7
Improving Patient, Family, and Public Education and Awareness About TMDs
The lack of credible information relayed to the public and professionals about the reality of the impact that TMD can have on one’s overall health and life results in patients continuing to suffer in silence and isolation because nobody—including family, friends, employers, etc.—can comprehend how multiple therapies, including years of treatments at exorbitant costs, cannot fix or alleviate the problem but seem to worsen it. It is always the fault of the patient when things don’t work out like they were told it would. Leaving the patient to question what they did wrong.
—The TMJ Association
It was difficult to get people to come and give recognition to this disorder. They don’t understand the seriousness.
—Beth B.
Patients, their families, the general public, and health care professionals need evidence-based information about temporomandibular disorders (TMDs). As detailed in the prior chapters, patients and their families face challenges in accessing appropriate diagnoses and care. Additionally, because orofacial pain and the symptoms potentially related to TMDs are experienced by a large number of individuals in the United States and globally, there is a need for raising awareness in the general public about these disorders and for providing accurate information and resources to help individuals cope with these conditions. As discussed in Chapter 6,
increased efforts are also needed to improve education and training on TMDs for a range of health care professionals.
The reasons identified by the committee for focusing efforts on patient and public education on TMDs include:
- The frequency and complexity of the symptoms of temporomandibular disorders: As discussed in Chapter 3, TMDs are common, not rare, and the public needs to know how to access the right treatment at the right time.
- Empowering the patient: Patients need to have a strong and knowledgeable voice in their care and need to be informed about the day-to-day efforts they can make to try to live their best possible lives with a TMD.
- Support from family and friends: Similarly, family members and friends who are well informed about TMDs can provide support.
- The range of TMDs and varying treatment approaches: As discussed in Chapter 2, TMDs are heterogeneous conditions that range from simple to complex. People who have pain or mechanical problems affecting the masticatory system need resources to allow them to determine if and when to seek a professional opinion, what type of health care professional to consult, and how to evaluate treatment options. Patients will need to navigate both dental and medical care systems to find the best care until these systems are coordinated in TMD assessment and management.
- Reducing stigma and misconceptions: TMDs, chronic pain, and chronic illnesses are often associated with misperceptions and misunderstandings. Because the condition can often not be seen, patients may be viewed by family, friends, and even health professionals as malingerers or not having a “real” condition.
- Raising awareness of the public and health care professionals: A public education campaign can educate the public and health care professionals about this complex condition. In addition, it can help mitigate the stigma discussed above.
The role of patients has taken on new dimensions in recent years as patient education has expanded into patient engagement and activation across the spectrum of involvement in research, prevention, and treatment opportunities (IOM, 2011a, 2014). As discussed in Chapters 5 and 6, patient-centered care is the focus of efforts in health care, including dental care, to involve patients in decisions on their treatment goals and options. In addition, patients must take an active part in day-to-day TMD management. Patients and stakeholders in the public are increasingly being valued in all facets of research and in policy development. These individuals are
valued for the insights they provide (including understanding the realities of living with disease, focusing on culturally relevant and patient-relevant questions, and incorporating outcome measures that assess differences that really matter). Patients and stakeholders also are involved in actions that can foster the implementation of efforts to improve health in communities (Woolf et al., 2016; Forsythe et al., 2019). Using tools to assess patient activation, researchers have found that patients who are more engaged in their care are more likely to have healthier outcomes in terms of general indicators of health, are more likely to engage in higher levels of healthy behaviors, and are less likely to have a hospitalization or emergency department visit; the combined effects result in cost savings (Greene et al., 2015; Okunrintemi et al., 2017).
The committee greatly benefited from the public testimony of a number of individuals with a TMD who described their experiences and lessons learned while speaking at the committee meetings or by providing written comments to the committee (see Chapter 1 and Appendix A).
This chapter identifies goals and priorities for providing evidence-based information on TMDs to patients, their families, health care professionals, and the general public and for engaging patients and other stakeholders in being a part of prevention, treatment, research, and communication efforts.
OVERCOMING STIGMA
There is a limited amount of research on stigma that is specific to TMDs. However, research on the impact of stigma from chronic pain, together with patient testimony provided to the committee, eloquently document the stigma suffered by individuals with a TMD and its consequences for patients. This chapter begins with a discussion of stigma, then turns to a discussion of actions that can be taken to help individuals, family members, and others become more knowledgeable about TMDs and proactive about self-care.
Stigma refers to attitudes and beliefs that lead people to reject, avoid, or fear those they perceive as being different. As outlined by Pescosolido and Martin (2015, p. 6), stigma involves “(a) distinguishing and labeling differences, (b) associating human differences with negative attributions or stereotypes, (c) separating ‘us’ from ‘them,’ and (d) experiencing status loss and discrimination.”
Stigmatizing attitudes and beliefs about TMDs can originate both internally—from the beliefs and attitudes of the individual experiencing a TMD—and externally—from the beliefs and opinions held by others, including family members, friends, health care professionals, employers and coworkers, the general public, and the media (see Figure 7-1). Chronic and complex TMDs represent a form of chronic pain that can profoundly
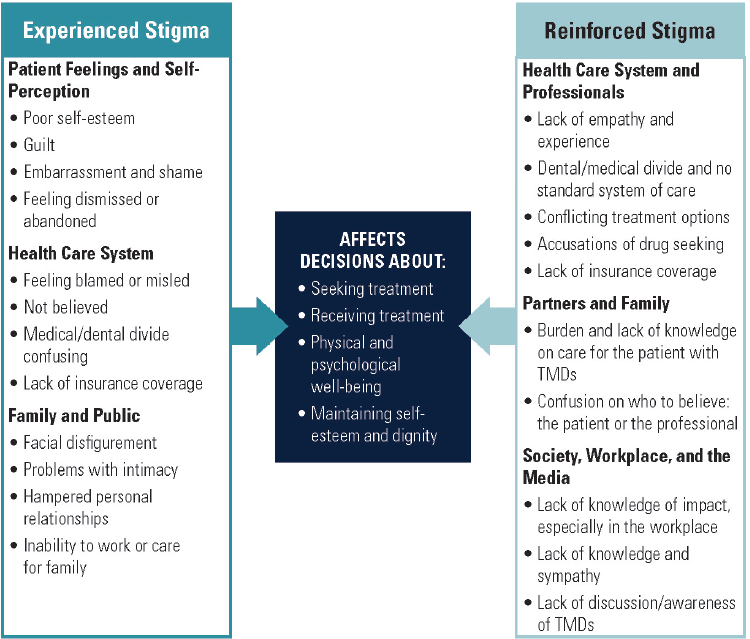
SOURCE: Adapted from NASEM, 2016.
