The final panel of the workshop was organized to accomplish two objectives: to explore ongoing and new ideas for addressing COVID-19 in the Black community and to examine the role of Black doctors, scientists, and engineers in partnering with others to generate community response and community resilience. Moderated by Cedric Bright, M.D. (East Carolina University Medical School), the panel consisted of Scot X. Esdaile (National Board member, NAACP), Martha Dawson, C.N.P., R.N., F.A.C.H.E. (National Black Nurses Association), Gilda Barabino, Ph.D. (Olin College), and Valerie Montgomery Rice, M.D. (Morehouse School of Medicine [MSM]).
GRASSROOTS PERSPECTIVE
Mr. Esdaile chairs the NAACP National Criminal Justice Committee and the Connecticut Boxing Commission, and helps organize the Gloves Not Guns youth initiative. He said he shared his perspectives as a “grassroots guy” who engages in the community. COVID-19 has hit the Black community not only related to health, Mr. Esdaile said, but also to education, caused by the digital gap and economic issues when children cannot attend school. In Connecticut alone, more than 800,000 people have filed for unemployment so far, and many are having trouble receiving their stimulus checks and other support. People are calling the NAACP for assistance in record numbers. Many NAACP leaders themselves have been hit hard by COVID-19.
As the information about COVID-19 began going out to the community, the protests against racism also started, he observed. NAACP has placed response teams in Minneapolis, Atlanta, Louisville, and elsewhere. He also expressed concern about Black voters being able to exercise their right to cast a ballot in elections.
To the participants of the workshop, he laid out a challenge:
You are our educated and the brightest in our community. We need you. The information that you have can help us commu-
nicate in barber shops, in housing projects, in communities. We need to get your expertise to our people. They trust you—they do not trust white doctors. They need to hear from our professionals.
He offered to serve as a bridge between Black doctors, scientists, and engineers, and the wider Black community. Dr. Bright commented that Mr. Esdaile’s comments serve as a reprise about the need for community trust between the doctor and patient for compliance.
NURSING PERSPECTIVE
Nurses have been on the front line in the COVID-19 crisis, and Dr. Dawson introduced a nursing perspective to the workshop. She noted there are 3.9 million registered nurses (RNs) in the United States, about 7.8 percent of whom are African American. The Black Nurses Association represents RNs, licensed practical nurses, and nursing students and has served as the voice for African American nurses for 50 years. She noted that the theme of the organization’s 2020 conference was on resilience and that the World Health Organization has designated this year as the “International Year of the Nurse and Midwife.”1
The association has been educating members and community partners about COVID-19. Another important role is to ensure nurses have sufficient personal protective equipment (PPE) and access to testing. In some epicenters, nurses were having more exposure from patients than doctors. Data on exposure by frontline workers are needed, and testing must take place at the health facilities themselves after nurses complete or start their shifts. There have been cases of managers not allowing testing of nurses or telling them to go home (and potentially infect family members) if they test positive. There is a mental health component to these situations. As she quoted from a New York nurse:
People keep telling us that we are heroes and are on the front lines of this pandemic; that we are in a war zone. But we never send our military to battle without the right equipment…. They are asking us to go into this environment, but we don’t have what we need to survive ourselves.
___________________
1 For more information, see https://www.icn.ch/news/2020-international-year-nurse-and-midwife-catalyst-brighter-future-health-around-globe.
Another focus of the Black Nurses Association is community service, Dr. Dawson explained. It was important to have done this work before the pandemic, she said, so that community relationships and connections were already established. “No one had to ask us who we were and what we were doing,” she said. “They knew us by name and by face.” Recent activities have included making and distributing face masks, coordinating food drives, and setting up a triage system to reach older adults.
In the policy and advocacy arena, the Black Nurses Association has participated in town halls with national, state, and local officials. They have also collaborated with other nursing organizations, including the National Coalition of Ethnic Minority Nurse Associations. Early on, they worked together on a paper on COVID-19 from a nursing perspective.2
They work with many other groups, including the National Medical Association, Rainbow Coalition, National Lawyers Association, and National Council of Negro Women, among others. Dr. Dawson emphasized, “We recognize that collective voices will make the difference.” When the protests began, members organized their own peaceful protests and cared for those who were hurt or injured while protesting, often at the end of their long hospital shifts.
