Summary1
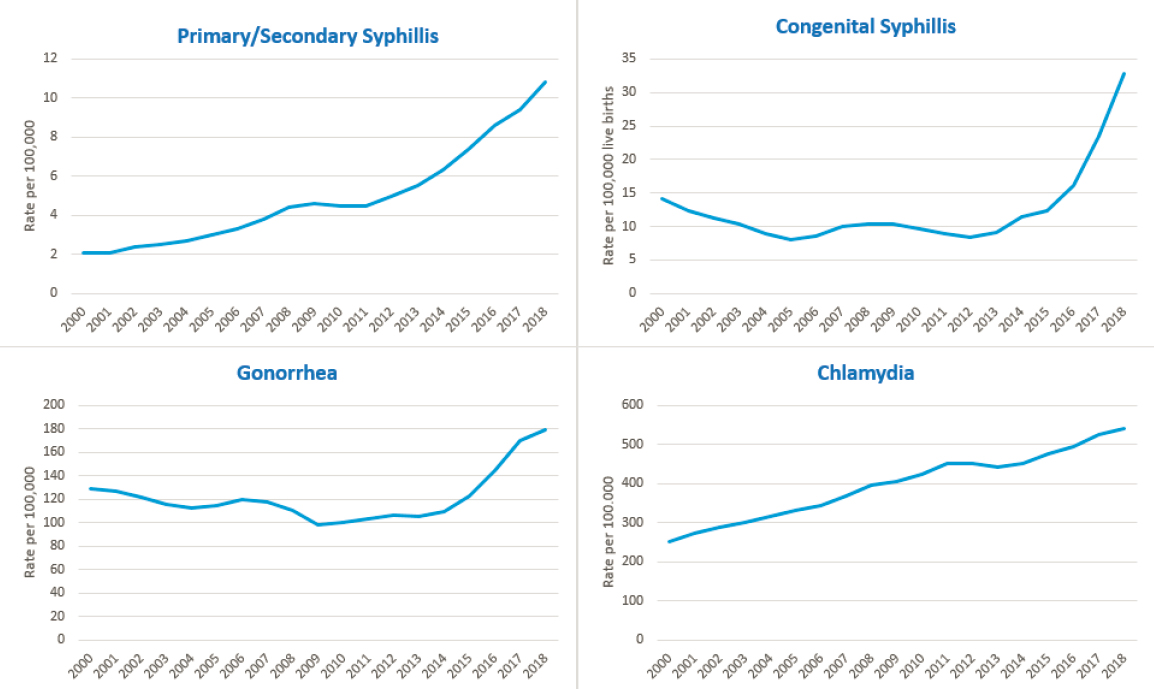
Sexual and reproductive health is of critical importance to overall health and well-being. The prevention and control of sexually transmitted infections (STIs)—a major component of sexual and reproductive health—however, has been chronically underfunded, stigmatized, and too frequently left out of national conversations around health. STIs are among the most common infections affecting humans and cause significant morbidity and mortality in the United States and globally. The Centers for Disease Control and Prevention (CDC) estimates that one in five people in the United States had an STI on any given day in 2018, totaling nearly 68 million estimated infections. Furthermore, an estimated 26 million new STIs occurred in 2018, representing an array of more than 30 viral, bacterial, and protozoal pathogens (see Box S-1 for key STI facts and statistics and Figure S-1 for STI rates over time). Chlamydia, gonorrhea, and syphilis lead the list of reportable U.S. STI infections; they are all preventable, easily diagnosed, and treatable with antibiotics.
Although diagnosed STI rates have increased across all populations in the United States, marginalized groups—youth; women; lesbian, gay, bisexual, transgender, and queer (LGBTQ+) people; and Black, Latino/a, American Indian/Alaska Native (AI/AN), and Native Hawaiian/other Pacific Islander people—continue to experience a disproportionate share of STI cases in the United States. Given the long-term sequelae, as well as
___________________
1 This Summary does not include references. Citations for the discussion presented in the Summary appear in the subsequent report chapters.
the direct medical and economic costs resulting from STIs, these conditions merit attention as a greater health priority, yet blame, embarrassment, shame, and stigma mean that STI epidemics are too often hidden or ignored. In 1997, the Institute of Medicine released a report, The Hidden Epidemic: Confronting Sexually Transmitted Diseases. Although great scientific advances have been made since then, demonstrating that efforts to prevent and treat STIs are not futile, many of the problems and barriers described in that report persist today. STIs remain an underfunded and comparatively neglected field of public health practice and research.
