4
The Role of Nurses in Improving Health Care Access and Quality
Of all the forms of inequality, injustice in health care is the most shocking and inhumane.
—Dr. Martin Luther King, civil rights activist
Health care equity focuses on ensuring that everyone has access to high-quality health care. As shown in the Social Determinants of Health and Social Needs Model of Castrucci and Auerbach (2019) (see Chapter 2), health care is a downstream determinant of health, but disparities in health care access and quality can
widen and exacerbate disparities produced by upstream and midstream determinants of health outcomes.
According to Healthy People 2020, access to quality health care encompasses the ability to gain entry into the health care system through health insurance, geographic availability, and access to a health care provider. Health care quality has been defined as “the degree to which health care services for individuals and populations increase the likelihood of desired outcomes and are consistent with current professional knowledge” (IOM, 1990, p. 4). The Agency for Healthcare Research and Quality (AHRQ) defines quality health care “as doing the right thing for the right patient, at the right time, in the right way to achieve the best possible results” (Sofaer and Hibbard, 2010). Nurses deliver high-quality care by providing care that is safe, effective, person-centered, timely, efficient, and equitable (IOM, 2001).
As noted, frameworks for social determinants of health (SDOH) place the health care system downstream, often operating in response to illness, rather than upstream, impacting the underlying causes of health outcomes (Castrucci and Auerbach, 2019). Therefore, health care itself does not address most of the upstream factors, or root causes of illness, that affect health equity; such upstream social factors as economic and housing instability, discrimination and other forms of racism, educational disparities, and inadequate nutrition can affect an individual’s health before the health care system is ever involved (Castrucci and Auerbach, 2019). Health equity is discussed in detail in Chapter 5. Some estimates indicate that a small portion of health outcomes is related to health care, while equity in health care is an important contributing factor to health equity (Hood et al., 2016; Remington et al., 2015).
Major shifts occurring both within society at large and within health care will transform the environment in which the next generation of nurses will practice and lead. These shifts encompass changing demographics, including declining physical and mental health; increased attention to racism and equity issues; the development and adoption of new technologies; and changing patterns of health care delivery. The widespread movement for racial justice, along with the stark racial disparities in the impacts of COVID-19, has reinforced the nursing profession’s ethical mandate to advocate for racial justice and to help combat the inequities embedded in the current health care system. The commitment to social justice is reflected in provision 9 of the Code of Ethics of the American Nurses Association (ANA, 2015), and its priority has been elevated by the increased demand for social justice within communities and society at large.
Changing health outcomes will require action at all levels—upstream, midstream, and downstream—and nurses have a major role at all levels in reducing gaps in clinical outcomes and improving health care equity. Nurses can strengthen their commitment to diversity, equity, and inclusion by leading large-scale efforts to dismantle systemic contributors to inequality and create new norms and competencies within health care. In that process, nurses will need to meet the
complex ethical challenges that will arise as health care reorients to respond to the rapidly changing landscape (ANA, 2020; Beard and Julion, 2016; Koschmann et al., 2020; Villarruel and Broome, 2020). To ensure nursing’s robust engagement with these major shifts in health care and society, investments in the well-being of nurses will be essential (ANA, 2015) (see Chapter 10).
This chapter examines ways in which nurses today work to improve health care equity, as well as their potential future roles and responsibilities in improving equity through efforts to expand access to and improve the quality of health care. Existing exemplars are also described, as well as implications of COVID-19 for health care access and quality.
NURSES’ ROLES IN EXPANDING ACCESS TO QUALITY HEALTH CARE
The United States spends more than $3.5 trillion per year on health care, 25 percent more per capita than the next highest-spending country, and under-performs on nearly every metric (Emanuel et al., 2020). Life expectancy, infant mortality, and maternal mortality are all worse in the United States than in most developed countries. In the United States, moreover, disparities in health care access and health outcomes are seen across racial lines; however, being able to use social and financial capital to buy the best health care is not necessarily associated with the world’s best health outcomes. Even among White U.S. citizens and those of higher socioeconomic status (SES), U.S. health indicators still lag behind those in many other countries (Emanuel, 2020). The U.S. population will not fully thrive unless all individuals can live their healthiest lives, regardless of their income, their race or ethnicity, or where they live. As discussed in Chapter 2, however, race and ethnicity, income, gender, and geographic location all play substantial roles in a person’s ability to access high-quality, equitable, and affordable health care. A variety of professionals from within and outside of health care settings participate in efforts to ensure equitable access to care. But the role of nurses in these efforts is key, given their interactions with individuals and families in providing and coordinating person-centered care for preventive, acute, and chronic health needs within health settings, collaborating with social services to meet the social needs of individuals, and engaging in broader population and community health through roles in public health and community-based settings.
Both in the United States and globally, the rapid growth in the number of older people in the population will likely lead to increased demand for services and programs to meet their health and social care needs (Donelan et al., 2019; Spetz et al., 2015), including care for chronic conditions, which account for approximately 75 percent of all primary care visits (Zamosky, 2013). The aging population will also bring change in the kinds of care the patient population will need. Older people tend to require more expensive care, and to need increasing
support in managing multiple conditions and retaining strength and resilience as they age (Pohl et al., 2018). These realities underscore the importance of designing, testing, and adopting chronic care models, in which teams are essential to managing chronic disease, and registered nurses (RNs) play a key role as chronic disease care managers (Bodenheimer and Mason, 2016). Studies of exemplary primary care practices (Bodenheimer et al., 2015; Smolowitz et al., 2015) define key domains of RN practice in primary care, including preventive care, chronic illness management, practice operations, care management, and transition care.
Since the passage of the Patient Protection and Affordable Care Act, substantial changes have occurred in the organization and delivery of primary care, emphasizing greater team involvement in care and expansion of the roles of each team member, including RNs (Flinter et al., 2017). Including RNs as team members can increase access to care, improve care quality and coordination for chronic conditions, and reduce burnout among primary care practitioners by expanding primary care capacity (Fraher et al., 2015; Ghorob and Bodenheimer, 2012; Lamb et al., 2015).
In primary care, RNs can assume
at least four responsibilities: 1) Engaging patients with chronic conditions in behavior change and adjusting medications according to practitioner-written protocols; 2) Leading teams to improve the care and reduce the costs of high-need, high-cost patients; 3) Coordinating the care of chronically ill patients between the primary care home and the surrounding healthcare neighborhood; and 4) Promoting population health, including working with communities to create healthier spaces for people to live, work, learn, and play. (Bodenheimer and Mason, 2016, pp. 11–12)
Findings from a 2013 study of The Primary Care Team: Learning from Effective Ambulatory Practices (LEAP) suggest that a large majority of LEAP primary care practices, regardless of practice type or corporate structure, use RNs as a key part of their care team model (Ladden et al., 2013). This contrasts with a study of 496 practices in the Centers for Medicare & Medicaid Services (CMS) Comprehensive Primary Care initiative (Peikes et al., 2014) that found that only 36 percent of practices had RNs on staff, compared with 77 percent of LEAP sites (Flinter et al., 2017).
The health needs of individuals exist across a spectrum, ranging from healthy people, for whom health promotion and disease prevention efforts are most appropriate, to people who have limited functional capacity as a result of disabilities, severe or multiple chronic conditions, or unmet social needs or are nearing the end of life. Access to quality health care services is an important SDOH, and equitable access to care is needed for “promoting and maintaining health, preventing and managing disease, reducing unnecessary disability and premature death, and achieving health equity” (ODPHP, 2020). Likewise, “strengthening
the core of primary care service delivery is key to achieving the Triple Aim of improved patient care experiences, better population health outcomes, and lower health care costs” (Bodenheimer and Mason, 2016, p. 23). The 2011 The Future of Nursing report echoes these themes:
while changes in the healthcare system will have profound effects on all providers, this will be undoubtedly true for nurses. Traditional nursing competencies, such as care management and coordination, patient education, public health intervention, and transitional care, are likely to dominate in a reformed healthcare system as it inevitably moves toward an emphasis on prevention and management rather than acute [hospital] care. (IOM, 2011, p. 24)
Given the increased evidence supporting the focus on addressing social needs and SDOH to improve health outcomes, these competencies are even more important a decade later. While progress has been made, there is still work to be done, and leveraging and expanding the roles and responsibilities of nurses can help improve access to care (Campaign for Action, n.d.).
