9
The Role of Systems and Policies in Providing Solutions to Nutrition Access and Equity During Pregnancy and Lactation
Evidence on relevant biological and physiological processes is fundamental to developing nutrition recommendations for women during pregnancy and lactation. However, dietary decisions and behaviors are made within structural, social, and environmental contexts. Consideration of social determinants of dietary intakes can help inform interventions at the individual, systems, and population levels. Session 8 of the workshop, moderated by Angela Odoms-Young, associate professor in the Department of Kinesiology and Nutrition and associate director of research, education, and training in the Office of Community Engagement and Neighborhood Health Partnerships at the University of Illinois at Chicago, explored the role of systems and policies in improving nutrition access and equity during pregnancy and lactation. Highlights from the session presentations are presented in Box 9-1.
SYSTEMS CHANGES FOR IMPROVING MATERNAL NUTRITION DURING PREGNANCY AND LACTATION AMONG U.S. WOMEN
Rafael Pérez-Escamilla, professor of public health, director of the Office of Public Health Practice, and director of the Global Health Concentration at the Yale School of Public Health, began by summarizing the main points of his presentation. Pérez-Escamilla stated that the health and nutrition of pregnant and lactating women are affected by strong socioeconomic inequities that are caused by social injustice, and recommended that systems approaches across the life span be used to address these inequities. These approaches would need to be intentional and assertive efforts, based
Socioeconomic Inequities
Strong socioeconomic inequities exist among pregnant and lactating women, asserted Pérez-Escamilla. Even after controlling for key socioeconomic confounders, non-Hispanic black, American Indian/Alaska Native, and U.S.-born Mexican women are at increased odds of being overweight or having obesity, as compared to their non-Hispanic white counterparts (Singh and DiBari, 2019). Rates of breastfeeding initiation, any breastfeeding, and exclusive breastfeeding are lower among black and American Indian/Alaska Native women (Li et al., 2019). Single women with children, who are potentially socioeconomically vulnerable, are at a higher risk of living in a food-insecure household (USDA ERS, 2019). Social injustice is the root cause of these inequities, indicated Pérez-Escamilla.
Appropriate Frameworks to Guide Research
“Addressing inequities in maternal nutrition during pregnancy and lactation requires first an in-depth understanding of the social, economic, physical, and health care systems surrounding pregnant and lactating women and their families across the life course,” said Pérez-Escamilla. He added that addressing inequities would also require consideration of the different layers or levels of the social ecological model.
Given strong interactions across different systems and levels that affect inequities, Pérez-Escamilla thought appropriate frameworks are needed to guide research. He offered the Community Energy Balance framework as an example (Kumanyika et al., 2012) (see Figure 9-1). This framework posits that the context-specific input from diverse stakeholders across the different layers of the social ecological model is central for the design, implementation, and evaluation of effective equitable interventions. “Some dimensions of this framework that are often neglected in practice are multidimensional acculturation processes and historical trauma resulting from colonialism and neocolonialism, as well as racism and other forms of structural discrimination,” noted Pérez-Escamilla.
on implementation science and on equity principles, from design through evaluation. In his remarks, Pérez-Escamilla touched on socioeconomic inequities, discussed appropriate frameworks to guide research, provided examples of the application of the principles, and offered his thoughts on research needs.
