Summary
ABSTRACT
Health inequities have persisted in the United States, and the factors that drive these inequities from preconception through early childhood are complex, interconnected, and systemic; they result from exposures and experiences that children and families encounter throughout their lives and across multiple generations. These exposures accumulate over the life course to exert a cumulative effect on health that is probabilistic, not deterministic. That is, the odds of good health are never fixed; individual exposures, experiences, and choices help set and adjust them over time. Specific subgroups of the population have varying rates of exposure to positive and negative experiences that shape choices and opportunities throughout the life course; therefore, from the very beginning, certain groups have different odds for good or poor health outcomes. Among the factors that may buffer negative outcomes in the early childhood period, supportive relationships between children and the adults in their lives are essential. Furthermore, reducing health disparities by addressing root causes, such as poverty and racism, is foundational to advance health equity.
Biologically, a number of critical systems develop in the prenatal through early childhood periods, and neurobiological development is extremely responsive to environmental influences during these stages. This report provides an overview of the core concepts of brain development and other body systems relevant to understanding the impact of early life adversity, including the mechanisms that link early life experiences to later outcomes. This information can be used by the public and policy makers to better inform effective actions for advancing health equity.
The committee provides both short- and long-term recommendations in several key areas that can be leveraged to improve health outcomes for children and families. Recommendations aimed at supporting caregivers include implementing paid parental leave and strengthening and expanding home visiting programs. Recommendations for creating supportive and stable early living conditions include improving economic security through increases in resources available to families to meet their basic needs; increasing the supply of high-quality affordable housing; and supporting and enforcing efforts to prevent and mitigate the impact of environmental toxicants. To maximize the potential of early care and education (ECE) to promote better health outcomes, the committee recommends developing a comprehensive approach to school readiness that explicitly incorporates health outcomes, developing and strengthening curricula that focus on key competencies of educators, and improving the quality of ECE programs and expanding access to comprehensive high-quality and affordable ECE programs. The committee recommends leveraging the health care system to make care in the preconception through early childhood periods more continuous, equitable, integrative, and comprehensive by transforming services to apply a life course perspective and address the social, economic, cultural, and environmental determinants of health. To mitigate the early life drivers of health inequities, there is no one-sector solution—the complex and interconnected root causes call for coordination across multiple sectors. Therefore, the committee provides recommendations for sector alignment and collaboration, as well as the need for child- and family-serving sectors to enhance detection of early life adversity, improve response systems, and develop trauma-informed approaches.
The committee identifies knowledge gaps and recommends multidisciplinary research efforts to bring new ideas and practical approaches to advance efforts to achieve health equity. However, substantial advances in knowledge in the past 20 years make it clear that policy makers, health providers, business leaders, and others in the public and private sectors do not need to wait any longer to take action.
Health inequities by race, ethnicity, socioeconomic status, geography, and other important demographic characteristics have persisted in the United States despite increasing evidence about their contributions to poor health. Research shows that exposures to factors that shape health trajectories can start early and are multigenerational; thus, the preconception, prenatal, and early childhood periods are critical to setting the odds for lifelong health. Importantly, science can inform actions in policy and practice to advance health equity1 and reduce health disparities.
___________________
1 Health equity is the state in which everyone has the opportunity to attain full health potential and no one is disadvantaged from achieving this potential because of social position or any other socially defined circumstance.
Neurobiological and socio-behavioral research indicate that early life experiences shape prenatal and early childhood development, and these experiences have a powerful impact on the developing brain and peripheral organ systems that impact health outcomes across the life course.
When different groups vary in their exposures to key experiences (both positive and negative), their odds for positive health diverge systematically over time, producing disparities in health outcomes across the life-span and across generations. These exposures accumulate over the life course to exert a cumulative effect on health that is probabilistic, not deterministic. That is, the odds of positive or negative health are never fixed; individual exposures, experiences, resilience, and choices help set and adjust them over time. Individuals’ distinct contexts also shape their choices and opportunities, and thus they have different odds of experiencing positive or negative health outcomes over time. Because the odds of these exposures are affected by policies and systems, advancing health equity will require more than individual-level interventions. It will necessitate systems-level changes, including changes to laws and policies and investment of resources, to improve the odds of positive experiences and reduce the odds of adverse exposures for all populations, especially those experiencing the most adversity.