For people who have difficulty accessing health care because of distance, lack of providers, lack of insurance, or other reasons, nurses are a lifeline to care that meets them where they are. Nurses work in areas that are underserved by other health care providers and serve the uninsured and underinsured. They often engage with and provide care to people in their homes, they work in a variety of clinics, they use telehealth to connect with people, and they establish partnerships and create relationships in schools and communities. In addition to expanding the capacity of primary care, nurses serve in vital roles during natural disasters and public health emergencies, helping to meet the surge in the need for care (see Chapter 8). Yet, the potential for nurses to advance health equity through expanded access to care is limited by state and federal laws and regulations that restrict nurses’ ability to provide care to the full extent of their education and training (see Chapter 3). Ways in which nurses can fulfill this potential to increase access to care for populations with complex health and social needs are discussed below.
INCREASING ACCESS FOR POPULATIONS WITH COMPLEX HEALTH AND SOCIAL NEEDS
Many individuals cannot access health care because of lack of insurance, inability to pay, and lack of clinics or providers in their geographic area. To bridge this gap, access to care is expanded through a variety of settings where nurses work, including federally qualified health centers (FQHCs), retail clinics, home health and home visiting, telehealth, school nursing, and school-based health centers, as well as nurse-managed health centers. Across all of these settings, nurses are present and facilitate access to health services for individuals and families, often serving as a bridge to social services as well.
Federally Qualified Health Centers
Through FQHCs—outpatient facilities located in a federally designated medically underserved area or serving a medically underserved population—nurses expand access to services for individuals regardless of ability to pay by helping to provide comprehensive primary health care services, referrals, and services that facilitate access to care. The role of advanced practice registered nurses (APRNs) in FQHCs has grown over time (NACHC, 2019). The emerging role of RNs in FQHCs is seen in increased interactions with patients, involvement in care management, and autonomy in the delivery of care. Nurses also work to address key social factors in partnership with care coordinators, health coaches, and social workers to improve health outcomes (Flinter et al., 2017).
Retail Clinics
Health care delivery in the United States has been undergoing transformation, and these changes provide new opportunities for more patients and greater access to nurses as new policies are implemented, new payment models take hold, resources are focused on SDOH, and consumerism shapes care choices. One change in particular since the prior The Future of Nursing report (IOM, 2011) has been and will continue to be impactful for nursing: the emergence of nontraditional health care entities, such as retail clinics. The evolution and rapid growth of these established retail clinics provide increased accessibility of basic care, health screenings, vaccines, and other services for some populations (Gaur et al., 2019). The number of such is growing rapidly, from around 1,800 in 2015 to 2,700 operating in 44 states and the District of Columbia by 2018.
Retail clinics provide more accessible primary care for some populations. In 2016, 58 percent of retail clinic visits represented new utilization instead of substitution for more costly primary care or emergency department visits (Bachrach and Frohlich, 2016). Many individuals and families use retail clinics for their convenience, which includes long hours of operation, accessible location, and walk-in policies, as well as low-cost visits. These attributes are important for those with lower income or without insurance who may not have a regular source of care or be able to access a primary care provider (Bachrach and Frohlich, 2016). However, research shows retail clinics are typically placed in higher-income, urban, and suburban settings with higher concentrations of White and fewer Black and Hispanic residents (RAND Corporation, 2016). The RAND Corporation (2016) study found that while 21 percent of the U.S. population lived in medically underserved areas, only 12.5 percent of retail clinics were located in these areas. RAND concluded that “overall, retail clinics are not improving access to care for the medically underserved.” Thus, while these new models of care have the potential to advance health care equity and population-level health, the available data do not indicate that this potential has been realized (RAND
Corporation, 2016). The equity impact of these retail clincs depends in large part on who utilizes the services, and whether the utilization patterns are similar to or different from those of traditional health care.
Retail clinics are staffed largely by nurse practitioners (NPs) (Carthon et al., 2017). These clinics in pharmacies and grocery stores often have been constrained by restrictive scope-of-practice laws. In 2016, a study by the University of Pennsylvania School of Nursing’s Center for Health Outcomes and Policy Research investigated scope-of-practice regulatory environments and retail-based clinic growth. Looking at three states with varying levels of scope-of-practice restrictions, the study found an association between relaxation of practice regulations and retail clinic growth. Evidence suggests that optimization of innovative health care sites such as retail clinics will require moving toward the adoption of policies that standardize the scope of practice for NPs, the providers who largely staff retail clinics (Carthon et al., 2017).
Home Health and Home Visiting
Visiting people in their homes can advance equitable access to quality health care. Home health care has increased access to care for many Americans, from older individuals to medically fragile children. Yao and colleagues (2021) recently explored trends in the U.S. workforce providing home-based medical care and found that less than 1 percent of physicians participating in traditional Medicare provide more than 50 home visits each year (a rate unchanged between 2012 and 2016). By contrast, the number of NPs providing home visits nearly doubled during that same period. Home health nurses address a fragmented system by coordinating care for patients transitioning from a tertiary care facility to ongoing health care within their own homes. Since the onset of the COVID-19 pandemic, these nurses have increasingly provided families with respite for caregivers and offered mental health services in many forms, but certainly in decreasing social isolation for elderly people. Delivering care at home has offered a window for physicians and NPs to see where patients live, to engage in telehealth video calls with family members present, and to see the features of neighborhoods that impact health (e.g., sidewalks, playgrounds, stairs).
With the expansion in the home health care industry driven by an aging population, home visiting nurses are essential to providing care and enhancing health care equity (Walker, 2019). Prior to 2020, Medicare rules allowed only physicians to order home health services for Medicare beneficiaries. However, the Coronavirus Aid, Relief, and Economic Security (CARES) Act permanently authorizes physician assistants and NPs to order home health care services for Medicare patients. In addition, CMS has instituted new policies outlining comprehensive temporary measures for increasing the capacity of the U.S. health care system to provide care to patients outside a traditional hospital setting amid the rising number of COVID-19-related hospitalizations nationwide. These measures include
both the Hospital Without Walls and Acute Hospital Care At Home programs, both initiated during the pandemic. Under previous federal requirements, hospitals had to provide services within their own buildings, raising concerns about capacity for treating COVID-19 patients, especially those requiring ventilator and intensive care. Under CMS’s temporary new rules, hospitals can transfer patients to outside facilities, such as ambulatory surgery centers, inpatient rehabilitation hospitals, hotels, and dormitories, while still receiving hospital payments under Medicare. Provision for at-home care, which is often preferred by patients, is especially important during a crisis such as the pandemic, when hospital care means family and/or caregivers cannot be present. Moreover, some research has shown home care to be less costly and to result in fewer readmissions relative to hospital care (Levine et al., 2020). These programs also will create new demand for nurses to work in the community and are the types of adaptations that occurred as a result of the COVID-19 pandemic that should remain permanent to expand high-quality access to care.
The locus of care delivery will continue to follow personal preferences of individuals and families. To improve health care access, nurses will need to be intentional about meeting patients where they are in the most literal sense, and to serve as advocates with and within public health, retail clinics, and health systems to ensure that patients can access the care they need in their homes and neighborhoods. Box 4-1 describes several innovative nurse-led, in-home care programs.
In addition to home health, nurse home visiting programs often include such services as health check-ups, screenings, referrals, and guidance in navigating other programs and services in the community (Child and Family Research Partnership, 2015). Growing evidence suggests that home visits by nurses during pregnancy and in the first years of a child’s life can improve the health and well-being of both child and family, including by promoting maternal and child health, prevention of child abuse and neglect, positive parenting, child development, and school readiness. This positive impact has been found to continue into adolescence and early adulthood (NASEM, 2019).
Telehealth
The proliferation of mobile devices and applications offers an opportunity for nurses to use telehealth more broadly to connect with individuals. Telehealth, including video visits, email, and distance education, serves as a tool to connect with people on an ongoing basis without their having to leave their homes, workplaces, or other settings, and allows for long-distance patient and clinician contact for purposes of clinical interventions, health promotion, education, assessment, and monitoring. The use of telehealth is especially helpful for those who have difficulty traveling to obtain care and those who reside in rural or remote areas. Vulnerable populations with multiple chronic illnesses, poor health literacy, and lack of supportive resources may benefit the most from telehealth use. However, use of telehealth or virtual health tools is limited by access to reliable Internet
connections and the availability of the necessary hardware, including smartphones, computers, or webcams. A recent report in the Journal of the American Medical Association looks at 41 FQHCs serving 1.7 million patients. Prior to the COVID-19 pandemic, there was minimal telehealth use at these facilities. During March 2020, FQHCs rapidly substituted in-person visits with telephone and video visits. For primary care, however, 48.5 percent of telehealth visits occured by telephone and 3.4 percent by video. In addition, CMS estimated that 30 percent of telehealth visits were audio-only during the pandemic. These numbers indicate that telehealth appointments for lower-income Americans were in large part audio-only, raising questions about the quality of care (Uscher-Pines et al., 2021).
