4
Evaluation of Respiratory Outcomes
Veterans who were deployed to the Southwest Asia Theater of Military Operations, in support of either the 1990–1991 Gulf War or post-9/11 conflicts, have consistently reported having poorer health and quality of life than veterans who served in the military during these conflicts but who were not deployed or were deployed elsewhere. This increase in adverse health effects has been seen not only in U.S. veterans but also in veterans of the coalition forces, including Australia, Canada, Denmark, and the United Kingdom. Although other reports (notably the Gulf War and Health series) have reviewed all health outcomes generally grouped by body system, this chapter examines the epidemiologic studies that focused on symptoms, conditions, and diseases of the respiratory tract and their relationship with exposure to airborne hazards from serving in Southwest Asia.
The spectrum of respiratory outcomes of interest is presented in order of nonspecific to more specific and moves through the respiratory tract from the nasal passages to the lungs. It begins with respiratory symptoms, including cough, wheeze, and shortness of breath, which are followed by upper airway conditions, including sinusitis and rhinitis, vocal cord dysfunction, and sleep apnea. A discussion of pulmonary function tests and the epidemiologic studies that used these objective measures is then presented because many of the conditions of the lower airway—the next section—reference those measures. Included in lower airway conditions and diseases are asthma; chronic obstructive pulmonary disease (COPD), chronic bronchitis, and emphysema; constrictive bronchiolitis; interstitial lung disease, which includes diagnoses of hypersensitivity pneumonitis, sarcoidosis, acute eosinophilic pneumonia, and pulmonary alveolar proteinosis; and infectious diseases of the lower airway. The available epidemiologic evidence on respiratory cancers is then described. The final outcome included in this chapter is mortality from respiratory diseases.
Each respiratory condition section starts with an overview of the condition, its symptoms, its diagnostic criteria and pathology where applicable, and its prevalence in the general U.S. population. That is followed by a summary of findings on that outcome from epidemiologic studies that were considered in previous National Academies assessments of respiratory health and military service in Southwest Asia. Those studies were not reassessed by the current committee; instead the committee relied on the assessments and inferences of those previous committees regarding those studies. Summaries and assessments of newly identified epidemiologic studies1 are then presented,
___________________
1Appendix C presents a table overview of the 57 newly reviewed epidemiologic studies that summarizes the study population, conflicts served (1990–1991 Gulf War or post-9/11), and respiratory outcomes assessed in each. Studies that used cohorts as specifically mentioned in the Statement of Task are noted.
ordered by conflict (post-9/112 first and 1990–1991 Gulf War second) and by country of origin; studies of U.S. military personnel are presented first, followed by studies of coalition forces. Within the post-9/11 literature, the studies are summarized with those from cohorts listed in the committee’s Statement of Task presented first, when applicable: Millennium Cohort Study, Study of Active Duty Military for Pulmonary Disease Related to Environmental Deployment Exposures (STAMPEDE), National Health Study for a New Generation of U.S. Veterans (NewGen), Comparative Health Assessment Interview (CHAI) Study, Pulmonary Health and Deployment to Iraq and Afghanistan Objective Study, Effects of Deployment Exposures on Cardiopulmonary and Autonomic Function Study, and research being conducted by the Department of Veterans Affairs’ War Related Illness and Injury Study Center (WRIISC) Airborne Hazards Center of Excellence. Then other studies of military personnel and veterans are summarized. Information on the committee’s process and criteria for identifying, reviewing, and assessing the literature as well as a description of the categories of association the committee used may be found in Chapter 3. Several of the studies reported results pertaining to multiple respiratory outcomes of interest. To minimize repetition, those studies are described in detail in Chapter 3, and only the relevant results pertaining to the outcome of interest are summarized in each section. The 32 studies that are summarized in Chapter 3 are Abraham and Baird, 2012; Abraham et al., 2014; AFHSC, 2010; Baird et al., 2012; Barth et al., 2014; Bullman et al., 2005; Dursa et al., 2016b; Eisen et al., 2005; Hines et al., 2013; Hooper et al., 2008; Kang et al., 2000; Karlinsky et al., 2004; Kelsall et al., 2004; Khalil et al., 2018; Krefft et al., 2017, 2020; Madar et al., 2017; Maule et al., 2018; Morris et al., 2014, 2019, 2020; NASEM, 2017; Pugh et al., 2016; Rohrbeck et al., 2016; Sharkey et al., 2015, 2016; Sim et al., 2015; Smith et al., 2002, 2008, 2009, 2012; and Zundel et al., 2019.
Each condition section ends with a synthesis of the findings and inferences that can be made from the epidemiologic literature on that condition, which is followed by a conclusion concerning the strength of the association between exposure to airborne hazards as encountered in the Southwest Asia theater and the condition of interest. Where the data permit, a conclusion is specific to the strength of the evidence by conflict cohort (1990–1991 Gulf War and post-9/11).
The committee relied on human epidemiologic studies to draw its conclusions about the strength of evidence regarding associations between deployment to Southwest Asia and respiratory health conditions observed in military personnel and veterans. Descriptive studies that present frequencies without modeling risk or odds and case series that lack a comparison group are included for completeness, especially for rare outcomes where there is a dearth of epidemiologic evidence. Often deployment is used as a surrogate of exposure, and a common comparison group is nondeployed individuals who served in the armed forces during the same time period. However, deployed service members experience different exposures for different durations, which may result in misclassification of exposure that would likely lead to underestimating associations. Inasmuch as military personnel must meet physical-health criteria when they enter the military and during the time they are on active duty, particularly when deployed, the group’s health status is usually better than that of their nondeployed counterparts or of the general population of the same age and sex. Further complicating the assessment of veterans’ health is that the diagnostic criteria or definitions for health conditions may be revised to reflect the evolving understanding of these conditions brought on by scientific and medical advances. These types of changes are normal in medical science, and it is likely that the diagnostic criteria for these conditions will further change in the future as knowledge about them grows. As future bodies review and compare studies using the old criteria and new diagnostic criteria, there may be differences in the incidence or prevalence of a condition that may result from the use of the revised criteria.
RESPIRATORY SYMPTOMS
Respiratory symptoms are relatively common and nonspecific. Several symptom complexes sometimes occur without definitive underlying diagnoses, such as chronic persistent cough, dyspnea, and wheezing. Broadly speaking, chronic persistent cough is a cough that lasts longer than 8 weeks but typically disappears once an underlying problem is treated. Chronic cough is associated with sleep disruption and can leave patients feeling exhausted.
___________________
2 As discussed in Chapter 1, the primary post-9/11 U.S. military operations in the Southwest Asia theater were Operation Enduring Freedom (OEF), Operation Iraqi Freedom (OIF), and Operation New Dawn (OND).
Severe cases of chronic cough can cause vomiting, lightheadedness, and rib fractures. Conditions typically associated with chronic cough include the following, either alone or in combination: post-nasal drip, asthma, gastroesophageal reflux disease, lung infections, and COPD. The use of various drugs, including drugs for treating high blood pressure, may also result in chronic cough (Mayo Clinic, 2019a). Additionally, chronic cough can have a psychogenic origin. Occupational and environmental risk factors include outdoor air pollution and allergens and also indoor irritant and allergenic agents, such as cigarette smoke, cooking fumes, animals, dust mites, fungi, and cockroaches (Tarlo, 2006). The population prevalence of chronic cough in the United States is estimated to be between 10% and 15% of the adult population (Song et al., 2015).
Dyspnea, or shortness of breath, is a sensation of difficulty breathing, breathlessness, or even suffocation. Chronic dyspnea is often associated with chronic respiratory diseases, including asthma, COPD, and interstitial lung diseases, such as pulmonary fibrosis (Mayo Clinic, 2019b). As is the case with chronic cough, dyspnea also has psychogenic causes. The prevalence of chronic dyspnea is highly variable, depending on the etiology (Rawat et al., 2019).
Wheeze is a high-pitched whistling sound made with breathing that occurs most commonly on expiration, although it can also be heard on inspiration. While typically associated with asthma or, less commonly COPD, it is a nonspecific finding that can be reported with several conditions, including congestive heart failure. In the studies reviewed, wheeze was based largely on self-report, although the use of International Classification of Diseases (ICD) coding to detect symptoms may also have included wheeze detected on physical examination. The value of self-reported wheeze is diminished by the variability in what patients understand to be wheeze; although this is true to some extent of all self-reported symptoms, it is especially acute with wheeze. For example, upper airway sounds will often be described by patients as wheeze.
Respiratory symptoms are arguably the most commonly studied health outcomes in association with deployment in the Southwest Asia Theater of Military Operations. This may be because they were often the only set of outcomes associated with any number of possible exposures; the fact that they are often observed in the absence of any other detectable respiratory health conditions; and, in many instances, they are among the earliest signs of health outcomes to be exhibited following an adverse respiratory exposure.
There are nevertheless significant challenges in interpreting findings of studies of respiratory symptoms, some of which are related to the nature of symptoms themselves as outcomes and others of which are specific to military deployment. These challenges need to be kept in mind when assessing studies that present information on symptoms. First, information on symptoms is typically collected through self-report. As such, symptoms are notoriously susceptible to information bias. In the military deployment setting, differential misclassification of the outcome can occur if those who have respiratory symptoms are more likely to recall inhalational exposures than those who are asymptomatic, or alternatively, if those who experienced inhalational exposures are more likely to report symptoms for any given degree of exposure. Second, and related to the first challenge, symptoms are subjective. Third, it can be difficult to be confident that symptoms did not predate exposure, such as an exposure during deployment, making it challenging to attribute reports of symptoms to deployment-related exposures.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
In general, previous Gulf War and Health committees grouped all non-cancerous respiratory conditions, including symptoms to specific diagnoses, together when summarizing the available literature. Over the course of the series, 15 studies included symptom outcomes. Those committees categorized studies as primary or secondary studies. In the current assessment, studies are grouped into those reviewed in previous reports and newer studies that have not been previously reviewed. Newer studies are then further categorized into those conducted using populations of U.S. military personnel and those using populations from other Gulf War coalition force countries. These are then classified into those investigating effects of deployment in general and those investigating specific exposures, such as burn pit exposures.
Symptoms were ascertained primarily by self-report, and most of these studies found that deployed veterans report higher levels of respiratory symptoms than nondeployed veterans regardless of country of origin. This trend continues even when studies were conducted several years after deployment. Each study suffers from various
methodologic weaknesses. The results related to respiratory symptoms are summarized below, but the uniformity of findings is striking, especially given that the same studies found Gulf War deployment status to be statistically significantly associated with self-reports of respiratory symptoms among cohorts of U.S., UK, and Australian veterans. The prior Gulf War and Health committees made conclusions based on grouping all respiratory symptoms and conditions and did not make separate conclusions for specific respiratory outcomes (Volumes 4, 8, and 10). The Volume 4 committee concluded
Respiratory symptoms are strongly associated with Gulf War deployment when using comparison groups of nondeployed veterans in most studies addressing this question. However, studies with objective pulmonary function measures find no association between respiratory illnesses with Gulf War deployment across the four cohorts in which this has been investigated. (IOM, 2006, p. 9)
The Volume 6 (IOM, 2008) committee was tasked with assessing the long-term health effects of deployment-related stress, and as such included respiratory outcomes. Based on several epidemiologic studies, including those that examined posttraumatic stress disorder and respiratory disease, that committee concluded that there was inadequate/insufficient evidence to determine whether an association exists between deployment to a war zone and chronic respiratory effects. The Volume 8 committee found that “self-reported symptoms and self-reported diagnoses related to respiratory disease have inconsistently but frequently shown an excess among Gulf War veterans” (IOM, 2010, p. 149). However, that committee also found that there appeared to be no increase in respiratory disease among Gulf War veterans when examined with objective measures of disease, pulmonary function studies, or mortality studies. Based on those findings, the Volume 8 committee concluded that there was insufficient/inadequate evidence to determine whether an association exists between deployment to the Gulf War and respiratory disease. That committee also concluded that there was limited/suggestive evidence of no association between deployment to the Gulf War and decreased lung function in the first 10 years after the war. Based on three newly identified studies of respiratory conditions and data submitted by the Department of Veterans Affairs (VA), the Volume 10 committee concurred with the Volume 8 committee and concluded that there is insufficient/inadequate evidence to determine whether an association exists between deployment to the Gulf War and respiratory disease. However, in a change from Volumes 4 and 8, the Volume 10 committee also concluded that there was limited/suggestive evidence of no association between deployment to the Gulf War and decreased lung function.
The committees of Volumes 2 (IOM, 2003a) and 9 (IOM, 2014) made conclusions specific to respiratory symptoms (grouped) based on associations with specific exposures, including insecticides, organic solvents, and mixtures (Volume 2) and blasts (Volume 9). The Volume 2 committee found that the available literature consisted primarily of cross-sectional studies on lung function that did not examine long-term, persistent outcomes after cessation of exposure, and many studies did not control for confounding by smoking and other common causes of lung disease. Therefore, the Volume 2 committee concluded that there was
- inadequate/insufficient evidence to determine whether an association exists between exposure to the insecticides that they were tasked to examine and persistent respiratory symptoms or impairment after cessation of exposure;
- limited/suggestive evidence of an association between high-level exposure to mixtures of organic solvents and reactive airways dysfunction syndrome, which would be evident with exposure and could persist for months or years; and
- inadequate/insufficient evidence to determine whether an association exists between exposure to the specific organic solvents examined or solvent mixtures and persistent respiratory symptoms or impairment after cessation of exposure.
The Volume 9 committee examined the evidence that exposure to explosive blasts may have on long-term effects on pulmonary function, respiratory symptoms, and exercise limitation as well as long-term effects after acute blast lung injury. Of the approximately 45 published peer-reviewed studies on long-term respiratory health effects of blast exposure considered, all were considered to be methodologically lacking. Acute injuries to the respiratory tract are quite common after blasts, but despite the obvious acute injuries and the high plausibility of long-term
sequelae, the Volume 9 committee found that there was a dearth of data on the long-term pulmonary outcomes of exposure to blast, and that the possibility of other long-term pulmonary consequences of blast exposure, such as the effect of explosion-related dust exposure, and of other exposures, such as smoking, had not been adequately examined. Therefore, the Volume 9 committee concluded that there was inadequate/insufficient evidence of an association between exposure to blast and long-term effects on pulmonary function, respiratory symptoms, exercise limitation, and long-term effects after acute blast lung injury.
1990–1991 Gulf War Veterans
The National Health Survey of Gulf War Era Veterans and Their Families (NHS), described in Chapter 3, is a population-based survey of U.S. Gulf War veterans that was conducted to estimate the prevalence of symptoms and other health outcomes in Gulf War veterans (n = 15,000) versus Gulf War–era veterans (n = 15,000) who were not deployed to the Persian Gulf (Kang et al., 2000). Questions regarding respiratory symptoms asked about coughing, shortness of breath, wheezing, and tightness in chest, with the severity of each also indicated (mild, severe, and total). Population prevalence rates were calculated using statistical analysis techniques to account for stratified random sampling of unequal probabilities of selecting various strata. Coughing was reported by 24% of deployed Gulf War veterans compared with 14% of nondeployed veterans (rate difference [RD] = 10, 95% confidence interval [CI] 9.9–10.1); and shortness of breath by 24% of deployed veterans compared with 11% of nondeployed veterans (RD = 13, 95%CI 12.9–13.1). Wheezing (22% vs 11%; RD = 11, 95%CI 10.9–11.1) and tightness in chest (21% vs 11%; RD = 10, 95%CI 9.9–10.1) were also reported nearly twice as frequently by deployed than by nondeployed veterans. Rate differences of the total frequencies were statistically significant (p ≤0.05) for all four outcomes. Smoking was not controlled for in the analyses; the authors note that a significantly higher proportion of Gulf War veterans than Gulf War–era veterans were smokers (34.7% vs 29.9%).
Karlinsky et al. (2004) collected data on pulmonary histories (including self-reported cough, sputum production, and shortness of breath when climbing stairs) and objective measurements of pulmonary function from 1,036 deployed and 1,103 nondeployed veterans who completed the clinical examination component of the third phase of the NHS. Examinations were performed 10 years after the 1990–1991 Gulf War. Deployed veterans were statistically significantly more likely than era veterans to self-report history of smoking (odds ratio [OR] = 1.31, 95%CI 1.03–1.67) and, separately, wheezing (OR = 1.67, 95%CI 1.06–2.62), but there was no difference between the groups for cough (OR = 1.12, 95%CI 0.80–1.57). Estimates for wheezing and cough were not adjusted for smoking status. Sputum production data were collected, but results were not reported.
Eisen et al. (2005) performed a cross-sectional analysis on health outcomes collected in a subset of 1,061 deployed and 1,128 nondeployed Gulf War veterans (the same population used by Karlinsky et al., 2004) who completed the clinical examination component of the third phase of the NHS. The investigators examined several outcomes, including “obstructive lung disease,” which was defined as “a history of lung disease (asthma, bronchitis, or emphysema) or pulmonary symptoms (wheezing, dyspnea on exertion, or persistent coughing with phlegm) and either the use of bronchodilators or at least 15% improvement in FEV13 after a short-acting bronchodilator” (Eisen et al., 2005, p. 884). No difference in these outcomes was found between deployed and nondeployed veterans (OR = 0.91, 95%CI 0.52–1.59); analyses were adjusted for age, sex, race, years of education, cigarette smoking, component (active versus reserves or National Guard), service branch, and rank. No findings on specific respiratory symptoms were reported.
Several other studies that reported on respiratory symptoms were conducted using specific subsets of U.S. 1990–1991 Gulf War veterans, identified by branch of service, military occupation, base location, or home state of residence.
The “Iowa study” was a cross-sectional survey of a representative sample of 4,886 military personnel from all service branches who were randomly selected from those who had listed Iowa as their home of record at the time of enlistment (Iowa Persian Gulf Study Group, 1997). Trained examiners using standardized questions, instruments, and scales interviewed the subjects. It was the first major population-based study of U.S. Gulf War veterans to group sets of symptoms into categories suggestive of known syndromes or disorders, such as fibromyalgia or
___________________
3 The amount of air that can be forcibly exhaled in 1 second after taking in the deepest breath possible.
depression. This work led to future research on what would become known as Gulf War illness. Doebbeling et al. (2000) conducted a factor analysis to identify patterns of symptoms and also reported higher frequency of both congested mucus or phlegm (10% difference, 95%CI 8–12) and bothered by a cough (10% difference; 95%CI 8–12) between deployed and nondeployed veterans to the Persian Gulf.
Proctor et al. (1998) examined nearly 300 service members who represented a stratified random sample of 2,949 troops from Fort Devens and 928 troops from New Orleans; both groups consisted of active-duty, reserve, and National Guard troops. The comparison group was Germany-deployed veterans from an air ambulance company (n = 48). The study described self-reported exposures to a variety of agents and included measures on the Expanded Combat Exposure Scale regarding exposure to chemical- and biologic-warfare agents. Relevant respiratory exposures included pesticides, chemical- and biologic-warfare agents, oil fire smoke, vehicle exhaust, smoke from tent heaters, and smoke from burning human waste. In comparison with veterans deployed to Germany during the Gulf War era, stratified random samples of both Gulf War cohorts (Fort Devens and New Orleans) had an increased prevalence of 51 out of 52 items on a health-symptom checklist, including pulmonary symptoms of “difficulty breathing or shortness of breath,” “common cold or flu,” and “rapid breathing.” ORs weighted for sampling design and participation base and adjusted for age, sex, and education (but not smoking, which was collected) were elevated for pulmonary symptoms for both deployed groups compared with Germany-deployed veterans but were not statistically significant.
Petruccelli et al. (1999) conducted a study of self-administered questionnaires from 1,599 U.S. soldiers from the 11th Armored Cavalry Regiment after their return from a 3-month mission in 1991 in Kuwait. Symptoms occurring before, during, and after the mission were collected, and each symptom was accompanied by a four-level frequency scale (never, occasionally, most days, and every day). Smoking status and changes in frequency were also captured; 45% of respondents were regular smokers or had been smokers at some time, 25% reported smoking more in Kuwait, and 12% reported smoking less or quitting. Compared with baseline (while the unit was based in Germany), respiratory symptoms reported more frequently for the Kuwait period were upper respiratory tract irritation, shortness of breath, and cough. Of the relatively few troops whose responses on wheezing changed, there were more than twice as many wheezing frequently while in Kuwait as there were during the post-return period. The proportion of soldiers recalling a recurrent cough in Kuwait was nearly twice as high among smokers (28.0%) as among nonsmokers (15.5%), but smoking status was not reported to correlate with other symptoms. Comparisons of soldiers with a self-reported history of allergies or asthma with those without these conditions showed soldiers with the conditions reported a higher incidence of shortness of breath (17.6% vs 8.6%) and cough (27.8% vs 18.8%) associated with the Kuwait period. Shortness of breath and fatigue were lower than baseline after soldiers returned to Germany. Cough, however, was substantially more frequent within a month after the Kuwait experience compared with what respondents considered normal for themselves. Shortness of breath and cough were both more likely to be reported for soldiers who reported spending more than 5 hours per day outdoors, felt that the oil-well fires were more severe than expected, had a different job than at their home base, reported flying insects to have been a significant problem, thought pollution was the worst part of deployment, noted heat exhaustion as problematic, and were injured in an ammunition dump explosion. Other factors were statistically significantly associated with new-onset or exacerbations of shortness of breath or cough separately. The proportion of respondents with symptoms occurring every day or most days increased with decreasing distance to fires; the strongest correlation with distance was demonstrated for cough.
Gray et al. (1999) included cough and shortness of breath in their examination of several self-reported conditions and symptoms among 527 deployed and 970 nondeployed active-duty Seabees (U.S. Navy construction battalions). Odds of having both cough (OR = 1.8, 95%CI 1.2–2.8) and shortness of breath (OR = 4.0, 95%CI 2.2–7.3) lasting at least 1 month were statistically significantly increased for deployed Seabees relative to nondeployed Seabees. When symptoms were compared by exposure categories among the deployed veterans, elevated ORs (p <0.05) for cough were found for veterans exposed to airborne hazards of smoke from oil-well fires, airplane fuel burned in tent heaters, and petroleum solutions sprayed over large areas as well as for those who used pyridostigmine bromide and ciprofloxacin. ORs for shortness of breath were statistically significantly increased for veterans exposed to airborne hazards of smoke from oil-well fires and petroleum solutions sprayed over large areas.
Gray et al. (2002) expanded the deployed and nondeployed cohorts that were first reported in Gray et al. (1999) to include all Seabees who had been on active duty during the time of the Gulf War regardless of whether they remained on active duty, were in the reserve, or had separated from service (n = 11,868 participants, 67.4% participation rate). Participants were divided into three exposure groups: 3,831 who had been deployed to the Gulf War, 4,933 who had been deployed elsewhere, and 3,104 who had not been deployed. Those who had been deployed to the Gulf theater had statistically significantly higher odds of ever smoking compared with nondeployed Seabees (OR = 3.09, 95%CI 2.79–3.42) and of current smoking compared with both Seabees deployed elsewhere (OR = 1.20, 95%CI 1.09–1.31) and nondeployed Seabees (OR = 2.68, 95%CI 2.37–3.04). When asked about shortness of breath, continual cough, and several other medical problems experienced in the past 12 months, Gulf theater–deployed Seabees reported higher frequencies of all 33 outcomes. Following adjustment for age, gender, active-duty versus reserve status, race/ethnicity, current smoking, and current alcohol drinking, ORs were statistically significantly elevated for shortness of breath for Gulf theater–deployed Seabees compared with both Seabees deployed elsewhere (OR = 3.14, 95%CI 2.68–3.68) and nondeployed Seabees (OR = 3.62, 95%CI 3.01–4.51). The odds of continual cough were also statistically significantly higher for Gulf theater–deployed Seabees compared with both Seabees deployed elsewhere (OR = 3.03, 95%CI 2.48–3.71) and nondeployed Seabees (OR = 2.70, 95%CI 2.11–3.44).
Using lists of eligible veterans from the Department of Defense (DoD), Steele (2000) conducted a population-based survey of veterans who listed Kansas as their home state of record (1,548 deployed and 482 nondeployed) and examined factors that may be related to Gulf War illness. The survey asked about 16 specific medical or psychiatric conditions, 37 symptoms, locations during the Gulf War (including whether the veterans were notified about the Khamisiyah demolitions), and vaccinations. Comparing deployed veterans with the nondeployed veterans after adjustment for sex, age, income, and education level, ORs were elevated for difficulty breathing or catching breath (OR = 4.09, 95%CI 2.49–6.17), persistent cough without a cold (OR = 2.20, 95%CI 1.49–3.26), wheezing in chest (OR = 2.51, 95%CI 1.57–4.01), and moderate or multiple respiratory symptoms (OR = 3.37, 95%CI 2.19–5.18).
Other Coalition Forces Veterans
Using results from the Australian Gulf War Veterans’ Health Study conducted in 2000–2002, Kelsall et al. (2004) examined respiratory health outcomes in 1,456 deployed veterans and 1,588 randomly sampled military personnel who served during the same time period but who were not sent to the Gulf theater. As part of the medical assessment and physical examination, spirometric tests were performed and a respiratory questionnaire was administered. Respiratory symptoms collected included wheeze, cough, sputum, and dyspnea experience in the previous 12 months, with additional more precise circumstances (e.g., wheeze only, wheeze when no cold, and wheeze with breathlessness). Deployed veterans reported all respiratory symptoms more frequently than did the comparison group in analyses that adjusted for age, height, weight, smoking, atopy, education, marital status, service, and rank for all symptoms except morning cough, day or nighttime cough, morning sputum, and nocturnal dyspnea. Table 4-1 summarizes these results.
Sim et al. (2015) reported the results of the Australian Gulf War Veterans’ Follow Up Health Study, which was conducted in 2011–2013. Respiratory health was assessed at both baseline and follow-up, but the scope of respiratory health data collected and the mode of data collection changed for some factors, which limited the ability to assess change over time for some of the outcomes. The follow-up study collected self-reported information on respiratory symptoms and medical conditions, including wheeze, cough, and sputum. Lung function tests were not included at follow-up. Gulf War veterans were statistically significantly more likely than the comparison group to report all measured symptoms of wheeze, cough, and sputum. Estimates were adjusted for age group, service branch, and rank estimated as of August 1990, and any atopy at baseline and current smoking status (never, former, current smoker). Wheeze was reported as overall in the last 12 months (risk ratio [RR] = 1.44, 95%CI 1.15–1.80) and as subcategories of wheeze with breathlessness (RR = 1.34, 95%CI 1.02–1.75) and wheeze present but not a cold (RR = 1.23, 95%CI 1.03–1.47). Three outcomes of cough were also presented, and again Gulf War veterans reported statistically significantly higher prevalence compared with the era veterans after estimates were adjusted: woken by nocturnal cough in the last 12 months (RR = 1.37, 95%CI 1.11–1.69), morning cough (RR = 1.67, 95%CI 1.26–2.23), and day- or nighttime cough (RR = 1.36, 95%CI 1.09–1.70). Questions on sputum were constrained to experience during winter, and the reported occurrences were found to be statistically significantly higher in
TABLE 4-1 Adjusted Odds Ratio (OR) and 95% Confidence Interval (95%CI) for Self-Reported Respiratory Symptoms in the Previous 12 Months in Australian Military Personnel Deployed to the 1990–1991 Gulf War Theater Compared with Nondeployed Era Veterans
| Respiratory Symptom | OR* | 95%CI |
|---|---|---|
| Wheeze only | 1.4 | 1.2–1.7 |
| Wheeze when no cold | 1.6 | 1.3–2.0 |
| Wheeze with breathlessness | 1.8 | 1.3–2.3 |
| Nocturnal chest tightness | 1.4 | 1.1–1.9 |
| Nocturnal cough | 1.4 | 1.1–1.7 |
| Morning cough | 1.2 | 0.9–1.5 |
| Day- or nighttime cough | 1.3 | 1.0–1.6 |
| Morning sputum | 1.2 | 1.0–1.5 |
| Spontaneous dyspnea | 1.6 | 1.1–2.2 |
| Post-exertional dyspnea | 1.3 | 1.1–1.6 |
| Nocturnal dyspnea | 1.5 | 1.0–2.2 |
* OR is adjusted for age, height, smoking, weight, atopy, education, marital status, service, and rank.
SOURCE: Kelsall et al., 2004.
Gulf War veterans than in the era veterans after estimates were adjusted: morning sputum in winter (RR = 1.38, 95%CI 1.10–1.74), day- or nighttime sputum in winter (RR = 1.31, 95%CI 1.06–1.63), and, as a subcategory of the day- or nighttime sputum, sputum most days for 3 months in two successive years (RR = 1.31, 95%CI 1.04–1.65).
Post-9/11 Veterans
As first described and assessed in Long-Term Health Consequences of Exposure to Burn Pits in Iraq and Afghanistan (IOM, 2011) and detailed in Chapter 3, the Armed Forces Health Surveillance Center (AFHSC, 2010) examined medical encounters using ICD-9 codes of Army and Air Force personnel 36 months after deployment to bases/camps with and without burn pits compared with personnel who were deployed to the Republic of Korea or who remained in the United States. Personnel who served within 3 miles of burn pits were considered exposed and were compared with personnel at bases without burn pits and those in the United States who had not deployed. When signs, symptoms, and ill-defined conditions involving the respiratory system and other chest symptoms (ICD-9 786) were examined using Poisson models, the incidence rate ratios (IRRs) were statistically significantly lower for troops deployed to Camp Buehring (no burn pit) (IRR = 0.79, 95%CI 0.67–0.94) and Korea (IRR = 0.91, 95%CI 0.89–0.94) than for the nondeployed U.S. cohort; no other statistically significant associations for the other locations with or without burn pits were found.
Additional analyses of respiratory health outcomes among troops deployed to areas with known burn pits were conducted by linking data AFHSC data with the Millennium Cohort Study. Multivariable logistic regression analyses were performed to evaluate associations between respiratory outcomes and three metrics of exposure within a 5-mile radius of the documented burn pits: dichotomous deployment near the documented burn pits, cumulative days exposed to the burn pits, and exposure to the burn pits at three different bases or camps in Iraq (Balad, Taji, or Speicher). Cumulative days exposed within a 5-mile radius of the documented burn pits were summed and categorized into quartiles, and service members within each of those quartiles were compared with those with no documented exposure to these burn pit sites. Analyses were adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, physical activity, service branch, military rank, pay grade, and occupation. For the analyses of respiratory symptoms, effect estimates were also adjusted for respiratory symptom prevalence at baseline (from the Millennium Cohort Study questionnaire). All covariates were measured at baseline, but smoking status was prospectively assessed using the follow-up questionnaire, as was physical activity. Com-
paring service members deployed within a 5-mile radius of a burn pit with those deployed outside of that radius, no statistically significant differences were seen for the respiratory symptoms of persistent or recurring cough or shortness of breath (OR = 1.04, 95%CI 0.95–1.14). After adjustment no statistically significant associations were found between cumulative days exposed within 5-miles of the documented burn pits and self-reported respiratory symptoms for any of the four quartiles or between respiratory symptoms and specific base/camp sites (p = 0.51) compared with those deployed outside of the 5-mile radius (AFHSC, 2010).
The committee responsible for the 2017 National Academies report Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry carried out an analysis of the initial months of data gathered from respondents to the registry questionnaire as part of its Statement of Task (NASEM, 2017). Based on data that were derived from the first 13 months of completed self-administered questionnaires (n = 46,404), representing approximately 1.0% of 1990–1991 Gulf War veterans and 1.7% of post-9/11 veterans that met the registry’s eligibility criteria, respiratory symptoms were queried using a checklist of symptoms. Those symptoms were cough for more than 3 weeks; sputum or phlegm production for more than 3 weeks; wheezing or whistling in the chest; shortness of breath or breathlessness; decreased ability to exercise; hay fever or other respiratory allergy; sore throat, hoarseness, or change in voice; chest pain, chest discomfort, or chest tightness; and chronic sinus infection or sinusitis. Analyses that reported “any respiratory symptoms” used any affirmative response to the checklist and did not break down reported results by specific symptoms, such as cough or wheeze. Most participants (74.4%) indicated at least one respiratory symptom during or after deployment. Analyses found increasing ORs of reporting “any respiratory symptom” with increasing self-reported exposure to burn pit emissions. Models were adjusted for sex, age, education level, body mass index (BMI), smoking status, unit component, rank, service branch, and occupation.
Update of the Scientific Literature on Respiratory Symptoms
Newer studies evaluating associations between deployment in the Southwest Asia Theater of Military Operations and respiratory symptoms include studies of both post-9/11 veterans and 1990–1991 Gulf War veterans. The studies differ in the exposure evaluated and outcome ascertainment. Several studies of post-9/11 veterans (Abraham et al., 2012; Baird et al., 2012; Krefft et al., 2017; Morris et al., 2014, 2019, 2020; Saers et al., 2017; Smith et al., 2009, 2012; Taylor and Ross, 2019) and two in 1990–1991 Gulf War veterans (Khalil et al., 2018; Maule et al., 2018) assessed exposure based on deployment to Southwest Asia. Some studies evaluated specific in-theater exposures, including deployment to areas with burn pits (Abraham et al., 2014; Rohrbeck et al., 2016; Sharkey et al., 2015, 2016; Smith et al., 2012), blast exposure (Jani et al., 2017a), and depleted uranium exposure in 1990–1991 Gulf War veterans (Hines et al., 2013).
Three studies (Butzko et al., 2019; Klein-Adams, 2019; Morris et al., 2013) were also identified that reported on the frequency of different respiratory symptoms in their respective study populations. Two of these studies (Butzko et al., 2019; Klein-Adams, 2019) used populations of Operation Enduring Freedom/Operation Iraqi Freedom (OEF/OIF) veterans referred to VA’s specialty clinic, WRIISC Airborne Hazards and Burn Pits Center of Excellence, which is one of the research initiatives specified in the Statement of Task. However, because there were no comparison groups included in these three studies, they cannot be used to help inform the association between respiratory symptoms and deployment to Southwest Asia.
Post-9/11 Veterans
Smith et al. (2009) examined newly reported respiratory symptoms (defined as persistent or recurring cough or shortness of breath) and other respiratory conditions among 46,077 Millennium Cohort Study participants who completed baseline (2001–2003) and follow-up (2004–2006) questionnaires. Respiratory symptoms were analyzed by deployment status (deployed versus nondeployed) and by cumulative time deployed (quartiles of days ranging from 0 days [nondeployed, referent group] to >270 days), while stratifying by service branch and controlling for military and demographic characteristics and smoking behavior. Multivariable logistic regression was used to compare the adjusted odds of the newly reported respiratory symptoms for deployed (n = 9,210) versus nondeployed (n = 29,783) participants. New-onset respiratory symptoms were more frequent in the deployed group
than in the nondeployed group (14% vs 10%, respectively). Among the deployed group, new-onset cough was reported by 937 personnel, and shortness of breath was reported by 606 personnel, whereas among the 3,038 nondeployed with new-onset respiratory symptoms, 2,051 reported cough and 1,464 reported shortness of breath. Deployed participants who reported new-onset respiratory symptoms were more likely to be male, to have been born in 1970 or later, to have never married, and to be consistent smokers than nondeployed personnel who reported respiratory symptoms. Smoking status did not significantly modify the relationship between deployment and newly reported respiratory symptoms (p = 0.23). Service branch was found to be a statistically significant effect modifier of deployment and newly reported respiratory symptoms (p <0.0001). Deployment was associated with respiratory symptoms in both Army (OR = 1.73, 95%CI 1.57– 1.91) and Marine Corps (OR = 1.49, 95%CI 1.06–2.08) personnel, but no difference in respiratory symptoms was found for Navy/Coast Guard or Air Force personnel. Deployment length was linearly associated with increased symptom reporting in Army personnel (p <0.0001). Respiratory symptoms were further examined by modeling cough and shortness of breath separately, and the findings were reported to remain consistent, with statistically significantly elevated odds of cough among Army (OR = 1.74, 95%CI 1.56–1.94) and Marine Corps (OR = 1.76, 95%CI 1.22–2.54) personnel and statistically significantly elevated odds of shortness of breath among Army personnel only (OR = 1.64, 95%CI 1.45–1.86). Additional models were used to assess associations between new-onset respiratory symptoms and cumulative deployment duration, adjusted for the same covariates as in the deployed-versus-nondeployed models. Among Army personnel there was an exposure–response relationship between deployment length and increasing adjusted odds of respiratory symptoms (p <0.0001) compared with no days of deployment. For Air Force and Marine personnel, there was no observed exposure–response relationship, and personnel in only one quartile of deployment exposure were found to have statistically significantly increased odds of developing respiratory symptoms compared with those in that same service branch who did not deploy. Although new-onset respiratory symptoms were associated with deployment compared with no deployment, the inconsistency in odds with cumulative exposure time suggests that specific exposures rather than deployment in general are determinants of post-deployment respiratory symptoms. In an analysis of deployed cohort members with self-reported information on deployment location (n = 9,861), 3,474 reported deployment to Iraq exclusively, 373 reported deployment to Afghanistan exclusively, 3,232 reported deploying to both Iraq and Afghanistan or to other locations in support of those military efforts, 486 reported sea-based deployments, 937 reported deployment to other locations, and 1,359 had been deployed to an unknown location. Of these six deployment locations, deployment exclusively to Iraq represented the highest proportion of newly reported respiratory symptoms (18%), followed by deployments exclusively to Afghanistan and to unknown locations (both 14%), deployments to Iraq and Afghanistan or to other countries in support of those efforts (12%), sea-based deployments (9%), and deployments to other locations (8%). Among the examined locations, statistically significant increased adjusted odds of respiratory symptoms were associated with deployment to Iraq exclusively (OR = 2.16, 95%CI 1.52–3.07), deployment to Afghanistan exclusively (OR = 1.87, 95%CI 1.17–2.99), deployment to unknown locations (OR = 1.77, 95%CI 1.22–2.59), and deployment to Iraq and Afghanistan or other countries in support of those operations (OR = 1.68, 95%CI 1.18–2.40). No difference in odds was observed between other deployment locations and respiratory symptoms. This study has a number of strengths, including its large population-based design, use of prospectively collected data on the same individuals, and control of multiple demographic, military, and lifestyle confounders in modeling associations.
Smith et al. (2012) investigated the effects of exposure to documented open-air burn pits within 2, 3, or 5 miles on self-reported respiratory symptoms of persistent or recurring cough or shortness of breath and other respiratory outcomes among Millennium Cohort Study Army and Air Force participants who were deployed to Iraq or Afghanistan after January 1, 2003, and who completed the baseline questionnaire and one of the follow-up assessment cycles through 2008. After individuals with missing data were excluded, 22,297 participants who had deployed were included in the analyses of respiratory symptoms; of these 3,585 had deployed to locations with documented burn pits. Similar proportions of newly reported respiratory symptoms in 2007 were found for those exposed and nonexposed within 3 miles of a burn pit (21.3% vs 20.6%, respectively). Those personnel who were deployed in proximity to documented burn pits were more likely to be younger, less educated, aerobically active, active duty, and to serve in the Army than those deployed to locations outside the 3-mile radius of a documented burn pit. Three proxy exposure metrics were modeled, and analyses were adjusted for demographic and military
characteristics, smoking status, and physical activity. When exposed participants were compared with participants who were deployed to other locations in Iraq and Afghanistan, no statistically significant associations in newly diagnosed self-reported respiratory symptoms were found (OR = 1.03, 95%CI 0.94–1.13). However, when self-reported respiratory symptoms as documented on the 2004–2006 reassessment were compared with those documented on the 2007–2008 assessment, those individuals deployed within a 3-mile radius had statistically significantly and substantially increased odds of continuing to report respiratory symptoms (OR = 4.85, 95%CI 4.49–5.25). No differences were found when service members deployed at each of the three sites with documented burn pits (Joint Base Balad, Camp Taji, or Camp Speicher) were compared with those deployed to areas outside of the 3-mile burn pit exposure radius. Air Force personnel deployed within a 2-mile radius of the burn pit at Joint Base Balad were found to have statistically significantly increased odds for respiratory symptoms (OR = 1.24, 95%CI 1.01–1.52) compared with those deployed to other locations. When investigating the effect of cumulative days exposed within a 3-mile radius of the burn pits, increasing number of days near the burn pits was not associated with the adjusted odds of new self-reported respiratory symptoms (p = 0.94). When examining the risk of respiratory symptoms within a 5-mile radius of the burn pit sites and outside of that radius, no differences were found for cumulative deployment length or camp location.
Morris et al. (2014) conducted a study, termed Study of Active Duty Military for Pulmonary Disease Related to Environmental Deployment Exposures (STAMPEDE I), of 50 active-duty U.S. military personnel recruited within 6 months after they had returned from deployment to Iraq or Afghanistan, all of whom had reported new-onset pulmonary symptoms. Participants completed a deployment questionnaire and underwent a physical exam as well as pulmonary function testing and several other tests and imaging. Largely, frequencies of respiratory symptoms of dyspnea, wheeze, cough, and sputum pre-deployment, during deployment, and post-deployment were reported. The mean frequency of each of the four symptoms continuously increased from pre-deployment to during deployment to post-deployment, although there was no statistical assessment of differences throughout these periods. The most frequent symptom at all three time points was dyspnea. Conclusions that can be drawn from this study are limited by the small number of cases examined at one medical center, the likelihood of referral bias, and the study design that lacked a comparison group, so measures of association could not be estimated.
Using data collected as part of STAMPEDE II, Morris et al. (2019) reported on respiratory health outcomes and the changes in lung function of Army soldiers recruited from Fort Hood, Texas, between 2011 and 2014 before (n = 1,693) and after (n = 843) deployment to Southwest Asia. Participants completed a baseline questionnaire on their respiratory health and underwent examinations that included chest radiography, spirometry, and impulse oscillometry; the questionnaire with additional questions on exposures was administered post-deployment, and each of the lung function tests was also repeated post-deployment. The respiratory symptoms collected by questionnaire were dyspnea, cough, wheezing, sputum production, and exercise intolerance, and for each symptom the frequency of occurrence from never to daily was also collected. The mean frequencies of all symptoms were highest during deployment and lowest pre-deployment. The post-deployment frequency of all symptoms was higher than pre-deployment levels but lower than during deployment levels. The highest mean frequency score (approximately 0.95, classified as mild—occurring less than twice weekly) was for cough during deployment. No clinically or statistically significant increase was found in symptoms during deployment compared with reported pre-deployment levels. Mean symptom scores related to airborne exposures experienced during deployment were quantified as less than mild for cough (0.26 ± 0.43), wheeze (0.08 ± 0.27), dyspnea (0.15 ± 0.35), decreased exercise tolerance (0.10 ± 0.30), and sputum production (0.09 ± 0.28). Logistic regression analysis was applied for spirometric obstruction, with significant results detected only for increasing age, although ORs were elevated for deployed soldiers who self-reported asthma or were obese, smokers, or male. Based on post-deployment symptoms, spirometric results were statistically significantly different only for wheeze between normal versus obstruction groups (mean ± standard deviation of 1.21 ± 0.55 vs 1.41 ± 0.79, p = 0.03, respectively). Smoking behavior changes relative to deployment were not considered when evaluating symptom frequency even though these data were collected pre- and post-deployment. Although respiratory symptoms were found to be elevated during deployment compared with pre- and post-deployment, even the highest levels were considered mild. The pattern of increased symptom prevalence during deployment compared with post-deployment was different from the pattern observed in the first STAMPEDE study, in which the prevalence of respiratory symptoms post-
deployment was higher than during deployment, although only 50 active-duty personnel were included in the earlier investigation (Morris et al., 2014).
Morris et al. (2020) reported on the results of STAMPEDE III, an investigation of clinical lung diseases in 380 military personnel who had deployed to Southwest Asia and reported having chronic respiratory symptoms temporally related to deployment. The post-deployment symptoms were reported to last 4.6 ± 3.6 years. At the time of examination, exertional dyspnea was reported by 75.1% of participants, and decreased exercise tolerance was reported by 72.6% of participants; other symptoms were common but less frequently reported—cough (55.2%), wheeze (42.1%), and sputum production (33.3%). Exertional dyspnea and decreased exercise had mean occurrences of slightly more than twice weekly. Sputum was reported least often. The frequency of self-reported symptoms before, during, and post-deployment all showed statistically significant increases (p <0.001). Frequencies were reported to be highest post-deployment, followed by during deployment, and lowest for before deployment. While data were available, no adjustment or stratification was made for smoking status or specific reported exposures and respiratory symptoms.
Abraham et al. (2012) conducted a cohort and nested case–control study to evaluate the relationship between deployment and respiratory system diseases (ICD-9 460–519) in U.S. military personnel. The cohort, which was created from DoD administrative and medical data, included 44,919 single deployers and 14,695 multiple deployers deployed to OEF/OIF through June 30, 2005. All service members had at least 6 months of data pertaining to visits before and after deployment. The researchers did not find evidence of an increase in respiratory symptoms based on deployment. The rate of respiratory symptom encounters (ICD-9-CM 786) among single deployers (53.8 encounters per 1,000 person-years; 95%CI 50.7–56.8) was higher than among multiple deployers (37.0 encounters per 1,000 person-years; 95%CI 32.6–41.4) in the pre-deployment period. Respiratory symptom rates for both single and multiple deployers increased after deployment. A nested case–control analysis was undertaken to examine the independent effects of deployment status and cumulative time in theater on incident post-deployment obstructive pulmonary disease onset, but primary diagnoses of respiratory symptoms were not included in the case definition. This study had several limitations, such as a lack of measurement of smoking and a lack of specific deployment-related exposure assessments.
Krefft et al. (2017) conducted a pilot study to examine the role of lung clearance index as an early marker of lung injury in a sample of 24 healthy volunteers and 28 symptomatic veterans who had deployed to Southwest Asia in support of post-9/11 operations. The symptomatic deployers had cough, chest tightness, wheezing, shortness of breath, or decreased exercise tolerance during or following deployment. Individuals who were found to have other explanations for their respiratory symptoms were excluded. The healthy controls were at least 18 years of age, had no history of pre-existing lung disease, and reported no respiratory illness in the 4 weeks preceding enrollment and testing. Both groups underwent lung clearance index testing to identify whether abnormalities were present in the peripheral airways of the lung. As part of their clinical evaluation, the veteran group completed testing of pre- and post-bronchodilator spirometry, lung volumes, and diffusing capacity; cardiopulmonary exercise tolerance testing; and chest computed tomography (CT) scans. Surgical lung biopsies were performed on 17 of the 28 veterans. Of the 28 veterans with respiratory symptoms, 17 were found to have definite and 11 were found to have probable deployment-related lung disease. The authors suggested that among veterans who deployed to Southwest Asia and have respiratory symptoms, deployment-related disease may be common. However, the small sample of veterans is highly selective as they were all symptomatic and were seen at an occupational lung disease clinic. Additionally, the study was not designed to evaluate the impacts of deployment to theater on the health of veterans, and no adjustments were made for confounders such as smoking, obesity, or age in the assessments that were made.
Several other studies were identified that focused on specific types of exposures experienced during deployment to the Southwest Asia theater. Of these, the effects of exposure to burn pits have been the most commonly studied (Abraham et al., 2014; Rohrbeck et al., 2016; Sharkey et al., 2015, 2016). Other exposures included fires at a sulfur plant in Iraq (Baird et al., 2012) and blasts (Jani et al., 2017a). In addition to studies of those cohorts that the committee was specifically charged with reviewing, several studies were published using the AFHSC collaborative study, and one study examined outcomes using VA’s Gulf War Era Cohort and Biorepository.
Abraham et al. (2014) built on the AFHSC (2010) analysis by adding an additional 12 months of follow-up (for a total of 48 months) of personnel deployed to four Southwest Asia theater sites with and without burn pits, along
with those deployed to Korea and a comparison population of service members who stayed in the United States. Both studies are described in additional detail in Chapter 3. Compared with the rates for nondeployed personnel, the rate of medical encounters for respiratory symptoms among personnel deployed to the four in-theater sites was elevated, adjusted for age, gender, race, and military rank (IRR = 1.25, 95%CI 1.20–1.30). Information on smoking was not factored into the analyses. Rates for personnel deployed to bases with burn pits (IRR = 1.24, 95%CI 1.19–1.29) and without burn pits (IRR = 1.28, 95%CI 1.20–1.37) were also statistically significantly elevated for respiratory symptoms (as well as for Joint Base Balad, Camp Taji, and Camp Arifjan, individually). Compared with the rates for personnel stationed in Korea, the rates of medical encounters for respiratory symptoms were no different for personnel stationed with exposure to burn pits. In the locations without burn pits, respiratory symptoms at Camp Arifjan were statistically significantly elevated (IRR = 1.12, 95%CI 1.03–1.20), but respiratory symptoms at Camp Buehring were statistically significantly reduced (IRR = 0.83, 95%CI 0.70–0.98). As compared with military personnel deployed at bases without burn pits (Arifjan and Buehring), there was no difference in rates of respiratory symptoms among those deployed in areas with burn pits (Balad and Taji) (IRR = 0.95, 95%CI 0.88–1.03).
The analyses by Sharkey et al. (2015) also used the same deployed and nondeployed populations as the AFHSC (2010) analysis but used a larger U.S.-based reference population and included an additional 12 months of data. Poisson models were adjusted for age, pay grade, sex, race, and service branch in this retrospective cohort study. As was found in the AFHSC (2010) analysis, the risks of respiratory symptoms for personnel deployed to four Southwest Asia bases and Korea were all similar to, or statistically significantly lower than, the risks for personnel who remained in the United States. IRRs were reported for the bases, but no comparisons between bases with and bases without burn pits were made. At 48 months follow-up, adjusted IRRs for “signs, symptoms, ill-defined conditions–respiratory symptoms and other chest symptoms” (International Classification of Diseases, Ninth Revision, Clinical Modification [ICD-9-CM] 786) remained lower for troops deployed to Camp Buehring, Kuwait—which did not have burn pits—than for the nondeployed U.S. reference cohort (IRR = 0.80, 95%CI 0.68–0.94). The same lower risk was observed for troops deployed to Korea compared with the nondeployed at 36 months (IRR = 0.91, 95%CI 0.89–0.94) and 48 months (IRR = 0.93, 95%CI 0.91–0.96). IRRs for personnel deployed to two other bases with burn pits (Joint Base Balad and Camp Taji, Iraq) and one without burn pits (Camp Arifjan, Kuwait) were no different than the nondeployed U.S. reference cohort.
Sharkey et al. (2016) extended the analysis of the data first analyzed by the AFHSC (2010) by adding additional Army or Air Force personnel who were deployed to Kabul (n = 5,670) and Bagram (n = 34,239) Air Force bases in Afghanistan—sites with similar, poor air quality—and Manas Air Force Base in Kyrgyzstan (n = 15,851)—a site with relatively better air quality, and extended the follow-up period of active-duty personnel to 12 years. Cases of symptoms, signs, and ill-defined conditions involving the respiratory system were defined as service members with a single inpatient or outpatient health care encounter coded ICD-9-CM 786 in any diagnostic position. IRRs were calculated and adjusted for age, sex, race, military rank, and prior medical encounters for symptoms, signs, and ill-defined conditions involving the respiratory system. Incidence rates for respiratory symptoms in the Kabul cohort were statistically significantly higher than the rates for personnel from all the other locations except the Manas group. IRRs were highest for Kabul-deployed personnel compared with nondeployed U.S.-stationed personnel (IRR = 1.52, 95%CI 1.43–1.62). Information on smoking was only available for Air Force personnel, and the authors report no evidence of confounding as RRs were similar with and without adjustment for smoking status. The use of ICD-9-CM codes implies severity of respiratory symptoms, and most individuals who have symptoms of cough or shortness of breath are unlikely to seek medical attention unless the conditions worsen or persist.
Rohrbeck et al. (2016) conducted a small study of 200 service members with known exposure to burn pits and 200 matched nondeployed service members, all selected from the Defense Medical Surveillance System, to examine differences in post-deployment respiratory health outcomes. Data from medical encounters, both hospitalizations and outpatient visits, in military treatment facilities were used to capture information on signs, symptoms, and ill-defined conditions involving respiratory system and other chest symptoms (ICD-9 786) regardless of diagnostic position. A total of 33 counts of respiratory symptoms were found in both the deployed cohort (with the majority for those deployed at Joint Base Balad [n = 30] versus Bagram Airfield [n = 3]) and among the nondeployed controls. Incidence rates (IRs) per 1,000 person-years were similar between the deployed cohort (IR = 69.5, 95%CI 45.8–93.2) and the nondeployed cohort (IR = 68.8, 95%CI 45.3–92.3). Using Cox proportional hazards regression, relative risks
were adjusted for age, sex, race/ethnicity, occupation, deployment history, and history of illness prior to deployment and the Bonferroni correction was applied. The risk of respiratory symptoms was found to be decreased for those deployed to Joint Base Balad compared with the nondeployed (RR = 0.41, 95%CI 0.15–1.13), which may be due, in part, to a healthy warrior (deployer) effect. Although burn pit exposure was documented, there was no information on deployment duties, job classification, or specific individual behaviors, including smoking.
Baird et al. (2012) examined the post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant near Mosul, Iraq, in 2003. Two were groups potentially exposed to the sulfur fire smoke plume—personnel involved in fighting the fire (n = 191) and personnel presumably downwind during the time of the fires (n = 6,341). These were compared with two unexposed groups: those that deployed to the area after the fire was extinguished (n = 2,284) and those deployed to other Southwest Asia locations contemporaneously with the time of the fire (n = 1,869). About one-quarter of presumed exposed personnel reported a change in health for the worse during deployment; health concerns were reported by 39% of the firefighters and 23% of the personnel downwind of the fires. Furthermore, 24% of firefighters self-reported cough, and 31% reported difficulty breathing. In the downwind group, 16% reported cough, and 14% reported shortness of breath. Overall, the frequency of encounters for respiratory signs, symptoms, and ill-defined conditions (ICD-9-CM 786) increased post-deployment, relative to the pre-deployment period for all four groups, but was statistically significant among the downwind group only. The age-adjusted standardized morbidity ratio for signs, symptoms, and ill-defined conditions involving the respiratory system and chest (ICD-9-CM 786) was not statistically significantly different from 1.0 when firefighters were compared with the contemporaneously deployed group (morbidity ratio = 1.05, 95%CI 0.61–1.61) but was statistically significantly decreased when firefighters were compared with the group deployed to the area before or after the fire (morbidity ratio = 0.57, 95%CI 0.33–0.88). Regarding the potentially exposed personnel who were deployed downwind of the fires, the standardized morbidity ratio for signs, symptoms, and ill-defined conditions involving the respiratory system and chest was slightly elevated when compared with the contemporaneously deployed group (morbidity ratio = 1.08, 95%CI 1.0–1.17) and statistically significantly decreased compared with the group deployed to the area before or after the fire (morbidity ratio = 0.58, 95%CI 0.54–0.63). Because the authors were concerned that differential misclassification bias would be introduced if the accuracy and completeness of post-deployment survey data was not independent of exposure to the sulfur fire in this population, comparisons of outcomes between the exposed and the unexposed group were not made. Confounding due to potential uncharacterized differences in risk factors, such as smoking behavior and other environmental or occupational exposures, between the sulfur fire exposed and unexposed groups cannot be ruled out.
Blast exposures were another common exposure of post-9/11 deployments. Jani et al. (2017a) used the responses of 42,558 service members and veterans who had participated in the Airborne Hazards and Open Burn Pit Registry between 2014 and 2015 to assess the association between self-reported blast exposure and self-reported current dyspnea or decreased ability to exercise. Blast exposure was reported by 74% of respondents overall—79% of those with current symptoms and 66% of those without current symptoms. Current dyspnea was reported by 61% of respondents. Following adjustment for self-reported age; sex; branch of service; BMI; smoking status; exposure to burn pit smoke; nonmilitary occupational exposure to dust, gas, smoke, chemical vapors, or fumes; and time since deployment, the odds of dyspnea or decreased ability to exercise were increased (OR = 1.66, 95%CI 1.5–1.7) among the group with blast exposure as compared with military personnel without blast exposure. This finding is limited by the self-selected voluntary nature and the reliance on self-reported exposures and outcomes of the registry data.
Other Coalition Forces Veterans
Two studies of foreign military service personnel were identified. In the first (Taylor and Ross, 2019) British service personnel stationed in Kabul, Afghanistan, a highly polluted city, from December 2016–August 2017 completed a respiratory health questionnaire that collected information on nasal congestion, shortness of breath, wheeze, cough, and sputum. Comparisons were made between service members stationed at a base in Kabul and those stationed on the outskirts of Kabul as well as between service members deployed over winter and over summer. The prevalence of symptoms of nasal congestion, shortness of breath, wheeze, and cough were higher among those stationed in the center of Kabul than in the outskirts, and these symptoms were reported to be higher in the winter season (ranging from approximately 50% to 80% in central
Kabul, depending on the symptom, and from 50% to 65% in the Kabul outskirts), which had higher air pollution concentrations than the spring (ranging from approximately 40% to 55% in central Kabul and from 15% to 45% in the Kabul outskirts). The higher prevalence of symptoms reported by those stationed in central Kabul, regardless of the season, than in those stationed in the city outskirts suggests that urban air pollution could have played a role in the differences in the frequency of symptoms that were reported.
