Proceedings of a Workshop
| IN BRIEF | |
|
April 2020 |
Army Combat Trauma Care in 2035
Proceedings of a Workshop—in Brief
The National Academies of Sciences, Engineering, and Medicine, under the auspices of the Board on Army Research and Development (BOARD), convened a workshop of leading military, researchers, medical, and intelligence professionals on November 18, 2019, to examine the future of Army combat trauma care and emerging medical advancements that could improve soldier survivability in high-intensity conflicts in 2035. Specifically, the workshop participants explored and discussed how bioengineering can return soldiers to the fight quicker; areas of Army tactical combat care that can be improved now; and future related threats, risks, and status of preparedness. Jim Bagian, University of Michigan, and Joan Bienvenue, University of Virginia, workshop co-chairs, welcomed the attendees with a special thank you to the military and members of organizations dedicated to ensuring the best care possible for those wounded.
DAY 1. KEY ELEMENTS OF COMBAT TRAUMA CARE, RELATED SYSTEMS, AND FUTURE OPERATIONAL ENVIRONMENTS
Overview of Tactical Combat Casualty Care, Including Point of Wounding. John Gandy, Vigilant Protective Health Solutions, provided the first presentation. He explained that in Tactical Combat Casualty1 Care (TCCC), 87 percent of combat deaths occur before the patient reaches a military hospital and 24 percent of those deaths may be preventable. Gandy noted that most preventable deaths are caused by hemorrhage and, to a much lesser degree, by airway obstruction. Current TCCC guidelines have been upgraded to include more beneficial methods of care, but Gandy noted there are still areas for improvement. For instance, these challenges can be ameliorated by the establishment of TCCC preparedness as a line-commander responsibility with oversight by the Chairman of Joint Chiefs of Staff (JCS). In his view, operational commanders should be responsible for ensuring adequate training and equipping of deployed forces and for documenting battlefield trauma care. Gandy also noted opportunities for improving future technologies, including technologies to slow or halt truncal hemorrhage and making available shelf-stable fluids that approach whole-blood capabilities.
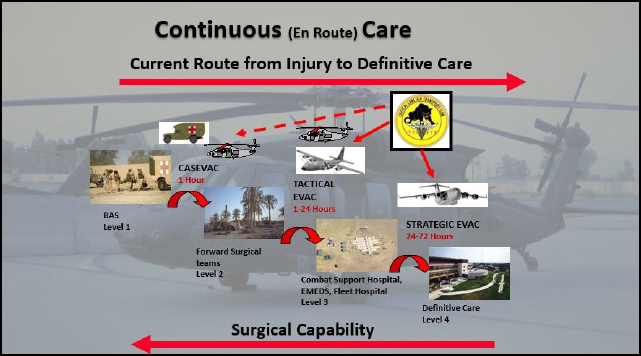
Continuum of Care. Jay Johannigman, Uniformed Services University of the Health Sciences and Brooke Army Medical Center, focused his presentation on the 24 to 72 hours that is typically required to move a patient from initial injury to definitive care (Figure 1). He contended that the medical community should adopt lightweight, modular, mobile core capabilities and life-saving interventions (LSIs) to push care closer to the battlefield. He also argued that an overemphasis on the Golden Hour2 concept is in some cases limiting the option
___________
1 Casualty refers to both injured and killed personnel.
2 The Golden Hour response time denotes Defense Secretary Robert Gates’ 2009 mandate that pre-hospital helicopter transport of critically injured combat casualties should take 60 minutes or less. (See, for example, R.S. Kotwal, J.T. Howard, J.A. Orman, B.W. Tarpey, J.A. Bailey, H.R. Champion, R.L. Mabry, et al., 2016, The effect of a Golden Hour policy on the morbidity and mortality of combat casualties, JAMA Surgery 151(1):15-24, doi:10.1001/jamasurg.2015.3104.)

of obtaining higher-quality care at a different time or facility. Effort is spent transporting a soldier to the closest medical center immediately following an incident instead of leveraging better care during longer-duration transport. For example, many LSIs can be accomplished earlier in the continuum of care rather than waiting until surgery, raising the possibility of death in the meantime. Quantifying that opportunity cost requires data, which is often lacking due to combat zone collection challenges and a lack of line leadership emphasis. He urged damage-control actions to extend survival by any means plus en-route care involving medical teams (physician, nurse, respiratory therapist, etc.) for air missions greater than 1-2 hours and up to 12 hours in duration. In summary, Johannigman emphasized the following four points:
- Data should be continuously captured, retained, and forwarded.
- Data that facilitates real-time care and guides review and change in the form of a trauma registry is critical.
- The Army should continue supporting, updating, and upgrading the trauma registry (the instrument panel).
- There is a need to break the paradigm of medical equipment procurement so as to not practice tomorrow’s medicine with today’s equipment.
Combat Casualty Mortality. Brian Eastridge’s, University of Texas Health (San Antonio), presentation at the workshop focused on preventing deaths after injuries and their implications for the Joint Trauma System (JTS) and warfighters. After referring to findings and recommendations of the 2016 National Academies report A National Trauma Care System: Integrating Military and Civilian Trauma Systems to Achieve Zero Preventable Deaths After Injury,3 he declared that a fundamental gap, the “missing dead” is a trauma system blind spot. Eastridge highlighted the value of mortality analysis and its relationship to the pillars of a modern trauma system. To extend survival time from point of injury to hospital in the case of hemorrhages, he said mitigation strategies need to include tourniquets, junctional hemorrhage control, intracorporeal hemostasis, freeze dried plasma, novel therapeutics, and the use of tranexamic acid.