There have been examples of telehealth activities that have demonstrated great success. The Mississippi Diabetes Telehealth Network, for example, implemented a program that uses telehealth in the home as a viable way to bring a care team to patients to assist them as they manage their illnesses. NPs provide daily health sessions and remote monitoring for individuals with diabetes (Davis et al., 2020; Henderson et al., 2014). A prospective, longitudinal cohort study design evaluated the relationship between using telehealth for chronic care management and diabetes outcomes over a 12-month period, finding a significant difference in HbA1c values from baseline to 3-, 6-, 9-, and 12-month values (Davis et al., 2020). In another example, Mercy Hospital, a virtual care center, delivers telehealth services to rural communities in Arkansas, Kansas, Missouri, and Oklahoma. One of its many services is Nurse on Call, which provides timely clinical advice and is available around the clock. In still another example, Banner Health’s skilled nursing model delivers home care combined with telehealth services to people at home instead of their having to move to a nursing home facility (Roth, 2018).
School Nursing
School nurses are front-line health care providers, serving as a bridge between the health care and education systems. Hired by school districts, health departments, or hospitals, school nurses attend to the physical and mental health of students in school. As public health sentinels, they engage school communities, parents, and health care providers to promote wellness and improve health outcomes for children. School nurses are essential to expanding access to quality health care for students, especially in light of the increasing number of students with complex health and social needs. Access to school nurses helps increase health care equity for students. For many children living in or near poverty, the school nurse may be the only health care professional they regularly access.
School nurses treat and help students manage chronic health conditions and disabilities; address injuries and urgent care needs; provide preventive and screening services, health education, immunizations, and psychosocial support; conduct behavioral assessments; and collaborate with health care providers,
school staff, and the community to facilitate the holistic care each child needs (Council on School Health, 2008; Holmes et al., 2016; HRSA, 2017; Lineberry and Ickes, 2015; Maughan, 2018). By helping students get and stay healthy, school health programs can contribute to closing the achievement gap (Basch, 2011; Maughan, 2018). According to Johnson (2017),
Healthy children learn better; educated children grow to raise healthier families advancing a stronger, more productive nation for generations to come. School nurses work to assure that children have access to educational opportunities regardless of their state of health. (p. 1)
Meeting the mental health needs of children can be particularly challenging. Researchers estimate that about a quarter of all school-age children and adolescents struggle with mental health issues, such as anxiety and depression. Approximately 30 percent of student health visits to the school nurse are for mental health concerns, often disguised by complaints of headaches and stomachaches (Foster et al., 2005). School nurses have experience with screening students at risk for a variety of such concerns and can assist students in addressing them (NASN, 2020a). However, most youth—nearly 80 percent—who need mental health services will not receive them (Kataoka et al., 2005); schools are not always equipped to deal with students’ emotional needs, and parents often lack the awareness or resources to get help for their children. Additionally, a recent study found disparities in access to mental health treatment for students along racial and ethnic lines (Lipson et al., 2018), and structural racism undergirds many risk factors for mental illness (see Chapter 2). The COVID-19 pandemic has revealed—and exacerbated—inequities among children of different incomes and races/ethnicities. School closures and social isolation have affected all students, but especially those living in poverty. In addition to the damage to student learning, the loss of access to mental health services that were offered by schools has resulted in the emergence of a mental health crisis (Leeb et al., 2020; Patrick et al., 2020; Singh et al., 2020).
Schools are increasingly being recognized not just as core educational institutions but also as community-based assets that can be a central component of building healthy and vibrant communities (NASEM, 2017). Accordingly, schools and, by extension, school nurses are being incorporated into strategies for improving health care access, serving as hubs of health promotion and providers of population-based care (Maughan, 2018). Yet, while there have been calls for every school to have access to a nurse (Council on School Health, 2016; NASN, 2020b), only 39.9 percent of schools employed a full-time nurse in 2017. The remainder of schools (39.3 percent) employed a part-time nurse or did not employ a nurse at all (25.2 percent) (Willgerodt, 2018). The availability and staffing levels of school nurses vary greatly by geography (Willgerodt, 2018) (see Figure 4-1).
To address the lack of health care resources in rural school settings, telehealth programs have been implemented with success (RHI, 2019). An example is
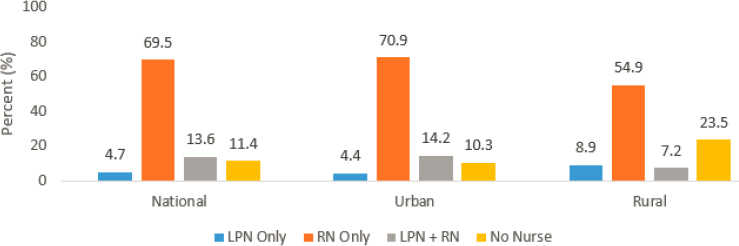
SOURCE: Data from Willgerodt, 2018.
Health-e-Schools, in which onsite school nurses connect sick students with health care providers. The program employs a full-time, off-site family NP who uses telehealth to evaluate and diagnose patients with such health issues as earaches, sore throats, colds, and rashes, as well as to provide sports physicals, medication, chronic disease management, and behavioral health care. It began as a telehealth program implemented by only 3 schools in 2011 and has since expanded to more than 80 schools serving more than 25,000 students. Health-e-Schools has helped increase classroom attendance and decrease the amount of time parents or guardians must take off from work to bring their children to appointments. This model relies heavily on the school nurses employed within each school district to serve as primary telehealth providers, thus requiring that funding be allocated to provide a school nurse in each school.
School-Based Health Centers
School-based health centers (SBHCs) also make care accessible to students in the school setting. In 2017, 2,584 SBHCs were operating in the United States (Love et al., 2019). SBHCs often operate as a partnership between the school and a community health organization, such as a community health center, hospital, or local health department; more than half are supported by or are an extension of FQHCs (SBHA, n.d.). SBHC services include primary care, mental health care, social services, dentistry, and health education, but vary based on community needs and resources as determined through collaborations among the community, the school district, and health care providers (CPSTF, 2015; HRSA, 2017). Services are provided by interprofessional teams of health care professionals that include nurses, mental health care providers, physicians, nutritionists, and others. As of 2017, NPs provided primary care services onsite and through telehealth services at 85 percent of SBHCs (Love et al., 2019; SBHA, 2018).
One example of an SBHC is the nurse-run Vine School Health Center (VSHC) located at the Vine Middle Magnet School in Knoxville, Tennessee, a
Title I school where 100 percent of the students qualify for free lunch. VSHC provides onsite and telehealth services to anyone up to 21 years of age who lives in the county. It also serves 10 other Title I schools through direct health care or telehealth services. The clinic is a partnership between the University of Tennessee College of Nursing and Knox County Schools and is staffed by nurses, nursing students, social workers, and special education professionals. Staff assist families with social needs, including food, housing, clothing, linkages to health insurance, and financial support for rent and utilities (AAN, 2015; Pittman, 2019). Services rendered during the 2016–2017 school year included 1,110 early and periodic screening, diagnostic and treatment (EPSDT) exams; 1,896 immunizations; 4,455 physical health visits; and 1,796 mental health clinic visits. VSHC estimates that its services enabled the avoidance of more than 2,500 potential emergency room visits per academic year, associated with savings of about $375,000 per year (AAN, 2015).
IMPROVING THE QUALITY OF HEALTH CARE
Access to comprehensive health care services is a precursor to equitable, quality health care. Nurses are uniquely qualified to help improve the quality of health care by helping people navigate the health care system, providing close monitoring and follow-up across the care continuum, focusing care on the whole person, and providing care that is culturally respectful and appropriate. Nurses can help overcome barriers to quality care, including structural inequities and implicit bias, through care management, person-centered care, and cultural humility.