Saers et al. (2017) examined the prevalence of self-reported respiratory symptoms (wheeze, wheeze with breathlessness, wheeze without a cold, nocturnal chest tightness, nocturnal breathlessness, and nocturnal cough) in the previous 12 months in a random sample of 1,032 Swedish military personnel from selected units (response rate 50%). Military personnel were either currently or previously stationed in Kosovo (in the period 2005–2008) or Afghanistan (2008–2009) and were matched on age, gender, smoking habits, BMI, and education level using a ratio of 1:1 to a general population sample of people who had participated in the Global Asthma and Allergy European Network study. The prevalence of all symptoms except nocturnal chest tightness and nocturnal breathlessness was statistically significantly increased (p <0.05) in the military personnel compared with the matched sample from the general population. The most common of the reported symptoms for the military versus the comparison group was nocturnal cough (26.6% vs 17.2%), and the least frequent symptom was nocturnal breathlessness (4.2% vs 4.1%). Analyses with logistic regression also showed statistically significantly increased odds of wheeze, wheeze with breathlessness, wheeze when not having a cold, and nocturnal cough in the military population compared with the general population. No difference in the prevalence of respiratory symptoms was found for military personnel who were stationed in Afghanistan (n = 682) versus Kosovo (n = 393). Within the group stationed in Afghanistan, an increasing number of months spent deployed was associated with increased odds of wheeze (p = 0.002), wheeze with breathlessness (p = 0.001), and nocturnal cough (p = 0.046). Military personnel who reported having been exposed to sandstorms had a higher prevalence of nocturnal coughing than those who were not exposed (29.6% vs 16.2%, p = 0.002). Duties that required regular transportation in vehicles versus duties that were more stationary were associated with a higher prevalence of wheeze (18.1% vs 11.4%, p = 0.046), wheeze with breathlessness (11.8% vs 5.1%, p = 0.02), and nocturnal chest tightness (10.2% vs 3.8%, p = 0.01). The finding of no difference in symptom prevalence between those stationed in Afghanistan and Kosovo calls into question the role of Southwest Asia deployment as a cause of the differences in prevalence relative to the general population.
1990–1991 Gulf War Veterans
Khalil et al. (2018) described the study design for the Gulf War Era Cohort and Biorepository, which was established by VA to be a nationally representative longitudinal cohort of U.S. veterans who served during the 1990–1991 Gulf War era. The pilot phase of the effort enrolled 1,275 veterans who completed all study requirements and were frequency-matched to the geographic distribution of the recruitment panel across U.S. Census regions; 900 (70.6%) of the veterans deployed to the Southwest Asia theater. Self-reported health outcomes of symptoms (in the past year) and health care provider–diagnosed conditions were stratified by users (n = 584) and nonusers (n = 679) of VA health care. Three respiratory symptoms were included, and for each the VA users reported higher frequencies than nonusers in the past 6 months: difficulty breathing or shortness of breath (43.5% vs 24.7%), frequent coughing without also having a cold (37.3% vs 23.3%), and wheezing (28.8% vs 16.3%). While the reported proportions of veterans with symptoms seem high, there was no formal assessment of differences in the frequency of symptoms between VA users and nonusers. Furthermore, there were no comparisons between deployed and nondeployed veterans and, hence, these results do not inform questions about the role of Gulf War deployment on increased risks of respiratory symptoms.
Hines et al. (2013) examined 37 1990–1991 Gulf War veterans who were enrolled in the VA Depleted Uranium Surveillance Program and had attended a biennial follow-up in 2011 to compare the likelihood of pulmonary health abnormalities in those with high body burdens of uranium (n = 12; >0.1 µg/g creatinine) versus those with low body burdens of uranium (n = 25; ≤0.1 µg/g creatinine). Using 24-hour creatinine-corrected urinary uranium as a validated marker of exposure, no statistically significant differences in the prevalence of any respiratory symptom—frequent cough, coughing up phlegm, shortness of breath, or wheezing—were observed in those with high versus low urinary uranium. Because smokers often report respiratory symptoms, the frequency of symptoms was also
compared between ever smokers and never smokers; the only symptom more frequently reported in ever smokers versus never smokers was frequent cough (p = 0.05). While the findings from this study made use of a rigorous exposure assessment through analysis of uranium in urinary samples, the findings are not particularly pertinent to this assessment, given that exposure to depleted uranium was uncommon.
Maule et al. (2018) conducted a meta-analysis of 21 studies published through 2017 on the prevalence of health symptoms, including respiratory symptoms, with those 21 studies representing more than 129,000 1990–1991 Gulf War–deployed and nondeployed era veterans. In pooled analyses, a higher combined prevalence of respiratory symptoms was found for deployed than for era veterans: coughing (19.2% vs 9.1%), wheezing (17.5% vs 8.6%), and shortness of breath (14.9% vs 5.1%). The bias assessment also demonstrated that Gulf War–deployed veterans continued to have higher odds of reporting all analyzed symptoms than Gulf War–era controls. ORs were reported for each symptom along with I2 statistics (a measure of the heterogeneity, or the percentage of variation across studies that is due to heterogeneity rather than chance). Although the odds of all respiratory symptoms were statistically significantly increased for Gulf War veterans compared with era veterans—shortness of breath (OR = 2.81, 95%CI 2.35–3.35; 6 studies), coughing (OR = 2.02, 95%CI 1.72–2.38; 11 studies), and wheezing (OR = 1.92, 95%CI 1.66–2.22; 5 studies)—the heterogeneity was considerable (>0.7) for all outcomes. The meta-analytic approach could not address concerns about either selection biases or information biases (due to self-reports of symptoms), which were common to all the included studies. However, the committee found that the methods used in this meta-analysis fairly summarize reported findings on respiratory symptoms, and the bias assessment provides assurance that reporting bias played little role. Moreover, the committee also notes that some other important deficiencies in the published studies, such as individual design and population selection, and their impacts on the findings were not addressed.
Synthesis
Previous reports in the Gulf War and Health series have concluded that “studies of Gulf War veterans based on self-reported symptoms and self-reported diagnoses have frequently, but inconsistently, shown an excess of respiratory conditions” (NASEM, 2016, p. 151). This conclusion was confirmed by the results of a recent meta-analysis of 21 studies of 1990–1991 Gulf War veterans that used self-reported respiratory symptoms (Maule et al., 2018).
Respiratory symptoms are generally presented as a group and may include cough, wheeze, dyspnea or shortness of breath, sputum or phlegm, exercise intolerance, and other nonspecific symptoms or symptoms that appear under specific conditions, such as “morning cough.” In the assessment of the first 13 months of Airborne Hazards and Open Burn Pit Registry data, at least one respiratory symptom of 13 possible symptoms was reported by 74.4% of participants.
The committee identified and evaluated 16 studies that evaluated associations between respiratory symptoms among post-9/11 veterans and 3 studies among 1990–1991 Gulf War veterans and deployment in the Southwest Asia Theater of Military Operations. The studies differ in how exposure was evaluated (e.g., deployment versus specific in-theater exposures) and in the heterogeneity of the respiratory symptoms assessed. Findings from these more recent studies are largely in line with those reported previously, with mixed evidence about associations between deployment and respiratory symptoms. In contrast to use of deployment to the Southwest Asia Theater of Military Operations as a metric for exposure, there were too few studies about specific exposures (e.g., burn pit exposure, blast exposure, or exposure to depleted uranium) upon which to base an assessment.
Among the research cohorts that were included in the committee’s Statement of Task, two studies from the Millennium Cohort Study and three studies from STAMPEDE evaluated respiratory symptoms in their respective populations. Among Millennium Cohort Study participants with follow-up through 2006, differences were detected by service branch, respiratory symptom, and exposure metric. For example, following adjustment for smoking and other risk factors, Smith et al. (2009) found positive associations between deployment and new-onset respiratory symptoms only for Army and Marine Corps personnel. When modeled separately, positive associations for cough were found for both Army and Marine Corps personnel, whereas odds of shortness of breath were elevated only among Army personnel. Furthermore, an increasing exposure–response relationship was found between duration of deployment and new-onset respiratory symptoms for Army personnel, but not for the other service branches.
In another analysis of the Millennium Cohort Study with the same follow-up as Smith et al. (2009), but restricted to Army and Air Force personnel who had deployed to locations with burn pits, Smith et al. (2012) reported no significant associations in newly diagnosed self-reported respiratory symptoms between those deployed to areas within 5 miles or 3 miles of burn pits compared with personnel deployed outside of the burn pit buffer zones; nor were there differences by base site. In addition, no significant associations were found when evaluating cumulative days exposed, deployment to a specific burn pit site, or deployment within a 2-mile radius of a burn pit, except for the latter metric, where U.S. Air Force personnel deployed to Joint Base Balad were found to have increased odds for respiratory symptoms relative to those deployed to other locations.
Three studies of STAMPEDE (Morris et al., 2014, 2019, 2020) examined respiratory symptoms. In the first analysis of 50 active-duty U.S. military personnel recruited within 6 months after they had returned from deployment to Iraq or Afghanistan (Morris et al., 2014), there is evidence of service personnel reporting increased frequency of dyspnea, wheeze, cough, and sputum continuously from pre-deployment to during deployment and post-deployment, with dyspnea being more frequently reported than the other respiratory symptoms. In a larger study of changes in respiratory health outcomes with data that were collected before and after deployment to Southwest Asia—STAMPEDE II—the proportion of service personnel reporting cough, dyspnea, and wheeze was higher post-deployment and during deployment than pre-deployment, with slightly lower frequencies postdeployment than during deployment (Morris et al., 2019). Although information on smoking was collected both pre- and post-deployment, it appears not to have been used in modeling differences. Because smoking rates typically increase during deployment, the lack of accounting for changes in cigarette smoking habits somewhat limits confidence in the conclusions that can be drawn from this otherwise strong study. A third study—STAMPEDE III—of 380 military personnel who had deployed to the Southwest Asia theater and reported having chronic respiratory symptoms similarly found that the frequency of self-reported symptoms pre-, during, and post-deployment all showed statistically significant increases (p <0.001) (Morris et al., 2020). Although information on smoking was collected in STAMPEDE both pre- and post-deployment, it appears not to have been used in these studies in making comparisons in changes in symptom frequency over time. Because smoking rates typically increase during deployment (Meadows et al., 2018), the lack of accounting for cigarette smoking habits limits the conclusions that can be drawn from this otherwise strong study.
Of the three studies of 1990–1991 Gulf War veterans reviewed, the most informative was the meta-analysis of 21 studies on prevalence of health symptoms, including respiratory symptoms, representing more than 129,000 1990–1991 Gulf War–deployed and nondeployed era veterans (Maule et al., 2018). In pooled analyses higher prevalence of coughing, wheezing, and shortness of breath was found for deployed than era veterans, and the odds of all three respiratory symptoms were statistically significantly increased for Gulf War veterans compared with era veterans, although the heterogeneity was considerable. While the findings from Hines et al. (2013) made use of a rigorous exposure assessment through analysis of uranium in urinary samples, the findings are not particularly pertinent, given that exposure to depleted uranium was uncommon.
Overall, the studies reviewed by the committee were subject to many of the same limitations as previously reviewed studies (lack of specific or objective exposure information or stratification of personnel by military occupations, lack of adjustment for potential confounding factors such as smoking). However, at least one study reported similar findings in models with and without cigarette smoking (Sharkey et al., 2016); therefore, there is a need to confirm the role of smoking as a potential confounder in future investigations given that the lack of control for smoking is often identified as a weakness in studies of military health. Some studies used ICD-9 codes—specifically 786 for signs, symptoms, and ill-defined conditions of the respiratory system—contained in medical encounter databases to attempt to overcome the subjective nature of symptom reporting. Use of this ICD-9 code also has some limitations, including that medical encounters outside of the administrative database population are not captured (such as visits that occur outside of DoD facilities), medical encounters capture only the more severe of the symptom spectrum, and outcome misclassification based on ICD coding is inevitable. However, the documentation of symptoms using ICD-9 codes and the ability to estimate incidence rates are important strengths.
Given the findings from all the reviewed studies, the available evidence suggests an association between service in the Southwest Asia theater and respiratory symptoms. Nonetheless, many of these studies have the potential for information bias, and some of them are also subject to potential selection bias due to the self-selection of partici-
pants into the studies, if those with symptoms and in-theater exposures are more likely to participate. The greatest concern for bias due to confounding relates to those studies in which there was no control for cigarette smoking.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is limited or suggestive evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of respiratory symptoms.
UPPER AIRWAY DISORDERS
The upper airway serves several critical functions. It is the first respiratory mucosa to encounter inhaled particulate matter (PM), gases, and fumes; it warms and humidifies inhaled air and filters large particles, including many common allergens; and it is the primary adsorptive surface for water-soluble gases, such as formaldehyde. It also removes substantial quantities of less soluble gases, such as ozone. Obstruction of the nasal passages may result in a change from nasal to oral breathing, especially with exertion. Oral breathing bypasses the filtering functions of the nose, increasing the hazard to the lower airways and the lungs (Bascom and Raford, 1994).
Rhinitis and Sinusitis
Rhinitis may be a consequence of mucosal irritation (irritant rhinitis) or immunological response (allergic rhinitis). Both seasonal and perennial antigens may cause allergic rhinitis, with the dominant antigens varying by region. Although recent research has focused primarily on the home as an important source of exposure to antigens such as house dust mites, cockroaches, and rodents, the workplace (e.g., office buildings) is also an important potential source of these antigens. There is some evidence, as has been demonstrated in relation to immunoglobin E (IgE)-mediated asthma, that exposure to environmental irritants such as ozone may enhance the likelihood of allergic rhinitis (Higgins and Reh, 2012); likewise, nasal instillation of diesel exhaust particles can increase in vivo IgE and cytokine production at the human upper respiratory mucosa, exacerbating allergic inflammation (Díaz-Sanchez et al., 1999). Allergic rhinitis typically presents with sneezing, rhinorrhea, and nasal congestion and may accompany occupational asthma. Symptoms may be immediate (occurring soon after exposure) or delayed (late-onset symptoms 8–24 hours after exposure). Upper respiratory sensitizers, including protein allergens (e.g., flour dust or laboratory animals) and low-molecular-weight chemicals (e.g., isocyanates), have been documented to cause work-related allergic rhinitis (Bascom and Raford, 1994). Around 19.9 million adults in the United States are diagnosed with allergic rhinitis per year, representing an annual incidence of around 8.1% of the adult population4 (CDC, 2017).
Irritant rhinitis is defined as rhinitis symptoms induced by dusts, chemicals, or fumes that are noxious to tissues. The mechanism is generally considered to be an activation of the sensory irritant receptors. The symptoms are similar to those of allergic rhinitis and may be due to exposures to chemicals such as formaldehyde and environmental tobacco smoke. The list of chemical agents known to cause irritant rhinitis is lengthy and most often dose dependent. The optimal treatment is avoidance (Bascom and Raford, 1994). In the United States, there are approximately 30 million people with irritant rhinitis (Scarupa and Kaliner, 2009).
Sinusitis is an inflammation in the sinuses. The frontal, ethmoid, maxillary, and sphenoid sinuses are paired cavities, lined with mucosa, in the anterior portion of the skull. Symptoms and signs suggesting acute sinusitis include purulent nasal discharge, facial pain or tenderness, nasal congestion, fever, and cough. Chronic sinusitis often presents with protracted nasal congestion, nasal discharge, and facial pain. Sinusitis is often preceded by a viral upper respiratory infection. Local edema, allergic rhinitis, and nasal polyps may obstruct the sinus ostium, leading to acute or chronic disease. Exposure to tobacco smoke, air pollutants, and several chemicals has been
___________________
4 Table A-2a. See https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2017_SHS_Table_A-2.pdf (accessed July 3, 2020).
shown to cause or exacerbate sinus disease. Around 30.8 million adults in the United States have been diagnosed with chronic sinusitis, representing a prevalence of around 12.5% of the adult population5 (CDC, 2017).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms as a group, which has included rhinitis and sinusitis when present. No conclusion was made specific to rhinitis or sinusitis. No studies reviewed in these previous volumes reported on outcomes of rhinitis, and only one study (Kang et al., 2000) reviewed in Volume 4, included sinusitis as a distinct health outcome. Kang et al. (2000) used information collected as part of VA’s NHS survey, a population-based retrospective cohort design, to estimate the prevalence of symptoms and other health outcomes in Gulf War veterans (n = 15,000) compared with era veterans (n = 15,000). Population prevalence rates were calculated using statistical analysis techniques to account for stratified random sampling of unequal probabilities of selecting various strata. Compared with nondeployed era veterans, Gulf War–deployed veterans had a significantly higher symptom prevalence of sinusitis experienced in the 12 months before the survey: 38.6% for deployed versus 28.1% for the nondeployed (RD = 10.47, 95%CI 10.32–10.62). Estimates were not adjusted for smoking or other factors.
As first described in the Respiratory Symptoms section, using results from the Australian Gulf War Veterans’ Health Study conducted in 2000–2002, Kelsall et al. (2004) investigated whether Australian Gulf War veterans had a higher-than-expected prevalence of recent symptoms and medical conditions that were first diagnosed in the period following the 1990–1991 Gulf War, and whether effects were associated with exposures and experiences that occurred during deployment. Self-reported “sinus problems” that were first diagnosed in 1991 or later were more frequent in Gulf War veterans than in the era veterans (11% vs 7%, respectively), and the difference was statistically significant after adjustment for service type, rank, age, education, and marital status (OR = 1.5, 95%CI 1.1–2.0). When sinus problems that were first diagnosed in 1991 or later were rated as “possible or probable” based on an assessment by a research team doctor, they were again more frequent in Gulf War veterans than in the era veterans (10% vs 7%, respectively), and the difference was again statistically significant after adjustment for service type, rank, age, education, and marital status (OR = 1.5, 95%CI 1.1–2.0).
Sim et al. (2015) reported on the results of the Australian Gulf War Veterans’ Follow Up Health Study, which was conducted in 2011–2013. Gulf War veterans were statistically significantly more likely than the comparison group to report doctor-diagnosed sinus problems (RR = 1.51, 95%CI 1.07–2.15), adjusted for age group, service branch, and rank estimated as of August 1990, for any atopy at baseline, and for current smoking status (never, former, current smoker).
The 2011 report on the long-term health consequences of burn pit exposure in Iraq and Afghanistan included studies of surrogate populations (firefighters, incinerator workers, communities near incinerators) who were exposed to chemicals known to be associated with burn pit emissions and primarily relied on Gulf War and Health: Volume 8 (IOM, 2010) for conclusions on the association between exposure and health outcomes in service members and veterans, except when new studies were identified. As in the Gulf War and Health series reports, conclusions on the association between exposure to burn pit emissions and respiratory symptoms, conditions, and diseases were presented as a group, and no studies of rhinitis or sinusitis were identified in service members or veterans (IOM, 2011).
Update of the Scientific Literature on Sinusitis and Rhinitis
Thirteen studies were identified that examined the occurrence of post-deployment rhinitis or sinusitis or both. However, five of the studies (Butzko et al., 2019; Dursa et al., 2016a; Korzeniewski and Brzozowksi, 2011; Korzeniewski et al., 2013; Sanders et al., 2005)—one of which was conducted by WRIISC investigators (Butzko et al., 2019)—did not include appropriate comparison groups or only provided descriptive statistics, and thus could not provide information to contribute to inferences that can be made regarding deployment to Southwest Asia and
___________________
5 Table A-2a. See https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2017_SHS_Table_A-2.pdf (accessed July 3, 2020).
sinusitis and rhinitis. For example, Dursa et al. (2016a) used data collected from the NewGen survey to examine the health outcomes of OEF/OIF veterans who use VA health care services and those who do not; however, although the models were adjusted for deployment to OEF/OIF, the inferences that can be made on the association between deployment to Southwest Asia and sinusitis are too limited to be considered informative.
Post-9/11 Veterans
Two of the studies (Barth et al., 2014, 2016a) used data collected from VA’s NewGen survey (detailed in Chapter 3) to examine the population prevalence of three self-reported doctor-diagnosed respiratory conditions (asthma, bronchitis, and sinusitis) in veterans who had deployed to Southwest Asia and those who had not. Barth et al. (2014) examined the association between deployment to Southwest Asia and self-reported doctor-diagnosed sinusitis among 13,162 deployed and 7,401 nondeployed veterans. Unweighted and weighted prevalences of sinusitis were calculated and stratified by time of diagnosis (before or after 2001), and logistic regression was used to calculate adjusted ORs for deployment status and sinusitis. Models were adjusted for birth year, sex, service branch, unit component, race/ethnicity, education, and smoking status. Separate models were constructed for diagnosis before 2001 and during or after 2001. For respiratory conditions diagnosed before 2001, the weighted prevalence for sinusitis was higher in the nondeployed group than in the deployed group (7.8% vs 4.9%). Among those with respiratory disease diagnosed prior to 2001, the weighted prevalence of sinusitis was higher in the deployed than in the nondeployed group (6.9% vs 5.6%). Among those with respiratory disease diagnosed during or after 2001, the deployed group had statistically significantly greater odds of sinusitis compared with nondeployed veterans (OR = 1.30, 95%CI 1.13–1.49). The observed effect of deployment was statistically significantly decreased among veterans with sinusitis diagnosed prior to 2001 (OR = 0.72, 95%CI 0.63–0.82).
Barth et al. (2016a) again used the NewGen data to expand on the analysis by Barth et al. (2014) to examine the prevalence of respiratory diseases and their association with self-reported respiratory exposures during military service for OEF/OIF deployed and nondeployed veterans. Logistic regression analyses were used to calculate weighted, adjusted odds of respiratory disease stratified by deployment status and controlled for sex, birth year, race/ethnicity, education, smoking status, unit component, service branch, and number of OEF/OIF deployments. Of the 3,190 veterans who self-reported doctor-diagnosed sinusitis, 15.1% (weighted) had no deployments, and 15.5% (weighted) had three or more deployments. Sinusitis was most frequent among women (22.6% weighted), those who served in the Air Force (17.6% weighted), those who had an advanced degree (22.0% weighted), and those who identified as former smokers (21.7%). Stratified by deployment status, 13% (weighted) of veterans with sinusitis were deployed to OEF/OIF, and 14.9% (weighted) of veterans with sinusitis were nondeployed. Whereas among all deployed veterans 95% (weighted) reported at least one respiratory exposure, only 13.1% (weighted) of the deployed with a diagnosis of sinusitis reported any respiratory exposure. Among deployed veterans, statistically significant increased odds of sinusitis were observed for all specific exposures and for both the high-exposure and low-exposure categories; the highest odds for sinusitis were for those categorized as high exposure (OR = 2.11, 95%CI 1.58–2.81) and for those who reported exposure to dust and sand specifically (OR = 1.80, 95%CI 1.44–2.23). For nondeployed veterans, statistically significant increased odds of sinusitis were also observed for all specific exposures and for both the high-exposure and low-exposure categories; the highest odds for sinusitis were again for those who were categorized as high exposure (OR = 2.54, 95%CI 2.00–3.21), and among specific exposures, industrial pollution had the highest odds (OR = 1.81, 95%CI 1.52–2.15). These results show that exposures were associated with the development of sinusitis in both deployed and nondeployed groups. A strength of this analysis is that it attempted to characterize the types of exposure associated with clinical respiratory outcomes.
Smith et al. (2008) used self-reported clinician-diagnosed health data from regular, active-duty participants from the first panel (2001–2003) of the Millennium Cohort Study (n = 37,798) to compare the agreement of 38 medical conditions—including sinusitis—with that obtained from electronic medical records based on ICD-9-CM codes. Any diagnostic code for these 38 conditions in any portion of the medical record indicated agreement with a self-reported medical condition of interest. Positive and negative agreement was used to compare self-reported data with those from electronic medical records. Prevalence of sinusitis (considered to be more likely to be acute or transient) was 14.8% (95%CI 14.5–15.1) for self-reported and 13.9% (95%CI 13.5–14.2) for the electronic medical record; 8.8% were exclusively recorded in the electronic medical record. The positive agreement between self-report and electronic medical record was 35.7%, and negative agreement (the condition was
not reported either by self-report or found in the medical record) was 89.2%. Sinusitis was examined by length of service in years, and the prevalence and agreement values varied with increasing length of service. In most cases, both prevalence and positive agreement increased with longer time in service. For example, the prevalence of sinusitis based on self-report increased from 8.7% among those with 0–5 years of service to 20.6% among those with ≥16 years of service. The prevalence of sinusitis based on electronic medical records increased from 12.8% among those with 0–5 years of service to 15.0% among those with 11–15 years of service but decreased to 14.2% for those with ≥16 years of service. For individuals with up to 10 years of service, the self-reported prevalence of sinusitis was lower than what was recorded in the electronic medical records.
Baird et al. (2012) examined the post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant near Mosul, Iraq, in 2003. Two groups were potentially exposed to the sulfur fire smoke plume—personnel involved in fighting the fire (n = 191) and personnel presumably downwind during the time of the fire (n = 6,341). These were compared with two unexposed groups: those that deployed to the area after the fire was extinguished (n = 2,284), and those deployed to other Southwest Asia locations contemporaneously with the time of the fire (n = 1,869). Rhinitis was assessed by comparing the percentage of those that reported runny nose (34% of firefighters and 28% in the downwind group); however, statistical testing of these differences was not conducted, limiting the informativeness of this study regarding an association between deployment and rhinitis.
Other Coalition Forces Veterans
Taylor and Ross (2019) conducted a study of UK service personnel who completed a respiratory questionnaire and who were stationed in Kabul, Afghanistan, a highly polluted city, in 2016–2017. The self-reported prevalence of nasal congestion was higher for personnel stationed in a compound in the center of Kabul than for those stationed in the outskirts of Kabul (96% vs 52%, respectively), suggesting that urban air pollution could have been responsible for the higher rates of symptoms. This study is limited in that it did not conduct statistical analyses of these differences or adjust for confounders and that it relied on self-reported symptoms.
1990–1991 Gulf War Veterans
Hooper et al. (2008) used DoD administrative data to examine the long-term hospitalization experiences, based on ICD-9-CM codes, of regular active-duty U.S. Gulf War veterans (n = 211,642) still on active duty between 1994 and 2004 (presented at 3-year intervals) versus veterans who had separated from military service (n = 321,806). For the 10-year combined observation period, there were 43,346 hospitalizations for those who remained on active duty after 1994. Of those hospitalizations, 12.2% (n = 2,872) were coded as being related to the respiratory system. For each diagnostic category, the top five primary diagnoses over the entire follow-up period were presented. Chronic sinusitis ranked fifth, at 8.9% (n = 255) of inpatient hospitalizations for respiratory diseases. Of the 4,031 veterans hospitalized for ill-defined conditions, 46.6% had respiratory system and other chest symptoms. Comparisons with the separated veteran group were not presented, nor were there comparisons of hospitalizations by specific Gulf War exposures, making this primarily a descriptive study and limiting its informativeness.
One study that used an objective measure of exposure to examine a variety of respiratory symptoms (including sinus trouble and frequent runny nose) was a study of those accidentally exposed to depleted uranium; the exposure was estimated objectively using an exposure biomarker (Hines et al., 2013). A subset (n = 37) of 1990–1991 Gulf War veterans who were enrolled in the VA Depleted Uranium Surveillance Program and had attended a biennial follow-up in 2011 were examined to compare the likelihood of pulmonary health abnormalities in those with high body burdens of uranium (n = 12; >0.1 µg/g creatinine) versus those with low body burdens of uranium (n = 25; ≤0.1 µg/g creatinine). Using 24-hour creatinine-corrected urinary uranium as a validated marker of exposure, no statistically significant differences in the prevalence of sinus trouble or frequent runny nose were observed in those with high versus low urinary uranium. Because smokers often report respiratory symptoms, the frequency of symptoms was also compared between ever smokers and never smokers; frequent runny nose and sinus trouble were not reported more frequently by ever smokers than by never smokers. While the findings from this study made use of a rigorous exposure assessment through analysis of uranium in urinary samples, the findings are not particularly pertinent to this assessment given that exposure to depleted uranium was uncommon.
Maule et al. (2018) conducted a meta-analysis on the prevalence of health symptoms, including sinus congestion, using 21 studies published through 2017, representing more than 129,000 1990–1991 Gulf War–deployed and nondeployed era veterans. In pooled analyses a higher combined prevalence of sinus congestion was found for deployed than for era veterans (40.4% vs 24.9%, respectively). ORs were reported for each symptom along with I2 statistics. Although the odds of sinus congestion were statistically significantly increased for Gulf War veterans compared with era veterans (OR = 1.63, 95%CI 1.46–1.81; nine studies), the heterogeneity was considerable (I2 = 0.75). The meta-analytic approach could not address concerns about either selection biases or information biases (due to self-reports of symptoms), which were common to all of the included studies. However, the committee found that the methods used in this meta-analysis fairly summarize reported findings on symptoms of sinus congestion, and the bias assessment provides assurance that reporting bias played little role. Moreover, the committee also notes that some other important deficiencies in the published studies, such as individual design and population selection and their impacts on the findings, were not addressed.
Synthesis
Volumes 4, 8, and 10 of the Gulf War and Health series addressed respiratory symptoms as a group and included rhinitis and sinusitis when present. None of these volumes reported a conclusion that was specific to rhinitis or sinusitis. The 2011 National Academies report on the long-term health consequences of burn pit exposure also presented respiratory symptoms, conditions, and diseases as a group, but it did not identify any studies of rhinitis or sinusitis in service members or veterans (IOM, 2011).
This report summarizes eight new studies that examined the occurrence of post-deployment sinusitis; five were conducted using populations of post-9/11 personnel, and three studies used 1990–1991 Gulf War veterans. Although symptom reports of sinusitis for deployed veterans were generally found to be increased, the inferences that can be drawn from these results are limited due to poor exposure characterization, namely using deployment as a surrogate for exposures encountered in theater; using data based only on self-report and recall; and presenting conclusions regarding deployment without taking into account details such as the number of deployments, the total days of deployment, or deployment to areas other than Southwest Asia. Furthermore, only some of the studies reviewed by the committee controlled for confounders, and those that did, did so incompletely, leading to uncertainty about whether a deployment-related effect was being observed.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of rhinitis or sinusitis.
Vocal Cord Dysfunction
Vocal cord dysfunction is characterized by paradoxical closure of the vocal cords during inspiration and sometimes exhalation. Signs and symptoms of vocal cord dysfunction resemble those of laryngeal edema, vocal cord paralysis, and frequently asthma. It is a functional disorder that serves as an important mimicker of asthma. Wheezing or stridor and acute shortness of breath are typical and are often dramatic, with the appearance of acute respiratory failure. Vocal cord dysfunction is most likely due to laryngeal hyper-responsiveness, with increased sensitivity of the laryngeal sensory receptors and heightened response of the glottic closure and cough reflexes to a number of triggers. Exercise and psychological factors have been identified as triggers. Exposure to irritants, including chemicals such as chlorine, ammonia, perfume, and other odors in the workplace, have been linked with vocal cord dysfunction. The diagnosis of vocal cord dysfunction is made during a direct visualization of the vocal cords during an attack. Inspiratory, anterior vocal cord closure with a posterior glottic chink is seen (Dunn et al., 2015). There is no precise information on the prevalence of vocal cord dysfunction in adults due to a lack of formal surveillance of the disease and inconsistencies in the disease definition in the epidemiologic literature (Kenn and Hess, 2008).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous reports in the Gulf War and Health series or other reports related to burn pit exposures (IOM, 2011) have not addressed whether deployment to Southwest Asia is related to vocal cord dysfunction.
Update of the Scientific Literature on Vocal Cord Dysfunction
The committee’s literature search identified four studies that evaluated vocal cord dysfunction. Two studies (Krefft et al., 2020; Morris et al., 2014)—one of which was conducted by the STAMPEDE investigators (Morris et al., 2014)—did not include a comparison group and so did not provide information that could contribute to inferences that can be made regarding deployment to Southwest Asia and vocal cord dysfunction. Morris et al. (2013) conducted a retrospective review that identified 48 U.S. military personnel evaluated at a level 3 evacuation medical center (Landstuhl, Germany) for vocal cord dysfunction; however, this retrospective case series is of limited relevance for the committee’s purposes because there was no comparison group and no data collected on exposures experienced during deployment.
Dion et al. (2013) evaluated the differences in vocal cord function and dysphonia between deployed and nondeployed U.S. Army soldiers in a cross-sectional medical records study using DoD military health system databases, which contain medical records for all DoD members and their families who receive care in the military health system. A retrospective search of the database was restricted to soldiers on active duty between January 1, 2008, and March 1, 2012. Diagnoses of dysphonia were identified using ICD-9 codes for various forms of dysphonia grouped into four categories, and individuals with any of the listed diagnosis codes before the study period were excluded. Deployment status was considered only during the study period (therefore, people who deployed before 2008 but not during the study period were counted in the nondeployed group). A total of 1,309,015 soldiers met the inclusion criteria, and of those, 4,921 soldiers had received a diagnosis of dysphonia; 1,895 had been deployed and 3,026 were nondeployed during the study period, resulting in a crude risk ratio of 1.13. Chi-squared analysis was used to determine statistical differences in the deployed versus nondeployed population of soldiers with dysphonia (p <0.001). A convenience sample of 292 soldiers was selected for further evaluation of known factors linked to dysphonia; it included all subjects from the Army-wide population who were enrolled in centers covered by the Brooke Army Medical Center institutional review board. Demographic, military, and additional health information (including diagnosis, reflux status, tobacco use, and alcohol use) were collected using the electronic medical records for each individual in the convenience sample. Multinomial logistic regression was used in a combined model for variables found on chi-squared analysis to be independent to determine associations and relevant ORs. Risk factors and exposures common to patients with dysphonia were not statistically different between deployed and nondeployed soldiers. Additionally, the type of dysphonia diagnosis was not significantly different between deployed and nondeployed soldiers. None of the reviewed parameters accounted for the difference in dysphonia rate between deployed and nondeployed soldiers, suggesting that occupational exposures of deployed soldiers account for the increase in the diagnoses of dysphonia.
Synthesis
Previous National Academies reports in the Gulf War and Health series and other related reports have not addressed vocal cord dysfunction. Only one identified study (Dion et al., 2013) specifically examined the association between vocal cord dysfunction and dysphonia with deployment to Southwest Asia. Although there was a statistical difference in dysphonia between deployed and nondeployed soldiers, the inferences that can be made are limited.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of vocal cord dysfunction.
Sleep Apnea
Sleep apnea is a disorder in which breathing repeatedly stops and starts while sleeping. There are three main types of sleep apnea: obstructive sleep apnea, central sleep apnea, and complex sleep apnea. Obstructive sleep apnea, the most common type, occurs when the muscles in the upper airway relax during sleep and is commonly associated with obesity or other conditions that increase the amount of tissue in the neck around the airway. It is characterized by loud snoring and daytime sleepiness. Central sleep apnea occurs when the brain does not send proper signals to the muscles that control breathing. Complex sleep apnea syndrome, also referred to as treatment-emergent central sleep apnea, is defined by having both obstructive and central sleep apnea (Mayo Clinic, 2020).
The prevalence of obstructive sleep apnea is not well characterized. One study, using in-laboratory polysomnography, estimated that the prevalence of obstructive sleep apnea in 602 middle-aged adults between 30 and 60 years of age was 9% for women and 24% for men (Young et al., 1993). There are some estimates of prevalence of sleep apnea among Southwest Asia theater veterans. Using data from the 2005–2014 National Survey on Drug Use and Health, Jackson et al. (2017) estimated that the prevalence of sleep apnea was more than 8% in 2014. They also pointed to an evaluation of OEF/OIF/OND veterans that found that 69.2% of 159 veterans screened were at high risk for obstructive sleep apnea.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous committees have noted that personnel deployed to Southwest Asia have reported more sleep problems or disturbances than nondeployed veterans (Bossarte, 2014; Cherry et al., 2001; Doebbeling et al., 2000; Goss Gilroy Inc., 1998; Gray et al., 1999, 2002; Ishoy et al., 1999; Kang et al., 2000; Nisenbaum et al., 2004; Proctor et al., 1998; Sim et al., 2015; Simmons et al., 2004; Steele, 2000; Unwin et al., 1999). Sleep apnea as a distinct outcome was only assessed by Sim et al. (2015) using data collected from the Australian Gulf War Veterans’ Follow Up Health Study conducted in 2011–2013. Sleep apnea (self-reported as being diagnosed with or treated for by a medical doctor) was reported by 70 (10.2%) of the Gulf War–deployed veterans and 63 (9.7%) of the nondeployed comparison group. The difference between the groups did not reach statistical significance (RR = 1.04, 95%CI 0.75–1.45) when adjusted for age group, service branch, and rank estimated as of August 1990, any atopy at baseline, and current smoking status (never, former, current smoker).
An analysis conducted by the AFHSC (2010) examined ICD-9-coded medical encounters at military facilities by Army and Air Force personnel within 36 months of April 2006 after deployment between 2005 and 2007 to Joint Base Balad or Camp Taji (with burn pits), Camp Buehring or Camp Arifjan (without burn pits), or the Republic of Korea (urban air pollution and PM exposure). Sleep apnea was examined using Poisson models, with analyses adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, physical activity, service branch, military rank, pay grade, and occupation. IRRs for sleep apnea were statistically significantly lower for personnel deployed to Joint Base Balad (IRR = 0.81, 95%CI 0.73–0.89), Camp Buehring (IRR = 0.63, 95%CI 0.40–0.99), and Korea (IRR = 0.87, 95%CI 0.81–0.93) compared with the nondeployed U.S. cohort; IRRs were no different for those deployed to Camp Arifjan (IRR = 1.08; 95%CI 0.92–1.26) or Camp Taji (IRR = 0.89; 95%CI 0.68–1.16).
Update of the Scientific Literature on Sleep Apnea
The committee identified 10 previously unreviewed studies that examined sleep apnea in Southwest Asia theater veterans. Four of the studies (Butzko et al., 2019; Dursa et al., 2016a; Morris et al., 2014, 2020) did not use appropriate comparison groups and thus did not provide information that could contribute to inferences that can be made regarding deployment to Southwest Asia and sleep apnea; these included two studies by STAMPEDE investigators (Morris et al., 2014, 2020) and one study involving veterans who had been referred to VA’s WRIISC specialty clinic (Butzko et al., 2019).
Post-9/11 Veterans
Smith et al. (2008) used self-reported clinician-diagnosed health data from regular, active-duty participants from the first panel (2001–2003) of the Millennium Cohort Study (n = 37,798) to compare the
agreement of 38 medical conditions, which included sleep apnea, with that obtained from electronic medical records based on ICD-9-CM codes. Any diagnostic code for these 38 conditions in any portion of the medical record indicated agreement with a self-reported medical condition of interest. Positive and negative agreement was used to compare self-reported data with that from electronic medical records. The prevalence of sleep apnea was 2.7% (95%CI 2.6–2.9) for self-report and 1.5% (95%CI 1.4–1.6) for the electronic medical records; 0.5% were exclusively recorded in the electronic medical record. The positive agreement between self-report and electronic medical record sleep apnea was 45.1%, and the negative agreement (the condition was not reported either by self-report or found in the medical record) was 98.8%.
Díaz Santana et al. (2017) used data collected from the NewGen survey to examine the prevalence of 19 self-reported, physician-diagnosed mental and physical health outcomes, including sleep apnea, between deployed (n = 12,705) and nondeployed (n = 7,124) veterans. Sampling weights were applied to account for nonresponse and temporal misclassification of deployment status in the sampling frame to enhance the accuracy and precision of the estimates. Weighted mean physical and mental component summary scores were calculated by demographic and military characteristics. Multivariable logistic regression analysis was performed, and weighted, adjusted ORs were presented for each of the 19 self-reported medical conditions and deployment status. Models were adjusted for gender, birth year, service branch, unit component, race/ethnicity, education, and VA health care user status. The weighted prevalence of sleep apnea was 10.3% for the deployed and 9.7% for the nondeployed; no difference in sleep apnea was observed between deployed veterans and nondeployed veterans (OR = 1.02, 95%CI 0.91–1.14).
Rohrbeck et al. (2016) conducted a cohort study that compared U.S. service members deployed to Iraq (2006–2008, n = 163) and Afghanistan (2011–2012, n = 37) with matched nondeployed service members (n = 200) to examine the association between exposure to burn pits and the occurrence of ICD-coded respiratory outcomes, including sleep apnea, after returning from deployment. Data from medical encounters, both hospitalizations and outpatient visits, in military treatment facilities were used to capture information on sleep apnea. A 3% increase in the incidence of sleep apnea was reported in the Iraq cohort compared with the nondeployed cohort, although this was not statistically significant due to the study being underpowered. Using Cox Proportional Hazards regression, relative risks were adjusted for age, sex, race/ethnicity, occupation, deployment history, and history of illness prior to deployment, and the Bonferroni correction was applied. No difference was found for developing sleep apnea in the deployed cohort compared with the nondeployed cohort (RR = 0.54, 95%CI 0.05–5.78). This analysis had several limitations, including its representativeness, its power for detecting differences in outcomes, its lack of individual exposure assessment, and its inability to control for smoking, which limits its contribution to the evidence base.
1990–1991 Gulf War Veterans
Khalil et al. (2018) described the study design for the Gulf War Era Cohort and Biorepository and preliminary results from the pilot phase of the effort, which had enrolled 1,275 veterans. Self-reported health outcomes of symptoms (in the past year) and health care provider–diagnosed conditions were reported stratified by users (n = 584) and nonusers (n = 679) of VA health care. Respiratory disease was not reported as a category, but sleep apnea was presented under other conditions by 39.2% of users and 21.2% of nonusers. While the reported proportions of veterans with sleep apnea seem high, there was no formal assessment of differences in the frequency of symptoms between VA users and nonusers. Furthermore, there were no comparisons between deployed and nondeployed veterans and, hence, these results do not inform questions about the role of Gulf War deployment on increased risk of sleep apnea.
Peacock et al. (1997) conducted a clinical assessment of 1990–1991 Gulf War veterans who participated in DoD’s Comprehensive Clinical Evaluation Program and who were seen at Brooke Army Medical Center to examine the prevalence of sleep apnea and hypopnea. After the veterans completed an initial survey that included information on symptoms, environmental exposures, vaccination history, and areas of deployment during the war, clinicians performed an interview and examination. Of the 192 veterans, 46 had histories suggestive of a sleep disorder and were referred for further evaluation to the pulmonary division for nocturnal polysomnography. Of the 46 who underwent further evaluation, 15 veterans met the criteria for sleep apnea or hypopnea, which was defined as a respiratory disturbance index greater than 15 in an individual who is experiencing symptoms. The authors report that a majority of those who met the criteria had symptoms of fatigue and memory loss. The study did not present comparisons with
veterans who were not referred for additional testing or with another group; confounding factors, such as age and weight, were collected and presented along with the results of the assessments only for those 15 individuals who met the criteria for sleep apnea or hypopnea, which severely limits the informativeness of this study.
Other Coalition Forces Veterans
Gwini et al. (2016) examined new onset of self-reported conditions in deployed Gulf War veterans using data collected from wave 1 and wave 2 of the Australian Gulf War Veterans’ Health Study. Veterans in wave 1, conducted in 2000–2002 (10 years after the Gulf War), were given a questionnaire that collected information on general health, physical and psychological health, military service history, and exposures during deployment and were also given a comprehensive health assessment, a full physical examination, blood work, and fitness tests; 81% (n = 1,456) of the deployed participated. Wave 2 was conducted in 2011–2013 and had a 50% participation rate. The follow-up study collected much of the same information as the original study, but it also inquired about additional outcomes. Participants were grouped into low (n = 272), moderate (n = 328), and high (n = 80) symptom reporting groups at wave 1 and assessed at wave 2 for selected symptoms and disease diagnosis to determine the new onset or incidence of particular conditions. Those who reported a condition of interest at wave 1 were excluded in the analyses of onset for wave 2. Respiratory health was assessed at both baseline and follow-up, but the scope of respiratory health data collected and the mode of data collection changed for some factors, which limited the ability to assess change over time for some of the outcomes. The wave 2 component of the study collected information on respiratory symptoms and medical conditions, including sleep apnea and asthma, assessed via self-report questionnaire. Logistic, nominal, and ordinal regressions were used for between-group comparisons. Regression models were adjusted for age group, service branch, and rank estimated as of August 1990, and smoking status, alcohol use, BMI, and highest educational level attained at wave 1. New onset of sleep apnea was increased in high versus low symptom reporters (OR = 9.40, 95%CI 3.47–25.46) and also in moderate versus low symptom reporters (OR = 2.63, 95%CI 1.17–5.88). The authors found that the odds of obesity and alcohol use increased over time and that smoking halved; these findings in risk factors were similar across symptom groups. The findings from the Australian Gulf War Veterans’ Health Study likely lack generalizability to studies of respiratory disorders in U.S. Gulf War veterans, primarily because 85% of the Australian Gulf war veterans were Navy personnel, who likely did not have the same exposures—even when off ship—as U.S. ground forces. Furthermore, no analyses were presented to compare differences in those who participated in wave 2 with those who did not, which was half the cohort, and therefore confounding by indication cannot be ruled out for wave 2 responders.
Synthesis
The committee identified and reviewed six studies that examined sleep apnea, three among post-9/11 service members and veterans and three among 1990–1991 Gulf War veterans. Prevalence of sleep apnea among post-9/11 veterans was relatively low and, for two of the studies, based on ICD codes in medical records. The prevalence of sleep apnea was higher among 1990–1991 Gulf War veterans and was based on self-report in the reviewed studies. Few of the studies reported effect estimates from comparisons of sleep apnea between deployed and nondeployed service members or veterans, and those that did, did not adjust for potential confounders, such as use of concurrent medications or conditions that may affect sleep. Therefore, as a whole, the available evidence on sleep apnea and associations with deployment are limited. A 2020 VA Office of Inspector General report indicates that sleep apnea has been the most prevalent service-connected disability of all the respiratory disabilities for which veterans received benefits since fiscal year 2013, which suggests that more attention to the issue would be appropriate (VA, 2020).
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of sleep apnea.
PULMONARY FUNCTION TESTING
Pulmonary function tests (PFTs) can be considered objective measures of how well the respiratory system is working. In epidemiologic studies, they may produce less outcome misclassification than self-reported measures and, potentially, less bias to the null. However, some common measurements—the forced vital capacity (FVC, the amount of air that can be forcibly exhaled from the lungs after taking the deepest breath possible), the forced expiratory volume in 1 second (FEV1, the amount of air that can be forcibly exhaled in 1 second after taking in the deepest breath possible), the ratio of FEV1 over FVC (FEV1/FVC), and some less common measurements, such as total lung capacity (TLC)—rely on the participant’s cooperation. Pulmonary function tests can be grouped into three sets of measures that use different equipment and procedures: spirometry, which includes FEV1, FVC, FEV1/ FVC, and forced expiratory flow between 25% and 75% of expired volume (FEF25–75%), sometimes performed before and after the administration of a bronchodilator; lung volumes, which include TLC, functional residual capacity (FRC), residual volume (RV), and airways resistance (Raw); and diffusing capacity, which includes diffusing capacity of the lung to carbon monoxide (DLCO) and the ratio of DLCO to alveolar volume (DL/VA). In many studies, airflow obstruction is defined as a situation involving FEV1/FVC <0.70 or less than the lower limit of normal based on reference equations from a normal population. There are also some more specialized and often less standardized test measures and methods, such as bronchoprovocation testing (e.g., methacholine challenge or bronchoprovocation); cardiopulmonary exercise testing; and air oscillation methods, such as the forced oscillation technique (FOT) and impulse oscillometry (IOS), which measures respiratory mechanics during normal breathing, distinguishing between small airway and large airway obstruction. Also included are exhaled gas analysis methods, such as exhaled nitric oxide, and multiple breath inert gas washout, which quantifies ventilation heterogeneity and uneven distribution of ventilation, of which the lung clearance index (LCI)6 is the most commonly reported parameter.
Findings from spirometry are the most commonly reported. Spirometry is nearly universally performed when lung function is measured because it is well standardized, relatively easy to perform, and remains the gold standard test for assessing the presence of common airways disorders, even though it may not adequately reflect the hyperinflation of the thorax largely responsible for the symptom of dyspnea that often accompanies airways disorders (O’Donnell et al., 2001). Spirometry also has important clinical relevance as loss of spirometric volumes and/or flow rates are often predictive of respiratory dysfunction.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Volumes 4 and 8 of the Gulf War and Health series of reports were consistent in concluding that “there appears to be no increase in respiratory disease among Gulf War veterans when examined with objective measures of disease. Pulmonary function studies have shown no significant excess of lung function abnormalities among Gulf War veterans” (IOM, 2006, p. 151, reproduced in IOM, 2010). The evidence was therefore classified as “limited/suggestive evidence of no association between deployment to the Gulf War and decreased lung function in the first 10 years after the war.” In the absence of any new studies on objective measures of lung function, the Volume 10 report (NASEM, 2016), like the Volume 8 report, also concluded “that there is limited/suggestive evidence of no association between deployment to the Gulf War and decreased lung function.” The 2011 IOM report Long-Term Health Consequences of Exposure to Burn Pits in Iraq and Afghanistan used literature in surrogate populations (firefighters, municipal incinerator workers, and residents who lived near municipal incinerators) to evaluate the potential for effects of exposure to burn pits, because very little research had been done in theater veterans. That committee found limited or suggestive evidence of an association only for decreased pulmonary function in firefighters.
The Gulf War and Health conclusions were based primarily on four epidemiologic studies (Gray et al., 1999; Ishoy et al., 1999; Karlinsky et al., 2004; Kelsall et al., 2004). The first was an early cross-sectional survey, conducted in 1994, of 527 active-duty veteran Gulf War Navy mobile construction battalion personnel
___________________
6 LCI is the cumulative expired volume at the point where end-tidal inert gas concentration falls below one-fortieth of the original concentration, divided by the FRC.
(Seabees) and an internal control group of 970 veteran Seabees from 14 commands who were not deployed to the Gulf War (Gray et al., 1999). Despite the fact that the Gulf War–deployed Seabees had a higher prevalence of respiratory symptoms than the nondeployed Seabees, cigarette smoking–adjusted mean spirometric measures of lung function were no different between the two groups. Ishoy et al. (1999) described a cross-sectional survey of 686 Danish Gulf War veterans (84% participation) deployed to the Persian Gulf during the period 1990–1997, mostly in peacekeeping roles, and 231 randomly selected nondeployed armed forces controls (58% participation) matched on age and sex. Again, in spite of those veterans who had been deployed in the Gulf War having a higher prevalence of respiratory symptoms than those who were not, mean spirometric measures of lung function were no different between the two groups. Although data on cigarette smoking were available, they were not used to adjust the lung function findings. Karlinsky et al. (2004) conducted a cross-sectional survey of a subset of participants selected from the 21,000 veterans who participated in the NHS and who lived close to a study examination center. Pulmonary function and self-reported respiratory symptoms were examined in 1,036 deployed and 1,103 nondeployed veterans who completed the clinical examination component of the third phase of the NHS. Spirometric measures were used to categorize study participants into the following five groups: normal, non-reversible airways obstruction, reversible airway obstruction, restrictive lung physiology, and small airway obstruction. Gulf War–deployed veterans and non–Gulf War–deployed veterans were similarly distributed across the five lung function categories. The distribution among lung function categories for those with exposure to the emissions from the 1991 destruction of a nerve agent storage complex at Khamisiyah, Iraq, did not differ from that of either other Gulf War–deployed or the nondeployed veterans. Although data on cigarette smoking were available and a history of tobacco smoking was more common in deployed than in nondeployed (51.1% vs 44.4%; p = 0.03), the analyses were not controlled for cigarette smoking.
Using results from the Australian Gulf War Veterans’ Health Study, in a cross-sectional study that included spirometric testing of Australian military personnel (Kelsall et al., 2004), with spirometric test results available for 1,341 deployed veterans and 1,340 nondeployed comparison group subjects, mean FEV1, FVC, peak expiratory flow rate, and FEF25–75% lung function levels in Australian Gulf War veterans were largely no different from those of military personnel who were not deployed to the Gulf. There were small, statistically significant increases in those deployed in mean FEV1/FVC (0.7%; 95%CI 0.2–1.1) and FEF75% levels (0.05; 95%CI 0.01–0.10) relative to those not deployed. The adjusted differences between means were calculated using robust linear regression, adjusting for age, height, smoking, weight, atopy, rank, service, education, and marital status.
Another study considered in the Volume 4 report was a prospective cohort study of 125 British bomb disposal engineers deployed to Kuwait for 5 months, in which spirometry was performed before deployment and throughout deployment, together with monitoring of PM10 (PM less than 10 microns in diameter) and gaseous pollutants (Coombe and Drysdale, 1993). Monitored mean PM10 concentrations were exceedingly high (~400 µg/m3), but gaseous pollutant concentrations were not. Although this was a relatively small study, it was unique given that spirometry was measured both before deployment to Kuwait and throughout the deployment. Of the possible spirometric measures available, the authors elected to report findings only on FEF25–75%. In the 100 participants who had both sets of spirometry, there was no average within-individual difference in the level of FEF25–75% obtained pre-deployment and the level measured shortly before the end of deployment, stratified either by cigarette smoking status or by self-reported smoke exposure.
Update of the Scientific Literature on Lung Function
There were several studies identified that analyzed lung function in post-9/11 veterans (Butzko et al., 2019; Davy et al., 2012; Falvo et al., 2016a,b; Holley et al., 2016; Krefft et al., 2017, 2020; Madar et al., 2017; Matthews et al., 2014; Morris et al., 2014, 2019; Szema et al., 2011; Weinstein et al., 2016). In addition, two studies were identified that evaluated the impact of service in the 1990–1991 Gulf War on pulmonary function (Hines et al., 2013; Lindheimer et al., 2019).
Post-9/11 Veterans
Morris et al. (2014) conducted a study (STAMPEDE I) of 50 active-duty U.S. military personnel recruited within 6 months after they had returned from deployment to Iraq or Afghanistan, all of whom reported new-onset pulmonary symptoms. Part of the physical examinations included measures of changes in pulmonary function using spirometry and oscillatory resistance measures. No adjustments for confounders were made. Investigators found baseline obstruction to be present in eight (16%) patients; two of whom had moderate obstruction (FEV1 <70% predicted), and six patients with mild obstruction (FEV1 >70% predicted). In three patients, the FEV1 was greater than 90% predicted. Seven of 44 (16%) had a positive methacholine bronchoprovocation test (defined as a 20% decrease in FEV1 at or below 4 mg/mL of methacholine) and another five (11%) had “borderline” hyperresponsiveness with a 20% decrease above the 4 mg/mL concentration cut-point up to 16 mg/mL. Results were used to provide a preliminary diagnosis for the entire patient cohort, although a full diagnosis could not be made in 14 patients. The study had the advantage of using objective outcome measures, but it was mostly descriptive in nature. Conclusions that can be drawn from this study are limited by the small number of cases examined at one medical center, the likelihood of referral bias, and the study design that lacked a comparison group, so measures of association could not be estimated.
Weinstein et al. (2016) evaluated exertional dyspnea among post-9/11 deployed military personnel using the same population as Morris et al. (2014), but at the time of this study the total population had increased from 50 to 240 service members. The physical exams included the same pulmonary function tests as described for Morris et al. (2014). Evaluations included full pulmonary function testing, impulse oscillometry, exhaled nitric oxide measurement, methacholine challenge testing, exercise laryngoscopy, cardiopulmonary exercise testing, and direct visualization of the central airways via fiberoptic bronchoscopy. The article then focuses on the results of five men and one woman who had no underlying lung disease and were identified as having symptomatic excessive dynamic airway collapse only during high levels of exertion. No comparisons with other participants or with specific deployment factors were made. Therefore, while this finding may be interesting, it is quite limited and difficult to attribute dynamic collapse of the central airways to inhalational exposures in Southwest Asia.
Using data collected as part of STAMPEDE II, Morris et al. (2019) reported on respiratory health outcomes and changes in the lung function of Army soldiers recruited from Fort Hood, Texas, between 2011 and 2014 before (n = 1,693) and after (n = 843) deployment to Southwest Asia. Participants completed a baseline questionnaire on their respiratory health and underwent examinations that included chest radiography, spirometry, and impulse oscillometry; the questionnaire with additional questions on exposures was administered post-deployment, and each of the lung function tests was also repeated post-deployment. Obstruction on spirometry was defined as FEV1/FVC below the lower limit of normal as defined by the National Health and Nutrition Examination Survey (NHANES) III reference values. Mean levels of percent predicted lung function (FEV1, FVC, FEV1/FVC) obtained using spirometry following deployment were slightly larger than those obtained before deployment, but this difference was not statistically significant. Results from the impulse oscillometry showed statistically significant improvement, with a reduction in resistance (at 5 Hz and 20 Hz) and reactance (at 5 Hz). A total of 116 (19%) individuals in the post-deployment cohort were found to have obstruction; 87 had obstruction before deployment, among 54 the obstruction persisted on post-deployment spirometry and in 33 the obstruction was no longer present on postdeployment testing. An additional 29 individuals had normal pre-deployment spirometry and developed obstruction after deployment. Using all post-deployment participants, no statistically significant change in spirometry values for those identified with obstruction were found. In individuals with pre- and post-deployment obstruction, there was a small improvement in FEV1, FVC, and FEV1/FVC. Of the 29 subjects who developed obstructive indices, 13 had an FEV1 of >90% predicted. Nearly one-third of the pre-deployment obstructed and pre- and postdeployment obstructed groups also had FEV1 of >90% predicted. Because certain factors may impact spirometry, subgroup analyses by cigarette smoking, self-reported asthma, and increased BMI were performed, and all three groups demonstrated slight improvement in post-deployment spirometry compared with pre-deployment values, but with only differences in FEV1 % predicted (p = 0.02) and FVC % predicted (p = 0.03) in the high BMI stratum being statistically significant. Logistic regression models were used to predict obstruction after deployment, and only age (p = 0.02) and self-reported asthma (p = 0.045) were found to be significantly predictive (not obesity,
smoking status, or sex). In soldiers with abnormal spirometry pre-deployment or history of asthma, no indication of worsening lung function was found post-deployment. This was a strong study in that it was large and collected measurements of lung function both before and after deployment, which allowed for a more direct assessment of deployment effects than is possible from cross-sectional studies of associations with exposure. However, the study would have been strengthened by including an analysis of mean within-subject change in lung function rather than a comparison of overall means pre- and post-deployment.