affect interactions as fundamental to human existence as smiling, laughing, speaking, eating, and intimacy. Patients with TMDs reported that they often do not feel believed by romantic partners, relatives, and friends. Practitioners may think that the chronic pain is imagined or exaggerated, leading patients to feel blamed, misled, or abandoned (De Ruddere and Craig, 2016). Employers, family members, and friends may dismiss pain as psychological. In testimony to the committee, some TMD patients reported that they experienced hostility from their work colleagues and a lack of understanding of the severity of their pain. Additionally, when seeking care, patients reported that they were often sent from dentists to physicians and back again or reported being dismissed without care and with little information on suggested next steps. Patients expressed their frustration at not knowing where to turn for quality care and noted that their primary care physicians and general dentists often did not know how to help them locate
qualified specialists. The opportunity for adequate treatment and follow-up of TMD care may be thwarted by the combination of uncertain diagnosis and the stigma perceived by the patient, family member, or public. Individuals with a TMD may hold back on sharing their symptoms, thoughts, or feelings with others because of concerns about stigmatization. Stigma can lead to poorer physical and psychological well-being, diminished self-esteem, and a loss of dignity. Thus, stigma adds to the burden of the condition and significantly affects health and quality of life.
Patients with other forms of chronic pain also report suffering from the stigmatization of their condition. As discussed further below, pain is invisible and, as such, is hard for family members, work supervisors, and others to quantify and understand. De Ruddere and Craig (2016, p. 1607) write,
In the context of chronic nonmalignant pain, an absence of clear tissue damage deviates from the widely held biomedical model, which presumes that clear physiological pathology underlies the pain experience. As well, most people understand pain through acute pain experience, which resolves relatively rapidly over time.
A survey of adults with chronic pain found that more than one-third experienced a sense of stigma in which they felt alienated, became socially withdrawn, or saw the legitimacy of their condition as being questioned (Waugh et al., 2014). A study by Marbach and colleagues (1990) explored the sources of stigma perceived by patients with TMD. The researchers found that often, TMD stigma was experienced by patients because of the lack of a known etiology for their condition and that, moreover, when the TMD was attributed to psychological causes, the patient experienced stigma.
As discussed in Chapter 3, sex differences have been reported in the prevalence of TMDs, with higher numbers of women reporting these disorders. Some patients who provided testimony to the committee noted that they experienced stigma associated with being a female with a TMD, which was manifest by the dismissiveness they experienced from some health care professionals or by being told that their disorder was largely a mental health concern. The stigma associated with chronic pain conditions has been well documented (Wakefield et al., 2018; Scott et al., 2019), and some evidence suggests that women may experience greater pain-related stigma than their male counterparts (Hoffmann and Tarzian, 2001; Driscoll et al., 2018). A study of 151 female patients with chronic facial pain found that the stigma they experienced largely resulted from pejorative labeling by clinicians (Marbach et al., 1990). Diagnostic and treatment decisions for chronic pain are also influenced by the gender and related stereotypes that may be held by some health care professionals (LeResche, 2011).
Stigma is also suffered by many individuals with other health conditions including epilepsy, hearing loss, mental illnesses, fibromyalgia, and HIV/AIDS (IOM, 2012; Corrigan, 2014; NASEM, 2016; Armentor, 2017; Ring and Lawn, 2019). Various types of approaches have been implemented to overcome the stigma attached to these conditions, including patient education efforts, public awareness campaigns, professional education and training, involving celebrities and media champions, and policy change advocacy. The results of anti-stigma interventions are difficult to measure and evaluate, and varying degrees of success have been seen in overcoming health-related stigmas to date (Cook et al., 2014; Corrigan, 2014). New avenues for research on understanding and overcoming stigma have been proposed, as has a public health framework for intervention strategies to reduce stigma using a multilevel approach focused on intrapersonal efforts (patient education and self-management, patient empowerment), interpersonal actions (support groups, broader education including professional and public education and awareness), and structural interventions (e.g., advocacy, changes in policies, leadership) (Slade et al., 2009; Cook et al., 2014; Pescosolido and Martin, 2015; De Ruddere and Craig, 2016; Dubin, 2017; Scott et al., 2019).
The committee believes that efforts to increase professional education and awareness about TMDs across the health care professions, including dentistry (see Chapter 6), as well as actions to improve the education of patients, families, and the general public (see next section) are part of the efforts needed to help reduce the stigma of TMDs and improve patient health and well-being.
INCREASING PATIENT AND FAMILY EDUCATION AND IMPROVING COMMUNICATION WITH HEALTH CARE PROFESSIONALS
Patients with a TMD and their families need to be able to make informed decisions when it comes to treatment and care. Education is key to this process.
