1
The Need to Intervene Early to Advance Health Equity for Children and Families
INTRODUCTION
Neurobiological and socio-behavioral research indicate that early life conditions, including social supports (e.g., supportive relationships) and adversity (e.g., chronic or severe stress), shape prenatal and early childhood health and development. These experiences have a powerful impact on developing biological systems that impact physical and mental health outcomes throughout life and are further influenced by the social determinants of health (SDOH) (e.g., education, housing, physical and social environment). Despite increasing evidence about what contributes to poor health, these health inequities have persisted, and for some populations and outcomes, they are worsening. Scientific evidence can be used to better inform efforts to advance health equity; this report uses that evidence to support policy actions, program development, practice changes, systems reform, and research priorities. (See Box 1-1 for a high-level overview of this chapter.)
THE PROBLEM
The United States spends much more on health care than any other Organisation for Economic Co-operation and Development (OECD) nation, yet it ranks poorly on most measures of population health (NRC and IOM, 2013; OECD, 2017). Significant, long-standing disparities exist in most health outcomes by education, income, race, ethnicity, geography, gender, neighborhood, disability status, sexual orientation, and citizenship
status (NASEM, 2017). Notably, the past few decades have marked a troubling rise in U.S. maternal mortality rates, including black-white disparities, while maternal mortality rates have declined globally (WHO, 2015). Similarly, disparities in infant mortality rates persist, where non-Hispanic black, American Indian/Alaska Native (AI/AN), and Hispanic babies experience higher rates of mortality before their first birthdays compared to non-Hispanic white and Asian and Pacific Islander babies (CDC, 2019b). Children in the United States rank behind their peers in most OECD nations in health status and key determinants of health, and they experience growing disparities on multiple measures of child well-being (OECD, 2009; Seith and Isakson, 2011) (see Box 1-2). For children living in both urban and rural communities, lack of access to critical resources is a major driver of increasing disparities, and this is compounded for economically disadvantaged groups. These disparities put children on a course for poor health outcomes later in life. For more information on maternal and child health disparities, see the section on Early Childhood and Maternal Health Disparities in the United States.
Many families in the United States do not receive health care when needed, receive it too late, and/or experience problems in quality; however, pathways to better health do not depend on health care alone. For example, children in relatively affluent communities, who ostensibly have easy access to the best mental health services, also show elevated distress compared to national norms—as do their low socioeconomic status (SES) counterparts, but due to a different set of life stressors (Korous et al., 2018). The factors that ultimately contribute to good health (such
as nutrition, stress, exposure to environmental toxicants) are on multiple interrelated causal pathways along the life-span (NASEM, 2017).
Over the past 100 years, there has been a strong trend toward the conflation of “health” and “health care,” where the health of an individual is considered only through a biomedical lens, not taking into account the multiple social and developmental determinants that drive health (Lantz, 2018). Instead, health has been erroneously equated with health care and health disparities erroneously equated with health care disparities. The result is a narrow policy focus on health care interventions to improve health. More recently, research and practice has shifted away from this prevailing paradigm to one that targets upstream factors that shape health (Hahn, 2019; NASEM, 2017).
The 2017 National Academies of Sciences, Engineering, and Medicine (the National Academies) report Communities in Action: Pathways to Health Equity reviewed the root causes of health disparities and concluded that health inequity arises from root causes that could be organized in two clusters:
- Intrapersonal, interpersonal, institutional, and systemic mechanisms (also referred to as “structural inequities”) that organize the distribution of power, and access to critical resources, differentially across lines of race, gender, social class, sexual orientation, gender expression, and other dimensions of individual and group identity, and
- Unequal allocation of and access to power and resources—including goods, services, and societal attention—which manifests itself in unequal social, economic, and environmental conditions, also called the “determinants of health” (NASEM, 2017, p. 7).
Therefore, health inequities are the result of more than individual choice or random occurrence. They are the result of the historical and ongoing interplay of inequitable structures, policies, and norms that shape lives. Interventions targeting the above factors hold the greatest promise for advancing health equity and promoting positive health outcomes at the population level.
Furthermore, the report concluded that
Health equity is crucial. Health equity is fundamental to the idea of living a good life and building a vibrant society because of its practical, economic, and civic implications. Promoting health equity could afford considerable economic, national security, social, and other benefits. Yet, recent research demonstrates that worsening social, economic, and
environmental factors are affecting the public’s health in serious ways that compromise opportunity for all (NASEM, 2017, Summary).
Health inequity is costly. Beyond significant costs in direct health care expenditures, health inequity has consequences for the U.S. economy, national security, business viability, and public finances considering the impact of poor health and disability on one’s ability to participate in the workforce, military service, or society. Addressing health inequities is a critical need that requires this issue to be among our nation’s foremost priorities (NASEM, 2017, Summary).
Given these findings, it is critical to address health disparities (differences in health outcomes) with a comprehensive approach—by treating all of the factors that impact individual health, such as education, employment, health systems and services, family, community, housing, income and wealth, physical and social environments, public safety, and transportation (SDOH), in addition to racism, discrimination, segregation, and poverty. To achieve equitable health outcomes in the prenatal through early childhood periods and throughout the life course, all of these contexts need to be addressed.
Health inequities are systemic challenges, and chronic childhood adversities have biological implications and affect childhood development, with lifelong impacts on health and well-being. When exposures to key experiences (both positive and negative) differ for specific groups (e.g., black/African American, AI/AN, Hispanic), their odds for good health diverge systematically over time, producing disparities in outcomes. Because the odds of these exposures are impacted by systems, advancing health equity will require more than individual-level interventions. It will require systems to change in ways that improve the odds of good experiences and reduce the odds of adverse exposures for specific populations.
The focus of this report is on how to best maximize well-being among all young children and families, especially those who are vulnerable at the outset—because life circumstances have rendered them statistically more likely to be on negative adjustment trajectories from early life onward. “Inequities” are operationally defined for the purpose of this report, in part, as the unequal likelihood of thriving or attaining positive adjustment outcomes over time because of differences in opportunity that lead to unfair and avoidable differences in health outcomes.
OPPORTUNITIES
Failing to address the context in which children live, grow, and learn undermines the potential of so many children. Evidence shows that
prevention and early intervention for children on at-risk trajectories works and is generally more effective and less costly than later intervention. Luckily, a great deal is known about the science of prenatal and childhood development and the biological mechanisms and effects of chronic adversity and adverse childhood experiences (ACEs) (see Chapters 2 and 3). Recent advances in science—especially around epigenetics,1 technology and data sharing, and cross-disciplinary collaboration—present an opportunity to systematically apply this knowledge to practice, policy, and systems changes. A large body of research now explicates the mechanisms by which early adversity can change the timing of sensitive periods of brain and other organ systems development, impacting the “plasticity”2 of developmental processes that are driven by experiences in the life of the young child and his or her family. It is now known that what takes place in early development has lifelong impacts—both positive and negative—on health and well-being. While diseases may appear clinically throughout the life-span, it is known that many diseases originate during early development (Gluckman et al., 2007; Heindel and Vandenberg, 2015). For example, altered nutrition, exposure to environmental chemicals, or stress during specific times of development can lead to functional biological changes, predisposing individuals to diseases that manifest later in life and affecting physical, mental, and cognitive functions.
This report employs the science of early development to inform multidisciplinary and developmentally appropriate systems to support optimal health and well-being for all children throughout their life-spans. The tremendous advances in the theoretical and empirical science in the past 30 years position practitioners and policy makers to take informed action to improve child health outcomes. There is now a firm understanding of the importance of the environment—the constant interplay of nurture–nature and biology–environment—on biological processes, including the impact of early adversity, poverty, and racism on lifelong health outcomes. While there is more to be discovered that will lead to a better understanding of best practices and address challenges of heterogeneity, research has advanced dramatically to apply new and more effective interventions now than ever before.
Given these advances and the understanding of how science can be used to advance health equity during early development, the Robert Wood Johnson Foundation (RWJF), as part of its Culture of Health Initiative,
___________________
1 The study of how genes are expressed due to changes in the environment and how these biological changes can be passed down from one generation to the next.
2 The process by which neurons within the brain change their gene expression, cellular architecture, connections with other neurons, and function in response to experiences and changes in the environment (i.e., change over time).
asked the Health and Medicine Division of the National Academies to (see Box 1-3 for the full Statement of Task)
- Provide a brief overview of stressors that affect prenatal through early childhood development and health;
- Identify promising models and opportunities for translation of the science to action;
- Identify outcome measures to enable subgroup analyses;
- Develop a roadmap to apply the science to tailored interventions (i.e., policies, programs, or system changes) based on biological, social, environmental, economic, and cultural needs; and
- Provide recommendations in these areas, including how systems can better align to advance health equity.
To respond to this charge, the Committee on Applying Neurobiological and Socio-Behavioral Sciences from Prenatal Through Early Childhood Development: A Health Equity Approach was formed. The committee applied a health equity frame and builds on the 2017 National Academies report Communities in Action: Pathways to Health Equity. As identified in the 2000 National Research Council and Institute of Medicine (NRC and IOM) report From Neurons to Neighborhoods: The Science of Early Childhood Development, prenatal through early childhood are critical phases of development for the production of health. This report reviews the science that has been developed since From Neurons to Neighborhoods.
The committee also adopted the life course approach to its work, which emphasizes a temporal and social perspective, while looking back across an individual’s life experiences—or across generations—to gain a better understanding of health outcomes (Braveman and Barclay, 2009). This approach takes into account an individual’s larger social, economic, and cultural context and that the trajectory of that individual’s life may be changed, negatively or positively, through interactions between the brain, body, and environment throughout the life-span. An individual’s health status and outcomes reflect the accumulation of experiences over the life course. Protective factors support positive, or flourishing, trajectories, while risk factors exacerbate the likelihood of poor trajectories (see Figure 1-1).
In line with the life course approach, the committee included the preconception period as an important focus of the report. The health of men and women before conception is important for pregnancy outcomes and the lifelong health of their children. During the preconception period, parents may be exposed to several types of stressors (e.g., chronic stress, environmental toxicants, poverty) that could have repercussions for the health of their future children even into adulthood.
For the purpose of this report, early childhood refers to birth through the onset of puberty and the beginning of adolescence (approximately 8 years of age). The committee uses the terms “preconception,” “prenatal,” “postpartum,” and “early childhood” to refer to the various periods of development. The committee uses the term “early development” to refer to the preconception through early childhood periods.
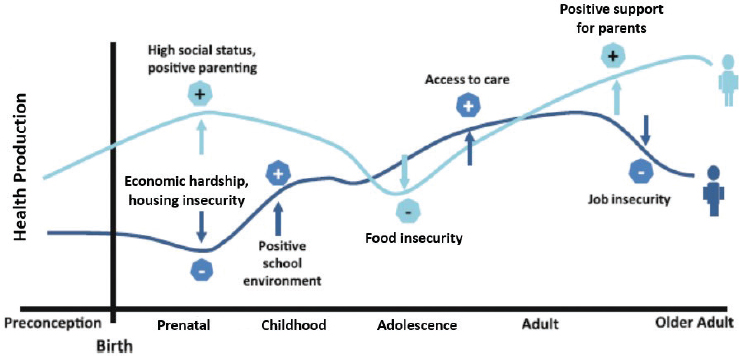
NOTE: This figure includes several examples; however, there are many other variables that impact health trajectories (see Chapter 3).
SOURCE: Adapted from Halfon et al., 2014.
Another National Academies study that was under way during the course of this study—also looking at the neurobiological and closed-behavioral sciences—covered adolescence (NASEM, 2019a).
The outcomes that the committee seeks to improve across the life course fall into four categories, adapted from the 2016 National Academies report Parenting Matters: Supporting Parents of Children Ages 0–8:
- Physical health and safety,
- Emotional and behavioral competence,
- Social competence, and
- Cognitive competence.
See Box 1-4 for definitions of key terms used in this report.
WHY INVEST IN EARLY INTERVENTION AND PREVENTION?