“Now is the time to talk about how to take care of our nurses,” Dr. Dawson said. National and regional partners have been helping with supplies, equipment, testing, and financial support, as well as virtual entertainment to provide much-needed mental health breaks. She welcomed additional partnerships to testing, supplies, and other necessities. Treatment is needed, as well as tracking and follow-up with people deemed “recovered.”
Reporting must be accurate, she stressed. When there was pressure to open the economy, she suspected the accuracy of some of those data to support the decision.
ENGINEERING PERSPECTIVE
Dr. Barabino, in providing an engineering perspective, said that COVID-19 has increased the need for engineers who are equipped to develop user-centered solutions that can address racial disparities. Their design skills, systems approach, and innovative mindset have the potential to combat the crisis in novel and impactful ways, she noted. When a disparity lens is applied, the engineering solutions are more robust and equitable.
___________________
2 See https://ncemna.org/ncemna-covid-19-positions-statement/.
Equipping engineers requires them to understand the complexities of racial disparities, as well as the public health concerns and historical context of differential medical treatment. For the past 8 years, she has led, along with Cato Laurencin, M.D., Ph.D., a national discussion involving biomedical engineering practitioners, faculty, and students that culminates in an annual symposium on engineering solutions to health disparities. The inaugural symposium in 2012 was highlighted by a keynote presentation by civil rights attorney Fred Gray; the most recent symposium featured a keynote by journalist and educator Linda Villarosa.3 During these symposia, engineers share their designs and approaches to eliminate disparities, such as screening tools and technologies that can be used in low-resource settings.
Dr. Barabino observed that Blacks and other underrepresented minorities are often drawn to fields with potential to give back to society and address health disparities. However,
the talent remains untapped, given the persistent underrepresentation of Blacks in engineering and other STEM [science, technology, engineering, and mathematics] fields. Blacks make up 5 percent of the science and engineering workforce and are largely missing among the academic leaders in science, engineering, and medicine.
In her own case, she related how she was drawn to medicine and engineering and to use engineering to solve problems in medicine. She has focused most of her research on sickle cell disease and public health concerns related to health disparities.
Collaborations between engineers and clinicians, such as clinical immersion and biodesign, allow for the identification of unmet needs and the pursuit of technical solutions to meet those needs. It can be done in training settings that range from courses co-led by engineering and medical schools to intensive short-term programs. Dr. Barabino has led a program called Coulter College, intensive 3-day programs on translation of biomedical innovations in which student teams are guided through a dynamic process to develop solutions to clinical needs, while also gaining a better understanding of resource constraints and disparities.4 Students
___________________
3 Ms. Villarosa wrote “A Terrible Price,” the April 29, 2020, New York Times Magazine article about the Zulu Club in New Orleans to which Dr. Yancy referred earlier in the workshop (see Chapter 3).
4 For more information, see https://whcf.org/coulter-foundation-programs/translational-research/coulter-college.
learn how to evaluate the best point of leverage within a clinical need, evaluate solutions, and balance clinical benefits alongside a viable commercial model. Such efforts will benefit from the expansion of a constant focus on underserved disparity populations, she commented.
Dr. Barabino also described COVID-19 work taking place within the National Academy of Engineering. A cross-generational call has been issued through the Grand Challenges Scholars Program and Frontiers of Education Communities.5 The charge is to collectively brainstorm on innovative engineering approaches to COVID-19 and its consequences. Examples include a paper-based COVID-19 test for at-home diagnostics, self-disinfecting N95 masks, wearable sensors for monitoring, and handless door openers.
To sum up, she said, engineers are poised and ready to address COVID-19. Exploiting that talent, particularly people coming out of the African American community with an eye toward elimination of disparities, can and will have lasting implications on the virus and its disproportionate toll on Blacks and African Americans.
MEDICAL SCHOOL PERSPECTIVE
Dr. Montgomery Rice shared how Morehouse School of Medicine is responding as a school, hospital, and community resource to COVID-19. She noted some of her comments would reiterate points made throughout the workshop.
