Proceedings of a Workshop
| IN BRIEF | |
|
December 2019 |
Advancing Effective Obesity Communications
Proceedings of a Workshop—in Brief
On September 16, 2019, the Roundtable on Obesity Solutions of the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine, held a public workshop, Advancing Effective Obesity Communications, in Washington, DC. The workshop explored effective communication of obesity-related issues by providing an overview of the current communications environment and addressing the complexity of identifying key audiences and developing targeted messages. Speakers discussed communications strategies to reach specific intermediary audiences, such as the public, decision makers, and policy makers. The workshop also explored challenges in communicating about obesity issues, which include aligning the intended meaning of messages with an individual’s perception of and response to those messages, addressing obesity bias and stigma through communications, and addressing misinformation.
This Proceedings of a Workshop—in Brief highlights the presentations and discussions that occurred at the workshop and is not intended to provide a comprehensive summary of information shared during the workshop.1 The information summarized here reflects the knowledge and opinions of individual workshop participants and should not be seen as a consensus of the workshop participants, the Roundtable on Obesity Solutions, or the National Academies.
OVERVIEW OF COMMUNICATIONS AND THE COMMUNICATIONS ENVIRONMENT
The workshop’s first session provided a grounding in the discipline of communications and an overview of effective communications strategies. Adelaide Feuer, senior vice president at Edelman, set the stage by sharing foundational communications concepts from a communications agency perspective. At its most simple form, began Feuer, communications includes a sender of information whose goal is to convey a message, and a receiver of that information. Public relations, she continued, is a strategic communication process that builds mutual trust among organizations, communicators, and their publics, according to the Public Relations Society of America. Public relations takes many forms, including organizational communications; brand communications; and public affairs communications, which includes science, research, and policy communications. Feuer explained that effective communications can help educate and produce awareness, build relationships and trust, and change attitudes and behaviors. These outcomes, she said, are indicators that measure the success of communications.
Feuer moved on to discuss macrolevel changes affecting communications, with a focus on two key areas. First is the global implosion of trust, she said, noting that Edelman’s annual survey of trust has measured a substantial erosion of trust worldwide, particularly in recent years. Feuer reported that according to the 2019 survey, consumers in the United States now consider peers more credible than academic experts, journalists, business leaders, and government officials, and they have subjective definitions of who they consider “experts” (see Figure 1).
Feuer displayed an illustration of the expert ecosystem, in which reputational influencers (e.g., credentialed thought leaders), cultural influencers (e.g., celebrities and bloggers), and media influencers simultaneously influence both one another and their target audiences, directly and through the audience’s peers.
The second macro-level change, said Feuer, is shifts in consumption of content. One source estimated that people filter up to 5,000 messages per day, she reported, many of which come from social media (Story, 2007). More recently, she added, occurrences of fake news and privacy concerns have contributed to decreased trust in search engines and social media platforms compared to primary journalism sources, according to Edelman’s survey.
___________________
1 The workshop agenda, presentations, and other materials are available at http://www.nationalacademies.org/hmd/Activities/Nutrition/ObesitySolutions/2019-SEP-16.aspx (accessed November 18, 2019).
![]()
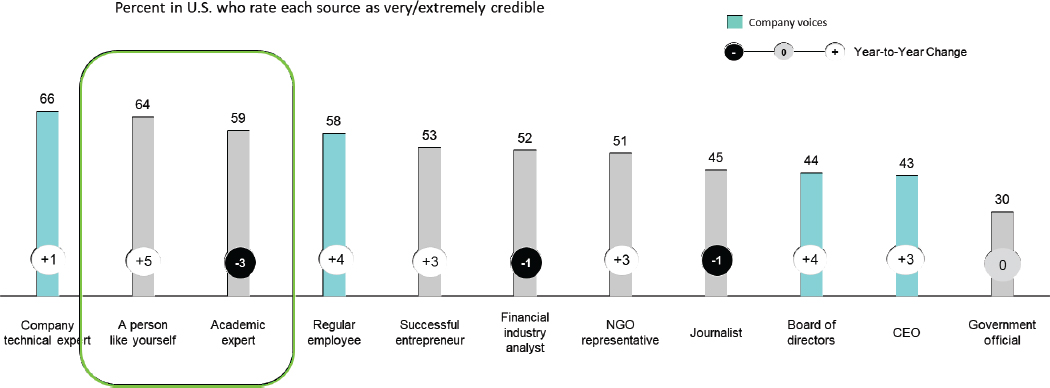
NOTES: The question that follows was asked of half of the sample, which was comprised of the United States general population. In general, when forming an opinion of a company, if you heard information about a company from each person, how credible would the information be—extremely credible, very credible, somewhat credible, or not credible at all? The responses were rated on a 4-point scale. The two boxes indicating “a person like yourself” and “academic expert” are circled. CEO = Chief Executive Officer; NGO = non-governmental organization.
