The workshop’s second panel featured short presentations by four panelists who spoke about different housing interventions to address patients’ non-medical, health-related social needs. The panelists were Robin Hacke, Executive Director of the Center for Community Investment; Ross Owen, Health Strategy Director at the Hennepin County, Minnesota, Accountable Care Organization (ACO); Angela Mingo, Director of Community Relations at Nationwide Children’s Hospital; and Bechara Choucair, Senior Vice President and Chief Community Health Officer at Kaiser Permanente. A discussion and question-and-answer session, moderated by Maurice Jones, President and Chief Executive Officer of Local Initiatives Support Corporation, followed the presentations.
ACCELERATING INVESTMENTS FOR HEALTHY COMMUNITIES
The Center for Community Investment, explained Robin Hacke, is in the business of helping communities unlock the capital they need to achieve their priorities for community development, which in many places is stable, healthy, and affordable homes for everyone in the community. She noted that 3 years ago, the Robert Wood Johnson Foundation asked the Center what it would take to have hospitals and health systems invest in increasing the stock of affordable housing. The resulting initiative, Accelerating Investments for Healthy Communities, is an intensive, 2-year initiative designed to help teams comprising health institutions (representing a mix of faith-based, safety net, academic, and children’s hospitals) and their community partners deploy assets to address social determinants of health with a primary emphasis on affordable housing as the basis for investing in community health.
There are, in fact, a number of health systems that have committed resources to develop and preserve affordable housing in their communities, even though they are not required or even incentivized to do so (see Table 3-1). The idea behind the Accelerating Investments for Healthy Communities initiative, said Hacke, is to see what would happen if the leaders of these health systems could expand that work and light a path for other institutions to follow. When her team examined the motivations
| Participating Institution | Focus Region |
|---|---|
| Bon Secours Mercy Health System | Baltimore, MD Cincinnati, OH |
| Dignity Health | San Bernardino, CA |
| Kaiser Permanente | Purple Line Corridor, Prince George’s/Montgomery Counties, MD |
| Nationwide Children’s Hospital | Columbus, OH |
| UPMC | Pittsburgh, PA |
NOTE: UPMC = University of Pittsburgh Medical Center.
SOURCES: Presented by Robin Hacke, April 26, 2019, at the Workshop on Investing in Interventions That Address Non-Medical, Health-Related Social Needs. Created by the Center for Community Investment.
of these health systems to invest upstream, they found that there were many, often within the same institution. Motivations included
- Investing upstream was part of the institution’s mission to foster health communities.
- Getting involved in upstream initiatives was a way of boosting the health system’s reputation in the community.
- It improved the systems’ competitiveness.
- It afforded an opportunity to gain experience with strategies that might reduce costs and improve outcomes as preparation for payment shifts from volume to value.
- Such investments might generate a positive return on investment (ROI).
- Investing upstream helped meet requirements and avoid penalties for readmissions.
She noted that the more such investments are viewed as an institutional imperative, the less important the narrow economic justification becomes.
What she has seen in this program is that health systems invest in a range of housing types that includes emergency shelters, transitional and supportive housing, public housing, subsidized and unsubsidized affordable housing, market-rate rental housing, and owned homes. Those that focus more on narrower ROI considerations tend to invest in emergency shelters, transitional housing, and supportive housing. What she is seeing among the leaders in this program is an interest in a broader set of affordable housing investments, including family housing; affordable housing for their own workforces, especially for the people who are at the lower end of the income spectrum; and the continuum of housing options that allows people to move through the spectrum as their needs change (see Figure 3-1). She noted that health systems do not need to do this work by themselves but should partner with the existing community development sector that works in the housing arena every day.
Health systems, said Hacke, should think broadly about the assets they can bring to the table. Community benefit dollars, she said, are like magic because they can be used for a wide range of purposes, but many institutions these days also have land that may not be necessary anymore for the health system’s purposes. They may also have pensions, foundation endowments, and insurance reserves with which they can make investments. “Thinking more holistically about the kinds of assets that can be brought to bear makes health systems much more powerful as a partner,” said Hacke.