There are many reasons to intervene in the prenatal through early childhood periods to prevent and mitigate adverse health outcomes both in early life and over the life course. First, preventing or reducing poor outcomes in the prenatal through early childhood periods generally leads to improved health outcomes later on and therefore can yield health care savings in the long term. For example, in 2007, the IOM reported that the cost associated with premature birth in the United States was $26.2 billion each year (IOM, 2007), and the Centers for Disease Control
and Prevention reported that the United States spends $147 billion in obesity-related health care costs each year (CDC, 2019a). Health care savings are also seen when preventing lead poisoning (Gould, 2009) and some childhood diseases. McLaughlin and Rank (2018) estimate that childhood poverty results in $192.1 billion in aggregate health costs (with another $96.9 billion due to child homelessness and $40.5 billion due to maltreatment). Furthermore, inequity is costly. As noted in Communities in Action (NASEM, 2017), advancing progress toward health equity (across the life course) could produce economic, national security, and other benefits for the nation. The report made the case that beyond the dollar cost of health care services (which itself is significant at $3.5 trillion in 2017, accounting for 17.9 percent of the nation’s gross domestic product [GDP]; CMS, 2017; Martin et al., 2018a), health inequities contribute to overall poor health for the nation and therefore have consequences for the U.S. economy, including diminished productivity in the business sector. In 2009, the Urban Institute projected that from 2009 to 2018, racial disparities in health will cost U.S. health insurers approximately $337 billion in total (Waidmann and Urban, 2009). Furthermore, the rising cost of health insurance and medical care for workers cuts into companies’ ability to make a profit and stay competitive (IOM, 2015; Shak et al., 2013).
Investing in early development through prevention and early intervention yields cost savings because the investment costs are often less than the downstream costs of poor health and development. For example, investing in high-quality early care and education (ECE) is one way to improve outcomes related to child health. Not only do early childhood intervention programs yield benefits in academic achievement, behavior, educational progression and attainment, and labor market success, among other domains, but well-designed early childhood interventions have been found to generate a return to society (Karoly et al., 2005).3Garcia et al. (2017) found a 13.7 percent return on investment for comprehensive, high-quality, birth-to-5 early education.4 From a public health perspective, a 2017 systematic review by Masters and colleagues found that national and public health interventions are highly cost-saving for interventions ranging from vaccination to larger determinants of health, though those focusing on the latter had a lower return on investment because they are more complex, resource intensive, and sustained.5
___________________
3 Studies looking at cost-effectiveness often rely on different underlying assumptions, limiting comparisons across studies and programs. However, overall studies have shown that investments in early childhood appear to save money in the longer term.
4 The study analyzed a wide variety of life outcomes, such as health, crime, income, IQ, schooling, and the increase in a mother’s income after returning to work due to child care.
5 The review included studies from Australia, Canada, Japan, New Zealand, the United Kingdom, the United States, and Western Europe.
Child maltreatment is costly to the nation as well. The total lifetime economic burden in the United States in 2008 resulting from new cases of fatal and nonfatal child maltreatment was approximately $124 billion (Fang et al., 2012). Furthermore, Bellis and colleagues (2017) found that disproportionate health expenditure in later life might be reduced through childhood interventions to prevent ACEs, showing the long-lasting costs of early adversity.
While the primary beneficiaries of prevention and early intervention efforts are children and their families, the nation as a whole also benefits through cost savings, a healthier and more productive workforce, and strengthened national security (NASEM, 2017).
CURRENT STATE OF CHILDREN’S HEALTH
Overall Well-Being of Children and Families in the United States
This section begins with a broad overview of the current state of child health in the United States, followed by a summary of key health disparities in child and maternal health in the country. Child health is the extent to which individual children or groups of children are able or enabled to (a) develop and realize their potential, (b) satisfy their needs, and (c) develop the capacities that allow them to interact successfully with their biological, physical, and social environments (NRC and IOM, 2004). Children in the United States are generally perceived to be healthier now than in the past because they are much less likely to encounter the major infections or debilitating diseases of past generations and are typically able to recover fully from “acute” childhood illnesses. However, ailments of the past have been replaced with chronic conditions (such as diabetes, asthma, obesity, depression, and anxiety), with large segments of U.S. children facing barriers to good health and well-being as a result of poverty, food insecurity, unsafe or unstable housing, and substantial adversity (such as ACEs) in the first few years of life.
Children who are born and raised in poverty are at particularly high risk for poor health outcomes, more problems in early development (e.g., lack of readiness for school at age 5, diagnoses of developmental delays and/or disorders), and higher rates of most childhood chronic conditions. Early adverse experiences have intermediate effects on physical and/or mental well-being and contribute to chronic disease and poor functioning in adulthood (Hughes et al., 2017; Shonkoff et al., 2012). In fact, these impacts are cumulative, and adults who experience adversity in childhood have substantially higher rates of heart disease, lung disease, metabolic syndrome, and other costly health conditions (see Chapters 2 and 3 for more information). Many of these health disparities are rooted in historical
practices and policies (such as segregation and redlining), and this historical legacy continues to shape the development of children today. (See Chapter 3 for a discussion on historical trauma and NASEM [2017] for an overview of historical injustices that impact health outcomes.)
Early Childhood and Maternal Health Disparities in the United States
This section provides a brief overview of child and maternal health disparities and indicators of health in the United States. It is not a comprehensive overview but rather highlights some of the key health disparities. The most recent data available are presented. Chapter 3 provides a detailed overview of health disparities and critical influences or factors that can either promote or hinder healthy development, with a focus on factors that shape inequities at the child/family level and the community and population levels.
Infant Mortality Rates
In 2015, infant mortality rates per 1,000 live births by race and ethnicity were as follows: non-Hispanic black (11.3), AI/AN (8.3), Hispanic (5.0), non-Hispanic white (4.9), and Asian/Pacific Islander (4.2) (CDC, 2019b) (see Figure 1-2). In 2014, infant mortality in rural counties was 6.55 deaths per 1,000 births, 6 percent higher than in small and medium
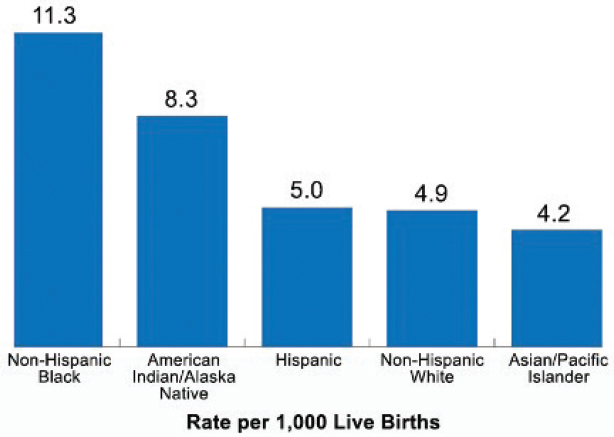
SOURCE: CDC, 2019b.
urban counties and 20 percent higher than in large urban counties (Ely et al., 2017). Neonatal mortality was 8 percent higher in both rural (4.11 per 1,000 births) and small and medium urban counties compared with large urban counties (Ely et al., 2017).
Mortality for infants of non-Hispanic white mothers in rural counties (5.95 per 1,000) was 41 percent higher than in large urban counties and 13 percent higher than in small and medium urban counties (Ely et al., 2017). For infants of non-Hispanic black mothers, mortality was 15 percent higher in small and medium urban counties and 16 percent higher in rural counties (12.08) compared with large urban counties (Ely et al., 2017).
Low Birth Weight
Low birth weight (LBW; less than 5.5 pounds at birth) babies are more at risk for many short- and long-term health problems, such as infections, delayed motor and social development, and learning disabilities (CDC, 2016). Causes of LBW include maternal smoking, use of alcohol, or lack of weight gain and social and economic factors, such as low income, low parental educational level, maternal stress, and domestic violence or other abuse (CDC, 2016).
LBW levels among race and Hispanic-origin groups in 2016 ranged from 6.97 percent for births to non-Hispanic white women to 13.68 percent for births to non-Hispanic black women. Rates among Hispanic subgroups ranged from 6.9 percent for births to Mexican women to 9.5 percent for births to Puerto Rican women (Martin et al., 2018b). In 2016, 14 percent of black infants were LBW, compared with 8 percent of Asian and Pacific Islander, 8 percent of AI/AN, 7 percent of white, and 7 percent of Hispanic infants. Among those of Hispanic origin in 2016, Puerto Rican infants were the most likely to be LBW (9 percent) (Child Trends, 2018b). In 2013, the most recent year that information for Asian and Pacific Islander subgroups was available, Asian Indian infants were the most likely to be LBW (11 percent), followed by Filipinos (9 percent). Black infants are also more than twice as likely as other infants to be very LBW—less than 3 pounds 5 ounces—at 2.9 percent in 2016, compared with between 1.1 and 1.2 percent for white and Hispanic infants, respectively (Child Trends, 2016b).
Chronic Childhood Diseases
Conditions that rarely lead to death in children and youth are now more prevalent: obesity, asthma, mental health conditions (especially attention-deficit/hyperactivity disorder, depression, and anxiety), and neurodevelopmental conditions (including autism spectrum disorders) (Perrin et al., 2007, 2014; Van Cleave et al., 2010). For example, in children
less than 18 years of age, asthma was prevalent among 8.1 percent of white non-Hispanic children, 12.6 percent of black non-Hispanic children, 8.2 percent of other non-Hispanic children, and 7.7 percent of Hispanic children. Among Hispanic children, 11.3 percent of Puerto Rican children and 6.2 percent of Mexican/Mexican American children had asthma (CDC, 2019c). During 2016, asthma affected children living in families with incomes of less than 100 percent of the federal poverty level (FPL) (10.5 percent) more than those living in families with incomes of ≥250 percent of the FPL (250 to <450 percent FPL: 6.9 percent; ≥450 percent FPL: 6.7 percent) (Zahran et al., 2018).
Mental and Behavioral Conditions
Particularly noteworthy is the growth of mental and behavioral conditions among children and youth. Recent work has documented their (a) high prevalence, (b) major impact on youth well-being and functioning, (c) common association with other chronic conditions, (d) high costs, and (e) complication of the course, treatment, and outcomes of most other conditions (Ghandour et al., 2012; Houtrow et al., 2014; Perrin et al., 2018). Importantly, most of these high-prevalence conditions occur at higher rates and usually higher severity among low-income children, even though the rate of growth has increased in all SES levels (Houtrow et al., 2014). Although all of these conditions have genetic components, they also often reflect the consequences of early childhood experiences and their influence through epigenetics and other physiological mechanisms. Furthermore, less than optimal access to and use of health care in early years can negatively affect these conditions over time.
Early Life Adversity
The impacts of early life adversity and disparities are discussed in detail in Chapters 2 and 3; however, a highlight of a few disparities is provided here. ACEs (including physical, emotional and sexual abuse, physical and emotional neglect, and household stressors, including parental mental illness, substance use or incarceration, parental separation or divorce, and domestic violence) are highly prevalent in all racial and socioeconomic groups. Almost 50 percent of children and adolescents (age 0–17) have experienced at least one category of ACE according to national population-based studies (Bethell et al., 2014), and black, Hispanic, and poorer children are exposed to more ACEs relative to white or wealthier children (Slopen et al., 2016).6 Foster care children are at
___________________
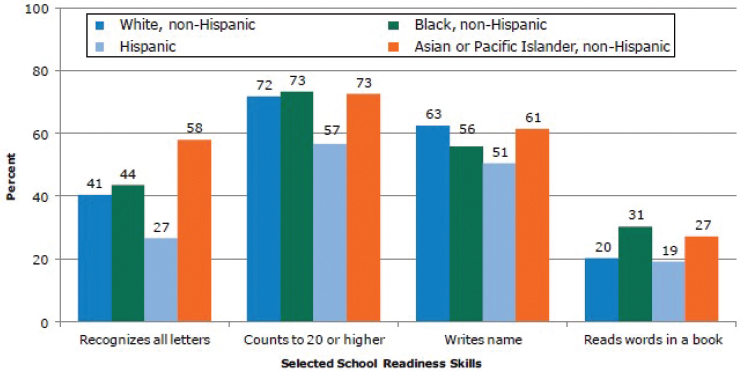
NOTES: Data represent parent reports of specific cognitive and literacy skills. Data are sourced from Child Trends’ analysis of the National Household Education Survey.
SOURCE: Child Trends, 2015.
between 1.5 and 7 times greater odds of having experienced any 1 of the 10 traditional ACEs compared to children not placed in foster care, even after controlling for race and ethnicity, parent education and employment, welfare services, and poverty status (Turney and Wildeman, 2017).
