2
California Wildfires: Past and Future
The first set of presentations at the workshop provided an overview of wildfires in California and, to provide a broader geographic context, a particular wildfire in southwestern Colorado. Speakers examined the contributions of climate change to more frequent and intense fires, the range of potential responses to wildfires, and some of the ways in which consideration of health equity can increase preparedness.
THE ROLE OF CLIMATE CHANGE IN CALIFORNIA WILDFIRES
“Climate change, which was knocking on our door in the late 1990s and early 2000s, has fully entered our living rooms,” said Benjamin Houlton, professor of global environmental studies and director of the John Muir Institute of the Environment at the University of California (UC), Davis. Today, climate change is manifesting itself in weather extremes, including hurricanes, droughts, and wildfires, all over the world, whether heat waves in India or flooding in the American Midwest or extreme heat events and wildfires in California, said Houlton. “Our continued reliance on fossil fuels and greenhouse gas emissions is putting its foot on the pedal in terms of creating risk.”
In a 2018 report, the Intergovernmental Panel on Climate Change (IPCC) warned that the world must limit global temperature increases to less than 1.5 degrees Celsius to avoid the worst impacts of climate change, including the loss of coral reefs and other ecosystems, the thawing of permafrost, heavy precipitation events, and forest fires (IPCC, 2018). But California has already exceeded a 1.5 Celsius degree rise in average temperature, Houlton observed (see Figure 2-1). Average temperatures will continue to fluctuate from year to year but will continue to rise over time. “We are already in a period in which we have dangerously interfered with the climate system, and that is causing massive changes here in California.”
California, which emits about 1 percent of the world’s greenhouse gases, has led the way among states in adopting policies to reduce emissions, including a cap-and-trade system. As another example of this commitment, Houlton noted that, under President Janet Napolitano’s leadership, UC announced the Carbon Neutrality Initiative in 2013, seeking to achieve net-zero greenhouse gas emissions in the university’s buildings and vehicle fleet by 2025. Nevertheless, the state is going to have to brace for an increasing number of climate impacts, he said.
A recent climate assessment conducted by Houlton, his colleague Jay Lund, and researchers from across California found that, based on climate change models, Sacramento’s climate in the latter half of the 21st century will resemble that of Phoenix (Houlton and Lund, 2018). Instead of the past average of 4 days per year above 104 degrees Fahrenheit in Sacramento—an average that may already be closer to 10 days per year—the city will experience an average of 40 days per year above 104 degrees. The result will be “substantial public health risk,” said Houlton. “We have to start preparing for these changes in extreme heat.”
Even as average temperatures have been rising in California, the state has experienced 8 of its 10 largest wildfires since 2000. The Camp Fire, which caused at least 85 fatalities and $16.5 billion in damage, was the most expensive natural disaster in the world in 2018. Furthermore, that
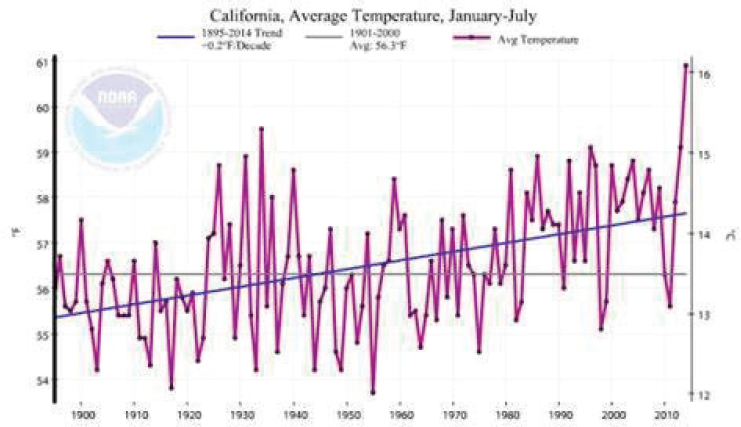
SOURCES: National Oceanic and Atmospheric Administration National Centers for Environmental information, Climate at a Glance: Statewide Time Series, published May 2019, retrieved on May 28, 2019, from https://www.ncdc.noaa.gov/cag. Presented by Benjamin Houlton.
$16.5 billion does not include the loss of potable water in many locations, the loss of economic activity, the disruption to schools, or other impacts, Houlton noted. The estimated loss “is a conservative estimate of the real impacts of a single fire event.”
Analysis of the biggest and most destructive wildfires shows that they tend to occur during drier and warmer conditions (Rohde, 2018). As conditions in California have become warmer and drier in recent years, the incidence of extreme wildfires has been growing. Other factors also play a role in larger and more destructive fires, including past fire suppression and ecological changes. However, Westerling et al. (2006) found that regional forest wildfire activity increased substantially since the mid-1980s and is strongly associated with warmer temperatures, earlier spring snowmelt, and increased climatic water deficit. Littell et al. (2009) concluded that roughly 39 percent (during the period 1916–2003) to 64 percent (during the period 1977–2003) of the fire area burned can be related directly to climate in the western United States, while Abatzoglou and Williams (2016) attribute at least half of the recent increases in burned western U.S. forest area to anthropogenic warming.