Scientific evidence shows that prevention and early intervention are effective for children on at-risk developmental trajectories. Recent advances in science, technology, data sharing, and cross-disciplinary collaboration present opportunities to apply this emerging knowledge systematically to practice, policy, and systems changes. Given the burgeoning science available to advance health equity during early development, the Robert Wood Johnson Foundation, as part of its Culture of Health Initiative, asked the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine to
- Provide a brief overview of stressors that affect prenatal through early childhood development and health;
- Identify promising models and opportunities for translation of the science to action;
- Identify outcome measures to enable subgroup analyses;
- Develop a roadmap to apply the science to tailored interventions (i.e., policies, programs, or system changes) based on biological, social, environmental, economic, and cultural needs; and
- Provide recommendations in these areas, including how systems can better align to advance health equity.
To respond to this charge, the Committee on Applying Neurobiological and Socio-Behavioral Sciences from Prenatal Through Early Childhood
Development: A Health Equity Approach was formed. The committee applied a health equity frame and built on the concepts of the 2017 report Communities in Action: Pathways to Health Equity. As identified in the 2000 National Research Council and Institute of Medicine report From Neurons to Neighborhoods: The Science of Early Childhood Development, prenatal through early childhood are critical phases of development that have lifelong impacts on health and well-being. This report reviews the science that has emerged since that landmark report.
The health of both men and women before they have children is important for not only pregnancy outcomes, but also the lifelong health of their children; thus, the committee included the preconception period as an important focus of the report. The committee also adopted the life course approach to its work because an individual’s health status and outcomes reflect the accumulation of experiences over the life-span. This approach takes into account an individual’s larger social, economic, and cultural context and acknowledges that the life trajectory may be changed, negatively or positively, through interactions between the brain, body, and environment. Protective factors (such as stable, high-quality caregiver relationships and economic security) support positive, or flourishing, trajectories; risk factors (such as exposure to abuse, neglect, or racism) exacerbate the likelihood of poor trajectories.
Children in the United States may be perceived to be healthier now than in the past because they are much less likely to encounter the major infections and debilitating diseases of past generations and are typically able to recover fully from “acute” childhood illnesses. However, ailments of the past have been supplanted with chronic physical (e.g., diabetes, asthma, obesity) and socio-emotional (e.g., depression, anxiety) conditions, with large subsets of U.S. children facing barriers to positive mental and physical health and well-being as a result of poverty, food insecurity, unsafe or unstable housing, neighborhood segregation, and other substantial adversities (such as adverse childhood experiences) in the first few years of life.
Children who are born and raised in poverty are at particularly high risk for poor health outcomes, more problems in early development (e.g., lack of readiness for school at age 5, diagnoses of developmental delays and/or disorders), and higher rates of most childhood chronic conditions (such as mental illness, developmental disabilities, obesity, and asthma). Early adverse experiences may have intermediate effects on school readiness, weight, and physical and/or mental well-being and contribute to chronic disease and poor functioning in adulthood. In fact, these impacts are cumulative, and adults who experience adversity in childhood have substantially higher rates of heart disease, lung disease, metabolic syndrome, and other costly health conditions.
CONCEPTUAL MODEL
The committee’s conceptual model (see Figure S-1) served as a unifying framework for its approach to this report. It is important to note that risk and protective factors can be transferred intergenerationally, which makes parents and other family and community primary caregivers a central focus of interventions to improve child health. Within the context of the life course, the diagram’s nested circles illustrate the complex sociocultural environment that shapes development at the individual level and the opportunities for interventions to improve individual health and developmental outcomes, as well as population health, well-being, and health equity. Individual social and biological mechanisms and culture operate and interact within and across the three levels.