Morris et al. (2020) reported on the results of STAMPEDE III, an investigation of clinical lung diseases in 380 military personnel who had deployed to Southwest Asia and reported having chronic respiratory symptoms temporally related to deployment. Participants completed a deployment questionnaire (deployment history, airborne exposures, smoking status, and pulmonary symptoms before, during, and after deployment), answered questions from the VA Airborne Hazards and Open Burn Pit Registry, and underwent a history and physical examination. Pulmonary function testing consisted of spirometry, lung volume, diffusing capacity, impulse oscillometry, and bronchodilator testing. Other tests included methacholine challenge, exercise laryngoscopy, high-resolution CT scan, electrocardiogram, and transthoracic echocardiography. Asthma was the most common diagnosis (n = 87, 22.9%), based on obstructive spirometry/impulse oscillometry and evidence of airway hyperreactivity, and 57 patients (15.0%) had reactivity with normal spirometry. Airway disorders were diagnosed for 25 individuals with laryngeal disorders and 16 individuals with excessive dynamic airway collapse. Interstitial lung disease was identified in 6 individuals, and 11 individuals had fixed obstructive lung disorders (this latter category included four cases of COPD and two cases of emphysema). Isolated pulmonary function abnormalities were identified in 40 individuals, and 16 individuals had miscellaneous disorders. Nearly one-third of the study population (n = 122) had normal results and were classified as undiagnosed exertional dyspnea. The authors made many comparisons between different diagnostic categories for demographics, PFT, IOS, and underlying comorbidities, but no comparisons were made to differentiate among length or location of deployment or number of deployments and effects on lung function. This study provides an important description of pulmonary function among a group of military personal with chronic respiratory symptoms who were previously deployed to Southwest Asia, but because there is not a comparison group it is unclear whether service in Southwest Asia is associated with changes in lung function. While data were available, no adjustment or stratification was made for smoking status or specific reported exposures and results of PFTs.
In one of the few studies attempting to examine potential long-term effects of post-9/11 deployment, Falvo et al. (2016a) conducted a cross-sectional assessment of 124 post-9/11 veterans who had been referred to VA’s WRIISC specialty clinic as part of a multiday clinical evaluation between May 2012 and February 2015. Standardized self-administered questionnaires were used to gather data on demographics, deployment length in Iraq or Afghanistan, frequency of deployment periods, smoking histories, and symptom histories. The total months in a deployment area of concern were used as a surrogate of exposure. Standard spirometry pre- and post-bronchodilator data were collected and related to the number of months deployed. The study was conducted on average 6.9 years after deployment when the average age of these veterans was 38 years. After adjustment for smoking, there was a statistically significant association between months deployed and increased percentage of bronchodilator change in FEV1 (p = 0.003). Although almost all of the lung function test results were in the normal range, 26% of study participants had a positive response to a bronchodilator of at least a 12% and 200 mL improvement in FEV1. This study has several limitations. The study sample is a highly selected group of veterans referred to a tertiary clinic, and information on deployment was self-reported. Furthermore, in the description of the statistical analysis, the equation for calculating percent FEV1 response to bronchodilator was the following: ([pre-bronchodilator FEV1 – post-bronchodilator FEV1] / pre-bronchodilator FEV1) × 100, which would be a negative value if there were a post-bronchodilator improvement, an improvement observed in the large majority of the participants. Presumably, this equation was an error in that the numerator should have the pre-bronchodilator value subtracted from the post-bronchodilator value, rather than the other way around. While no firm conclusions can be drawn from this study because of these limitations, it nevertheless points to the need for studies including longer follow-up time periods, rather than immediate post-deployment assessments.
Falvo et al. (2016b) conducted a retrospective review of pulmonary function testing, including DLCO, in 143 veterans referred to VA’s WRIISC specialty clinic. The results of lung function tests were categorized into normal, restrictive, and obstructive. More than 75% of the sample had normal lung volumes and spirometry; however,
an isolated reduction in DLCO was observed in 30% of the sample of post-9/11 veterans. The observation of an isolated reduction in DLCO is reported to be unusual in primary-care-seeking dyspneic patients (<1%), so this finding provides some evidence that deployment may be related to a reduction in lung function. The deployment length was similar between those with normal (12.9 months ± 8.7) and reduced (10.3 months ± 7.4) DLCO. This study suffers from many flaws, including having a small sample size and making no adjustment for confounders.
Butzko et al. (2019) tested the utility of the forced oscillation technique on 178 OEF/OIF veterans referred to WRIISC who had normal spirometry and chronic unexplained respiratory symptoms. In this sample of veterans, spirometry was normal in 71.3%, of whom 124 had acceptable forced oscillation technique data; 75% of the 124 who had normal spirometric measures had one or more abnormal measures on forced oscillation, which the investigators suggested indicated distal airways obstruction. However, no comparison group was available, which makes it difficult to draw any conclusions as to whether this finding is unusual or is one that would be expected in a comparable group of veterans not deployed to Iraq or Afghanistan. The clinical significance of these findings is therefore undetermined.
Szema et al. (2011) conducted a retrospective study using data collected by the Northport, New York, VA Medical Center Research and Development Committee. To examine if the deployed were more likely to have asthma or respiratory symptoms requiring the use of spirometry than nondeployed service members, they included U.S. military service members who were deployed to OEF/OIF (n = 1,816, 25%) or elsewhere (n = 5,335, 75%) (matched on age and gender) who were discharged from active duty and who were examined between March 1, 2004, and December 1, 2010. This study is a follow-on to Szema et al. (2010), which focused on asthma diagnosis. To be eligible for spirometry, patients must have had symptoms and a diagnosis in their medical record and be referred by a physician. For veterans who had spirometry, comparisons were made by deployment location. Of those who had spirometry, 34.9% were smokers compared with 5.1% of those who did not have spirometry. Also, 72% of those who had spirometry (and clinical symptoms warranting a diagnosis) were deployed to Iraq or Afghanistan. Service members who underwent spirometry were stratified by deployment location and then matched for age, height, and weight. FEV1 and FVC were statistically significantly lower for those deployed in Iraq or Afghanistan than for those deployed elsewhere, but no difference was observed for FEV1/FVC (p = 0.63). An important limitation of this study is that raw FEV1 and FVC are largely meaningless unless adjusted for age, height, and sex. This is typically accomplished by using reference equations that incorporate age and height for men and women separately and reporting the percent of predicted values, which was not done. Those veterans deployed in Iraq or Afghanistan were shorter and older than those deployed stateside. Because both increased age in adults and shorter stature result in lower levels of lung function, the findings on FEV1 and FVC reported in this study are uninterpretable. The study is also limited by a lack of adjustment of confounders.
Matthews et al. (2014) conducted a retrospective review of DoD electronic medical records to identify trends in the frequency and severity of COPD based on pulmonary function tests in service members relative to their deployment history. Inpatient and outpatient records were queried to identify active-duty personnel from all service branches with the ICD-9 code for either “emphysema” (492.8) or “chronic airway obstruction, not elsewhere classified” (496) for 5 consecutive years from 2005 to 2009. Individuals with diagnosis of asthma (493) or chronic bronchitis (490) were excluded. Medical records review was limited to those individuals with a minimum of three outpatient encounters with the listed diagnosis of COPD/emphysema during the study period. Deployment information was obtained from the AFHSC, and individuals were classified into deployers and nondeployers based on whether they had deployed to Southwest Asia during or since 2003. Clinical symptoms, smoking history, pulmonary function testing, and radiographs obtained during the diagnostic workup were reviewed. A total of 371 patients with diagnosed COPD or emphysema were identified; 194 (52.3%) had deployed and 177 (47.7%) did not deploy to Southwest Asia since 2003. Of those deployed, 68% had a documented history of smoking compared with 62% of those nondeployed. Specific comparisons were made for age, FEV1 (% predicted), FEV1 post-bronchodilator (% predicted) and percent change, FVC (% predicted), FEV1/FVC, TLC, RV, and DLCO. Spirometry was documented in a total of 270 (73%) individuals, including both in the deployed (n = 155) and the nondeployed (n = 115) groups. According to t-tests, decreases in lung function were not statistically significantly different between the deployed and nondeployed individuals for all measures except TLC (% predicted) (p = 0.03). There was an overall reduction in the % predicted FEV1 (75.5 ± 17.1%) compared with normal reference values and a cor-
responding decrease in the FEV1/FVC (67.9 ± 10.4) consistent with airway obstruction. Mean % predicted TLC was 100.8 (± 15.2%), the % predicted RV was 116.7 (± 43.7%), and the % predicted DLCO was 83.4 (± 21.8), all of which were within normal predicted values. Airway obstruction was identified by spirometry in only 67% of the individuals diagnosed with COPD. Among individuals with a documented smoking history and spirometry data, 65% of those deployed and 46% of those nondeployed met established diagnostic criteria for COPD. Disease severity as measured by the Global Initiative for Chronic Obstructive Lung Disease (GOLD) criteria, was similar for deployed and nondeployed subjects: 30% versus 33% for those with mild disease, 57% versus 60% for those with moderate disease, and 14% versus 7% for those diagnosed with severe disease. Although the investigators concluded that despite evidence of increased respiratory symptoms in deployed military personnel, the impact of deployment on increased diagnosis of COPD or severity of disease appears minimal, this study lacked a prospective design and adequate adjustment for confounders of the relationship between deployment and pulmonary function. It is clear from the analyses conducted that—in this relatively young population (average age 40)—only about half had an adequate workup to assess the diagnosis of COPD. For example, smoking history was missing in about 35% of cases, pulmonary function testing was recorded in only about 55% of cases, and among these only about 25% had documented obstruction and only about 25% had assessments for alpha-1 antitrypsin deficiency despite their relatively young ages.7 The authors were aware of these limitations, which they speculate may be related to the nature of the retrospective databases, and they suggest that longer and more complete follow-up is necessary. Unfortunately, given the nature of the database being assessed, it is unlikely that further follow-up alone will be adequate. An alternative study design with prospective assessment would be needed because it is unlikely that the retrospective review of existing records will substantially improve.
Holley et al. (2016) conducted a retrospective review of 267 patients referred to the pulmonary clinics at Walter Reed National Military Medical Center and Fort Belvoir Community Hospital from February 2012 through May 2013 for unexplained respiratory complaints. All had at least one spirometry test performed following deployment in support of OEF/OIF, and the purpose of the study was to analyze associations between lung function and demographic and deployment characteristics. Spirometry was performed pre- and post-bronchodilator administration, and DLCO tests were performed in subsets of the veterans. Prevalence of abnormal spirometry was categorized as follows: 17% obstructed, 11% “restricted,” and 3% mixed obstructed and restricted. Mean DLCO was 95% of predicted, and 10% were below the lower 5th percentile cutoff point. Only 6% responded to bronchodilator administration. Lung function measures (mean % predicted values for FEV1, FVC, FEV1/FVC, FEV3/FVC, DLCO, and the carbon monoxide transfer coefficient) were not related to total number of deployments, deployment to Afghanistan versus other countries, deployment to Iraq versus other countries, total days deployed, months since the most recent deployment, reserve versus active duty, or land- versus sea-based deployments. Current or prior tobacco use was not associated with statistically significantly lower mean values for FEV1, FVC, or FEV1/FVC % predicted. However, because of the small sample size, this study had a limited ability to detect differences related to deployment.
Krefft et al. (2017) conducted a small pilot study to examine the role of lung clearance index as an early marker of lung injury in a sample of 24 healthy volunteers and 28 symptomatic veterans who had deployed to Southwest Asia in support of post-9/11 operations. The symptomatic deployers had cough, chest tightness, wheezing, shortness of breath, or decreased exercise tolerance during or following deployment. Individuals who were found to have other explanations for their respiratory symptoms were excluded. The healthy controls were at least 18 years of age, had no history of pre-existing lung disease, and reported no respiratory illness in the 4 weeks preceding enrollment and testing. Both groups underwent lung clearance index testing to identify whether abnormalities were present in the peripheral airways of the lung. As part of their clinical evaluation, the veteran group completed tests of pre- and post-bronchodilator spirometry, lung volumes, and DLCO in accordance with American Thoracic Society (ATS) standards. Abnormal spirometry was defined as an FVC percent predicted below the lower limit of normal (LLN), an FEV1 percent predicted below the LLN, or an FEV1/FVC ratio below the LLN. Spirometry reference values were obtained from NHANES III. Lung volume reference values were based on the 1995 ATS/European Respiratory Society (ERS) workshop, and reference values for DLCO were obtained from the Crapo prediction set. An abnormal
___________________
7 Alpha-1 antitrypsin deficiency is a risk factor for COPD (NHLBI, 2020a).
cardiopulmonary exercise tolerance (volume of oxygen [VO2] max <85% predicted) was observed in 52% of symptomatic deployers, abnormally elevated residual volume >120% was observed in 25% of symptomatic deployers, DLCO <80% predicted was observed in 21% of symptomatic deployers, abnormal spirometry was observed in 18% of symptomatic deployers, and FEF25–75% <LLN was observed in 18% of symptomatic deployers. Of the 28 veterans with respiratory symptoms, 17 were found to have definite and 11 were found to have probable deployment-related lung disease. Lung clearance indexing tests were abnormal in 82% of the symptomatic veterans, but also in 54% of the healthy controls, and they were more often abnormal in symptomatic veterans than were other detailed tests. Using t-tests adjusted for age, smoking status, and BMI, mean lung clearance index scores were compared between the veteran and the control group; mean lung clearance index scores were not statistically significantly different in the veterans (7.42, 95%CI 7.13–7.71) than in the controls (7.06, 95%CI 6.74–7.39, p = 0.10). Given that there was no comparison group in this study for the PFT, this study provides limited evidence of the impact of deployment to the Southwest Asia theater on pulmonary function. The small sample of veterans was highly selective as they were all symptomatic and were seen at an occupational lung disease clinic.
Krefft et al. (2020) aimed to describe deployment-related respiratory disease and the diagnostic utility of resting and exercise PFT with a retrospective study of 127 military personnel, veterans, and civilian contractors who supported military operations in Southwest Asia with new-onset respiratory symptoms presenting between 2009 and 2017 and referred to a single occupational lung disease clinic. Detailed medical, occupational, and smoking histories were collected. Of the 127 patients, 113 underwent PFT including pre- and post-bronchodilator spirometry, lung volumes determined by plethysmography, and DLCO measurement. The authors used logistic regression to determine whether abnormal physiologic findings were predictive of those with deployment-related distal lung disease. The researchers observed decreased DLCO to be significantly associated with a deployment-related distal lung disease, defined based on histopathology. Low DLCO was found in those with both deployment-related distal lung disease and deployment-related asthma (OR = 7.9, 95%CI 1.01–62.6, p = 0.05), and in those with deployment-related distal lung disease without asthma (OR = 4.6, 95%CI 1.4–15.1, p = 0.01). No other abnormal physiologic findings were individually associated with deployment-related distal lung disease diagnosis. The researchers concluded that obtaining baseline spirometry in defense force personnel before deployment may be useful in identifying changes linked to deployment exposures. The study is limited for the committee’s purposes because it includes only cases and does not including a control group.
Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center from January 2005 through December 2012 in 391 service members (137 had deployed to Southwest Asia prior to biopsy [deployed] and 254 had not deployed before the biopsy [nondeployed]). According to electronic medical records, 41% of the deployed and 56% of the nondeployed personnel were prior smokers; whether changes in smoking habits occurred during deployment or at the time of biopsy is not documented. Spirometric measures were extracted from the medical records, and comparisons were made based on Southwest Asia deployment status using independent means t-tests. The nondeployed group had slightly lower FVC (77.1% vs 83.2%; p = 0.03) but no difference based on TLC (79.9% vs 81.8%, p = 0.66). DLCO was lower in the nondeployed group (58.4% vs 72.0%; p <0.05). In addition to the limitations of this study noted in Chapter 3, the results were applicable only to those with respiratory disease that required biopsy.
Other Coalition Forces Veterans
Davy et al. (2012) performed a review of the respiratory health of Australian Defence Force personnel deployed to the Southwest Asia theater as part of the Middle East Area of Operations Prospective Health Study. The study population was defined as Australian Defence Force personnel who deployed after June 2010 and returned from that deployment by June 2012. Of the total eligible population of 3,074, a group of 156 completed pre- and post-deployment questionnaires, a physical examination, and spirometry test results that were usable for research purposes. FEV1 and % predicted FEV1 values from pre-deployment to post-deployment were found to be statistically significantly larger for those who deployed for 9–12 months (change in % predicted = 3.9, 95%CI 1.26–6.55) and lower for those who deployed for 6–7 months (change in % predicted = −2.80, 95%CI −4.42– −1.17) or 8 months (change in % predicted = −3.42, 95%CI –5.18– −1.67). These results suggest improved lung function following deployment in those deployed for a longer duration.
This finding may be a result of selection bias as those deployed for a longer duration may have been healthier than those deployed for shorter periods.
1990–1991 Gulf War Veterans
Hines et al. (2013) examined 37 1990–1991 Gulf War veterans who were enrolled in the VA Depleted Uranium Surveillance Program and had attended a biennial follow-up in 2011 to compare the likelihood of pulmonary health abnormalities in those with high body burdens of uranium (n = 12; >0.1 µg/g creatinine) versus those with low body burdens of uranium (n = 25; ≤0.1 µg/g creatinine). Participants attended a 3-day, inpatient clinical assessment that included a detailed medical and exposure history, physical examination, laboratory studies, and a comprehensive assessment of pulmonary health and function that included pulmonary function tests, CT chest-imaging studies, and IOS. Overall, pulmonary function tests were normal, and veterans with high urinary uranium content did not have statistically significantly different PFT values compared with those with low urinary uranium. No statistically significant differences in the prevalence of chest CT abnormalities or IOS between high and low urinary uranium groups were found. While the findings from this study made use of a rigorous exposure assessment through analysis of uranium in urinary samples, the findings are not particularly pertinent to this assessment, given that exposure to depleted uranium was uncommon.
Cardiopulmonary exercise testing was performed in a small number of lifelong nonsmoking veterans who were referred to VA’s WRIISC specialty clinic (Lindheimer et al., 2019). Twenty veterans described as having Gulf War illness were compared with 14 unmatched controls (consisting of both veterans and civilians). Spirometry was performed in accordance with standard guidelines using commercially available equipment that was calibrated prior to each participant. Spirometric indices of FVC, FEV1, and FEV1/FVC were obtained and expressed as a percent of predicted. The researchers found that both the Gulf War illness and the control groups had a similar minute ventilation at maximal exercise, but those with Gulf War illness on average had a ventilatory pattern characterized by larger tidal volume (breath volume) and lower respiratory rate (breathing rate) compared with the controls in achieving the same minute ventilation (total volume of air expired each minute). These findings suggest that deployed veterans with Gulf War illness might have a different ventilatory pattern during exercise, but no information was provided about Gulf War veterans without Gulf War illness.
Synthesis
Volumes 4, 8, and 10 of the Gulf War and Health series concluded “that there was limited/suggestive evidence of no association between deployment to the Gulf War and decreased lung function in the first 10 years after the war.” The new studies in 1990–1991 Gulf War veterans did not introduce evidence to support a revised conclusion. As described in Chapter 3, the grade of evidence, “Limited/Suggestive Evidence of No Association,” is assigned when
there are several adequate studies, covering the full range of levels of exposure that humans are known to encounter, that are consistent in not showing an association between an in-theater exposure and a respiratory health outcome in humans. In other cases, there is evidence from human or animal studies, but the heterogeneity of exposures, outcomes, and methods leads to inconsistent findings that preclude the committee from identifying an association between exposure and effect.
The studies included in this report differ from the findings of the previous Gulf War and Health reports in that they also include those who served in post-9/11 conflicts. The question to address now is whether the grade of evidence should remain the same based on studies of post-9/11 Gulf War exposures as the ones that were determined based on regarding exposures in the 1990–1991 Gulf War.
The most significant of the more recent studies is the relatively large STAMPEDE II study of those deployed to post-9/11 conflicts (Morris et al., 2019) in which measurements of lung function were performed both before and after deployment, allowing for a more direct assessment of deployment effects than is possible from cross--
sectional studies of associations with exposure. The mean levels of percent predicted lung function obtained following deployment were slightly larger than those obtained before deployment. A limitation of this study is that the investigators missed an opportunity to carry out a more appropriate analysis of mean within-subject change in lung function rather than a comparison of overall means pre- and post-deployment, which assumes that the two measures are independent—which they are not given that the two measures were obtained from the same individuals. The most likely impact of carrying out the proper analysis would typically be to reduce the variance in the effect measures and the degrees of freedom of the statistical test used to test for differences; that is, the variance of the lung function studies done either before or after deployment would be greater than the variance of the individual differences in level of lung function, which would have resulted in greater power to detect a difference between the pre- and post-level of lung function. The difference in means of the pre- and post-deployment lung function (as was done), however, should theoretically be the same as the mean of the within-individual differences. This difference was still detected in the published analysis in spite of the poorer power. An additional advantage of carrying out a paired within-individual analysis is the ability to evaluate subgroups of individuals with different patterns of lung function change, allowing for more focused analyses or clinical follow-up.
Other recent studies summarized earlier that assessed effects of deployment were plagued by an absence of comparison groups (Butzko et al., 2019), were analyzed in such a way as to be hard to interpret (Falvo et al., 2016a; Szema et al., 2011), or were based on a population that may not represent all theater veterans (Madar et al., 2017). These studies do not add to or detract from the evidence of no association with level of lung function.
Associations with exposure were not observed among studies that used IOS (or FOT), cardiopulmonary exercise testing, bronchial responsiveness, or LCI, while demonstrating the promise of these tests in assessing abnormalities of lung function in Southwest Asia, to date, in the absence of appropriate comparison groups, they have been of little value in assessing the role of Southwest Asia exposures. Falvo et al. (2016a) studied the response to a bronchodilator in relation to self-reported duration of deployment, but the study was limited by the use of a highly selected sample and self-reported information on deployment. The one study in which IOS was done both pre- and post-deployment found slight improvement in the oscillometric measures after deployment (Morris et al., 2019); however, the authors did not use an analysis that accounted for the paired nature of the data for this analysis either.
Deterioration of lung function is most likely to be observed with longitudinal studies that include pre- and post-deployment measures of lung function. The findings of Morris et al. (2019) and others have been used to argue that there is no role for surveillance spirometry in those being deployed to or returning from deployment in the theater who are asymptomatic. The arguments are based on concerns about cost and measurement reliability and about the very low frequency of detecting abnormalities in those individuals without symptoms or pre-existing respiratory conditions. While these points are valid, there remain at least two important questions that could be addressed with surveillance spirometry: (1) Would pre-deployment spirometry be useful in detecting those at risk of deployment-related respiratory problems? and (2) Would pre-deployment spirometry be useful in the assessment of post-deployment respiratory problems? The latter question is based on an understanding that baseline measurements of lung function allow for an assessment of change in function, whereas post-deployment measurements alone do not. For example, someone may have had a relatively high level of lung function prior to deployment and experienced a marked fall in lung function related to deployment but still have a post-deployment level within the normal range. Conversely, someone may have had a relatively low level of lung function at baseline with little or no change in lung function following deployment. With only a post-deployment measurement, both may have had a similar level of lung function measured post-deployment, but the first experienced a concerning deployment-related decline in lung function while the second did not. A post-deployment spirometry alone could not distinguish the two, whereas pre- and post-deployment spirometry could. Furthermore, because of the great concern about Gulf War exposures triggering irritant-induced asthma, surveillance spirometry before deployment performed before and after inhalation of a bronchodilator would be even more useful in assessing post-deployment respiratory problems.
An additional issue that has not been addressed by studies of in-theater exposures and lung function to date is that of the long-term or chronic impacts of exposures on lung function. Studies to address that question would require some form of surveillance lung function measurements. Improved exposure measurement could improve
confidence in the evidence of theater exposure on health effects. In light of all of the above, the question as to the value of surveillance spirometry should therefore remain open.
Conclusions
The current committee concurs with previous committees and concludes that there is limited or suggestive evidence of no association between deployment to the 1990–1991 Gulf War and changes in lung function. Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent deterioration of lung function in post-9/11 veterans. Chapter 5 includes observations and recommendations for future research that may provide greater insight on this issue.
LOWER AIRWAY DISORDERS
The lower airways, where gas conduction occurs, consist of the trachea, bronchi, and bronchioles. The trachea divides into the bronchi and the bronchioles through an extensive branching network ending with the terminal bronchioles. The airways then lead to the respiratory bronchioles, alveolar ducts, and alveolar sacs (alveoli), where gas exchange occurs, allowing oxygen molecules to cross from the alveoli to the capillaries (Tortora and Dickerson, 2018).
Diseases of the lower airway occur from many different physiological processes and include asthma, COPD (including emphysema and chronic bronchitis), bronchiolitis, interstitial lung diseases (including hypersensitivity pneumonitis, sarcoidosis, acute eosinophilic pneumonia, pulmonary alveolar proteinosis, and idiopathic interstitial pneumonias), and infectious diseases that impact the lower airway (including acute bronchitis, pneumonia, and tuberculosis). Diseases of pulmonary vascular circulation, such as pulmonary embolism, were not considered. Lower respiratory diseases that have been studied in theater veterans are summarized below. Each section begins with a description of the condition, its known causes and frequency of occurrence, and any common challenges in interpreting findings of the studies of it before presenting summaries of the identified epidemiologic studies in veterans. As for the Upper Airway Disorders section, each condition section ends with a synthesis followed by a conclusion on the strength of association between deployment to Southwest Asia and the respiratory condition of interest.
Asthma
Asthma is a chronic inflammatory disease of the airways that causes symptoms of coughing, wheezing, shortness of breath, and chest tightness that are accompanied by a narrowing of the airways causing airflow obstruction (GINA, 2019). The symptoms and severity of airflow obstruction vary over time, and “asthma attacks” are often triggered by environmental and occupational exposures (Mayo Clinic, 2018a). Environmental triggers include indoor and outdoor allergens and airborne pollutants, such as biologic allergens (dust mites, cockroaches, animal dander, and mold), environmental tobacco smoke, irritant chemicals, traffic pollution, ground-level ozone, and combustion byproducts (Chabra and Gupta, 2019). Occupational exposures can either cause asthma (“occupational asthma”) or exacerbate existing asthma (“work-exacerbated asthma”). In some cases, occupational exposures can both cause asthma and perpetuate ongoing symptoms. Work-exacerbated asthma can be assessed by documenting the relationship between the timing of symptoms with workplace activity or exposures as well as by documenting changes in lung function (Hennenberger et al., 2011; Redlich et al., 2014).
Asthma is a common disease in the United States and affects 7.7% of adults over 18 years of age.8 The annual incidence of occupational asthma ranges from 12 to 170 cases per million people working. The prevalence of adult asthma that is occupational is estimated to be 5% to 15% across many different industries (Chabra and Gupta,
___________________
8 See https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2017_SHS_Table_A-2.pdf (accessed August 19, 2019).
2019). Reportedly, asthma is associated with service in the Southwest Asia theater. A few retrospective studies have observed a higher prevalence of new-onset asthma among Southwest Asia veterans than among those not deployed (Rivera et al., 2018), and since 2003 the prevalence of asthma has been increasing among those receiving VA care (Pugh et al., 2016).
In order to study asthma it is necessary to have a standard case definition. Asthma is defined, according to international guidelines, as “a heterogeneous disease usually characterized by chronic airway inflammation. It is defined by the history of respiratory symptoms such as wheeze, shortness of breath, chest tightness, and cough that vary over time and in intensity, together with variable expiratory airflow limitation” (GINA, 2019). The gold standard in research is often a physician diagnosis of asthma or evidence of bronchial hyperresponsiveness demonstrated through physiologic PFT, such as methacholine challenge tests (Coates et al., 2017) or pre- and post-bronchodilator spirometry (Graham et al., 2019; Sá-Sousa et al., 2014).
Outcome measures in asthma research include the assessment of asthma control based on standard questionnaires, spirometry, asthma exacerbations, and health-related quality of life. Asthma control is defined by the presence of daytime and nighttime asthma symptoms and the risk of future exacerbations. Spirometry is another outcome that is a crucial component in assessing asthma. The variables of interest include FEV1, FVC and FEV1/FVC ratio, and bronchodilator responsiveness (change in FEV1 or FVC after bronchodilator administration according to standard protocols) (Graham et al., 2019). These are typically assessed over time, which allows for the evaluation of within-person changes. Asthma exacerbations should be assessed using a standard approach, such as that put forward in the ATS/ERS consensus statement in standardizing endpoints for asthma clinical trials (Reddel et al., 2009).
Asthma exacerbations should be assessed within a standard approach (Reddel et al., 2009), which may include severe, moderate, and mild exacerbations. Frequently, severe exacerbations include the need for systemic corticosteroids or acute care use, such as an unscheduled doctor visit, emergency department visit, or hospitalization. Moderate exacerbations include the need for additional asthma controller medications. Mild exacerbations are more challenging to assess and are likely reflected in standard measures of asthma control (loss of control on asthma questionnaires is equivalent to a mild exacerbation).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
As noted in previous reports that focused on veterans deployed to the Southwest Asia theater (IOM, 2006, 2010; NASEM, 2016, 2017), asthma and related symptoms, such as wheezing and shortness of breath, have consistently been a concern among veterans after deployment. Nonetheless, the Volume 10 committee concluded that there was insufficient or inadequate evidence to determine whether an association exists between deployment to the Gulf War and respiratory disease, based on cohort studies of 1990–1991 Gulf War–deployed and nondeployed service members from four countries (Australia, Denmark, United Kingdom, and United States). Committees for Volumes 4, 8, and 10 did not make separate conclusions for asthma. The committees for Volumes 6 and 8 concluded that there was inadequate or insufficient evidence to determine whether an association exists between deployment to the Gulf War and respiratory disease. This conclusion was a change from Volume 4, in which that committee concluded that respiratory symptoms were strongly associated with Gulf War deployment when using comparison groups of nondeployed veterans. The Volume 10 committee concurred with the Volume 8 committee. It concluded that based on the literature reviewed in previous volumes and the few new studies, there was insufficient or inadequate evidence to determine whether an association exists between deployment to the 1990–1991 Gulf War and respiratory disease.
The next part of this section summarizes the results of asthma outcomes that were reported in the 19 studies of service members of veterans that examined diagnoses or self-reported asthma included in prior Gulf War and Health reports (Cowan et al., 2002; Dursa et al., 2016b; Eisen et al., 2005; Goss Gilroy Inc., 1998; Gray et al., 2002; Iowa Persian Gulf Study Group, 1997; Kang et al., 2000, 2009; Karlinsky et al., 2004; Kelsall et al., 2004; Lange et al., 2002; Li et al., 2011; Sim et al., 2015; Simmons et al., 2004; Smith et al., 2006; Steele, 2000; Unwin, 1999; VA, 2014a,b). The studies of 1990–1991 Gulf War veterans showed mixed results. Several of these studies examined multiple respiratory outcomes, grouped symptoms and conditions, relied on self-reports of respiratory
diagnoses and symptoms, and did not adjust for known confounders, such as obesity. The studies are summarized below, beginning with studies of U.S. veterans, followed by UK, Canadian, and Australian veterans. Background information on large studies is provided for context.
1990–1991 U.S. Gulf War Veterans
Large cohort studies of 1990–1991 Gulf War veterans include VA’s NHS and several that focused on state-specific cohorts or cohorts with particular military jobs. Several cohorts of foreign military forces have also been assembled and followed, and these studies are described after the studies of U.S. veterans.
National Health Survey of Gulf War Era Veterans and Their Families
As described in Chapter 3, VA conducted a population-based study consisting of three waves to examine the prevalence of health outcomes and symptoms in deployed Gulf War veterans and Gulf War–era veterans, known as the NHS. Three studies analyzed and reported on asthma collected from wave 1 (Eisen et al., 2005; Kang et al., 2000; Karlinsky et al., 2004), two publications reported on asthma collected from wave 2 (Kang et al., 2009; Li et al., 2011), and one publication examined outcomes of asthma using data collected from wave 3 (Dursa et al., 2016b). The design and details of the NHS are described in Chapter 3.
Kang et al. (2000) used information collected as part of the NHS to estimate the prevalence of symptoms and other health outcomes in Gulf War veterans (n = 15,000) compared with era veterans (n = 15,000). Population prevalence rates were calculated using statistical analysis techniques to account for the stratified random sampling of unequal probabilities of selecting various strata. The estimated population prevalence of asthma during the 12 months prior to the survey was 4.7% for the deployed and 3.7% for the nondeployed (RD = 0.97, 95%CI 0.91–1.03), a statistically significant difference; however, estimates were not adjusted for smoking or other factors.
Karlinsky et al. (2004) examined pulmonary function and self-reported pulmonary histories (including self-reported respiratory symptoms, physician visits and hospitalizations, and outcomes of asthma, bronchitis, and emphysema) in 1,036 deployed and 1,103 nondeployed veterans who completed the clinical examination component of the third phase of the NHS. Deployed veterans were statistically significantly more likely than nondeployed veterans to self-report a history of smoking (OR = 1.31, 95%CI 1.03–1.67), but there was no difference for self-reported asthma (OR = 0.90, 95%CI 0.50–1.62), self-reported physician visits for pulmonary complaints (which included asthma) (OR = 1.07, 95%CI 0.51–2.24), or self-reported pulmonary hospitalizations (which again included asthma) (OR = 0.91, 95%CI 0.13–6.51). Estimates were not adjusted for demographic factors or smoking status.
Eisen et al. (2005) performed a cross-sectional analysis on health outcomes collected in a subset of 1,061 deployed and 1,128 nondeployed Gulf War veterans (the same population used by Karlinsky et al., 2004) who completed the clinical examination component of the third phase of the NHS. The investigators examined several outcomes, including “obstructive lung disease,” which was defined as
a history of lung disease (asthma, bronchitis, or emphysema) or pulmonary symptoms (wheezing, dyspnea on exertion, or persistent coughing with phlegm) and either the use of bronchodilators or at least 15% improvement in FEV1 after a short-acting bronchodilator. (Eisen et al., 2005, p. 884)
No difference in these outcomes was found between deployed and nondeployed veterans (OR = 0.91, 95%CI 0.52–1.59) in analyses that were adjusted for age, sex, race, years of education, cigarette smoking, component (active versus reserves or National Guard), service branch, and rank. Similarly, no difference for the grouped outcome of “asthma, bronchitis, or emphysema” (OR = 1.07, 95%CI 0.65–1.77), adjusted using the same factors as above, was found for deployed versus nondeployed participants.
Kang et al. (2009) assessed changes in the health status of 1990–1991 Gulf War–deployed and era veterans using data collected as part of the follow-up survey conducted 10 years after the 1995 baseline survey of the NHS. Participants were from the same population used in the baseline survey. A total of 6,111 deployed veterans and 3,859 nondeployed era veterans participated in the follow-up survey. The prevalence of self-reported doctor-diagnosed asthma was 16.0% among the deployed and 12.7% among the nondeployed. The risk of asthma was statistically significantly higher for deployed veterans than for era veterans after adjusting for age, gender, race,
BMI, current cigarette smoking, rank, service branch, and unit component (active versus National Guard or reserve) (RR = 1.24, 95%CI 1.12–1.38). The study was limited by a low response rate and lacked a mechanism for verification of self-reports.
Using data collected as part of the same follow-up survey as Kang et al. (2009), Li et al. (2011) also assessed changes in the health status of Gulf War–deployed and era veterans using data from the 1995 baseline survey compared with data collected on the same group of participants in a 2005 follow-up survey. Repeated measurement data were used from 5,469 deployed Gulf War veterans and 3,353 nondeployed era veterans who participated in both surveys. The prevalence of self-reported doctor-diagnosed asthma among the deployed decreased from 5.2% in 1995 to 4.9% in 2005, but the difference did not show a true decrease because the timeframe queried about the doctor’s diagnosis was different between the surveys (12 months for 1995 versus 4 weeks for 2005). Among the era veterans, the prevalence of self-reported doctor-diagnosed asthma increased from 3.5% in 1995 to 4.0% in 2005. Neither change was found to be statistically significant. Persistence risk ratios and incidence risk ratios were calculated after adjustment for demographic and military service characteristics (age <46 years or ≥46 years in 2005, gender, race, rank, service branch, service component, BMI, and current cigarette smoking) through Mantel-Haenszel stratified analysis. Deployed veterans were statistically significantly less likely to report persistent asthma than era veterans (RR = 0.76, 95%CI 0.59–0.97), although the deployed had a nonstatistically significant increased risk of new-onset asthma (RR = 1.26, 95%CI 0.94–1.68).
Dursa et al. (2016b) conducted a 2012–2013 follow-up survey that collected data from 8,104 deployed and 6,148 era veterans who had participated in the (1993–1995) NHS reported by Kang et al. (2000). An increased risk of self-reported asthma was observed in Gulf War–deployed veterans when compared with the nondeployed veterans (10.2% vs 9.0%; OR = 1.22, 95%CI 1.04–1.44), after adjustment for age, race, sex, BMI, smoking status, service branch, and unit component.
Other Studies of U.S. 1990–1991 Gulf War Veterans
As first described in the Respiratory Symptoms section, Gray et al. (2002) re-examined the question of symptoms and exposures among deployed and nondeployed Seabees by expanding the deployed and nondeployed cohorts that were first reported in Gray et al. (1999) to include all Seabees who had been on active duty during the time of the Gulf War regardless of whether they remained on active duty, were in the reserve, or had separated from service (n = 11,868 participants, participation rate = 67.4%). Participants were divided into three exposure groups: 3,831 who had been deployed to the Gulf War, 4,933 who had been deployed elsewhere, and 3,104 who had not been deployed. Those who had been deployed to the Gulf theater had statistically significantly higher odds of ever smoking than the nondeployed Seabees (OR = 3.09, 95%CI 2.79–3.42) and higher odds of current smoking than both Seabees deployed elsewhere (OR = 1.20, 95%CI 1.09–1.31) and nondeployed Seabees (OR = 2.68, 95%CI 2.37–3.04). Gulf theater–deployed Seabees also reported a greater frequency of lung diseases (not defined in the paper) than those Seabees who were deployed elsewhere (OR = 1.43, 95%CI 0.86–2.39) and nondeployed Seabees (OR = 1.68, 95%CI 0.91–3.12), but neither estimate was statistically significant. When asked about asthma and several other medical problems experienced in the past 12 months, Gulf theater–deployed Seabees reported higher frequencies of all 33 outcomes. Following adjustment for age, gender, active-duty versus reserve status, race/ethnicity, current smoking, and current alcohol drinking, ORs for asthma were increased but did not reach statistical significance for Gulf theater–deployed Seabees compared with Seabees deployed elsewhere (OR = 1.36, 95%CI 0.99–1.87), but the odds of asthma were statistically significantly increased for Gulf theater–deployed Seabees relative to nondeployed Seabees (OR = 1.82, 95%CI 1.23–2.69).
As described in Respiratory Symptoms, the “Iowa study” was a cross-sectional survey of a representative sample of 4,886 military personnel from all service branches who were randomly selected from those who had listed Iowa as their home of record at the time of enlistment (Iowa Persian Gulf Study Group, 1997). Trained examiners used standardized questions, instruments, and scales to interview the participants. This work led to future research on what would become known as Gulf War illness. As part of this work, the prevalence of self-reported symptoms and illnesses among deployed Gulf War personnel versus nondeployed personnel included asthma. Both deployed and nondeployed groups were stratified by regular military versus National Guard/reserve. The estimated prevalence of asthma was 6.7% of deployed regular military personnel, 9.4% of deployed National Guard/reserves, 3.8% of nondeployed regular military personnel, and 6.1% of nondeployed National Guard/-
reserves. Differences in the prevalence rates of asthma were calculated and adjusted for age, sex, race, service branch, and rank. There was a statistically significant increase in asthma for all deployed versus nondeployed personnel (prevalence difference = 2.3, 95%CI 0.7–3.9) and deployed versus nondeployed National Guard/reserve personnel (prevalence difference = 2.9, 95%CI 0.5–5.2). No statistically significant difference in asthma prevalence was found for deployed versus nondeployed regular personnel (prevalence difference = 1.8, 95%CI −0.3–3.8).
As also first described in Respiratory Symptoms, Steele (2000) conducted a population-based survey of veterans who listed Kansas as their home state of record (1,548 deployed and 482 nondeployed); the primary intention was to examine factors that might have been related to Gulf War illness. The survey asked about 16 specific medical or psychiatric conditions, 37 symptoms, locations during the Gulf War (including whether the veterans were notified about the Khamisiyah demolitions), and vaccinations. Physician-diagnosed or physician-treated asthma that was reported to have occurred post-1990 was much greater for deployed Gulf War veterans (n = 63) than for the nondeployed veterans (n = 9), and the odds of having asthma were statistically significantly increased after adjustment for sex, age, income, and education level, but not smoking status (OR = 2.08, 95%CI 1.02–4.26).
Smith et al. (2006) conducted a large study that examined DoD administrative data of post-deployment hospitalization events at DoD facilities among active-duty service members with one deployment in order to compare the experience of Gulf War veterans (August 1, 1990–July 31, 1991) with that of personnel deployed to Southwest Asia after the war for peacekeeping missions or to Bosnia (1995–1998). Complete deployment and demographic data were available for 455,465 Gulf War veterans, for 249,047 post-war Southwest Asia–deployed personnel, and for 44,341 Bosnia-deployed personnel. Data were collected from these groups on hospitalization encounters for any cause and for 14 broad ICD-9-CM diagnostic categories (including respiratory system) as well as for specific diagnoses, including asthma. No statistically significant differences in asthma hospitalization were found between Gulf War–deployed service members and the Southwest Asia peacekeeping service members (HR = 1.22, 95%CI 0.96–1.56) or the Bosnia-deployed service members (HR = 0.86, 95%CI 0.56–1.31). Analyses were adjusted for demographic factors (gender, age, marital status, race/ethnicity) and military characteristics (pay grade, service branch, occupation, pre-deployment hospitalization), but not for smoking status.
VA provided the Gulf War and Health Volume 10 committee with a health care use report for Gulf War–deployed and Gulf War–era veterans who sought care in VA facilities from October 2001 to December 2013. The report presented the prevalence of diagnoses of diseases by ICD-9 code categories. For each category of disease, the 10 most frequent diagnoses for deployed and nondeployed Gulf War veterans who sought health care in VA between 2002 and 2013 were presented. A veteran can have multiple diagnoses with each health care encounter and therefore may be counted in multiple categories, but the person is counted only once in any single diagnostic category. A total of 286,995 Gulf War–deployed and 296,635 era veterans received care at VA over the approximately 11-year period (VA, 2014a,b). These VA health care users represent 46% of all deployed Gulf War veterans and 36% of all nondeployed era veterans. Concerning the diseases of the respiratory system (ICD-9 categories 460–519), asthma was diagnosed in 16.7% of 105,481 deployed Gulf War veterans and in 16.5% of 97,539 nondeployed veterans. No effect estimates were calculated.
Studies with Modeled Exposure to Oil-Well Fire Smoke
Three studies of U.S. service members or veterans (Cowan et al., 2002; Lange et al., 2002; Smith et al., 2002) specifically examined asthma diagnoses or symptoms associated with modeled exposure to oil-well fires. Cowan et al. (2002) conducted a case–control study of 873 Gulf War veterans with a diagnosis of asthma in the medical record versus 2,464 controls without asthma or other respiratory system diagnoses who were participants in the DoD Comprehensive Clinical Evaluation Program. Demographic information was obtained from the DoD Gulf War Registry, and oil-well fire smoke exposure was based on the National Oceanic and Atmospheric Administration atmospheric advection and diffusion model. For those with self-reported exposure, the odds of asthma were statistically significantly increased (OR = 1.56, 95%CI 1.23–1.97); this increase remained with cumulatively modeled intermediate and high exposure and when the data were adjusted for sex, age, race, military rank, and smoking history. The effect was seen in former smokers and never smokers, but not current smokers.
Lange et al. (2002) used a cross-sectional study design to examine exposure to smoke from oil-well fires (self-reported and modeled) and self-reported asthma symptoms assessed via structured interviews conducted 5
years after the 1990–1991 Gulf War for a subset of 1,560 Iowa veterans. Modeled exposures were developed using a geographic information system to integrate spatial and temporal records of smoke concentrations with troop movements ascertained from Global Positioning Systems records during the period of oil-well fires (February–October 1991). Exposure was presented by quartiles. The overall prevalence of asthma symptoms was 8.3% for the study population; current smokers had more than twice the prevalence of symptoms of asthma than never smokers (13.3% vs 4.9%, respectively). ORs (adjusted for sex, age, race, military rank, smoking history, military service, and level of preparedness for war [based on the responses to six questions]) showed asthma increased with increasing self-reported exposure, but not when exposure to smoke from oil-well fires was modeled, limiting the support for an increased risk of asthma symptoms among these Gulf War veterans. The use of population-based sampling improved the generalizability of the results.
Smith et al. (2002) used DoD hospitalization data (ICD-9-CM codes) from August 1991 through July 1999 and exposure models to examine associations between respiratory diseases, including asthma, among 405,142 active-duty service members who served in the 1990–1991 Gulf War at the time of the oil-well fires. Service members were categorized as exposed (n = 337,077) and nonexposed (n = 68,065) to oil-well fires and no statistically significant difference was found for hospitalizations due to asthma between exposed (n = 745) and nonexposed (n = 135) veterans (RR = 0.90, 95%CI 0.74–1.10) after adjustment for demographic and military characteristics (not specified). However, asthma is not typically a condition that requires hospitalization.
Other Coalition Forces Veterans
Using results from 1,424 deployed veterans and 1,548 nondeployed comparison veterans who participated in the Australian Gulf War Veterans’ Health Study conducted in 2000–2002, Kelsall et al. (2004) reported no difference in self-reported asthma or doctor-diagnosed asthma overall (OR = 1.2, 95%CI 0.9–1.5; effect estimates were the same for both self-report and doctor-diagnosed), adjusted for age, height, smoking, weight, atopy, rank, service, education, and marital status. The current use of an asthma medication was not different between deployed and comparison veterans (OR = 1.4, 95%CI 0.9–2.2), adjusted for the same factors. Kelsall et al. (2004) then used a more specific definition of asthma, including an attack of asthma or being woken by an attack of shortness of breath at any time in the previous 12 months or current use of asthma medication, and applied the same model adjustments. The odds of suggestive asthma were statistically significantly increased for deployed veterans compared with the nondeployed veterans (OR = 1.4, 95%CI 1.1–1.9). A fourth category of asthma—doctor-diagnosed in 1991 or later and rated as a possible or probable diagnosis—was no different between deployed and nondeployed veterans (OR = 1.2, 95%CI 0.8–1.8), adjusted for service type, rank, age, education, and marital status only. A subgroup analysis was conducted that examined exposure to smoke from oil-well fires (no exposure compared with any, low, or high) among the deployed veterans, using only the more specific definition of asthma. No difference in asthma was found for any, low, or high exposure, or for exposure to dust storms, or for deployments that were completed before versus after the air war.
Using data collected from the Australian Gulf War Veterans’ Follow Up Health Study conducted in 2011–2013 (described in detail in Chapter 3, and for other results cited throughout this chapter), Sim et al. (2015) found that self-reported asthma was not statistically significantly different for Gulf War veterans (14.4%) than for the comparison group (12.2%) (RR = 1.13, 95%CI 0.86–1.50). Estimates were adjusted for age group, service branch, and rank estimated as of August 1990, for any atopy at baseline, and for current smoking status (never, former, current smoker). Self-reported, doctor-confirmed asthma was reported by 12.6% of Gulf War and 11.2% of comparison veterans, frequencies that were similarly not statistically significantly different when adjusted for the same demographic, lifestyle, and military factors (RR = 1.09, 95%CI 0.81–1.47). Subcategories of asthma attack in the last 12 months (RR = 1.56, 95%CI 0.89–3.74) and currently taking asthma medication (RR = 1.42, 95%CI 0.91–2.21) were also not statistically significantly different for Gulf War and era veterans.
Two studies assessed asthma in UK Gulf War veterans. Simmons et al. (2004) used data collected as part of a large mail survey on British Gulf War veterans. The exposed cohort consisted of all UK Gulf War veterans, and the unexposed cohort consisted of a random sample of nondeployed UK military personnel from the same period. The survey was designed largely to assess reproductive outcomes among Gulf War veterans. However, it contained open-ended questions about their current health and changes in their health since 1990 that were then categorized into outcomes, including asthma and respiratory problems not otherwise specified. Although the numbers of surveys
returned in the study were large (25,084 by Gulf War veterans and 19,003 by era veterans), the participation rates were low (47.3% and 37.5% of male and female Gulf War veterans, respectively, and 57.3% and 45.6% of male and female nondeployed veterans, respectively). Approximately 61% of Gulf War veterans reported at least one new medical symptom or disease since 1990, compared with 37% of nondeployed veterans. Asthma was reported by 2.6% of Gulf War respondents and 2.1% of era veterans. After adjusting for age at survey, service, and rank at time of Gulf War, serving status at the time of the survey, alcohol consumption, and smoking, the odds of reporting asthma were significantly increased among Gulf War respondents compared with era veterans (OR = 1.2, 95%CI 1.1–1.4).
Unwin et al. (1999) conducted a cross-sectional postal survey from 1997 to 1998 to compare the health profiles of veterans and military service members from the United Kingdom (n = 8,195; overall response rate 65.1%). The study population was randomly selected, and the sample was stratified into three cohorts: deployed Gulf War veterans and military service personnel (n = 2,961) who served in the Gulf region between September 1, 1990, and June 30, 1991 (response rate = 70.4%); deployed military personnel who had served in Bosnia (n = 2,620) between April 1992 and February 1997 (response rate = 61.9%); and veterans and military personnel who were in the armed forces on January 1, 1991 (n = 2,614) but were not deployed to the Gulf War (era cohort) (response rate = 62.9%). Women were oversampled, but the data analysis was restricted to men only because the roles and background health complaints of females were different from those reported by males. ORs were calculated, and the proportions of symptoms, disorders, and exposures were compared between the Gulf cohort and the two comparison cohorts. Study investigators controlled for potential confounders, including sociodemographic (age, marital status, education, employment), military (rank, still serving or discharged), and lifestyle (smoking, alcohol consumption) factors. Asthma was reported by 6.5% of respondents in the Gulf War cohort, 4.5% of the Bosnia cohort, and 3.7% of the era cohort. Gulf War cohort participants had higher odds of asthma than Bosnia cohort participants both in the logistic regression model that controlled for sociodemographic and lifestyle variables (OR = 1.2, 95%CI 0.9–1.6) and in the logistic regression model that controlled for sociodemographic variables plus the general health questionnaire (OR = 1.2, 95%CI 0.8–1.6); however, neither of these results was statistically significant. Compared with era veterans, Gulf War participants reported statistically significantly increased odds of asthma both in the logistic regression model that controlled for sociodemographic and lifestyle variables (OR = 1.8, 95%CI 1.4–2.4) and in the logistic regression model that controlled for sociodemographic variables plus general health questions (OR = 1.6, 95%CI 1.2–2.1). The strengths of this study included the use of two different military control groups that came from a large, randomly selected, population-based study population and the fact that it accounted for pre-existing health status and cigarette smoking. One of its limitations was its reliance on unverified self-reported medical symptoms and conditions; however, the committee believed, based on the results of the analyses presented, that differential non-response and recall bias were both unlikely.
Using the results of a survey mailed to the entire cohort of Canadian Gulf War veterans who had been deployed to the Gulf War and a comparison group of personnel who had deployed elsewhere during the same period (overall response rate was 64.5%), Canadian Gulf War veterans were found to have statistically significantly higher odds of reported asthma (OR = 2.64, 95%CI 1.97–3.55) than elsewhere-deployed veterans when adjusted for tobacco smoking, income, and rank (Goss Gilroy Inc., 1998).
Post-9/11 Veterans
The AFHSC (2010) examined medical encounters of U.S. Army and Air Force personnel 36 months after deployment between 2005 and 2007 to Joint Base Balad, Contingency Operating Base Speicher, or Camp Taji in Iraq (all three of which used burn pits for waste management); to Camp Beuhring or Camp Arifjan in Kuwait (which did not use burn pits); or to installations in the Republic of Korea. Service members who were never deployed and stationed only in the continental United States in the same period were used as the comparison population. Asthma was examined using Poisson models that were adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, physical activity, service branch, military rank, pay grade, and occupation. IRRs for asthma were statistically significantly lower for troops deployed to Joint Base Balad (IRR = 0.81, 95%CI 0.73–0.91) and Korea (IRR = 0.91, 95%CI 0.86–0.96) compared with the nondeployed U.S. cohort. No differences in asthma were found for those deployed to Camps Arifjan, Buehring, or Taji compared with the nondeployed U.S. cohort. The investigators also conducted additional analyses using data from the baseline and first follow-up cycles of the Millennium Cohort Study. Multivariable logistic regression adjusted
for the same factors as used in the Poisson models was used to compare the adjusted odds of asthma associated with three metrics of exposure within a 5-mile radius of the documented burn pits: dichotomous deployment near the documented burn pits, cumulative days exposed to the burn pits (presented by quartiles), and exposure to the burn pits at three different campsites (Balad, Taji, or Speicher). The incidence of new-onset asthma was 1.62% for participants with putative exposure to burn pits and 1.63% for the nonexposed. For new-onset asthma, there was no statistically significant difference between service members deployed outside of a 5-mile radius of a burn pit location and those deployed within that radius (OR = 0.89, 95%CI 0.66–1.19). Deployment of cumulative days exposed within 5 miles of the documented burn pits was not associated with increased risk for new-onset asthma for any of the quartiles of exposure compared with the nonexposed group. Furthermore, the odds of new-onset asthma associated with exposure at specific campsites were not increased compared with those deployed outside of the 5-mile radius (p = 0.59).
The committee responsible for the 2017 National Academies report Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry carried out an analysis of the initial months of data gathered from respondents to the registry’s questionnaire (NASEM, 2017). The data were derived from the first 13 months of completed questionnaires (n = 46,404), representing approximately 1.0% of the 1990–1991 Gulf War veterans and 1.7% of post-9/11 veterans who met the registry’s eligibility criteria. Outcomes of asthma were characterized by self-reports of health care provider diagnoses, while exposures to burn pits and other airborne hazards were determined by self-report and by DoD data on the number and location of deployments; 13.0% of respondents self-reported asthma during or after deployment. The committee also synthesized exposure metrics by combining the responses to questions regarding specific exposures. Analyses—which controlled for sex, age, education level, BMI, smoking status, unit component, rank, service branch, and occupation—indicated that the airborne exposure measures had strong and consistent associations with a self-report of asthma. These associations were observed for several indicators of burn pit exposure as well as for a range of other deployment exposures, such as exposures to diesel/exhaust/fuel, construction, dust, and combat. However, the report detailed a number of issues with the quality and limitations of the registry’s information, which led the committee to conclude that the results of the analyses could not be taken at face value and that the identified associations might be an artifact of the population’s selection and the limitations of the self-reported exposure and disease data.
Update of the Scientific Literature on Asthma
This section presents studies of service members and veterans who served in the post-9/11 conflicts followed by studies of veterans who served in the 1990–1991 Gulf War. Within each population, studies that analyzed data from the same cohort are presented together.
Studies that merely described asthma among theater veterans were excluded from consideration. Dursa et al. (2016a) and Cypel et al. (2016) aimed to evaluate asthma diagnoses among Southwest Asia veterans, but neither study evaluated the impact of deployment on asthma diagnosis, and therefore neither study is summarized. Dursa et al. (2016a) evaluated differences in asthma among VA health care users and nonusers. Cypel et al. (2016) examined the sociodemographic, military, and health characteristics of current cigarette smokers, former smokers, and nonsmokers among OEF/OIF veterans and estimated the smoking prevalence to better understand cigarette use in this population. Similarly, Dursa et al. (2019) examined differences in asthma and COPD (among other health outcomes) between females and males who were deployed and nondeployed to the 1990–1991 Gulf War, but differences in asthma prevalence between deployed and nondeployed veterans were not reported, limiting the usefulness of this analysis in informing associations between deployment to Southwest Asia and respiratory outcomes. STAMPEDE I, II, and III, which are all detailed in the PFT section, also presented the prevalences of asthma in their study populations (Morris et al., 2014, 2019, 2020). In STAMPEDE I, asthma was diagnosed in eight participants (16.0%) (Morris et al., 2014). In STAMPEDE II soldiers with abnormal spirometry pre-deployment or asthma history (n = 39) had no indication of worsening lung function post-deployment. Logistic regression models were used to predict obstruction after deployment, and self-reported asthma (p = 0.045) was found to be significantly predictive. In STAMPEDE III, asthma was diagnosed in 87 patients (22.9%) based on obstructive spirometry/impulse oscillometry and evidence of airway hyperreactivity (Morris et al., 2020). Other
studies were identified that reported the total number of individuals with asthma but did not conduct comparisons of this information (Butzko et al., 2019; Morris et al., 2013; Sanders et al., 2005) and therefore are not summarized.
Post-9/11 Veterans
This section includes several studies from the large cohorts that the committee was asked to pay particular attention to as well as smaller studies that used a population from a particular region or care center.
Smith et al. (2008) used self-reported clinician-diagnosed health data from regular, active-duty participants from the first panel (2001–2003) of the Millennium Cohort Study (n = 37,798) to compare the agreement of 38 medical conditions, which included asthma, with that obtained from electronic medical records based on ICD-9-CM codes. Any diagnostic code for these 38 conditions in any portion of the medical record indicated agreement with a self-reported medical condition of interest. Both positive and negative agreement were used to compare self-reported data with those from electronic medical records. Prevalence was 5.8% (95%CI 5.6–6.0) for self-reported asthma and 3.9% (95%CI 3.7–4.1) for electronic medical record–documented asthma; 1.9% was exclusively recorded in the electronic medical records. The positive agreement between self-report and electronic medical records for asthma was 42.0%, and negative agreement (the condition was not reported either by self-report or found in the medical record) was 97.1%. When reports of asthma were examined by length of service (0–5, 6–10, 11–15, and ≥16 years), the self-reported prevalence of asthma was higher than what was recorded in the electronic medical records.