Based on an ensemble of global climate models, and using the business-as-usual scenario in terms of global greenhouse gas emissions, which is the current trajectory of emissions, the mean area burned in California, compared with the period 1961–1990, will increase by a projected 77 percent by the end of this century (Westerling, 2018). Extreme wildfires—those larger than 10,000 hectares, or 24,710 acres—will occur 50 percent more frequently. “We will likely be seeing fires that will make the previous fires look small by comparison.”
The vegetation of California is also expected to change dramatically as the climate changes. Dass et al. (2018) predicted that grasslands will expand and forestlands will shrink, with the transition from trees to grass often involving wildfires. Treatment of forestlands through tree thinning and controlled burns can reduce these losses, Houlton noted. Comparing the periods 2070–2099 and 1961–1990, a management scenario that treated about 30 percent of the vegetated area was projected to reduce the Sierra Nevada area burned by the end of the century by 16 to 31 percent (Westerling, 2018). Similarly, Liang et al. (2018) showed that large-scale restoration of forests reduced the incidence of extreme wildfire events.
Wildfire risk reduction is expensive—California is already spending more than $200 million per year in such efforts. But many other pathways to the same end are available, Houlton said. California is starting to see the emergence of green bonds, where investors fund municipalities and industries that are using hydroelectric power, and those industries deploy a workforce to clear forest environments and reduce wildfire risk (see Figure 2-2). The return on investment for the industries is a reduction in mudslides and other events that disrupt the operation of hydroelectric power plants.
Another option, said Houlton, would be to start treating climate change as a pandemic. Houlton said that more than 250 million people are being exposed to health hazards associated with climate change worldwide. “That rises to the level of what I would consider a pandemic, but it is obviously quite different in terms of the way that it manifests itself. This is a major question that I hope we can make inroads on as we move forward in solving the challenge.”
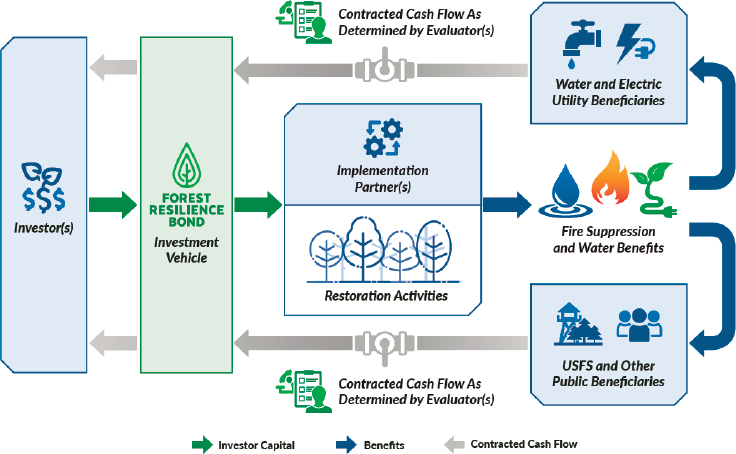
NOTE: USFS = U.S. Forest Service.
SOURCE: Presented by Benjamin Houlton.
HEALTH AND MEDICAL RESPONSES TO THE CALIFORNIA WILDFIRES
In California, the Emergency Medical Services Authority within the Department of Health and Human Services partners with the Department of Public Health to provide Emergency Support Function (ESF) #8, which is the public health and medical response to disasters. California has been planning for decades to respond to earthquakes, but it had not done specific planning for fires, said Howard Backer, director of the California Emergency Medical Services Authority. As a result, “our response to fires has all been empirically developed. Obviously, the same emergency management principles apply to fires, but there is a very distinct pattern of need that is emerging.”
The providers of emergency medical services have multiple responsibilities. They respond to 911 calls and to multi-casualty incidents. They have a role in the evacuation of patients from facilities and in the movement of patients to safe facilities or shelters. They help to ensure that displaced populations get medical care. As Backer pointed out, UC Davis was the closest large medical center to the Camp Fire. It both provided medical personnel to travel to the Chico area and accepted patients from the fire area.