First, to lay out the problem, COVID-19 itself does not discriminate, yet communities of color are disproportionately impacted. There has been no consistent collection and reporting of data, and when data are released, they are not granular enough to paint the full picture. Current COVID-19 tracking websites and data platforms are not able to drill down to the local level to reveal just how entrenched these inequities are. Looking at data from Georgia points out these gaps. For example, among whites, the data show that about the same proportion of males and females are infected, but a large number of cases are not broken out by race and sex. Looking at health-care workers, there are more African American than white cases, and females are also disproportionately affected. These data show the large numbers of vocational nurses and other workers in nursing homes and other long-term care
___________________
5 For more information, see http://www.engineeringchallenges.org/GrandChallengeScholarsProgram.aspx.
facilities who come in direct and frequent contact with patients. Especially in the early days of the pandemic, they did not have adequate access to PPE, and the impact can thus be seen.
Social Distancing
“The virus does not discriminate,” Dr. Montgomery Rice stressed. “Blacks and whites have an equal chance of being infected by a COVID19 person in close proximity. It is what happens when we get infected that results in higher rates of morbidity and mortality.” The reality behind employment and housing patterns reveal the difficulty in heeding public health guidance such as to socially distance. Specifically:
- Nearly 25 percent of employed Hispanic and Black or African American workers are employed in service industry jobs, compared with 16 percent of non-Hispanic whites.
- Hispanic workers account for 17 percent of total employment, but 53 percent of the agricultural workforce.
- Black or African American workers make up 12 percent of all employed workers, but 30 percent of licensed practical and licensed vocational nurses.
- Members of racial and ethnic minorities may be more likely to live in densely populated areas.
In terms of employment, Dr. Montgomery Rice pointed out that the risks may be greater for workers in essential industries who work outside the home, including some people who may need to continue working in these jobs because of their economic circumstances. Related to housing, as noted earlier, people in densely populated areas may find it more difficult to practice prevention measures such as social distancing.
She stressed the need for accurate data that can drill down to the county, zip code, and neighborhood levels. An example is a study in San Francisco that tested 4,160 residents in the Mission district between April 25 and 28. Sixty-two people tested positive. Of these 62 people, 95 percent of them were Latinx and 90 percent were essential workers. They were leaving to go out to work. About the same percentage had an annual income of less than $50,000 and lived in a household of at least three people.
Morehouse School of Medicine conducted a study of Georgia’s 159 counties. MSM researchers found counties with more Black residents
have higher rates of COVID-19 (Gaglioti et al., 2020). In fully adjusted models, every 1 percent increase in the proportion of the Black population in a county resulted in a 2.3 percent increase in that county’s confirmed COVID-19 confirmed case rates. No other ecologic variables (county-level poverty, uninsured rate, or population rate) were significant.
A partnership between MSM, the Google Foundation, and the CDC Foundation is directly addressing the lack of meaningful data. The partners will build a comprehensive, public-facing data platform; establish a health equity task force and data consortium to work to ensure standardization of COVD-19 data at the national, state, and local levels; and develop evidence-based practices for socioculturally responsive resources to provide technical assistance to local and state health organizations to improve their COVID-19 response. In addition, and most significantly, the day of the workshop itself, MSM announced that it received a $40 million grant from the Department of Health and Human Services Office of Minority Health to develop the National COVID-19 Resiliency Network (NCRN). The NCRN will encompass six foundational areas: (1) identify and engage communities through local, state, and national partners; (2) develop new and nurture existing partnerships; (3) create culturally and linguistically appropriate outreach to diverse communities; (4) use technology to link communities to health-care and social services; (5) monitor and evaluate for quality improvement; and (6) document and disseminate strategies and findings.
Five priority areas impacted by COVID-19 were selected for Phase 1 of the NCRN. They include a county in Georgia, with African Americans as a highly vulnerable community; three parishes in Louisiana, with African Americans and incarcerated people as the vulnerable communities; Navajo Nation, with Native Indian population; New York City, with African American, Hispanic, and Asian vulnerable populations; and a rural consortium consisting of a county in Texas with a higher number of Hispanic migrant workers and in Alaska with Alaskan Native population. The effort is built on a community-centered approach developed at MSM in 2017 entitled PETAL (Prioritize health equity, Engage the community, Target health disparities, Act on data, and Learn and improve) (see Figure 5-1).
