In response to a mandate of the 2010 Patient Protection and Affordable Care Act, the National Institutes of Health (NIH) asked the Institute of Medicine (IOM) to examine the state of the science regarding pain research, care, and education, which led to the 2011 IOM report Relieving Pain in America (IOM, 2011b). One of the outcomes of that report was the development of a National Pain Strategy1 and the creation of the Interagency Pain Research Coordinating Committee (IPRCC).2 In 2016, the U.S. Food and Drug Administration asked the National Academies to provide an update on the science of pain research, care, and education; characterize the opioid epidemic and evidence on strategies to address it; and identify actions and research questions needed to respond to the epidemic since publication of the 2011 IOM report. In response to this request, the National Academies published the report Pain Management and the Opioid Epidemic: Balancing Societal and Individual Benefits and Risks of Prescription Opioid Use (NASEM, 2017).
The focus on pain at the federal level has resulted in many initiatives aimed at supporting research to advance pain management and combat the opioid epidemic. Several participants at the workshop highlighted many of these efforts.
___________________
1 For more information about the National Pain Strategy, see https://iprcc.nih.gov/sites/default/files/HHSNational_Pain_Strategy_508C.pdf (accessed February 6, 2019).
2 For more information on IPRCC, see https://iprcc.nih.gov (accessed February 6, 2019).
NIH HEAL INITIATIVE
The NIH HEAL (Helping to End Addiction Long-TermSM) Initiative3 was launched in 2018 as a transagency effort to accelerate scientific efforts aimed at addressing the opioid crisis, said Linda Porter, director of pain policy and planning at the National Institute of Neurological Disorders and Stroke (NINDS). According to David Shurtleff, deputy director of the National Center for Complementary and Integrative Health (NCCIH), a portion of the HEAL Initiative is an offshoot of the NIH Health Care Systems Research Collaboratory,4 a program established in 2012 to engage health care delivery organizations as research partners in pragmatic and implementation studies (see Figure 5-1). The Collaboratory’s experience in conducting clinical trials allowed NIH to move forward with the HEAL Pragmatic and Implementation Studies for the Management of Pain (PRISM) to reduce opioid prescribing. These projects must be embedded in health care systems and are supported by a coordinating center that helps them design studies and reach milestones, said Shurtleff. They address three key issues: (1) systems change to improve adherence to evidence-based guidelines for pain management; (2) integration of evidence-based approaches for pain management into health systems; and (3) informing national coverage determination decisions through partnerships with the Centers for Medicare & Medicaid Services.
The HEAL Initiative is divided into two components: First, to develop and implement therapies for opioid use disorders, including a focus on neonatal opioid withdrawal; and second, to better understand the neurobiology of pain and accelerate development of new approaches to treat both acute and chronic pain, said Porter. On the pain side, the HEAL Initiative has devoted resources to build infrastructure and incentivize partners to develop new analgesics, including small molecules, natural products, biologics, and devices. This infrastructure will include human- and animal-based tissue screening platforms to support early-stage drug development; new and refined animal models that better reflect the human condition; and clinical research networks to support clinical trials, said Porter. Biomarker discovery and validation will be woven throughout all HEAL programs on
___________________
3 For more information on the NIH HEAL Initiative, see https://www.nih.gov/research-training/medical-research-initiatives/heal-initiative (accessed February 6, 2019).