Smith et al. (2009) examined newly reported asthma and other respiratory conditions among 46,077 Millennium Cohort Study participants who completed baseline (2001–2003) and follow-up (2004–2006) questionnaires. Multivariable logistic regression was used to compare the adjusted odds of new asthma relative to deployment status (deployed versus nondeployed) stratified by service branch and adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, service component, military pay grade, and occupational code. Because personnel in different service branches are likely to experience different deployment-related exposures, analyses were stratified by service branch. The adjusted OR for newly reported asthma in deployed versus nondeployed personnel varied, though not statistically significantly for any of the branches, with the highest observed in Army personnel (OR = 1.06, 95%CI 0.77–1.44) and the lowest in Marine Corps personnel (OR = 0.56, 95%CI 0.15–1.98). When the analysis was restricted to deployed cohort members with self-reported information on deployment location (n = 9,861), the investigators stated that the odds of asthma were not statistically different in any of the deployment locations examined, but estimates were not provided.
Smith et al. (2012) investigated the effects of exposure to documented open-air burn pits within 2, 3, or 5 miles on asthma and other respiratory outcomes among Millennium Cohort Study Army and Air Force participants who were deployed to Iraq or Afghanistan after January 1, 2003, and who completed the baseline questionnaire and one of the follow-up assessment cycles through 2008. After excluding individuals with missing data, 20,077 participants who had deployed were included in the analyses of new-onset asthma. Similar proportions of newly reported asthma in 2007 were found for those exposed and nonexposed within 3 miles of a burn pit (1.7% vs 1.6%, respectively). At the end of follow-up, after adjusting for demographic, behavioral, and military characteristics, the odds of newly reported asthma were statistically significantly increased for women (OR = 1.78, 95%CI 1.38–2.32) and Army personnel (OR = 2.27, 95%CI 1.70–3.03), whereas both those who did and did not meet standards for aerobic activity were at reduced risk for asthma compared with those who could not perform aerobic activity. Three proxy exposure metrics were modeled, and analyses were adjusted for demographic and military characteristics, smoking status, and physical activity. Newly reported asthma was not statistically significantly associated with deployment within 3 miles of burn pits (OR = 0.94, 95%CI 0.70–1.27) when compared with deployments to other regions of Iraq or Afghanistan with no documented burn pit exposure. Similarly, deployments within 3 miles of each of the three burn pit sites compared with deployments outside this radius were not associated with increased odds of new-onset asthma: Joint Base Balad (OR = 0.84, 95%CI 0.56–1.25), Camp Taji (OR = 1.53, 95%CI 0.91–2.58), or Camp Speicher (OR = 0.76, 95%CI 0.42–1.38). Similarly, increasing number of cumulative days of exposure within a 3-mile radius of the burn pits was not associated with new-onset asthma compared with cohort members with no burn pit exposure (p = 0.63). The findings of no association with new-onset asthma for deployment status, cumulative deployment length, and camp location were consistent when examining the risk within 5 miles of the burn pits.
Rivera et al. (2018) examined the risk factors for new-onset asthma among eligible Millennium Cohort Study participants (n = 75,770) deployed to Iraq, Afghanistan, noncombat zones, or sea locations during OIF or OEF. The exposure of interest was combat deployment in support of OEF/OIF during the entire follow-up period (October 2000–October 2006), and participants were categorized as nondeployed, deployed without combat, and deployed with combat. The Contingency Tracking System database at the Defense Manpower Data Center (DMDC) was used to extract deployment information. Within the study population, 1,055 (4.6%) of women and 1,452 (2.7%) of men developed asthma during the follow-up time period. Women and men who were not deployed had the highest rates of new-onset asthma (5.0% and 3.1%, respectively), followed by individuals with combat experience (4.4% and 2.7%, respectively). Women reported higher rates of new-onset asthma than men for all strata: exposure of interest, demographic factors, birth year, marital status, education, BMI, military service, service component, occupation, pay grade, smoking status, environmental exposures, stressors, and posttraumatic stress disorder. Among those who deployed and had combat experience, both men and women had a statistically significantly increased risk for new-onset asthma (RRmen = 1.30, 95%CI 1.14–1.47; RRwomen = 1.25, 95%CI 1.05–1.46) compared with men and women who did not deploy, after adjusting for all covariates. No statistically significant differences were found for the association between new-onset asthma and multiple deployments. There was a statistically significant association between a deployment duration of 401–600 days and new-onset asthma in men (RR = 1.35, 95%CI 1.02–1.78), after adjustment for demographic and military factors, including prior deployment to Bosnia, Kosovo, or Southwest Asia between January 1, 1998, and September 1, 2001. The three other deployment lengths that were evaluated (1–200 days, 201–400 days, and >600 days) were not associated with increased asthma. The limitations of this study include the potential for recall or reporting bias, that there was no validation of self-reported new-onset asthma diagnosis with medical charts, the fact that the exact timing of asthma onset could not be ascertained as the questionnaire assessed onset of asthma over the past 3 years, and that questions regarding combat exposure were not specific to a particular deployment.
Using data collected as part of the NewGen Study, Barth et al. (2014) examined the association between deployment to Southwest Asia and self-reported doctor-diagnosed asthma among 13,162 deployed and 7,401 nondeployed veterans. The unweighted and weighted prevalence of asthma was calculated and stratified by diagnosis before or after 2001, and logistic regression was used to calculate adjusted ORs for deployment status and asthma. The models were adjusted for birth year, sex, service branch, unit component, race/ethnicity, education, and smoking status. Separate models were constructed for diagnosis before 2001 and during or after 2001. For those diagnosed before 2001, the weighted prevalence for asthma was higher in the deployed than in the nondeployed (3.7% vs 2.0%). Among those with respiratory disease diagnosed in 2001 or later, the weighted prevalence of asthma was again higher in the deployed than in the nondeployed veterans (3.4% vs 3.3%). Among those diagnosed during or after 2001, the deployed group had odds of asthma that were similar to those of the nondeployed veterans (OR = 1.08, 95%CI 0.89–1.30), but for those diagnosed prior to 2001 the odds of asthma were statistically significantly lower among deployed versus nondeployed veterans (OR = 0.57, 95%CI 0.47–0.70).
Barth et al. (2016a) again used data from the NewGen study to expand on the analysis by Barth et al. (2014) to examine the prevalence of self-reported doctor-diagnosed respiratory diseases and their association with self-reported respiratory exposures during military service for OEF/OIF deployed and nondeployed veterans. Logistic regression analyses were used to calculate weighted, adjusted odds of asthma stratified by deployment status and controlled for sex, birth year, race/ethnicity, education, smoking status, unit component, and service branch, and number of OEF/OIF deployments. A total of 1,366 veterans self-reported asthma (802 deployed and 559 nondeployed). Among the deployed veterans, statistically significant increased odds of asthma were observed for all specific exposures and for both the high-exposure and low-exposure categories; the highest odds for asthma were for those categorized as high exposure (OR = 1.49, 95%CI 1.01–2.20) and with dust and sand as a specific exposure (OR = 1.46, 95%CI 1.06–2.00). For nondeployed veterans, statistically significant increased odds of asthma were also observed for all specific exposures and for both the high-exposure and low-exposure categories; the highest odds for asthma were again for those with categorized as high exposure (OR = 1.92, 95%CI 1.40–2.62) but highest for burning trash or feces as a specific exposure (OR = 1.64, 95%CI 1.29–2.08). These results show that exposures were associated with the development of asthma in both deployed and nondeployed groups, but the confidence intervals for the adjusted ORs all overlap between the deployed and nondeployed groups.
Abraham et al. (2014) built on the AFHSC (2010) analysis by adding an additional 12 months of follow-up (for a total of 48 months) of personnel deployed to four Southwest Asia theater sites with and without burn pits, along with those deployed to Korea and a comparison population of service members who stayed in the United States. Compared with the rate for nondeployed personnel, the rate of medical encounters for new-onset asthma (defined as one hospitalization or at least two outpatient encounters with ICD-9 code 493) among personnel deployed to the four in-theater sites was elevated (IRR = 1.54, 95%CI 1.33–1.78), adjusted for age, gender, race, and military rank. Information on smoking was not factored into the analyses. Compared with the nondeployed U.S. group, rates for bases with burn pits (IRR = 1.59, 95%CI 1.35–1.87) and without burn pits (IRR = 1.39, 95%CI 1.07–1.79) were also statistically significantly elevated for new-onset asthma (as well as for Joint Base Balad and Camp Arifjan, individually). Compared with the rate for personnel stationed in Korea, the rates of medical encounters for asthma were no different between personnel stationed in sites with and without exposure to burn pits. As compared with military personnel deployed at bases without burn pits (Arifjan and Buehring), there was no difference in rates of asthma among those deployed in areas with burn pits (Balad and Taji) (IRR = 0.93, 95%CI 0.69–1.25). These findings indicate that the risk of new-onset asthma is elevated but that the risk is not associated with burn pits specifically.
The analyses by Sharkey et al. (2015) also used the same deployed and nondeployed populations as the AFHSC (2010) analysis but used a larger U.S.-based reference population and included an additional 12 months of data. Their methods also differed from those of Abraham et al. (2014); all three studies are discussed in greater detail in Chapter 3. This retrospective cohort study used Poisson models that were adjusted for age, pay grade, sex, race, and service branch. As was found in the AFHSC (2010) analysis, the risks of respiratory illnesses for personnel deployed to four Southwest Asia bases and Korea were all similar to, or statistically significantly lower than, the risks for personnel who remained in the United States. IRRs were reported for each base location, but no comparisons between bases with and without burn pits were made. IRRs for new-onset asthma (ICD-9-CM: 493) were statistically significantly lower for personnel deployed to Joint Base Balad, Iraq—which had a burn pit—at both the 36-month follow-up (IRR = 0.81, 95%CI 0.73–0.91) and the 48-month follow-up (IRR = 0.82, 95%CI 0.74–0.91) compared with the nondeployed U.S. cohort. The same statistically significantly lower risk was observed for troops deployed to Korea compared with the nondeployed U.S. group at 36 months (IRR = 0.91, 95%CI 0.86–0.96) and 48 months (IRR = 0.91, 95%CI 0.86–0.97). There were no statistically significant differences in new-onset asthma for the other deployed locations compared with the nondeployed cohort. Information on smoking was only available for Air Force personnel, and the authors report that no significant difference in risk for any of the health outcomes of interest was found after adjusting for smoking status.
Baird et al. (2012) examined the post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant near Mosul, Iraq, in 2003. Two were groups potentially exposed to the sulfur fire smoke plume—personnel involved in fighting the fire (n = 191) and personnel presumably downwind during the time of the fire (n = 6,341). These were compared with two unexposed groups: those who deployed to the area after the fire was extinguished (n = 2,284) and those deployed to other Southwest Asia locations contemporaneously with the time of the fire (n = 1,869). Asthma encounters (ICD-9-CM 493) were statistically significantly less likely for the potentially exposed personnel downwind of the fire than for the group deployed to the area after the fire was extinguished (standardized mortality ratio [SMR] = 0.62, 95%CI 0.53–0.71), but there was no difference between the downwind personnel and the contemporaneously deployed group. Firefighters were less likely to have post-deployment medical encounters for asthma than the contemporaneously deployed group (SMR = 0.91, 95%CI 0.29–1.87) and the group deployed to the area after the fire (SMR = 0.62, 95%CI 0.20–1.27), although neither difference was statistically significant. The inverse association for observed asthma may reflect the short follow-up time and the young age of the population being studied as well as the lack of adjustment for other potentially important confounders, including smoking and other environmental or occupational exposures, between the sulfur-fire exposed and unexposed groups.
Abraham and Baird (2012) conducted a case-crossover study of short-term (i.e., 0- and 1-day lagged) exposures to ambient PM less than 2.5 microns in aerodynamic diameter (PM2.5) and less than 10 microns in diameter (PM10) and cardiovascular and respiratory medical encounters (ICD-9 460–519) among 2,838 U.S. military personnel deployed to Southwest Asia. PM exposure was assessed using data collected over a period of approximately 1
year at 15 military bases, including 6 sites in Iraq, 4 in Kuwait, 2 in Afghanistan, 1 in Qatar, and 1 in the United Arab Emirates. Site-specific estimates were first obtained and then pooled using meta-analytic techniques to generate OR for a 10-µg/m3 increase in PM2.5 or PM10. Ambient levels were routinely high at the bases assessed, but no statistically significant associations between PM and respiratory outcomes were observed in the young, relatively healthy, deployed military population. Of the 343 encounters for COPD and allied conditions (ICD-9 490–496), though, 327 (95%) were reported to be for asthma (ICD-9 493). Following adjustment for temperature, barometric pressure, and relative humidity, all pooled effect estimates at lag 0 and lag 1 were close to 1.0, and none achieved statistical significance. Similar results were obtained in sensitivity analyses in models that evaluated 2-day lagged exposures as well as PM estimates using imputed data for missing values. No consistent pattern was found for associations between PM and asthma or any other condition (specific effect estimates not presented). The adjusted ORs for a 10-µg/m3 increase in ambient PM2.5 and a qualifying medical encounter were not statistically significant for the current (lag_0) day (OR = 0.92, 95%CI 0.77–1.11) and previous (lag_1) day (OR = 1.01, 95%CI 0.95–1.07). The estimates for a 10-µg/m3 increase in PM10 were again not statistically significant at lag_0 (OR = 0.99, 95%CI 0.97–1.03) and lag_1 (OR = 1.00, 95%CI 0.97–1.02). Overall, increases in ambient PM were not found to increase asthma incidence. This study is one of the few studies with objectively measured exposure, the strengths and limitations of which are summarized in Chapter 3.
Sharkey et al. (2016) extended the analysis of the AFHSC (2010) report by adding additional Army or Air Force personnel who were deployed to Kabul (n = 5,670) and Bagram (n = 34,239) Air Force Bases in Afghanistan—sites with similar, poor air quality—and Manas Air Force Base in Kyrgyzstan (n = 15,851), a site with relatively better air quality, and extended the follow-up period of active-duty personnel to 12 years. Asthma cases were defined as a study participant having either one inpatient or at least two outpatient health care encounters labeled with ICD-9-CM-coded asthma-related visits. Deployment-location-specific IRRs for asthma were calculated after excluding any study participants with a history of diagnosis of asthma, and the models were adjusted for age, rank (defined at the start of follow-up), sex, and race. Information on smoking was available only for Air Force personnel, and the authors report no evidence of confounding as RRs were similar with and without adjustment for smoking status. IRRs were highest for active-duty service members deployed to Kabul compared with the U.S. reference group (IRR = 1.61, 95%CI 1.22–2.12), but there were no differences when compared with the Korea (IRR = 1.01, 95%CI 0.69–1.49), Manas (IRR = 1.03, 95%CI 0.72–1.49), or Bagram (IRR = 1.01, 95%CI 0.75–1.35) reference groups, after adjusting for age, sex, and military rank.
Liu et al. (2016) examined the associations between assumed geographic and self-reported burn pit emissions exposure and respiratory and cardiovascular outcomes in participants of VA’s Airborne Hazards and Open Burn Pit Registry. The study included 4,343 participants who completed the registry questionnaire by April 30, 2015, and, of these, 2,663 participants deployed for at least 30 days from January 1, 2003, to June 30, 2007, within 2 miles of burn pits in Joint Base Balad or Camp Taji in Iraq, and 1,680 participants were deployed for at least 30 days to Kuwait (but not to Joint Base Balad or Camp Taji) during that timeframe. There were no documented burn pits at Kuwait bases. Two surrogate measurements of burn pit emissions exposure were used in the analysis: days of deployment near burn pits and self-reported total hours of burn pit smoke exposure. Associations were presented by quartiles of burn pit exposure. Self-reported diagnoses were compared with VA medical record information for 2,857 respondents who used VA health care at least once between January 2007 and November 2015. Participants who reported having been diagnosed with a condition before deployment were excluded from both the analyses of self-report and the comparisons with VA medical records for that condition. All demographic characteristics (except marital status), military characteristics, and other factors, such as in-person clinical examination request and smoking status, were found to be statistically significantly associated with deployment days within 2 miles of the burn pit sites. Associations between demographic, lifestyle (with exception of smoking), and military service variables and self-reported burn pit smoke exposure amount were all found to be statistically significantly associated with self-reported burn pit smoke exposure. Models were adjusted for demographic, lifestyle (including smoking status), and military service characteristics. No statistically significant associations were found for any of the quartiles of deployment time within 2 miles of the burn pit locations and asthma, either from self-report or as identified in VA medical records, after adjusting for demographic, lifestyle, and military service variables. Likewise, no statistically significant associations were found for any of the quartiles of total hours of burn pit smoke exposure and
asthma, either from self-report or as identified in VA medical records, after adjusting for demographic, lifestyle, and military service variables. This study is most limited by the use of self-reported exposures and by the fact that the study population consists of a self-selected group of individuals.
Pugh et al. (2016) conducted a retrospective cohort study to examine the prevalence of chronic lung diseases, including asthma, based on ICD-9-CM codes and military deployment using VA health care data from 760,621 U.S. veterans deployed to combat operations in Iraq or Afghanistan who received care from VA between October 1, 2002, and September 30, 2011. The prevalence of asthma was calculated for each year between 2003 and 2011 using the number of unique OEF/OIF veterans who received care from VA during the year as the denominator for that year, and the data were examined for any changes in prevalence during that time. Generalized estimating equations analysis was used to determine if the log-odds of having a diagnosis of asthma increased from 2003 to 2011; estimates were adjusted for demographic characteristics, multiple deployments, tobacco use, and traumatic brain injury (TBI). Over the study period, 25,592 (3.4%) individuals had a diagnosis of asthma; they were more likely to be male, white, and to have served in the Army; 26.5% were classified as tobacco users, and 14.6% had a TBI diagnosis. Based on the generalized estimating equations analysis and controlling for demographic and clinical characteristics, the odds of diagnosis of asthma were statistically significantly higher in 2011 than in other earlier years of the study. Moreover, the odds of asthma were statistically significantly increased for the 31–40 years and 41–50 years age groups (but not ≥51 years) compared with the ≤30 years age group, as well as for those with a TBI diagnosis (OR = 1.47, 95%CI 1.42–1.53) and tobacco users (OR = 1.17, 95%CI 1.14–1.21). Individuals who had multiple deployments were statistically significantly less likely to have a recorded asthma diagnosis (OR = 0.93, 95%CI 0.91–0.96) than individuals with only one deployment. Although the study population was large and included a more objective measure of asthma using ICD-9-CM codes, the temporal sequence between deployment and the onset of asthma is unknown, and the population was limited to those who received care within the VA health system. Because the veterans studied may have been too young for many to have developed symptoms of chronic pulmonary diseases, these results may be subject to both selection and ascertainment biases. Although it appears that what was reported as change in prevalence by year is really incidence of new diagnoses; however, new cases may be a mixture of incident and prevalent cases, with some patients coming to VA to receive care when disease becomes severe enough to need treatment, and therefore these are prevalent cases that are considered incident in that they were not previously counted.
Szema et al. (2010) conducted a retrospective cohort study—described previously in the pulmonary function section—in U.S. military service members who were deployed to OEF/OIF or elsewhere (matched on age and gender) using data collected by the Northport, New York, VA Medical Center Research and Development Committee to examine if the deployed were more likely to have asthma or respiratory symptoms requiring the use of spirometry than were nondeployed service members. The clinical guidelines for a diagnosis of asthma at Veterans Affairs Medical Centers include
recurrent episodes of respiratory symptoms (cough, wheeze, dyspnea, and exercise-induced shortness-of-breath) with spirometric evidence of airway obstruction based on the forced expiratory volume in 1 second/forced vital capacity (FEV1/FVC) or forced expiratory flow at 25–75% at rest, with improvement of symptoms after bronchodilators. (Szema et al., 2010, p. e68)
Spirometry was obtained, when available, from patient medical records. Asthma diagnoses for military personnel aged 18–45 years were examined among patients who were residents of Long Island, and who were discharged from active duty and were examined between March 1, 2004, and May 1, 2007. Service members were grouped by deployment location (Iraq/Afghanistan for a 1-year tour of duty versus United States) and by ICD-coded diagnosis of asthma in VA records. Crude ORs stratified by gender and age group were calculated for associations between deployment and asthma. Of the 6,233 patients in the study sample, 290 had asthma—61 (6.6%) of deployed and 229 (4.3%) of nondeployed—and the odds of asthma were increased for deployed service members compared with nondeployed service members (OR = 1.58, 95%CI 1.18–2.11). This study is most limited by the selection bias resulting from using a study population based on one VA clinic, which may have a different distribution of risks for asthma than the rest of the post-9/11 population. Furthermore, study investigators used deployment during
2003–2007 as a crude measure of exposure, making it likely that misclassification of exposure occurred. Although ICD-coded asthma diagnoses were used, it was not clear if people with pre-existing asthma were removed from the population. Spirometry was performed on only a subset of asthmatics, and no pre-spirometry measures were available for comparison. Finally, only crude ORs were presented, and no adjustment for several potential confounders was included.
Abraham et al. (2012) conducted a cohort and nested case–control study to evaluate the relationship between deployment and respiratory system diseases (ICD-9 460–519) in U.S. military personnel. Cases (n = 532) of postdeployment diagnosis of obstructive pulmonary disease, defined as ICD-9-CM codes 490–496, and controls (n = 2,128) were selected from those who were free of respiratory diagnoses within 6 months before their deployment. Controls were matched on the year of case definition and the year of the last encounter during the study period for controls as well as the total number of post-deployment medical encounters. Conditional logistic regression analyses were used to examine the independent effects of the number of deployments at diagnosis and of the cumulative time in theater up to diagnosis on post-deployment obstructive pulmonary disease encounter, controlling for potential confounders (gender, age, grade, occupation, time in theater, number of deployments, service branch, and tobacco-related diagnoses). The vast majority of obstructive pulmonary disease encounters were for either asthma (46%) or bronchitis (50%). Adjusted odds of having an obstructive pulmonary disease encounter were not different for multiple deployers compared with single deployers (OR = 1.08, 95%CI 0.82–1.42). This study had several limitations, such as a lack of measurement of smoking and a lack of specific deployment-related exposure assessments. Additionally, given that asthma and other obstructive lung diseases were all considered together, the study findings do not provide specific information on the impact of service in Southwest Asia and asthma.
1990–1991 Gulf War Veterans
Four studies of 1990–1991 Gulf War veterans and outcomes of asthma were identified since the publication of the Gulf War and Health: Volume 10 report; three studies examined U.S. Gulf War veterans. Three of those are cohort studies, and the fourth is a meta-analysis of studies that compared Gulf War–deployed and Gulf War–era–nondeployed veterans. These are presented before the study of new-onset asthma in Australian Gulf War veterans.
Hines et al. (2013) conducted a small study using 24-hour creatinine-corrected urinary uranium as a validated marker of exposure in 1990–1991 Gulf War veterans who were enrolled in the VA Depleted Uranium Surveillance Program and had attended a biennial follow-up in 2011 (n = 37) to compare the likelihood of pulmonary health abnormalities in those with high body burdens of uranium (n = 12; >0.1 µg/g creatinine) versus those with low body burdens of uranium (n = 25; ≤0.1 µg/g creatinine). Two participants self-reported asthma, and both had low urinary uranium, providing some evidence that depleted uranium may have limited impact on asthma. Of these two veterans with self-reported asthma, one was a never smoker and one was an ever smoker, which did not result in any statistically significant differences of asthma by smoking status.
Zundel et al. (2019) compared survey results from a follow-up survey of a cohort of 1990–1991 Gulf War veterans (401 males and 47 females) who returned from deployment in 1991 through Fort Devens, Massachusetts, with data from the 2013–2014 NHANES (n = 2,949). The veterans were asked to report if a doctor had ever diagnosed them with any of nine chronic medical conditions, including asthma. The analyses were restricted to veterans of white race with at least a high school education, and they were stratified by sex. The analyses were also weighted to account for demographic differences between cohorts. The prevalence of asthma was higher among the Fort Devens cohort than reported by NHANES for men (13.6% vs 10.9%, respectively), but the difference was not statistically significant (OR = 1.29, 95%CI 0.75–2.23). For women, the prevalence of asthma was lower among the Fort Devens cohort than among the NHANES cohort (10.3% vs 18.6%, respectively), but the difference was not statistically significant (OR = 0.50, 95%CI 0.22–1.17). When the prevalence of asthma was compared for men stratified by age group (40s, 50s, and 60s), no difference between Fort Devens and NHANES was found for any of the age groups. For the Ft. Devens exposure analyses, there were no differences on any of the demographic variables between veterans who were exposed and those who were unexposed to chemical or biologic warfare or pyridostigmine bromide pills, but analyses for exposure were adjusted for gender and current smoking status. For those exposed to chemical or biologic warfare, the prevalence of asthma was higher than among the unexposed (18.5% vs 10.3%, respectively), but this difference was not statistically significant (OR = 1.94, 95%CI 0.90–4.20).
Similarly, the prevalence of asthma was slightly higher for those exposed to pyridostigmine bromide pills than for the unexposed (12.5% vs 11.5%, respectively), but this difference was not statistically significant (OR = 1.13, 95%CI 0.51–2.51). Finally, asthma prevalence was compared between men and women of the Fort Devens cohort; no difference in prevalence was found after adjustment for age, race, education, and current smoking (OR = 1.57, 95%CI 0.53–4.68). This study has several limitations, including its generalizability, its use of self-reported conditions, and its low response rate.
In a meta-analysis of 21 studies published through 2017 on prevalence of health symptoms, including asthma, representing more than 129,000 1990–1991 Gulf War–deployed and nondeployed era veterans, Maule et al. (2018) found that in pooled analyses a higher combined prevalence of asthma was found for deployed than for era veterans (4.8% vs 3.4%, respectively). ORs were reported for each outcome along with I2 statistics (a measure of the heterogeneity, or the percentage of variation across studies that is due to heterogeneity rather than chance). The odds of asthma were statistically significantly increased for Gulf War veterans compared with era veterans (OR = 1.38, 95%CI 1.20–1.58; seven studies), and the heterogeneity was substantial (I2 = 0.47). The meta-analytic approach could not address concerns about either selection biases or information biases (due to self-reports of symptoms), concerns that were common in all of the included studies. Moreover, the committee also notes that some other important deficiencies in the published studies, such as individual design and population selection, and their impacts on the findings were not addressed.
Other 1990–1991 Gulf War Coalition Forces Veterans
As first described in the section on Sleep Apnea, Gwini et al. (2016) examined new onset of self-reported conditions in deployed Australian Gulf War veterans using data collected from wave 1 (conducted 10 years after the Gulf War) and wave 2 (conducted about 10 years after wave 1 and 20 years after the Gulf War) of the Australian Gulf War Veterans’ Health Study. Both wave 1 and wave 2 used a questionnaire to collect information on general health, physical and psychological health, military service history, and exposures during deployment, and they also included a comprehensive health assessment, a full physical examination, blood work, and fitness tests for each individual. For this analysis, Gulf War veterans were grouped into low (n = 272), moderate (n = 328), and high (n = 80) symptom reporting groups at wave 1 and assessed at wave 2 for selected symptoms and disease diagnosis to determine new onset or the incidence of particular conditions, one of which was asthma. Those who reported the prevalence of a condition of interest at wave 1 were excluded in the analyses of onset for wave 2. Logistic, nominal, and ordinal regressions were used for between-group comparisons. Regression models were adjusted for age group, service branch, and rank estimated as of August 1990, smoking status, alcohol use, BMI, and highest educational level attained at wave 1. New-onset asthma was no different between the high- and the low-symptom reporters (OR = 2.12, 95%CI 0.44–10.22) or between the moderate- and the low-symptom reporters (OR = 0.51, 95%CI 0.12–2.10). The authors found that the odds of obesity and alcohol use increased over time, and the odds of smoking halved; these findings were similar across symptom groups. The findings from the Australian Gulf War Veterans’ Health Study likely lack generalizability to studies of respiratory disorders in U.S. Gulf War veterans, primarily because 85% of the Australian Gulf war veterans were Navy personnel, who likely did not have the same exposures—even when off ship—as U.S. ground forces. Furthermore, no analyses were presented to compare differences in those who participated in wave 2 with those who did not, which was half the cohort, and therefore confounding by indication cannot be ruled out for wave 2 respondents.
Lung Function and Asthma Severity
Some recent studies have used tests of lung function to assess whether Gulf War exposures affect asthma severity.
DelVecchio et al. (2015) reviewed DoD medical records from the Medical Evaluation Board to identify 400 consecutive active-duty Army personnel from 2005 to 2009 with an ICD-9 code for asthma who underwent fitness-for-duty evaluations for asthma. Of these 400, spirometry was performed on 355, of whom 227 were also assessed for bronchodilator response, and another subset had a methacholine challenge study. Deployment information was obtained from the AFHSC. Spirometry was compared between those deployed (defined as having been deployed to Southwest Asia at least once for at least 60 days) and those not deployed. Among the deployed, comparisons were also made between those diagnosed with asthma pre-deployment and those diagnosed post-deployment.
FEV1 (% predicted), either pre- or post-bronchodilator, and FEV1/FVC were not significantly different in those deployed compared with those not deployed. Among those deployed there were no differences in those diagnosed with asthma pre-deployment versus those diagnosed post-deployment. The rationale for making these comparisons is not clear. It is not obvious what is learned by comparing the level of lung function in those deployed who had a diagnosis of asthma before deployment and those who had a diagnosis only after deployment. What is of interest here is whether asthma severity, as reflected by measures of lung function or bronchial responsiveness, is worsened with deployment-related Gulf War exposures. This study provides no information that bears on that question.
Although not published at the time of writing, the committee reviewed a submitted paper, Woods et al. (2018),9 which updated the DelVecchio et al. (2015) study to include information on 642 active-duty Army personnel with a diagnosis of asthma. The record review was expanded to include those deployed to Southwest Asia between 2003 and 2015. Only 71 individuals had both pre- and post-deployment spirometry. The use of inhaled corticosteroids or long-acting beta agonists, medications commonly used to manage all but very mild or intermittent chronic asthma, was very infrequent (6.6% and 5.3%, respectively), indicating that these individuals for the most part had very mild asthma (Michael J. Morris, Pulmonary Disease Service, Brooke Army Medical Center, personal communication, October 4, 2019). Mean pre- and post-deployment FEV1 was 86% of predicted and 87% of predicted, respectively, and not statistically significant (p = 0.56). FVC was 94% of predicted and 95% of predicted, respectively, and again not statistically significant (p = 0.46). In the subgroup of individuals with bronchodilator testing who had worse baseline control of asthma, pre- and post-deployment FEV1 was 80% and 84% of predicted (p = 0.16) and FVC was 92% and 97% of predicted (p = 0.04), respectively. No statistically significant change in pre- and postdeployment inhaled corticosteroid and long-acting beta agonist use was reported. The authors reported a trend for increased FEV1 and increased FVC after deployment in the group that had bronchodilator testing as well as for those who had worse baseline control of asthma prior to deployment. The comparison of lung function measures both pre- and post-deployment in those with asthma in this study, which is the only study in which this was done, more directly addresses the question of asthma severity and Southwest Asia exposures than DelVecchio et al. (2015). Although the statistical power of this study to detect adverse effects of deployment is limited, the findings provide evidence that deployment was not associated with worsening of asthma in those with very mild or intermittent asthma, at least as measured by spirometry and response to bronchodilator. Whether asthma control was worse during deployment was not addressed.
In a retrospective observational cohort study of 1,193 active-duty soldiers and contractors returning from OEF or OIF deployment through a single processing center, Roop et al. (2007) used a questionnaire to compare the prevalence, severity, and impact of respiratory symptoms occurring in asthmatics and nonasthmatics. The questionnaire collected information on demographics; smoking history, including changes to patterns during deployment; and the respiratory outcomes of shortness of breath, cough, wheezing, sputum production, chest pain/tightness, and allergy symptoms (sneezing, rhinorrhea, or eye irritation). Respondents were asked about the timing of these outcomes (before or during deployment) and to rank the frequency of respiratory symptoms. They were also asked whether respiratory symptoms impeded job activities and whether they sought medical attention for breathing problems during deployment. Those who reported a previous diagnosis of asthma were asked about the diagnosis method and the frequency of day/night asthma symptoms (e.g., shortness of breath, wheezing, cough). For a subgroup analysis, well-controlled asthmatics were identified as those reporting daytime asthma symptoms “never” or “less than two times per week” and nocturnal symptoms “never” or “less than once per month,” based on established guidelines. Asthmatic respondents were asked about medication use (e.g., daily to control their asthma or as needed) and to name the medications. Comparisons were made between nonasthmatics and asthmatics, between well-controlled and uncontrolled asthmatics, and between smokers and nonsmokers. McNemar’s test was used to compare changes in the variable distribution during deployment versus before deployment. The mean age of participants was 38 ± 11 years, 83% (n = 977) were male, and 31% (n = 375) were past or present smokers. A previous asthma diagnosis was reported by 61 individuals (5%). New or increased symptoms of shortness of breath during deployment (mean change in Borg dyspnea score, 2.4 ± 2.0) were reported by 155 (13%). During deployment, the respiratory symptoms reported to have increased most were cough (37%) and allergic rhinitis symptoms (38%). During deployment respiratory symptoms affected job performance in 153 participants (13%). A total of 186 participants (16%) sought
___________________
9Woods et al. (2018) is available from the National Academies’ public access file.
medical attention for respiratory complaints; of these, 52 received a temporary duty limitation. Of those seeking medical attention, 19 were hospitalized, of whom 6 required evacuation from the area and 6 required evacuation from the theater of operations. Before deployment, subjects with a history of asthma noted a higher prevalence of all respiratory symptoms and reported more trouble performing their military duties. During deployment, these individuals continued to report more chest wheezing (p <0.001) and sputum production (p <0.05) than nonasthmatics, but statistically significant differences between those with and without asthma were not observed for cough, chest tightness, or allergic symptoms. During deployment, asthmatic personnel continued to have more respiratory symptoms while performing military duties and sought medical attention more frequently than nonasthmatic personnel (44% vs 14%; p <0.001). The increased percentage of persons reporting respiratory symptoms and functional limitations during deployment was similar in those with and without asthma. Among those who were asymptomatic before deployment, there was no statistically significant difference in the proportion of asthmatics and nonasthmatics who developed new symptoms during deployment. Of those who had reported being asthmatic before deployment, 55 (90%) reported taking medications only as needed. Sixteen (26%) asthmatic individuals were considered poorly controlled, and they reported statistically significantly more wheezing, cough, sputum production, and chest pain/tightness than those in the well-controlled group, both before and during deployment (p <0.05 for all symptoms). The poorly controlled group also reported more difficulty with physical training than the well-controlled group (p <0.05). Poorly controlled asthmatics sought medical attention for respiratory symptoms more often than well-controlled asthmatics (n = 11, 69% vs n = 14, 35%; p <0.05). About 11% of respondents were past smokers, and 20% (n = 234) were active smokers at the time of the survey. During deployment, 59% of the active smokers reported smoking more heavily, and 12% reported smoking less. Both before and during deployment those with a history of smoking reported a higher prevalence of all respiratory symptoms except allergies. There was no significant difference in the performance of field duties between smokers and nonsmokers. Smoking rates were similar among asthmatics (n = 21, 34%) and nonasthmatics (n = 350, 31%), but it was more common in the poorly controlled asthmatics group than in the well-controlled group (n = 10, 63% vs n = 8, 20%; p <0.01). During deployment, after controlling for smoking, compared with well-controlled asthmatics the poorly controlled asthmatics had significantly more wheezing, cough, sputum production (p <0.01 for all), and chest pain/tightness (p <0.05) as well as greater difficulty passing the physical fitness test, running in formation, and wearing the chemical protective mask (p <0.05 for all). Although there was a 95% response rate to the questionnaire and the study sample size was relatively large, there were several limitations to this study. All information was based on self-report, with no medical record or other objective test validation. The authors noted the possibility of underreporting by those fearing curtailment to professional opportunities and overreporting by those seeking disability or benefits. The number of self-reported asthmatics was relatively small, and the study sample was derived from soldiers redeployed through one processing center. The authors also noted that few of the respondents were in traditional combat specialties (infantry, armor, field artillery) but also said that many deployed to Southwest Asia undergo activities and exposures that are similar to those of traditional combat soldiers. Those who were evacuated from theater with severe respiratory problems may not have been redeployed and thus would have been excluded from the sample.
Synthesis
Based on the asthma studies of 1990–1991 Gulf War veterans summarized previously in Gulf War and Health Volumes 4, 8, and 10 and new studies reviewed in that population in this report, the committee found no evidence of a difference in asthma diagnoses among studies of Gulf War veterans.
Studies of asthma among post-9/11 veterans were mixed in terms of observing a relationship between asthma diagnosis and deployment to Southwest Asia. Among the Millennium Cohort studies there were mixed results, but each analyzed slightly different research questions. Smith et al. (2009) was a null study and observed that deployers had similar proportions reporting asthma. Smith et al. (2012) observed that women and army personnel had increased odds of an asthma diagnosis but did not observe an association with deployments to regions with burn pits compared with other regions of Iraq and Afghanistan. Rivera et al. (2018) observed that women and men who had combat experience had an increased risk of a new asthma diagnosis. NewGen studies also showed varying relationships between deployment to Southwest Asia and asthma. Barth et al. (2014) found no difference
between asthma diagnosis after 2001 comparing deployed with nondeployed veterans. Barth et al. (2016a) found associations between some exposures and asthma, but the risks of those exposures were similar between the deployed and nondeployed groups.
Other studies that examined the impact of specific exposures on asthma did not observe a positive association. Baird et al. (2012), who evaluated the influence of exposure to the Al Mishraq sulfur mine fire on asthma, observed that asthma encounters were less likely for firefighters and other highly exposed groups. Abraham et al. (2012) observed that increases in ambient PM did not increase asthma incidence. Using data from the burn pits registry, Liu et al. (2016) observed no association between burn pit exposure and asthma.
Studies not mentioned in the Statement of Task also had mixed results. The studies of the AFHSC and similar studies that used DoD medical records data had findings that differed slightly due to differences in reference groups or exposure estimates. Abraham et al. (2014) observed that the rates of medical encounters for asthma were higher among those deployed to Southwest Asia than among the nondeployed and that rates of medical encounters for asthma were similar between those deployed to Southwest Asia and those deployed to Korea. On the other hand, Sharkey et al. (2015) observed largely null associations with deployment and asthma development and had a larger comparison group than Abraham et al. (2014). Sharkey et al. (2016) observed an increased incidence of asthma among those deployed to Kabul compared with the U.S. reference group, but not compared with the other control locations. Pugh et al. (2016) examined the impact of multiple deployments to theater and found no association between multiple deployments and asthma incidence. Szema et al. (2010) found associations between deployment to theater and asthma incidence compared with those in a U.S.-based comparison group.
One of the reasons for the observation of these mixed findings is that the military has been allowing more active-duty service members with asthma. Specifically, during the times of these study periods there were changes in the ability to obtain a medical waiver for asthma and in the policy of including asthma as a diagnosis that medically disqualified individuals from enlistment. These changes resulted in an increasing prevalence of asthma as a chronic lung disease, and such temporal changes may have influenced study findings (Garshick, 2019). Another limitation is that all of the studies relied on either participant self-report of asthma, which may lead to an over-reporting of outcomes (Smith et al., 2008), or apply administrative data, which may under-report cases by excluding encounters outside of a specific medical system (such as VA or DoD health systems) and may only identify the most severe encounters. Epidemiologic studies that use standardized measures of evaluating asthma, such as those recommended in the ATS/ERS consensus statement in standardizing endpoints for asthma clinical trials (Reddel et al., 2009), may be more likely to find an association if there is one.
The question of deployment-related worsening of asthma as determined by spirometric measures was addressed essentially by only one study that was submitted but not yet published. That study (Woods et al., 2018), as did the Morris et al. (2019) study, described in detail in the PFT section, used both pre- and post-deployment spirometry, but in contrast to the Morris et al. (2019) study, Woods et al. (2018) used paired analyses where appropriate. The study provided evidence that deployment was not associated with a persistent worsening of asthma in those with very mild or intermittent asthma, at least when asthma severity was assessed by spirometry and response to bronchodilator. Whether asthma control was worse during deployment was not addressed. Roop et al. (2007) used standard questionnaires to compare the prevalence, severity, and impact of respiratory symptoms occurring in asthmatics and nonasthmatics. They found that during deployment, asthmatic personnel had more respiratory symptoms while performing military duties and sought medical attention more frequently than nonasthmatic personnel, but the results may suffer from recall bias due to the retrospective nature of the design. Studies evaluating the impact of deployment on asthma control and risk of exacerbations should be considered, especially given that the prevalence of asthma has been increasing among those receiving VA care since 2003 (Pugh et al., 2016) and that there are likely more people with asthma in the military due to the changes in the policies for receiving medical waivers.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of asthma.
Chronic Obstructive Pulmonary Disease, Emphysema, and Chronic Bronchitis
COPD is a common, preventable, and treatable disease characterized by persistent respiratory symptoms and by airflow obstruction that is due to airway or alveolar abnormalities. The most common cause of COPD is cigarette smoking (NHLBI, 2020b), but it can also be the result of exposure to noxious particles or gases. The term “COPD” is applied to a family of obstructive pulmonary diseases that primarily includes chronic bronchitis and emphysema.
Chronic bronchitis is an inflammation of the lining of the bronchial tubes that is manifested by mucous hypersecretion and defined as a cough and or phlegm production four to six times per day, 4 or more days per week for more than 3 months of the year. The symptoms can include cough, mucous production, wheezing, and difficulty breathing. The most common cause of chronic bronchitis is cigarette smoking. Outdoor air pollution and vapors, dusts, gases, and fumes in the indoor environment or workplace can also contribute to the condition. Chronic bronchitis is a relatively common illness in the United States, with an estimated prevalence of 3.4% in adults over 18 years of age in 2018 (CDC, 2018).
Emphysema is another phenotype of COPD that is characterized by the destruction of the elastic fibers of the alveolar walls resulting in the collapse of small airways, air trapping, and impaired expiratory airflow. As is true for chronic bronchitis, smoking is the most common cause of emphysema, but workplace exposure to some vapors, dusts, gases, and fumes as well as to indoor biomass smoke and other pollutants has also been linked to the disease. Emphysema had an estimated prevalence of 1.3% in adults over 18 years of age in the United States in 2018 (CDC, 2018).
Over the past several years, there has been a concerted effort to establish standardized clinical assessment criteria for the diagnosis of chronic bronchitis and emphysema. Standardized questions about the symptoms of cough, sputum production, wheeze, and dyspnea have been used for over 40 years to define chronic bronchitis (Ferris, 1978). For COPD and emphysema, spirometric testing has been used to establish the diagnosis and to assess the severity of disease. The standard clinical measurement is the ratio of a person’s FEV1, to his/her FVC. While a post-bronchodilator fixed FEV1/FVC ratio of less than 0.7 is generally considered a spirometric criterion for airflow limitation (GOLD, 2018), age-adjusted FEV1/FVC at the lower limit of normal (from large-scale representative general populations) has been offered as an alternative (Shirtcliffe et al., 2007). The two methods produce minor differences in scoring in that GOLD yields a slightly higher estimate of false-negative diagnoses in younger subjects (less than age 40) and a slightly greater number of false-positives in older populations (over age 50) (Culver, 2006). Because most studies to date have been done in relatively young populations, the impact of using these different criteria would be greater. This concern does not influence the committee’s conclusion because the incidence of COPD was consistently observed to be relatively low across studies. There have also been efforts to advance other diagnostic tools, such as CT scans, to confirm the anatomical lesions associated with suspected airways obstruction.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Studies of COPD, chronic bronchitis, and emphysema in active-duty personnel and veterans who have served in the Southwest Asia theater have been reviewed in multiple previous volumes of the National Academies Gulf War and Health series (IOM, 2005, 2006, 2010; NASEM, 2016) and related reports (IOM, 2011; NASEM, 2017). The only time when conclusions regarding these outcomes were specifically offered in these earlier reports was in Volume 3 (IOM, 2005), which addressed health effects related to exposure to fuels, combustion products, and propellants. The committee responsible for that report—which relied on literature published through early 2004 and which considered studies of occupationally exposed populations in addition to military personnel and veterans—came to the following determinations from its assessment of the epidemiologic evidence:
- There is inadequate/insufficient evidence of an association between exposure to combustion products and the development of COPD as defined by irreversible airflow obstruction.
- There is inadequate/insufficient evidence of an association between short-term exposure (less than 1 year) to combustion products and chronic bronchitis.
- There is inadequate/insufficient evidence of an association between exposure to combustion products and the development of emphysema.
- There is inadequate/insufficient evidence to determine whether an association exists between exposure to fuels and any specific, nonmalignant respiratory outcomes, including bronchitis and emphysema.
Later literature reviews presented in Volumes 4, 8, and 10 (IOM, 2006, 2010; NASEM, 2016) addressed non-cancerous respiratory disease in general. As noted elsewhere in this chapter, the committees responsible for those reports concluded that the then-available literature constituted insufficient or inadequate evidence to determine whether an association existed between deployment to the theater and respiratory disease, including COPD, chronic bronchitis, and emphysema. Neither Long-Term Health Consequences of Exposure to Burn Pits in Iraq and Afghanistan (IOM, 2011) nor Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry (NASEM, 2017) drew conclusions about specific respiratory health outcomes.
The committee responsible for the 2017 National Academies report Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry carried out an analysis of the initial months of data gathered from respondents to the registry’s questionnaire (NASEM, 2017). The data were derived from the first 13 months of completed questionnaires (n = 46,404), representing approximately 1.0% of the 1990–1991 Gulf War veterans and 1.7% of post-9/11 veterans who met the registry’s eligibility criteria. Health outcomes were characterized by self-reports of health care provider–diagnosed conditions; exposures to burn pits and other airborne hazards were based on self-report and on DoD data on the numbers and locations of deployments. A total of 14.3% of respondents self-reported emphysema, chronic bronchitis, or COPD during or after deployment. The committee synthesized exposure metrics by combining the responses to questions regarding specific exposures. A number of analyses were conducted using these measures, controlling for age, sex, smoking history, and BMI. In summary, these indicated that the airborne exposure measures had strong and consistent associations with a self-report of diagnosed emphysema, chronic bronchitis, or COPD. The associations were observed for several indicators of burn pit exposure as well as for a range of other deployment exposures, such as exposures to diesel/exhaust/fuel, construction, dust, and combat. However, the report detailed a number of issues with the quality and limitations of the registry’s information, which led the committee to conclude that the results of the analyses could not be taken at face value and that the identified associations might be an artifact of the population’s selection and the limitations of the self-reported exposure and disease data.
The sections below summarize salient results from epidemiologic studies that address COPD, chronic bronchitis, emphysema, and other allied conditions in military and veteran populations who served in the Southwest Asia theater and Afghanistan. Summaries of some of those studies that are recapped elsewhere in the chapter or in previous reports are more abbreviated. In the course of their work, the committee identified relevant studies dating from before the publication of Volume 10 that had not been previously addressed in National Academies reports. These are placed in the Update of the Scientific Literature section, even though they are from earlier times. Studies are categorized by country, beginning with those addressing U.S. veterans; those resulting from the same research initiative are grouped together.
1990–1991 Gulf War Veterans
The 1995 NHS, a population-based study of U.S. Gulf War veterans, yielded information used by multiple investigators to examine chronic obstructive lung disease in military personnel deployed to the theater compared with nondeployed era veterans. The population prevalence rates were calculated using statistical analysis techniques to account for a stratified random sampling of unequal probabilities of selecting various strata. Regarding bronchitis specifically, Kang et al. (2000) found that compared with nondeployed era veterans, Gulf War–deployed veterans had a statistically significantly higher self-reported prevalence of bronchitis (not differentiated between acute or chronic) experienced in the 12 months before the survey: 11.2% for deployed versus 7.7% for the nondeployed (RD = 3.57, 95%CI 3.48–3.66); however, estimates were not adjusted for smoking or other factors.
Eisen et al. (2005) performed a cross-sectional study on health outcomes collected from a subset of 1,061 deployed and 1,128 nondeployed Gulf War veterans who responded to the NHS and who completed the clinical examination component of the third phase of the NHS. No increase in the prevalence of self-reported asthma,
bronchitis, or emphysema (presented as a group) was observed among the deployed veterans compared with nondeployed veterans in models that adjusted for age, sex, race, years of education, cigarette smoking, component (active versus reserves or National Guard), service branch, and rank (OR = 1.07, 95%CI 0.65–1.77). Obstructive lung disease was defined by the investigators as “a history of lung disease (asthma, bronchitis, or emphysema) or pulmonary symptoms (wheezing, dyspnea on exertion, or persistent coughing with phlegm) and either the use of bronchodilators or at least 15% improvement in FEV1 after a short-acting bronchodilator” (Eisen et al., 2005, p. 884). Given this definition, no increase in obstructive lung disease was observed among deployed personnel (OR = 0.91, 95%CI 0.52–1.59) adjusted as above. However, information presented in a companion paper by Karlinsky et al. (2004)—summarized next—indicates that “bronchitis” was not differentiated as acute or chronic during data collection, weakening the relevance of the paper to an evaluation of COPD.
Karlinsky et al. (2004) examined data on the same deployed 1990–1991 Gulf War veterans and nondeployed Gulf War–era veterans population as Eisen et al. (2005). A total of 1,036 deployed and 1,103 nondeployed veterans met their selection criteria. In this analysis, the odds for current prevalence of self-reported bronchitis (not specified as acute or chronic) (OR = 1.08, 95%CI 0.50–2.34) and emphysema (OR = 4.45, 95%CI 0.74–26.68) were not different between the cohorts. Estimates were not adjusted (including for smoking history, although smoking data were collected). Demographic variables were similar in the deployed and nondeployed groups, and a history of tobacco smoking was more common in deployed veterans than in nondeployed veterans (51% vs 44%). Other limitations of the study include inadequacies in the description of the sampling strategy used and offering no explanation of how the groups were matched for analysis purposes.
Kang et al. (2009) used data from the 10-year follow-up of the NHS baseline survey to obtain self-reports of physician-diagnosed chronic medical conditions in the same population. A statistically significant excess of self-reported, physician-diagnosed chronic bronchitis or emphysema was found among 6,111 deployed Gulf War veterans compared with 3,859 nondeployed era veterans (RR = 1.47, 95%CI 1.30–1.65), adjusted for age, gender, race, rank, service branch, unit component, BMI, and current cigarette smoking.
Dursa et al. (2016b) conducted a 2012–2013 cross-sectional follow-up survey that collected data from 8,104 deployed and 6,148 era veterans who had participated in the 1993–1995 NHS (Kang et al., 2000). Both the NHS and follow-up assessments of it are described in greater detail in Chapter 3. A statistically significant difference between the deployed and nondeployed veterans in self-reports of physician-diagnosed COPD was found (8.4% vs 6.3%; OR = 1.48, 95%CI 1.23–1.78). The OR was adjusted for age, race, sex, BMI, smoking status, service branch, and unit component. The Volume 10 (NASEM, 2016) committee that previously reviewed this paper noted that this result must be viewed with caution because the diagnosis of COPD was taken from a retrospective assessment of VA records in which the proportion attributed to “bronchitis, not otherwise specified” (ICD-9 490) was included as part of those counted as having new-onset COPD.
Two additional relevant studies of veterans of Southwest Asia theater conflicts were previously addressed in earlier National Academies Gulf War and Health reports.
Lange et al. (2002) used a cross-sectional study design to examine exposure to smoke from oil-well fires (self-reported and modeled) and self-reported bronchitis symptoms assessed via structured interviews conducted 5 years after the 1990–1991 Gulf War for a population-based sample of 1,560 Iowa veterans. Modeled exposures were developed using a geographic information system to integrate spatial and temporal records of smoke concentrations, with troop movements ascertained from Global Positioning Systems records during the period of oil-well fires (February–October 1991). Exposure was presented by quartiles. Cases of bronchitis were assessed on the basis of self-reported cough and phlegm production, but these questions pertained to symptoms in the preceding month only; the overall prevalence of bronchitis symptoms was 4.7% for the study population. Current smokers had more than twice the prevalence of bronchitis symptoms as never smokers (6.3% vs 3.0%, respectively). There was no association between the modeled measure of exposure to oil-fire smoke and symptoms of bronchitis for any of the quartiles or with increasing magnitude of exposure. In contrast to the modeled exposures, there was a statistically significant association observed between the self-reported measure of exposure to oil-fire smoke and symptoms of bronchitis, whereby the risk of bronchitis increased with increasing magnitude of exposure, and the relationship for most quartiles was statistically significant. All effect models were adjusted for sex, age, race, military rank, smoking history, military service, and level of preparedness for war (based on the responses to six
questions). The use of population-based sampling improves the generalizability of the results. Its major weakness was the failure to use a standard epidemiologic definition of bronchitis, making it impossible to distinguish between acute and chronic symptoms.
Smith et al. (2002) used DoD hospitalization data (ICD-9-CM codes) from August 1991 through July 1999 and exposure models to retrospectively examine associations between respiratory diseases, including chronic bronchitis and emphysema, among 405,142 active-duty service members who served in the 1990–1991 Gulf War at the time of the oil-well fires. Service members were categorized as exposed (n = 337,077) and nonexposed (n = 68,065) to oil-well fires. There was no difference in modeled exposure to oil-well fires and the risk of hospitalization for chronic bronchitis adjusted for age, length of service, salary and pay grade, oil-well smoke exposure status, and number of days in the Gulf theater between exposed (n = 45) and nonexposed (n = 11) veterans (RR = 0.78, 95%CI 0.38–1.57). Similarly, there was no statistically significant difference between exposed (n = 48) and nonexposed (n = 8) veterans for emphysema (RR = 1.36, 95%CI 0.62–2.98), adjusted for unspecified demographic and military characteristics. Because most adults who have chronic bronchitis are never hospitalized for the condition, this analysis would not be expected to have captured most cases, only those that are most severe, which is evident from the relatively small number of cases identified over the 8-year period. No information was available on cigarette smoking or other exposures that may be related these outcomes.
Other 1990–1991 Gulf War Coalition Forces Veterans
Two studies of cohorts of veterans of the Australian Defence Force include information on COPD and related diseases.
Using data collected from 1,424 deployed veterans and 1,548 nondeployed comparison veterans who participated in the 2000–2002 Australian Gulf War Veterans’ Health Study, Kelsall et al. (2004) conducted an analysis of respiratory health outcomes, including chronic bronchitis. The results of other respiratory outcomes have been reported in the applicable outcomes sections of this chapter. As part of the medical assessment and physical examination, spirometric tests were performed, and a respiratory questionnaire was administered. Three definitions were applied for chronic bronchitis, and modeled effect estimates controlled for age, height, weight, smoking, atopy, rank, service, education, and marital status. Self-reported, doctor-diagnosed chronic bronchitis prevalence was not different between deployed and comparison veterans (OR = 1.1, 95%CI 0.9–1.5). The second definition for chronic obstructive bronchitis—“cough for as long as 3 months in each of the past 2 years and FEV1/FVC <70%” (Kelsall et al., 2004, p. 898)—again found no difference between deployed and comparison veterans (OR = 1.0, 95%CI 0.4–2.3). For the third definition used—“doctor-diagnosed bronchitis first diagnosed in 1991 or later and rated as a possible or probable diagnosis” (Kelsall et al., 2004, p. 899)—deployed veterans were found to have higher adjusted OR (OR = 1.9, 95%CI 1.2–3.1). A so-called working definition of emphysema was used that yielded no difference between deployed and comparison veterans (OR = 1.0, 95%CI 0.8–1.4). The authors identified the strengths of their study as including its objective measures of health and the use of a randomly sampled military comparison group, and its potential weaknesses as including recall bias and unidentified confounding factors, such as work exposures.
Using data collected from the Australian Gulf War Veterans’ Follow Up Health Study conducted in 2011–2013, which was collected 10 years after the 2000–2002 baseline investigation and 20 years after the 1990–1991 Gulf War, Sim et al. (2015) examined data on 697 deployed veterans and 659 nondeployed veterans. Deployed veterans were no more likely to report a doctor-confirmed diagnosis of chronic bronchitis (RR = 1.03, 95%CI 0.74–1.43) but more likely to report emphysema or COPD (RR = 2.14, 95%CI 0.60–7.66), although neither result was statistically significant. Estimates were adjusted for age group, service branch, and rank estimated as of August 1990 as well as for any atopy at baseline and current smoking status (never, former, current smoker). When a standardized symptom-based definition of chronic bronchitis was applied, a statistically significant difference was observed (RR = 1.51, 95%CI 1.17–1.96), adjusted for the same demographic, military, and lifestyle characteristics. The researchers note that the number of self-reported, doctor-confirmed chronic bronchitis cases was significantly elevated at baseline (number not reported), which affected their calculation at follow-up, as did the small number of cases of emphysema or COPD (eight in deployed personnel; four in the comparison group).