School Readiness
School readiness7 is an important indicator for future child well-being, and there are deep disparities across race and ethnicity (see Chapter 7 for a detailed overview of the importance of ECE). Figure 1-3 provides examples of important measures of school readiness by race and Hispanic origin. Using 2016 National Survey of Children’s Health data, Ghandour et al. (2018) found that only 41.8 percent of 3- to 5-year-olds in the United States were estimated to be on track in all four domains of school readiness. Overall, Hispanic children are less likely to show cognitive/literacy readiness skills than are white, black, or Asian/Pacific Islander children.
___________________
7 That is, children possessing the skills, knowledge, and attitudes necessary for success in school and for later learning and life. The concept of “school readiness” is broader than cognitive or pre-academic skills, such as early literacy and math. However, comparable data across communities or states are limited mostly to such outcomes, which are what is presented here. All states have developed some form of school readiness assessment, and most of them focus on children’s social-emotional development, approaches to learning, and physical health and development, as well as cognitive abilities (Daily et al., 2010).
In 2012, 27 percent of Hispanic 3- to 6-year-olds could recognize all 26 letters of the alphabet, compared with 41 and 44 percent, respectively, of white and black children. Asian/Pacific Islander children had the highest rate of recognizing all of the letters, at 58 percent. A similar pattern in the ability to count to 20 and write their name was seen by race, although Asian/Pacific Islander children were similar to their white and black counterparts (Child Trends, 2015). Young pre-K children living in poverty are much less likely to have cognitive and early literacy readiness skills than are children living above the poverty threshold. Disparities in all measures of early school readiness by income level were greatest in 1999, but these narrowed in 2007 (Child Trends, 2015).
Poverty
Poverty affects large numbers of U.S. children. A 2019 National Academies report, A Roadmap to Reducing Child Poverty, estimated that in 2015, more than 9.6 million children under 18 years of age lived in poverty, as measured by the Supplemental Poverty Measure (SPM) (NASEM, 2019b). Thus, 13 percent of the child population lived in households with annual incomes ranging from $22,000 to $26,000 for a family of four. Moreover, of those 9.6 million children, 2.1 million lived in “deep poverty,” defined as having family resources below half of the poverty line—$11,000 to $13,000 annual income. An additional 22 percent of U.S. children live in “near poverty” households, defined as between 100 and 150 percent of the SPM poverty line. These 16.7 million children live in households that frequently pay more in taxes than they receive in tax credits, reducing their net incomes (NASEM, 2019b). Many U.S. families with children face persistent problems related to poverty, including inadequate housing, clothing, and food for their children, and health problems accompany those deficits.
Health Insurance Coverage
From 2008 to 2016, the rate of uninsured children steadily decreased from 9.7 to 4.7 percent. However, the percentage of uninsured children increased to 5 percent in 2017 (Alker and Pham, 2018). See Figure 1-4 for the rate of uninsured children from 2008 through 2017.
For the percentage breakdown of the number of uninsured children by race and ethnicity in 2016 and 2017, see Figure 1-5. As the figure shows, for black, white, Asian/Native Hawaiian/Pacific Islander, and Hispanic children, the rate of children without insurance increased from 2016 to 2017. In the same 2-year period, the rate of children without insurance decreased for AI/AN children by 0.2 percent. However, the rate of children without insurance for this group is far higher than for other racial
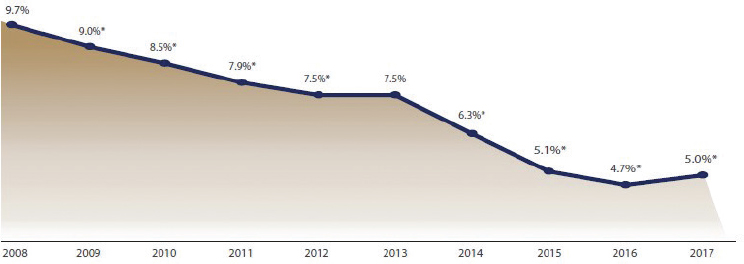
NOTES: * Change is significant at the 90 percent confidence level. Significance is relative to the prior year. 2013 was the only year that did not show a significant 1-year increase or decrease in the national rate of uninsured children. The Census began collecting data for the health insurance series in 2008; therefore, there is no significance available for 2008. Data are sourced from Table HIC-5, Health Insurance Coverage Status and Type of Coverage by State—Children Under 19: 2008 to 2017, Health Insurance Historical Tables, U.S. Census Bureau American Community Survey.
SOURCE: Alker and Pham, 2018.
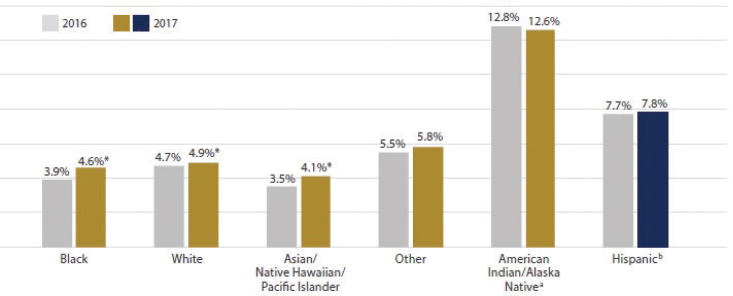
* Change is significant at the 90% confidence level.
a Indian Health Service is not considered insurance coverage by the Census Bureau. See the methodology section for more information.
b Hispanic refers to a person’s ethnicity, and these children may be of any race. See the methodology section for more information.
SOURCE: Alker and Pham, 2018.
and ethnic groups at 12.8 percent in 2016 and 12.6 percent in 2017 (Alker and Pham, 2018). In 2017, 27 states and Washington, DC, had significantly lower rates of children without insurance than the national rate of 5.0 percent, and 11 states had no statistically significant difference from the national rate. However, 12 states had significantly higher rates, with the highest rates of children without insurance in Texas (10.7 percent), Alaska (9.6 percent), and Wyoming (9.5 percent).
MATERNAL HEALTH IN THE UNITED STATES
Women in other high-income countries fare better in terms of access to health care and health status than women in the United States. U.S. women in have the highest rate of maternal mortality because of complications from pregnancy or childbirth and among the highest rates of cesarean sections, and maternal mortality rates are rising for them while declining in other countries (see Figure 1-6). For the past six decades, black women have died at a rate that ranges from three to four times that of white women, with 38.9 deaths per 100,000 live births among black women versus 12 deaths per 100,000 live births among white women as of 2010 (Creanga et al., 2015; MHTF, n.d.). AI/AN women also fare worse than white women, with approximately twice as many pregnancy-related deaths per 100,000 live births. Some researchers point to structural drivers of maternal mortality disparities in the United States, such as racism
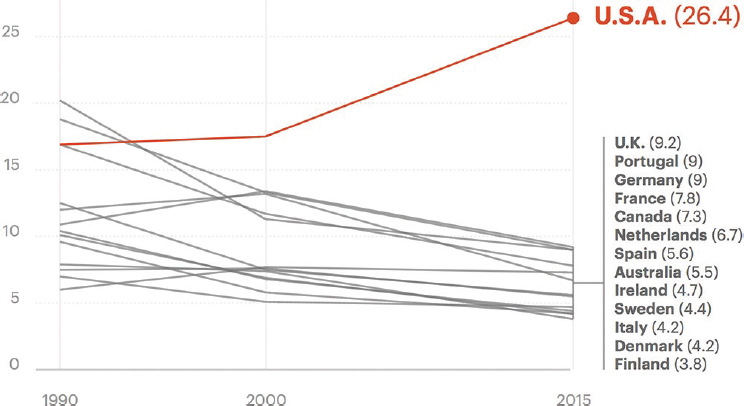
NOTE: Data from GBD 2015 Maternal Mortality Collaborators, 2016.
SOURCES: Martin and Montagne, 2017. Courtesy of Propublica.
and discrimination (ACOG, n.d.) and adverse changes in chronic diseases and insufficient health care access (Nelson et al., 2018). See Chapter 5 for a detailed overview of preconception through postpartum care.
Prenatal Care
Access to prenatal care varies across race and ethnicity groups. In 2016, about 77 percent of women who gave birth initiated prenatal care in the first trimester. However, only 66.5 percent of black, 72.0 percent of Hispanic, 63.0 percent of AI/AN, and 55.9 percent of Native Hawaiian or other Pacific Islander women received it, whereas 82.3 percent of non-Hispanic white women did (Osterman and Martin, 2018). People of color are much more likely to be affected by late initiation of prenatal care, which is most common in Pacific Islanders at 18.4 percent, with non-Hispanic white women at 3.3 percent. AI/AN women have a 9.2 percent chance of late prenatal care initiation, and black women have a 7.0 percent chance (Osterman and Martin, 2018). (See Chapter 5 for more statistics and information on prenatal care.)
CURRENT ENVIRONMENT FOR CHILDREN AND FAMILIES
In the past 20 years, much has changed in the landscape in which prenatal to childhood development takes place in the policy and funding environment and the social, economic, and cultural context. The following section outlines some of these important changes.
Changes in the Funding and Policy Environment
Federal spending (not including tax reductions) on children under 18 increased from $210 billion in 2000 to $375 billion in 2017, driven largely by increased health spending on Medicaid, which nearly tripled between 2000 and 2017, and the Children’s Health Insurance Program (CHIP) (Isaacs et al., 2018) (see Table 1-1). Federal spending on nutrition, income security, ECE, and housing also increased substantially between 2000 and 2010, though many programs have seen a decline in federal support since 2010. Approximately 61 percent of federal expenditures in 2017 served children in low-income families through means-tested programs and tax provisions (Isaacs et al., 2018).
