5
The Role of the Community
The experiences of individuals living with dementia and their families are shaped in countless ways by the circumstances in which they live. Chapter 2 reviews the interacting forces that influence individuals’ cognitive health and the ways in which the environment shapes both risk and protective factors across the life span. This chapter looks more closely at the role of the immediate community. There are many kinds of communities; individuals and families are part of multiple overlapping communities, most of which are relevant to the experience of dementia. Traditions, foodways, attitudes about aging, and other attributes of families and cultural groups have important influences on health and well-being. So, too, do characteristics of the physical and built environment and other aspects of the geographic areas in which people live (neighborhoods, towns, cities). More broadly, community has been defined as “any configuration of individuals, families, and groups whose values, characteristics, interests, geography, or social relations unite them in some way,” and in general, the term refers both to places and the people who live in them (National Academies of Sciences, Engineering, and Medicine [NASEM], 2017, p. 1).
Looking specifically at the implications for dementia, communities shape the exposures and behaviors that influence dementia risk from early life through adulthood. (See Chapters 1 and 2 for discussion of how interacting experiences and factors influence cognitive health throughout life.) Community context also affects the way people interpret the meaning of the experience of having dementia or living with someone with the disease, the expectations they have of social interactions, and the availability of resources. Thus, the community is a key context in which interventions
may improve outcomes for people living with dementia and their families and caregivers. Understanding community context can provide insights into disease progression as well, and cultural traditions, challenges, and local cultural knowledge may facilitate understanding of new ways to see problems and seek answers to them.
What makes it urgent to consider dementia through a community lens is that communities in the United States vary dramatically in both the harms and opportunities their residents experience. This chapter provides an overview of the contexts that fundamentally shape health and quality of life for individuals living with dementia, including a detailed examination of disparities in community characteristics and opportunities, and how those factors can mitigate or exacerbate the challenges of dementia. It also reviews what is known about opportunities at the community level to ameliorate the challenges for individuals, families, and caregivers. The chapter closes with directions for research to improve understanding of the effects of community characteristics on residents’ cognitive health and on the experiences of those who develop dementia and their caregivers.
First, to bring to life the profound influence of place and community on people living with dementia and their caregivers, Box 5-1 presents a personal reflection. Each individual story and commentary the committee heard reflected unique circumstances but also widely shared experiences and reactions, and challenges that affect people across the country. While our focus was on research and policy responses to reduce the negative impacts of dementia on individuals and families, experiences in our own circles of family and friends touched by these diseases were another source of insight. Box 5-1 is the account of how one committee member’s caregiving experience has been affected by the community context in which her father lives.
DISPARITIES THAT AFFECT THE IMPACT OF DEMENTIA
Communities in the United States vary across multiple dimensions: size; geography and climate; rural, suburban, or urban character; demographic makeup; comparative wealth; cultural perspective; and much more. Some of the differences reflect historical realities that have introduced and sustained profound inequities and injustices. As noted by the authors of a 2017 National Academies’ report, such community conditions as concentrated poverty, low housing values, and low high school graduation rates not only reflect the nation’s history of structural racism and economic injustice but also are closely linked to poorer health outcomes and poorer conditions for health (NASEM, 2017). In many regions, current conditions reflect the lasting legacy of slavery; the forced relocation of Indigenous groups and other minorities; segregation laws; and other discriminatory events, policies, and
laws. These legacies from the past, along with more recent developments, such as “redlining” of neighborhoods to discourage investment in places where people of color lived, resulted in the displacement of vulnerable populations and the fragmentation of their communities (see, e.g., Fullilove and Wallace, 2011). These issues are well documented elsewhere but are a critical backdrop for understanding how the impacts of dementia vary from place to place in the United States (e.g., Riley, 2018; Bailey et al., 2017; NASEM, 2017; Lewis et al., 2020; Jervis et al., 2018). This section looks first at how the characteristics of disadvantaged communities may influence cognitive health and then at the amplifying impact of racism on such effects.
Links Between Community Characteristics and Cognitive Health
Research on the disparities in health outcomes associated with this history has established links between structural inequities evident at the community level and such basic indicators of population health as infant mortality and life expectancy, as well as diseases that are part of the pathway to dementia (e.g., stroke and diabetes) (see Chapter 2 for more information) (Goins et al., 2021; Lewis et al., 2020; Jervis et al., 2018). These inequities include such factors as poor housing conditions, higher levels of chronic stress and trauma, limited neighborhood cohesion, and segregation (NASEM, 2017). Other research has linked factors that have been associated with dementia risk, such as educational attainment; adult stress; cardiovascular health; and exposure to air pollution; and community characteristics including poverty, crime rate, social cohesion, rurality, and quality of transportation networks (Leventhal and Brooks-Gunn, 2000; Hill et al., 2005; Lawrence et al., 2017; Nieuwenhuijsen, 2018).
Research has shown the relevance of community context for health across the life course. For example, work on children’s development has shown how interactions among complex neurobiological processes and characteristics of the physical and social environment shape the health and even the brains of developing children from before they are born. Indeed, these factors also affect reproductive health and thus the development of
young people’s future offspring (NASEM, 2019a). Maternal stress, nutrition, environmental toxins, prenatal care, and other factors have all been linked to neurocognitive development, particularly the development of language, executive function, and memory (Sherman, 2014).
Researchers have also looked closely at specific community populations to understand how risks and protections function. For example, studies of Mexican American communities have yielded insights about how being a part of such a community can be protective: one longitudinal study, for example, showed that older people who lived in neighborhoods with greater percentages of Mexican American residents had lower rates of cognitive decline (Sheffield and Peek, 2009). Epidemiologists have documented health benefits of social support and cultural preservation among older Mexican Americans in the Southwest, and even suggested that the benefits of social resources could outweigh the harms of socioeconomic disadvantage (Eschbach et al., 2004). Other work has suggested that the social capital benefits of being part of a community (e.g., networks of family and friends) foster resilience that can buffer stresses experienced among immigrant groups in the United States (Alegría et al., 2017). Protections against cross-group tensions and the influence of collective action to improve community conditions have been identified as possible sources of resilience.
More generally, there is evidence that larger social networks and greater levels of social support are associated with improved overall cognition (Kelly et al., 2017). Emotional social support has been associated with lower incidence of cognitive impairment and improved functioning (Yin et al., 2020; Ellwardt et al., 2013).
Nevertheless, the interactive effects of neighborhood characteristics are not fully understood. For example, family support has been strongly associated with self-rated mental health, but the relationship among neighborhood social cohesion and resources, language, and other sociodemographic factors and cognitive health merits further study (National Latino and Asian American Study;1Mulvaney-Day et al., 2007). Moreover, segregated neighborhoods also have the potential to isolate individuals from broader community resources, and promote alienation and social stagnation. Research is needed to determine their role in the cognitive health of immigrants and racial/ethnic minority groups in the United States (Alegría et al., 2017).
Little research has directly explored how major features of communities influence the development of dementia, the experience of living with dementia, and its impact on caregivers. The work that is available points to associations between disparities in the prevalence of dementia and such measures of neighborhood disadvantage as income and education level,
___________________
1https://www.massgeneral.org/mongan-institute/centers/dru/research/past/nlaas
housing quality, and employment (Powell et al., 2020). Some research on environmental stressors and exposures illustrates the specific connections among social stratification (by race and ethnicity, gender, socioeconomic status, and rural/urban residence), community stressors and assets, and dementia outcomes (Guo et al., 2019; Wu et al., 2015a, 2015b).
Community stressors potentially place people at greater risk of poor cognitive function and dementia through a variety of mechanisms. The dementia experience (overall quality of life and rate of progression of disease) may be influenced by, for example, how easy it is for individuals to engage in physical activity in the community or to avoid isolation and develop and maintain strong social relationships. Community conditions may also add to caregivers’ stress or affect their well-being if, for example, the challenge of providing care is exacerbated by physical distance from or inadequacy of resources and supports.
The mechanisms involved may be physical. For instance, people living in highly segregated neighborhoods are more likely to be exposed to pollutants that exceed thresholds for neurotoxicity and can cause neurodegeneration, thus directly or indirectly influencing diseases that are part of the pathway to dementia. Air pollution is one example. The presence of outdoor particulate air pollutants is associated with higher levels of cognitive impairment in cross-sectional studies and with faster rates of cognitive decline in longitudinal studies. Some recent evidence also documents that community stressors may heighten the negative consequences of particulate air pollutants for dementia risk (Ailshire et al., 2017; Ailshire and Clarke, 2015; Ailshire and Crimmins, 2014; Cacciottolo et al., 2017; Clifford et al., 2016; Power et al., 2016). Both outdoor and indoor particulate air pollutants (perhaps resulting from, e.g., heating/cooking fires) may increase the risk of dementia or influence its symptoms and progression (Saenz et al., 2018; Caldwell et al., 2019; Choi and Matz-Costa, 2018; Dong and Bergren, 2017; Gobbens and van Assen, 2018). Such stressors have been found to have disproportionate effects for racial/ethnic minorities, groups of lower socioeconomic status, and rural residents, although research findings on these disparities are sparse and mixed (Millar, 2020; Rote et al., 2017).