SOURCE: Copyright 2019. Adapted from 2019 Edelman Trust Barometer. General Population, U.S. Used with permission from Edelman. Presented by Adelaide Feuer, September 16, 2019.
To conclude her presentation, Feuer mentioned an approach to communications planning that begins by clarifying objectives, followed by developing a research-informed messaging strategy and narrative that is distributed and amplified using selected messengers and optimized platforms. Finally, she said, success is measured by quantifying how many people were reached and qualifying who they were, as well as assessing shifts in those people’s attitudes and behaviors.
Kasisomayajula “Vish” Viswanath, Lee Kum Kee Professor of Health Communication in the Department of Social and Behavioral Sciences at the Harvard T.H. Chan School of Public Health and in the McGraw-Patterson Center for Population Sciences at the Dana-Farber Cancer Institute, presented five points related to the twenty-first century’s revolution in information and communications technologies.
First, he began, is the proliferation of platforms and purposeful misinformation. He stated that both exposure to and consumption of information is staggering, adding that they occur alongside what he termed a marketization of misinformation that has resulted from the ability of anybody to produce and share information. Viswanath shared an estimate that more than 2.5 quintillion bytes of data are created each day, a deluge of information that circulates with little gatekeeping (Ahmad, 2018).
The second point he made is that the production of science and health information is not in the realm of scientists alone. A host of actors and stakeholders control the distribution and interpretation of this information, he explained, such as the mass media, the private sector, activist groups, and health systems. Health and science professionals underestimate the private sector’s “oppositional communications,” he suggested, which he said influence perceptions of risk, promote social norms and risk behaviors, and drown out accurate scientific information. He illustrated health communicators’ challenges of competing with these messages by referencing public data on marketing budgets for three prominent brands that sell tobacco products, sugary beverages, and fast food.
Third, Viswanath went on, information does not equal communication. People may have challenges interpreting and acting on information, he said, because they receive apparently contradicting information or false information that they may not recognize as false, and because they have an inaccurate understanding of disease etiology.
Fourth, Viswanath declared that how something is said is as important as what is said. He explained that certain features or formats of messages interact with individual attributes of the audience and influence how they process information. The framing of messages is also critical, he pointed out, because it affects the extent to which the broader context of the message is represented.
Fifth, there are inequalities in communications as there are in health outcomes, Viswanath stated, elaborating that there is a different distribution of communications resources among different social groups. Social determinants such as socioeconomic class, race, ethnicity, and degree of rurality/urbanicity affect access to and use of information. The concept of intersectionality plays out in this realm, he noted, referring to overlapping social categorizations describing an individual or a group, such as being both African American and having a low income, that create interdependent systems of disadvantage. Internet
access is strongly associated with per capita income, he pointed out, but even among those who have access, socioeconomic status influences how health information is processed and used. Such inequalities are neither trivial nor natural, he asserted, suggesting that institutional solutions could help design systems to bridge inequalities.
A panel discussion following Feuer and Viswanath’s presentations opened with remarks from Suzi Gates, communication team lead in the Centers for Disease Control and Prevention (CDC) Division of Nutrition, Physical Activity, and Obesity, and Rebecca Puhl, professor of human development and family sciences at the University of Connecticut and deputy director of the Rudd Center for Food Policy and Obesity.
Gates opened by noting that in community health, communications refers to the strategic use of marketing principles to advance programmatic objectives. These kinds of communications go beyond pamphlets and brochures, she underscored, and can be used as an intervention to affect norms and advance policy, systems, and environmental changes that facilitate healthy behaviors. Gates highlighted three key learnings from her experience working on the VERB social marketing campaign to increase physical activity among children ages 9–13: first, the importance of precisely defining an audience and identifying its values and barriers to performing healthy lifestyles; second, specify objective(s); and third, grow and evolve with the audience as the surrounding social and communications environments shift.
Gates briefly reviewed several examples of strategic communications efforts in communities nationwide to promote healthy living among various population groups, including campaigns to reduce sugary drink consumption and promote physical activity. Gates affirmed that as well-researched, adaptable efforts, these campaigns were instrumental in laying a foundation for obesity-related policy and environmental changes.