4 For more information on the NIH Collaboratory, see http://rethinkingclinicaltrials.org (accessed February 6, 2019).
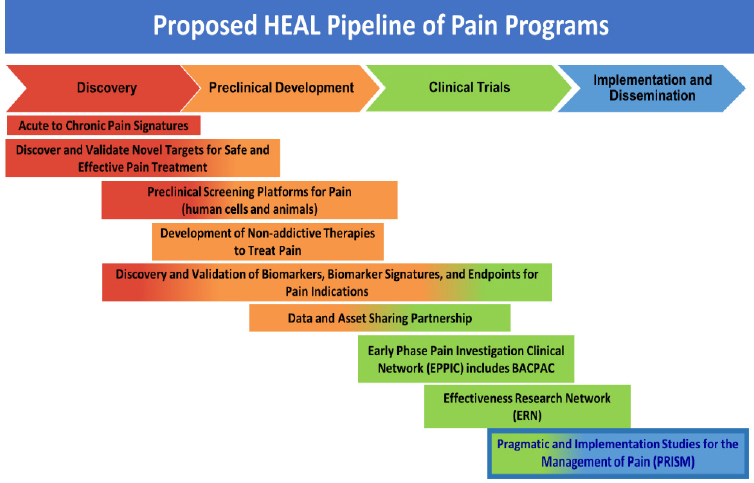
SOURCE: Presented by David Shurtleff, December 4, 2018.
both the pain and addiction sides, she added, noting that biomarkers will be defined broadly to include anything from phenotypic characteristics to blood biomarkers and predictive signatures. A Common Fund program to identify signatures of the transition from acute to chronic pain5 is included as part of the HEAL Initiative.
Porter mentioned two other consortia relevant to the workshop discussions that are folded into the HEAL Initiative: The NIH Back Pain Consortium (BACPAC)6 and the Pain Management Effectiveness Research
___________________
5 For more information on the Acute to Chronic Pain Signatures (A2CPS) program, see https://www.nih.gov/news-events/news-releases/nih-research-program-explore-transition-acute-chronic-pain (accessed February 6, 2019).
6 For more information on the NIH Back Pain Research Consortium (BACPAC), see https://www.niams.nih.gov/grants-funding/funded-research/nih-back-pain-consortium-bacpac-research-program (accessed February 6, 2019).
Network (ERN).7 She said BACPAC will provide opportunities to look at integrative care, while the Pain Management ERN will support comparative effectiveness research trials for many different modalities, including nonpharmacological therapies.
National Center for Complementary and Integrative Health
NCCIH plays a prominent role in the pragmatic aspects of the HEAL Initiative, said Shurtleff. He described a clinical research pipeline that funds studies across the continuum from basic and mechanistic work through translational research, intervention, refinement, and optimization; efficacy and effectiveness; and pragmatic studies and dissemination. These studies are designed to elucidate how natural products and mind–body treatments work, whether the impact can be measured reliably in humans, what modifications might enhance impact adherence, how treatment effectiveness compares with other treatments or controls, and how effective the treatment is likely to be in real-world conditions. Shurtleff added that natural products account for about half of the NCCIH research investment.
Wendy Weber, branch chief for clinical research in the Complementary and Integrative Health Branch, Division of Extramural Research at NCCIH, mentioned a forthcoming Request for Applications that has since been announced, specifically calling for research studies within health systems that will test different models to determine how best to change care to better adhere to the current guidelines, implement services, and overcome access barriers.8
NIH Pain Management Collaboratory
The Pain Management Collaboratory9 is a partnership among NIH, the Department of Defense (DoD), and the Department of Veterans Affairs (VA) that supports pain-focused pragmatic clinical trials of nonpharmacological approaches embedded in the VA and military health systems, said
___________________
7 For more information on the NIH HEAL Pain Management Effectiveness Research Network, see https://painconsortium.nih.gov/Funding_Research/NIH-HEAL-Effectiveness-Research-Program-Pain (accessed February 6, 2019).
8 For more information on the RFAs associated with PRISM, see httpts://nccih.nih.gov/grants/heal (accessed February 13, 2018).
9 For more information on the Pain Management Collaboratory, see https://painmanagementcollaboratory.org (accessed February 6, 2019).
Robert Kerns. Shurtleff said they have successfully launched 11 demonstration projects and are looking ahead to how they will implement new treatment approaches into care when and if they demonstrate effectiveness.