Crime, noise, and neighborhood disorder also affect communities’ quality of life, residents’ sense of community, and a variety of physical and psychological outcomes (Caldwell et al., 2019; Choi and Matz-Costa, 2018; Dong and Bergren, 2017; Gobbens and van Assen, 2018). Although little research links these aspects of community directly to dementia risk, quality of life for individuals living with dementia, and impacts on caregivers, an abundance of research documents the associations between these neighborhood attributes and self-reported health, frailty, physical health conditions, perceived stress, and emotional well-being (depression, anxiety) (Diez Roux
et al., 2016; Cagney et al., 2005; Rodrigues et al., 2021). For example, chronic exposure to community noise in diverse urban environments has been linked to poor cognitive performance, dementia, and Alzheimer’s disease (Weuve et al., 2020). Poor communities have greater exposure to damaging noise as well (Agrawal et al., 2008).
The Role of Race and Ethnicity
The above factors may harm the health of residents of any disadvantaged community, urban or rural, in any region. When they intersect with racial/ethnic disparities and structural or direct racism, the effects can be even more detrimental. Many people of color reside in poor communities, independent of their own income level, and residential segregation by race has been historically persistent in many regions of the United States. Black, Latinx, and Native American people are disproportionately likely to live in high-poverty census tracks in the United States. These realities affect health in a number of ways (Williams and Collins, 2001; Solomon et al., 2019; Bailey et al., 2017). Segregated neighborhoods tend to have more limited health care facilities and supermarkets relative to other neighborhoods, for example. They also have fewer parks and green spaces compared with White neighborhoods, which limits opportunities for exercise and socializing (Nardone et al., 2021; South et al., 2015).
Because of residential segregation, people of color are also more likely to be exposed to such environmental hazards as air pollution (Woo et al., 2019; Bravo et al., 2016) and noise pollution (Casey et al., 2017), as well as environmental stressors such as violence (Levy et al., 2020). As noted above, there is reason to believe that these stressors have disproportionate effects on racial/ethnic minorities, among other groups.
Chapter 2 reviews the large body of evidence of connections between educational attainment and cognitive health, and it has long been understood that significant disparities in educational attainment are linked to social and economic disadvantage (see, e.g., Duncan and Murnane, 2011; Gamoran, 2001; Garcia et al., 2018). For numerous reasons, particularly the way public education is funded in the United States, students in disadvantaged and highly segregated communities have historically had more limited educational opportunities relative to their peers in other communities, and these disparities continue to translate to differences in educational attainment and other outcomes. Looking at the association with dementia risk, a 2020 study showed that Black people who had not completed high school had the greatest lifetime burden of dementia because they experienced earlier onset of symptoms (Farina et al., 2020). Evidence that decreasing dementia prevalence may be associated with increases in educational attainment overall supports this connection (Wu et al., 2017; Downer et
al., 2019; Hayward et al., 2021). In addition, a recent study showed that between 2000 and 2014, the prevalence of dementia in the United States decreased across racial/ethnic groups, but especially among non-Hispanic Black adults aged 65–74, and that improvements in educational attainment likely contributed to this outcome (Hayward et al., 2021).
Finally, some researchers have explored the effects of poverty and discrimination experienced by members of minority groups on dementia risk and progression (Williams and Earl, 2007; Zuckerman et al., 2008). A hypothesis is that racial and economic stressors in individuals’ communities may lead to depressed mood or physiological changes that in turn may increase the risk or severity of dementia (Barnes et al., 2012; Zahodne et al., 2017). The relationship between experiences of discrimination and the development of dementia is an area that deserves further study (Barnes and Bennett, 2014).
There has also been little research directly linking community-level efforts with reductions in dementia-related disparities. There is reason to hope that programs designed to reduce disparities in the social determinants of health may also reduce disparities in dementia through their influence on health behaviors that have been associated with reduced dementia risk, such as eating a healthy diet, engaging in physical exercise, having social connections, and limiting exposure to tobacco and excess alcohol (see Chapter 2). More fundamental approaches to breaking down disparities and barriers, such as increasing the minimum wage, ensuring universal access to health care, and implementing food and housing security programs, could be expected to have benefits for cognitive health (NASEM, 2019b). These important issues are beyond the scope of this report, but research to explore such links will be valuable.
LOOKING THROUGH A COMMUNITY LENS
As discussed in Chapters 2 and 3, cognitive health is influenced throughout the life course by many factors that confer protection or risk, many of which are modifiable. Chapter 2 examines the connections between specific risk factors, such as smoking, cardiovascular health, and social factors (e.g., education and income level), and disparities in cognitive health across population groups. The resources a community affords and the stressors it imposes likely influence not only people’s health before they experience cognitive decline but also the experiences they and their caregivers have after diagnosis. As discussed above, these effects are a key reason for stark disparities in dementia prevalence and outcomes.
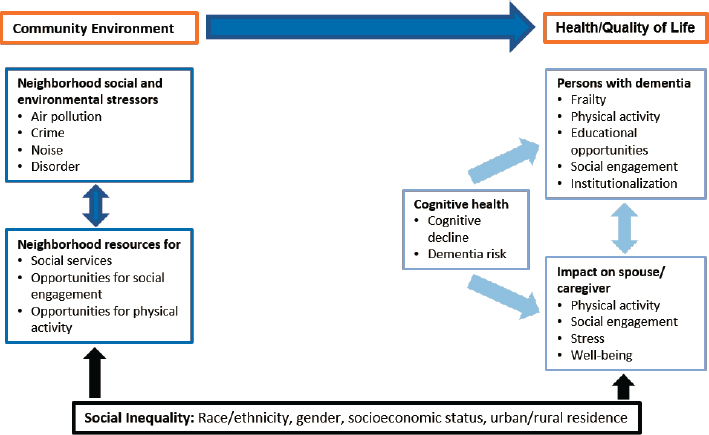
Figure 5-1 illustrates the dynamic relationship among the experiences of individuals and families and the ways in which community characteristics can influence them. The community environment depicted here includes
both conditions that affect people who are living with dementia, such as neighborhood resources, and those that may have an impact throughout the life course, such as air pollution, which may alter brain development and function early in life, conferring risk that is carried forward and may affect cognitive aging and the development of disease (Cacciottolo et al., 2017; Ailshire et al., 2017).
Figure 5-1 illustrates the connections between the community context and the cognitive health and quality of life of people living with dementia, but it is also important to understand that these connections potentially vary in important ways across different types of communities defined by race and ethnicity, socioeconomic status, and rural or urban character. As noted above, racial/ethnic segregation affect how community stressors and resources influence dementia risk and the quality of life for people living with dementia. As the personal narrative at the beginning of the chapter (Box 5-1) illustrates, resources and stressors faced by rural elderly persons living with dementia differ in significant ways from those encountered in urban areas. Communities also differ in their economic resources and how neighborhoods are potentially socioeconomically stratified, illustrating yet another way in which inequality across communities influences the connections within communities. As yet, researchers have not found clear ways to use a community lens to understand dementia experiences in the population. However, Figure 5-1 points to possible avenues that researchers could pursue to understand the structural origins of dementia.
An example of the importance of adopting a community lens in dementia research is social isolation, which is common among older adults generally and is strongly associated with dementia. As noted in Chapter 2, it is difficult to know whether social isolation is a cause of cognitive decline, an effect, or both, but it is associated with increased risk of the development of dementia and accelerated disease progression (Wilson et al., 2007; Sundström et al., 2020; Sutin et al., 2020; NASEM, 2020). Social isolation may also influence the well-being of individuals living with dementia and their caregivers (Latham and Clarke, 2016). Among individuals with dementia, greater social isolation may increase the risk for moderate and severe loneliness (Victor et al., 2020), whereas larger social networks with close friends are associated with better cognition among individuals with dementia that may mitigate the effects of loneliness (Balouch et al., 2019). In turn, social networks themselves often reflect inequalities across communities in terms of rural/urban residence, racial/ethnic segregation, and socioeconomic resources.
While the link between loneliness and dementia is not fully understood, hypotheses about the connection between lack of social interaction and loneliness and dementia include the “use it or lose it” theory, which posits that reduced use of the brain for social relationships may lead to atrophy (Hultsch et al., 1999). At the same time, dementia may exacerbate social isolation, such as when a person loses word-finding skills and other attributes that facilitate connection. Loneliness may also compromise the neural system and render individuals more susceptible to the damaging effects of cognitive decline (Wilson et al., 2007). Compared with adults without dementia, adults with dementia may experience increased difficulty dealing with feelings that arise from social isolation and loneliness (Cohen-Mansfield and Perach, 2015). Many other community factors are thought to play a role in cognitive aging and the quality of life experienced by persons living with dementia and their caregivers.
OPPORTUNITIES TO SUPPORT COMMUNITIES
Communities can play a pivotal role in reducing challenges for individuals living with dementia, families, and caregivers. They can strive to support cognitive resilience for older individuals by promoting education and intellectual stimulation earlier in life, for example (Larson, 2010). They can provide parks and recreational facilities, as well as resources that directly serve the elderly, people living with dementia, and caregivers. Overall, however, the research on how communities can improve outcomes related to dementia has not yet firmly established what approaches are most effective and how they can be implemented. This section focuses on
opportunities to build the knowledge base for improvements in this regard in the coming decade.
