


Combing through patient records in the 1890s, a young New York surgeon named William Coley noticed something intriguing: After multiple surgeries to remove an egg-sized tumor on a man’s left cheek, the area became infected and the patient developed a high fever. The case was deemed hopeless. Yet, in the coming weeks, inexplicably, the tumor shrank and eventually disappeared.
The stunning observation made Coley wonder: If a cancer shrank after an unintended infection, why not purposefully rev up a patient’s immune system to fight off his or her tumor? During the past century, that bold idea fueled a line of research leading to a revolutionary treatment strategy that earned a 2018 Nobel Prize and has effectively treated thousands of people with cancer.
Traditionally, cancer patients have had three therapeutic options: cut it out (surgery), blast it away (radiation), or kill it with chemicals (chemotherapy). Now some patients with once fatal cancers are finding hope in therapies that work by Coley’s paradigm—empowering the patient’s own immune cells to kill the tumor.
The researchers whose findings ushered in this groundbreaking strategy had no intention of curing cancer, at least not initially. “I’m a basic scientist. I wanted to know how T cells work,” Jim Allison, chair of the Department of Immunology at the MD Anderson Cancer Center at The University of Texas, said in a 2018 news conference. He and Tasuku Honjo, an immunologist at Kyoto University in Japan, had just won the Nobel Prize in medicine. “I’m lucky … to see my work 20 years later really helping patients,” Allison said.
In the early 1990s, scientists knew that T cells were important for fighting infections but understood little about how these white blood cells were controlled. “It was kind of like space. You didn’t know what was out there,” recalls Matthew Krummel, then a graduate student in Allison’s lab at the University of California, Berkeley. “You had some glimmers of light coming through the telescope—evidence of proteins on the cell surface, but you didn’t know what they did.”
Rather than angling toward a specific disease or application, the research was driven by a fundamental curiosity about the molecular signals that turn on T cells—more like “there’s this molecule, no one’s looked at it before, I wonder what it might do,” says Krummel, who now leads his own research lab at the University of California, San Francisco.
At the time, immunologists had come up with the “two-signal model” for T cell activation. Signal 1 transmits through a cell-surface protein complex known as the T-cell receptor. Recognizing bits of proteins on the surface of other cells, the T-cell receptor gives specificity to the immune response—much like a car key inserted into the ignition turns it on. But making the T cell “go” requires a second signal.
Of the millions of T cells cruising through a body, only a tiny fraction binds to any given virus, bacterium, or other harmful invader. That interaction is Signal 1. Only with a second molecular interaction—Signal 2—do those T cells rapidly multiply.
Gordon Freeman, an immunologist at the Dana-Farber Cancer Institute in Boston, Massachusetts, identified a key component of Signal 2—a set of molecules known as B7 on the surface of immune cells that have been turned “on.” When B7 interacts with a T cell surface protein called CD28, the T cell revs up and multiplies. That interaction is “a gas pedal for activation,” Freeman says. Without Signal 2, the T cell falls into a trance, like an idling engine.
Meanwhile, other labs had their eyes on another cell surface protein called CTLA4, a cousin of CD28 discovered in 1987. Early experiments suggested CTLA4 signals act as a brake. That idea found further support when Allison and Krummel showed that specialized immune proteins called antibodies could control the activity of T cells in a lab dish. The researchers could dial up T cell activity with an antibody that attaches to CD28, then dial it back down with an antibody that attaches to CTLA4.
CTLA4’s importance solidified when other groups genetically engineered mice without the protein. “The mice die of autoimmune disease if they lack CTLA4,” says Harvard Medical School immunologist Arlene Sharpe, who generated one of these “gene knockout” mouse strains. Another lab reported similar findings. Those gene knockout studies “conclusively proved CTLA4 is a brake, because when you lose it, the mouse becomes overrun with activated T cells,” says Jedd Wolchok, a clinician-scientist at the Memorial Sloan Kettering Cancer Center in New York. He treated cancer patients in early clinical trials of the therapies that were developed from those lab findings.