Puhl focused her comments on the role of stigma and discrimination in the current obesity communications environment. Negative attitudes toward people who have obesity have been long ingrained in society, she maintained, noting that society’s weight stigma interferes with the ability to effectively communicate about obesity.
Puhl summarized findings from her team’s research on the role of stigma in obesity communications. According to several national experimental studies, Puhl said that when the public is exposed to stigmatizing messages in public health campaigns targeting obesity, the result is less motivation, lower intent, and less self-confidence to change health behaviors. When nonstigmatizing messages are used, she said, in contrast, the result is increased motivation for behavior changes especially when messages focus on specific health behavior changes rather than on weight.
In news media communications, Puhl said that obesity is often described as an issue of personal responsibility to be solved at the individual level. That narrative is overly simplistic, she cautioned, and is as problematic as news stories’ visual depictions of people with obesity. Puhl said that content analyses have found that about two-thirds of the visual images of children and adults with obesity are portrayed in a stigmatizing manner. She elaborated that public attitudes worsen and biases increase in response to such images—even if the narrative’s written content is neutral—but that attitudes improve when nonstigmatizing images are used. Research on obesity communications in social, entertainment, and other forms of media has produced similar findings, Puhl added, and declared that a clear disconnection exists between what scientists and health professionals know about obesity and what society communicates about obesity.
Lastly, Puhl called for improving obesity communications in health care settings. Health care providers receive little training in communicating with patients about weight, she said, and weight stigma can create harmful implications during these conversations. Puhl advocated for language that is sensitive, supportive, and empowering, rather than stigmatizing or shaming. Fundamentally, she said in closing, it is important that communications are respectful and inclusive of people of diverse backgrounds who are affected by obesity.
WORKSHOP OVERVIEW
Following the first session’s overview of communications, Sylvia Rowe, president of SR Strategy, framed the remainder of the workshop. To align communications approaches with goals, she said, it is important to consider the desired outcomes. Rowe informed participants that the rest of the workshop will examine the broader goals and consider the what, why, and who with regard to communications efforts. The workshop planning committee chose to narrow its focus on communications to obesity solutions, Rowe explained, and identified three key audiences for those communications: the broader publics; decision makers such as teachers, parents, community leaders, or health professionals; and policy makers. She outlined that session 2 will address where to start with the three audiences, and sessions 3 and 4 will move into the practical approaches to communicating effectively, including model successes, lessons learned, gaps, and evaluation metrics.
WHAT’S WORKING AND WHAT’S CHALLENGING IN THE OBESITY SOLUTIONS COMMUNICATIONS LANDSCAPE
The workshop’s second session explored the complexities of communicating solutions to obesity and examined data and insights that help illuminate and address those complexities.
Patricia (Patty) Nece, vice chair of the Obesity Action Coalition and chair of its weight bias task force, spoke as an advocate of people living with obesity and provided a perspective on how obesity communications have resonated with her from a patient perspective. Nece shared candidly about her lifelong experience with obesity, describing a “lifetime full of stigma and shame and blame.”
She listed examples of messages that people with obesity encounter as they try to address their weight, such as both dieting and antidieting messages; claims about fast-acting, weight-reduction solutions; and exercise and fitness programs that exaggerate their purported results. Nece called this array of confusing information and marketing materials “the noise” and added that the clear messages pervading the communications landscape convey that people in higher-weight bodies are “less than” in society and are failures for not controlling their weight. She shared both explicit and subtle examples of messages that convey weight bias or focus solely on personal responsibility and fail to acknowledge broader contextual and biological factors that influence weight. She appealed for more realistic messages to come to the forefront, such as addressing underlying physiological and environmental influences on weight, the long-term nature of weight management efforts, and the supporting role that health care providers can play.
Next, Nece reviewed the variety of organizational viewpoints and movements about how to respond to and address obesity. Though this diversity of viewpoints could contribute to “the noise,” she suggested, these entities have common ground as they all urge elimination of the weight bias, stigma, and discrimination that harm people of higher weight. Lastly, Nece emphasized the importance of tailoring weight management interventions to the cultural orientations of participants.
