4
New Ways of Thinking about Children’s Mental Health
During the September webinar, Neal Halfon, director of the UCLA Center for Healthier Children, Families, and Communities, and Kimberly Hoagwood, professor of child and adolescent psychiatry at the New York University School of Medicine, led participants through an overview of challenges and trends, introducing analytical frameworks to provide methods for tackling these problems. Halfon argued that a new way of thinking is needed, given the changing epidemiology of children’s mental health, the numerous hidden factors and disparities that play a role, and the projected health, family, and economic costs of this burden. This chapter’s outline of these various analytic frameworks focuses on explaining the Three Horizons perspective on improving health systems and gives examples of mental health programs that have implemented this approach across the country. Finally, it concludes by explaining future opportunities and challenges in order to give direction to the Forum on Children’s Well-Being and other invested stakeholders on future steps.
ANALYTICAL FRAMEWORKS
Halfon offered three frameworks that can help to make sense of complex systems and problems: life course health development, 3.0 health system transformation, and three horizons.
Life Course Health Development
Life course health development (LCHD) provides a new way of thinking about the origins and development of children’s mental health and well-being, Halfon explained. Instead of looking at health as discreet episodes, LCHD illuminates how health and disease develop across the life course and even across generations (Barry, 2019). As a framework, it focuses on multiple ways that risk and protective factors can impact a person during sensitive periods of development and condition behaviors and biology. The dynamic relational environment encompassing the family of the individual, their community, their environment, and the policies influencing them can result in different physiological and developmental adaptations that should be taken into account. LCHD also takes into account multiple factors and time-specific, time-dependent effects leading to different patterns of health development trajectories.
By using LCHD, Halfon said, we want to figure out ways to reduce the risk factors and increase the protective factors over an individual’s life from the prenatal period through old age. For those children that fall into the at-risk category, this could include things like parent training, language stimulation, and high-quality early childhood education. Focusing on these can help improve the health development trajectory for an individual as a child ages (see Figure 4-1).
3.0 Health System Transformation
Over the last several years, the health care system has been evolving from an infectious-disease response system to a system that focuses on chronic disease, noted Halfon. The first era of health care, what we might refer to as Medical Care 1.0, focused on acute infectious disease, short time frames for care, and insurance-based financing, the main goal being to reduce the number of deaths. As the system progressed, it transitioned over the last few decades into a second era, Health Care 2.0, which increasingly focused on chronic disease, longer time frames, chronic disease management and prevention, and the extension of a disability-free life in addition to simply reducing deaths. Halfon urged a transition toward a third era, a Health System 3.0, that will shift the focus toward achieving optimal health instead of just reducing disease. Using the LCHD framework, this new system would monitor health across a person’s life course, invest in population-based prevention, and reach toward the overarching goal of optimizing health for all. Importantly, Halfon pointed out, this 3.0 transformation framework does not assume that change is linear in every case, even though it implies a sequential evolution of the complex system (Halfon et al., 2014). Realistically, the transformation itself is subject to
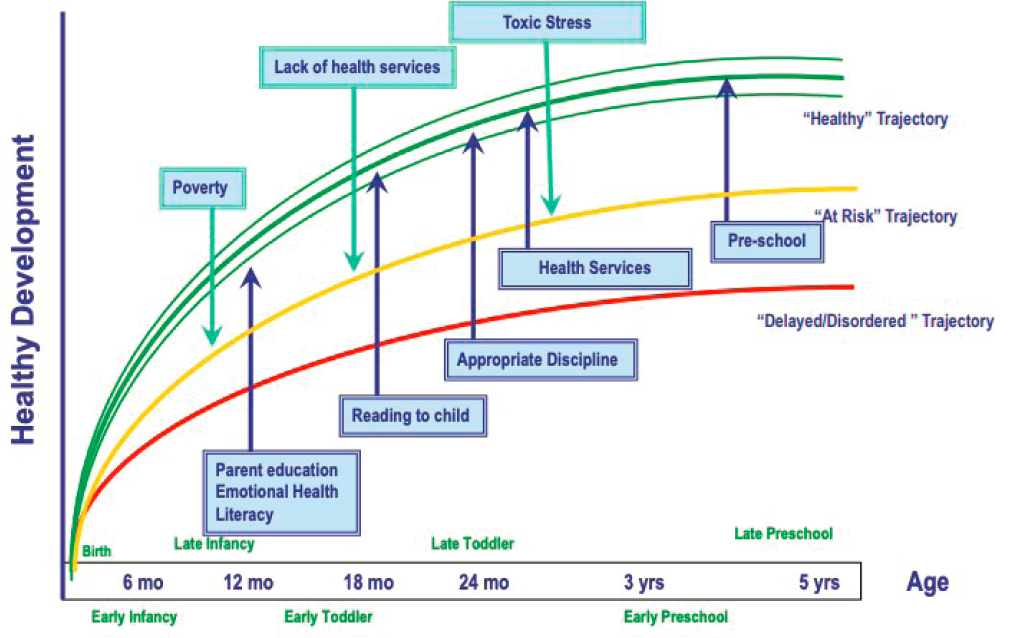
SOURCE: Neal Halfon presentation, September 16, 2019.