Post-9/11 Veterans
The AFHSC (2010) examined medical encounters of U.S. Army and Air Force personnel 36 months after deployment to Joint Base Balad, Contingency Operating Base Speicher, or Camp Taji in Iraq (all
three of which used burn pits for waste management); Camp Buehring or Camp Arifjan in Kuwait (which did not use burn pits); or to installations in the Republic of Korea, from 2005 to 2007. Service members who were never deployed and stationed only in the continental United States in the same period were used as a comparison population. IRRs of COPD were calculated using Poisson models that were adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, physical activity, service branch, military rank, pay grade, and occupation. COPD was statistically significantly lower for troops deployed to Joint Base Balad (IRR = 0.91, 95%CI 0.84–0.99), Camp Buehring (IRR = 0.62, 95%CI 0.44–0.88), and Korea (IRR = 0.83, 95%CI 0.78–0.88) than for the nondeployed U.S. cohort. No differences in COPD incidence were found for those deployed to Camps Arifjan or Taji compared with the nondeployed U.S. cohort. The investigators also conducted additional analyses using data from the baseline and first follow-up cycles of the Millennium Cohort Study. Multivariable logistic regression was used to compare the adjusted odds—using the same factors as used in the Poisson models, including smoking and physical activity—of COPD associated with three metrics of exposure within a 5-mile radius of the documented burn pits: dichotomous deployment near the documented burn pits, cumulative days exposed to the burn pits (presented by quartiles), and exposure to the burn pits at three different campsites (Balad, Taji, or Speicher). The incidence of newly reported chronic bronchitis or emphysema was 1.54% for participants with putative exposure to burn pits and 1.46% for the nonexposed group. Deployment within 5 miles of a documented burn pit was not associated with increased odds for newly reported chronic bronchitis or emphysema (OR = 0.87, 95%CI 0.64–1.18; p = 0.36). In addition, no association of chronic bronchitis or emphysema was found for cumulative days in proximity to a burn pit for any of the quartiles of exposure compared with the nonexposed group. An analysis that examined the outcomes at Joint Base Balad, Contingency Operating Base Speicher, and Camp Taji separately found that the odds of chronic bronchitis or emphysema were not increased in association with deployment within 5 miles of the sites compared with those deployed outside of the 5-mile radius (p = 0.33).
Update of the Scientific Literature on COPD, Emphysema, and Chronic Bronchitis
Epidemiologic studies of COPD, chronic bronchitis, or emphysema in Southwest Asia theater veterans that have not previously been addressed in National Academies reports are summarized below, grouped by the source of the data and addressed in order of their publication. Studies of post-9/11 U.S. veterans are presented first, followed by studies of post-9/11 coalition forces, and the sections end with summaries of U.S. 1990–1991 Gulf War veterans. Some additional studies that were identified were not included in this section because they were descriptive studies, did not include a comparison group, or grouped COPD, emphysema, and chronic bronchitis with several other outcomes that made these outcomes indistinguishable. Such studies included publications from the STAMPEDE initiative (Morris et al., 2014, 2020) and one in veterans who had been referred to VA’s WRIISC specialty clinic (Butzko et al., 2019).
Post-9/11 Veterans
The Millennium Cohort Study—an ongoing prospective epidemiologic research effort intended to evaluate the impact of military exposures, including deployment, on long-term health outcomes—has published three papers to date (early 2020) that address the respiratory health outcomes addressed in this section.
Smith et al. (2008) used self-reported, clinician-diagnosed health data from regular, active-duty participants from the first panel (2001–2003) of the Millennium Cohort Study (n = 37,798) to compare the agreement of 38 medical conditions, which included chronic bronchitis and emphysema, with that obtained from electronic medical records based on ICD-9-CM codes. Any diagnostic code for these 38 conditions in any portion of the medical record indicated agreement with a self-reported medical condition of interest. Both positive and negative agreement were used to compare self-reported data with those from electronic medical records. The prevalence of chronic bronchitis was 3.3% (95%CI 3.1–3.4) for self-reported and 4.0% (95%CI 3.8–4.2) for electronic medical record–documented cases; 3.5% were exclusively recorded in the electronic medical records. The positive agreement between self-report and electronic medical records for chronic bronchitis was 12.9%, and negative agreement was 96.7%. The prevalence of emphysema was 0.6% (95%CI 0.5–0.7) for self-reported and 0.2% (95%CI 0.1–0.2) for electronic medical record–documented cases; 0.2% were exclusively recorded in the electronic medical record. The positive agreement between self-report and electronic medical records for emphysema was 2.7% and negative agreement
(the condition was not reported either by self-report or found in the medical record) was 99.6%. When reports of chronic bronchitis were examined by length of service (0–5, 6–10, 11–15, and ≥16 years), for all periods the self-reported prevalence of chronic bronchitis was lower than what was recorded in the electronic medical records.
Smith et al. (2009) examined newly reported chronic bronchitis and emphysema and other respiratory conditions among 46,077 Millennium Cohort Study participants who completed baseline (2001–2003) and follow-up (2004–2006) questionnaires. Logistic regression was used to compare the adjusted odds of new chronic bronchitis or emphysema (grouped) in relation to deployment status (deployed versus nondeployed) stratified by service branch and adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, service component, military pay grade, and occupational code. The adjusted OR for newly reported chronic bronchitis or emphysema in deployed versus nondeployed personnel varied according to service branch, though it was not statistically significant for any of the branches, with the highest OR observed in Army personnel (OR = 1.25, 95%CI 0.94–1.67) and the lowest in Navy and Coast Guard personnel (OR = 0.79, 95%CI 0.42–1.46). When the analysis was restricted to deployed cohort members with self-reported information on deployment location (n = 9,861), the investigators stated that the odds of chronic bronchitis or emphysema were not statistically different in any of the deployment locations examined, although estimates were not provided.
Smith et al. (2012) investigated the effects of exposure to documented open-air burn pits within 2, 3, or 5 miles on chronic bronchitis or emphysema and other respiratory outcomes among Millennium Cohort Study Army and Air Force participants who were deployed to Iraq or Afghanistan after January 1, 2003, and who completed the baseline questionnaire and one of the follow-up assessment cycles through 2008. After excluding individuals with missing data, 3,585 individuals who deployed within 3 miles of a burn pit were compared with 18,712 individuals who deployed to Iraq or Afghanistan but outside that zone for the analyses of new-onset chronic bronchitis or emphysema. Similar proportions of newly reported chronic bronchitis or emphysema in 2007 were found for those exposed within 3 miles of a burn pit and those nonexposed (1.5% vs 1.6%, respectively). At the end of follow-up, and after adjusting for demographic, behavioral, and military characteristics, the odds of newly reported chronic bronchitis or emphysema were statistically significantly increased for women (OR = 1.77, 95%CI 1.36–2.30), consistent smokers (OR = 1.61, 95%CI 1.24–2.10), and Army personnel (OR = 1.82, 95%CI 1.38–2.41), whereas younger individuals and those who did and did not meet the standards for aerobic activity were at reduced risk for chronic bronchitis or emphysema compared with those who could not perform aerobic activity. Three proxy exposure metrics were modeled, and the analyses were adjusted for demographic and military characteristics, smoking status, and physical activity. Neither newly reported chronic bronchitis nor emphysema was statistically significantly associated with deployment within 3 miles of burn pits (OR = 0.91, 95%CI 0.67–1.24) when compared with deployments to areas with no documented burn pit exposure and adjusted for demographic, behavioral, and military covariates. Similarly, no statistically significant associations for new-onset chronic bronchitis or emphysema were found when those deployed at each of the three sites with documented burn pits (Joint Base Balad, Camp Taji, or Camp Speicher) were compared with those deployed outside of the 3-mile radius exposure window. An increasing number of cumulative days of exposure within a 3-mile radius of the burn pits was not associated with the adjusted odds of new-onset chronic bronchitis or emphysema compared with cohort members with no burn pit exposure (p = 0.76). Findings of no association with new-onset chronic bronchitis or emphysema for deployment status, cumulative deployment length, and camp location were consistent when examining the risk within 5 miles of the burn pits.
Using data collected as part of the NewGen Study, Barth et al. (2014) examined the association between deployment to Southwest Asia and self-reported doctor-diagnosed bronchitis (did not distinguish between acute and chronic) among 13,162 deployed and 7,401 nondeployed veterans. Unweighted and weighted prevalence of bronchitis were calculated and stratified by diagnosis before or after 2001, and logistic regression was used to calculate adjusted ORs for deployment status and bronchitis. The models were adjusted for birth year, sex, service branch, unit component, race/ethnicity, education, and smoking status. Separate models were constructed for diagnosis before 2001 and during or after 2001. For those diagnosed before 2001, the weighted prevalence for bronchitis was higher in the nondeployed than in the deployed (4.5% vs 6.6%), and deployment was associated with statistically significant decreased odds of bronchitis (OR = 0.73, 95%CI 0.63–0.84). Among those with respiratory disease diagnosed in 2001 or later, the weighted prevalence of bronchitis was slightly higher in the
deployed than in the nondeployed veterans (5.9% vs 5.3%), and there was no difference in the odds of bronchitis between the deployed and nondeployed groups (OR = 1.12, 95%CI 0.96–1.30).
Barth et al. (2016a) again used data from the NewGen study to expand on the analysis by Barth et al. (2014) to examine the prevalence of self-reported doctor-diagnosed respiratory diseases and their association with self-reported respiratory exposures during military service for OEF/OIF deployed and nondeployed veterans. Logistic regression analyses were used to calculate weighted, adjusted odds of bronchitis (not specified as chronic or acute) stratified by deployment status and controlled for sex, birth year, race/ethnicity, education, smoking status, unit component, service branch, and number of OEF/OIF deployments. A total of 2,588 veterans self-reported bronchitis (1,615 deployed and 970 nondeployed). Among deployed veterans, the highest odds for bronchitis were for those categorized as high exposure (OR = 2.49, 95%CI 1.70–3.63) and for diesel, kerosene, or other petrochemical fumes as a specific exposure (OR = 1.79, 95%CI 1.48–2.16). For nondeployed veterans, statistically significant increased odds of bronchitis were observed for all specific exposures and for both the high-exposure and low-exposure categories; the highest odds for bronchitis for specific exposures were for smoke for oil fires (OR = 1.67, 95%CI 1.33–2.09) and industrial pollution (OR = 1.67, 95%CI 1.38–2.03). These results show that exposures were associated with the development of bronchitis in both deployed and nondeployed groups, but the confidence intervals for the adjusted ORs all overlap between the deployed and nondeployed groups.
Abraham et al. (2014) built on the AFHSC (2010) analysis by adding an additional 12 months of follow-up (for a total of 48 months) of personnel deployed to four Southwest Asia theater sites with and without burn pits, along with those deployed to Korea and a comparison population of service members who stayed in the United States. The IRR of medical encounters for “COPD and allied conditions” was the same for those deployed to in-theater locations as for nondeployed personnel after adjustment for age, gender, race, and military rank (IRR = 1.12, 95%CI 0.96–1.31). Other models—which examined rates for personnel at in-theater bases with and without burn pits, and for personnel at the individual bases—all yielded no difference in adjusted IRRs compared with the U.S. group of service members. Information on smoking was not factored into the analyses. When service members deployed to in-theater locations were compared with those deployed to Korea, however, a statistically-significant increase for COPD and allied conditions was observed (IRR = 1.24; 95%CI 1.03–1.48). Additional analyses that adjusted for the same demographic and military factors found that the difference was statistically significant for personnel at the two bases without burn pits (IRR = 1.37; 95%CI 1.04–1.82) but not for personnel at the two with burn pits (IRR = 1.16; 95%CI 0.95–1.43). While the study found that deployment to the Southwest Asia theater, but not necessarily potential exposure to burn pits, was associated with an elevated post-deployment rate of COPD and allied conditions, smoking was not factored into these analyses, and that smoking behavior during deployment is a likely plausible causal intermediate between deployment and the incidence of respiratory conditions needs to be considered.
The analyses by Sharkey et al. (2015) also used the same deployed and nondeployed populations as the AFHSC (2010) analysis but used a larger U.S.-based reference population and included an additional 12 months of data. Its methods also differ from Abraham et al. (2014); all three studies are discussed in greater detail in Chapter 3. This retrospective cohort study used Poisson models that were adjusted for age, pay grade, sex, race, and service branch to calculate IRRs for COPD (ICD-9-CM 490–492, 494–496) at two time periods: up to 36 months after the baseline data were gathered and up to 48 months afterwards. Outcome ascertainment was limited to encounters that occurred at a military hospital or care center. At 36 months of follow-up, the risks of COPD at the four Southwest Asia bases and Korea sites examined were all similar to, or statistically significantly lower than (Balad, Buehring, and Korea), the risks for personnel who remained in the United States. Similar results were found at the 48-month follow-up, with Balad, Buehring, and Korea again showing statistically significantly lower adjusted incidence rates of COPD compared with the U.S. cohort. No observed association between COPD and serving at locations with burn pits was found.
Sharkey et al. (2016) extended the analysis of the AFHSC (2010) report by adding additional populations of Army or Air Force personnel who were deployed to Kabul (n = 5,670) and Bagram (n = 34,239) Air Force Bases in Afghanistan—sites with similar, poor air quality—and Manas Air Force Base in Kyrgyzstan (n = 15,851)—a site with relatively better air quality—and extended the follow-up period of active-duty personnel to 12 years. COPD cases were identified when an individual had either an inpatient or at least two outpatient health care encounters
labeled with ICD-9-CM 490–492 or 494–496 in any diagnosis coding position. IRRs were calculated and adjusted for age, sex, race, and military rank. No statistically significant differences for COPD were found between the Kabul cohort and the other location cohorts.
Liu et al. (2016) examined the associations between assumed geographic and self-reported burn pit emissions exposure and respiratory and cardiovascular outcomes in participants in VA’s Airborne Hazards and Open Burn Pit Registry (first described in the Asthma section). The study included 4,343 participants who completed the registry questionnaire by April 30, 2015; of these, 2,663 participants deployed for at least 30 days from January 1, 2003, to June 30, 2007, within 2 miles of burn pits in Joint Base Balad or Camp Taji in Iraq, and 1,680 participants were deployed for at least 30 days to Kuwait (but not to Joint Base Balad or Camp Taji) during that timeframe. There were no documented burn pits at Kuwait bases. Two surrogate measurements of burn pit emissions exposure were used in the analysis: days of deployment near burn pits and self-reported total hours of burn pit smoke exposure. Associations were presented by quartiles of burn pit exposure. Self-reported diagnoses were compared with VA medical record information for 2,857 respondents who used VA health care at least once between January 2007 and November 2015. Participants who reported having been diagnosed with a condition before deployment were excluded from both the analyses of self-report and the comparisons with VA medical records for that condition. All demographic characteristics (except marital status), military characteristics, and other factors, such as in-person clinical examination request and smoking status, were found to be statistically significantly associated with deployment days within 2 miles of the burn pits sites. Associations between demographic, lifestyle (with exception of smoking), and military service variables and self-reported burn pit smoke exposure amount were found to be statistically significantly associated with self-reported burn pit smoke exposure. Models were adjusted for demographic, lifestyle (including smoking status), and military service characteristics. A strong exposure–response association was found between cumulative days deployed within a 2-mile radius of a burn pit and self-reported emphysema, chronic bronchitis, or COPD (p-trend = 0.01; n = 537). The same association was not observed, however, when VA medical record diagnoses (ICD-9 491, 492, and 493.2) were used in place of the self-report (p-trend = 0.88; n = 104). When the number of self-reported hours per day of burn pit smoke exposure was used as the measure in place of days deployed near a burn pit, the exposure–response association with self-reported emphysema, chronic bronchitis, or COPD was strongly statistically significant (p-trend = 0.0005; n = 527), but the association did not persist when VA medical records diagnoses were instead used to characterize the diseases (p-trend = 0.40; n = 100). The limited correlation between self-reported diagnoses and the diagnoses recorded in VA medical records may suggest a misidentification of self-reported health conditions, which in turn implies that analyses performed using self-reported diagnoses may likewise be affected. This study is most limited by the use of self-reported exposures and the fact that the study population consists of a self-selected group of individuals.
Abraham and Baird (2012) conducted a case-crossover study of short-term (i.e., 0- and 1-day lagged), exposures to ambient PM2.5 and PM10 and cardiovascular and respiratory medical encounters (ICD-9 460–519) among 2,838 U.S. military personnel deployed to Southwest Asia. PM exposure was assessed using data collected over a period of approximately 1 year at 15 military bases. Site-specific estimates were first obtained and then pooled using meta-analytic techniques to generate OR for a 10 µg/m3 increase in PM2.5 or PM10. Ambient levels were routinely high at the bases assessed, but no statistically significant associations between PM and respiratory outcomes were observed in the young, relatively healthy deployed military population. Of the 343 encounters for COPD and allied conditions, though, 327 (95%) were reported to be for asthma (ICD-9 493), indicating that 16 could be attributed to all of the other ICD-9 codes, including COPD, emphysema, and chronic bronchitis. Specific estimates for the association of PM exposure and COPD and related conditions were not calculated.
Baird et al. (2012) examined the post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant near Mosul, Iraq, in 2003. Two were groups potentially exposed to the sulfur fire smoke plume—personnel involved in fighting the fire (n = 191) and personnel presumably downwind during the time of the fire (n = 6,341). These were compared with two unexposed groups: those who deployed to the area after the fire was extinguished (n = 2,284) and those deployed to other Southwest Asia locations contemporaneously with the time of the fire (n = 1,869). Age-adjusted standardized morbidity ratios, for COPD encounters (ICD-9-CM 490–496, inclusive) were statistically significantly lower for the potentially exposed personnel downwind of the fire compared with the group deployed to the area after the fire was extin-
guished (standardized morbidity ratio = 0.62, 95%CI 0.53–0.71). The age-adjusted standardized morbidity ratio for COPD and allied conditions was not statistically significantly different from 1.0 when firefighters were compared with the contemporaneously deployed group (morbidity ratio = 0.73, 95%CI 0.27–1.43), but it was statistically significantly decreased when firefighters were compared with the group deployed to the area before or after the fire (morbidity ratio = 0.41, 95%CI 0.15–0.79). The authors acknowledge that the inverse association for COPD that was observed may reflect the short follow-up time and the young age of the population being studied and note that significant confounders, including smoking and other environmental or occupational exposures were not controlled for in the analysis.
As previously described in the Pulmonary Function Testing section, Matthews et al. (2014) conducted a retrospective review of DoD electronic medical records to identify trends in the frequency and severity of COPD according to PFTs in service members based on their deployment history. Inpatient and outpatient records were queried to identify active-duty personnel from all service branches with the ICD-9 code for either “emphysema” (492.8) or “chronic airway obstruction, not elsewhere classified” (496) for 5 consecutive years from 2005 to 2009. Individuals with a diagnosis of asthma (493) or chronic bronchitis (490) were excluded. The medical records review was limited to those individuals with a minimum of three outpatient encounters with the listed diagnosis of COPD/emphysema during the study period. Deployment information was obtained from the AFHSC, and individuals were classified into deployers and nondeployers based on whether they had deployed to Southwest Asia during or since 2003. Clinical symptoms, smoking history, PFT, and radiographs obtained during the diagnostic workup were reviewed. A total of 371 patients with diagnosed COPD or emphysema were identified; 194 (52.3%) had deployed and 177 (47.7%) had not deployed to Southwest Asia since 2003. Of the deployed, 68% had a documented history of smoking, compared with 62% of the nondeployed. Specific comparisons were made for age, FEV1 (% predicted), FEV1 post-bronchodilator (% predicted) and percent change, FVC (% predicted), FEV1/FVC, TLC, RV, and DLCO, and they are presented in the summary of this study in the Pulmonary Function Testing section. Among the individuals with a documented smoking history and spirometry data, 65% of those deployed and 46% of those nondeployed met established diagnostic criteria for COPD. The disease severity, as measured by the GOLD criteria, was similar for deployed and nondeployed individuals: 30% versus 33% for those with mild disease, 57% versus 60% for those with moderate disease, and 14% versus 7% for those diagnosed with severe disease. Although the investigators concluded that the impact of deployment on increased diagnosis of COPD or severity of disease appeared minimal, this study lacked a prospective design and adequate adjustment for confounders of the relationship between deployment and pulmonary function. In this relatively young population (average age 40), only about half had an adequate workup to assess the diagnosis of COPD.
Pugh et al. (2016) conducted a retrospective cohort study to examine the prevalence of chronic lung diseases, including COPD, based on ICD-9-CM codes and military deployment using VA health care data from 760,621 U.S. veterans deployed to combat operations in Iraq or Afghanistan who received care from VA between October 1, 2002, and September 30, 2011. The prevalence of COPD was calculated for each year between 2003 and 2011 using the number of unique OEF/OIF veterans who received care from VA during the year as the denominator for that year. and the data were examined for any changes in prevalence during that time. Generalized estimating equations analysis was used to determine if the log-odds of having a diagnosis of COPD increased from 2003 to 2011. Estimates were adjusted for demographic characteristics, multiple deployments, tobacco use, and TBI to determine if log-odds of diagnosis increased from 2003 to 2011. Over the study period, 5,998 (0.8%) individuals had a diagnosis of COPD.10 They were more likely to be male, white, and have served in the Army; their average age was 42 years; 56.9% were classified as tobacco users; and 16.2% had a TBI diagnosis. In comparison, the average age of those without lung disease was 34 years, and 21% were tobacco users. A consistent and statistically significant pattern of increasing prevalence of COPD was found in the cohort, with an average increase in the log-odds per year of 0.06 (95%CI 0.05–0.08) after controlling for demographic, military, and personal characteristics, including smoking. Based on the generalized estimating equations analysis and controlling for demographic and clinical characteristics, the odds of diagnosis of COPD
___________________
10 Defined as chronic bronchitis (ICD-9-CM 491), emphysema (492), bronchiectasis (494), and chronic airway obstruction, not elsewhere classified (496).
were statistically significantly higher in 2011 than in the other, earlier years of the study. Moreover, the odds of COPD were statistically significantly increased for all age groups over 30 years as well as for those with a TBI diagnosis (OR = 1.51, 95%CI 1.38–1.64) and tobacco users (OR = 4.45, 95%CI 4.18–4.73). Individuals who had multiple deployments were statistically significantly less likely to have a COPD diagnosis (OR = 0.92, 95%CI 0.86–0.98) than individuals with only one deployment. As would be expected from general population trends, the prevalence increased with age, and women were less likely than men to have a COPD diagnosis. The nature of exposures during deployment could not be assessed; however, reports of blast injury as reflected by TBI were also associated with increasing rates of COPD. Confirmation of the diagnosis of COPD with pulmonary function measurement was not available, and the authors pointed out that, because the use of VA resources is voluntary11 and because the veterans studied may have been too young for many to have developed symptoms of chronic pulmonary diseases, these results may be subject to both selection and ascertainment biases. Although it appears that what was reported as change in prevalence by year is really incidence of new diagnoses; however, new cases may be a mixture of incident and prevalent cases, with some patients coming to VA to receive care when disease becomes severe enough to need treatment, and therefore these are prevalent cases that are considered incident in that they were not previously counted.
Krefft et al. (2017) conducted a small pilot study to examine the role of lung clearance index as an early marker of lung injury in a sample of 24 healthy volunteers and 28 symptomatic veterans who had deployed to Southwest Asia in support of post-9/11 operations. The 28 veterans had been referred to an occupational lung disease clinic for evaluation of unexplained respiratory symptoms (cough, chest tightness, wheezing, shortness of breath, or decreased exercise tolerance) with onset during or following deployment. The control group consisted of individuals who were at least 18 years of age, had no history of pre-existing lung disease, and reported no respiratory illness in the 4 weeks preceding enrollment and testing. Participants underwent lung clearance index testing to identify whether abnormalities were present in the peripheral airways of the lung. As part of their clinical evaluation, members of the deployed group completed tests of pre- and post-bronchodilator spirometry, lung volumes, and diffusing capacity and also had cardiopulmonary exercise tolerance testing and chest CT scans. Surgical lung biopsies were performed on 17 of the 28 deployers. Of the 28 with respiratory symptoms, 17 were found to have definite and 11 were found to have probable deployment-related lung disease, which was defined as the presence of one or more of these findings: emphysema/hyperinflation, bronchiolitis, and granulomatous pneumonitis in a deployer with respiratory symptoms. Given that the controls did not undergo PFT, that the small sample of veterans is highly selective as they were all symptomatic and were seen at an occupational lung disease clinic, and that specific diagnoses of the deployed were grouped as deployment-related lung disease, as well as the other limitations described in Chapter 3, this study has limited utility in examining the impact of deployment to the Southwest Asia theater on occurrence of respiratory disease.
Krefft et al. (2020) aimed to describe deployment-related respiratory disease and the diagnostic utility of resting and exercise PFT with a retrospective study of 127 military personnel, veterans, and civilian contractors who supported military operations in Southwest Asia, with new-onset respiratory symptoms presenting between 2009 and 2017 and referred to a single occupational lung disease clinic. Of the 127 patients, 113 underwent PFTs, the results of which are described in the summary of this study under the Pulmonary Function Testing section of this chapter. Lung biopsies were performed in 52 patients (51 video-assisted thoracoscopic surgeries, 1 transbronchial cryobiopsy) and reviewed for several diagnoses. The most common abnormality on the 52 lung biopsies was hyperinflation/emphysema, seen in 69% of the biopsies. All the biopsies had at least one of the three case definition findings of distal lung disease (hyperinflation/emphysema, bronchiolitis, and granulomatous pneumonitis). Deployment distal lung disease was diagnosed in 87 of the 127 patients. Comparisons were made between those with and without histologic findings of distal lung disease (controlling for age), however, these findings are not specific to COPD or emphysema. Thus, this study is limited for the committee’s purposes because it includes only cases that are grouped as distal lung disease and does not include a nondeployed or elsewhere-deployed control group.
Abraham et al. (2012) conducted a cohort and nested case–control study to evaluate the relationship between deployment and respiratory system diseases (ICD-9 460–519) in U.S. military personnel. Cases (n = 532) of post-
___________________
11 Veterans who use VA services are more likely to report that they have multiple medical conditions than those who do not (Meffert et al., 2019).
deployment diagnosis of obstructive pulmonary disease, defined as ICD-9-CM 490–496, and controls (n = 2,128) were selected from those who were free of respiratory diagnoses within 6 months before their deployment. Controls were matched on the year of case definition and the year of the last encounter during the study period as well as on the total number of post-deployment medical encounters. Conditional logistic regression analyses were used to examine the independent effects of the number of deployments at diagnosis and the cumulative time in theater up to diagnosis on post-deployment obstructive pulmonary disease encounter, controlling for potential confounders (gender, age, grade, occupation, time in theater, number of deployments, service branch, and tobacco-related diagnoses). The study does not provide any specific information on COPD, chronic bronchitis, or emphysema. The majority of obstructive pulmonary disease encounters were for either asthma (46%) or bronchitis (50%). No statistically significant difference in odds of an obstructive pulmonary disease encounter was found for multiple deployers relative to single deployers (OR = 1.08, 95%CI 0.82–1.42). This study had several limitations, such as a lack of measurement of smoking and a lack of specific deployment-related exposure assessments. Additionally, given that asthma and other obstructive lung diseases were all considered together, the findings do not provide specific information on the impact of service in Southwest Asia and COPD.
Other Coalition Force Veterans
Davy et al. (2012) performed a review of the respiratory health of Australian Defence Force personnel deployed to the Southwest Asia theater as part of the Middle East Area of Operations Prospective Health Study. The study population was defined as Australian Defence Force personnel who deployed after June 2010 and returned from that deployment by June 2012. Information on smoking behavior, self-reported exposures, length of time in theater, and other potential influences were collected but were not presented. Of the total eligible population of 3,074, 156 completed pre- and post-deployment questionnaires and a physical examination that yielded spirometry test results of sufficient quality to be usable for research purposes. The investigators found that four participants met the GOLD criteria at pre-deployment only, five at post-deployment only, and four at both pre- and post-deployment. They commented that, aside from these findings, “the respiratory health of this sample was well within the normal range” (Davy et al., 2012, p. 247). Information on smoking behavior, self-reported exposures, length of time in theater, and other potential influences was collected but was not presented relative to the COPD observations. Furthermore, because of the small sampling fraction of the eligible population that was studied, the results are not generalizable.
Saers et al. (2017) examined the prevalence of self-reported chronic bronchitis in a random sample of 1,032 Swedish military personnel who were either currently or previously stationed in Kosovo (in the period 2005–2008) or Afghanistan (2008–2009) compared with that of a 1:1 matched Swedish general population sample that included matching on age, gender, smoking habits, BMI, and education level. Additional methodologic details of this study are provided in the summary of this study that appears in the Respiratory Symptoms section. Chronic bronchitis was identified by affirmative response to the question “Are you used to having a cough almost every day with sputum production that lasts for at least 3 months every year during the winter?” The prevalence of chronic bronchitis over the preceding 12 months was statistically significantly greater in the military personnel than in the matched population (12.3% vs 8.2%; p = 0.003). The prevalence was no different in the 682 service personnel stationed in Afghanistan from those stationed in Kosovo. In those stationed in Afghanistan, there was a significantly higher prevalence of chronic bronchitis in those exposed to sandstorms than in those not exposed to sandstorms (13.6% vs 7.3%; p = 0.04). Although the design of this study was limited and therefore the inferences that can be made based on its results are also limited, the finding of no difference in symptom prevalence between those stationed in Kosovo and those stationed in Afghanistan calls into question the role of Southwest Asia deployment as a cause of the differences in prevalence relative to the general population.
1990–1991 Gulf War Veterans
Hines et al. (2013) conducted a small study using 24-hour creatinine-corrected urinary uranium as a validated marker of exposure in 1990–1991 Gulf War veterans who were enrolled in the VA Depleted Uranium Surveillance Program and had attended a biennial follow-up in 2011 to compare the likelihood of pulmonary health abnormalities in those with high body burdens of uranium (n = 12; >0.1 µg/g creatinine) versus those with low body burdens of uranium (n = 25; ≤0.1 µg/g creatinine). No statistically significant differences were observed for respiratory symptoms, abnormal pulmonary function values, or the prevalence of chest
CT abnormalities in those with high (n = 12) versus low (n = 12) urinary uranium. In the 22 participants in whom one or more parenchymal nodules were observed based on CT, 15 had emphysema (42%), but this was reported to be mild in 12 of them, and those with a history of smoking were significantly more likely to have emphysema (p = 0.001) than those with no history of smoking. While the findings from this study made use of a rigorous exposure assessment through analysis of uranium in urinary samples, the findings are not particularly pertinent to this assessment, given that exposure to depleted uranium was uncommon.
Khalil et al. (2018) described the study design for the Gulf War Era Cohort and Biorepository and provided preliminary results from the pilot phase of the effort, which had enrolled 1,275 veterans, 900 of whom had deployed to Southwest Asia. Self-reported health outcomes of symptoms (in the past year) and health care provider–diagnosed conditions were reported stratified by users (n = 584) and nonusers (n = 679) of VA health care in the past year. A supplemental table for the paper that was posted to the web reported that of the 1,275 subjects who responded to the survey question asking whether a doctor or other health care provider had told them that they had chronic lung disease (COPD, emphysema, or bronchitis), 82 (6.4%) answered yes (9.2% of VA users and 4.0% of nonusers). While the reported proportions of veterans with chronic lung disease seems higher than expected, there was no formal assessment of differences in the frequency of chronic lung disease between VA users and nonusers. Furthermore, there were no comparisons between deployed and nondeployed veterans and, therefore, these results do not inform questions about the role of Gulf War deployment on increased risk of chronic lung disease.
Zundel et al. (2019) compared survey results from a cohort of 1990–1991 Gulf War veterans (401 males and 47 females) who returned from deployment in 1991 through Fort Devens, Massachusetts, with data from the 2013–2014 NHANES (n = 2,949). The veterans were asked to self-report if a doctor had ever diagnosed them with any of nine chronic medical conditions, including chronic bronchitis. Analyses were restricted to veterans of white race with at least a high school education and stratified by sex. Analyses were weighted to account for demographic differences between cohorts. The prevalence of chronic bronchitis was higher among the Fort Devens cohort than NHANES for men (10.2% vs 2.59%, respectively), and the difference was statistically significant (OR = 4.50, 95%CI 2.02–10.03). Similarly, the prevalence of chronic bronchitis was higher among women of the Fort Devens cohort than NHANES (13.2% vs 10.6%, respectively), but in this case the difference was not statistically significant (OR = 1.28, 95%CI 0.43–3.82). When the prevalence of chronic bronchitis was compared for men stratified by age group (40s, 50s, and 60s), no difference between Fort Devens and NHANES was found for men in their 40s. However, chronic bronchitis was statistically significantly higher for Fort Devens men than for NHANES men in their 50s (OR = 3.94, 95%CI 1.24–12.51) and 60s (OR = 4.83, 95%CI 1.09–22.36), although the estimates were not precise. For the Fort Devens exposure analyses, veterans who were exposed and unexposed to chemical or biologic warfare or pyridostigmine bromide pills did not differ on any of the demographic variables. For those exposed to chemical or biologic warfare, the prevalence of chronic bronchitis was higher than for the unexposed (16.0% vs 5.7%, respectively), and the difference was statistically significant (OR = 4.00, 95%CI 1.43–11.20) adjusted for gender and current smoking status. Similarly, the prevalence of chronic bronchitis was higher for those exposed to pyridostigmine bromide pills than for the unexposed (13.1% vs 8.0%, respectively), but this difference was not statistically significant (OR = 1.66, 95%CI 0.68–4.09). Finally, prevalence of chronic bronchitis was compared between men and women of the Fort Devens cohort; no difference in prevalence was found after adjustment for age, race, education, and current smoking (OR = 0.46, 95%CI 0.18–1.18). This study has several limitations, including its generalizability, use of self-reported conditions, and low response rate.
Synthesis
Studies of COPD, chronic bronchitis, and emphysema in active-duty personnel and veterans who have served in the Southwest Asia theater have been reviewed in multiple previous volumes of the National Academies Gulf War and Health series (IOM, 2005, 2006, 2010; NASEM, 2016) and related reports (IOM, 2011; NASEM, 2017), but with one exception—Volume 3 (IOM, 2005)—non-cancerous respiratory diseases were grouped under a single conclusion of “insufficient or inadequate evidence to determine whether an association existed between deployment to the theater and respiratory disease.” This conclusion was based in part on analyses of data from the population--
based NHS, conducted in 1995, that found no difference in risks or odds of deployment to Southwest Asia in support of the 1990–1991 Gulf War and outcomes of COPD, chronic bronchitis, or emphysema when adjusted for smoking. However, follow-up surveys of veterans who participated in the NHS conducted 10 years later found increased risks of COPD, chronic bronchitis, or emphysema after adjustment for demographic and military factors as well as smoking behavior. Studies that categorized deployed service members by specific exposures encountered in theater, such as oil-well fires, that also accounted for length of deployment or levels of exposures (Lange et al., 2002; Smith et al., 2002) and also adjusted for demographic, military, and smoking found no association with chronic bronchitis or emphysema. Likewise, results from the population-based study of Australian Gulf War veterans, also adjusted for demographic and military characteristics and smoking, found no increased odds of emphysema or self-reported doctor-diagnosed chronic bronchitis compared with nondeployed veterans, except for bronchitis first diagnosed in 1991 or later. A follow-up study of the Australian veterans conducted 10 years after the baseline analysis again found that after adjustment for demographic and military factors and current smoking status, deployed veterans were not statistically significantly more likely to report a doctor-confirmed diagnosis of chronic bronchitis, emphysema, or COPD. When a standardized symptom-based definition of chronic bronchitis was applied, a statistically significant difference was observed adjusted for the same demographic, military, and lifestyle characteristics.
The committee identified and evaluated 21 studies that evaluated associations between deployment to Southwest Asia and COPD, chronic bronchitis, or emphysema; 18 among post-9/11 veterans and 3 studies among 1990–1991 Gulf War veterans. The studies differ in how exposure was evaluated (e.g., deployment versus specific in-theater exposures), and which outcomes were addressed (some studies grouped one or more of these outcomes, others presented estimates for each outcome separately, and some included only one of these outcomes). Findings from these more recent studies are largely in line with those reported previously in the Gulf War and Health series, with mostly null associations between deployment and COPD, chronic bronchitis, and emphysema.
Of the cohorts specified in the Statement of Task, three studies were identified and assessed that used data collected from the Millennium Cohort Study (Smith et al., 2008, 2009, 2012) and two studies used NewGen data (Barth et al., 2014, 2016a) to examine outcomes of chronic bronchitis and emphysema. The most informative of these studies was Smith et al. (2009), which examined newly reported chronic bronchitis and emphysema (grouped) among 46,077 Millennium Cohort Study participants, and found that newly reported chronic bronchitis or emphysema (adjusted for smoking and other factors) in deployed versus nondeployed personnel varied by service branch, but none was statistically significantly elevated. When the analysis was restricted to deployed cohort members with self-reported information on deployment location, the odds of chronic bronchitis or emphysema were not statistically different in any of the deployment locations examined. The results from Smith et al. (2012) are described below along with other studies that examined burn pit–specific exposures and associations with COPD, chronic bronchitis, or emphysema. The two studies that used data collected as part of the NewGen Study (Barth et al., 2014, 2016a) examined the association between deployment to Southwest Asia and self-reported, doctor-diagnosed bronchitis (they did not distinguish between acute and chronic). When year of diagnosis was stratified by before or after 2001, adjusted odds (which included smoking) of bronchitis differed. For those diagnosed before 2001, deployment was associated with statistically significant decreased odds of bronchitis, but among those with respiratory disease diagnosed in 2001 or later, there was no difference in the odds of bronchitis between the deployed and nondeployed groups (Barth et al., 2014). Barth et al. (2016a) then examined specific military exposures and found that the highest adjusted odds (which again included smoking) of bronchitis among deployed veterans were for those categorized as “high exposure” and who self-reported as exposed to diesel, kerosene, or other petrochemical fumes. Nondeployed veterans also had statistically significant increased odds of bronchitis for all specific exposures and for both the high-exposure and low-exposure categories. These results show that exposures were associated with development of bronchitis in both deployed and nondeployed groups, but the confidence intervals for the adjusted ORs all overlap between the deployed and nondeployed groups.
In contrast to use of deployment to the Southwest Asia Theater of Military Operations as a metric for exposure, some studies examined specific exposures (e.g., burn pits [Abraham et al., 2014; AFHSC, 2010; Liu et al., 2016; Sharkey et al., 2015; Smith et al., 2012], fires and fumes from oil wells or sulfur plants [Baird et al., 2012; Barth et al., 2016a], blast [Pugh et al., 2016], or depleted uranium [Hines et al., 2013]) upon which to draw an
assessment. In a study of prevalence of self-reported chronic bronchitis in a random sample of Swedish military personnel who were either currently or previously stationed in Kosovo or Afghanistan compared with that of a matched Swedish general population sample, Saers et al. (2017) found that the prevalence of chronic bronchitis over the preceding 12 months was statistically significantly greater in the military personnel than in the matched population, but prevalence was no different in the service personnel stationed in Afghanistan than in those stationed in Kosovo. In those stationed in Afghanistan, there was a significantly higher prevalence of chronic bronchitis in those exposed to sandstorms than in those not exposed to sandstorms. Among the three studies that examined COPD, chronic bronchitis, or emphysema in U.S. 1990–1991 Gulf War veterans, few inferences can be made on the association of deployment and these outcomes because the sample sizes were small (Hines et al., 2013), did not make comparisons based on deployment to Southwest Asia (Khalil et al., 2018), or they used a highly selected sample and comparison that do not allow for generalizations (Zundel et al., 2019).
Several studies examined exposures of post-9/11 service members or veterans to burn pits, and the association with COPD, chronic bronchitis, or emphysema was mixed, with a majority finding no association. Three studies used overlapping data (although period of follow-up and size of the nondeployed population were different for each) of medical encounters several years after deployment to areas with or without burn pits or stationed in Korea compared with those who were never deployed and remained in the continental United States (Abraham et al., 2014; AFHSC, 2010; Sharkey et al., 2015). In general, risk of COPD was not increased for troops deployed to burn pit locations relative to the nondeployed U.S. service members in analyses that both did and did not adjust for smoking and other demographic and military factors. Deployment within 5 miles of a documented burn pit was not associated with increased odds for newly reported chronic bronchitis or emphysema compared with deployments outside of the 5-mile radius, and no association of chronic bronchitis or emphysema was found for cumulative days in proximity to a burn pit for any of level of exposure compared with the nonexposed group (AFHSC, 2010). Abraham et al. (2014), who did not adjust for smoking, found that COPD and allied conditions were statistically significantly increased for personnel at the two bases without burn pits but not for the two locations with burn pits relative to the nondeployed U.S. population. Sharkey et al. (2015) also found that the risks of COPD at the same bases as examined by the AFHSC (2010) and Abraham et al. (2014) were all similar to, or statistically significantly lower than, the risks for personnel who remained in the United States at 36 months and 48 months of follow-up. No observed association between COPD and locations with burn pits was found. Based on comparisons with the Korean-stationed group, these studies support that deployment to the Southwest Asia theater, but not necessarily potential exposure to burn pits, may be associated with an elevated post-deployment rate of COPD and allied conditions. Sharkey et al. (2016) extended their 2015 analysis by adding locations in Afghanistan, sites with poor air quality similar to those previously assessed, and a base in Kyrgyzstan, that had relatively better air quality, and they extended the follow-up period of active-duty personnel to 12 years. No statistically significant differences for COPD (identified by ICD-9-CM codes) were found between the Kabul cohort and the other location cohorts. In an analysis of Millennium Cohort Study data to examine the effects of exposure to documented open-air burn pits within 2, 3, or 5 miles on chronic bronchitis or emphysema, Smith et al. (2012) found that adjusted odds of newly reported chronic bronchitis or emphysema were statistically significantly increased for women, consistent smokers, and Army personnel. When three proxy measures of burn pit exposures were examined, no associations were found for deployment within 3 miles of burn pits and new-onset chronic bronchitis or emphysema when compared with deployments to areas with no documented burn pit exposure; for individual sites with documented burn pits compared with those deployed outside of the 3-mile radius exposure window; or for an increasing number of cumulative days of exposure within a 3-mile radius of the burn pits compared with cohort members with no burn pit exposure. Findings of no association with new-onset chronic bronchitis or emphysema for deployment status, cumulative deployment length, and camp location were consistent when examining the risk within 5 miles of the burn pits. Finally, Liu et al. (2016) examined the associations between assumed geographic and self-reported burn pit emissions exposure (within 2 miles) and self-reported emphysema, chronic bronchitis, or COPD in participants of VA’s Airborne Hazards and Open Burn Pit Registry. Burn pit emissions exposure was determined by quartiles of days of deployment near burn pits and, separately, quartiles of self-reported total hours of burn pit smoke exposure. Self-reported diagnoses were compared with VA medical record information. Smoking was not found to be statistically significantly associated with self-reported burn pit smoke exposure. A strong exposure–response association
was found between cumulative days deployed within a 2-mile radius of a burn pit and self-reported emphysema, chronic bronchitis, or COPD (adjusted for smoking), but the same association was not observed when VA medical record diagnoses (based on ICD-9 codes) were used in place of self-report. Likewise, when the number of self-reported hours per day of burn pit smoke exposure was used as the measure of exposure, the exposure–response association with self-reported emphysema, chronic bronchitis, or COPD was strongly statistically significant, but the association did not persist when VA medical records diagnoses were instead used to characterize the diseases.
Several studies used ICD-9 codes to examine associations with COPD, chronic bronchitis, or emphysema and deployment or specific deployment-related exposures. Baird et al. (2012) examined post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant in Iraq in 2003 and found inverse associations for COPD (statistically significantly lower morbidity ratios for fighters, and separately, the potentially exposed personnel downwind of the fire compared with the group deployed to the area after the fire was extinguished), which may reflect a relatively short follow-up time and lack of adjustment for significant confounders, including smoking and other environmental or occupational exposures. Pugh et al. (2016) conducted a retrospective cohort study to examine the prevalence of chronic lung diseases, including COPD, based on ICD-9-CM codes and military deployment, using VA health care data. Over the study period, 5,998 (0.8%) individuals had a diagnosis of COPD (ICD-9-CM 491, 492, 494, 496); 56.9% were classified as tobacco users compared with 21% who did not have lung disease. Odds of COPD were statistically significantly increased for all age groups over 30 years, for those with a TBI diagnosis, and tobacco users. Individuals who had multiple deployments were statistically significantly less likely to have a COPD diagnosis compared with individuals with only one deployment, adjusted for demographic characteristics, multiple deployments, tobacco use, and TBI. The nature of exposures during deployment could not be assessed; however, reports of blast injury as reflected by TBI were also associated with increasing rates of COPD.
A number of issues remain unresolved in the assessment of the relationship between airborne hazards exposure in the Southwest Asia theater and COPD. There is—as is the case in almost all airborne hazards research in military and veteran populations—a lack of specification in defining exposure. Most of the studies the committee reviewed use deployment status as an exposure proxy, and when specific deployment locations are taken into account, the details of duration or intensity are often missing. On the diagnostic side, either self-report or (more rarely) chart review is most often used to document the conditions. The committee was forced to rely on studies that used retrospective administrative databases rather than planned investigations, which greatly weakened their ability to draw informed conclusions.
In addition, there seems to be a lack of understanding, when these studies are reported of the need to account for the fact that few of the veterans examined have reached an age when one would expect to see increased risk of being diagnosed as having COPD—an expectation that derives from the well-established association between chronic cigarette smoking and the disease.12 This is further confounded by the practice followed in multiple studies of treating bronchitis as a singular outcome, rather than differentiating between the acute and chronic forms of the disease.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of chronic obstructive pulmonary disease, including chronic bronchitis and emphysema. It notes that one would expect chronic obstructive pulmonary disease to be detectable only after a longer period of follow-up than was available for most of these studies. Chapter 5 includes a description of epidemiologic study designs that might, if it were possible to carry them out, provide greater insight on this issue.
___________________
12 If, however, an occupational exposure model of COPD is used, one could entertain the possibility of short-term intense exposures causing COPD that might be detected after only a short period of follow-up.
Constrictive Bronchiolitis
The diagnostic category of bronchiolitis contains several small airway diseases, which are defined by the presence of bronchiolar inflammation, fibrosis, or both (Singer et al., 2016). Further classification is based on the location of the fibrosis and inflammation within the bronchiole (e.g., luminal, mural, or peribronchiolar) and the cellular components of the inflammatory infiltrate (e.g., neutrophilic, lymphocytic, histiocytic) (Singer et al., 2016). Prior to the ATS/ERS classification in 2001, the term “bronchiolitis obliterans” occasionally referred to cases of bronchiolitis obliterans organizing pneumonia, which were characterized by intraluminal polyps of granulation tissue (ATS and ERS, 2002). These cases are now classified as the small airway component of organizing pneumonia. Obliterative bronchiolitis, also called bronchiolitis obliterans or constrictive bronchiolitis, is defined histopathologically by the presence of subepithelial fibrosis (Colby, 1992; Epler and Colby, 1983). This fibrotic constrictive lesion develops externally to the airway lumen, constricting the airway by encircling it with eventual obliteration of the lumen. This is distinct from the inflammatory proliferative lesion that develops internally from the airway wall, filling the lumen with an inflammatory polypoid lesion or buds of granulation tissue, and which is referred to as proliferative bronchiolitis and also as cryptogenic organizing pneumonia and, previously, bronchiolitis obliterans organizing pneumonia (Epler, 2010).
Studies of constrictive bronchiolitis are difficult to conduct because the disease is difficult to diagnose, both on clinical testing and on lung biopsy. Noninvasive diagnostic tests often have low sensitivity (true positive rate), so the diagnosis of constrictive bronchiolitis often requires thoracoscopic lung biopsy. Histologic diagnosis is dependent on the proper inflation and staining of pathologic samples. Otherwise the condition may be misdiagnosed due to tissue artifact. The lesions of constrictive bronchiolitis may be patchy and occupy only a short segment of a longer bronchiole. Because of this patchy nature, there may be false negatives on lung biopsy, and specific techniques should be used to increase sensitivity for diagnosis. These methods include performing multiple “step” sections from the paraffin-embedded tissue block and performing elastic stains (e.g., Voerhoff von Giesson, Movatt pentachrome) to highlight the presence of increased fibrosis occupying the space between the epithelial basement membrane and the small airway elastica. There are other histologic clues that may aid in diagnosis due to their frequent association with constrictive bronchiolitis. These clues include foamy macrophage accumulation within terminal bronchioles, cholesterol granuloma formation (stasis granulomas), smooth muscle hypertrophy, and proximal bronchiolectasis and bronchiectasis with chronic inflammation. These additional histologic features are non-specific and should not be used to diagnose constrictive bronchiolitis in the absence of subepithelial fibrosis. For example, bronchiolar smooth muscle hyperplasia has been described in asthma and COPD (Colby, 1998).
Further diagnostic challenges arise from a histologic artifact that occurs secondarily to post-biopsy ex vivo smooth muscle contraction in lung tissue (and other types of tissues) (Thunnissen et al., 2016). In these biopsies the bronchiolar smooth muscle tends to show circumferential constriction, which results in a decrease in airway diameter. This constriction results in accentuated differences when the airway is compared with the paired pulmonary artery, as the arteries tend to show longitudinal constriction and do not show significant diminution of luminal diameter. This effect is less commonly observed in lobectomy and pneumonectomy specimens in which formalin is perfused through the airways, resulting in inflation of the bronchioles and alveoli. The histologic appearance of decreased bronchiole luminal diameter, bronchiolar epithelial scalloping, and prominence of the smooth muscle layer all can indicate possible side effects of this ex vivo smooth muscle contraction. Figure 4-1 consists of three panels. Panel 4-1a (left) displays a normal bronchiole with a typical airway wall anatomy. Panel 4-1b (middle) depicts the pathology seen in constrictive bronchiolitis in which fibrous tissue (scarring) is deposited between the epithelial basement membrane and the elastic tissue layer, resulting in a narrowing of the bronchiolar lumen and subsequent airflow obstruction. Panel 4-1c (right) shows how, if a biopsy specimen is not inflated, it can create an artificial narrowing of the airway, which may be misdiagnosed as constrictive bronchiolitis. In light of the above issues in diagnosis, a recognition of subepithelial fibrosis is necessary to differentiate authentic cases of constrictive bronchiolitis from histologic mimics.
Both constrictive bronchiolitis and proliferative bronchiolitis can be caused by environmental and occupational inhalation exposures. Historically, constrictive bronchiolitis was caused by accidental exposures to high concentrations of toxic gases, such as chlorine and oxides of sulfur and nitrogen. More recently, diacetyl-containing food
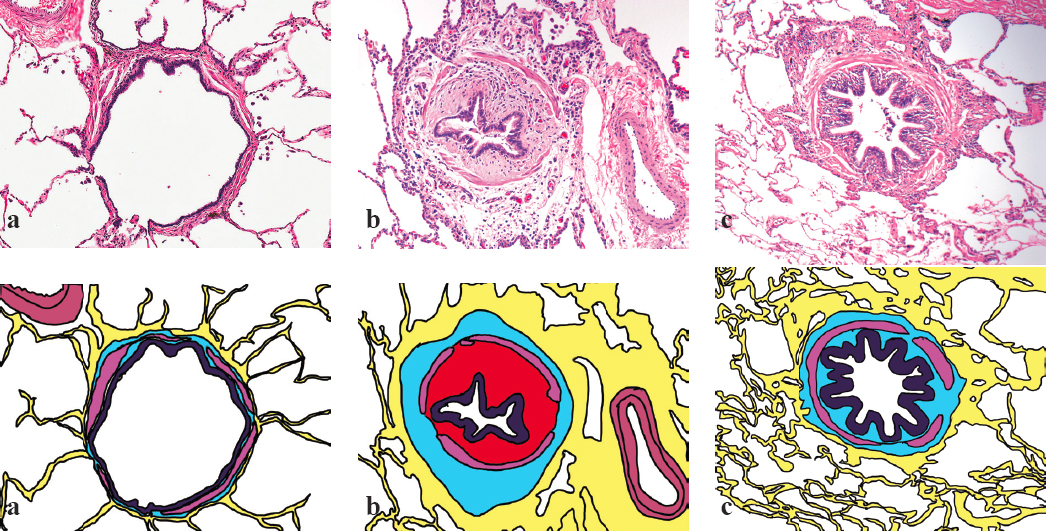
4-1a (top left): A normal bronchiole from a resected inflated lung shows a typical airway wall with layers of ciliated respiratory epithelium, subepithelial basement membrane, elastica, and smooth muscle, all in close continuity.
4-1a (bottom left): A corresponding line drawing highlights the close apposition of smooth muscle (pink), elastica and subepithelial connective tissue (light blue), and epithelium (purple).
4-1b (top middle): In constrictive bronchiolitis there is a deposition of fibrous tissue between the epithelial basement membrane and the elastic tissue layer. This scarring results in a narrowing of the bronchiolar lumen.
4-1b (bottom middle): A corresponding line drawing shows the separation of the smooth muscle (pink) and the elastica and subepithelial connective tissue (light blue) from the epithelium (purple) due to the presence of dense fibrosis (red).
4-1c (top right): In specimens that are not inflated with formalin through the airway (including most surgical wedge biopsies and all transbronchial biopsies) it is common to have smooth muscle contraction, resulting in an artifactual narrowing of the airway. This can be mistaken for constrictive bronchiolitis but can be differentiated from it by the lack of scar tissue between the epithelial basement membrane and the elastic tissue layer.
4-1c (bottom right): A corresponding line drawing shows that the smooth muscle (pink) has contracted and the lumen of the airway has narrowed, but the epithelium (purple) is still in close continuity with the subepithelial connective tissue and elastica (light blue) and smooth muscle.
flavorings and other flavoring chemicals have been shown to cause constrictive bronchiolitis (Kreiss, 2013). A 2013 review of the literature on occupational causes of constrictive bronchiolitis that focused on literature published between 2009 and 2012 highlighted the difficulties with the pathologic description of constrictive bronchiolitis (Kreiss, 2013). Whereas constrictive bronchiolitis following high-dose acute exposures often results in fixed airflow limitation without a response to bronchodilator on spirometry testing, a more indolent form of bronchiolitis associated with exertional dyspnea and cough, with more subtle lung function abnormalities, and without a recognized hazardous exposure is a more common presentation. The review included studies of biopsy-confirmed case series of constrictive bronchiolitis from U.S. soldiers, Iranian survivors of sulfur mustard gassing, hospital-based studies, and flavoring-related cases, all documenting that indolent cases of constrictive bronchiolitis can have normal spirometry or either restrictive or obstructive abnormalities. High-resolution CT studies can be normal
or can reflect air trapping and mosaic attenuation on expiratory films. Constrictive bronchiolitis is a rare disease without required surveillance, so prevalence estimates in the general U.S. population are unknown.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms as a group, but none of the studies reviewed in these previous volumes reported on outcomes of constrictive bronchiolitis. The 2011 report on long-term health consequences of burn pit exposure in Iraq and Afghanistan identified constrictive bronchiolitis as a disease that warranted further study as to whether burn pit exposure is associated with development of the disease (IOM, 2011). That determination was based on reports of several cases among soldiers deployed to bases with burn pits (Bartoo, 2010; King et al., 2008; Miller, 2009) and on a study by King et al. (2011). However, because constrictive bronchiolitis is one of the outcomes specifically included in this committee’s Statement of Task, it is included in the update of the scientific literature.
In response to these cases of chronic bronchiolitis, the U.S. Army Surgeon General requested a further study by the Center for Health Promotion and Preventive Medicine at Fort Campbell, Kentucky (APHC, 2010). The exploratory analysis of chronic or recurring lung disease among veterans exposed to the Mosul sulfur fire in 2003 (191 Army firefighters and 6,341 soldiers located within 50 km of the fire) compared with unexposed deployed troops found no association between exposure to the fire and chronic bronchiolitis, but the possibility of health effects could not be ruled out. Follow-up was conducted through June 2007.
One of the questions included in VA’s Airborne Hazards and Open Burn Pit Registry asks if a participant has ever been told by a health care professional that he or she had constrictive bronchiolitis. The question was restricted to those who had answered that they had been told by a health care professional that they had a lung disease or condition other than asthma, emphysema, chronic bronchitis, or COPD. Among the 4,333 participants eligible to answer this question, 501 (11.6%) reported yes, 2,984 (68.9%) said no, and 848 (19.6%) did not respond (NASEM, 2017). No additional analyses were conducted for constrictive bronchiolitis in the report.
Update of the Scientific Literature on Constrictive Bronchiolitis
There is some evidence that constrictive bronchiolitis may be more common among military personnel who have been deployed to Southwest Asia. The committee identified four studies of constrictive bronchiolitis in U.S. service members deployed in support of OEF/OIF (King et al., 2011; Krefft et al., 2020; Madar et al., 2017; Morris et al., 2020). Studies that grouped outcomes of constrictive bronchiolitis with other diagnoses (Krefft et al., 2017) were not included in this section. Although less robust and of limited value compared with full published analyses, four abstracts that were published as conference posters at the American Thoracic Society’s 2017 annual meeting are included for completeness because constrictive bronchiolitis is an outcome of special focus in the committee’s Statement of Task.