Brian Dunn, chief behavioral officer at Concentric Health Experience, described how behavioral economic concepts were translated into a marketing campaign that counters weight bias as it advertises a branded medication to treat obesity. The campaign’s images and videos depict diverse people with larger bodies as hard-working individuals who are connected to others and are engaged in healthy behaviors as they pursue long-term weight management, aspects that Dunn said were deliberately crafted in an intent to counter fundamental attribution error. He explained that this error occurs when an individual (often automatically) assigns character flaws to a person with obesity, such as assumptions that he or she is weak willed or lazy. Communications that use narrative and implicit messages have been demonstrated to be more powerful in countering attribution error than explicit messages, Dunn explained. When the implicit messages are shown with high frequency in the communications sphere, Dunn said that it creates an availability heuristic, which he described as the ease with which something comes to mind serving as an index of how true it is perceived to be.
Dunn moved on to discuss quantitative linguistics, a strategy that he suggested could be applied to the rich, publicly available data in social media to help solve the problem of nonrepresentative sampling of the U.S. population. Social media data represent inputs from nearly all populations, he indicated, adding a caveat that people more than 65 years of age are underrepresented in his study. He presented preliminary data from a study of digital phenotyping in which massive volumes of social media data language were analyzed to identify people with overweight or obesity who were talking about treatments or were interested in seeking treatment. The discourse in the sample was polarized in sentiment, Dunn pointed out, identifying it as a “stunning” near symmetry of positive and negative discourse, contrary to his hypothesis that negative sentiment would be associated with stronger, more frequent cycles of treatment seeking. He also shared data indicating the sample’s overwhelming and consistent negative sentiment regarding one’s own physical and emotional states. He said people are suffering tremendously—even more so compared to samples of people with mood disorders—urging compassionate treatment.
Christopher Gallagher, president and founder of Potomac Currents, LLC, discussed communicating with decision maker and policy maker audiences. Much progress has occurred over the past decade, he observed, with regard to helping federal and state policy makers understand that obesity is a complex, chronic disease warranting patients’ access to evidence-based treatment avenues across the care continuum. Yet, this progress has been theoretical in some ways, he suggested, describing that policy statements from organized medicine and state government associations support access to and coverage of a spectrum of obesity treatment modalities, but health plans often deny coverage for obesity treatment based on false assumptions about the condition (i.e., that it is a lifestyle condition and treatment is elective or cosmetic in nature). Still, examples of tangible progress exist, Gallagher acknowledged, highlighting changes in coverage policies that break down barriers to treatments such as bariatric surgery, Food and Drug Administration–approved obesity drugs, and obesity screening and intensive behavioral therapy. Gallagher added, the U.S. Pharmacopeia also finalized a new independent drug classification system, that now includes a category for anti-obesity agents that he said is expected to preclude public and private health plans from excluding coverage.
Gallagher shifted to discuss how these examples of progress were accomplished. He stated his belief that the key to advocacy is a willingness to take the first step to open a dialogue with a person and work to foster a relationship. He described
additional integral steps, including building a strong base, growing membership numbers, and training advocates to effectively lobby for the changes they want to see. Building and joining broad coalitions demonstrates that many voices are calling for change, he added, referencing the example of the Obesity Care Advocacy Network, a coalition that unites and coordinates stakeholders in the health care community to elevate obesity treatment needs on the national agenda. Gallagher noted in closing that it would be helpful to have a champion for obesity, someone with a personal connection to the condition who can stand up for obesity issues and broaden their national visibility.
Brian Southwell, senior director of the Science in the Public Sphere program in the Center for Communication Science at RTI International and adjunct professor and Duke-RTI scholar at Duke University, opened by emphasizing a reason to find hope in the state of obesity communications: the opportunity to meet people where they are and engage with them as they pursue health and connectedness to others. Turning to discuss challenges and opportunities in communicating about obesity, Southwell explained that audiences are not a blank slate; they have had a lifetime of socialization during which they developed mental models of how health processes work, and they were exposed to various information environments that shaped their thinking about obesity-related issues. In that context, Southwell described how popular understanding reflects many inputs, including mass media coverage, social network diffusion, the iterative nature of science, and human memory constraints and information-processing tendencies.
Best practices suggest that presenting accurate information is not enough, Southwell said, and appealed for more attention to the dimensions of salience and trust. Obesity issues are not on most people’s daily radar, Southwell maintained, and though public attention may spike briefly in response to widely reported news on the topic, he suggested that a steady drumbeat would help keep obesity more salient and improve public understanding. He also indicated that earning people’s trust in the source of information is crucial to achieving their adherence to and engagement with the information.
Shifting to the plethora of inaccurate information in the communications landscape, Southwell proposed that humans misunderstand their own vulnerabilities to misinformation. Failure to fulfill innate desires for either social connection or hope for the future affords opportunities for science communications challenges, he suggested. Continuing, he said that people’s sharing of misinformation may be driven less by their assessment of its truth and more by a bias to accept information at face value (at least initially) as well as the need to connect with others and seek information that is perceived to offer hope of improving one’s life.