DISCUSSION
Dr. Bright congratulated Dr. Montgomery Rice and Morehouse School of Medicine on the Office of Minority Health grant and noted that the work can serve as the kind of experiment on the impact of investment
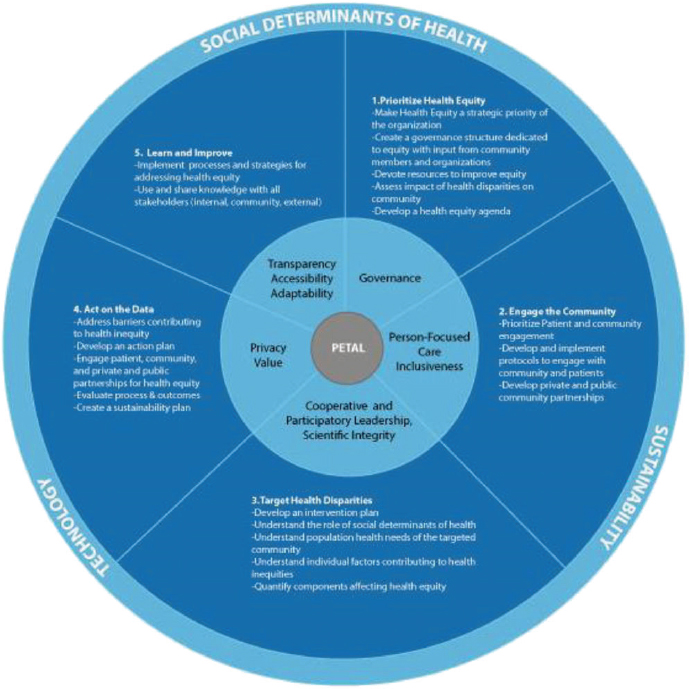
SOURCE: Brooks et al., 2017.
discussed in the previous session (see Chapter 4). He then asked the presenters for their ideas about changing the focus of the health-care system from the physician to the patient in a community. Dr. Montgomery Rice noted COVID-19 has shown that care can be delivered in many ways, such as via telehealth, which may help meet patients where they are. Dr. Barabino noted engineers are being trained to understand patient needs by talking directly with them before designing technologies. Engineers are also learning how to enhance existing tools, such as those related to imaging and communications. From a systems perspective, Dr. Dawson suggested a shift in resources so that more funding is directed to community health promotion and prevention. Currently, she said, most health-care dollars are spent
on treatment for the critically ill, and the continued lack of public health funding has complicated efforts to respond to the pandemic. Incentivizing physicians to help patients stay healthy may be one solution, she suggested. Insurance reimbursement for telemedicine began with the pandemic, but it could have been in place before this. In addition, more research support to understand the health benefits of safe water, cleaner environments, food security, and improved housing would also be important, she said. The Black Nurses Association has focused on how to provide care to people who are incarcerated, in the juvenile system, in foster care, and in other group situations. NAACP has participated in protests to raise concerns about the COVID-19 risks within prisons, Mr. Esdaile said, and has branches in many correctional facilities. He pointed to the inequality in who is being released from prisons because of the risks related to COVID-19.
A discussion about testing followed. It was acknowledged that some people have been reluctant to be tested because of fear of isolation from family or job loss if they test positive. Dr. Dawson called for more education at the community level so people understand that testing can prevent further infection to others. She also stressed the urgency to “go to bat” for essential workers, especially paraprofessionals, and open up the discussion about why they do not have sick leave or unemployment insurance. Dr. Montgomery Rice noted that the testing requirement at Morehouse School of Medicine involved communication and engagement with employees and students. The testing provided a baseline and has also served as a model on how to return to work and school.
A participant asked about universal access to broadband internet, the lack of which has emerged as a setback during COVID-19. Dr. Barabino explained the digital divide is not a technology problem, but a lack of political will. She urged a push on policy makers to create publicly owned networks to extend broadband to all communities.