CDC, through the National Association of County and City Health Officials (NACCHO), asked the National Academies to review the current state of STIs in the United States, including the economic burden, current public health strategies and programs (including STI diagnostics, vaccines, monitoring and surveillance, and treatment), and barriers in the health care system, to provide advice on future public health programs,
policy, and research in STI prevention and control. This report follows three studies commissioned by the National Coalition of STD Directors in 2018–2019, and the first STI National Strategic Plan that was developed by the Department of Health and Human Services (HHS) and released in December 2020. The release of these reports and the synergies among them presents a timely opportunity to execute the recommendations provided in this National Academies report.
COMMITTEE’S APPROACH
The committee’s primary emphasis is on addressing the growing epidemics of chlamydia, gonorrhea, and syphilis, but the framework and recommendations presented in this report are intended to strengthen the response to a broad range of STIs. Although HIV is an STI of significant concern, the committee’s charge precludes it from providing HIV-specific recommendations (the report sponsors—CDC and NACCHO—asked the committee to focus its recommendations on STIs other than HIV, given the alarming increases in rates of STIs). Thus, the committee’s consideration of HIV focused on understanding the interplay between HIV and other STIs and how current public health programs can integrate and leverage separate HIV and STI prevention, care, and research programs.
The committee’s conceptual framework is depicted in Figure S-2. The framework’s core elements emphasize the importance of interrelated social ecological factors in the varied manifestations of STI pathogens, social and structural determinants of health and health inequities, intersectionality, and the recognition that sexual health is inextricably linked to overall health and well-being across the life span. The committee views human sexuality as a vital element of mutually consensual love and pleasure, as well as the fundamental prerequisite for procreation. Prevention and control efforts for STIs that are nested within a sexual health paradigm are more likely to prevent and control STIs than efforts nested within a risk framework, as the latter are steeped in and proliferate victim blaming, stigma, marginalization, and discrimination. Therefore, the committee concludes that biomedical approaches to STI prevention and control cannot be optimally effective without also addressing root causes of poor health and STI risk, namely, the structural and social determinants of health, such as poverty, unequal access to quality health care, stigma, racism, and discrimination. Moreover, successful application of this framework requires a shift in current siloed funding mechanisms to an integrated and sustained funding approach that not only addresses STIs as discrete health outcomes but also addresses interpersonal, community, institutional, and other societal factors that influence STI risk, prevention, health care access, delivery, and treatment.
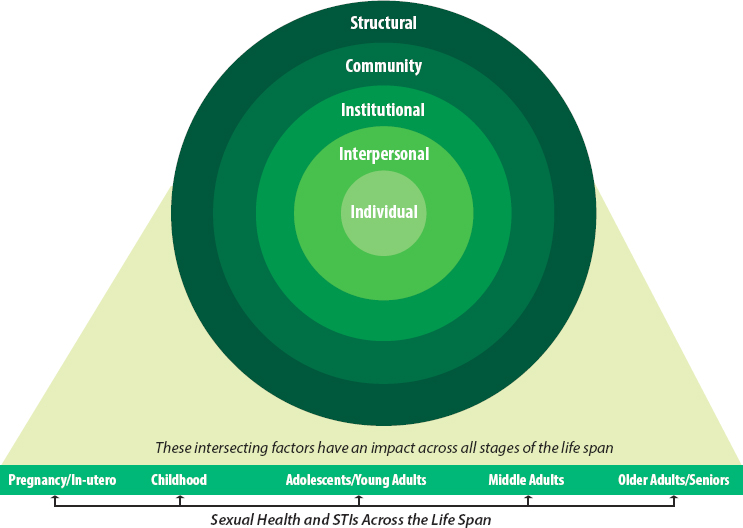
NOTE: This figure illustrates the multiple interrelated influences on STI risk, prevention, health care access, delivery, and treatment across the life span.
The committee is concluding its work as the nation and the world continue to grapple with the acute COVID-19 and chronic HIV/AIDS pandemics. There is a growing challenge of misinformation that is exacerbating the decline of trust in public institutions in general, including public health agencies. Adhering to public health guidance has life-or-death implications, whether for prevention of COVID-19, HIV, congenital syphilis, or other STIs with potentially lifelong consequences. The burden of responding to the COVID-19 pandemic has been felt heavily by STI programs. Under-resourced STI programs have had to compete for resources with a major new public health threat, and their staff have been diverted to the COVID-19 response. This has translated into less attention to STI services and fewer critical services being delivered. The nation pays an increasing price for neglecting to fund public health and thereby neglecting STIs or placing them in funding competition with other urgent infectious diseases control priorities. The COVID-19 pandemic has exposed weaknesses in public health preparedness due to weak
infrastructure, an under-capacitated and under-resourced workforce, and limited surge capacity. Because STIs are infectious diseases that also require testing, treatment, and partner notification, and the STI workforce has deep expertise of relevance to pandemic responses, strengthening STI infrastructure and expanding its workforce offers the dual benefits of achieving stronger STI control and better positioning the nation for future public health threats.