In the first study from February 2004 through December 2009, King et al. (2011) evaluated 80 soldiers at Fort Campbell, Kentucky, who had respiratory symptoms and who were referred to the clinic because of exercise intolerance resulting from exertional dyspnea. All the soldiers had been deployed to Iraq or Afghanistan, and all underwent extensive evaluation of occupational and environmental exposures. Of the 80 soldiers, 49 were referred for video-assisted thoracoscopic lung biopsy, and 38 of the referred 49 were diagnosed with constrictive bronchiolitis. Constrictive bronchiolitis was defined as an increase in wall thickness of more than 20% as compared with normal thickness, and this thickness could be due to subepithelial fibrosis, smooth muscle hypertrophy, or both. The airway thickening was due to smooth muscle (7 cases), fibrous tissue (3 cases), and mixed smooth muscle and fibrous tissue (28 cases). Other small airway findings included respiratory bronchiolitis, bronchiolar inflammation, pigment deposition with polarizable material, and bronchial-associated lymphoid tissue. Results on pulmonary function and cardiopulmonary exercise testing for the soldiers with constrictive bronchiolitis were compared with results for historical military control subjects (69 asymptomatic active-duty soldiers who were evaluated at an army tertiary care center in 2002). The 38 soldiers with constrictive bronchiolitis had a variety of military jobs; 35 were men; 25 were lifetime nonsmokers, 7 were active smokers, and 6 were former smokers; and 28 had served in
northern Iraq in 2003 and reported having been exposed to smoke from the Mosul sulfur-mine fire. Other reported exposures included dust storms (n = 33), incinerated solid waste in burn pits (n = 24), and incinerated human waste (n = 18). However, 11 of the soldiers who underwent biopsy reported having had no exposure to the sulfur-mine fire or any other exposure. Physical chest examinations were normal in all the soldiers. High-resolution CT tests were performed on 37 soldiers, and 25 of them had normal results. PFT showed some decreased values when compared with military controls, but results were generally within normal limits. Letters to the editor regarding this analysis included questions regarding other exposures, particularly to chlorine gas (Zarogiannis and Matalon, 2011); pre-biopsy workups for asthma, exercise-induced bronchospasm, and vocal-cord dysfunction (Morris and Zacher, 2011); and questions regarding the histopathologic diagnosis of constrictive bronchiolitis (Kuschner, 2011). The authors responded, offering additional details of the testing protocol. The committee finds this case series to be relevant to its charge but notes that a non-standard, broad definition of constrictive bronchiolitis was used, which may have overdiagnosed the condition due to tissue artifact (Thunnissen et al., 2016).
Following the publication by King et al. (2011), there was interest in whether other populations of service members that had undergone biopsies would show a similar high prevalence of constrictive bronchiolitis. Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or the Joint Pathology Center from January 2005 through December 2012 in 391 service members (137 had deployed to Southwest Asia prior to biopsy [deployed] and 254 had not deployed before the biopsy [nondeployed]). According to electronic medical records, 41% of the deployed and 56% of the nondeployed personnel were prior smokers; whether changes in smoking habits occurred during deployment or at the time of biopsy is not documented. Histologic diagnoses were categorized into 10 major histologic groups, one of which was small airways disease, which would include diagnoses of constrictive bronchiolitis; no cases of constrictive bronchiolitis were found in those who had deployed to Southwest Asia either prior to or after biopsy. In addition to the limitations of this study noted in Chapter 3, the identification of constrictive bronchiolitis was limited by the relatively small sample size, which was underpowered for detecting rare outcomes.
Krefft et al. (2020) aimed to describe deployment-related respiratory disease and the diagnostic utility of resting and exercise PFT with a retrospective study of 127 military personnel, veterans, and civilian contractors who supported military operations in Southwest Asia and who presented with new-onset respiratory symptoms between 2009 and 2017 and referred to a single occupational lung disease clinic. Detailed medical, occupational, and smoking histories were collected. Of the 127 patients, 113 underwent PFT as described in the summary of this study in the Pulmonary Function Testing section of this chapter. Chest CT scans were available for 118 of 127 symptomatic patients. Lung biopsies were performed in 52 patients. Deployment-related respiratory diseases were classified as proximal and/or distal. Distal lung disease included any one or more of the following on surgical lung biopsy: emphysema under low- or high-power magnification, histopathologic findings of hyperinflation/emphysema, bronchiolitis, non-necrotizing granulomatous inflammation, small airways inflammation, peribronchiolar fibrosis, or granulomatous pneumonitis. Bronchiolitis as a broad category was observed in 60% of biopsies. The non-specific terminology resulting from combining all forms of bronchiolitis into a broad category limited the inferences that could be made regarding constrictive bronchiolitis specifically. Although at least one case of constrictive bronchiolitis was described, the total number of cases was not given. The authors noted that the histologic abnormalities in symptomatic deployers represent a broader spectrum of distal lung injury than just constrictive bronchiolitis. Comparisons were made between those with and those without histologic findings of distal lung disease, which is not specific to constrictive bronchiolitis. Thus, this study is limited for the committee’s purposes because it is essentially descriptive, and it groups cases of interest into a larger category of distal lung disease and does not include a nondeployed or elsewhere-deployed control group.
Morris et al. (2020) reported the initial results of a detailed investigation of clinical lung diseases in military personnel deployed to the Southwest Asia theater under the auspices of the STAMPEDE III research initiative described in Chapter 3. STAMPEDE participants with chronic respiratory symptoms (n = 380) underwent a comprehensive cardiopulmonary evaluation that included a history and physical examination. Laboratory tests, radiographic imaging, and PFTs were performed, and the participants completed a questionnaire that elicited information on their deployment history, airborne exposures, smoking, and pulmonary symptoms before, during, and after deployment. Obstructive lung disease was observed in 11 (2.9%) patients; one case was diagnosed as
bronchiolitis. Seven of the 11 obstructive lung disease patients indicated that they were smokers, and no lung biopsies were performed.
In an identified conference poster, Jani et al. (2017b) examined whether service members participating in VA’s Airborne Hazards and Open Burn Pit Registry who self-reported a diagnosis of constrictive bronchiolitis have unique identifiable risk factors compared with those not reporting this diagnosis. Using a case–control design, 433 cases (affirmative response to the question of having ever been told they had constrictive bronchiolitis by a health care professional) were matched in a 1:2 ratio on age ± 1 year and sex with service members who responded no to that question. Potential risk factors were compared between the groups. Of those reporting a diagnosis of constrictive bronchiolitis, 90.1% were male, 45.2% were overweight, and 60.6% never smoked (9.4% reported current smoking and 25.5% reported past smoking). Cases reported comorbid respiratory conditions more frequently than controls, including chronic bronchitis (61.5% vs 19.3%, respectively), COPD (24.1% vs 0.2%), and asthma (47.0% vs 12.2%). The authors concluded that registry participants who self-reported a diagnosis of constrictive bronchiolitis self-reported other respiratory conditions more frequently than controls and that this may reflect uncertainty or confusion about diagnosed conditions. Given that participation in the registry is voluntary and no comparisons were made with nonregistry participants, self-selection bias is a concern. Using logistic regression, a diagnosis of constrictive bronchiolitis was found to increase with increasing levels of exposure to smoke from burn pits.
The lung biopsies from the King et al. (2011) cohort have been evaluated using various histologic, morphologic, and immunochemical methods in three studies presented in abstract form at international conferences (Gutor et al., 2019; Polosukhin et al., 2017, 2018). In the first study, Polosukhin et al. (2017) examined lung parenchymal tissue specimens from 12 veterans with confirmed constrictive bronchiolitis and 10 veterans without lung disease and who had never smoked to evaluate the hypothesis that constrictive bronchiolitis in service members may be the result of direct damage to the airway epithelium by airborne toxins due to incomplete epithelial regeneration, leading to long-term impairment of the epithelial barrier in distal airways. A mouse model of constrictive bronchiolitis was also developed and tested. Histologic sections were evaluated with hematoxylin and eosin, trichrome (for fibrosis), alpha-tubulin (for localization of cilia), immunoglobulin A (IgA) and polymeric immunoglobulin, or IgA and p65 subunit of nuclear factor kappa B (NF-κB) (looking for evidence of decreased immune capacity) or were hybridized to a bacterial 16s rRNA gene probe (to look for evidence of bacterial infection). The specimens from veterans with constrictive bronchiolitis showed the histologic presence of inflammation and subepithelial fibrosis and a loss of multi-ciliated cells in the bronchioles. Additional findings included decreased polymeric immunoglobulin receptor (pIgR) expression and reduced secretory IgA on the bronchiolar surface, evidence of bacterial invasion across the epithelium barrier, and NF-κB activation in epithelial cells. Significance testing was not reported. The reported findings suggest that airborne toxins may result in long-term epithelial remodeling resulting in decreased immune capacity and increased susceptibility to infection.
In the second study, Polosukhin et al. (2018) examined lung parenchymal tissue from 26 soldiers with constrictive bronchiolitis, 8 civilians with nondeployment constrictive bronchiolitis, 50 smokers with COPD, 24 lifelong nonsmokers, and 15 former smokers without lung disease. Tissue sections were evaluated with H&E, trichrome (for fibrosis), alpha-tubulin (for localization of cilia), IgA and polymeric immunoglobulin, or IgA and p65 subunit of NF-κB (looking for evidence of decreased immune capacity), or neutrophil elastase (for identification of neutrophils) or CD68 (for identification of macrophages), or else they were hybridized to a bacterial 16s rRNA gene probe (to look for evidence of bacterial infection). The abstract text did not indicate whether the pathologist conducting the examination was blinded as to exposure status. The COPD patients showed goblet cell metaplasia and stratification. A loss of multi-ciliated cells was the most common abnormality in constrictive bronchiolitis. Both diseases showed reduced secretory IgA, and 19% of small airways in constrictive bronchiolitis contained bacterial DNA within the epithelium. Significance testing was not reported. The results of constrictive bronchiolitis cases combined both the soldiers and the civilians, so it is unclear whether differences in constrictive bronchiolitis may be due to factors of deployment. The results suggested that there were different pathways for airway remodeling in COPD and constrictive bronchiolitis.
In the third study abstract, Gutor et al. (2019) described examining lung parenchymal tissue from 27 soldiers with constrictive bronchiolitis, 55 smokers with COPD, 8 lifelong nonsmokers, and 10 former smokers without lung disease. Histologic sections were evaluated with H&E, PAS (for mucus identification), PicroSirius Red (for fibrosis
evaluation), CD19, CD4, and CD8 (for B, T-helper, and T-cytotoxic cells). Airways were examined for inflammation, wall thickening, collagen content, and the number of alveolar attachments. The lungs of patients with COPD showed inflammation, wall remodeling and thickening, and a loss of alveolar attachments. Airways in patients with constrictive bronchiolitis showed wall fibrosis and inflammation. Significance testing was not reported. Fibrosis of small airways in constrictive bronchiolitis was found to be insufficient to cause airflow obstruction. This finding is supportive of the claim that the diagnostic criteria used in making the original diagnoses in King et al. (2011) were too sensitive and have resulted in a group of mixed small airway diseases and normal lung biopsies being called constrictive bronchiolitis.
Synthesis
Constrictive bronchiolitis is a rare disorder, the prevalence of which is not established in the general population. Diagnosis requires a biopsy, and the disease may be misdiagnosed if samples are not properly inflated. It was not identified with any frequency in the military population until 2008, when the cohort that underwent surgical lung biopsy from King et al. (2011) was published. Subsequent studies (Krefft et al., 2020; Madar et al., 2017; Morris et al., 2020) and analyses published as conference abstracts, some of which lacked lung biopsies, have described rare additional cases of constrictive bronchiolitis. Although participants in VA’s Airborne Hazards and Open Burn Pit Registry have self-reported high numbers of diagnoses (Jani et al., 2017b; NASEM, 2017), these cases are unconfirmed (responses to health questions were not verified with medical records) and may have been indicated due to uncertainty or confusion about diagnosed conditions. Three conference abstracts that evaluated the lung biopsies from the King et al. (2011) cohort using different histologic, morphologic, and immunochemical methods (Gutor et al., 2019; Polosukhin et al., 2017, 2018) found evidence of different pathways for airway remodeling in COPD and in constrictive bronchiolitis and indicated that the diagnostic criteria used in making the original diagnoses in King et al. (2011) were too sensitive, resulting in false-positive diagnoses of constrictive bronchiolitis. Therefore, the available published information on the relationship between deployment to Southwest Asia and subsequent development of constrictive bronchiolitis is lacking, which limits the inferences that can be made.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of constrictive bronchiolitis.
Interstitial Lung Diseases
Diseases that involve the parenchymal or gas exchanging units of the lung are referred to collectively as the interstitial lung diseases. Interstitial lung diseases can be divided into those that are associated with known causes and those that are idiopathic. Known causes include occupational and environmental exposures to inorganic dusts (e.g., asbestos, crystalline silica, and coal mine dust, which all cause pneumoconiosis), organic dusts (which cause hypersensitivity pneumonitis), drugs (such as some anticancer agents), and radiation therapy–induced lung injury. Alveolar-filling diseases, including pulmonary alveolar proteinosis (PAP) and acute eosinophilic pneumonia (AEP), are often grouped under the rubric of interstitial lung diseases. Autoimmune interstitial lung diseases commonly occur in association with connective tissue diseases (e.g., rheumatoid arthritis, systemic lupus erythematosus, and scleroderma). Interstitial lung diseases without known causes include sarcoidosis and the idiopathic interstitial pneumonias. The major idiopathic interstitial pneumonias are further characterized as respiratory bronchiolitis–interstitial lung disease, desquamative interstitial pneumonia, idiopathic pulmonary fibrosis (or usual interstitial pneumonia), idiopathic nonspecific interstitial pneumonia, cryptogenic organizing pneumonia, and acute interstitial pneumonia (ATS and ERS, 2013). All the interstitial lung diseases are diagnosed based on a typical constellation of clinical findings, including medical and exposure histories, lung function
testing, chest imaging abnormalities, and targeted laboratory testing, often but not always with lung biopsy. The following sections review the epidemiologic literature on interstitial lung diseases that were examined in relation to deployment to Southwest Asia.
Sarcoidosis
Sarcoidosis is an inflammatory disease that most commonly affects the lung but may involve any other organ system as well. Localized collections of white blood cells (called granulomas) are characteristic of the lung inflammation in sarcoidosis and may progress to permanent scarring. This inflammation may cause symptoms of dyspnea, cough, chest tightness, and fatigue and may lead to lung function and gas exchange abnormalities. The diagnosis of sarcoidosis is based on three major criteria: a compatible clinical presentation, finding nonnecrotizing granulomatous inflammation in one or more tissue samples, and the exclusion of alternative causes of granulomatous lung disease (Crouser et al., 2020). Although environmental factors are suspected, the causes of sarcoidosis are unknown (NHLBI, 2015). Sarcoidosis closely resembles chronic beryllium disease, which is caused by exposure and immunologic sensitization to beryllium dust and fumes. Beryllium is a lightweight metal used in airplane and other types of metal parts. A careful exposure history in combination with specialized laboratory testing for beryllium sensitization is necessary to distinguish chronic beryllium disease from sarcoidosis. A recent study using the U.S. Optum database estimated the overall sarcoidosis incidence in the U.S. population to be 7.6–8.4 cases per 100,000 population per year and the prevalence to be 59.0–60.1 cases per 100,000 population, or 0.6% (Gerke et al., 2017). Following the September 11, 2001, World Trade Center attack, an increase in sarcoidosis was found in populations who were exposed to the area, including fire department, rescue, and recovery workers (Hena et al., 2018). Population estimates of the number of sarcoidosis cases in veterans who have deployed to the Southwest Asia theater were not available; however, sarcoidosis is included in the estimates of interstitial lung disease in this population (estimated prevalence of 0.3%) (Pugh et al., 2016).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous reports have not addressed whether deployment to Southwest Asia is associated with sarcoidosis. Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, but none of the studies reviewed in these previous volumes reported on the outcomes of sarcoidosis. However, Gulf War and Health: Volume 3 reviewed the epidemiologic literature to determine whether sarcoidosis is associated with combustion byproducts, and that committee concluded that there was inadequate/insufficient evidence to determine whether an association exists between exposure to combustion products and sarcoidosis. The 2011 report on the long-term health consequences of burn pit exposure in Iraq and Afghanistan used surrogate populations of individuals with exposures known to be associated with burn pit emissions (firefighters, incinerator workers, communities near incinerators) and relied on the assessments of studies of service members and veterans in Gulf War and Health: Volume 8 (IOM, 2010) for conclusions on the association between exposure and health outcomes in service members and veterans, except when new studies were identified. Like the Gulf War and Health series, respiratory symptoms, conditions, and diseases were presented as a group, and no studies of sarcoidosis were identified in service members or veterans (IOM, 2011).
Update of the Scientific Literature on Sarcoidosis
Four studies that examined sarcoidosis in post-9/11 veterans were identified (Banoei et al., 2019; Forbes et al., 2019; Madar et al., 2017; Morris et al., 2020). However, the analysis of STAMPEDE III (Morris et al., 2020) reported that only 6 people of the 380 in the study were diagnosed with interstitial lung diseases (which would include sarcoidosis), which does not help to inform knowledge about this outcome. One descriptive study that presented cases of sarcoidosis in 1990–1991 Gulf War veterans is also included for completeness (Hooper et al., 2008).
Post-9/11 Veterans
Banoei et al. (2019) conducted a small case–control study to evaluate whether veterans (n = 13) with sarcoidosis exhibited different plasma metabolomic and metallomic profiles than civilians (n = 30) with sarcoidosis. Sarcoidosis was defined as the presence of clinical signs and symptoms of pulmonary sarcoidosis or the presence or history of bilateral hilar lymphadenopathy on chest imaging, along with biopsy-
proven sarcoid-like granulomas in pulmonary samples, with the exclusion of other granulomatous conditions, including mycobacterial infection. To further analyze the metabolomic profiles of veterans without sarcoidosis who had similar exposure histories, 35 veterans with COPD were selected as controls, matched by race, gender, and deployment history. Civilians were recruited from the University of Miami Sarcoidosis Program and veterans from the Miami Veterans Administration Sarcoidosis Program. Proton nuclear magnetic resonance spectroscopy, hydrophilic interaction liquid chromatography mass spectrometry, and inductively coupled plasma mass spectrometry were used to quantify metabolites and metal elements in plasma samples. Multivariate data analysis was applied to reduce the complexity of metabolomics data and for data mining. Principal component analysis was performed to find outliers, trends, and similarities, using data sets derived from the plasma samples for the evaluation of interrelations and groupings of metabolomics data between veterans and civilians with pulmonary sarcoidosis and veterans with COPD. There were no significant differences in age, race, or lung function between veterans and civilians with sarcoidosis. Veterans with sarcoidosis differed from civilians, according to metabolic and metallomics profiles, but metabolomics and metallomics profiles were similar for veterans with sarcoidosis and veterans with COPD. The authors concluded that environmental risk factors may be important in the development of different molecular phenotypic responses of sarcoidosis.
Forbes et al. (2019) conducted a retrospective chart review using ICD-9-coded medical encounter data from the Defense Medical Surveillance System of all active-duty military personnel who were diagnosed with sarcoidosis from 2005 to 2010. Deployment dates and locations were obtained through the Armed Forces Health Surveillance Branch. Electronic medical records were reviewed for dates of diagnosis, temporal relationships between diagnosis and deployment, symptoms pre- and post-deployment, spirometry, diffusing capacity, radiographic staging, and treatment course. A total of 478 cases of pulmonary sarcoidosis were identified (determined by an inpatient encounter coded with both ICD-9 135 in any diagnostic position or two or more outpatient encounters with both codes ICD-9 135 and ICD-9 517.8 in any diagnostic position within 90 days). Of the identified cases, 400 (83.6%) had tissue biopsies showing granulomatous inflammation consistent with sarcoidosis, and the remaining 78 cases were diagnosed based on clinical findings without tissue confirmation. The diagnosis of sarcoidosis was established with a tissue diagnosis in 68% of the deployed cohort. Of the cases, 80% were male, 38.7% were never deployed, 11.7% were diagnosed prior to deployment, and 50.2% were diagnosed post-deployment. In the pre- and post-deployment cohorts, 76% had documented lung involvement. Overall differences in spirometry and in the radiographic stage of sarcoidosis were not identified. Annual incidence rates were assessed; the authors calculated an annual incidence rate of pulmonary sarcoidosis to be 11.19 per 100,000 person-years. The annual rates of sarcoidosis decreased significantly over the 6-year study period (p = 0.025) for all service branches combined. Army personnel were assessed separately because their rate was found to be twice that of all other services combined (IRR = 2.07, 95%CI 1.81–2.36), but the decrease in rates of sarcoidosis observed among active-duty Army personnel over the 2005–2010 time period was not statistically significant (p = 0.560). No statistically significant linear trend was observed for annual rates of pulmonary sarcoidosis among service members who had deployed in support of OEF/OIF/OND (p = 0.674), but the annual rate was statistically significant for those who did not deploy (p = 0.006). The authors concluded that their data did not suggest that military deployment to Southwest Asia is associated with any increase in disease severity based on spirometric or radiographic findings, but that there is a correlation between nondeployment and the development of sarcoidosis. The findings were limited by the retrospective analysis of data collected based on ICD codes from electronic health records, which may not be representative or completely clinically documented. Furthermore, asymptomatic sarcoidosis cases would not have been identified since there is no routine pre- or post-deployment radiographic screening of military personnel. In addition, a diagnosis of active sarcoidosis may preclude deployment, contributing to a finding of higher rates of disease in nondeployers and resulting in substantial detection bias.
Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center from January 2005 through December 2012 in 391 service members (137 had deployed to Southwest Asia prior to biopsy [deployed] and 254 had not deployed before the biopsy [nondeployed]). According to electronic medical records, 41% of the deployed and 56% of the nondeployed personnel were prior smokers; whether changes in smoking habits occurred during deployment or at the time of biopsy is not documented. Histologic diagnoses were categorized into 10 major histologic groups,
one of which was granulomatous disease, which would include diagnoses of sarcoidosis. The major histologic group granulomatous disease (which includes sarcoidosis) had no association with deployment status (16.1% vs 9.1%; p = 0.21), but within this group, the histologic category of non-necrotizing granulomas was more common among deployed participants (22 vs 23; p = 0.038); this was the only one of the 38 histologic categories that was more common in deployed participants. Logistic regression estimates indicate that non-necrotizing granuloma diagnosis was predicted by deployment status, with deployed individuals 2.4 times more likely to have this diagnosis than nondeployed individuals, an effect constant across age groups, gender, ethnicity, and tobacco use. In addition to the limitations of this study noted in Chapter 3, the inclusion of non-surgical samples may have enhanced the ability to diagnose sarcoidosis, if it had been present, and the several cases of non-necrotizing granulomas would have been lost from the study had these small tissue samples been excluded from analysis.
1990–1991 Gulf War Veterans
Hooper et al. (2008) used DoD administrative data to examine the long-term hospitalization experience based on ICD-9-CM codes of regular active-duty U.S. Gulf War veterans (n = 211,642) still on active duty between 1994 and 2004 (presented at 3-year intervals) compared with veterans who had separated from military service (n = 321,806). For the 10-year combined observation period, there were 43,346 hospitalizations for those who remained on active duty after 1994. Of those hospitalizations, 12.2% (n = 2,872) were coded as related to the respiratory system. For each diagnostic category, the top five primary diagnoses over the entire follow-up period were presented. Sarcoidosis ranked fifth at 7.1% (n = 79) of inpatient hospitalizations under the category of infectious and parasitic diseases (n = 1,115 for the category). However, sarcoidosis is not known to be an infectious or parasitic disease, and hospitalization data likely underrepresent those with chronic pulmonary sarcoidosis where treatment rarely requires hospitalization, limiting the generalizability of this study. This descriptive study is further limited by the lack of comparisons with the separated veteran group and the fact that no information was presented on hospitalizations stratified by Gulf War exposures.
Synthesis
Sarcoidosis is a multi-system inflammatory disorder that most commonly affects the lung. The clinical presentation ranges from asymptomatic disease to a progressive relapsing form. There is substantial variability in the number of organs involved with sarcoidosis, and the disease can be difficult to distinguish from others with similar clinical and histologic features, further contributing to diagnostic uncertainty. Sarcoidosis was not examined as an independent outcome in many of the previous reports of the Gulf War and Health series, and Volume 3 of the series found inadequate/insufficient evidence to determine whether an association exists between exposure to combustion products and sarcoidosis.
A small set of studies was identified that specifically examined sarcoidosis in relation to deployment to Southwest Asia. In a small case–control study (Banoei et al., 2019), according to metabolic and metallomics profiles, veterans with sarcoidosis were similar to veterans with COPD but differed from civilians with sarcoidosis. Forbes et al. (2019) performed chart reviews of the 478 cases of sarcoidosis diagnosed among all active-duty personnel from 2005 to 2010 using ICD-9-coded medical encounter data from the Defense Medical Surveillance System. Of the identified cases, 38.7% never deployed, 11.7% were diagnosed prior to deployment, and 50.2% were diagnosed post-deployment. Overall differences in spirometry and in radiographic stage of sarcoidosis were not identified between those who had deployed and those who did not. The annual rates of sarcoidosis decreased significantly over the 6-year study period for all service branches combined, but the rate for Army personnel was found to be twice that of all other services combined. These data do not suggest that military deployment to Southwest Asia is associated with any increase in disease severity based on spirometric or radiographic findings, but there does appear to be a correlation between nondeployment and the development of sarcoidosis. Asymptomatic sarcoidosis cases would not have been identified since there is no routine pre- or post-deployment radiographic screening of military personnel. In addition, a diagnosis of active sarcoidosis may preclude deployment, contributing to a finding of higher rates of disease in nondeployers and resulting in a substantial detection bias. Among the 391 biopsies of non-neoplastic lung disease among service members who were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center from January 2005 through December 2012, Madar et al. (2017) found that 35.0% had deployed to Southwest Asia prior to the biopsy. The major histologic group granulomatous disease (which includes sarcoidosis) had no association with deployment status, but within this group, the histologic category of
non-necrotizing granulomas was significantly more common among deployed participants. Logistic regression estimates indicate that non-necrotizing granuloma diagnosis was predicted by deployment status, with deployed individuals 2.4 times more likely to have this diagnosis than nondeployed individuals, an effect constant across age groups, gender, ethnicity, and tobacco use. The inclusion of non-surgical samples may have enhanced the ability to diagnose sarcoidosis and would have led to an underestimation of other diagnoses, such as bronchiolitis and idiopathic interstitial lung diseases, that require surgical lung biopsy for diagnostic confirmation. The other two studies identified that reported on sarcoidosis (Hooper et al., 2008; Morris et al., 2020) were descriptive and thus cannot be used to inform inferences about an association between deployment to Southwest Asia and sarcoidosis.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of sarcoidosis.
Hypersensitivity Pneumonitis
“Pneumonitis” is a general term that refers to inflammation of the gas-exchanging part of lung tissue. Hypersensitivity pneumonitis, sometimes included under the more generic term of “granulomatous pneumonitis,” is a disease in which the lungs become inflamed due to an immunologic reaction to an inhaled dust, or a chemical or biologic agent. Pereira et al. (2016) assert that “the disease is best classified as acute and chronic.” Environmental and occupational causes of hypersensitivity pneumonitis include exposure to particulates from bird droppings and feathers, to airborne bacteria and molds, and to several low-molecular-weight chemicals, which cause specific types of the disease, such as bird fancier’s lung, farmer’s lung, hot tub lung, and isocyanate hypersensitivity pneumonitis (Mayo Clinic, 2018b). The prevalence of hypersensitivity pneumonitis is unknown due to the challenges in identifying causal exposures and in clinical diagnosis. The difficulty in determining prevalence is compounded by the lack of standardized epidemiologic criteria for diagnosis. The estimated prevalence of hypersensitivity pneumonitis varies by industry, region, and work practices. Interstitial lung disease registries consistently show that hypersensitivity pneumonitis is in the top five most commonly occurring interstitial lung diseases worldwide and represents up to 15% of all interstitial lung diseases (Quirce et al., 2016).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, but none of the studies reviewed in these previous volumes reported on the outcomes of hypersensitivity pneumonitis. The 2011 report on the long-term health consequences of burn pit exposure in Iraq and Afghanistan used surrogate populations with exposures known to be associated with exposures to burn pit emissions (firefighters, incinerator workers, communities near incinerators) and relied on the assessments of studies of service members and veterans in Gulf War and Health: Volume 8 (IOM, 2010) for conclusions on the association between exposure and health outcomes in service members and veterans, except when new studies were identified. As with the Gulf War and Health series, respiratory symptoms, conditions, and diseases were presented as a group, and hypersensitivity pneumonitis was not one of the outcomes mentioned (IOM, 2011).
Update of the Scientific Literature on Hypersensitivity Pneumonitis
Krefft et al. (2020) aimed to describe deployment-related respiratory disease and the diagnostic utility of resting and exercise PFTs with a retrospective study of 127 military personnel, veterans, and civilian contractors who supported military operations in Southwest Asia, who presented with new-onset respiratory symptoms between 2009 and 2017, and who were referred to a single occupational lung disease clinic. Detailed medical, occupational, and smoking histories were collected, and 113 of the 127 underwent PFT, as described previously in the Pulmonary Function Testing section of this chapter, chest CT scans were available for 118 of 127 symptomatic patients, and lung biopsies were performed in 52 patients. Deployment-related respiratory diseases were classified as proximal and/or distal. Distal lung disease included any one or more of the following: emphysema under low- or high-power magnification, histopathologic findings of hyperinflation/emphysema, bronchiolitis, non-necrotizing granulomatous inflammation, small airways
inflammation, peribronchiolar fibrosis, or granulomatous pneumonitis on surgical lung biopsy. Granulomatous pneumonitis (50%) accompanied by lymphocytic interstitial inflammation was identified in half of the biopsies. Detailed descriptions of the histologic findings were not discussed. The study design precluded an assessment of the prevalence of granulomatous pneumonitis in symptomatic personnel who had deployed to Southwest Asia. This was primarily a descriptive case series that focused on describing the clinical spectrum of proximal and distal respiratory diseases found in those with persistent respiratory symptoms following deployment, and there was no comparison group. Comparisons were made between those with and without histologic findings of distal lung disease, which is not specific to pneumonitis. Thus, this study is limited for the committee’s purposes of inferences that can be made between deployment to Southwest Asia and hypersensitivity pneumonitis.
Synthesis
Hypersensitivity pneumonitis is an immune-mediated interstitial lung disease that occurs in susceptible individuals following exposure to one or more environmental antigens. Although hypersensitivity pneumonitis is one of the more common interstitial lung diseases, variability in disease definitions and in clinical presentation and challenges in antigen-exposure recognition limit assessments of incidence and prevalence in military populations. Only one study, Krefft et al. (2020), examined outcomes of hypersensitivity pneumonitis in a small group of personnel who supported military operations in Southwest Asia over a 9-year period, but because no comparisons were made, this study is of limited use for making inferences.
Conclusions
Based on the results of the one available study of military personnel and veterans reviewed in this report, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of hypersensitivity pneumonitis.
Idiopathic Interstitial Pneumonias
The idiopathic interstitial pneumonias (IIPs) are a heterogeneous group of diffuse pulmonary diseases resulting from inflammation and fibrosis of lung tissue. Diagnosis relies on an integrated approach using multidisciplinary discussion among clinicians, radiologists, and, when appropriate, pathologists (ATS and ERS, 2002). Clinical data including symptom presentation, exposures, smoking status, associated diseases, lung function, and laboratory and imaging findings, sometimes with surgical lung biopsy, are needed for diagnosis. There are six major idiopathic interstitial pneumonias: respiratory bronchiolitis–interstitial lung disease and desquamative interstitial pneumonia (both of which are smoking related), idiopathic pulmonary fibrosis (or usual interstitial pneumonia) and idiopathic nonspecific interstitial pneumonia, grouped as chronic fibrosing IIPs; and cryptogenic organizing pneumonia and acute interstitial pneumonia, grouped as acute/subacute IIPs. Additionally, there are two rare idiopathic interstitial pneumonias, idiopathic lymphoid interstitial pneumonia and pleuroparenchymal fibroelastosis, and a category of IIPs termed unclassifiable (ATS and ERS, 2013). IIPs linked to smoking and the very rare or unclassifiable IIPs are not discussed.
Acute interstitial pneumonia is an idiopathic interstitial lung disease that is clinically characterized by a sudden onset of dyspnea and the rapid development of respiratory failure. It is histologically characterized by diffuse alveolar damage, often with organizing pneumonia or fibrosis. The definition of acute interstitial pneumonia excludes patients with acute respiratory distress syndrome (ARDS) attributable to an identifiable cause as well as patients with underlying fibrotic lung disease or systemic disorders known to be associated with lung involvement, such as connective tissue disease (Miller et al., 2019). Acute interstitial pneumonia is a rare illness in the U.S. general population (Vourlekis, 2004).
Idiopathic pulmonary fibrosis (IPF) occurs when the air sacs (alveoli) of the lungs become damaged and scarred. This scarred tissue can interfere with the exchange of oxygen from the lungs into the bloodstream. In the United States, IPF is a rare disease affecting about 100,000 people (roughly 0.03%), with 30,000 to 40,000 new cases diagnosed each year. Familial pulmonary fibrosis is less common than the sporadic form of the disease. Only a small percentage of cases of IPF appear to run in families (NLM, 2019). Data on pulmonary fibrosis in Southwest Asia theater veterans are unknown; one study estimated that 0.3% of OEF/OIF veterans who received care at VA hospitals and clinics had interstitial lung disease, including pulmonary fibrosis (Pugh et al., 2016).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous reports have not addressed whether deployment to Southwest Asia is associated with idiopathic interstitial pneumonias. Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, but none of the studies reviewed in these previous volumes reported on outcomes of idiopathic interstitial pneumonias.
Update of the Scientific Literature on Idiopathic Interstitial Pneumonias
As summarized under Sarcoidosis in this section, Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center over a 7-year period (2005–2012) in 391 service members (35% had deployed to Southwest Asia prior to biopsy [deployed] and 65% had not deployed before the biopsy [nondeployed]). According to electronic medical records, the deployed and nondeployed personnel differed by several demographic factors and by smoking status. Histologic diagnoses were categorized into 10 major histologic groups, of which idiopathic interstitial pneumonia was one group. This histologic group had the most cases, totaling 118 (30.2%) of all individuals. This histologic group was statistically significantly more common in the nondeployed participants (n = 90, 35.4%) than in the deployed group (n = 28, 20.4%), and it was the only major histologic group to show a statistically significant difference between deployed and nondeployed participants, p <0.01. Multivariable logistic regression models indicated that deployment did not significantly predict the diagnosis of the idiopathic interstitial pneumonia group, but increasing age was a significant predictor (p <0.001), as would be expected since idiopathic interstitial pneumonias typically occur in older age groups. Within the idiopathic interstitial pneumonia group, two histologic categories were significantly more common in the nondeployed than in the deployed individuals: organizing pneumonia (n = 45, 17.7% vs 14, 10.2%, respectively; p = 0.015) and usual interstitial pneumonia (n = 18, 7.1% vs n = 3, 2.2%, respectively; p = 0.040).
Pugh et al. (2016) conducted a retrospective cohort study to examine the prevalence of chronic lung diseases, including COPD, based on ICD-9-CM codes and military deployment using VA health care data from 760,621 U.S. veterans deployed to combat operations in Iraq or Afghanistan who received care from VA between October 1, 2002, and September 30, 2011. Interstitial lung diseases, including pneumoconiosis (500–508), postinflammatory pulmonary fibrosis (515), pulmonary eosinophilia (518.3), and pulmonary interstitial/infiltrative disorders (518.89), were grouped for analysis. A total of 2,372 diagnoses (0.3% of the study population) of interstitial lung disease were found over the study period, with the majority of cases being male (89.8%), white (57.5%), having served in the Army (70.0%), and enlisted (89.3%). Just over one-third (36.3%) used tobacco, and 15.7% had a diagnosed TBI. The prevalence of interstitial lung disease was calculated for each year between 2003 and 2011, and the data were examined for any changes in prevalence during that time; no differences were reported compared with 2011 (calculated using log-odds and controlling for demographics, multiple deployments, smoking, and the presence of TBI). Compared with individuals 30 years of age or younger, older age was statistically significantly associated with interstitial lung disease, as was African American race (compared with white) and females compared with males. Moreover, both smoking (OR = 1.83, 95%CI 1.66–2.02) and TBI (OR = 1.88, 95%CI 1.62–2.19) were statistically significantly associated with increased odds of a diagnosis of interstitial lung disease. No difference in the odds of interstitial lung diseases was found for individuals who had multiple deployments compared with those who had a single deployment (OR = 0.98, 95%CI 0.89–1.09). The nature of exposures during deployment could not be assessed, and the temporal sequence between deployment and diagnosis of interstitial lung disease is unknown. Because the veterans studied may have been too young for many to have developed symptoms of chronic pulmonary diseases, these results may be subject to both selection and ascertainment biases.
Synthesis
The heterogeneous group of idiopathic interstitial pneumonias comprises, by definition, pneumonias of unknown etiology. Idiopathic pulmonary fibrosis, desquamative interstitial pneumonia, and respiratory bronchiolitis are more common in smokers and occur mainly in older age groups (>50 years of age). Previous National Academies reports have not addressed whether deployment to Southwest Asia is associated with idiopathic interstitial pneumonias. Two studies of post-9/11 service members were identified that examined the outcomes of IIPs. In their retrospective review of biopsies that were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center, Madar et al. (2017) identified a total of 118 cases of interstitial pneumonias (30.2% of
all biopsies). This diagnosis was statistically significantly more common in the nondeployed than in the deployed group. Within the IIP group, two histologic categories were significantly more common in the nondeployed than in deployed individuals: organizing pneumonia and usual interstitial pneumonia. Pugh et al. (2016) examined the prevalence of chronic lung disease and military deployment using health care system data from 760,621 U.S. veterans deployed to combat operations in Iraq or Afghanistan who received care from VA. A total of 2,372 interstitial lung diseases were identified and grouped for analysis. Compared with individuals 30 years of age or younger, older age was statistically significantly associated with interstitial lung disease, as was African American race (compared with white), and females compared with males. No statistically significant difference was found between those who served in the Army and members of each of the other service branches or between individuals who experienced multiple deployments and individuals with a single deployment. Both smoking and TBI were statistically significantly associated with a diagnosis of interstitial lung disease.
Conclusions
Based on the results of the two available studies of military personnel and veterans reviewed in this report, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of idiopathic interstitial pneumonias.
Acute Eosinophilic Pneumonia
Eosinophilic pneumonias are a heterogeneous group of non-infectious lung disorders where the percentage of eosinophils (a type of white blood cell) is increased in lung and peripheral blood. Eosinophilic pneumonia is characterized by the infiltration of eosinophils into lung tissue. The disease can be either acute or chronic, and both are rare. Environmental and occupational exposures that have been associated with AEP include smoking (active and passive, particularly new-onset smoking); toxins, including the inhalation of cocaine and heroin, vaping, or water pipe use of tobacco or marijuana; and inhaled dusts, such as from the World Trade Center smoke (Rom et al., 2002; Sine et al., 2018). There are no reported AEP incidence rates in the general population of U.S. adults (De Giacomi et al., 2018). One study estimates the incidence rate of AEP among U.S. military personnel deployed to Iraq to be 9.1 per 100,000 person-years over the study period (Shorr et al., 2004).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous reports have not addressed whether deployment to Southwest Asia is associated with eosinophilic pneumonia. Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, but none of the studies reviewed in these previous volumes reported on outcomes of eosinophilic pneumonia.
Update of the Scientific Literature on Acute Eosinophilic Pneumonia
As summarized in Chapter 3 and under Sarcoidosis and IIPs in this section, Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or the Joint Pathology Center from January 2005 through December 2012 in 391 service members (137 had deployed to Southwest Asia prior to biopsy [deployed] and 254 had not deployed before the biopsy [nondeployed]). According to electronic medical records, 41% of the deployed and 56% of the nondeployed personnel were prior smokers; whether changes in smoking habits occurred during deployment or at the time of biopsy is not documented. Histologic diagnoses were categorized into 10 major histologic groups, of which eosinophilic pneumonia was one group. One case of AEP was identified in the nondeployed group, and one case of chronic eosinophilic pneumonia was identified in the deployed group. No statistically significant association was found with deployment status when multivariable binary logistic regression models were conducted on this outcome. In addition to the limitations of this study noted in Chapter 3 and other outcome-specific limitations discussed in other sections, eosinophilic pneumonia is rare and does not typically require lung biopsy for clinical diagnosis, resulting in substantial detection bias.
The Operation Iraqi Freedom Severe Acute Pneumonitis Epidemiology Group reported bilateral pneumonitis requiring intubation and mechanical ventilation in 19 U.S. military personnel deployed in the U.S. Central Com-
mand area of operations during March–August 2003 (OIF SAPEG, 2003). Two patients died. Of the 19 patients, 18 were men (median age 25 years; range 19–47 years), 12 were full-time active duty personnel, and 7 were in the reserves/National Guard. Service branches included Army (17), Navy (1), and Marine Corps (1); 11 were junior enlisted personnel, 7 were noncommissioned officers, and 1 was an officer. Military specialties included combat arms (8), engineering (3), transportation (2), signal corps (2), medical services (2), and military police (1). At the time they became ill, the individuals were located in Iraq (13), Kuwait (3), Djibouti (1), Qatar (1), and Uzbekistan (1). Other than two patients from the same unit with an onset of illness 4 months apart, no apparent geographic or unit-level clustering was identified. Of the 19 patients, the majority (15) smoked cigarettes or cigars, including the 10 patients whose cases were either confirmed or probable (based on the finding of eosinophilia). Nine of these 10 patients had begun smoking tobacco during deployment, compared with none of the 9 patients whose cases were suspected (based on respiratory failure from pneumonitis but without eosinophilia). All had been exposed to heat, dust, and varying amounts of environmental pollution (e.g., smoke). This was the first description of military deployment associated with AEP and included some with “possible” AEP before additional clinical and epidemiologic investigation was available.
In a follow-up to the 2003 report, Shorr et al. (2004) reported an expanded case series of morbidity and mortality from AEP in U.S. service members who were deployed in or near Iraq. Between March 2003 and March 2004, 18 definite or probable cases of AEP were identified prospectively from combat support hospitals in the U.S. Central Command area of responsibility and retrospectively using military records among a population of 183,000 service members. The incidence was 9.1 per 100,000 person-years (95%CI 4.3–13.3). Of the 18 identified cases, 2 died (1 definite and 1 probable), resulting in a case-fatality rate of 11%. A standardized questionnaire was used to interview surviving patients and capture demographic, exposure, and clinical data. The cases were heterogeneous with respect to military occupation, specific location of deployment, and the timing of the onset of illness. A shorter version of the standardized questionnaire (absent the clinical collection tool) was self-administered in Iraq to a convenience sample of 72 members of the respective military units of the two soldiers who died (termed controls). Exposure questions included questions on the use of tobacco products (cigarettes and cigars); dust; sleeping location and duration; petroleum products; bulk ammunition; solvents or other chemicals; medical waste; close contact with the local population or prisoners of war; local sources of water; burning vehicles or buildings; human waste or other refuse; local foods; animals or animal droppings; insects; over-the-counter and prescription medications; insect repellants; and pesticide, fungicide, or herbicide application. Smoking status was categorized as nonsmoker, new-onset smoker, or chronic smoker. New-onset smoking was defined as initiation of smoking in the theater or immediately preceding deployment among former nonsmokers or prior smokers (who restarted after at least 1 year of cessation). Of the 16 surviving patients, 12 received follow-up evaluations that included a complete history and physical examination, allergen testing, clinical screening for the presence of atopy, repeat chest radiography, and PFT. Eosinophil cationic protein levels were measured, and many of the initial laboratory and serologic tests were repeated. The exams were specifically looking for evidence of recurrence, development of chronic eosinophilic pneumonia, or evolution of some new collagen vascular disease. The surviving patients were also re-interviewed using a standardized questionnaire. A detailed tobacco product analysis of samples of cigarettes and cigars available in the theater region was undertaken to test for several potential environmental agents. There was no evidence of a common source of exposure, person-to-person transmission, or similar time of disease onset. The most frequently reported exposures among patients were smoking tobacco (100%), fine airborne sand or dust (94%), convoy operations (76%), and close contact with the local population (71%). Tobacco smoking was the only exposure that was more common among patients than controls. All the patients in the theater reported smoking tobacco, and 14 (78%) were new-onset smokers. In contrast, 48 controls (67%) in the theater reported smoking tobacco, and only 2 reported that they started during this deployment. Military personnel who were new-onset smokers had a statistically significantly increased risk of AEP compared with controls (p <0.001). No other toxin or exposure was identified to account for the high incidence of acute eosinophilic pneumonia.
Sine et al. (2018) performed a retrospective chart review of 43 cases of AEP contained in the Army Public Health Center registry of military cases from March 2003 to March 2010 and treated at Landstuhl Regional Medical Center, Germany, after evacuation from the Southwest Asia theater. Because the intention of the study was to
compare these cases with those of other case series in order to make recommendations regarding changes in the diagnostic criteria for AEP, the inferences that can be made regarding AEP and possible exposures are limited. However, it was reported that 91% of the 43 were smokers, and 77% had recently started or restarted smoking. The cases include the same 18 cases as reported by Shorr et al. (2004) supplemented with additional cases for an additional 6 years (until 2010).
Synthesis
Previous National Academies reports have not addressed whether deployment to Southwest Asia is associated with eosinophilic pneumonia. AEP is a rare and potentially severe febrile respiratory disease that was first described in military personnel in a case series in 2003 (OIF SAPEG, 2003), then expanded to encompass a total of 18 cases deployed in or near Iraq over a 13-month period between 2003 and 2004 (Shorr et al., 2004). The majority were men, all used tobacco, and nearly all reported exposure to airborne dust. Epidemiologic investigation pointed to smoking, particularly new-onset smoking, as the most likely risk factor, though data were limited by similarities in environmental exposures between cases and controls and the lack of individual exposure characterization. An additional case series was identified that included the same cases as presented in Shorr et al. (2004) and identified 25 more cases through March 2010, but no comparisons of risk factors were made, limiting the usefulness of this study for the committee’s purposes. In their review of lung biopsies evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center, Madar et al. (2017) reported that there was one case of AEP in the deployed group and one case in the nondeployed group. Because of the small number of cases and the fact that AEP does not typically require biopsy, this study is not informative for examining AEP.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of acute eosinophilic pneumonia.
Pulmonary Alveolar Proteinosis
PAP is a diffuse lung disease in which lipoproteinaceous material composed principally of surfactant proteins accumulates in alveoli and blocks oxygen from diffusing into the blood, resulting in a feeling of breathlessness (dyspnea). PAP can be grouped into three major categories: primary PAP, secondary PAP, and congenital PAP (more accurately called disorders of surfactant production and clearance). Primary PAP is characterized by reduced granulocyte-macrophage colony-stimulating factor stimulation of alveolar macrophages, which reduces the ability of the macrophages to remove surfactant from alveoli (NORD, 2017). Secondary PAP has been associated mainly with exposure to high concentrations of respirable crystalline silica but has also been described in association with other hazardous exposures, including metal fumes (indium, aluminum) and several organic and inorganic dusts (Hwang et al., 2017; Ishii et al., 2011). PAP is a rare syndrome in the United States. One study using a large insurance claims database estimated the prevalence to be 6.87 per million in the general population, similar in males and females, and increasing with age (McCarthy et al., 2018). The pooled occupational exposure prevalence of PAP (i.e., the percentage of the total prevalence linked to workplace exposures) has been estimated at 29% (95%CI 21–37%) (Blanc et al., 2019).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Previous reports have not addressed whether deployment to Southwest Asia is associated with PAP. Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, but none of the studies reviewed in these previous volumes reported on outcomes of PAP.
Update of the Scientific Literature on Pulmonary Alveolar Proteinosis
As summarized in several outcomes in this section, Madar et al. (2017) retrospectively reviewed a series of biopsies of non-neoplastic lung disease that were evaluated at the Armed Forces Institute of Pathology or Joint Pathology Center over a 7-year period (2005–2012) in 391 service members (35% had deployed to Southwest Asia prior to biopsy [deployed] and 65%
had not deployed before the biopsy [nondeployed]). According to electronic medical records, the deployed and nondeployed personnel differed by several demographic factors and smoking status. Histologic diagnoses were categorized into 10 major histologic groups, and PAP was included under the category of “other.” There was one case of PAP in the nondeployed group. This outcome was not included in regression analyses.
Synthesis
All forms of PAP are rare disorders of surfactant production and clearance. Secondary causes of PAP, such as exposure to high concentrations of dust from respirable crystalline silica, aluminum, titanium, or indium-tin oxide, have not been described in association with Southwest Asia military deployment. Only one study (Madar et al., 2017) identified a case of PAP, and no comparisons were made.
Conclusions
Based on the results of the one available study of military personnel and veterans reviewed in this report, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and subsequent development of pulmonary alveolar proteinosis.
Infectious Lower Respiratory Diseases
The terms “bronchitis,” “acute bronchitis,” “pharyngitis,” “acute respiratory infection,” and even “cold” are nonspecific and overlapping, which makes them problematic for analyzing findings from epidemiologic investigations. Acute respiratory infections are common in the military population, especially among recruits and in other military environments, where close and crowded living conditions, physical and psychological stresses, environmental challenges, and demanding physical training all lead to more intense exposure as well as a state of relative immune compromise (Sanchez et al., 2015). In their review of respiratory infections in the U.S. military, Sanchez et al. (2015) stated that the incidence of hospitalizations for respiratory disease among recruits exceeds that among comparable civilian adults by 3- to 4-fold. Respiratory infections represent the most commonly diagnosed medical condition in recruits and personnel involved in advanced individual training phases, and they are estimated to account for 36,000 to 100,000 medical encounters affecting an estimated 25,000 to 80,000 recruits each year. Among non-recruit active-duty personnel, respiratory infections were estimated to account for 300,000–400,000 medical encounters and to affect 200,000–600,000 service members each year during the influenza seasons in 2012–2014. Exposure to novel respiratory pathogens may occur during deployments in areas where these diseases are endemic. During military deployments in the 1990–1991 Gulf War and Balkan peacetime engagements in the 1990s, novel respiratory infections accounted for 14% of all medical encounters. Wartime respiratory illness rates were estimated to be approximately 15% per month in Iraq and Afghanistan in 2003–2004 and in 2005–2006.
In a cross-sectional survey of 15,459 U.S. military personnel deployed to Iraq or Afghanistan during 2003–2004 who were participating in a rest-and-recuperation program, Sanders et al. (2005) found that respiratory illness, specifically cough or cold experienced during deployment, was self-reported by 69.1% of the personnel and that of these, 17.1% of cases were reported to be severe enough to seek medical care. An additional 2.6% reported that they had developed pneumonia. Of those reporting respiratory illness, 38.9% smoked (at least half a pack of cigarettes per day), and of the smokers, 47.6% had started or restarted smoking during deployment. Similarly, Riddle et al. (2008) found that 24% of 3,374 troops who were deployed to Afghanistan, Iraq, or Kuwait between April 2006 and March 2007 and completed deployment questionnaires reported that they had experienced at least one acute respiratory illness episode while deployed. Half of those who reported an acute respiratory illness episode sought care for it.
Acute Bronchitis
Acute bronchitis is an inflammation of the lining of the tracheobronchial tree, typically in association with a respiratory infection. Cough is the most common symptom; although the cough may initially be non-productive, it typically evolves to where it is producing thickened mucus. Acute bronchitis usually improves within 1 week to 10 days without lasting effects, though the cough may linger for several weeks. Acute bronchitis is usually caused
by viral infection. The environmental and occupational exposures that increase the risk of acute infectious bronchitis include smoking (passive and active) and airborne irritants, such as vapors or metal fumes (Mayo Clinic, 2017).
Acute bronchitis is common in the general U.S. population, and it is estimated that about 5% of the general population reports an episode of acute bronchitis per year (Singh et al., 2020). Similarly, acute bronchitis and other respiratory infections are common in the U.S. military serving in Southwest Asia, as noted above. Being in the military increases the risk of acute infections owing to environmental and lifestyle factors, such as living in barracks, close proximity, and stress, but whether deployment to Southwest Asia specifically increases the risk has not been systematically studied.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Although several studies of bronchitis were identified in 1990–1991 Gulf War veterans, only one specified acute bronchitis (Smith et al., 2002). As described under other outcomes in this chapter, Smith et al. (2002) used DoD hospitalization data (ICD-9-CM codes) from August 1991 through July 1999 to retrospectively examine associations between respiratory diseases, including acute bronchitis, and modeled exposure to oil-well fires among 405,142 active-duty service members who served in the 1990–1991 Gulf War at the time of the oil-well fires. Service members were categorized as exposed (n = 337,077) and nonexposed (n = 68,065) to oil-well fires, and no statistically significant difference in risk was found for acute bronchitis between exposed (n = 93) and nonexposed (n = 16) service members (RR = 1.09, 95%CI 0.62–1.90). These estimates were stated to be adjusted for demographic and military characteristics, but it was not clear which factors were adjusted for; smoking status was not collected. Analyses were limited to morbidity severe enough to require admission to a DoD hospital for inpatient care, a major limitation for an analysis of acute bronchitis, which rarely requires hospitalization, as is evident by the relatively few cases identified over the 8-year follow-up period.
As cited throughout this chapter, the AFHSC (2010) collected data on acute respiratory infections (ICD-9 460–466), which include acute bronchitis. The analysis examined medical encounters at military facilities by Army and Air Force personnel within 36 months of April 2006, after deployment to Joint Base Balad or Camp Taji (with burn pits), Camp Buehring or Camp Arifjan (without burn pits), or the Republic of Korea (urban air pollution and PM exposure) from 2005 to 2007. Poisson models that were adjusted for sex, birth year, marital status, race/ethnicity, education, smoking status, physical activity, service branch, military rank, pay grade, and occupation were used to calculate IRRs. Although several hundred cases of acute respiratory infections were reported for personnel in the Army and Air Force across all locations combined, acute respiratory infections were statistically significantly lower for service members deployed at all bases except Camp Arifjan (which showed no difference) than for service members who remained in the United States.
Update of the Scientific Literature on Acute Bronchitis
Five studies of acute bronchitis in post-9/11 service members and veterans were identified. Three of these were in U.S. personnel. The other two were descriptive studies of Polish coalition forces (Korzeniewski and Brzozowksi, 2011; Korzeniewski et al., 2013) that reported on the incidence of acute respiratory infections experienced in theater; since neither of these compared incidence rates in the deployed forces to rates among nondeployed service members or another appropriate comparison group, they provide no information to contribute to inferences that can be made regarding deployment to Southwest Asia and acute bronchitis.
Baird et al. (2012) examined the post-deployment respiratory health status of U.S. Army personnel potentially exposed to emissions from the fire at the Al-Mishraq sulfur plant near Mosul, Iraq, in 2003. Two were groups potentially exposed to the sulfur fire smoke plume—personnel involved in fighting the fire (n = 191) and personnel presumably downwind during the time of the fire (n = 6,341). These were compared with two unexposed groups: those who deployed to the area after the fire was extinguished (n = 2,284), and those who deployed to other Southwest Asia locations contemporaneously with the time of the fire (n = 1,869). Acute respiratory infection encounters (ICD-9-CM 460–466, inclusive) included acute bronchitis, although this outcome was not examined separately. The age-adjusted standardized morbidity ratio for acute respiratory infection was not statistically significantly different from 1.0 when firefighters were compared with the contemporaneously deployed group (morbidity ratio = 1.25, 95%CI 0.93–1.63) but was statistically significantly decreased when firefighters were compared with the group
deployed to the area before or after the fire (morbidity ratio = 0.74, 95%CI 0.54–0.96). Regarding the potentially exposed personnel who were deployed downwind of the fires, the standardized morbidity ratio for encounters for acute respiratory infections were statistically significantly increased when compared with the contemporaneously deployed group (morbidity ratio = 1.18, 95%CI 1.12–1.24), and statistically significantly decreased compared with the group deployed to the area before or after the fire (morbidity ratio = 0.70, 95%CI 0.66–0.73). Confounding due to potential uncharacterized differences in risk factors, such as smoking behavior and other environmental or occupational exposures, between the sulfur fire exposed and unexposed groups cannot be ruled out.
Sharkey et al. (2015) used the same deployed and nondeployed populations as the AFHSC (2010) analysis described previously but used a larger U.S.-based reference population and included an additional 12 months of data. This retrospective cohort study used Poisson models that were adjusted for age, pay grade, sex, race, and service branch to calculate IRRs for acute respiratory infections (ICD-9-CM 460–466)—which includes acute bronchitis—at two time periods: up to 36 months after the baseline data were gathered and up to 48 months afterward. The risks of acute respiratory infections at the four Southwest Asia bases and Korea sites examined were all statistically significantly lower (with the exception of Arifjan, which did not meet statistical significance) than the risks for personnel who remained in the United States. Similar results were found at the 48-month follow-up, with all groups except Arifjan again showing statistically significantly lower adjusted incidence rates of acute respiratory infections compared with the U.S. cohort. No observed association between acute respiratory infections and locations with burn pits was found.
Soltis et al. (2009) analyzed incidence and risk factors for self-reported acute respiratory illness in 2,872 troops deployed to Iraq, Afghanistan, and Kuwait who completed a self-reported questionnaire and a clinic health questionnaire between February 2005 and February 2006. Overall, 39.5% reported having at least one acute respiratory infection while deployed, with a rate of 15.0 episodes per 100 person-months among those who completed the voluntary deployment questionnaire and 24.8 episodes (95%CI 23.2–26.5) per 100 person-months among those who completed the clinic health screening form. Of these, 18.5% sought medical care and 33.8% reported having decreased job performance. Negative binomial regression analysis found female sex, service in the Navy, and a lack of flush toilets to be independently associated with increased rates of acute respiratory illness. Deployment to OIF, increasing age, and higher rank were also associated with an increased risk of acute respiratory illness. The study allowed a broad sampling of deployed U.S. troops at three sites during a defined time period with two different data sources for comparison. The study was limited by the self-reported data that lacked medical confirmation, by possible recall bias of those who were symptomatic, and by possible selection bias due to an under-representation of certain ranks and branches.
Synthesis
Acute respiratory illnesses (including acute bronchitis) are among the most commonly reported diagnoses during U.S. military deployments to Southwest Asia (Sanchez et al., 2015). Morbidity from acute infectious respiratory illnesses is particularly notable during the combat phase of operations, where there may be limited access to adequate hygiene and where the effects on individual and unit effectiveness may be substantial (Sanders et al., 2005). The contributions of exposure to either acute airborne hazards, such as the al-Misraq sulfur mine fire, or chronic daily PM, in addition to factors such as close and crowded living quarters, physical and psychologic stresses, and demanding physical training—causing more intense exposure and potentially having effects on immune status—are difficult to characterize except in aggregate from available published studies.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of acute bronchitis.