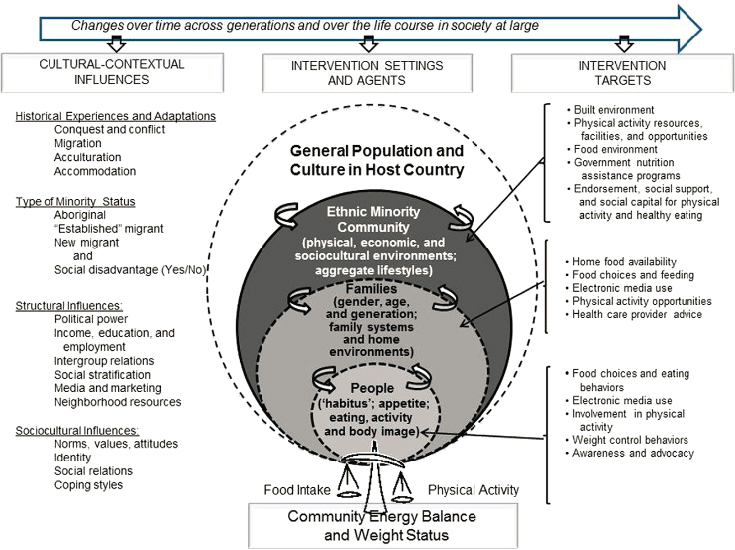
SOURCES: Presented by Rafael Pérez-Escamilla. Reprinted from Preventive Medicine, 55/5, Kumanyika, S., W. C. Taylor, S. A. Grier, V. Lassiter, K. J. Lancaster, C. B. Morssink, and A. M. Renzaho, Community energy balance: A framework for contextualizing cultural influences on high risk of obesity in ethnic minority populations, 371–381, Copyright (2012), with permission from Elsevier.
Examples of the Application of the Principles
Pérez-Escamilla highlighted some applications of the principles he discussed relevant to pregnancy and lactation. Examples included breastfeeding, specific healthy food and physical activity policies, and modeling food system improvements.
Breastfeeding
Over the past several years, breastfeeding rates have continued to improve in the United States (Li et al., 2019). Pérez-Escamilla suggested that expansion in the coverage and improvements in the quality of the Baby-Friendly Hospital Initiative across the care continuum contributed to the improved breastfeeding rates. He explained that Baby-Friendly Hospital
coverage was intentionally increased in Southern states, as this region had the highest concentration of minority groups, including African Americans, and the lowest breastfeeding rates in the country. Implementation research also enhanced the success of the initiative, Pérez-Escamilla said. An analysis from Merewood et al. (2019) found that implementation of the Baby-Friendly Hospital Initiative in hospitals in Louisiana, Mississippi, Tennessee, and Texas increased breastfeeding initiation, increased exclusive breastfeeding, and decreased the breastfeeding initiation disparities between African American and white infants.
Efforts have also sought to scale up breastfeeding promotion, protection, and support. To facilitate this work, Pérez-Escamilla et al. (2012) developed the Breastfeeding Gear Model (see Figure 9-2). The model, already tested in eight countries across five regions of the world, shows that evidence-based advocacy can promote political will, leading to breastfeeding legislation and the corresponding release of resources needed to properly scale up breastfeeding programs. Fundamental to this model are
breastfeeding protection measures, including paid maternity benefits for women employed in the formal and informal economy sectors, and prevention of unethical marketing of infant formulas, noted Pérez-Escamilla. He also indicated that success relies on having a well-trained and diverse workforce responsible for implementing the breastfeeding programs at the health care and community levels. The model also calls for effective communication campaigns for behavior change, operations research, and a decentralized coordinating entity.
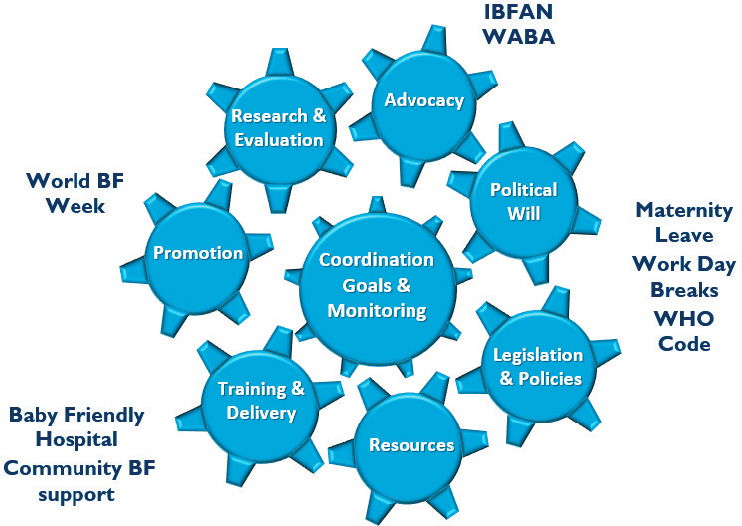
NOTE: BF = breastfeeding; IBFAN = International Baby Foods Action Network; WABA = World Alliance for Breastfeeding Action; WHO = World Health Organization.
