Disabilities, Washington, DC, December 7.
SSA. 2017b. Listing of impairments—Adult listings (Part A). https://www.ssa.gov/disability/professionals/bluebook/AdultListings.htm (accessed April 3, 2019).
SSA. 2018a. Occupational information system project. https://www.ssa.gov/disabilityresearch/occupational_info_systems.html (accessed April 3, 2019).
SSA. 2018b. OIS project frequently asked questions. https://www.ssa.gov/disabilityresearch/ois_project_faqs.html (accessed April 3, 2019).
SSA. 2018c. POMS DI 24508.005: Impairment meets a listing. https://secure.ssa.gov/apps10/poms.nsf/lnx/0424508005 (accessed April 3, 2019).
SSA. 2018d. POMS DI 24508.010: Impairment or combination of impairments equaling a listing—Medical equivalence. https://secure.ssa.gov/apps10/poms.nsf/lnx/0424508010 (accessed April 3, 2019).
SSA. 2018e. POMS DI 24510.001: Residual functional capacity (RFC) assessment—Introduction. https://secure.ssa.gov/poms.nsf/lnx/0424510001 (accessed April 3, 2019).
SSA. 2018f. POMS DI 24510.006: Assessing residual functional capacity (RFC) in initial claims (SSR 96-8P). https://secure.ssa.gov/poms.nsf/lnx/0424510006 (accessed April 3, 2019).
SSA. 2018g. SSR 96-8P: Policy interpretation ruling Titles II and XVI: Assessing residual functional capacity in initial claims. https://www.ssa.gov/OP_Home/rulings/di/01/SSR9608-di-01.html (accessed April 3, 2019).
SSA. 2019. Substantial gainful activity. https://www.ssa.gov/oact/cola/sga.html (accessed April 3, 2019).
SSA. n.d. Mental residual functional capacity assessment form SSA-4734-F4-SUP. http://ssaconnect.com/tfiles/SSA-4734-F4-SUP.pdf (accessed April 3, 2019).
Stineman, M. G., and J. E. Streim. 2010. The biopsycho-ecological paradigm: A foundational theory for medicine. Physical Medicine and Rehabilitation 2(11):1035–1045. doi: 10.1016/j.pmrj.2010.06.013.
WHO (World Health Organization). 2001. International classification of functioning, disability and health. Geneva, Switzerland: WHO.
WHO. 2002. Towards a common language for functioning, disability and health: ICF. Geneva, Switzerland: WHO.
WHO. 2013. How to use the ICF: A practical manual for using the International Classification of Functioning, Disability and Health. Geneva, Switzerland: WHO.
| Listing | Examples of Functional Criteria |
|---|---|
| Listing 1.00 Musculoskeletal System |
Examples of Functional Criteria
|
| 2.00 Special Senses and Speech |
|
| 4.00 Cardiovascular System |
|
| 7.00 Hematological Disorders |
|
| 8.00 Skin Disorders |
|
| 10.00 Congenital Disorders That Affect Multiple Body Systems |
|
| 11.00 Neurological Disorders |
|
| 12.00 Mental Disorders |
|
| Listing | Examples of Functional Criteria |
|---|---|
| 14.00 Immune System Disorders |
|
SOURCE: SSA, 2017b.
























