4
The Role of Health Care in Developing the Health Workforce
Warren Newton, the forum representative from the American Board of Family Medicine, opened the session on health care’s role in developing its workforce by saying, “The pace of change and the amplitude of change in health care is stunning.” He continued by describing changes in health care organizations, including the shift toward pay-for-value and population health, that are dramatically changing the requirements of tomorrow’s workforce. Although these changes are already under way, said Newton, most health system leaders have been focusing largely on finance and
governance, rather than workforce issues. This provides an opportunity for health education professionals to “manage up,” informing health system leadership about how to best educate and prepare the clinicians needed to support new systems of care. With new competencies, and new professions being formed (e.g., interprofessional practice, practice facilitators, community health workers), he said, educational institutions should “put their heads to the ground, hear the footsteps, and try to produce what will be needed as their graduates” look to the future. Education needs to adapt to not just what the market is, but to what it will be; there needs to be continuous dialogue between the workplace and education in order to facilitate these changes. With this in mind, Newton introduced speakers who would discuss how practice and academia can work together on workforce issues.
INTERPROFESSIONAL DEDICATED EDUCATION UNITS
Guardia Banister, executive director of the Institute for Patient Care at Massachusetts General Hospital (MGH), and Mary Knab, director of impact practice at MGH Institute of Health Professions (IHP), spoke together about an innovative collaboration between their institutions called Interprofessional Dedicated Education Units (IPDEUs). Banister echoed what other speakers had said about the ongoing changes in the health care system: the population is growing older, patients are becoming more complex, there is a documented failure to adequately treat pain, and there is a shift toward a value-based payment system. While there are transitions toward ambulatory and in-home care, said Banister, it is important to remember that “acute care is not going to go away.” There will always be critically ill patients who require an intensive level of care, she said, and there is a need for providers who are able to take care of these patients and their families. Another shift, said Banister, is toward recognizing the diversity among and number of providers who take care of patients (see Figure 4-1). There are many different disciplines involved in taking care of a patient, she said, and it is critical that these professionals work collaboratively.
Banister described how the IPDEU program got its start and how it evolved over time. The first iteration of the program, called “IPDEU 1.0,” had student pairs from different professions spend 1 half day each week for one semester focusing on interprofessional collaborative practice and their own disciplinary knowledge. Frontline clinicians served as clinical instructors with Banister noting that, because these clinicians were delivering care every day, “they were current in terms of their knowledge and their preparation.” The clinicians included nurses, occupational therapists (OTs), physical therapists (PTs), and speech-language pathologists (SLPs). There were also clinical faculty coordinators (CFCs) who acted as bridges between the academic and practice environments. The CFCs coordinated
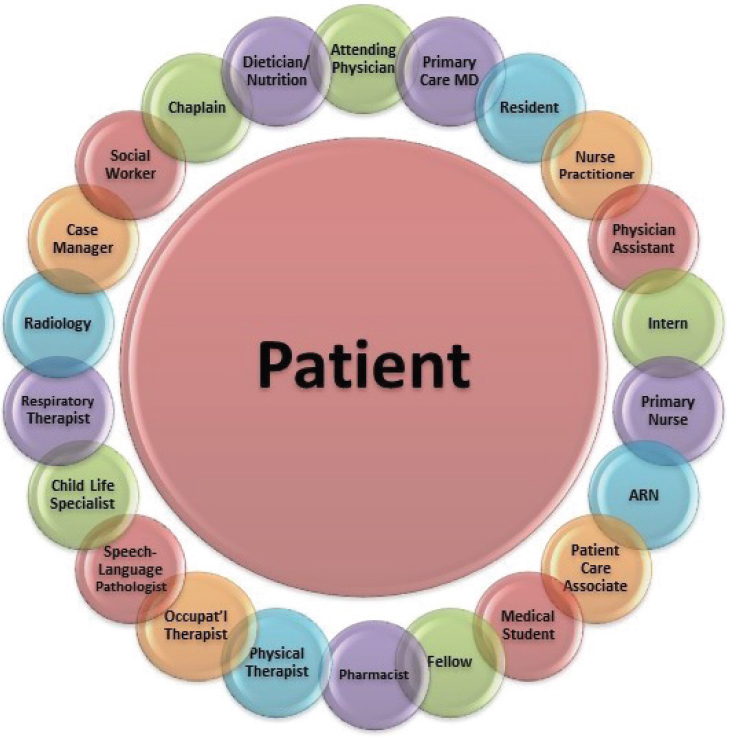
NOTE: ARN = Association of Rehabilitation Nurses.
