2
Practice and Policy Examples to Promote Family Well-Being: Successes and Challenges
The speakers whose presentations are covered in this chapter come from the federal, state, county, and tribal and community levels. They represent a variety of states and geographic areas, all of which are notably affected by the opioid crisis, and they have been working for the last several years on programs to help families, especially mothers and children.
FEDERAL LEVEL
The workshop featured two speakers from the federal level who are intimately involved in programs related to addressing parents and families plagued by the opioid crisis. The first speaker, J. Alice Thompson, is the Maternal Opioid Misuse model lead at the Center for Medicare & Medicaid Innovation (CMMI) in the Centers for Medicare & Medicaid Services (CMS). CMMI was created under the Affordable Care Act with a goal of testing innovative service delivery and payment models. The second speaker, Justine Larson, is the senior medical adviser for the Office of the Chief Medical Officer at the Substance Abuse and Mental Health Services Administration (SAMHSA). Both speakers highlighted lessons and successes that have been realized through their work, while noting there are continuing challenges, especially related to sustainability of funding when grants are used and the varying regulations of states’ Medicaid programs.
Center for Medicare & Medicaid Innovation
Thompson, a social science researcher, began by explaining that the purpose of CMMI is to test models, but the models have to meet one of three strict statutory requirements for success before they can be scaled up and replicated:
- quality improves; cost neutral;
- quality neutral; cost reduced; or
- quality improves; cost reduced (best-case scenario)
In terms of the opioid crisis, she described the road map developed by CMS, focusing on prevention, treatment, and data: see Figure 2-1.
Thompson went on to describe two key models related to the opioid crisis that CMMI has been working on, noting that because the CMMI budget is considerably larger than those of many other federal agencies, she believes the agency has great potential to influence changes. CMMI is very focused on aligning payments with either evidence-based or successful models of care. Knowing that increased funding doesn’t necessarily result in integrated care, sometimes even contributing to fragmentation, she said, CMMI tries to give states the ability to address this fact by embedding a learning and best practices sharing system in all models. The agency is also working on getting the system to operate in real time, as evaluations that occur 5 years after something is implemented do not allow rapid sharing of lessons that can address the current problem across communities.
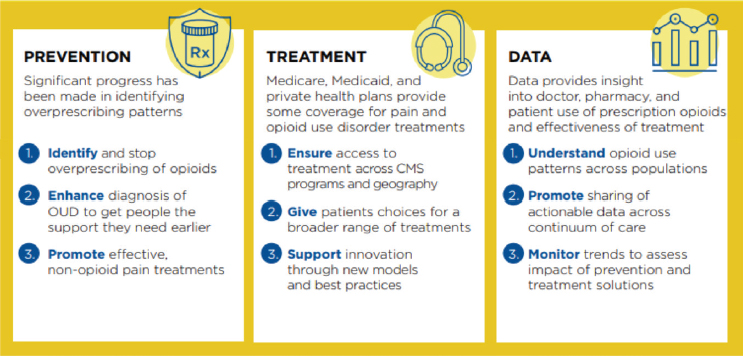
SOURCE: Centers for Medicare & Medicaid Services (2019).
Before describing each program in detail, Thompson mentioned two disadvantages to the CMMI models. One is that their focus is limited to children and families covered under the Medicare/Medicaid/Children’s Health Insurance Program (CHIP) umbrella, as the agency does not have the ability to change eligibility at the federal or state policy level. For example, Medicaid coverage covers women up to 60 days postpartum; while CMMI would be interested in continuing postpartum coverage for a longer time, it is bound by state Medicaid rules. The second disadvantage is that because these are federal programs, CMMI is looking at this issue from a national level, so it is more of a top-down approach, which can have limitations.
The first CMMI model Thompson described is called Integrated Care for Kids (InCK), a child-centered local service delivery and state payment model with the goals of reducing expenditures and improving quality of care for children covered by Medicaid and CHIP. The agency hopes to improve coordination and integration of a variety of services for children at risk of adverse outcomes, which demands cross-sector work. Grants or contracts for the 7-year model are awarded to lead organizations and the state Medicaid agency.1 This time frame includes 2 years for states to think through some key fundamentals before launching a program. A state develops a plan to encompass what the needs are and who should be involved (beyond the health sector). Once the funding is disbursed, the state and its partners develop an advanced payment model to be able to cover all of the necessary services. While states that achieve their goals can continue to receive funding, many programs are grant based so there is a sustainability concern for new programs. Some of the model interventions being used include
- early identification of health-related needs and risk factors by assessing children’s needs;
- integrated care coordination and case management of physical, behavioral, and other health services; and
- funding and support for development of a state-specific advanced payment model and infrastructure.