What she has seen so far is that there are two levels of transformation that have to happen for this work to go forward. One occurs inside
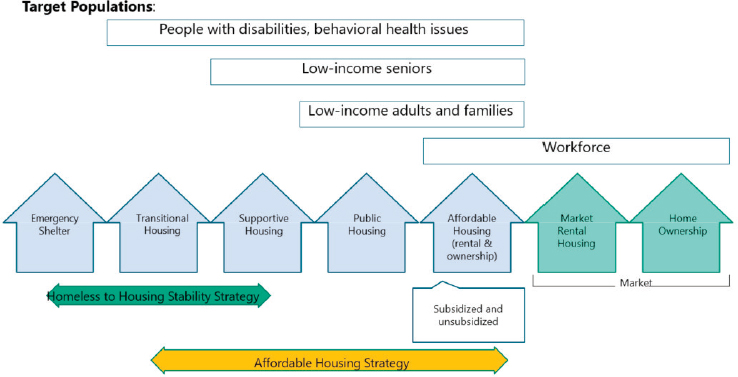
SOURCES: Presented by Robin Hacke, April 26, 2019, at the Workshop on Investing in Interventions That Address Non-Medical, Health-Related Social Needs. Created by the Center for Community Investment from content by Marjan Eggermont’s Housing Continuum model. Information available at http://sixeightfour.blogspot.com/2009/03/housing-continuum.html (accessed July 30, 2019).
the health system when a leader steps up and says this is something that is part of the health system’s business, and the other occurs when the health system reaches out to the community to find a partner than can articulate the community’s vision for what it needs as a means of avoiding unintended consequences. Hacke noted the importance of involving financial and real estate experts who can bring ideas about how to leverage land and structure leases so that buildings are financially stable. Also important, she said, is to not think in terms of one investment of 100 units but in terms of a pipeline of investments the health system can help develop through partnerships. Finally, she said, health systems have a role to play as a convener of a range of partners to meet regularly and build momentum.
MEDICAID ACCOUNTABLE CARE ORGANIZATION
Hennepin Health, explained Ross Owen, is an ACO focused on caring for complex Medicaid enrollees in Minnesota’s largest county, which for the past 30 years has functioned as a department of county government with its own Medicaid health plan operating on a capitated reimbursement arrangement with the state Medicaid agency. Hennepin Health’s
ACO is anchored by a county-affiliated teaching hospital and level 1 trauma center, and it includes a system of primary care clinics and federally qualified health centers that serve anchoring roles in the neighborhoods they serve. Hennepin Health’s operating model includes linkages with county human services and the public health department, which runs a system of clinics to provide health care for the homeless. Though historically, health care, human services, and public health were not good at working together, Owen said Hennepin Health linked them together with a governance model that includes a shared electronic health record (EHR), collaborative decision making, integration of data and services, a risk-sharing funding model, and an infrastructure to measure impact.
Most of those served by Hennepin Health were brought into the health system through Medicaid expansion, said Owen, so the services the ACO offers reflect the needs of that historically uninsured or under-insured population of adults. He noted that as a health system, Hennepin Health has what he characterized as an interesting cross-sector view of how these new beneficiaries not only present clinically with social needs but are touching other part of the system that are intended to address those social needs (see Figure 3-2). As a result, there were many largely disconnected funding streams converging on the same high-risk, high-cost, high-need population.