Cultural attitudes and values that are evident at the community level can have significant effects on the experience of living with dementia (Calia et al., 2019). It has been suggested that some cultural groups’ negative impressions of dementia can have the effect of stripping people living with the disease of their personhood and keeping them at a distance from resources that support other aging residents (Kitwood, 1998; Gaugler et al., 2019; Grenier et al., 2017). In other settings, acceptance of dementia and a tradition of engagement with declining elders are the norm. In traditional Chinese culture, for example, dementia is an accepted part of the aging process and is not necessarily viewed as requiring specialty care by non–family members (Cipriani and Borin, 2015). People in some Native American communities share this perspective, while others view dementia as a signal of death (Adamsen et al., 2021; Lewis et al., 2020; Kramer, 1996; Cipriani and Borin, 2015).
Recognizing the influences of attitudes and values, some have suggested reframing dementia not as solely a biological disease but as a process integrating biology with the influence of community and culture (Gaugler et al., 2019). This approach is consistent with the social model of disease and helps shift the focus from the limitations of the individual to the ways in which the community either supports or constricts the options of individuals and families.
This section explores some of the types of resources communities afford to individuals living with dementia and their families, issues and disparities that affect the availability of those resources, ways to build community resilience, and examples of innovative living arrangements that are attracting attention.
Types of Resources
Neighborhood resources are community supports that can allow persons with dementia to live active and engaged lives and provide help with the challenges faced by their caregivers (Ng et al., 2018; Clarke et al., 2015). As with stressors, there is evidence that such resources are associated with both the risk of dementia and disease progression. For example, a resource that provides stimulating activities and social interaction may support the maintenance of cognitive reserve that slows cognitive decline and reduces the risk of dementia or helps mitigate the effects of neurotoxicity on disease progression among persons with dementia.
As discussed above, researchers have established individual-level associations between social engagement, social isolation, and loneliness and dementia outcomes (e.g., Liang et al., 2020; Penninkilampi et al., 2018;
Saczynski et al., 2006). Substantially less research has assessed the effects of the variety of resources available in the community, such as religious institutions, adult day care centers, or residential care facilities (Clarke et al., 2015; Du Toit et al., 2019). One reason for this gap may be the lack of data that can be used to explore this issue. Investigators often fail to consider collecting information about the types and numbers of community resources available to and utilized by people living with dementia and their caregivers. This information might be collected by conducting a community needs assessment that includes some discussion with people living with dementia and their caregivers.
A study currently under way at the University of Southern California illustrates the value of this type of research (see University of Southern California, 2020). The researchers have developed a data resource for contextual information that can be linked to large population studies of individuals, such as the Health and Retirement Study or the National Aging and Health Trends Study.2 The contextual data span key community domains, including social, physical, built, and resource environments, that can be linked to communities in which study participants live. This contextual information offers new conceptually important measures that previously have not been widely considered in dementia studies. For the general category of “resources for social interaction and mental stimulation,” for example, measures of libraries, gardens and museums, churches, and community centers will allow an in-depth characterization of this community environment domain. The study is attending to the temporal and spatial scales at which contextual data are available while also developing a new data infrastructure to examine ways in which communities influence the dementia experience.
Other work has suggested the potential benefits of neighborhood access to green space as well, including association with physical activity and opportunities for social contact, that have been identified as protective of cognitive health (James et al., 2015). These are among the few domains to focus on positive attributes rather than harmful factors—an important consideration in addressing the requirements for wellness and satisfaction for those living with dementia.
Other resources include the Area Deprivation Index, a measure of socioeconomic deprivation developed by the Health Resources and Services Administration that provides useful information about urban areas but is less useful for insights about rural areas. Researchers in the United Kingdom have also initiated large-scale studies to examine this issue, with the goal of enhancing opportunities for social engagement in communities
___________________
(Swarbrick et al., 2019; Zuelsdorff et al., 2020; Kind and Buckingham, 2018).
A Patchwork of Resources and Supports
Communities across the United States have a range of structures in place to address the needs of people living with dementia and their caregivers. Among other functions, they provide information; link people to agencies and organizations that offer supports and services; and deliver care, services, and supports directly. As discussed above, communities also have features that are indirectly supportive or beneficial, such as parks, religious institutions, and other amenities in which people living with dementia can share. Studies of older adults who live alone indicate that home visitation from nurses, peer visitation to share a meal, and community e-health monitoring with telephone counseling appear to improve health outcomes so that older people can age in place (Ahn et al., 2018; McHugh Power et al., 2016; Jung and Lee, 2017).
The resources and supports provided by communities vary for many reasons. Communities differ in size, in their histories and geographic locations, in the demographic characteristics of their populations, and in many other ways. They also differ in both a political and policy sense: they are located within states and localities each with its own guidelines, regulations, laws, and resources relevant to persons with dementia and their caregivers. Funding streams from both the state and the federal government vary and reach the community in different ways. For example, a federal agency may provide block grants to states for social programs, which allow states autonomy in how to use the funds (often without accountability and guidelines). States, in turn, largely determine how to disperse the funds to their own local communities. Communities themselves vary in the level of funding they have to work with, in their approach to investing in the social and economic well-being of their populations, and in the kinds of regulations they adopt to protect vulnerable groups.
People living in rural communities face challenges and inequities that are comparable to those in urban and suburban communities but may require different responses (Warshaw, 2017). In rural areas, for example, access to resources and care may require traveling long distances and time off from work for individuals living with dementia and their caregivers. Health- and medicine-related needs in rural areas are not well addressed in general, and this has been an underresearched area of public health (NASEM, 2021; Bolin et al., 2015). Researchers have noted that medical care tends to be oriented toward large population centers for economic reasons, and efforts to improve the structure and delivery of care tend to focus on those areas as well (a phenomenon that has been called “structural
urbanism” [Probst, 2019]). Nevertheless, older adults living in rural areas have assets and opportunities that can be leveraged in prevention, detection, and care for dementia. For instance, among many Indigenous peoples of America, cultural and traditional teachings and practices passed on by elders can build resilience for communities, and social engagement with family and community has been associated with reduced risk of cognitive decline, as noted above (Alzheimer’s Association and Centers for Disease Control and Prevention, 2019).
These issues have not been well studied, but one example of an effort to address the challenges in rural areas is the collocation of health care training programs with residential facilities for older adults, which has facilitated multigenerational learning and exchange (NASEM, 2021). Another is use of mobile respite services to increase access to care in rural areas, which has been tried in Australia (Alzheimer’s Australia, 2007).
There are many ways in which support can be provided at the local level to individuals living with dementia and their caregivers. These include providing resources for physical activity (e.g., parks, recreational centers) and for social interaction and mental stimulation (e.g., libraries, museums, dementia-related choral groups), as well as the institutions that provide health care, long-term care in the home or in a facility, and hospice and palliative care (discussed in Chapter 6).
Supplementary resources are difficult to categorize, and the sorts of support they provide overlap. In general, however, such resources provide support for everyday tasks, such as grocery shopping and transportation, and offer adult day care/respite care and other kinds of emotional support and information. It is important to note that funding for community-based programs both varies across communities and fluctuates within communities. Some resources are without cost to residents who have access to them, but others have costs that can be substantial. Thus, many are more accessible to people with higher incomes and levels of education. Moreover, the COVID-19 pandemic has altered the way many of these entities function, with major implications for people nationwide. For example, beginning early in the pandemic, most community-based services were no longer provided in person. Disruption due to the pandemic aside, however, sources of support include the following:
- Religious institutions. Many churches, synagogues, mosques, and other religious institutions organize activities for individuals living with dementia and support groups for caregivers.
- Local agencies that offer or coordinate services for the elderly and provide such functions as checking in on seniors, home assessments, meal services and food delivery, and ride service. These may be agencies of a city, county, or other jurisdiction or private
- nonprofit entities designated by local government to provide these services, often coordinating the use of state or federally funded efforts to support the elderly. A key national resource for communities is the network of Area Agencies on Aging (Administration for Community Living, 2021). The Administration on Aging has also developed a consumer-oriented website to assist people who need services.3
- Senior centers and adult day care centers. Approximately 10,000 senior centers in the United States provide meal and nutrition programs; health, fitness, and wellness programs; transportation; day care programs; and other services. They typically rely on multiple funding sources, including government funds and funds raised by volunteers and donated by businesses (National Council on Aging, 2015).
- Private agencies. For families that can afford their services, geriatric care managers and social workers who are either affiliated with nonprofit organizations or in private practice provide supports that include regular visits with individuals living with dementia; coordination of medical care, other services, and paid caregivers; drivers experienced with elderly clients or those with dementia; and counseling and information for family members struggling with the challenges of being a caregiver.
- Support groups. Examples include local Alzheimer’s Association chapters and local Alzheimer’s agencies, which provide such resources as in-person peer mentoring support groups and 24/7 helplines.
- Structured living arrangements. Such arrangements are designed to meet the needs of people living with dementia, either alone or with family caregivers, who do not need or wish to live in a long-term care facility. In some of these arrangements, people live in alternative housing, while in others they remain in their homes but with neighborhood community structures filling gaps. Such arrangements include naturally occurring retirement community supportive service programs (NORC programs), village and green house models, and dementia friendly communities (Greenfield et al., 2012; Graham et al., 2017; Lin, 2017).