For people living with chronic pain, patient education resources have been found to help in identifying ways to control and cope with pain, in connecting with psychosocial supports, and in encouraging the use of self-management strategies for the patient to take an active role in the recovery process (IOM, 2011b; see Chapter 5). People with TMD symptoms need resources that help them explore all of the options for treatment or non-treatment and that empower them not only to ask the questions that can determine the most effective course of action for them, but also to develop and sustain effective coping strategies.
In addition to the critical need for high-quality patient education resources and opportunities, it is also important to have evidence-based
resources for family members and caregivers, who can play an important role in supporting the person with pain. A 1997 American Chronic Pain Association (ACPA) survey of family members living with a person with pain found that family members often experience emotions and fears that are similar to those felt by the person with pain, even though they themselves do not feel the physical pain (Cowan et al., 1998). In response to this important information, the association developed a Family Matters video series that explored the challenges that families deal with regarding a family member in pain and efforts to improve the quality of family life (ACPA, 2019e). In discussing the costs of pain, especially chronic pain, the Institute of Medicine (IOM) report on pain stated,
Family members find that their relationship with their loved one changes, and to the extent that they must take on new roles (as caregiver and morale booster) and greater responsibilities in the family (e.g., grocery shopping, chores, errands), the burden on them increases. (IOM, 2011b, p. 94)
Where do most people get their information about TMDs? The literature review by the committee did not identify any published studies specific to information-seeking behaviors for people with a TMD. Overall, the public finds health information through an array of sources, including the Internet and health care professionals, with a resulting potential for inequities and disparities in information access for disadvantaged consumer groups (Ramsey et al., 2017). In a study examining the information-seeking experiences of 190 people with fibromyalgia, the source that participants turned to most frequently was the Internet, but participants also sought out information from health care professionals, family members, and friends (Chen, 2012). Similar information avenues are also likely sought by individuals with a TMD and their families.
With a wide variety of available health-related websites, the accuracy of the health information available on the Internet is quite varied and has been a source of ongoing concern for patients and clinicians (Gottlieb, 2000; Storino et al., 2016). Thus, having credible evidence-based websites on TMDs is critical for accurate patient- and family-based education. A study examining the websites of 255 dental professionals found that a large percentage had misinformation on the diagnosis and management of TMDs (Desai et al., 2016). The researchers noted inaccuracies in attributing TMDs solely to occlusal problems or malocclusion and in labeling TMDs as a singular disorder.
Identifying the key components contributing to the quality of patient communications continues to be an area of extensive activity and research. Given the complexity of the health care field and the ever evolving knowledge base, it is critical that patient resources be understandable, culturally
sensitive, and available in multiple languages and formats and that they recognize that audiences may vary in educational level, age, location, and access to technology (CDC, 2019b). A 2019 National Academies workshop focused on strategies for improving the public’s health by increasing awareness (via resources that adhere to health literacy guidelines) about the impacts that oral health has on overall health and well-being and also on how overall health affects oral health (NASEM, 2019).
The committee heard a number of patients report that they and their families found it quite challenging to navigate through the array of information about TMDs and to identify what information was valid and evidence based. The ideas presented below are meant as a starting point for discussion and actions on improving patient and family information resources.
Communication Resources and Tools
One problem that many patients encounter is describing their pain and its impact on their lives. Pain is invisible and cannot be validated other than to believe the report of pain by the patient. Continuing to improve resources to help patients describe their pain and the symptoms (including TMD- and comorbidity-related symptoms) being experienced is important in moving this field forward. Several brief assessment tools are used in clinical settings that ask patients to convey the intensity of the pain being experienced through visual or numeric measures and have been found to be fairly reliable, including the Brief Pain Inventory and the Visual Analogue Scale (Bijur et al., 2001; Keller et al., 2004). Other pain assessment measures are developed to focus specifically on the pain experienced due to a given health condition (Hawker et al., 2011). Face depiction scales (e.g., the Wong-Baker faces pain-rating scale) have also been used in health care, most often with children (Khatri and Kalra, 2012; Afsal et al., 2019).
Improved resources and tools are needed for use by patients with TMD symptoms. Examples of resources that could be used, adapted, and evaluated for use by patients with a TMD in tracking their pain and in talking with their health care professional include a set of pain management and communication tools developed by the ACPA (2019d). The ACPA interactive web-based Head Pain Map allows the person with pain to identify on the diagram of the head the specific places on the face where pain is felt, the intensity of that pain, the nature of the pain (e.g., steady, throbbing, burning), and associated symptoms (ACPA, 2019a). The map and information can be printed out to discuss with the patient’s health care providers. The Diagnostic Criteria for Temporomandibular Disorders includes a pain map for paper administration, with separate sections for the oral cavity, face, and body (due to the associated required level of detail for each region); it
has been translated into 15 languages (INfORM, 2013). Pain logs are also useful and are available as interactive tools for patients to record and keep track of the nature, intensity, and functional impacts of their pain (ACPA, 2019b; see examples in Figures 7-2 and 7-3).
The development and evaluation of TMD-related educational resources should focus on the full range of information sought by patients and their families, from the initial exploration of symptoms to valid diagnostic and treatment approaches, to sources of peer support and consumer roadmaps for the types of health care professionals to consult with and seek for treatment. Ideally these roadmaps would be adapted from the multistakeholderdeveloped, comprehensive care guidelines that are a recommendation of this report (see Chapter 5). The demographics of patients with TMDs (see Chapter 3) make this an especially relevant area of information seeking and gathering for teens and young adults. Strategies and campaigns focused on disseminating evidence-based data and resources via social media will be important. Ensuring that resources and communication tools are designed with these target audiences in mind, in addition to broader age groups, is critical, as are communications about what is known regarding the transitions to early and later adulthood with a TMD.