The second model Thompson described is the Maternal Opioid Misuse (MOM) model, which is expected to launch in 2020. This model focuses on improved quality and reduced costs for Medicaid-beneficiary pregnant and postpartum women with opioid use disorders and their infants. After feedback from stakeholders that the critical “wraparound services” (e.g.,
___________________
1 State applications for participation in this program are currently under review, and funding will be awarded to up to eight states.
family patient support, referral to community services) are not always reimbursable, or how to reimburse for them is unclear and so results in billing difficulties, CMMI developed this model with hopes of improving care for both mothers and infants, as well as increasing treatment funding for service delivery. The aim for this 5-year program is to ensure sustainability by the state Medicaid agencies, so by year 3 many of the services are being covered by the state or reimbursed as they transition away from the CMMI funding.
During the discussion, Thompson was asked about the types of payment models being considered in CMMI, and she shared some of the challenges. When the InCK team began its work, they started with pediatric accountable care organizations and hoped to find innovation. However, because people are typically uncomfortable taking on risk with children, there are very few advanced payment models for pediatric populations. She said the agency has similar challenges with pregnant women using opioids. While there might be best practices at various stages, no one is willing to do a payment bundle with that vulnerable population. In terms of cost, she said CMMI has been working with CMS actuaries to look at longer-term cost savings. Policy makers do know that such programs as the Accountable Health Communities model and Medicare Diabetes Prevention Program save money in the long term, but because these programs are focused on prevention, the savings will take several years to realize, which can often lead to a difficult conversation in the first few years of implementation.
Substance Abuse and Mental Health Services Administration
Larson began her presentation with some grim statistics of drug misuse in recent years, noting that 27 million people in the United States are using prescription or illicit opiates. For women of childbearing age (ages 15–44), 109,000 used heroin and 98,000 misused prescription opiates in 2013–2014. In describing this population, she also commented that poly-substance abuse, that is, the abuse of multiple substances such as alcohol or other drugs, is also common in women with opioid use disorder. Moreover, substance abuse in pregnant women has been rising at alarming rates, especially in the category of opioids: see Figure 2-2.
The unfortunate consequences of this substance abuse for pregnant women, beyond their own poor health and well-being, are the withdrawal and ongoing symptoms in babies as soon as they are born. The immediate adverse effects include premature deliveries, increased lengths of hospital stay, lower birthweights, and higher rates of neonatal abstinence syndrome. Studies on cognitive and academic development of children with the syndrome or those born to mothers who misused substances are beginning to show a widening gap as children get older when they are compared with
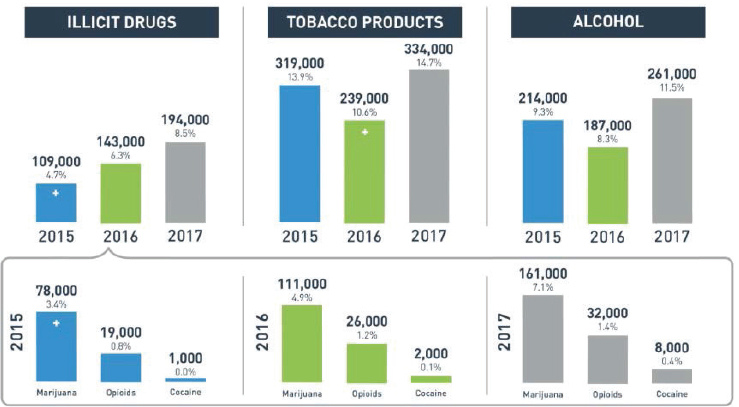
SOURCE: Substance Abuse and Mental Health Services Administration (2018).
unaffected children. Even though differences may not be apparent at birth, the gaps in neurocognitive, behavioral, and developmental outcomes become clear as children reach preschool and school age (Larson et al., 2019).