As noted earlier, limited research has thus far been conducted on community resources for people living with dementia and their caregivers, nor has there been any systematic collection of data about the nature of and methods for evaluating programs that deliver such supports. Evaluation is
___________________
costly, and where funding is tight, as it is for many community resources, evaluation may seem like a luxury. However, data collection and research to identify the features that make some of these approaches effective, particularly such purposeful innovations as dementia friendly communities, is both essential and lacking (Buckner et al., 2018, 2019; Phillipson et al., 2019).
Building Community Responsiveness and Resilience
To advance beyond the current patchwork of community resources described above, it is important to consider what constitutes a responsive and resilient community that can support people living with dementia in remaining safely at home for as long as possible. One key attribute of such a community is a robust formal network of agencies that provide both medical and social services, such as visiting nurse associations, home care companies, elderly housing, meal distribution programs, and day care and senior centers. Such a community also typically has a network of volunteer groups advocating for the elderly with government authorities. When these two sets of actors join to advocate for government funding and set the agenda for local nonprofit foundations, the conditions for a resilient community exist. When only fee-for-service agencies are present, they may collaborate but in a limited fashion, each focused on its own organizational survival, not necessarily on supporting the agenda of the elderly population in general.
Other entities make important contributions to responsive and resilient communities. Community foundations, for example, fund nonprofit agencies, community initiatives, and other efforts, some of which focus specifically on aging. Foundations can provide leadership to social service delivery agencies and advocacy groups, and potentially galvanize community volunteers, political leaders, and media attention. Many religious organizations are centers for social engagement and volunteerism that have impact beyond their own membership and are important resources in disadvantaged neighborhoods and for racial/ethnic minority groups, but little is known about how such groups support people living with dementia and their caregivers. Local businesses have traditionally been another source of funding and other support. However, corporate consolidations have had an impact on business leaders’ involvement with local issues.
Unfortunately, there is fairly scant research on the function of communities with respect to the needs of aging populations, and research on the nonprofit sector rarely focuses on issues associated with aging. Systematic attention to this issue is needed using community-level data about nonprofit entities, interagency interaction, and related topics. Research examining community-based agencies for the elderly and the relationship between what agencies offer and population outcomes is sorely needed;
such research can be supported by linking data about community agencies to Medicare data.
The conduct of such research is hampered, however, by the lack of well-developed conceptual models for how community supports can be beneficial, and an infrastructure for testing hypotheses about the observable relationships between interlinked agencies and community resilience and the outcomes experienced by persons living with dementia. There are community-based programs in operation throughout the country, and it is likely that many, if not most, are providing meaningful supports, but few are well documented and rigorously evaluated. As more data become available and greater attention is focused on these issues, it will be possible to learn more about what differentiates communities that are and are not able to implement multifaceted programs to help frail and isolated subgroups of the population. At present, there is no single social science discipline in which these issues are a recognized focus, so a multidisciplinary, team-based approach would likely be best for this research.
Housing for People Living with Dementia
The majority of people with dementia live in the community, either with others (57%) or on their own (24%). The remainder live in residential care settings, such as assisted living (6%) and nursing homes (13%) (Lepore et al., 2017). But the need for residential care rises as the disease progresses and will grow as the population ages. In a recent nationally representative survey of people aged 60–72, 42 percent said that if they had dementia, they would want to live in a place where they could get help with daily activities and health care. Another 14 percent desired a place where they could get help with daily activities. The remaining 46 percent said they would choose to live in a community-based setting (LeadingAge, 2019).
There is reason for clear concern that people with dementia living at home in the community have substantial unmet needs for care and services, but documentation of these needs and to what extent they are met is scarce. Those who live at home are at higher risk for falls, unmanaged behavioral symptoms, pain, sleep disturbances, and environmental challenges (Gitlin et al., 2014). However, the evidence on the use of home- and community-based services by people with dementia is scant. In addition, there are few reliable measures of the quality of these supports.
Approximately 4.7 million very low-income older adults meet the eligibility requirements for affordable housing, although only about a third of them receive such assistance (Joint Center for Housing Studies of Harvard University, 2019). Waiting lists average 2 to 3 years but may be as long as 10 years. As a result, once older individuals obtain a subsidized unit, they remain there as long as possible. However, services available to
these residents tend to be limited, despite evidence that combining services with housing can enable people to remain in the community longer, thus supporting their preferences while also avoiding more costly care settings (Sanders et al., 2015).
At the national level, the BOLD Infrastructure for Alzheimer’s Act, passed into law in 2018, is a valuable new resource for localities. This act charged the Centers for Disease Control and Prevention (CDC) with three broad goals: establishing public health centers of excellence in addressing Alzheimer’s disease and related dementias, providing funds to support public health departments, and improving data collection and reporting and analysis of data.4 Together with other CDC initiatives designed to promote healthy aging, this act was designed to strengthen the support infrastructure throughout the country. States have begun receiving grants under the act, although further congressional approval will be needed to fully fund the provisions of the law.5
Researchers and local service providers (e.g., Area Agencies on Aging) in the United States and in other countries have devised numerous creative innovations at the community level to serve the needs of people living with dementia and their caregivers. Such efforts have targeted, for example, expanded access to long-term care, training in best practices for interacting with people living with dementia, collaborations to facilitate aging in place, and the provision of transportation. The committee could not systematically survey such innovations but explored several that show promise, recognizing that most are at present accessible primarily in communities with ample resources. While there is some research on these and similar efforts, more systematic evaluation of their functioning and impacts, their implementation challenges, and obstacles to their availability in low-income communities is needed.
Dementia Friendly Communities
Many governmental and advocacy groups are developing initiatives that fall under the umbrella of “dementia friendly communities.” Such communities foster understanding of people living with dementia and focus on the assets they bring to the community and ways of engaging them and their caregivers in decisions about care and other issues (Alzheimer’s Association, 2016; see also Alzheimer’s Association, n.d.). They generally offer education and training for varied members of the community and may also include respite care and other services for family caregivers.
___________________
4https://www.cdc.gov/aging/bold/index.html for more information
Figure 5-2 illustrates one approach to the design of a dementia friendly community.
In the United States, Minnesota was an early adopter of this approach. Its program, ACT on Alzheimer’s, became a national model. The White House Conference on Aging in 2015 promoted the development of other, similar initiatives, resulting in the creation of Dementia Friendly America, a “national network of communities, organizations and individuals seeking to ensure that communities across the United States are equipped to support people living with dementia and their caregivers” (Dementia Friendly America, 2021).
The World Dementia Council and the World Health Organization (WHO) are collaborating on a number of initiatives related to dementia friendly communities, many of which are developed by advocates in collaboration with local government. Typical of such interventions is the Dementia Friends program, which has included more than 15 million participants spread across nearly a fifth of all nations. While there is some evidence of participant satisfaction, the nature and duration of any impacts from these programs have not been systematically studied. At the 2019 Tokyo Dementia Summit, WHO announced a new dementia friendly
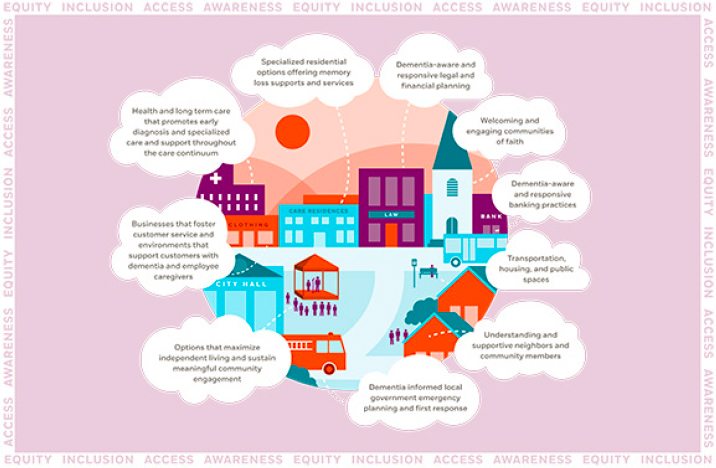
SOURCE: Dementia Friendly America (2021). Reprinted with permission of the Dementia Friendly America initiative at the National Association of Area Agencies on Aging.
toolkit, intended to provide practical tools for planning and implementing dementia-inclusive communities; it is currently being field tested (World Dementia Council, 2019). However, efforts such as the development of this toolkit have been focused largely on the needs of wealthy countries experiencing high levels of population aging rather than the needs of disadvantaged communities.
Research is needed to better understand the essential characteristics of effective dementia friendly communities and their possible effects on such outcomes as quality of life, caregiver stress, and disease progression, as well as possible problems, such as cost and inequitable access. It will also be important to document the interorganizational and social infrastructure and community leadership required to implement the dementia friendly community approach successfully in diverse communities.
Caregiver Support: Washington State
Washington State has developed a multifaceted Family Caregiver Support Program (FCSP) that aims to expand access to long-term care supports and services for state residents. Of the caregivers served, 53 percent are caring for individuals with Alzheimer’s disease or dementia (Office of the Assistant Secretary for Planning and Evaluation, 2019). FCSP uses an evidence-based screening tool, the Tailored Caregiver Assessment and Referral System, to assess the needs of family caregivers and determine the types and levels of care they and their care recipients need. Those who complete the assessment are eligible for baseline FCSP services, and caregivers whose scores indicate a higher level of need are granted access to additional supports and services.