Peer Support
As described by patients with a TMD who provided testimony to the committee, a serious consequence of living with chronic TMD pain is that it can be isolating. Because of the invisibility of pain, its impact on daily life, and the challenges in communicating about pain severity, patients can feel cut off from family, friends, and activities. Peer support has been shown to be an effective means of establishing connections with other people who are also experiencing pain or other health problems, and the sharing of experiences can bring important quality-of-life benefits (Heisler, 2010; Fisher et al., 2015). Peer groups can also provide opportunities for teaching the self-management skills needed to cope with the many issues of living with pain. For example, in a study of veterans living with chronic pain, the benefits of participating in peer support groups were identified as making interpersonal connections, providing and receiving encouragement and support, and facilitating the use of pain self-management strategies (Matthias et al., 2016; see also the self-management section in Chapter 5).
Peer support groups, both online and in person, are vital to the work and outreach of many patient advocacy organizations. The TMJ Association has been active in this area and hosts on their website several ways to connect with others experiencing TMDs. The TMJ Association’s online TMJ Café is a discussion community where users can ask questions, discuss concerns and share experiences, and find out about social media peer
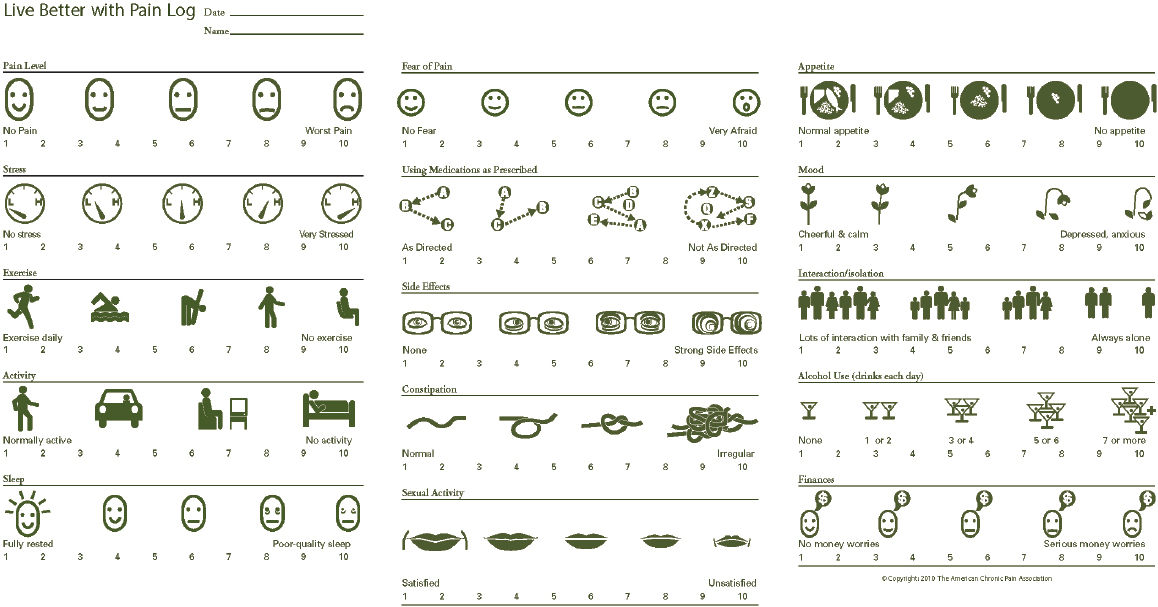
SOURCE: ACPA, 2019b.
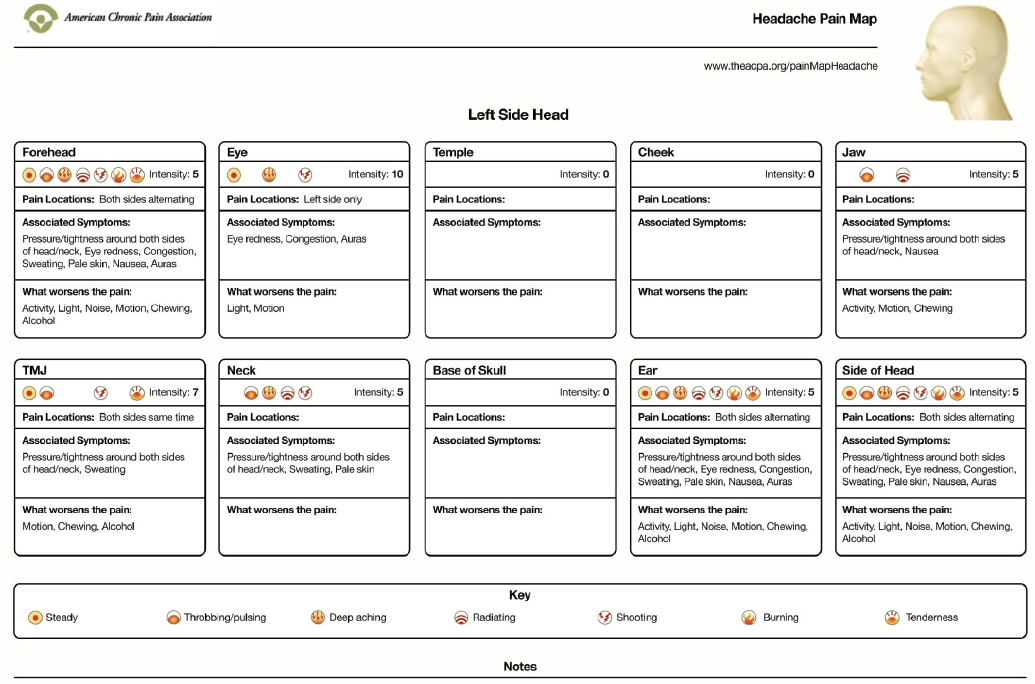
SOURCE: ACPA, 2019a.
networks (The TMJ Association, 2019a). Additionally, The TMJ Association offers a way to connect with a TMJ support contact person through individual patient support (The TMJ Association, 2019b). Peer support groups and related resources are also available through the ACPA (2019c) and other relevant patient-focused organizations active on social media platforms.