Other countries, a participant noted, have provided a universal basic income for workers to stay home while they pay for their needs. Dr. Montgomery Rice noted that not all workers could be covered under such a system—hospital health-care providers, for example, have to work on site. Dr. Camara Jones related her recent experience providing congressional testimony.6 She acknowledged the statements made at the hearing that
___________________
6 Dr. Jones testified before the House Committee on Education and Labor on June 22, 2020. Her written statement can be found here: https://edlabor.house.gov/imo/media/doc/JonesCamaraPhyllisTestimony062220202.pdf.
the prepandemic unemployment rate was low, but pointed out that many people, and disproportionately people of color, worked in jobs that did not pay livable wages. She said she found disingenuous the discourse about going back to work to help people of color, rather than pursue the type of universal basic income implemented in New Zealand and some European countries to get the pandemic under control.
Dr. Montgomery Rice said a prerequisite is the belief in the universal value of everyone. That belief does not prevail in this country, which is why opportunities are segmented, she continued, but more people are recognizing this now and are interested in solutions, as evidenced by the high participation in the day’s workshop presentations and discussions. “We should not have been surprised when we started to see the differences in mortality based on race and ethnicity with COVID-19 because there aren’t many diseases that we can think of that don’t disproportionately impact Black people. But we had to spend a fair amount of time so people would recognize that it did not have to do with the fact that our skin is black, that it is actually that people could not socially distance,” Dr. Montgomery Rice said. Given this understanding, she continued, “As scientists, we need to make decisions that are evidence based. We are going to be able to provide good data to affirm the differences, but then the data has to be used to create interventions.” She invited workshop participants to request data and to create partnerships at the national, state, and local levels, recognizing that confounding factors can make each community’s situation unique. Dr. Dawson noted that income inequality must be addressed. Dr. Jones referred to an earlier comment by Dr. Marcia McNutt (see Chapter 4) that progress can widen disparities unless an equity lens is applied.
A participant asked about use of convalescent plasma as a treatment for COVID-19. The presenters said they did not have sufficient information to comment, but several clinical trials are taking place, including, according to Dr. Bright, at East Carolina University. More broadly, Dr. Montgomery Rice commented, “as we see those research studies come online, it will be important to see that persons of color are participating and not just giving the plasma. So many times we are not participating in the clinical trials, so we do not know what the impact will be in our communities and if the outcomes will be different.”
Dr. Jones asked Mr. Esdaile what workshop participants should know, based on his work with the NAACP and in the community. He replied, “You as experts need to have an understanding that the information you have is not in the neighborhoods that need it the most…. [People] are in
desperate straits to save their families and educate their children; they are scared and nervous right now.” Help is needed from trusted sources to put pertinent information into laypersons’ terms and to build bridges with young people, community activists, and others in the communities that are most vulnerable. Celebrities such as Dr. Dre have huge marketing reach, but do not have the scientific knowledge, and he suggested merging the talents and skills of rap and other artists with scientists and health-care providers to develop a comprehensive, if unconventional strategy to get into communities. Dr. Montgomery Rice said the MSM grant will undertake efforts like these. Dr. Dawson said she and other Black nurses have been talking on the radio and doing other types of community outreach. “Young people want to hear from you; they trust your expertise,” Mr. Esdaile reiterated.
Dr. Cora Marrett observed that the discussion reinforces the need for two-sided communication. “It’s not just that the community needs to hear from physicians and researchers,” she said. “We need to hear from communities about what is most effective.” The Roundtable can serve as one way to facilitate these linkages, she said.
REFERENCES
Brooks, D., M. Douglas, N. Aggarwal, S. Prabhakaran, K. Holden, and D. Mack. 2017. Developing a framework for integrating health equity into the learning health system. Learning Health Systems. DOI: 10.1002/lrh2.10029.
Gaglioti, A., M. Douglas, C. Li, P. Baltrus, M. Blount, and D. Mack. 2020. County-Level Proportion of Non-Hispanic Black Population Is Associated with Increased County Confirmed COVID-19 Case Rates after Accounting for Poverty, Insurance Status, and Population Density. White Paper. https://www.msm.edu/RSSFeedArticles/2020/May/documents/County-Level-Proportion-of-AA-Case-Rate-of-COVID19.pdf.