One thing Owen said that the Hennepin Health team has learned in working with the Medicaid expansion population is that the interface of
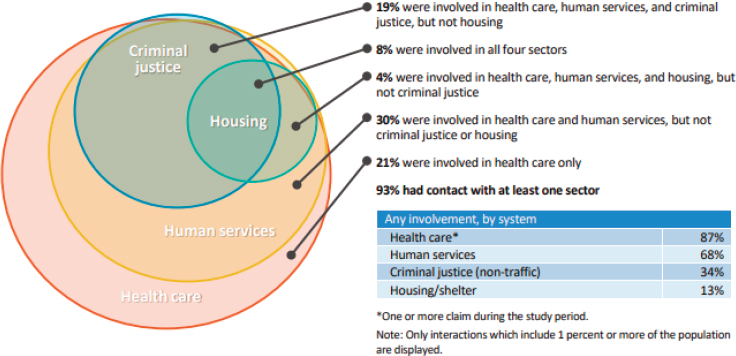
SOURCES: Presented by Ross Owen, April 26, 2019, at the Workshop on Investing in Interventions That Address Non-Medical, Health-Related Social Needs. Reproduced with permission from the Center for Health Care Strategies, Inc.; Bodurtha et al., 2017.
health care with other parts of the system looks different from the perspective of those other parts. As an example, he said that when Medicaid expansion rolled out in Minnesota, it was thought of by many as adding coverage for a small niche populations. However, when Owen and his colleagues looked at insurance coverage from the perspective of county’s homeless shelter system, they learned that over half of the emergency shelter stays in the community were by individuals who were suddenly covered by Medicaid. “From the perspective of the housing sector, that coverage became very important, and the set of tools and services made possible by that coverage really changed things overnight in terms of resources and the ability to serve that population,” said Owen.
With the obvious overlap of housing instability and health care needs, Hennepin Health has rolled out a variety of interventions intended to connect housing and health care and reduce acute care costs. One intervention involved hiring county-employed social workers and deploying them into the medical system to provide what Hennepin Health calls social service navigation. These social services navigators, for example, help discharged patients transition into stable housing for which they may already be eligible. Hennepin Health has also developed a data mining operation that uses location proxies to identify homelessness from information in the EHR.
In his concluding remarks, Owen encouraged the workshop participants to think about local government as one place where different sectors of service delivery, public policy, and funding tend to converge. Doing so, he said, offers the opportunity to draw out and recognize the interactions among these different sectors and to think more strategically about where to invest funds at the places where those sectors intersect.
HEALTHY NEIGHBORHOODS HEALTHY FAMILIES
As an urban planner working for a health care organization, Angela Mingo is excited to hear discussions about how the built environment can improve health and to see the housing and health care sectors working together to find solutions that benefit community and individual health. In that regard, she noted that Nationwide Children’s Hospital (NCH) now thinks of the neighborhood as its patient and is making investments in affordable housing as a means of improving the health of the neighborhoods it serves, and by extension, the families that live in those neighborhoods.
Her organization’s Healthy Neighborhoods Healthy Families initiative is taking a five-pronged approach to address the social determinants of health in the neighborhoods immediately adjacent to its main campus. In partnership with local stakeholders, Healthy Neighborhoods Healthy Families is looking for ways to improve health and wellness, education, and workforce and economic development; develop more affordable
housing options; and create safe and accessible neighborhoods. She noted, for example, that if a child lives in an unsafe neighborhood and cannot play and exercise outside, it is likely his or her health will be affected adversely. As part of its education initiative, the program encourages its employees to serve as mentors in the neighborhood. “In the case of an NCH mentor, when discussing health and wellness with their elementary school students, the discussion pivoted to the safety plan at home and how they plan for gun violence and things of that nature versus not being able to go outside and play because it simply is not safe,” said Mingo.
Healthy Neighborhoods Healthy Families has partnered with a faith-based community development corporation involved in affordable housing to revitalize the homes of current owners, eliminate blighted properties in the neighborhood, and increase home ownership. Though the initial stretch goal was to improve 100 properties, the program has been able to improve more than 300 homes over the past decade through a combination of improving vacant and blighted residential properties, financing infill housing, and expanding housing opportunities overall for residents in the neighborhoods. So far, NCH has invested more than $7 million in affordable housing and leveraged more than $25 million from other sources. Mingo explained that when the program started, it focused on home ownership but quickly realized that affordable housing was in such demand in its neighborhoods that it needed to also work to increase the stock of affordable rental housing.