Communications Among Patients and Health Care Professionals
The patient–clinician exchange is paramount to the patient-centered care model, and the reciprocal nature of this interaction brings with it responsibilities on both sides. This chapter is focused on actions for patients and their families and the general public, but one key to making communications successful is improving education and training for health care professionals on TMDs and enhancing their communication skills (see Box 7-1; Chapter 6). Patients also have responsibilities to be engaged and to express their concerns. Additionally, patients have rights to expect listening, engagement, and communication from their health care professionals (see Box 7-1). Although patient–clinician communication is generally thought of as a one-on-one encounter between the patient and clinician, there are also
responsibilities for health care organizations to facilitate patient-centered communications through multiple avenues, including patient education materials, organizational signage, patient forums, and training health care professionals to improve their communication skills (Wynia and Osborn, 2010) and to incorporate validated shared decision-making tools into such considerations as whether to have surgery.
Researchers have found that a patient’s active participation in a health care visit increases a physician’s patient-centered communication (Cegala and Post, 2009). In a study of more than 6,000 patients with atherosclerotic cardiovascular disease, researchers found a strong relationship between patient–clinician communication and improvements in outcomes, including the use of health care resources, health care costs (decreases in costs), and the use of evidence-based therapies (Okunrintemi et al., 2017). Efforts are being made to improve communication between patients and health care professionals. A study by Sondell and Soderfeldt (1997) found differences in how medical and dental consultations and care are generally organized and provided. Medical and other health consultations are often more sequentially organized, aimed at diagnosis, prescribing treatment, providing treatment, and reviewing progress. Dental consultations may be more parallel in structure, often occurring at the same time as treatments and often in the location where the procedures are or will be occurring. These variations may affect the nature and extent of patient–clinician communications. Training can be provided to patients so that they can help in effectively setting agendas and delivering concise biopsychosocial histories that will lead to more accurate diagnoses and better partnerships with their health care professionals (Dwamena et al., 2009).
The Institute for Healthcare Improvement developed an Ask Me 3 campaign to encourage people to ask three basic questions of their health care professionals:
- What is my main problem?
- What do I need to do?
- Why is it important for me to do this? (IHI, 2019)
Many factors are important in patients finding value in talking with health care professionals. A study by Haverfield and colleagues (2017) found that patients recognized that it was their responsibility to be open to sharing their experiences with the clinician, and they identified key elements that enhanced communications. The key elements included the patients’ interest in talking with a health care professional who avoids judgments in discussions of pain, with whom they have established trust (often through time), and who is willing to talk about preferences and engage in shared decision making. Patients also indicated that the clinician’s listening
behavior is an important factor in satisfactory communications (Haverfield et al., 2017).
As discussed above, ongoing efforts to develop, implement, and evaluate tools to assist patient–clinician communication (e.g., pain maps, pain logs/journals, shared decision making) provide the mechanisms for patients to provide more visually based or chronologically based descriptions of the pain that they are experiencing. Patients can also benefit from the broader set of public education efforts designed to improve communications between patients and health care professionals. Importantly, patients also need to know and exercise their rights to information and seeking multiple opinions on their health conditions (see Box 7-2).
RAISING PUBLIC AWARENESS AND KNOWLEDGE ABOUT TMDs
The 2011 IOM report on pain noted, “Currently, public education about pain is not conducted in a large-scale, systematic, coordinated,
and strategic way” (IOM, 2011b, p. 189), and compared the lack of an organized approach with the more organized efforts on smoking cessation, cancer, end of life, and Alzheimer’s disease. The extent of public awareness about TMDs has not been assessed as far as the committee could determine. However, given the challenges expressed to the committee by patients and health care professionals, the need for increased public awareness has become evident.
The avenues for raising public awareness and improving knowledge that have been successfully used for other health conditions include:
- Public awareness campaigns.
- Designating a specific month or day to focus on the disease or disorder and planning community-based activities or campaigns at that time. September is designated as Pain Awareness Month.
- Identifying high-profile individuals with a connection to TMDs who can share their personal stories and act as spokespeople.
- Additionally, the 2011 IOM report included the following list of educational tools that are useful in reaching the public:
- website content, listservs, videos, and social media;
- fact sheets and leaflets distributed to target audiences and available at multiple locations, including schools, health facilities, workplaces, wellness classes, places of worship, and other public venues;
- informational reports and studies;
- signs at health facilities and in health professionals’ offices; and
- media outreach including to television and movie scriptwriters.
One avenue for raising public awareness is through public education campaigns, which are often multimedia efforts to engage the general public and provide one or more key messages about the health condition, with links provided for those interested in further information. Public health campaigns are often initiated as government agency efforts or through public–private partnerships because of the broad constituencies needed to develop, evaluate, fund, and carry out these efforts on varying media platforms. Formative and ongoing evaluations of the campaigns are critically important to keeping the messages relevant and tracking health or health behavior outcomes. For example, the Centers for Disease Control and Prevention’s Screen for Life: National Colorectal Cancer Action Campaign started in 1999 with more than 200 focus groups that assessed knowledge and messaging, and there have been ongoing evaluations of the campaign (CDC, 2019a). The National Pain Strategy outlines a detailed set of objectives, strategies, and deliverables for a national public awareness campaign on the seriousness and impact of chronic pain (see Box 7-3) that can be
applied or extended to TMDs. The numerous avenues for communication (e.g., messaging apps, social media, online videos, health-focused television or cable programs) offer possibilities for disseminating TMD-related information (Li et al., 2016; Devan et al., 2019). For example, Basch and colleagues (2017) examined the content of 100 videos on YouTube that focused on TMDs and found that most of them provided some information on defining TMDs and many discussed treatments, but no assessment was done of the evidence-based quality of the information.