The state legislature has increased funding for FCSP, allowing it to lower eligibility thresholds and increase the number of caregivers receiving additional services, which in turn has reduced reliance on Medicaid long-term care services (Witten, 2019). Eligible state workers can also receive payroll deductions to cover the cost of such services as home-delivered meals, adaptive equipment, and training for family caregivers; the value of the benefit can be as high as $36,500 annually.
Aging in Place Challenge Program: Canada
Canada’s National Research Council has developed a model for long-term care, the Aging in Place Challenge Program, designed to reduce costs to the Canadian government and shift the focus of nursing homes to those with the highest need. The developers hope to decrease the number of older adults who require nursing home care across Canada by 20 percent by
2031. The program aims to improve the quality of life for older adults and their caregivers and involves collaboration among academic, not-for-profit, and industrial partners.
The Village Movement: Beacon Hill, Boston, Massachusetts
Beacon Hill Village, located in the Beacon Hill district of Boston, is a self-governing community of adults 50 and older who work together to support independence and aging in place. Founded in 1999, Beacon Hill Village was a pioneer in the village movement, in which neighbors collaborate to empower seniors to live in their communities. There are now more than 300 villages; a number of governments, including those of Washington, DC, and New York State, have promoted village movements locally to encourage this volunteer-supported approach to aging in place (Capital Region Collaborative, 2021). Such villages provide programs, activities, and opportunities for community engagement to encourage active, healthy lives as residents grow older.
Researchers studying the movement have reported some positive results, including feelings of improved confidence and perceptions of support among residents helped by a village; reduced likelihood of institutionalization; and the perception that membership in a village was altruistic and had social benefits (Graham et al., 2016; Wurm and Benyamini, 2014; Robertson et al., 2016; Dunkle et al., 2019). Study of a California example of the village approach showed that participants were more likely to remain in their homes and were better able to take care of their homes and themselves (Graham et al., 2017). However, a limitation of these studies is that the vast majority of participants in the village model have been White, wealthy, educated, and female. More research is needed to examine how this model can be transferred to more diverse communities and how effective it is for individuals with advancing dementia.
RESEARCH DIRECTIONS
There is strong evidence that community factors shape the exposures and behaviors that influence dementia risk and the availability of resources for people living with dementia. This evidence reinforces the point that dementia is not just a biological disease but one that reflects the interactions among biological processes and social and cultural influences that occur across the life span. Researchers have not yet fully documented many of the most important direct impacts of community on dementia or produced clear evidence about interventions to counter negative influences
on cognitive health at the community level. At the same time, community supports are providing key resources, and innovative approaches to the design of communities in which people living with dementia can thrive show promise. However, limited evidence documents outcomes for these approaches and identifies their essential components, and their application to diverse contexts and populations has yet to be systematically demonstrated.
The committee identified high-priority research needs for building understanding of the effects of community characteristics on the experiences of people living with dementia and the ways in which communities can support these individuals and their caregivers. These research needs fall into four areas, summarized in Conclusion 5-1; Table 5-1 lists detailed research needs in each of these areas.
CONCLUSION 5-1: Research in four areas is needed to facilitate the development of communities that are well equipped to support people living with dementia and their caregivers and families, allowing those with dementia to live independently for as long as possible and mitigating the negative effects of past and current socioeconomic and environmental stressors:
- Systematic analysis of the characteristics of communities that influence the risk of developing dementia and the experience of living with the disease, with particular attention to the sources of disparities in dementia incidence and disease trajectory.
- Collection of data to document the opportunities and resources available in communities both historically and currently and evaluation of their impact, with particular attention to disparities in population groups’ access to resources and including development of the infrastructure needed for data collection.
- Analysis of the community characteristics needed to foster dementia friendly environments, including assessment of alternative community models that foster dementia friendly environments in communities that have different constellations of resources and serve diverse populations.
- Evaluation of innovative approaches to adapting housing, services, and supports so that persons with dementia can remain in the community and out of institutional care.
TABLE 5-1 Detailed Research Needs
| 1: Community Characteristics That Affect Dementia Risk |
|
| 2: Opportunities and Resources |
|
| 3: Characteristics of Dementia Friendly Communities |
|
|
|
| 4: Innovative Approaches |
|
REFERENCES
Adamsen, C., Manson, S.M., and Jiang, L. (2021). The association of cultural participation and social engagement with self-reported memory problems among American Indian and Alaska elders. Journal of Aging Health, 33(7–8_suppl), 60S–67S. https://doi.org/10.1177/08982643211014971
Administration for Community Living. (2021). Area Agencies on Aging. https://acl.gov/programs/aging-and-disability-networks/area-agencies-aging
Agrawal, Y., Platz, E.A., and Niparko, J.K. (2008). Prevalence of hearing loss and differences by demographic characteristics among U.S. adults: Data from the National Health and Nutrition Examination Survey, 1999-2004. Archives of Internal Medicine, 168(14), 1522–1530. https://doi.org/10.1001/archinte.168.14.1522
Ahn, J-A., Park, J., and Kim, C-J. (2018). Effects of an individualised nutritional education and support programme on dietary habits, nutritional knowledge and nutritional status of older adults living alone. Journal of Clinical Nursing, 27, 2142–2151.
Ailshire, J.A., and Clarke, P. (2015). Fine particulate matter air pollution and cognitive function among U.S. older adults. Journals of Gerontology: Series B, 70(2), 322–328. https://doi.org/10.1093/geronb/gbu064
Ailshire, J., and Crimmins, E.M. (2014). Fine particulate matter air pollution and cognitive function among older U.S. adults. American Journal of Epidemiology, 180(4), 359–366. https://doi.org/10.1093/aje/kwu155
Ailshire, J., Karraker, A., and Clarke, P. (2017). Neighborhood social stressors, fine particulate matter air pollution, and cognitive function among older U.S. adults. Social Science and Medicine, 172, 56–63. https://doi.org/10.1016/j.socscimed.2016.11.019
Alegría, M., Álvarez, K., and DiMarzio, K. (2017). Immigration and mental health. Current Epidemiology Reports, 4(2), 145–155. https://doi.org/10.1007/s40471-017-0111-2
Alzheimer’s Association. (n.d.). Community Environments. https://www.alz.org/professionals/public-health/core-areas/community-environments
———. (2016). Public Health Spotlight: Dementia-Friendly Communities. https://www.alz.org/media/Documents/spotlight-dementia-friendly-communities.pdf
Alzheimer’s Association and Centers for Disease Control and Prevention. (2019). Healthy Brain Initiative: Road Map for Indian Country. Chicago, IL: Alzheimer’s Association. https://www.cdc.gov/aging/healthybrain/pdf/HBI-Road-Map-for-Indian-Country-508.pdf
Alzheimer’s Australia. (2007). Support Needs of People living with Dementia in Rural and Remote Australia. https://www.dementia.org.au/sites/default/files/20070200_Nat_SUB_SuppNeedsPplLivDemRurRemAus.pdf
Bailey, Z.D., Krieger, N., Agénor, M., Graves, J., Linos, N., and Bassett, M.T. (2017). Structural racism and health inequities in the USA: Evidence and interventions. Lancet, 389(10077), 1453–1463. https://doi.org/10.1016/S0140-6736(17)30569-X
Balouch, S., Rifaat, W., Chen, H.L., and Tabet, N. (2019). Social networks and loneliness in people with Alzheimer’s dementia. International Journal of Geriatric Psychiatry, 34(5). https://doi.org/10.1002/gps.5065
Barnes, L.L., and Bennett, D.A. (2014). Alzheimer’s disease in African Americans: Risk factors and challenges for the future. Health Affairs, 33(4), 580–586.
Barnes, L.L., Lewis, T.T., Begeny, C.T., Yu, L., Bennett, D.A., and Wilson, R.S. (2012). Perceived discrimination and cognition in older African Americans. Journal of the International Neuropsychological Society, 18, 856–865.