SOURCES: Presented by Rafael Pérez-Escamilla. Adapted and reprinted from Pérez-Escamilla et al., 2012 with permission.
Specific Healthy Food and Physical Activity Policies
Pérez-Escamilla briefly mentioned select policies that have contributed to improvements in dietary quality and physical activity levels by taking a systems approach. He touched on behavioral economic approaches, such as taxing sugar-sweetened beverages, providing incentives for Supplemental Nutrition Assistance Program (SNAP) participants to purchase more fruits and vegetables, and front-of-package labeling. Removal of trans fatty acids from the food supply served as another example. Pérez-Escamilla also cited the Open Streets initiative, which has been used in Latin America and several U.S. cities to promote physical activity. Although these policies have evidence of having a beneficial effect, no studies have specifically assessed the effect among pregnant and lactating women, noted Pérez-Escamilla.
Modeling Food System Improvements
With the ability to account for complex systems and inequities, agent-based modeling techniques can be used to predict the effect of policies or interventions on lifestyle and obesity outcomes. One such model showed that the negative effect that neighborhood racial segregation has on dietary quality would require both improving preference for healthy foods and providing access to those foods at a low cost (Auchincloss et al., 2011). Pérez-Escamilla suggested that this finding substantiates the need for both SNAP-Education (SNAP-Ed), together with the SNAP fruit and vegetable incentive program.
Thoughts on Research Needs
To end his prepared remarks, Pérez-Escamilla offered his thoughts on four key research areas. First, he believed a need exists to determine optimal dietary and physical activity patterns for pregnant and lactating women. Second, he thought further exploration into how different systems can facilitate and support optimal nutrition during these key life stages was needed. Third, he suggested evidence was needed on the effect of existing policies on the dietary quality and physical activity of pregnant and
lactating women. Finally, he thought efforts should be made to improve modeling approaches that take into account inequities. On this last point, Pérez-Escamilla reminded the audience that “the predictions are only going to be as good as the data upon which they are based.”
USING NUTRITION SCIENCE TO REDUCE PERINATAL HEALTH DISPARITIES
Kate Keenan, professor of psychiatry and behavioral neuroscience in the Department of Psychiatry at the University of Chicago, explained that nutrition has the potential to influence mental health, serve as a preventive intervention, and reduce health disparities. In her remarks, Keenan described the research on the effects of stress on health and her work using nutrition to modulate stress.
Effects of Stress
Stress exposure is one of the contributing factors for why poverty confers risk for health disparities, stated Keenan. These stress effects and health disparities appear early in life. As such, Keenan’s group has taken a prenatal programming perspective in considering the long-term health ramifications of maternal stress during pregnancy. Fetal exposure to high maternal glucocorticoid concentrations is thought to be a key mechanism for how prenatal stress influences a child’s stress architecture, noted Keenan.
Compared to their white counterparts, pregnant black American women experience higher levels and different types of stress, said Keenan. Pregnant black women living in poverty have higher rates of adverse birth outcomes (Giscombé and Lobel, 2005) and greater risk for poor nutrition (Fowles and Gabrielson, 2005), and their children are more likely to exhibit deficits in attention, behavior, and emotion regulation, she indicated.
Using Nutrition to Modulate Stress
Various nutrition interventions have been used to support and protect brain function, asserted Keenan. For instance, the risk of neural tube defects is reduced with folic acid supplementation (Locksmith and Duff, 1998). Individuals with phenylketonuria can prevent mental retardation with a low phenylalanine diet (NIH Consensus Development Panel, 2001). Iron supplementation among deficient children and adolescents leads to improvement in cognition and behavioral functioning (Lozoff, 2007). Some studies have also found that fatty acid supplementation may affect stress regulation, although much of this work was conducted in nonpregnant, Asian populations that evaluated test-taking anxiety, noted Keenan.