external pressures from the surrounding environment such as technological advances and changes in health care policies such as the Affordable Care Act and changes to Medicare and Medicaid financing. A system transformation approach has stimulated a redesign of population-based strategies in order to improve early childhood health and mental health by addressing the social and developmental determinants of mental health (Darling, 2020; Sederer, 2015).
Three Horizons
Hoagwood introduced the Three Horizons model, saying that the search for the right framework not only aids the improvement of children’s mental health, it builds our systems of knowledge, which promotes the design of better health systems.
There are multiple layers of influences on mental, emotional, and behavioral health that include embedded contextual factors that can affect children over time (see Figure 4-2).
She explained the varying levels of influence, saying that the environment influences gene expression and can shape neurodevelopment. While this is a newer area of knowledge, Hoagwood added, the National Institutes of Health (NIH) is currently doing a lot of exciting work on neurogenesis that is worth following. Experiences at the individual level as well as family and community characteristics can affect the conception, gestation, childbirth, and development of a child. Even conditions in the broader society that are created through policy-driven factors, racism, systemic inequality, and poverty can have a significant impact on development at various levels.
Hoagwood described the Three Horizons approach to studying global problems, an interdisciplinary approach to transformation that leads to systemic change through tapping different types of knowledge (Sharpe et al., 2016). It is designed for complex problems with uncertain predictive models and can be explained as follows:
- Horizon 1. A pattern of incremental change that is losing its fit with the direction things are going.
- Horizon 2. A turbulent domain of disruptive transformation and innovation in response to a changing landscape.
- Horizon 3. An emerging pattern that is appearing and growing on the fringes of the existing system.
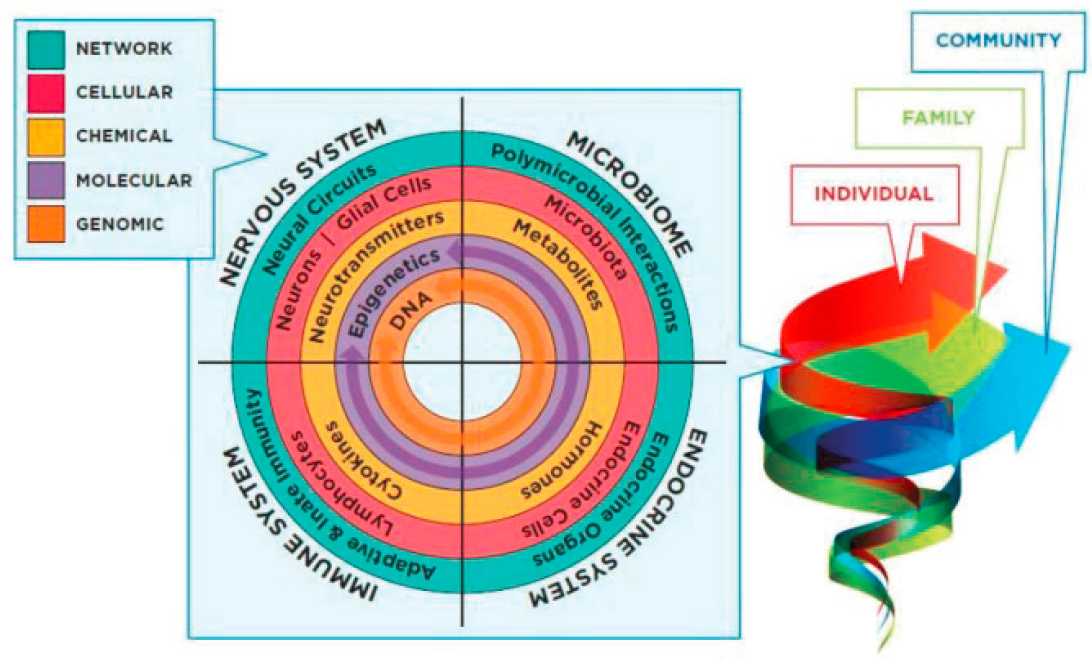
SOURCE: National Academies of Sciences, Engineering, and Medicine, 2019, Figure 2-2.