Bolin, J.N., Bellamy, G.R., Ferdinand, A.O., Vuong, A.M., Kash, BA., Schulze, A., and Helduser, J.W. (2015). Rural healthy people 2020: New decade, same challenges. Journal of Rural Health, 31(3), 326–333. https://doi.org/10.1111/jrh.12116
Bravo, M.A., Anthopolos, R., Bell, M.L., and Miranda, M.L. (2016). Racial isolation and exposure to airborne particulate matter and ozone in understudied U.S. populations: Environmental justice applications of downscaled numerical model output. Environment International, 92–93, 247–255. https://doi.org/10.1016/j.envint.2016.04.008
Buckner, S., Mattocks, C., Rimmer, M., and Lafortune, L. (2018). An evaluation tool for age-friendly and dementia friendly communities. Working With Older People, 22(1). https://www.emerald.com/insight/content/doi/10.1108/WWOP-11-2017-0032/full/html
Buckner, S., Darlington, N., Woodward, M., Buswell, M., Mathie, E., Arthur, A., Lafortune, L., Killett, A., Mayrhofer, A., Thurman, J., and Goodman, C. (2019). Dementia friendly communities in England: A scoping study. International Journal of Geriatric Psychiatry, 34(5), 1235–1243. https://doi.org/10.1002/gps.5123
Cacciottolo, M., Wang, X., Driscoll, I., Woodward, N., Saffari, A., Reyes, J., Serre, M.L., Vizuete, W., Sioutas, C., Morgan, T.E., Gatz, M., Chui, H.C., Shumaker, S.A., Resnick, S.M., Espeland, M.A., Finch, C.E., and Chen, J.C. (2017). Particulate air pollutants, APOE alleles and their contributions to cognitive impairment in older women and to amyloidogenesis in experimental models. Translational Psychiatry, 7(1), e1022. https://doi.org/10.1038/tp.2016.280
Cagney, K.A., Browning, C.R., and Wen, M. (2005). Racial disparities in self-rated health at older ages: What difference does the neighborhood make? The Journals of Gerontology: Series B, 60(4), S181–S190. https://doi.org/10.1093/geronb/60.4.s181
Caldwell, J.T., Lee, H., and Cagney, K.A. (2019). Disablement in context: Neighborhood characteristics and their association with frailty onset among older adults. Journals of Gerontology: Series B, 74(7), e40–e49. https://doi.org/10.1093/geronb/gbx123
Calia, C., Johnson, H., and Cristea, M. (2019). Cross-cultural representations of dementia: An exploratory study. Journal of Global Health, 9(1), 011001. https://doi.org/10.7189/jogh.09.01101
Capital Region Collaborative. (2021). The Village Movement. https://crvillages.org/villages/the-village-movement
Casey, J.A., Morello-Frosch, R., Mennitt, D.J., Fristrup, K., Ogburn, E.L., and James, P. (2017). Race/ethnicity, socioeconomic status, residential segregation, and spatial variation in noise exposure in the contiguous United States. Environmental Health Perspectives, 125(7), 077017. https://doi.org/10.1289/EHP898
Choi, Y.J., and Matz-Costa, C. (2018). Perceived neighborhood safety, social cohesion, and psychological health of older adults. Gerontologist, 58(1), 196–206. https://doi.org/10.1093/geront/gnw187
Cipriani, G., and Borin, G. (2015). Understanding dementia in the sociocultural context: A review. International Journal of Social Psychiatry, 61(2), 198–204. https://doi.org/10.1177/0020764014560357
Clarke, P.J., Weuve, J., Barnes, L., Evans, D., and de Leon, C.M. (2015). Cognitive decline and the neighborhood environment. Annals of Epidemiology, 25(11), 849–854.
Clifford, A., Lang, L., Chen, R., Anstey, K.J., and Seaton, A. (2016). Exposure to air pollution and cognitive functioning across the life course—A systematic literature review. Environmental Research, 147, 383–398. https://doi.org/10.1016/j.envres.2016.01.018
Cohen-Mansfield, J., and Perach, R. (2015). Interventions for alleviating loneliness among older persons: A critical review. American Journal of Health Promotion, 29(3), e109–e125.
Dementia Friendly America. (2021). What is DFA?. https://www.dfamerica.org/what-is-dfa
Diez Roux, A.V., Mujahid, M.S., Hirsch, J.A., Moore, K., and Moore, L.V. (2016). The impact of neighborhoods on CV risk. Global Heart, 11(3), 353–363. https://doi.org/10.1016/j.gheart.2016.08.002
Dong, X., and Bergren, S. (2017). The associations and correlations between self-reported health and neighborhood cohesion and disorder in a community-dwelling U.S. Chinese population. Gerontologist, 57(4), 679–697. https://doi.org/10.1093/geront/gnw050
Downer, B., Garcia, M.A., Raji, M., and Markides, K.S. (2019). Cohort differences in cognitive impairment and cognitive decline among Mexican-Americans aged 75 years or older. American Journal of Epidemiology, 188(1), 119–129. https://doi.org/10.1093/aje/kwy196
Du Toit, S., Shen, X., and McGrath, M. (2019). Meaningful engagement and person-centered residential dementia care: A critical interpretive synthesis. Scandinavian Journal of Occupational Therapy, 26(5), 343–355. https://doi.org/10.1080/11038128.2018.1441323
Duncan, G.J., and Murnane, R.J., Eds. (2011). Whither Opportunity? Rising Inequality, Schools, and Children’s Life Chances. New York: Russell Sage Foundation.
Dunkle, R., Harlow-Rosentraub, K., Pacce, G., and Coppard, L. (2019). Joining and remaining: Factors that contribute to membership in a village. Innovation in Aging, 3(Suppl 1), S277–S278. https://doi.org/10.1093/geroni/igz038.1028
Ellwardt, L., Aartsen, M., Deeg, D., and Steverink, N. (2013). Does loneliness mediate the relation between social support and cognitive functioning in later life? Social Science & Medicine, 98, 116–124. https://doi.org/10.1016/j.socscimed.2013.09.002
Eschbach, K., Ostir, G.V., Patel, K.V., Markides, K.S., and Goodwin, J.S. (2004). Neighborhood context and mortality among older Mexican Americans: Is there a barrio advantage? American Journal of Public Health, 94(10), 1807–1812. https://doi.org/10.2105/ajph.94.10.1807
Farina, M.P., Hayward, M.D., Kim, J.K., and Crimmins, E.M. (2020). Racial and educational disparities in dementia and dementia-free life expectancy. Journals of Gerontology: Series B, 75(7), e105–e112.
Fullilove, M.T., and Wallace, R. (2011). Serial forced displacement in American cities, 1916–2010. Journal of Urban Health, 88(3). https://doi.org/10.1007/s11524-011-9585-2
Gamoran, A. (2001). American schooling and educational inequality: A forecast for the 21st century. Sociology of Education (Extra Issue: Current of Thought: Sociology of Education at the Dawn of the 21st Century), 74, 135–153. https://doi.org/10.2307/2673258
Garcia, M.A., Saenz, J., Downer, B., and Wong, R. (2018). The role of education in the association between race/ethnicity/nativity, cognitive impairment, and dementia among older adults in the United States. Demographic Research, 38, 155–168. https://doi.org/10.4054/DemRes.2018.38.6
Gaugler, J.E., Bain, L.J., Mitchell, L., Finlay, J., Fazio, S., Jutkowitz, E., Banerjee, S., Butrum, K., Gaugler, J., Gitlin, L., Hodgson, N., Kallmyer, B., Le Meyer, O., Logsdon, R., Maslow, K., and Zimmerman, S. (2019). Reconsidering frameworks of Alzheimer’s dementia when assessing psychosocial outcomes. Alzheimer’s and Dementia: Translational Research and Clinical Interventions, 5, 388–397. https://doi.org/10.1016/j.trci.2019.02.008
Gitlin, L., Hodgson, N., Piersol, C.V., Hess, E., and Hauck, W. (2014). Correlates of quality of life for individuals with dementia living at home: The role of home environment, caregiver, and patient-related characteristics. American Journal of Geriatric Psychiatry, 22(6), 587–597. https://doi.org/10.1016/j.jagp.2012.11.005
Gobbens, R.J.J., and van Assen, M.A.L.M. (2018). Associations of environmental factors with quality of life in older adults. Gerontologist, 58(1), 101–110. https://doi.org/10.1093/geront/gnx051
Goins, R.T., Winchester, B., Jiang, L., Grau, L., Reid, M., Corrada, M., Manson, S.M., and O’Connell, J. (2021). Cardiometabolic conditions and all-cause dementia among American Indians and Alaska Native peoples. Journal of Gerontology: Series A. https://doi.org/10.1093/gerona/glab097
Graham, C., Scharlach, A.E., and Kurtovich, E. (2016). Do villages promote aging in place? Results of a longitudinal study. Journal of Applied Gerontology, 37(3), 310–331. https://doi.org/10.1177/0733464816672046
Graham, C.L., Scharlach, A.E., and Stark, B. (2017). Impact of the village model: Results of a national survey. Journal of Gerontological Social Work, 60(5), 335–354. https://doi.org/10.1080/01634372.2017.1330299
Greenfield, E.A., Scharlach, A., Lehning, A., and Davitt, J. (2012). A conceptual framework for examining the promise of the NORC program and village models to promote aging in place. Journal of Aging Studies, 26(3), 273–284.
Grenier, A., Lloyd, L., and Phillipson, C. (2017). Precarity in late life: Rethinking dementia as a ‘frailed’ old age. Sociology of Health & Illness, 39(2), 318–330. https://doi.org/10.1111/1467-9566.12476
Guo, Y., Chan, C.H., Chang, Q., Liu, T., and Yip, P. (2019). Neighborhood environment and cognitive function in older adults: A multilevel analysis in Hong Kong. Health & Place, 58, 102146. https://doi.org/10.1016/j.healthplace.2019.102146
Hayward, M.D., Farina, M.P., Zhang, Y.S., Kim, J.K., and Crimmins, E.M. (2021). The importance of improving educational attainment for dementia prevalence trends from 2000–2014, among older non-Hispanic Black and White Americans. Journals of Gerontology: Series B. https://doi.org/10.1093/geronb/gbab015
Hill, T.D., Ross, C.E., and Angel, R.J. (2005). Neighborhood disorder, psychophysiological distress, and health. Journal of Health and Social Behavior, 46(2), 170–186. https://doi.org/10.1177/002214650504600204
Hultsch, D.F., Hertzog, C., Small, B.J., and Dixon, R.A. (1999). Use it or lose it: Engaged lifestyle as a buffer of cognitive decline in aging? Psychology and Aging, 14(2), 245–263.