Structural inequities operate at the outer level, the “socioeconomic and political drivers.” Structural inequities are deeply embedded in policies, laws, governance, and culture; they organize the distribution of power and resources differentially across individual and group characteristics (i.e., race, ethnicity, sex, gender identity, class, sexual orientation, gender expression, and others). The next level represents social, economic, cultural, and environmental states (i.e., the social determinants of health [SDOH]). In the model, these interdependent factors are
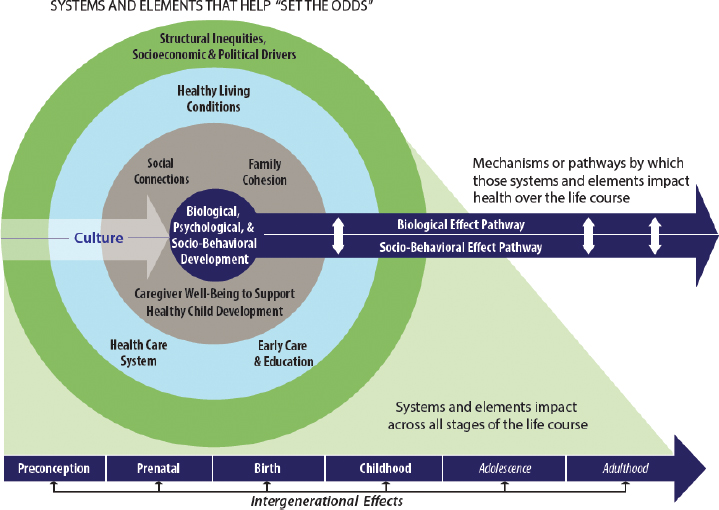
grouped into three domains—healthy living conditions, health care, and education. These domains were identified by the committee based on the available evidence and existing resources as important for targeting prenatal and early childhood interventions and are the primary foci of Chapters 5–7. The next level represents the factors that most directly and proximally shape children’s daily experiences and routine patterns: family cohesion and social connections, which also affect access to critical resources for health, well-being, and development in early life (see Chapter 4). The innermost circle and crosscutting arrows—biological, psychological, and socio-behavioral development—are the focus of Chapters 2 and 3.
THE SCIENCE OF EARLY DEVELOPMENT: CORE CONCEPTS
Based on its review of the science, the committee updated and adapted the core concepts from the 2000 report From Neurons to Neighborhoods and identified 12 core concepts of early development, with a focus on health equity. The evidence underlying these concepts is described in Chapters 2–4, and this evidence guided the committee in its development of recommendations that apply the science of early development. In brief, these concepts include the following (see Chapter 1 for more detailed descriptions of each concept):
- Biology–environment interaction impacts health and development.
- Brain development proceeds in well-defined but continuous steps.
- Major physiological systems develop rapidly during pregnancy and early childhood.
- The early caregiving environment is crucial for long-term development.
- The developing child plays an important role in interactions and development.
- The development of executive functions is a key aspect of early childhood development.
- Trajectories—positive or negative—are not immutable.
- There is variability in individual and group development.
- Experiences across environmental contexts play a significant role in early development.
- Disparities in access to critical resources matter.
- Health outcomes are the result of experiences across the life course.
- Early interventions matter and are more cost effective than later ones.
A large body of recent research provides insights into the mechanisms by which early adversity in the lives of young children and their families can change the timing of sensitive periods of brain and other organ system development and impact the “plasticity”2 of developmental processes. In the past two decades, there has been a convergence of research that has led to many of the advances described in this report. First, a wave of neurobiological studies in model systems and humans found that responses to pre- and postnatal early life stress are rooted in genetic and environmental interactions that can result in altered molecular and cellular development that impacts the assembly of circuits during sensitive periods of development. The demonstration that certain systems involved in cognitive and emotional development are more sensitive to early disturbances that activate stress response networks, such as the frontal cortex, hippocampus, amygdala, and the hypothalamic-pituitary-adrenal axis, provided a basis for both short- and long-term functional consequences of early life stress.
Many of the new scientific advances in neuroscience are still in development, and more research is needed to apply these new findings in clinical and public health practice and to use them to inform policies. In particular, greater effort and support are needed to develop, implement, and evaluate programs based on scientific discoveries regarding the optimal timing for interventions. However, new research has clarified that altered nutrition, exposure to environmental chemicals, and chronic stress during specific times of development can lead to functional biological changes that predispose individuals to manifest diseases and/or experience altered physical, socio-emotional, and cognitive functions later in life. The committee provides information about major biological responses to stressors and new discoveries that have contributed to advancing knowledge about how and when to intervene to improve health outcomes for children.