Altogether, federal spending on children in 2017 accounted for 9.4 percent of total federal outlays (see Figure 1-7), and it is projected to fall to 6.9 percent. In contrast, federal spending on adults through Social Security, Medicare, and Medicaid accounted for 45 percent of total federal outlays, which is projected to grow to 50 percent by 2028 (Isaacs et al., 2018). It should also be noted that federal spending on children
TABLE 1-1 Federal Expenditures on Children by Program, Selected Years 1960–2017
| 1960 | 1980 | 2000 | 2010 | 2017 | |
|---|---|---|---|---|---|
| 1. Health | 0.2 | 7.6 | 36.8 | 95.1 | 111.9 |
| Medicaid | — | 6.9 | 32.8 | 80.7 | 89.9 |
| CHIP | — | — | 1.7 | 8.5 | 15.4 |
| Vaccines for children | — | — | 0.7 | 4.0 | 4.4 |
| Other health | 0.2 | 0.8 | 1.6 | 1.9 | 2.1 |
| 2. Nutrition | 1.5 | 22.5 | 30.9 | 60.8 | 58.0 |
| SNAP (food stamps) | — | 11.7 | 13.4 | 36.1 | 30.6 |
| Child nutrition | 1.5 | 9.1 | 12.7 | 18.3 | 22.3 |
| Special Supplemental food (WIC) | — | 1.6 | 4.8 | 6.4 | 5.0 |
| 3. Income Security | 14.6 | 33.6 | 46.4 | 58.0 | 54.3 |
| Social Security | 7.0 | 17.7 | 18.6 | 22.3 | 20.8 |
| Temporary Assistance for Needy Families | 4.8 | 11.0 | 15.9 | 17.2 | 12.8 |
| Supplemental Security Income | — | 0.9 | 6.7 | 11.0 | 10.5 |
| Veterans benefits | 2.5 | 3.5 | 2.1 | 3.5 | 6.8 |
| Child support enforcement | — | 0.9 | 4.4 | 4.9 | 4.1 |
| Other income security | 0.3 | –0.4 | –1.3 | –1.0 | –0.6 |
| 4. Education | 3.0 | 18.7 | 30.3 | 76.1 | 41.6 |
| Education for the Disadvantaged (Title I, Part A) | — | 8.3 | 11.8 | 21.9 | 16.2 |
| Special education/IDEA | — | 2.1 | 6.9 | 19.4 | 12.7 |
| School improvement | — | 2.0 | 3.5 | 6.0 | 4.4 |
| Innovation and improvement | — | — | — | 1.1 | 1.3 |
| Impact Aid | 1.7 | 1.8 | 1.2 | 1.4 | 1.5 |
| Dependents’ schools abroad | 0.2 | 0.9 | 1.3 | 1.3 | 1.2 |
| Other education | 0.1 | 2.5 | 3.9 | 25.1 | 4.3 |
| 5. Early Education and Care | -- | 2.1 | 10.8 | 15.5 | 14.9 |
| Head Start (including Early Head Start) | — | 2.1 | 6.2 | 9.0 | 8.9 |
| Child Care and Development Fund | — | — | 4.6 | 6.6 | 5.7 |
| Other early education and care | — | — | — | — | 0.3 |
| 6. Social Services | — | 4.6 | 10.7 | 11.2 | 10.1 |
| Foster care | — | 0.8 | 6.0 | 4.9 | 4.9 |
| Adoption assistance | — | — | 0.2 | 2.6 | 2.5 |
| 1960 | 1980 | 2000 | 2010 | 2017 | |
|---|---|---|---|---|---|
| Other social services | — | 3.9 | 4.5 | 3.6 | 2.7 |
| 7. Housing | — | 2.8 | 8.3 | 10.7 | 9.5 |
| Section 8 low-income housing assistance | — | 1.4 | 6.5 | 8.0 | 7.7 |
| Low-rent public housing | — | 0.6 | 1.1 | 1.3 | 1.0 |
| Other housing | — | 0.8 | 0.8 | 1.4 | 0.7 |
| 8. Training | — | 6.4 | 1.5 | 2.2 | 1.2 |
| 9. Refundable Portions of Tax Credits | — | 3.1 | 34.5 | 81.8 | 74.0 |
| Earned income tax credit | — | 3.1 | 33.3 | 54.8 | 53.1 |
| Child tax credit | — | — | 1.1 | 25.4 | 19.4 |
| Premium tax credit | — | — | — | — | 0.6 |
| Other refundable tax credits | — | — | — | 1.6 | 0.8 |
| 10. Tax Reductions | 41.2 | 50.1 | 93.1 | 105.1 | 106.2 |
| Dependent exemption | 40.6 | 42.3 | 39.7 | 36.0 | 37.8 |
| Exclusion for employer-sponsored health insurance | NA | 4.1 | 13.7 | 21.5 | 22.9 |
| Child tax credit (nonrefundable portion) | — | — | 26.8 | 33.4 | 29.9 |
| Earned income tax credit (nonrefundable portion) | — | 1.8 | 5.9 | 5.3 | 7.0 |
| Dependent care credit | — | — | 3.2 | 3.8 | 3.3 |
| Other tax reductions | 0.7 | 1.9 | 3.7 | 5.1 | 5.3 |
| TOTAL EXPENDITURES ON CHILDREN | 60.5 | 151.5 | 303.2 | 516.4 | 481.5 |
| OUTLAYS SUBTOTAL (1–9) | 19.3 | 101.4 | 210.1 | 411.3 | 375.3 |
NOTES: Numbers in billions of 2017 U.S. dollars. CHIP = Children’s Health Insurance Program; IDEA = Individuals with Disabilities Education Act; SNAP = Supplemental Nutrition Assistance Program; WIC = Special Supplemental Nutrition Program for Women, Infants, and Children.
SOURCE: Isaacs et al., 2018.
(which accounted for 34 percent of total public spending on children) in 2017 represented only 2 percent of the GDP in the United States, which is well below that of other developed nations. An international comparison of public spending on children from 1985 to 2000 ranked U.S. spending (2.4 percent of GDP) as the second lowest among 20 OECD countries, much less than the 9.6 percent median across OECD countries (Lynch, 2006).
One of the most important changes in the policy landscape over the past 20 years has been the Patient Protection and Affordable Care
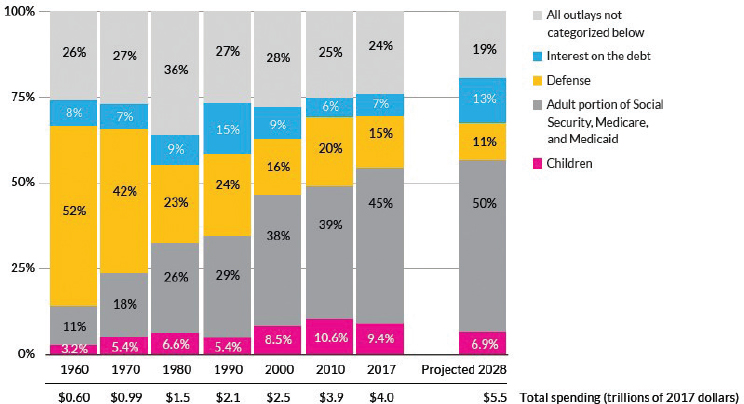
NOTES: Authors’ estimates based primarily on Congressional Budget Office, The Budget and Economic Outlook: 2018 to 2028 (Washington, DC: Congressional Budget Office, 2018), and Office of Management and Budget, Budget of the United States Government, Fiscal Year 2019 (Washington, DC: U.S. Government Printing Office, 2018) and past years. For more source information, see the appendix in Isaacs et al., 2018. Numbers may not sum to totals because of rounding.
SOURCE: Isaacs et al., 2018. Republished with permission of Urban Institute, from Kid’s Share 2018, Isaacs et al., 2018; permission conveyed through Copyright Clearance Center, Inc.
Act (ACA), which expanded health care access for children and families through a combination of Medicaid expansions, private insurance reforms, and premium tax credits (Kaiser Family Foundation, 2019). The uninsured rate among women ages 19–34 decreased from 25 percent in 2010 to 14 percent in 2016 (Gunja et al., 2017), which has significant implications for preconception and prenatal health. The ACA requires coverage for women’s preventive services at no cost-sharing, including well-woman visits, and eliminates exclusions for preexisting conditions (e.g., pregnancy and depression), which improves access for women with chronic conditions (Gunja et al., 2017). The ACA mandates coverage for essential health benefits (EHBs), which include maternity care and mental health services. For children, the ACA requires coverage for preventive services at no cost-sharing and EHBs, eliminated exclusions for preexisting conditions, and prohibits lifetime dollar limits, which improves access for children with special health care needs (National MCH Workforce Development Center, 2015). Even though the ACA did
not substantially increase children’s eligibility for Medicaid (or CHIP), the process of parents seeking enrollment in Medicaid or exchange plans led to their learning of their children’s eligibility, which increased child enrollment substantially. Presently, it is unclear how recent policy changes to deregulate consumer protections under the ACA and to restrict eligibility, enrollment, and benefits through Medicaid waivers will impact health care access and equity for children and families. (See Chapter 5 for more about the ACA.)
Federal funding for ECE has steadily increased over the past 10 years; however, total spending on ECE in the United States remains limited. Only 0.5 percent of the U.S. GDP is spent on ECE, whereas other peer nations spend 1 percent or more (OECD, 2019). Recent increases include lawmakers approving an $890 million increase for Early Head Start and Head Start, including $170 million for Early Head Start—Child Care Partnerships, from fiscal year (FY) 2016 levels to FY 2019 levels (FFYF, 2018; see Chapter 7 for more on these programs). In addition, in response to decades of early childhood and brain development research, policy makers, advocates, program administrators, and other leaders in the child care community have advanced a number of policies and initiatives that recognize child care programs as opportunities to improve children’s development rather than solely as work-support programs. As a result, for example, the most recent reauthorization of the Child Care Development Block Grant8 provides for more continuity of care by allowing parents to receive subsidies for 1 year, even if their income, work, or education status changes during that period. There has also been more attention paid to increased compensation for the workforce. For example, states and local communities have developed a number of strategies to enhance compensation for early childhood educators, including tax credits, wage supplements (often tied to attaining higher education or credentials), targeted increases for child care subsidy rates, salary scales, provision of benefits, and parity with K–12 teachers. More recently, there has been greater recognition from policy makers, advocates, and ECE practitioners of the importance of ECE program leaders (including elementary school principals).
CHANGES IN THE ECONOMIC, SOCIAL, AND CULTURAL ENVIRONMENT
Income inequality has been growing—the income gap between higher- and lower-income individuals has increased substantially over the past
___________________
8 See https://www.acf.hhs.gov/occ/ccdf-reauthorization (accessed July 29, 2019).
30 years (NASEM, 2017).9 Those with incomes in the top 10 percent average 9 times the income of those in the bottom 90 percent, and those with incomes in the top 0.1 percent have more than 188 times the income of the bottom 90 percent (Inequality.org, n.d.). Lasting effects of the 2008 recession include displacement of vulnerable populations, which exacerbated the impact on both their health and their economic well-being and resulted in greater income inequality and wealth inequality (Smeeding, 2012).
People of color continue to face structural barriers when it comes to securing quality housing, health care, employment, and education (NASEM, 2017; Pager and Shepherd, 2008). For example, data suggest that schools are becoming increasingly segregated by poverty and race, which has implications for which communities have access to high-quality, well-funded education (Boschma and Brownstein, 2016; Darling-Hammond, 1998). Racism also continues to be a pressing problem, and it is built into systems, as seen by racial profiling by law enforcement officers, disproportionate suspension and expulsion rates of young boys of color (see Chapter 7), and the difficulty that some subgroups have in breaking the cycle of poverty (see Chapter 6). Chapter 3 expands on these issues and the impact they have on the health of children and families.
In terms of family structure, American families have changed, with a Pew Research Center (2015b) survey finding that there is no longer one dominant family type in the United States today (as compared to 1980, where 61 percent of children were living with married parents in their first marriage—today, that number is 46 percent) (see Figure 1-8). Pew also found, for example, that two-parent households are no longer the norm as rates of divorce, remarriage, and cohabitation have increased. This decline has been offset by an almost threefold increase in those living with just one parent—typically the mother (10.5 percent of children age 18 or younger lived with only a mother in 2018, compared to 2.4 percent living with the father only [U.S. Census, 2018]). Women who are single or living with a nonmarital partner account for 4 in 10 births in the United States. Single-parent families are more than 4 times more likely to be poor than are two-parent families (Pascoe et al., 2016), and this can affect their ability to invest time and resources in their children, which would have longer-term implications for the persistence of poverty across generations. More mothers (of children 18 or younger) have also entered the workforce (70 percent), with 40 percent of them being the primary earner (Pew Research Center, 2015a).
___________________
9 There are several different ways to measure income inequality, including the use of different datasets, that lead to different results (with no single source that illustrates all of the major trends in inequality) (CBPP, 2018). However, regardless of the method or data used, results consistently show an increase in income inequality in the past three decades. See a draft paper by Auten and Splinter (2018) for additional analysis that argues that income inequality has not grown as much as others have estimated.
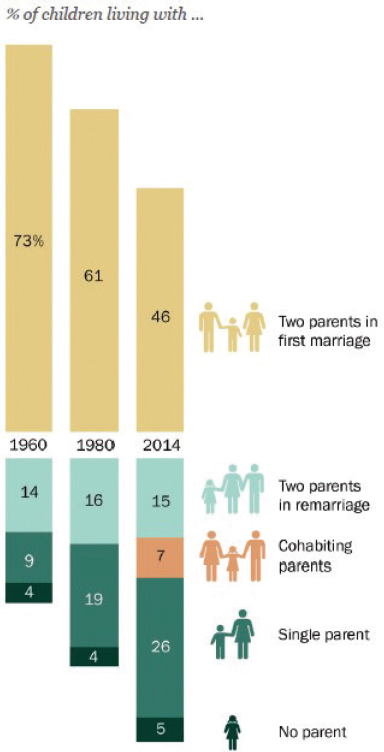
NOTES: Based on children under 18. Data regarding cohabitation are not available for 1960 and 1980; in those years, children with cohabiting parents are included in “one parent.” For 2014, the total share of children living with two married parents is 62 percent after rounding. Figures do not add up to 100 percent due to rounding. Data are sourced from Pew Research Center’s analysis of 1960 and 1980 decennial census and 2014 American Community Survey.
SOURCE: Pew Research Center, 2015b.
The makeup of children in the United States has changed as well. In 2000, 61 percent of all U.S. children were non-Hispanic white; in 2016 that number was 51 percent, with the proportion of children with Hispanic origins growing from 17 to 25 percent between 2000 and 2016. The percentage of non-Hispanic black children has stayed relatively constant since 1980 (14 to 15 percent) (Child Trends, 2018c). From 1994
to 2017, the population of children of immigrants10 grew by 51 percent, from 18 to 27 percent (Child Trends, 2018a). These children are mainly second-generation immigrants (16.7 million), with first-generation immigrants making up a much smaller number (2.9 million, which is 3 to 5 percent of all children). In 2016, 33 percent of U.S. children lived in a household where more than one language is spoken (dual-language learners), with Spanish being the most common other language for these children (Child Trends, 2016).