Mingo noted that Hacke’s Center for Community Investment has been a key player in helping NCH accelerate its work and identify novel approaches to financing affordable housing. One approach that has proven successful uses what Mingo called a capital stack structure that combines several types of debt with varying levels of risk into a $15 million pool for investing in affordable rental properties, with NCH putting aside $1.5 million as a loan loss reserve (see Figure 3-3). Thanks to this fund, Healthy Neighborhoods Healthy Families should be able to improve 170 additional rental properties in a short period of time, said Mingo.
One thing she and her colleagues have learned through this work is that anchor institutions such as hers cannot do this work alone. “We have to identify the partners within our communities who are already in this space and who may need an opportunity to really accelerate their work by leveraging bigger partnerships,” said Mingo. She also noted that her large nonprofit organization has learned an incredible amount about investing in the community from the small nonprofit community development corporation with which it has partnered. Another lesson learned from Healthy Neighborhoods Healthy Families is that partnerships matter not just at the local level, but at the state and federal levels, too.
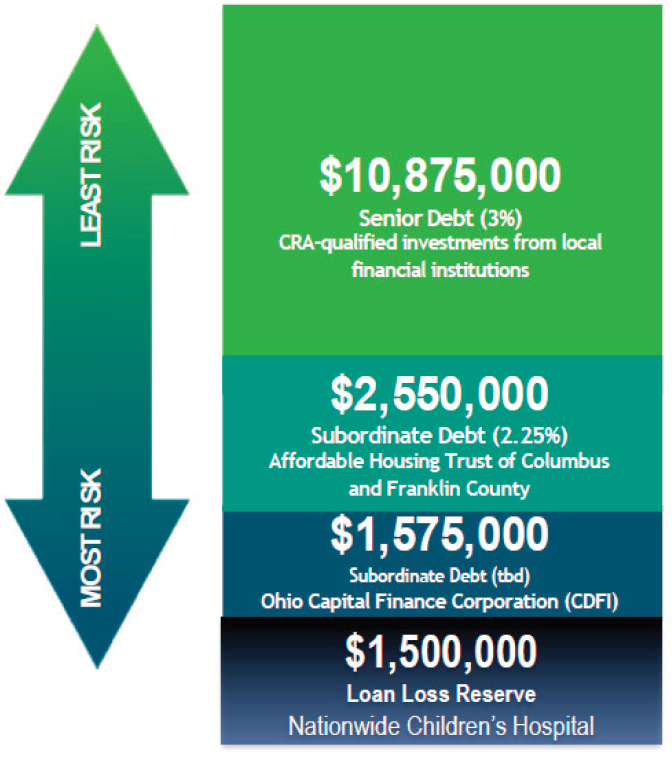
NOTE: CDFI = Community Development Financial Institution; CRA = Community Reinvestment Act.
SOURCES: Presented by Angela Mingo, April 26, 2019, at the Workshop on Investing in Interventions That Address Non-Medical, Health-Related Social Needs. Created by the Center for Community Investment with content provided by Nationwide Children’s Hospital.
SOLVING AMERICA’S HOUSING CRISIS REQUIRES ALL HANDS ON DECK
One lesson Kaiser Permanente, the largest nonprofit integrated health system in the country, has learned over the years is that health care services are not going to be enough to optimize the health of its 12.4 million members because health happens in the communities in which those
members live, learn, play, and work. “For us to be able to optimize their health, knowing that they stay with us for many years, it is important that we think about their needs in those communities,” said Bechara Choucair. Kaiser Permanente’s approach to thinking about its members’ health, he added, is to think about their social health in the same integrated manner that it thinks about physical and mental health. This involves looking at each individual’s housing and transportation needs, food insecurity, and social isolation, but it also looks at the conditions that led to the development of those social needs.