It makes sense that the immune system would have brakes to counteract the gas pedals. After your body clears an infection, Sharpe says, brakes are “important for returning the immune system to its basal state because too much inflammation can cause tissue damage.”
A flurry of studies fleshing out how T cells are regulated inspired scientists to consider using these immune cells to modulate disease. The concept was a bit of a leap. In the early 1990s many scientists doubted the immune system could have any specificity for tumor cells “given that cancer looks a lot like yourself,” Krummel says.
Yet, “there was a core group of us, maybe a few dozen, who didn’t lose hope,” Wolchock says. “And I think what was responsible for us not losing hope was the science.”
In that regard Allison was a visionary. As the field struggled to understand the brakes and gas pedals when T cells fight infection, Allison recalled an experiment he had done years prior, which hinted that T cells, under the right circumstances, were capable of fighting tumors. In those studies, mice that would ordinarily die from implanted melanoma cells managed to reject the tumor if the tumor cells were genetically engineered to make “gas pedal” B7 proteins.
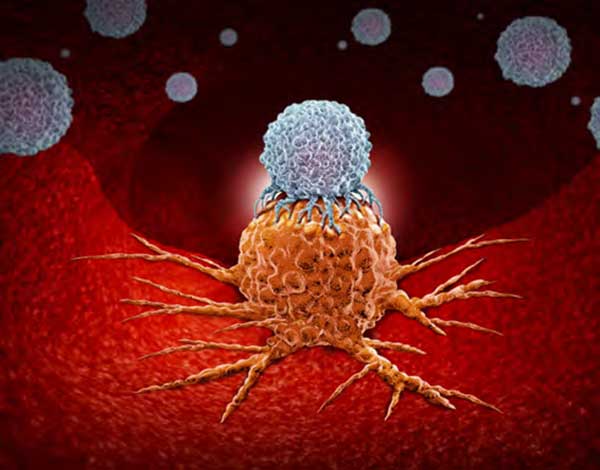
That result suggested that T cells idled when cancers lacked “Signal 2.” Without gas pedal signaling, T cells remained apathetic while the tumor grew and spread.
Curious, Allison and Krummel wondered what would happen if the foot came off the brake pedal in T cells. Using antibodies that block CTLA4, the T cells activated and attacked the cancer cells. This approach, which became the basis of current cancer immune therapies known as “checkpoint inhibitors,” was a simpler way of waking the immune system to fight cancer. “All we had to do was put in the antibody, and the T cell response got better,” Krummel says.
That landmark study was one in a series of experiments driven by the same fundamental question—how T cells recognize and respond to targets—in which many labs probed the function of molecules on the cell surface. But Honjo, the man who shared the Nobel Prize with Allison, took a genetic approach. In a search for proteins involved in a process known as programmed cell death, Honjo and co-workers came upon one that they named PD-1. It is now the target of the most widely used checkpoint inhibitor drugs.
Intrigued to find PD-1 on the surface of activated T cells, Honjo’s team did further experiments to probe the protein’s function. They deleted the gene in mice and saw the animals develop autoimmune disease. This suggested that PD-1—like CTLA4—dampens the immune response.
Unbeknownst to Honjo’s team in Japan, Freeman and Sharpe had landed on the other side of the PD-1 pathway while searching for molecules that look like B7. The husband–wife duo found two cell-surface molecules, now called PD-L1 and PD-L2, and showed they are binding partners for PD-1. Independently, a team at the Mayo Clinic discovered a molecule that they named B7-H1, which turns out to be PD-L1, but they did not realize its connection to PD-1.
Freeman and Sharpe teamed with Honjo’s group and reasoned that blocking the dampening effect of PD-1 could boost recognition of tumor cells by the immune system. Sure enough, Honjo’s 2002 study confirmed that an anti-PD-L1 blocking antibody helped mice fight tumors.