Kerns noted that they have encountered a challenge related to the capacity for conducting this kind of research in primary care settings within a large, integrated health system like the VA. Given the many competing demands in these settings, organizational leaders, leaders in the primary care setting, or clinicians and staff do not necessarily consider research a priority, he said. Patient and clinician education and messaging will be key factors to spark the interest of practicing clinicians and increase the likelihood that they will stay engaged with this research, Kerns added. Access issues add to the difficulty of designing pragmatic trials in many of these health systems as well, said Fritz.
Office of Behavioral and Social Science Research
The NIH Office of Behavioral and Social Science Research (OBSSR)10 was created by Congress in recognition of the importance of behavioral and social sciences to the NIH mission. OBSSR was created more than 20 years ago to encourage the advancement and coordination of behavioral and social sciences research at NIH. The current OBSSR strategic priorities include increasing the synergy between basic and applied research; enhancing the methods, measures, and data infrastructures to encourage a more cumulative “behavioral and social sciences; and facilitating the adoption of behavioral and social sciences research findings in health research and practice.” OBSSR also helps to encourage and support the integration of behavioral and social sciences into trans-NIH activities, including those addressing the opioid and pain crises; to communicate with various stakeholders about behavioral and social sciences research, said Wendy B. Smith, associate director of OBSSR. For example, in 2018 as part of the NIH Cutting Edge Series to Combat the Opioid Crisis, OBSSR help lead the coordination of a meeting in collaboration with the National Institute on Drug Abuse (NIDA), NCCIH, NINDS, and the National Institute on Minority Health and Disparities that invited experts with a wide variety of experience and expertise to identify social and behavioral research contributions and priorities to help address the opioid and pain
___________________
10 For more information about OBSSR, including funding opportunities, see https://obssr.od.nih.gov (accessed February 6, 2019).
crises, said Smith. This meeting included a panel focused on incorporating nonpharmacological approaches for the treatment of opioid abuse and chronic pain management and included discussions about the importance of both implementing these new methods as well as de-implementing methods that are not found to be effective.11 To address the objectives of the OBSSR strategic priorities, the central functions of the Office include focusing on communicating results, coordinating efforts across institutes and centers, training the next generation of behavioral and social scientists, shaping scientific policies and procedures to facilitate the OBSSR agenda, and conducting evaluation activities that help address important research gaps and track progress, Smith added.
National Center for Medical Rehabilitation Research
Within the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the National Center for Medical Rehabilitation Research (NCMRR)12 funds rehabilitation research and coordinates related efforts across NIH and other federal agencies, said Alison Cernich, director of NCMRR. People with disabilities are often prescribed opioids for pain and are at higher risk for chronic pain due to inactivity, inability to move certain body parts, spasticity, and contractures, she said. Thus, NCMRR’s research funding priorities include examining how people adapt to disability by using devices and technologies that enhance function, manage chronic pain, and access effective nonpharmacological treatments for pain such as fitness facilities. As an example of the importance of this research, Cernich noted that recent surveys indicate that 78 to 80 percent of fitness facilities lack access for people with disabilities, which not only prevents them from gaining the benefits of nonpharmacological and multimodal approaches to pain management, but also leads to social isolation. NCMRR also supports research aimed at identifying objective and real-world measures of pain and function, developing multimodal approaches to managing pain and disability, and promoting the continued effective treatment of pain when children make the transition to adult care, said Cernich.
___________________
11 For a summary of the OBSSR meeting Contributions of Social and Behavioral Research in Addressing the Opioid Crisis, see https://www.nih.gov/heal-initiative/full-summary-contributions-social-behavioral-research-addressing-opioid-crisis (accessed February 6, 2019).
12 For more information about NCMRR, including funding opportunities, see https://www.nichd.nih.gov/about/org/ncmrr (accessed February 6, 2019).
PATIENT-CENTERED OUTCOMES RESEARCH INSTITUTE
The Patient-Centered Outcomes Research Institute (PCORI)13 was created in 2010 to fund comparative clinical effectiveness research guided by and using data obtained from patients, caregivers, and the broader health care community, said Christine Goertz, chief operating officer of the Spine Institute for Quality and vice chair of the PCORI Board of Governors. PCORI also is mandated to provide the public, patients, and clinicians with information about the evidence gathered in funded studies and implementing the results of their research, said Goertz.