In a step toward preventing mental disorders in children, Keenan’s group conducted a small pilot study called the Nutrition and Pregnancy Study (NAPS) (Keenan et al., 2014). The concept underpinning NAPS was that difficulty regulating stress hormones in the context of high-stress exposure in mothers during pregnancy would have adverse effects on fetal development, pregnancy outcomes, and infant stress modulation. Keenan’s team tested whether fish oil supplementation containing 450 mg/day of docosahexaenoic acid (DHA) could interrupt this maternal–infant stress cycle. The study randomized 66 black women, 16–21 weeks gestation to receive either the supplement or placebo. Participants were generally healthy Medicaid recipients who consumed less than two servings of fish per week. At 30 weeks gestation, women in the active supplement group had lower perceived stress and lower circulating cortisol concentrations, leading to more modulated responses to stressor tests, as compared to the placebo group. At 4 months of age, infants of women in the active supplement group were heavier and more likely to have an Apgar score of 9. These infants were also found to have a modulated response to a standard stress test, as compared to their counterparts from the placebo group. These results have led Keenan’s team to design a more rigorous randomized controlled trial with 162 women that will explore the measures included in the pilot study and also include markers of inflammation, patterns of stress response, and maternal genotypes.
FOOD INSECURITY AND STRESS AS COMMON CHALLENGES TO OPTIMAL NUTRITION DURING PREGNANCY
Optimal nutrition is critical for maternal well-being, mental health, and physical health, as well as for fetal development, said Barbara Laraia, professor of public health nutrition in the Division of Community Health Sciences at the University of California, Berkeley. Nutrition is strongly influenced by food security and stress, she added to provide context for her remarks. Over the course of her presentation, Laraia discussed relationships between food security, stress, and nutrition; described a mindfulness-based intervention during pregnancy; identified an example initiative to end food insecurity during pregnancy; and offered her thoughts on future directions.
Relationships Among Food Security, Stress, and Nutrition
Laraia suggested that food insecurity and stress are key nutritional indicators. Acute exposures to food insecurity and stress influence food preferences and can promote over- or undereating, and under chronic exposure they promote intake of highly palatable foods and shape food patterns and eating behaviors. Both food insecurity and stress can also influence metabolism, noted Laraia.
At a national level, 9 percent of U.S. pregnant women reported worrying about not having enough food or worried about food running out (i.e., marginally food secure), whereas 12 percent experienced episodic food shortages (i.e., food insecure) (Gamba et al., 2016). More than one-third of women below 300 percent of the poverty level experience some level of food insecurity, reported Laraia. In California, one-third of women have food insecurity and 41 percent of women with food insecurity experienced prenatal depressive symptoms. Three-quarters of women with food insecurity reported having one or multiple severe hardships, such as job loss, lack of emotional or practical support, or domestic violence.
Among both pregnant and nonpregnant populations, food insecurity has been found to be strongly associated with stress, depression, and anxiety, said Laraia. The Pregnancy, Infection, and Nutrition (PIN) Study, for instance, reported that food insecurity was associated with greater gestational weight gain and gestational diabetes. Women with food insecurity were found to have greater changes in stress, scored higher on an eating disorder inventory, consumed more saturated fat, and had greater increases from their prepregnancy body mass index at 12 months postpartum, as compared to food-secure women. “Food insecurity has a prolonged effect,” observed Laraia.
A Mindfulness-Based Intervention During Pregnancy
The interrelationship between food insecurity, stress, and nutrition led Laraia’s group to develop an 8-week mindfulness-based intervention that focused on stress reduction, healthy eating, and physical activity. A total of 200 low-income pregnant women with overweight or obesity were randomized into intervention and control groups. Women in the intervention group had significant reductions in stress, perceived stress, and depression and higher scores in awareness (a mindfulness concept). Although all participants gained weight over the course of pregnancy, the intervention group was at greater odds of gaining weight below the Institute of Medicine pregnancy weight gain guidelines. The intervention group also scored lower on an oral glucose tolerance test.