Care Management
In the current health care system, care is often disjointed, with processes varying between primary and specialty care and between traditional and emerging care sites. People may not understand the processes of the health care system, such as where they will receive care, how to make appointments, or the various providers with whom they may come into contact. Perhaps most important, patients may not understand why all the providers across settings where they receive care should be knowledgeable about the services they receive and the problems that have been identified to ensure seamless, continuous high-quality care. Social factors affecting people with complex health needs may also adversely affect their ability to receive optimal care. Care management, care coordination, and transitional care are activities that nurses perform as members of a health care team to decrease fragmentation, bolster communication, and improve care quality and safety. A care management approach is particularly important for people with complex health and social needs, who may require care from multiple providers, medical follow-up, medication management, and help in addressing their social needs.
Care management—a set of activities designed to “enhance coordination of care, eliminate duplication of services, reduce the need for expensive medical services, and increase patient engagement in self-care”—helps ensure seamless care (CHCS, 2007; Goodell et al., 2009). The components of care management include care coordination, transitional care, and social care.
Care coordination is defined as the “deliberate organization of patient care activities between two or more participants (including the patient) involved in a patient’s care to facilitate the appropriate delivery of healthcare services.” It is needed both to overcome obstacles of the health care system, such as fragmentation, communication, and billing/cost, and to increase access (McDonald et al., 2007, p. 4).
Transitional care entails coordinating care for people moving between various locations or levels of care, providing navigation, coordination, medication reconciliation, and education services (Storfjell et al., 2017). The Transitional Care Model, developed by Mary Naylor (see Box 4-2), and the Care Transitions Intervention, developed by Eric Coleman, are prominent nurse-centered care models focused on the often disjointed transition from an inpatient hospital stay to follow-up ambulatory care. Both models engage people with chronic illness from hospitalization to postdischarge, and employ a nursing coach or team “to manage clinical, psychosocial, rehabilitative, nutritional and pharmacy needs; teach or coach people about medications, self-care and symptom recognition and management; and encourage physician appointments” (Storfjell et al., 2017, p. 27). Both reduce readmissions and costs (Storfjell et al., 2017).
Health care delivery models that incorporate social care have created critical roles for nurses in coordinating care across providers and settings and collaborating with other professionals and community resources to improve the health of individuals with complex health and social needs. Chapter 5 provides examples of nurse-centered programs incorporating social care. Nurses are vital to carrying out these functions of care management. Common to nurses’ roles are functions including providing care coordination, developing care plans based on a person’s needs and preferences, educating people and families within care settings and during discharge, and facilitating continuity of care for people across settings and providers (ANA, n.d.).
Person-Centered Care
The person-centered care model embraces personal choice and autonomy and customizes care to an individual’s abilities, needs, and preferences (Kogan et al., 2016; Van Haitsma et al., 2014). Through person-centered care, nurses collaborate with people, including the patient and other care team members, to deliver personalized quality care that addresses physical, mental, and social needs (CMS, 2012; Terada et al., 2013). Features of person-centered care include an emphasis on codesign of interventions, services, and policies that focus on what the person and
community want and need; respect for the beliefs and values of people; promotion of antidiscriminatory care; and attention to such issues as race, ethnicity, gender, sexual identity, religion, age, socioeconomic status, and differing ability status (Santana et al., 2018). And person-centered care focuses not only on the individual but also on families and caregivers, as well as prevention and health promotion. Integrating person-centered care that improves patient health literacy is necessary to ensure patient empowerment and engagement and maximize health outcomes. Health literacy ensures that “patients know what they must do after all health care encounters to self-manage their health” (Loan et al., 2018, p. 98).
Research has demonstrated the efficacy of person-centered care, for example, in reducing agitation, neuropsychiatric symptoms, and depression, as well as improving quality of life, for individuals with dementia (Kim and Park, 2017). In another example, people with acute coronary syndrome receiving person-centered care reported significantly higher self-efficacy (Pirhonen et al., 2017). Person-centered care is person-directed, such that people are provided with sufficient information to help them in making decisions about their care and increase their level of engagement in care (Pelzang, 2010; Scherger, 2009), and nurses who engage people in their care are less likely to make mistakes (Leiter and Laschinger, 2006; Prins et al., 2010; Shiparski, 2005). Person-centered care leads to better communication between patients and caregivers and improves quality of care, thereby increasing patient satisfaction, care adherence, and care outcomes (Hochman, 2017).
Cultural Humility
As discussed in Chapter 2, implicit bias can lead to discrimination against others. In particular, structural racism in health care compromises the ability to deliver culturally competent care (Evans et al., 2020).
Historically, nursing has been at the forefront of advocacy, and there are many examples of how nurses have addressed, and are addressing, inequities in many aspects of our teaching, research, scholarship, and practice. Yet, there remain too many examples of structural racism throughout nursing and we must be open to continuing to examine, identify, and change these within our own profession. (Villaruel and Broome, 2020, p. 375)
Nurses may contribute to structural inequities in how they facilitate or hamper access to quality health care services since they are frequently the first point of contact for many individuals who need care. Cultural humility—“defined by flexibility; awareness of bias; a lifelong, learning-oriented approach to working with diversity; and a recognition of the role of power in health care interactions” (Agner, 2020, p. 1)—is therefore essential for nurses.
Cultural humility enables nurses to participate in more respectful partnerships with patients in order to advance health care equity. According to Foronda and colleagues (2016), cultural humility has been found to result in effective
treatment, decision making, communication, and understanding; better quality of life; and improved care. In contrast, clinicians with implicit bias may show less compassion toward and spend less time and effort with certain patients, leading to adverse assessment and care (Narayan, 2019). Because implicit bias can negatively affect patient interactions and health outcomes, it is important for nurses to be aware of their bias and how it may directly or indirectly impact patient interactions and the quality of care they provide (Hall et al., 2015).
Multiple strategies exist to help nurses achieve cultural humility and manage implicit bias to ensure that they provide high-quality, equitable care. Chapter 7 details the importance of incorporating cultural humility in nursing education. Instead of focusing broadly on the general population, quality improvement interventions characterized by cultural humility focus on needs that are unique to people of color (POC) and tailor care to overcome cultural and linguistic barriers that cause disparities in care (Green et al., 2010). With this approach, data on disparities are used to assess an intervention, with an emphasis on addressing barriers that are specific to underrepresented groups (ANA, 2018; Green et al., 2010; Villarruel and Broome, 2020). Box 4-3 describes culturally and linguistically appropriate services, designed to equip nurses with the knowledge, skills, and awareness to provide high-quality care for all patients regardless of cultural or linguistic background.
When nurses are educated and empowered to act at multiple levels—upstream, midstream, and downstream—they help reduce the effects of structural inequities generated by the health care system. This includes education about how structural inequities may affect their practice environments (as well as research and policy) and, by association, the people with whom they work in clinical and community-based settings (see the detailed discussion of nursing education in Chapter 7).
IMPLICATIONS OF COVID-19 FOR HEALTH CARE EQUITY
The COVID-19 pandemic has highlighted the pivotal role of nurses in addressing health care equity. During public health emergencies, nurses in hospitals and in public health and other community settings need to function collaboratively and seamlessly. The pandemic has heightened the need for team-based care, infection control, person-centered care, and other skills that capitalize on the strengths of nurses (LaFave, 2020). Broadening of scope-of-practice regulations and expansion of telehealth services during the COVID-19 pandemic have allowed nurses to practice to the full extent of their education and training, providing equitable care and increasing access to care.
The surge of critically ill people due to the pandemic created the need to rapidly increase the capacity of the health care workforce, especially to replenish workforce members who needed to quarantine or take time to care for sick family members or friends (Fraher et al., 2020). In response, multiple governors issued executive orders expanding the scope of practice for NPs. As of April 10, 2020, five states (Kentucky, Louisiana, New Jersey, New York, and Wisconsin) had temporarily suspended all practice agreement requirements, providing NPs with full practice authority (AANP, 2020). Thirteen states (Alabama, Arkansas, Indiana, Massachusetts, Michigan, Mississippi, Missouri, Oklahoma, Pennsylvania, South Carolina, Tennessee, Texas, and West Virginia) had enacted a temporary waiver of selected practice agreement requirements. By December 7, 2020, executive orders had expired for Kansas, Michigan, and Tennessee, and all practice agreement requirements had been temporarily suspended for Kentucky, Louisiana, New Jersey, New York, Virginia, and Wisconsin (AANP, 2020). Maintaining these broadened scopes of practice for nurses after the pandemic has ended would increase NPs’ opportunities to increase access to quality health care for individuals with complex health and social needs.