PCORI has had two major initiatives focused on nonopioid treatment options, the prevention of unsafe prescribing, and the management of long-term prescription opioid use. As of November 2018, Goertz said PCORI had awarded nearly $94 million to fund comparative effectiveness research studies on managing or treating noncancer pain, including the use of nonpharmacological therapies such as CBT, physical therapy, manual therapy, exercise, mindfulness, and acupuncture as well as education, self-management, and system-level interventions such as integrative care coordination.
DEPARTMENT OF VETERANS AFFAIRS
The VA manages the largest federal health system in the United States, providing integrated care to 6 million patients each year at more than 160 hospitals and more than 1,000 other care sites, said David Atkins. He added that because both chronic pain and opioid use are higher in military veterans than in other population groups, the VA is a good place to study pain care; for a large organization such as the VA, the biggest challenges is how to deliver evidence-based and patient-centered multimodal care in a reliable, scalable, accountable, and affordable way.
Nonetheless, progress has been made, said Atkins. As of 2015, 93 percent of VA medical centers offer at least two CIH modalities, he said, noting that chiropractic care has been standard in the VA for more than a decade. Massage and mindfulness approaches are also widely used by vet-
___________________
13 For more information about PCORI, including funding opportunities, see https://www.pcori.org (accessed February 6, 2019).
erans, who have a high burden of comorbid mental health disorders, substance abuse, and social isolation—all factors that can influence the pain experience, said Atkins.
In fiscal year 2018, the VA research portfolio consisted of 151 projects, including studies exploring nonpharmacological approaches such as biobehavioral, technology, activity, and CIH-based interventions. Atkins said that evidence gaps remain, particularly with regard to delivering these interventions across a broad organization, identifying well-qualified providers, implementing multimodal care in a primary care setting, and demonstrating both effectiveness and cost-effectiveness of different therapies.
DEPARTMENT OF DEFENSE
The DoD military health system, which provides cradle-to-grave care for 9.5 million beneficiaries, including combat and noncombat personnel, families, and retirees, also funds and conducts research and develops and implements policies, according to Eric Schoomaker, Lieutenant General, U.S. Army (retired) and former U.S. Army Surgeon General and Commanding General of the U.S. Army Medical Command. DoD research initiatives and priorities related to pain management focus on translating and implementing evidence-based and effective care into practice and tackling opioid overuse and misuse while recognizing the need for opioids in combat settings, he said. Indeed, Schoomaker suggested that the shift in focus from pain to opioids over the past few years may need rethinking because more than 75 percent of patients with opioid use disorder start with problems in pain management. He noted that DoD initiatives must align with other federal agencies, especially the VA.
Schoomaker referenced the 2010 DoD published task force report that recommended a comprehensive pain management strategy, citing good evidence of effectiveness for CIH modalities, especially yoga and tai chi.14 He questioned why payers are still debating whether these modalities should be covered and why the provider community has not embraced them, especially in light of the cumulative evidence of their effectiveness (as discussed in Chapter 3), the absence of evidence for effectiveness for the most commonly used therapy for chronic pain—chronic opioids—and
___________________
14 To read the Office of the Army Surgeon General’s Pain Management Task Force report, see http://www.dvcipm.org/site/assets/files/1070/pain-task-force-final-report-may-2010.pdf (accessed February 6, 2019).
the relative safety of CIH while opioid use, misuse, and diversion have spawned an unprecedented national public health crisis (further explored in Chapter 7). Schoomaker added that since the task force report was published, DoD has recognized acupuncture, biofeedback, meditation, music therapy, mindfulness meditation, medical massage, and chiropractic as evidence-based complementary and alternative therapeutic modes.