Overview of the Joint Trauma System. Mary Ann Spott, Defense Health Agency, presented the JTS as a collection of policies, training, and medical materials. A primary JTS goal is to ensure every injured military member has an optimal chance for survival and maximum potential for functional recovery. The JTS aims to serve as a reference body for all trauma care, establish care standards, and coordinate the transition of research into practice. Spott noted that several gaps include tight Department of Defense (DoD) resourcing, difficulty in obtaining and retaining proficient trauma clinicians, and challenges obtaining surgical and evacuation teams for operations. She proposed solutions including full funding for research, fostering better military-civilian partnerships, requiring more trauma and critical-care teams in broader DoD, and increasing trauma-team specialists in all services. She noted additional areas for improvement, such as a seamless system of trauma care; standardizing data collection and performance improvement to include quality control/assurance mechanisms; and continued work on preventable deaths.
Burns. Lee Cancio, Army Institute of Surgical Research, presented the subject of burn care and treatment, noting that burns complicate approximately 5 to 10 percent of combat casualties and that there could be an increased number of burn injuries in future conflicts. He identified the three burn-care phases, which must be addressed simultaneously, as immediate, critical, and rehabilitation-return to duty. He described gaps includ-
___________________
3 National Academies of Sciences, Engineering, and Medicine, 2016, A National Trauma Care System: Integrating Military and Civilian Trauma Systems to Achieve Zero Preventable Deaths After Injury, The National Academies Press, Washington, D.C.
ing plasma, resuscitation, infection diagnosis (which is the leading cause of death in burn patients), and massive burns and pain. Suggested solutions, he noted, include using technology for early detection of infection and developing more rapid skin-culture techniques such as bilaminar (dermis, epidermis) cultured skin for grafting massive burns, as well as pharmacologic options to enhance wound healing.
Fluid Resuscitation for Hemorrhagic Shock. Don Jenkins, University of Texas Health (San Antonio), presented on the topic of hemorrhagic shock. Jenkins explained that the first step is to identify the patient is in shock. He noted pre-hospital resuscitation with blood products limits the risk of death due to hemorrhage and that providing whole blood, plasma, platelets, and dried plasma to rural or austere environments will save lives. He noted that U.S. military care providers must be proficient in use of these products. He noted that the San Antonio/STRAC (Southwest Texas Advisory Council) has essentially recreated a military-like prehospital blood program for civilian use. This allows us to better refine and study the process and potentially serve as a proving ground for how to best implement a whole blood program in future conflicts.
Military Combat Injury Scale (MCIS) and Military Functional Incapacity Scale (MFIS). Harald Scheirich, SimQuestSolutions, presented on the topic of MCIS and MFIS scales. MCIS puts injury coding into a military context, and MFIS establishes a tactical interpretation of these codes. This, he noted, enables more objective measures of care and decision making. He explained that the system was developed because existing injury scales are inadequate for coding combat injuries. He explained that the five-level MCIS was developed by a multiservice panel of experts because existing injury scales were inadequate for coding combat injuries. The model assigns an immediate tactical functional capacity scale (the MFIS) to minor and moderate injuries. He noted that the MCIS severity level 1 is minor, level 2 is moderate (possible impairment in immediate ability to shoot, move, or communicate), level 3 is serious and should be treated within 6 hours at a medical treatment facility, and the scale continues from there. MFIS levels are similar (e.g., MFIS level 2 is “Injured: not fully functional; likely able to contribute to sustaining mission,” and MFIS level 3 is “Lost to mission”). In summary, Scheirich said that MCIS is a medically valid, robust, simple interface tool for use by engineers, modelers, and other relevant medical researchers and personnel.
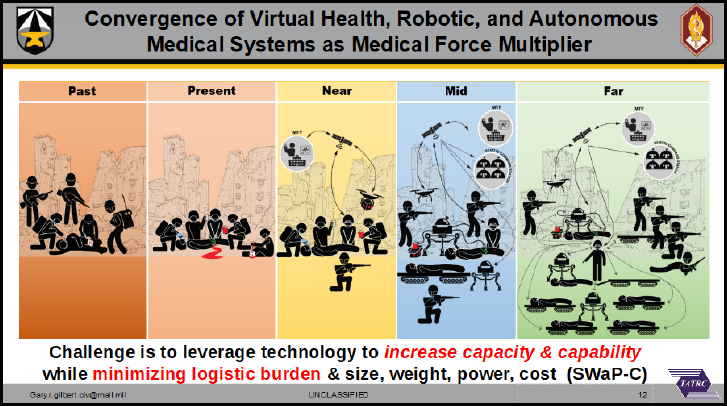
Virtual and Autonomous Systems in Remote and Multi-Domain Scenarios. Gary Gilbert, Army Medical Research and Development Command, gave a presentation on the applications of virtual systems to support medical operations in remote locations. He argued that virtual health (VH) is a broad discipline encompassing traditional telemedicine and tele-health concepts as well as artificial intelligence (AI), in addition to medical robotics and autonomous systems (MED-RAS). Current VH and MED-RAS research priorities are aimed at future solutions for combat traumas in multi-domain operations. Forces will be dispersed over vast distances and diverse terrains, delaying evacuations and increasing the need for prolonged care up front. He suggested that autonomous casualty care could help in the future by leveraging technology, as shown in the right three segments of Figure 2. He also suggested prioritizing research for intelligent medic-assist decision support, manned and unmanned patient extraction, robotic perception, and tele-robotic surgery.