Hospitals are also redeploying health care workers—physicians, NPs, nurses, and others—from areas with decreasing patient volumes (resulting from, for example, limitations on elective procedures) to higher-need intensive care unit (ICU), acute care, and emergency service areas. For example, nurse anesthetists have been redeployed from operating rooms to ICUs to intubate and place central lines for patients in the surge response to COVID-19 (Brickman et al., 2020). As of December 2020, CMS was finalizing changes that allow NPs to “supervise the
performance of diagnostic tests within their scope of practice and state law, as they maintain required statutory relationships with supervising or collaborating physicians” (CMS, 2020a). These changes will help make permanent some of the workforce flexibilities that were allowed during the pandemic.
Although much attention has been paid to the dire need for health care supplies and hospital beds to treat patients with severe cases of COVID-19, less attention has been directed at impacts of the pandemic on communities; their ability to weather the crisis; and individuals’ physical, mental, and social health. Nurses, including public health nurses, working in and with communities continue to be critical to efforts to contain the COVID-19 pandemic, as well as other pandemics that may occur in the future.
Older Adults
Older adults have been disproportionately affected by COVID-19, and older POC are even more likely to experience disproportionate morbidity and mortality. CMS data show that Black Medicare beneficiaries were hospitalized four times as often and contracted the virus nearly three times as often compared with Whites of similar age (CMS, 2020b; Godoy, 2020). According to the Centers for Disease Control and Prevention (CDC), 8 of 10 deaths from COVID-19 in the United States have been among adults 65 and older (Freed et al., 2020). Nursing homes have been particularly hard hit and faced multiple unique challenges in serving those most vulnerable to the virus.
The pandemic has had significant emotional, social, and mental health effects on older adults and their caregivers, and nurses and nursing assistants in nursing homes have borne a great burden in carrying out the front-line work of trying to keep residents healthy, care for recovered patients, and help mitigate isolation and its detrimental effects on residents. These tasks in many cases have been performed in the absence of residents’ family members and friends, who have not been allowed to visit as part of efforts to prevent the spread of infection. Inside nursing homes, the nursing staff have had to act as both caregivers and confidants, carrying out their usual tasks while also supporting many residents through confusion, depression, and suicidal ideation. In multigenerational homes, additional steps have been required to mitigate COVID-19 risk for older adults, such as using separate bathrooms, wearing masks within the household if someone is sick, or avoiding visitors. Demand for home health nursing services, inclusive of following strict public health measures (masks, handwashing, quarantining), has increased during the pandemic.
Changes in Medicare policy during the COVID-19 pandemic have given older adults greater access to a variety of mental health services, including those provided in their homes. Access to telehealth has also been expanded to meet the urgent need to provide safe access to care. Medicare payment for telehealth visits in nursing homes was previously restricted to rural areas, but under the
1135 waiver and the Coronavirus Preparedness and Response Supplemental Appropriations Act, CMS temporarily broadened access to telehealth services to ensure that Medicare beneficiaries could access services from the safety of their homes (CMS, 2020b). Accordingly, NPs and other health care professionals have used telehealth to screen people for COVID-19 and treat noncritical illnesses that can be managed at home.
Telehealth also has helped address concerns about workforce capacity for adult health care due to the surging numbers of COVID-19 cases and reports of exposure among health care workers: “as many as 100 health care workers at a single institution have to be quarantined at home because of COVID-19” (Hollander and Carr, 2020). NPs who are quarantined because of exposure can provide telehealth services. It is important to note that the barriers discussed earlier due to restrictive scope-of-practice regulations may include limitations on providing telehealth services across state lines. Recognition of clinical licenses across states, such as through interstate agreements, could ease these barriers (NQF, 2020).
Children
Although CDC has reported that COVID-19 poses a relatively low risk for children, research on natural disasters has shown that, compared with adults, children are more vulnerable to the emotional impact of traumatic events that disrupt their daily lives. The pandemic has required that children make significant adjustments to their routines (e.g., because of school and child care closures and the need for social distancing and home confinement), disruptions that may interfere with a child’s sense of structure, predictability, and security. Young people—even infants and toddlers—are keen observers of people and environments, and they notice and react to stress in their parents and other caregivers, peers, and community members (Bartlett et al., 2020). While most children eventually return to their typical functioning when they receive consistent support from sensitive and responsive caregivers, others are at risk of developing significant mental health problems, including trauma-related stress, anxiety, and depression. Children with prior trauma or preexisting mental, physical, or developmental problems, as well as those whose parents struggle with mental health disorders, substance misuse, or economic instability, are at especially high risk for emotional disturbance. Thus, in addition to keeping children physically safe during a public health emergency such as the COVID-19 pandemic, it is important to care for their emotional health (Bartlett et al., 2020).
Barriers to mental health care result in serious immediate and long-term disadvantages for young people, especially students of color. Mental health—a key component of children’s healthy development—was already a growing concern prior to the pandemic and the concurrent nationwide protests in response to racial injustice and anti-Black racism, with the demand for mental health
services among U.S. adolescents increasing in the past decade (Mojtabai et al., 2020). This concern has been fueled by increases in the incidence of anxiety and depression, as well as a trend in which victims of suicide have been younger. As noted earlier, programs such as Nurse-Family Partnership (see Box 4-1), as well as school nurses and school-based health centers, represent channels through which nurses can assist children and families with health care access to address mental health needs.
The health care system is being transformed by an increased focus on community-based coordinated care and the use of technology to improve communication so as to achieve better population health outcomes at lower cost. At the local level, providers in public health and school settings can collaborate strategically to increase their community’s capacity to address the root causes of illness and improve overall population health by implementing broad social, cultural, and economic reforms that address SDOH. Such collaboration can benefit the entire health care system by leading to seamless care, reducing duplicative services, and lowering the costs of care.
CONCLUSIONS
Whether in an elementary school, a hospital, or a community health clinic, nurses work to address the root causes of poor health. As the largest and consistently most trusted members of the health care workforce, nurses practice in a wide range of settings. They have the ability to manage as well as collaborate within teams and connect clinical care, public health, and social services while building trust with communities. However, nurses are limited in realizing this potential by state and federal laws that prohibit them from working to the full extent of their education and training. The COVID-19 pandemic in particular has revealed that the United States needs to do a much better job of linking health and health care to social and economic needs, and nurses are well positioned to build that bridge.
Conclusion 4-1: Nurses have substantial and often untapped expertise to help individuals and communities access high-quality health care, particularly in providing care for people in underserved rural and urban areas. Improved telehealth technology and payment systems have the potential to increase access, allowing patients to obtain their care in their homes and neighborhoods. However, the ability of nurses to practice fully in these and other settings is limited by state and federal laws that prohibit them from working to the full extent of their education and training.
Conclusion 4-2: Nurses are uniquely qualified to improve the quality of health care by helping people navigate the health care system;
providing close monitoring, coordination, and follow-up across the care continuum; focusing care on the whole person; and providing care that is culturally respectful and appropriate. Through a team-based approach, nurses can partner with professionals and community members to lead and manage teams and connect clinical care, public health, and social services while building trust with communities and individuals.
REFERENCES
AAN (American Academy of Nursing). 2015. Interprofessional practice at the Vine School Health Center: A school-based nurse-managed clinic. American Academy of Nursing: Edge Runners. https://www.aannet.org/initiatives/edge-runners/profiles/edge-runners--interprofessional-practice-vine-school (accessed June 19, 2019).
AANP (American Association of Nurse Practitioners). 2020. COVID-19 state emergency response: Suspended and waived practice agreement requirements. https://www.aanp.org/advocacy/state/covid-19-state-emergency-response-temporarily-suspended-and-waived-practice-agreement-requirements (accessed April 13, 2020).
Agner, J. 2020. Moving from cultural competence to cultural humility in occupational therapy: A paradigm shift. American Journal of Occupational Therapy 74(4):7404347010.
ANA (American Nurses Association). 2015. Code of ethics for nurses with interpretive statements. Silver Spring, MD: American Nurses Association.