The largest federal source of funding to respond to STIs is appropriated to CDC’s Division of STD Prevention (DSTDP). DSTDP’s funding over the past two decades has remained flat (with a 40 percent reduction in inflation-adjusted dollars). Although the committee’s charge did not specifically ask it to make recommendations related to funding levels and other necessary resource allocations for STIs, the committee notes that some of the recommendations will require new or substantial realignment of resources to implement and the authority and political support to modify existing systems and policies. Furthermore, because the committee’s primary focus was on providing clear policy guidance and a framework for action, it does not uniformly offer specific implementation steps or metrics for each recommendation. The committee understands that resources, policies, and stakeholders vary across the country and that additional voices, including public stakeholders and STI program staff at all levels of government, will be needed to guide implementation of the committee’s recommendations.
The committee has organized its recommendations under four action areas:
- Adopt a sexual health paradigm.
- Broaden ownership and accountability for responding to STIs.
- Bolster existing systems and programs for responding to STIs.
- Embrace innovation and policy changes to improve sexual health.
1. ADOPT A SEXUAL HEALTH PARADIGM2
Integrating Sexual Health as a Key Dimension of Healthy Living
The nation’s response to STIs has mostly focused on individual risk factors and individual behavior change, and has failed to address structural and social elements that foster infection and disease. Since the beginning of the 20th century, approaches focusing on infectious disease sequelae have tended to fuel stigma and shame and therefore have not
___________________
2 Note that recommendations are not presented in numerical order, as the Summary has grouped them by topic; however, all report recommendations are presented.
been successful in fully addressing STI prevention and control. A holistic approach that focuses on sexual health in the context of broader health and well-being is needed. To carry out this change, significant work is needed to eradicate stigma and educate the U.S. population on what it means to be sexually healthy and where and how individuals can access comprehensive sexual health services.
The committee acknowledges that the United States is a diverse country of almost 330 million people, and how one operationalizes a sexual health paradigm will inevitably vary. This paradigm shift is needed, however, given the history of how marginalization has contributed to the proliferation of STIs. Society is paying a cost for this marginalization, and significantly shifting the cultural environment to be supportive of a sexual health framework will take significant dedication and investment and the strategic actions outlined in this report (for more on this topic, see Chapter 12). The committee does not view this as a political issue or one that needs to be in conflict with religious beliefs or ethical standards. For example, promoting sexual health in a manner that facilitates STI prevention, diagnosis, and treatment does not constrain faith communities from discussing sexual responsibility and sexual health in a way that is consistent with their own faith traditions and ethical frameworks. The committee holds an inclusive vision of respect and appreciation for diversity in religious belief, culture, gender, and sexual orientation.
The clinical focus in the current health system emphasizes the harmful effects of STIs on women and newborns without adequately addressing the health of others, including sexual and gender minority and non-binary or gender-expansive individuals. The committee notes, in particular, the striking negligence toward promoting the health of men, including their roles in transmitting STIs. Too often, public policies have failed to encourage men to consider their own health-seeking behaviors, in terms of both shaping a conception of what sexual health means for them and offering clear guidance for when and how men should access health services.
Recommendation 12-1: The Department of Health and Human Services (HHS) should develop a vision and blueprint for sexual health and well-being that can guide the incorporation of a sexual health paradigm across all HHS programs, including the major public insurance programs (Medicaid, Medicare, and the Children’s Health Insurance Program), as well as the public health programs operated throughout the department, including the Centers for Disease Control and Prevention, the Health Resources and Services Administration, the Indian Health Service, and the Substance Abuse and Mental Health Services Administration. The plan should align sexual health and well-being with other dimensions of health—physical, mental, and emotional.
- A holistic approach to sexual health programs should include new approaches and strategies for specifically engaging men (including men who have sex with men) with readily available male-centered sexual health specialty services and the implementation of sexual and reproductive health services in primary care.