Future Operational Environments, Gaps, Needs, and Opportunities. Gerald Leverich, Army Training and Doctrine Command (G2), gave a presentation on the changing character of warfare, which will include proliferation of weapons of mass destruction, multi-domain operational conflicts, regional insurgencies, near-peer or peer competitors, new forms of weaponry (lasers, rail guns, advanced energetics) and cyber and space conflict. In contrast to recent counter-insurgency conflicts, the scale, lethality, and ranges involved will be much larger, resulting in long delays until necessary treatment can be rendered, and mass casualties will likely be experienced both on land and on sea.
DAY 2, PART I. MILITARY LEADERSHIP, PLANNING, AND TRAINING
Role of Military Line Leadership and Ensuring Excellence in Combat Casualty Care. Jim Geracci (Col. Army Retired, MD), Ascension Healthcare Texas and former Chief Medical Officer (Command Surgeon) U.S. Army III Corps, addressed the critical role of line leadership. He summarized the legacy of battlefield medical innovation over the last century and discussed the role of TCCC in special operations. He explained there is no substantive TCCC linkage to doctrine, capability development, and training, in addition to lack of TCCC ownership among Army leadership. Areas for improvement include a policy to establish TCCC as standard training, providing first-responder TCCC certification training for every soldier, and clear General Officer–level guidance that highlights medical care as “commander’s business.” He indicated that a promising sign was a March
2018 DoD instruction on medical readiness training,4 which included the policy that TCCC is the DoD care standard for responders and all service members are to receive TCCC training and certification.
Joint Medical Planning Tools. Mike Galarneau, Naval Health Research Center, discussed a range of planning capabilities (e.g., a knowledge warehouse and medical-planners toolkit) that can estimate parameters like casualties and expeditionary medical requirements based on scenario inputs. He also described a joint planning tool that helps medical planners improve medical systems in the expeditionary environment and provides analysis of medical risks and courses of action. Galarneau explained a gap in the Navy’s system is because today’s planning is informed by ground-oriented data over the past 15 years and does not account for those injured on board or in the water after ships are damaged or sunk. He noted that environmental conditions (e.g., water temperature, availability of life-preserving equipment, hypothermia, etc.), degraded mission performance (as other ships conduct personnel recovery and casualty care), and the threat of chemical, biological, radiological, and nuclear agents must also be accounted for.
Initial, Recurring, Personalized, Mission-Specific Competence Assessment and Team-Based Training. Jeffrey Beaubien, Aptima Inc., focused his presentation on opportunities to modernize military medical training and education. He pointed to big data and AI as the future of training at scale and discussed a notional system architecture, buttressed by instructional and assessment content, for modernizing talent management and the technology ecosystem (advanced distributed-learning tools like the experience application programming interface [xAPI]). Beaubien identified immediate opportunities for improvement, such as performance measurement via xAPI, the need for big data that encompasses formal, informal, and lifelong learning events, and leveraging AI-based tools for personalized learning, conducting training at scale, and continued organizational improvement.
Integration with Line Tactical Training, Synthetic Training Environment, and Medical Simulation. Dan Irizarry, Global Special Operations Forces Foundation, presented on a path to improved combat trauma care through medical training and simulation. Contrasting this with past methods (lecture halls) and common practice today (instruction manuals), he identified shortfalls (e.g., not measuring comprehension effectively) that could be addressed with advanced techniques and future technologies, especially simulation. He argued that accomplishing this will require a top-down mandate with bottom-up implementation and careful integration into the synthetic training environment (STE) through a series of near- and longer-term measures, such as reconfigurable, virtual, collective (small-large groups) trainers; scalable simulation software; training delivery to points of need across all formation sizes; training management tools with unrestricted access to create dynamic and realistic scenarios; and tools that enable big data and AI/machine learning (ML) to assess training effectiveness across all training devices. (See Figure 3 for an overview of STE capabilities.)
How Long Can the Military’s Golden Hour Last? Advancing Technology, Training, and Expectations for Multi-Domain Operations. Todd Rasmussen, Uniformed Services University of the Health Sciences (via VTC), discussed the Golden Hour concept and stated that the United States has fallen short in establishing an integrated (military-civilian) national-trauma action plan, in part by assuming that low casualty rates could be achieved in technology-enabled future wars. He believes the military should remain focused on new ways
___________________
4 Office of the Under Secretary of Defense for Personnel and Readiness, 2018, “DoD Instruction 1322.24, Medical Readiness Training (MRT),” March 16, https://jts.amedd.army.mil/assets/docs/policies/MRT-DoDI-1322-24.pdf.
for JTS to extend and refine the Golden Hour through technologies, training, and expectations. His examples included ways to improve resuscitative care, new endo-vascular devices coupled with automated drug and fluid delivery tools, wearable bio-sensors, expansive data collection, telemedicine, antimicrobial dressings and self-expanding foams, devices to diagnose concussive traumatic brain injuries, devices for brain-wave- and eye-tracking, rapid blood tests, and drones to deliver supplies or conduct evacuations. He noted that each of these will require new training requirements and the JTS should ensure that DoD in utilizing the STE is prepared to address them. Rasmussen noted that expectations regarding triage categories; that is, the prioritization of which injuries are most treatable may need to change. In some scenarios, the military may need to categorize the severely injured or incapacitated as delayed or expectant. A participant suggested that the changing or lengthening of the Golden Hour to the “Golden Period” (up to a day or a few days with an acceptance of higher casualties) needs to be considered for future operational scenario and estimates regarding resource availability.