Evidence shows that populations from immigrant backgrounds and ethnic and racial enclaves might bring or develop particular child-rearing practices that lead to strengths and weaknesses in their children’s adaptations and success in other environments. For example, Galindo and Fuller (2010) have shown that Latino children have higher social-emotional skills in preschool but some of the academic skills of low-income Latino children lag beyond other groups. School success as measured by grades is associated with different family constellations and practices in immigrant populations, such as Cambodian, Dominican, and Portuguese populations (García Coll and Kerivan Marks, 2009). When examining cultural variation, no particular parenting or household composition is associated with success across all domains of child outcomes, aside from preventing extreme neglect, abuse, or lack of stimulation.
A more general cultural shift has been the increase in personal-use technology (e.g., computers, tablets, mobile phones), which has advanced at a rapid pace in the past 20 years. The divide in access to digital devices has decreased significantly, with more families having access to smart-phones across socioeconomic lines. Access to other devices, however, continues to create a digital divide that children in non-mainstream populations have to surpass. School districts across the country are integrating technology into the classroom. The health care field has advanced in the area of telehealth, providing greater remote access to health care providers. This access can have positive and negative effects, and it can even increase inequities when not used properly.
ABOUT THIS REPORT
Report Conceptual Model
The committee’s conceptual model (see Figure 1-9) served as a unifying framework for the committee’s approach to the report, aiming to improve prenatal through early childhood development with a health equity approach. The model adapts elements and concepts from the
___________________
10 Immigrant children are defined here as those who have at least one foreign-born parent.
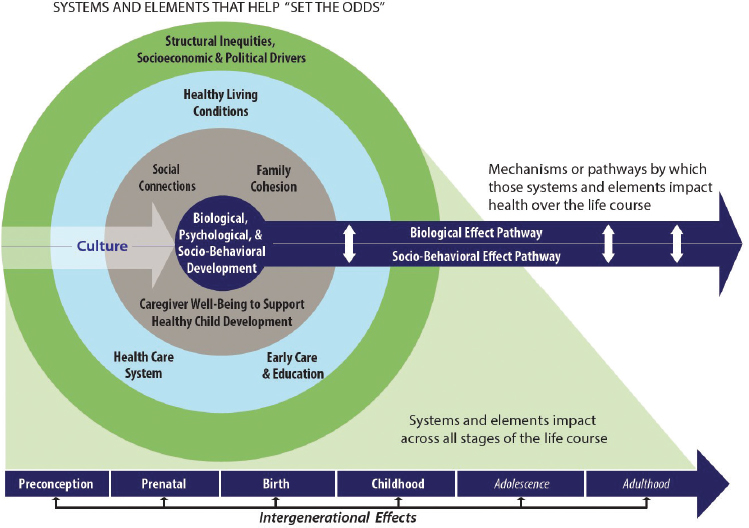
NOTE: The elements and systems included in the nested circles impact every stage of the life course.
World Health Organization (WHO) Commission on Social Determinants of Health conceptual framework (WHO, 2010), the socio-ecological model (Bronfenbrenner, 1979; McLeroy et al., 1988; NASEM, 2017; Velez-Agosto et al., 2017), a model of children’s health and its influences (NRC and IOM, 2004), and the life course health development model (Halfon et al., 2014).
Building on the life course model, this figure shows early development within the context of the life course stages, beginning with preconception and ending with adulthood along the bottom. It is important to note that risk and protective factors can be transferred intergenerationally, which makes the parent or primary caregiver and/or the parent–child dyad a central focus of intervention. With the necessary supports and conditions, healthy biological, socio-emotional, cognitive, and socio-behavioral development increase across the life course.
Within the context of the life course, the diagram’s nested circles illustrate the complex sociocultural environment that shapes development at the individual level and the opportunities for interventions to improve individual health and developmental outcomes and population health, well-being, and health equity. The context and conditions here continue
to play an important role in health and well-being throughout the life course. Individual social and biological mechanisms operate and interact within and across the three levels.
The outer level, “socioeconomic and political drivers,” is adapted from the WHO social determinants framework and represents the level at which structural inequities operate. These structural inequities are deeply embedded into policies, laws, governance, and culture; they organize the distribution of power and resources differentially across characteristics of identity (i.e., race, ethnicity, gender, class, sexual orientation, and others) (NASEM, 2017; WHO, 2010).
The next level represents social, economic, and environmental conditions (i.e., the SDOH): education, employment, health systems and services, housing, income and wealth, physical environment, transportation, public safety, and social environment. In the model, these nine interdependent factors are grouped into three domains that the committee has identified, based on the available evidence and existing resources, as important for targeting prenatal and early childhood interventions: healthy living conditions, ECE, and health systems and services. These domains in the gray and light blue circles are the primary foci of Chapters 5–7, and each is discussed in terms of evidence-based solutions, opportunities for intervention, barriers, promising models, and research needs.
The next level represents the factors that most directly and proximally shape children’s daily experiences and routine patterns; these include caregiver well-being and support and attachment and family cohesion, which affect social connections in early life.
Culture, according to Velez-Agosto and colleagues (2017), operates at various levels, including all of the levels in the committee’s conceptual model. Systems, such as ECE and health care, have cultures and also enact in their daily operations ways of conceptualizing the child’s development, how to promote it, and what resources have to be accessed in order to correct illness and developmental problems. Cultures can also be sources of strength, providing support for coping with life demands and toxic stress (García Coll et al., 1996). Families and communities also have cultures that are similarly enacted in daily routines and in developmental goals and expectations. Inequities might arise from lack of understanding of normative cultural frameworks between any of these levels, lack of respect and acceptance for different ways of being that are considered normative in other settings, and lack of access to critical resources, such as high-quality ECE and health care, due to racism and discrimination (García Coll et al., 1996).
Types of Interventions
The committee deployed lessons from the latest insights in neurobiological and closed-behavioral sciences that define how early childhood experiences translate into health outcomes and inequities across the life course in order to offer promising practices or transformational levers that might help move the needle in a positive direction. In its Statement of Task (see Box 1-3), the committee was asked to look at interventions defined as policies, programs, or system changes. What is meant by each of these is briefly described below (see Box 1-5 for examples).
Systems
Systems are a collection of interacting, interdependent parts that function as a whole. For the purposes of this report, most of the systems are social constructs and are organized around a key functional area (education, health care, criminal justice). Systems have existing patterns and
structures that define how people tend to move through them. A few essential features that define a system include
- Structures: The essential organizational components of a system, including how it is governed.
- Flows: How information, money, or people move through and are configured in relation to each other.
- Goals: The actions the system is trying to accomplish—its purpose or function.
- Rules and Norms: How a system is organized and what can and cannot happen within it.
- Paradigms: Assumptions that system makes that inform how things are organized and flow within it.
These features could be thought about in the context of a single system or considered through a social ecosystem lens and applied to how systems interact with each other.
Programs
A program is a targeted or specialized pathway by which a specific group of people move through a system or between a set of systems—a change in the system’s structures or flows for certain kinds of clients. It is often driven by a recognition that the standard approaches are not achieving the system’s goals for some people. Programs usually do not change the goals or rules or the system itself; rather, they generally offer a new way to achieve improved outcomes within the current system’s structures (such as a support group for new mothers offered in a primary care setting).
Policy
Policy is a shift in the overarching legal or regulatory structure that governs how systems operate or interact with one another. Policies usually set the rules, goals, norms, or paradigms within which systems establish structures and flows, and they may also set the limits on the types of exceptions or changes that systems can put in place. Some policies can impact large swathes of the population, such as laws, regulations, court rulings, administrative rules, or executive orders, and often have consequences when not followed. Some policies have a smaller scope, such as guidelines issued by professional organizations, recommendations of expert panels, or local programs.
In general, policies, systems, and programs can be thought of as nested within each other. The impact profile of efforts at any given level may be constrained by what is happening in the others—promising programs that do not consider the potential limitations that the policy environment places on potential adoption and spread will not be as useful as those that do.
Committee’s Methodology
As discussed above, an intervention could consist of policies, programs, or system changes, or a combination of those approaches. The literature on the effectiveness and applicability of interventions provides important information for assessing which interventions are most effective and suitable for a general or more specific population. However, many interventions have not been adequately evaluated for their effectiveness—in general, for a specific outcome, or when brought to scale. In addition, studies vary in dimensions such as appropriateness of design and setting, quality of execution, interactions with other interventions, and consideration of economic consequences.
With the above in mind, the committee examined the available literature, conducting a comprehensive review from the peer-reviewed and gray literature.11 This entailed a systematic search of academic and governmental databases and websites for studies that evaluated or assessed the effects of interventions. Where possible, the committee relied on existing systematic reviews and meta-analyses with strong methodologies and existing comprehensive reviews.
Comparisons across studies are needed to better assess intervention opportunities; however, such comparisons are often not available or difficult to interpret due to methodological strengths and limitations relating to the nature of the study design and the data collected. For example, what is considered the gold standard research design to show that a program does in fact lead to the results it is trying to achieve—the randomized controlled trial (RCT)—may not always be feasible. This is because RCTs are not appropriate in all settings, particularly not to study community-level interventions, and for some interventions, randomization can be considered ethically objectionable if it denies a service or treatment known to be beneficial (Center on the Developing Child at Harvard University, 2016). While large-scale, multiyear RCTs will continue to be
___________________
11 The date range for the search was 2013–2019. Search terms included the following categories: prenatal and early childhood, neurobiological, socio-behavioral, biology/biomarkers, health indicators/outcomes, structural inequities, social determinants of health, and model/intervention.
important to demonstrate program impacts, there is also an important role for short-term, flexible study methodologies to test program components and subgroup variability and allow for mid-course corrections and enhancements (such corrections are not possible in traditional RCTs) (Center on the Developing Child at Harvard University, 2016). While there is nothing fundamental in the design of an RCT that precludes investigating heterogeneous effects in different populations, to do so requires careful consideration of the sample size and identification of subgroups of interest prior to the randomization. As a result, many RCTs have not been able to answer important questions about variability in effects across subpopulations or which components of an intervention are driving the results. While RCTs can be used to study the effect of separate program components, it is difficult to use RCTs to examine complex programs with multiple dimensions (or for community-level interventions). RCTs remain a critical tool for studying the effectiveness of programs, but it is important to note their limitations as well. (See Chapter 8 for a research recommendation on this topic.)
Because of the limitations of RCTs in some contexts, and limitations of observational studies that are correlational in nature, researchers have increasingly used “natural experiments” to estimate causal effects. Such studies harness changes in state and local policies that generate plausibly random or quasi-random variation in exposure to a given service or treatment to estimate its causal effect on outcomes of interest (see Angrist and Pischke, 2009, for an overview of these methods). Despite the limitations of estimation based on observational data, careful use of observational data has many advantages. First, it is very useful for identifying associations that can be more rigorously studied using other approaches. Second, in some cases, careful use of natural experiments or other research designs can minimize the bias from confounding. Finally, some questions are, by their nature, not amenable to randomized trials and so can only be studied using observational data. The way data are gathered across study designs also varies, as data collection may occur for different outcomes at different points in time, so the data may be incomplete and therefore hard to compare.
When reviewing the science on a certain intervention or policy, there may be cases with strong evidence for one or more important outcomes and weaker (or mixed, or null) evidence for one or more other outcomes. This does not mean that the intervention or policy should not be considered or implemented. If there is a strong theoretical basis for making the change (e.g., from a biological pathway or development standpoint) and strong evidence for one or more salient health outcomes that is being targeted and has a large population health impact, the intervention or policy could be deemed appropriate despite its limitations. This is true for several interventions and policies recommended in this report.