ANA. 2018. The nurse’s role in addressing discrimination: Protecting and promoting inclusive strategies in practice settings, policy, and advocacy. Silver Spring, MD: American Nurses Association.
ANA. 2020. Nurses, ethics and the response to the COVID–19 pandemic. Silver Spring, MD: American Nurses Association.
ANA. n.d. Care coordination and the essential role of nurses. https://www.nursingworld.org/practice-policy/health-policy/care-coordination (accessed February 21, 2020).
Bachrach, D., and J. Frohlich. 2016. Retail clinics drive new health care utilization and that is a good thing. Health Affairs 35(3). doi: 10.1377/hlthaff.2015.0995.
Bartlett, J. D., J. Griffin, and D. Thomson. 2020. Resources for supporting children’s emotional well-being during the COVID-19 pandemic. Child Trends. https://www.childtrends.org/publications/resources-for-supporting-childrens-emotional-well-being-during-the-covid-19pandemic (accessed March 23, 2021).
Basch, C. E. 2011. Healthier students are better learners: A missing link in school reforms to close the achievement gap. Journal of School Health 81(10):593–598.
Beard, K. V., and W. A. Julion. 2016. Does race still matter in nursing? The narratives of African-American nursing faculty members. Nursing Outlook 64(6):583–596.
Bodenheimer, T., and D. Mason. 2016. Registered nurses: Partners in transforming primary care. In Preparing registered nurses for enhanced roles in primary care, chaired by T. Bodenheimer and D. Mason. Conference conducted in New York, sponsored by the Josiah Macy Jr. Foundation. https://macyfoundation.org/assets/reports/publications/macy_monograph_nurses_2016_webpdf.pdf (accessed March 23, 2021).
Bodenheimer, T., L. Bauer, S. Syer, and J. N. Olayiwola. 2015. RN role reimagined: How empowering registered nurses can improve primary care. Oakland, CA: California Health Care Foundation.
Brickman, D., A. Greenway, K. Sobocinski, H. Thai, A. Turick, K. Xuereb, D. Zambardino, P. S. Barie, and S. I. Liu. 2020. Rapid critical care training of nurses in the surge response to the coronavirus pandemic. American Journal of Critical Care 29(5):e104–e107.
Campaign for Action. n.d. Issues. https://campaignforaction.org/issues (accessed November 12, 2020).
Carthon, J., M. Brooks, T. Sammarco, D. Pancir, J. Chittams, and K. W. Nicely. 2017. Growth in retail-based clinics after nurse practitioner scope of practice reform. Nursing Outlook 65(2):195–201.
Castrucci, B., and J. Auerbach. 2019. Meeting individual social needs falls short of addressing social determinants of health. Health Affairs Blog 10.
CHCS (Center for Health Care Strategies). 2007. Care management definition and framework. https://www.chcs.org/media/Care_Management_Framework.pdf (accessed January 18, 2020).
Child and Family Research Partnership. 2015. The top 5 benefits of home visiting programs. https://childandfamilyresearch.utexas.edu/top-5-benefits-home-visiting-programs (accessed February 13, 2020).
CMS (Centers for Medicare & Medicaid Services). 2012. 2012 Nursing home action plan: Action plan for further improvement of nursing home quality. Baltimore, MD: Centers for Medicare & Medicaid Services.
CMS. 2020a. Trump administration finalizes permanent expansion of medicare telehealth services and improved payment for time doctors spend with patients. https://www.cms.gov/newsroom/press-releases/trump-administration-finalizes-permanent-expansion-medicare-telehealth-services-and-improved-payment (accessed November 13, 2020).
CMS. 2020b. Trump administration issues call to action based on new data detailing COVID-19 impacts on medicare beneficiaries. https://www.cms.gov/newsroom/press-releases/trump-administration-issues-call-action-based-new-data-detailing-covid-19-impacts-medicare (accessed November 13, 2020).
Council on School Health. 2008. Role of the school nurse in providing school health services. Pediatrics 121(5):1052–1056. doi: 10.1542/peds.2008-0382.
Council on School Health. 2016. Role of the school nurse in providing school health services. Pediatrics 137(6):e20160852.
CPSTF (Community Preventive Services Task Force). 2015. Vaccination programs: Standing orders. https://www.thecommunityguide.org/findings/vaccination-programs-standing-orders (accessed September 3, 2020).
Davis, T. C., K. W. Hoover, S. Keller, and W. H. Replogle. 2020. Mississippi diabetes telehealth network: A collaborative approach to chronic care management. Telemedicine and e-Health 26(2):184–189.
Donelan, K., Y. Chang, J. Berrett-Abebe, J. Spetz, D. I. Auerbach, L. Norman, and P. I. Buerhaus. 2019. Care management for older adults: The roles of nurses, social workers, and physicians. Health Affairs 38(6):941–949.
Emanuel, E. J., E. Gudbranson, J. Van Parys, M. Gørtz, J. Helgeland, and J. Skinner. 2020. Comparing health outcomes of privileged US citizens with those of average residents of other developed countries. JAMA Internal Medicine 181(3):339–344. doi: 10.1001/jamainternmed.2020.7484.
Evans, M. K., L. Rosenbaum, D. Malina, S. Morrissey, and E. J. Rubin. 2020. Diagnosing and treating systemic racism. The New England Journal of Medicine 383:274–276.
Flinter, M., C. Hsu, D. Cromp, M. D. Ladden, and E. H. Wagner. 2017. Registered nurses in primary care: Emerging new roles and contributions to team-based care in high-performing practices. Journal of Ambulatory Care Management 40(4):287.
Foronda, C., D. L. Baptiste, M. M. Reinholdt, and K. Ousman. 2016. Cultural humility: A concept analysis. Journal of Transcultural Nursing 27(3):210–217.
Foster, S., M. Rollefson, T. Doksum, D. Noonan, G. Robinson, and J. Teich. 2005. School Mental Health Services in the United States, 2002–2003. Rockville, MD: Substance Abuse and Mental Health Services Administration.
Fraher, E., J. Spetz, and M. D. Naylor. 2015. Nursing in a transformed health care system: New roles, new rules. Philadelphia, PA: Leonard Davis Institute of Health Economics, University of Pennsylvania.
Fraher, E. P., P. Pittman, B. K. Frogner, J. Spetz, J. Moore, A. J. Beck, D. Armstrong, and P. I. Buerhaus. 2020. Ensuring and sustaining a pandemic workforce. New England Journal of Medicine 382(23):2181–2183.
Freed, M., J. Cubanski, T. Neuman, J. Kates, and J. Michaud. 2020. What share of people who have died of COVID-19 are 65 and older—and how does it vary by state? https://www.kff.org/coronavirus-covid-19/issue-brief/what-share-of-people-who-have-died-of-covid-19-are-65-and-older-and-how-does-it-vary-by-state/?utm_campaign=KFF-2020-Coronavirus&utm_medium=email&_hsmi=2&_hsenc=p2ANqtz-_U7Q7mXfWllySGkBOyS9wZp2ff8zbbx ZycmAlJ0dVoHaHEJEriXDh5kBTFf6WHimqSHlyPNoqoaQnTdJu0fjLVEkmSPg&utm_content=2&utm_source=hs_email (accessed October 5, 2020).
Gaur, K. C., M. Sobhani, and L. A. Saxon. 2019. Retail healthcare update: Disrupting traditional care by focusing on patient needs. The Journal of mHealth. https://thejournalofmhealth.com/retail-healthcare-update-disrupting-traditional-care-by-focusing-on-patient-needs (accessed April 20, 2021).
Gerchow, L., L. R. Burka, S. Miner, and A. Squires. 2021. Language barriers between nurses and patients: A scoping review. Patient Education and Counseling 104(3):534–553.
Ghorob, A., and T. Bodenheimer. 2012. Share the care™: Building teams in primary care practices. Journal of the American Board of Family Medicine 25(2):143–145.
Godoy, M. 2020 (June 22). Black Medicare patients with COVID-19 nearly 4 times as likely to end up in hospital. National Public Radio. https://www.npr.org/sections/health-shots/2020/06/22/881886733/black-medicare-patients-with-covid-19-nearly-4-times-as-likely-to-end-up-in-hosp (accessed March 25, 2021).
Goodell, S., T. Bodenheimer, and R. Berry-Millett. 2009. Care management of patients with complex health care needs. Princeton, NJ: Robert Wood Johnson Foundation.