Regarding the nation’s affordable housing crisis, Choucair pointed out that as rental costs outpace income growth, many of its members start living in substandard housing, which can mean exposures to lead and other environmental pollutants and an increase in health care costs. He cited figures from the National Center for Healthy Housing showing that unsafe and unhealthy housing costs more than $300 billion annually. The nation’s housing crisis is also leading to a significant increase in the homeless population and an accompanying decrease in life expectancy for those affected individuals. “We know that the mortality rate of somebody on the street is three to four times higher than that of somebody who is housed,” said Choucair. “We know that if you are homeless, your life expectancy is about 27 years lower than it is for those who are housed.” In terms of controlling health care costs, individuals who are homeless and admitted to the hospital stay 2 to 3 days longer than those who are housed. Their chances of being readmitted after discharge are 50 percent higher.
Policy can serve as a key lever to address housing affordability, said Choucair. As a partner in the CityHealth project that John Auerbach discussed in the previous panel session, Kaiser Permanente identified nine policies that improve health, including one policy on inclusionary zoning. Kaiser Permanente is now working with the 40 largest cities in the country to make sure those cities have adopted policies that call for developers to dedicate a certain percentage of the units they build to be affordable, whether for low- or moderate-income individuals. It is also a national partner with Mayors & CEOs for U.S. Housing Investment, a bipartisan coalition of 24 mayors across the country that is working with the federal government to ensure there is the continued ability to invest in affordable housing stocks.
To power its non-medical initiatives in the community, Kaiser Permanente has committed $200 million in impact investment funds. One of its first investments is the Housing for Health Fund, which provides equity financing to help mission-oriented developers in the San Francisco Bay area purchase buildings that are at risk of becoming unaffordable and help the people that live in those buildings to continue to do so. This
fund’s first investment was in a multiunit building in Oakland that will now maintain affordability for years to come, said Choucair. The second fund, RxHome Fund, offers low interest rate loans to every Kaiser Permanente community with the sole purpose of preserving and expanding housing affordability in those communities.
Kaiser Permanente is carrying out another non-medical initiative to address the homelessness crisis in partnership with Community Solutions. This community-based organization works with 70 communities across the nation to use data to identify veterans and others who are chronically homeless and get those individuals into stable housing. Since 2015, said Choucair, this program has helped house more than 100,000 people in those 70 communities and helped 10 of those communities eliminate chronic homelessness. Kaiser Permanente is helping expand to 15 new communities in which Kaiser Permanente has members. Another project, conducted in Oakland, California, worked with community partners to identify by name the 515 people in Oakland who are 50 and older, have one or more chronic medical problem, and are homeless. Kaiser Permanente is now working with a group of community-based organizations to get all 515 of these individuals off the street and has made significant progress over a 4-month period to do just that.
DISCUSSION
Mikelle Moore from Intermountain Healthcare asked the panelists for ideas on how health care systems can act as a convener of other sectors. Hacke replied that because health care in many ways straddles the private and not-for-profit sectors and because chief executive officers of health institutions have a certain gravitas associated with them, she has found that health system leadership has an unusually powerful voice in discussions that cross sectors or in advocacy campaigns. Owen agreed with and added that it is important to bring together the leadership of multiple health systems to avoid the risk of them trying to separately engage the same nonprofit and government partners. It is also important, he said, for health systems to be willing to share data and knowledge equally with the other health systems in a partnership. “If we could collaborate instead of compete, we could have a model that is easier to engage with and would send more consistent signals at the community level as to where the health care system wants to engage with the community,” said Owen.