- The plan should include strategies for improving sexual health services that address the needs of priority populations, such as women, adolescents, and young adults, and expand attention and resources to underserved populations including Black, Latino/a, and Indigenous populations; people who use drugs; people who engage in sex work; transgender; and gender-expansive populations.
HHS has an important role in catalyzing the shift the committee recommends, but it is imperative that other partners and leaders within the federal government, health systems, and society help to adopt and implement these changes. The vision and action plan should include a course of action for individuals, health care providers, and community members to promote positive sexual health over the life span by giving individuals more agency over their personal preferences and choices, acknowledging the role of culture in influencing these choices, and highlighting structural inequities and barriers to optimal health. Reorienting popular conceptions of well-being to include sexual health is the overarching framework for all recommendations in this report and establishes a new foundation for successful STI prevention and control.
2. BROADEN OWNERSHIP AND ACCOUNTABILITY FOR RESPONDING TO STIs
Better Support for Parents and Guardians to Model Sexual Health
Although maturing children learn information about sexual health in many ways (including via social media), parents and guardians (hereafter “parents”) play a central role in supporting adolescent and young adult sexual and reproductive health and STI prevention. The committee recognizes that not all young people can rely on understanding parents to offer this guidance, and having supporting parents does not negate the need to create additional sources to complement or substitute for supportive parents. Nonetheless, to fully leverage their role, parents need evidence-based guidance on effective parenting strategies for sexual health promotion and STI prevention.
Recommendation 12-2: Federal agencies and relevant professional organizations should equip parents with evidence-based guidance to engage in developmentally appropriate, comprehensive sexual health education and dialogue and to identify actionable steps for their children. Specifically, the committee recommends the following:
- The Department of Health and Human Services (HHS), through the Centers for Disease Control and Prevention (CDC) Division of STD Prevention, CDC Division of Adolescent Health and School Health, the Indian Health Service, and other key public health service agencies, should develop a national, parent-focused communication campaign to promote and guide parental communication with adolescents regarding sexual health and sexually transmitted infection (STI) prevention.
- HHS, including CDC, the Health Resources and Services Administration, and the National Institutes of Health, should develop a compendium of existing evidence-based resources and programs for parental education and skills training on adolescent and young adult sexual health and STI prevention. In addition, there should be continued research investments to improve existing, and to develop new, evidence-based resources and programs.
-
Guidelines should be developed for pediatric and adolescent health care to support skills training and educate parents in promoting adolescent and young adult sexual health, including the prevention of STIs. This would include the following:
- Delivering evidence-based programs for parental education and skills training that are colocated as an extension of regular care, and
- Providing training resources for providers that facilitate direct communication with parents regarding sexual health and STI prevention in their children.
Engage Community Stakeholders to Create Opportunities for Dialogue About Sexual Health
A limitation of the historical response to STI prevention and control is that community stakeholders (e.g., families, schools and educators, faith-based organizations, and workplaces) lack the resources and capacity to engage in sexual health dialogue to improve STI outcomes. Thus, the committee concludes that elevating the promotion of sexual health in partnership with community stakeholders could create a fruitful avenue for improving STI outcomes. Nonetheless, more direction and support
are needed to empower communities to engage in such dialogue and to provide resources for tailoring messages and information to be appropriate for communities’ specific contexts, needs, and priorities.
Recommendation 12-3: The Centers for Disease Control and Prevention Division of STD Prevention should take steps to expand community knowledge of sexual health and promote actions that lead to a greater understanding of healthy sexuality by encouraging and supporting public dialogue and the adoption of evidence-based interventions in various community settings (families, schools, faith communities, community-based organizations, and workplaces).
3. BOLSTER EXISTING SYSTEMS AND PROGRAMS FOR RESPONDING TO STIs
Enhance Federal Leadership and Support
DSTDP provides critical leadership in guiding the nation’s federal STI response. The committee supports maintaining and enhancing this role, including encouraging DSTDP to be more assertive and, in some cases, more prescriptive in its grants to states and local jurisdictions to establish minimum national standards of data reporting and STI care. Furthermore, STI professionals, especially within state and local health departments, have critical knowledge and expertise that need to be the foundation of any efforts to improve the national response to STI prevention and control. For CDC and states to effectively prevent and control STIs, accurate STI surveillance is essential for understanding the epidemiology of reportable STIs. The surveillance data, however, are difficult to interpret because they rely on case reporting, which is ecologic, and periodic population-based studies are too small for meaningful subpopulation analyses.