Hall, W. J., M. V. Chapman, K. M. Lee, Y. M. Merino, T. W. Thomas, B. K. Payneand, and T. Coyne-Beasley. 2015. Implicit racial/ethnic bias among health care professionals and its influence on health care outcomes: A systematic review. American Journal of Public Health 105(12):e60–e76.
Henderson, K., T. C. Davis, M. Smith, and M. King. 2014. Nurse practitioners in telehealth: Bridging the gaps in healthcare delivery. Journal for Nurse Practitioners 10(10):845–850.
HHS (U.S. Department of Health and Human Services). n.d. National Culturally and Linguistically Appropriate Services Standards. https://thinkculturalhealth.hhs.gov/clas/standards (accessed October 7, 2020).
Hirschman, K. B., E. Shaid, K. McCauley, M. V. Pauly, and M. D. Naylor. 2015. Continuity of care: The transitional care model. Online Journal of Issues in Nursing 20(3).
Hochman, O. 2017. Patient-centered care in healthcare and its implementation in nursing. International Journal of Caring Sciences 10(1):596.
Hollander, J. E., and B. G. Carr. 2020. Virtually perfect? Telemedicine for COVID-19. New England Journal of Medicine 382:1679–1681. doi: 10,1056/NEJMp2003539.
Holmes, B. W., M. Allison, R. Ancona, E. Attisha, N. Beers, C. De Pinto, and T. Young. 2016. Role of the school nurse in providing school health services. Pediatrics 137(6):e20160852.
Hood, C. M., K. P. Gennuso, G. R. Swain, and B. B. Catlin. 2016. County health rankings: Relationships between determinant factors and health outcomes. American Journal of Preventive Medicine 50(2):129–135.
HRSA (Health Resources and Services Administration). 2017. School-based health centers. https://www.hrsa.gov/our-stories/school-health-centers/index.html (accessed October 5, 2020).
IOM (Institute of Medicine). 1990. Medicare: A strategy for quality assurance. Vol. I. Washington, DC: National Academy Press.
IOM. 2001. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
IOM. 2011. The future of nursing: Leading change, advancing health. Washington, DC: The National Academies Press.
Johnson, K. 2017. Healthy and ready to learn: School nurses improve equity and access. Online Journal of Issues in Nursing 22(3).
Kataoka, S. H., L. Zhang, and K. B. Wells. 2005. Unmet need for mental health care among US children: Variation by ethnicity and insurance status. American Journal of Psychiatry 159(9):1548–1555.
Kim, S. K., and M. Park. 2017. Effectiveness of person-centered care on people with dementia: A systematic review and meta-analysis. Clinical Interventions in Aging 12:381.
Kitzman, H., D. L. Olds, C. R. Henderson, Jr., C. Hanks, R. Cole, R. Tatelbaum, K. M. McConnochie, K. Sidora, D. W. Luckey, D. Shaver, K. Engelhardt, D. James, and K. Barnard. 1997. Effect of prenatal and infancy home visitation by nurses on pregnancy outcomes, childhood injuries, and repeated childbearing. A randomized controlled trial. JAMA 278(8):644–652.
Kogan, A. C., K. Wilber, and L. Mosqueda. 2016. Person-centered care for older adults with chronic conditions and functional impairment: A systematic literature review. Journal of the American Geriatrics Society 64(1):e1–e7.
Koschmann, K. S., N. K. Jeffers, and O. Heidari. 2020. “I can’t breathe”: A call for antiracist nursing practice. Nursing Outlook 68(5):P539–P541.
Ladden, M. D., T. Bodenheimer, N. W. Fishman, M. Flinter, C. Hsu, M. Parchman, and E. H. Wagner. 2013. The emerging primary care workforce: Preliminary observations from the primary care team: learning from effective ambulatory practices project. Academic Medicine 88(12):1830–1834.
LaFave, S. 2020 (May 13). Nurses are leading the COVID-19 response around the globe: Patricia Davidson discusses how the pandemic is highlighting work that nurses do during crisis situations and beyond. Johns Hopkins Hub. https://hub.jhu.edu/2020/05/13/patricia-davidson-nursing-covid-19 (accessed November 12, 2020).
Lamb, G., R. Newhouse, C. Beverly, D. Toney, S. Cropley, C. Weaver, E. Kurtzman, D. Zazworsky, M. Rantz, B. Zierler, M. Naylor, S. Reinhard, C. Sullivan, K. Czubaruk, M. Weston, M. Dailey, C. Peterson, and Task Force Members. 2015. Policy agenda for nurse-led care coordination. Nursing Outlook 63(4):521–530. doi: 10.106/j.outlook.2015.06.003.
Leeb, R. T., R. H. Bitsko, L. Radhakrishnan, P. Martinez, R. Njai, and K. M. Holland. 2020. Mental health–related emergency department visits among children aged <18 years during the COVID-19 pandemic—United States, January 1–October 17, 2020. https://www.cdc.gov/mmwr/volumes/69/wr/mm6945a3.htm (accessed December 3, 2020).
Leiter, M. P., and H. K. S. Laschinger. 2006. Relationships of work and practice environment to professional burnout: Testing a causal model. Nursing Research 55(2):137–146.
Levine, D. M., K. Ouchi, B. Blanchfield, A. Saenz, K. Burke, M. Paz, K. Diamond, C. Put, and J. L. Schnipper. 2020. Hospital-level care at home for acutely ill adults: A randomized controlled trial. Annals of Internal Medicine 172(2):77–85.
Lineberry, M. J., and M. J. Ickes. 2015. The role and impact of nurses in American elementary schools: A systematic review of the research. The Journal of School Nursing 31(1):22–33.
Lipson, S. K., A. Kern, D. Eisenberg, and A. M. Breland-Noble. 2018. Mental health disparities among college students of color. Journal of Adolescent Health 63(3):348–356.
Loan, L. A., T. A. Parnell, J. F. Stichler, D. K. Boyle, P. Allen, C. A. VanFosson, and A. J. Barton. 2018. Call for action: Nurses must play a critical role to enhance health literacy. Nursing Outlook 66(1):97–100.
Love, H. E., J. Schlitt, S. Soleimanpour, N. Panchal, and C. Behr. 2019. Twenty years of school-based health care growth and expansion. Health Affairs 38(5):755–764.
Maughan, E. D. 2018. School nurses: An investment in student achievement. Phi Delta Kappan 99(7):8–14.
McDonald, K. M., V. Sundaram, D. M. Bravata, R. Lewis, N. Lin, S. A. Kraft, and D. K. Owens. 2007. Closing the quality gap: A critical analysis of quality improvement strategies. In AHRQ Technical Reviews and Summaries. Vol. 7: Care Coordination. Rockville, MD: Agency for Healthcare Research and Quality.
Michalopoulos, C., S. S. Crowne, X. A. Portilla, H. Lee, J. H. Filene, A. Duggan, and V. Knox. 2019. A summary of results from the MIHOPE and MIHOPE-strong start studies of evidence-based home visiting. Washington, DC: Office of Planning, Research, and Evaluation, Administration for Children and Families, U.S. Department of Health and Human Services.
Miller, T. R. 2015. Projected outcomes of nurse-family partnership home visitation during 1996–2013, USA. Prevention Science 16(6):765–777.
Mojtabai R., and M. Olfson. 2020. National trends in mental health care for US adolescents. JAMA Psychiatry 77(7):703–714.
NACHC (National Association of Community Health Centers). 2019. Community health center chartbook. http://www.nachc.org/wp-content/uploads/2019/01/Community-Health-Center-Chartbook-FINAL-1.28.19.pdf (accessed March 21, 2020).
Narayan, M. C. 2019. CE: Addressing implicit bias in nursing: A review. American Journal of Nursing 119(7):36–43.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press.
NASEM. 2019. Vibrant and healthy kids: Aligning science, practice, and policy to advance health equity. Washington, DC: The National Academies Press.
NASN (National Association of School Nurses). 2020a. School nurse workload: Staffing for safe care. https://www.nasn.org/advocacy/professional-practice-documents/position-statements/ps-workload (accessed April 15, 2019).
NASN. 2020b. NASN calls for 10,000 more school nurses. https://schoolnursenet.nasn.org/nasn/blogs/nasn-profile/2020/04/22/nasn-calls-for-10000-more-school-nurses (accessed March 26, 2021).