About the Report Recommendations
The committee provides a range of recommendations for practice, policy, and systems change, including recommendations that will take time and sustained commitment to achieve and recommendations that could be implemented immediately or in the near term. Some of the committee’s recommendations will be difficult to implement; however, the degree of difficulty in implementing any given recommendation does not mean it is not worth pursuing. Achieving health equity for children will require attention and commitment from a range of sectors. For example, in Chapter 8, the committee discusses the need for better alignment among the many children- and family-serving sectors in the United States. Although there are many barriers to achieving alignment, there is also great opportunity to make long-lasting reductions in long-standing and persistent inequities. Furthermore, inequities that originate at the system and institutional levels will require solutions that target policy and structures. Given this understanding, the committee provides the recommendations with the long-term outcomes in mind and the goal of both improving the current state and making strides today to establish systems where inequities will no longer be the status quo. Where possible, the committee also recommends or highlights ways to leverage existing programs that either embrace the core scientific principles laid out in this report (see the Core Concepts below and Chapter 2) or have a strong basic structure from which to build (e.g., home visiting). Therefore, the committee makes some recommendations for improving programs that are not optimally or extensively implemented but have the potential to be updated, scaled, or better used to promote related services that advance health equity.
Given the fragmented nature of many systems in the United States (e.g., the health care system has both public and private payers and multiple entities that set guidelines for care and accountability), many of the committee’s recommendations are directed to multiple actors with varying roles and responsibilities, each of whom is important to advancing child and family outcomes. Furthermore, as a matter of jurisdiction, some recommendations are better targeted to varying levels of government (e.g., local, state, tribal, and territorial). To address deeply rooted inequities, which play out across multiple sectors, some recommendations entail a comprehensive approach that requires partnerships across sectors and levels of government—this is consistent with Communities in Action (NASEM, 2017), which identifies cross-sector collaboration as a key element for promoting health equity in communities.
Resources Resources will be needed to implement many of the recommendations in this report. The root causes of structural inequities are
found in differential access by virtue of race or ethnicity to resources for some groups, due in part to certain laws and policies (NASEM, 2017; see also Chapter 3). Calling for change of any kind to advance health equity will require changes to laws, policies, and other sources of inequity so as not to perpetuate structural racism and discrimination. Decision makers and leaders can coordinate, integrate services, and educate on all of these issues, but if the resources are not there to back the needed changes, the change likely will not occur. The committee was asked by RWJF to identify what practice, policy, and systems changes need to be implemented, based on what is known from developmental science; however, the committee was not tasked to identify the sources or mechanisms for funding those changes. In a few instances, the committee was able to provide estimates of the potential costs for implementing its recommendations using existing estimates. Doing so, however, was complicated when those estimates did not include cost savings from improved health outcomes resulting from the intervention, producing a one-sided picture.
Although the committee was not asked to identify the mechanisms and sources for implementing the report recommendations, there are many extant mechanisms and proposals for funding various public or population health activities. For example, taxes on tobacco, alcohol, and other products (such as sugary beverages) have been used to channel resources and shape economic incentives (NASEM, 2018b). An IOM (2012) committee proposed establishing a tax on medical care transactions to provide a long-term financing structure to cover public health services. Other mechanisms—both within and outside the health sector—include federal or state Wellness Trusts (Prevention Institute, 2015), hospital community benefit expenditures (Rosenbaum et al., 2015), community wealth building (including the role of anchor institutions; see Porter et al., 2019), and Children’s Services Councils.12 (A National Academies Proceedings of a Workshop—in Brief [NASEM, 2018b] provides an overview of several of these options and others.) Each of these financing mechanisms has advantages and disadvantages that would need to be weighed for the specific intervention or program for which it is considered.
Promising Models
In its Statement of Task, the committee was asked to identify promising examples of models that apply the science of early development to health equity. The committee adapted the selection criteria used in the Communities in Action: Pathways to Health Equity (NASEM, 2017) report
___________________
12 See, for example, http://flchildrenscouncil.org/about-cscs/overview (accessed June 17, 2019).
to guide this process.13 The committee used the three sets of criteria from the 2017 National Academies report (see Appendix A for a list of all of the selection criteria), which were informed by research and practice-based evidence and the expertise of the committee members. The committee made a few additions based on the focus of this report (the prenatal through early childhood period) and removed those not relevant to this study. The first set consists of six core criteria, which need to be met by all of the promising models. These core criteria ensure that the examples chosen are substantively significant. The committee used these promising models as examples throughout the report to highlight bright spots that have been able to use what is known from the science to advance health equity in the preconception through early childhood periods. Furthermore, “promising” does not imply that the model is new but rather that it is a program or intervention that met the committee’s core criteria, and each promising model has a unique approach and is at a different phase of development: some have been around for more than 30 years and have changed based on evaluations or input from users, while others have emerged in the past few years. In Chapters 4–7, three promising models were identified for each chapter (each model is summarized in a box). These examples are not blueprints, and exact replicas might not work with all populations or locations; however, the lessons learned and approaches used prove valuable to those working to create positive change toward health equity during the preconception through early childhood periods. Note that throughout the report, the committee cites many other examples of current practices and programs that illustrate the topic being discussed; however, those examples may not meet all of the committee’s criteria (and are not labeled as promising models).
The first core criterion requires that the model’s main focus be during the prenatal and/or early childhood period, as that is the focus of this report; this inevitably involves the mother (or other primary caregiver). The second notes that the intervention is informed by findings from the neurobiological, socio-behavioral, and/or biological sciences—also a focus of this report.
The third core criterion is that the model addresses at least one (preferably more) of the nine SDOH identified by the 2017 National Academies report: education, employment, health systems and services, housing, income and wealth, the physical environment, public safety, the social environment, and transportation. “This criterion was informed by the wealth of literature suggesting the importance of targeting the social and economic conditions that affect health, especially at the community
___________________
13 The original criteria from the 2017 National Academies report are available at https://www.nap.edu/read/24624/chapter/7#323 (accessed July 29, 2019).
level” (Bradley et al., 2016; Galea et al., 2011; Heiman and Artiga, 2015; Hood et al., 2016; NASEM, 2017; Wenger, 2012). Furthermore, this criterion is basic to the committee’s charge, which posits that the SDOH need to be addressed to reduce health inequities. The fourth criterion is that the model is designed to have or has evidence of having an impact on a group or population that experiences health inequities.
The fifth core criterion “states that the solution needs to be multisectoral, meaning that it engages one or more sectors” (ideally, at least one “nontraditional” sector, meaning other than public health or health care). Multisector collaboration is a powerful lever for addressing health inequities and building a culture of health (APHA, 2015; Danaher, 2011; Davis et al., 2016; Kottke et al., 2016; Mattessich and Rausch, 2014). Engaging stakeholders across multiple sectors provides the opportunity for innovative and cost-effective methods to sustain solutions at the community level (NASEM, 2017).
The sixth core criterion requires the solution to be evidence informed.
This entails an assessment of evidence or the best available information to identify a problem and develop a solution that has a measurable outcome. Here, there is considerable flexibility in terms of the type of evidence that will qualify. This flexibility is based on the understanding that low-resource communities that suffer from health inequities often do not have the infrastructure, personnel, or financial resources to provide the highest standard of evidence. (NASEM, 2017, p. 326)
The sixth core criterion is that there needs to be an evaluation plan with identified outcome measures to track the impact of the intervention.
The second set of criteria—aspirational criteria—reflects the elements, processes, and outcomes of interventions that the committee identified as valuable for promoting health equity. This set of criteria highlights important features of interventions, such as nontraditional partners or nonhealth domains (e.g., community organizers, public libraries, Parent Teacher Association groups) and an intervention being interdisciplinary and/or multilevel (the intervention has multiple levels of influence, such as individual, family, organizational/institutional, or governmental).
THE SCIENCE OF EARLY DEVELOPMENT: CORE CONCEPTS
Based on its review of the science, the committee updated the core concepts from the 2000 NRC and IOM report From Neurons to Neighborhoods and identified 12 core concepts of early development, with a focus on equity. The evidence behind these concepts is described in Chapters 2–4, and this evidence guided the committee in developing recommendations that are responsive to the science of early development.
- Biology–environment interaction impacts health and development: Human long-term social, emotional, behavioral, cognitive, and physical health is shaped by genetic, epigenetic, and environmental factors that integrate biological information at the level of molecular, cellular, and organ systems with the family, neighborhood, and culture in which the individual is embedded. These developmental processes start before conception through a dynamic and continuous interaction between biology and aspects of the environment and extend throughout the life-span.
- Brain development proceeds in well-defined but continuous steps: Human developmental processes are now conceptualized as continuous, rather than occurring in discrete stages as was originally thought. A sequence of temporally well-defined sensitive periods (sometimes referred to as “critical periods”) of brain maturation—in tandem with environmental influences—lead to the acquisition of social, emotional, and cognitive skills. During these sensitive periods, early adverse experiences influence brain development and can alter the trajectories of development in each of these functional domains, impacting long-term well-being.
- Major physiological systems develop rapidly in pregnancy and early childhood: It is now known that physiological systems other than the brain, such as the immune system, microbiome, and endocrine system, can also be influenced preconceptionally. Like the brain, these systems begin to develop prenatally, with early sensitive pre- and postnatal periods that can be disrupted by early adversity. These early influences can have long-term consequences for mental and physical health.
- The early caregiving environment is crucial for long-term development: The family and community caregiving professionals have a central role in early childhood development, indicating the need for a multigenerational approach to ensuring optimal growth and development. The child thrives in healthy relationships throughout childhood, but relationships with parents are the building blocks for subsequent relationships and child outcomes. For example, maternal–child interactions impact the well-being of both mother and child, where a positive mother–child relationship rests on good maternal well-being (whereas prolonged maternal distress impairs parenting and the quality of attachment).
- The developing child plays an important role in interactions and development: Children are active participants in their own development, reflecting the intrinsic human drive to explore and master one’s environment. Early experiences create biological
- structures, and shape psychological and behavioral adjustment, in ways that influence how the child will react and act in response to later environmental demands.
- The development of executive functions14 is a key aspect of early childhood development: The emergence and maturation of executive functions (inhibitory control, mental flexibility, and working memory) are a cornerstone of early childhood development. Executive function maturation continues through early adulthood and contributes to the health, well-being, and productivity of adults.
- Trajectories—positive or negative—are not immutable: The developing child remains vulnerable to risks and open to protective influences through adolescence and young adulthood, although early life represents the stage at which interventions are most effective in positively influencing a child’s development.
- There is variability of individual and group development: Individual children demonstrate significant variability in these sensitive periods of brain development and in response to interventions. This variability often makes it difficult to distinguish among typical development, maturational delays, transient disorders, and persistent impairments or to predict response to treatment. Understanding this heterogeneity of development and individual differences in access and responsiveness to interventions is a major goal.
- Experiences across environmental contexts play a significant role in early development: Children can be more or less sensitive to experiences due in part to their biological makeup, but this is impacted powerfully by multiple family and community factors. These include family interactions and adversity, accessibility to community programs and interventions, and environmental factors, such as quality and stability of housing, toxic environmental exposures, food accessibility, early childhood education, family support, and culture. Effective interventions can alter the course of development throughout childhood by changing the balance between risk and protective processes, leading to more adaptive outcomes.
___________________
14 Executive function (and self-regulation) skills “are the mental processes that enable us to plan, focus attention, remember instructions, and juggle multiple tasks successfully. Just as an air traffic control system at a busy airport safely manages the arrivals and departures of many aircraft on multiple runways, the brain needs this skill set to filter distractions, prioritize tasks, set and achieve goals, and control impulses” (Center for the Developing Child at Harvard University, see https://developingchild.harvard.edu/science/key-concepts/executive-function [accessed June 17, 2019]).
- Disparities in access to critical resources matter: Disparities in health and developmental outcomes result from not only health care disparities but also disparities and inequities in family and community factors. Achieving equity in health and developmental outcomes in young children requires addressing health care disparities and also ensuring those family and neighborhood conditions in which all children and families can be healthy and thriving.
- Health outcomes are the result of experiences across the life course: Birth and early developmental outcomes are influenced by the health of the mother and father not only during pregnancy but also before and between pregnancies and across the life course, starting with their own prenatal and early life experiences. Disparities in the child’s birth and early developmental outcomes are therefore the consequences of not only differential exposures during pregnancy and early childhood but of differential parental life course trajectories set forth by early programming mechanisms and influenced by cumulative life adversity.
- Early interventions matter and are generally more cost effective than later ones: Family-based interventions that consider both risk and resilience and are informed by or sensitive to the mores and values of the target population can potentially positively change developmental pathways. The integration of various levels of services that are community based and have supportive policies in place tends to be more effective.