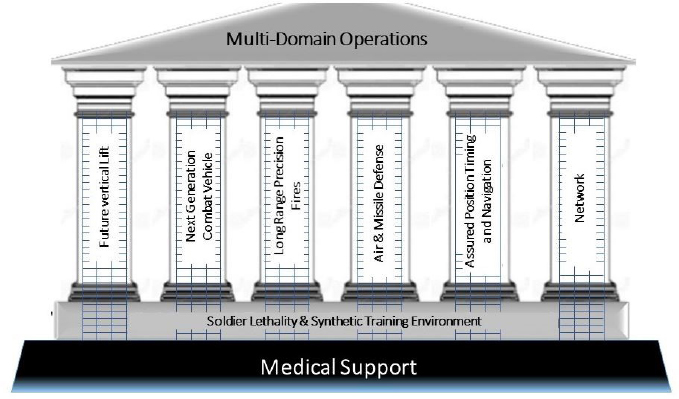
Ever Adapting for the Warfighter: Combat Casualty Care for the Future Battlespace. Michael Davis, Army Medical Research and Development Command, focused his presentation on the combat casualty care research program (CCCRP) and its portfolios of battlefield resuscitation, prolonged field care, neurotrauma, and en-route care. He identified medical support as a key enabler of multi-domain battle in line with other advancements in technology (Figure 4). He suggested changing the Golden Hour concept to a “Golden Day” to emphasize that battle will require overcoming many challenges (e.g., casualty volumes, triage, and damage-control surgery delays). Davis described numerous potential medical advances including bio-sensors, next-generation REBOA (resuscitative endovascular balloon occlusion of the aorta), extracorporeal life support, drone transport, automated cranial decompression, rapid and uncompromising pain management, hemorrhage-control drugs and smart tourniquets, triage algorithms and decision support.
DAY 2, PART II. ORGANIZATIONAL AND LEADERSHIP FACTORS
Challenges to Improving Combat Casualty Care. Cord Cunningham, U.S. Special Operations Command, described in his presentation the cyclical nature of U.S. medical preparedness for the next war, principally due to a loss of leadership focus. He highlighted the dips in ownership, data and metrics, pre-hospital and trauma expertise, research and development (R&D), and hospital culture. Regarding medical corps officer training and development, he noted that there are too few critical wartime specialties. Regarding reporting mechanisms, he noted that individual medical readiness is tracked but proficiency is generally not, although it could be improved by including proficiency metrics into preparedness reporting.
Turning to research priorities, he noted that they tend toward a materiel focus over human-factor solutions. He argued that more focused research on training methodologies is needed, as are increased prolonged-care and hold capabilities. This could be improved by focusing on task-shifting training and increased scope as far forward as possible, as opposed to the more expensive research needed to advance en-route care. He argued that organizations with command emphasis result in better outcomes, due to leadership support, and that the JCS Chairman should be clearly delineated as the lead for casualty response.
Performance Improvement and Data Analysis. Mary Ann Spott’s second presentation focused on JTS data collection and performance improvements to enhance trauma readiness and outcomes. Quality assurance and quality care were emphasized as key metrics to be tracked and is critical for leadership decision making. Spott noted

that the JTS does not have a robust system that tracks these metrics at the current time. She described a continuous cycle of data collection and analysis that, among other benefits, identifies gaps in research, knowledge, and materiel. She noted that some of this effort translates to the civilian sector and described in detail barriers to data collection and performance improvement, along with proposed solutions (e.g., improved prehospital data collection, effective lessons learned, use of video recordings).
Training and Readiness, Defense Health Agency. Ruben Garza, Defense Medical Modeling and Simulation Office, described in his presentation three medically relevant types of simulations: live (real people, real systems), virtual (real people, simulated systems, and constructive (simulated people, simulated systems, but utilizing input from real situations). Garza’s office manages development and execution of service-shared modeling and simulation capabilities to support medical education, training, and preparedness.
Panel Discussion of Organizational and Leadership Factors. This panel5 consisted of five members, Cord Cunningham, John Gandy, Jim Geracci, Brian Eastridge, and Warren Dorlac, University of Colorado Health. The panelists discussed the importance of data collection as a foundation for evidence-based program improvement, but also noted gaps in the data-collection process. These include a lack of reliable pre-hospital (tactical) data (as noted by Geracci), as well as the data from medical examiners on-battlefield deaths (as noted by Eastridge). Dorlac advocated that data automation tools are the key to speeding collection and analysis. Some of the panelists expressed a view that near-term improvements in data collection and analysis can be gained with little more than focused leadership attention and would be of benefit to the entire military medical enterprise. Panelists discussed who should own responsibility for battlefield medicine preparedness, with some emphasizing that it resides with the line commanders and others arguing that it should fall to the CJCS and Secretary of Defense. Bagian remarked that the medical mission is a service to achieve the mission of the military, so if that is done correctly, then all the components (such as R&D) will be focused towards that same goal.
William Millonig, Scholar and Acting Director of BOARD, asked the participants to put themselves in the Army Chief Scientist’s role and say where they would put research and why. Cunningham said he would put research into leveraging a technology in the training environment, perhaps by focusing on the human factor in a simple-methodology way, to increase medical and casualty-response skills. Eastridge noted that the medic, the corpsman, will save the most lives of the wounded on the battlefield and urged that R&D be focused on those front-line providers trained to a complete level of mastery. Gandy suggested training to better standards and using new technologies. He described a device that a medic or non-surgeon could use to slow or halt truncal bleeding—shelf-stable products that approach actual blood in their effects on the battlefield—and a device to quantify and diagnose shock and to triage. He argued that requirements validation is critical to drive research priorities and effective R&D in support of line leadership’s priorities. Geracci favored putting more research money on blood and blood components and the rest on persistent gaps remaining in hemorrhage control. Considering research and what the future battlefield could be, Dorlac said that he would push for an unmanned casualty-evacuation platform.