Key Messages for the General Public
The committee recognizes that public campaigns are costly and complex to mount, but it believes that the numbers of people with TMDs and the problems identified in seeking appropriate care warrant moving ahead
with exploring a campaign that would need to be validated and well tested, grounded in the evidence base, and attentive to delivering clear messages that are understandable to individuals with different levels of health literacy (IOM, 2004).
Some key messages to include in public messaging are noted below, but these should be augmented and refined by appropriate stakeholders, including patients, health care professionals, health agencies, and media groups. Chapter 5 provides more details on self-management messages. Possible key messages include the following:
- Not all TMDs are the same. A variety of disorders can affect the jaw joint or its associated muscles and nerves. TMDs can range from those that are short term and require no treatment to those that are long term, complex, and require more involved treatments.
- Avoid harm. Historically, some treatments have led to worsening rather than alleviating TMD symptoms and dysfunction. An improved understanding of treatment options and outcomes for TMDs has led to an increased focus on holistic management and avoidance of aggressive surgical interventions early in the disease process. Surgical treatment is indicated for some patients, but it is rarely the complete solution. When needed, surgery should be performed by specialists with knowledge and experience in this condition. As noted in the NIH brochure on TMD treatment, “less is often best” in treating these disorders (NIDCR, 2013).
- Explore options for care. Be informed and seek evidence-based and interprofessional approaches to care (across medicine, dentistry, nursing, physical therapy, integrative health, and other relevant care pathways), particularly for severe pain and complex cases. Inquire about different treatment options and self-care approaches. When symptoms are severe or have not been relieved with the initial treatment, consider seeking care from health care professionals with specialty training in orofacial pain or in a dedicated multidisciplinary program for the treatment of orofacial pain.
- Be empowered to ask questions, seek person-centered care, and get multiple opinions. A basic right of patients is the right to ask for information to make an informed decision and to seek more than one opinion from health professionals and other patients. The focus of care should be on the total health and well-being needs of each individual, with time taken for discussion with and input from the patient. Frequently, persons with TMDs may also have other related health conditions, and so this holistic approach is needed. Furthermore, patients who are in pain need to be validated and to know they can seek more information and additional opinions.
- The knowledge base underlying the biology of TMDs and the care of patients is in its infancy. Research on the mechanisms and biology of TMDs, their epidemiology, and approaches to TMD care are needed before evidence-based guidelines can be developed and implemented. This will make navigating the current care landscape difficult and underscores the need for conservative treatments as starting points for TMD care.
CONCLUSION AND RESEARCH PRIORITIES
The lack of awareness about TMDs was identified as a barrier to patient care and to patients and families making informed decisions. The committee’s discussions focused on the need to overcome stigmas that may be associated with TMDs and with facial pain and to provide evidence-based
resources for patients, their families, and the general public. The committee acknowledges that significant amounts of time, energy, and financial resources and commitments are required to carry out these efforts and urges strong collaborative efforts involving professional associations and patient advocacy groups, along with federal agency and other partners, that are needed to move this work forward.
Research on the educational aspects of TMD diagnosis and care has been limited. Throughout this chapter, the committee has identified improvements that are needed to fully educate potential patients, families, health care professionals, and the general public on TMDs.
Conclusion 7-1: Building evidence-based communication resources will require attention to:
- Developing guidelines for the evaluation of communication resources on temporomandibular disorders (TMDs) (including health literacy evaluations) and then using the guidelines to evaluate existing educational resources and tools as a basis for improvements and for building new resources;
- Developing evidence-based consumer roadmaps and websites to help individuals and families identify trusted sources for evidence-based information and referrals; and
- Working with advocacy organizations and health professional associations to ensure widespread dissemination of evidence-based information on TMDs.
The committee provides the following research priorities (see Box 7-4). As outlined in Chapter 8, there are a number of actions that can be taken to improve patient, family, and professional education; to raise awareness in the general public; and to reduce stigma.
REFERENCES
ACPA (American Chronic Pain Association). 2019a. Head pain map. http://www.theacpa.org/pain-management-tools/communication-tools/tracking-tools/head-pain-map (accessed July 10, 2019).
ACPA. 2019b. Pain log. https://www.theacpa.org/pain-management-tools/communicationtools/tracking-tools/pain-log (accessed July 10, 2019).
ACPA. 2019c. Support groups. https://www.theacpa.org/about-us/support-groups (accessed July 10, 2019).
ACPA. 2019d. Pain management tools. https://www.theacpa.org/pain-management-tools (accessed July 10, 2019).
ACPA. 2019e. Family matters series. https://www.theacpa.org/pain-management-tools/videos/support (accessed September 23, 2019).
ACPA. 2019f. Basic rights. https://www.theacpa.org/pain-management-tools/basic-rights (accessed July 10, 2019).
Afsal, M. M., A. Khatri, N. Kalra, R. Tyagi, and D. Khandelwal. 2019. Pain perception and efficacy of local analgesia using 2% lignocaine, buffered lignocaine, and 4% articaine in pediatric dental procedures. Journal of Dental Anesthesia and Pain Medicine 19(2):101–109.
Armentor, J. L. 2017. Living with a contested, stigmatized illness: Experiences of managing relationships among women with fibromyalgia. Qualitative Health Research 27(4):462–473.
Back, A. L., R. M. Arnold, W. F. Baile, J. A. Tulsky, and K. Frayer-Edwards. 2005. Approaching difficult communication tasks in oncology. CA: A Cancer Journal for Clinicians 55(3):164–177.