OVERVIEW OF THE STUDY PROCESS AND REPORT
To address its charge, the committee gathered information through a variety of means. It held two information-gathering meetings that were webcast live, in August and October 2018 (the meeting agendas are listed in Appendix B). The committee also held deliberative meetings throughout the study process. The committee received public submissions of materials for its consideration throughout the course of the study.15 The committee’s online activity page provided information to the public about its work and facilitated communication with the public.16
Throughout this report, the committee provides conclusions and recommendations. Chapter 2 provides an overview of healthy development from conception through early childhood, including what is new in the science of development since the publication of From Neurons to Neighborhoods (NRC and IOM, 2000). It aims to demystify the “black box”
___________________
15 Public access materials can be requested from paro@nas.edu.
16 See nationalacademies.org/earlydevelopment (accessed July 29, 2019).
of development for the public, practitioners that work with children, and policy makers and to convey that we know enough about early development to act now to advance health equity for children and families. Chapter 3 provides an overview of the critical influences or factors that can either promote or hinder healthy development, with a focus on factors that shape inequities at the child/family level and the community and population levels across the SDOH. Chapter 4 focuses on how to best foster children’s healthy psychosocial development, emotional adjustment, and physical health using what science has shown about risk and resilience and the importance of healthy relationships among children and families in high-risk contexts. Chapter 5 explores the role of the health care system in advancing health equity and what the system would need to look like from preconception through early childhood to meet the developmental needs of children. Chapter 6 provides recommendations on how to better meet the fundamental needs of families and children through economic security, stable and safe housing, and protection from environmental toxicants. Chapter 7 discusses the critical role of ECE and how it can serve as a platform for advancing health equity for children and families. Chapter 8 addresses needed systems changes and summarizes the opportunities to overcome barriers to strengthen a systems approach, the key stakeholders who need to be involved, and necessary alignment, measures, and research based on the committee’s assessment of the literature in Chapters 2–7. Finally, Chapter 9 highlights the main findings and concepts discussed throughout this report and summarizes the report recommendations, laying out a roadmap for applying and advancing the science of early development.
CONCLUDING OBSERVATIONS
The science of early development is clear. Long-term physical health and emotional, behavioral, social, and cognitive competence is shaped by genetic, epigenetic, and environmental factors, including their interactions, before conception and through the life-span. There are risk factors that necessitate action at the practice, policy, and systems levels that take into account the full range of factors that impact health and well-being. These actions need to be taken before insults to early development occur; however, the science of plasticity indicates that it is never too late to intervene. These actions need to take a life course, multigenerational approach to make progress on health inequity, because the well-being of a child depends on the well-being of a parent/caregiver. Multipronged, cross-sector interventions, focused on prevention, early detection, and mitigation and working at the policy, system, and program levels, are needed to move toward health equity.
REFERENCES
ACOG (American College of Obstetricians and Gynecologists). n.d. Racial disparities in maternal mortality in the United States: The postpartum period is a missed opportunity for action. https://www.acog.org/-/media/Departments/Toolkits-for-Health-Care-Providers/Postpartum-Toolkit/ppt-racial.pdf?dmc=1&ts=20190716T2208336641 (accessed July 16, 2019).
Alker, J., and O. Pham. 2018. Nation’s progress on children’s health coverage reverses course. Washington, DC: Georgetown University Health Policy Institute, Center for Children and Families.
Angrist, J. D., and J. Pischke. 2009. Mostly harmless econometrics: An empiricist’s companion. Princeton, NJ: Princeton University Press.
APHA (American Public Health Association). 2015. Opportunities for health collaboration: Leveraging community development investments to improve health in low-income neighborhoods. Washington, DC: American Public Health Association.
Auten, G., and D. Splinter. 2018. Income inequality in the United States: Using tax data to measure long-term trends. http://davidsplinter.com/AutenSplinter-Tax_Data_and_Inequality.pdf (accessed August 12, 2019).
Bellis, M., K. Hughes, K. Hardcastle, K. Ashton, K. Ford, Z. Quigg, and A. Davies. 2017. The impact of adverse childhood experiences on health service use across the life course using a retrospective cohort study. Journal of Health Services Research & Policy 22(3):168–177.
Bethell, C. D., P. Newacheck, E. Hawes, and N. Halfon. 2014. Adverse childhood experiences: Assessing the impact on health and school engagement and the mitigating role of resilience. Health Affairs 33(12):2106–2115.
Boschma, J., and R. Brownstein. 2016. The concentration of poverty in American schools. https://www.theatlantic.com/education/archive/2016/02/concentration-poverty-americanschools/471414 (accessed July 13, 2019).
Bradley, E. H., M. Canavan, E. Rogan, K. Talbert-Slagle, C. Ndumele, L. Taylor, and L. A. Curry. 2016. Variation in health outcomes: The role of spending on social services, public health, and health care, 2000–09. Health Affairs (Project Hope) 35(5):760–768.
Braveman, P., and C. Barclay. 2009. Health disparities beginning in childhood: A life-course perspective. Pediatrics 124(Suppl 3):S163–S175.
Bronfenbrenner, U. 1979. The ecology of human development: Experiments by nature and design. London: Harvard University Press.
Campbell, F., G. Conti, J. J. Heckman, S. H. Moon, R. Pinto, E. Pungello, and Y. Pan. 2014. Early childhood investments substantially boost adult health. Science 343(6178):1478–1485.
CBPP (Center on Budget and Policy Priorities). 2018. A guide to statistics on historical trends in income inequality. https://www.cbpp.org/research/poverty-and-inequality/a-guide-to-statistics-on-historical-trends-in-income-inequality (accessed July 13, 2019).
CDC (Centers for Disease Control and Prevention). 2016. Reproductive and birth outcomes. https://ephtracking.cdc.gov/showRbLBWGrowthRetardationEnv.action (accessed April 17, 2019).
CDC. 2019a. Division of nutrition, physical activity and obesity at a glance. https://www.cdc.gov/chronicdisease/resources/publications/aag/dnpao.htm (accessed July 13, 2019).
CDC. 2019b. Infant mortality. https://www.cdc.gov/reproductivehealth/maternalinfanthealth/infantmortality.htm (accessed July 15, 2019).
CDC. 2019c. Most recent asthma data. https://www.cdc.gov/asthma/most_recent_data.htm (accessed July 16, 2019).
Center on the Developing Child at Harvard University. 2016. From best practices to breakthrough impacts: A science-based approach to building a more promising future for young children and families. Cambridge, MA: Harvard University.
Center on the Developing Child at Harvard University. n.d. Toxic stress. https://developingchild.harvard.edu/science/key-concepts/toxic-stress (accessed July 13, 2019).
Child Trends. 2015. Early school readiness. https://www.childtrends.org/wp-content/uploads/2016/03/indicator_1457981601.385.pdf (accessed July 16, 2019).
Child Trends. 2016. Dual language learners. https://www.childtrends.org/indicators/dual-language-learners (accessed July 13, 2019).
Child Trends. 2018a. Immigrant children. https://www.childtrends.org/indicators/immigrant-children (accessed July 13, 2019).
Child Trends. 2018b. Low and very low birthweight infants. https://www.childtrends.org/indicators/low-and-very-low-birthweight-infants (accessed July 5, 2019).
Child Trends. 2018c. Racial and ethnic composition of the child population. https://www.childtrends.org/indicators/racial-and-ethnic-composition-of-the-child-population (accessed July 13, 2019).
CMS (Centers for Medicare & Medicaid Services). 2017. National health expenditures 2017 highlights. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/Downloads/highlights.pdf (accessed July 16, 2019).
Creanga, A. A., C. J. Berg, C. Syverson, K. Seed, F. C. Bruce, and W. M. Callaghan. 2015. Pregnancy-related mortality in the United States, 2006–2010. Obstetrics & Gynecology 125(1):5–12.
Daily, S., S. Burkhauser, and T. Halle. 2010. A review of school readiness practices in the States: Early learning guidelines and assessments. Child Trends: Early Childhood Highlights 1(3):1–12.
Danaher, A. 2011. Reducing health inequities: Enablers and barriers to inter-sectoral collaboration. Ontario, Canada: Wellesley Institute.
Darling-Hammond, L. 1998. Unequal opportunity: Race and education. Washington, DC: The Brookings Institution.
Davis, R., S. Savannah, M. Harding, A. Macaysa, and L. F. Parks. 2016. Countering the production of inequities: An emerging systems framework to achieve an equitable culture of health. Oakland, CA: Prevention Institute.
Ely, D. M., A. K. Driscoll, and T. J. Mathews. 2017. Infant mortality rates in rural and urban areas in the United States, 2014. NCHS data brief no. 285. Hyattsville, MD: National Center for Health Statistics.
Fang, X., D. S. Brown, C. S. Florence, and J. A. Mercy. 2012. The economic burden of child maltreatment in the United States and implications for prevention. Child Abuse and Neglect 36(2):156–165.
FFYF (First Five Years Fund). 2018. After recent historic progress, early childhood education could be a unifying issue for a divided Congress. https://www.ffyf.org/after-recent-historic-progress-early-childhood-education-could-be-a-unifying-issue-for-a-divided-congress (accessed July 13, 2019).
Galea, S., M. Tracy, K. J. Hoggatt, C. Dimaggio, and A. Karpati. 2011. Estimated deaths attributable to social factors in the United States. American Journal of Public Health 101(8):1456–1465.
Galindo, C., and B. Fuller. 2010. The social competence of Latino kindergartners and growth in mathematical understanding. Developmental Psychology 46(3):579–592.
Garcia, J. L., J. J. Heckman, D. E. Leaf, and M. J. Prados. 2017. Quantifying the life-cycle benefits of a prototypical early childhood program. NBER Working Papers from National Bureau of Economic Research, No. 23479.
García Coll, C., and A. Kerivan Marks. 2009. Immigrant stories: Ethnicity and academics in middle childhood. New York: Oxford University Press.
García Coll, C., K. Crnic, G. Lamberty, B. H. Wasik, R. Jenkins, H. V. Garcia, and H. P. McAdoo. 1996. An integrative model for the study of developmental competencies in minority children. Child Development 67(5):1891–1914.
GBD (Global Burden of Diseases, Injuries, and Risk Factors) 2015 Maternal Mortality Collaborators. 2016. Global, regional, and national levels of maternal mortality, 1990–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 338:1775–1812.
Ghandour, R. M., M. D. Kogan, S. J. Blumberg, J. R. Jones, and J. M. Perrin. 2012. Mental health conditions among school-aged children: Geographic and sociodemographic patterns in prevalence and treatment. Journal of Developmental and Behavioral Pediatrics 33(1):42–54.
Ghandour, R. M., K. Anderson Moore, K. Murphy, C. Bethell, J. Jones, R. Harwood, J. Buerlein, M. Kogan, and M. Lu. 2018. School readiness among U.S. children: Development of a pilot measure. Child Indicators Research 1–23.
Gluckman, P. D., M. A. Hanson, and A. S. Beedle. 2007. Early life events and their consequences for later disease: A life history and evolutionary perspective. American Journal of Human Biology 19(1):1–19.
Gould, E. 2009. Childhood lead poisoning: Conservative estimates of the social and economic benefits of lead hazard control. Environmental Health Perspectives 117(7):1162–1167.
Grinshteyn, E., and D. Hemenway. 2016. Violent death rates: The US compared with other high-income OECD countries, 2010. American Journal of Medicine 129(3):266–273.
Gunja, M., S. Collins, M. Doty, and S. Beutel. 2017. How the Affordable Care Act has helped women gain insurance and improved their ability to get health care: Findings from the Commonwealth Fund Biennial Health Insurance Survey, 2016. https://www.commonwealthfund.org/publications/issue-briefs/2017/aug/how-affordable-care-act-has-helped-women-gain-insurance-and (accessed July 16, 2019).
Hahn, R. A. 2019. Two paths to health in all policies: The traditional public health path and the path of social determinants. American Journal of Public Health 109(2):253–254.
Halfon, N., K. Larson, M. Lu, E. Tullis, and S. Russ. 2014. Lifecourse health development: Past, present and future. Maternal and Child Health Journal 18(2):344–365.
Heckman, J. J., J. E. Humphries, and G. Veramendi. 2018. Returns to education: The causal effects of education on earnings, health, and smoking. Journal of Political Economy 126(Suppl 1):S197–S246.
Heiman, H., and S. Artiga. 2015. Beyond health care: The role of social determinants in promoting health and health equity. Washington, DC: Kaiser Family Foundation.
