Proceedings of a Workshop
INTRODUCTION1
The United States faces a significantly aging population as well as a growing share of the population that is living longer with multiple chronic conditions. To provide high-quality care to people of all ages living with serious illness, it is critical that the nation develop an adequately trained and prepared workforce consisting of a range of professionals, including physicians, nurses, social workers, direct care workers, and chaplains. As noted by James Tulsky, chair of the Department of Psychosocial Oncology and Palliative Care at the Dana-Farber Cancer Institute, chief and professor of the Division of Palliative Medicine at Brigham and Women’s Hospital, and professor of medicine and co-director of the Center for Palliative Care at Harvard Medical School, “for those of us who actually lead [serious illness care] programs, we know how difficult it is, and we struggle with this workforce issue.”
To explore some of the key workforce-related challenges to meeting the needs of people with serious illness, the Roundtable on Quality Care
___________________
1 The planning committee’s role was limited to planning the workshop, and the Proceedings of a Workshop was prepared by the rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants and are not necessarily endorsed or verified by the National Academies of Sciences, Engineering, and Medicine, and they should not be construed as reflecting any group consensus.
for People with Serious Illness of the National Academies of Sciences, Engineering, and Medicine (the National Academies) hosted a workshop in Washington, DC, on November 7, 2019. The Roundtable on Quality Care for People with Serious Illness serves to convene stakeholders from government, academia, industry, professional associations, nonprofit advocacy groups, and philanthropies. Inspired by and expanding on the work of the 2015 Institute of Medicine (IOM) consensus study report Dying in America: Improving Quality and Honoring Individual Preferences Near the End of Life (IOM, 2015), the roundtable aims to foster ongoing dialogue about crucial policy and research issues to accelerate and sustain progress in care for people of all ages experiencing serious illness.
This workshop, Building the Workforce We Need to Care for People with Serious Illness, unfolded over five sessions. The opening session provided context with an overview of the current state of the workforce for serious illness care and projections of future workforce needs. The second session focused on developing a workforce that specializes in care for people with serious illness, and speakers addressed different approaches to developing that workforce, including specialty training in geriatrics and palliative care, university-based certificate programs, and integrating interprofessional palliative care education into the undergraduate curriculum, particularly in the field of social work.
The workshop’s third session focused on efforts to prepare all health care professionals, not just those specializing in palliative care, to care for people with serious illness. Speakers addressed the gap between what health care professionals are trained to do and what they actually need to do in their daily practices and discussed several approaches to closing that gap. The fourth session took up the topic of developing the workforce for providing community-based care for those with serious illness, with speakers discussing who is included in community-based care, what their specific roles are, and where opportunities exist to expand that workforce and the capabilities of those who provide community-based care. The workshop’s final session focused on the use of interprofessional teams to effectively care for people with serious illness.
In her introductory remarks, Brynn Bowman, vice president of education at the Center to Advance Palliative Care (CAPC) and co-chair of the workshop planning committee, recounted two personal stories that highlighted the importance of developing the workforce to care for people with serious illness. The first involved a discussion she had with the leader of the small palliative care program at the hospital where her grandmother
was being treated for brain cancer, who told her that while the budget was available to recruit more providers to the team, they could not find anyone willing to move to that area of the country. “She freely admitted that her team was not able to see all of the patients who could have benefited from her care,” recalled Bowman.
Several weeks later, Bowman’s aunt fell ill suddenly and died in the hospital. As her aunt was being treated in the intensive care unit, Bowman asked the care team if she could organize a family meeting to talk about her aunt’s care and treatment preferences. “I could see the anxiety and hear it in the voices of her care team, not because they did not care about my Aunt Marilyn or because they did not think that having that conversation was important, but because they did not know how to approach it. I could see that they had not had training and the skills needed to have a discussion with my aunt about what really mattered to her,” recounted Bowman. As a result, her aunt’s family and care team both had trouble navigating difficult decisions during her aunt’s last week of life.
Bowman noted that the workforce represents the critical point at which the system and its policies affect patient care and patient interactions. She added that the workforce issue has many components, and given time constraints, the workshop would not include presentations on issues related to payment and reimbursement of interdisciplinary team members nor the use of family and other unpaid caregivers. While acknowledging that both topics are incredibly important, she noted that they were beyond the scope of this 1-day workshop.
Bowman reminded workshop participants that in October 2018, the National Consensus Project (NCP) published a fourth edition of its clinical practice guidelines2 for quality palliative care that explicitly outlined what quality palliative care in community care settings should include and how nonspecialty programs and practices can align care of their seriously ill patients with the guidelines. Bowman pointed out that the fourth edition also acknowledges that not every care setting will have a specialty palliative care team and outlines how nonspecialty programs can use these guidelines to improve the quality of care.
Brenda Nevidjon, chief executive officer (CEO) of the Oncology Nursing Society and co-chair of the workshop planning committee, shared that this workshop was dedicated to the memory of Ruth McCorkle (see
___________________
2 For more information, see https://www.nationalcoalitionhpc.org/ncp (accessed February 24, 2020).
Appendix A). Nevidjon noted that McCorkle’s contributions to shaping the field cannot be overstated, and her legacy extends far beyond her direct impact on the 70 doctoral and 30 postdoctoral students that she mentored during her career. Nevidjon added that McCorkle was also one of the earliest nurses inducted into the National Academy of Medicine.
In her opening comments of the workshop, Nevidjon recalled her personal experiences of the deaths of her mother and mother-in-law. In her opinion, her mother had received quality care for her illnesses for more than a decade and, as a result, died “a good death,” while her mother-in-law did not have the same quality care for her illnesses and thus did not have a good death. She noted that some of the differences in these experiences may be attributable to workforce issues.
This Proceedings of a Workshop summarizes the presentations and discussions that took place over the course of the day-long workshop. A broad range of views were presented. Box 1 provides a summary of individual workshop participants’ suggestions for potential actions. The Statement of Task and the workshop agenda are in Appendixes B and C, respectively. The speakers’ presentations (as PDF and video files) are archived online.3
OVERVIEW OF THE CURRENT STATE OF THE WORKFORCE FOR SERIOUS ILLNESS CARE AND FUTURE NEEDS
The United States will mark an important demographic turning point in 2030: all members of the baby boomer generation will be over 65, and older individuals will outnumber children in the United States for the first time in history (U.S. Census Bureau, 2019). This demographic shift, explained Michelle Washko, director of the National Center for Health Workforce Analysis (NCHWA) at the Health Resources and Services Administration (HRSA), will have “massive implications” for the U.S. health care system because individuals over 65 are disproportionately represented in the highest tiers of health care spending, while those over 85 have the highest per capita use of health services (IOM, 2008).
To provide a broader contextual perspective, Washko shared four high-level priorities of the Department of Health and Human Services (HHS): combating the opioid crisis, shifting to value-based care, health insurance reform, and drug pricing.
___________________
3 For more information, see http://nationalacademies.org/hmd/Activities/HealthServices/QualityCareforSeriousIllnessRoundtable/2019-NOV-07.aspx (accessed February 28, 2020).
In addition, she said, HHS is focusing on building and training the workforce to truly understand and address the social determinants of health and to achieve health equity. “This is something that those of us who have worked in the areas of aging, disability, and serious and chronic illness have been shouting about for a long time,” explained Washko.
Noting that individuals with serious illness tend to use more health care services, Washko pointed out that the sufficiency, distribution, and quality of the health care workforce that cares for those individuals are increasingly important components of improving the overall health of the population. Washko expanded on those four important issues:
- Sufficiency: Is there equilibrium in the supply of and demand for health workers, or are there occupations with shortages or oversupplies?
- Distribution: Are occupations distributed evenly in all geographic areas, so as to ensure access to health care for the entire U.S. population?
- Quality: Is the health workforce well trained in evidence-based practices that result in better care? Which occupations provide what services, and who else can provide that kind of care?
- Data: How do we improve the evidence base within a disparate health care system?
Washko explained that workforce insufficiency and maldistribution issues significantly complicate the health care landscape because they can immediately constrain access to essential care and treatment for millions of individuals. “In other words, one can argue that if a consumer does not have physical or virtual access to a particular type of health care provider, they do not have access to the type of care that person offers,” said Washko.
Washko explained that a key challenge to understanding whether the U.S. workforce is sufficient to meet the needs of those with serious illness is that the workforce comprises a diverse group of clinical and support occupations, and there is no current consensus on precisely which occupations constitute the workforce for those with serious illness. For example, occupations such as long-term and palliative care providers are often considered to be the backbone of that workforce. However, individuals with serious illness are also heavy users of services from many different health care professionals. “Thus, I would posit that any health care or health support occupation should be considered a part of the workforce treating those with serious ill-
ness,” said Washko. Even if the U.S. workforce as a whole were sufficient to effectively care for everyone with serious illness, she noted, maldistribution would still be a major issue.
In terms of quality, Washko emphasized that it is important for the nation to push for continual improvement in workforce quality by encouraging the development of cutting-edge curricula, training in various specialty settings, and unique treatments for special populations. To that end, she said, building, redistributing, and reshaping the health care workforce must be aligned with other efforts to address social determinants of health and improve overall delivery of services to individuals, including those with serious illness. “Further, we must move toward improved coordination and interprofessional training and teams,” she added.
Understanding and being able to address these issues starts with an evidence base, but, as Washko explained, data on the U.S. health care workforce are “good, but not great.” The lack of sufficiently informative data, she explained, is a symptom of a disparate health care system in which, for example, many occupations are licensed at the state level and others are not licensed at all. To remedy this data shortage, the Patient Protection and Affordable Care Act created NCHWA4 and mandated that it develop projections for health care occupations. Washko explained that NCHWA has developed a health workforce simulation model that estimates current-day supply and demand of a specific occupation and offers projections for the next 15 years.
To date, this model has generated workforce projections for primary care, nursing, internal medicine subspecialties, surgical specialties, women’s health, long-term services and supports, oral health, and behavioral health. These projections reveal that there will be shortages for the majority of these occupations if there are no shifts in use over the next 15 years, with the aging population being the major driver. If anything, said Washko, indicators suggest that there will be greater use of health services over the next 15 years, which means demand will likely be even higher than the model forecasts.
One exercise NCHWA staff conducted was to model a number of “what-if scenarios,” such as the demand if the nation were able to improve population health in certain domains that allowed people to age in a more healthy way or if access to services improved for those segments of the population that experience health disparities. While these types of intellectual
___________________
4 For more information, see https://bhw.hrsa.gov/national-center-health-workforce-analysis (accessed April 3, 2020).
exercises are important, Washko acknowledged that they are substantially weaker foundations on which to build programs and implement policy. She said that NCHWA has several ongoing initiatives to generate foundational data, including the National Sample Survey of Registered Nurses and the National Health Workforce Accounts5 program that reports information on the U.S. health workforce to the World Health Organization.
In conclusion, Washko stressed that the nation’s health care and health support workforces are evolving in size, location, and other dimensions, such as quality, which is a trend seen globally. She also noted that research on the health care and health support workforces in the context of a complex changing health care system is continuing to expand, which requires that data on these workforces must improve in order to provide meaningful information about specific occupations, measure outcomes, and gain increasingly granular levels of understanding about the workforce.
DEVELOPING THE WORKFORCE TO SPECIALIZE IN CARE FOR PEOPLE WITH SERIOUS ILLNESS
Karen Bullock, professor and head of the Department of Social Work at North Carolina State University, opened the first session of the workshop. Referring to Washko’s presentation, she noted that there is clearly a need for a well-prepared, well-credentialed, culturally competent workforce to meet the needs of seriously ill patients. Bullock added that the speakers from the workshop’s first session will build on Washko’s presentation and address policy priorities to address the misdistribution of the workforce and improve the quality of care.
Projections for the Palliative Care Specialty Workforce
Arif Kamal, associate professor of medicine, population health sciences, and business administration at Duke University, began his presentation by noting that he would focus on two specialties: specialty palliative care and geriatric medicine and gerontology. Referring back to the NCP clinical practice guidelines, noted by Bowman, Kamal explained that though this framework was established in the late 1990s, the eight domains of quality care have essentially remained the same. Based on his experience, Kamal
___________________
5 For more information, see https://bhw.hrsa.gov/health-workforce-analysis/data/national-sample-survey-registered-nurses (accessed March 5, 2020).
emphasized that addressing the psychosocial and cultural aspects of care is critically important to providing quality care to those facing serious illness.
Kamal described the integration of specialty palliative care as a funnel, in which palliative care specialists can serve as stewards and educators across the health system to help primary care clinicians provide foundational palliative care, while these specialists also provide additional support as a patient’s needs become more complex (see Figure 1). He added that, historically, palliative care grew out of the hospice movement and was heavily focused on prognosis and stage of disease. Now, he said, the field is shifting the focus to the complexities of treating patients and their unmet needs in an effort to better understand the services they should receive.
Kamal pointed out that specialist palliative care clinicians have the opportunity to be agents of change in the health system but cannot do it alone. He suggested considering “any person that touches a patient with serious illness as part of the palliative care team and engaging their skills and expertise to care for the patient.” Doing so would acknowledge that all of these individuals should be provided training so they have the skills, expertise, and interest to broaden the care team and the care for patients in many ways, regardless of geographic location.
Kamal added that it is important to embrace a champion of palliative care, even if that individual has not yet completed additional training. In
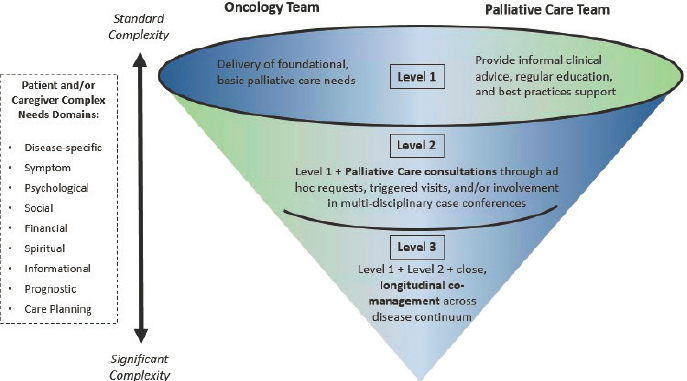
SOURCES: As presented by Arif Kamal, November 7, 2019; adapted from Kaufmann and Kamal, 2017.