Challenging Trends for Improving Health Systems: Three Horizons View
To help clarify these concepts, Hoagwood provided details and examples for each of the three horizons and applied this framework to issues related to children’s mental health (see Figure 4-3).
Horizon 1 – Knowledge Expansion
Horizon 1 centers around knowledge expansion, and its positive aspects include an abundance of evidence-based practices, data on cost-benefit ratios, and an amplification of the LCHD model. Hoagwood underscored that implementing this approach is challenging and that barriers, such as costs and the burden of additional training, should be expected. There are also approximately 61 different implementation frameworks but very few practical tools or examples to leverage. She also noted several disruptive changes in children’s mental health systems, including a 42 percent drop in funding from the National Institutes of Mental Health (NIMH) for children’s mental health research since 2005. Overall investment in children’s services research hovers around 2 percent of the overall NIMH budget, but even at the state level, she said, investment in children’s mental health is just absent.
Horizon 2 – Disruptive Changes
Horizon 2 focuses more on disruptive changes such as the digital domination of health care, which includes changing mental health models. Other disruptive changes include seeing the entire family as a service unit, developing quality indicators for children’s services to improve continuous accountability in quality improvement, and the breakdown of boundaries between fields, leading to a multidisciplinary approach to policy making that includes science. This explosion of knowledge and increased accessibility to information has also included misinformation that hinders good decision making and has slowed down progress in certain areas. As an example of this type of disruptive change, Hoagwood described the 2019 Core Set of Children’s Health Care Quality Measures for Medicaid and Children’s Health Insurance Program (Centers for Medicare and Medicaid Services [CMS], 2019). She said that there are far fewer quality indicators related to children’s mental or behavioral health. Since the core set will be mandated by CMS in 2024 for reporting by states, these measures will be an important lever for changing provider behavior.
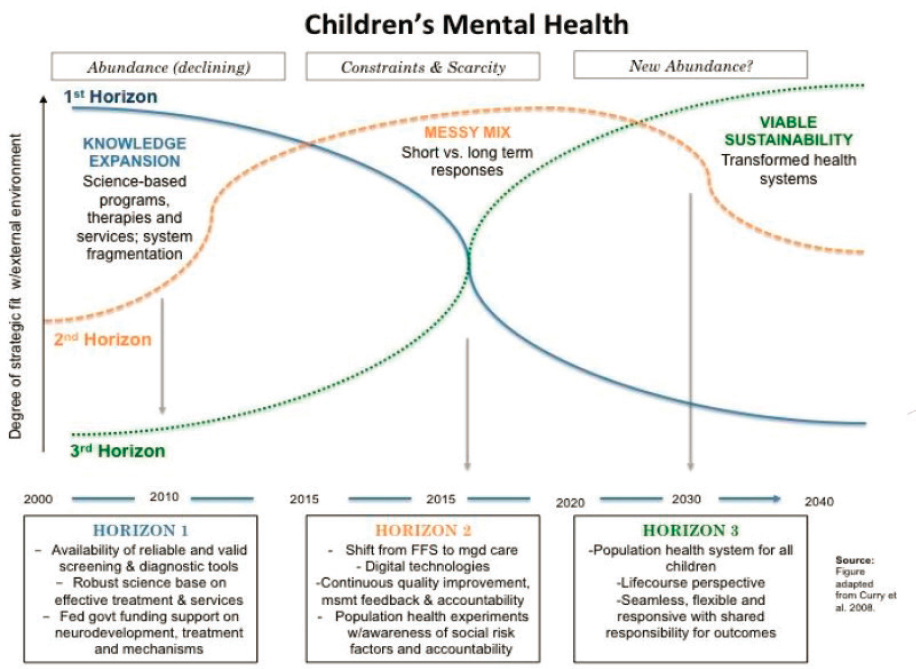
SOURCE: Curry and Hodgson, 2008.