Pneumonia
Pneumonia is caused by an infection that inflames the lung air sacs. The air sacs fill with fluid or pus (purulent material), causing cough with phlegm, fever, chills, decreased oxygen saturation, and difficulty breathing. A variety
of organisms, including bacteria, viruses, and fungi, can cause pneumonia (Mayo Clinic, 2018c). Pneumonia is a common illness in the U.S. general population and is the primary diagnosis for an estimated 527,000 emergency department visits per year (CDC, 2016).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Few studies reviewed in previous Gulf War and Health volumes reported on pneumonia as an outcome. In their followup study of the health of Australian Gulf War veterans, conducted in 2011–2013, Sim et al. (2015) found 38 (5.5%) of the Gulf War–deployed and 17 (2.6%) of the comparison era veterans self-reported doctor-diagnosed or treated pneumonia since January 2001, resulting in a statistically significantly increased risk of pneumonia for veterans who had deployed to the Gulf War (RR = 1.87, 95%CI 1.03–3.39) after adjusting for age group, service branch, and rank estimated as of August 1990 and for any atopy at baseline and current smoking status (never, former, current smoker).
The AFHSC (2010) collected data on pneumonia and influenza (ICD-9 480-488). The analysis examined medical encounters at military facilities by Army and Air Force personnel within 36 months of April 2006, after deployment to Joint Base Balad or Camp Taji (with burn pits), Camp Buehring or Camp Arifjan (without burn pits), or the Republic of Korea (urban air pollution and PM exposure) from 2005 to 2007. Fewer than 30 cases were reported for both service branches and across all locations combined. Given this small number, the differences in incidence rates were not calculated.
Update of the Scientific Literature on Pneumonia
Eight studies of pneumonia in post-9/11 service members were identified (five in U.S. personnel and three among foreign personnel). However, the three studies of foreign coalition forces (Aoun et al., 2014; Korzeniewski and Brzozowksi, 2011; Korzeniewski et al., 2013) were descriptive studies that reported on the incidence of pneumonia infections experienced in the Southwest Asia theater but did not compare incidence rates among deployed groups or between deployed groups and a nondeployed or other appropriate comparison group, and thus they could not provide information to contribute to inferences that can be made regarding deployment to Southwest Asia and pneumonia. Two studies of post-9/11 U.S. service members were also excluded because they do not inform the evidence base of whether deployment to Southwest Asia is associated with differences in infectious respiratory diseases. Sanders et al. (2005) only reported on the self-reported prevalence of conditions without making any comparisons to nondeployed or other groups of deployed personnel, and Riddle et al. (2008) reported on grouped acute respiratory illness compared with historical data.
Post-9/11 Veterans
Abraham and Baird (2012) conducted a case-crossover study of short-term, for example, 0- and 1-day lagged, exposures to ambient PM2.5 and PM10 and cardiovascular and respiratory medical encounters (ICD-9 460–519) among 2,838 U.S. military personnel deployed to Southwest Asia. PM exposure was assessed using data collected over a period of approximately 1 year at 15 military bases. Of the qualifying health encounters, 83.5% were acute respiratory infections (n = 2,495), with an additional 1.6% (47) attributable to pneumonia and influenza. Ambient levels were routinely high at the bases assessed, but no statistically significant associations between PM and respiratory outcomes were observed in the young, relatively healthy, deployed military population. In addition to the several potential sources of bias detailed in Chapter 3, the statistical power of the assessment was limited by both the short (1-year) duration of the study and the small population under study—and likely also by the small magnitude of the effect of PM exposure on the risk of acute respiratory events in this population.
Eick et al. (2011) conducted a retrospective cohort study of 1,000 service members deployed between June 30, 2004, and June 30, 2007. The authors tested pre- and post-deployment sera for the presence of antibodies to different pathogens, including Chlamydia pneumoniae and Mycoplasma pneumoniae. The DoD Serum Repository, which maintains serum specimens collected from service members, was asked to identify service members who had at least two serum specimens available, collected within the 60 days preceding and following the deployment start and end dates, respectively. If multiple specimens met the requirements, the specimens collected closest to the deployment start and end dates were selected. From an original cohort of 14,360 personnel with appropriate samples, 1,000 were chosen randomly. Characteristics were similar between the study subjects and the total deployed cohort; most were white men. However, the study sample was more likely to be female (12.0% vs
9.4%, p = 0.0046) and in the Air Force (46.0% vs 24.7%, p <0.0001) compared with the total deployed cohort. Additionally, study subjects were more likely to have deployed in 2005 and 2006 than the total deployed cohort (p <0.0001). Pre-deployment seroprevalence for C. pneumonia was observed in 651 personnel (65.1%; 95%CI 62.2–68.1), and seroconversion during deployment was observed in 33 (10.2% of susceptibles; 95%CI 6.9–13.5). Pre-deployment seroprevalence for M. pneumonia was observed in 219 personnel (21.9%; 95%CI 19.4–24.5), and seroconversion during deployment was observed in 29 (3.7% of susceptibles; 95%CI 2.4–5.0). Seroprevalence and seroconversion percentages were stratified by demographic (age category, gender, and race) and military (service, component, year of deployment, length of deployment, number of previous deployments, and time since entry into military service) risk factors. Seroprevalence and seroconversion were compared among categories within these specific demographic, service, and deployment categories. The characteristics that were significantly associated with seroprevalence or seroconversion were included in a multivariate analysis to calculate adjusted ORs. Trends in seroprevalence and seroconversion percentages by these categories were assessed when appropriate. Self-reported symptoms (cough, runny nose, fever, weakness, headache, chest pain, trouble breathing, diarrhea, and vomiting) occurring during the deployment and reported on the post-deployment health assessment forms were compared between seroconverters and nonseroconverters overall and for each pathogen. Overall, 14.2% of service members seroconverted to at least one of six pathogens not including influenza; when influenza seroconversion was included, the rate increased to 30.1%. Pre-deployment seropositivity for C. pneumoniae and M. pneumoniae was different by race, and it was higher in black individuals than in white individuals (OR = 1.9, 95%CI 1.2–2.9 and OR = 1.7, 95%CI 1.1–2.5, respectively). After adjustment black participants still had higher odds of seropositivity to these pathogens compared with white participants. Black participants also had higher odds of M. pneumoniae seroconversion during the deployment than white participants (11.1% vs 2.3%, respectively; OR = 5.0, 95%CI 2.2–11.7). There was a decreasing trend of M. pneumoniae seropositivity with increasing year of deployment (29.3% in 2004 to 10.4% in 2007, z-statistic = 0.0012), a trend that held after adjustment for age and race. Overall, serologically confirmed respiratory infections were common among 2004–2007 OEF deployers, sometimes at higher rates than found in the overall U.S. population. Limitations of the study include a lack of information on smoking status, recall bias on the post-deployment health assessment, and possible false-positive and false-negative seroconversion tests.
1990–1991 Gulf War Veterans
One study of long-term hospitalization experience based on ICD-9-CM codes of DoD administrative data, which has been described throughout this chapter, of regular active-duty U.S. 1990–1991 Gulf War veterans still on active duty between 1994 and 2004 (n = 211,642) compared with veterans who had separated from military service (n = 321,806) was also identified (Hooper et al., 2008). For the 10-year combined observation period, the top five primary diagnoses of respiratory system diseases (n = 2,872) were presented, and pneumonia (organism unspecified) ranked second at 12.1% (n = 347). Although the number of pneumonia diagnoses was presented for the entire follow-up period for the active-duty group, no comparisons with the separated group were presented, thereby limiting the informativeness of this study.
Synthesis
Respiratory infections are common in deployed military personnel, but data linking lower respiratory infections, especially pneumonia, to hazardous inhalational exposures are limited. Only one study that reported on outcomes of pneumonia (Sim et al., 2015) was reviewed in the Gulf War and Health series; 1990–1991 Australian Gulf War–deployed veterans had a statistically significantly increased risk of self-reported doctor-diagnosed or treated pneumonia 10 years after service compared with Gulf War–era veterans. Conclusions regarding associations between respiratory outcomes and deployment to Southwest Asia in the Gulf War and Health series grouped all respiratory health outcomes and did not make separate conclusions for any infectious respiratory disease. Three new studies were identified that examined outcomes of pneumonia, two among post-9/11 veteran populations and one follow-up of 1990–1991 Gulf War veterans. Abraham and Baird (2012) examined pneumonia, among other respiratory health outcomes, and high ambient PM levels among U.S. service members deployed to Southwest Asia post-9/11 and found no statistically significant associations for pneumonia. Eick et al. (2011) conducted a retrospective cohort study of 1,000 deployed service members and found that serologically confirmed respiratory infections were common, with 30.1% of deployed service members having seroconverted to at least one of seven respiratory pathogens. While black race was associated with higher odds of M. pneumoniae seroconversion
during the deployment compared with white race, there was a decreasing trend of M. pneumoniae seropositivity with increasing years of deployment, and this decreasing trend remained after adjustment for age and race. In the study of long-term hospitalizations of 1990–1991 Gulf War veterans (Hooper et al., 2008), the number of cases of pneumonia was presented but no comparisons of effect estimates were presented.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of pneumonia.
Tuberculosis
Tuberculosis (TB), caused by infection with the organism Mycobacterium tuberculosis, tends to be a chronic illness; left untreated, particularly in immunocompromised hosts, TB infection can lead to death. TB most commonly infects the lungs but can involve other organ systems, including the skin, kidney, spine, and brain. Exposure occurs primarily from person-to-person transmission, although rare cases of iatrogenic transmission through contaminated medical equipment have occurred. Not everyone infected with TB bacteria becomes sick. Asymptomatic TB infection, which generally is not transmissible, is referred to as latent TB infection (LTBI). People with an active TB lung infection are usually symptomatic and can be contagious. The time course for disease onset following exposure is quite variable as disease may occur soon after infection (within weeks). Others develop a re-activated illness years later, especially if they develop a disease associated with a weakening of their immune system (Mayo Clinic, 2016). Environmental contributions to TB infections include crowded living conditions, exposures to tobacco smoke (Schmidt, 2008), and indoor air pollution from biomass stoves (Lin et al., 2007) in settings where active disease is more prevalent. In 2018 there were 9,029 TB cases or 2.8 cases of TB per 100,000 persons in the United States.
TB is not common in U.S. military populations. LTBI affects between 3.1% and 5.0% of the U.S. population, but the figure is 1% in military-aged groups. Although countries in the Southwest Asia theater are TB endemic, the prevalence of TB disease among military populations remains lower—0.4 cases per 100,000 in 2012—than in the U.S. population, largely because of the healthy warrior effect. Deployment to TB endemic areas is estimated to be responsible for 24% of cases in the active component military, but the activation of untreated LTBI existing prior to entry into military service is still the most important source of subsequent TB disease. However, one study, which may have excluded groups with the highest risk of LTBI, estimated that LTBI prevalence among deployed service members was the same as in the nondeployed population (Mancuso, 2017).
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Volumes 4, 8, and 10 of the Gulf War and Health series have discussed respiratory symptoms, conditions, and diseases as a group, and infectious diseases were generally either excluded entirely or grouped in the studies reviewed. However, Gulf War and Health: Volume 5 reviewed the epidemiologic literature on associations between deployment to the Gulf War and infectious diseases. No cases of active TB lung infection were recognized in military personnel who served in either Operation Desert Storm or Operation Desert Shield (Hyams et al., 1995). In many soldiers in some units, however, tuberculin skin tests were negative before the Gulf War and positive afterward (Oster and Sanford, 1992), indicating LTBI. Among the military personnel deployed to OEF and OIF, approximately 2.5% of those given pre- and post-deployment TB skin tests converted from negative to positive. TB skin test conversion is pathognomonic of relatively recent exposure to Mycobacterium tuberculosis; thus, transmission of M. tuberculosis occurred within some military units deployed to Southwest Asia.
Update of the Scientific Literature on Tuberculosis
Only one study that reported on outcomes of tuberculosis was identified. Khalil et al. (2018) described the study design for the Gulf War Era Cohort and Biorepository and provided preliminary results from the pilot phase of the effort, which had enrolled 1,275 veterans, 900 of whom had deployed to Southwest Asia. Self-reported health outcomes of symptoms (in the past year) and health care
provider–diagnosed conditions were reported stratified by users (n = 584) and nonusers (n = 679) of VA health care in the past year. A supplemental table for the paper that was posted to the web reported that of the 1,275 subjects who responded to the survey question asking whether a doctor or other health care provider had ever told them that they had tuberculosis, 28 (2.2%) answered yes (2.2% of both VA users and nonusers). No formal assessment of differences in the frequency of tuberculosis between VA users and nonusers was made nor were comparisons made between deployed and nondeployed veterans and, hence, these results do not inform questions about the role of Gulf War deployment on increased risk of TB.
Synthesis
The prevalence of both latent and active tuberculosis lung infection is low in U.S. military populations compared with the general U.S. population. Only one new study of TB was identified. Khalil et al. (2018) showed that approximately 2.5% of military personnel deployed to the 1990–1991 Gulf War who were given pre- and post-deployment TB skin tests converted from negative to positive, indicating that transmission of M. tuberculosis occurred within some military units deployed to Southwest Asia. The study did not compare rates of conversion between those who deployed and those who did not, limiting the conclusions that can be made from it regarding the role of deployment exposures and risk for TB.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of tuberculosis.
RESPIRATORY CANCERS
The committee’s Statement of Task directed it to pay particular attention to cancer in its examination of respiratory health outcomes associated with airborne exposures in the Southwest Asia theater. It considered the following cancers as relevant to their charge: lung cancer (carcinoma of the lung or bronchus), cancer of the esophagus, and oral, nasal, and pharyngeal cancers. In addition to studies that examined these cancers individually, studies that grouped these outcomes as “respiratory system cancers” were also reviewed.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Studies of respiratory cancers were summarized in Volumes 2, 3, 4, 8, and 10 of the National Academies Gulf War and Health series (IOM, 2003a, 2005, 2006, 2010; NASEM, 2016). The statements of task for these committees shaped their approach to these summaries. The committees responsible for Volumes 2 and 3 were charged with evaluating the scientific evidence that addressed whether a statistical association existed between exposure to specific agents and illnesses. The epidemiologic literature considered was thus different than what has been examined here, including not just studies of active duty personnel and veterans who served in the Southwest Asia theater but also studies of civilian cohorts that were exposed to the same or similar agents under different circumstances, for different durations, and at different exposure levels than the military populations. Volume 2, which evaluated the evidence regarding insecticides and solvents, reported that there was inadequate or insufficient evidence to determine whether an association existed between exposure to these agents and the cancers of interest.13 The committee responsible for Volume 3 concluded that there was sufficient evidence of an association between exposure to combustion products and lung cancer as well as limited or suggestive evidence of an association between exposure to combustion products and cancers of the nasal cavity and nasopharynx, cancers of the oral cavity and oropharynx, and laryngeal cancer. Inadequate or insufficient evidence existed to draw a conclusion about an association between exposures to fuels and these outcomes.
___________________
13 The committee could not reach consensus on whether the association between tetrachloroethylene exposure and lung cancer was inadequate or insufficient, or whether there was limited or suggestive evidence of an association.
Volumes 4 and 8—which addressed the health effects of serving in the 1990–1991 Gulf War—did not report a specific conclusion regarding any respiratory cancer. Both noted that many veterans were still too young for cancer diagnoses and that for most cancers the follow-up period after the Gulf War was probably too short to expect the onset of cancer. The Volume 10 committee concluded that “there is insufficient/inadequate evidence to determine whether an association exists between deployment to the Gulf War and any form of cancer, including lung cancer” (NASEM, 2016, p. 95).
Neither Long-Term Health Consequences of Exposure to Burn Pits in Iraq and Afghanistan (IOM, 2011) nor Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry (NASEM, 2017) drew conclusions about respiratory cancers.
In the summaries presented below, studies are categorized by country, beginning with those addressing U.S. veterans, and are listed in the order in which they were published. The text is largely derived from the earlier National Academies reports.
1990–1991 Gulf War Veterans
As summarized under other outcomes in this chapter, Smith et al. (2002) used DoD hospitalization data (ICD-9-CM codes) from August 1991 through July 1999 to retrospectively examine associations between modeled exposure to oil-well fires and respiratory diseases, including respiratory cancers, among 405,142 active-duty service members who served in the 1990–1991 Gulf War at the time of the oil-well fires. Service members were categorized as exposed (n = 337,077) and nonexposed (n = 68,065) to oil-well fires, and no difference in the risk of malignant neoplasms of the respiratory and intrathoracic organs was found between the exposed (n = 49) and unexposed (n = 10) groups (RR = 1.10, 95%CI 0.56–2.17), adjusted for demographic and military characteristics (not specified). The relatively short observation period (8 years) was identified as a limitation of this study for assessing cancer risk, and no information on smoking was included in models of effect estimates.
Young et al. (2010) examined proportional cancer incidence among all 621,902 U.S. veterans deployed to the Gulf War and 746,248 era veterans. Era veterans were a stratified random sample of veterans from all services who served during the conflict but were not deployed to the Persian Gulf region. Veterans diagnosed with cancer between 1991 and 2006 were identified using data from the DMDC, which was linked to central cancer registries in 28 states and the VA Central Cancer Registry. The 28 state registries captured 84% of the U.S. population, based on the 2000 U.S. Census; cancer cases were grouped into 30 categories. Logistic regression models that controlled for age, race, and sex were used to determine whether the proportion of veterans with a diagnosed cancer differed between deployed and era veterans. Crude and adjusted proportional incidence ratios (PIRs) were calculated to determine differences by specific cancer type; adjustments were made for sex, diagnosis age, diagnosis age squared, diagnosis year, race, branch of service, unit type, and registry group. For cancer types with statistically significant adjusted PIRs, standardized incidence ratios (SIRs) were calculated. SIRs compared the Gulf War veterans and era veterans with the general population, adjusted for sex, race, and age. A total of 21,075 incident cancer diagnoses were identified—8,211 among the deployed veterans and 12,864 among the era veterans—and of these, 2,796 were identified from the VA Central Cancer Registry. Lung cancer was the only site-specific cancer examined that was found to have a significantly higher proportion among deployed veterans than among era veterans (PIR = 1.15, 95%CI 1.03–1.29). It remained statistically significant when further analysis compared the proportional incidence of lung cancer in Army and Marine (ground troop) veterans with era veterans (PIR = 1.21, 95%CI 1.07–1.38). SIRs comparing deployed and era veterans with the general U.S. population were also calculated. Neither deployed nor era veterans showed significantly increased risks of lung cancer compared with the general population. Three additional respiratory cancer outcomes were also examined; none yielded statistically significant outcomes for either the comparison between all Gulf War veterans and era veterans or for that between Gulf War ground troop veterans and era veterans. For “oral cavity and pharynx” cancer, the adjusted PIRs were 0.97 (95%CI 0.83–1.13) and 0.98 (95%CI 0.81–1.17), respectively; for esophageal cancer they were 0.85 (95%CI 0.63–1.15) and 0.82 (95%CI 0.57–1.18), respectively; and for “other respiratory system” cancers they were 1.01 (95%CI 0.78–1.30) and 1.07 (95%CI 0.79–1.45, respectively). The investigators adjusted for some demographic, diagnostic, and military factors, but no data on smoking status were available so this factor was not included in the adjusted models.
The length of follow-up was, at most, 15 years, which may not be enough time for certain cancers, such as lung cancer, to develop if there was a Gulf War etiologic factor. Additionally, the numbers of incident cancer diagnoses are likely to be underestimated because 22 states were not represented, which may alter the PIR as it is affected by the relative frequencies of other cancer types. Also, of the 28 state cancer registries that were included, not all covered the full time period. Major strengths of the study are that it used the entire population of deployed Gulf War veterans and a large and representative sample of era veterans and that it used cancer registry data—as opposed to mortality, hospitalization, or self-reported diagnoses—to assess cancer incidence outcomes. The sample size was large enough to provide adequate statistical power to detect relatively small differences in lung cancer between veteran groups and between each veteran cohort and the general U.S. population. However, data on smoking were not available, and the analyses could thus not be adjusted for this potential confounder.
Other 1990–1991 Gulf War Coalition Forces Veterans
As part of the Australian Gulf War Veterans’ Follow Up Health Study, cancer incidence rates were examined through 2008 in the entire cohort of 1,871 Australian Gulf War veterans and a comparison group of 2,922 veterans who were frequency matched based on age, sex, rank category, and service branch (Sim et al., 2015). Incident cancers were identified and linked to the cohort using the Australian Cancer Database. Its data include the date of cancer diagnosis, site, histology, the Australian state in which the cancer was diagnosed, date of death (if applicable), and the ICD-10 codes for the type of cancer. Hazard ratios (HRs) were used to make comparisons between the two veteran groups, and standardized incidence ratios were used to make comparisons between each veteran group and the Australian population. Because women veterans composed only 2% of the Australian deployed cohort and no deployed women developed cancer in the 18-year follow-up, women were excluded from the cancer incidence analyses. There were fewer than five lung, trachea, and bronchus cancers in both the Gulf War veterans and the comparison group. The calculated standardized incidence rate was 4.2 (95%CI 0.06–3.00) in the veterans cohort and 5.2 (95%CI 0.13–2.07) in the comparison group. While the study adjusted for some factors, such as age, service branch, and rank, it did not adjust for other important potential confounders, such as smoking, BMI, and alcohol use.
Macfarlane et al. (2003) assessed all first diagnoses of malignant cancer using the UK National Health Service Central Register in UK service member and veterans. The deployed group consisted of all military personnel who served in the Persian Gulf in the period September 1990–June 1991 (n = 51,721). The comparison group was randomly selected from members of the armed services who were in service on January 1, 1991, but not deployed in the Persian Gulf and was stratified to match the deployed cohort on age, sex, service branch, rank, and level of fitness for active service (n = 50,755). Follow-up was from April 1, 1991, until a diagnosis of cancer, emigration, death, or July 31, 2002, whichever came first. The IRR for bronchus, lung, and trachea cancer was 0.41 (95%CI 0.10–1.73) after adjusting for sex, age, service branch, rank, smoking, and alcohol consumption. This result was based on a very small number of cases—three in the deployed cohort and five in the comparison group—which raises concerns about its reliability.
The Canadian Department of National Defence used the national mortality database and the national cancer registry to examine mortality rates and cancer incidence among Canadian Gulf War veterans from 1991 through 1999 (Statistics Canada, 2005). Two cohorts were established—the deployed cohort of 5,117 service members who served in the Persian Gulf between August 24, 1990, and September 30, 1991, and the nondeployed cohort of 6,093 service members who were eligible for deployment but who were not deployed. During the follow-up period, three deaths from respiratory cancers were identified in the deployed cohort and “a number less than 3” in the nondeployed cohort. The incidence density ratio was 2.36 (95%CI 0.39–14.2), adjusted for age and sex. In addition to the small sample size (and therefore low statistical power to detect associations if they exist), the limitations of this study include the relatively short follow-up (which would not allow the identification of long-term effects of deployment) and the lack of information on potential confounding factors, such as smoking and other lifestyle factors.
Post-9/11 Veterans
The committee responsible for the 2017 National Academies report Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry carried out an analysis of the initial months of data gathered
from respondents to the registry’s questionnaire (NASEM, 2017). The data were derived from the first 13 months of completed questionnaires (n = 46,404), representing approximately 1.0% of the 1990–1991 Gulf War veterans and 1.7% of post-9/11 veterans who met the registry’s eligibility criteria. While data were collected on self-reported esophageal and lung cancer, the committee determined that these were unlikely to be informative because the questions were too general, insufficient time had elapsed since the exposures for effects to manifest, and the population was too young for most cancers to have developed; for these reasons the committee did not analyze them.
Update of the Scientific Literature on Respiratory Cancers
The committee identified nine studies (Díaz Santana et al., 2017; Dursa et al., 2016a,b; Hooper et al., 2008; Khalil et al., 2018; Rohrbeck et al., 2016; Smith et al., 2006, 2008; Zundel et al., 2019) that addressed cancer outcomes in theater veterans that had not previously been summarized in earlier National Academies reports. However, only two specifically presented data for respiratory cancers (Khalil et al., 2018; Rohrbeck et al., 2016). Studies that only report on cancers or malignant neoplasms as a group without distinguishing respiratory cancers do not contribute to informing the evidence base on the association between deployment to Southwest Asia and respiratory-specific outcomes, including cancer. The studies that examined mortality from respiratory cancers are summarized under the Mortality section.
Post-9/11 Veterans
Rohrbeck et al. (2016) conducted a limited cohort study that compared U.S. service members deployed to Iraq (2006–2008, n = 163) and Afghanistan (2011–2012, n = 37) with matched nondeployed service members (n = 200) to examine the association between exposure to burn pits and the occurrence of ICD-coded respiratory outcomes, including neoplasms of the oral cavity and neoplasms of the respiratory organs, after return from deployment. Service members were recruited using data from the Defense Medical Surveillance System. Data from medical encounters in military treatment facilities, both hospitalizations and outpatient visits, were used to capture information on neoplasms; however, no encounters for these outcomes were observed.
1990–1991 Gulf War Veterans
Khalil et al. (2018) described the study design for the Gulf War Era Cohort and Biorepository and provided preliminary results from the pilot phase of the effort, which had enrolled 1,275 veterans, 900 of whom had deployed to Southwest Asia. Self-reported health outcomes of symptoms (in the past year) and health care provider–diagnosed conditions were reported, stratified by users (n = 584) and nonusers (n = 679) of VA health care in the past year. A supplemental table for the paper that was posted to the web notes that none of the 1,256 subjects who responded to the survey question indicated that a doctor or other health care provider had ever told them that they had lung cancer. As the study participants consented to further contact and analyses of the data and biospecimens they provided, this cohort may be useful in future studies of respiratory cancer and other outcomes.
Synthesis
The only studies of respiratory cancer outcomes in theater veterans that have been published to date address the military personnel who participated in the 1990–1991 Gulf War. As is true for all the outcomes reviewed by the committee, the studies are plagued by poor exposure characterization, with self-reports or location information being used as proxies for measured exposure levels. Several report such a small number of respiratory cancer outcomes that the risk estimates have large confidence intervals. Some, although not all, fail to account for potential confounding by cigarette smoking—the most important risk factor for lung cancer. And the earlier studies summarized by previous National Academies committees note that cancers associated with environmental exposures may have long latency periods and that too little time may have passed since in-theater exposures to see their effects. As a consequence, no conclusions can be drawn from this body of literature.
Smith et al. (2008), who performed an analysis of data obtained as part of the Millennium Cohort Study, found that military deployment was associated with smoking initiation among never smokers and with smoking resumption among those who had stopped. This finding, among others, led Krefft et al. (2015) to argue that tobacco smoking should be considered a deployment-related exposure that contributes to lung cancer risk. There is no question that cigarette smoking is an important risk factor for a number of cancers of interest. However, lacking sufficiently representative data on either the quantitative excess of smoking associated with deployment or its continuation post-deployment, the attributable risk associated with this change in smoking behavior cannot be estimated.
Conclusions
Based on the epidemiologic studies of military personnel and veterans reviewed in this and previous National Academies reports, the committee concludes that there is inadequate or insufficient evidence of an association between airborne hazards exposures in the Southwest Asia theater and the subsequent development of respiratory cancers. While data exist on 1990–1991 Gulf War veterans, the committee notes that no studies have been published concerning those who participated in the post-9/11 conflicts and that—even if such studies were available—the amount of time since exposure may only now be long enough to justify new incidence studies of respiratory cancers in this cohort.
MORTALITY
The committee’s Statement of Task directed it to pay particular attention to excess mortality in military personnel who served in the Southwest Asia theater. This section evaluates the results of epidemiologic studies of overall mortality and, where the information is available, respiratory disease–related causes of death among service members and veterans in the 1990–1991 Gulf War and post-9/1114 cohorts.
The section begins with a brief summary of the mortality studies evaluated in previous Gulf War and Health volumes, with an emphasis on findings regarding mortality from respiratory disease–related causes and the conclusions those committees drew from that evidence. Next, a description of each of the newly identified studies of mortality is presented along with each study’s salient results. Studies of overall mortality, of cancers of the respiratory system, and of non-cancerous respiratory conditions are considered separately.
Summary of Epidemiologic Studies Reviewed in Previous Gulf War and Health and Related Reports
Periodically throughout the Gulf War and Health series, committees have examined mortality overall and, when possible, by cause (Volumes 4, 8, and 10). Through Volume 10, 19 studies of mortality among 1990–1991 Gulf War veterans have been reviewed and assessed (Barth et al., 2009; Bossarte, 2014; Bullman et al., 2005; DASA, 2005, 2009; Gackstetter et al., 2006; Gray et al., 2000; Haley, 2003; Kang and Bullman, 1996, 2001; Knapik et al., 2009; Lincoln et al., 2006; Macfarlane et al., 2000, 2005; Shaw et al., 1991; Sim et al., 2015; Statistics Canada, 2005; UK Ministry of Defence, 2014; Zwerling et al., 2000). These studies examined mortality for veterans from Australia, Canada, the United Kingdom, and the United States who were deployed to Iraq or in the surrounding theater of operations in support of Operation Desert Shield or Operation Desert Storm. Some of these veterans may also have been deployed in the post-9/11 conflicts, but they were selected for inclusion in the study cohorts based on their 1990–1991 Gulf War service. Some studies examined overall mortality or specific causes that did not include respiratory diseases (e.g., Barth et al. [2009], which examined mortality from neurologic conditions only). Most comparisons were made between the deployed Gulf War veterans and nondeployed era veterans, although some studies were able to make comparisons between deployed veterans who were exposed and those who were nonexposed to a particular agent (such as nerve agents at Khamisiyah). In general, the popula-
___________________
14 The primary post-9/11 U.S. military operations in the Southwest Asia theater were Operation Enduring Freedom (OEF), Operation Iraqi Freedom (OIF), and Operation New Dawn (OND).
tions examined in the Australian, Canadian, and UK studies were small, reflecting the relatively limited number of personnel deployed from these countries.
Empirical analyses reviewed by prior Gulf War and Health committees that examined all disease-specific causes of mortality found either no difference (Bullman et al., 2005; DASA, 2009; Kang and Bullman, 1996; Macfarlane et al., 2000, 2005) or lower mortality rates for deployed 1990–1991 Gulf War veterans compared with nondeployed veterans, a finding consistent with studies of U.S. (Bossarte, 2014), UK (UK Ministry of Defense, 2014), and Australian (Sim et al., 2015) veterans. For the purposes of this report, the only relevant mortality studies were those that reported on respiratory-specific conditions (Bossarte, 2014; Bullman et al., 2005; DASA, 2009; Kang and Bullman, 1996, 2001; Macfarlane et al., 2000, 2005; Sim et al., 2015; Statistics Canada, 2005; UK Ministry of Defence, 2014).
Non-Cancerous Respiratory Conditions
Mortality from respiratory conditions in Gulf War veterans has been examined in veterans from Canada (Statistics Canada, 2005), the United Kingdom (DASA, 2009; Macfarlane et al., 2000, 2005; UK Ministry of Defence, 2014), and the United States (Bossarte, 2014; Bullman et al., 2005; Kang and Bullman, 1996, 2001). None of these studies adjusted for smoking status.
The first mortality study of U.S. 1990–1991 Gulf War veterans covered 1991–1993 and included the entire deployed cohort (n = 695,515) and a nondeployed era cohort (n = 746,291). The study found an elevated difference in respiratory system disease mortality that included the null (mortality rate ratio [MRR] = 1.27, 95%CI 0.60–2.70) (Kang and Bullman, 1996). However, when compared with the U.S. population, both Gulf War veterans (SMR = 0.14, 95%CI 0.07–0.23) and era veterans (SMR = 0.11, 95%CI 0.06–0.18) had a statistically significantly lower risk of death due to respiratory illness. An updated mortality study of the same cohort through December 31, 1997 (Kang and Bullman, 2001), found no statistically significant differences between the deployed and nondeployed veteran groups, stratified by sex, for respiratory mortality; both deployed and nondeployed veterans had statistically significant lower respiratory mortality than the general U.S. population.
In a study of cause-specific mortality through December 31, 2000, of deployed U.S. veterans considered to be exposed or not exposed to nerve agents released from the destruction of the Khamisiyah munitions storage facility in 1991, no increase in mortality due to respiratory conditions was seen in the putatively exposed veterans (RR = 1.03, 95%CI 0.62–1.72; adjusted for age) (Bullman et al., 2005). Similarly, no difference in risk for respiratory disease mortality was observed when the investigators divided the exposed group into persons exposed for 1 day only or for 2 days compared with people who were not exposed (exposure based on the 2000 plume model), adjusted for age, race, sex, rank, and unit component. VA’s presentation to the Volume 10 committee (Bossarte, 2014) included mortality rates for respiratory conditions for both deployed and nondeployed Gulf War veterans over a 20-year period (1991–2011). No statistically significant differences were found between the two groups (MRR = 0.96, 95%CI 0.86–1.06) adjusted for race, sex, age, branch of service, and unit component.
Other 1990–1991 Gulf War Coalition Forces Veterans
In the first UK study to assess mortality, conducted through March 31, 1999, Macfarlane et al. (2000) found no excess deaths due to conditions of the respiratory system in either deployed or nondeployed veterans after adjusting for age only (MRR = 1.0, 95%CI 0.13–7.47). An update of the same cohort through 2004 (Macfarlane et al., 2005) also found no statistically significant excess of deaths related to respiratory disease (MRR = 1.64, 95%CI 0.58–4.66), after adjusting for age only. In the analysis conducted by the Defence Analytical Services and Advice, 13 deaths due to respiratory diseases were reported among deployed UK veterans and 12 deaths among comparable age-adjusted era veterans, resulting in no difference for age-adjusted mortality (MRR = 1.06, 95%CI 0.47–2.39). An update of that analysis conducted by the UK Ministry of Defence (2014), again found few deaths due to respiratory diseases (34 of 1,506 total deaths among the deployed veterans and 36 [adjusted] of 1,583 total deaths among the nondeployed veterans), and the difference remained not statistically significant (MRR = 0.93, 95%CI 0.58–1.49; adjusted for age). Specific types of respiratory system conditions were not presented for either UK analysis. Standardized mortality ratios for respiratory diseases comparing deployed and nondeployed veterans with the age- and gender-adjusted UK population were not calculated.
Statistics Canada (2005) conducted a mortality follow-up study of Canadian Gulf War veterans and compared them with randomly selected Canadian veterans who were eligible but not deployed to the Gulf War and to the general Canadian population. There were too few deaths from respiratory disease to make meaningful comparisons between the veteran cohorts and the general population, and smoking status was not available.
Given that, in the mortality studies reviewed, few deaths due to respiratory causes were reported and no statistically significant excess of mortality due to respiratory disease was found among Gulf War veterans compared with nondeployed era veterans or the general, country-specific population, the Volume 10 committee concluded that there was limited or suggestive evidence of no association between deployment to the Gulf War and mortality from respiratory disease. Notably, in all these studies of 1990–1991 Gulf War veterans, the populations are relatively young, and a large number of deaths from chronic respiratory diseases would not be expected.
Cancers
Studies that assessed mortality from all types of cancers in previous Gulf War and Health volumes did not find an increased risk in deployed versus nondeployed veterans (Barth et al., 2009; Bullman et al., 2005; DASA, 2009; Kang and Bullman, 2001; Macfarlane et al., 2000, 2003, 2005; Sim et al., 2015; Statistics Canada, 2005; UK Ministry of Defence, 2014). Given the maximum follow-up period of about 10 years for most of these studies, prior committees concluded that, in general, many veterans were still too young to have developed the most common forms of cancer and that, for most cancers, the follow-up period after the Gulf War was probably too short to expect the onset of any exposure-related cancers, let alone death from such cancers. Smoking status was not available or included in any of these studies of cancer mortality.
In a study of cause-specific mortality through December 31, 2000, of deployed U.S. veterans considered to be exposed or not exposed to nerve agents as a result of the Khamisiyah munitions destruction in 1991, no increase in mortality due to lung cancer was observed in the exposed veterans overall (RR = 0.72, 95%CI 0.47–1.10) when adjusted for age, race, sex, rank, and unit component or when stratified by days of exposure (1 day or 2 or more days), compared with the nonexposed (Bullman et al., 2005). The Volume 10 committee considered a presentation of an original data analysis from VA to the committee that included mortality rates for all cancers and, specifically, for lung cancer over a 20-year period (1991–2011) (Bossarte, 2014), but it was given less weight than the published epidemiologic studies. No statistically significant difference was observed between the deployed and nondeployed veterans with regard to death from any cancer (MRR = 0.99, 95%CI 0.95–1.03) when adjusted for race, sex, age, branch of service, and unit component). Mortality rates for lung cancer were calculated for each veteran group but were only compared with the general U.S. population, not to each other. The lung cancer mortality rates for both deployed and nondeployed veterans were statistically significantly lower than those for the general U.S. population (SMR deployed = 0.60, 95%CI 0.57–0.64; SMR nondeployed = 0.59, 95%CI 0.56–0.62).
Other 1990–1991 Gulf War Coalition Forces Veterans
The UK statistical report (DASA, 2009), which had a follow-up period of 16 years, found no difference in the number of malignant neoplasms of respiratory and intrathoracic organs in deployed versus nondeployed UK Gulf War veterans (MRR = 0.75, 95%CI 0.48–1.18). A subset of that category—malignant neoplasms of the bronchus and lung, which formed a majority of the malignant respiratory neoplasms—similarly exhibited no differences between deployed and era veterans (MRR = 0.71, 95%CI 0.45–1.13). An updated analysis of this cohort (UK Ministry of Defence, 2014) included an additional 6 years of follow-up. Between April 1, 1991, and December 31, 2013 (approximately 22 years), 404 neoplasm deaths out of 911 disease-related deaths were reported among deployed veterans and 455 (adjusted) neoplasm deaths out of 1,035 disease-related deaths in nondeployed veterans (MRR = 0.89, 95%CI 0.78–1.02; adjusted for age). Site-specific malignant neoplasm deaths were reported for respiratory and intrathoracic organs (54 vs 87 [adjusted] in deployed and era veterans, respectively); bronchus and lung cancers were reported as a subset of these. Lung cancer mortality was statistically significantly lower for deployed Gulf War veterans (n = 49) compared with nondeployed veterans (n = 82, adjusted) (MRR = 0.60, 95%CI 0.42–0.85) after adjustment for age. The nondeployed comparison group was similar to the deployed group in age, gender, service, regular/reservist status, and rank. Standardized mortality
ratios for respiratory cancers comparing deployed and nondeployed veterans with the age- and gender-adjusted UK population were not calculated.
Whereas the Volume 8 committee did not reach any conclusions regarding the association between deployment to the Gulf War and mortality from any cancer, the Volume 10 committee concluded that there was insufficient or inadequate evidence of an association between deployment to the Gulf War and mortality from any form of cancer. No conclusions were made for specific cancers, such as lung cancer.
Update of the Scientific Literature on Mortality
Eight studies of mortality that had not been previously summarized in the Gulf War and Health series were identified by the committee in its literature search (Barth et al., 2016b; Belenkiy et al., 2014; Bollinger et al., 2015; Gray and Kang, 2006; Hooper et al., 2010; Maynard et al., 2018a,b; Shorr et al., 2004). Some of these studies were conducted in post-9/11 populations (Belenkiy et al., 2014; Bollinger et al., 2015; Hooper et al., 2010; Shorr et al., 2004), which were considered to be outside the population of interest in some of these earlier reports. Of the eight studies, six were excluded from further consideration because one was a review that did not offer any new or original information (Gray and Kang, 2006), one was a case series of AEP that included deaths but was not designed to assess population-level mortality (Shorr et al., 2004), one assessed mortality related to trauma rather than to disease (Belenkiy et al., 2014), two publications by Maynard et al. (2018a,b) examined the association between disability rating for veterans with service-connected conditions and either cause of death or 1-year mortality rates, and Hooper et al. (2010) conducted a mortality analysis using the participants of Panel 1 of the Millennium Cohort Study and different sources of death data to compare the all-cause mortality experience. Bollinger et al. (2015) is summarized for completeness, but it reported on overall deaths, not on deaths from respiratory conditions or other conditions.
Using the same population of 621,901 Gulf War–deployed veterans and 746,247 nondeployed veterans originally studied by Kang and Bullman (2001) and summarized in Volume 4, Barth et al. (2016b) continued their mortality follow-up of all causes and disease-specific causes through 2004. The total follow-up period was 13 years, and several comparisons were made: deployed Gulf War veterans who were potentially exposed to nerve agents at Khamisiyah versus those who were not; deployed Gulf War veterans versus nondeployed era veterans; and deployed and nondeployed veterans versus the standardized U.S. population. To be eligible for inclusion, Gulf War–deployed veterans must have served in the Persian Gulf between August 1, 1990, and March 1, 1991; troops that arrived in the region after March 1, 1991, were excluded. Vital status was determined using VA’s Beneficiary Identification and Records Locator Subsystem in combination with the Social Security Administration Death Master File. Cause of death data were determined from death certificates in VA claim files or from the National Death Index Plus, which is part of the National Center for Health Statistics. Deaths were coded using ICD-9 codes. Data on demographics and military characteristics were from DoD’s DMDC. Over the 13-year period, 10,869 deaths among deployed Gulf War veterans and 14,716 deaths among nondeployed era veterans were reported. Adjusted RRs were presented that were derived from a Cox proportional hazard model after controlling for age, race, sex, service branch, type of unit, and length of follow-up. Smoking status was not ascertained or included in the models. Although both estimates were statistically significant, a slightly lower rate of death from all causes was found for deployed versus nondeployed males (RR = 0.94, 95%CI 0.95–0.99) and a slightly higher rate of death was found for deployed versus nondeployed females (RR = 1.15, 95%CI 1.03–1.28). When mortality from all disease-related causes was examined, the adjusted RR was statistically significantly lower for deployed versus nondeployed males (RR = 0.93, 95%CI 0.90–0.97), and the difference for deployed versus nondeployed females was higher but did not reach statistical significance (RR = 1.10, 95%CI 0.96–1.27). The data on cause of death were missing for 770 (7.1%) deceased Gulf War veterans and for 1,090 (7.4%) deceased era veterans. With respect to deaths from respiratory system disorders (ICD-9 460–519), which do not include cancers, there were 192 deaths in the deployed veterans (180 males and 12 females) and 318 deaths in the nondeployed veterans (291 males and 27 females). No statistically significant differences were found for deployed versus nondeployed males (RR = 0.95, 95%CI 0.78–1.15) or females (RR = 1.07, 95%CI 0.54–2.11). Comparisons with the U.S. population were presented for respiratory system disorders, stratified by
sex and age adjusted. SMRs comparing deployed veterans to this population showed that deaths from respiratory system disorders were statistically significantly lower for deployed veterans overall (SMR = 0.30, 95%CI 0.26–0.34) and for both males (SMR = 0.30, 95%CI 0.25–0.34) and females (SMR = 0.33, 95%CI 0.17–0.57), separately. Similar findings of a statistically significantly lower risk of death from respiratory system disorders were found among the nondeployed veterans compared with the U.S. population for both males (SMR = 0.32, 95%CI 0.28–0.35) and females (SMR = 0.30, 95%CI 0.20–0.44). The deficits in mortality rates compared with the general U.S. population support the “healthy soldier effect.”
Mortality risks and adjusted RRs (derived from a Cox proportional hazards model after controlling for sex, race, type of unit, age, and oil-well fire smoke exposure) for lung cancer and non-cancer respiratory system conditions, and for COPD (ICD-9 490–492, 494, 496) specifically, were also estimated for the subset of the deployed population who were exposed to nerve agents from the Khamisiyah demolition for 1 day or ≥2 days compared with nonexposed deployed veterans. Exposure at Khamisiyah was based on the 2000 plume model from Winkenwerder (2002), the limitations of which have been discussed in other reports. Among those exposed to nerve agents from Khamisiyah, 58 deaths from lung cancer occurred among the 1-day-exposed group, 10 deaths in the ≥2 days-exposed group, and 163 in the nonexposed deployed group. Compared with the nonexposed deployed, adjusted RRs were not statistically significant for the 1-day exposed (RR = 0.78, 95%CI 0.57–1.06) or the ≥2 days exposed (RR = 0.78, 95%CI 0.39–1.53). For non-cancer respiratory system conditions, there were 32 deaths among 1-day exposed, 7 deaths among the ≥2 days exposed, and 77 deaths among the nonexposed deployed veterans. Similar to the case with lung cancer, the adjusted RRs for non-cancer respiratory system conditions showed no statistically significant differences between 1-day exposed (RR = 1.00, 95%CI 0.65–1.55) or the ≥2 days exposed (RR = 1.60, 95%CI 0.73–3.55) and the nonexposed deployed veterans. For COPD there were 11, 3, and 21 deaths, respectively, in the 1-day exposed, ≥2 days exposed, and nonexposed deployed veterans. Comparisons with the nonexposed deployed veterans showed no statistically significant differences for COPD for 1-day exposed (RR = 1.23, 95%CI 0.57–2.65) or the ≥2 days exposed (RR = 2.45, 95%CI 0.69–8.76) veterans. Although there appears to be an exposure–response effect, the point estimates are imprecise because the number of events is small.
Bollinger et al. (2015) evaluated mortality rates for post-9/11 veterans using several different comparison populations—the general U.S. population; enrollees in the VA health care system, users of VA health care, and nonusers of VA health care15; and an active-duty military cohort (which included activated National Guard and Reserve members)—to determine whether the “healthy soldier effect” and “healthy warrior survivor effect” contributed to different rates of mortality. The intention was to determine whether the mortality experience of post-9/11 veterans differed from that of previous veteran cohorts by examining the ways in which the healthy soldier effect operates in VA enrollees and DoD active duty service members compared with the U.S. population. Data sources were the VA OEF/OIF/OND Roster file, VA “mini” vital status file of mortality data, and DoD’s DMDC Reporting System. For inclusion in the VA cohort, individuals had to have contact with the VA health care system at least once between October 2001 and September 30, 2011 (most veterans do complete an initial assessment check-in); individuals were excluded if their ages were missing or their deaths were combat related. The final VA cohort was 899,737 individuals consisting of 765,029 (85%) veterans who had used VA health care and 134,708 (15%) veterans who did not use VA health care in the 10-year period. The DoD active-duty military cohort consisted of persons deployed in support of OEF/OIF/OND from January 2002 through December 2011 (n = 4,619,178); deaths that were combat related were excluded. Mortality rates for the U.S. population were calculated using 2002–2010 data from the Centers for Disease Control and Prevention (CDC) Wonder system that was sex, age, and race/ethnicity adjusted for people aged 18–72 years. The total numbers of included deaths were 4,055 for VA health care users, 193 for non-VA health care users, 10,390 for the DoD active-duty cohort, and 7,890,897 for the U.S. population. Standardized mortality ratios using indirect standardization were calculated to control for the different age structures of VA, DoD, and U.S. populations. Mortality rates were standardized to U.S. age-, race-, and sex-specific mortality and applied to the age structure of VA and DoD populations to get an expected number of deaths. These rates standardized to DoD age-, rank-, component-, and branch-specific
___________________
15 VA health system enrollees, VA health care users, and non-VA health care users were broken out because these groups have different demographic characteristics that influence mortality.
mortality were applied to VA cohorts’ age, rank, component, and branch structure to get an expected number of deaths in order to evaluate whether mortality differences between VA and DoD cohorts were due to military-specific characteristics. Smoking status was not available. SMRs cannot be compared across populations with different age distributions, so Bollinger et al. (2015) estimated a directly standardized relative risk (DSRR) using the standardized mortality rate and the population standard for each age group to allow for comparisons between groups. The DoD population was statistically significantly younger than the VA cohorts of health care users and nonusers (34.2 years vs 34.4 years and 33.1 years, respectively). Compared with the U.S. population, VA health care users had a statistically significantly higher risk of all-cause mortality (SMR = 3.15, 95%CI 3.1–3.25; DSRR = 2.86), as did the DoD active-duty cohort (SMR = 1.47, 95%CI 1.44–1.49; DSRR = 1.19), but there was no difference for nonusers of VA health care (SMR = 0.92, 95%CI 0.79–1.05; DSRR = 0.79). When the VA cohort was compared with the DoD cohort, VA health care users had a statistically significantly increased risk of all-cause mortality (SMR = 2.34, 95%CI 2.26–2.41; DSRR = 2.28), but nonusers of VA health care had a statistically significantly decreased risk of all-cause mortality (SMR = 0.63, 95%CI 0.55–0.72; DSRR = 0.62). The results of these analyses suggest that overall OEF/OIF/OND veterans who use VA have higher-than-expected mortality compared with the general U.S. population. When the results were stratified by demographic characteristics, the SMRs and DSRRs were similar for males and females in VA and DoD cohorts. The SMRs varied by race and age groups for VA and DoD populations. Mortality ratios were highest in the youngest veterans (<24 years); SMR = 5.29, 1.43, and 2.47 for VA users, VA nonusers, and DoD cohort, respectively, compared with the U.S. population. Mortality rates were lowest in the oldest veterans (40–72 years), SMR = 1.37, 0.38, and 0.38, respectively, compared with the U.S. population. When VA users were stratified by race, SMRs were 3.75, 3.13, and 1.64 for white non-Hispanic, Hispanic, and black non-Hispanic, respectively. By contrast, in the DoD population, the SMRs for white non-Hispanic, Hispanic, and black non-Hispanic were 1.09, 1.87, and 2.33, respectively. The OEF/OIF/OND cohort of 4.6 million individuals differs from previous military cohorts in that the conflicts have continued longer than any other war or conflict and have resulted in multiple deployments and longer durations for more individuals. In addition, survival from battlefield injuries has improved, which results in higher rates of disability among this cohort of veterans.
This study is not directly relevant to the question of increased mortality from respiratory conditions associated with exposures in the OEF/OIF/OND conflicts; however, it does provide a context for evaluating mortality and potential inferences to respiratory conditions. Given the relatively short follow-up of relatively young populations (55% of the VA cohort and 59.3% of the DoD cohort were younger than 24 years), most of the deaths are likely due to causes other than chronic disease, although the cause-specific information was not presented. The SMRs were highest for the younger age groups across the two VA and the DoD cohorts. The observed lower SMRs for older veterans with longer military service is consistent with a healthy soldier survivor effect, reflecting the fact that healthier soldiers tend to have longer military service. These trends in SMRs are also consonant with patterns observed for certain occupational cohorts, such as chemical workers. The elevated SMR in the active DoD population may be a consequence of relaxed eligibility standards—higher weight, lower scores on aptitude tests, criminal and medical waivers, and lack of a high school diploma—applied to meet recruitment goals for the Afghanistan and Iraq conflicts, which would lead to service members being more comparable with the general U.S. population. An alternate explanation may be that these military personnel faced serious non-combat-related health hazards during deployment to OEF/OIF/OND. Without being able to distinguish between these two explanations, SMRs are not interpretable as measures of excess mortality risk related to respiratory hazards in theater. Moreover, because only all-cause mortality was considered, the higher mortality rates in the youngest age group are more likely driven by external causes (e.g., motor vehicle accidents, suicide, drug overdose) than disease—particularly respiratory disease—specific causes. These findings suggest that the health advantage typically observed in military populations (the “healthy warrior effect”) is mitigated for the post-9/11 cohort.
Limitations of Mortality Studies
Military personnel deployed to Afghanistan and the Southwest Asia theater and those serving in the armed forces but not deployed to that theater may offer reasonably comparable groups for examining many health outcomes,
including death, but there are issues in the conduct and use of mortality studies that must be considered. A major limitation of the mortality studies discussed in this section is the short follow-up period. In general, more time is required for the potential contributory effects of aging on the development of putative risk of exposure resulting in death before investigators will be able to assess whether deployed veterans are experiencing increased mortality compared with their nondeployed counterparts, particularly for conditions with established risk factors and long latencies, such as cancer, or conditions that have deteriorating and protracted courses, such as chronic respiratory diseases.
Most of the mortality studies discussed here relied on data from the National Death Index. Although the information in these indexes is taken from death certificates, which are completed by different types of health professionals with varying levels of expertise in assessing cause of death, there are stringent requirements and rules that likely minimize misclassification. Misclassification of the cause of death is more likely when the cause is more specific (e.g., all-cause deaths versus deaths from COPD). Large sample sizes can compensate for bias toward the null caused by nondifferential misclassification. The most reliable cause of death information is typically provided by medical examiners and physician providers; those records are less likely to have nondifferential misclassification bias, especially for causes of death that may have links to specific exposures or require knowledge of underlying pathology (IOM, 2003b). Furthermore, knowledge of or review of the decedent’s medical and exposure history is known to improve the accuracy of death certificate data.
Finally, few studies have been published with enough power to assess cause-specific mortality rates among deployed and nondeployed Gulf War veterans from the United States or any coalition country (e.g., Australia, Canada, United Kingdom). In addition to large cohort studies comparing deployed and nondeployed veterans, nested case–control studies among the deployed may yield efficient and more suitable comparisons between deceased or “sick” veterans (cases) and “non-sick” veterans (controls). Another factor to consider is competing risks of death, which is especially problematic when the competing causes of death are not independent of each other (such as when they are both associated with the exposure, as in the case of silicosis and lung cancer in a mortality study of silica exposure). Completeness of follow-up information is also an important consideration between veterans who use VA medical care and those who do not. For example, veterans using VA medical care are likely to be more easily traced and to have more available information on underlying medical conditions and behaviors, such as smoking.
Synthesis
Based on the mortality studies of 1990–1991 Gulf War veterans summarized previously in Gulf War and Health Volumes 4, 8, and 10 and the one new study of deaths from non-cancer respiratory conditions in post-9/11 veterans over 10 years of follow-up (Barth et al., 2016b), the committee found no statistically significant excess of mortality due to respiratory disease among either the post-9/11 or Gulf War veteran cohorts. There do not appear to be differences in mortality between deployed and nondeployed veterans for the studies that looked at short-term follow-up (up to 13 years for 1990–1991 Gulf War veterans), but whether there are longer-term mortality differences is uncertain. Given the decades that have passed since the last mortality study of 1990–1991 Gulf War veterans was conducted, the committee does not believe continued confidence in those finding is warranted. The inferences possible from future studies of mortality would be improved by using internal analyses that compare higher- and lower-exposed veterans (assuming adequate exposure assessment measures) rather than analyses comparing all veterans to the general population. For mortality studies of 1990–1991 Gulf War or post-9/11 veterans, this requires that a retrospective exposure assessment be conducted as a necessary component of any future mortality study if it is to produce useful unbiased estimates of mortality risk. Taken altogether, the existing literature supports the need to examine effect modification of respiratory outcomes associated with burn pit and other exposures by education, income, race, and other measures of socioeconomic status in future studies of veterans and service members. To be informative, future studies of service members and veterans should ascertain smoking habits and adjust for them.
Conclusions
The current committee concurs with previous committees and concludes that there is inadequate or insufficient evidence of an association between deployment to the Southwest Asia theater during the 1990–1991 Gulf War and subsequent mortality from respiratory disease. The committee further concludes that there is inadequate or insufficient evidence of an association between deployment to the post-9/11 conflicts and subsequent mortality from respiratory disease; it notes that no studies of mortality have separated respiratory disease from other causes. Chapter 5 notes that data are readily available to fill the knowledge gaps identified in the existing mortality literature and offers a recommendation on future research that would address them.
FINAL OBSERVATIONS
In the course of its review, the committee assessed more than 55 epidemiologic studies that met its inclusion criteria, which included that the study address a respiratory health outcome in service members who were deployed to Southwest Asia, examine outcomes with relation to a comparison group, and present an empirical analysis of the data rather than simply list descriptive statistics. The committee also considered the results of previous evaluations of respiratory outcomes contained in the National Academies Gulf War and Health series and other related reports that examined epidemiologic evidence in military and veteran populations, and exposure to burn pits specifically.
Although most of the committee’s conclusions fall under the category of “inadequate or insufficient evidence to determine an association,” it wishes to emphasize that this should not be interpreted as meaning that there is no association between respiratory health outcomes and deployment to Southwest Asia, but rather that the available data are, on the whole, of insufficient quality to make a scientific determination. Notably, most of the studies reviewed by the committee did not perform objective exposure assessment, and the majority relied on deployment as a surrogate for exposure. As noted several times throughout this report, many studies make the implicit assumption that all deployed veterans had the same exposures to airborne hazards, which likely leads to bias of the effect estimate toward the null due to nondifferential exposure misclassification. More plainly stated, if an epidemiologic study of an adverse exposure combines data from subjects with high exposure together with data from subjects with low or no exposure, any effect of that exposure will be diluted.
Given these limitations in the current body of literature, the committee concludes that a new approach is needed that will allow researchers to better examine and answer the question of whether certain respiratory outcomes are associated with deployment to Southwest Asia. This new approach is not one that is intended to reprise a common theme in academia of “more research is needed” or to suggest that the only alternative is to undertake work that will take many years to bear fruit. While new data collection may be necessary in some circumstances, well conducted epidemiologic studies are possible today using retrospective designs that are able to account for confounding factors, such as smoking habits; to combine and analyze existing data in innovative ways; to standardize outcome ascertainment methods to allow for better comparability of results; and to improve estimation of exposure.16
The report’s next chapter (Chapter 5) offers a number of suggestions for how to move forward. It identifies data sources, potential methods, and collaborating organizations that could be used to leverage available exposure and health outcomes information to address the question of the impact of deployment to Southwest Asia on respiratory health.
REFERENCES
Abraham, J. H., and C. P. Baird. 2012. A case-crossover study of ambient particulate matter and cardiovascular and respiratory medical encounters among U.S. military personnel deployed to Southwest Asia. Journal of Occupational and Environment Medicine 54(6):733–739.