Considering all of the research findings, Larson said, SAMHSA identified several priorities, including understanding the interactions of various substances, optimizing maternal pharmacology, including the role of fathers, and figuring out the right service delivery models that will result in the best longitudinal outcomes. One of the agency’s future efforts in this area will be education, she noted, in response to information from colleagues at other health agencies—such as the Administration for Children and Families and the Health Resources and Services Administration—that people working in early childhood systems want to help but don’t know how to connect parents to appropriate treatment programs for adult substance use.
Larson also shared some of the resources and initiatives available through SAMHSA related to family well-being and pregnant women with opioid use disorders. Numerous policy and practice considerations are included in the agency’s A Collaborative Approach to the Treatment of Pregnant Women with Opioid Use Disorders (Substance Abuse and Mental Health Services Administration, 2016). SAMHSA has also developed high-level federal workgroups to convene stakeholders across several federal agencies to better synergize policies and funding and to orient programs to best serve families, such as shifting to more family-based rather than individually focused treatments. These workgroups include one focused
on the impact of opioids on young children and families, as well as on the 2015 Protecting Our Infants Act, which addresses problems related to prenatal opioid exposure and includes several mandates for the Department of Health and Human Services. Additional resources and fact sheets that Larson shared are described in Box 2-1.
STATE AND COUNTY LEVELS
The two presentations covered in this section represent the state and county levels to examine some of the programs that are closer to the ground and use different approaches for services targeting communities.
Children’s Services Society of Utah
Bacall Hincks, administrator for the Grandfamilies Kinship Care Program at the Children’s Service Society of Utah, began by describing the motivation for the inception of the program in 2002. Many people began coming to the agency who were grandparents taking care of young children and did not feel equipped to do so. She defined “kinship care” as not just grandparents, but also other members of an extended family or even close neighbors or friends who have stepped in to care for children when the parents aren’t able to do so. The benefits of having children raised by family instead of entering the foster care system include increased permanency for the children, more safety in the home, and better mental health outcomes. Also important, she said, the children are able to retain some ties to their cultural identity and often report a greater sense of belonging and stability (Epstein, 2017).
With all of this in mind, Hincks said, the agency created the Grandfamilies Program with a focus on various tiers of intervention for this population in Utah. Interventions include case management services, support groups at various age levels, and counseling services specifically for youth, recognizing that most children who enter the agency’s care have at least four adverse childhood experiences.2 Providing some mental health prevention services can help ensure they have healthier futures. Some of the program’s support group activities include the following:
- Adult support groups: Discuss parental rights, issues with loss and grief, the challenges with parenting two generations (in the case of grandparents). The agency also provides education on substance abuse and addiction, as well as risk and protective factors for children in kinship care.
- Children and teen support groups: Introduce interpersonal skills, develop healthy self-esteem, and normalize living in a different family situation. The program also teaches coping skills, such as how to handle peer pressure and anger management.
- Friend 2 Friend (after graduating from previous programs): Offer peer support and ongoing connections through social activities for children, teens, and families. The program organizes a wide range of activities, including summer BBQs and parties, art therapy, and tickets to local events.
___________________
2 “Adverse childhood experience” is a term used to describe all types of abuse, neglect, and other traumatic experiences that occur to children under age 18. These potentially traumatic events can have lasting negative impacts on physical, mental, and emotional health and well-being. See more at https://www.cdc.gov/violenceprevention/childabuseandneglect/acestudy/index.html.
Responding to a question about handling grief for those children who have lost parents, Hincks acknowledged that Utah has ranked very high in rates of overdose deaths, so the agency is familiar with this burden. She explained that the program uses trauma-focused cognitive behavioral therapy3 and also employs therapists that specialize in grief and loss. And though loss due to death is permanent, the program often does similar grief work with children whose parents may still be alive but have effectively lost them because of drugs. She added that this grief can be compounded with other feelings, which emerges as a larger issue with older kids, who often feel guilty about not being able to stop their parents abuse, and fear—especially when mom or dad is in recovery—that they will not be able to prevent them from relapsing. Given the amount of heavy psychological work that the program undertakes, Hincks also commented on the importance of resilience training for staff members. Many of the social programs and events can be just as beneficial for the staff as the people in the program, as it gives them a chance to see positivity and hope amid what can be a lot of negativity and loss.