Horizon 3 – Transformative Changes
Horizon 3 reflects a transformative change approach. Current trends that are pointing toward this horizon include the increasing focus on promoting children’s well-being rather than just treating pathology as a population-level responsibility. This is similar to what Halfon described in the Health System 3.0 model. This third horizon will focus not only on clinical disorders but on social determinants of health as well as on local experimentation. One example of an initiative that utilizes this perspective focuses on the first 3 years of children’s lives (that is, their first 1,000 days), the development of community-level support and services for children and their families, and close monitoring for the purposes of mitigating adverse experiences (Darling et al., 2020). An idea of this scale and focus would likely not have been possible 15 years ago.
Another example Hoagwood featured was the National Children’s Hospital in Columbus, Ohio, and its 2017–2022 strategic plan called Journey to Best Outcomes. To carry out the plan’s mandate to improve assistance for high-need families, the hospital adopted neighborhoods in low-income and minority neighborhoods in their area where residents faced the highest risk. Recognizing the embedded nature of children within families and the effect natural, manmade, and social environments can have on their overall mental and emotional health, the hospital partnered with businesses to invest in employment and housing. The housing vacancy rates decreased in areas they focused on and hiring rates increased, both of which are factors that influence family and child well-being.
In closing, Hoagwood said the third horizon provides a road map to health policies and community interventions that cross development trajectories across the life course (see Figure 4-4). This integrated approach can also provide the change in thinking necessary to enable the provision of intergenerational services, as well as policy strategies that cross systems and use creative financing options. If providers can take the evidence base that exists and put it into play at different parts of the continuum, she explained, then hopefully we can start to see better outcomes for these children and families.
FUTURE OPPORTUNITIES AND CHALLENGES
Following Hoagwood’s presentation, participants discussed opportunities and challenges to supporting children’s mental health. Children’s mental health policy research has been a neglected area of science thus far. This is changing with several new NIH-funded studies and centers focused directly on these issues. Policy impact studies—comparing outcomes associated with different kinds of policies—have not been undertaken in this country yet
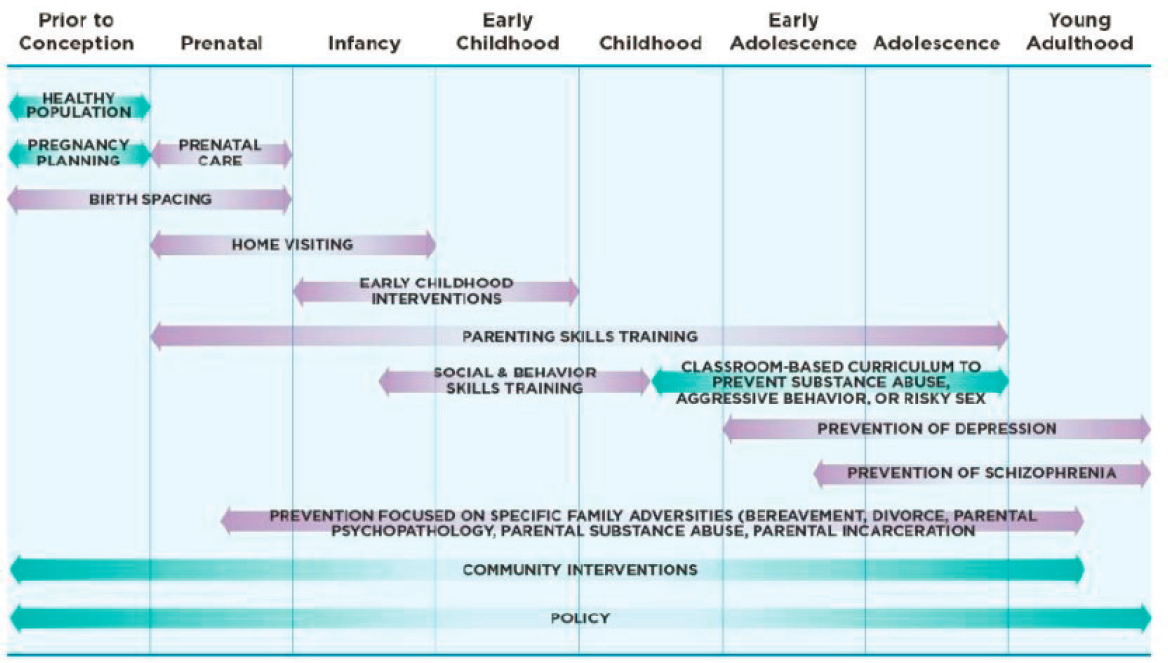
SOURCE: The National Academies of Sciences, Engineering, and Medicine, 2019, Figure 1-4.