Basch, C. H., J. Yin, N. D. Walker, A. J. de Leon, and I. C. Fung. 2017. TMJ online: Investigating temporomandibular disorders as “TMJ” on YouTube. Journal of Oral Rehabilitation 45:34–40.
Bijur, P. E., W. Silver, and E. J. Gallagher. 2001. Reliability of the visual analog scale for measurement of acute pain. Academic Emergency Medicine 8(12):1153–1157.
CDC (Centers for Disease Control and Prevention). 2019a. About the Screen for Life campaign. https://www.cdc.gov/cancer/colorectal/sfl/about.htm (accessed July 18, 2019).
CDC. 2019b. Health literacy. https://www.cdc.gov/healthliteracy/index.html (accessed December 3, 2019).
Cegala, D. J., and D. M. Post. 2009. The impact of patients’ participation on physicians’ patient-centered communication. Patient Education and Counseling 77(2):202–208.
Chen, A. T. 2012. Information seeking over the course of illness: The experience of people with fibromyalgia. Musculoskeletal Care 10(4):212–220.
Cook, J. E., V. Purdie-Vaughns, I. H. Meyer, and J. T. A. Busch. 2014. Intervening within and across levels: A multilevel approach to stigma and public health. Social Science & Medicine 103:101–109.
Corrigan, P. W. 2014. The stigma of disease and disability: Understanding causes and overcoming injustices. Washington, DC: American Psychological Association.
Cowan, P., N. Kelly, C. Passero, and E. Covington. 1998. ACPA Family Manual A manual for families of person with pain. Rocklin, CA: ACPA.
De Ruddere, L., and K. D. Craig. 2016. Understanding stigma and chronic pain: A state-of-the art review. Pain 157(8):1607–1610.
Desai, B., N. Alkandari, and D. M. Laskin. 2016. How accurate is information about diagnosis and management of temporomandibular disorders on dentist websites? Oral Surgery, Oral Medicine, Oral Pathology, and Oral Radiology 122(3):306–309.
Devan, H., H. K. Godfrey, M. A. Perry, D. Hempel, B. Saipe, L. Hale, and R. Grainger. 2019. Current practices of health care providers in recommending online resources for chronic pain management. Journal of Pain Research 12:2457–2472.
Driscoll, M. A., M. T. Knobf, D. M. Higgins, A. Heapy, A. Lee, and S. Haskell. 2018. Patient experiences navigating chronic pain management in an integrated health care system: A qualitative investigation of women and men. Pain Medicine 19(Suppl 1):S19–S29.
Dubin, R. E. 2017. Acknowledging stigma: Its presence in patient care and medical education. Canadian Family Physician 63:906–908.
Dwamena, F. C., B. Mavis, M. Holmes-Rovner, and A. Loyson. 2009. Teaching medical interviewing to patients: The other side of the encounter. Patient Education and Counseling 76(3):380–384.
Fisher, E. B., G. X. Ayala, L. Ibarra, A. L. Cherrington, J. P. Elder, T. S. Tang, M. Heisler, M. M. Safford, and D. Simmons. 2015. Contributions of peer support to health, health care, and prevention: Papers from Peers for Progress. Annals of Family Medicine 13(Suppl 1):S2–S8.
Forsythe, L. P., K. L. Carman, V. Szydlowski, L. Fayish, L. Davidson, D. H. Hickam, C. Hall, G. Bhat, D. Neu, L. Stewart, M. Jalowsky, N. Aronson, and C. U. Anyanwu. 2019. Patient engagement in research: Early findings from the Patient-Centered Outcomes Research Institute. Health Affairs 38(3):359–367.
Fortin, A. H., F. C. Dwamena, R. M. Frankel, and R. C. Smith. 2012. Smith’s patient centered interviewing: An evidence-based method. Third edition. New York: McGraw-Hill.
Gottlieb, S. 2000. Health information on internet is often unreliable. BMJ [online]. https://www.bmj.com/content/321/7254/136.3.full (accessed July 15, 2019).
Greene, J., J. H. Hibbard, R. Sacks, V. Overton, and C. D. Parrotta. 2015. When patient activation levels change, health outcomes and costs change, too. Health Affairs 34(3):431–437.
Haverfield, M. C., K. Giannitrapini, C. Timko, and K. Lorenz. 2017. Patient-centered pain management communication from the patient perspective. Journal of General Internal Medicine 33(8):1374–1380.
Hawker, G. A., S. Mian, T. Kendzerska, and M. French. 2011. Measures of adult pain. Arthritis Care & Research 63(S11):S240–S252.
Heisler, M. 2010. Different models to mobilize peer support to improve diabetes self-management and clinical outcomes: Evidence, logistics, evaluation considerations and needs for future research. Family Practice 27(Suppl 1):i23–i32.
Hoffmann, D. E., and A. J. Tarzian. 2001. The girl who cried pain: A bias against women in the treatment of pain. The Journal of Law, Medicine, & Ethics 29(1):13–27.
IHI (Institute for Healthcare Improvement). 2019. Ask Me 3: Good questions for your good health. http://www.ihi.org/resources/Pages/Tools/Ask-Me-3-Good-Questions-for-Your-Good-Health.aspx (accessed July 11, 2019).
INfORM (International Network for Orofacial Pain and Related Disorders Methodology). 2013. Pain map. https://ubwp.buffalo.edu/rdc-tmdinternational/tmd-assessmentdiagnosis/dc-tmd (accessed November 1, 2019).
IOM (Institute of Medicine). 2004. Health literacy: A prescription to end confusion. Washington, DC: The National Academies Press.