Mingo commented that bringing together government and other nonprofit organizations enables the partners to find their common goals and leverage the investments each partner brings to the table to make bigger investments than would otherwise have been possible. She noted that NCH is the primary health care organization involved in the housing
investment program she discussed, and that it has been able to engage the leadership of various financial institutions who are looking at opportunities for high-impact projects. Choucair added that the Bay Area Council, a coalition of more than 300 of the largest business in the region, issued a report around homelessness that is helping to mobilize businesses and community organizations to get involved in partnerships to address the housing crisis and commit hundreds of millions of dollars to this effort.
Auerbach asked the panelists if there was something that the federal government could do to help scale successful local activities to other parts of the country. Hacke suggested the federal government should create a more rigorous requirement around community benefit that emphasizes efforts addressing the social determinants of health and to allow Medicaid funding to go for housing in more direct ways that are not a function of individual waivers. Mingo noted that what she is seeing is that many of the health systems investing in housing are mission driven. To encourage other health care systems to join in, the federal government might try to identify incentives that apply more broadly across the health care enterprise. ACOs, she pointed out, are at risk for their populations from birth until they mature into adulthood, a motivating factor for investing in the social determinants.
Owen said he would like to see the federal government create data standards and regulations around data privacy that would make data sharing easier across health care systems and community organizations. His second proposal was to change how the federal government reimburses risk-bearing entities in a way that incorporates information about the social needs of different patient populations. “If we did not spend a dollar more but recognized that social complexity is a predictor of health care costs, it could open more opportunities for health care organizations to be a resource and make this work possible,” said Owen.
Choucair had a list of five actions the federal government could take:
- Make sure affordable housing is an integral part of any potential infrastructure plan.
- Maximize funding for existing programs that work, such as Section 9 housing vouchers and the U.S. Department of Housing and Urban Development’s (HUD’s) Veterans Affairs Supportive Housing program.
- Fund replications of successful programs, and tie them to some of the U.S. Department of Health and Human Services’ programs that support people with substance use disorders or mental health issues.
- Create new competitive HUD funding modeled after the U.S. Department of Transportation’s Transportation Investment Gen
- erating Economic Recovery grants that push for innovation and out-of-the-box thinking on affordable housing.
- Create a housing stabilization fund that would provide one-time, short-term emergency housing assistance for people, so they do not end up on the street.
Katherine Berliner from the Center for Medicare & Medicaid Innovation asked the panelists to discuss one barrier each of their organizations has overcome. Hacke replied that this is a space where the perfect is the enemy of the good. “What we are learning is that if you get started in a way that authentically values community voice and you reach out to partners in an effort to do things together rather than alone, you will hear what the right answer is, and that right answer is different from place to place,” said Hacke. In her opinion, getting to the right answer is more about an approach and mindset than about any specific best practice. “The advice we are hearing is to say you want to help, then listen, and do what you are told,” she said.
Owen responded that it is easiest to gain both political and organizational momentum in these kinds of efforts by starting with obvious low-hanging fruit that will reduce health care costs in the short term. It is important to recognize, though, that there is a limit to what economic self-interest can accomplish, and it is probably not enough to fix the root causes of the social determinants and social needs.
Responding to a question about the degree that these interventions are replicable in a value-based world, Hacke said the problem is not so much that the solutions are not known, but that the nation and health care systems are not implementing them. Choucair countered that for an integrated health system such as Kaiser Permanente, value-based care is baked into the organization’s DNA. “For me, that puts the work we do at the core of our business strategy as opposed to this nice thing we do on the side,” said Choucair, who added this is why Kaiser Permanente has a chief community health officer as well as a chief medical officer.
Joanne Lynn from Altarum noted that a recent paper in the journal Health Affairs projected that a significant proportion of Americans age 75 and older will not be able to afford housing in another decade. Choucair replied that he was so disturbed by that projection that he sent it to every member of Kaiser Permanente’s national executive team and every regional president and executive medical directors. What he would like to see developed is the ability to use the EHR to predict who will need what interventions and be proactive about addressing their needs before they reach the point of having a housing crisis or food crisis, for example.
This page intentionally left blank.