Recommendation 12-4: The Centers for Disease Control and Prevention (CDC) should modernize its core sexually transmitted infection (STI) activities to strengthen the timely monitoring of STIs with less reliance on estimated rates based on case reports, to inform proper treatment of persons with STIs, and to increase consistency and accountability across jurisdictions. The committee recommends a three-pronged approach:
-
Modernize surveillance activities to enable more rapid release of data:
- Automate case reporting of reportable STIs.
- Release a preliminary STD Surveillance Report within 6 months of the reporting period, with a revised report later in the year.
-
- Explore the use of new data sources to capture STI incidence (critically, both cases and numbers tested), such as electronic medical records, commercial databases, health information exchanges, clinical and pharmacy data, social media/online searches, and artificial intelligence, and invest in better data integration efforts within the National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention (NCHHSTP).
- Develop a publicly available STI dashboard to raise public awareness and accountability.
-
Improve timeliness of the STI treatment guidelines:
- The CDC STI treatment guidelines should be updated and disseminated annually, and more frequently if necessary, to better address real-time changes to the STI epidemic and emerging treatments and technologies. The entirety of the guidelines should undergo comprehensive reviews no less frequently than every 5 years.
-
Increase accountability and establish new funding requirements:
- CDC should engage in a data standardization partnership across NCHHSTP and with grantees to develop and publish a core set of STI indicators with standardized definitions of terms. To promote the use of these standardized data, CDC should set a condition of awards for its funding programs to require that every grantee report surveillance and other data to CDC consistent with these new data standards.
- CDC should also make a condition of awards the requirement that states engage in a broad and meaningful stakeholder engagement process. This should include representatives of local health departments, heavily affected communities, health insurance programs and exchanges, federally qualified and other health centers, Ryan White HIV/AIDS Program recipients, Substance Abuse and Mental Health Services Administration recipients, and others to develop a multi-year state or major municipalities STI prevention and control plan that
- leverages disparate assets within the state or major municipalities for establishing STI prevention and care priorities, aligning STI and HIV priorities;
- establishes benchmarks; and
- creates a process for monitoring and reporting on progress toward achieving established benchmarks.
The committee recognizes the large differences in staff capacity across health departments and other impediments to rapid integration of reporting standards. Therefore, the proposed partnership should consider the current starting point and recommend phased implementation (if needed) to account for current serious limitations in the capacity to carry out surveillance and monitoring efforts at the state or local levels. Furthermore, the committee is not recommending a specific model for stakeholder engagement. HIV programs have long experience with HIV prevention community planning, as well as Ryan White services planning. DSTDP may consider ways to integrate STI consultation and resource allocation processes within these existing mechanisms or may determine that such an approach is inappropriate or not the best model, as critical STI stakeholders not involved in HIV planning processes would be excluded (see Chapter 12 for additional discussion).
Strengthen Local Efforts to Plan and Coordinate the STI Response
To ensure the delivery of comprehensive sexual health services, local jurisdictions need to conduct, and be held accountable for, a broad and meaningful stakeholder engagement process to identify the range of available community assets to support the STI response and establish prevention and care priorities for their jurisdictions based on needs assessments. Working in tandem with the preceding recommendation for CDC to require statewide STI prevention and control plans, the committee recommends:
Recommendation 12-5: The Centers for Disease Control and Prevention (CDC) should encourage local health departments to develop and implement comprehensive plans for sexually transmitted infection (STI) prevention and control. This should be done by funding key partners, such as the National Association of County and City Health Officials (NACCHO) and the National Coalition of STD Directors (NCSD), to develop resources and provide technical assistance to state and local health departments on how to conduct a meaningful stakeholder consultation process, how to develop a plan that offers strategic support for improving STI outcomes leveraging all available community assets, and how to monitor implementation and keep the public informed of progress toward achieving the plan’s objectives. The plans should do the following:
- Include community-wide needs assessments, oversampling high-priority populations, that determine the adequacy of available sexual health services in their jurisdictions and explore the creation of new, improved, and easier access points for sexual
- health promotion in a stigma-free environment, including STI screening and treatment services that take advantage of current rapid and self-testing technologies.
- Identify mechanisms to meet the needs of underserved and highly impacted populations.
- Establish formalized, funded relationships with trusted community-based organizations to deliver critical STI prevention and care services.
CDC, in collaboration with the National Network of STD Prevention Training Centers, NACCHO, and NCSD, should develop STI Resource Centers (SRCs) for clinical consultation, workforce development, and technical assistance to support the planning process and provide consultation to individual clinical STI providers. At a minimum, these SRCs should be operational at the level of state and large municipal jurisdictions.