ROADMAP FOR APPLYING AND ADVANCING THE SCIENCE OF EARLY DEVELOPMENT
With the goal of decreasing health inequities, the broad question this report addresses is, “For those children who are placed at risk for negative outcomes, what can be done—guided by science-based evidence—to expediently and effectively move each of them toward positive developmental health trajectories?” In this report, the committee provides
___________________
2 The process by which neurons within the brain change their gene expression, cellular architecture and connections with other neurons, and function in response to experiences and changes in the environment (i.e., change over time).
recommendations for practice, policy, and systems changes to achieve this goal. The roadmap the committee has put forth includes a suite of key strategies to advance health equity3:
- Intervene early—In most cases, early intervention programs are easier to implement, more effective, and less costly.
- Support caregivers—This includes both primary caregivers and caregivers in systems who frequently interact with children and their families.
- Reform health care system services to promote healthy development—Redesign the content of preconception, prenatal, postpartum, and pediatric care while ensuring ongoing access, quality, and coordination.
-
Create supportive and stable early living conditions:
- Reduce child poverty and address economic and food security,
- Provide stable and safe housing, and
- Eliminate exposure to environmental toxicants.
- Maximize the potential of early care and education to promote health outcomes.
- Implement initiatives across systems to support children, families, other caregivers, and communities—Ensure trauma-informed systems, build a diverse and supported workforce, and align strategies that work across sectors.
- Integrate and coordinate resources across the education, social services, criminal justice, and health care systems, and make them available to translate science to action.
In this report, the committee provides a range of recommendations for practice, policy, and systems changes, including recommendations that will take time and sustained commitment to achieve and recommendations that could be implemented immediately or in the near term. Some of the committee’s recommendations will be difficult to implement; however, the degree of difficulty in implementing any given recommendation does not determine the value of pursuing it. Where possible, the committee also recommends or highlights ways to leverage existing programs that either embrace the core scientific principles laid out above or have a strong basic structure from which to build.
___________________
3 Note that recommendations are not always presented in numerical order, as the summary has grouped them by topic in some cases; however, all report recommendations are presented.
Supporting Family Cohesion and Social Connections
The construct of resilience4 from developmental science is important, as it implies the ability to correct what otherwise might have been negative trajectories, given major life stressors. To set the foundation for the committee’s considerations on the topic of supporting family systems, the committee discusses universal principles of human development pertaining to the broad domain encompassing children’s psychological and behavioral adjustment (see Chapter 4). For example, for children, the single most important factor in promoting positive psychosocial, emotional, and behavioral well-being is having a strong, secure attachment to their primary caregivers—usually their mothers. Strong attachment presupposes effective parenting behaviors in everyday life, and “effective parenting” changes in complexity with development over time.
There is an urgent need to develop preventive interventions well suited for fathers and other male caregivers; existing approaches that are developed for and tested with women cannot be assumed to generalize to other caregivers with equal effectiveness (e.g., in the successful recruitment, retention, and support of men and fathers who take care of young children).
Specific subgroups of children have unique needs and challenges when adjusting to adversity. Careful attention to potent subculture-specific processes needs to be paid in working with subgroups well known to face serious inequities in relation to mental health—including families experiencing chronic poverty; immigrants; lesbian, gay, bisexual, transgender, and queer (LGBTQ) children; LGBTQ parents; children who are separated from parents due to incarceration, foster care, or other reasons; and children exposed to high achievement pressures, usually in relatively affluent communities.
___________________
4 There are two essential conditions that make up resilience: (1) exposure to significant threat or severe adversity, and (2) achievement of positive adaptation despite major assaults on the developmental process.
In addition to addressing major goals relevant for children in general (e.g., fostering caregiver well-being and minimizing maltreatment), programs need to include components that specifically address unique risk and protective processes within these subgroups of children.
A growing body of evidence suggests that home visiting by a nurse, a social worker, or an early educator during pregnancy and as needed in the first years of a child’s life improves a wide range of child and family outcomes, including promotion of maternal and child health, prevention of child abuse and neglect, positive parenting, child development, and school readiness. These positive effects continue well into adolescence and early adulthood. Researchers, program leaders, and policy makers need to focus on expanding the concept of tailored home visiting to advance knowledge on which programs and activities are best for which family, in which communities, and for what outcomes.
State policy makers should further expand support for evidence-based home visiting services through the use of general funds, Medicaid, and a combination of multiple funding streams. HRSA and ACF should support research to continue to ensure program effectiveness and accountability
of the expanded program. Expansion of home visiting programs should be done in conjunction with the expansion of other public investments and services.