Wise County, Virginia
Chuck Slemp, commonwealth attorney for Wise County (and the city of Norton), Virginia, described the demographics and geography of his community to better depict the situation and challenges. Located in a far western corner of Virginia, 22 percent of the total county population and 28 percent of the children live below the poverty line. The county is also at the epicenter of the opioid crisis, with overdose deaths that average 48 per 100,000 population—one of the highest rates in the state. Unfortunately, he noted, the county also has a high rate of drug-related driving under the influence offenses, as well as high rates of children in foster care and children who have been abused or neglected. With many people leaving the community because of reduced job options in the coal industry, Slemp described the budget challenges he faced: he was asked to cut significant amounts from salaries, schools, and public funding. Yet, he said, the jails were expanding, and the county was spending more than $3 million per year to incarcerate people, with the majority of cases being drug related.
With all of this as a backdrop, Slemp emphasized people’s realization that a generation of children in their community was now being raised by grandparents and great-grandparents, and the justice system could do something about it. After much discussion with people in the community and
___________________
3 Trauma-focused cognitive behavioral therapy is an evidence-based treatment for children and adolescents affected by trauma and their parents or caregivers. See more at https://tfcbt.org/about-tfcbt.
civic leaders, the county created an alternative sentencing program called Wise Works: it is designed to include community service programs that allow low-level offenders an opportunity to complete community service in lieu of jail time. The offenders are not paid, but the program tracks the hours that they work until they reach their “alternative sentence.” Types of community service range from litter pickup and lawn mowing to working in a soup kitchen, a food bank, or an animal shelter. The program has 25 different community organizations that participate, allowing needed work to be done, keeping people out of prison and with their families, and also oftentimes providing them with valuable job skills and stimulating more engagement in their community. Importantly, for those offenders who have children, they are also able to stay at home and provide care instead of that responsibility falling on other family members or people in the community.
Slemp highlighted some of the success stories in the program as well as the benefits to the community after just a few years of operation. Many graduates of the program have gone on to obtain full-time employment, and several current participants are being considered at their service sites for employment opportunities. As of April 2019, the program has had 67 participants, with more than 2,000 hours worked by each one, with a successful completion rate of 63 percent. On the community side, he said, the county saved thousands of tax dollars by not paying daily incarceration fees, as well as not paying for the service work that has been completed. The savings to Wise County totaled $425,334 in jail costs; and in just the last quarter, the county received roughly $340,000 back from the jail in overpayments. These savings allowed the county to avoid laying off teachers and closing schools this year, which had been considered due to tight budgets.
Responding to questions about the ethics of free labor, Slemp agreed the issue requires a careful balance: The county tries to focus the program mainly on giving each person a chance to change his or her future and on prosecuting the right people so that the environment is no longer conducive to drug use and offenses. For example, he said, since he joined the attorney’s office 3 years ago, the county has shut down three doctor’s offices that were responsible for drug distribution, which has resulted in a decrease in drug crimes. While it is too soon to do a robust evaluation of recidivism rates, Slemp said, he has noticed a positive trend and is hopeful the community will continue down this path.
TRIBAL AND COMMUNITY LEVELS
The final set of presentations focused on the work being done in the communities most affected by the opioid crisis. It featured three speakers from different parts of the country sharing some of their challenges and successes on the ground in addressing the well-being of families and children.
Bighorn Valley, Montana
Shelly Sutherland, chief community development officer at Bighorn Valley Health Center in Montana, described her community as mainly Native American. She said 70 percent of the county lies within Crow Nation, but it also includes the northern Cheyenne reservation, so the center serves two tribes across the county. Unfortunately, she said, the community has very high needs but low resources: It is in last place of the 48-county health rankings in the state. Some of the challenges include high rates of smoking, sexually transmitted diseases, teen pregnancy, and poverty and few employment opportunities. With the economic hit to the coal industry, these challenges, paired with a population to mental health provider ratio as high as 1,910:1, result in many people turning to substance abuse.