Given these insights about the problem of misinformation, Southwell proposed three steps:
- Consider the interaction of human psychology, new norms, governance, and various systems;
- Monitor and seek to understand, rather than prejuding, the public information environments that contribute to collective public understanding on an issue; and
- Build and maintain trust between science institutions and citizens by acknowledging shared interests in promoting the public’s health and well-being.
LESSONS FROM THE FIELD: POTENTIAL FOCUS AREAS FOR OBESITY SOLUTIONS COMMUNICATIONS
The workshop’s third session presented four perspectives on best practices for developing effective strategies and messages for communicating obesity solutions to key audiences.
Gary Foster, chief scientific officer at WW International, Inc., focused on treatment messaging for people who are engaged in a weight-loss program. He began with an overview of cultural trends in the public’s goals and approaches to weight loss, beginning with the “thinner is better” outlook—even if the consequence was unhealthy calorie deprivation—that characterized the landscape 15-plus years ago. In 2015, Foster continued, WW found that people had shifted to a broader, more holistic approach that included more emphasis on physical activity and on a focused and positive mindset, and an emerging consideration of food quality. People were less weight focused than they were previously, he recalled, and had more realistic expectations for an achievable healthy weight. Since then, Foster said that approaches have broadened even more to include the pursuit of more energy, increased confidence, and a connection to an individual’s values such as role modeling or improved well-being.
Even the most efficacious weight-loss treatments will not be effective, Foster asserted, if they do not meet people where they are. People want to lose weight, he clarified, but they also want to achieve wellness in physical, mental, and social senses. To achieve those goals, he continued, they want credible science and common sense that translate to practical guidance for applying realistic, sustainable habits to their lifestyles. He added that seeking strategies that fit one’s lifestyle is part of the cultural trend of personalization.
Foster described WW’s programmatic approach as one that translates science into behaviors and habits that result in improved health and well-being (i.e., meeting consumer goals and values). He urged language that uses warm, encouraging
tones instead of judgmental and academic tones, and provided specific examples of verbiage that the brand carefully avoids, along with preferred alternatives. For example, terms such as weight (or wellness) journey or way of living are favored over those that imply temporary, short-term solutions such as (diet) plan. WW also avoids moral language, such as the terms cheat, excuse-proof, or good/bad, which he said contribute to stereotypes.
Foster ended by urging the identification and use of techniques to enhance self-compassion and body positivity as a bridge to an improved weight or wellness journey, noting that self-criticism derails this journey. He referenced WW’s popular hashtag “#NSV” (non-scale victories) as an example of celebrating nonweight outcomes related to improvements in body image, self-worth, and small steps toward success. He proposed that these important outcomes will also help drive weight-loss success and improve health and comorbidity.
Luis Garcia, president and lead strategist of the culture-inspired marketing firm MarketVision, shared lessons from the VERB youth media campaign’s efforts to reach Hispanic audiences. Understanding a group’s culture helps communicators appreciate how values and beliefs influence that group’s behaviors, he began, and emphasized a shift from pushing messages into the market to engaging people in a collective experience that they help design. Garcia said that this process involves a focused definition of the target audience and the desired behavior along with the constant iteration of messaging, testing, and refining.
To achieve VERB’s goal of increasing physical activity among tweens (ages 9–13 years), Garcia said that CDC enlisted various specialists to develop strategic communications for different segments of the target audience. His team at MarketVision discovered that Hispanic audiences valued providing a good future for the next generation, so the team developed parent-directed messages that connected physical activity as an indicator of health and thus a means of providing for one’s children.
The campaign’s VERB brand was developed to encourage kids to choose an activity and play for an hour each day, Garcia explained, and was about fun and belonging to a movement. Messages were delivered in media, schools, and communities where local programs could promote their activity offerings. A parallel campaign existed for parents, focused on moms, Garcia continued, to educate them about active kids and encourage support of their children’s physical activity. Parents gravitated toward signing a national pledge of support to keep their kids active, he noted, which reinforced the idea of joining a movement. Partnerships and media integration were cultivated to help sustain the messages after the campaign’s funding was exhausted, which Garcia said created ripple effects.