An Example Initiative to End Food Insecurity During Pregnancy
Laraia highlighted San Francisco as taking a citywide approach to end food insecurity among pregnant women. The initiative, initially funded from the city’s soda tax, took a systems-level approach and began with a community health assessment with hospitals, local government, federal food programs, emergency food, and several nongovernmental organizations. In focus groups, women explained that they face social, emotional,
and logistical issues in getting the food they need. To help pregnant women overcome some of these barriers, the initiative colocated federal food programs and provided additional $40 vouchers for fresh fruits and vegetables. Preliminary data suggests San Francisco’s initiative has decreased food insecurity, reduced the proportion of women who perceive themselves as food insecure, increased vegetable consumption, and, as compared to historically matched data, decreased preterm birth.
Future Directions
Laraia concluded her presentation by offering her ideas for key future directions. Acknowledging that food security is a major stress that is highly prevalent in the United States, she thought that better food security and nutrition monitoring was needed. Laraia suggested that access to fruits and vegetables needed to be improved. Finally, she said that new organizational models facilitating food security during pregnancy would be valuable.
HOW WIC SUPPORTS PREGNANCY AND LACTATION
In her presentation, Darlena Birch, senior public health nutritionist at the National WIC Association (NWA), described how her organization and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) have worked to promote nutrition access and equity among pregnant and lactating women. Birch provided an overview of WIC and NWA, identified key ways WIC addresses health equity, discussed relevant legislation, and highlighted select opportunities that exist.
Overview of WIC and NWA
Funded by the U.S. Department of Agriculture (USDA) since 1974, WIC operates in 89 state agencies, all 50 states, 5 U.S. territories, and 33 Indian Tribal Organizations. Program participants include pregnant and postpartum women, infants, and children younger than 5 years of age. In addition to the supplemental food benefit, WIC provides nutrition education, breastfeeding support, and referrals to health and social services.
NWA is a national nonprofit that seeks to educate, guide, and support WIC staff and provide member-driven advocacy. The organization also promotes research and innovation to improve WIC. “Our vision is a nation of healthier women, children, and their families,” said Birch. She emphasized that NWA is not part of or affiliated with USDA and is not responsible for writing, implementing, or enforcing program guidelines.
Over the past 30 years, there have been several substantial changes that have affected WIC. Birch highlighted the following milestones:
- 1990—A separate supplemental food package was created for exclusively breastfeeding women.
- 1992—The Farmers Market Nutrition Program was introduced, allowing participants to purchase fresh fruits and vegetables at farmers’ markets.
- 1997—USDA’s first breastfeeding campaign was launched. The campaign was updated in 2008.
- 2004—The Breastfeeding Peer-Counseling Program was started.
- 2007—USDA’s Interim Final Rule to change the WIC Food Packages took place. Changes included the addition of a cash value voucher to purchase fruits and vegetables and allowances to purchase whole grain and milk substitutes. The changes went into effect in 2009.
- 2017—The National Academies of Sciences, Engineering, and Medicine provided recommendations for further updates to the food packages, which are still under review at USDA.
- 2019—NWA helped to secure full funding ($90 million) for the Breastfeeding Peer-Counseling Program.
Birch noted some current efforts that have implications for WIC. Notably, the 2020–2025 Dietary Guidelines for Americans will be the first edition of the guidelines to provide guidance specifically for pregnant women and children younger than 2 years of age. Birch stated that NWA has participated in the oral and written comment opportunities for this process. To support program innovation, NWA has secured funds from partners including the Centers for Disease Control and Prevention, Robert Wood Johnson Foundation, the David & Lucile Packard Foundation, American College of Obstetricians and Gynecologists, the Walmart Foundation, and others. Local and state WIC agencies have used the grants for projects with a focus on health equity.
Examples of How WIC Addresses Health Equity
Birch explained that NWA has recently adopted a health equity framework to better guide its efforts to address health disparities and inequities within the WIC community and the population at large. The organization “defines health equity as the ability of all individuals and families to achieve optimal health, irrespective of their identity, race, ability, or class,” she said.