Kamal’s view, nurses and nurses’ aides, who are likely to spend more time with a patient than the palliative care specialist is, would be ideal candidates to receive more training. So too would be a hospitalist who may not have the time to take part in a full fellowship in palliative care but who, with some training, could serve as the champion for advance care planning for every patient on their ward. “What we do not want to say is, ‘you are not a specialist palliative care person, you did not do fellowship training, so let us handle this work,’” said Kamal. “What we want to say is, let us embrace that person who has that interest and potentially wants to gain some further expertise and bring them into the fold.” These champions can provide a deeper understanding of the conversations with patients and caregivers, particularly for practices that cannot fully staff the interdisciplinary model put forward in the NCP clinical practice guidelines. Kamal added that such a network could also allow palliative care teams to connect with one another and create a community of learners that could advance the entire field.
Kamal highlighted the results of a recent survey of 3,000 individuals in the palliative care specialty workforce and associated workforce projections (Kamal et al., 2019). Modeling the impact of two policy changes—one that would increase palliative care fellowships by 25 per year for the next 10 years and one that would focus on reducing physician burnout—Kamal and his colleagues found that increasing the number of fellowships available would have what he characterized as a dramatic effect on increasing the number of palliative care specialists over the next 40 years (Kamal et al., 2019) (see Figure 2).
Kamal noted, however, that the study also found that there is likely to be a reduction in palliative care specialists over the next 15 years, regardless of the steps taken today, as a result of retirements from a workforce whose current average age is 56. Kamal explained that this reduction will increase the ratio of eligible Medicare patients per palliative care specialist from approximately 800:1 today to 1,400:1 in the next 15 years (see Figure 3). According to Kamal, meeting the needs of the Medicare and non-Medicare population eligible for palliative care would require every palliative care specialist to visit with 46 patients per day. “That is frankly impossible to do and maintain quality and value,” he said.
Kamal ended his remarks by identifying several policy changes to expand the total palliative care workforce. The first was to support passage of the Palliative Care and Hospice Education and Training Act (PCHETA).6
___________________
6 For more information, see https://csupalliativecare.org/pcheta-2018 (accessed February 28, 2020).
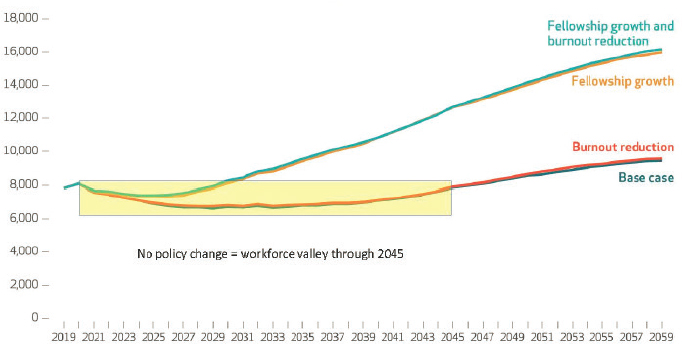
SOURCES: As presented by Arif Kamal, November 7, 2019; Kamal et al., 2019; published by Project HOPE/Health Affairs as Kamal, Arif H., Steven P. Wolf, Jesse Troy, Victoria Leff, Constance Dahlin, Joseph D. Rotella, George Handzo, Phillip E. Rodgers, and Evan R. Myers. “Policy changes key to promoting sustainability and growth of the specialty palliative care workforce.” Health Affairs (Millwood). 2019, vol. 38, no. 6: 910–918. The published article is archived and available online at www.healthaffairs.org.
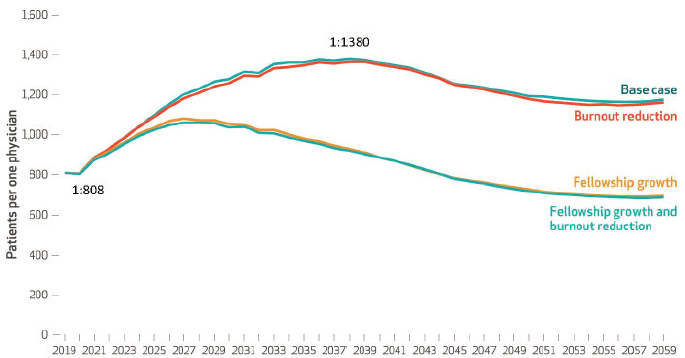
SOURCES: As presented by Arif Kamal, November 7, 2019; Kamal et al., 2019; published by Project HOPE/Health Affairs as Kamal, Arif H., Steven P. Wolf, Jesse Troy, Victoria Leff, Constance Dahlin, Joseph D. Rotella, George Handzo, Phillip E. Rodgers, and Evan R. Myers. “Policy changes key to promoting sustainability and growth of the specialty palliative care workforce.” Health Affairs (Millwood). 2019, vol. 38, no. 6: 910–918. The published article is archived and available online at www.healthaffairs.org.
Second, he stressed the importance of expanding advanced training opportunities that do not involve fellowships as a means of including and embracing all the members of the interdisciplinary team. Third, he pointed to the need for further research on the specialty palliative care workforce. Fourth, he called for reimbursement for team-based care, which he noted involves embracing and recognizing the hard work done by non-billable health care providers in palliative care. Finally, he suggested actions to prevent the increasingly serious problem of clinician burnout (NASEM, 2019b).
University-Based Certificate Programs
One important specialty palliative care pipeline comprises the more than two dozen university-based certificate programs in palliative care, explained Jennifer Moore Ballentine, executive director of The California State University (CSU) Shiley Institute for Palliative Care. Recognizing that there is often confusion between certificate and certification programs, Ballentine began her remarks by differentiating the two (see Table 1).
To put university-based certificate programs in context, Ballentine explained that there are currently 157 sites offering 403 physician fellowships7 in palliative care, approximately 12 sites and 15 slots for advanced practice registered nurse (APRN) fellowships,8 and 5 sites offering social work fellowships in palliative care. She pointed out that the University of Maryland and the University of Colorado Denver recently created interprofessional master’s degree programs in palliative care.
Ballentine explained that nearly all university-based certificate programs confer academic credit rather than continuing education credits or hours, and they charge academic tuition. Most enroll one cohort per year of 6–30 students, and almost all require students to apply to the relevant nursing, social work, or graduate schools. She pointed out that The CSU Shiley Institute’s comprehensive certificate programs for registered nurses (RNs), APRNs, chaplains, and social workers with their master of social work (M.S.W.) are offered several times each year and confer continuing education credits at a lower price point without requiring graduate admis-
___________________
7 For more information, see https://apps.acgme.org/ads/Public (accessed April 6, 2020).
8 For more information, see https://www.mjhspalliativeinstitute.org/fellowships; https://www.nursepractitionerschools.com/blog/np-fellowship-residency-programs; https://www.graduatenursingedu.org/nurse-practitioner-residency-programs; and https://advancingexpertcare.org/HPNAweb/Palliative_Care_APRN_Fellowship.aspx (all accessed April 6, 2020).
TABLE 1 Differences Between Certificate Programs and Certification
| Certificate Programs | Certification |
|---|---|
|
|
SOURCE: As presented by Jennifer Moore Ballentine, November 7, 2019.
sion; most social work programs offer continuing education credits rather than academic credits. Most certificate programs are accessible to people not otherwise enrolled in a university and are either online or include online modules plus an in-person component.
Each program, said Ballentine, has special features based on specific goals and perceived needs. For example, the University of Washington’s interprofessional program emphasizes palliative care program design along with communication, while Smith College’s social work certificate features months of mentorship and advisement. The CSU Shiley Institute’s APRN certificate, which emphasizes real-world skills and nurturing nurse leaders, can be completed in 9 months. At least two organizations offer certificate programs for chaplains, and The CSU Shiley Institute offers two certificate programs in pediatric specialty care. Only one program, the University of Iowa, offers a certificate program in palliative care for pharmacists as part of its Pharm.D. program.
In talking with the leaders of some of these programs, Ballentine identified a number of key challenges and barriers, including enrolling adequate numbers of students to meet revenue goals. “A number of these programs were launched with support from grants or donations and are now facing challenges in sustainability,” she noted. A few, in fact, were on hiatus because of low enrollment, while other programs had long waiting lists. She also heard about the challenges of balancing the costs to students, enrollment goals, flexibility, and depth of content. “Everyone agrees that palliative care is an interprofessional, interpersonal practice with a strong emphasis on soft skills in addition to scientific rigor, but adding an in-person or clinical component to the educational programs significantly increases cost and inconvenience,” said Ballentine. She added that the interprofessional programs all struggle with attracting professionals beyond nurses and physicians. Measuring impact and outcomes is also a challenge for any professional educational program, she added.
Ballentine called out several policy recommendations that have been made in the past and that either have led to action, such as the establishment and growth of certificate programs, or need to be promoted further:
- Establish education, clinical training, certifications, and licensure requirements for palliative care specialty.
- Emphasize pain, symptom management, communication, and interprofessional collaboration.
- Create opportunities for training throughout career for all clinicians.
- Increase undergraduate and graduate content on serious illness/end-of-life care.
- Increase the number of specialty training opportunities, such as fellowships and residencies.
Additionally, she noted that some see the need for a consensus process to establish minimum characteristics and content of university-based certificate programs. In fact, she noted, one program director told her that a small consortium of faculty program directors has undertaken a Delphi process to identify required and recommended characteristics of interprofessional palliative care programs (Donesky et al., 2020). Others note that different students will have different needs, so it will be important to preserve variety across programs.
Ballentine said it would be beneficial to have some consistency and standardization for continuing education and continuing medical education requirements for all disciplines across states and to include specific requirements for palliative care skills among them. She explained that only 2 states have specific continuing education requirements in palliative care–related skills for nurses,9 and only 12 states have such requirements for physicians.10 Ballentine also called for undergraduate curricula to contain significant palliative care and serious illness care content for all health professions. Toward that end, The CSU Shiley Institute created a faculty toolkit11 for palliative care curriculum integration.
___________________
9 For more information, see https://www.aaaceus.com/state_nursing_requirements.asp (accessed April 6, 2020).
10 For more information, see https://www.boardvitals.com/blog/cme-requirements-by-state (accessed April 6, 2020).
11 For more information, see https://csupalliativecare.org/programs (accessed February 28, 2020).
Ballentine highlighted other important steps to address workforce shortages:
- Expand and standardize the scope of practice for APRNs and physician assistants (PAs) to fill physician shortages, especially in rural areas.
- Funders: Prioritize curriculum development, training programs, and clinical placements with solid outcome expectations.
- Health care delivery organizations: Commit resources to ongoing education and training in palliative care aligned to organizational goals.
In closing Ballentine echoed Kamal’s call to action, and encouraged passing and implementing the PCHETA.
Interprofessional Palliative Education and Its Integration into Undergraduate Curricula
Barbara Head, professor of palliative care and medical education at the University of Louisville School of Medicine and associate professor at the Kent School of Social Work, began her remarks by emphasizing that “interprofessional education is much more than having students of various disciplines sitting together in a classroom listening to the same lecture and sharing the same assignments.” Rather, she added, interprofessional education occurs in a collaborative, interactive environment where students learn from and with each other, with the goal of developing knowledge, skills, and attitudes that result in interprofessional team behaviors and competence. Ideally, according to Head, interprofessional education is incorporated throughout the entire curriculum and integrated vertically, through early clinical experiences, and horizontally, by bringing disciplines and professions together (Buring et al., 2009).
Interprofessional education is important, she continued, because it can train health professionals to gain core competencies for interprofessional collaborative and patient-centered practice that can meet the quadruple aim of better outcomes for patients, improved patient experience, lower cost, and improved clinician experience. Such training is particularly important in palliative care, which by its nature requires the efforts of a team. “Palliative care practitioners should be experts on teamwork and collaboration,” said Head, adding that “we should lead the teaching of these skills and
standard setting for interprofessional education.” Head emphasized that “I cannot tell you how many of our students say that they had never considered palliative care as a career choice, but after they had observed palliative care clinicians and learned about the type of work that palliative care teams do, they are considering palliative care for their future career choice.”
Head noted that organizations such as the National Academies, the American Association of Colleges of Nursing (AACN), the World Health Organization, the American Association of Medical Colleges, and the Liaison Committee on Medical Education have all recognized the value of interprofessional education. “The earlier we teach future practitioners how to work in a team, the more competent they will be when they enter the workforce,” observed Head. “Unfortunately, students of the health care professions are most often taught in academic silos that are difficult to overcome.”
Head pointed out that there are many challenges to developing interprofessional education, including the following:
- Ensuring equal representation of different disciplines,
- Adding new components to already crowded curricula,
- Building curricula on best practices,
- Improving faculty expertise in interprofessional education,
- Managing the logistics of getting students from different disciplines together,
- Finding time for face-to-face learning activities,
- Ensuring comprehensive evaluation, and
- Ensuring sustainability.
Head described how she and her colleagues, with funding from a 5-year grant from the National Cancer Institute (NCI) and the participation of a committed faculty team, were able to develop and implement a mandatory, interdisciplinary palliative care oncology curriculum at the University of Louisville School of Medicine. The resulting Interdisciplinary Curriculum for Oncology Palliative Education (iCOPE12) program has now been in operation for 11 years and is considered a permanent part of the curriculum for medical, nursing, chaplaincy, and social work students. Head and her colleagues have also developed the InterProfessional Education eXchange
___________________
12 For more information, see www.icopeproject.org (accessed January 9, 2020).
(iPEX13) program as a national program to advance interprofessional education in cancer care. This program recruits eight faculty teams per year; the goal, said Head, is to train and mentor 160 faculty to lead interprofessional palliative care in oncology at 32–35 institutions and in so doing, create a national resource network for interprofessional education in palliative care.
Head and her colleagues, with support from the Gordon and Betty Moore Foundation, were able to conduct the first national survey (Head et al., 2019) of advanced hospice and palliative care social workers. Head explained that an advisory committee reviewed how the nearly 500 survey respondents rated a long list of job tasks in which specialty hospice and palliative care social workers engage, ending up with 140 job tasks that are specifically included in their work (Head et al., 2019). From that list, subject-matter experts who were trained in test item development established specifications for the certification exam. Some of the tasks rated with the highest importance included the following:
- Performing psychosocial assessment from a patient- or family-centered care perspective,
- Assessing patient’s and family’s coping skills,
- Providing emotional support and/or counseling,
- Conducting home visits,
- Maintaining professional boundaries,
- Identifying and reporting abuse and neglect (as mandated by law), and
- Adhering to requirements regarding confidentiality and release of information.
She noted that the survey respondents had an average of 16 years of work experience, suggesting a shortage of social workers at the younger end of the age spectrum. There was an equal representation of respondents from urban, suburban, and rural settings. The majority of respondents had a master’s degree and were female and white (Head et al., 2019). Head emphasized that diversity is an important issue to consider as we work to develop the workforce for serious illness care.