Garcia reported that the campaign generated an impressive 74 percent brand awareness in its first year and demonstrated increases in physical activity among target audiences. His lessons learned include the importance of focusing on a specific goal for a specific audience, incorporating culture-inspired stories, employing an iterative strategic marketing approach, and sustaining impact through partnerships. Today’s world is very different than it was when VERB was implemented, Garcia said, pointing out greater health consciousness and advances in digital technologies that have enabled the delivery of immediate, personalized results.
Moving forward, Garcia suggested that framing physical activity as a gain can help Hispanics overcome barriers that hinder their motivation to be active. Spending time with family is an important cultural value, he said, and suggested promoting physical activity as an opportunity to connect with family, such as while taking a walk. He also mentioned that using technology to nudge and gamify desired behaviors can help break long-term goals into small steps. Lastly, he noted that technology’s exponential growth has led to a largely decentralized world, creating an unprecedented opportunity for engaging new collaborators to be part of “swarm intelligence,” that is, cross-functional collaboration that uses design thinking to create and iterate solutions across a connected but decentralized system.
Marla Hollander, national partnerships manager for Voices for Healthy Kids, a joint initiative of the Robert Wood Johnson Foundation and the American Heart Association, discussed messaging to national, state, and local policy makers as it relates to the initiative’s efforts to advance public policy changes that create healthier communities. She focused on campaign research and development, the area of the initiative’s work that builds tools and resources to help advocates deliver messages.
Hollander explained that when communicating with political decision makers (and the people who influence them) about public policy change, effective messages start with values and use the right words. The initiative’s message research found that a values-based perspective that resonates with people across political and geographical lines is that every child deserves the right to be healthy. Hollander next shared a chart of language to emphasize and corresponding language to avoid. For example, describing the environment that makes it challenging to eat healthy and be active is favored over describing personal behavior, and invoking a sense of cooperation and partnership to address obesity are preferred over language that describes the problem as a “war” and uses words like “bombard” that trigger trauma. Describing the goal of helping children grow up at a healthy weight and in healthy communities is more effective than talking about preventing childhood obesity, she continued, as is using a gain-based frame.
When it comes to advocates delivering messages to policy makers, Hollander said that a good technique is to identify issues and solutions together as a community, then customize the messages. She emphasized that the messengers matter, particularly in local policy because issues tend to be more personal and people tend to trust local lawmakers more than those at the state or federal level. Show how everyone in the community can benefit from the proposed solution, she suggested, using
stories to illustrate the gaps in the community. Rather than saying “The problem is…,” Hollander said to lead with the solution and the benefits it is expected to confer, emphasizing effectiveness (keeping the focus on the intended effect) instead of cost-efficiency (which can lead to short-term or scarcity thinking). More information on this topic is found in the initiative’s health equity messaging guide for policy advocates, Hollander said in closing.
Paula Clayton, public health consultant to the National Association of Chronic Disease Directors, described an assessment of state-level decision maker support for evidence-based approaches to chronic disease prevention. She explained the goal was to understand state decision makers’ views related policy approaches for healthy eating and active living that resonate with them in their current environments to better understand the forces at play when communicating with these decision makers. The assessment was multipronged and qualitative, Clayton said, and included a literature review of how evidence is used by policy makers and what messages and values have been employed; interviews with key informants such as state health department leaders, public health advocates, and legislators; and focus groups of local leaders in public health, political administration, and business.
Clayton elaborated on the assessment’s findings, starting with the literature review. Its main points were to use targeted, tailored messages presented in a concise and engaging manner; incorporating data (including cost data) and stories; and providing well-cited, unbiased information that is relevant to constituents. She went on to share learnings from the broader assessment, beginning with the context that legislators have a lot of issues to understand and want information at the time decisions are being made. They are concerned about a proposed policy’s (economic) impact to business and agriculture, she reported, and recognize that issues of local control (i.e., planning, land use, transportation, recreation, infrastructure, and zoning) may limit statewide implementation of policies. State leaders look to success at the local level when deciding whether to support a policy at the state level, Clayton explained, adding that state, regional, and local data are more valuable than national data. She also acknowledged that obesity prevention is a lower priority than other pressing legislative issues, and that declining state revenues also threaten funding.
Finally, Clayton highlighted the assessment’s findings related to the critical role of the state health department, which she reported was seen as a convener and collaborative partner, an expert resource for implementing healthy eating and active living strategies, and a bridge to other state agencies that can help support these policies. She referenced topic-specific guides for healthy eating, active living, and early care and education that summarize the assessment’s complete findings and practice applications (National Association of Chronic Disease Directors, 2019).