IOM. 2011a. Patients charting the course: Citizen engagement and the learning health system: Workshop summary. Washington, DC: The National Academies Press.
IOM. 2011b. Relieving pain in America: A blueprint for transforming prevention, care, education, and research. Washington, DC: The National Academies Press.
IOM. 2012. Epilepsy across the spectrum: Promoting health and understanding. Washington, DC: The National Academies Press.
IOM. 2014. Partnering with patients to drive shared decisions, better value, and care improvement: Workshop proceedings. Washington, DC: The National Academies Press.
Keller, S., C. M. Bann, S. L. Dodd, J. Schein, T. R. Mendoza, and C. S. Cleeland. 2004. Validity of the Brief Pain Inventory for use in documenting the outcomes of patients with non-cancer pain. Clinical Journal of Pain 20(5):309–318.
Khatri, A., and N. Kalra. 2012. A comparison of two pain scales in the assessment of dental pain in East Delhi children. ISRN Dentistry. doi: 10.5402/2012/247351.
LeResche, L. 2011. Defining gender disparities in pain management. Clinical Orthopaedics and Related Research 469(7):1871–1877.
Li, X., Z. R. Xu, N. Tang, C. Ye, X. L. Zhu, T. Zhou, and Z. H. Zhao. 2016. Effect of intervention using a messaging app on compliance and duration of treatment in orthodontic patients. Clinical Oral Investigations 20(8):1849–1859.
Marbach, J. J., M. C. Lennon, B. G. Link, and B. P. Dohrenwend. 1990. Losing face: Sources of stigma as perceived by chronic facial pain patients. Journal of Behavioral Medicine 13(6):583–604.
Matthias, M. S., M. Kukla, A. B. McGuire, and M. J. Bair. 2016. How do patients with chronic pain benefit from a peer-supported self-management intervention? A qualitative investigation. Pain Medicine 17:2247–2255.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Hearing health care for adults: Priorities for improving access and affordability. Washington, DC: The National Academies Press.
NASEM. 2019. Integrating oral and general health through health literacy practices. Washington, DC: The National Academies Press.
NIDCR (National Institute of Dental and Craniofacial Research). 2013. Less is often best in treating TMJ disorders. https://www.nidcr.nih.gov/sites/default/files/2017-09/less-is-best-tmj.pdf (accessed August 30, 2019).
NIH (National Institutes of Health). 2016. National pain strategy. https://www.iprcc.nih.gov/sites/default/files/HHSNational_Pain_Strategy_508C.pdf (accessed July 18, 2019).
Okunrintemi, V., E. S. Spatz, P. Di Capua, J. A. Salami, J. Valero-Elizondo, H. Warraich, S. S. Virani, M. J. Blaha, R. Blankstein, A. A. Butt, W. B. Borden, K. Dharmarajan, H. Ting, H. M. Krumholz, and K. Nasir. 2017. Patient-provider communication and health outcomes among individuals with atherosclerotic cardiovascular disease in the United States. Circulation: Cardiovascular Quality and Outcomes 10(4).
Pescosolido, B. A., and J. K. Martin. 2015. The stigma complex. Annual Review of Sociology 41:87–116.
Racich, M. J. 2009. What are 3 key elements of the TMD patient interview. Journal of the Canadian Dental Association 75(3):197–198.
Ramsey, I., N. Corsini, M. D. J. Peters, and M. Eckert. 2017. A rapid review of consumer health information needs and preferences. Patient Education and Counseling 100(9):1634–1642.
Ring, D., and S. Lawn. 2019. Stigma perpetuation at the interface of mental health care: A review to compare patient and clinician perspectives of stigma and borderline personality disorder. Journal of Mental Health 12:1–21.
Scott, W., L. Yu, S. Patel., and L. M. McCracken. 2019. Measuring stigma in chronic pain: Preliminary investigation of instrument psychometrics, correlates, and magnitude of change in a prospective cohort attending interdisciplinary treatment. Journal of Pain 20(10):1164–1175.
Slade, S. C., E. Molloy, and J. L. Keating. 2009. Stigma experienced by people with nonspecific chronic low back pain: A qualitative study. Pain Medicine 10(1):143–154.
Sondell, K., and B. Soderfeldt. 1997. Dentist-patient communication: A review of relevant models. Acta Odontologica Scandinavica 55:116–126.
Storino, A., J. Castillo-Angeles, A. A. Watkins, C. Vargas, J. D. Mancias, A. Bullock, A. Demirjian, J. Moser, and T. S. Kent. 2016. Assessing the accuracy and readability of online health information for patients with pancreatic cancer. JAMA Surgery 151(9):831–837.
The TMJ Association. 2019a. TMJ Café: Temporomandibular disorders support and discussion community. https://www.inspire.com/groups/tmjcafe (accessed July 11, 2019).
The TMJ Association. 2019b. TMJ support community. http://www.tmj.org/Page/29/14 (accessed July 11, 2019).
Wakefield, E. O., W. T. Zempsky, R. M. Puhl, and M. D. Litt. 2018. Conceptualizing pain-related stigma in adolescent chronic pain: A literature review and preliminary focus group findings. Pain Reports 3(Suppl 1):e679.
Waugh, O. C., D. G. Byrne, and M. K. Nicholas. 2014. Internalized stigma in people living with chronic pain. Journal of Pain 15(5):550e1–550e9.
Woolf, S. H., E. Zimmerman, A. Haley, and A. H. Krist. 2016. Authentic engagement of patients and communities can transform research, practice, and policy. Health Affairs 35(4):590–594.
Wynia, M. K., and C. Y. Osborn. 2010. Health literacy and communication quality in health care organizations. Journal of Health Communications 15(Suppl 2):102–115.
This page intentionally left blank.
