DAY 3, PART I. HUMAN PERFORMANCE
Human Performance Optimization and Total Force Fitness. Travis Lunasco, Consortium for Health and Military Performance (Uniformed Services University of the Health Sciences), described a capability-based blueprint (CBB) as a commander’s tool to realign delivery of human performance (HP) and total force fitness
___________________
5 Some of the panel members provided previous presentations during earlier phases of the workshop.
(TFF) services in support of warfighters.6 Lunasco showed that HP optimization applies knowledge, skills, and emerging technologies to improve and preserve abilities of warfighters to execute mission-essential tasks and therefore should be a core responsibility. He discussed CBB workshop results indicating how TFF domains could be supported with community-based participation (e.g., by leadership, various support agencies, subject-matter experts, embedded teams, etc.) and lead to realignments and HP enhancements. On metrics, he used a critical task of fixed-target acquisition to illustrate tracing various combat conditions and exposures to physical, psychological, and spiritual health issues. Information like this, he argued, could then inform service delivery, composition, and training of embedded teams. His recommendations included integrating CBB techniques into technical-school and leadership training.
Human Performance Optimization. Chetan Kharod, Uniformed Services University of the Health Sciences, gave a presentation on HP optimization. He emphasized the human weapon system and that humans are more important than hardware. He discussed health issues in several TFF domains: psychological (stress, anxiety, depression, suicide), social (relationships, divorce), and physical (daily tasks, ergonomics). He discussed wellness, occupational health, checking human “plumbing-hardware-software,” preserving force and family, and resiliency in the TFF domains. Kharod described a range of health programs in the National Guard, Army, Air Force, and Navy. Focusing on domain wellness programs, he addressed features like purpose and belonging, embedded resources, and measurement and analysis.
Practical Application of Military Human Performance Program. Karen Daigle, Army Special Operations Command, stated in her presentation on the military HP program that because the human weapon system is so critical, HP will remain highly relevant in future battles and proper optimization can decrease chances of combat trauma. She indicated that DoD’s TFF program ought to be operational and operator-centric rather than a siloed and generic-wellness focused and that domain-expert facilitators should be available to execute the program (e.g., registered dietitians and cooks for appropriate nutrition). Daigle summarized a range of HP program gaps followed by opportunities for improvement, such as standardizing education and training for leadership and HP team members; requiring HP programs to include all preparedness domains and a balance of domain components (proactive, active, reactive); and establishing a career-spanning surveillance system with active and passive data inputs.
Improvements to Personal Protective Equipment and Warfighter Survivability Based on Real-Time Combat Trauma Information. Nick Tsantinis, Army Natick Soldier Systems Center, described examples of personal protective equipment (PPE; eyewear, helmets, body armor) and said that current armor provides approximately 19 percent body coverage. He discussed helmet and body-armor improvements (e.g., weight reductions) and explained trade-space between protection and lethality. He described the iterative process of creating PPE requirements and developing, testing, and fielding PPE. During that process, PPE encumbrances must be balanced with mission needs (e.g., shoot, move, and communicate). His analysis of gaps and improvements focused primarily on data needs, both the need for better data collection and the inability to obtain data that already exists, on combat injuries that could help enhance future PPE developments (e.g., better protection from blasts, wearing heavy equipment, carcinogens, low-velocity head impacts, etc.).
Closing Discussion with the Presenters. Russ Kotwal moderated a brief dialog with this session’s speakers focused on data needs and ownership of medical-related services. The speakers stressed the need for better access to data to help design and develop PPE. Bagian asked the speakers to comment on where ownership of battlefield medicine should reside. Kharod believes that “battlefield medicine is owned by the commander,” and Daigle added that commanders “have to want it, it can’t be thrust upon them.” Garza indicated that leadership has to see the individual as a weapon system, same as a rifle or jet, and suggested blending medical services into the operational model.
DAY 3, PART II. BIOENGINEERING FOR IMPROVED FUNCTIONAL OUTCOMES
George Christ, Planning Committee Member and University of Virginia, opened with remarks about regenerative medicine and tissue engineering, noting that restoring full form and function was the goal of postmedivac, not field care. He suggested that creative thinking about technologies application in austere envi-
___________________
6 TFF is a composite of the following seven preparedness domains: physical, environmental, medical and dental, spiritual, nutritional, psychological, and social.
ronments, with a focus on regenerative bio-materials (e.g., freeze-dried cells and tissues), tissue preservation, and important limb-salvage technology, could help focus efforts on getting soldiers back into the fight more quickly. He speculated that major steps forward will be in combining antibiotics with various materials (ones that can be carried in a pouch, be hydrated, and have regenerative and void-filling properties) and applying a wound dressing, or bracing a limb, as major steps forward. Noting that challenges with risk acceptance, market size, and regulations are considerable, he pointed out that many technologies have been developed and gone into clinical trials for different applications than envisioned.