REFLECTIONS ON ADVANCING EFFECTIVE COMMUNICATIONS OF OBESITY SOLUTIONS
The workshop’s final session included opening remarks and a panel discussion that reflected on the workshop’s prior three sessions to discuss themes and future directions. April Oh, program director in the Health Communication and Informatics Research Branch at the National Cancer Institute, began the session with a brief presentation of her reflections. She offered four key points that relate to bridging from problem to solution.
Oh’s first point was to challenge traditional assumptions about health and obesity-related behavior research. She listed six assumptions that she said are barriers to successful implementation and potential impact of messages. The first is that communications and messages are static, but Oh pointed out that the current communications environment operates on a 24-hour news cycle and the relevance of a given topic and public’s attention can be ephemeral. A second assumption is that obesity is often described as a choice, Oh observed, instead of a chronic disease that is stimulated by obesogenic environments. Third, stakeholders may think that obesity-related messages are the best or the only messages, she continued, but this is not true because health is not a priority or value shared by all. Fourth, the assumption that people will trust evidence-based messages runs counter to the phenomenon of diminishing trust in government and institutions, Oh said, and reiterated that people already know what they should be doing. Therefore, the assumption that knowledge is enough to change behavior is false, she added as number five. The sixth assumption was that consumers, patients, and communities are homogeneous, but Oh countered that they are all different.
Oh’s second point was the importance of addressing communications inequalities. She referenced disparities in the prevalence of obesity and its risk factors across the United States, listing several social determinants of health that drive the disparities. These determinants contribute to inequitable distribution of information, she maintained, in the forms of inequitable access, inequitable distribution of information channels, and inequitable capacity and resources to act on information that is received. Oh called for addressing these inequalities by embedding cross-sector partnerships within messaging efforts. Obesity solutions messages interact across socioecological levels and systems, she noted, and are more effective if adapted for different audiences and channels. She urged consideration of the “stickiness” of messages across levels through effective engagement and of identifying trusted influencers within levels.
Oh’s third point was to shape the narrative using a community-driven codesigning process, which she said engages and empowers all stakeholders in communities to develop messages that reflect their goals and values. Codesigning also allows for the iteration of messages, she noted, which is well suited for the 24-hour news cycle and its continuous introduction of new
messages.
Lastly, Oh described differences among diffusion, dissemination, and implementation of information. Diffusion is “letting it happen”—the passive, untargeted spread of information; dissemination is “helping it happen”—the targeted distribution of information and intervention materials to a specific audience; and implementation is “making it happen”—applying strategies to change policy and practice in specific settings. Oh urged a focus on implementation of obesity solutions communications, referencing the RE-AIM model to highlight five dimensions of evaluation of implementation: reach, effectiveness, adoption, implementation, and maintenance.
Following Oh’s remarks, four panelists shared brief reflections on their lessons and thoughts for future directions: Viswanath; Nece; Dietram Scheufele, Taylor-Bascom Chair in Science Communication and Vilas Distinguished Achievement Professor at the University of Wisconsin–Madison and the Morgridge Institute for Research; and Kevin Ronneberg, vice president and associate medical director at HealthPartners.
Ronneberg highlighted the dilemma of normalizing versus not normalizing healthy weight and suggested that the field dedicate time to determine where it wants to position itself in order to avoid unintended consequences. Given the emotion around the topic of obesity and the balance between individual responsibility and social determinants or social drivers, he elaborated, the right positioning is critical to establishing solutions that will resonate and be acted upon by stakeholders. He noted that several participants had shared a practice of avoiding using the words obesity or overweight, and cautioned to not allow this practice to result in creating solutions that focus on interim outcomes, such as nutrition or physical activity, that do not affect weight. Lastly, he encouraged the identification of process measures and indicators to clarify the achievement of success in communicating about overweight and obesity.
Viswanath underscored that communications cannot solve all obesity problems, but that it is worth broadening the boundary to consider communications’ contribution. Issues of equity are central to anything communications can do, he asserted, pointing out that though efforts to highlight attention to the issue of obesity over the past two to three decades have been successful, disparities in the prevalence of obesity are still pervasive. Next, he urged the clarification of goals, such as changes at the individual, policy, or cultural level, because different communications strategies align to different goals. He added that continuous evaluation fosters the agility to make mid-course corrections. Finally, he called for a social mobilization strategy to demand public support for obesity solutions, lest other social problems and issues continue to be more salient.