Informed by the survey, the National Association of Social Workers created a certification program in hospice and palliative care social work, and Head pointed out that a certification program is important because it
___________________
13 For more information, see https://www.ipexproject.org (accessed March 6, 2020).
requires verification of knowledge and competency based on passing an evidence-based exam that reflects the essential knowledge and skills required for specialty practice. Head noted that nursing and medicine have had specialty certification programs for more than 20 years and that certification can lead to recognizing the importance of a discipline’s practice (Head et al., 2019).
Head explained that certification as an advanced hospice and palliative care social worker requires passing the exam, 2 years of experience in palliative care over the preceding 5 years, licensure as required by the individual’s state, and a social work degree from a school accredited by the Council on Social Work Education. In addition, individuals must attest that they practice in accordance with the National Association of Social Workers Code of Ethics. While individuals with a bachelor’s degree in social work can gain certification, they are required to have 3 years of supervised post-degree experience. Head said that 420 social workers applied to take the certification exam in 2019, and 351 passed (Head et al., 2019).
In closing, Head expressed a hope that certification programs would help attract and retain social workers. She emphasized that certification validates the specialty of palliative and hospice social work and recognizes the social worker with advanced practice skills as an essential member of the team.
Panel Discussion
Following the session’s presentations, Bullock led off the panel discussion, noting the common themes that were presented around interprofessional education and training, as well as evidence-based approaches to care for people with serious illness. Bullock invited Laura Dingfield, assistant professor of clinical medicine, director of education in the Penn Palliative Care program, and program director of the Hospice and Palliative Medicine Fellowship at the University of Pennsylvania’s Perelman School of Medicine, to share information on a developing pilot program.14 Dingfield explained that the University of Pennsylvania created a pilot program aimed at mid-career faculty physicians seeking specialty training in hospice and palliative medicine. She pointed out that often, mid-career physicians cannot realistically or feasibly leave their practices to complete 12 months of full-time
___________________
14 For more information, see https://www.capc.org/blog/palliative-pulse-the-palliative-pulse-february-2019-addressing-a-workforce-crisis-innovation-training-for-hpm-specialists (accessed March 6, 2020).
fellowship training. Moreover, their expertise may make 12 months of training redundant. The goal of the program, Dingfield explained, is to decrease barriers to specialty education for mid-career physicians so as to allow them to continue their current professional practice while also pursuing part-time specialty training. She noted that the fellows can finish the coursework at their own pace, on a flexible, part-time basis. The program uses a competency-based framework with rigorous assessment of specialty-level competencies prior to graduation. Dingfield said she believes this program may address some of the issues in specialty workforce training related to sufficiency and maldistribution that Washko raised in her presentation.
Bullock then invited Denise Hess, executive director of the Supportive Care Coalition, representing the Association of Professional Chaplains, to provide an overview of the workforce issues facing professional health care chaplains. Hess noted that professional health care chaplains face the same workforce issues as the other fields involved in caring for those with serious illness. Chaplains, she explained, are trained and preferably board-certified health care professionals who help individuals use their own internal spiritual and emotional resources in service of their healing. Chaplains can also be a resource for improving the general well-being of the interdisciplinary team.
Hess identified two primary workforce issues. The first is the high level of variability in professionalism across an estimated 10,000 chaplains working in the United States. According to Hess, chaplains are one of the few health care professionals not required to be board certified. She explained that it is estimated that less than half of all chaplains are board certified by a nationally recognized certifying body. She called on employers to change that situation. “We need employers to write into the job descriptions a requirement for board-certified chaplains, either upon hire or within 2 years of hire,” she said.
Hess pointed out that two of the major chaplain-certifying bodies have introduced a specialty certification in hospice and palliative care, although according to Hess, fewer than 40 chaplains had received such certification at the time of the workshop. Hess acknowledged that chaplains have not had the same uptake of certification as their social services colleagues and, again, called on employers to require that chaplains have certification and, in so doing, drive the demand for it. “I do not think anyone on a professional interdisciplinary health care team would consider for a moment hiring an unlicensed or non-board-certified physician, advanced practice clinician, nurse, or social worker. We need to raise the industry standard so that it is the norm to hire board-certified and advanced and specialty certified chaplains,” she added.
The second main workforce issue, according to Hess, is that there is great underuse of chaplains in the serious illness workforce even though the NCP clinical practice guidelines clearly include the spiritual domain as an important component of serious illness care. That domain, she said, should be addressed by professional chaplains, yet the latest data from CAPC indicate that about 60 percent of interdisciplinary care teams are incomplete, with the chaplain being the team member most often missing.15 “Emphasizing the valuable role that chaplains play in caring for people with serious illness,” Hess noted: “We can do a great deal if we are allowed to practice at the top of our license.” In fact, she added, there is a growing research base indicating that chaplains can have a positive effect on outcomes that are important for reimbursement and that patients with serious illness want to talk about their spiritual, emotional, and existential needs with a chaplain (Balboni et al., 2010, 2011; Flannelly et al., 2012; Marin et al., 2015). “It is important to them,” said Hess. “They feel as if they are cared for as a whole person.” As an added benefit, chaplains can also help address burnout issues, mortal distress issues, and ethical dilemmas experienced by care team members, Hess pointed out. She reiterated the importance of raising the industry standard so that practices are expected to hire board-certified chaplains, just as they would be expected to hire licensed and board-certified physicians and nurses.
Bullock asked the panelists to expand on the challenges they face when caring for people with serious illness. Kamal remarked that the specialty field is relatively young, and one challenge is determining how often and at what time a patient needs to be seen by a palliative care team to produce a meaningful effect. Another challenge is defining minimum quality measures and measuring the distribution of implementation of such measures across the country for different practice settings. Kamal also pointed out that the field is learning as it grows, and he is encouraged by the steps taken to promote culture change through increased understanding of the social determinants of health. Washko commented that, because the field is growing so fast, it has been hard to develop the evidence base needed to answer some of the key policy and programmatic questions that would enable the field to identify the best way forward.
Another challenge, according to Dingfield, is that recruitment of the different professions into serious illness care is also not keeping up with the demand, nor is funding to pay for additional training. She explained that residency funding caps have not increased for physician training since the
___________________
15 For more information, see https://www.capc.org (accessed March 3, 2020).
Balanced Budget Act16 of 1997. This limits institutions’ abilities to expand traditional training programs. Dingfield concluded that change will likely require fundamentally rethinking ways to recruit the specialty workforce into educational programs for certification and board eligibility.
Audience Discussion
Tulsky began the audience discussion session by asking the panelists how to reduce redundancy among interprofessional teams where everyone is practicing to the top of their license. He explained that he often sees, for example, a nurse practitioner (NP) and a physician seeing the same patient at the same time or an NP and a physician working independently and filling the same role but being paid differently. Washko responded that research has begun to look at productivity and team composition to consider ways to restructure the roles of team members to extend, for example, the time a physician can use with a patient. She explained that the patient would receive the same amount and quality of care, but the team member responsible for delivering that care might shift.
Diane Meier, director of CAPC and vice chair and professor in the Icahn School of Medicine at Mount Sinai, pointed out that Dingfield’s program represents a radical change in the way that specialty education is delivered, in that the program is competency based with rigorous assessment rather than simply time based. Meier asked Washko if the workforce projections showed a physician shortage across all medical specialties or only within subspecialties. Washko responded that there is no extreme shortage or oversupply in any specialty, and she views the biggest issue as maldistribution. In her view, balancing the maldistribution of physicians with consideration of the quality and scope of practice concerns will help minimize the issues created by an insufficient workforce. Amy Berman, senior program officer at The John A. Hartford Foundation, noted that the presentations lacked reference to data on the nursing profession. In 2018, the Hospice and Palliative Credentialing Center, in partnership with the Hospice and Palliative Nurses Association, approved more than 3,600 new certifications and recertifications in addition to the 18,000 health care professionals currently certified in specialty hospice and palliative care.17
___________________
16 For more information, see https://www.congress.gov/bill/105th-congress/housebill/2015/text/enr (accessed March 3, 2020).
17 For more information, see https://advancingexpertcare.org/annual-reports (accessed March 6, 2020).
Responding to Nevidjon’s question about reliable data that would be needed to influence policy change for workforce distribution, adequacy, and competency, Washko noted that there are many emerging and unrecognized occupations. She explained that including an occupation on a census survey means it can then be classified with the federal government and begin to be considered in funding decisions. However, Washko added that even with well-categorized occupations like physicians or surgeons, the data sources are often different and therefore still only produce estimates.
Darci Graves from the Centers for Medicare & Medicaid Services (CMS) noted that when she was a medical school faculty member two decades ago, she found that chaplains, in addition to the spiritual care they provide, were able to help facilitate the communication skills of medical students. “We had experiential exercises where students had to leave their white coats at home and were able to shadow chaplains in the hospitals on their rounds and see them engage with patients in a nonclinical way, and they learned from hearing that more holistic story,” she explained. Kamal, who was one of Graves’s students then, said that particular training had a lifelong impact on how he interacts with patients. Several other workshop attendees voiced their support for the valuable role that chaplains play in serious illness care.
Phillip Rodgers, director of the Adult Palliative Medicine Program at the University of Michigan and representative of the American Academy of Hospice and Palliative Medicine, noted that the field could use a set of standards for interprofessional education and certifying interprofessional education teams and perhaps even a separate accrediting body for interprofessional, competency-based education. Head agreed that setting these kinds of standards would be important for the field. She added that the Interprofessional Education Collaborative program has set standards for interprofessional education based on four core competency domains: roles and responsibilities, interprofessional communication, values and ethics, and teamwork—but these are not specific to palliative care education. Current efforts to develop such standards, said Ballentine, are incremental at best and involve dealing with a variety of intervening and overlapping considerations. In her view, achieving consistency in training across the United States is perhaps unattainable, “but it is something to think about and strive for.”
Amy Melnick, executive director of the National Coalition for Hospice & Palliative Care, noted that there is a bill in Congress—the Provider
Training in Palliative Care Act18—that would allow specialty palliative care providers to access loan repayment programs offered by the National Health Service Corps. Washko added that the intent of this bill is to increase access to care in areas that are the most underserved.
PREPARING ALL HEALTH PROFESSIONALS TO CARE FOR PEOPLE WITH SERIOUS ILLNESS
Miguel Paniagua, medical advisor for Solution Design and Delivery for the National Board of Medical Examiners and adjunct professor of medicine at the Perelman School of Medicine at the University of Pennsylvania, opened the second session of the workshop. Referencing Kamal’s presentation, he shared that this session would focus on how to deputize others to do the work that we know is important and prepare all health professionals to care for people with serious illness.
ELNEC: 20 Years of Providing Palliative Care Education
Betty Ferrell, director of nursing research and education, professor at the City of Hope National Medical Center, and principal investigator for the End-of-Life Nursing Education Consortium19 (ELNEC), recounted that when she was a nursing student about 40 years ago, there was no content at all in the entire nursing curriculum on palliative care, hospice, pain, or end-of-life care. Yet, when she graduated, she went to work on a 40-bed oncology unit and learned about the issues related to end-of-life care while on the job. This experience, she said, illustrates the enormous gap that still exists between what health professionals are trained to do and what they actually do in their daily practices with the patients they hope to serve well.
Nurses, said Ferrell, absolutely have a central role to play in palliative care because there is no other health profession that spends more time at the bedside. Nurses support patients’ physical, psychological, social, and spiritual needs and are trained to collaborate with other team members. “Nurses are central to interdisciplinary care and serious illness,” said Ferrell, who, together with her ELNEC collaborators, has developed curricula
___________________
18 For more information, see https://www.congress.gov/bill/116th-congress/senatebill/1921 (accessed March 9, 2020).
19 For more information, see https://www.aacnnursing.org/ELNEC (accessed April 3, 2020).
to educate nurses from all backgrounds and levels of education about the issues related to caring for people with serious illness (Ferrell et al., 2015).
Ferrell explained that the ELNEC project began in 2000 with a grant from the Robert Wood Johnson Foundation and has maintained important partnerships with the City of Hope and AACN for the past 20 years. Ferrell noted that they began with a generic core curriculum but soon realized it did not meet all palliative care needs. There are now eight curricula designed to meet the needs of practicing clinicians, ranging from pediatrics to geriatrics, and in various settings, such as critical care units and long-term care facilities. Each curriculum includes models on palliative nursing care, pain and symptom management, ethical issues and cultural considerations, communication, loss, grief and bereavement, and the final hours of life. The courses also offer in-person and online training and address topics such as budgeting, quality improvement, and leadership. Over ELNEC’s 20 years of work, Ferrell and her colleagues have trained 24,500 ELNEC trainers who returned to their home institutions and educated more than 735,000 nurses, NPs, and nurses’ aides (ELNEC, 2019). The ELNEC curricula, she noted, have been translated into 11 languages and are used in every state in the United States, the District of Columbia, 100 countries, and every continent except Antarctica. Ferrell added that access to the entire ELNEC curriculum, which was developed for undergraduate and graduate nursing schools, is $29 per student (ELNEC, 2019).
Ferrell explained that there are three key themes in every ELNEC curriculum: the family is the unit of care; nurses play a vital role as advocates, particularly for underserved communities; and honoring culture is important. She noted that all teaching exercises are inclusive of diverse communities and pay attention to the unique needs of vulnerable populations. The curricula also stress end-of-life issues, which affect all systems of care, and ways in which financial issues can influence end-of-life care. Another important theme is that palliative care is needed for people with all serious illnesses as well as for sudden death, such as in the emergency department.
From the project’s inception, ELNEC has included evaluation of outcomes as an integral part of the program (Malloy et al., 2007; Marshall, 2001; Matzo et al., 2004; Sherman et al., 2004, 2005). Ferrell described several ELNEC projects that are having an important impact on workforce issues. For example, the ELNEC APRN project includes clinical content and information budgeting, quality improvement, education, and leadership for both adult and pediatric APRNs. At the time of the workshop, ELNEC had held 14 APRN courses and trained 845 adult and 100
pediatric APRNs. In another project, funding from the NCI is enabling ELNEC to offer five courses that provide oncology APRNs with the tools and resources to prepare them to be palliative care generalists. Ferrell noted that as of September 2019, 286 oncology APRNs from 44 states and the District of Columbia had participated in three courses. For a third project, ELNEC was asked to create a curriculum20 for every Department of Veterans Affairs (VA) facility and train all nurses working in VA acute care settings to provide better care for veterans.