Bioengineered Materials for Improved Wound Healing Panel. Robert Christy, Army Institute of Surgical Research, gave a presentation on next-generation dressings for burns and soft-tissue injuries. He said that burns comprise 8 to 11 percent of combat casualties, with small burns being 80 percent of that amount and large burns (greater 20 percent body area) constituting the remainder. Small burns can be treated in theater for return to duty, whereas large burns require evacuation and treatment with improved material solutions, such as skin substitutes, and temporary coverings. He described the use of several imaging techniques, such as forward-looking infrared, to assist burn assessment. He offered other technical approaches to prevent the progression of burn effects, infections, and for temporary wound coverage, as well as criteria for developing point-of-injury products for wound healing (ready application, ease of use). He suggested that technology goals should include broad-spectrum antimicrobial wound dressings, enzyme-based debridement, skin substitutes, and non-opioid analgesics.
Luke Burnett, KeraNetics, discussed regenerative medicine challenges (e.g., stove-piped technologies) in the context of conflict in 2035 and noted concerns about “over-hype” slowing progress in the field. He noted that there’s a long way to go but it is difficult to fund necessary testing of incremental solutions because the public thinks we have already solved these issues. He also addressed the larger worldwide market and considered the question, Are there short-term solutions to tissue regeneration that meet grant (academic) and investor (industry) timelines? After describing “functional fibrosis” results, Burnett proposed a similar stepwise approach where researchers set realistic expectations, address gaps (few clinical studies), and establish a crawl-walk-run clinical plan that includes industry collaborators. After describing Keratin, a bio-material that combines advantages of synthetic and biologic bio-materials, and showing muscle-defect pre-clinical test results, analyses, and commercialization considerations, he summarized his conclusions. He argued that future conflicts will likely require redefining prolonged field care and need new, far-forward solutions that can regenerate and repair soft-tissue wounds, volumetric muscle loss, and organ defects.
Jennifer Elisseeff, Johns Hopkins University, discussed rebuilding the wounded, today and tomorrow, with regenerative medicine. Given that tissue and organ loss remain a trauma challenge, she noted that clinical translation in tissue engineering is slow and often has disappointing results. On the current state of advanced repair, she illustrated transforming skin, tissue reconstruction, and transplant-tolerance immunotherapy. As to regenerative-medicine gaps, she asked, “What really matters in repair and what are therapeutically-relevant parameters?” She believes the near future could bring regenerative immunotherapies and inhibitory targets, including pain. Longer term, she looked to “liquid biopsy” for defining injury and personalized trauma care. Elisseeff moved on to numerous medical situations that could involve regeneration, such as muscle healing and repair, non-healing and healing cases, and pain. Her view of personalized trauma treatment in 2035 included a “picture” of injuries and possible trajectories of infection and treatment; a diagnostic of systemic “healing” state; a liquid biopsy of injury profile; injury-related pain treatment; and local-regional advanced manufacturing.
Future of Tissue Bioengineering Panel. Chris Dearth highlighted the prominence of extremity injuries and the leading role of DoD’s Extremity Trauma and Amputation Center of Excellence in mitigating, treating, and rehabilitating those injuries. Using examples of volumetric muscle loss and composite-tissue injuries, he presented opportunities for bioengineering, including a light but rugged battlefield exo-skeleton. He stated that future conflicts will likely result in prolonged field care of injured soldiers and tissue bioengineering technologies can play an active role within such care. Most available technologies are not yet able to be used in such environments; thus, consideration should be given to leveraging or re-purposing complementary commercially available technologies for DoD needs. Dearth noted that DoD’s medical system is ideally positioned to lead advocacy for materiel and knowledge advancements for treating traumatic extremity injuries within an austere environment, thereby increasing joint-force readiness.
Lisa Larkin, University of Michigan, after noting the prevalence of musculoskeletal conditions (over half of DoD disabilities), showed current tissue-engineering models. Focusing on volumetric muscle loss, she described experiments with rats and then larger animals (sheep) that could model tissue creations of the size
needed for humans. She also showed some promising results of nerve re-routing into muscle tissues. Areas for improvement, such as protecting grafts from fibrotic infiltration and scaling up enough cells to match human volumes, were also discussed. She listed the following time-phased opportunities for improvement: near-immediate, which could realize tissue foundry lines for mass production of cells and tissue; 5 years, which could realize continued product development and validation of tissue-engineering products for use in battle-removed combat-zone settings; and 15 years, which could realize “off-the-shelf” transportable tissues that aid in healing traumatic tissue damage.
Michael Yaszemski, Mayo Clinic, Tissue Engineering and Biomaterials Laboratory (via VTC), discussed biomaterials for regeneration. He first pointed out that research must begin with a clear description of an unmet medical need. The research question should be based on that need and constant interaction should occur among researchers, clinicians, regulatory, and industrial colleagues. Turning to musculoskeletal and neurologic tissue regeneration, he discussed current options, gaps, and novel regenerative treatment opportunities. He also addressed current options for bone regeneration, including bone-regeneration scaffolds—preformed, injectable, and moldable. Yaszemski also discussed the engineering of tendon, ligament, and cartilage tissue, skeletal muscle re-engineering, engineered skin and skin substitutes, nerve regeneration, electrically conductive scaffolds, first human use of a Mayo Nerve Tube, and spinal-cord regeneration. He summarized with two points: care close to the action with early return to duty in an austere area is likely to be possible and applicable for many injuries, but not all; and some injured personnel where transport to another location will remain essential (e.g., an 80 percent burn). He noted that an opportunity exists to identify injuries that are amenable to austere-environment care and those that are not.