Scheufele appealed for abandoning the knowledge deficit model of thinking, which he described as the idea that if people only knew the science, their behaviors would be more aligned with expert recommendations. Information-centered communications campaigns that are based on this model have null results at best, he pointed out, and polarizing effects at worst. Second, Scheufele observed that the concept of framing recurred throughout the workshop; he warned against speculation about framing effects, emphasizing that the most successful campaigns were extremely well researched and tested. He called framing “a researchable problem” that warrants due attention to determine how to target different audiences with obesity solutions messages. Third, Scheufele said that message discipline is crucial in a competitive message environment, particularly where other communicators have more money than obesity communicators. Well-organized campaigns have a clear message that is regularly amplified by partners, he explained, noting that this helps consumers sort through and extract messages to consistently take away. Scheufele’s final point was that storytelling and narrative, which he said have been put forward as a solution to many issues, may be risky because they are agnostic to truth. Unless an obesity narrative is a vehicle for conveying the evidence base supporting a solution, he warned that competition for the best story may find obesity solutions narratives at the losing end.
Nece proposed focusing on an initial audience for obesity solutions communications, noting insufficient resources to target all audiences at once. Then, identify that audience’s values and a frame that will resonate with them, and set goals. She endorsed other participants’ suggestions that stigma and bias are a cross-cutting, soft target, and highlighted the promise of using implicit messages to provide a counternarrative. She applauded a number of other strategies shared throughout the day: giving hope, highlighting a solution’s benefits to all, meeting people where they are, providing common-sense messages, and helping people with obesity cultivate self-compassion. Nece said that her personal experience corroborates the concept that self-acceptance at the outset of a weight-loss journey leads to better outcomes.
Following the panel discussion, Rowe returned to deliver closing remarks. She emphasized the importance of proactively and strategically aligning communications with the goals for obesity solutions. Rowe acknowledged that many questions and challenges persist, but she took an optimistic view that the field has “an enormous amount of opportunity in this area.”♦♦♦
REFERENCES
Ahmad, I. 2018. How much data is generated every minute? Infographic. https://www.socialmediatoday.com/news/how-muchdata-is-generated-every-minute-infographic-1/525692 (accessed November 18, 2019).
National Association of Chronic Disease Directors. 2019. Assessing decision-maker support for chronic disease prevention: Effective messages for decision-makers related to healthy eating and active living. https://www.chronicdisease.org/page/HEAL-policy-guides (accessed November 18, 2019).
Story, L. 2007. Anywhere the eye can see, it’s likely to see an ad. https://www.nytimes.com/2007/01/15/business/media/15everywhere.html?pagewanted=all&_r=1&mtrref=undefined&gwh=4D7D7E634A81137B42BB5D792DC423D8&gwt=pay&assetType=PAYWALL (accessed November 18, 2019).
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Emily A. Callahan as a factual summary of what occurred at the workshop. The statements made are those of the rapporteur or individual meeting participants and do not necessarily represent the views of all workshop participants, the planning committee, or the National Academies of Sciences, Engineering, and Medicine.
**The National Academies of Sciences, Engineering, and Medicine’s planning committees are solely responsible for organizing the workshop, identifying topics, and choosing speakers. The responsibility for this published Proceedings of a Workshop—in Brief rests with the rapporteur and the institution.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Carol Byrd-Bredbenner, Rutgers University, Dietram Scheufele, University of Wisconsin–Madison, and Lauren Shern, National Academies of Sciences, Engineering, and Medicine, served as the review coordinator.
SPONSORS: This workshop was partially supported by the Academy of Nutrition and Dietetics; Alliance for a Healthier Generation; American Academy of Pediatrics; American College of Sports Medicine; American Council on Exercise; American Society for Nutrition; Banner Health; Bipartisan Policy Center; Blue Cross Blue Shield of North Carolina Foundation; The California Endowment; ChildObesity180/Tufts University; Edelman; General Mills, Inc.; Greater Rochester Health Foundation; Health Partners, Inc.; The JPB Foundation; The Kresge Foundation; Mars, Inc.; National Recreation and Park Association; Nemours; Nestlé Nutrition; Novo Nordisk; Obesity Action Coalition; The Obesity Society; Partnership for a Healthier America; Reebok, International; Reinvestment Fund; Robert Wood Johnson Foundation; SHAPE America; Society of Behavioral Medicine; Wake Forest Medical Center; WW International, Inc.; and YMCA of the USA.
For additional information regarding the workshop, visit nationalacademies.org/obesitysolutions.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2019. Advancing effective obesity communications: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/25649.
Health and Medicine Division

Copyright 2019 by the National Academy of Sciences. All rights reserved.