Intervention trials have shown strong benefits of relational interventions, such as interventions to foster strong attachments, and group-based supports in communities for caregivers and their families. The core components of several effective interventions suggest that in addition to providing particular skills, improving the overall well-being of caregivers (especially mothers) is the most critical “engine” of change.
It is necessary to consider measures that should be included in evaluating results of large-scale preventive interventions targeting young children and their mothers. Given the need to identify individuals at risk for early adversity and the toxic stress response, regular brief assessments of the mothers’ depressive symptoms, stress, feelings of rejection to the child, any involvement with child protective services, and the degree to which they have positive, buffering relationships in their lives should occur routinely.
Leveraging the Health Care System to Promote Health Equity
The health care system can serve as a platform, along with public health and other sectors, to address the social determinants that underlie many health inequities. However, the current health care system focuses mainly on clinical goals and addresses other determinants of health in fragmented and highly variable ways. U.S. health care provides only limited attention to integration of health care for the whole family, health care across the life course, or integration of mental and behavioral health into clinical care. Recognizing that preconception through early childhood are sensitive and important life periods to optimize health outcomes, care
during these periods needs to become more continuous (access), equitable (quality), integrative (delivery), and comprehensive (content); therefore, the committee offers the following recommendations:
Improving Access to Health Care
Achieving this recommendation will require actively promoting inclusion in coverage and care.
Improving Quality of Care
- performance, and other strategies to enhance accountability; and
- Health care–related workforce development entities should expand efforts to increase diversity, inclusion, and equity in the health care workforce, including diversity-intensive outreach, mentoring, networking, and leadership development for underrepresented faculty and trainees.
Needed metrics include social determinants and social risk measures; cross-sector developmental measures that move beyond common indicators of child development, including mental and behavioral health; and disparities as explicit measurement domains that hold providers accountable for not just delivering services but also improving outcomes. Workforce development (as noted in bullet 3) will need to be addressed by several entities, including the Accreditation Council for Graduate Medical Education and specialty boards, professional schools, training programs, teaching hospitals, including children’s hospitals, and funders of graduate education in health professions (CMS, HRSA, and others).
Organization and Integration of Health Care Services
Achieving this recommendation will require disseminating multidisciplinary team-based care models in community settings; developing integrated models for preconception, prenatal, postpartum, and pediatric care delivery modes; adopting and spreading integrated, whole-family and family-centered care models; developing and using new technologies that improve care and improve accessibility; aligning payment reform with health creation rather than service delivery; and developing systemic and cross-sector collaboration.
Transforming the Content of Care
This work should take place in a larger framework of social and reproductive justice and include more diverse voices, especially from communities most affected by adverse birth and child health outcomes. Such a shift will require that the health care system recognize the impact of both adverse and enriching experiences across the life course and cumulative effects on health and well-being by the health care system. It will also require integrating attention to social and environmental determinants as well as trauma assessment and response into clinical practice.
Although health care plays an integral role in advancing health equity, health care alone cannot meaningfully address health inequities, nor is it the primary actor or leader. Cross-sectoral and multidisciplinary collaboration is essential for decreasing health inequities.
Creating Healthy Living Conditions for Early Development
Reducing or managing caregiver stress is key to giving caregivers the capacity, supports, and resources to care for their children and serve as buffers against adversity. Addressing the primary needs of families and children is critical to achieving this goal. The committee identified four areas of fundamental needs that, if met, would have an impact on health inequities: (1) food security, (2) safe and stable housing, (3) economic stability and security, and (4) safe physical environments.