Heindel, J. J., and L. N. Vandenberg. 2015. Developmental origins of health and disease: A paradigm for understanding disease cause and prevention. Current Opinion in Pediatrics 27(2):248–253.
Hood, C. M., K. P. Gennuso, G. R. Swain, and B. B. Catlin. 2016. County health rankings: Relationships between determinant factors and health outcomes. American Journal of Preventive Medicine 50(2):129–135.
Houtrow, A. J., K. Larson, L. M. Olson, P. W. Newacheck, and N. Halfon. 2014. Changing trends of childhood disability, 2001–2011. Pediatrics 134(3):530–538.
Hughes, K., M. A. Bellis, K. A. Hardcastle, D. Sethi, A. Butchart, C. Mikton, L. Jones, and M. P. Dunne. 2017. The effect of multiple adverse childhood experiences on health: A systematic review and meta-analysis. Lancet Public Health 2(8):e356–e366.
Inequality.org. n.d. Income inequality in the United States. https://inequality.org/facts/income-inequality (accessed July 16, 2019).
IOM (Institute of Medicine). 2007. Preterm birth: Causes, consequences, and prevention. Washington, DC: The National Academies Press.
IOM. 2012. For the public’s health: Investing in a healthier future. Washington, DC: The National Academies Press.
IOM. 2015. Business engagement in building healthy communities: Workshop summary. Washington, DC: The National Academies Press.
Isaacs, J. B., C. Lou, H. Hahn, A. Hong, C. Quakenbush, and C. E. Steuerle. 2018. Kids’ share 2018: Report on federal expenditures on children through 2017 and future projections. Washington, DC: The Urban Institute.
Kaiser Family Foundation. 2019. The uninsured and the ACA: A primer—key facts about health insurance and the uninsured amidst changes to the Affordable Care Act. https://www.kff.org/report-section/the-uninsured-and-the-aca-a-primer-key-facts-about-healthinsurance-and-the-uninsured-amidst-changes-to-the-affordable-care-act-how-have-health-insurance-coverage-options-and-availability-changed (accessed July 16, 2019).
Karoly, L. A., M. R. Kilburn, and J. S. Cannon. 2005. Early childhood interventions: Proven results, future promise. Santa Monica, CA: RAND.
Korous, K., J. Causadias, R. H. Bradley, and S. Luthar. 2018. Unpacking the link between socioeconomic status and behavior problems: A second-order meta-analysis. Development and Psychopathology 30(5):1889–1906.
Kottke, T. E., M. Stiefel, and N. P. Pronk. 2016. “Well-being in all policies”: Promoting cross-sectoral collaboration to improve people’s lives. Preventing Chronic Disease 13:160155.
Lantz, P. 2018. The medicalization of population health: Who will stay upstream? The Milbank Quarterly 97(1):36–39.
Lynch, J. 2006. Age in the welfare state. London: Cambridge University Press.
Martin, A., M. Hartman, B. Washington, A. Catlin, and the National Health Expenditure Accounts Team. 2018a. National health care spending in 2017: Growth slows to post–great recession rates; share of GDP stabilizes. Health Affairs 38(1):96–106.
Martin, J. A., B. E. Hamilton, M. J. K. Osterman, A. K. Driscoll, and P. Drake. 2018b. Births: Final data for 2016. National Vital Statistics Reports 67(1). https://www.cdc.gov/nchs/data/nvsr/nvsr67/nvsr67_01.pdf (accessed August 12, 2019).
Martin, N., and R. Montagne. 2017. U.S. has the worst rate of maternal deaths in the developed world. https://www.npr.org/2017/05/12/528098789/u-s-has-the-worst-rate-of-maternal-deaths-in-the-developed-world (accessed June 25, 2019).
Masters, R., E. Anwar, B. Collins, R. Cookson, and S. Capewell. 2017. Return on investment of public health interventions: A systematic review. Journal of Epidemiology and Community Health 71(8):827–834.
Mattessich, P. W., and E. J. Rausch. 2014. Cross-sector collaboration to improve community health: A view of the current landscape. Health Affairs (Project Hope) 33(11):1968–1974.
McFarlane, A. C. 2010. The long-term costs of traumatic stress: Intertwined physical and psychological consequences. World psychiatry: Official Journal of the World Psychiatric Association (WPA) 9(1):3–10.
McLaughlin, M., and M. R. Rank. 2018. Estimating the economic cost of childhood poverty in the United States. Social Work Research 42(2):73–83.
McLeroy, K. R., D. Bibeau, A. Steckler, and K. Glanz. 1988. An ecological perspective on health promotion programs. Health Education Quarterly 15(4):351–377.
MHTF (Maternal Health Task Force). n.d. Maternal health in the United States https://www.mhtf.org/topics/maternal-health-in-the-united-states (accessed July 16, 2019).
Muennig, P., D. Robertson, G. Johnson, F. Campbell, E. P. Pungello, and M. Neidell. 2011. The effect of an early education program on adult health: The Carolina Abecedarian project randomized controlled trial. American Journal of Public Health 101(3):512–516.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Parenting matters: Supporting parents of children ages 0–8. Washington, DC: The National Academies Press.
NASEM. 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press.
NASEM. 2018a. Building sustainable financing structures for population health: Insights from nonhealth sectors: Proceedings of a workshop. Washington, DC: The National Academies Press.
NASEM. 2018b. Exploring tax policy to advance population health, health equity, and economic prosperity: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press.
NASEM. 2019a. The promise of adolescence: Realizing opportunity for all youth. Washington, DC: The National Academies Press.
NASEM. 2019b. A roadmap to reducing child poverty. Washington, DC: The National Academies Press.
National MCH Workforce Development Center. 2015. The Affordable Care Act: A working guide for MCH professionals. http://www.amchp.org/Transformation-Station/Transformation_Station_Documents/ACA-guide.pdf (accessed June 18, 2019).
Nelson, D., M. Moniz, and M. Davis. 2018. Population-level factors associated with maternal mortality in the United States, 1997–2012. BMC Public Health 18:1007.
NRC and IOM (National Research Council and Institute of Medicine). 2004. Children’s health, the nation’s wealth: Assessing and improving child health. Washington, DC: The National Academies Press.
NRC and IOM. 2013. Health in international perspective: Shorter lives, poorer health. Washington, DC: The National Academies Press.
OECD (Organisation for Economic Co-operation and Development). 2009. United States country highlights—doing better for children. https://www.oecd.org/unitedstates/43590390.pdf (accessed June 25, 2019).
OECD. 2014. Society at a glance 2014: OECD social indicators. http://www.oecd.org/els/soc/OECD2014-SocietyAtAGlance2014.pdf (accessed June 18, 2019).
OECD. 2017. Health at a glance 2017—OECD indicators. https://read.oecd-ilibrary.org/social-issues-migration-health/health-at-a-glance-2017_health_glance-2017-en#page1 (accessed July 13, 2019).
OECD. 2019. PF3.1: Public spending on childcare and early education. http://www.oecd.org/els/soc/PF3_1_Public_spending_on_childcare_and_early_education.pdf (accessed July 13, 2019).
Osterman, M. J. K., and J. A. Martin. 2018. Timing and adequacy of prenatal care in the United States, 2016. National Vital Statistics Reports 67(3):1–14.
Pager, D., and H. Shepherd. 2008. The sociology of discrimination: Racial discrimination in employment, housing, credit, and consumer markets. Annual Review of Sociology 34:181–209.
Pascoe, J. M., D. L. Wood, J. H. Duffee, and A. Kuo. 2016. Mediators and adverse effects of child poverty in the United States. Pediatrics 137(4).
Perrin, J. M., S. R. Bloom, and S. L. Gortmaker. 2007. The increase of childhood chronic conditions in the United States. JAMA 297(24):2755–2759.
Perrin, J. M., L. E. Anderson, and J. Van Cleave. 2014. The rise in chronic conditions among infants, children, and youth can be met with continued health system innovations. Health Affairs 33(12):2099–2105.
Perrin, J. M., J. R. Asarnow, T. Stancin, S. P. Melek, and G. K. Fritz. 2018. Mental health conditions and health care payments for children with chronic medical conditions. Academic Pediatrics 19(1):44–50.
Pew Research Center. 2015a. The American family today. https://www.pewsocialtrends.org/2015/12/17/1-the-american-family-today (accessed July 16, 2019).
Pew Research Center. 2015b. Parenting in America: Outlook, worries, aspirations are strongly linked to financial situation. Washington, DC: Pew Research Center.
Porter, J., D. Fisher-Bruns, and B. H. Pham. 2019. Anchor collaboratives: Building bridges with place-based partnerships and anchor institutions. Washington, DC: Democracy Collaborative.
Prevention Institute. 2015. Sustainable investments in health: Prevention and wellness funds. Oakland, CA: Blue Shield of California Foundation, The Kresge Foundation, and The California Endowment.
Rosenbaum, S., D. A. Kindig, J. Bao, M. K. Byrnes, and C. O’Laughlin. 2015. The value of the nonprofit hospital tax exemption was $24.6 billion in 2011. Health Affairs 34(7):1225–1233.
Seith, D., and E. Isakson. 2011. Who are America’s children: Examining health disparities among children in the U.S. New York: National Center for Children in Poverty.
Shak, L., L. Mikkelsen, R. Gratz-Lazarus, and N. Schneider. 2013. What’s good for health is good for business: Engaging the business community in prevention efforts. Oakland, CA: Prevention Institute.
Shonkoff, J. P., A. S. Garner, American Academy of Pediatrics Committee on Psychosocial Aspects of Child and Family Health, Committee on Early Childhood, Adoption, and Dependent Care, Section on Developmental and Behavioral Pediatrics. The lifelong effects of early childhood adversity and toxic stress. Pediatrics 129(1):e232–e246.
Slopen, N., J. P. Shonkoff, M. A. Albert, H. Yoshikawa, A. Jacobs, R. Stoltz, and D. R. Williams. 2016. Racial disparities in child adversity in the U.S.: Interactions with family immigration history and income. American Journal of Preventive Medicine 50(1):47–56.
Smeeding, T. 2012. Income, wealth, and debt and the great recession. Stanford, CA: Stanford Center on Poverty and Inequality.
Turney, K., and C. Wildeman. 2017. Adverse childhood experiences among children placed in and adopted from foster care: Evidence from a nationally representative survey. Child Abuse and Neglect 64:117–129.
U.S. Census. 2018. Table FG10, family groups 2018. https://www2.census.gov/programssurveys/cps/techdocs/cpsmar18.pdf (accessed July 16, 2019).
Van Cleave, J., S. L. Gortmaker, and J. M. Perrin. 2010. Dynamics of obesity and chronic health conditions among children and youth. JAMA 303(7):623–630.
Velez-Agosto, N. M., J. G. Soto-Crespo, M. Vizcarrondo-Oppenheimer, S. Vega-Molina, and C. García Coll. 2017. Bronfenbrenner’s bioecological theory revision: Moving culture from the macro into the micro. Perspectives on Psychological Science 12(5):900–910.
Waidmann, T., and Urban Institute. 2009. Estimating the cost of racial and ethnic health disparities. Washington, DC: Urban Institute. http://www.urban.org/UploadedPDF/411962_health_disparities.pdf (accessed July 13, 2019).
Walmsley, R. n.d. World prison population list. London: International Centre for Prison Studies King’s College London School of Law.
Wenger, M. 2012. Place matters: Ensuring opportunities for good health for all. Washington, DC: Joint Center for Political and Economic Studies.
WHO (World Health Organization). 2010. A conceptual framework for action on the social determinants of health. Social determinants of health discussion paper 2. Geneva, Switzerland: World Health Organization.
WHO, UNFPA (United Nations Population Fund), World Bank Group, United Nations Population Division. 2015. Trends in maternal mortality: 1990 to 2015: Estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. https://www.who.int/reproductivehealth/publications/monitoring/maternal-mortality-2015/en (accessed August 12, 2019).
Zahran, H. S., C. M. Bailey, S. A. Damon, P. L. Garbe, and P. N. Breysse. 2018. Vital signs: Asthma in children—United States, 2001–2016. Morbidity and Mortality Weekly Report 67(5):149–155.
This page intentionally left blank.
















