(although they have in Europe), making it difficult to know what policy choice will be beneficial under which conditions. These kinds of studies will be valuable in the future. In addition, Hoagwood said, there is a need for research on innovative financing options, especially as there are numerous states and local communities engaged in innovative thinking about these issues.
One participant noted that the lack of physical exercise and unstructured play, as well as the sometimes difficult culture and climate in public schools posed challenges for children’s mental health. Hoagwood suggested using the National Training and Technical Assistance Center within the Substance Abuse and Mental Health Services Administration as a resource for guidance. Creating treatment models specific to local contexts can be challenging and may depend on the community resources that are not adequately equipped to support the communities. Hoagwood also mentioned an alternative approach of a telemedicine model being implemented by the University of Utah to address mental health in school systems.
Hoagwood added that the new and emerging knowledge is shifting the understanding of how to decide where to direct interventions. Research in the past decade has largely focused on individuals instead of relational issues, but now, early relational health (ERH) models are disrupting current models of treatment. These emerging models emphasize the influence of relationships at all levels on mental health such as relationships between parents and children, families and neighborhoods, and the microbiome and the environment. Such models fit well with current trends that emphasize intergenerational approaches and the context of embedded environments, she explained. Advancing knowledge about early relational health is critical and may well lead to new models for both promotion, prevention, and treatment of children’s mental health.
Halfon mentioned the work being done by the Life Course Intervention Research Network in which groups of researchers are focusing on life-stage-specific issues and interventions. Within the network, he said, Mark Feinberg from Penn State is focusing on family-level co-parenting interventions aimed at influencing life trajectories, which will then positively impact the health development of children (Feinberg, 2003). Feinberg is building on Family Foundations, an intervention program that implements co-parenting skills to reduce intrafamily conflict (Feinberg and Kan, 2008; Feinberg and Jones, 2018). A school group led by Mitchel Wong, professor of medicine and public health, and Rebecca Dudovitz, professor of pediatrics at UCLA, is also forming to rethink the effect schools can have on life course health development trajectories through redesign and restructuring of the school environment.
Halfon highlighted responsiveness as an important aspect of the Three Horizons approach, saying that if we know that early childhood
development is based on the relational contexts in ERH and that is being threatened, then how do we respond? Do we respond through a service system or with an ecosystem approach? For example, he described the International Futures Forum in Scotland, which addresses complex issues and uses the Three Horizons model.1 When confronted with high rates of elderly hospitalizations in the winter months due to loneliness and isolation, they tried to alter the pattern instead of just dispatching social workers to reduce hospitalizations. They had more people in the neighborhoods take on caregiving roles and used a people-powered solution instead of the service system. In an analogous way, prevention of mental health disorders and the promotion of optimal mental health trajectories may emerge from new ways (or third-horizon approaches) to transforming the ecosystems where children live, learn, grown, and develop.
One participant asked about communication and messaging challenges in this area. Hoagwood highlighted the promising use of youth peer-support specialists, saying that kids who have already been through the system and lived through trauma can be tremendous leaders once they are able to process their own challenges and grow. Halfon also added that youth movements around the country are driving change, pointing to the 2018 Parkland High School shooting and the resulting student-led gun control movement that emerged as an example.
Halfon continued, addressing innovations in finance that involve payment bundling. By moving payment systems to Accountable Health Communities programs, he said, services could potentially be bundled into life course ecosystem bundles that would package services for community members that range from 9 months to 5 years of age. Doing this would allow family resource centers to be created that could provide ERH services. Model accountable health community programs are already in place, but the length of implementation time and the specific tailoring of such model designs to fit the community it serves creates barriers to scaling them up (Counts et al., 2018; Roiland et al., 2020).
___________________
1 For more on the International Futures forum, see https://www.internationalfuturesforum.com.
This page intentionally left blank.