Food Security
Given the importance of good nutrition for brain growth and development (during the preconception, prenatal, and early childhood periods), the committee concludes that providing resources to ensure families have access to sufficient and healthy foods can improve birth and child health outcomes. Because safety net programs such as WIC and SNAP have been shown to improve birth and child (and adult) health outcomes and to reduce food insecurity, the committee recommends:
Safe and Stable Housing
Evidence suggests that lack of affordable or quality housing, housing instability, and overcrowding have significantly detrimental effects on the health, well-being, and development of infants, children, and families. Housing affordability and quality is an acute problem that disproportionately affects people of color and contributes to health inequities among children. Over half of black and Hispanic renters live in unaffordable housing, and health issues related to poor-quality housing, such as elevated blood lead levels and asthma, are more prevalent among these renters. Current federal housing programs are not adequately funded, and there are not enough safe, affordable housing units in high-opportunity areas. Additional funding for programs can move families out of poverty and allow them to reallocate money for other basic needs that support child health and development. Incentives and/or regulations, along with
enhanced programming, can increase the supply of affordable housing. Recognizing the centrality of housing to health and healthy child development, the committee recommends:
Economic Stability and Security
Children’s well-being and life course outcomes are strongly related to family income. Given the strong evidence that economic security matters, an important factor in reducing health disparities in early childhood is to ensure that families with young children have adequate resources. The committee concludes that public programs that provide resources to families in the form of cash, tax credits, or in-kind benefits improve childhood well-being and life course outcomes and that these effects are long lasting. Furthermore, while income support programs that are contingent on employment status or based on earned income have positive benefits for families, they should avoid regulations and policies that might have unintended consequences for childhood outcomes through negative effects on family relationships and attachments, breastfeeding, and caregiver stress.
Additional income support for families with young children through paid parental leave would recognize the special needs of infants and their caregivers. Unpaid parental leave through the Family and Medical Leave
Act does not cover all employees, and most families with low incomes cannot afford to take an unpaid leave.
This recommendation focuses on strategies that are likely to have particularly important impacts on health outcomes for young children. A child allowance would fill in some of the gaps in the current safety net and particularly benefit the lowest-income children and those most at risk of poor health outcomes. The key advantage of a child allowance (over, for example, tax credits) is that funds are available to families on an ongoing monthly basis rather than once per year. In addition, under the current structure of the child and working-family tax credits, the lowest-income families receive few benefits. Children whose parents are in unstable employment or not employed suffer the short- and long-term health consequences of living in poverty. Reducing health disparities requires reaching these children during their earliest years, regardless of parental employment. Increased SNAP benefits and housing allowances would address current inadequacies in both of these programs and provide targeted support for the critical food and housing needs of young children.
Environmental Exposures and Exposure to Toxicants
There are numerous potential environmental toxicants that may be transmitted through the air, water, soil, and consumer products with which food and water come into contact. Many of these occur naturally in the environment (e.g., arsenic, radon, etc.), and many more are released through human-based processes (e.g., heavy metals, chemicals from plastic production and degradation, and particulates). The embryonic, fetal, and early childhood periods represent greater risk than adulthood for adverse mental and physical health outcomes from environmental exposures due to children’s smaller size, proportionally large intake of food, air, and water
to body weight, and rapid developmental processes that may be influenced and disrupted by chemicals and toxicants. As a result of toxicant exposures, children may suffer from a variety of developmental problems, chronic conditions, and even premature death. Poverty, substandard and/or unstable housing, minority racial/ethnic status, and proximity to known sources of pollutants heighten children’s risk of exposure and poor health and developmental outcomes. The committee identified three areas where current efforts could be improved to prevent and mitigate the impact of environmental toxicants in the prenatal through early childhood periods:
In Chapter 6, the committee also discusses the role of civil rights strategies to promote healthy communities for developing children.
Promoting Health Equity Through Early Care and Education
While most of the attention on early care and education (ECE)5 has focused on whether it improves children’s cognitive and socio-emotional development and academic readiness, research shows that ECE affects various other child health outcomes, including children’s physical, emotional, and mental health. ECE programs increase children’s cognitive, social, and health outcomes through enhancing their motivation for school and readiness to learn and the early identification and intervention of problems that impede learning. This, in turn, helps children improve their cognitive ability and social and emotional competence, while increasing their access to and use of preventive health care. Access to ECE may lead to lower risk of dropping out of school, greater school engagement, and subsequently better educational attainment, which lead to increased income and decreased social and health risks, resulting in greater health equity.
Allocation of Adequate Resources to Support ECE Programs and Educators
Intentional policies and allocation of adequate resources to support these programs and educators are needed for ECE programs to contribute significantly to a health promotion and equity strategy.
___________________
5 ECE can be defined as nonparental care that occurs outside of the child’s home. ECE services may be delivered in center-, school-, or home-based settings.
- The Office of Child Care and the Office of Head Start at the federal level, along with state, local, tribal, and territorial early care and other education agencies, should assess the full cost of implementing standards that promote health outcomes and equity as described above, including supporting educators’ own health and well-being, and work with Congress to align funding levels of the major federal ECE programs—child care subsidy and Head Start—accordingly.