Soon after, Honjo and the Mayo Clinic team showed that antibodies blocking PD-1 could slow tumor growth in mice. There were “a lot of hands on this in a short time” as scientists followed up on these findings, recalls Wolchok.
Years later, though, the hope of translating promising lab results into treatments for patients took a hit when a clinical trial was halted in 2006 because an immune-boosting drug caused multi-organ failure in some trial participants. Intended to treat B cell chronic lymphocytic leukemia and rheumatoid arthritis, that drug, theralizumab, hyperstimulated CD28, a key component of the “gas pedal” on most T cells.
Still, buoyed by the wave of earlier discoveries unlocking T cells’ potential to fight tumors, scientists at Medarex—which was bought in 2009 by biopharma giant Bristol-Myers Squibb—developed antibodies that attach to CTLA4, and later to PD-1. Merck and several other companies have generated other antibodies to block the PD-1 signaling pathway.

In a clinical trial, the anti-CTLA4 checkpoint inhibitor (a drug called ipilimumab) extended the lives of some people with metastatic melanoma who would otherwise face a poor prognosis. One such individual was a 22-year-old woman who came to Wolchok in 2004 with stage 4 melanoma that had spread to multiple organs. Several prior therapies had failed to slow the progression of her cancer when she entered the ipilimumab trial. After four treatments, her cancer disappeared. Fourteen years later, she is leading a healthy life—raising two children and running half marathons.
Although some patients’ cancers eventually become resistant to ipilimumab, the therapy has improved the 5-year survival rate for metastatic melanoma from 5 to 20 percent. “It doesn’t sound like much, but boy, if you’re one of those [additional] 15 percent, it’s a big difference,” says Wolchok. “It opened the door that immunotherapy was real and could work, that we had a foothold on which to climb higher. PD-1 was next in line.”
Anti-PD-1 immune therapy (called nivolumab) stole the show at the American Society of Clinical Oncology meeting in summer 2012. “The hall was packed,” recalls Freeman. The PD-1 antibody developed by Bristol-Myers Squibb had been tested in a first-in-human trial involving a broad range of cancers, including melanoma and kidney, colon, and lung cancer. For a trial meant to test primarily for the toxicity of a new drug, “the surprising thing was that there were responses with really significant tumor shrinkage in a variety of tumor types,” Freeman says. Plus, people tolerated anti-PD-1 much better than anti-CTLA4, experiencing fewer side effects.
Cancer immunotherapies are now approved by the U.S. Food and Drug Administration to treat 13 cancers. But they carry a $100,000 to $250,000 price tag, and a recent analysis estimates that less than 13 percent of U.S. patients respond to current immunotherapies. So scientists are creating new immune treatments and looking for ways to better predict which patients will benefit.
Some researchers are developing drugs that target additional T cell brakes and gas pedals. Still others are testing new approaches that enliven the defense system’s first responders, innate immune cells, in hope of further invigorating T cells’ tumor killing. Dating back to Coley’s century-old fascination with the infection-induced tumor regression, the growth of the cancer immunotherapy field presents a powerful example of how basic curiosity fuels fundamental discoveries that can ultimately produce life-prolonging therapies.
This article was written by Esther Landhuis for From Research to Reward, a series produced by the National Academy of Sciences. This and other articles in the series can be found at www.nasonline.org/r2r. The Academy, located in Washington, DC, is a society of distinguished scholars dedicated to the use of science and technology for the public welfare. For more than 150 years, it has provided independent, objective scientific advice to the nation.
Please direct comments or questions about this series to Cortney Sloan at csloan@nas.edu.
Photo and Illustration Credits:
William Coley: https://commons.wikimedia.org/wiki/File:William_Coley_1892.jpg;
Jim Allison: National Academy of Sciences; T cell attacking cancer cell: Lightspring/Shutterstock; Arlene Sharpe:
Courtesy of WBUR/Jesse Costa, photographer, http://www.wbur.org.
© by the National Academy of Sciences. All rights reserved. These materials may be reposted and reproduced solely for non-commercial educational use without the written permission of the National Academy of Sciences.