Establish New Payment and Coverage Options to Close Gaps in Access to STI Coverage and Services
Effective public health efforts to control the transmission of infectious diseases benefit the whole population, yet many people are not reached by the current fragmented health care system. Many individuals experience financial barriers to STI screening and treatment services because of their insurance status, immigration status, and/or ability to afford copayments or coinsurance for treatment and services.
Recommendation 10-1: The Department of Health and Human Services and state governments should identify and support innovative programs to ensure that sexually transmitted infection (STI) prevention and treatment services are available through multiple venues and ensure that federal and state governments maximize access opportunities for individuals who face health care access barriers. Priority populations for these efforts should include persons ineligible for coverage, persons who face affordability barriers (including high out-of-pocket costs), and persons who will not access STI services without confidentiality guarantees (such as adolescents and young adults with insurance coverage through parents or guardians).
Approaches to be explored include special Medicaid initiatives, such as incentives to expand Medicaid or other options to fill coverage gaps, state plan amendments and waivers, the establishment of a federally
supported supplemental grant program to provide STI testing and treatment at no cost through various safety net programs, promulgation of new 340B Drug Pricing Program guidance to expand coverage for STI services (including for population-based expedited partner therapy and HIV PrEP services), and funding initiatives to support comprehensive sexual health clinics and new access points for sexual health services.
Support and Expand the STI Workforce
The workforce for STI prevention and treatment has not been adequately supported to meet the needs of the nation. Beyond STI specialists, the existing clinical health care workforce includes a large subset of practitioners and stakeholders who are traditionally not involved directly in sexual health service delivery.
Recommendation 11-1: Sexual health promotion should be operationalized and prioritized in practice guidelines and training curricula for U.S. health professionals. Sexually transmitted infection (STI) prevention and management should be incentivized and facilitated as a focus area of practice for both the clinical workforce and important segments of nonclinical public health and social services professionals. The committee recommends five programmatic priorities for implementing this recommendation:
- Clinical practice guidelines and benchmarks developed by health professional organizations should more heavily emphasize the importance of consistent delivery of recommended sexual health services (e.g., sexual histories, vaccinations, and routine STI screening). Relevant professional organizations include but are not limited to the American Medical Association, the National Medical Association, the American Nurses Association, the National League for Nursing, the Association of Nurse Practitioners, the American Academy of Physician Assistants, the American Academy of Pediatrics, the Society for Adolescent Health and Medicine, the American College of Physicians, the American Academy of Family Physicians, the American College of Obstetrics and Gynecology, the Infectious Diseases Society of America, and the HIV Medicine Association.
- Licensing bodies for primary care generalists (i.e., primary care physicians, nurse practitioners, physician assistants, and nurses) and behavioral health specialists should formulate a minimum sexual health skill set (e.g., taking a sexual history and understanding the basics of STI prevention, being aware
- of guidelines for STI screening and treatment, and understanding HIV prevention and care) to be reflected in formal training programs and yearly continuing medical education, continuing medical units, and continuing education requirements.
- The Centers for Disease Control and Prevention (CDC) and state and local health departments, in collaboration with STI/HIV expert providers and the regional STI prevention training centers, should serve as a resource of clinical expertise for primary care providers and nonclinical health and social services professionals and paraprofessionals. This should be accomplished through consultation, technical assistance, and continuing education (see also Recommendation 12-5).
- CDC should identify federal and state policy actions that would most effectively expand the available workforce to address STI prevention, screening, and treatment. Policies that identify new reimbursement models and promote the ability of advance practice clinicians, pharmacists, community health workers, and other health care workers to provide STI services should be identified and communicated to state policy makers and to encourage state legislatures to reduce or eliminate the scope of practice barriers.
- The Centers for Medicare & Medicaid Services, the Health Resources and Services Administration, CDC, and other agencies should explore public–private partnerships to address logistical and regulatory barriers to workforce expansion. The use of emerging technologies (e.g., point-of-care STI testing and treatment referrals) and delivery models (e.g., telehealth services, pharmacy-based health care) for sexual health services are two innovative examples that can extend the reach of the STI workforce.