Panel Discussion of Bioengineering the Future Panel. Christ moderated this panel on the future of bioengineering. An early question during the panel concerned the current Centers of Excellence with a relatively low number of patients was, Can civilian patients be brought in, or should patients be sent elsewhere? Yaszemski’s answer was a combination of both, especially because veterans can now go to civilian institutions for specialized care. Another question involved tissue sources in far-forward settings, where there could be many instant deaths, and possibilities of using some of that tissue. Larkin referred to current work with plastic surgery to obtain the discarded tissues and bring them back to a laboratory and obtain cells (which is difficult), but sterile movement from a battlefield environment back to an area for generating tissues would be limited. Christ asked the panelists if there are any unsolved scientific challenges. Burnett responded to this with the challenge of scalability, in both cell and material space. Many technologies start off with rat models and micro-liter scales, but for large animals, making kilos becomes a challenge. Elisseeff thought another issue is the gap between large-animal models and people. Returning to surgical discards, she believed they represent a cautious opportunity for sensors and technology to improve our understanding of human versus large-animal differences. Christy suggested that, eventually (after clinics), tissues could be capable of being pushed forward for battlefield use. Larkin agreed with the scalability challenge but emphasized the need to diminish fibrotic response. Christ identified short-term applications where materials can be scaled easier than tissues to provide functions—for example, fill voids temporarily, maybe promote healing, provide antibiotics, wrap a leg, and brace an arm or leg. Elisseeff agreed and added that automated manufacturing could enable scale up and delivery.
A participant asked a question about the role of exoskeletons. Burnett said that the challenge there is combining different technologies necessary for such systems to work, for which it is necessary to plan a regulatory and clinical pathway to get through the development process quickly, not 15 years and hundreds of millions of dollars later. Elisseeff added that the tendency is to put off healing to preserve for later repair that could have negative consequences because fibrosis causes chronic inflammation and pain. Christy thought it may end up being a two-step process where exoskeletons are used on the battlefield to keep soldiers mobile until they can get to a facility where they can benefit from some of the cellular therapies.
Christ asked panelists what areas they would suggest now for advanced R&D dollars, based on quick field use or even longer term, and how that money would be invested in knowing resources are limited. Burnett said there are clinical studies for void fillers using developed, cheap, and fast material systems. He noted that clinical experience will provide market opportunities that will expand into other desirable areas. Larkin echoed clinical studies, observing that it is expensive to get even four or five grafts implanted into large animals, let alone humans. She followed by noting that scalability is a huge problem because it will be necessary to deliver thousands of these. Elisseeff suggested looking at new targets for regeneration. She thought clinical studies show potential new targets that might be easier to hit, and significant heterogeneity raises the opportunity to detect and address it. Christy suggested pain management and being able to get things manufactured as fast as possible to the quality needed for regeneration. Yaszemski concluded with a long state-
ment, summarized as follows: To improve many lives, there are ways to treat hemorrhage (including internal hemorrhage), easy applications for cartilage fracture, etc. That type of capability and some of what Eastridge discussed are being worked on to make them easy to apply and be effective. “We lose a lot of lives that do not need to be lost if we can stop internal and external hemorrhage in a good operating field.”
DAY 3, PART III. FINAL THOUGHTS AND WRAP UP
This session focused on key takeaways to maximize warfighters’ ability to accomplish their mission and, if injured, survive and return quickly to function. Five major themes were covered.
Theme 1. Several participants believed that only this top level of leadership can instill this culture. Kotwal believed that line organizations do not consistently consider combat trauma care and combat medical care (CTC-CMC) employment as part of their direct responsibilities and ownership.
Theme 2. Several participants believed that the impact and efficacy of R&D efforts to prepare for 2035 will be diminished without top leadership addressing the many identified gaps. Kotwal added that without this level of leadership commitment, little can be expected to change.
Theme 3. Several participants supported two top-leader-oriented challenges, which Bagian synthesized as follows: (1) military commanders should view CTC-CMC as a core responsibility to assure preparedness, then results would likely improve, as demonstrated by special operations units and conventional forces using this approach; and (2) military commanders should ensure that CTC-CMC assets are trained, equipped, and manned, and held accountable to the same standards of excellence demanded of other support assets (intel, logistics, etc.).
Several participants’ comments evidenced the strong belief that the highest levels of Pentagon leadership need to recognize CTC-CMC as a fundamental requirement to preserve combat power. They can then create a chain of responsibility, a culture of accountability, and address the moral imperative. Bagian emphasized that committed leadership is essential to ensure the necessary scale in effort and resource allocation; communications; enforcement of policies and processes; and efforts to effectively address the gaps in data collection and documentation related to CTC; training standardization and modernization for practitioners; talent management; standards of care; and R&D.
Theme 4. Several participants could identify with some of the R&D items discussed, and many participants identified with multiple R&D categories, especially bio-materials.
Bagian’s remarks identified the following crosscutting gaps:
- R&D leadership and some researchers not focused on getting individuals back into the fight;
- Not recognizing advantages of sensors on an individual;
- Not accepting the fact that tactics, techniques, and technologies act as force multipliers;
- The success of improvement initiatives (R&D or otherwise) depend on commander acceptance;
- An inadequate link between casualty data and protection-systems design and optimization, especially for protection-system R&D (Kotwal emphasized making sure data can be used functionally); and
- A need for more operationally relevant metrics and data to support R&D and other improvements (Kotwal emphasized that to get that data, commanders need to reinforce its collection importance).
Bagian also noted that bio-materials R&D also needs more clinical trials, materials, and ability to scale from laboratory-sized results to human-sized results; also needed is more R&D on pain management, infection control, tissue interfaces, and ability to retain form and function. Christ stressed the importance of trying these technologies in clinical trials on bio-materials, as they are relatively “low-hanging fruit.” He also said that scale is important for both price and practicality, and he re-emphasized pain management, possibly doing some of that work in connection with bio-materials R&D. On tissue R&D, Christ said, “You can make an individual tissue, but if you don’t connect it to the ones around it’s not going to perform at a high level. . . . you can’t move a joint unless it’s attached to a bone.”