The 911 response is quickly overwhelmed in rural areas during disasters, Backer remarked. At that point, other units are pulled in from surrounding areas, including units used for inter-facility transport and other purposes. California has about 40 ambulance strike teams, consisting of 5 ambulances plus a lead vehicle, which can come from other jurisdictions to work in the field for 3 days without having to go back to their home base. California also has a national ambulance contract, which is used quite often in the southeastern United States to respond to hurricanes but has rarely been used in California. “We had ambulances and wheelchair vans and buses and all levels of transportation staged. You call them up and they pick up people in an orderly fashion—that is, when you have time,” he stated. In the case of the Camp Fire, there was not enough time. In the evacuation of the Adventist Feather River Hospital in Paradise (e.g., the employees of the hospital, fire personnel, and visitors loaded patients in any available vehicle in addition to local ambulances because the ambulance strike teams could not reach the hospital in time). During the Napa/Sonoma fires of 2018, more than 200 residents of a center for the severely disabled, many with special beds, medications, and other medical equipment, had to be evacuated not once but twice, eventually to fairgrounds 50 miles from the center. “We had to basically re-create a hospital within an exhibition hall,” said Backer. In addition, the staff of the facility left their local communities and traveled to the fairgrounds to take care of their patients “because these patients have highly specialized needs, and it would be very challenging for providers unfamiliar with them to provide optimal care.”
Many kinds of professionals responded to the Camp Fire, including 135 members of California Medical Assistance Teams, staff from health care systems, 70 California Air and Army National Guard members, 28 National Disaster Medical System task force team members, 116 disaster health care volunteers, and 419 California Veterinary Medical Reserve Corps volunteers.
The California Health and Human Services Agency (CHHSA) tracks the availability and status of all licensed facilities, not just acute care facilities and long-term care facilities, but convalescent homes, residential care, and other facilities licensed by the Department of Social Services. CHHSA maintains a Geographic Information System map with the locations of these facilities on which it can overlay fire perimeter and smoke plume maps, enabling monitoring and response to the health, medical, and social services needs generated by a wildfire. “This is the type of thing that we have to get used to now,” said Backer. CHHSA also has statutory responsibility for ESF #6, which coordinates mass care and shelter.
The Camp Fire generated up to 50,000 evacuees, destroyed more than 18,000 structures (including almost 14,000 residences), and caused at least 85 fatalities. Most of those who died were elderly, observed Backer. “This
was a retirement community. Most of these people were in their 70s. They could not get out and get away from this fire fast enough.” The survivors ended up in multiple shelters in Chico, Oroville, and other communities. “It was our job to provide medical care for these survivors,” said Backer.
The disability community had been urging emergency personnel to treat everyone in general population shelters, not medical shelters, but that created special challenges with the Paradise evacuees, said Backer. “It was an elderly community with a lot of health problems that resulted in a much higher level of medical need. Every one of those shelters had to have a medical operation.” Replacing medication was especially difficult given how quickly people had to evacuate, requiring that pharmaceutical areas be set up in the shelters. Emergency personnel also took advantage of the federal emergency pharmaceutical program for uninsured patients to fill prescriptions at no cost.
California has a system to access medical records that can be switched on during disasters.1 That was very helpful during the Camp Fire, said Backer, not only for knowing what medications people were on but also their medical problem lists.
Public health was also at risk, as demonstrated by a norovirus outbreak that occurred in multiple shelters. Norovirus is highly infectious through interpersonal contact or contact with objects in the environment and can be aerosolized through vomiting, all of which led to a spreading outbreak. Local and state public health departments sent in infection-control nurses who went from shelter to shelter training staff on optimal infectious precautions and control measures. The emergency shelters initially had only about one-third of the ratios of toilets and showers to population needed under these conditions. “We brought in more hand-washing stations, showers, and toilets, and set up services to get them cleaned multiple times each day,” which required that the workers use adequate protection. Isolation tents were set up at every shelter to keep the sick away from the general shelter population. All of these measures finally enabled emergency response workers to get the outbreak under control. Medical personnel also started giving flu shots, because California was headed into the flu season.
This kind of medical and public health response requires “a large management structure,” said Backer. Incident management teams worked both in the field and in the department to manage logistics.
Backer closed by briefly discussing the prospect of voluntary power shutdowns. After the Camp Fire, utility companies announced that when the wind reaches a certain velocity with low humidity, power companies plan to turn off the power to avoid starting fires and avoid the liability
___________________
1 For more information, see http://www.ca-hie.org/initiatives/pulse (accessed October 17, 2019).
for the fires. But many patients depend on power for their wheelchairs, oxygen concentrators, ventilators, and other equipment, and medical facilities and emergency departments all need power. “We might be evacuating medical facilities because we will not know how long the power is going to be out, and their generators malfunction or are not adequate to provide necessary services,” said Backer. The emergency response may even need to consider establishing power shelters to provide power for recharging critical devices.
LESSONS FROM COLORADO
About 1 year before the workshop, the 416 Fire in southwestern Colorado became the sixth largest fire in Colorado’s history. Liane Jollon, executive director of San Juan Basin Public Health in Durango, Colorado, which is the local public health agency, explained that many of the 70,000 or so people in the two-county area are involved in the outdoor and tourism industries or are retirees or telecommuters. As a result, up to half of the economy in the area is at risk from wildfires or other significant disasters.