In summarizing 20 years of work, Ferrell said there are a number of challenges to broader dissemination of these types of curricula, starting with what she characterized as the incredibly limited funding available for education projects and to support nurses in taking courses. She noted that the NCI is the only institute at the National Institutes of Health that offers the R2521 training mechanism. “There is so much that needs to happen in every other population beyond oncology, but there is such limited money for education,” said Ferrell. She noted that when there are scholarships available, nurses take these courses. Another challenge is that nursing extends across all clinical areas, and keeping all the necessary curricula updated requires an enormous amount of staff time, for which there is no funding.
Ferrell stressed that ELNEC’s collaborations with AACN and the Oncology Nursing Society have been vital. The train-the-trainer model has been remarkably successful, and those who have become trainers now offer more than 200 ELNEC courses annually (ELNEC, 2019).
In closing, Ferrell offered a personal message: “If someone you love is seriously ill, you would want their symptoms well managed, support for your family, good communication, spiritual and psychosocial support, and a death that respects and honors their life.” That will not happen, she observed, “unless clinicians are trained to provide that care.”
Equipping Mid-Career Clinicians with Core Skills for Serious Illness Care
One outcome of the aging of the U.S. population is that most of the health care workforce is going to be working with patients who have seri-
___________________
20 For more information, see https://www.wehonorveterans.org/elnec-%E2%80%93-veterans-updated-curriculum (accessed March 9, 2020).
21 For more information, see https://researchtraining.nih.gov/programs/researcheducation/r25 (accessed February 28, 2020).
ous illness, noted Brynn Bowman, vice president for education at CAPC. Moreover, many of those individuals will be seen outside of the hospital, in settings such as primary care, where most of the workforce has not received any training in the communication skills required to have meaningful conversations with patients about their goals of care and complex symptom management or how to support family caregivers.
Bowman pointed out that clinicians graduating today have more exposure to palliative care because the majority of academic medical centers have specialty palliative care teams. However, much of the workforce currently practicing does not have such exposure to palliative care. In fact, a survey22 by The John A. Hartford Foundation, the California Health Care Foundation, and the Cambia Health Foundation found that 70 percent of physicians practicing today had never received training in how to have compassionate advance care planning conversations and that those conversations cause practicing physicians a great deal of anxiety. “This is what we want to address in training nonspecialists in core palliative care skills,” she said. One reason doing so is important is that provider communication has been found to be one of the biggest factors correlating to hospital readmission (Sullivan and Ellner, 2015). “When clinicians are not trained in these skills and thus do not use these skills, the outcomes for our patients are poor,” said Bowman.
For the past 20 years, CAPC has been developing technical assistance to support the design of high-quality specialty palliative care programs, and in 2015, it launched a self-study, online curriculum for mid-career clinicians from all specialties, disciplines, and care settings. This online curriculum provides training in pain and symptom management, communication, caregiver support, and disease-specific strategies. While acknowledging that online courses cannot address all training gaps, particularly for communication skills, which are improved greatly from in-person training, Bowman emphasized that such courses can help clinicians understand that they have gaps in their skill sets and that it is possible to fill them.
The critical design elements for the CAPC curriculum, which Bowman said can apply to other curricula as well, include a focus on interprofessional practice and features that motivate organizations to endorse this training or require their clinicians to take it. In addition to ensuring that clinicians receive continuing education credits for these courses, CAPC has also cre-
___________________
22 For more information, see https://www.johnahartford.org/dissemination-center/view/advance-care-planning-poll (accessed March 5, 2020).
ated a certificate of designation that clinicians can include in their résumés and that organizations can use as a differentiator in their hiring decisions, according to Bowman. Accessibility and ease of use are particularly important with online courses and technology, she added.
Another important design element is to incorporate the best adult learning practices available so that they are interactive and capture the attention and hearts of busy practicing clinicians. For example, CAPC’s courses are filled with quiz questions that clinicians must answer correctly to move on. “We know that our clinician audience does not like to get wrong answers,” observed Bowman. “This is one of the techniques that we have used to achieve engagement in our learning and make sure that that learning is reinforced and then put into practice,” she explained.
Over the past 5 years, more than 47,000 individual health care professionals have completed 350,000 courses.23 More than 14,000 users now have a CAPC certificate of designation for completing a full training unit, such as on communication, and 90 percent of users have reported they are likely to change their practices after taking a single course. One survey found that before achieving a certificate in pain management, only 9 percent of respondents strongly agreed they were confident in their ability to manage their patients’ pain. That increased to 51 percent after earning the certificate. Bowman noted that annual course completions increased from almost 27,000 in 2015 to more than 114,000 in just the first 9 months of 2019, which reflects engagement by individual clinicians and recognition from organization leaders that these skills are important.
Bowman identified several factors that make it difficult to reach as many clinicians as possible, including that effective training has often been contingent on palliative care leadership. It is important to have a palliative care leader who can speak with colleagues from other specialties and convince them of the importance of this training. The problem is that palliative care leaders often lack the time to do this type of outreach and education work, which limits the capacity to scale training programs and also contributes to clinician burnout. According to Bowman, one solution is to position palliative care leaders as strategic partners in population management for seriously ill patients and allocate time for them to participate in educational activities. Bowman also highlighted the importance of recruiting champions from a range of clinical specialties.
___________________
23 For more information, see https://www.capc.org/blog/celebrating-20-years-milestones (accessed April 16, 2020).
Another factor, noted Bowman, is physician engagement. Most physicians have heavy workload and training requirements. Offering continuing medical education credits may help increase physician engagement, as may including requirements for training in undergraduate- and graduate-level medical education. In addition, some physicians may feel that palliative care should be delivered exclusively by the palliative care team and not by other clinicians. The solution here, said Bowman, is to emphasize the message that palliative care encompasses not only specialist palliative care skills, but rather, the skills needed by all clinicians who seek to provide high quality health care for people with serious illness.
Lastly, Bowman pointed out that training alone is not sufficient to create practice change: it is incumbent on leaders of provider organizations to prioritize culture change around serious illness care to ensure that clinicians not only receive training but have the structural support to use those skills. Bowman shared that the American Hospital Association (AHA) has now partnered with CAPC to stress to the AHA membership how important it is to prioritize serious illness care. CAPC has also worked with several health plans to train case managers and medical directors on how to best interact with training clinicians who are trying to determine if their patients might need access to specialty palliative care and case management.
In closing, Bowman noted that all specialty palliative care training programs have likely reached only 10–15 percent of the more than 4.6 million practicing physicians, PAs, NPs, registered nurses, and social workers that will work with seriously ill patients at some point (BLS, 2018; Fulmer et al., 2018; The George Washington University Health Workforce Institute and School of Nursing, 2017; KFF, 2019; NCCPA, 2018). “It is not enough, but it is enough to tell us that this is possible if we keep chipping away. We know what patients’ needs are. We know how to deliver training and what different effective mechanisms there are—it is time to execute,” she concluded.
The Role of an Accrediting Organization
At any given time in the United States, there are more than 140,000 physicians in one of more than 11,000 residency or fellowship training programs (ACGME, 2020a), and each program has to include common program requirements to receive accreditation, said Eric Holmboe, chief research, milestone development, and evaluation officer at the Accreditation Council for Graduate Medical Education (ACGME). Among the require-
ments are competencies in interpersonal and communication skills and systems-based practices that include issues related to all patients with serious illness, but particularly in terms of meeting patient and family end-of-life goals. These are competencies, Holmboe pointed out, that every physician is supposed to be attending to, not just palliative care specialists.
Each competency, he explained, includes a statement on its background and intent, which explains why these requirements are important and are core features across all training programs. For example, the background and intent section on interpersonal and communication skills explains that when there are no more medications or interventions that can achieve a patient’s goals or provide meaningful improvements in quality or length of life, a discussion about the patient’s goals, values, and choices surrounding the end of life is one of the most important conversations that can occur. Residents must learn to participate effectively and compassionately in these meaningful human interactions, for the sake of their patients and themselves. Holmboe reiterated that this applies to all residents and fellows, not just those in palliative care programs.
Holmboe noted that training is an intense development process even for practicing clinicians, which makes it important to embed teaching these competencies into the process and take them to the bedside, rather than simply presenting them in a lecture or two (Pusic et al., 2015). The challenge, he said, is how to have residents and fellows use these skills at the bedside when interacting with patients (see Box 2).
Holmboe emphasized that training programs make the ultimate decisions about who is competent and will enter the workforce. End-of-life care is embedded within the health system and community, so “preparing programs to train effectively in these competencies is really important,” said Holmboe.
The milestones are also being used to measure education outcomes other than medical knowledge. “Do not get me wrong—knowledge is important,” said Holmboe. “It is essential, but it is insufficient. We need these other skills.” Those outcomes cannot be measured by a test, he explained, but require observation by and feedback from those supervising residents and fellows. “This is a cultural change we are all going to have to get more comfortable with,” he said.
Holmboe described ACGME’s assessment system, noting that multiple assessments will generate data that go to a clinical competency committee. The committee then judges where a learner is developmentally and provides feedback to the resident or fellow (and the program itself) to help the
learner and program improve. Holmboe explained that ACGME now has national milestone data that the organization is using to provide feedback to programs. “For the first time, we have learning analytics that will be available to our core specialties to see how they compare against their peers nationally and how they are performing in each of these competencies,” he said. ACGME is also offering a 6-day course in assessment skills three times per year and has partnered with 11 regional assessment hubs that offer 2- to 3-day sessions in direct observation training for clinician educators.
Holmboe explained that ACGME uses a mechanism called the Advancing Innovation in Residency Education pathway that encourages programs to develop innovative models for residency and fellowship education. He added that ACGME has approved two pilot programs in hospice and palliative care, including the one Dingfield spoke about earlier. Another program at the University of Colorado Medical School is part of its interprofessional palliative care certificate program and allows mid-career physicians in rural and underserved areas to train through distance learning.
Holmboe pointed out that there is also a pilot program in geriatrics, and several others are currently being developed.
In closing, Holmboe observed that education, when done well, is what he called a “co-produced service” (Batalden, 2018). In that context, he explained, residents, fellows, and faculty need to co-produce education to create higher value.
Educating Nurses in Palliative Care
Deborah Trautman, president and CEO of AACN, noted that one of AACN’s first efforts in end-of-life palliative care was to work with ELNEC and the City of Hope on developing what was called a peaceful death document. Over time, AACN and ELNEC have also developed palliative care competencies for undergraduate and graduate nursing students. Given that nurses often spend the most time with patients as compared to other health care professionals, Trautman asserted that this is both an opportunity and a responsibility to capitalize on that time and initiate and continue difficult conversations about the end of life.
AACN has also developed three sets of essential elements that every baccalaureate, master’s, and doctorate degree for advanced practice nursing curriculum should include. These are not standards, Trautman explained, but do serve to help nursing schools to implement curricula, evaluation processes, and teaching processes to ensure that their graduates have the competencies they need. Each of the three essentials contains explicit content on end-of-life and palliative care issues and the need to implement patient and family care around the resolution of these issues, such as symptom management, support of rituals, and respect for patient and family preferences.
Trautman noted a need to continue building skills and commitment across the nursing profession in order to continuously evolve learning, comfort, and expertise in caring for patients with serious illness. She explained that there are still many barriers to overcome, such as adequately preparing faculty, the lack of up-to-date resources, the variation of content in different programs, and the accessibility of potentially false information online. Trautman added that nurses can advocate for patients and families and help them understand the information that is available to them. In her opinion, there are opportunities for everyone in interprofessional team-based care to create a better environment for patients.
Regarding the modules in the ELNEC curriculum, Trautman noted that they have received positive reviews and are continually revised to
include new information. Each module contains testimonials, case studies, brief video clips, quizzes designed to mimic the licensing exam all nurses must pass, and content on both pediatric and geriatric palliative care. A program evaluation that looked at the ELNEC undergraduate curriculum found that between January 2017 and September 2019, more than 330 schools of nursing from 48 of 50 states and the District of Columbia had enrolled in the program, accounting for 74 percent of bachelor’s degree and prelicensure programs. Around 30,500 students completed the curriculum, and an 18-month post-course evaluation found that at least 97 percent of students believed the six modules were relevant to their practice, presented the information effectively, and resulted in the students changing their practice (Buller et al., 2019; Dahlin et al., 2017; Ferrell et al., 2015, 2018).
Trautman noted that primary palliative care nursing education is critical today because 90 percent of U.S. hospitals with 300 or more beds now have palliative care programs (Dumanovsky et al., 2016), and the expectation is that new graduates will have the necessary training to work in or with those programs. There are barriers, however, that AACN’s more than 840 member schools face in meeting that expectation, starting with faculty being unprepared to focus on palliative and end-of-life care and lacking the resources they need to address these issues in the classroom. Trautman noted that other barriers include a lack of space in current curricula and outdated or inaccurate curricular context (Ferrell et al., 2016). “We must make sure not only that we are providing education but that the ongoing continuing education has the most current and up-to-date information,” she said. Trautman also commented that while more than 330 nursing schools use the ELNEC curricula (ELNEC, 2019), the other AACN member schools need to demonstrate that they are including this content in their curricula and developing competencies using some other strategy.
In the future, said Trautman, most care is not going to be delivered in the hospital, so more health systems are creating palliative care programs that will work outside of the hospital walls. As those programs develop, she noted, it will be important for all members of palliative care teams to support one another to be as skillful as possible when interacting with patients and families.
In conclusion, Trautman observed that the nursing profession has come to understand that while conveying content is central to educating future health care professionals, it will be more important to help them develop critical thinking skills so they can best apply that information. AACN is re-envisioning the essentials to focus more on competency-based education.
Audience Discussion
During the discussion session following the speaker presentations, Marian Grant, a consultant for several national palliative care organizations, including the Coalition to Transform Advanced Care, commented that there are several progressive payers promoting community-based palliative care by requiring physicians and clinicians in their network to take courses on this topic. She added that this can serve as a systems-level impetus for clinicians to develop additional skills.
Replying to a question by Rodgers as to whether there was some way to harmonize continuing medical education across all fields so that programs would integrate with one another and collaborate on developing common skills, such as communication, Holmboe said that this is exactly what he and his colleagues are trying to accomplish. Holmboe explained that there were initially six general competencies for medicine, and it was largely left up to programs to figure out how to implement them. This resulted in a variety of terms and definitions used to describe the same competencies, so one goal of developing milestones was to create a “shared mental model” that could be used across specialties.