Accelerate Research and Development for Biomedical Interventions
Recent scientific advances provide the means for improving STI diagnosis, but they are currently underused. Continuing evolution of antimicrobial resistance has threatened the continued efficacy and ease of STI treatment, especially for Neisseria gonorrhoeae. In addition, the pipeline for developing both new antimicrobials and vaccines for STI prevention has been constrained by an unfavorable business case that suggests the need for public engagement of the private sector, as has been done with HIV/AIDS and COVID-19. In the absence of ready access to reliable diagnostic tests, syndromic diagnosis for persons with genitourinary symptoms remains common, but it is imprecise, fails to address the frequent
occurrence of unrecognized infection, and is contrary to principles of good antimicrobial stewardship.
Recommendation 7-1: To improve the efficacy and reach of tools for sexually transmitted infection (STI) management and prevention, the National Institutes of Health should prioritize development of point-of-care (POC) diagnostic tests; development of diagnostic tests for active syphilis; promotion of public–private partnerships (PPPs) to develop new antimicrobials; and expedited development of vaccines. Specifically:
- POC diagnostics: Prioritize development of POC diagnostic tests to reduce the interval between testing and treatment. Use of these POC tests should be promoted to reduce opportunities for transmission. Optimally, POC tests should be inexpensive, rapid, and receive a Clinical Laboratory Improvement Amendments waiver to permit increased testing at sites providing health care or at home.
- New diagnostics for syphilis: Promote development of new, innovative diagnostic tests for active syphilis that distinguish untreated, active syphilis from previously treated infection, which is required to effectively control syphilis.
- Antimicrobials and vaccines for STI treatment and prevention: Subsidize and encourage PPPs with the goals of developing new, readily accessible antimicrobials for STI treatment and expediting development of vaccines for prevention of high-priority STIs such as chlamydia, gonorrhea, syphilis, and herpes.
Deploy Psychosocial and Behavioral Interventions for Sexual Health
Psychosocial and behavioral interventions to promote sexual health and prevent STIs are underused and have not been adopted and sustained in clinical or community practice. These interventions, in conjunction with biomedical, structural, informatics/technological, and health service interventions, are integral to a comprehensive strategy for sexual health and STI prevention and control. In addition, comprehensive sexual health education taught in schools is effective in delaying the initiation of sexual behavior, promoting sexual health, and reducing risk for STIs in students. School-based sexual health education programs across the United States are highly variable, with no nationwide policy on the subject. Community intervention strategies also can promote sexual health and prevent STIs,
including in racial and ethnic minorities and marginalized groups who live and socialize in high-STI-prevalence, low-resourced communities. Such approaches require sustained funding, however, and other supportive resources for them to be effective.
Recommendation 8-1: The Department of Health and Human Services (HHS) should take steps to expand the reach of psychosocial and behavioral interventions to prevent and control sexually transmitted infections at the individual, interpersonal, and community level. This can be accomplished by developing sustainable funding mechanisms to deliver those interventions; establishing standard guidelines for school-based comprehensive sexual health education; and developing, evaluating, and disseminating community-based approaches:
- HHS should develop new mechanisms that provide sustainable funding for dissemination, adoption, and scale up of evidence-based psychosocial and behavioral interventions by a wide range of stakeholders, including community-based organizations, parent–teacher associations, workplaces, faith-based organizations, and pediatric and primary care practices.
- The Centers for Disease Control and Prevention (CDC) Division of Adolescent and School Health should work in partnership with parents and guardians, parent–teacher associations, states, districts, and local school boards to establish standard evidence-based guidelines for school-based comprehensive sexual health education that is grounded in psychosocial and behavioral theories and research. To ensure that each student receives medically accurate, age-appropriate, and culturally inclusive comprehensive sexual health education in elementary, middle, and high school, dedicated staff, including school-based nurses and health educators, should be trained, provided adequate time, and given necessary resources.
- CDC, in collaboration with state and local departments of health, should develop and evaluate the efficacy of promising community-based approaches that are grounded in psychosocial and behavioral research, extend reach into affected communities, foster ongoing collaboration with community stakeholders for capacity building and sustainability, and provide allocation of sustained dedicated resources for formative work, intervention implementation, evaluation, replication, and scale up of evidence-based interventions.