- Health and human service entities, the federal Early Learning Interagency Policy Board, state Early Childhood Advisory Councils, and federal, state, local, tribal, and territorial agencies that oversee home visiting and ECE programs should ensure greater programmatic coordination and policy alignment to ensure effective allocation of resources.
- The Office of Planning, Research & Evaluation in the Administration for Children and Families, along with the U.S. Department of Education, should examine the feasibility and seek resources to conduct (a) an implementation study to examine the design and implementation of this comprehensive ECE approach that incorporates health standards and (b) an outcomes study that examines the impact on children’s school readiness and achievement, and health outcomes, with particular attention to eliminating disparities and gaps prior to school entry.
Health-Focused Competencies of the ECE Workforce
Policies and systems that prepare and support early childhood educators and program leaders, including those in public schools, need to incorporate the latest evidence about how to support children’s school readiness and success by fostering their health and well-being. This would entail providing comprehensive supports and resources to degree granting institutions and preparation programs, including the development of curricula, textbooks, practicum experiences, toolkits, and fact sheets.
Access and Affordability to ECE Programs
Maximizing the impact of ECE on positive early childhood development and health and well-being at the community or population level will require increasing public funds for ECE programs. Currently, eligibility for ECE programs is limited, and among eligible families, access is low due to lack of funding and availability of programs and services. Therefore, even if existing publicly funded programs have the resources to provide robust supports that improve young children’s health and well-being, these will not reach most children, especially those who live in low-income households or confront adverse experiences and toxic stress.
The strategic plan should be modeled after and build on the relevant performance standards of Early Head Start and Head Start, which emphasize mixed settings, the whole child, family and community engagement, transition between home and school, and continuous quality improvement. It should also strengthen those program components discussed in Chapter 7 that lead to stronger school readiness and health outcomes, including mitigation of the impact of adverse experiences and toxic stress for children, families, teachers, and staff. Critical components include a comprehensive social-emotional strategy that encompasses both the classroom (curriculum, teacher training and support) and program/school (leadership, culture and climate) levels and educators who have competencies described in Recommendation 7-2.
Systems Approach
Advancing health equity in the preconception through early childhood periods cannot be achieved by any one sector alone—it will take action, collaboration, and alignment across all sectors that frequently interact with children, families, and the professionals who serve them. Systems are a collection of interacting, interdependent parts that function as a whole. For the purposes of this report, most of the systems are social constructs and are organized around a key functional area (e.g., education, health care, housing). Systems change is not an easy strategy, it seldom yields speedy returns, and it may not be sufficient without an investment of resources designed to take advantage of new and better aligned approaches. However, given that disparities are systematically generated, it is likely a necessary precursor to real and widespread advances in health equity. The committee identified eight crosscutting recommendation areas where multiple sectors need to take action, based on review of the evidence in Chapters 1–7 and the committee’s collective expertise. In brief (additional details available in Chapter 8), the committee recommends:
- and social services; those standards should be replicated and implemented across systems.
- Recommendation 8-4: Develop a transdisciplinary and diverse workforce to implement culturally competent service delivery models. The workforce should reflect the diversity of populations who will engage in sector services.
- Recommendation 8-5: Improve access to programs or policies that explicitly provide parental or caregiver supports and help build or promote family attachments and functioning by engaging with the families as a cohesive unit. For families with intensive support needs, develop programs or initiatives designed to provide comprehensive wraparound supports along a number of dimensions, such as health care, education, and social services, designed to address needs related to the social determinants of health that are integrated and community based.
- Recommendation 8-6: Integrate care and services across the health continuum, including the adoption of models that provide comprehensive support for the whole person in a contextually informed manner, leveraging and connecting existing community resources wherever possible, with a focus on prevention.
- Recommendation 8-7: Invest in programs that improve population health and in upstream programs that decrease long-term risk and poor health outcomes. These changes should be accompanied by accountability metrics to ensure that the spending is tangibly and demonstrably in service to the goals behind the original funding, but offer more flexibility in how those goals are achieved.