Berman asked about the role of clinical sites and how organizations such as ACGME will push academic institutions not only to prepare the workforce but also to prepare or improve their clinical sites. Holmboe noted that one part of ACGME’s accrediting system is a Clinical Learning Environment Review, which includes a site visit and measures how residents and fellows are being incorporated into institutional practices. He added that growing research shows that the performance of an institution and the quality of care that the institution delivers are associated with the quality of care that its graduates provide. “If the institution is not enabling high-quality care, people will come out insufficiently prepared, despite whatever abilities or capabilities they may have. I think we have underrecognized the profound impact of the environment and the institutional practices,” Holmboe said.
DEVELOPING THE WORKFORCE FOR COMMUNITY-BASED CARE
Tamarah Duperval-Brownlee, chief community impact officer of Ascension and president and CEO of Providence Health System, shared that the workshop’s third session would describe the community-based care workforce, its roles, and the people to whom it provides care and support.
Duperval-Brownlee added that this workforce can vary depending on regulation, payment, and setting and that the speakers would highlight potential opportunities for advancing its role.
The Current and Projected Workforce for Community-Based Care
Joanne Spetz, professor at the Philip R. Lee Institute for Health Policy Studies, associate director of research at the Healthforce Center at the University of California, San Francisco (UCSF), and director of the UCSF Health Workforce Research Center on Long-Term Care, explained that the community-based care workforce includes a wide array of health care professionals, including physicians, nurses, pharmacists, physical and occupational therapists, personal care and home health aides, community health workers and navigators, home health nurses, community paramedics, social workers and licensed clinical social workers, spiritual care providers, peer providers, and family caregivers. According to Spetz, the majority of care for people with serious illness is often supplied by informal caregivers—who are doing “high-skill, high-stress, and high-need work to support people with serious illness.” These caregivers are often not included in discussions of integration, coordination, and information sharing.
Spetz presented data from the Bureau of Labor Statistics (BLS) on the number of people involved in providing community-based care (see Figure 4). She pointed out the limitations of the data, such as the classification of people by occupation and industry. Spetz explained that some occupations, such as peer providers, do not exist in the data and that many people in such jobs are not employed in the health and social service industries. Spetz also noted that personal care aides are not considered health care professionals and are instead included in the same category as hairdressers and personal trainers—rather than categorized alongside home health aides. Spetz added that if you combined personal care and home health aides, the total number of people employed in these occupations would surpass registered nursing, which is the largest single health care occupation in the United States.24 Spetz called attention to the small number of community health workers included in the BLS data, but she attributed this underrepresentation to the fact that current occupational surveys are not accurately capturing them.
___________________
24 For more information, see https://www.bls.gov/opub/ted/2015/registered-nurseshave-highest-employment-in-healthcare-occupations-anesthesiologists-earn-the-most.htm (accessed March 6, 2020).
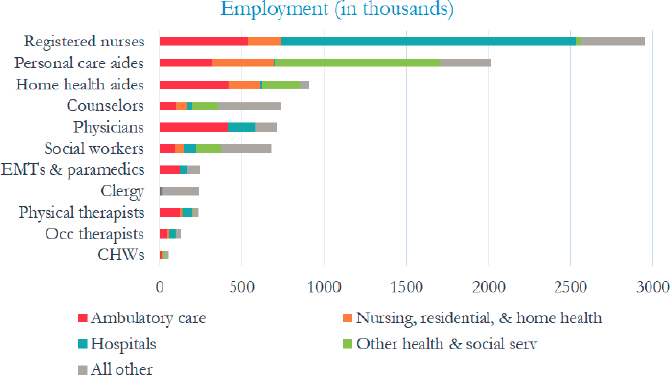
NOTE: CHW = community health worker; EMT = emergency medical technician.
SOURCES: As presented by Joanne Spetz, November 7, 2019; BLS, 2015.
Spetz explained that there will be more than 1 million new home health and personal care aides added to the workforce from 2016 to 2026, according to BLS projections. She noted that the settings in which these aides will work will vary from providing services to people with disabilities through home health care agencies to working in nursing facilities. Many of those who work in the broader community- and home-based workforce are unlicensed, she noted, and their education consists largely of short-term, on-the-job training (see Table 2). “Those individuals are educated and prepared for their work through a variety of different strategies that include a great deal of hands-on experiential opportunities,” explained Spetz.
The trade-off with short-term, on-the-job training, said Spetz, is that the workers do not have the opportunity to invest in skill development to the degree that might be ideal. In addition, employers and society at large tend to write them off as untrained and unskilled, which is unfair in her view. “If you have ever watched a good community health worker or home care aide in their job, that moniker of unskilled is the most inappropriate moniker you could ever hear,” said Spetz.
Spetz pointed out the range of job titles for community health workers (e.g., navigators, coordinators, “promotoras”), which adds to the confusion regarding who is doing what in community-based care. Moreover, training requirements across the different occupations can vary even among jobs
TABLE 2 Education and Licensing of the Community-Based Health Care Workforce
| Education | Training | Licensed? | |
|---|---|---|---|
| Registered nurses | Associate’s/bachelor’s | None | Licensed |
| Personal care aides | High school | Short-term OJT | None |
| Home health aides | Post-HS cert | Short-term OJT | Certified |
| Counselors | Master’s | Internship | Licensed |
| Physicians | Doctorate | Internship | Licensed |
| Social workers | Master’s | Internship | Licensed |
| EMTs and paramedics | Post-HS cert | None | Licensed |
| Clergy | Bachelor’s | Moderate OJT | None/Certified |
| Physical therapists | Doctorate | None | Licensed |
| Occ therapists | Master’s | None | Licensed |
| CHWs | High school | Short-term OJT | None |
NOTE: CHW = community health worker; EMT = emergency medical technician; HS = high school; Occ = occupational; OJT = on-the-job training.
SOURCE: As presented by Joanne Spetz, November 7, 2019.
that sound as if they should be identical, also increasing the confusion, explained Spetz.
Training for home and personal care aides is particularly problematic, she said. There are no federal standards, and requirements vary even across state Medicaid programs. While CMS has developed core competencies, there has been little research measuring the impact of training.
Spetz identified an additional challenge as the lack of a rational or organized payment structure for community-based care. Home care has specific financing challenges, she noted, in that most people pay privately, and Medicaid has multiple programs that are not consistent with one another. In addition, the self-direction options allow beneficiaries to select their aide or how to spend their benefits, including hiring family members in some states, but there is little research on the effect of self-direction on care quality and outcomes. The plethora of unconnected programs, said Spetz, leads to inconsistency and confusion for this workforce.
Many of the occupations involved in providing community-based care are racially and ethnically diverse, which can form the basis for providing culturally competent care but also add a communication challenge across teams, Spetz pointed out. This workforce is also economically vulnerable,
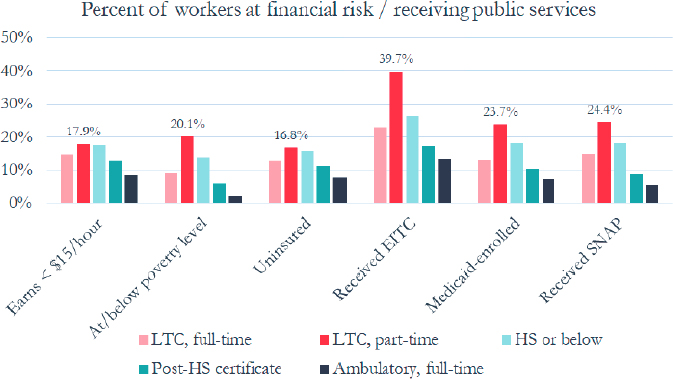
NOTE: EITC = Earned Income Tax Credit; HS = high school; LTC = long-term care, SNAP = Supplemental Nutrition Assistance Program.
SOURCES: As presented by Joanne Spetz, November 7, 2019; BLS, 2015.
with 18 percent of the part-time, long-term care workforce earning less than $15 per hour and 20 percent earning wages at or below the poverty level (see Figure 5). Many of these workers do not have health insurance themselves. Low payment levels combined with low-quality supervision, a lack of autonomy, underappreciation, occupational safety concerns, and unstable hours of work have led to high rates of turnover, which are associated with poor client outcomes. “Quite frankly, their career ladders are often better working in fast food, where they could become a shift manager,” said Spetz.
In closing, Spetz noted that there are opportunities for change. For instance, Medicare and Medicaid’s use of value-based payments could incentivize broader use of the community-based workforce. Another approach is to increase payments for home- and community-based services with wage pass-through requirements, in which payment increases must be used for wage increases. In addition, some states are establishing training standards and opportunities for growth: Washington State,25 for example, requires 75 hours of entry-level training for home care aides and wage increases for advanced skills. Research can also provide insights to support
___________________
25 For more information, see http://www.myseiubenefits.org/wp-content/uploads/2015/05/SEIU-CaseStudy.pdf (accessed April 2, 2020).
best management practices and evaluate the effect of wage increases and training on costs and outcomes. “I think this workforce is so important and so unappreciated and there are huge opportunities to move forward with it,” said Spetz. She concluded her remarks by pointing out that “we have plenty of skill and talent and passion to draw from in this workforce.”
Maximizing the Role of the Home Care Worker
Home care workers are significant in helping patients manage their conditions and remain living in their homes and community, said Angelina Drake, chief operating officer of PHI. Home care workers also play an indirect role by enabling family members to remain in their jobs and earn a living while knowing that their loved ones are receiving the care they need. However, Drake noted, as the demand for the services that home care workers provide increases as the U.S. population ages, it is imperative to build a system with a strong and stable home care workforce to support this demand. “We cannot do that until we have a system that values home care work and the people who provide it,” she said.
Drake also challenged the notion that home care work is unskilled or low skilled. Reflecting on her own experiences as a home care worker in Florida, Drake recalled how she had a client in her 80s who was in the early stages of dementia and had lung disease that required 24-hour oxygen support. “For me to provide her with quality care, I needed to understand these conditions, how they affected her body systems, and how they would affect her daily life,” she explained. “I needed to understand her plan of care and the signs and symptoms to look out for that could indicate that her conditions were worsening.” With another client, an outgoing man in his 90s suffering from chronic leg pain following a fall, she had to draw on her communication, self-management, and problem-solving skills to understand what was at the root of his frustration when he needed help with a task that he had been able to do independently.
Home care work requires both physical and emotional strength, noted Drake, recalling how there were days when managing a client’s mood swings could be as physically and emotionally demanding as the physical stress of moving them from their bed to a wheelchair. Home care workers are also tasked with ensuring the safety and security of their clients, she noted. Given these demands, Drake explained, home care is not low-skill work but rather middle-skill work that draws on an array of diverse skills that are constantly at play. However, the systems that govern home care training, regulation, and
payment do not consider home care to be a middle-skill job. “It is this type of systemic lack of investment and trust in home care work that has helped shape the poor job quality in this field over time,” said Drake.
Reiterating the challenges facing home care workers that Spetz noted, including low wages, inconsistent and largely part-time hours, a lack of benefits, poorly enforced training, disrespect, and isolation, Drake said that the median annual income of the home workforce (including personal care aides, home health aides, and nursing assistants) is just more than $16,000 per year, with hourly wages averaging $11.52 nationally (PHI, 2019). “This is not a job that is sustainable for individuals and certainly not for families,” said Drake. For this reason, among others, employers of home care workers, she said, are dealing with significant recruitment challenges exacerbated by a turnover rate that can be as high as 82 percent26 annually (PHI, 2019).
The home care workforce is largely made up of women, people of color, and immigrants, said Drake—and a legacy of discrimination has shaped the poor job quality in the field. “We have put less value on work that is performed in the home, and we have valued home care less because of who has traditionally performed it,” said Drake. She emphasized that “if we want real solutions to strengthen this workforce to care for people with serious illness, we have to understand and try to reconcile these historically discriminatory relationships and put in policies and practices that address the inequity that is based on workers’ gender, ethnicity, race, and country of origin.”
Home care workers, according to Drake, often feel unprepared for the complexity of the work they do and are disconnected from the delivery of health care and social services. The result, in her view, is that the health care system is not optimizing the benefits to patient health and well-being that home care workers could be providing. For Drake, what is needed is to “recognize that home care workers are underutilized and undervalued, [and] we can then develop solutions that affect both of these dimensions of the challenges facing this workforce.” She stressed that “we can train home care workers to do more, measure that impact on patient well-being and measure the cost savings associated with this impact, and use that argument to drive the business case for investing some of that savings back into job quality for this workforce.”
Drake observed that home care workers communicate frequently with the patient and family caregivers, putting them in a position to develop
___________________
26 For more information, see https://homehealthcarenews.com/2019/05/home-care-industry-turnover-reaches-all-time-high-of-82 (accessed April 2, 2020).
trust, understand their patients’ conditions and habits, and spot changes that signal that something abnormal is happening. At the same time, the patient and family members’ communication with the traditional care team is often inconsistent and incomplete. Drake pointed out that what is needed is quality and consistent communication between the home care worker and the traditional care team that could better inform decisions made about the patient’s treatment and care.
Improving communication requires a care model that views the home care worker as part of the patient’s health care team; that, in turn, requires providing enhanced training around clinical factors to enable home care workers to understand their patients’ diagnoses and ways to manage them in the home, explained Drake. Home care workers also need training on the social and environmental determinants of health, how to identify stressors, and how to support a patient’s social connections. Drake pointed out that a home care worker who can identify food insecurity, for example, could relay that information to the care team’s social worker, who could then connect the patient to food supports in the community.
Drake noted that “upskilling”27 through additional and enhanced training often keeps home care workers within their existing scope of practice and has not been associated with a promotion. Drake believes that it should be paired with wage improvement and workflow innovations that bring workers’ observations to the care team. There are some models, she explained, where home care workers call in to an automated phone system after each shift and answer a series of yes or no questions about changes in a client’s condition. The answers are sent to a clinical registered nurse who can then provide real-time feedback if necessary. In addition to a regular and structured reporting process, home care workers should have access to a care manager or registered nurse at any time as a means of improving their ability to do triage and understand what the next care steps should be. There are also opportunities, said Drake, to develop advanced roles for home care workers where someone with experience can serve as a trusted liaison from the home care environment to the care team, though that requires training care team members to listen to and value home care workers’ observations.