Two examples of how WIC addresses health equity are the Breastfeeding Peer-Counseling Program and the nutrition support it provides. The
Breastfeeding Peer-Counseling Program embeds cultural competency, said Birch, noting “peer counselors come from the same neighborhoods, speak the same language, and share common cultural beliefs with [the program participants they counsel].” With respect to nutrition support, WIC seeks to close nutrition and breastfeeding gaps, and does so through education, supplemental foods, breastfeeding promotion and support, and referrals.
Relevant Legislation
Birch explained that legislation has the ability to support or limit program access, eligibility, and participation. She described recently considered pieces of legislation that would or have had programmatic implications. First, the WIC Act seeks to extend child eligibility, postpartum eligibility, and infant certification periods. Second, the Community Access, Resources, and Education (CARE) for Families Act seeks to further extend the referral networks by creating partnerships to link community and clinics. Third, the Supporting Healthy Mothers and Infants Act creates federal nutrition education materials for opioid use and neonatal abstinence syndrome. Finally, Birch noted that while the 2019 U.S. Department of Homeland Security public charge rule explicitly excluded WIC, Medicaid and SNAP were included. This rule has the potential to limit the nutrition support individuals and families receive and could have community-level ramifications, she suggested. Birch added a recent Supreme Court decision allows the public charge rule to be implemented in 49 states.
Select Opportunities to Improve Public Health
To conclude her remarks, Birch offered NWA’s ideas for improving public health and WIC. The organization is a proponent of increased funding for the WIC Breastfeeding Peer-Counseling Program. NWA supports legislation related to pregnant and lactating women and will continue its legislative efforts, and it is actively following and engaging in the 2020–2025 Dietary Guidelines for Americans process. Thinking more broadly, NWA sees its members across the country as a resource for developing and promoting science-based innovations.
PANEL DISCUSSION
The four session presenters took part in a panel discussion, moderated by Odoms-Young. The discussion explored the implications of the advances of the science on nutrition during pregnancy and lactation on programs, policies, and population health; examined current needs to improve nutri-
tion during these two key life stages; and touched on models to bring changes to scale.
In her first question, Odoms-Young asked the panelists to reflect on the new evidence presented over the course of the workshop and consider the implications of this research for their work and, more generally, to population health. “I think that we sometimes underestimate the power of education,” offered Keenan, suggesting that pregnant women are quite receptive to information. Laraia thought that there is a disconnection between the highly palatable foods readily available in the food supply and current recommendations. She proposed improving access to foods that better align with what is recommended. From Pérez-Escamilla’s perspective, studying the diet–microbiome connections is critical in order to have a better understanding of how the microbiome modulates the relationship between maternal intake and early-life dietary exposures with maternal and child health outcomes. However, Pérez-Escamilla indicated that recommendations on nutrition and physical activity do not have to wait for the biological mechanisms to be fully understood. He suggested that dietary patterns across the life course should be the focus, rather than single nutrients, bioactive compounds, or food groups. Encouraged by the advances in knowledge, Birch thought the gaps that still exist highlight opportunities for research and innovation. Turning to applications to WIC, Birch felt encouraged that the supplemental food packages are based on sound science, and indicated that emerging evidence could further strengthen the program.
Next, Odoms-Young asked the panelists for changes that could be implemented now to improve the nutrition of pregnant and lactating women at the population level. Birch described Go to WIC, NWA’s vision for expanding access to program services to all women nationwide, regardless of income level. Pérez-Escamilla recommended better coordination between a wide variety of systems and sectors, including food and agriculture, health, social protection, and education. Regarding social determinants of health, he drew on an example of his work for the Brazilian government, evaluating food security policies between 2003 and 2010. While the government had hoped to show that improvements in socioeconomic inequities were a result of program, policies, or universal health care, the analysis revealed that 75 percent could be attributed to economic growth and more equitable distribution of wealth. He said:
In the long term, if we don’t address the social determinants of health through an equity lens, we are not going to be able to solve this very serious public health problem related to the lack of access to healthy dietary, physical activity, and mental health state for many, many low-income women and families in our country.