Sutherland explained that the mission of the Bighorn Valley Health Center is to identify the health needs and focus on improving social determinants of health to improve overall outcomes. To do this, the center first focuses on direct resource connection, providing a “warm handoff” to other services through community-based organizations for those who need it. Another focus area is early childhood; and in 2012, the center launched a best beginnings coalition that features evidence-based home visiting programs including parents as teachers and the importance of self-care. Unfortunately, though the coalition offers prenatal services, many mothers do not receive any prenatal care because of the limited availability in the county. There are no labor and delivery services in the county, so pregnant women get referred to larger hospitals in Billings—which can be more than 1 hour away—for delivery when they are around 30 weeks into the pregnancy. The center’s third main focus area is substance abuse and opioid use disorder including both prevention and treatment aspects. Bighorn Valley also has nurses conduct home visits with pregnant women and families to promote healthy pregnancies and provide connections to all potential resources before babies are born, tackling both healthy pregnancy and substance use disorders.
In closing, Sutherland emphasized that the center uses the Communities That Care4 framework, which guides intergenerational work in increasing protective factors while mitigating the impact of risk factors for the families in her community. The core philosophy is integration, so everyone is working to integrate their programs across the spectrum with an underlying thread of strengthening families and improving resilience in the face of the many challenges that remain in their county.
___________________
4 Communities That Care is a prevention program that uses a public health approach to prevent youth problem behaviors. See more at https://www.communitiesthatcare.net/about.
Comanche Nation, Oklahoma
Martin Flores, the partnership for success specialist representing the Comanche Nation and the South Plains Tribal Health Board in southwest Oklahoma, opened his remarks with a full introduction of himself in his native Comanche language. He described the local program—IAMNDN—which stands for I am native drug-free nations. The IAMNDN goal is to prevent underage drinking and misuse of prescription medications and bridge the gaps among youth, adults, and elders in the community. He highlighted a fundamental piece of the program: learning and focusing on their culture and using that as a form of prevention. IAMNDN educates youth on the “old ways” of doing things within the Comanche culture, their language, the history of their tribe, the challenges they have been through, and tries to instill more of a positive identity that can prevent them from misusing or abusing substances. To give more of a visual example of some of the strategies the program uses, Flores showed an IAMNDN video for the workshop attendees.5
In response to a question on staff resilience, he added that they also use their cultural and historical methods for self-reflection. With an emphasis on spirituality, he said, they use sweat lodges, Native American churches, and teepees to try and purify themselves of negativity, all of which have a lot of meaning in their culture. Following a question about the difficulty of balancing evidence-based projects with culturally appropriate applications, Flores explained that the program’s funder, SAMHSA, has been very flexible in terms of cultural adaptation and has allowed them to adapt the requirements to their program and needs.
Nationwide Children’s Hospital, Columbus, Ohio
Kelly Kelleher, vice president of community health at Nationwide Children’s Hospital, began his presentation by noting that reducing opioid use requires intervention at several levels. The first step is to discuss reducing poverty and building resilience in local communities in central Ohio, he said, and he introduced some of the hospital’s key principles to improve lives for their neighborhood. These principles support a public health approach for the 34 counties covered by their hospital:
- Reduce the quantity of drugs in the community.
- Keep families together.
- Keep families out of poverty.
___________________
5 The video can be found on YouTube at https://www.youtube.com/watch?v=WeScy_XgrhY&feature=youtu.be.
Kelleher elaborated that the hospital has several efforts on reducing overprescribing to achieve the first principle. Related to the second principle, he noted that the Columbus city attorney recently announced support for removing misdemeanor bail requirements for people of low socioeconomic status in the community. Without bail reform, he said, keeping families from some communities together will be extremely difficult.
Expanding on the third principle, he reiterated a suggestion from earlier workshop discussion on developing a common set of talking points across geographic areas and civic levels to be able to strongly articulate evidence on poverty reduction in terms of housing and eviction policies, wage policies, and employment policies. In Columbus, he continued, 65 percent of all evictions are young, single women with children, who are disproportionately black. Regarding employment, which can be especially important for health outcomes, there are still many states that have rules preventing the hiring of people with a criminal record. Sometimes this can be overcome on an individual case-by-case basis, but it’s currently a form of guerilla warfare, he said, calling for a broader policy change to really influence the ability of families to stay together with gainful employment.