Several demonstration projects that combine upskilling and care team integration of the home care workforce have shown promise in terms of reducing emergency department visits and avoidable hospitalizations and
___________________
27 For more information, see https://www.healthaffairs.org/do/10.1377/hblog20190227.420595/full (accessed February 28, 2020).
improving client satisfaction with care (CLTCEC, 2016; Scales, 2017; SEIU, 2017). Drake noted that as the field builds on these and other demonstrations, it will be important to address the incentives for payers, which means measuring clinical outcomes such as emergency department visits, hospitalizations, and delays in going to a nursing home. For home care worker employers, it will be important to assess workforce retention and satisfaction. “These small pilots should build the momentum for us to generate interest among funders to develop larger pilots, and from there, we can build the evidence base that we are going to need to create real change in this industry and get adoption of these models by state departments of health and large insurers,” said Drake.
Drake said that upskilling the workforce and integrating home care workers with the care team are just a few components of addressing the issue of job quality—policy solutions are also needed. She suggested increased funding for home care services overall, with targeted pass-through dollars for wages and other job quality improvements, and targeting pass-through dollars for training in Medicaid home care service reimbursement rates. She encouraged state and federal agencies to fund workforce innovations that pilot care team integration, upskilling, and advanced role interventions for home care workers. She cited the Direct Creation, Advancement, and Retention of Employment Opportunity Act,28 which would fund this type of innovation.
According to Drake, upskilling the workforce should also be paired with workflow innovations that bring workers’ observations to a care team through a regular and structured reporting process. She added that this also requires training other members of the care team to value and respect home care workers’ observations.
In closing, Drake noted the need for training standards that emphasize competency development and reflect the needs of today’s long-term care patient. She encouraged state-level incentives for home care credentials that are transferrable. “If a home care worker is receiving additional training and responsibilities, the skills they develop need to be valued across the employment landscape,” Drake explained. She said that the moral case for improving wages in this field is not working. Morever, according to Drake, the case for improving job quality in this field based only on population projections, however compelling, is also not working. “I believe that if we
___________________
28 For more information, see https://edlabor.house.gov/imo/media/doc/2019-09-19%20Direct%20Care%20Fact%20Sheet.pdf (accessed February 28, 2020).
really want to move the needle here, we need a strong business case for investing in this workforce, but we also need more popular pressure,” said Drake. “We need people talking about the role of home care in their lives, how it affects their families when they cannot easily access or afford quality care, and the impact that it has on their families as well as the impact on workers who are unable to have a sustainable job,” she concluded.
Advancing a Well-Trained Workforce to Care for an Aging America
Amy York, executive director of Eldercare Workforce Alliance,29 explained that the IOM’s report Retooling for an Aging America: Building the Health Care Workforce (IOM, 2008) challenged her colleagues to think about how care is delivered and how to prepare the workforce that provides that care. The report stressed how team-based care can improve the workforce. York noted that although the size of the overall health workforce has grown since the report’s release, it has not been sufficient to meet the demand today, let alone future demand.
Referring to Drake’s presentation, York agreed that the direct care workforce that provides long-term services and supports to older adults is largely invisible. While most people are unaware of the need for this workforce until they or a family member requires help, York sees that changing, particularly at the state level. This new awareness, she said, is partly a result of the critical shortage of health care providers with specialized training in geriatrics—whether board-certified geriatricians or direct care workers.
York explained that when families need help caring for a loved one, they turn to paid help, primarily the direct care workforce, who provide hands-on care that allows individuals to remain at home as long as and live as independently as possible. The majority of home care workers are personal care aides (HHS, 2017). In 2015, the demand was approximately 2.3 million direct care workers, and based on the projected demand, an estimated 3.4 million direct care workers will be needed in long-term care settings by 2030 (HHS, 2017).
York pointed out that the 2008 IOM report recommended increasing salaries for direct care workers to make them commensurate with the increased responsibilities that workers are asked to shoulder. While salaries have risen in the intervening 10-plus years, the increase has been insufficient
___________________
29 For more information, see https://eldercareworkforce.org/about/who-we-are (accessed March 9, 2020).
in terms of making a difference in their daily lives, explained York. The IOM report also recommended increasing opportunities for comprehensive training. York explained that when the report was developed in 2008, personal care aides and community health workers were the only members of the care team that were not required to have a competency-based license or certification. Today, said York, there are still no federally mandated competencies, professional, or education standards for personal care aides, though some states do have some requirements. “We need to make this a federal standard and have competencies and skill sets to meet the needs of older adults,” said York.
Social workers are another important member of the care team that is often forgotten when talking about workforce demands. According to a 2017 report on the social work workforce, the number of social workers has increased since 2006, and a substantial number without specialty or geriatric training report that older adults make up a large portion of their caseloads (Salsberg et al., 2017). Among people with M.S.W. degrees going into health care, 26.2 percent are working with older adults; of all people with M.S.W. degrees entering the workforce, only 4 percent work with older adults and are in gerontology (Salsberg et al., 2017).
Turning to the subject of care coordination, York described it as an approach to facilitate better communication among individuals, family members, and service providers. She noted that although communication between providers has improved, the health care system continues to struggle to include others. She cited a recent National Academies report, Integrating Social Care into the Delivery of Health Care: Moving Upstream to Improve the Nation’s Health (NASEM, 2019a), which recommended building a workforce to integrate social care into health care delivery systems. “This is especially important in the care of older adults with complex care needs and social support needs,” said York, who noted that the Older Americans Act of 196530 provides for services that support the social needs of older adults, though it is significantly underfunded.
In terms of solutions to current and projected workforce shortages, York referred to the Geriatric Workforce Enhancement Program
___________________
30 The Supporting Older Americans Act of 2020 was passed in the U.S. Senate on March 3, 2020, and will reauthorize the Older Americans Act through 2024. For more information, see https://www.congress.gov/bill/116th-congress/house-bill/4334/text (accessed March 6, 2020).
(GWEP),31 which she explained is the only federal program addressing the health care workforce with the goal of maximizing patient and family engagement to improve outcomes for older adults. York pointed out that HRSA awarded grants in June 2019 to 48 locations in 35 states and 2 territories. These grants will help those sites integrate geriatrics into primary care and transform clinical training environments to provide more coordinated and comprehensive care. York added that the awards will help develop providers who can assess and address the needs of older adults and their families and caregivers.
York noted that HRSA reinstated the Geriatrics Academic Career Award (GACA)32 program, which provides incentives for many on the care team to pursue training and educational opportunities in geriatrics. She cited a 2017 survey that found that 92 percent of GACA recipients said the award facilitated their professional development and that the awards resulted in reaching an estimated 40,700 additional learners caring for older adults (Foley et al., 2017).
In closing, York highlighted a number of steps to take to adequately develop the workforce to care for people with serious illness, including a review of the recommendations in previous National Academies consensus study reports to see where the nation is falling short. She also suggested integrating care teams across health care, the direct care workforce, and social work; expanding training in geriatrics for the entire health care workforce by expanding programs such as GWEP and GACA; and professionalizing the direct care workforce with competency and professional standards, high-quality training, and higher wages.
Innovations in Community-Based Care
Lauran Hardin, senior advisor of partnerships and technical assistance for the Camden Coalition of Healthcare Providers’ National Center for Complex Health and Social Needs, began her presentation by sharing her personal experiences with serious illness. She learned the importance of the workforce for serious illness at the age of 12, when she became a caregiver for her mother, who had been diagnosed with multiple sclerosis. This expe-
___________________
31 For more information, see https://www.hrsa.gov/grants/find-funding/hrsa-19-008 (accessed February 28, 2020).
32 For more information, see https://www.hrsa.gov/grants/find-funding/hrsa-19-007 (accessed February 28, 2020).
rience, as well as experiences with other family members with serious illness and her professional career working in hospice, children’s hospice, palliative care, and complex care, have reinforced Hardin’s belief that there is a critical need for community-based support and integration of care teams.
Hardin explained that the Camden Coalition seeks to improve the health and well-being of a relatively small group of people who repeatedly cycle through multiple health care, social service, and other systems but do not derive lasting benefit. These outliers, noted Hardin, represent 5 percent of the population and 50 percent of the nation’s health care expenditures (HHS, 2019). Hardin explained that the Camden Coalition believes that redesigning ecosystems for individuals with complex health and social needs can bend the cost curve and improve their quality of life. The Coalition provides care to such individuals in the Camden, New Jersey, region through its community-based model with a combination of nurses and community health workers supported by a social worker (referred to as “The Care Team”). The model uses data to triage people daily in the community to identify those with the highest risk. Care teams then engage these individuals at the bedside and ask if they would be interested in receiving care coordination services from the Camden Coalition. If they agree, the team engages them in care planning at the bedside. Hardin noted that the Camden Coalition’s patients, together with its Care Team, have identified 16 different domains, most of which are not medical, that are important for engaging individuals in bedside care planning (see Figure 6).
In discussing the core competencies of the workforce caring for complex populations, Hardin pointed out that motivational interviewing and trauma-informed care33 are among the most important. Other important tenets of care include developing authentic healing relationships, accompaniment, harm reduction, being patient centered, and focusing on patient strengths. Also essential to success, she added, is hiring the right people, supporting their physical and mental health, and making a commitment to self- and team-based care.
Hardin briefly discussed the results of a collaborative effort that focused on each person holistically,34 conducted by her team with Adventist Health in
___________________
33 For more information, see http://nationalacademies.org/hmd/Reports/2019/improvingaccess-to-and-equity-of-care-for-people-with-serious-illness-pw.aspx (accessed March 9, 2020).
34 For more information, see https://www.youtube.com/watch?v=5ltCGJTofrM (accessed March 6, 2020).
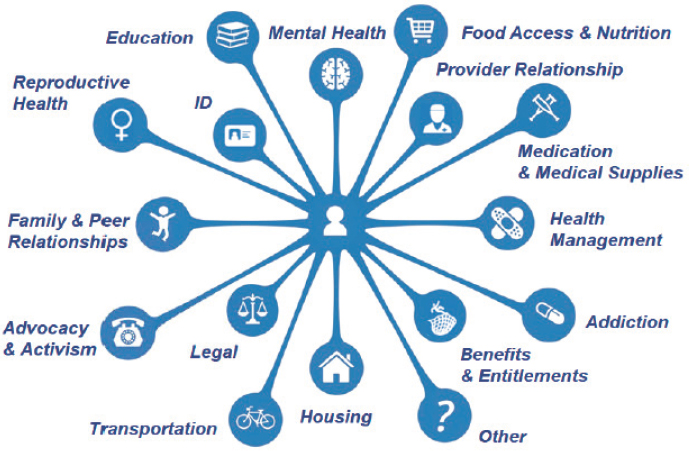
SOURCE: As presented by Lauran Hardin, November 7, 2019; reprinted with permission from the Camden Coalition of Healthcare Providers.
Lake County, California, which has some of the poorest health outcomes in all of California. Hardin described the key components of the care model as:
- Designing care to meet the needs of the unique population in the community;
- Using data to explore the problems that need solving;
- Mapping the existing assets and partners in the community;
- Integrating comprehensive assessment, including the social determinants of health;
- Asking patients what matters most to them;
- Including patients and family caregivers in program design; and
- Designing structures for rapid cycle process improvement to address the root causes of the problems facing the community (Hardin et al., 2016).
In terms of outcomes, the project team found reduced acute health care utilization and strengthened community partnerships in the first 12 months of the project. Hardin reported that hospital use fell 44 percent; use of community services, such as the jail, emergency medical system, and the police, fell 83 percent; and costs dropped 71 percent in the pilot population with
intervention. Hardin added that primary care visits increased 133 percent, and housing use rose 93 percent (Hardin et al., 2020).
In closing, Hardin emphasized that from a policy and competency perspective, teaching health care providers to address the social determinants of health is critical. She recounted how, when she worked in a hospital, she was sending people home with a diabetic management program when they did not have a refrigerator to store their medications. “If we do not start looking deeper, our ability to really serve the needs of patients and families with serious illness is not met,” she concluded.
Audience Discussion
Opening the discussion session, Duperval-Brownlee reiterated the main points of the presentations in the workshop’s third session, including
- The opportunity to improve taxonomy of occupations to better capture the importance of those roles and influence changes in payment structures;
- The importance of articulating the value of home care workers to address issues of wage congruency and job quality, particularly for women and people of color;
- The opportunity to integrate care teams across the health care system and professionalize the direct care workforce; and
- The importance of involving the person being served when designing a system of care delivery.
Ballentine asked how the recent California legislation35 that reclassifies large categories of contract workers as employees would affect the community-based care workforce. Spetz responded that this legislation has created opportunities to establish worker protections for home- and community-based health workers, though it is still unclear if the legislation pertains to agency-based health workers. She noted that some home- and community-based health workers in California are represented by unions, which are creating opportunities for them to develop additional skills.
Hannah-Alise Rogers from HRSA asked Drake to elaborate on why the moral argument for improving the circumstances of home care workers
___________________
35 For more information, see https://leginfo.legislature.ca.gov/faces/billNavClient.xhtml?bill_id=201920200AB5 (accessed March 5, 2020).
has been ineffective and to discuss the need for the field to develop a business case to support aligning incentives across different funders. Drake responded that the moral argument is difficult because people do not like to discuss issues of illness, disability, limited mobility, and death and dying. Additionally, there are deeper issues entrenched in our culture that inform people’s expectations around gender and who can and should provide care, said Drake. Drake further explained that changes to the Fair Labor Standards Act36 in 2013 helped home care workers by making them subject to minimum wage and overtime pay provisions. She remarked that while the wage gains that have resulted have been meaningful to these workers, these and other improvements have been incremental and insufficient to address their comprehensive needs. Drake then noted that PHI developed a “blueprint for a business case.” Drake cautioned, however, that there are insufficient data and access to partners to fully flesh out this approach. Hardin added that large insurers are becoming interested in developing mechanisms to pay for home-based care. The push is coming from employers who are seeing the impact of the stresses of caring for family members on worker absenteeism and illness costs. “Large insurers are starting to get very interested in what is a sustainable system for providing this care,” said Hardin.
Rodgers noted that an interdisciplinary team is essential, but often the hourly care becomes the responsibility of the family, particularly if they cannot afford a home health aide. He noted that the current payment structure—where some benefits are offered through Medicaid but there are high out-of-pocket costs—likely applies downward wage pressure and asked how we can advocate as a system to professionalize and fund direct home care workers. Spetz responded that the separation of different programs is problematic—some states do realize that higher pay and better working conditions would reduce turnover rates and produce positive cost savings downstream. However, she said, if Medicaid is paying for those services, any reduction in hospitalization rates benefits Medicare, and so the states will not see a return on investment.