Building on the concept of access, Laraia emphasized the importance of addressing the food supply to ensure low-income women can purchase nutritious foods. Offering a slightly different take on the question, Keenan stated, “I struggle with the tension of focusing on pregnancy.” Acknowledging that pregnancy has served as a prime opportunity to engage and educate women, Keenan also considered it a burden to be hyperfocused on this single period. She thought a broader approach was needed that establishes healthy eating patterns early in life and engages with people at multiple levels.
Finally, Odoms-Young asked if there were any models that could be used to bring nutrition recommendations to scale. Birch wondered if existing public health nutrition interventions (e.g., iodized salt, fluoridated water, folic acid fortification) are underappreciated, given that we do not have overt deficiencies in the population. Agreeing with earlier comments from Laraia, Pérez-Escamilla thought the food system needed change. He noted that the political system does not currently facilitate such improvements and suggested that change will likely stem from empowering grassroots, local food system initiatives.
QUESTIONS FROM THE AUDIENCE
After the panel discussion, session speakers took questions from the audience. Topics covered included international models for nutrition and breastfeeding counseling, WIC eligibility, and community-based participatory research.
International Models for Nutrition and Breastfeeding Counseling
Reflecting on Birch’s comment regarding the Go to WIC concept, Cindy Turner-Maffei of the Healthy Children Project wondered where women who are not currently eligible for WIC can receive reliable information and asked the panelists if there were less cost-intensive models for nutrition and breastfeeding counseling in other countries that could be implemented in the United States. Although she did not have a specific model in mind, Birch said that higher breastfeeding rates are found in regions of the world where breastfeeding is engrained in the culture. She acknowledged that several historical factors have contributed to low breastfeeding rates in the United States, and suggested improvements could be made by building a community of support. On the concept of support, Pérez-Escamilla added that late pregnancy through the first 2 weeks postpartum is a critical window of opportunity for breastfeeding support from well-trained, qualified professionals. Laraia noted that the United States is the only Westernized country without maternal and paternal leave.
WIC Eligibility
An unidentified member of the audience questioned the amount of effort and resources used to determine WIC eligibility and asked if there were innovative ways to decide who qualifies for nutrition assistance. Birch was not aware of any research on this specific topic but noted that efforts have been made to reduce the amount of paperwork needed for enrollment. She added that the WIC Act would help to alleviate some of the burden by extending the infant certification period. There have also been suggestions to link databases with Medicaid and SNAP, as these programs require similar paperwork, but Birch indicated that bringing this to fruition has proved challenging. She explained that, at this time, participation in Medicaid or SNAP can be used as a proof of income for WIC eligibility. On the concept of linking programs, Odoms-Young stated that this had been done for the National School Lunch Program, where there is community-level eligibility. She thought such an approach could reduce both burden and stigma. A member of the audience mentioned that Virginia has tried facilitating enrollment in assistance programs with the expansion of Medicaid in the past year.
Community-Based Participatory Research
Recognizing that different communities need different solutions to address inequities, Anna Maria Siega-Riz of the University of Massachusetts Amherst echoed the idea that community-based participatory research is needed and asked to what extent tailoring at the community level was feasible. Pérez-Escamilla said that communities affected by historical trauma (e.g., Native Americans) often feel as though they are viewed by outside groups as having a problem that needs to be fixed. He explained that constructive, asset-based, community-based participatory research allows for the knowledge, traditions, and experience of the community to guide the development of interventions. Implementation science for nutrition calls for community consultation, including the consideration of needs, assets, preferences, and ideas for solutions prior to implementing a program, Pérez-Escamilla noted. He acknowledged that one of the challenges, from a scientific perspective, is that adaptations are at odds with fidelity, and indicated that a promising area of future research in implementation science is determining core and adaptable features of a program. Leanne Redman of the Pennington Biomedical Research Center shared that her group is being funded by the National Institutes of Health to conduct a statewide randomized controlled trial in the Louisiana WIC program. Her group spent 1.5 years performing formative research. She underscored the importance of community-based participatory research, noting that women who took part were engaged and invested in the process and provided important insight.
This page intentionally left blank.
