Naylor, M. D., D. Brooten, R. Campbell, B. S. Jacobsen, M. D. Mezey, M. V. Pauly, and J. S. Schwartz. 1999. Comprehensive discharge planning and home follow-up of hospitalized elders: A randomized clinical trial. Journal of the American Medical Association 281(7):613–620.
Naylor, M. D., D. A. Brooten, R. L. Campbell, G. Maislin, K. M. McCauley, and J. S. Schwartz. 2004. Transitional care of older adults hospitalized with heart failure: A randomized, controlled trial. Journal of the American Geriatrics Society 52(5):675–684.
Naylor, M. D., K. B. Hirschman, A. L. Hanlon, K. H. Bowles, C. Bradway, K. M. McCauley, and M. V. Pauly. 2014. Comparison of evidence-based interventions on outcomes of hospitalized, cognitively impaired older adults. Journal of Comparative Effectiveness Research 3(3):245–257.
NQF (National Quality Forum). 2020. The care we need: Driving better health outcomes for people and communities. https://thecareweneed.org/wp-content/uploads/2020/08/Full-Report-The-Care-We-Need-Update-Aug-2020.pdf (accessed November 12, 2020).
ODPHP (Office of Disease Prevention and Health Promotion). 2020. Discrimination. Healthy People 2020. https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-health/interventions-resources/discrimination (accessed April 13, 2020).
Olds, D. L., H. Kitzman, E. Anson, J. A. Smith, M. D. Knudtson, T. Miller, R. Cole, C. Hopfer, and G. Conti. 2019. Prenatal and infancy nurse home visiting effects on mothers: 18-year follow-up of a randomized trial. Pediatrics 144(6):e20183889.
OPRE (Office of Planning, Research and Evaluation). 2020. Home visiting evidence of effectiveness review: Brief—December 2020. Washington, DC: U.S. Department of Health and Human Services.
Patrick, S. W., L. E. Henkhaus, J. S. Zickafoose, K. Lovell, A. Halvorson, S. Loch, M. Letterie, and M. M. Davis. 2020. Well-being of parents and children during the COVID-19 pandemic: A national survey. Pediatrics 146(4):e2020016824.
Peikes, D. N., R. J. Reid, T. J. Day, D. D. F. Cornwell, S. B. Dale, R. J. Baron, R. S. Brown, and R. J. Shapiro. 2014. Staffing patterns of primary care practices in the comprehensive primary care initiative. The Annals of Family Medicine 12(2):142–149.
Pelzang, R. 2010. Time to learn: Understanding patient-centered care. British Journal of Nursing 19(14):912–917.
Pirhonen, L., E. H. Olofsson, A. Fors, I. Ekman, and K. Bolin. 2017. Effects of person-centered care on health outcomes—A randomized controlled trial in patients with acute coronary syndrome. Health Policy 121(2):169–179.
Pittman, P. 2019. Rising to the challenge: Re-embracing the Wald model of nursing. The American Journal of Nursing 119(7):46–52.
Prins, M. A., P. F. Verhaak, M. Smolders, M. G. Laurant, K. Van Der Meer, P. Spreeuwenberg, and J. M. Bensing. 2010. Patient factors associated with guideline-concordant treatment of anxiety and depression in primary care. Journal of General Internal Medicine 25(7):648–655.
RAND Corporation. 2016. The evolving role of retail clinics. Santa Monica, CA: RAND Corporation.
Remington, P. L., B. B. Catlin, and K. P. Gennuso. 2015. The county health rankings: Rationale and methods. Population Health Metrics 13(1):11.
RHI (Rural Health Information Hub). 2019. Health-e-Schools. https://www.ruralhealthinfo.org/project-examples/806 (accessed August 17, 2020).
Roth, M. 2018. 3 ways telehealth tackles aging-related needs. https://www.healthleadersmedia.com/innovation/3-ways-telehealth-tackles-aging-related-needs (accessed December 3, 2020).
Santana, M. J., K. Manalili, R. J. Jolley, S. Zelinsky, H. Quan, and M. Lu. 2018. How to practice person-centered care: A conceptual framework. Health Expectations 21(2):429–440.
SBHA (School Based Health Alliance). 2018. 2016-17 national school-based health care census. https://www.sbh4all.org/wp-content/uploads/2019/05/2016-17-Census-Report-Final.pdf (accessed September 3, 2020).
SBHA. n.d. Core competencies. http://www.sbh4all.org/resources/core-competencies (accessed September 3, 2020).
Scherger, J. E. 2009. Future vision: Is family medicine ready for patient-directed care. Family Medicine 41(4):285–288.
Shiparski, L. A. 2005. Engaging in shared decision making: Leveraging staff and management expertise. Nurse Leader 3(1):36–41.
Singh, S., D. Roy, K. Sinha, S. Parveen, G. Sharma, and G. Joshi. 2020. Impact of COVID-19 and lockdown on mental health of children and adolescents: A narrative review with recommendations. Psychiatry Research 293:113429.
Smolowitz, J., E. Speakman, D. Wojnar, E. M. Whelan, S. Ulrich, C. Hayes, and L. Wood. 2015. Role of the registered nurse in primary health care: Meeting health care needs in the 21st century. Nursing Outlook 63(2):130–136.
Social Programs that Work. n.d. What works in social policy? https://evidencebasedprograms.org (accessed December 1, 2020).
Sofaer, S., and J. Hibbard. 2010. Best practices in public reporting No. 2: Maximizing consumer understanding of public comparative quality reports: Effective use of explanatory information. Rockville, MD: Agency for Healthcare Research and Quality.
Spetz, J., L. Trupin, T. Bates, and J. M. Coffman. 2015. Future demand for long-term care workers will be influenced by demographic and utilization changes. Health Affairs 34(6):936–945.
Storfjell, J., B. Winslow, and J. Saunders. 2017. Catalysts for change: Harnessing the power of nurses to build population health in the 21st century. Princeton, NJ: Robert Wood Johnson Foundation.
Szanton, S. L., Q.-L. Xue, B. Leff, J. Guralnik, J. L. Wolff, E. K. Tanner, C. Boyd, R. J. Thorpe, Jr., D. Bishai, and L. N. Gitlin. 2019. Effect of a biobehavioral environmental approach on disability among low-income older adults: A randomized clinical trial. JAMA Internal Medicine 179(2):204–211.
Terada, S., E. Oshima, O. Yokota, C. Ikeda, S. Nagao, N. Takeda, and Y. Uchitomi. 2013. Person-centered care and quality of life of patients with dementia in long-term care facilities. Psychiatry Research 205(1–2):103–108.
United HealthCare. 2018. United HealthCare House Calls: Together, we can help your patients achieve better health outcomes. https://www.uhcprovider.com/content/dam/provider/docs/public/health-plans/HouseCalls-Program-Overview.pdf (accessed March 23, 2021).
Uscher-Pines, L., J. Sousa, M. Jones, C. Whaley, C. Perrone, C. McCullough, and A. J. Ober. 2021. Telehealth use among safety-net organizations in California during the COVID-19 pandemic. JAMA 325(11):1106–1107.
Van Haitsma, K., S. Crespy, S. Humes, A. Elliot, A. Mihelic, C. Scott, and A. R. Heid. 2014. New toolkit to measure quality of person-centered care: Development and pilot evaluation with nursing home communities. Journal of the American Medical Directors Association 15(9):671–680.
Villarruel, A. M., and M. E. Broome. 2020. Beyond the naming: Institutional racism in nursing. Nursing Outlook 68(4):375–376.
Walker, T. 2019. Home healthcare market to expand in 2020. Managed Healthcare Executive. https://www.managedhealthcareexecutive.com/article/home-healthcare-market-expand-2020 (accessed March 26, 2020).
Willgerodt, M. A. 2018. School nursing practice in the United States: An introduction to NASN infographics. NASN School Nurse 33(4):239–243.
Yao, N., J. B. Mutter, J. D. Berry, T. Yamanaka, D. T. Mohess, and T. Cornwell. 2021. In traditional Medicare, modest growth in the home care workforce largely driven by nurse practitioners. Health Affairs 40(3):478–486.
Zamosky, L. 2013. Chronic disease: A growing challenge for PCPs. Medical Economics 90(15):30–32, 35–36.




