Grant shared an experience she had with a patient when discussing hospice care. He and his family could not afford hospice care, and their insurance company was willing to pay the higher cost of keeping him in the hospital. However, he did not want to stay in the hospital. Grant noted that if the insurance company would cover home care, the overall costs would be lower,
___________________
36 For more information, see https://www.dol.gov/agencies/whd/compliance-assistance/handy-reference-guide-flsa (accessed April 2, 2020).
but he and his family would be required to assemble a team of home health and social workers for 24/7 care because there is not a comparable, established infrastructure for home care. Hardin responded that creating affordable transitional housing in communities, outside of the long-term care environment, is an exciting emerging trend. York added that Area Agencies on Aging are beginning to provide these services, but they need additional funding.
Terri Maxwell, chief clinical officer for Turn-Key Health, noted that the speakers discussed the importance of the social determinants of health, yet payment policies are often stuck in a medical model that requires physicians and NPs to be team leaders. She asked about ways to advocate for restructuring payment policies to create scalable models that fairly compensate team members. York responded that this will require advocacy at the state level. Hardin added that she thinks value-based payment in accountable care organizations can help create this change because they no longer focus on increasing billable visits. Drake noted that the solutions need to demonstrate impact on patient outcomes and cost savings in order to gain access to public funding mechanisms.
Spetz called for clinician leaders and health executives to step up and say that every member of the care team needs to be involved, that there is more than enough work for everyone. Allowing a home care aide to be involved in medication administration, for example, is not going to hurt anyone else’s job. “There is opportunity for professional advocacy, especially when you start talking about scope of practice, and who owns what, and recognizing that so much of what needs to happen is not in the medical realm per se,” said Spetz. In fact, she called on everyone with a clinical role to speak out any time they hear a colleague put down the unskilled workforce. “It really is a responsibility that we all have,” she said.
Patrick Ross from the Joint Commission asked how to upskill the workforce without adding a training requirement up front that could create another barrier to entry and exacerbate the workforce shortage in the process. Drake noted that, in her experience, workers want to learn additional skills that would positively impact patients, and having quality, accessible training programs can help people feel well supported in their job and add value to their role.
USING INTERPROFESSIONAL TEAMS EFFECTIVELY TO CARE FOR PEOPLE WITH SERIOUS ILLNESS
JoAnne Reifsnyder, executive vice president of clinical operations and chief nursing officer of Genesis HealthCare, opened the final session of the
workshop by noting that she was struck by how the experiences that people had shared throughout the day highlighted the difficult and complex system within which care for people with serious illness is provided. She added that the final session was designed to address the principles and ideals of integrated care and interprofessional teams that had been brought up in other sessions throughout the day.
Creating and Sustaining a Culture of Palliative Care in Long-Term Care Settings
Sister M. Peter Lillian Di Maria, director of the Avila Institute of Gerontology, Inc., described long-term care as “the orphan of health care, one that does not have a strong voice in the health care system and one that is always fighting to get the care and services that individuals need.” Since its founding in 1929, the Carmelite Sisters for the Aged and Infirm have focused on treating the whole person. The Avila Institute was incorporated in 1988 and is the education arm of the Carmelite Sisters. Based on the work of Dr. Michael Brescia of Calvary Hospital in New York, its Central Ethics Committee designed a formalized palliative care program that provides care that addresses the five domains of pain: physical, emotional, spiritual, mental, and family. Sister Di Maria and her fellow Carmelite Sisters decided to stop focusing on the lack of reimbursement for palliative care and instead worked to figure out how to have team members feel supported in the care that they provide every day.
The organization created a steering committee to oversee all aspects of the palliative care program culture and curriculum. That committee, including members of the nursing staff, administration, social services, and pastoral care and the medical director, enumerated all the steps needed to support all health system staff—nurses, social workers, chaplains, certified nursing assistants, dietary staff, and housekeepers—at a facility that did not originally have a dedicated palliative care team. “If we do not instill in our entire staff what palliative care is, then the housekeeper or dietitian is going to miss a palliative care moment,” said Sister Di Maria.
Sister Di Maria explained that this initiative resulted in an interdisciplinary palliative care unit team for each floor in their long-term care facility, whose members participate in ongoing education and pass along their learnings to the rest of the staff and residents’ family members. She explained that educating family members is key, particularly when a resident has dementia. She explained that each palliative care unit team has
a coordinator who runs a weekly meeting to ensure that every person is assessed for the five domains of pain, interventions are developed for pain, and hospice care is arranged for those at the end of life. She explained that the coordinators were already running weekly meetings, but now they were asked to specifically address residents’ palliative care needs.
Sister Di Maria said that creating a compassionate environment and culture that supports palliative care requires four components:
- Education (through programs such as ELNEC and CAPC)
- Streamlined tools to assess all types of pain
- Teamwork to develop the best solutions for each individual
- The flexibility and willingness to make changes as residents’ needs change
Sister Di Maria pointed out that training is the most important aspect of implementing a culture of palliative care, stressing that all staff members need to be trained in the principles of palliative care, the importance of identifying the five domains of pain, the differences between palliative and hospice care, and how their department contributes to the overall palliative care culture. In terms of training, she shared that the ELNEC curricula have proven to be valuable. She reported that she and her colleagues ran a pilot assessment program in six of her organization’s long-term care homes and found that three or four questions were sufficient to identify a resident’s clinical needs, and two or three additional questions allowed staff to get to the heart of what a person was experiencing in terms of spiritual and emotional pain.
Sister Di Maria elaborated that in a culture supportive of palliative care, team members gain an understanding of its importance for residents, staff, and family, and they learn to continue to use palliative care terms whenever possible. The goal, she said, is to have ongoing conversations about ways to bring peace to every resident’s life and to make it the team’s mission to discover what individual residents care about most. When the teams meet, team members come with a worksheet for each resident that includes what is known about them, the challenges they face, and what brings meaning to their life. “We want to make sure that each unit establishes a comforting and healing environment,” she explained. Sustaining this culture involves using regular feedback from evaluation tools to maintain and improve the quality of care.
In closing, Sister Di Maria focused on two important areas for change: reimbursement for those who specialize in geriatric palliative care, and the need for a full-time position that allows a person to be responsible for
overseeing palliative care in long-term care facilities. She also emphasized the importance of looking at increased specialization in palliative care, such as for dementia.
Caring for the Seriously Ill Child at Home
Pediatric palliative care is provided primarily to children who are not expected to reach adulthood, explained Jody Chrastek, pediatric advanced complex care team coordinator at Fairview Home Care and Hospice. She noted that some children in her program live for a few hours, while others live for years. Chrastek pointed out that while the number of children dying is decreasing, the number born with complex health care needs is increasing. She noted estimates that more than 3 million children could benefit from pediatric palliative care, adding that research has shown that it can reduce health care costs by 11 percent per month and the average number of days in the hospital by 32 percent (Friebert and Williams, 2015).
Fairview Health Services, a nonprofit that serves 16 counties surrounding and including Minneapolis and St. Paul, Minnesota, started its pediatric complex, palliative, and hospice care team in 2013 and has grown by cross-training the health system’s clinicians. The pediatric advanced complex care team includes doctors, nurses, other health professionals, and family members. Chrastek added that many of the children often have five or six health care providers. In addition, with the parents’ permission, the team also includes people in the community who have contact with these children, such as the school nurses, county employees, day care staff, and members of the religious community. Chrastek noted that all of these individuals usually have only limited information about a child’s care plan or their advance directives. “By bringing them into the team, we can provide good, extensive care for these children,” said Chrastek. She also noted that the teams work with the extended-hour nurses, who have often been with families for some time and have developed a deep relationship with the child and family members.
The goal of creating these teams, she said, is to have good continuity from the hospital to the clinic, home, and other locations that play a role in a child’s life. “Through this continuity, we want aggressive pain and symptom management, good care coordination, and psychosocial support so that we can make sure the children and family are getting the care they need,” said Chrastek. A key feature of the program, she added, is its flexibility, which goes beyond the typical hospice, palliative care, or home care model. One child, for example, came to the program in hospice, as he was
expected to die from a neurodegenerative disease, but he soon moved to palliative care and then to care for complex medical conditions, as he passed birthday after birthday.
Fairview’s program covers 16 counties in Minnesota, and Chrastek and her colleagues reach out to patients in need in rural areas as well. Given the distance from the Twin Cities and the vagaries of upper Midwest weather, in-person visits are not always possible, so they make sure there is a family member who can support the broader family and a local public health nurse or emergency medical technician who can help set up medication or medical equipment if needed. They also work with local physicians using videoconferencing, and a strong collaborative relationship connects rural patients with those who can provide additional support.
Chrastek explained that training and education, as other workshop speakers had noted, are critically important to enable staff to provide the best care for children facing serious illness. She noted that it is also important to support the care providers in the form of an accountability partner. Chrastek’s accountability partner is a social worker who can tell when she needs a break and a little self-care. Chrastek pointed out that teams require a great deal of work and evolve slowly—sometimes with a few bumps along the way. Toward that end, good communication among team members is critical, as is a mechanism for resolving conflicts when they develop.
Chrastek noted that her team is paid less than half of what it costs for a visit, and that has to change. Funding, she explained, needs to focus on providing services at home, be flexible and responsive to a patient’s needs, and be accessible across boundaries and insurance companies.
In closing, Chrastek reiterated the need for palliative care education for all clinicians, accessibility to services, appropriate funding, and program flexibility. “Above all, we want compassion,” she concluded.
Reaching Rural Areas Through Technology
Jeanie Youngwerth, director of the palliative care curriculum and Palliative Care Program at the University of Colorado School of Medicine, and her colleagues are leveraging telehealth to bring an innovative care model and interdisciplinary team to care for individuals with serious illness in rural areas of Colorado. She described how an advanced practice provider, social worker, and chaplain from a rural hospital can form a team at the patient’s bedside via telehealth, with a board-certified hospice and palliative care physician collaborating remotely from an urban hospital.
Youngwerth explained that a needs assessment revealed that clinicians of all disciplines identified a gap in care: they struggled to discern a patient’s values and what matters most to them. She noted that this is the responsibility of not just a palliative care physician but the interdisciplinary team. Given the reported gap in care, Youngwerth and her colleagues aimed to leverage telehealth to bring an innovative model of interdisciplinary team care to rural hospitals. She explained that although telehealth has been shown to provide significant benefits to patients in underserved and rural areas, including increased access and reduced cost of care, the challenge is whether patients and families will accept this type of care. “Our experience has been that patients and families receive it quite well,” said Youngwerth. She added that telehealth facilitating interdisciplinary team approaches can also help reduce burnout and increase staff retention. Youngwerth recounted how the physicians in outlying areas have recognized the importance of the telehealth approach. She reported that after working as part of these palliative care teams, several health care professionals have gone on to complete graduate work in palliative care through the University of Colorado. Youngwerth added that one physician is taking advantage of the alternative pathway palliative care fellowship program for mid-career clinicians that Holmboe discussed earlier in the workshop.
Youngwerth explained that of the 19 patients seen in the first 4 months of the telehealth program, 95 percent reported finding the program helpful. In addition, there was a 26 percent increase in advance care planning as a result of the program (Stinson et al., 2019). The only negative was that 30 patients were not seen because the telehealth program is only available for 2 half-days per week, limiting the program’s capacity.
Youngwerth explained that it is possible to address workforce shortages by leveraging programs such as the interprofessional Master of Science in Palliative Care Program at the University of Colorado Denver’s Anschutz Medical Campus. She shared that two providers on the rural telehealth team were enrolled in the program. The goal is for the telehealth program to eventually transition into a self-sustaining community specialist palliative care program, scaling back the need for specialty-level palliative care physicians to join virtually. She remarked that the next steps for her program are to bring telehealth to the patient’s home and expand it to other rural areas of the state. She pointed out that she and her colleagues have observed that the members of interdisciplinary palliative care teams seeing patients together as a team appear to be able to support one another and better absorb and deal with conflict, trauma, and working with patients
who are suffering. It is her hope that this type of support will reduce burnout, increase resiliency, and help maintain a healthy workforce.
In terms of policy actions, Youngwerth called for the support of PCHETA, expanding Medicare reimbursements for telehealth under the Telehealth Enhancement Act of 2015,37 and adding and expanding benefits for home-based palliative care services, including round-the-clock crisis response capabilities. She noted that she plans to apply for the Medicaid Upper Payment Limit38 as a means of extending the telehealth program into Colorado’s mountain and rural communities. She also promoted eliminating cost-sharing so that patients would not have copays for remote visits. Finally, she called for expanding graduate medical education funding to include fellowship slots for training interdisciplinary palliative care team specialists and to support providers in community-based specialist training programs.
Panel Discussion
Reifsnyder invited Bullock and Ferrell to join the panel discussion and encouraged them to reflect on the final session’s presentations. Bullock remarked how refreshing it was to hear speakers validate and affirm the important role of social workers in the care team. For too long, she said, social workers have been trying to earn a seat at the table and get people to understand what it is they do and how they contribute to and are effective members of care teams.
Ferrell, commenting on the education approaches she heard discussed, said she believes that a combination of these approaches is needed to produce the workforce to meet the demands for practitioners of all levels of skill and experience to care for those with serious illness. She noted that the ELNEC program receives calls from hospice programs that are caring for children yet do not have any staff members trained in the special needs of pediatric patients. “This is where there is a big need to train existing staff,” explained Ferrell. While ELNEC can share its pediatric curriculum with program staff, they still need to go to an established program at a children’s hospital to obtain the necessary clinical experience and observe how care
___________________
37 For more information, see https://www.congress.gov/bill/114th-congress/housebill/2066 (accessed March 6, 2020).
38 The Upper Payment Limit is a federal limit placed on fee-for-service reimbursement of Medicaid providers.
is provided in the pediatric setting. She added that there is still the need to have pediatric expertise available by telehealth so that they can have the necessary support when they take on a child with serious illness.
Referring to the most recent NCP clinical practice guidelines, Ferrell pointed out that it includes a substantial emphasis on the role of the social worker. In particular, the guidelines address the importance of relying on social workers to conduct mental health assessments in terms of psychosocial supports because psychiatrists are not always available. Bullock added that social workers are uniquely trained in cultural competence regarding psychosocial assessments. Ferrell pointed out that “all of us in the field of palliative care need to rethink the distribution of work. It is not just a matter of give us more people but of who is doing what.” Ferrell also noted that other health care professionals, such as PAs, are coming to the table to be included as part of palliative care teams. “When we invite new people to the table who have not been there, that is the day that our patients in all areas will be much better served,” Ferrell explained.