Abraham, J. H., S. F. DeBakey, L. Reid, J. Zhou, and C. P. Baird. 2012. Does deployment to Iraq and Afghanistan affect respiratory health of US military personnel? Journal of Occupational and Environmental Medicine 54(6):740–745.
___________________
16 For example, American Thoracic Society/European Respiratory Society consensus statement on standardizing endpoints for clinical asthma trials and clinical practice (Reddel et al., 2009).
Abraham, J. H., A. Eick-Cost, L. L. Clark, Z. Hu, C. P. Baird, R. DeFraites, S. K. Tobler, E. E. Richards, J. M. Sharkey, R. J. Lipnick, and S. L. Ludwig. 2014. A retrospective cohort study of military deployment and postdeployment medical encounters for respiratory condition. Military Medicine 176(5):540–546.
AFHSC (Armed Forces Health Surveillance Center), the Naval Health Research Center, and the U.S. Army Public Health Command. 2010. Epidemiological studies of health outcomes among troops deployed to burn pit sites. Silver Spring, MD: Defense Technical Information Center.
Aoun, O., C. Roqueplo, and C. Rapp. 2014. Spectrum and impact of health problems during deployment: A prospective, multicenter study of French soldiers operating in Afghanistan, Lebanon and Côte d’Ivoire. Travel Medicine and Infectious Disease 12(4):378–384.
APHC (Army Public Health Command). 2010. Screening health risk assessments, Joint Base Balad, Iraq, 11 May–19 June 2009. Aberdeen Proving Ground, MD: Army Public Health Command. July.
ATS and ERS (American Thoracic Society and European Respiratory Society). 2002. American Thoracic Society/European Respiratory Society international multidisciplinary consensus classification of the idiopathic interstitial pneumonias. American Journal of Respiratory Critical Care Medicine 165(2):277–304.
ATS and ERS. 2013. An official American Thoracic Society/European Respiratory Society statement: Update of the international multidisciplinary classification of the idiopathic interstitial pneumonias. American Journal of Respiratory Critical Care Medicine 188:733–748.
Baird, C. P., S. DeBakey, L. Reid, V. D. Hauschild, B. Petruccelli, and J. H. Abraham. 2012. Respiratory health status of U.S. Army personnel potentially exposed to smoke from 2003 Al-Mishraq Sulfur Plant Fire. Journal of Occupational and Environment Medicine 54(6):717–723.
Banoei, M. M., I. Lupe, R. Dowlatabadi Bazaz, M. Campos, H. J. Vogel, B. W. Winston, and M. Mirsaeidi. 2019. Metabolomic and metallomic profile differences between veterans and civilians with pulmonary sarcoidosis. Scientific Reports 9:19584.
Barth, S. K., H. K. Kang, T. A. Bullman, and M. T. Wallin. 2009. Neurological mortality among U.S. Veterans of the Persian Gulf War: 13-year follow-up. American Journal of Industrial Medicine 52(9):663–670.
Barth, S. K., E. K. Dursa, M. R. Peterson, and A. Schneiderman. 2014. Prevalence of respiratory diseases among veterans of Operation Enduring Freedom and Operation Iraqi Freedom: Results from the National Health Study for a New Generation of U.S. Veterans. Military Medicine 179(3):241–245.
Barth, S. K., E. K. Dursa, R. Bossarte, and A. Schneiderman. 2016a. Lifetime prevalence of respiratory diseases and exposures among veterans of Operation Enduring Freedom and Operation Iraqi Freedom Veterans: Results from the National Health Study for a New Generation of U.S. Veterans. Journal of Occupational and Environmental Medicine 58(12):1175–1180.
Barth, S. K., H. K. Kang, and T. Bullman. 2016b. All-cause mortality among U.S. veterans of the Persian Gulf War: 13-year follow-up. Public Health Reports 131(6):822–830.
Bartoo, C. 2010. Soldiers’ mysterious lung disease identified. The Reporter (Vanderbilt University Medical Center’s Weekly Newspaper), February 12. https://www.mc.vanderbilt.edu/reporter/index.html?ID=8270 (accessed May 2, 2020).
Bascom, R., and P. Raford. Upper airway disorders. 1994. In L. Rosenstock and M. Cullen, eds., Textbook of clinical occupational and environmental medicine. Philadelphia, PA: W.B. Saunders Company. Pp. 322–326.
Belenkiy S. M., A. R. Buel, J. W. Cannon, C. R. Sine, J. K. Aden, J. L. Henderson, N. T. Liu, J. B. Lundy, E. M. Renz, A. I. Batchinsky, and L. C. Cancio. 2014. Acute respiratory distress syndrome in wartime military burns: Application of the Berlin criteria. Journal of Trauma Acute Care Surgery 76(3):821–827.
Blanc, P. D., I. Annesi-Maesano, J. R. Balmes, K. J. Cummings, D. Fishwick, D. Miedinger, N. Murgia, R. N. Naidoo, C. J. Reynolds, T. Sigsgaard, K. Toren, D. Vinnikov, and C. A. Redlich. 2019. The occupational burden of nonmalignant respiratory disease. An official American Thoracic Society and European Respiratory Society Statement. American Journal of Respiratory and Critical Care Medicine 199(11):1312–1334.
Bollinger, M. J., S. Schmidt, J. A. Pugh, H. M. Parsons, L. A. Copeland, and M. J. Pugh. 2015. Erosion of the healthy solider effect in veterans of U.S. military service in Iraq and Afghanistan. Population Health Metrics 13:8.
Bossarte, R. M. 2014. Presentation to the Institute of Medicine Committee on Gulf War: Veterans’ Health. December 3, 2014. Department of Veterans Affairs Office of Public Health, Washington, DC.
Bullman T. A., C. M. Mahan, H. K. Kang, and W. F. Page. 2005. Mortality in U.S. Army Gulf War veterans exposed to 1991 Khamisiyah chemical munitions destruction. American Journal of Public Health 95(8):1382–1388.
Butzko, R. P., A. M. Sotolongo, D. A. Helmer, J. C. Klein-Adams, O. Y. Osinubi, A. R. Berman, R. Ortiz-Pacheco, and M. J. Falvo. 2019. Forced oscillation technique in veterans with preserved spirometry and chronic respiratory symptoms. Respiratory Physiology and Neurobiology 260:8–16.
CDC (Centers for Disease Control and Prevention). 2016. National hospital ambulatory medical care survey: 2016 emergency department summary tables. https://www.cdc.gov/nchs/data/nhamcs/web_tables/2016_ed_web_tables.pdf (accessed August 4, 2020).
CDC. 2017. Age-adjusted percentages (with standard errors) of selected respiratory diseases among adults aged 18 and over, by characteristics: United States, 2017. https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2017_SHS_Table_A-2.pdf (accessed September 6, 2019).
CDC. 2018. Summary health statistics tables for U.S. adults: National Health Interview Survey, 2018. https://ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2018_SHS_Table_A-2.pdf (accessed August 21, 2020).
Chabra, R., and M. Gupta. 2019. Allergic and environmental induced asthma. In StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing.
Cherry, N., F. Creed, A. Silman, G. Dunn, D. Baxter, J. Smedley, S. Taylor, and G. J. Macfarlane. 2001. Health and exposure of United Kingdom Gulf War veterans. Part I: The pattern and extent of ill health. Journal of Occupational and Environment Medicine 58:291–298.
Coates, A. L., J. Wanger, D. W. Cockcroft, B. H. Culver, K. H. Carlsen, Z. Diamant, G. Gauvreau, G. L. Hall, T. S. Hallstrand, I. Horvath, F. H. C. de Jongh, G. Joos, D. A. Kaminsky, B. L. Laube, J. D. Leuppi, and P. J. Sterk. 2017. ERS technical standard on bronchial challenge testing: General considerations and performance of methacholine challenge tests. European Respiratory Journal 49:1–17.
Colby, T. V. 1992. Pathologic aspects of bronchiolitis obliterans organizing pneumonia. Chest 102(1):38S–43S.
Colby, T. V. 1998. Bronchiolitis. Pathologic considerations. American Journal of Clinical Pathology 109(1):101–109.
Coombe, D., and S. Drydale. 1993. Assessment of the effects of atmospheric oil pollution in post war Kuwait. Journal of the Royal Army Medical Corps 139(3):95–97.
Cowan, D. N., J. L. Lange, J. Heller, J. Kirkpatrick, and S. DeBakey. 2002. A case–control study of asthma among U.S. Army Gulf War veterans and modeled exposure to oil well fire smoke. Military Medicine 167(9):777–782.
Crouser, E. D., L. A. Maier, K. C. Wilson, C. A. Bonham, A. S. Morgenthau, K. C. Patterson, E. Abston, R. C. Bernstein, R. Blankstein, E. S. Chen, D. A. Culver, W. Drake, M. Drent, A. K. Gerke, M. Ghobrial, P. Govender, N. Hamzeh, W. E. James, M. A. Judson, L. Kellermeyer, S. Knight, L. L. Koth, V. Poletti, S. V. Raman, M. H. Tukey, and Gloria E. Westney, on behalf of the American Thoracic Society Assembly on Clinical Problems. 2020. Diagnosis and detection of sarcoidosis: An official American Thoracic Society clinical practice guideline. American Journal of Respiratory Critical Care Medicine 201(8):e26–e51.
Culver, B. H. 2006. Interpretation of spirometry: We can do better than the GOLD standard. Respiratory Care 51(7):719–721.
Cypel, Y. S., K. Hamlett-Berry, S. K. Barth, D. E. Christofferson, V. J. Davey, S. Eber, A. I. Schneiderman, and R. M. Bossarte. 2016. Cigarette smoking and sociodemographic, military, and health characteristics of Operation Enduring Freedom and Operation Iraqi Freedom veterans: 2009–2011 National Health Study for a New Generation of US Veterans. Public Health Reports 131(5):714–727.
DASA (Defence Analytics Services and Advice). 2005. 1990/1991 Gulf Conflict—UK Gulf veterans mortality data: Causes of death. Newport, South Wales, UK: National Statistics.
DASA. 2009. 1990/1991 Gulf Conflict—UK Gulf veterans mortality data: Causes of death, 31 Dec 2008. Bath, UK: National Statistics.
Davy, C., A. Dobson, E. Lawrence-Wood, M. Lorimer, K. Moores, A. Lawrence, K. Horsley, A. Crockett, and A. McFarlane. 2012. The Middle East Area of Operations (MEAO) health study: Prospective study. University of Adelaide, Centre for Military and Veterans Health, Adelaide, Australia. https://www.defence.gov.au/Health/Home/Docs/130318MEAOProspectiveStudyReportVol1.pdf (accessed April 2, 2020).
De Giacomi, F., R. V. Eunhee, S. Yi, and J. H. Ryu. 2018. Acute eosinophilic pneumonia: Causes, diagnosis, and management. American Journal of Respiratory and Critical Care Medicine 197(6):728–736.
DelVecchio, S. P., J. F. Collen, L. L. Zacher, and M. J. Morris. 2015. The impact of combat deployment on asthma diagnosis and severity. Journal of Asthma 53(4):363–369.
Díaz-Sanchez, D., M. P, Garcia., M. Wang, M. Jyrala, and A. Saxon. 1999. Nasal challenge with diesel exhaust particles can induce sensitization to a neoallergen in the human mucosa. Journal of Allergy and Clinical Immunology 104(6):1183–1188.
Díaz Santana, M. V., S. Eber, S. Barth, Y. Cypel, E. Dursa, and A. Schneiderman. 2017. Health-related quality of life among U.S. veterans of Operations Enduring Freedom and Operation Iraqi Freedom: Results from a population-based study. Military Medicine 182(11/12):e1885–e1891.
Dion, G. R., C. L. Miller, R. G. Ramos, P. D. O’Connor, and N. S. Howard. 2013. Characterization of voice disorders in deployed and nondeployed U.S. Army soldiers. Journal of Voice 27(1):57–59.
Doebbeling, B. N.,W. R. Clarke, J. C. Torner, R. F. Woolson, M. D. Voelker, D. H. Barrett, and D. A. Schwartz. 2000. Is there a Persian Gulf War syndrome? Evidence from a large population-based survey of veterans and nondeployed controls. American Journal of Medicine 108(9):695–704.
Dunn, N. M., R. K. Katial, and F. C. L. Hoyte. 2015. Vocal cord dysfunction: A review. Asthma Research and Practice 1(1):1–8.
Dursa, E. K., S. K. Barth, R. M. Bossarte, and A. I. Schneiderman. 2016a. Demographic, military, and health characteristics of VA health care users and nonusers who served in or during Operation Enduring Freedom or Operation Iraqi Freedom, 2009–2011. Public Health Reports 131(6):839–843.
Dursa, E. K., S. K. Barth, A. I. Schneiderman, and R. M. Bossarte. 2016b. Physical and mental health status of Gulf War and Gulf Era Veterans. Journal of Occupational and Environmental Medicine 58(1):41–46.
Dursa, E. K., S. K. Barth, B. W. Porter, and A. I. Schneiderman. 2019. Health status of female and male Gulf War and Gulf Era veterans: A population-based study. Womens Health Issues 29(Suppl 1):S39–S46.
Eick, A. A., D. J. Faix, S. K. Tobler, R. L. Nevin, L. E. Lindler, Z. Hu, J. L. Sanchez, V. H. MacIntosh, and K. L. Russell. 2011. Serosurvey of bacterial and viral respiratory pathogen among deployed U.S. service members. American Journal of Preventive Medicine 41(6):573–580.
Eisen, S. A., H. K. Kang, F. M. Murphy, M. S. Blanchard, D. J. Reda, W. G. Henderson, R. Toomey, L. W. Jackson, R. Alpern, B. J. Parks, N. Klimas, C. Hall, H. S. Pak, J. Hunter, J. Karlinsky, M. J. Battistone, M. J. Lyons, and Gulf War Study Participating Investigators. 2005. Gulf War veterans’ health: Medical evaluation of a U.S. cohort. Annals of International Medicine 142(11):881–890.
Epler, G. R. 2010. Diagnosis and treatment of constrictive bronchiolitis. F1000 Medicine Reports 2(32):1–5.
Epler, G. R., and T. V. Colby. 1983. The spectrum of bronchiolitis obliterans. Chest 83(2):161–162.
Falvo, M. J., J. H. Abraham, O. Y. Osinubi, J. Klein, A. M. Sotolongo, D. Ndirangu, L. A. Patrick-DeLuca, and D. A. Helmer. 2016a. Bronchodilator responsiveness and airflow limitation are associated with deployment length in Iraq and Afghanistan Veterans. Journal of Occupational and Environment Medicine 58(4):325–328.
Falvo, M. J., D. A. Helmer, J. C. Klein, O. Y. Osinubi, D. Ndirangu, L. A. Patrick-DeLuca, and A. M. Sotolongo. 2016b. Isolated diffusing capacity reduction is a common clinical presentation in deployed Iraq and Afghanistan veterans with deployment-related environmental exposures. Clinical Respiratory Journal 12:795–798.
Ferris, B. G. 1978. Epidemiology Standardization Project. II. Recommended respiratory disease questionnaires for use with adults and children in epidemiological research. American Review of Respiratory Disease 118:7–57.
Forbes, D. A., J. T. Anderson, J. A. Hamilton, F. A. Rawlins, C. Tinkelpaugh, J. H. Abraham, and M. J. Morris. 2019. Relationship to deployment on sarcoidosis staging and severity in military personnel. Military Medicine 185(5–6):e804–e810.
Gackstetter, G. D., T. I. Hooper, S. F. DeBakey, A. Johnson, B. E. Nagaraj, J. M. Heller, and H. K. Kang. 2006. Fatal motor vehicle crashes among veterans of the 1991 Gulf War and exposure to munitions demolitions at Khamisiyah: A nested case–control study. American Journal of Industrial Medicine 49(4):261–270.
Garshick, E. 2019. Service and Health Among Deployed Veterans (SHADE). Update: VA cooperative study #595: Pulmonary health and deployment to Southwest Asia and Afghanistan. Presentation before the Committee on the Respiratory Health Effects of Airborne Hazards Exposures in the Southwest Asia Theater of Military Operations. October 3, 2019.
Gerke, A. K., M. A. Judson, Y. C. Cozier, D. A. Culver, and L. L. Koth. 2017. Disease burden and variability in sarcoidosis. Annals of the American Thoracic Society 14(6):S421–S428.
GINA (Global Initiative for Asthma). 2019. Global strategy for asthma management and prevention. https://ginasthma.org/wp-content/uploads/2019/06/GINA-2019-main-report-June-2019-wms.pdf (accessed April 30, 2020).
GOLD (Global Initiative for Chronic Obstructive Lung Disease). 2018. Global strategy for prevention, diagnosis and management of COPD (2018 Report). www.goldcopd.org/wp-content/uploads/2017/11/GOLD-2018-v6.0-FINAL-revised-20-Nov_WMS.pdf (accessed March 28, 2020).
Goss Gilroy Inc. 1998. Health study of Canadian forces personnel involved in the 1991 conflict in the Persian Gulf: Volume 1. Ottawa, Canada: Goss Gilroy Inc. and Department of National Defence.
Graham, B. L., I. Steenbruggen, M. R. Miller, I. Z. Barjaktarevic, B. G. Cooper, G. L. Hall, et al. 2019. Standardization of spirometry: 2019 update. An official American Thoracic Society and European Respiratory Society technical statement. American Journal of Respiratory and Critical Care Medicine 200(8):e70–e88.
Gray, G. C., and H. K. Kang. 2006. Healthcare utilization and mortality among veterans of the Gulf War. Philosophical Transaction of the Royal Society B 361:553–569.
Gray, G. C., K. S. Kaiser, A. W. Hawksworth, F. W. Hall, and E. Barrett-Connor. 1999. Increased postwar symptoms and psychological morbidity among U.S. Navy Gulf War veterans. American Journal of Tropical Medicine and Hygiene 60(5):758–766.
Gray, G. C., T. C. Smith, H. K. Kang, and J. D. Knoke. 2000. Are Gulf War veterans suffering war-related illnesses? Federal and civilian hospitalizations examined, June 1991 to December 1994. American Journal of Epidemiology 151(1):63–71.
Gray, G. C., R. J. Reed, K. S. Kaiser, T. C. Smith, and V. M. Gastanaga. 2002. Self-reported symptoms and medical conditions among 11, 868 Gulf War-era veterans: The Seabee Health Study. American Journal of Epidemiology 155(11):1033–1044.
Gutor, S., R.-H. Du, R. F. Miller, B. W. Richmond, P. P. Massion, T. S. Blackwell, and V. V. Polosukhin. 2019. The histopathological basis of airflow limitation in small airways disease. In C108. COPD: Phenotype, mechanism, and treatment. American Journal of Respiratory and Critical Care Medicine 199:A5784.
Gwini, S. M., H. L. Kelsall, J. F. Ikin, M. R. Sim, A. C. McFarlane, and A. B. Forbes. 2016. New onset of chronic diseases and changes in lifestyle risk factors among Gulf War veterans. Journal of Occupational and Environmental Medicine 58(8):770–777.
Haley, R. W. 2003. Excess incidence of ALS in young Gulf War veterans. Neurology 61(6):750–756.
Hena, K. M., J. Yip, N. Jaber, D. Goldfarb, K. Fullam, K. Cleven, W. Moir, Rachel Zeig-Owens, M. P. Webber, D. M. Spevack, M. A. Judson, L. Maier, A. Krumerman, A. Aizer, S. D. Spivack, J. Berman, T. K. Aldrich, and D. J. Prezant. 2018. Clinical course of sarcoidosis in World Trade Center–exposed firefighters. Chest 153(1):114–123.
Henneberger, P. K., C. A. Redlich, D. B. Callahan, P. Harber, C. Lemiere, J. Martin, S. M. Tarlo, O. Vandenplas, and K. Toren. 2011. An official American Thoracic Society statement: Work-exacerbated asthma. American Journal of Respiratory and Critical Care Medicine 184(3):368–378.
Higgins, T. S., and D. D. Reh. 2012. Environmental pollutants and allergic rhinitis. Current Opinion in Otolaryngology & Head and Neck Surgery 20(3):209–214.
Hines, S. E., P. Gucer, S. Kligerman, R. Breyer, J. Centeno, J. Gaitens, M. Oliver, S. Engelhardt, K. Squibb, and M. McDiarmid. 2013. Pulmonary health effects in Gulf War I service members exposed to depleted uranium. Journal of Occupational and Environmental Medicine 55(8):937–944.
Holley, A. B., M. Sobieszczyk, M. Perkins, B. M. Cohee, C. B. Costantoth, D. L. Mabe, R. Liotta, J. H. Abraham, P. R. Holley, and J. Sherner. 2016. Lung function abnormalities among service members returning from Iraq or Afghanistan with respiratory complaints. Respiratory Medicine 118:84–87.
Hooper, T. I., S. F. Debakey, B. E. Nagaraj, K. S. Bellis, B. Smith, T. C. Smith, and G. D. Gackstetter. 2008. The long-term hospitalization experience following military service in the 1991 Gulf War among veterans remaining on active duty, 1994–2004. BMC Public Health 8:60.
Hooper, T. I., G. D. Gackstetter, C. A. LeardMann, E. J. Boyko, L. A. Pearse, B. Smith, P. J. Amoroso, and T. C. Smith. 2010. Early mortality experience in a large military cohort and a comparison of mortality data sources. Population Health Metrics 8:15.
Hwang, J. A., J. H. Song, J. H. Kim, M. P. Chung, J. W. Song, Y. W. Kim, S. M. Choi, S. I. Cha, S. T. Uh, C-S Park, S. H. Jeong, Y. B. Park, H. L. Lee, J. W. Shin, E. J. Lee, Y. Jegal, H. K. Lee, J. S. Park, and M. S. Park. 2017. Clinical significance of cigarette smoking and dust exposure in pulmonary alveolar proteinosis: A Korean national survey. BMC Pulmonary Medicine 17(1):147.
Hyams, K. C., K. Hanson, F. S. Wignall, J. Escamilla, and E. C. Oldfield. 1995. The impact of infectious diseases on the health of U.S. troops deployed to the Persian Gulf during Operations Desert Shield and Desert Storm. Clinical Infectious Disease 20(6):1497–1504.
IOM (Institute of Medicine). 2003a. Gulf War and health: Volume 2: Insecticides and solvents. Washington, DC: The National Academies Press.
IOM. 2003b. Medicolegal death investigation system. Washington, DC: The National Academies Press.
IOM. 2005. Gulf War and health: Volume 3: Fuels, combustions, products, and propellants. Washington, DC: The National Academies Press.
IOM. 2006. Gulf War and health: Volume 4: Health effects of serving in the Gulf War. Washington, DC: The National Academies Press.
IOM. 2008. Gulf War and health: Volume 6: Physiologic, psychologic, and psychosocial effects of deployment-related stress. Washington, DC: The National Academies Press.
IOM. 2010. Gulf War and health: Volume 8: Update of health effects of serving in the Gulf War. Washington, DC: The National Academies Press.
IOM. 2011. Long-term health consequences of exposure to burn pits in Iraq and Afghanistan. Washington, DC: The National Academies Press.
IOM. 2014. Gulf War and health: Volume 9: Long-term effects of blast exposure. Washington, DC: The National Academies Press.
Iowa Persian Gulf Study Group. 1997. Self-reported illness and health status among Gulf War veterans. JAMA 277(3):238–245.
Ishii, H., R. Tazawa, C. Kaneko, T. Saraya. Y. Inoue, E. Hamano, Y. Kogure, K. Tomii, M. Terada, T. Takada, M. Hojo, A. Nishida, T. Ichiwata, B. C. Trapnell, H. Goto, and K. Nakata. 2011. Clinical features of secondary alveolar proteinsis: Pre-mortem cases in Japan. European Respiratory Journal 37:465–468.
Ishoy, T., P. Suadicani, B. Guldager, M. Appleyard, H. O. Hein, and F. Gyntelberg. 1999. State of health after deployment in the Persian Gulf: The Danish Gulf War Study. Danish Medical Bulletin 46(5):416–419.
Jackson, M., B. J. Bercerra, C. Marmolejo, R. M. Avina, N. Henley, and M. B. Becerra. 2017. Prevalence and correlates of sleep apnea among U.S. male veterans, 2005–2014. Preventing Chronic Disease 14(E46):1–5.
Jani, N., M. J. Falvo, A. Sotolongo, O. Y. Osinubi, C. Tseng, M. Rowneki, M. Montopoli, S. W. Morley, V. Mitchell, and D. A. Helmer. 2017a. Blast injury and cardiopulmonary symptoms in US veterans: Analysis of a national registry. Annals of Internal Medicine 167(10):753–755.
Jani, N., M. Falvo, A. Sotolongo, O. Osinubi, C. L. Tseng, M. Rowneki, M. Montopoli, S. Morley, V. Mitchell, and D. Helmer. 2017b. Self-reports of constrictive bronchiolitis among service members participating in the Veterans Administration and Department of Defense Airborne Hazards and Open Burn Pit Registry. Chest 152(4):A822.
Kang, H. K., and T. A. Bullman. 1996. Mortality among U.S. veterans of the Persian Gulf War. New England Journal of Medicine 335(20):1498–1504.
Kang, H. K., and T. A. Bullman. 2001. Mortality among U.S. veterans of the Persian Gulf War: 7-year follow-up. American Journal of Epidemiology 154(5):399–405.
Kang, H. K., C. M. Mahan, K. Y. Lee, C. A. Magee, and F. M. Murphy. 2000. Illnesses among United States veterans of the Gulf War: A population-based survey of 30,000 veterans. Journal of Occupational and Environmental Medicine 42(5):491–501.
Kang, H. K., B. Li, C. M. Mahan, S. A. Eisen, and C. C. Engel. 2009. Health of U.S. veterans of 1991 Gulf War: A follow-up survey in 10 years. Journal of Occupational and Environmental Medicine 51(4):401–410.
Karlinsky, J. B., M. Blanchard, R. Alpern, S. A. Eisen, H. Kang, F. M. Murphy, and D. J. Reda. 2004. Late prevalence of respiratory symptoms and pulmonary function abnormalities in Gulf War I veterans. Archives of Internal Medicine 164(22):2488–2491.
Kelsall, H. L., M. R. Sim, A. B. Forbes, D. P. McKenzie, J. F. Ikin, M. J. Abramson. 2004. Respiratory health status of Australian veterans of the 1991 Gulf War and the effects of exposure to oil fire smoke and dust storms. Thorax 59(10):897–903.
Kenn, K., and M. M. Hess. 2008. Vocal cord dysfunction: An important differential diagnosis of bronchial asthma. Deutsches Ärzteblatt International 105(41):699–704.
Khalil, L., R. B. McNeil, K. J. Sims, K. A. Felder, E. R. Hauser, K. M. Goldstein, C. I. Voils, N. G. Klimas, M. T. Brophy, C. M. Thomas, and R. L. Whitley. 2018. The Gulf War Era Cohort and Biorepository: A longitudinal research resource of veterans of the 1990–1991 Gulf War Era. American Journal of Epidemiology 187(11):2279–2291.
King, M. S., R. Miller, J. Johnson, M. Ninan, E. Lambright, A. F. Shorr, and J. Sheller. 2008. Bronchiolitis in soldiers with inhalation exposures in the Iraq War. Poster presented at the American Thoracic Society’s 104th International Conference, Toronto, Canada, May 2008.
King, M. S., R. Eisenberg, J. H. Newman, J. J. Tolle, F. E. Harrell, Jr., H. Nian, M. Ninan, E. S. Lambright, J. R. Sheller, J. E. Johnson, and R. F. Miller. 2011. Constrictive bronchiolitis in soldiers returning from Iraq and Afghanistan. New England Journal of Medicine 365(3):222–230.
Klein-Adams, J. C., A. M. Sotolongo, J. M. Serrador, D. S. Ndirangu, and M. J. Falvo. 2019. Exercise-induced broncho-constriction in Iraq and Afghanistan veterans with deployment-related exposures. Military Medicine 185(3–4):e389–e396.
Knapik, J. J., R. E. Marin, T. L. Grier, and B. H. Jones. 2009. A systematic review of post-deployment injury-related mortality among military personnel deployed to conflict zones. BMC Public Health 9:231–253.
Korzeniewski, K., and R. Brzozowski. 2011. Sickness profile among Polish troops deployed to Afghanistan in the years 2003–2005. International Maritime Health 62(1):63–70.
Korzeniewski, K., A. Nitsch-Osuch, M. Konarski, A. Guzek, E. Prokop, and K. Bieniuk. 2013. Prevalence of acute respiratory tract diseases among soldiers deployed for military operations in Iraq and Afghanistan. Advances in Experimental Medicine and Biology 788:117–124.
Krefft, S. D., M. Strand, J. Smith, C. Stroup, R. Meehan, and C. Rose. 2017. Utility of Kung clearance index testing as a noninvasive marker of deployment-related lung disease. Journal of Occupational and Environmental Medicine 59(8):707–711.
Krefft, S. D., J. Wolff, L. Zell-Baran, M. Strand, E. B. Gottschall, R. Meehan, and C. S. Rose. 2020. Respiratory diseases in post-9/11 military personnel following Southwest Asia deployment. Journal of Occupational and Environmental Medicine 62(5):337–343.
Kreiss, K. 2013. Occupational causes of constrictive bronchiolitis. Current Opinion in Allergy Clinical Immunology 13(2):167–172.
Kuschner, W. G. 2011. Constrictive bronchiolitis in soldiers: Reply. New England Journal of Medicine 365(18):1744.
Lange, J. L., D. A. Schwartz, B. N. Doebbeling, J. M. Heller, and P. S. Thorne. 2002. Exposures to the Kuwait oil fires and their association with asthma and bronchitis among Gulf War veterans. Environmental Health Perspectives 110(11):1141–1146.
Li, B., C. M. Mahan, H. K. Kang, S. A. Eisen, and C. C. Engel. 2011. Longitudinal health study of U.S. 1991 Gulf War Veterans: Changes in health status at 10-year follow-up. American Journal of Epidemiology 174(7):761–768.
Lin, H. H., M. Ezzati, and M. Murray. 2007. Tobacco smoke, indoor air pollution and tuberculosis: A systematic review and meta-analysis. PLOS Medicine 4 (1):e20.
Lincoln, A. E., T. I. Hooper, H. K. Kang, S. F. Debakey, D. N. Cowan, and G. D. Gackstetter. 2006. Motor vehicle fatalities among Gulf War Era veterans: Characteristics, mechanisms, and circumstances. Traffic Injury Prevention 7(1):31–37.
Lindheimer, J. B., D. B. Cook, J. C. Klein-Adams, W. Qian, H. Z. Hill, G. Lange, D. S. Ndirangu, G. R. Wylie, and M. J. Falvo. 2019. Veterans with Gulf War illness exhibit distinct respiratory patterns during maximal cardiopulmonary exercise. PLOS ONE 14(11):1–14.
Liu, J., N. Lezama, J. Gasper, J. Kawata, S. Morley, D. Helmer, and P. Ciminera. 2016. Burn pit emissions exposure and respiratory and cardiovascular conditions among Airborne Hazards and Open Burn Pit Registry participants. Journal of Occupational and Environmental Medicine 58(7):e249–e255.
Macfarlane, G. J., E. Thomas, and N. Cherry. 2000. Mortality among UK Gulf War veterans. Lancet 356(9223):17–21.
Macfarlane, G. J., A. M. Biggs, N. Maconochie, M. Hotopf, P. Doyle, and M. Lunt. 2003. Incidence of cancer among UK Gulf War veterans: Cohort study. British Medicine Journal 327(7428):1373–1375.
Macfarlane, G. J., M. Hotopf, N. Maconochie, N. Blatchley, A. Richards, and M. Lunt. 2005. Long-term mortality amongst Gulf War veterans: Is there a relationship with experiences during deployment and subsequent morbidity? International Journal of Epidemiology 34(6):1403–1408.
Madar, C. S., M. R. Lewin-Smith, T. J. Franks, R. A. Harley, J. S. Klaric, and M. J. Morris. 2017. Histological diagnoses of military personnel undergoing lung biopsy after deployment to Southwest Asia. Lung 195(4):507–515.
Mancuso, J. D. 2017. Tuberculosis screening and control in the U.S. military in war and peace. American Journal of Public Health 107(1):60–67.
Matthews, T., J. Abraham, L. L. Zacher, and M. J. Morris. 2014. The impact of deployment on COPD in active duty military personnel. Military Medicine 179(11):1273–1278.
Maule, A. L., P. A. Janulewicz, K. A. Sullivan, M. H. Krengel, M. K. Yee, M. McClean, and R. F. White. 2018. Meta-analysis of self-reported health symptoms in 1990–1991 Gulf War and Gulf War–era veteran. BMJ Open 8(e016086):1–12.
Maynard, C., R. Trivedi, K. Nelson, and S. D. Fihn. 2018a. Disability rating age at death, and cause of death in U.S. veterans with service-connected connections. Military Medicine 183(11–12):e371–e376.
Maynard, C., K. Nelson, and S. D. Fihn. 2018b. Disability rating and 1-year mortality among veterans with service-connected health conditions. Public Health Reports 133(6):692–699.
Mayo Clinic. 2016. TB risk factors. https://www.cdc.gov/tb/topic/basics/risk.htm (accessed August 5, 2019).
Mayo Clinic. 2017. Bronchitis. https://www.mayoclinic.org/diseases-conditions/bronchitis/symptoms-causes/syc-20355566 (accessed July 22, 2019).
Mayo Clinic. 2018a. Asthma. https://www.mayoclinic.org/diseases-conditions/asthma/symptoms-causes/syc-20369653 (accessed July 22, 2019).
Mayo Clinic. 2018b. Pneumonitis. https://www.mayoclinic.org/diseases-conditions/pneumonitis/symptoms-causes/syc-20352623 (accessed July 22, 2019).
Mayo Clinic. 2018c. Pneumonia. https://www.mayoclinic.org/diseases-conditions/pneumonia/symptoms-causes/syc-20354204 (accessed July 19, 2019).
Mayo Clinic. 2019a. Chronic cough. https://www.mayoclinic.org/diseases-conditions/chronic-cough/symptoms-causes/syc-20351575 (accessed August 5, 2019).
Mayo Clinic. 2019b. Shortness of breath. https://www.mayoclinic.org/symptoms/shortness-of-breath/basics/definition/sym-20050890 (accessed August 5, 2019).
Mayo Clinic. 2020. Sleep apnea. https://www.mayoclinic.org/diseases-conditions/sleep-apnea/symptoms-causes/syc-20377631 (accessed July 4, 2020).
McCarthy, C., R. Avetisyan, B. C. Carey, C. Chalk, and B. C. Trapnell. 2018. Prevalence and healthcare burden of pulmonary alveolar proteinosis. Orphanet Journal of Rare Diseases 13(129):1–5.
Meadows, S. O., C. C. Engel, R. L. Collins, R. L. Beckman, M. Cefalulu, J. Hawes-Dawson, M. Waymouth, A. M. Kress, L. Sontag-Padilla, R. Ramchand, and K. M. Williams. 2018. 2015 Department of Defense Health Related Behaviors Survey (HRBS). RAND Health Quarterly 8(2):5.
Meffert, B. N., D. M. Morabito, D. A. Sawicki, C. Hausman, S. M. Southwick, R. H. Pietrzak, and A. J. Heinz. 2019. U.S. veterans who do and do not utilize VA healthcare services: Demographic, military, medical, and psychosocial characteristics. Primary Care Companion for CNS Disorders 21(1):1–18.
Miller, D., S. Sazgar, and B. Natt. 2019. The Hamman Rich Syndrome: A case of recurrent acute interstitial pneumonia. In C65. Diffuse Parenchymal Lung Diseases: Basic and Clinical Studies. American Journal of Respiratory and Critical Care Medicine A5439. https://www.atsjournals.org/doi/abs/10.1164/ajrccm-conference.2019.199.1_MeetingAbstracts.A5439 (accessed May 13, 2020).
Miller, R. 2009. Airway injury in U.S. soldiers following service in Iraq and Afghanistan. In U.S. Senate Committee on Veterans’ Affairs Hearing. http://www.veterans.senate.gov/imo/media/doc/miller_100809.pdf (accessed August 31, 2020).
Morris, M. J., and L. L. Zacher. 2011. Constrictive bronchiolitis in soldiers: Reply. New England Journal of Medicine 365(18):1743–1744.
Morris, M. J., R. T. Oleszewski, J. B. Sterner, and P. F. Allan. 2013. Vocal cord dysfunction related to combat deployment. Military Medicine 178(11):1208–1212.
Morris, M. J., D. W. Dodson, P. F. Lucero, G. D. Haislip, R. A. Gallup, K. L. Nicholson, and L. L. Zacher. 2014. Study of Active Duty Military for Pulmonary Disease Related to Environmental Deployment Exposures (STAMPEDE). American Journal of Respiratory and Critical Care Medicine 190(1):78–84.
Morris, M. J., A. J. Skabelund, F. A. Rawlins III, R. A. Gallup, J. K. Aden, and A. B. Holley. 2019. Study of Active Duty Military Personnel for Environmental Deployment Exposures: Pre- and Post-Deployment Spirometry (STAMPEDE II). Respiratory Care 64(5):536–544.
Morris, M. J., R. J. Walter, E. T. McCann, J. H. Sherner, C. Murillo, B. Barber, J. C. Hunninghake, and A. B. Holley. 2020. Clinical evaluation of deployed military personnel with chronic respiratory symptoms: Study of Active Duty Military for Pulmonary Disease Related to Environmental Deployment Exposures (STAMPEDE) III. Chest 157(6):1559–1567.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016. Gulf War and health: Volume 10: Update of health effects of serving in the Gulf War, 2016. Washington, DC: The National Academies Press.
NASEM. 2017. Assessment of the Department of Veterans Affairs Airborne Hazards and Open Burn Pit Registry. Washington, DC: The National Academies Press.
NHLBI (National Heart, Lung, and Blood Institute). 2015. Sarcoidosis. https://www.nhlbi.nih.gov/health-topics/sarcoidosis (accessed July 22, 2019).
NHLBI. 2020a. Alpha-1 antitrypsin deficiency. https://www.nhlbi.nih.gov/health-topics/alpha-1-antitrypsin-deficiency (accessed March 28, 2020).
NHLBI. 2020b. COPD. https://www.nhlbi.nih.gov/health-topics/copd (accessed March 25, 2020).
Nisenbaum, R., K. Ismail, S. Wessely, C. Unwin, L. Hull, and W. C. Reeves. 2004. Dichotomous factor analysis of symptoms reported by U.K. and U.S. veterans of the 1991 Gulf War. Population Health Metrics 2(1):8.
NLM (National Library of Medicine). 2019. Idiopathic pulmonary fibrosis. https://ghr.nlm.nih.gov/condition/idiopathic-pulmonary-fibrosis#statistics (accessed August 5, 2019).
NORD (National Organization for Rare Disorders). 2017. Pulmonary alveolar proteinosis. https://rarediseases.org/rare-diseases/pulmonary-alveolar-proteinosis (accessed August 5, 2019)
O’Donnell, D. E., S. M. Revill, and K. A. Webb. 2001. Dynamic hyperinflation and exercise intolerance in chronic obstructive pulmonary disease. American Journal of Respiratory and Critical Care Medicine 164:770–777.
OIF SAPEG (Operation Iraqi Freedom Severe Acute Pneumonitis Epidemiology Group). 2003. Severe acute pneumonitis among deployed U.S. military personnel—Southwest Asia, March–August 2003. Morbidity and Mortality Weekly Report 52(36):857–859.
Oster, C. N., and J. P. Sanford. 1992. Febrile illness in a desert storm veteran. Hospital Practice (Office Edition) 27(11):145–148, 151, 155–160.
Peacock, M. D., M. J. Morris, M. A. Houghland, G. T. Anders, and H. M. Blanton. 1997. Sleep apnea–hypopnea syndrome in a sample of veterans of the Persian Gulf War. Military Medicine 162(4):249–251.
Pereira, C. A, A. Gimenez, L. Kuranishi, and K. Storrer. 2016. Chronic hypersensitivity pneumonitis. Journal of Asthma and Allergy 9:171–181.
Petruccelli, B. P., M. Goldenbaum, B. Scott, R. Lachiver, D. Kanjarpane, E. Elliott, M. Francis, M. A. McDiarmid, and D. Deeter. 1999. Health effects of the 1991 Kuwait Oil Fires: A survey of U.S. Army troops. Journal of Occupational and Environment Medicine 41(6):433–439.
Polosukhin, V. V., B. Richmond, R. Du, L. B. Ware, J. Lee, R. F. Miller, A. Harris, and T. S. Blackwell. 2017. Loss of multi-ciliated epithelium and impaired mucosal immunity in lungs of soldiers with constrictive bronchiolitis. Abstract, Session D98: Insights into environmental exposure in asthma, COPD, and constructive bronchiolitis. American Journal Respiratory and Critical Care Medicine 195:A7337. https://www.atsjournals.org/doi/abs/10.1164/ajrccm-conference.2017.195.1_MeetingAbstracts.A7337 (accessed May 13, 2020).
Polosukhin, V. V., B. W. Richmond, R.-H. Du, L. B. Ware, J. W. Lee, A. L. Harris, R. F. Miller, and T. S. Blackwell. 2018. Comparative histological and morphometrical analysis of small conducting airways in constrictive bronchiolitis and chronic obstructive pulmonary disease. Abstract, Session B64: COPD: Lung Function, Imaging and Pathophysiology. American Journal of Respiratory and Critical Care Medicine 197:A3914. https://www.atsjournals.org/doi/pdf/10.1164/ajrccm-conference.2018.197.1_MeetingAbstracts.A3914 (accessed May 13, 2020).
Proctor, S. P., T. Heeren, R. F. White, J. Wolfe, M. S. Borgos, J. D. Davis, L. Pepper, R. Clapp, P. B. Sutker, J. J. Vasterling, and D. Ozonoff. 1998. Health status of Persian Gulf War veterans: Self-reported symptoms, environmental exposures and the effect of stress. International Journal of Epidemiology 27(6):1000–1010.
Pugh, M. J., C. A. Jaramillo, K. Leung, P. Faverio, N. Fleming, E. Mortensen, M. E. Amuan, C. Wang, B. Eapen, M. Restrepo, and M. J. Morris. 2016. Increasing prevalence of chronic lung disease in veterans of the Wars in Iraq and Afghanistan. Military Medicine 181(5):476–481.
Quirce, S., O. Vandenplas, P. Campo, M. J. Cruz, F. de Blay, D. Koschel, G. Moscato, G. Pala, M. Raulf, J. Sastrem, A. Siracusa, S. M. Tarlo, J. Walusiak-Skorupa, and Y. Cormier. 2016. Occupational hypersensitivity pneumonitis: An EAACI position paper. Allergy 71(6):765–779.
Rawat, D., H. Basit, and S. Sharma. 2019. Dyspnea. In: StatPearls. Treasure Island, FL: StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK499965 (accessed July 3, 2020).
Reddel, H. K., D. R. Taylor, E. D. Bateman, L. P. Boulet, H. A. Boushey, W. W. Busse, T. B. Casale, P. Chanez, P. L. Enright, P. G. Gibson, J. C. de Jongste, H. A. M. Kerstjens, S. C. Lazarus, M. L. Levy, P. M. O’Byrne, M. R. Partridge, I. D. Pavord, M. R. Sears, P. J. Sterk, S. W. Stoloff, S. D. Sullivan, S. J. Szefler, M. D. Thomas, and S. E. Wenzel. 2009. An official American Thoracic Society/European Respiratory Society Statement: Asthma control and exacerbations: Standardizing endpoints for clinical asthma trials and clinical practice. American Journal of Respiratory and Critical Care Medicine 180(1):59–99.
Redlich, C. A., S. M. Tarlo, J. L. Hankinson, M. C. Townsend, W. L. Eschenbacher, S. G. Von Essen, T. Sigsgaard, and D. N. Weissman. 2014. Official American Thoracic Society Technical Standards: Spirometry in the occupational setting. American Journal of Respiratory and Critical Care Medicine 189(8):984–994.
Riddle, M. S., D. R. Tribble, S. D. Putnam, et al. 2008. Past trends and current status of self-reported incidence and impact of disease and nonbattle injury in military operations in Southwest Asia and the Middle East. American Journal of Public Health 98(12):2199–2206.
Rivera, A. C., T. M. Powell, E J. Boyko, R. U. Lee, D. J. Faix, D. D. Luxton, and R. P. Rull. 2018. New-onset asthma and combat deployment: Findings from the Millennium Cohort Study. American Journal of Epidemiology 187(10):2136–2144.
Rohrbeck, P., Z. Hu, and T. M. Mallon. 2016. Assessing health outcomes after environmental exposures associated with open pit burning in deployed U.S. service members. Journal of Occupational and Environmental Medicine 58(85):S104–S110.
Rom, W. N., M. Weiden, R. Garcia, T. A. Yie, P. Vathesatogkit, D. B. Tse, G. McGuiness, V. Roggli, and D. Prezant. 2002. Acute eosinophilic pneumonia in a New York City firefighter exposed to World Trade Center dust. American Journal of Respiratory and Critical Care Medicine 166(6):797–800.
Roop, S.A., A. S. Niven, B. E. Calvin, J. Bader, and L. L. Zacher. 2007. The prevalence and impact of respiratory symptoms in asthmatics and nonasthmatics during deployment. Military Medicine 172(12):1264–1269.
Sá-Sousa, A., T. Jacinto, L. Azevedo, M. Morais-Almeida, C. Robalo-Cordeiro, A. Bugalho-Almeida, et al. 2014. Operational definitions of asthma in recent epidemiological studies are inconsistent. Clinical and Translational Allergy 4(1):24.
Saers, J., L. Ekerljung, B. Forsberg, and C. Janson. 2017. Respiratory symptoms among Swedish soldiers after military service abroad: Association with time spent in a desert environment. European Clinical Respiratory Journal 4:1–6.
Sanchez, J. L., M. J. Cooper, C. A. Myers, J. F. Cummings, K. G. Vest, K. L. Russell, J. L. Sanchez, M. J. Hiser, and C. A. Gaydos. 2015. Respiratory infections in the U.S. military: Recent experience and control. Clinical Microbiology Reviews 28(3):743–800.
Sanders, J. W., S. D. Putnam, C. Frankart, R. W. Frenck, M. R. Monteville, M. S. Riddle, D. M. Rockbrand, T. W. Sharp, and D. R. Tribble. 2005. Impact of illness and non-combat injury during Operations Iraqi Freedom and Enduring Freedom (Afghanistan). American Journal of Tropical Medicine and Hygiene 73(4):713–719.
Scarupa, M. D., and M. A. Kaliner. 2009. Nonallergic rhinitis, with a focus on vasomotor rhinitis clinical importance, differential diagnosis, and effective treatment recommendations. World Allergy Organization Journal 2(3):20–25.
Schmidt, C. W. 2008. Linking TB and the environment: An overlooked mitigation strategy. Environmental Health Perspectives 116(11):A478–A485.
Sharkey, J. M., C. Baird, A. Eick-Cost, L. Clark, Z. Hu, S. Ludwig, and J. Abraham. 2015. Review of epidemiological analyses of respiratory health outcomes after military deployment to burn pit locations with respect to feasibility and design issues highlighted by the Institute of Medicine. In C. P. Baird and D. K. Harkins (eds.), Airborne hazards related to deployment. Fort Sam, TX: Borden Institute, U.S. Army Medical Department Center and School. Pp. 291–304.
Sharkey, J. M., J. H. Abraham, L. L. Clark, P. Rohrbeck, S. L. Ludwig, Z. Hu, and C. P. Baird. 2016. Postdeployment respiratory health care encounters following deployment to Kabul, Afghanistan: A retrospective cohort study. Military Medicine 181(3):265–271.
Shaw, E., L. Hermansen, W. Pugh, and M. White. 1991. Disease and non-battle injuries among Navy and Marine Corps personnel during Operation Desert Shield/Desert Storm. US Naval Health Research Center. https://apps.dtic.mil/dtic/tr/fulltext/u2/a250652.pdf (accessed June 18, 2020).
Shirtcliffe, P., M. Weatherall, S. Marsh, J. Travers, A. Hansell, A. McNaughton, S. Aldington, H. Muellerova, and R. Beasley. 2007. COPD prevalence in a random population survey: A matter of definition. European Respiratory Journal 30(2):232–239.
Shorr, A. F., S. I. Scoville, S. B. Cersovsky, C. D. Shanks, C. F. Ockenhouse, B. I. Smoak, W. W. Carr, and B. P. Petruccelli. 2004. Acute eosinophilic pneumonia among U.S. military personnel deployed in or near Iraq. JAMA 292(24):2997–3005.
Sim, M., D. Clarke, B. Forbes, D. Glass, S. Gwini, J. Ikin, H. Kelsall, D. McKenzie, B. Wright, A. McFarlane, M. Creamer, and K. Horsley. 2015. Australian Gulf War Veterans’ Follow Up Health Study technical report. Canberra, Australia: Department of Veterans’ Affairs. https://www.dva.gov.au/sites/default/files/files/consultation%20and%20grants/healthstudies/gulfwar/follow_up2015/aus_gulf_war_follow_up_tech_report2015.pdf (accessed June 18, 2020).
Simmons, R., N. Maconochie, and P. Doyle. 2004. Self-reported ill health in male UK Gulf War veterans: A retrospective cohort study. BMC Public Health 4(1):27.
Sine, C. R., P. D. Hiles, S. L. Scoville, R. L. Haynes, P. F. Allan, T. J. Franks, M. J. Morris, and E. C. Osborn. 2018. Acute eosinophilic pneumonia in the deployed military setting. Respiratory Medicine 137:123–128.
Singer, J. P., K. Jones, and S. C. Lazarus. 2016. Bronchiolitis and other intrathoracic airway disorders. In J. K. Stoller, V. C. Broaddus, R. J. Mason, J. D. Ernst, T. E. King, Jr., S. C. Lazarus, J. F. Murray, J. A. Nadel, and A. Slutsky (eds.), Murray and Nadel’s textbook of respiratory medicine, 6th ed. Philadelphia, PA: Elsevier Saunders. Pp. 897–911.
Singh, A., A. Avula, and E. Zahn. 2020. Acute bronchitis. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK448067 (accessed June 18, 2020).
Smith, B., T. C. Smith, M. A. K. Ryan, and G. C. Gray. 2006. A comparison of the postdeployment hospitalization experience of U.S. military personnel following service in the 1991 Gulf War, Southwest Asia after the Gulf War, and Bosnia. Journal of Occupational and Environmental Hygiene 3(12):660–670.
Smith, B., L. K. Chu, T. C. Smith, P. J. Amoroso, E. J. Boyko, T. I. Hooper, G. D. Gackstetter, and M. A. K. Ryan. 2008. Challenges of self-reported medical conditions and medical records among members of a large military cohort. BMC Medical Research Methodology 8(37):1–10.
Smith, B., C. A. Wong, T. C. Smith, E. J. Boyko, G. D. Gackstetter, and M. A. K. Ryan for the Millennium Cohort Study Team. 2009. Newly reported respiratory symptoms and conditions among military personnel deployed to Iraq and Afghanistan: A prospective population-based study. American Journal of Epidemiology 170(11):1433–1442.
Smith, B., C. A. Wong, E. J. Boyko, C. J. Phillips, G. D. Gackstetter, M. A. Ryan, T. C. Smith, and Millennium Cohort Study Team. 2012. The effects of exposure to documented open-air burn pits on respiratory health among deployers of the Millennium Cohort Study. Journal of Occupational and Environmental Medicine 54(6):708–716.
Smith, T. C., J. M. Heller, T. I. Hooper, G. D. Gackstetter, and G. C. Gray. 2002. Are Gulf War veterans experiencing illness due to exposure to smoke from Kuwaiti oil well fires? Examination of Department of Defense hospitalization data. American Journal of Epidemiology 155(10):908–917.
Soltis, B. W., J. W. Sanders, S. D. Putnam, D. R. Tribble, and M. S. Riddle. 2009. Self reported incidence and morbidity of acute respiratory illness among deployed U.S. military in Iraq and Afghanistan. PLOS ONE 4(7):e6177.
Song, W., Y. Chang, S. Faruqi, J. Kim, M. Kang, S. Kim, E. Jo., M. Kim, J. Plevkova, H. Park, S. Cho, and A. H. Morice. 2015. The global epidemiology of chronic cough in adults: A systematic review and meta-analysis. European Respiratory Journal 45:1479–1481.
Statistics Canada. 2005. The Canadian Persian Gulf Cohort Study: Detailed report. http://www.veterans.gc.ca/pdf/about-us/research-directorate/gulf-war-linkage-project.pdf (accessed July 28, 2020).
Steele, L. 2000. Prevalence and patterns of Gulf War illness in Kansas veterans: Association of symptoms with characteristics of person, place, and time of military service. American Journal of Epidemiology 152(10):992–1002.
Szema, A. M., M. C. Peters, K. M. Weissinger, C. A. Gagliano, and J. J. Chen. 2010. New-onset asthma among soldiers serving in Iraq and Afghanistan. Allergy and Asthma Proceedings 31:e67–e71.
Szema, A. M., W. Salihi, K. Savary, and J. J. Chen. 2011. Respiratory symptoms necessitating spirometry among soldiers with Iraq/Afghanistan War lung injury. Journal of Occupational and Environmental Medicine 53(9):961–965.
Tarlo, S. M. 2006. Cough: Occupational and environmental considerations: ACCP evidence-based clinical practice guidelines. Chest 129(1):186S–196S.
Taylor, N., and D. Ross. 2019. Fumes and faeces in Kabul. BMJ Military Health 166(3):171–174.
Thunnissen, E., H. J. Blaauwgeers, E. M. de Cuba, C. Y. Yick, and D. B. Flieder. 2016. Ex vivo artifacts and histopathologic pitfalls in the lung. Archives of Pathology & Laboratory Medicine 140(3):212–220.
Tortora, G. J., and B. H. Derrickson. 2018. Principles of anatomy and physiology. New York: John Wiley & Sons.
UK (United Kingdom) Ministry of Defence. 2014. National statistics notice: 1990/1991 Gulf conflict—UK Gulf veterans mortality data: Causes of death. Bristol, UK: UK Ministry of Defence.
Unwin, C., N. Blatchley, W. Coker, S. Ferry, M. Hotopf, L. Hull, K. Ismail, I. Palmer, A. David, and S. Wessely. 1999. Health of UK servicemen who served in Persian Gulf War. Lancet 353:169–178.
VA (Department of Veterans Affairs). 2014a. Diagnoses among deployed Gulf War veterans who used VA health care services, from 1st Qtr FY 2002 through 4th Qtr FY 2013. Preliminary draft. Washington, DC: Veterans Health Administration.
VA. 2014b. Diagnoses among non-deployed Gulf War veterans who used VA health care services, from 1st Qtr FY 2002 through 4th Qtr FY 2013. Preliminary draft. Washington, DC: Veterans Health Administration.
VA. 2020. Opportunities missed to contain spending on sleep apnea devices and improve veterans’outcomes. Office of Inspector General, Office of Audits and Evaluations. Veterans Health Administration. Report #19-00021-41. https://www.va.gov/oig/pubs/VAOIG-19-00021-41.pdf (accessed August 20, 2020).
Vourlekis, J. S. 2004. Acute interstitial pneumonia. Clinics in Chest Medicine 25(4):739–747.
Weinstein, D. J., J. E. Hull, B. L. Ritchie, J. A. Hayes, and M. J. Morris. 2016. Exercise-associated excessive dynamic airway collapse in military personnel. Annals of the American Thoracic Society 13(9):1476–1482.
Winkenwerder, W. 2002. U.S. demolition operations at Khamisiyah. Final report. Washington, DC: Department of Defense. https://gulflink.health.mil/khamisiyah_iii (accessed June 17, 2020).
Woods, J., B. Barber, and M. J. Morris. 2018. The effect of deployment on pulmonary function in active duty military members with asthma. Abstract, Session C106: Occupational Lung Epidemiology. https://www.atsjournals.org/doi/abs/10.1164/ajrccm-conference.2018.197.1_MeetingAbstracts.A6082 (accessed August 24, 2020).
Young, H. A., J. D. Maillard, P. H. Levine, S. J. Simmens, C. M. Mahan, and H. K. Kang. 2010. Investigating the risk of cancer in 1990–1991 U.S. Gulf War veterans with the use of state cancer registry data. Annals of Epidemiology 20(4):265–272.
Young, T., M. Palta, J. Dempsey, J. Skatrud, S. Weber, and S. Badr. 1993. The occurrence of sleep-disordered breathing among middle-aged adults. New England Journal of Medicine 328(17):1230–1235.
Zarogiannis, S. G., and S. Matalon. 2011. Constrictive bronchiolitis in soldiers: Reply. New England Journal of Medicine 365(18):1743.
Zundel, C. G., M. H. Krengel, T. Heeren, M. K. Yee, C. M. Grasso, P. A. Janulewicz Lloyd, S. S. Coughlin, and K. Sullivan. 2019. Rates of chronic medical conditions in 1991 Gulf War veterans compared to the general population. International Journal of Environmental Research and Public Health 16(6):949.
Zwerling, C., J. C. Torner, W. R. Clarke, M. D. Voelker, B. N. Doebbeling, D. H. Barrett, J. A. Merchant, R. F. Woolson, and D. A. Schwartz. 2000. Self-reported postwar injuries among Gulf War veterans. Public Health Reports 115(4):346–349.
This page intentionally left blank.
















































































