Crosscutting Research Needs
A tremendous amount is known about what works to advance health equity in early development (and the lifelong benefits of doing so), and efforts to translate this science into action and to scale up effective interventions needs to be accelerated. Many interventions have shown promising results at a small scale but have not been fully tested across multiple settings or in diverse communities and populations. Others have promising preliminary data but require more evidence. In addition, the evidence around systems and policy changes—the work needed to address inequities with a multisector and systems-based approach—remains less certain than programmatic evidence in many cases precisely because it is complex and set in shifting environments that make confident attribution of effects challenging. In Chapter 8, the committee recommends newly designed and adapted
research strategies to help translate science to action across sectors, including needed data to inform subgroup analyses and elucidate the complex causality related to health inequities to better design interventions across sectors.
An important caution, however, is that although targeted research is needed to address population heterogeneity with more precision, enough is already known to act now to advance health equity in the prenatal and early childhood periods. The research recommended below is important to continually improve efforts and increase impact but should not impede action. Here the committee provides guidance on charting the course for future research to better meet the health and social needs of the nation’s children in the future and, specifically, to advance health equity.
-
- Conduct research that measures the impact of chronic stress on all relevant organ systems and determines the specific molecular and biological pathways of interaction during the pre- and postnatal periods, which are directly relevant to potential interventions to address health disparities.6
Many of the items in this recommendation will require recruiting diverse populations, with explicit attention to addressing racial/ethnic and socioeconomic inequities in developmental outcomes.
Measuring Success
The committee has identified a number of measures and indicators that can currently be measured and are important for tracking progress within each of the systems that act as key leverage points for early childhood development discussed in this report. For example, for caregivers, the committee proposes measuring maternal depression and stress, feelings of rejection or hostility to the child, available support for mothers, and any contact with child protective services. However, other measures will be needed. To further the ability for subgroup and other analyses and continuous data collection on both successes and failures, the following are needed (see Chapter 8 for more detail):
Understanding and measuring cumulative exposure. A number of factors impact early life development, ranging from influences in the microsocial or family environment, such as attachment, nurturing, and maternal well-being, to institutional levers, such as access to prenatal care or effective responses to trauma exposure, to macrosocial forces, such as racism and poverty. Effective tools already exist to measure exposure to some of these factors but there are few methods for empirically understanding how exposures to risks or protective factors accumulate and combine over time to establish a cumulative overall risk profile.
Understanding the interaction among developmental pathways. There are few frameworks for understanding the multidirectional relationship between the biological, social-behavioral, and psychological development of young children. In particular, understanding how these interactions may vary across the life course in response to changing plasticity of biological systems, different stages of personal and cognitive development,
___________________
6 For reference, this is Recommendation 2-1 in this report.
and different life conditions and accumulated experiences is critical to building a health equity strategy.
Measuring interactions between systems. Models that can estimate “integrated risk” by combining key data from across the sectors where people live their lives are needed. Similarly, measures that examine results from cross-sector collaboration can help in documentation and accountability.
Improving methods to assess complex causality. Perhaps the biggest challenge facing health equity research is complex causality. Many of the preferred tools of science, such as randomized controlled trials, are designed to control for and isolate single causes rather than embrace complex, interrelated causality that may include multilevel, multidirectional, and nested effects—for which a larger toolbox of strategies is needed. For example, there needs to be greater exploration of effective community-based intervention approaches that use existing resources (e.g., as in “natural experiments”).
CONCLUSION
The advances in the science of early development are ready to be acted on—there is no reason to wait for this additional science before taking action. Long-term psychological, behavioral, and physical health is shaped by biological and environmental factors, including their interactions, before conception and throughout the life course. This interplay necessitates action at the practice, policy, and systems levels that takes into account the full range of factors that shape health and well-being. These actions need to be taken before insults to early development occur. The science of plasticity shows that it is never too late to intervene but that early identification and intervention are generally more effective and cost-saving and require less effort. (See Box S-1 for a high-level overview of the report’s findings and Table 9-1 for a summary of recommended actions in this report.) Furthermore, these actions need to take a life course, multigenerational approach to decrease health inequity, as children’s well-being depends on the well-being of the primary caregivers and the quality of their relationship. Progress toward health equity can be achieved through multipronged, cross-sector interventions that focus on prevention, early detection, and mitigation and that work at the practice, policy, and systems levels to address the SDOH. The committee hopes that the roadmap laid out in this report will catalyze the steps that need to be taken across systems to close the health equity gap and improve the lives of our nation’s children.
This page intentionally left blank.




