4. EMBRACE INNOVATION AND POLICY CHANGES TO IMPROVE SEXUAL HEALTH
Address Structural Inequities, Including Structural Racism, That Hinder STI Prevention and Control
Structural inequities related to sexual orientation, gender identity, race and ethnicity, and national origin, among others, are pervasive, increase STI risk, perpetuate stigma, and undermine access to STI prevention and treatment among marginalized populations. Very few structural interventions that address STIs, including the effect of intermediary social determinants of health influenced by structural racism and other health inequities, have been developed. Examining and addressing the structural determinants of STIs and STI inequities will require bold vision. This vision needs to be bolstered by a long-term commitment with multidisciplinary, intersectoral, and interagency collaboration and supported through dedicated cross-agency funding from the National Institutes of Health, CDC, Health Resources and Services Administration, and private foundations and funders. This will demand steadfast political will at all levels of government and sustained community engagement and mobilization. Due to their focus on addressing the root causes of poor health and their downstream social determinants, these efforts stand to have the greatest impact on preventing STIs and STI inequities in the United States.
Recommendation 9-1: The Secretary of Health and Human Services (HHS) should acknowledge structural racism and other forms of structural inequities as root causes of sexually transmitted infection (STI) outcomes and inequities and as threats to sexual health.
HHS should lead a whole-of-government response that engages all relevant federal departments and agencies to develop a coordinated approach to reduce negative STI outcomes and address inequities in the U.S. population by promoting sexual health and eliminating structural inequities that are barriers to STI prevention, testing, and treatment among marginalized groups.
In mounting this response, the Secretary should:
- consult broadly with affected communities and critical stakeholders to conduct a national landscape analysis that assesses social and structural barriers that prevent access to STI services. The focus should be on identifying communities with high morbidity and limited access to affordable and desirable STI prevention and care services and resources in order to develop
- a national holistic plan for ongoing monitoring of the national STI infrastructure and STI burden, including interrelated structural and social determinants of health inequities;
- establish a priority research agenda, including a data-collection strategy that organizes data on STI outcomes and their structural and social determinants among marginalized populations;
- strengthen partnerships with, funding for, and technical assistance to state and local health departments and community-based organizations;
- foster greater collaboration across health and human services agencies; and
- report regularly to the public on progress for addressing STI outcomes and inequities.
Harness Technological Innovation to Improve STI Prevention and Control
To keep pace with the rapid advancements in technology and its effects on sexual health, it is essential that the field of public health implements policy based on three important considerations: (1) social media and mobile-app-based technological innovations have been primarily created by industry, and industry experts and companies needed to be included in the public health response to STIs; (2) tools based on artificial intelligence (AI) will become increasingly better at targeting individuals and changing their behaviors; and (3) the ethical considerations around technological tools are evolving faster than policies that can address issues of concern. Public health agencies need to frequently and regularly evaluate new tools and public views about them to determine the best course of action for the changing ethical landscape.
The question of whether new technologies pose STI transmission risk is no longer relevant, given that they are nearly ubiquitous and impossible to prevent. Instead, the relevant questions are how, why, when, and where these technologies increase risk; how, when, and where they can be leveraged to promote sexual health; and how public health can integrate this knowledge into daily STI prevention and control efforts to ensure safe and ethical oversight (see Chapter 6 for a discussion of implementation, cost, and feasibility considerations).
Recommendation 6-1: The Centers for Disease Control and Prevention (CDC) should expand its capacity to use technology for sexually transmitted infection (STI) prevention and control. To accomplish this, CDC should recruit seasoned individuals from the private and public sectors with experience in digital behavior
change and team science to work collaboratively with agency public health and marketing staff. It should develop timely and open data systems and deploy artificial intelligence–based mass marketing strategies to advance STI prevention.
Achieving this recommendation would entail that CDC undertake regular dialogue with leading industry and nonprofit experts, along with STI providers and community representatives; assess its STI data management capacity; and partner with state and local health departments to use highly targeted AI-based digital mass communication strategies to better address STIs.
CONCLUSION
Despite the dedicated commitment of many individuals and agencies, STI research, policy, and services continue to suffer from neglect. Relatively flat federal investments and declining state and local investments in the face of all-time high numbers of reported cases of STIs underscore the failure of the STI crisis to capture the attention of the public and policy makers. The committee’s exploration of the complexities of the challenge, however, has instilled in its members a firm belief that it is possible to create a different and better future where fewer people are infected, fewer babies are born with STIs, and people entering adolescence and continuing across the life span are taught the language and skills to conceptualize and enact their own vision for what it means to be sexually healthy.
The committee’s recommended changes are challenging, yet it is possible to reduce the impact of STIs on society and take the bold actions recommended in this report to prevent and control STIs in the immediate future and long term. In turn, this can create a positive and comprehensive sexual health platform, so that the United States can return to the ultimate task of planning for the elimination of these serious health threats.




