SOURCE: Presented by Banister and Knab, November 13, 2018.
all aspects of the program, including facilitation of end-of-day debriefing sessions in which the students and clinical instructors discussed their experiences. Unfortunately, said Banister, it quickly became apparent that this model was unsustainable: The logistics were complicated, the program needed additional staff to be successful, and only 12 students per semester could participate. In addition, she said, while comfortable with clinical teaching in general, the clinical instructors were frustrated by the pressures of trying to teach both discipline-specific information as well as interprofessional collaborative practice to students from their own and other professions.
Knab said there was great potential in the program despite these challenges, so the team decided to revamp the model. The new program, “IPDEU 2.0,” was entirely focused on the interprofessional aspects of care delivery. The time commitment for the program was also shortened, meeting only 2 half days over 2 weeks. Interprofessional student dyads spend 1 half day with an instructor from nursing, and the other with an OT, PT, or SLP. Clinical instructors were renamed interprofessional practice instructors (IPIs), and their role was redefined to have a sole focus on teaching interprofessional collaborative practice. During the 1 half-day session, said Knab, IPIs saw their normal caseload and engaged students in active observation and discussion, highlighting their collaborations with other care team members. Each session ended with a wrap-up debrief. These changes to the program, said Knab, made it scalable and sustainable. Each semester, approximately 144 students go through the program, involving 3 acute care units (2 medical units and 1 cardiac stepdown unit). The program can be scaled up further by adding other units or days of the week.
This project, said Banister, is “truly an academic–practice partnership,” and a team effort. Knab said IPDEU is “one of those gems that really functions at that nexus of academia and practice” and that part of the reason is a shared commitment (at all levels) to exemplary practice and student success. Clinical faculty coordinators actively bridge practice and education, educate and support the IPIs, and are “on the front lines” while the IPDEU experience is in progress. Knab noted that simply placing students in clinical settings does not equate to a true academic–practice partnership. A true partnership, she said, requires building a relationship based on shared values and a shared commitment, as well as involvement from leaders at all levels. IPDEU uses a shared resource model in which both the MGH and the IHP bear some costs for the programs. Everyone involved, from deans to unit directors, is invested in the program and is actively involved in making it work for all stakeholders. The most important stakeholders, Knab stressed, are the patients and their families.
The IPDEU program has impacted not just the students, Knab explained, but also the clinicians and patients involved. Students have described how the program helped them learn to be “compassionate with patients and advocate for them” and also how it improved their understanding of interprofessional team interactions in patient care. Instructors, said Knab, are making changes in their own practices based on their experiences in the IPDEU program. While acting as IPIs, clinicians emphasize the importance of interprofessional collaboration and seek to demonstrate its value in care delivery. Knab described one such instructor as saying, “I noticed [my] increased emphasis on persistence and follow-through surrounding interprofessional [teamwork] in my personal practice.” She further illustrated similar stories from other clinicians, indicating that instructors
are “carrying this culture, carrying these values, and making [them] visible in ways that go well beyond” the program itself. Banister added that such changes to practice impact patients, as well; for example, a provider who has been working on an interprofessional team may notice that a patient would benefit from a consultation with a different type of provider (e.g., respiratory therapist) and would then help make that connection. Maria Tassone with the University of Toronto Centre for Interprofessional Education remarked on these benefits to providers and patients as demonstrating the value of having students in the practice environment, while adding that this is an “important key message that we need to be sharing.”
Catherine Grus, representing the American Psychological Association, asked Banister and Knab how they are helping others duplicate the model they created. Banister replied that they have a three-pronged approach for spreading the word about the model. First, they present the model in forums, conferences, and symposiums. This has encouraged others to try it. Banister noted that their model is “not perfect” and encouraged people who implement the program to adapt it to their own cultures and environments. Second, the team has compiled a manuscript describing details of the program, which is under peer review for publication so that it can be shared with a wider audience. Third, said Knab, they are working with the National Center to consider a collaboration on outcomes research documenting the impact of the IPDEU model.
The next question was asked by Susan Skochelak, representing the American Medical Association, who asked Banister and Knab about their hopes for students participating in the IPDEU program. Knab expressed her opinion of wanting students to have “light bulb” moments and to realize that even the best provider needs to work as part of a team in order to fully meet patients’ needs. She added that although the IPDEU experience is short, she hoped students would take what they had learned into their other clinical experiences and always keep “an eye toward … interprofessional aspects of care delivery.”