Two months before the 416 Fire, southwestern Colorado was in a state of exceptional drought, the most intense category of the five drought conditions. The next month, May 2018, a drought task force established by the governor came to the area to learn what its needs would be because of the drought. Planning proceeded for potential impacts to agriculture, municipal water, wildlife, public health, water quality, tourism, energy, and the economy, with a particular focus on health equity. For example, the state identified agricultural needs associated with the drought, though local planners knew the local communities had seen many years of dryland farming with limited income and rangeland issues. “People were selling off cattle and not performing economically. That was an issue,” said Jollon. Similarly, on a local level, half the population in the area is on small public water systems or wells, and many people haul water to their residences. When municipal systems run short, people cannot buy water to haul. “We have people with domestic shortages long before we reach statewide issues,” said Jollon.
Another issue was that the area had an emerging issue with its homeless population. “When public lands are closed, this population has nowhere to live, raising a major health equity issue that,” said Jollon, “no one was prepared for.”
The state drought task force did not focus on the potential for wildfire impacts, despite the obvious risks. Then, on June 1, 2018, the 416 Fire broke out. San Juan Basin Public Health responded by providing planning and evacuation support for medical and health facilities, evacuation support for individuals with additional needs, information on air quality and health for the community, help with the multiple mudslides and debris flows that started while the fire was still burning, and disaster assistance centers. Jollon cited several lessons learned from this experience:
- Additional consultation is needed with long-term care facilities to support their evacuation needs.
- Additional time and support are needed to evacuate persons with complex medical needs, mobility limitations, or a need for medical equipment.
- Additional time is needed to create or translate materials into other languages (primarily Spanish).
- People experiencing homelessness pose additional considerations when they come to shelters or need resources.
- People had many questions about the impact of air quality on individuals with specific needs.
In general, the community did not have the right things in place to meet the needs of the area’s most vulnerable populations, Jollon said, creating a deficit that local government agencies and nonprofit organizations worked to fill. She also called attention to the mudslides and debris flows that resulted from the fire. These “proved to be more traumatic and more difficult for the community” than the fire, she said, “and also had larger impacts on our more vulnerable populations.”
Though the community sought to get the word out that it was open for business, the poor air quality drove down tourism. As a result, sales tax receipts dropped 25 percent in June. “June is like our December,” said Jollon. In retail, “December is where you make all your money. In our communities, folks put it in the bank in June, and they make it through the year based on what they did in June. Many businesses closed. We still have vacancies in the downtowns that were affected by this fire a year later. That was unexpected,” she said.
San Juan Basin Public Health pushed to open a disaster assistance center during the response to the fire to meet the needs of people who were economically displaced. In a tourist economy, many were working in jobs without a safety net, she said. She added,
We have restaurant workers. We have lodging workers. We have folks who work on the train, and the train was not running because the public lands
were closed. We have folks who do outdoor recreation and mountains and rivers. None of these folks were getting paychecks, and certainly they do not work in sectors where there is a safety net.
The disaster assistance center opened about 1 week into the fire and played an important role in the response and recovery.
Since the fire, San Juan Basin Public Health has received some health equity funding to bring together community partners who serve underserved and vulnerable populations with emergency managers. The goal is to bridge the disconnect between these two groups to prepare for both the short- and long-term needs of people affected by wildfires and other natural disasters. “Wildfire is not a short-duration incident,” Jollon concluded. “It has a long history of health equity issues.”
DISCUSSION
During the question-and-answer period, Houlton noted, in response to a question about water quality, that much water contamination occurs because of flame retardants. Also, if a house is burned, household chemicals can be released into local water systems, and some toxins accumulate in ash. “My sense is that, in the Camp Fire, you are looking at at least a decade of significant impacts to the water and soil, and perhaps longer depending on circumstances,” he said. “It needs much more research.” Jollon also noted that contamination is both an acute and a long-term problem. During fires, small public water systems are often compromised because of backflow if the pumps are not turned on. People can return home to no water or to contaminated water and not know it.
In response to a question about the role of environmental health divisions, Jollon noted that these are mostly small and local in Colorado. Her agency was not in charge of air quality, for example, but it was in charge of quality advisement for drinking-water and restaurant inspections. It concentrated its work on the domestic water supply and on making sure that when restaurants reopened after the fire, they were serving safe food.
Kizer noted that for many years he oversaw environmental health when he was director of health for California. In California, some of the larger counties have their own environmental health divisions. For many of the smaller counties, including the counties usually impacted by wildfires, the state assumes that role and oversees responses to wildfires, including their environmental aspects.