Kelleher next turned to details on a few relevant clinical programs for helping families affected by opioids at his institution. With Ohio as one of the worst states in the United States regarding opioid death rates, he emphasized the consequential challenge for babies, with Nationwide Children’s Hospital seeing the largest number of babies with neonatal abstinence syndrome (NAS) in the United States, and they have very long average lengths of stay. Figure 2-3 shows the rates for opioid overdose deaths per 100,000 deaths and NAS per 1,000 births for the country, Ohio, and Rhode Island. Kelleher used Rhode Island as a comparison to Ohio, drawing on data from the Neighborhood Health Plan of Rhode Island (Neighborhood Health Plan of Rhode Island, 2018).
In addition to these burdens, Kelleher said, the hospital also began to recognize that many women in treatment had limited knowledge about sexual health and actually did not want to become pregnant at all but were not using effective birth control methods. Some of the treatment clinics he is involved with reported more than 90 percent of pregnancies being unwanted. With all of this in mind, he described some of the programs that have been put into place in central Ohio to try and address these issues at four stages: preconception, prenatal, immediate delivery/postpartum, and hospital discharge up to 90 days. He also offered three considerations that they have to keep in mind while working with women affected by opioids:
- stigma and fear of losing custody of their children;
- history of abuse and trauma from trafficking, drug trade, and violence; and
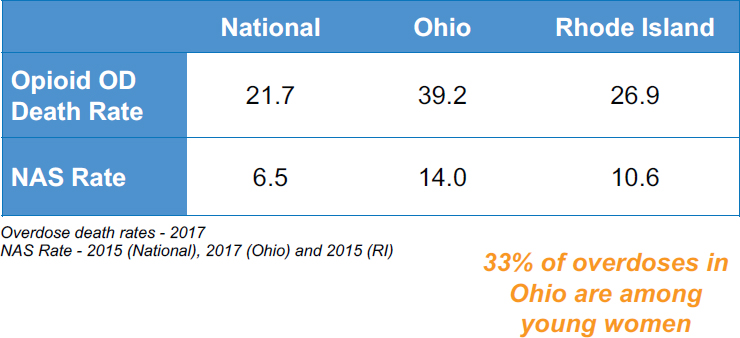
NOTE: NAS = neonatal abstinence syndrome.
SOURCES: Kelly Kelleher presentation, June 6, 2019. Data from Centers for Disease Control and Prevention, Kaiser Family Foundation, Neighborhood Healthy Plan of Rhode Island, and Ohio Department of Health.
- trust in legal substance use providers but often not in other health care providers.
Because of the strong trust that most women had in their substance use providers, the program decided to locate most of their resources and services at those locations for Columbus. All of the large facilities that provide medication-assisted therapy in Columbus to young women are now also beginning to offer primary care and women’s health services. They are branding the centers under a “women’s health” umbrella, which can help to address stigma; they have made automated appointments available; and they are adding mobile sites to increase access. Finally, for the immediate postpartum/delivery and discharge periods, they are focusing on adjusting typical neonatal intensive care unit care to be more appropriate and specific for the needs of babies with NAS. As a result, the average length of stay for babies was reduced from 58 days in 2009 to 29 in 2012 and then to 17 in 2018.
In addition to this different type of provider training, the program is also working to address challenges in the transition period and moving mothers and their babies to “step-down” facilities, which can provide an intermediate level of care for patients. Although neither the mothers nor their babies may need the acute clinical services available in a hospital, keeping them in hospitals has often been the only way to provide joint services because of insurance rules. To try to help this situation, Kelleher explained,
the Partners for Kids Program,6 is working to be able to get the needed extra days of hospitalization paid for and be able to discharge the mothers and babies to transitional residences where they can be in a home environment with supportive care, surrounded by other women experiencing the same challenges. Kelleher concluded with an emphasis on the importance of partnerships in work of the Nationwide Children’s Hospital, noting that continued efforts to try and speak the same language as treatment groups, health care providers, and community groups will go a long way in serving their populations.
___________________
6 Partners for Kids is a pediatric accountable organization that partners Nationwide Children’s Hospital with more than 1,000 doctors. See more at https://partnersforkids.org.