James, P., Banay, R.F., Hart, J.E., and Laden, F. (2015). A review of the health benefits of greenness. Current Epidemiology Reports, 2(2), 131–142. https://doi.org/10.1007/s40471-015-0043-7
Jervis, L.L., Cullum, C.M, Cox, D., and Manson, S.M. (2018). Dementia assessment in American Indians. In G. Yeo, L.A. Gerdner, and D. Gallagher-Thompson (Eds.), Ethnicity and the Dementias, 3rd edition (pp. 108–123). New York: Routledge.
Joint Center for Housing Studies of Harvard University. (2019). Housing America’s Older Adults 2019. https://www.jchs.harvard.edu/sites/default/files/reports/files/Harvard_JCHS_Housing_Americas_Older_Adults_2019.pdf
Jung, H., and Lee, J-E. (2017). The impact of community-based eHealth self-management intervention among elderly living alone with hypertension. Journal of Telemedicine and Telecare, 23, 167–173.
Kelly, M.E., Duff, H., Kelly, S., McHugh Power, J.E., Brennan, S., Lawlor, B.A., and Loughrey, D.G. (2017). The impact of social activities, social networks, social support and social relationships on the cognitive functioning of healthy older adults: A systematic review. Systematic Reviews, 6(1), 259. https://doi.org/10.1186/s13643-017-0632-2
Kind, A.J.H., and Buckingham, W.R. (2018). Making neighborhood-disadvantage metrics accessible—The neighborhood atlas. New England Journal of Medicine, 378(26), 2456–2458. https://doi.org10.1056/NEJMp1802313
Kitwood, T. (1998). Toward a theory of dementia care: Ethics and interaction. Journal of Clinical Ethics, 9, 23–34.
Kramer, B.J. (1996). Dementia and American Indian populations. In G. Yeo and D. Gallagher-Thompson (Eds.), Ethnicity and the Dementias (pp. 175–181). Washington, DC: Taylor & Francis.
Larson, E.B. (2010). Prospects for delaying the rising tide of worldwide, late-life dementias. International Journal of Geriatric Psychiatry, 22(8), 1196–1202.
Latham, K., and Clarke, P. (2016). Neighborhood disorder, perceived social cohesion, and social participation among older Americans: Findings from the National Health & Aging Trends Study. Journal of Aging and Health, 30(1). https://doi/org/10.1177/0898264316665933
Lawrence, E., Hummer, R.A., and Harris, K.M. (2017). The cardiovascular health of young adults: Disparities along the urban-rural continuum. ANNALS of the American Academy of Political and Social Science, 672(1), 257–281. https://doi.org/10.1177/0002716217711426
LeadingAge. (2019). How Do Older Baby Boomers Envision Their Quality of Life If They Need Long-Term Care Services? https://leadingage.org/sites/default/files/HOW%20DO%20OLDER%20BABY%20BOOMERS%20ENVISION_FINAL.pdf
Lepore, M., Ferrell, A., and Wiener, J. (2017). Living Arrangements of People with Alzheimer’s Disease and Related Dementias: Implications for Services and Supports. https://aspe.hhs.gov/system/files/pdf/257966/LivingArran.pdf
Leventhal, T., and Brooks-Gunn, J. (2000). The neighborhoods they live in: The effects of neighborhood residence on child and adolescent outcomes. Psychological Bulletin, 126(2), 309–337. https://doi.org/10.1037/0033-2909.126.2.309
Levy, B.L., Phillips, N.E., and Sampson, R.J. (2020). Triple disadvantage: Neighborhood networks of everyday urban mobility and violence in U.S. cities. American Sociological Review, 85(6), 925–956. https://doi.org/10.1177/0003122420972323
Lewis, J.P., Manson, S.M., Jernigan, V., and Noonan, C. (2020). “Making sense of a disease that makes no sense”: Understanding Alzheimer’s disease and related disorders among caregivers and providers in Alaska. Gerontologist, 61(3), 363–373. https://doi.org/10.1093/geront/gnaa102
Liang, J., Aranda, M.P., and Lloyd, D.A. (2020). Association between role overload and sleep disturbance among dementia caregivers: The impact of social support and social engagement. Journal of Aging and Health, 32(10), 1345–1354. https://doi.org/10.1177/0898264320926062
Lin, S.Y. (2017). “Dementia-friendly communities” and being dementia friendly in healthcare settings. Current Opinion in Psychiatry, 30(2), 145–150. https://doi.org/10.1097/YCO.0000000000000304
McHugh Power, J.E., Lee, O., Aspell, N., McCormack, E., Loftus, M., Connolly, L., Lawlor, B., and Brennan, S. (2016). RelAte: Pilot study of the effects of a mealtime intervention on social cognitive factors and energy intake among older adults living alone. British Journal of Nutrition, 116, 1573–1581.
Millar, R.J. (2020). Neighborhood cohesion, disorder, and physical function in older adults: An examination of racial/ethnic differences. Journal of Aging and Health, 32(9), 1133–1144. https://doi.org/10.1177/0898264319890944
Mulvaney-Day, N.E., Alegría, M., and Sribney, W. (2007). Social cohesion, social support, and health among Latinos in the United States. Social Science & Medicine, 64(2), 477–495. https://doi.org/10.1016/j.socscimed.2006.08.030
Nardone, A., Rudolph, K.E., Morello-Frosch, R., and Casey, J.A. (2021). Redlines and greenspace: The relationship between historical redlining and 2010 greenspace across the United States. Environmental Health Perspective, 129(1), 17006. https://doi.org/10.1289/EHP7495
NASEM (National Academies of Sciences, Engineering, and Medicine). (2017). Communities in Action: Pathways to Health Equity. Washington, DC: The National Academies Press. https://doi.org/10.17226/24624
———. (2019a). Fostering Healthy Mental, Emotional, and Behavioral Development in Children and Youth: A National Agenda. Washington, DC: The National Academies Press. https://doi.org/10.17226/25201
———. (2019b). Investing in Interventions that Address Non-Medical, Health-Related Social Needs: Proceedings of a Workshop. Washington, DC: The National Academies Press. https://doi.org/10.17226/25544
———. (2020). Social Isolation and Loneliness in Older Adults: Opportunities for the Health Care System. Washington, DC: The National Academies Press. https://doi.org/10.17226/25663
———. (2021). Population Health in Rural America: Proceedings of a Workshop. Washington, DC: The National Academies Press. https://doi.org/10.17226/25989
National Council on Aging. (2015). Get the Facts on Senior Centers. https://www.ncoa.org/article/get-the-facts-on-senior-centers#intraPageNav4
Ng, T.P., Nyunt, M., Shuvo, F.K., Eng, J.Y., Yap, K.B., Hee, L.M., Chan, S.P., and Scherer, S. (2018). The neighborhood built environment and cognitive function of older persons: Results from the Singapore Longitudinal Ageing Study. Gerontology, 64(2), 149–156. https://doi.org/10.1159/000480080
Nieuwenhuijsen, M.J. (2018). Influence of urban and transport planning and the city environment on cardiovascular disease. Nature Reviews Cardiology, 15(7), 432–438. https://doi.org/10.1038/s41569-018-0003-2
Office of the Assistant Secretary for Planning and Evaluation. (2019, October 21). Expanding Access to LTSS through Caregiver Support. https://aspe.hhs.gov/advisory-council-october-2019-meeting-presentation-expanding-access-ltss
Penninkilampi, R., Casey, A.N., Singh, M.F., and Brodaty, H. (2018). The association between social engagement, loneliness, and risk of dementia: A systematic review and meta-analysis. Journal of Alzheimer’s Disease, 66(4), 1619–1633. https://doi.org/10.3233/JAD-180439
Phillipson, L., Hall, D., Cridland, E., Fleming, R., Brennan-Horley, C., Guggisberg, N., Frost, D., and Hasan, H. (2019). Involvement of people with dementia in raising awareness and changing attitudes in a dementia friendly community pilot project. Dementia (London, England), 18(7-8), 2679–2694. https://doi.org/10.1177/1471301218754455
Powell, W.R., Buckingham, W.R., and Larson, J.L. (2020). Association of neighborhood-level disadvantage with Alzheimer Disease neuropathology. JAMA Network Open, 3(6), e207559. https://doi.org/10.1001/jamanetworkopen.2020.7559
Power, M.C., Adar, S.D., Yanosky, J.D., and Weuve, J. (2016). Exposure to air pollution as a potential contributor to cognitive function, cognitive decline, brain imaging, and dementia: A systematic review of epidemiologic research. Neurotoxicology, 56, 235–253. https://doi.org/10.1016/j.neuro.2016.06.004
Probst, J., Eberth, J.M., and Crouch, E. (2019). Structural urbanism contributes to poorer health outcomes for rural America. Health Affairs (Project Hope), 38(12), 1976–1984. https://doi.org/10.1377/hlthaff.2019.00914