Millonig raised a question to the panelists: In what areas must government lead because the commercial sector will not provide support due to lack of a business case? Christ pointed to technology-development
resources as an area where the government can provide more leadership. Bagian, followed by others, mentioned regulatory inertia as a challenge to commercial sector activity in the field. He emphasized that the need for reforms and noted that they will not happen without sustained leadership attention. A risk-adverse culture in government was also highlighted by the panelists as a challenge. Bienvenue mentioned the following key areas in which the government could assist the commercial sector: difficulties with the translation from research to development and production, the challenges in funding that gap between researchers and developers, and the difficulty in providing requirements to researchers ahead of time. Several participants agreed that tightening the link between research, acquisition, and operational use was essential to improve progress in this area.
Kotwal focused on primary, secondary, and tertiary prevention. The first was on funding human performance to make and keep the human, the most valuable weapon system, truly effective. Second was preventing and mitigating injuries with helmets, body armor, and vehicle armor—all need to progress commensurate with the threat and in step with each other. The third prevention would be care, for which Eastridge emphasized hemorrhage control and blood; and so research needs to address shelf-stable solutions where any can be used in the field to control hemorrhage—for limbs and junctional areas as well as topical regions. Kotwal also stated the need for some type of equivalent blood replacement that is preferably shelf-stable, that can be used in a pre-hospital setting, such as by a non-medical first responder.
Margaret Moore, Louisiana State University, discussed resources required for training, standardization, and validation of teams providing CTC-CMC using military and civilian partnerships, both to generate the volume of relevant clinical experience, as well as the synthetic training environments needed to prepare for future operational scenarios. Howard Champion stressed the need to get clear capability requirements written and distributed, for without them, acquiring funding will be very difficult. In addition, he urged investment for technology-assisted training (moving capabilities in military non-medical training environments to military medical training environments) and attention to developing triage guidelines and operational decision support for prolonged field care. Carolina Cruz-Neira, University of Arkansas, Little Rock, offered an umbrella comment. The government, strongly and urgently, has to create a culture where preserving the human in the battle is the most important weapon, tool, and asset. Optimization is needed so that those humans are healthy and prepared to the level they need to be. “If we think about a machine,” we have the infrastructure and training in place so that a machine can be repaired on time and ready to function.
On medical simulation, Dan Irizarry suggested an explosion in civilian hospitals’ use of medical simulation. Therefore, he said, the government should lead development of a combat-focused simulation capability. Daigle believed the government would have to research operationally relevant human-performance optimization issues.
Theme 5. Several participants believed that several, if not all, of these gaps could be addressed in the near term without waiting for longer-term R&D, assuming there would be a mandate and funding to do so. Referring to previous other studies, such as A National Trauma Care System,7 which highlighted some of these issues, and to the TCCC successes driven by small but dedicated groups in the past, Bagian hoped that consistent top leadership action would be taken. That hope appeared to be shared by several participants.
Finally, Bagian offered a collection of workshop-generated thoughts that included the following:
- Not personalizing human weapon system performance improvement, including individual care and nutrition;
- Not scaling training for 2035 casualty possibilities;
- Lack of command ownership of health promotion and protection activities;
- Lack of tailoring medical care to match the individual warfighter, unit, culture, and mission;
- Current stovepipes in the seven fitness domains (“silos of excellence”), inhibiting integration of all domains;
- Inability to field and improve technologies that have already been developed; and
- Not integrating military medical activities into the synthetic training environment and utilizing data and state-of-art engineering knowledge used elsewhere in DoD to personalize training.
___________________
7 National Academies of Sciences, Engineering, and Medicine, 2016, A National Trauma Care System.
DISCLAIMER: This Proceedings of a Workshop—In Brief has been prepared by Norman Haller as a factual summary of what occurred at the meeting. He was assisted by staff members Steven Darbes and Sarah Juckett. The committee’s role was limited to planning the event. The statements made are those of the individual workshop participants and do not necessarily represent the views of all participants, the planning committee, or the National Academies. This Proceedings of a Workshop—In Brief was reviewed in draft form by Warren Dorlac, University of Colorado; Joan Bienvenue, University of Virginia; and Cherie Chauvin, Naval Studies Board, National Academies of Sciences, Engineering, and Medicine, to ensure that it meets institutional standards for quality and objectivity. The review comments and draft manuscript remain confidential to protect the integrity of the process.
PLANNING COMMITTEE: James Bagian (NAE), University of Michigan; Joan Bienvenue, University of Virginia; Howard Champion, SimQuest; George Christ, University of Virginia; Carolina Cruz-Neira, University of Arkansas, Little Rock; Russ Kotwal, Joint Trauma System, Defense Health Agency; Margaret Moore, Louisiana State University Health Science Center
RAPPORTEUR: Norman Haller
STAFF: William Millonig, Acting Director; Sarah Juckett, Program Officer; Steven Darbes, Program Officer; Aanika Senn; Program Coordinator, Cameron Malcom; Senior Program Assistant
SPONSORS: This workshop was supported by the Department of the Army.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2020. Army Combat Trauma Care in 2035: Proceedings of a Workshop—in Brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/25724.
Division on Engineering and Physical Sciences

Copyright 2020 by the National Academy of Sciences. All rights reserved.