Reifsnyder asked Chrastek to elaborate on what it takes to cross-train or work with the existing workforce to develop the competencies and capabilities needed to support a program. Chrastek replied that when she and her colleagues started their program, they were cross-training adult clinicians to provide care to pediatric patients and met with significant resistance from the clinicians. Listening to their fears was required to address them. It is important, though, she added, to have resources available so that these cross-trained clinicians can get help when they encounter a situation that makes them feel uncomfortable.
Referring to Youngwerth’s suggestion that the structure of a team can contribute to building resilience, Reifsnyder asked if she anticipated seeing the same cohesion with a telehealth approach. Youngwerth noted that she has observed in hospital, outpatient, and community settings that when teams are able to work together and there are different disciplines supporting one another, team members feel more supported in the face of their patients’ conflict, trauma, and suffering than when they work on their own with a patient. She believes that team-based support can turn what could be a psychologically and emotionally burdensome situation into a more positive experience. Youngwerth proposed that researchers should examine whether the interdisciplinary team approach can be a key factor for improving wellness in health care.
Audience Discussion
Responding to a question about expanding telehealth efforts throughout Colorado, Youngwerth noted that they are looking to reach more rural community hospitals. She pointed out that a large portion of the population in the more remote areas is covered by Medicaid and that she and her colleagues are exploring a potentially new funding mechanism through Medicaid’s upper payment limit. Bullock shared her perspective as a member of the site visit team for the Circle of Life Award,39 describing Youngwerth’s program as “exceptional and comprehensive.”
Rodgers noted that a challenge in the uptake of telehealth in the context of Medicare is that the reimbursement rules are currently quite restrictive and require that the patient live in a designated workforce shortage area. In addition, patients cannot be in their own homes, which is contrary to the desire of patients to receive palliative or hospice care in their homes. Telehealth is being adopted in the emerging value-based payment space, he noted. As an example, he cited the team at ProHEALTH Care40 in New York, which is leveraging telehealth in combination with home visits by registered nurses or trained medical assistants who then connect to physicians or APRNs at the clinic.
Ferrell cautioned that most of the palliative care teams with which she is familiar are so overwhelmed just managing their own work that they may not have the capacity to expand and take on telehealth. In her opinion, a better approach would be for palliative care programs to take advantage of existing telehealth networks and work with the APRN or social workers who may already be involved with providing telehealth services. Nevidjon said she heard a speaker at a conference several months earlier who said that the most important policy health care should be advocating for at the federal level is to have a national plan for 5G deployment across the country through a public–private partnership. Nevidjon recounted that the speaker contended that such a policy would make a significant difference in terms of providing access to health care.
In addition, Nevidjon applauded Sister Di Maria’s work in creating a palliative care culture. Nevidjon shared that she felt hopeful that such a
___________________
39 For more information, see https://www.aha.org/about/awards/circle-life (accessed March 6, 2020).
40 For more information, see https://www.prohealthcare.com (accessed March 6, 2020).
culture could be a catalyst to elevate palliative care and address the current and projected workforce shortages.
CLOSING REMARKS
Before adjourning the workshop, Bowman recapped the key themes from the day. The first theme was the need to integrate palliative care education into standard clinical education in all its forms. According to Bowman, this serves as a call to action, to both the national organizations that set curriculum requirements and the teaching institutions that implement those requirements, and as an opportunity to attract more providers to specialty palliative care.
A second key theme was the importance of tending to the health and resilience of specialty team members who do not always feel supported in that work, and for the home health care workers who play such a giant role in providing care for individuals with serious illness. A third theme was the need to continually make the case that training in palliative care skills for practicing, mid-career clinicians is good for patients, good for clinicians, and good for the organizations that employ them.
While payment was not a major focus area for this workshop, Bowman recalled that the need to alter payment policies was noted by several speakers. Bowman reminded workshop participants that while the field pursues policy changes related to payment, and as the health care industry moves toward value-based care arrangements, there are steps that can be taken today with training and technology that can still move the field forward and expand the workforce. She also noted the importance of treating culture change as an intervention. As a final comment, Bowman encouraged the workshop participants to think about the individual role they can play in their various organizations to move the needle on improving care for people with serious illness.
REFERENCES
ACGME (Accreditation Council for Graduate Medical Education). 2020a. Accreditation Council for Graduate Medical Education. https://acgme.org/About-Us/Overview (accessed March 9, 2020).
ACGME. 2020b. Milestones by specialty. https://www.acgme.org/What-We-Do/Accreditation/Milestones/Milestones-by-Specialty (accessed March 9, 2020).
Balboni, T. A., M. E. Paulk, M. J. Balboni, A. C. Phelps, E. T. Loggers, A. A. Wright, S. D. Block, E. F. Lewis, J. R. Peteet, and H. G. Prigerson. 2010. Provision of spiritual care to patients with advanced cancer: Associations with medical care and quality of life near death. Journal of Clinical Oncology 28(3):445–452.
Balboni, T., M. Balboni, M. E. Paulk, A. Phelps, A. Wright, J. Peteet, S. Block, C. Lathan, T. Vanderweele, and H. Prigerson. 2011. Support of cancer patients’ spiritual needs and associations with medical care costs at the end of life. Cancer 117(23):5383–5391.
Batalden, P. 2018. Getting more health from healthcare: Quality improvement must acknowledge patient coproduction—an essay by Paul Batalden. BMJ 362:k3617.
BLS (Bureau of Labor Statistics, Department of Labor). 2015. Registered nurses have the highest employment in health care occupations; anesthesiologists earn the most. https://www.bls.gov/opub/ted/2015/registered-nurses-have-highest-employment-in-healthcare-occupationsanesthesiologists-earn-the-most.htm (accessed March 9, 2020).
BLS. 2018. Occupational employment and wages, May 2018. https://www.bls.gov/oes/current/oes291141.htm (accessed April 6, 2020).
Buller, H., R. Virani, P. Malloy, and J. Paice. 2019. End-of-life nursing and education consortium communication curriculum for nurses. Journal of Hospice & Palliative Nursing 21(2):E5–E12.
Buring, S. M., A. Bhushan, A. Broeseker, S. Conway, W. Duncan-Hewitt, L. Hansen, and S. Westberg. 2009. Interprofessional education: Definitions, student competencies, and guidelines for implementation. American Journal of Pharmaceutical Education 73(4):59.
CLTCEC (California Long-Term Care Education Center). 2016. Care team integration and training of home care workers—impact study. Los Angeles, CA: California Long-Term Care Education Center.
Dahlin, C. M., P. J. Coyne, J. Paice, P. Malloy, C. A. Thaxton, and A. Haskamp. 2017. ELNEC-APRN: Meeting the needs of advanced practice nurses through education. Journal of Hospice & Palliative Nursing 19(3):261–265.
Donesky, D., K. de Leon, A. Bailey, A. Doorenbos, R. Fink, C. Hurd, P. Ling, and L. Kitko. 2020. Excellence in postlicensure interprofessional palliative care education: Consensus through a Delphi survey. Journal of Hospice & Palliative Nursing 22(1):17–25.
Dumanovsky, T., R. Augustin, M. Rogers, K. Lettang, D. E. Meier, and R. S. Morrison. 2016. The growth of palliative care in U.S. hospitals: A status report. Journal of Palliative Medicine 19(1):8–15.
ELNEC (End-of-Life Nursing Education Consortium). 2019. Fact sheet. https://www.aacnnursing.org/Portals/42/ELNEC/PDF/ELNEC-Fact-Sheet.pdf (accessed March 9, 2020).
Ferrell, B., P. Malloy, and R. Virani. 2015. The end of life nursing education nursing consortium project. Annals of Palliative Medicine 4(2):61–69.
Ferrell, B., P. Malloy, P. Mazanec, and R. Virani. 2016. CARES: AACN’s new competencies and recommendations for educating undergraduate nursing students to improve palliative care. Journal of Professional Nursing 32(5):327–333.
Ferrell, B., P. Mazanec, P. Malloy, and R. Virani. 2018. An innovative end-of-life nursing education consortium curriculum that prepares nursing students to provide primary palliative care. Nurse Educator 43(5):242–246.
Flannelly, K. J., L. L. Emanuel, G. F. Handzo, K. Galek, N. R. Silton, and M. Carlson. 2012. A national study of chaplaincy services and end-of-life outcomes. BMC Palliative Care 11(1):10.
Foley, K. T., C. C. Luz, K. V. Hanson, Y. Hao, and E. M. Ray. 2017. A national survey on the effect of the geriatric academic career award in advancing academic geriatric medicine. Journal of the American Geriatrics Society 65(5):896–900.
Friebert, S., and C. Williams. 2015. NHPCO’s facts and figures: Pediatric palliative & hospice care in America. Alexandria, VA: National Hospice and Palliative Care Organization.
Fulmer, T., M. J. Koren, S. Hernández, and A. Hult. 2018. Physicians’ views on advance care planning and end-of-life care conversations. Journal of the American Geriatrics Society 66(6):1201–1205.
The George Washington University Health Workforce Institute and School of Nursing. 2017. Profile of the social work workforce. https://www.cswe.org/Centers-Initiatives/Initiatives/National-Workforce-Initiative/SW-Workforce-Book-FINAL-11-08-2017.aspx (accessed April 6, 2020).
Hardin, L., A. Kilian, and M. Olgren. 2016. Perspectives on root causes of high utilization that extend beyond the patient. Population Health Management 20(6):421–423.
Hardin, L., S. Trumbo, and D. Wiest. 2020. Cross-sector collaboration for vulnerable populations reduces utilization and strengthens community partnerships. Journal of Interprofessional Education & Practice 18:100291.
Head, B., B. Peters, A. Middleton, C. Friedman, and N. Guman. 2019. Results of a nationwide hospice and palliative care social work job analysis. Journal of SocialWork in End-of-Life & Palliative Care 15(1):16–33.
HHS (Department of Health and Human Services), Health Resources and Services Administration, National Center for Health Workforce Analysis. 2017. Long-term services and supports: Direct care worker demand projections, 2015–2030. Rockville, MD: Department of Health and Human Services.
HHS. 2019. Kaiser Family Foundation Analysis of Medical Expenditure Panel Survey. https://datawrapper.dwcdn.net/eBKim/3 (accessed March 6, 2020).
IOM (Institute of Medicine). 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
IOM. 2015. Dying in America: Improving quality and honoring individual preferences near the end of life. Washington, DC: The National Academies Press.
Kamal, A. H., S. P. Wolf, J. Troy, V. Leff, C. Dahlin, J. D. Rotella, G. Handzo, P. E. Rodgers, and E. R. Myers. 2019. Policy changes key to promoting sustainability and growth of the specialty palliative care workforce. Health Affairs 38(6):910–918.
Kaufmann, T. L., and A. H. Kamal. 2017. Oncology and palliative care integration: Cocreating quality and value in the era of health care reform. Journal of Oncology Practice 13(9):580–588.
KFF (Kaiser Family Foundation). 2019. State Health Facts—Providers and service use. https://www.kff.org/state-category/providers-service-use (accessed April 6, 2020).
Malloy, P., E. Sumner, R. Virani, and B. Ferrell. 2007. End-of-life nursing education consortium for pediatric palliative care (ELNEC-PPC). The American Journal of Maternal Child Nursing 32(5):298–304.
Marin, D. B., V. Sharma, E. Sosunov, N. Egorova, R. Goldstein, and G. F. Handzo. 2015. Relationship between chaplain visits and patient satisfaction. Journal of Health Care Chaplaincy 21(1):14–24.
Marshall, P. L. 2001. End of life care: Ethical issues. The Kansas Nurse 76(7):4–7.
Matzo, M. L., D. W. Sherman, P. Nelson-Marten, A. Rhome, and M. Grant. 2004. Ethical and legal issues in end-of-life care: Content of the end-of-life nursing education consortium curriculum and teaching strategies. Journal for Nurses in Staff Development 20(2):59–68.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2019a. Integrating social care into the delivery of health care: Moving upstream to improve the nation’s health. Washington, DC: The National Academies Press.
NASEM. 2019b. Taking action against clinician burnout: A systems approach to professional well-being. Washington, DC: The National Academies Press.
NCCPA (National Commission on Certification of Physician Assistants). 2018. 2018 statistical profile of certified physician assistants by specialty: Annual report. https://www.nccpa.net/research (accessed April 6, 2020).
PHI. 2019. U.S. home care workers: Key facts. https://phinational.org/resource/u-s-home-care-workers-key-facts-2019 (accessed March 9, 2020).
Pusic, M. V., K. Boutis, R. Hatala, and D. A. Cook. 2015. Learning curves in health professions education. Academic Medicine 90(8):1034–1042.
Salsberg, E., L. Quigley, N. Mehfoud, K. Acquaviva, K. Wyche, and S. Sliwa. 2017. Profile of the social work workforce. Washington, DC: The George Washington University Health Workforce Institute and School of Nursing.
Scales, K. 2017. Success across settings: Six best practices in promoting QCQJ. Bronx, NY: PHI International.
SEIU (Service Employees International Union). 2017. Innovations in home care: Better health. Better care. Lower costs. Washington, DC: Service Employees International Union.
Sherman, D. W., M. L. Matzo, P. Coyne, B. R. Ferrell, and B. K. Penn. 2004. Teaching symptom management in end-of-life care: The didactic content and teaching strategies based on the end-of-life nursing education curriculum. Journal for Nurses in Staff Development 20(3):103–117.
Sherman, D. W., M. L. Matzo, E. Pitorak, B. R. Ferrell, and P. Malloy. 2005. Preparation and care at the time of death: Content of the ELNEC curriculum and teaching strategies. Journal for Nurses in Staff Development 21(3):93–102.
Stinson, M., E. Belanger-Shugart, K. Morrison, and M. Scott. 2019. Compassionate technology: Palliative care telemedicine in the rural hospital setting (QI741). Journal of Pain and Symptom Management 57(2):478.
Sullivan, E. E., and A. Ellner. 2015. Strong patient-provider relationships drive healthier outcomes. Harvard Business Review. https://hbr.org/2015/10/strong-patient-provider-relationships-drive-healthier-outcomes (accessed April 28, 2020).
U.S. Census Bureau. 2019. By 2030, all baby boomers will be age 65 or older. https://www.census.gov/library/stories/2019/12/by-2030-all-baby-boomers-will-be-age-65-or-older.html (accessed March 6, 2020).


































