Riley, A. (2018). Neighborhood disadvantage, residential segregation, and beyond—Lessons for studying structural racism and health. Journal of Racial and Ethnic Health Disparities, 5, 357–365. https://doi.org/10.1007/s40615-017-0378-5
Robertson, D., Killimannis, B., and Kenny, R. (2016). Negative perceptions of aging predict longitudinal decline in cognitive function. Psychology and Aging, 31(1), 71–81. https://doi.org/10.1037/pag0000061
Rodrigues, D.E., César, C.C., Xavier, C.C., Caiaffa, W.T., and Proietti, F.A. (2021). Exploring neighborhood socioeconomic disparity in self-rated health: A multiple mediation analysis. Preventive Medicine, 145, 106443. https://doi.org/10.1016/j.ypmed.2021.106443
Rote, S.M., Angel, J.L., and Markides, K. (2017). Neighborhood context, dementia severity, and Mexican American caregiver well-being. Journal of Aging and Health, 29(6), 1039–1055. https://doi.org/10.1177/0898264317707141
Saczynski, J.S., Pfeifer, L.A., Masaki, K., Korf, E.S., Laurin, D., White, L., and Launer, L.J. (2006). The effect of social engagement on incident dementia: The Honolulu-Asia Aging Study. American Journal of Epidemiology, 163(5), 433–440. https://doi.org/10.1093/aje/kwj061
Saenz, J.L., Wong, R., and Ailshire, J.A. (2018). Indoor air pollution and cognitive function among older Mexican adults. Journal of Epidemiology and Community Health, 72(1), 21–26. https://doi.org/10.1136/jech-2017-209704
Sanders, A., Smathers, K., Patterson, T., Stone, R., Kahn, J., Marshall, J., and Alecxih, L. (2015). Service Availability in HUD-Assisted Senior Housing: Findings from a Survey on the Availability of Onsite Services in HUD-Assisted Senior Housing. Washington, DC: LeadingAge. http://www.ltsscenter.org/resource-library/Service_Availability_in_HUD_Assisted_Senior_Housing.pdf
Sheffield, K.M., and Peek, M.K. (2009). Neighborhood context and cognitive decline in older Mexican Americans: Results from the Hispanic Established Populations for Epidemiologic Studies of the Elderly. American Journal of Epidemiology, 169(9), 1092–1101. https://doi.org/10.1093/aje/kwp005
Sherman, C. (2014). Environmental Influence on the Developing Brain: A Report from the Fifth Annual Aspen Brain Forum. Dana Foundation. https://dana.org/article/environmental-influence-on-the-developing-brain
Solomon, D., Maxwell, C., and Castro, A. (2019, August 7). Systemic Inequality: Displacement, Exclusion, and Segregation. Center for American Progress. https://www.americanprogress.org/issues/race/reports/2019/08/07/472617/systemic-inequality-displacement-exclusion-segregation
South, E.C., Kondo, M.C., Cheney, R.A., and Branas, C.C. (2015). Neighborhood blight, stress, and health: A walking trial of urban greening and ambulatory heart rate. American Journal of Public Health, 105(5), 909–913. https://doi.org/10.2105/AJPH.2014.302526
Sundström, A., Adolfsson, A.N., Nordin, M., and Adolfsson, R. (2020). Loneliness increases the risk of all-cause dementia and Alzheimer’s disease. Journals of Gerontology: Series B, 75(5), 919–926.
Sutin, A.R., Stephan, Y., Luchetti, M., and Terracciano, A. (2020). Loneliness and risk of dementia. Journals of Gerontology: Series B, 75(7), 1414–1422.
Swarbrick, C.M., Doors, O., Scottish Dementia Working Group, Educate, Davis, K., and Keady, J. (2019). Visioning change: Co-producing a model of involvement and engagement in research (innovative practice). Dementia, 18(7–8), 3165–3172. https://doi.org/10.1177/1471301216674559
University of Southern California. (2020). Contextual Data Resource for Aging Surveys. https://gero.usc.edu/cbph/cdr
Victor, C.R., Rippon, I., Nelis, S.M., Martyr, A., Litherland, R., Pickett, J., Hart, N., Henley, J., Matthews, F., Clare, L., and IDEAL programme team. (2020). Prevalence and determinants of loneliness in people living with dementia: Findings from the IDEAL programme. International Journal of Geriatric Psychiatry, 35(8), 851–858. https://doi.org/10.1002/gps.5305
Warshaw, R. (2017, October 31). Health Disparities Affect Millions in Rural U.S. Communities. Association of American Medical Colleges. https://www.aamc.org/news-insights/health-disparities-affect-millions-rural-us-communities
Weuve, J., D’Souza, J., Beck, T., Evans, D.A., Kaufman, J.D., Rajan, K.B., de Leon, C., and Adar, S.D. (2020). Long-term community noise exposure in relation to dementia, cognition, and cognitive decline in older adults. Alzheimer’s & Dementia, 17(2) 525–533. https://doi.org/10.1002/alz.12191
Williams, D.R., and Collins, C. (2001). Racial residential segregation: A fundamental cause of racial disparities in health. Public Health Reports, 116(5), 404–416. https://doi.org/10.1093/phr/116.5.404
Williams, D.R., and Earl, T.R. (2007). Commentary: Race and mental health—More questions than answers. International Journal of Epidemiology, 36, 758–760.
Wilson, R.S., Krueger, K.R., Arnold, S.E., Schneider, J.A., Kelly, J.F., Barnes, L.L., Tang, Y., and Bennett, D.A. (2007). Loneliness and risk of Alzheimer Disease. Archives of General Psychiatry, 64(2), 234–240.
Witten, D. (2019). When Medicaid in Washington State Will Pay for a Nursing Home, Assisted Living, or Home Health Care. Nolo. https://www.nolo.com/legal-encyclopedia/whenwashington-state-medicaid-will-pay-for-long-term-care.html
Woo, B., Kravitz-Wirtz, N., Sass, V., Crowder, K., Teixeira, S., and Takeuchi, D.T. (2019). Residential segregation and racial/ethnic disparities in ambient air pollution. Race and Social Problems, 11(1), 60–67. https://doi.org/10.1007/s12552-018-9254-0
World Dementia Council. (2019). Impacts of Dementia Friendly Initiatives: Presenting a Global Evidence Base for Dementia Friendly Initiatives. https://worlddementiacouncil.org/sites/default/files/2020-12/DFIs%20-%20Paper%202_V15.pdf
Wu, Y.T., Prina, A.M., and Brayne, C. (2015a). The association between community environment and cognitive function: A systematic review. Social Psychiatry and Psychiatric Epidemiology, 50(3), 351–362. https://doi.org/10.1007/s00127-014-0945-6
Wu, Y.T., Prina, A.M., Jones, A.P., Barnes, L.E., Matthews, F.E., Brayne, C., and Medical Research Council Cognitive Function and Ageing Study. (2015b). Community environment, cognitive impairment and dementia in later life: Results from the Cognitive Function and Ageing Study. Age and Ageing, 44(6), 1005–1011. https://doi.org/10.1093/ageing/afv137
Wu, Y.T., Beiser, A.S., Breteler, M.M.B., Fratiglioni, L., Helmer, C., Hendrie, H.C., Honda, H., Ikram, M.A., Langa, K., Lobo, A., Matthews, F., Ohara, T., Pérès, K., Qiu, C., Seshadri, S., Sjölund, B., Skoog, I., and Brayne, C. (2017). The changing prevalence and incidence of dementia over time—Current evidence. Nature Reviews Neurology, 13(6), 327–339. https://doi.org10.1038/nrneurol.2017.63
Wurm, S., and Benyamini, Y. (2014). Optimism buffers the detrimental effect of negative self-perceptions of ageing on physical and mental health. Journal of Psychological Health. https://doi.org/10.1080/08870446.2014.891737
Yin, S., Yang, Q., Xiong, J., Li, T., and Zhu, X. (2020). Social support and the incidence of cognitive impairment among older adults in China: Findings from the Chinese Longitudinal Healthy Longevity Survey Study. Frontiers in Psychiatry, 11, 254. https://doi.org/10.3389/fpsyt.2020.00254
Zahodne, L.B., Manly, J.J., Smith, J., Seeman, T., and Lachman, M.E. (2017). Socioeconomic, health, and psychosocial mediators of racial disparities in cognition in early, middle, and late adulthood. Psychology and Aging, 32(2), 118.
Zuckerman, I.H., Ryder, P.T., Simoni-Wastila, L., Shaffer, T., Sato, M., Zhao, L., and Stuart, B. (2008). Racial and ethnic disparities in the treatment of dementia among Medicare beneficiaries. Journals of Gerontology: Series B, 63(5), S328–S333.
Zuelsdorff, M., Larson, J.L., Hunt, J.F.V., Kim, A.J., Koscik, R.L., Buckingham, W.R., Gleason, C.E., Johnson, S.C., Asthana, S., Rissman, R.A., Bendlin, B.B., and Kind, A.J.H. (2020). The Area Deprivation Index: A novel tool for harmonizable risk assessment in Alzheimer’s disease research. Alzheimer’s & Dementia, 6(1), e12039. https://doi.org/10.1002/trc2.12039
This page intentionally left blank.


