CVS WORKFORCE INITIATIVES
CVS Health, said its Manager of Workforce Initiatives, Charnetia Young, is more than just a retail pharmacy. CVS Health has more than 250,000 employees (who work in every state except Wyoming) and covers a gamut of health care industries such as retail pharmacy, mail order pharmacy, prescription drug insurance, retail clinics, long-term care, and home infusion therapy. Because of this diversity of health care services, said Young, CVS Health employs a significant number of health care professionals. For example, CVS is one of the largest employers of nurse practitioners and registered nurses (RNs) in the United States.
As CVS Health expands its scope of health services, said Young, changes in the health care landscape have created challenges for it. First, health professionals are increasingly expanding their roles and practicing at the top of their licenses. This change is partly due to a shortage of professionals, said Young; when there is a shortage of RNs, licensed practical nurses are employed to fill the gap. Second, there is a low unemployment rate currently. For a company like CVS that needs to hire more people, said Young, this means that available workers are either individuals who have been out of the workforce or individuals with significant barriers to employment. Third, education and training programs often do not meet the needs of business. CVS has employed its own methods to train professionals both for the jobs of today and the jobs of the future. Young noted that employers often feel as if students are unprepared to enter the workforce for a number of reasons. Students might be lacking soft or hard skills. They might be trained on brand new technologies that businesses are not using yet. Young also said that educational institutions tend to change more slowly, whereas CVS can “pivot quickly” to change training curricula when the needs of the business change; and that “fail fast and fail cheap” is a motto they believe in. Finally, she said, there is a need for increasingly diverse talent to treat an increasingly diverse patient population. Because patients may be more comfortable with providers who are similar to them, “the more diverse the workforce is, the better off an employer will be.”
The workforce initiatives department at CVS, said Young, works with more than 1,200 partners across the United States in order to recruit, train, and support its health care workforce. Young cited the reason for this program as “We need a workforce and it’s not out there, so we’ve got to build it.” The department runs a number of programs, which include apprenticeships, externships, internships, mock store training, incumbent worker training, and on-the-job training. Through these types of programs, said Young, the department has made a significant impact, as demonstrated through these numbers:
- 20,000 youth per year are hired for summer programs
- 20 percent of CVS employees are “mature workers” over age 50
- 35,000 associates per year are trained at CVS regional learning centers
- 8,000 plus registered apprenticeships
- 1,000,000 youth have been exposed to the Pathways to Pharmacy careers program
- 110,000 people have transitioned off of public assistance and into careers with CVS Health
Young noted that these programs and achievements, particularly the transitioning of people off of public assistance, would not be possible without assistance from CVS’s 1,200 partners, who help ensure wraparound and supportive services.
Lisa Howley, representing the Association of American Medical Colleges, asked Young about the clinical training experiences CVS offers for students. Young said these programs are the “bread and butter” of talent recruitment, and that there are benefits for both the students and for CVS. First, she said, clinical training allows a student “to see if this is an environment they would like to be in.” She noted that many students have a bias against working in retail clinics or retail pharmacies, but getting them in the door allows them to see the extent of the services offered and the impact they are making on the community. Second, the clinical programs allow CVS to evaluate whether a student is an appropriate fit or ready for the particular environment, and to identify gaps that may need to be filled. For example, the pharmacy clinical rotation program exposes students to different experiences over the course of 4 years. Upon graduation, the student receives a job offer. Young noted that this allows CVS “to address gaps earlier while they are still students and they are still in a learning framework.” Young discussed other training opportunities at CVS, including initial job training and continuing education and development. CVS also offers employees assistance with additional education, such as providing support for clinicians seeking their M.B.A. degrees.
Gerri Lamb with Arizona State University asked Young if CVS has worked with academic organizations to better align the needs of the business with the training of their students and, if not, what it would take to do that. Young responded that CVS has had success in increasing the skill competencies of pharmacists. She noted that it was “a little easier to move the needle” because CVS employs so many pharmacists: “When you’re the largest employer of pharmacists in the U.S. and you say that something needs to change—and I hire 70 percent of all your students at every school across the country—you change, right?” With other clinician groups, she said, it is not quite as easy to impact education and training. Young said that CVS wants to collaborate with academia in order to ensure that CVS’s voice is heard and to help identify the gaps between academia and practice.
Frank Ascione, who represents the University of Michigan on the forum, asked Young to elaborate on how CVS—a for-profit organization—affects the CVS health care model. Young said “businesses have to be profitable” or they cannot continue offering products and services. As a result, clinicians who run programs within CVS have to be competent in patient care, increasing profits and decreasing costs. CVS’s goals, said Young, are to “reduce cost, increase quality, and improve access,” adding that these goals must be pursued while also keeping the bottom line in mind.
This page intentionally left blank.








